Abstract
ABO blood type has been reported as a potential factor influencing SARS-CoV-2 infection, but so far mostly in studies that involved small samples, selected population and/or used PCR test results. In contrast our study aimed to assess the association between ABO blood types and SARS-CoV-2 infection using seroprevalence data (independent of whether or not individuals had symptoms or sought for testing) in a large population-based sample. Our study included 67,340 French participants to the SAPRIS-SERO multi-cohort project. Anti-SARS-CoV-2 antibodies were detected using ELISA (targeting the proteins spike (S) and nucleocapsid (NP)) and seroneutralisation (SN) tests on dried blood spots collected in May–November 2020. Non-O individuals (and especially types A and AB) were more likely to bear anti SARS-CoV-2 antibodies (ELISA-S, 2964 positive cases: ORnon-Ovs.O = 1.09[1.01–1.17], ORAvs.O = 1.08[1.00–1.17]; ELISA-S/ELISA-NP/SN, 678 triple positive cases: ORnon-Ovs.O = 1.19 [1.02–1.39], ORAvs.O = 1.19[1.01–1.41], ORABvs.O = 1.43[1.01–2.03]). Hence, our results provided additional insights into the dynamic of SARS-CoV-2 infection, highlighting a higher susceptibility of infection for individuals of blood types A and AB and a lesser risk for blood type O.
Similar content being viewed by others
Introduction
Since 2020, the world has been struggling with the COVID-19 (Coronavirus Disease 2019) pandemic caused by the SARS-CoV-2 (Severe Acute Respiratory Syndrome Coronavirus 2). The research community has mobilized to identify potential risk factors associated with SARS-CoV-2 infection and COVID-19 severity, in an effort to better understand the dynamic of infection, pinpoint individuals at higher risk and help prevent the disease and related adverse outcomes. Early reports comparing the distribution of ABO blood types between individuals infected or not by the SARS-CoV-2, suggested that ABO blood types could be related to the risk of SARS-CoV-2 infection1,2,3,4, as previously observed for SARS-CoV5 but also for other infectious diseases6,7. These studies and others published since then8,9,10,11 suggested that individuals with blood type O had a lower risk of SARS-CoV-2 infection and that type A individuals would be more at risk, with yet some remaining inconsistencies, especially for B or AB types for which results are less robust. However, these results were obtained in selected populations (e.g., patients, blood donors) of various sample size (mostly under 15,000) and mostly using PCR test results (e.g., from questionnaires or registries) hence reflecting a population that sought for testing, with the exception of a recent report using seroprevalence data in ≈32,600 blood donors11. In contrast, this short report provides insights into the associations between ABO blood types and SARS-CoV-2 infection assessed from seroprevalence data obtained between May and November 2020 through the systematic screening for anti-SARS-CoV-2 antibodies in a large population-based sample of French adults.
Methods
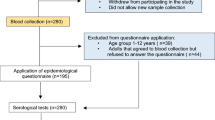
The SAPRIS (“SAnté, Perception, pratiques, Relations et Inégalités Sociales en population générale pendant la crise COVID-19”) study was set up in April 2020 to investigate various aspects of the COVID-19 crisis (COVID-19 infection/diagnosis and experience of lockdown), based on a consortium of existing French prospective cohort studies. In May 2020, participants from the Constances, E3N-E4N and NutriNet-Santé cohort studies answering SAPRIS questionnaires were also invited to take part in the SAPRIS-SERO project which aimed to estimate the seroprevalence of antibodies against SARS-CoV-2 at the population level, as previously described12,13. Briefly, between May and November 2020 (during or at the end of the first wave, pre-vaccine period), participants received self-sampling kits by mail to collect dried blood spots from which were detected anti-SARS-CoV-2 antibodies (IgG) directed against the S1 domain of the spike protein (S) and the nucleocapsid protein (NP) using ELISA (Euroimmun®, Lübeck, Germany), as well as neutralizing anti-SARS-CoV-2 antibodies (SN) using an in-house micro-neutralization assay. ELISA-S and ELISA-NP tests were considered to be positive with an optical density ratio ≥ 1.1, indeterminate between 0.8 and 1.1, and negative < 0.8. The SN test was considered to be positive with a titre ≥ 40. ELISA-NP and SN tests were performed whenever the optical density ratio for ELISA-S was ≥ 0.7. Positivity (vs. negativity) to ELISA-S test and positivity (vs. negativity) to all three ELISA-S, ELISA-NP and SN tests (associated to more symptomatic COVID-19 in a previous study in SAPRIS-SERO13) were considered as outcomes. Characteristics of the participants including ABO and RhD blood types were collected from questionnaires as part of each cohort follow-up or from the shared SAPRIS questionnaire. Associations between the seroprevalence of antibodies against SARS-CoV-2 and blood types were studied using multi-adjusted logistic regression models stratified by cohort and including the following covariates: sex (men/women), age (≥ 18– < 40, 40–49, 50–59, 60–69, ≥ 70 years old), month of blood collection, residential area during the lockdown: city size (rural, < 20,000, 20–100,000, ≥ 100,000 inhabitants) and French administrative region. Additional covariates linked to the risk of SARS-CoV-2 infection were included in sensitivity analyses: weight status, smoking status, educational level, professional activity during lockdown, socio-professional category, number of individuals at home during lockdown and alcohol intake. All tests were two-sided and P < 0.05 was considered statistically significant. Analyses were carried out using SAS 9.4 (SAS Institute Inc., USA).
