Abstract
Pericardial effusions requiring pericardiocentesis have multiple causes that vary among geographical regions and health contexts. This procedure can be performed for diagnostic or therapeutic indications. The purpose of this study was to identify the principal causes of pericardial effusions and indications for pericardiocentesis, exploring differences among groups. This was a retrospective case series of patients who underwent pericardiocentesis for pericardial effusion in a single center in Latin America. Demographic, clinical, echocardiographic, and procedural variables were recorded and analyzed. The primary outcome was to determine the causes of pericardial effusions in these patients and the indication (diagnostic, therapeutic, or both). The results are presented in two groups (inflammatory and noninflammatory) according to the cause of the pericardial effusion. One hundred sixteen patients with pericardial effusion underwent pericardiocentesis. The median age was 58 years (IQR 46.2–70.7), and 50% were male. In the noninflammatory pericardial effusion group, there were 61 cases (53%), among which neoplastic pericardial effusion was the most frequent cause (n = 25, 40.9%). In the inflammatory group, there were 55 cases (47%), and the main cause was postpericardiectomy syndrome after cardiac surgery (n = 31, 56.4%). The principal indication for pericardiocentesis was therapeutic (n = 66, 56.8%). Large pericardial effusion without hemodynamic effect of cardiac tamponade was significantly more frequent in the inflammatory group (p = 0.03). In conclusion, the principal cause of pericardial effusion in patients who underwent pericardiocentesis was postpericardiectomy syndrome after cardiac surgery, followed by neoplastic pericardial effusion. Pericardiocentesis is mainly a therapeutic procedure.
Similar content being viewed by others
Introduction
The pericardium is a tissue that can be affected by different systemic and cardiac illnesses. There are two phenotypic responses to a variety of injuries: acute inflammation and/or fluid accumulation1. The pericardium contains 10–50 mL of serous fluid between the visceral and parietal pericardium with a pressure between − 5 and 5 cmH2O. The increase in this fluid is known as pericardial effusion, which can produce an increase in the pericardium cavity pressure, restricting ventricular filling and decreasing cardiac output, which leads to cardiac tamponade2,3. Pericardiocentesis has been described since the 1970s and is a diagnostic and therapeutic procedure for treating pericardial effusion based on symptoms and echocardiographic findings4,5. However, according to the guidelines, the indications for invasive diagnostic techniques are some of the unmet needs in pericardial disease2.
Furthermore, pericardial effusion etiologies in patients who have undergone pericardiocentesis are variable for geographic regions6,7,8 and have changed over the years9. Therefore, these case series attempted to identify the principal causes of pericardial effusion and the indications for this procedure, exploring differences in clinical variables.
Methods
Study design and data collection
We present a case series of patients who underwent pericardiocentesis for pericardial effusion by interventional cardiology staff in a single center in Bogotá, Colombia between 2017 and 2018. We reviewed the database of the interventional cardiology service and selected the pericardiocentesis cases of patients over 18 years old. We classified pericardial effusion into inflammatory and noninflammatory causes based on different expert reviews10,11,12. Clinical and echocardiographic characteristics were collected based on guidelines of pericardial disease2,3, and procedural technical aspects and outcomes were also described1 (Supplementary Table 1). Patients without clinical or procedural information were excluded. The Institutional Ethics Committee (IEC) of Fundación Cardioinfantil, Instituto de Cardiología (Bogotá, Colombia) approved the study. It was carried out within the ethical principles for medical research on human beings according to the Declaration of Helsinki—59th General Assembly, Seoul, Korea, October 2008. Furthermore, informed consent waived was approved by the IEC of Fundación Cardioinfantil, Instituto de Cardiología (IEC Record No. 48-2020) due to the study's retrospective nature.
Primary and secondary outcomes
The primary outcome was the causes of pericardial effusion in patients who required pericardiocentesis and their indications (diagnostic, therapeutic, or both). The causes were classified into two groups (inflammatory and noninflammatory), which in turn were divided into specific causes. Secondary outcomes were clinical and echocardiographic characteristics. Patients who underwent a pericardial window were identified, and their causes were also established. Success rates and procedural complications were additionally evaluated.
Statistical analysis
The results are presented in two groups according to the cause of pericardial effusion, inflammatory and noninflammatory, and in specific causes for all the pericardiocentesis procedures conducted during the observation period. Age, weight, height, and drained liquid volume are presented as the medians and interquartile ranges. Other demographic (sex), clinical (indications and results of pericardiocentesis), and echocardiographic characteristics (effusion size and localization) are presented as absolute and relative frequencies. Fisher’s test or the χ2 test was used to compare clinical and echocardiographic results between the groups, and a p-value < 0.05 was considered statistically significant. SPSS v22 was used to conduct all statistical analyses.
