Abstract
Primary Sjögren’s syndrome (pSS) is an autoimmune disease with frequent neurological involvement. Memory complaints are common, but their precise patterns remain unclear. We wanted to characterize patterns of neurocognitive profiles in pSS patients with cognitive complaints. Only pSS patients with memory complaints were included, prospectively. Cognitive profiles were compiled through a comprehensive cognitive evaluation by neuropsychologists. Evaluations of anxiety, depression, fatigue, sleep disorders and quality of life were performed for testing their interactions with cognitive profiles. All 32 pSS patients showed at least borderline cognitive impairment, and 17 (53%) exhibited a pathological cognitive profile: a hippocampal profile (37%), a dysexecutive profile (22%), and an instrumental profile (16%) (possible overlap). Regarding the secondary objectives: 37% of patients were depressed, and 48% exhibited a mild-to-severe anxiety trait. Sleep disorders were frequent (excessive daytime sleepiness (55%), high risk for sleep apnea (45%), and insomnia (77%)). Cognitive impairments could not be explained alone by anxiety, depression or sleep disorders. Fatigue level was strongly associated with sleep disorders. Our study highlights that cognitive complaints in pSS patients are supported by measurable cognitive impairments, apart from frequently associated disorders such as depression, anxiety or sleep troubles. Sleep disorders should be screened.
Similar content being viewed by others
Introduction
Primary Sjögren’s syndrome (pSS) is an autoimmune disease with glandular (sicca syndrome) and extra-glandular B lymphocytic infiltration, not associated with concomitant autoimmune diseases such as rheumatoid arthritis or systemic lupus erythematosus. Among extra-glandular manifestations of pSS, psycho-cognitive troubles are frequently observed1,2, with a prevalence varying from 10 to 60%3,4,5. These cognitive symptoms have a negative impact on patient’s quality of life6,7, may contribute to fatigue (a major burden in pSS), or underlie depression8, and thus impact the burden on the health system1. Most patients report “brain fog” symptoms2, described as memory lapses, forgetfulness, mental confusion, diminished ability to concentrate, to organize, or to anticipate future events. The precise neuropsychological pattern of pSS is not fully deciphered, however, executive functions are often abnormal9,10. The interplay between cognitive complaints, cognitive impairment, fatigue, depression11, sleep disorders12, and pain is not fully understood in pSS.
Thus, we aimed to describe the precise patterns of neurocognitive profiles from a cohort of pSS patients with cognitive complaints via an extensive and comprehensive neuropsychological approach. In addition, we deciphered the relationships between cognitive profile, fatigue, depression, anxiety, sleep disorders and self-reported quality of life, and herein propose a tailored management of cognitive complaints in pSS patients.
Materials and methods
Patients
We prospectively included all consecutive adult pSS patients with unexplained cognitive complaints, characterized by memory loss, attention troubles, or “brain fog”, followed between November 2016 and January 2019 in the department of internal medicine of Montpellier university hospital. Patients with pre-existing conditions or treatments interfering with cognitive complaints were excluded (i.e. diagnosed depression, or damage of central nervous system). The diagnosis of pSS was assessed by experienced physicians, based on ACR/EULAR (American College of Rheumatology/EUropean League Against Rheumatism) diagnosis criteria13. The history of the disease, including clinical, biological (presence of antinuclear antibodies (ANA), and anti-SSa, and/or anti-SSb), pathological, and radiological findings, such as treatment strategies and main cardiovascular risk factors were recorded. Systemic involvement of the disease was defined by lung, cardiac, kidney, hematological or neurological involvements of the disease. The level of activity of pSS was assessed according to the EULAR Sjögren’s Syndrome Disease Activity Index (ESSDAI)14, and the patient-reported evaluation used the EULAR Sjögren’s Syndrome Patient Reported Index (ESSPRI), including a self-evaluation of pain, fatigue, and sicca syndrome14. Both were done at the moment of the baseline cognitive assessments.
Cognitive assessments
A large battery of cognitive tests was performed including: educational level, ranging from 1 to 715; the Mac Nair scale; the French cognitive complaint questionnaires (QPC)16; Mini-mental state (MMSE)17; the French version of the Free and Cued Reminding Selective Test (FCRST)18; digit span; Digit Symbol Substitution Test (DSST) (subpart of Wechsler Adult Intelligence Scale-Fourth Edition, WAIS-IV)19; Trail making test (TMT)20; Rey-Osterrieth complex figure test21; Verbal Fluency Test (VFT); Categorical Naming Test (CNT)22; the Stroop Color and Word and Interference Test23; Visual Object and Space Perception (VOSP)24; the picture naming test (D080)25; and the praxis’ tests26. A list of all tests is available in Supplementary Table 1.
The result of each test was classified into three categories: (1) normal; (2) borderline scores, without clinical impact; (3) and pathological scores. As no pathological cognitive threshold was validated in pSS population, we determined the threshold using previous validated values in < 60yo-adults, using Z-scores for the neuropsychological tests done or percentiles. Details on pathological and borderline thresholds for each test and survey are available in Supplementary Table 2. These thresholds were established including the age, sex and educational level of each patient. Some cognitive functions abnormalities may overlap on several tests (Supplementary Tables 1 and 2).
