Abstract
The effectiveness of the tongue right positioner (TRP) use on oral and swallowing functions remains unclear. To investigate the effects of TRP use on tongue function in patients with dysphagia. This interventional study included eight participants with dysphagia who visited a university dental hospital. The measurement variables included tongue pressure (TP) as the primary outcome and lip and tongue movements, peak nasal inspiratory flow, and changes in the tongue and suprahyoid muscle regions on ultrasonography as the secondary outcomes. Each participant was asked to use a TRP for at least 8 h every night for 2 months. The measurement variables before and after the intervention were compared using the paired t test and Wilcoxon signed-rank test. TP after intervention (31.5 ± 13.1 kPa) was significantly higher than that before intervention (23.0 ± 13.4 kPa), while other measurement variables did not significantly improve. Numerous exercises have been suggested to improve TP; however, most require patients’ adherence to instructions. In contrast, although participants did not perform active exercises, most participants in this study observed an improved TP. Our findings show that TRP can greatly improve TP after 2 months of usage.
Trial registration number: University Hospital Medical Information Network Clinical Trials Registry (UMIN000040253, date of first registration: 27/04/2020).
Similar content being viewed by others
Introduction
The tongue heavily interacts with the hard and soft palate during speech production as well as mastication and deglutition, cooperating with the lips, mandible, pharynx, and larynx. Therefore, tongue function impairment negatively influences speech production, masticatory, and swallowing movements, leading to dysphagia. Quantitative evaluation of the tongue function is essential for dysphagia rehabilitation, and tongue pressure (TP) is used as a quantitative and convenient index of tongue strength. However, decreased TP is associated with reduced swallowing and masticatory function1,2. TP can also be decreased by dysphagia-causing conditions, such as cerebrovascular diseases3, neuromuscular dysfunction4, Parkinson’s disease5, and sarcopenia6. In addition, recent evidence suggests that TP may also be decreased in patients with cognitive decline and mild cognitive impairment7,8. Therefore, a reduction in TP should be considered since it may serve as a valuable index for rehabilitation in dysphagia cases. Regarding the relationship between clinical symptoms and TP, prolonged mealtime, decrease in meal amount9, the occurrence of aspiration10, and pharyngeal residue11 have been reportedly associated with decreased TP. Consequently, it is necessary to improve TP during rehabilitation using exercises such as balloon tongue resistance12, tongue protrusion13, and tongue pressure resistance14 trainings.
The tongue right positioner (TRP) (Fig. 1) is an oral device that was initially developed for orthodontic treatment15. Since TRP aligns the tongue’s position in the oral cavity, it is also used in patients with obstructive sleep apnea (OSA)16. The device partially inhibits the back and forward movements of the tongue. Therefore, it is believed that the strength of swallowing-related muscles increases to compensate for the inhibited tongue movements. A study reported that TRP increases the strength of suprahyoid muscles, such as geniohyoid and stylohyoid muscles15. Therefore, we hypothesized that TRP could potentially improve the strength of the tongue muscle. To the best of our knowledge, the effects of TRP on tongue function were investigated in patients with dysphagia for the first time.
Methods
Ethical considerations
This single-arm study was conducted per the Declaration of Helsinki of 1975, revised in 2013, and was approved by the Ethics Committee of the Tokyo Medical and Dental University (D2020-023). Written informed consent was obtained from all participants.
Participants
Patients who visited a university dental hospital between September 2020 and September 2021 and had dysphagia were enrolled in this study. The inclusion criteria were as follows: (1) at least three of the six anterior teeth in the upper jaw remained, (2) at least two of the five molars on both the right and left sides of the upper jaw remained, (3) the lingual frenulum was not short, (4) those who could handle the use of the TRP, and (5) those who agreed to join this study. The exclusion criteria were the following: (1) inability to follow instructions, (2) altered consciousness, and (3) tracheostomy. Eight male patients with an average age of 58.8 ± 12.3 years received TRP intervention.
