Abstract
The local immune-inflammatory response elicited by severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2) infection is still poorly described, as well as the extent to which its characteristics may be associated with the outcome of critical Coronavirus disease 2019 (COVID-19). In this prospective monocenter study, all consecutive COVID-19 critically ill patients admitted from February to December 2020 and explored by fiberoptic bronchoscopy with bronchoalveolar lavage (BAL) were included. Biological assays, including digital ELISA cytokine profiling and targeted eicosanoid metabolomic analysis, were performed on paired blood and BAL fluid (BALF). Clinical outcome was assessed through the World Health Organization 10-point Clinical Progression Scale (WHO-CPS) at the 28th day (D28) following the admission to intensive care unit. A D28-WHO-CPS value higher than 5 defined a poor outcome. Seventy-six patients were included, 45 (59%) had a poor day-28 outcome. As compared to their counterparts, patients with D28-WHO-CPS > 5 exhibited a neutrophil-predominant bronchoalveolar phenotype, with a higher BALF neutrophil/lymphocyte ratio, a blunted local type I interferon response, a decompartimentalized immune-inflammatory response illustrated by lower BALF/blood ratio of concentrations of IL-6 (1.68 [0.30–4.41] vs. 9.53 [2.56–19.1]; p = 0.001), IL-10, IL-5, IL-22 and IFN-γ, and a biological profile of vascular endothelial injury illustrated by a higher blood concentration of VEGF and higher blood and/or BALF concentrations of several vasoactive eicosanoids. In critically ill COVID-19 patients, we identified bronchoalveolar and blood immune-inflammatory biomarker signature associated with poor 28-day outcome.
Similar content being viewed by others
Introduction
During the coronavirus disease 2019 (COVID-19) pandemic caused by severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2), it has been observed that less than 3% of individuals who are infected with the virus require hospital care1. Among them, up to one third develop the severe form of the disease, mainly acute respiratory failure, requiring admission to an intensive care unit (ICU)2,3,4 with an in-ICU mortality ranging from 28 to 42% in Europe5,6,7,8. In this severely affected population, an altered immuno-inflammatory systemic response has been described, with a marked systemic release of pro-inflammatory cytokines and an impaired interferon (IFN) type-1 response9,10,11,12, but with important differences at the individual level13. Given these findings, therapeutic targets have been proposed and immunomodulatory drugs have been investigated for SARS-CoV-2 infection. However, despite intensive research efforts, corticosteroids and tocilizumab remain the only medication that suggest a mortality benefit in randomized controlled trials14. This highlights the need to deepen our pathobiological understanding of the host immune-inflammatory response elicited by SARS-CoV-2 infection. Specifically, a better characterization of the immune-inflammatory response within affected lungs is warranted. To date, knowledge from studies in patients with severe COVID-19 describes perturbations of all cellular subpopulations in the lung microenvironment15,16 and high concentrations of pro-inflammatory cytokines within the epithelial lining fluid17,18, with a high heterogeneity among patients. Investigations in clinical settings are needed to better characterize the bronchoalveolar cellular landscape and the biochemical characteristics of the local host response and to establish the extent to which this local signature may be associated with the course of severe COVID-19.
To gain insight into this issue, we report observations of bronchoalveolar lavage (BAL) in 76 COVID-19 patients admitted to the ICU of a University teaching hospital in Paris, France during the first two waves of the pandemic in 2020. We focused on characterizing the cellular and biochemical patterns of the local host response. We hypothesized that some bronchoalveolar and blood immune-inflammatory biomarkers might be associated with a poor 28-day outcome in critical COVID-19.
Methods
Study design and patient selection
We conducted a comprehensive observational monocenter study in the ICU of Tenon Hospital in Paris, France. From February 15th to December 15th, 2020, all adult patients with PCR-confirmed SARS-CoV-2 infection on nasopharyngeal swabs or lower respiratory tract specimens were screened, and those having undergone a fiberoptic bronchoscopy with BAL were included.
Data collection
Demographics, comorbidities, clinical and routine laboratory parameters, radiological findings, and microbiological investigations were collected on ICU admission, as well as outcomes and therapeutic management, including medical therapies and organ supports during ICU stay.
Severity at admission was assessed through the Simplified Acute Physiology Score (SAPS) II19,20, the Sequential Organ Failure Assessment (SOFA) score21 and the World Health Organization 11-point Clinical Progression Scale (WHO-CPS)22.
Immunocompromised status was defined by at least one of the following conditions: splenectomy, HIV infection, long-term steroid therapy, other long-term immunosuppressive therapy, solid organ transplantation, and malignant hemopathy or cancer.
Clinical outcome was assessed through the WHO-CPS on the 28th day following ICU admission (D28-WHO-CPS).
Sample collection
Fiberoptic bronchoscopy with BAL was performed by clinician’s decision as part of routine care. The procedure consisted of instillation/suction of three consecutive syringe volumes (50 mL each) of sterile saline into a distal bronchus during fiberoptic bronchoscopy. The washed territory was usually the most abnormal on chest imaging. The first syringe (5 to 20 mL) of re-aspired bronchoalveolar lavage fluid (BALF) was dedicated exclusively to bacteriological investigations (for more details regarding the microbiological workup, see the electronic supplementary material (ESM)). A BALF sample (minimum 15 mL) was systematically sent to the cytology laboratory, with a paired blood sample (EDTA) for concomitant cytological analysis. The remaining collected BALF was dispensed in dry tubes for routine laboratories (virology, mycology, parasitology, see the ESM).
Routine blood tests were performed daily as part of routine care. On the day of BAL, blood from dry tubes was centrifuged at 1600 rpm for 7 min at 4 °C, and serum was aliquoted (200 µL) and stored at − 80 °C less than 2 h after sampling for biochemical investigations.
