Abstract
Secondary epidermoid cyst of the penis is a very rare epidermoid cyst that occurs in the penis. The purpose of this study was to investigate the relationship between the occurrence of secondary epidermoid cyst of penis and circumcision-related factors, and to provide possible reasonable and effective suggestions for circumcision. The data of all patients who visited the clinic for epidermoid cysts of the penis from September 2000 to September 2021 in Xiangya Hospital were collected. A retrospective study was carried out on whether the patients had been circumcised and the surgical method, anesthesia method, cyst location, surgical age, postoperative wound infection, whether they were phimosis patients, and the level of the surgeon. Among the 24 patients followed up, 95.8% had a history of circumcision, and only 4.2% had no history of circumcision, and the more traumatic surgical methods developed secondary epidermoid cyst of the penis after surgery the higher the probability. Injecting anesthesia at the base of the penis increases the chances of developing a secondary epidermoid cyst of the penis. Postoperative secondary epidermoid cyst of the penis were mainly located in the anterior segment and posterior segment, and the anterior segment had a higher proportion, followed by the posterior segment. Secondary epidermoid cyst of the penis occur mainly in adults. Postoperative wound infection accelerates the appearance of secondary epidermoid cyst of the penis. Patients with phimosis have an increased probability of developing secondary epidermoid cysts of the penis after surgery. The incidence of secondary epidermoid cysts and postoperative infection after manual circumcision by the attending physician was higher than that of the chief physician. Circumcision, injection of anesthesia at the base of the penis, ligation of the penis, and postoperative wound infection may be the etiologies and triggers of secondary epidermoid cysts of the penis. Adults and phimosis patients may be high-risk groups. Lower-level surgeons may increase the odds of postoperative secondary epidermoid cysts of the penis, and it is recommended that surgery be performed by a clinically-experienced, higher-level surgeon. The indications for circumcision should be strictly evaluated and the operation should be performed as soon as possible, and the less invasive surgical method and anesthesia method should be selected. Reduce irrelevant operations during surgery and avoid wound infection after surgery.
Similar content being viewed by others
Introduction
Epidermoid cysts are one of the common benign lesions in dermatology, accounting for about 90% of resectable cysts1,2. The affected population is mainly adults3,4, and it can occur in any part, mainly in the head, neck and trunk5,6. Epidermoid cysts rarely worsen7,8,9, but rare malignancies may develop over time3,10. Epidermoid cysts of the penis are one of the types of epidermoid cysts, but they are very rare and usually painless11. The clinical manifestations are mainly the progressive enlargement of the cyst, and inflammatory pain may be manifested after infection or rupture of the cyst wall4. Treatment is based on complete surgical excision. At present, the etiology of penile epidermoid cysts is still controversial12, and there are reports in the literature that it may be caused by residual congenital material, or damage to the hair follicle structure due to trauma, infection, and other reasons13,14,15. The occurrence of secondary epidermoid cysts of the penis after circumcision has been noted, and so far there has never been any literature on the specific relationship between the occurrence of secondary epidermoid cysts of the penis and circumcision. The purpose of this study was to specifically analyze the relationship between secondary epidermoid cysts of the penis and circumcision-related factors, and to provide possible reasonable and effective suggestions for circumcision.
Methods
The data of all patients with epidermoid cysts of the penis from September 2000 to September 2021 in Xiangya Hospital were collected. Whether the patient has been circumcised and the surgical method, anesthesia method, cyst location, surgical age, postoperative wound infection, whether it is a phimosis patient, and the level of the surgeon were investigated. In this study, a total of 27 patients with penile epidermoid cysts were identified. Among them, 2 patients could not be contacted due to wrong phone numbers, and 1 patient refused to communicate and did not complete the follow-up, so only 24 patients were finally investigated. Among them, 23 patients had a history of circumcision, and 1 patient had no history of circumcision.
Ethical approval
This study has been reviewed by the Ethics Committee of Xiangya Hospital of Central South University, and the ethics number is: 202,111,212. Due to the spread of COVID-19 during the follow-up period, no written informed consent was signed, but the patient was informed in detail by telephone and verbal consent was obtained from the patient himself or his legal guardian. As the follow-up took place during a special period of covid-19 transmission, verbal consent was also approved by the Ethics Committee of Xiangya Hospital of Central South University. All data in this study were obtained from patient dictation. This study was conducted in strict accordance with the Declaration of Helsinki.