Intervention
Tongue right positioner
The TRP (Tongue Lab Japan, Kyoto, Japan), patented by Tongue Lab., Paris, France, was provided to all participants. It is a custom-made removable oral device consisting of a resin button and a transverse arch (Fig. 1). The device was positioned along the maxillary arch, with the transverse arch extending from the first molar to the hard palate at the same height as the upper teeth. The resin button was located in the middle of the palate, and it opposed tongue movements. During the study, participants were asked to visit the hospital three times to receive the intervention. On the first visit, dental arch impressions were recorded to create a plaster model, which was sent to a dental laboratory to fabricate the personalized TRP. The participants receiving the TRPs were informed about their usage on the second visit, and they were asked to wear the device for at least 8 h every night while sleeping. Additionally, they were asked to return for a follow-up visit after 2 months to evaluate the effect of TRP use. Participants did not perform any active training during the interventional period.
Outcome
The outcome variables were assessed at the beginning of the study and at the 2-month follow-up visit. In this study, TP was the primary outcome, and the secondary outcomes were tongue and lip movement speed, peak nasal inspiratory flow (PNIF), and ultrasound assessment of swallowing-related muscles.
Measurement
The measurements were performed by dentists who belong to the department of dysphagia rehabilitation in a university hospital and are accustomed to using the measurement devices. Before the measurements, the dentists calibrated the usage of all measurement devices employed in this study.
Tongue pressure
TP was evaluated using a JMS tongue pressure measurement device (JMS Co. Ltd., Hiroshima, Japan). Participants in the sitting position were asked to place the balloon in their mouth and hold the plastic pipe with their upper and lower central incisors with their lips closed. A dentist held the probe in the correct position while recording the measurements. The participants were then asked to push the balloon with their tongue against their hard palate for 7 s with maximum pressure. The TP was measured three times, and the average value was recorded as described previously17,18.
Tongue and lip movement speed
The tongue and lip movements were evaluated using oral diadochokinesis (ODK). ODK was measured using the KENKO-KUN Handy, an oral function-measuring device (Takei Scientific Co., Ltd., Niigata, Japan). Participants were asked to pronounce a monosyllable as quickly as possible for 5 s. The device recorded the number of repetitions for each syllable and calculated the number of syllables produced per second. The monosyllables ‘‘pa,’’ ‘‘ta,’’ and ‘‘ka’’ were used to evaluate the ability of the lips, the tip of the tongue, and the posterior region of the tongue, respectively19,20.
Ultrasonographic assessment of swallowing-related muscles
The cross-sectional area of the geniohyoid muscle (CSA of the GH) and the thickness of the tongue were evaluated using an ultrasonic measuring device (SonoSite M-turbo, Fujifilm, Tokyo, Japan) in B mode21,22 to evaluate swallowing-related muscles. The geniohyoid muscle was selected to represent the suprahyoid muscles. Participants were asked to gently close their mouths while facing forward in the sitting position to evaluate the CSA of the GH. The probe was placed with ultrasonic gel at the midline of the mouth floor to cover the geniohyoid muscle (sagittal), and it adhered adequately to the skin without applying pressure to the tissue. The probe was placed perpendicular to the Frankfurt plane on a line connecting the first mandibular molars of the left and right, including the second premolar, to evaluate the thickness of the tongue. The probes were brought into close contact with the lower surface of the mandible covered with ultrasonic gel22,23. The transverse section of the tongue was depicted at rest, with the participant facing forward in the sitting position.
The intraclass correlation coefficients (ICC) (1,1) and (2,1) were calculated to evaluate the reliability of the examiner. ICC (1,1) 0.925 and (2,1) 0.966 is used for measuring the CSA of the GH, and ICC (1,1) 0.936 and (2,1) 0.925 for the thickness of the tongue, which revealed high reliability. ImageJ software (National Institutes of Health, Bethesda, MD, USA) was used for image processing. The CSA of the GH and tongue thickness were measured thrice and twice, respectively, and the mean values were recorded. During the analysis, the examiner was blinded to the information, including the names of the participants and whether the image was taken at baseline or at follow-up.