Cytological analysis (BALF and blood)
The total cell count of BALF was determined using a KOVA cell chamber. BALF was then centrifuged (200 g for 5 min at 10 °C), the cell pellet was diluted in phosphate buffered saline, and May–Grunwald–Giemsa-stained cytocentrifuge preparations (Cytospin 3; Shandon Scientific, Cheshire, UK) were performed to assess differential cell counts (macrophages, lymphocytes, and neutrophils). BALF cell-free supernatants were stored at − 80 °C less than 2 h after sampling.
Blood and BALF (same-day samples) lymphocyte phenotyping were performed as part of routine care. In fresh whole blood, the absolute count and percentage of lymphocyte subpopulations were measured with an AQUIOS flow cytometer (Beckman Coulter) as per manufacturer instructions for use. BALF lymphocyte phenotyping was done after filtration, two washes of BALF cells, and staining with TetraCHROME CD45-FITC/CD4-PE/CD8-ECD/CD3-PC5 antibody cocktail (Beckman Coulter, #6607013). Data were acquired and analyzed on a Navios flow cytometer (Beckman Coulter).
Biochemical investigations (BALF and blood)
Cytokines
Cytokine concentrations were measured in frozen/thawed BALF cell-free supernatant and serum (same-day samples). Cytokine abbreviations are all gathered in the ESM. The Simoa™ (single molecule array) HD-1 analyzer (Quanterix, Lexington, MA, USA) was used for the ultrasensitive immunodetection (digital ELISA) of granulocyte–macrophage colony-stimulating factor (GM-CSF), interleukin-2 (IL-2), interferon-α (IFN-α), and vascular endothelial growth factor (VEGF) using single-plex bead-based assays, according to manufacturer instructions. The Quanterix® SP-X™ imaging and analysis platform allowed determination of the concentrations of IL-1β, IL-4, IL-5, IL-6, IL-8, IL-10, IL-12p70, IL-22, IFN-γ, and tumor necrosis factor-α (TNF-α) using the Human CorPlex Cytokine Panel Array from Quanterix Corporation. B-cell activating factor (BAFF) concentrations were quantified using ELISA kits from R&D Systems (Bio-Techne, Lille, France). Each cytokine concentration in the samples was interpolated from the calibration curve by multiplying it by the dilution factor, and the concentration was then expressed in pg/mL. Samples with non-detectable values were evaluated according to the limit of detection value (LOD); samples above the detection range were replaced by the upper limit of quantification (ULOQ).
Eicosanoids
Eicosanoid metabolomic analysis was adapted and performed, as previously described elsewhere, in serum23,24 and in BALF cell-free supernatants25. Eicosanoid abbreviations are all gathered in the ESM. Briefly, 100 µL of serum or 1 ml of BALF cell-free supernatant was supplemented with an internal standard mix (Cayman Chemical, Interchim France) consisting of 6 deuterated species (for details, see the ESM). Lipid metabolites were isolated by solid phase extraction from a 60 mg Strata X column (Phenomenex, Le Pecq, France). The extracted samples were evaporated and reconstituted in 100 µL of mobile phase (H20/ACN/Acetic Acid, 60/40/0.02). The eicosanoids were separated by reversed-phase liquid chromatography using a Kintex Evo C18 column (Phenomenex). The molecular species were analyzed by tandem quadrupole mass spectrometer (6500QTrap, ABSciex, Les Ulis France) operated in the negative-ionization mode via multiple-reaction monitoring (113 MRM) of M-H > Fragment transitions that were optimized for selectivity and sensitivity26. Quantification was performed using MultiQuant 2.1 software (ABSciex). Twenty-five external standards (for details, see the ESM) were assayed under the same conditions, and quantitation was achieved by the stable isotope dilution method. External standards included two eicosanoid mixtures prepared by Cayman Chemical (for details, see the ESM). Semi-quantitative analyses were performed for the other lipid species, including 82 molecular species.
Data processing and statistical analysis
Patients were grouped according to their D28-WHO-CPS. A value higher than 5 (D28-WHO-CPS > 5) defined a poor 28-day outcome, whereas a value equal to or lower than 5 (D28-WHO-CPS ≤ 5) defined a good 28-day outcome. A value higher than 5 meant either that the patient needed organ support(s) (high flow oxygen or non-invasive ventilation or mechanical ventilation, and/or dialysis, and/or vasopressors, and/or extra-corporeal membrane oxygenation) or that the patient was deceased.
Continuous data were expressed as median [first through third quartiles] and were compared using the non-parametric Mann–Whitney test. Categorical data were expressed as a number (percentage) and were evaluated using the chi-square test or Fischer exact test. Two-sided p values less than 0.05 were considered significant.
Biological data were combined and subjected to multivariate analysis and regression versus the 28-day WHO-CPS category. The raw data were processed with multivariate data analysis SIMCA 15 software (Sartorius-Umetrics, Västerbotten, Sweden). Prior to modeling, a principal component analysis (PCA) was achieved in order to define the major trends in the overall variability of the biological data using a non-supervised approach. Secondly, orthogonal partial least-squares discriminant analysis (OPLS-DA) was performed after scaling the variables with unit-variance (UV) scaling. Such a statistical analysis was conducted to assess whether immune-inflammatory biomarkers from the BALF and blood are associated with the 28-day outcome.
Ethical considerations
This study was approved by the institutional review board of Sorbonne University (Reference CER-2020-54) according to French regulations. All participants (or their relatives) gave consent to participate.
Results
Patient selection
During the study period, 178 consecutive patients with severe COVID-19 were admitted to the ICU of Tenon Hospital, 82 of whom underwent a fiberoptic bronchoscopy with BAL, at a median time of 2.5 [1-6] days after ICU referral and 13 [9-17] days after symptom onset. The main reason for performing a fiberoptic bronchoscopy with BAL was to rule out a coinfection and/or a superinfection, especially when respiratory tract secretions were scarce, which made it difficult for clinicians to collect endotracheal aspirate. During the first wave of the pandemic in France (February 15th to May 31st), 39/102 (38%) patients underwent a fiberoptic bronchoscopy with BAL, as compared with 43/76 (57%) during the second wave (June 1st to December 15th). The procedure failed to provide exploitable fluid in 6 patients. The remaining 76 patients (38 recruited during each wave) were studied (Fig. 1).