Informed consent
This study uses coding to hide all identifiable information of patients, and will follow the principles of scientific research risk control, privacy protection, and special protection. This research promises to comply with the requirements of scientific research management standards, and the research content will not cause harm and risk to the research subjects. The research subjects will be based on the principle of voluntariness, the right to know is guaranteed, and the rights and privacy of the research subjects will be protected to the greatest extent possible.
Results and discussion
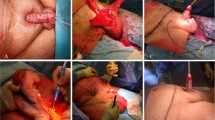
The etiology of penile epidermoid cyst has not been fully clarified. It has been reported in the literature that after neonatal circumcision, secondary epidermoid cysts of the penis may occur as a complication16, and the specific mechanism has not been studied.According to the etiology, epidermoid cysts of the penis are roughly divided into congenital and secondary epidermoid cysts of the penis17. Congenital epidermoid cysts of the penis may result from abnormal closure of the embryonic median raphe18,19. According to relevant literature reports, the occurrence of secondary epidermoid cysts of the penis may be due to trauma, surgery, and inflammation20,21,22, but no further research and analysis were conducted, which is also the significance of this study (Table 1). In this study, we found that regardless of circumcision or injection of anesthesia at the root of the penis, the incidence of postoperative secondary epidermoid cysts of the penis will increase, and the more traumatic surgical methods, the incidence of secondary epidermoid cysts of the penis (Tables 2 and 3). This may be related to the implantation of epidermal tissue into the dermis, occlusion of hair follicles, and obstruction of exocrine ducts after surgery and invasive procedures with injection of anesthesia at the base of the penis23. Patients undergoing three different surgical procedures were observed and found to have the highest incidence of secondary epidermoid cysts after manual circumcision (Table 3). The main reason may be that manual circumcision involves more operative steps than ligation and stapler circumcision. The ligation circumcision and stapler circumcision can be sutured at the same time as the overly long foreskin is removed. The time is short, the speed is fast, the effect is ideal, and there is no need for repeated operations. Manual circumcision requires a rubber band to ligate the base of the penis before the operation to reduce bleeding during the operation. After that, the overly long foreskin needs to be completely excised, and then the wound is sutured intermittently. In this process, the skin of the penis needs to be pulled and fixed with toothed forceps repeatedly. The presence of these invasive procedures described above greatly increases the risk of epidermal tissue implantation into the dermis, postoperative hair follicle occlusion, exocrine duct occlusion, and postoperative infection. This may be the main reason for the higher incidence of secondary epidermoid cysts after manual circumcision. In this study, all patients undergoing manual circumcision had the base of the penis bandaged with a rubber band before surgery to reduce bleeding, a procedure that may result in damage to the skin of the penis, which may promote secondary. The occurrence of penile epidermoid cysts, but the specific pathogenesis needs further study. From the location of the secondary epidermoid cysts of the penis, we found that when the secondary epidermoid cysts of the penis occurred in the posterior segment, the anesthesia was injected into the root of the penis, which may be related to the epidermal injection debris during the injection of anesthesia at the root of the penis24 (Table 4). Therefore, whether we can consider using other anesthesia methods to replace penile root injection anesthesia, which not only relieves the pain of anesthesia, but also reduces the occurrence of secondary epidermoid cysts of the penis after surgery.Relevant literature reports that the incidence of secondary epidermoid cysts of the penis is mainly adults3,4. Among the 23 patients with a history of circumcision in our study, 19 were adults and only 4 were minors (Tables 1 and 5). Is there a higher risk of secondary epidermoid cysts of the penis after adult circumcision?To avoid postoperative secondary epidermoid cysts of the penis, should surgery be recommended for male patients with indications for circumcision in adolescence? Of course, this requires more data to illustrate. Post-operative wound infection is a common complication after circumcision25, and post-circumcision wound infection may lead to occlusion of hair follicles or obstruction of exocrine ducts22, thereby increasing the occurrence of secondary epidermoid cysts of the penis. In this study, we did find that in patients with postoperative infection, the appearance of secondary epidermoid cysts of the penis was earlier (Tables 6 and 7), so the prevention of infection after circumcision is very important.Phimosis is one of the indications for circumcision, and it has been reported that secondary epidermoid cysts of the penis occurred in patients after phimosis23. In this study, we found that patients with phimosis had a higher rate of secondary epidermoid cysts of the penis (Table 8), probably due