Abstract
We evaluated whether previous inguinal hernia repair may affect the choice of prostate carcinoma treatment in a population-based cohort. It has been suggested that previous laparoscopic inguinal hernia repair (LIHR) could limit the subsequent possibility of performing a prostatectomy. Several small studies have suggested otherwise. The study cohort included all new prostate cancer cases in Finland 1998–2015 identified through the Finnish cancer registry. Data on the treatment of prostate cancer and surgical inguinal hernia repairs in 1998–2016 was obtained from the HILMO hospital discharge registry. After linkage, the study cohort included 7206 men. Of these, 5500 had no history of inguinal hernia, 1463 had an open hernia repair, and 193 had a minimally invasive repair (LIHR). Compared to men with no history of hernia repair, those with previous hernia repairs were more likely to undergo prostatectomy over radiation therapy as the primary treatment for prostate cancer HR 1.34 (CI 95% 1.19–1.52). The association did not depend on the method of hernia repair, HR 1.58 (CI 95% 1.15–2.18), in men with previous LIHR. The increased likelihood of choosing prostatectomy over radiation therapy concerns all type prostatectomies. Previous hernia repair is not a limiting factor when choosing treatment for prostate cancer.
Similar content being viewed by others
Introduction
Inguinal hernia repair is a common surgical procedure in Western countries. It can be performed with either an open or minimally invasive approach. Synthetic mesh reinforces the inguinal canal structures by local scarring and adhesions in both techniques. In laparoscopic inguinal hernia repair (LIHR), the mesh is placed into the preperitoneal space over the internal inguinal ring and iliac vessels. Mesh can be fixed in place by sutures, glue, or tackers. Alternatively, a self-adhesive mesh can be used. Totally extraperitoneal (TEP) and Transabdominal preperitoneal (TAPP) procedures are called LIHR techniques. LIHR is used primarily in Finland on recurrent or bilateral inguinal hernias1,2,3.
Prostate cancer (Pca) is the most common cancer among men in Europe. Active surveillance (AS) is a widely accepted management strategy for men with low-risk Pca. If AS is selected, it is possible to avoid potential side effects of the Pca treatment without compromising long-term oncological outcomes4,5. Radical prostatectomy (RP) and external beam radiation therapy (EBRT) are primary curative-intent treatment methods for localized Pca. Robot-assisted laparoscopic radical prostatectomy (RALP) is the leading operative technique in Finland, as in many other countries worldwide. In addition, pelvic lymph node dissection (PLND) is performed in high- and intermediate-risk cases6.
Several case reports and studies were published in the early 2000s describing the difficulties of performing radical prostatectomy and, in some cases aborting the operation in patients with the previous LIHR7,8. The reason was severe adhesions obliterating the preperitoneal space. This spurred debate on RP’s safety and feasibility after LIHR. More recent studies have reported that RALP can be performed safely and with good oncological results after LIHR9,10,11. Recently published articles has described feasibility of simultaneous RALP and LIHR operations12,13.
Here we explore how previous inguinal hernia repair and its technique are associated with primary PCa treatment at the population level. The primary hypothesis is that patients with a history of LIHR are more often treated with EBRT.
Material and methods
Study cohort
The National Research and Development Centre for Welfare and Health administrator permitted to use the national hospital discharge registry HILMO and Finnish Cancer Registry (FCR). The study cohort was formed by linking information from these two registries.
HILMO database registers contain information on diagnoses (as ICD-10 codes) and medical procedures (coded according to Nordic Classification of Surgical Procedures) from all in- and outpatient hospital visits and treatment dates. All Finnish health care units must report information to HILMO. All inguinal hernia repairs among men during 1998–2016 in Finland were identified from HILMO. 1998 was chosen as the ICD-10 coding system was adopted in Finland then. The last year with complete data available was 2016 at the time of data collection. The procedures were identified using Nordic Classification of Surgical Procedures (NOMESCO) codes for the search (Supplementary Table 1). Further inguinal hernia cases were also identified based on ICD-10 codes K40 and K41. We also collected information on common co-morbid conditions: atrial fibrillation (I48), chronic obstructive pulmonary disease (J44), asthma (J45), kidney insufficiency (N18), diabetes (E10-E14), sleep apnea (G47.3), heart condition (I20-I21, I25, I34-I37, I42.0, I42.9, I50), stroke acute or post (I63 and I69), deteriorating brain disease (F00-F03, G30, G20), liver disease (K70-K76) and other cancers besides prostate cancer (Supplementary Table 2). These conditions were chosen as they are included in the Charlson comorbidity index, commonly used to describe the load of comorbidities14.
