Abstract
There are knowledge gaps regarding healthy lifestyle (HLS) interventions in fire academy settings and also concerning the impacts of the pandemic on training. We enrolled fire recruits from two fire academies (A and B) in New England in early 2019 as the historical control group, and recruits from academies in New England (B) and Florida (C), respectively, during the pandemic as the intervention group. The three academies have similar training environments and curricula. The exposures of interest were a combination of (1) an HLS intervention and (2) impacts of the pandemic on training curricula and environs (i.e. social distancing, masking, reduced class size, etc.). We examined the health/fitness changes throughout training. The follow-up rate was 78%, leaving 92 recruits in the historical control group and 55 in the intervention group. The results show an HLS intervention improved the effects of fire academy training on recruits healthy behaviors (MEDI-lifestyle score, 0.5 ± 1.4 vs. − 0.3 ± 1.7), systolic blood pressure (− 7.2 ± 10.0 vs. 2.9 ± 12.9 mmHg), and mental health (Beck Depression score, − 0.45 ± 1.14 vs. − 0.01 ± 1.05) (all P < 0.05). The associations remained significant after multivariable adjustments. Moreover, a 1-point MEDI-lifestyle increment during academy training is associated with about 2% decrement in blood pressures over time, after multivariable adjustments (P < 0.05). Nonetheless, the impacts of pandemic restrictions on academy procedures compromised physical fitness training, namely in percent body fat, push-ups, and pull-ups.
Similar content being viewed by others
Introduction
Accumulating evidence shows firefighting can lead to not only acute accidents and injuries1,2, but also to chronic disease3,4,5. Occupational hazards such as chemicals, extreme temperature, particles, and heavy physical demands due to firefighting have been widely investigated6,7, while emerging evidence discloses an unhealthy nutritional environment and sedentary behavior, which may contribute to chronic lifestyle-related diseases that are prevalent among firefighters3,8,9, including cancers, obesity, hypertension, cardiomegaly, coronary heart disease and other cardiovascular disease (CVD)4,5,8,10.
Physical fitness is of great interest in public safety workforces. Positive associations have been observed between physical fitness and training performance, lower occupational injury rates, decreased risk of subsequent CVD events, and decreased mortality11,12,13,14,15,16. Despite physical fitness requirements during academy training17, most fire departments do not require ongoing fitness training and most firefighters are obese/ overweight18. Studies have shown fire academy training does improve fire recruits’ health and fitness, but most of the benefits are lost soon after recruits become probationary firefighters17,19. A work environment that includes long sedentary periods, inadequate fitness requirements, insufficient and interrupted sleep, and a culture that may encourage unhealthy diets contributes to obesity, substandard fitness and chronic disease risks9.
Various preventive strategies and interventions have been attempted. Accumulating exercise interventions and physical training programs conducted among firefighters show positive effects on improving body composition, aerobic capacity, muscle power, endurance, and strength20,21. Other health promotion interventions including nutritional instruction and psychological resilience training also have beneficial effects on career firefighters’ body mass index (BMI), health behaviors, and mental health22,23,24.
Fire recruits are future firefighters who undergo academy training to be equipped with the professional skills and functional capacities needed for fire service. In the USA, fire academy training generally ranges between 12 and 20 weeks for career firefighters9. While existing evidence shows that academy training improves fire recruits’ physical fitness17, our previous study demonstrated that recruits’ blood pressures, both systolic and diastolic, increased by more than 2 mmHg throughout the training on average, despite other improved health parameters19. In addition, in the same study, we found that traditional academy training did not improve recruits’ dietary behaviors19. To our knowledge, while quite a few intervention studies on career firefighters have been conducted20,21,22,23,24, there is no existing health behavior/ lifestyle intervention research on fire recruits, although evidence has shown that early health education does have long-lasting health benefits25 and a healthy lifestyle (HLS) can be a potential solution for firefighters’ health concerns9.