Results
Clinical and demographic characteristics
A total of 116 patients with pericardial effusion underwent pericardiocentesis. The median age was 58 years (IQR 46.2–70.7), and 50% were men. The most common symptom was dyspnea (n = 50, 43.1%). Echocardiographic tamponade signs without clinical manifestations were present in 59 (50.8%) cases. Regarding pericardial effusion presentation, large pericardial effusion without a hemodynamic effect was significantly more frequent in the inflammatory group (p = 0.03), whereas cardiac tamponade with clinical manifestations was more frequent in the noninflammatory group, without significant differences. Forty-two (36.2%) patients had received anticoagulants before the procedure, with warfarin being the most frequent. There were no other significant differences among the groups when comparing the baseline clinical characteristics. Other clinical characteristics are described in Table 1.
Pericardial effusion causes in patients who underwent pericardiocentesis
Pericardial effusion of inflammatory causes
Pericardial effusion of inflammatory cause was identified in 55 patients (47%). The principal etiology of inflammatory pericardial effusion was late pericardial effusion postcardiac surgery related to postpericardiectomy syndrome, which presented in 31 (56%) cases. Late pericardial effusion postcardiac surgery was defined as pericardial effusion that presented ten days after surgery, usually related to an inflammatory reaction of post pericardiectomy syndrome. The second most common etiology was idiopathic pericarditis (n = 8, 14.5%). In the infectious pericardial effusion etiologies (n = 6, 10.9%), only one case was related to Mycobacterium tuberculosis. Other causes are described in Table 2 and Fig. 1.
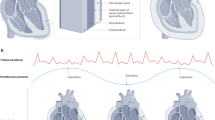
Central illustration. (a) Fluoroscopy guidance pericardiocentesis with the puncturing needle crossing the pericardium (red line). (b) Guidewire around the heart shadow (blue line) and pericardium space that contains PE between the pericardium and heart shadow (yellow arrow). (c) Percentages of specific causes in the inflammatory and noninflammatory groups. Percentage of diagnostic, therapeutic or both indications for pericardiocentesis in the inflammatory and noninflammatory groups. *There were no cases of only diagnostic indication for pericardiocentesis in the non-inflammatory group. Percentage of pericardial effusion composition in the groups and pericardial effusion composition examples.
Pericardial effusion of noninflammatory causes
Pericardial effusion of noninflammatory cause was identified in 61 patients (53%), with neoplastic etiology being the most common cause, with 25 (40.9%) cases. Breast cancer (n = 6) followed by myelodysplastic syndromes (n = 4) were the most frequent etiologies of neoplastic pericardial effusion. Only one case was related to anticoagulation therapy. Early pericardial effusion postcardiac surgery was defined as pericardial effusion that presented during the first ten days after surgery with a possible relationship to microvascular bleeding and was classified as a noninflammatory cause (n = 13, 21.3%) (Fig. 1). The main type of cardiac surgery related to pericardial effusion was aortic valve replacement (n = 10), in which only 4 patients were classified as early pericardial effusion. Only nine patients required a pericardial window after pericardiocentesis, with persistent pericardial effusion being the principal cause.
Echocardiographic characteristics
Most of the pericardial effusions were large (n = 70, 60.3%) and had a circumferential distribution (n = 80, 68.9%). The most frequent signs of intrapericardial pressure augmentation were diastolic collapse of the right atrium and/or right ventricle (n = 73, 62.9%) and variations in E velocities during respiration across the mitral valve and/or tricuspid valve (n = 59, 50.8%). There were no significant differences between the groups in echocardiographic findings. Additional echocardiographic findings are described in Supplementary Table 2.
Procedural technical aspects and outcomes
The procedure was successful in 98% of the cases. There were two perforations of the cardiac chambers, one of which required emergent cardiac surgery. The most common approach was subxiphoid guided by fluoroscopy (n = 114, 98.2%). The principal indication for pericardiocentesis was therapeutic (n = 66, 56.8%) (Supplementary Table 3). There were no cases of only diagnostic indication for pericardiocentesis in the non-inflammatory group. Moreover, in the independent analyses for each indication (diagnostic, therapeutic or both), the diagnostic indication for pericardiocentesis was significantly more frequent in the inflammatory group (p = 0.04).