Clinical characteristics and outcomes of the study population
Baseline characteristics of the study population, management, and outcomes are reported in Table 1. Briefly, the patients included 54 (71%) males, were aged 64 [52–70] years, were moderately overweight, and frequently had comorbidities and immunosuppression (n = 21; 28%). Forty-five (59%) patients had a D28-WHO-CPS > 5. As compared with their counterparts, patients with a poor 28-day outcome were older and less likely to be obese.
Despite a higher frequency of acute kidney injury on ICU admission in patients with a poor 28-day outcome, the baseline severity according to the SAPS II, SOFA score, WHO-CPS, and biomarkers such as C-reactive protein and lymphopenia did not differ between the groups.
Corticosteroids, mainly hydrocortisone, were administered to most patients. No patient received antiviral drugs. Patients with a poor 28-day outcome experienced a more complicated course, with a higher incidence of ICU-acquired pneumonia and a greater need for organ support. The median length of ICU stay was 21 [13-38] days. Overall, the 28-day was 20% (for more details regarding the distribution of the study population over the classes of D28-WHO-CPS, see Table A in the ESM).
Characteristics of BAL
Most BAL procedures (95%) were performed on intubated and mechanically ventilated patients, with a median time from ICU admission to BAL collection of 2.5 [1-6] days and a median time from intubation to BAL collection of 1 [1-4] day. The timing of BAL and specific therapies received on or before the day of BAL did not differ between groups (Table 2). Forty-one patients underwent a CT-scan in the 4 days preceding BAL (for more details regarding the investigations performed for each patient, see Table B in the ESM). Patients with a D28-WHO-CPS > 5 had a higher incidence of extensive lesions (> 50% of lung parenchyma involvement) as compared with their counterparts. The median volume of BALF recovery was 60 [50–75] mL, with no difference between groups. The BALF culture enabled the diagnosis of bacterial coinfection in 14 (18%) patients, and no additional bacterial documentation was obtained using other specimens such as blood or urine. A SARS-CoV-2 reverse transcriptase polymerase chain reaction (RT-PCR) was performed in the BALF of 43 patients. No difference was observed between groups regarding either its positivity rate or the cycle threshold (Ct) value in positive patients.
Cytological findings
The total BALF cell count of did not differ between groups, whereas marked differences were observed in the differential cell counts (Table 3). Patients with a poor 28-day outcome displayed a neutrophil-predominant phenotype, while the others exhibited a macrophage-predominant phenotype. No obvious link was observed between the neutrophil count and the bacterial documentation in BALF (Fig. 2; see also Figure A in the ESM). The BALF and blood lymphocyte count, and the phenotyping did not differ between groups. Eventually, patients with a poor 28-day outcome displayed a much higher BALF neutrophil/lymphocyte ratio, as compared with their counterparts.
Contributions of main cellular types (macrophages, lymphocytes and neutrophils) in bronchoalveolar lavage fluid in critically ill COVID-19 patients, according to the 28-day WHO-CPS. Stacked bars represent the percentages of macrophages (green), lymphocytes (grey) and neutrophils (red) in bronchoalveolar lavage fluid (BALF). Each vertical line represents data from one single patient. Stars point out patients with a bacterial documentation in BALF. Patients were grouped according to the World Health Organization 10-point Clinical Progression Scale (WHO-CPS) at 28-day. A score value higher than 5 (D28-WHO-CPS > 5) defined a poor 28-day outcome, whereas a score value equal or lower than 5 (D28-WHO-CPS ≤ 5) defined a good 28-day outcome.
Cytokine findings
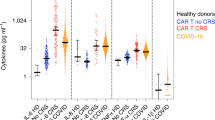
Fifteen cytokines were quantified in the BALF (n = 58) and blood (n = 52) (same-day samples) (Fig. 3). In line with neutrophil-predominant phenotypes, we observed higher BALF and blood concentrations of IL-8 (p < 0.05) in patients with D28-WHO-CPS > 5, as compared with their counterparts. We then calculated the BALF/blood ratio for the concentration for each cytokine (Figure B and C, in the ESM). Compared with patients having a good 28-day outcome, we observed in those with a poor 28-day outcome a decompartmentalized acute phase response, with a higher blood concentration of IL-6 (67.2 [22.4–156] vs. 29.3 [14.7–38.7]; p = 0.006) but lower BALF/blood ratios for IL-6 (1.68 [0.30–4.41] vs. 9.53 [2.56–19.1]; p = 0.001), IL-10 (0.17 [0.07–1.00] vs. 1.57 [0.26–3.10]; p = 0.003], and IFN-γ (0.79 [0.17–2.86] vs. 2.69 [1.38–7.66); p = 0.022)]. Additionally, we observed in patients with a poor 28-day outcome a lesser local type I IFN response, with a lower BALF concentration and BALF/blood ratio of concentration (p < 0.05) for IFN-α.
Cytokine profiling of blood and bronchoalveolar lavage fluid in critically ill COVID-19 patients, according to the 28-day WHO-CPS. Data are presented as box and whiskers plots (N = 26–32 per group). Patients were grouped according to the World Health Organization 10-point Clinical Progression Scale (WHO-CPS) at 28-day. A score value higher than 5 (D28-WHO-CPS > 5) defined a poor 28-day outcome, whereas a score value equal or lower than 5 (D28-WHO-CPS ≤ 5) defined a good 28-day outcome. Groups were compared using the non-parametric Mann–Whitney test for bronchoalveolar lavage fluid (BALF) concentrations, BALF/blood ratio of concentrations and blood concentrations of each cytokine. All the concentrations are expressed in pg/mL.