Since March 2020, the COVID-19 pandemic has affected millions of workers all around the world26. While mitigation policies such as lockdowns and remote work have been implemented, they are not applicable to essential occupations, including training new firefighters27. Previous literature has demonstrated the risk of cluster transmission of SARS-CoV-2 (the virus causing COVID-19) infection among fire academies and its associated mental health impacts28. In fact, as fire academies needed to keep running during the pandemic, some adjustments to the existing training curriculum have been adopted to comply with public health regulations, such as mandated masking and increased social distancing. These adjustments include limiting class size, canceling large-group activities, conforming to social distancing during physical training, etc. Little is known about whether such adjustments influence the quality of academy training and its associated effects on recruits’ health and fitness. Therefore, we conducted this study to investigate the effects of (1) a healthy lifestyle (HLS) intervention and (2) an adjusted training curriculum due to the COVID-19 pandemic, by comparing the recruits from intervened academy classes to historical controls.
Methods
Study design and study population
In this time-controlled intervention study, a historical control group was used to evaluate the effects of the interventions. Therefore, two fire recruit populations were enrolled; (a) the control group comprised of two classes of recruits going through the academy training with existing, pre-pandemic training curricula and (b) the intervention group consisted of two classes of recruits enrolled during the pandemic and also receiving an HLS intervention.
The control group was recruited in early 2019 from two fire academies (academy A and B) in the New England area19,29. Both academies provide a 15–16 week training program that meets National Fire Protection Association (NFPA)’s standards, NFPA 1001: Standard for Fire Fighter Professional Qualifications. Except for minor differences between the two (for example, academy B requires recruits to stay overnight in the academy on training days while recruits at academy A go home every day after training, and academy B provides additional aquatic classes as part of their physical training), the recruits comprising the historical control group across academies were comparable according to our previous19 and current studies.
For the intervention group, we enrolled fire recruits from one fire academy in New England (academy B) and one in Florida (academy C) in late 2020. The training in academy C resembles that in academy B, regarding NFPA standards and overnight staying requirement, with similar training durations of 15 and 13 weeks for academies B and C, respectively.
All enrolled fire recruits who were older than 18 years old and provided informed consent were included. Those who did not consent to participate in the study or lacking essential demographic information (i.e., age and sex) were excluded. The current study is part of the “Fire Recruit Health Study” approved by the Institutional Review Board of Harvard T.H. Chan School of Public Health (IRB18-1902). We followed the Declaration of Helsinki throughout the study.
Selected health outcomes
The outcomes selected for study included body composition, blood pressure, physical fitness testing, mental health screens, and lifestyle behaviors. All academies, except academy C, had complete data collection, while academy C provided only subjective outcomes (i.e. questionnaire). The related measurements were described in our previous studies19,29 and are summarized below.
Recruits’ BMI and percent body fat were examined as body composition outcomes. A clinic stadiometer (Portable Stadiometer 213, SECA, Hamburg, Germany) and a Bioelectrical Impedance Analysis scale (BIA) (BC-418 Segmental Body Composition, Tanita, Tokyo, Japan or InBody 230, Seoul, South Korea) using athletic mode, operated by experienced physical trainers or medical personnel, were used to retrieve the parameters. The measurements were performed at entry to the academy, mid-training (i.e. 8th week for academy A and 7th week for academy B), and academy graduation. Body composition data were not available at academy C.
Blood pressures were measured using an automated and calibrated sphygmomanometer (10 series, Omron, Kyoto, Japan), following professional guidelines30. The measurements were done before recruits started their daily training or during rest break. Each recruit was asked to rest seated for at least 5 min before being measured in a sitting position. The automated sphygmomanometer would then take three readings, with 1-min interval between each, and record an average. Blood pressures measurements were conducted at entry to academy and graduation, and were not available at academy C.
Select physical fitness outcomes were push-ups, pull-ups, and 1.5-mile running time, with each measurement taken at entry to academy, mid-training, and at graduation. These are existing tests used by the academies to evaluate recruits’ physical performance over time. Push-ups were determined as the number a recruit performed continuously in one minute, without breaking the cadence. Pull-ups were counted as the number in single trial with good cadence and overhead grip. Running time for 1.5 miles was recorded in minutes. Physical fitness testing results were not available at academy C.