Based on this extensive evaluation, and according to the expertise of the neuropsychologists’ team, pSS patients’ cognitive skills were classified into three categories: (1) global memory impairment (at least one confirmed deficit in FCRST or digit span); (2) global executive functions impairment (a defect in at least three executive components among mental flexibility, planning, inhibition, initiation and/or spontaneous recovery, assessed through DSST, TMT, Rey-Osterrieth complex figure test, VFT, CNT and Stroop test); or (3) global instrumental functions impairment (impairment in one of the different functions among gnosis, praxis and/or language, assessed through praxis’ test, VOSP and DO80). A global neurocognitive profile was established integrating those results. The global cognitive profile was classified as pathological if ≥ 1 subcategory (memory, executive or instrumental functions) was classified as pathological; and the global cognitive profile was classified as borderline if ≥ 1 subcategory was classified as borderline.
Fatigue and sleep disorders
Because of the broad spectrum of fatigue manifestations, fatigue was evaluated with three dimensions: (1) the Chalder Fatigue scale (14 self-reported questions assessing physical and mental fatigue, a score ≥ 9 assessing pathological fatigue for the youngers)27; (2) the Multidimensional Fatigue Inventory (MFI) including 20 items about general fatigue, physical fatigue, mental fatigue, reduction of daily activities, and decreased motivation28; (3) the ESSPRI, including a Likert scale for fatigue, from 0 to 1014. Results were adjusted to 100 for ease of plotting on radar charts. In addition, pain level was evaluated through the ESSPRI subscale14. Sleep disorders were described by the Berlin questionnaire (probability of sleep apnea disorder)29; the Epworth Sleepiness Scale (ESS) assessing the global quality of the sleep according to daily sleepiness30; and Insomnia Severity Index (ISI) used for the severity of insomnia31.
Psychiatric comorbidities
Depression was evaluated by the French version of the 21-item self-questionnaire Beck Depression Inventory version II (BDI)32: depression is diagnosed when score > 13 and a severe depression when > 29. Anhedonia was evaluated through Chapman’s scale33. We evaluated self-esteem through the Rosenberg self-esteem scale34: low or very low self-esteem < 31/41 points. Anxiety was assessed by the French version of State Trait Anxiety Inventory (STAI)35, which is representative of the “usual” anxiety state of the subject.
Quality of life
To analyze the health-related quality of life (HR-QoL), we used the EuroQol 5 Dimensions (EQ-5D) and the Short-Form 36 (SF-36), widely used in autoimmune diseases. The EQ-5D refers to five dimensions of HR-QoL: mobility; independence; daily activities; pain or discomfort; anxiety or depression feelings (poor level of HR-QoL was defined with a Time Trade-Off value < 0.5). The self-reported SF-36 assesses patients’ quality of life (QoL) in eight domains: physical functioning, social functioning (social limitations), role limitations due to physical health, bodily pain, general health, mental health, role limitations due to emotional problems, health thinking (general health perception). The score is summarized into two levels: the physical component score (PCS), and the mental component score (MCS). Lower scores represent worse QoL.
MRI investigations
Brain MRIs were performed concomitantly to cognitive tests, in a subgroup of volunteer pSS patients (all patients were offered a brain MRI) (3 T [MAGNETOM Skyra, Siemens Healthcare, Erlangen, Germany], T1- and T2-weighted imaging, and the FLAIR sequence). Brain atrophy and white matter hyperintensity lesions load were evaluated by visual rating. Fazekas’ scale quantifies the white matter hyperintensities attributed to the chronic small vessel ischemia (vascular burden). A score > 0 is considered as pathological. Scheltens’ score aims at estimating the hippocampal atrophy: a score of 1 is considered as pathological (beginning atrophy).
Statistical analysis
All quantitative data were expressed as mean ± [standard deviation], and qualitative variable were presented as proportion (%). Between-group comparisons of quantitative variables were performed using the Student T-test if both distributions followed a normal distribution and the Mann–Whitney U-test if not. The Chi2 test (or Fisher test when appropriate) was used to compare categorical variables frequencies in the two group. p values under 0.05 were considered as significant. Correlation analysis were performed with Pearson correlation coefficient because of normality of the 2 distributions compared. We compared demographical and pSS characteristics, the prevalence of fatigue, pain, psychiatric disorders, and sleep disorders, and brain MRI results, between pSS patients with and without pathological cognitive profile, patients with and without poor self-reported quality of life (according to EQ-5D), and patients with or without pathological fatigue score (according to Chalder Fatigue scale). Missing data were not included in the analysis. Data and statistical analyses were performed using SAS software (SAS® 9.4; SAS institute inc., Cary, NC, USA).
Ethical concern
Our study was conducted in accordance with the local ethical committee of the University Hospital center of Montpellier (Accreditation number 198711; Institutional review board 2018_IRB-MTP_06-08), and in accordance with the Declaration of Helsinki. All included subjects gave informed written consent to participate in the study.