to the need for more invasive procedures during surgery in patients with phimosis. Therefore, it is necessary to explain the postoperative complications to the phimosis patients in detail before the operation, and avoid irrelevant invasive operations as much as possible during the operation, so as to avoid the probability of postoperative secondary epidermoid cysts of the penis.We found a higher incidence of secondary epidermoid cysts and postoperative infections after manual circumcision in the attending physician than in the chief physician (Table 9). This may be related to the lack of clinical experience of the attending physician, and there are many steps in manual circumcision. Low-level surgeons added ineffective manipulations in the process, further damaging the skin of the penis. It is also possible that with the increase of operation steps and the increase of operation time, the probability of infection is increased, and postoperative infection is more likely to occur, thereby inducing secondary epidermoid cysts of the penis. The diagnosis of secondary epidermoid cyst of the penis is easily confused with lipomas, fatty cysts, dermoid cysts, boils, and carbuncles26. A diagnosis must be made before treatment in order to decide on a treatment plan. Diagnosis mainly depends on the following points: (1) Medical history: whether there is a history of trauma and inflammation, especially whether there is a history of circumcision (2) Physical examination: a skin mass with a clear boundary can be seen on inspection, and a painless palpable mass can be palpated by palpation. Non-volatile compressible substances (3) Auxiliary examination: round or oval hypoechoic mass under color Doppler ultrasound (4) Pathological examination: keratin filling, fibrous tissue coverage27, secretory cell formation under immunohistochemistry Factors 1 and 1028, the most important of which is to carry out pathological examination. The main treatment is surgery, especially after it is known that it may turn into a malignant direction, such as squamous cell carcinoma and basal cell carcinoma29,30,31. Most of the local anesthesia surgery can be successfully resected, a small part requires general anesthesia, in order to avoid recurrence, the cyst wall must be completely removed. All surgically removed secondary epidermoid cysts of the penis should be confirmed histopathologically 32. Since secondary epidermoid cysts are very rare, this study was limited by the limited number of cases collected. However, we found some association and regularity between secondary epidermoid cysts and circumcision-related factors in a limited number of cases, which is a very meaningful study for surgeons. This will help surgeons to make more reasonable choices in circumcision operation methods, anesthesia methods, operation age, and selection of surgeons, and make clearer recommendations on the prevention of postoperative infection.
Conclusion
Circumcision, injection of anesthesia at the base of the penis, ligation of the penis, and postoperative wound infection may be the etiologies and triggers of secondary epidermoid cysts of the penis. Adults and phimosis patients may be high-risk groups. Lower-level surgeons may increase the odds of postoperative secondary epidermoid cysts of the penis, and it is recommended that surgery be performed by a clinically-experienced, higher-level surgeon. The indications for circumcision should be strictly evaluated and the operation should be performed as soon as possible, and the less invasive surgical method and anesthesia method should be selected. Reduce irrelevant operations during surgery and avoid wound infection after surgery.
Data availability
Almost all the data of this study has been included in the manuscript. Since the patients did not agree to disclose personal privacy information, this study cannot provide relevant personal privacy information including the patient's name, telephone number, home address, etc.
References
Faltaous, A. A. et al. A rare transformation of epidermoid cyst into squamous cell carcinoma: a case report with literature review. Am. J. Case Rep. 20, 1141–1143 (2019).
Sorenson, E. P. et al. Scalp dermoids: A review of their anatomy, diagnosis, and treatment. Childs Nerv. Syst. 29(3), 375–380 (2012).
Van Hoang, T. et al. Overview of epidermoid cyst. Eur. J. Radiol. Open 6, 291–301 (2019).
de Mendonça, J. C. G. et al. Epidermoid cyst: Clinical and surgical case report. Ann. Maxillofac. Surg. 7, 151–154 (2017).
Sabhlok, S., Kalele, K., Phirange, A. & Kheur, S. Congenital giant keratinous cyst mimicking lipoma: Case report and review. Indian J. Dermatol. 60(6), 637 (2015).
Blanco, G. et al. Orbital intradiploic giant epidermoid cyst. Arch. Ophthalmol. 119, 771–773 (2001).
Lopez-Rios, F., Rodriguez-Peralto, J. L., Castano, E. & Benito, A. Squamous cell car- cinoma arising in a cutaneous epidermal cyst. Am. J. Dermatopathol. 21(2), 174–177 (1999).
Bauer, B. S. & Lewis, V. L. Carcinoma arising in sebaceous and epidermoid cysts. Ann. Plast. Surg. 5(3), 222–224 (1980).
Yaffe, H. S. Squamous cell carcinoma arising in an epidermal cyst. Arch. Dermatol. 118(12), 961 (1982).
Dutta, M. et al. Epidermoid cysts in head and neck: our experiences, with review of literature. Indian J. Otolaryngol. Head Neck Surg. 65, 14–21 (2013).
Suwa, M. et al. Epidermoid cyst of the penis: a case report and review of the literature. Int. J. Urol. 7, 431–433 (2000).