Ethics approval and informed consent
The SAPRIS-SERO study (registered #NCT04392388) was conducted in accordance with the relevant guidelines and regulations and was approved by the ethics committee CPP Sud-Méditerranée III on April 27th 2020 and by the CNIL #920,193. All participants provided written or electronic informed consent for participation in each cohort and a specific electronic informed consent for participation in the SAPRIS-SERO study.
Results
Our study included 67,340 participants, among which 2964 with a positive seroprevalence of anti SARS-CoV-2 antibodies according to the ELISA-S test and 64,376 participants who tested negative (respectively 678 triple positive and 64,011 triple negative to ELISA-S, ELISA-NP and SN tests). Characteristics of participants are shown in Table 1.
Higher odds of presenting anti SARS-CoV-2 antibodies (Table 2) were observed in participants belonging to non-O blood types (ELISA-S: OR non-O vs. O = 1.09 [1.01–1.17], ELISA-S/ELISA-NP/SN: OR non-O vs. O = 1.19 [1.02–1.39]) and especially to blood type A (ELISA-S: ORA vs. O = 1.08 [1.00–1.17], ELISA-S/ELISA-NP/SN: OR A vs. O = 1.19 [1.01–1.41]) and AB (ELISA-S/ELISA-NP/SN: OR AB vs. O = 1.43 [1.01–2.03]). In analyses combining ABO and RhD blood types, higher odds were observed in participants with blood types A- (ELISA-S: OR A- vs. O+ = 1.16 [1.00–1.35]), A + (ELISA-S/ELISA-NP/SN: OR A+ vs. O+ = 1.24 [1.03–1.48]) and AB + (which represented the majority of AB participants, ELISA-S: OR AB+ vs. O+ = 1.24 [1.02–1.51], ELISA-S/ELISA-NP/SN: OR AB+ vs. O+ = 1.60 [1.11–2.30]). No association was observed comparing RhD positive and negative blood types overall.
Additional adjustments in sensitivity analyses did not change the results of increased odds of positive seroprevalence in non-O participants (ELISA-S: OR non-O vs. O = 1.09 [1.01–1.18], ELISA-S/ELISA-NP/SN: OR non-O vs. O = 1.19 [1.02–1.39]).
Discussion
In this study, we used seroprevalence data obtained from screening a large population-based sample from 3 French prospective cohorts to assess the associations between ABO blood types and the risk of SARS-CoV-2 infection. Our results showed a decreased seroprevalence of anti-SARS-CoV-2 antibodies in type O individuals compared to all others. Among non-O blood types, types A and AB were more likely positive for SARS-CoV-2 infection. No association was observed with type B or RhD types.
These results confirmed prior observations obtained in other population settings, namely a decrease risk of infection for type O individuals and an increase risk for type A individuals, with some indication of increased risk for type AB individuals as well, thus strengthening the evidence towards a differential susceptibility of SARS-CoV-2 infection according to ABO blood types. Yet, most studies so far involved registry or hospital data of SARS-CoV-2 positivity from PCR test results in patients or blood donors in comparison to the general population8,9,10 and fewer studies used seroprevalence data, mostly in small samples, with the exception of a recent report in 32,600 blood donors11. In turn, our study used seroprevalence data and a screening design whereby a large population-based sample of 67,340 participants involved in the SAPRIS-SERO project received a dried blood spot sampling kit. This allowed us to test for SARS-CoV-2 infection in a single general population, regardless whether the participants sought testing or had symptoms, allowing detecting a large panel of infected cases.