Results
Demographical, immunological, and radiological characteristics of pSS patients
All consecutive pSS volunteers with unexplained cognitive complaints were included: 32 (31 female and 1 male) (Supplementary Fig. 1). None of them withdrew participation. Their main characteristics are listed in Table 1. The median age was 58 years old [51–69], with a mean disease duration of 11.8 years [± 8.3]. Fifty-nine percent of the population had an educational level of bachelor or higher [2–7]. Seventy-five percent of patients were positive for ANA (37.5% for anti-SSa and/or SSb). Seven patients had lung involvement of the disease (21.9%). Five patients (15.6%) had peripheral neurological symptoms (4 cases of small fiber neuropathy and 1 case of ganglionopathy). Brain MRIs analysis revealed Fazekas’ score > 0 in 20/25 patients with available data (80%). Scheltens’ scale was at 1 in 6/24 patients (25%). Patients with brain MRIs did not differ from those without brain MRIs on pSS characteristics and neuropsychological assessments.
Neuropsychological assessments
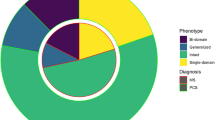
Eighty-six percent of patients presented an abnormal memory complaint according to Mac Nair scale or Cognitive complaint questionnaire. A cognitive impairment was identified in all patients (Table 2). In total, 84% of patients exhibited borderline or pathological scores for memory functions, 94% for executive functions, and 30% for instrumental functions. Fifty-three percent of patients exhibited a pathological neurocognitive profile in at least one cognitive function. Thirty-seven percent of them exhibited pathological memory functions, 22% pathological executive functions, and 17% pathological instrumental functions (some exhibited overlapping profiles) (Fig. 1). The praxis were not significantly affected, apart from the visuoconstructive praxis for a few subjects, probably due to impaired visuospatial skills. Details including thresholds values of each test are shown in Supplementary Table 2.
Fatigue, pain, psychiatric comorbidities, sleep disorders, and quality of life
An abnormal level of fatigue was observed in 32% of pSS, according to the Chalder Fatigue scale (Table 3; Fig. 2B). The median ESSPRI score for pain level was 6/10 [3.5–9]. According to BDI, twelve patients were depressed, 42% with a severe form of depression (Table 3). Forty-eight percent had a mild-to-very severe anxiety trait (≥ 46). In addition, 53% had poor self-esteem. A subgroup of patients (25%) with characterized pathological cognitive profile did not show any psychiatric disorder (Fig. 3).
Radar charts of (A) patient-reported health-related quality of life and (B) fatigue. Short-form 36 evaluation of quality of life, median score of subcomponent (low scores are associated with poor quality of life): PF Physical functioning, SF social functioning, RP role physical (limitations in daily activities associated to physical status), BP Bodily pain, GH general health, MH mental health, RE role emotional (limitations in daily activities associated to psychological status), VT vitality, HT health thinking. Fatigue evaluation according to patients’ self-reported fatigue (median, reported as percentage of total score; high score is associated with higher fatigue); ESSPRI EULAR Sjögren’s syndrome patient reported index, MFI Multidimensional fatigue inventory and its components. To improve clarity, scores were adjusted to 100.
Heatmap showing the distribution of cognitive profiles and associated psychiatric and sleep disorders among 32 primary Sjögren’s patients with cognitive complaints. Darker colours represent worse outcomes. The cluster of 8 patients with cognitive complaints, pathological cognitive disorders, but without anxiety or depression (outlined in red), suggests another underlying pathophysiological mechanism for cognitive troubles. Systemic involvement of the disease is more frequent among patients with pathological cognitive profile.
Sleep disorders were frequent: 55% had an excessive daytime sleepiness, 45% were considered at risk for sleep apnea, and 71% suffered from insomnia (7 had moderate, and 3 had severe insomnia) (Table 3).
Quality of life was impaired in many patients. According to EQ-5D evaluation, 11 patients described their HR-QoL as mild (0–0.5, n = 8) or worse than death (< 0, n = 3) (Table 3). The Physical Component Score (SF-36 PCS) was worse than the Mental Component Score (SF-36 MCS) (Student test, p = 0.007). Most patients complained of severe limitations in daily activities because of physical status, while the objective measures of the disease’s activity (ESSDAI) were not high. They did not feel limited in daily activities by psychological status (Fig. 2A).
Subgroup analyses: characteristics of the pSS patients with objective global cognitive dysfunction, with poor HR-QoL, or high level of fatigue
We compared the demographical, clinical, neuro-cognitive, and biological evaluations of the 17 pSS patients with pathological global cognitive profiles to the 15 other pSS patients. A systemic involvement of the disease (other than sicca syndrome, skin or joint symptoms) was more frequent in these patients with pathological global cognition (65% vs 27%, p = 0.03). However, they did not exhibit more frequent depression, anxiety, sleep disorders, fatigue, pain, or worse QoL (Table 4).