Regarding cytokines that reflect an adaptative immune response, we observed in patients with a poor 28-day outcome several signals that suggested a decompartmentalized adaptative response, with lower BALF/blood ratios for IL-2, IL-5, and IL-22 (p < 0.05), and a trend toward a lower BALF/blood ratio for BAFF. Finally, we quantified the growth factor VEGF in both BALF and blood, and we observed a higher BALF concentration in patients with a poor 28-day outcome compared with their counterparts (9.32 [3.29–22.8) vs. 4.03 [1.20–18.9]; p = 0.024).
Multivariate analysis and eicosanoid findings
The eicosanoid metabolomic work-up allowed to detect and quantify 107 molecular species (absolute quantification and semi-quantitative analysis of 25 and 82 molecular species, respectively) in BALF (n = 42) and blood (n = 42) (same-day samples). This inflammatory lipidome included a variety of bioactive lipid mediators that play a critical role in the regulation of inflammation. The complexity of the pathways involved led us to explore the dynamic lipidome in both the local (BALF) and systemic (blood) compartments during SARS-CoV-2 infection using liquid chromatography – mass spectrometry (LC/MS). The relative proportion of metabolites derived from arachidonic acid through cyclooxygenase (COX), lipoxygenase (LOX), and cytochrome P450 pathways, as well as metabolites derived from linoleic acid, linolenic acid, docosahexaenoic acid, and eicosapentaenoic acid were determined to assess the composition of bioactive lipids in blood and BALF. The selected panel included lipid mediators involved in pro- and anti-inflammatory processes. All the lipid metabolites, as well as the cytokines (BALF, blood and BALF/blood ratios) and cell counts were included in a multivariate analysis, which was intended to identify biological profiles associated with clinical outcomes. Multivariate analysis was restricted to the patients (n = 42) for whom all the biological data were available. The variables were screened stepwise according to their respective variable influence on projection (VIP) (Figures D, in the ESM). Among the 20 most discriminating laboratory variables (Fig. 4), 11 were eicosanoids in BALF (11,12-epoxy-5Z,8Z,14Z-eicosatrienoic acid (11,12-EET); 12S-hydroxy-5Z,8E,10E-heptadecatrienoic acid (12-HHTrE); 20-hydroxy-5Z,8Z,11Z,14Z-hydroxyeicosatetraenoic acid (20-HETE); thromboxane B2 (TxB2)) and blood (4-hydroxy-5E,7Z,10Z,13Z,16Z,19Z-docosahexaenoic acid (4-HDoHE); 8,9-epoxy-5Z,11Z,14Z-eicosatrienoic acid (8,9-EET); 11,12-EET; 20-HETE; adrenic acid; 5-hydroxy-6E,8Z,11Z,14Z,17Z-eicosapentaenoic acid (5-HEPE); 5-oxo-6E,8Z,11Z,14Z-eicosatetraenoic acid (5-oxo-ETE)), 7 were cytokines in blood (TNF-α, IL-5, IL-8), BALF (IFN-α) and the BALF/blood ratio (IL-6, IL-10, IFN-γ), and 2 were cell variables (BALF percentages of neutrophils and macrophages). The univariate comparison test focusing on eicosanoids confirmed these findings. We observed, in particular, a vascular endothelial injury eicosanoid signature in both blood and lung compartments, with higher blood concentrations of 8,9-EET and 11,12-EET (p < 0.05) and higher BALF concentrations of 20-HETE and TxB2 (p < 0.05) in patients with a poor 28–day outcome, as compared with their counterparts (Fig. 5). In addition, we observed increased blood concentrations of the neutrophil-active eicosanoids 4-HDoHE and 5-oxo-ETE (p < 0.05), as well as a tendency toward 5-HEPE (precursor of 5-oxo-6E,8Z,11Z,14Z,17Z-eicosapentaenoic acid (5-oxo-EPE)) in patients with a poor 28–day outcome, as compared with their counterparts.
Supervised orthogonal partial least squares discriminant analysis (OPLS-DA) obtained from critically ill COVID-19 patients, according to 28-day WHO-CPS. Patients were grouped according to the World Health Organization 10-point Clinical Progression Scale (WHO-CPS) at 28-day. A score value higher than 5 (D28-WHO-CPS > 5) defined a poor 28-day outcome, whereas a score value equal or lower than 5 (D28-WHO-CPS ≤ 5) defined a good 28-day outcome. (A) Loading plots summarize the relationship of the 20 most discriminating variables labeled according to their association to D28-WHO-CPS ≤ 5 (green dots) and D28-WHO-CPS > 5 (red dots). (B) VIP (Variable Influence on Projection) plots summarize the importance of the 20 most discriminating variables. Histogram is colored according to the variable associations to D28-WHO-CPS ≤ 5 (green bars) and D28-WHO-CPS > 5 (red bars). BALF bronchoalveolar lavage fluid.
Eicosanoid profiling of blood and bronchoalveolar lavage fluid of critically ill COVID-19 patients, according to the 28-day WHO-CPS. Data are presented as box and whiskers plots (N = 16–26 per group). Patients were grouped according to the World Health Organization 10-point Clinical Progression Scale (WHO-CPS) at 28-day. A score value higher than 5 (D28-WHO-CPS > 5) defined a poor 28-day outcome, whereas a score value equal or lower than 5 (D28-WHO-CPS ≤ 5) defined a good 28-day outcome. Groups were compared using the non-parametric Mann–Whitney test for bronchoalveolar lavage fluid (BALF) concentrations and blood concentrations of each eicosanoid. All the concentrations are expressed in pg/mL.