We used a questionnaire to examine participants’ mental health and lifestyle behaviors, administered at their entry to the academy and at graduation. The questionnaire was comprised of components derived from validated questionnaires, incorporating a modified version of Beck Depression Inventory for Primary Care (BDI-PC) (total scoring 0–18)31, Patient Health Questionnaire (PHQ-9) (total scoring 0–27)32, and a modified version of Posttraumatic Stress Disorder Checklist (PCL-5) (total scoring 0–76)33, with higher scores indicating worse mental health. As to lifestyle behaviors, the questionnaire contained items needed to calculate the MEDI-lifestyle score29, which is a 7-item healthy lifestyle score ranging from 0 to 7, embodying BMI, smoking history, dietary pattern (measured by the PREDIMED score, a 14-item Mediterranean Diet adherence screener34), physical activity35, sedentary behavior (measured by time spent watching television), daily sleep time, and afternoon naps. In particular, one point was given for each of the following: no smoking in the last 6 months, physical activity equivalent to greater than 16 METs-h/wk, PREDIMED score more than or equal to nine points, BMI less than or equal to 30 kg/m2, TV screen time less than 2 h/day, sleeping time between 7 and 8 h/day, and taking daytime naps; otherwise a value of 0 would be given to each item.
Interventions
Compared with the historical control group, the intervened classes underwent the following changes in the existing training materials implemented by the academies.
First, the academies adopted an HLS intervention throughout the 13- or 15-week training based on the firefighters’ Mediterranean pyramid24, which illustrates a healthy lifestyle combination of balanced nutrition, regular physical activity, restorative sleep, positive social and family connections with resiliency strategies, and the avoidance of tobacco and other toxic substances. Each participant was given (a) access to a web-based toolkit (https://www.hsph.harvard.edu/firefighters-study/feeding-americas-bravest/) that includes information and resources for “Survival Mediterranean Style”, (b) a half-hour talk on healthy lifestyle at the entry to the academy training, (c) a waterproof, plastic paper sheet illustrating the firefighters’ Mediterranean pyramid, (d) a refrigerator magnet with the Mediterranean pyramid on it, (e) weekly nutrition/lifestyle tips throughout the academy training, and (f) an introduction to meditation/breathing exercise apps (for example, the Calm app (San Francisco, USA)). Except for (e), all intervention materials were given at the beginning of the academy training. The participants were able to review the HLS contents via the provided measures throughout the training period. While the practice of the HLS is voluntary, sponsored olive oil was supplied to the central kitchen of academy B and consumed by the fire recruits when they stayed at the academy on weekdays, and academy C gave each recruit of the intervened class a WHOOP (Boston, USA) wearable device that tracked recruits’ fitness and physiological parameters. Notably, weekly homework such as practicing a healthy recipe was assigned along with the weekly tips to the recruits. With the collaboration with the academies, extra training credits were given as incentives if the recruits showed their adherence to the HLS outside regular training time.
Second, as the intervention classes were trained during the COVID-19 pandemic, some curriculum adjustments were made to conform to public health policies. These changes included face masking required at all times during the training, limited class size, and shifting large group activities (such as group running) to small group physical training to increase social distancing. Moreover, previously there was a weekly 1-h aquatic training in the swimming pool at academy B, but since the pool was closed, the aquatic classes were replaced by weekly 1-h joint mobility exercise, in which recruits conducted a whole-body slow paced, yoga-like stretching workout.
Statistical analysis
Baseline characteristics and select health outcomes were reported as mean ± standard deviation or median (Q1-Q3) for continuous variables after checking for normality, or number (%) for categorical variables, and compared between groups using the t-test or the Wilcoxon rank sum test, as appropriate, for continuous variables and the Pearson's Chi-squared test with Yates' continuity correction or the Fisher’s exact test, as appropriate, for categorical variables.
Furthermore, we computed the changes in select health outcomes over time during academy training by calculating the longitudinal difference “the measurement at graduation—the measurement at baseline”, and presenting them as mean ± standard deviation, after checking normality. The differences in temporal changes between the intervention group and the control group were compared using the t-test.
For multivariable adjustment, mixed effects models were built incorporating the interaction term “Intervention Group × Time” to examine whether the health changes over time during academy training differed between the two groups. Potential confounders based on our domain knowledge and the baseline characteristics comparisons were included into the models. These are age, sex, baseline percent body fat, baseline push-ups, and/or baseline BDI-PC scores.
Finally, we built multivariable adjusted linear models to regress the health changes on the change of MEDI-lifestyle score, in order to demonstrate the changes in health per unit changes of MEDI-lifestyle score. For these models, the health changes throughout training were defined as percent changes from baseline measurements, except for those variables with any values of zero at baseline (i.e. pull-ups, BDI-PC, PCL-5, and PHQ-9).