The pSS patients with a poor level of HR-QoL according to EQ-5D had a higher pain level (ESSPRI pain subcategory, p < 0.001), a moderate-to-high self-evaluation of the disease activity (ESSPRI score ≥ 4, p = 0.01), and a poor physical component score (SF-36, p < 0.01). ESSPRI score was inversely correlated to SF-36 PCS (Pearson correlation coefficient − 0.486, p = 0.01). However, they did not show higher anxiety level, or more frequent depression, sleep disorder, or excessive fatigue in comparison with patients without poor HR-QoL (Supplementary Table 3).
The patients with higher levels of fatigue were younger (p < 0.001), had less systemic involvement of the disease (p = 0.03) and fewer dysfunctions in global memory (p = 0.046) compared to those with lower level of fatigue (Supplementary Table 4). They showed an increased pain level according to ESSPRI pain subcategory (p = 0.02). Their self-evaluation of quality of life (SF-36 MCS) was worse than the self-evaluation of patients with less fatigue. Interestingly, these patients had more excessive daytime sleepiness (p = 0.01), and a higher insomnia score (p = 0.03) (Supplementary Table 4).
ESSDAI level was not correlated to the observed cognitive disorders, sleep disorders, fatigue or QoL level.
Patients with pathological cognitive profiles did not show more pathological brain MRIs considering Fazekas scores and Scheltens’ scores in comparison with pSS patients without pathological cognitive profiles (p = 1 and p = 0.36, respectively).
Discussion
In this study, we analyzed a cohort of pSS patients with cognitive complaints through an extensive neuro-cognitive battery and comorbidities assessments, to decipher the role of each component in the cognitive profile. In accordance with literature data36, pSS patients presented mainly memory complaints and more than half of them exhibited pathological scores for global memory, executive functions, or instrumental functions. The proportions of patients with impaired executive functions and visuospatial skills are consistent with previous studies4,9,10,36. However, our approach, including a wide range of tests and a personalized comprehensive evaluation of each patient, was more sensitive than previous studies, and allowed an early detection of cognitive impairments (borderline scores), and their interpretation with other cofounding factors. We observed memory impairments in 37% of the patients, which may contribute to an increased risk of developing mild cognitive impairment (MCI), and possibly to the “brain fog” complaints sometimes antedating the diagnosis of pSS2. This memory impairment is also consistent with literature data reporting an increased risk for dementia in pSS patients5,37,38,39,40, especially among pSS patients under age 60 without comorbidities (Taiwanese population-based epidemiological study41). However, we did not observe any characterized dementia. These findings illustrate the central position of cognitive impairment in pSS42,43, and highlight the significance of patients’ complaints for cognitive frailty. As cognitive frailty is measurable with neuropsychological tests, we consider that cognitive complaint deserves an in-depth investigation in pSS patients to better characterize the cognitive profiles and prognosis, and propose specific strategies.
Since associated psychiatric and sleep disorders greatly interfere with cognitive complaints44, we also investigated these conditions in our pSS patients. We found that 47% of all pSS patients with cognitive complaints exhibited a profile of anxiety and/or depression, potentially contributing to cognitive complaints. Our findings are consistent with the literature, in which depression and anxiety are widely described among pSS patients45,46,47,48. As they are frequent, depression and anxiety should be systematically screened and managed in pSS patients. However, these psychiatric comorbidities alone cannot explain the observed pathological cognitive profile in our study.
We also assessed whether sleep troubles could contribute to cognitive disorders, in addition to anxiety and depression. Indeed, among the 55% of our pSS patients with cognitive complaints but without anxiety or depression, 71% had a sleep disorder. The main troubles were excessive sleepiness, risk of sleep apnea and insomnia. Nevertheless, we did not demonstrate any significant association between sleep disorders and cognitive profiles. Regardless of cognitive profile, sleep troubles are clearly associated with fatigue, another overarching hallmark of pSS8,49, that greatly affects pSS patients’ quality of life6. In our study, more than one third of patients presented fatigue, which is consistent with previous reports50. More interestingly, the fatigue level was highly correlated with excessive daytime sleepiness and insomnia, suggesting a serious impact of sleep troubles on fatigue in pSS patients51. Sleep disorders are increased in pSS patients47: reduced sleep efficiency, higher rate of awakenings, and higher rate of hypopnea have been described52,53. Interestingly, some mechanisms could contribute to hypopnea in pSS, including an obstructive mechanism (airway collapse during sleep already documented in this disease12) and a potential dysregulation of central nervous system (more precisely of breathing centers). In our opinion, there is a need for an early diagnosis of sleep disorders in pSS patients, especially in those with a high level of fatigue. For this purpose, the Berlin questionnaire, Epworth sleepiness scale and Insomnia severity index, (internationally validated screening tools), could be easily used in daily practice to identify candidate patients for polysomnography. A potential immunological hypothesis explaining fatigue was not investigated here, and remains to be proven in pSS. However, some studies underlined an inverse correlation between level of fatigue in pSS and pro-inflammatory cytokines, such as interferon-γ-induced protein-10, tumor necrosis factor-α, lymphotoxin-α and interferon-γ54,55. These interesting results should not obscure other hypotheses that could contribute to fatigue in pSS, including pain (as demonstrated here), anxiety, depression, or cognitive troubles56.