Finnish Cancer Registry was used to obtain information on newly diagnosed prostate cancer cases in Finland between 1998 and 2015, altogether 11,699 cases. Most cancer diagnoses in Finland are included in the FCR database, with 99% coverage15. The database contains information on the date of diagnosis, tumor extent at diagnosis, primary treatment, and date of death. Supplementary information on prostate cancer management was added from the HILMO database by searching for codes indicating radiation therapy (KE002, KE009, WF002, WF099), open prostatectomy (KEC00), or laparoscopic prostatectomy (KEC01). Robot-assisted surgery was identified by code ZXC96.
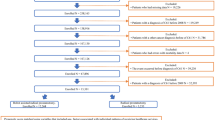
Linking the information from the registries is possible because of the unique personal social security number given to all Finnish residents. After the data linkage study population was limited to men with sufficient data and PCa managed primarily by prostatectomy or radiation therapy, 7206 men. Of these, 5550 had no history of inguinal hernia operation, 1463 had open, and 193 had laparoscopic inguinal hernia operation before PCa management (Fig. 1).
In compliance with Finnish legislation, need for ethics board approval was waived as the study was based entirely on routinely collected registry data16. Keeper of each registry that was used as the data source gave approval for the study. The study was carried out by following good clinical practice (GCP) and Declaration of Helsinki.
Data analysis
Statistical Package for Social Science for Windows, version 26.0 (SPSS), was used for all statistical analyses. P-value < 0.05 was set for statistical significance.
Ethical approval
For this type of article, informed consent is not required. When The National Research and Development Centre for Welfare and Health permitted to use the registers, they have inspected the research plan. During that process, they checked the plan to fulfill the research's ethical standards as well as the requirements of the Finnish legislation. The need for informed consent was waived as the study used routinely collected register data, which is standard practice in Finland. Tampere University Hospital research unit and the local ethics committee were informed of the permission to use the registers .The ethics committee waived their process and did not demand any actions to be taken.
Results
Population characteristics
Radical prostatectomy was equally common in men with inguinal hernia repair and those without it (69% vs. 62%, respectively). Age at diagnosis was similar among men with or without hernia repair. Comorbidities were divided equally. Subjects with a history of inguinal hernia repair often had other cancers besides prostate cancer, atrial fibrillation, diabetes, and heart disease. The open hernia group had less often localized cancer, but the number of cases with missing information was higher (Table 1).
Likelihood of radicalprostatectomy as a primary prostate cancer treatment by previous inguinal hernia repair history
Subjects with a history of inguinal hernia repair were more likely to be treated with RP rather than EBRT as the primary treatment modality HR 1.34 (CI 95% 1.19–1.52). The risk association was strongest for robot-assisted laparoscopic prostatectomy when previous hernia repair had been done using the LIHR technique; HR 9.10 (CI 95% 6.20–13.53). However, the size of this subgroup was small. RALP was more popular than EBRT after inguinal hernia repair with both open and LIHR techniques (Table 2).
Subgroup analyses
We estimated whether the method or number of previous hernia repairs would modify the likelihood of choosing radiation therapy over prostatectomy. The likelihood of prostatectomy was similar among men with a history of laparoscopic bilateral hernia repair HR 1.93 (CI 95% 1.09–3.45) and men with open bilateral inguinal hernia repair HR 2.39 (CI 95% 1.38–4.10). The number of subjects with a history of bilateral hernia was low in both open (21 EBRT and 63 RP) and laparoscopic (19 EBRT and 47 RP) repair groups (Table 3).