All P values reported are two-tailed and a P < 0.05 was considered statistically significant. We used the R software (version 3.6.3) to conduct the statistical analyses.
Sensitivity analysis
With regard to the differences in training across academies, we conducted further sensitivity analysis limiting to fire recruits at the academy with both historical control class and intervention class available, which is academy B. In fact, there was one more class at academy B that took place in early 2020, receiving the lifestyle intervention, but undergoing unexpected training interruption for 3 months due to the initial COVID-19 outbreak. By comparing the three classes at academy B (i.e. the historical control class, COVID-19 interrupted class, and the intervention class), we were able to examine the effects of the intervention as well as the impact of the 3-month training interruption on recruits’ health. Notably, only the body composition and fitness testing data are available for the COVID-19 interrupted class.
In addition, while there were differences in the intervention contents across the academies B and C, as described above, we further conducted secondary analyses to investigate if the health changes differed between the two populations (i.e., the fire recruits comprising the intervention group from academy B and C, respectively) throughout academy training. Since objective data were not available at academy C, only subjective measurements (i.e., behavioral and mental health outcomes) could be compared.
Ethics approval and consent to participate
The study is part of the “Fire Recruit Health Study”, which was approved by the Institutional Review Board of Harvard T.H. Chan School of Public Health (IRB18-1902), and we followed the Declaration of Helsinki throughout the study.
Results
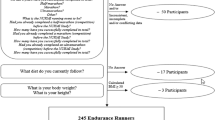
A total of 172 recruits were eligible for the main analyses, including 101 in the historical control group and 71 in the intervention group. Among them, 95 (94.1%) from the control group and 69 (97.2%) from the intervention group consented to participate. After excluding those with missing essential data (i.e. age and sex) and those failing to complete the academy training, 92 (91.1%) in the control arm, comprised of 56 from academy A and 36 from academy B, and 55 (77.5%) in the intervention arm, comprised of 37 from academy B and 18 from academy C, were included in the analyses.
There was no significant difference in recruits’ age (28.6 ± 5.1 years vs. 29.3 ± 5.2 years, P = 0.428) and sex (96.7% male vs. 100.0% male, P = 0.293) between the two groups, while the control group showed lower baseline percent body fat (20.5 ± 6.9% vs. 23.9 ± 7.2%, P = 0.013) and performed more baseline push-ups (37.7 ± 14.1 vs. 28.7 ± 10.9, P < 0.001) than the intervention group. Moreover, the intervention group reported more depressive symptoms (i.e. higher BDI-PC score) at baseline (BDI-PC IQR: 0–1 vs. 0–0, P = 0.013) (Table 1).
Table 2 demonstrates the select outcome changes over time during academy training. While both groups show decreased percent body fat and increased push-ups and pull-ups throughout training, less improvement is observed in the intervention group (percent body fat change: − 0.2 ± 2.8% vs. − 1.8 ± 3.5%, P = 0.013; push-ups change: 8.2 ± 4.9 vs. 16.8 ± 10.4, P < 0.001; pull-ups change: 2.8 ± 2.5 vs. 5.8 ± 5.1, P = 0.001). On the other hand, the intervention group reported more lifestyle improvement than the control (MEDI-lifestyle score change: 0.5 ± 1.4 vs. − 0.3 ± 1.7, P = 0.005), and a greater decrease in depressive symptoms (BDI-PC score change: − 0.45 ± 1.14 vs. − 0.01 ± 1.05, P = 0.023). In addition, systolic blood pressure was lowered in the intervention group but got higher in the control group throughout academy training (− 7.2 ± 10.0 mmHg vs. 2.9 ± 12.9 mmHg, P < 0.001) (Table 2, Fig. 1).
Box plots showing the distributions of recruits’ selected health profiles at baseline, mid-training, and academy graduation comparing (a) the historical control group (n = 92) and (b) the intervention group (n = 55). A. Body fat; B. systolic blood pressure; C. BDI-PC (Beck Depression Inventory for Primary Care); D. MEDI-lifestyle score; E. push-ups; F. pull-ups. The plots were derived from the recruits whose data were available at each time point. Post-hoc paired analysis with Holm adjustments were demonstrated by *P < 0.05, **P < 0.01, ***P < 0.001, ****P < 0.0001. Body fat, systolic blood pressure, push-ups, pull-ups, and MEDI-lifestyle score are only available for one academy of the intervention group (n = 37).