Apart from sleep troubles, cognitive dysfunctions could result from other mechanisms involving immune-mediated processes54. In our study, pSS patients with clinical-assessed cognitive impairments exhibited a more pronounced extra-glandular phenotype (excluding skin and joint involvement) than the others. Consistently, Seelinger et al. reported that the level of cognitive impairment was correlated to ESSDAI scores, in their series of 64 pSS patients with neurological involvement36. Notably, cognitive dysfunction could partially result from encephalitis or multiple-sclerosis-like disorders, whose risk is increased in pSS57,58. Furthermore, the interferons (all types) could underlie cognitive dysfunction and probably merit further investigation59, since these cytokines are known to be associated with fatigue or depression in pSS54,60. A recent study gives weight to neuronal injury, since higher levels of neurofilament light chain protein were found in cerebrospinal fluid (CSF) of pSS patients with visuospatial processing impairments and motor dysfunctions61. Taken together, all these findings suggest that cognitive impairment in pSS should be further investigated using new diagnostic tools such as biomarkers (blood, CSF) and/or innovative radiological approaches. Diffusion tensor imaging and resting state functional MRI, focusing on functional connectivity and microstructural changes, would be particularly interesting in this field62. Previous studies with more classical imaging techniques (MRI, (99 m)Tc-ECD brain SPECT) have not been able to document clearly the brain inflammatory patterns in pSS, although they demonstrated some abnormalities63,64.
Finally, all these symptoms (fatigue, cognitive complaints and sleep disorders) could have contributed to the altered quality of life that we and others observed in pSS. Thus, in our study, the self-evaluation of QoL was mildly-to-severely reduced in one third of our patients65. Furthermore, self-evaluation of disease activity (ESSPRI) was correlated to poor HR-QoL (EQ-5D), as reported previously66. Our results are also in line with previous findings on the elements of QoL most altered67: the physical health (SF-36) was bad among pSS patients, while the level of limitations due to mental health was not severely self-evaluated.
This illustrates the frequently observed discrepancies between subjective symptoms and objective measures in pSS patients68. As previously reported in pSS66, no relationship was found between the doctors’ evaluation of the disease activity (ESSDAI) and the self-evaluation of quality of life. Moreover, in our study, self-evaluated fatigue (Chalder Fatigue scale) and disease activity (ESSPRI or ESSDAI) were not linked, in accordance with literature69. These discrepancies make a comprehensive approach of neurocognitive patterns in pSS methodologically challenging.
The strength of our study was the various methodological approaches used. Our patients underwent a wide range of tests, performed by neuropsychologists, allowing personalized expertise, with a precise cognitive diagnosis for each patient, integrating educational level. This is a sensitive approach to detect early cognitive impairments. However, we only studied a small- sized sample, and included patients from our own hospital recruitment, which is not representative of the global pSS population (especially regarding SGB results and autoantibody positivity). Moreover, we only included patients complaining of cognitive disorders. Our results may thus not be translatable to the general population of pSS patients. This is a preliminary observational study. As an exploratory study, we performed multiple comparison only for descriptive purpose, not for decision-making70. Larger studies are needed to confirm these data, especially epidemiological studies integrating psychotropic drug prescriptions among pSS patients. Our approach is difficult to translate in daily practice, since an experienced team of neuropsychologists and physicians cannot be involved routinely. Thus, we would recommend to perform firstly a screening of pSS patients for depression and anxiety with routine tools such as STAI or BDI. Other already validated tools exploring cognitive complaints (such as Montreal cognitive assessment (MoCa) or Brief Cognitive Symptoms Inventory (BCSI)) could also be used, and probably in an easier way for daily practice71.
Conclusion
Cognitive complaints and fatigue concern a large proportion of pSS patients and represent complex clinical situations. Here, we found that global memory, executive functioning and attentional resources are objectively impaired in pSS patients with cognitive complaints. However, their tight interplay with depression and anxiety should be considered by physicians in daily practice and may require psychological or even psychiatric management. Screening for sleep disorders could be helpful in patients with fatigue or cognitive complaints. Further studies are required to validate our proposals for screening and management and should also include extensive cognitive evaluation, and maybe biomarkers or specific brain imaging (measuring brain functional connectivity and microstructural changes).
Data availability
Detailed data are available on reasonable request to the corresponding author.
References
Maciel, G. et al. Hospitalisation rates among patients with primary Sjögren’s syndrome: a population-based study, 1995–2016. RMD Open 4, e000575 (2018).
Manzo, C., Martinez-Suarez, E., Kechida, M., Isetta, M. & Serra-Mestres, J. Cognitive function in primary Sjögren’s syndrome: A systematic review. Brain Sci. 9, 85 (2019).
Delalande, S. et al. Neurologic manifestations in primary Sjögren syndrome: A study of 82 patients. Medicine (Baltimore) 83, 280–291 (2004).
Morreale, M. et al. Neurological involvement in primary Sjögren syndrome: A focus on central nervous system. PLoS ONE 9, e84605 (2014).