Among participants, who had two or multiple inguinal hernia repairs before PCa treatment, it was still more likely to have prostatectomy over EBRT HR 1.20 (CI 95% 0.90–1.62). Again, the number of subjects in this subgroup was low, with 70 cases in EBRT and 141 cases in prostatectomy groups (Table 3).
Further, we studied whether the increase in minimal-invasive techniques in inguinal hernia repair during our study period may modify the likelihood of choosing RP. Since LIHR has become more popular since 2000, the study population was stratified by PCa diagnosis date as early (1.1.1998–31.12.2006) and late (1.1.2007–31.12.2015) cases. Timing of PCa diagnosis did not significantly modify the choice of prostate carcinoma treatment among subjects with previous open hernia repair; HR 1.65 (CI 95% 1.33–2.05) in the early group versus HR 1.38 (CI 95% 1.16–1.62) in the late group. The outcome was similar among subjects with a history of laparoscopic hernia repair, although group size was small in both early and late groups (Table 4).
Discussion
Our population-based cohort study results do not support the assumption that previous hernia repair would limit surgical management of PCa. Even LIHR is not a limiting factor when choosing a treatment modality for Pca patients. Conversely, men with a history of hernia repair were more likely to be managed with prostatectomy than EBRT. It may reflect this group’s general fitness for surgical operations and positive attitudes towards procedures.
In the early 2000s, patients were warned that the LIHR technique would limit the possibility of performing a prostatectomy later. Although this may be true for open prostatectomy, most recent studies have shown that RALP could be safely performed with good oncological results after previous inguinal hernia repai9,10,11. Mini-invasive, especially robot-assisted laparoscopic prostatectomy, has become the preferred choice over the open technique. During the same period, the number of LIHR operations has risen constantly. Our subgroup analyses suggest that this trend may not affect the likelihood of undergoing prostatectomy to any significant degree. LIHR has had a very modest effect on RALP when considering operative, hospital stay, blood loss, or complications17,18,19. However, PLND is more demanding and, in some cases, impossible to perform20. Nevertheless, it does not limit choosing radical prostatectomy as the primary management. Recently studies have been published about feasibility of simultaneous RALP and LIHR. Naturally this would not aid those subjects that have had the LIHR operation done previously12,13.
Register-based studies are a good imprint of real life. Our study population is based on the entire population of Finland. Thus generalizability of our results in the general Nordic population is good. We confirmed previous results that inguinal hernia repair before prostate carcinoma does not limit later surgical treatment options.
Our study has several limitations. We did not have data on whether lymphadenectomy was performed during prostatectomy, even though we had information on cancer extent. The registries we used did not contain information on BMI. A lengthy study period means there has been a transition in surgical techniques. Furthermore, some participants may have had an inguinal hernia repair before 1998. It may have caused bias towards the null but does not limit our inference on the increased likelihood of choosing prostatectomy.
Conclusions
Our population-based cohort study confirms that open or laparoscopic inguinal hernia operation does not limit prostatectomy use for PCa management. In clinical practice it would mean that Pca treatment can be tailored according to the patient, comorbidities and cancer.
Data availability
The dataset of this study is not publicly available. However, on reasonable request, derived data supporting the findings of this study are available from the corresponding author after approval from Finnish Social and Health Data Permit Authority Findata.
References
Simons, M. P. et al. European Hernia society guidelines on the treatment of inguinal hernia in adult patients. Hernia 13, 343–403 (2009).
The Herniasurge Group et al. International guidelines for groin hernia management. Hernia 22, 1–165 (2018).
Wauschkuhn, C. A., Schwarz, J., Boekeler, U. & Bittner, R. Laparoscopic inguinal hernia repair: Gold standard in bilateral hernia repair? Results of more than 2800 patients in comparison to literature. Surg. Endosc. 24, 3026–3030 (2010).
Maggi, M. et al. The long-term risks of metastases in men on active surveillance for early stage prostate cancer. J. Urol. 204, 1222–128 (2020).