The associations remained significant after multivariable adjustments. Table 3 shows that the intervention group had less improvement in percent body fat, push-ups, and pull-ups over time, but more improvements in MEDI-lifestyle score, systolic blood pressure, and BDI-PC questionnaire, after accounting for recruits’ age, sex, baseline percent body fat, baseline push-ups, and/or baseline BDI-PC score (all P < 0.05 for the interaction term “Intervention Group × Time”).
In order to examine whether the changes in health (i.e. the difference “the measurement at graduation—the measurement at baseline”) were related to the changes in healthy lifestyle, we pooled both groups together and built multivariable linear regression models with the same covariates as the mixed models used for Table 3, with additional adjustments for different academy classes (i.e. control group or intervention group) to account for intervention effects. The results show that a 1-point MEDI-lifestyle increment during academy training is associated with 1.95% and 2.73% decrements in systolic and diastolic blood pressure, respectively (both P < 0.05). We did not observe significant associations between the change in MEDI-lifestyle score and other select health outcomes (Table 4).
In the sensitivity analyses limited to classes from academy B and adding one more class that received the healthy lifestyle intervention but sustained an unexpected 3-month training interruption due to the COVID-19 pandemic, we found no significant differences in the select outcomes when comparing the intervention class to the control. However, when comparing the COVID-19 interrupted class to the control, the recruits’ BMI decreased by 0.33 more per measurement time (i.e. baseline, mid-training, to graduation) than the control (P = 0.036) after multivariable adjustments. Nonetheless, the COVID-19 interrupted class shows an average of 1.3 fewer push-ups and 0.58 min additional running time for 1.5 mile run per measurement time than the control class (both P < 0.05 in the multivariable adjusted mixed effects models). When comparing the COVID-19 interrupted class with the intervention class, the difference in the 1.5 mile running time remained significant (0.58 min more per measurement time after multivariable adjustment, P < 0.001) (Supplemental Tables S1–S4, Supplemental Fig. S1).
For the secondary analyses comparing the health changes throughout academy training across academy B and C from the intervention group, there were no significant differences in the changes of PREDIMED score, physical activity, sleeping and napping behaviors, and the BDI-PC score. Nonetheless, those from the academy C showed more decreased TV screening time (− 1.21 ± 1.6 vs. − 0.14 ± 1.7 h/d, P = 0.029), more decreased PCL-5 score (− 4.3 ± 9.5 vs. − 0.2 ± 4.6, P = 0.045), and more decreased PHQ-9 score (− 1.7 ± 3.0 vs. 0.0 ± 1.5) throughout academy training.
Discussion
In our present intervention study using a historical control group, we investigated the combined effects of (1) a healthy lifestyle intervention and (2) an adjusted training curriculum due to the COVID-19 pandemic on fire recruits’ health and fitness during academy training. Our novel findings show the MEDI-lifestyle score increased over time by 0.5 points more in the intervention group than the control group, and systolic blood pressure and self-reported depressive symptoms had greater decrements during the training. In fact, each MEDI-lifestyle score increment during the study period is associated with 1.95% and 2.73% decrement in systolic and diastolic blood pressure, respectively. Nonetheless, we also found that the intervention group had smaller reductions in body fat and had less push-ups/pull-ups improvement than the control group, which is likely due to the pandemic-required adjustments in the training curriculum.
To our knowledge, the current work is the first lifestyle intervention study in a fire academy setting, while unfortunately that could not be a pure lifestyle intervention but one impacted by unprecedented adjustments in the training curriculum due to the pandemic. It is biologically implausible to attribute the finding of increased MEDI-lifestyle scores over time to pandemic-related restrictions in the curriculum. Therefore, it is likely that the lifestyle intervention does improve recruits’ healthy lifestyle behaviors. In fact, a Swiss study investigating the effect of a healthy eating promotion program on career firefighters shows modest improvements on eating habits after one-year follow-up36, although the findings were limited by a lack of control group and a small sample size (n = 28). Another study on fourteen volunteer firefighters demonstrated that a 30-min health promotion educational intervention increased participants’ health literacy37. Accordingly, our results show that the intervened fire recruits improved their HLS behaviors, using a well-defined control group, a more intensive lifestyle intervention, and an adequate follow-up period.