This differential susceptibility to SARS-CoV-2 infection according to blood types could be due to the incorporation of ABH antigens on the envelop of SARS-CoV-2 virions, leading to a likelihood of infection from one individual to another following ABO incompatibility9,10. As type O individuals carry both anti-A and anti-B antibodies, they would be less susceptible to primary infection by SARS-CoV-2 viruses enveloped with type A or B-like patterns such as those excreted by non-O individuals. In contrast, type A individuals, carrying anti-B antibodies, would be susceptible to infection by viruses excreted by type O and type A individuals (i.e., 42% and 44% of the French population respectively), while type AB individuals carrying neither anti-A or anti-B antibodies would be susceptible to infection by individuals of all group types, which is why type A or AB are particularly at risk for SARS-CoV-2 infection. Type B individuals carrying anti-A antibodies are susceptible to infection by viruses excreted by type O and type B individuals but type B is less represented in the French population (10%) which may explain why no significant association was observed for these individuals. Another hypothesis, yet less supported by available data relates to the entry of SARS-CoV-2 in host’s cells, that would be facilitated by antigen A9,14. Finally, non-O individuals are at higher risk of thromboembolism, a common complication of COVID-19, hence beyond infection, non-O individuals could also be at higher risk of severe cases of COVID-199,10.
Our study strengths pertained to the systematic screening for anti-SARS-CoV-2 antibodies targeting a large well-characterized sample, hence providing data from positive and negative cases within the same population, as well as the use of seroprevalence allowing the detection of cases that may or may not have symptoms or sought testing. Yet, some limitations should also be acknowledged. First, although large, our sample size may have still been limited to have sufficient power in analyses combining ABO and RhD blood types, especially for rarer blood types. Next, misclassification of individuals as ‘negative’ may have arisen from imperfect sensitivity of the ELISA-S test (85–90%, the specificity being > 95%)15,16 and from the decrease of anti-SARS-CoV-2 antibodies over time (with no detectable antibodies 4–5 months post-infection in half of participants in a recent report11). Yet, the sample collection was performed between May and November 2020, the first and second waves of the pandemic occurring in spring and fall 2020 in France, so that antibodies should still be detectable in most participants. Finally, the observational nature of the study makes it difficult to assess the extent to which participants have actually been exposed to the virus. Although lifestyle-related exposure to the virus is mostly unlikely to have been differential according to blood types, we adjusted our models on several covariates related to the spatial distribution of the epidemic since it could also relate to blood types, considering the distribution of ABO blood types in different regions or populations. However, we did not have access to racial and ethnic data as the collection of such data is generally not permitted in the framework of French cohort studies. Finally, our data only reflect infections occurring before November 2020, that is, before the emergence of variants but also before the large-scale vaccination campaigns.
To conclude, this study adds to the current body of evidence providing data on the association between ABO blood types and the risk of SARS-CoV-2 infection from screening a large sample from the general population using seroprevalence data. Our results confirmed a higher susceptibility of infection for individuals of blood types A and AB and a lesser risk for blood type O, thereby providing additional insights into the dynamic of SARS-CoV-2 infection. However, considering the magnitude of association and the current mechanistic hypotheses related to blood type incompatibility (hence a collective rather than individual type of protection), type O individuals are not without risk of infection and protective measures remain the best way of preventing SARS-CoV-2 transmission and infection.
Data availability
Data from the study are protected under the protection of health data regulation set by the French National Commission on Informatics and Liberty (Commission Nationale de l’Informatique et des Libertés, CNIL). The data can be made available upon reasonable request to the corresponding author (m.deschasaux@eren.smbh.univ-paris13.fr), after a consultation with the steering committee of the SAPRIS-SERO study. The French law forbids us to provide free access to SAPRIS-SERO data; access could however be given by the steering committee after legal verification of the use of the data. Please, feel free to come back to us should you have any additional question.
References
Zhao, J. et al. Relationship between the ABO blood group and the coronavirus disease 2019 (COVID-19) susceptibility. Clin. Infect. Dis. 73, 328–331 (2021).
Göker, H. et al. The effects of blood group types on the risk of COVID-19 infection and its clinical outcome. Turk J. Med. Sci. 50, 679–683 (2020).
Abdollahi, A., Mahmoudi-Aliabadi, M., Mehrtash, V., Jafarzadeh, B. & Salehi, M. The novel coronavirus SARS-CoV-2 vulnerability association with ABO/Rh blood types. Iran J. Pathol. 15, 156–160 (2020).
Gallian, P. et al. Lower prevalence of antibodies neutralizing SARS-CoV-2 in group O French blood donors. Antivir. Res. 181, 104880 (2020).
Cheng, Y. et al. ABO blood group and susceptibility to severe acute respiratory syndrome. JAMA 293, 1450–1451 (2005).
Lindesmith, L. et al. Human susceptibility and resistance to Norwalk virus infection. Nat. Med. 9, 548–553 (2003).
Batool, Z., Durrani, S. H. & Tariq, S. Association of ABO and Rh blood group types to hepatitis B, hepatitis C, HIV and Syphillis infection, a five year’experience in healthy blood donors in a tertiary care hospital. J Ayub. Med. Coll. Abbottabad 29, 90–92 (2017).