Kinebuchi, Y. et al. Epidermoid cyst of the penis: a case report. Nihon Hinyokika Gakkai Zasshi 94, 452–455 (2003).
Asarch, R. G. et al. Median raphe cysts of the penis. Arch. Dermatol. 115, 1084–1086 (1979).
Shah, S. S. et al. Giant epidermoid cyst of penis. Urology 14, 389–391 (1979).
Alvarez Múgica Miguel,Jalón Monzón Antonio,González Alvarez Roberto C et al.[Giant intertesticular epidermoid cyst].[J].Arch Esp Urol,2006,59:297–9.
Nobeyama, Y. & Nakagawa, H. Case of epidermal cyst on the glans penis. J Dermatol. 40(7), 575–577. https://doi.org/10.1111/1346-8138.12176.Epub (2013).
Park, H. J. et al. Penile epidermal inclusion cyst: A late complication of penile girth enhancement surgery. J. Sex Med. 5, 2238–2240 (2008).
Otsuka, T., Ueda, Y., Terauchi, M. & Kinoshita, Y. Median raphe (parameatal) cysts of the penis. J. Urol. 159, 1918–1920 (1998).
Goyal, N. K., Trivedi, S., Dwivedi, U. S. & Singh, P. B. Congenital mucus retention cyst of penis presenting as skin papilloma. Urology 69, 381 (2007).
Craigen, M. A. & Anderson, E. G. Traumatic epidermal inclusion cysts due to shoe impingement: A report of two cases. Foot Ankle 11, 239–241 (1991).
Shah, S. S. et al. Giant epidermoid cyst of penis. Urology 14, 389–91 (1979).
Onuigbo, W. I. Vulval epidermoid cysts in the Igbos of Nigeria. Arch. Dermatol. 112, 1405–1406 (1976).
Khanna, S. Epidermoid cyst of the glans penis. Eur. Urol. 19, 176–177 (1991).
Rattan, J., Rattan, S. & Gupta, D. K. Epidermoid cyst of the penis with extension into the pelvis. J. Urol. 158, 593–594 (1997).
Ettanji, A. et al. Foreskin necrosis - complication following self-circumcision. Urol. Case Rep. 38, 101671 (2021).
Wollina, U. et al. Epidermoid cysts - a wide spectrum of clinical presentation and successful treatment by surgery: A retrospective 10-year analysis and literature review. Open Access Maced. J. Med. Sci. 6, 28–30 (2018).
Hazra, S. P. et al. Epidermoid cyst of the glans penis. Indian J. Dermatol. Venereol. Leprol. 80, 279 (2014).
Broekaert, D. et al. An investigation of cytokeratin expression in skin epithelial cysts and some uncommon types of cystic tumours using chain-specific antibodies. Arch. Dermatol. Res. 282, 383–91 (1990).
Liau, J. L. et al. Basal cell carcinoma arising from an epidermal cyst: When a cyst is not a cyst. Case Rep. Dermatol. 7, 75–78 (2015).
Sze, S. et al. Squamous cell carcinoma arising from a vulval epidermal cyst. J. Obstet. Gynaecol. Res. 42, 1623–1626 (2016).
Aljufairi, E. & Alhilli, F. Merkel cell carcinoma arising in an epidermal cyst. Am. J. Dermatopathol. 39, 842–844 (2017).
Morritt, A. N., Tiffin, N. & Brotherston, T. M. Squamous cell carcinoma arising in epidermoid cysts: report of four cases and review of the literature. J. Plast. Reconstr. Aesthet. Surg. 65, 1267–1269 (2012).
Funding
This research was funded by the Hunan Provincial Natural Science Foundation of China (2021JJ40868) and the National Natural Science Foundation of China (No. 82001738).
Author information
Authors and Affiliations
Contributions
Study concept and design: K.D., J.Y., Acquisition of data: K.D., J. Y., R.T., Analysis and interpretation of data: K.D., J.Y., Drafting of the manuscript: J.Y., R.T., Critical revision of the manuscript for important intellectual content: K.D., J.Y.
Corresponding author
Ethics declarations
Competing interests
I confirm that this manuscript has not been submitted for publication elsewhere. All authors have significantly contributed to the manuscript and all agree with its contents. None of the authors has any potential financial conflict of interest related to this manuscript.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Yu, J., Tang, R. & Ding, K. Analysis of related factors between the occurrence of secondary epidermoid cyst of penis and circumcision. Sci Rep 12, 13563 (2022). https://doi.org/10.1038/s41598-022-16876-y
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41598-022-16876-y
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.