Blanc, F. et al. Cognitive dysfunction and dementia in primary Sjögren’s syndrome. ISRN Neurol. 2013, 501327 (2013).
Koçer, B. et al. Cognition, depression, fatigue, and quality of life in primary Sjögren’s syndrome: Correlations. Brain Behav. 6, e00586 (2016).
Faurholt-Jepsen, M. et al. Patient-evaluated cognitive function measured with smartphones and the association with objective cognitive function, perceived stress, quality of life and function capacity in patients with bipolar disorder. Int. J. Bipolar Disord. 8, 31 (2020).
Gairy, K., Knight, C., Anthony, P. & Hoskin, B. Burden of illness among subgroups of patients with primary Sjögren’s syndrome and systemic involvement. Rheumatology (Oxford) https://doi.org/10.1093/rheumatology/keaa508 (2020).
Riega-Torres, J. C. L. et al. Cognitive dysfunction in Sjögren’s syndrome using the montreal cognitive assessment questionnaire and the automated neuropsychological assessment metrics: A cross-sectional study. Int. J. Rheum. Dis. 23, 1019–1023 (2020).
Tezcan, M. E. et al. Primary Sjögren’s syndrome is associated with significant cognitive dysfunction. Int. J. Rheum. Dis. 19, 981–988 (2016).
Albrecht, K. et al. Comorbidity and health care utilisation in persons with Sjögren’s syndrome: A claims data analysis. Clin. Exp. Rheumatol. 38(Suppl 126), 78–84 (2020).
Yeh, T.-C. et al. Risk of obstructive sleep apnea in patients with Sjögren syndrome and Behçet’s disease: A nationwide, population-based cohort study. Sleep Breath. 24, 1199–1205 (2020).
Shiboski, C. H. et al. 2016 American college of rheumatology/European league against rheumatism classification criteria for primary Sjögren’s syndrome: A consensus and data-driven methodology involving three international patient cohorts. Ann. Rheum. Dis. 76, 9–16 (2017).
Seror, R. et al. Validation of EULAR primary Sjögren’s syndrome disease activity (ESSDAI) and patient indexes (ESSPRI). Ann. Rheum. Dis. 74, 859–866 (2015).
Poitrenaud, J., Eustache, F. & Agniel, A. Neuropsychologie Clinique des Démences : Evaluations et Prise en Charge (Solal, 1995).
Thomas-Anterion, C., Honore-Masson, S., Berne, G., Ruel, J. & Laurent, B. Le questionnaire de plainte cognitive (QPC) : Un outil de recherche de plainte suspecte d’évoquer une maladie d’Alzheimer. In L’année gérontologique, pp. 56–65 (2003).
Folstein, M. F., Folstein, S. E. & McHugh, P. R. ‘Mini-mental state’. A practical method for grading the cognitive state of patients for the clinician. J. Psychiatr. Res. 12, 189–198 (1975).
Van der Linden, M. et al. L’épreuve de rappel libre/rappel indicé à 16 items (RL/RI-16). in Vol. L’évaluation des Troubles de la Mémoire. Présentation de Quatre Tests de Mémoire Episodique (Avec Leur Etalonnage) (Marseille : Solal, 2004).
Wechsler, D. Wechsler Adults Intelligence Scale WAIS-III (Editions du Centre de Psychologie Appliquée, 2000).
Tombaugh, T. Trail making test A and B: Normative data stratified by age and education. Arch. Clin. Neuropsychol. 19, 203–214 (2004).
Berry, D., Allen, R. & Schmitt, F. Rey-Osterrieth complex figure: Psychometric characteristics in a geriatric sample. Clin. Neuropsychol. 5(2), 143–153 (1991).
Cardebat, D., Doyon, B., Puel, M., Goulet, P. & Joanette, Y. Formal and semantic lexical evocation in normal subjects performance and dynamics of production as a function of sex, age and educational level. Acta Neurol. Belg. 90, 207–217 (1990).
Stroop, J. Studies of interference in serial verbal reactions. J. Exp. Psychol. 18(6), 643–662 (1935).
Warrington, E. K. & Merle, J. The Visual Object and Space Perception Battery (Thames Valley Test Company, 1991).
Deloche, G. & Hannequin, D. Test de Dénomination Orale D’images. (les Editions du Centre de Psychologie Appliquée).
Peigneux, P. et al. A neuropsychological and functional brain imaging study of visuo-imitative apraxia. Rev. Neurol. (Paris) 156, 459–472 (2000).
Chalder, T. et al. Development of a fatigue scale. J. Psychosom. Res. 37, 147–153 (1993).
Schwarz, R., Krauss, O. & Hinz, A. Fatigue in the general population. Onkologie 26, 140–144 (2003).
Netzer, N. C., Stoohs, R. A., Netzer, C. M., Clark, K. & Strohl, K. P. Using the Berlin questionnaire to identify patients at risk for the sleep apnea syndrome. Ann. Intern. Med. 131, 485–491 (1999).
Johns, M. W. A new method for measuring daytime sleepiness: The Epworth sleepiness scale. Sleep 14, 540–545 (1991).