Peak nasal inspiratory flow
A previous report33 on pediatric patients shows that TRP corrects the position of the tongue and improves upper airway patency. Therefore, we also measured PNIF in this study. The PNIF was evaluated using a portable PNIF meter (Clement Clarke International, Harlow, Essex, UK). Participants who held their heads parallel to the floor in a seated position were asked to inhale with their mouths closed as firmly and quickly as possible through the mask, starting from the end of full expansion. The reliability has been established previously24,25, with a correlation coefficient of approximately 92%26. The measurement was performed three times, and the average value was recorded as described previously27.
Other measurements
The Barthel index (BI), the functional oral intake scale (FOIS) scores, and the dysphagia severity scale (DSS) of the participants were recorded. The BI is an index of daily living activities consisting of 10 questions, with scores between 0 and 100. A higher score was associated with a higher physical function28. The FOIS, which is a seven-point scale, was recorded to assess the oral intake level, and a higher point was associated with a higher intake level. DSS is a seven-point scale, with scores of 1, 2, 3, 4, 5, 6, and 7 indicating saliva aspiration, food aspiration, water aspiration, occasional aspiration, oral problems, minimal problems, and within normal limits and no symptoms of dysphagia, respectively. The reliability of the BI, FOIS, and DSS has been verified previously6,29,30,31. At the 1- and 2-month follow-up visits, in addition to the measurement, the participants were asked whether they wore TRP every night, and if they did not, the number of times they forgot.
Statistical analysis
The Shapiro–Wilk test was used to test the normality of all data, after which the paired t test and Wilcoxon signed-rank test were used for the analysis of parametric and non-parametric data, respectively, using the Japanese version of SPSS for Windows (version 25 J; IBM Japan, Ltd., Tokyo, Japan). Significant differences were considered at a corrected p < 0.05. A post hoc analysis was performed to calculate the effect size (ES) of each variable using G*Power 3.1 (Kiel University, Kiel, Germany). ES was defined as large for r > 0.5, medium for 0.3 < r < 0.5, small for 0.1 < r < 0.3, and without effect for r < 0.1.
Ethics approval
This single-arm study was conducted per the Declaration of Helsinki of 1964, revised in 2013, and was approved by the Ethics Committee of the Tokyo Medical and Dental University (D2020-023).
Consent to participate
Written informed consent was obtained from all participants.
Results
Eight participants (all men, average age of 58.8 ± 12.3 years) were enrolled in this study. Table 1 shows the characteristics of the participants. Dysphagia-causing diseases included neuromuscular diseases (n = 3) and cerebrovascular diseases (n = 2). The participants’ median BI, FOIS, and DSS scores were 85 (25–100), 6.5 (2–7), and 3.5 (2–4), respectively. Table 2 shows the differences in TP, ODK, PNIF, and ultrasonographic assessment of swallowing-related muscles before and after TRP use. A significant improvement was found in TP (p = 0.034, r = 0.84). The ES of each measurement item was also calculated. Of the eight participants, the ODK of one participant with cerebral infarction could not be evaluated because of expressive aphasia after cerebral infarction. There were no other missing data. All eight participants wore TRP every night during the 2-month intervention period. Figure 2 shows a comparison of TP between the baseline and follow-up values of each participant. Of the eight participants, seven showed improvements in TP. Figure 3 shows box plots of the measurement items with medium or large ES.
Comparison of tongue pressure between baseline and follow-up values for each participant. Each number indicates the participant’s number in Table 1.
Box plots of measurement items with medium or large effect sizes. The left (dark grey) and right (light grey) box plots in each measurement item reveal baseline and follow-up values, respectively. The top and bottom of the vertical line show the maximum and minimum values, respectively, and the box in the middle illustrates the interquartile range. The horizontal line in the middle of the box shows the median value, and the cross mark shows the mean value. TP tongue pressure, ODK oral diadochokinesis, PNIF peak nasal inspiratory flow.