Walker, C. H., Marchetti, K. A., Singhal, U. & Morgan, T. M. Active surveillance for prostate cancer: Selection criteria, guidelines, and outcomes. World J. Urol. 40, 35–42 (2022).
von Bodman, C. et al. Predicting biochemical recurrence-free survival for patients with positive pelvic lymph nodes at radical prostatectomy. J. Urol. 184, 143–148 (2010).
Katz, E. E., Patel, R. V., Sokoloff, M. H., Vargish, T. & Brendler, C. B. Bilateral laparoscopic inguinal hernia repair can complicate subsequent radical retropubic prostatectomy. J. Urol. 167, 637–638 (2002).
Cook, H., Afzal, N. & Cornaby, A. J. Laparoscopic hernia repairs may make subsequent radical retropubic prostatectomy more hazardous. BJU Int. 7, 729 (2003).
Horovitz, D., Feng, C., Messing, E. M. & Joseph, J. V. Extraperitoneal vs. transperitoneal robot-assisted radical prostatectomy in patients with a history of prior inguinal hernia repair with mesh. J. Robot. Surg. 4, 447–454 (2017).
Do, H. M. et al. Previous laparoscopic inguinal hernia repair does not adversely affect the functional or oncological outcomes of endoscopic extraperitoneal radical prostatectomy. Urology 77, 963–967 (2011).
Haifler, M., Benjamin, B., Ghinea, R. & Avital, S. The impact of previous laparoscopic inguinal hernia repair on radical prostatectomy. J. Endourol. 11, 1458–1462 (2012).
Chiacchio, G. et al. Simultaneous inguinal hernia repair with monofilament polypropylene mesh during robot-assisted radical prostatectomy: Results from a single institute series. Medicina 5, 59050820. https://doi.org/10.3390/medicina59050820 (2023).
Rogers, T. et al. Robotic radical prostatectomy with concomitant repair of inguinal hernia: is it safe?. J. Robot. Surg. 12, 325–330 (2018).
Charlson, M. E., Pompei, P., Ales, K. L. & MacKenzie, C. R. A new method of classifying prognostic comorbidity in longitudinal studies: Development and validation. J. Chronic Dis. 40, 373–383 (1987).
Pukkala, E. et al. Nordic cancer registries–an overview of their procedures and data comparability. Acta Oncol. (Madr.) 57, 440–455 (2018).
Finnish legilation on medical research. https://www.finlex.fi/fi/laki/ajantasa/1999/19990488#L2P5a.
Al-Shareef, A. H. et al. Effects of previous hernia repair on extraperitoneal robot-assisted radical prostatectomy: A matched-pair analysis study. J. Endourol. 29, 1143–1147 (2015).
Picozzi, S. C. M. et al. Feasibility and outcomes regarding open and laparoscopic radical prostatectomy in patients with previous synthetic mesh inguinal hernia repair: Meta-analysis and systematic review of 7497 patients. World J. Urol. 33, 59–67 (2015).
Spernat, D., Sofield, D., Moon, D., Louie-Johnsun, M. & Woo, H. Implications of laparoscopic inguinal hernia repair on open, laparoscopic, and robotic radical prostatectomy. Prostate Int. 2, 8–11 (2014).
Bakker, W. J., Roos, M. M., Meijer, R. P. & Burgmans, J. P. J. Influence of previous laparo-endoscopic inguinal hernia repair on performing radical prostatectomy: A nationwide survey among urological surgeons. Surg. Endosc. 35, 2583–2591 (2021).
Funding
The funding was supported by competitive research funding of expert responsibility area of Pirkanmaa Hospital District for M. Ahtinen and TJ Murtola.
Author information
Authors and Affiliations
Contributions
M.A., J.V., and T.M. planned the study design. M.A. and T.M. analyzed the material M.A., and T.M wrote the manuscript text. J.V. gave critical comments on the text. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Ahtinen, M., Vironen, J. & Murtola, T.J. Previous inguinal hernia surgery does not limit the likelihood of choosing prostatectomy as primary prostate cancer therapy. Sci Rep 14, 9943 (2024). https://doi.org/10.1038/s41598-024-60451-6
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41598-024-60451-6
Keywords
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.