Pericardial effusion compositions and indications for pericardiocentesis are described in Fig. 1. There were no significant differences between the groups in pericardial effusion composition/type. Despite that, when we analyzed the composition of the pericardial effusion in each cause (Supplementary Table 4), we found hydropericardium composition was more frequent in the neoplastic cases in the non-inflammatory group. At the same time, hemopericardium was most common in post-cardiac surgery- late pericardial effusion in the inflammatory group. Intrahospital mortality was 4.3%, although none of the deaths were related to the procedure.
Discussion
This case series identified postpericardiectomy syndrome (late pericardial effusion postcardiac surgery) as the main etiology of pericardial effusion in patients undergoing pericardiocentesis, in contrast with previous studies where the main causes reported were neoplastic, infectious, or idiopathic7,8. The largest registry of pericardiocentesis, published almost 20 years ago, evaluated different etiologies of pericardial effusion over the last three decades of the twentieth century in a single center. The results of that study showed a change in the causes of pericardial effusion over time, with postcardiac surgery, neoplastic, and cardiac perforations after invasive procedures being the most frequent during the nineties9. Our study describes similar results when evaluating specific causes, suggesting an increase in complex cardiovascular procedures.
In our study, the female sex was slightly more frequent (50.9%) compared with other series where the frequency reported of males was between 51–55%7,8,9. However, in our concept, there were no significant differences between the sex in the different case series. Furthermore, the average age between the studies is under 75 years, as in our series. Despite the causes of pericardial effusion that require pericardiocentesis varies among the regions and the period of recruitment, our case series of pericardiocentesis is comparable with others that recruited patients from other regions such as Europe, North America, and Asia7,8,9,13. Moreover, comparing the principal causes with other recent case series (last 20 years), the causes were similar (post-surgical, neoplastic, and iatrogenic)8,13. However, one case series from Singapore report pulmonary infection diseases as the third most common cause of the pericardial effusion13. While other one reported tuberculous pericarditis as their second most frequent cause of pericardial effusion8, this result was in China, a country with more incidence of tuberculosis14 than the rest of the countries with case series of pericardiocentesis in our knowledge. Additional demographic and clinical characteristics of other case series compared with ours are described in Table 3.
Our modified classification of pericardial effusion into inflammatory and noninflammatory etiologies was based on different expert reviews10,11,12; this classification allows clustering different causes that inflame, injures, or reduced lymphatic drainage of the pericardium that can result in an effusion. When comparing these two groups, we found that large pericardial effusion without hemodynamic effect was significantly more frequent in the inflammatory group, while in the noninflammatory group, cardiac tamponade with clinical manifestation was more common, but without a significant difference. This may be related to the specific etiologies in each group that could generate an acute or chronic volume overload in the pericardium cavity. This classification may help to simplify the indication and optimal timing for pericardiocentesis in patients with pericardial effusions since the hemodynamic effect was less common in the inflammatory group than in the noninflammatory group. Our results are according to a previous study where the principal causes of large pericardial effusion without tamponade were acute idiopathic pericarditis and idiopathic pericardial effusion; causes classified in our study as inflammatory causes7.
We also divided pericardial effusion postcardiac surgery into two types. Early pericardial effusion, which appears by the tenth postoperative day, may be related to microvascular bleeding, and late pericardial effusion is defined as pericardial effusion that presents after ten days of the procedure and is attributed to an inflammatory reaction of the pericardium15. This classification was based on previous studies where the maximum effusion in the postoperative state was on the tenth day after surgery16. In our study, the median time of pericardial effusion postcardiac surgery that required pericardiocentesis was 11.5 days (IQR = 7.0–19.7). In early and late pericardial effusion, 63% of the cases were anticoagulated, but in none of the cases was anticoagulation attributed as a cause of the effusion. However, a recent study found that postoperative anticoagulation treatment was a risk factor for subacute cardiac tamponade (defined > 48 h after cardiac surgery), a feature that could be related to these effusions17.
In our series, no case underwent only diagnostic pericardiocentesis in the non-inflammatory group. However, it was diagnostic and therapeutic in 39.3% of this group, compared with other studies, where the pericardiocentesis yield for diagnostic in 19%7.
In addition, similarly to other series9,13, the most frequent composition of pericardial effusion in our research was hemopericardium, followed by hydropericardium in both groups (Table 3); however, within our specific cause composition analyses, the hydropericardium was a more frequent composition in the neoplastic etiology.