Discussion
The TRP was employed for patients with dysphagia for the first time, showing that TP increased after 2-month use. Interestingly, although three participants had progressive disease, TP increased. Therefore, the device can serve as a valuable tool for functional rehabilitation of the tongue in patients with such diseases.
A decrease in TP was observed in only one of the eight participants. However, the TP of this participant at baseline was 40.8 kPa, which was not significantly low despite the presence of dysphagia, with a decrease of only 0.8 kPa. Therefore, TRP may not have been very useful in this case. However, TRP could be suitable for dysphagia caused by low TP.
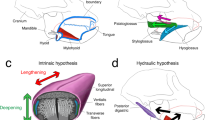
Although a few mechanisms associated with TRP and improvement in TP have been reported, a possible explanation might be the lingual–hypoglossal reflex. When filiform papillae on the tongue are mechanically stimulated, the tongue’s tip curves upward, the tongue hollows from side to side with the upward curvature of the lateral edges, and the posterior part is depressed32,33. Consequently, TRP may cause this reflex and could enhance the strength of the tongue’s intrinsic and extrinsic muscles, which play a role in protrusion and retrusion. The improved tongue muscles could have increased TP, and TRP has been used to manage OSA16. The relationship between tongue protrusion strength in an arousal state and upper airway patency has been previously reported34. TP evaluation suggests that TRP improves the genioglossal muscle strength, contributing to tongue protrusion.
The ultrasonographic evaluation revealed that the CSA of the GH did not improve in this study (p = 0.484, r = 0.25). Although an association between TP and the geniohyoid muscle has been reported15, the mechanism of increased TP with TRP use could be owing to the enhanced tongue muscles rather than the suprahyoid muscles. However, it remains unclear whether TRP improved the geniohyoid muscle function in this study owing to the small sample size; therefore, additional research is required to clarify the effectiveness of TRP on the geniohyoid muscle function in a larger sample size. The thickness of the tongue did not improve (p = 0.588, r = 0.21) despite the improvement of TP. Tongue muscle strength increases without muscle hypertrophy at the beginning of muscular exercises because of neural adaptation35. The improvement in TP in this study can be attributed to this phenomenon.
The ODK and PNIF were also measured. The ‘Pa’ of ODK (r = 0.45) and PNIF (r = 0.48) during the follow-up visit tended to increase, but when compared with that of baseline, no significant differences were found. There may be a significant difference between baseline and follow-up values in future studies with a larger sample size. In this study, cases of some patients with progressive disease should have been adjusted or homogenized. Although the improvement was not significant, the PNIF scores increased. This finding is consistent with a previous study36. Similarly, the ‘Pa’ of ODK also increased. However, the reason behind this finding remains unclear. A possible explanation might be the reduction in mouth breathing caused by increased PNIF. Previously, adults’ mouth breathers had reduced nasal patency and lower PNIF scores than that of nasal breathers37. Particularly, mouth breathing is associated with weak lip muscle strength38. Therefore, TRP improved lip closure reflected in the ‘pa’ of ODK and PNIF. Moreover, the lip-closure strength should also be measured in future studies.
In contrast, the ‘ta’ and ‘ka’ of ODK decreased slightly. In the ‘ta’ of the ODK, the score of four participants, including the three participants with progressive neuromuscular diseases, increased whereas that of the other two decreased. The ‘ka’ scores of the two participants decreased, while no change was observed in that of the remaining participants. The improvement in the ‘ta’ could be explained by enhanced genioglossal muscle strength, similar to the improvement in TP. However, the ‘ka’ did not change or decrease. Of the two participants whose ‘ka’ decreased, one had progressive disease, and the other had a history of cerebral infarction. The ‘ta’ and ‘ka’ of ODK reflect the anterior and posterior movements of the tongue, respectively. TRP could maintain the movement of the anterior tongue despite the presence of progressive diseases.