Significant decrements in blood pressures among the intervention group is another novel finding of our present study. For the control group, recruits receiving the existing fire academy curriculum actually had increased blood pressures throughout the training, despite improved body composition and physical fitness19. Since hypertension and CVD are prevalent diseases in the fire service workforce3,38, it is important to implement vascular health and blood pressure interventions39. In fact, evidence has shown that a greater adherence to a healthy dietary pattern is associated with better cardiometabolic profiles40,41. In addition, our previous research on fire recruits also demonstrates a negative association between healthy lifestyle adherence and hypertension prevalence29. In agreement with the literature, we found that the healthy lifestyle intervention group had lowered blood pressures during academy training, and per one point increment in MEDI-lifestyle score throughout training is associated with around 2% decrement in both systolic and diastolic blood pressure, highlighting the effectiveness of the healthy lifestyle intervention.
We found in the present study that recruits attending academy training during the COVID-19 pandemic were more depressed at baseline. While the qualification/ entry exams for becoming a fire recruit remained the same, it is not surprising that living through the pandemic would be associated with an increase in recruits’ depressive symptoms at baseline. In fact, evidence has shown psychological distress is of great public health concern among the general population in the midst of the pandemic42. The fear of being infected, a sense of liberty deprivation due to quarantine and lock-down, being socially isolated, and worrying about transmission among family members could all contribute to the substantial psychological impacts42,43,44,45,46. Fortunately, research demonstrates that adopting a healthy lifestyle has benefits against depression. In an 8-year prospective study of 14,908 participants who were initially depression-free, an optimal healthy lifestyle adherence (a combination of the Mediterranean diet, increased physical activity, optimal sleep pattern, decreased sedentary period, no smoking, moderate drinking, optimal BMI, and positive social connections) was associated with a 32% lower risk of incident depression47. Accordingly, we found the lifestyle-intervened recruits had more improved depressive symptoms throughout academy training than the historical control group. In addition, the findings of our secondary analyses are indicative of the potential effectiveness of wearable devices on fire recruits’ behavioral and mental health, as those given wearable devices (i.e., those from academy C) reported more improvement in TV screening time, PCL-5, and PHQ-9 scores.
To our knowledge, there is no existing literature examining how pandemic-related adjustments in training curricula could affect physical fitness. In our current study, the intervention group shows suboptimal training effects on recruits’ body fat and pull-up/push-up capacities, and a 3-month training interruption compromised recruits’ aerobic fitness (i.e. 1.5-mile running) improvements. In fact, research on the general population has shown the physical distancing and lock-down policies generally reduce people’s physical activity and fitness48,49. Despite a lack of evidence on fire recruits, firefighters, or other emergency respondents, professional recommendations for competitive athletes’ training during the pandemic have been conservative, with lower intensity and more flexibility50,51. Since long-term detraining could decrease muscle mass, strength, and endurance52, the observed decreased aerobic function improvement among the interrupted class is not surprising. In addition, a study on military recruits after a COVID-19 cluster outbreak shows decreased fitness among affected personnel, compared with others receiving the same military training53. Accordingly, we found an adjusted academy training curriculum due to the pandemic improved recruits’ fitness less than the historical control group. This is likely because of conservative changes made to the training, reduced self-exercise during rest time, and possible subclinical/ asymptomatic transmission among recruits. Therefore, future research is warranted to see if the academy training effects and capacities on physical fitness will meet pre-pandemic levels as the COVID-related restrictions are getting relaxed and herd immunity is increasing (due to vaccination and prior infection).
The present study has several strengths. First, we adopted a time-controlled design, using a historical control group as the reference, which is the most rigorous study design regarding the research aims. While fire recruits undergo academy training in groups, randomization at the individual level is inappropriate because of potential spillover effects54. Historical academy classes that had the same entry qualification exams ensure the exchangeability with the intervention classes. In addition, we adjusted for potential confounders to estimate the true associations. Third, almost all (> 94%) recruits in each group consented to participate in the study, and more than 75% of them completed the study follow-up. The relatively high participation and follow-up rate minimize possible selection bias. Finally, we used well-defined and validated tools to examine the health outcomes, freeing the study from information bias.