Discussion
Here, we report a series of 76 critical COVID-19 patients with immune-inflammatory marker assays on peripheral and alveolar samples, including extensive cytokine and eicosanoid analysis in 42 of them. Our findings, represented schematically in Figures E and F (in the ESM), are as follows: 1/ a neutrophil-predominant bronchoalveolar phenotype with a high neutrophil/lymphocyte ratio was associated with a poor 28-day outcome; 2/ cytokine and eicosanoid profiles were suggestive of a vascular endothelial injury and a decompartmentalized immune response, but a lesser type I IFN response in the subset of patients having a WHO-CPS value of 6 or greater at 28 days; 3/using a multi-marker approach, we identified an immune-inflammatory biomarker signature associated with the 28-day outcome.
In the cytological description of the bronchoalveolar landscape in the early stages of critical COVID-19, we identified a mixed alveolitis, with neutrophils as the main cellular type, in line with previous reports in severe SARS-CoV-2 infection27,28 and other virus-associated lower respiratory tract infections29,30. We found an association between the BALF neutrophil percentage and the clinical outcome in line with the trend observed by Pandolfi et al.27. In addition, we observed an elevated neutrophil/lymphocyte ratio in the BALF of patients with a poor 28-day outcome, in accordance with previous studies that identified the prognosis value of this ratio in blood in the early stages of COVID-1931,32.
Neutrophils are key effector cells in the acute phase response, but they may be responsible for host damage through the release of granule proteolytic enzymes, generation of reactive oxygen species, and production of extracellular traps when their local recruitment is intense and prolonged, as observed in the lungs of critically ill COVID-19 patients33,34,35. Accordingly, we observed a very high pulmonary-to-systemic gradient for IL-8, a key neutrophil chemoattractant36, which was almost ten times more concentrated in BALF than in blood, as previously reported37. In patients with a 28-day poor outcome, we observed higher BAL and blood concentrations of IL-8, in line with previous reports showing its association with COVID-19 severity38,39. Altogether, our findings support a marked neutrophil-predominant alveolar phenotype in patients with a poor 28-day outcome, which may participate in the dysregulated innate immune response in severe COVID-19, as reported in severe influenza infection40.
Qualitative anomalies of circulating neutrophils, reported as immature and/or dysfunctional, have also been described in severe COVID-19 patients34,41,42,43,44,45. In our study, the analysis of the eicosanoid metabolites brought additional insights. Two potent stimulators (5-oxo-ETE and 5-HEPE, precursor of 5-oxo-EPE) of neutrophil intrinsic functions such as migration, degranulation, and aggregation, which are produced by neutrophils themselves and act through autocrine-paracrine signaling46, were increased in the blood samples of patients with a poor 28-day outcome. Additionally, the blood concentration of 4-HDoHE, an eicosanoid produced from docosahexaenoic acid through the 5-lipoxygenase pathway by a wide variety of immune cells including neutrophils, showed a similar increment (p < 0.05) in patients with a poor 28-day outcome. Our findings are in line with those of Tam et al., who observed that 5-lipoxygenase-derived mediators were strongly correlated with severity in a mouse model of influenza infection47. Cell–cell interactions play a putative role in COVID-19-associated pulmonary vascular injury, especially interactions involving neutrophils and activated endothelial cells48,49. Accordingly, several biomarkers of endothelial activation and/or injury have been shown to be significantly elevated in severe COVID-19 patients; some of these biomarkers are correlated with an increased mortality43,50,51,52,53. In line with those findings, we observed a significantly higher BAL concentration of VEGF, a pro-angiogenic factor expressed under hypoxia, in patients with a poor 28-day outcome as compared with their counterparts. Moreover, the lipidomic analysis showed elevated BALF concentrations of the vasoactive eicosanoids TxB2 and 20-HETE in patients with a poor 28-day outcome. TxB2 is derived from TxA2, and it has been shown to play a key role in neutrophil adhesion and endothelium activation in experimental models of acute lung injury54. 20-HETE, one of the main cytochrome P450-dependent eicosanoids, is a hypoxia-induced mediator of oxidative stress and pulmonary arterial smooth muscle proliferation in murine pulmonary hypertension55. Interestingly, 20-HETE has been shown to promote endothelial dysfunction through the NF-κB signaling of vascular angiotensin-converting enzyme mRNA56. In our study, this eicosanoid signature of vascular injury was also evidenced in the systemic compartment, as patients with a poor 28-day outcome displayed higher blood concentrations of cytochrome P450-dependent vasoactive lipids 8,9-EET, and 11,12-EET than did their counterparts57,58.
COVID-19-associated pulmonary vascular injury may lead to a loss of integrity in the air-blood barrier59. The subsequent leak of alveolar fluid determines the loss of lung compartmentalization, as was illustrated for murine ventilator-induced lung injury decades ago60 and in isolated lung models61,62. Hyperpermeability may promote the extravasation of pro-inflammatory mediators from alveoli to the systemic compartment, ultimately leading to a marked systemic inflammatory response and subsequent multi-organ failure63. As an illustration, Hadjhadj et al. described a high IL-6 protein level within the blood but a low RNA level, suggesting high pulmonary production followed by massive release to the systemic compartment, especially in the most severe patients9. Accordingly, we described lower BAL/blood ratios for IL-6, IFN-γ, and IL-10 in patients with a poor 28-day outcome, as has been reported in patients with pneumonia-related ARDS for the main pro-inflammatory cytokines64.
Several limitations of our study can be underlined. First, our study was monocentric and used a number of patients that could be augmented in the future. Second, changes in therapeutic management between the first and second waves of the pandemic could be a source of variability. Third, biological work-up was not completely achieved in all patients, resulting in missing data in cytokines and eicosanoids analysis. This highlighted the difficulty to conduct translational research in a context of pandemic-driven ICU overload. Third, we chose a composite endpoint (28-day WHO-CPS), which had been previously used in cohorts of severely ill COVID-19 patients65,66,67. Indeed, considering the predictable hospital mortality, we did not choose hospital death as primary endpoint, because the relative low frequency of the event (death) would have favored the absence of difference between groups. Finally, for a better understanding of the disease, in vitro metabolomic studies on affected cells could corroborate the statistical associations between initial biological profiles and clinical outcomes.