This study had some limitations. First, only eight participants were included. Further, as we conducted this pilot study before conducting a randomized controlled trial with both TRP and placebo groups, we did not include a control group. Furthermore, confounding factors were not considered in this study. In the subsequent randomized controlled trial, the sample size will be set using the effect size calculated from the result of this study. Additionally, the participants were heterogeneous: the BIs, the FOIS scores, and the DSS ranged from 25 to 100, 2 to 7, and 2 to 4, respectively. Therefore, more studies are required with a larger number of male and female participants to clarify the effectiveness of TRP use in improving oral function. Second, although TP increased, the ultrasound assessment showed no improvement, suggesting that the muscle characteristics did not change after wearing TRP. Third, the increase in TP may be due to the lingual–hypoglossal reflex. However, it was difficult to prove that the reflex had actually occurred. Fourth, we only verbally confirmed the participants’ usage of TRP at 1- and 2-month follow-up visits. Although the compliance of the participants in this study was adequate that all of them wore TRP every night for the 2-month period, a checklist should be distributed to confirm the achievement rate in a future study. Fifth, we did not find any changes in DSS scores, evaluated by videoendoscope, between the initial and 2-month follow-up visits. The range of each DSS score is wide, and the DSS score does not reflect the movement of swallowing-related organs. Moreover, we could not evaluate the tongue’s position. Since the previous study indicated that TRP could improve the tongue’s position, leading to the increase of PNIF, we should have evaluated its position using videofluorography. Lastly, since the period of TRP usage was 2 months, TP possibly decreases after patients stop TRP usage. However, it remains unclear whether the effect of TRP continues even after the interventional period. Therefore, the long-term effect of TRP usage should also be evaluated in the future.
This is the first study to consider the oral or swallowing function of TRP users. Therefore, a randomized controlled trial should be conducted in future studies to emphasize the effectiveness of TRP in oral function. Considering that the ES of TP is 0.84 in this study, 48 participants, including 24 with TRP and placebo oral device (α = 0.05, power = 0.8), are required. Furthermore, since we did not observe any changes via the videoendoscope, swallowing evaluations with videofluorography should be conducted to observe the changes in swallowing kinematics and anatomical characteristics in future studies.
Numerous exercises have been suggested to improve TP14,39,40. However, most required patients to follow instructions. In contrast, although participants did not perform active exercises, most participants in this study observed an improvement in TP. In particular, participants Nos. 2 and 5 whose TP, BI, and swallowing function were low (Table 1) showed an increase in TP after 2 months of TRP use. This suggests that TRP can be useful for patients with dysphagia who cannot perform active exercises because of the low daily living activities. Additionally, TRP is a noninvasive and removable oral device, and caregiver assistance is required only during device insertion and removal. Therefore, TRP can be used even in situations with limited assistance. Furthermore, no adverse events, such as desorption, were reported in this study.
Conclusion
This pilot study showed that TRP might improve TP in patients with dysphagia.
Data availability
The datasets generated during and/or analyzed during the current study are available from the corresponding author upon reasonable request.
References
Aoki, Y., Kabuto, S., Ozeki, Y., Tanaka, T. & Ota, K. The effect of tongue pressure strengthening exercise for dysphagic patients. Jpn. J. Compr. Rehabil. Sci. 6, 129–136 (2015).
Hara, K. et al. Association between tongue muscle strength and masticatory muscle strength. J. Oral Rehabil. 46, 134–139 (2019).
Nakamori, M. et al. Prediction of pneumonia in acute stroke patients using tongue pressure measurements. PLoS ONE 11, e0165837 (2016).
Umemoto, G., Tsuboi, Y., Kitashima, A., Furuya, H. & Kikuta, T. Impaired food transportation in Parkinson’s disease related to lingual bradykinesia. Dysphagia 26, 250–255 (2011).
Minagi, Y. et al. Relationships between dysphagia and tongue pressure during swallowing in Parkinson’s disease patients. J. Oral Rehabil. 45, 459–466 (2018).