Bastien, C. H., Vallières, A. & Morin, C. M. Validation of the Insomnia Severity Index as an outcome measure for insomnia research. Sleep Med. 2, 297–307 (2001).
Beck, A. T., Ward, C. H., Mendelson, M., Mock, J. & Erbaugh, J. An inventory for measuring depression. Arch. Gen. Psychiatr. 4, 561–571 (1961).
Kosmadakis, C. S., Bungener, C., Pierson, A., Jouvent, R. & Widlöcher, D. Translation and validation of the revised social anhedonia scale (SAS Social Anhedonia Scale, M.L. Eckblad, L.J. Chapman et al., 1982). Study of the internal and concurrent validity in 126 normal subjects. Encephale 21, 437–443 (1995).
Gray-Little, B., Williams, V. & Hancock, T. An itemresponse theory analysis of the Rosenberg self-esteem scale. Personal. Soc. Psychol. Bull. 23(5), 443–451 (1997).
Spielberger, C. D. State-Trait Anxiety Inventory for Adults Sampler Set: Manual, Instrument and Scoring Guide (Mind Garden Inc, 1983).
Seeliger, T. et al. Cognitive impairment in patients with Neuro-Sjögren. Ann. Clin. Transl. Neurol. https://doi.org/10.1002/acn3.51123 (2020).
Yoshikawa, K. et al. Prevalence of Sjögren’s syndrome with dementia in a memory clinic. J. Neurol. Sci. 322, 217–221 (2012).
Liliang, P.-C. et al. Population-based study suggests an increased risk of Alzheimer’sdisease in Sjögren’s syndrome. Clin. Rheumatol. 37, 935–941 (2018).
Lin, T.-M. et al. Autoimmune rheumatic diseases increase dementia risk in middle-aged patients: A nationwide cohort study. PLoS ONE 13, e0186475 (2018).
Goulabchand, R. et al. Hospitalization risks for neurological disorders in primary Sjögren’s syndrome patients. J. Clin. Med. 11, 1979 (2022).
Hou, T.-Y. et al. Higher risk of dementia in primary Sjogren’s syndrome. Ann. Clin. Transl. Neurol. 6, 633–641 (2019).
Pego-Reigosa, J. M., Restrepo Vélez, J., Baldini, C., Fernández, R.-F. & de Larrinoa, Í. Comorbidities (excluding lymphoma) in Sjögren’s syndrome. Rheumatology (Oxford) 60, 2075–2084 (2021).
Manzo, C., Serra-Mestres, J. & Isetta, M. Comment on: Comorbidities (excluding lymphoma) in Sjögren’s syndrome. Rheumatology https://doi.org/10.1093/rheumatology/keab602 (2021).
Segal, B. et al. Primary Sjögren’s Syndrome: health experiences and predictors of health quality among patients in the United States. Health Qual Life Outcomes 7, 46 (2009).
Liu, Z. et al. Health-related quality of life and psychological status of women with primary Sjögren’s syndrome: A cross-sectional study of 304 Chinese patients. Medicine (Baltimore) 96, e9208 (2017).
Cui, Y. et al. Anxiety and depression in primary Sjögren’s syndrome: a cross-sectional study. BMC Psychiatr. 18, 1–8 (2018).
Hsieh, M.-C., Hsu, C.-W., Lu, M.-C. & Koo, M. Increased risks of psychiatric disorders in patients with primary Sjögren’s syndrome-a secondary cohort analysis of nationwide, population-based health claim data. Clin. Rheumatol. 38, 3195–3203 (2019).
Azarfar, A., Ahmed, A. & Bég, S. Prevalence of anxiety, depression, sleep disturbance, fibromyalgia, obesity, and gastroesophageal disease in patients with rheumatic diseases. Curr. Rheumatol. Rev. https://doi.org/10.2174/1573397116666201211124815 (2020).
Segal, B. et al. Prevalence, severity, and predictors of fatigue in subjects with primary Sjögren’s syndrome. Arthritis Rheum. 59, 1780–1787 (2008).
Karageorgas, T. et al. Fatigue in primary Sjögren’s syndrome: Clinical, laboratory, psychometric, and biologic associations. Arthritis Care Res. (Hoboken) 68, 123–131 (2016).
Dardin, L. P. et al. Correlation of sleep quality with fatigue and disease activity among patients with primary Sjögren’s syndrome: A cross-sectional study. Sao Paulo Med. J. 138, 146–151 (2020).
Cui, Y. et al. Prevalence, correlates, and impact of sleep disturbance in Chinese patients with primary Sjögren’s syndrome. Int. J. Rheum. Dis. 23, 367–373 (2020).
Usmani, Z. A. et al. Sleep disordered breathing in patients with primary Sjögren’s syndrome: A group controlled study. Sleep Med. 13, 1066–1070 (2012).
Davies, K. et al. Fatigue in primary Sjögren’s syndrome (pSS) is associated with lower levels of proinflammatory cytokines: A validation study. Rheumatol. Int. 39, 1867–1873 (2019).