Banchelli, F. et al. The role of ABO blood type in patients with SARS-CoV-2 infection: A systematic review. J. Clin. Med. 11, 3029 (2022).
Pereira, E. et al. ABO blood group and link to COVID-19: A comprehensive review of the reported associations and their possible underlying mechanisms. Microb. Pathog. 169, 105658 (2022).
Pendu, J. L., Breiman, A., Rocher, J., Dion, M. & Ruvoën-Clouet, N. ABO blood types and COVID-19: Spurious, anecdotal, or truly important relationships? A reasoned review of available data. Viruses 13, 160 (2021).
Gallian, P. et al. SARS-CoV-2 IgG seroprevalence surveys in blood donors before the vaccination campaign, France 2020–2021. (2022). https://doi.org/10.1101/2022.07.29.22278190.
Carrat, F. et al. Age, COVID-19-like symptoms and SARS-CoV-2 seropositivity profiles after the first wave of the pandemic in France. Infection 50, 257–262 (2022).
Carrat, F. et al. Antibody status and cumulative incidence of SARS-CoV-2 infection among adults in three regions of France following the first lockdown and associated risk factors: A multicohort study. Int. J. Epidemiol. 50, 1458–1472 (2021).
Schetelig, J. et al. Blood group A epitopes do not facilitate entry of SARS-CoV-2. J. Intern. Med. 290, 223–226 (2021).
Patel, E. U. et al. Comparative performance of five commercially available serologic assays to detect antibodies to SARS-CoV-2 and identify individuals with high neutralizing titers. J. Clin. Microbiol. 59, 02257–02320 (2021).
Rikhtegaran Tehrani, Z. et al. Performance of nucleocapsid and spike-based SARS-CoV-2 serologic assays. PLoS ONE 15, e0237828 (2020).
Acknowledgements
The authors warmly thank all the volunteers of the Constances, E3N-E4N and NutriNet-Santé cohorts for their continuous participation in the study and for participating in the SAPRIS-SERO project. We thank the CEPH-Biobank staff for their adaptability and the quality of their work. In the virology department, we thank Dr Nadège Brisbarre and the technical staff for impeccable management of samples and serological assays.
Funding
The SAPRIS/SAPRIS-SERO projects received funding from ANR (Agence Nationale de la Recherche, #ANR-20-COVI-000, #ANR-10-COHO-06), Fondation pour la Recherche Médicale (#20RR052-00), and Inserm (Institut National de la Santé et de la Recherche Médicale, #C20-26). The NutriNet-Santé cohort study was supported by the following public institutions: Ministère de la Santé, Santé Publique France, Institut National de la Santé et de la Recherche Médicale (INSERM), Institut National de Recherche pour l'Agriculture, l'Alimentation et l'Environnement (INRAE), Conservatoire National des Arts et Métiers (CNAM) and Université Sorbonne Paris Nord. The CONSTANCES cohort benefits from grant ANR-11-INBS-0002 from the French National Research Agency. CONSTANCES is supported by the Caisse Nationale d’Assurance Maladie, the French Ministry of Health, the Ministry of Research, and the Institut National de la Santé et de la Recherche Médicale (INSERM). CONSTANCES is also partly funded by AstraZeneca, Lundbeck, L’Oréal, and Merck Sharp & Dohme Corp. The E3N-E4N cohort is supported by the following institutions: Ministère de l'Enseignement Supérieur, de la Recherche et de l'Innovation, INSERM, University Paris-Saclay, Gustave Roussy, the MGEN, and the French League Against Cancer. Study investigators are independent from the funders. Funders had no role in the study design, the collection, analysis, and interpretation of data, the writing of the manuscript, or the decision to submit the article for publication.
Author information
Authors and Affiliations
Consortia
Contributions
The authors’ contributions were as follows – M.D.T., M.T. conceptualized the study and defined the analytical strategy; F.S.E.: performed statistical analyses; M.D.T. supervised statistical analyses and drafted the manuscript; M.T.: supervised statistical analyses and writing; F.S.E., N.D.P., Y.E., J.A., P.G., S.H., G.S., M.Z., E.W., X.dL, F.C., M.T., SAPRIS-SERO study group: played a key role in the acquisition of the data. All authors critically helped in the interpretation of results, revised the manuscript and provided relevant intellectual input. They all read and approved the final manuscript. M.D.T. and M.T. had primary responsibility for the final content.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Deschasaux-Tanguy, M., Szabo de Edelenyi, F., Druesne-Pecollo, N. et al. ABO blood types and SARS-CoV-2 infection assessed using seroprevalence data in a large population-based sample: the SAPRIS-SERO multi-cohort study. Sci Rep 13, 4775 (2023). https://doi.org/10.1038/s41598-023-30714-9
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41598-023-30714-9
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.