Maeda, K. & Akagi, J. Decreased tongue pressure is associated with sarcopenia and sarcopenic dysphagia in the elderly. Dysphagia 30, 80–87 (2015).
Egashira, R. et al. Low tongue strength and the number of teeth present are associated with cognitive decline in older Japanese dental outpatients: A cross-sectional study. Int. J. Environ. Res. Public Health 17, 8700 (2020).
Suzuki, H. et al. Patients with mild cognitive impairment diagnosed at dementia clinic display decreased maximum occlusal force: A cross-sectional study. BMC Oral Health 21, 665 (2021).
Namasivayam, A. M., Steele, C. M. & Keller, H. The effect of tongue strength on meal consumption in long term care. Clin. Nutr. 35, 1078–1083 (2016).
Nakamori, M. et al. Relationship between tongue pressure and dysphagia diet in patients with acute stroke. PLoS ONE 16, e0252837 (2021).
Ono, T. et al. Influence of bite force and tongue pressure on oropharyngeal residue in the elderly. Gerodontology 24, 143–150 (2007).
Robbins, J. et al. The effects of lingual exercise on swallowing in older adults. J. Am. Geriatr. Soc. 53, 1483–1489 (2005).
Fujiu-Kurachi, M. et al. Tongue pressure generation during tongue-hold swallows in young healthy adults measured with different tongue positions. Dysphagia 29, 17–24 (2014).
Namiki, C. et al. Tongue-pressure resistance training improves tongue and suprahyoid muscle functions simultaneously. Clin. Interv. Aging 14, 601–608 (2019).
Mauclaire, C., Vanpoulle, F. & Saint-Georges-Chaumet, Y. Physiological correction of lingual dysfunction with the “Tongue Right Positioner”: beneficial effects on the upper airways. Int. Orthod. 13, 370–389 (2015).
Mauclaire, C., Wullman, P., Belattar, A., Vanpoule, F., Bancel, R., Saint-Georges-Chaumet, Y. Intérêts de la rééducation linguale avec le dispositif TRP pour le traitement des troubles respiratoires obstructifs du sommeil. Med. Sommeil 16:43 (in French). https://www.researchgate.net/publication/337632031_Interets_de_la_reeducation_linguale_avec_le_dispositif_TRP_pour_le_traitement_des_troubles_respiratoires_obstructifs_du_sommeil (2019).
Utanohara, Y. et al. Standard values of maximum tongue pressure taken using newly developed disposable tongue pressure measurement device. Dysphagia 23, 286–290 (2008).
Shimizu, A. et al. Effect of low tongue pressure on nutritional status and improvement of swallowing function in sarcopenic dysphagia. Nutrition 90, 111295 (2021).
Ito, K. et al. A comparison of methods for the measurement of oral diadochokinesis. Ronen Shika Igaku (Jpn J. Gerodontol.) 24, 48–54 (2009) ((in Japanese)).
Ziegler, W. Task-related factors in oral motor control: Speech and oral diadochokinesis in dysarthria and apraxia of speech. Brain Lang. 80, 556–575 (2002).
Yabunaka, K. et al. Ultrasonographic evaluation of geniohyoid muscle movement during swallowing: A study on healthy adults of various ages. Radiol. Phys. Technol. 5, 34–39 (2012).
Ogawa, N. et al. Ultrasonography to measure swallowing muscle mass and quality in older patients with sarcopenic dysphagia. J. Am. Med. Dir. Assoc. 19, 516–522 (2018).
Yoshimi, K. et al. Relationship between swallowing muscles and trunk muscle mass in healthy elderly individuals: A cross-sectional study. Arch. Gerontol. Geriatr. 79, 21–26 (2018).
Cho, S. I., Hauser, R. & Christiani, D. C. Reproducibility of nasal peak inspiratory flow among healthy adults: assessment of epidemiologic utility. Chest 112, 1547–1553 (1997).