Conclusions
In critically ill COVID-19 patients with a poor 28-day outcome, we observed a neutrophil-predominant bronchoalveolar phenotype, a blunted type I IFN local response, and a vascular endothelial injury that resulted in a decompartmentalized immune-inflammatory response.
Data availability
De-identified individual-participant data underlying the findings described in this manuscript can be shared upon reasonable request.
Abbreviations
- 4-HDoHE:
-
4-Hydroxy-5E,7Z,10Z,13Z,16Z,19Z-docosahexaenoic acid
- 5-HEPE:
-
5-Hydroxy-6E,8Z,11Z,14Z,17Z-eicosapentaenoic acid
- 5-HETE-d8:
-
5-Hydroxyeicosatetraenoic acid-d8
- 5-oxo-ETE:
-
5-Oxo-6E,8Z,11Z,14Z-eicosatetraenoic acid
- 5-oxo-EPE:
-
5-Oxo-6E,8Z,11Z,14Z,17Z-eicosapentaenoic acid
- 8,9-EET:
-
8,9-Epoxy-5Z,11Z,14Z-eicosatrienoic acid
- 11,12-EET:
-
11,12-Epoxy-5Z,8Z,14Z-eicosatrienoic acid
- 12-HETE:
-
12S-hydroxy-5Z,8Z,10E,14Z-eicosatetraenoic acid
- 12-HETrE:
-
12S-hydroxy-8Z,10E,14Z-eicosatrienoic acid
- 12-HHTrE:
-
12S-hydroxy-5Z,8E,10E-heptadecatrienoic acid
- 14(15)-EET:
-
14(15)-Epoxy-5Z,8Z,11Z-eicosatrienoic acid
- 18-HEPE:
-
18-Hydroxy-5Z,8Z,11Z,14Z,16E-eicosapentaenoic acid
- 20-HETE:
-
20-Hydroxy-5Z,8Z,11Z,14Z- hydroxyeicosatetraenoic acid
- Adrenic:
-
Adrenic acid
- BAFF:
-
B-cell activating factor
- BAL:
-
Bronchoalveolar lavage
- BALF:
-
Bronchoalveolar lavage fluid
- CFU:
-
Colony forming unit
- CMV:
-
Cytomegalovirus
- COX:
-
Cyclooxygenase
- CT-scan:
-
Computed-tomography scan
- EDTA:
-
Ethylenediaminetetraacetic acid
- ELISA:
-
Enzyme-linked immunosorbent assay
- GM-CSF:
-
Granulocyte–macrophage colony-stimulating factor
- ICU:
-
Intensive care unit
- IFN:
-
Interferon
- IL:
-
Interleukin
- LC/MS:
-
Liquid chromatography–mass spectrometry
- LOX:
-
Lipoxygenase
- PCR:
-
Polymerase chain reaction
- RT-PCR:
-
Reverse transcriptase polymerase chain reaction
- TNF:
-
Tumor necrosis factor
- Tx:
-
Thromboxane
- VEGF:
-
Vascular endothelial growth factor
- WHO-CPS:
-
World health organization 10-point clinical progression scale
References
Salje, H. et al. Estimating the burden of SARS-CoV-2 in France. Science 369(6500), 208–211 (2020).
Karagiannidis, C. et al. Case characteristics, resource use, and outcomes of 10 021 patients with COVID-19 admitted to 920 German hospitals: An observational study. Lancet Respir. Med. 8(9), 853–862 (2020).
Lewnard, J. A. et al. Incidence, clinical outcomes, and transmission dynamics of severe coronavirus disease 2019 in California and Washington: Prospective cohort study. BMJ 369, m1923 (2020).
Docherty, A. B. et al. Features of 20 133 UK patients in hospital with covid-19 using the ISARIC WHO clinical characterisation protocol: Prospective observational cohort study. BMJ 369, m1985 (2020).
Clinical characteristics and day-90 outcomes of 4244 critically ill adults with COVID-19: A prospective cohort study. Intensive Care Med. 47(1), 60–73 (2021).
Rouzé, A. et al. Relationship between SARS-CoV-2 infection and the incidence of ventilator-associated lower respiratory tract infections: A European multicenter cohort study. Intensive Care Med. 47(2), 188–198 (2021).
Ferrando, C. et al. Clinical features, ventilatory management, and outcome of ARDS caused by COVID-19 are similar to other causes of ARDS. Intensive Care Med. 46(12), 2200–2211 (2020).
Richards-Belle, A. et al. COVID-19 in critical care: Epidemiology of the first epidemic wave across England, Wales and Northern Ireland. Intensive Care Med. 46(11), 2035–2047 (2020).
Hadjadj, J. et al. Impaired type I interferon activity and inflammatory responses in severe COVID-19 patients. Science 369(6504), 718–724 (2020).
Zhou, R. et al. Acute SARS-CoV-2 infection impairs dendritic cell and T cell responses. Immunity 53(4), 864–877 (2020).
Arunachalam, P. S. et al. Systems biological assessment of immunity to mild versus severe COVID-19 infection in humans. Science 369(6508), 1210–1220 (2020).
Leisman, D. E. et al. Cytokine elevation in severe and critical COVID-19: A rapid systematic review, meta-analysis, and comparison with other inflammatory syndromes. Lancet Respir. Med. 8(12), 1233–1244 (2020).
Dorgham, K. et al. Distinct cytokine profiles associated with COVID-19 severity and mortality. J. Allergy Clin. Immunol. 147(6), 2098–2107 (2021).