The rate of complications in our study was 2%, similar to other series that are between 0.79–2%7,8,9,13, although most pericardiocentesis was guided by fluoroscopy and not by echocardiogram. The mortality was low and not related to the procedure; the pericardial effusion causes of patients who died were neoplastic (n = 4) and infectious (n = 1). In other studies, pericardial effusion caused by cancer and percutaneous cardiac interventions were related to intrahospital mortality18,19. The percentage of patients who needed pericardiocentesis after a percutaneous coronary intervention was 18%, and none of them had fatal outcomes during hospitalization.
The echocardiographic findings are the principal tools used to perform pericardiocentesis in patients without clinical manifestation of cardiac tamponade11,20, a feature that was frequent in our patients. This could be related to the specific etiologies that caused a slow accumulation of pericardial fluid, leading to cardiac tamponade only after larger volumes.
Aside from the retrospective nature of the study, a potential limitation of this data set is the limited number of patients from a single center. Moreover, we obtained the chemistry pericardial fluid analysis information in only a few cases because it is not routinely evaluated, and for that reason, it was not included. We also know that the causes of pericardial effusions in patients who underwent pericardiocentesis are variable and according to other series depend more on the geographical area. Although our institution performs a high volume of cardiovascular procedures and is located in an urban area, which could influence the results, it also admits patients from diverse regions of our country with different diseases that can compromise the pericardium.
This case series reports real data of the causes of pericardial effusion leading to pericardiocentesis in a developing country, that is comparable with developed countries. We believe that this is the largest series of pericardiocentesis published in Latin America, which changes the paradigm that has considered tuberculous pericarditis as the principal etiology of pericardial effusion in developing countries21, which represents only one case in our series. These findings are in accordance with the decreasing rate of tuberculosis in the world during recent decades14 and highlight the need for multicenter studies to elucidate the epidemiology of pericardial effusion in developing countries.
Conclusion
Pericardiocentesis is mostly a therapeutic procedure with a low rate of complications and mortality. The pericardial effusions after cardiac surgery, related to neoplastic disease and after a percutaneous coronary intervention, were the main etiologies in patients who underwent pericardiocentesis. The inflammatory causes of pericardial effusion had milder clinical manifestations compared with noninflammatory causes.
Change history
14 November 2022
A Correction to this paper has been published: https://doi.org/10.1038/s41598-022-23921-3
References
Dudzinski, D. M., Mak, G. S. & Hung, J. W. Pericardial diseases. Curr. Probl. Cardiol. 37(3), 75–118. https://doi.org/10.1016/j.cpcardiol.2011.10.002 (2012).
Adler, Y. et al. 2015 ESC Guidelines for the diagnosis and management of pericardial diseases: The Task Force for the Diagnosis and Management of Pericardial Diseases of the European Society of Cardiology (ESC) endorsed by: The European Association for Cardio-Thoracic Surg. Eur. Heart J. 36(42), 2921–2964. https://doi.org/10.1093/eurheartj/ehv318 (2015).
Imazio, M. & Adler, Y. Management of pericardial effusion. Eur. Heart J. 34(16), 1186–1197. https://doi.org/10.1093/eurheartj/ehs372 (2013).
Loukas, M. et al. Pericardiocentesis: A clinical anatomy review. Clin. Anat. 25(7), 872–881. https://doi.org/10.1002/ca.22032 (2012).
Maggiolini, S., De Carlini, C. C. & Imazio, M. Evolution of the pericardiocentesis technique. J. Cardiovasc. Med. 19(6), 267–273. https://doi.org/10.2459/JCM.0000000000000649 (2018).
Corey, G. R. et al. Etiology of large pericardial effusions. Am. J. Med. 95(2), 209–213 (1993).
Sagrista-Sauleda, J., Merce, J., Permanyer-Miralda, G. & Soler-Soler, J. Clinical clues to the causes of large pericardial effusions. Am. J. Med. 109(2), 95–101 (2000).
Ma, W. et al. Causes of moderate to large pericardial effusion requiring pericardiocentesis in 140 Han Chinese patients. Herz 37(2), 183–187. https://doi.org/10.1007/s00059-011-3428-5 (2012).
Tsang, T. S. M. et al. Consecutive 1127 therapeutic echocardiographically guided pericardiocenteses: Clinical profile, practice patterns, and outcomes spanning 21 years. Mayo Clin. Proc. 77(5), 429–436. https://doi.org/10.4065/77.5.429 (2002).