Teixeira, R. U. F., Zappelini, C. E. M., Alves, F. S. & da Costa, E. A. Peak nasal inspiratory flow evaluation as an objective method of measuring nasal airflow. Braz. J. Otorhinolaryngol. 77, 473–480 (2011).
Starling-Schwanz, R. et al. Repeatability of peak nasal inspiratory flow measurements and utility for assessing the severity of rhinitis. Allergy 60, 795–800 (2005).
Sawa, A. et al. Assessment of screening for nasal obstruction among sleep dentistry outpatients with obstructive sleep apnea. Dent. J. (Basel) 8, 119 (2020).
Mahoney, F. I. & Barthel, D. W. Functional evaluation: The Barthel index. Md State Med. J. 14, 61–65 (1965).
Sainsbury, A., Seebass, G., Bansal, A. & Young, J. B. Reliability of the Barthel index when used with older people. Age Ageing 34, 228–232 (2005).
Crary, M. A., Mann, G. D. C. & Groher, M. E. Initial psychometric assessment of a functional oral intake scale for dysphagia in stroke patients. Arch. Phys. Med. Rehabil. 86, 1516–1520 (2005).
Nishimura, K. et al. Accuracy of dysphagia severity scale rating without using videoendoscopic evaluation of swallowing. Jpn. J. Compr. Rehabil. Sci. 6, 124–128 (2015).
John, R. R., Chandrasekaran, B. & Murugadoss, P. Lingual hypoglossal reflex: An unusual reflex of head and neck. J. Maxillofac. Oral Surg. 18, 366–370 (2019).
Miller, A. J. Oral and pharyngeal reflexes in the mammalian nervous system: Their diverse range in complexity and the pivotal role of the tongue. Crit. Rev. Oral Biol. Med. 13, 409–425 (2002).
Kanezaki, M., Ogawa, T. & Izumi, T. Tongue protrusion strength in arousal state is predictive of the airway patency in obstructive sleep apnea. Tohoku J. Exp. Med. 236, 241–245 (2015).
Cullins, M. J., Krekeler, B. N. & Connor, N. P. Differential impact of tongue exercise on intrinsic lingual muscles. Laryngoscope 128, 2245–2251 (2018).
Mauclaire, C., Vanpoulle, F., Belattar, A. & Saint-Georges-Chaumet, Y. Importance of the lingual reeducation by the tongue right positioner on the upper airways permeability in young orthodontic patients. Sleep Med. 24, 161–165 (2017).
Trevisan, M. E. et al. Respiratory mode, nasal patency and palatine dimensions. CoDAS 27, 201–206 (2015) ((in Portuguese)).
Ismail, A. M. A. Oral rehabilitation using the lip muscle trainer: A narrative review. PTJ 11, 139–144 (2021).
Park, T. & Kim, Y. Effects of tongue pressing effortful swallow in older healthy individuals. Arch. Gerontol. Geriatr. 66, 127–133 (2016).
Oh, J. C. Effects of resistive jaw-opening exercise with elastic resistance bands on suprahyoid muscle activation and tongue strength in the elderly: A pilot study. Folia Phoniatr. Logop. 73, 376–383 (2021).
Funding
Fifty percent of the cost for proofreading by Editage and article publishing charges were paid for by Tongue Lab Japan, Kyoto, Japan. In addition, eight tongue right positioner devices and one peak nasal inspiratory flow meter were provided by Tongue Lab Japan for this study.
Author information
Authors and Affiliations
Contributions
All authors contributed to the study’s conception and design. Material preparation, data collection, and analysis were performed by R.Y., K.H., C.N., T.O., and A.S. The first draft of the manuscript was written by R.Y., and all authors commented on previous versions of the manuscript. All authors read and approved the final manuscript. All participants signed informed consent for the publication of their data.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Yanagida, R., Hara, K., Namiki, C. et al. Effects of tongue right positioner use on tongue pressure: a pilot study. Sci Rep 13, 3289 (2023). https://doi.org/10.1038/s41598-023-30450-0
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41598-023-30450-0
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.