Sterne, J. A. C. et al. Association between administration of systemic corticosteroids and mortality among critically ill patients with COVID-19: A meta-analysis. JAMA 324(13), 1330–1341 (2020).
Bost, P. et al. Host-viral infection maps reveal signatures of severe COVID-19 patients. Cell 181(7), 1475-1488.e12 (2020).
Liao, M. et al. Single-cell landscape of bronchoalveolar immune cells in patients with COVID-19. Nat. Med. 26(6), 842–844 (2020).
Blot, M. et al. CXCL10 could drive longer duration of mechanical ventilation during COVID-19 ARDS. Crit. Care 24(1), 632 (2020).
Dentone, C. et al. Bronchoalveolar lavage fluid characteristics and outcomes of invasively mechanically ventilated patients with COVID-19 pneumonia in Genoa, Italy. BMC Infect. Dis. 21(1), 353 (2021).
Le Gall, J. R., Lemeshow, S. & Saulnier, F. A new simplified acute physiology score (SAPS II) based on a European/North American multicenter study. JAMA 270(24), 2957–2963 (1993).
Supady, A. et al. Outcome prediction in patients with severe COVID-19 requiring extracorporeal membrane oxygenation—A retrospective international multicenter study. Membranes 11(3), 170 (2021).
Vincent, J. L. et al. The SOFA (Sepsis-related Organ Failure Assessment) score to describe organ dysfunction/failure On behalf of the Working Group on Sepsis-Related Problems of the European Society of Intensive Care Medicine. Intensive Care Med. 22(7), 707–710 (1996).
A minimal common outcome measure set for COVID-19 clinical research. Lancet Infect. Dis. 20(8): e192–7 (2020).
Deems, R. et al. Detection and quantitation of eicosanoids via high performance liquid chromatography-electrospray ionization-mass spectrometry. Methods Enzymol. 432, 59–82 (2007).
Quehenberger, O. et al. Lipidomics reveals a remarkable diversity of lipids in human plasma. J. Lipid Res. 51(11), 3299–3305 (2010).
Thakare, R. et al. Simultaneous LC-MS/MS analysis of eicosanoids and related metabolites in human serum, sputum and BALF. Biomed. Chromatogr. BMC 32, 3 (2018).
Dumlao, D. S. et al. High-throughput lipidomic analysis of fatty acid derived eicosanoids and N-acylethanolamines. Biochim. Biophys. Acta 1811(11), 724–736 (2011).
Pandolfi, L. et al. Broncho-alveolar inflammation in COVID-19 patients: A correlation with clinical outcome. BMC Pulm. Med. 20(1), 301 (2020).
Zhou, Z. et al. Heightened innate immune responses in the respiratory tract of COVID-19 patients. Cell Host Microbe 27(6), 883-890.e2 (2020).
Choi, S.-H. et al. Usefulness of cellular analysis of bronchoalveolar lavage fluid for predicting the etiology of pneumonia in critically ill patients. PLoS ONE 9(5), e97346 (2014).
Guihot, A. et al. Low titers of serum antibodies inhibiting hemagglutination predict fatal fulminant influenza A(H1N1) 2009 infection. Am. J. Respir. Crit. Care Med. 189(10), 1240–1249 (2014).
Liu, J. et al. Neutrophil-to-lymphocyte ratio predicts critical illness patients with 2019 coronavirus disease in the early stage. J. Transl. Med. 18(1), 206 (2020).
Fu, J. et al. The clinical implication of dynamic neutrophil to lymphocyte ratio and D-dimer in COVID-19: A retrospective study in Suzhou China. Thromb. Res. 192, 3–8 (2020).
Grant, R. A. et al. Circuits between infected macrophages and T cells in SARS-CoV-2 pneumonia. Nature 590(7847), 635–641 (2021).
Parackova, Z. et al. Disharmonic inflammatory signatures in COVID-19: Augmented neutrophils’ but impaired monocytes’ and dendritic cells’ responsiveness. Cells 9, 10 (2020).
Shaath, H. et al. Single-cell transcriptome analysis highlights a role for neutrophils and inflammatory macrophages in the pathogenesis of severe COVID-19. Cells 9, 11 (2020).
Kunkel, S. L. et al. Interleukin-8 (IL-8): The major neutrophil chemotactic factor in the lung. Exp. Lung Res. 17(1), 17–23 (1991).
Ronit, A. et al. Compartmental immunophenotyping in COVID-19 ARDS: A case series. J. Allergy Clin. Immunol. 147(1), 81–91 (2021).
Li, S. et al. Clinical and pathological investigation of patients with severe COVID-19. JCI Insight 5, 12 (2020).
Zhang, X. et al. Viral and host factors related to the clinical outcome of COVID-19. Nature 583(7816), 437–440 (2020).
Camp, J. V. & Jonsson, C. B. A role for neutrophils in viral respiratory disease. Front. Immunol. 8, 550 (2017).
Schulte-Schrepping, J. et al. Severe COVID-19 is marked by a dysregulated myeloid cell compartment. Cell 182(6), 1419-1440.e23 (2020).
Silvin, A. et al. Elevated calprotectin and abnormal myeloid cell subsets discriminate severe from mild COVID-19. Cell 182(6), 1401-1418.e18 (2020).
Meizlish, M. L. et al. A neutrophil activation signature predicts critical illness and mortality in COVID-19. Blood Adv. 5(5), 1164–1177 (2021).
Nicolai, L. et al. Immunothrombotic dysregulation in COVID-19 pneumonia is associated with respiratory failure and coagulopathy. Circulation 142(12), 1176–1189 (2020).
Combadière, B. et al. LOX-1-expressing immature neutrophils identify critically-ill COVID-19 patients at risk of thrombotic complications. Front. Immunol. 12, 752612 (2021).