Vakamudi, S., Ho, N. & Cremer, P. C. Pericardial effusions: Causes, diagnosis, and management. Prog. Cardiovasc. Dis. 59(4), 380–388. https://doi.org/10.1016/j.pcad.2016.12.009 (2017).
Sinnaeve, P. R. & Adriaenssens, T. A contemporary look at pericardiocentesis. Trends Cardiovasc. Med. 29(7), 375–383. https://doi.org/10.1016/j.tcm.2018.10.016 (2019).
Azarbal, A. & LeWinter, M. M. Pericardial effusion. Cardiol. Clin. 35(4), 515–524. https://doi.org/10.1016/j.ccl.2017.07.005 (2017).
Cheong, X. P. et al. Causes and prognosis of symptomatic pericardial effusions treated by pericardiocentesis in an Asian academic medical centre. Singap. Med. J. 61(3), 137–141. https://doi.org/10.11622/smedj.2019065 (2020).
World Health Organization. Global Tuberculosis Report. 1–277. https://apps.who.int/iris/bitstream/handle/10665/329368/9789241565714-eng.pdf?ua=1.
Khan, N. K. et al. Incidence, presentation and risk factors of late postoperative pericardial effusions requiring invasive treatment after cardiac surgery. Interact. Cardiovasc. Thorac. Surg. 24(6), 835–840. https://doi.org/10.1093/icvts/ivx011 (2017).
Weitzman, L. B. et al. The incidence and natural history of pericardial effusion after cardiac surgery—An echocardiographic study. Circulation 69(3), 506–511. https://doi.org/10.1161/01.cir.69.3.506 (1984).
Leiva, E. H. et al. Factors associated with delayed cardiac tamponade after cardiac surgery. Ann. Card. Anaesth. 21(2), 158–166. https://doi.org/10.4103/aca.ACA_147_17 (2018).
Ho, M.-Y. et al. Pericardiocentesis adverse event risk factors: A nationwide population-based cohort study. Cardiology 130(1), 37–45. https://doi.org/10.1159/000368796 (2015).
Sethi, A., Singbal, Y., Kodumuri, V. & Prasad, V. Inpatient mortality and its predictors after pericardiocentesis: An analysis from the Nationwide Inpatient Sample 2009–2013. J. Interv. Cardiol. 31(6), 815–825. https://doi.org/10.1111/joic.12563 (2018).
McIntyre, W. F., Jassal, D. S. & Morris, A. L. Pericardial effusions: Do they all require pericardiocentesis?. Can. J. Cardiol. 31(6), 812–815. https://doi.org/10.1016/j.cjca.2015.01.006 (2015).
Syed, F. F., Ntsekhe, M. & Mayosi, B. M. Tailoring diagnosis and management of pericardial disease to the epidemiological setting. Mayo Clin. Proc. 85(9), 866. https://doi.org/10.4065/mcp.2010.0377 (2010) (author reply 866).
Author information
Authors and Affiliations
Contributions
J.H.P., K.M., J.C. and D.E. wrote the main manuscript text and prepared central illustration. J.H.P., A.P., J.B. and A.P. collected the data. J.H.P. and K.M. analysed the data. All authors reviewed the manuscript.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
The original online version of this Article was revised: The original version of this Article contained an error in the Abstract. “In conclusion, the principal indication for pericardiocentesis was therapeutic (n = 66, 56.8%). Large pericardial effusion without hemodynamic effect of cardiac tamponade was significantly more frequent in the inflammatory group (p = 0.03). The principal cause of pericardial effusion in patients who underwent pericardiocentesis was postpericardiectomy syndrome after cardiac surgery, followed by neoplastic pericardial effusion. Pericardiocentesis is mainly a therapeutic procedure.” now reads: “The principal indication for pericardiocentesis was therapeutic (n = 66, 56.8%). Large pericardial effusion without hemodynamic effect of cardiac tamponade was significantly more frequent in the inflammatory group (p = 0.03). In conclusion, the principal cause of pericardial effusion in patients who underwent pericardiocentesis was postpericardiectomy syndrome after cardiac surgery, followed by neoplastic pericardial effusion. Pericardiocentesis is mainly a therapeutic procedure.”
Supplementary Information
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
del Portillo-Navarrete, J.H., Pizano, A., Benavides, J. et al. Unveiling the causes of pericardial effusion in a contemporary case series of pericardiocentesis in Latin America. Sci Rep 12, 16010 (2022). https://doi.org/10.1038/s41598-022-19339-6
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41598-022-19339-6
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.