Howard Tripp, N. et al. Fatigue in primary Sjögren’s syndrome is associated with lower levels of proinflammatory cytokines. RMD Open 2, e000282 (2016).
Omdal, R., Mellgren, S. I. & Norheim, K. B. Pain and fatigue in primary Sjögren’s syndrome. Rheumatology (Oxford) https://doi.org/10.1093/rheumatology/kez027 (2019).
Mekinian, A. et al. Primary Sjögren’s syndrome: Central and peripheral nervous system involvements. Clin. Exp. Rheumatol. 38(Suppl 126), 103–109 (2020).
Fauchais, A.-L., Magy, L. & Vidal, E. Central and peripheral neurological complications of primary Sjögren’s syndrome. Presse Med. 41, e485-493 (2012).
de Oliveira, F. R. et al. Neurological and inflammatory manifestations in Sjögren’s syndrome: The role of the Kynurenine metabolic pathway. Int. J. Mol. Sci. 19, 3953 (2018).
Del Papa, N. et al. The role of interferons in the pathogenesis of Sjögren’s syndrome and future therapeutic perspectives. Biomolecules 11, 251 (2021).
Tjensvoll, A. B. et al. Neurofilament light is a biomarker of brain involvement in lupus and primary Sjögren’s syndrome. J. Neurol. https://doi.org/10.1007/s00415-020-10290-y (2020).
Zhang, X.-D. et al. Altered hippocampal functional connectivity in primary Sjögren syndrome: A resting-state fMRI study. Lupus 29, 446–454 (2020).
Lauvsnes, M. B. et al. Loss of cerebral white matter in primary Sjögren’s syndrome: A controlled volumetric magnetic resonance imaging study. Eur. J. Neurol. 21, 1324–1329 (2014).
Le Guern, V. et al. Cognitive function and 99mTc-ECD brain SPECT are significantly correlated in patients with primary Sjogren syndrome: a Case-control study. Ann. Rheum. Dis. 69, 132–137 (2010).
Miyamoto, S. T., Valim, V. & Fisher, B. A. Health-related quality of life and costs in Sjögren’s syndrome. Rheumatology (Oxford) https://doi.org/10.1093/rheumatology/key370 (2019).
Cornec, D. et al. Severe health-related quality of life impairment in active primary Sjögren’s syndrome and patient-reported outcomes: Data from a large therapeutic trial. Arthritis Care Res (Hoboken) 69, 528–535 (2017).
Cui, Y. et al. The impact of disease activity and psychological status on quality of life for Chinese patients with primary Sjögren’s syndrome. Patient Prefer. Adherence 12, 1513–1519 (2018).
Alunno, A. et al. Discrepancy between subjective symptoms, objective measures and disease activity indexes: The lesson of primary Sjögren’s syndrome. Clin. Exp. Rheumatol. 36(Suppl 112), 210–214 (2018).
Mæland, E., Miyamoto, S. T., Hammenfors, D., Valim, V. & Jonsson, M. V. Understanding fatigue in Sjögren’s syndrome: Outcome measures biomarkers and possible interventions. Front. Immunol. 12, 703079 (2021).
Bender, R. & Lange, S. Adjusting for multiple testing–when and how?. J. Clin. Epidemiol. 54, 343–349 (2001).
Segal, B. M., Rhodus, N., Moser Sivils, K. L. & Solid, C. A. Validation of the brief cognitive symptoms index in Sjögren syndrome. J. Rheumatol. 41, 2027–2033 (2014).
Acknowledgements
We sincerely thank Sarah Kabani for editing the manuscript.
Funding
This study did not receive any funding.
Author information
Authors and Affiliations
Contributions
Conceptualization (E.C., D.E., R.G., A.G., S.N., P.G.); Data curation (E.C., D.E., R.G., S.N., Au.M.); Formal analysis (E.C., R.G., L.A.G., S.N., A.G., P.G.); Investigation (E.C., D.E., E.C., S.N., Au.M., N.M.dC.); Methodology (S.N., L.A.G., A.l.M., R.G., A.G.); Validation (L.A.G., A.G., A.l.M., A.L.Q., R.G., P.G.); Visualization (R.G., A.l.M., A.L.Q., A.G., P.G.); Writing original draft and editing (E.C., D.E., R.G., S.N., L.A.G., N.M.dC., A.l.M., A.LQ., A.G., P.G.). All authors reviewed the manuscript.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Goulabchand, R., Castille, E., Navucet, S. et al. The interplay between cognition, depression, anxiety, and sleep in primary Sjogren’s syndrome patients. Sci Rep 12, 13176 (2022). https://doi.org/10.1038/s41598-022-17354-1
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41598-022-17354-1
This article is cited by
-
Age-associated B cell infiltration in salivary glands represents a hallmark of Sjögren’s-like disease in aging mice
GeroScience (2024)
-
Development and validation of a nomogram for predicting fatigue in patients with primary Sjögren’s syndrome
Clinical Rheumatology (2024)
-
Fatigue and sleep quality in Chinese adults with connective tissue disease: A cross-sectional study
Sleep and Breathing (2024)
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.