Powell, W. S. & Rokach, J. Biosynthesis, biological effects, and receptors of hydroxyeicosatetraenoic acids (HETEs) and oxoeicosatetraenoic acids (oxo- ETEs) derived from arachidonic acid. Biochim. Biophys. Acta 1851(4), 340–355 (2015).
Tam, V. C. et al. Lipidomic profiling of influenza infection identifies mediators that induce and resolve inflammation. Cell 154(1), 213–227 (2013).
Gu, S. X. et al. Thrombocytopathy and endotheliopathy: Crucial contributors to COVID-19 thromboinflammation. Nat. Rev. Cardiol. 18(3), 194–209 (2021).
Laforge, M. et al. Tissue damage from neutrophil-induced oxidative stress in COVID-19. Nat. Rev. Immunol. 20(9), 515–516 (2020).
Ackermann, M. et al. Pulmonary vascular endothelialitis, thrombosis, and angiogenesis in Covid-19. N. Engl. J. Med. 383(2), 120–128 (2020).
Goshua, G. et al. Endotheliopathy in COVID-19-associated coagulopathy: Evidence from a single-centre, cross-sectional study. Lancet Haematol. 7(8), e575–e582 (2020).
Young, B. E. et al. Viral dynamics and immune correlates of COVID-19 disease severity. Clin. Infect. Dis. 73(9), e2932–e2942 (2020).
White, D. et al. Evaluation of COVID-19 coagulopathy; laboratory characterization using thrombin generation and nonconventional haemostasis assays. Int. J. Lab. Hematol. 43(1), 123–130 (2021).
Zarbock, A., Singbartl, K. & Ley, K. Complete reversal of acid-induced acute lung injury by blocking of platelet-neutrophil aggregation. J. Clin. Invest. 116(12), 3211–3219 (2006).
Wang, J. et al. Role of 20-hydroxyeicosatetraenoic acid in pulmonary hypertension and proliferation of pulmonary arterial smooth muscle cells. Pulm. Pharmacol. Ther. 64, 101948 (2020).
Garcia, V. et al. 20-HETE activates the transcription of angiotensin-converting enzyme via nuclear factor-κB translocation and promoter binding. J. Pharmacol. Exp. Ther. 356(3), 525–533 (2016).
Zhu, D. et al. Epoxyeicosatrienoic acids constrict isolated pressurized rabbit pulmonary arteries. Am. J. Physiol. Lung Cell Mol. Physiol. 278(2), L335-343 (2000).
Pozzi, A. et al. Characterization of 5,6- and 8,9-epoxyeicosatrienoic acids (5,6- and 8,9-EET) as potent in vivo angiogenic lipids. J. Biol. Chem. 280(29), 27138–27146 (2005).
Wu, M. A. et al. Hypoalbuminemia in COVID-19: Assessing the hypothesis for underlying pulmonary capillary leakage. J. Intern. Med. 289(6), 861–872 (2021).
Haitsma, J. J. et al. Ventilator-induced lung injury leads to loss of alveolar and systemic compartmentalization of tumor necrosis factor-alpha. Intensive Care Med. 26(10), 1515–1522 (2000).
Tutor, J. D. et al. Loss of compartmentalization of alveolar tumor necrosis factor after lung injury. Am. J. Respir. Crit. Care Med. 149(5), 1107–1111 (1994).
Tremblay, L. et al. Injurious ventilatory strategies increase cytokines and c-fos m-RNA expression in an isolated rat lung model. J. Clin. Invest. 99(5), 944–952 (1997).
Parsons, P. E. et al. Lower tidal volume ventilation and plasma cytokine markers of inflammation in patients with acute lung injury. Crit. Care Med. 33(1), 1–6 (2005).
Bendib, I. et al. Alveolar compartmentalization of inflammatory and immune cell biomarkers in pneumonia-related ARDS. Crit. Care 25(1), 23 (2021).
Writing Committee for the REMAP-CAP Investigators, Estcourt LJ, Turgeon AF, McQuilten ZK, et al. Effect of convalescent plasma on organ support-free days in critically ill patients with COVID-19: A randomized clinical trial. JAMA 326(17), 1690–1702 (2021).
Kyriazopoulou, E. et al. Early treatment of COVID-19 with anakinra guided by soluble urokinase plasminogen receptor plasma levels: A double-blind, randomized controlled phase 3 trial. Nat. Med. 27(10), 1752–1760 (2021).
Ghosn, L. et al. Interleukin-6 blocking agents for treating COVID-19: a living systematic review. Cochrane Database Syst. Rev. 3(3), 13881 (2021).
Acknowledgements
Authors thank all the health professionals who cared for the patients.
Author information
Authors and Affiliations
Contributions
G.V., M.F. and A.L. designed the study. D.F., G.T. and T.E. performed lipidomics. K.D., C.P. and Gu.Go. performed cytokine dosages. L.M.J. performed viral investigations. A.F. and C.P. performed cytological analysis. Gr.Ge. did the biobanking. V.L., C.B., A.G., M.D., M.T., A.E. and A.P. recruited ICU patients and contributed to the acquisition of clinical data. G.V., G.B. and A.L. performed statistical analysis. G.V. drafted the manuscript. K.D., A.F., L.M.J., G.T., A.P., J.C., Gu.Go., M.F. and A.L. revised the manuscript critically for important intellectual content. All authors approved the final version of the manuscript. G.V. had full access to all the data and takes responsibility for the integrity of the data.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Voiriot, G., Dorgham, K., Bachelot, G. et al. Identification of bronchoalveolar and blood immune-inflammatory biomarker signature associated with poor 28-day outcome in critically ill COVID-19 patients. Sci Rep 12, 9502 (2022). https://doi.org/10.1038/s41598-022-13179-0
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41598-022-13179-0
This article is cited by
-
Cell and cytokine analyses from bronchoalveolar lavage in non-critical COVID-19 pneumonia
Internal and Emergency Medicine (2023)
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.