However, there are some limitations to our study. One of them is that we cannot test the pure effects of a single intervention. In the current study, the outcome differences are due to the combined effects from the two interventions (i.e. a lifestyle intervention and the pandemic related training curriculum adjustments). Although the effects could be differentiated based on existing literature and knowledge, there may be synergism or other interactions between the two interventions, which prevents us from identifying the pure effects due to either one of the exposures. Second, the objective measurements for the intervention group are not available at academy C, reducing the sample size and associated statistical power for those outcomes. Additionally, as the intervention classes took place in the midst of the pandemic, there may be unmeasured confounding factors related to the pandemic, such as decreased physical activity during weekends and rest time, reduced social contacts, and less traveling during holidays. Finally, since the present study was designed to examine the combined effects of all HLS intervention measures, we could not tell which individual measures are the most effective.
Conclusions
In conclusion, the present study shows fire recruits receiving a combination of a lifestyle intervention and COVID-19 related curriculum adjustments during academy training had more improvements than the historical control group with respect to HLS scores, blood pressure, and depressive symptoms. On the other hand, likely due to pandemic impacts on training, the intervention group experienced less improvement in body fat, push-ups, and pull-ups. In order to examine the real changes due to the intervention, a future study enrolling additional, post-pandemic academy classes that are more comparable to the historical control group and sustain a pure lifestyle intervention is warranted.
Data availability
The datasets used and/or analyzed in the current study are available from the corresponding author on reasonable request.
References
Orr, R., Simas, V., Canetti, E. & Schram, B. A profile of injuries sustained by firefighters: A critical review. Int. J. Environ. Res. Public Health. 16, 3931 (2019).
Frost, D. M., Beach, T. A., Crosby, I. & McGill, S. M. The cost and distribution of firefighter injuries in a large Canadian Fire Department. Work 55, 497–504 (2016).
Kales, S. N. & Smith, D. L. Firefighting and the heart: Implications for prevention. Circulation 135, 1296–1299 (2017).
Soteriades, E. S., Kim, J., Christophi, C. A. & Kales, S. N. Cancer incidence and mortality in firefighters: A state-of-the-art review and meta-analysis. Asian Pac. J. Cancer Prev. 20, 3221–3231 (2019).
Soteriades, E. S., Smith, D. L., Tsismenakis, A. J., Baur, D. M. & Kales, S. N. Cardiovascular disease in US firefighters: A systematic review. Cardiol. Rev. 19, 202–215 (2011).
Frost, D. M., Beach, T. A., Crosby, I. & McGill, S. M. Firefighter injuries are not just a fireground problem. Work 52, 835–842 (2015).
Marsh, S. M., Gwilliam, M., Konda, S., Tiesman, H. M. & Fahy, R. Nonfatal injuries to firefighters treated in U.S. emergency departments, 2003–2014. Am. J. Prev. Med. 55, 353–360 (2018).
Korre, M., Smith, D. & Kales, S. N. Obesity and health in the North American Fire Service: Research points the way to positive culture change. Occup. Med. (Lond). 68, 160–162 (2018).
Sotos-Prieto, M., Jin, Q., Rainey, D., Coyle, M. & Kales, S. N. Barriers and solutions to improving nutrition among fire academy recruits: A qualitative assessment. Int. J. Food Sci. Nutr. 70, 771–779 (2019).
Kales, S. N., Soteriades, E. S., Christophi, C. A. & Christiani, D. C. Emergency duties and deaths from heart disease among firefighters in the United States. N. Engl. J. Med. 356, 1207–1215 (2007).
Bakker, E. A., Sui, X., Brellenthin, A. G. & Lee, D. C. Physical activity and fitness for the prevention of hypertension. Curr. Opin. Cardiol. 33, 394–401 (2018).
Baur, D. M., Christophi, C. A., Tsismenakis, A. J., Cook, E. F. & Kales, S. N. Cardiorespiratory fitness predicts cardiovascular risk profiles in career firefighters. J. Occup. Environ. Med. 53, 1155–1160 (2011).
Bycura, D. K., Dmitrieva, N. O., Santos, A. C., Waugh, K. L. & Ritchey, K. M. Efficacy of a goal setting and implementation planning intervention on firefighters’ cardiorespiratory fitness. J. Strength Cond. Res. 33, 3151–3161 (2019).
Yang, J. et al. Association between push-up exercise capacity and future cardiovascular events among active adult men. JAMA Netw Open. 2, e188341. https://doi.org/10.1001/jamanetworkopen.2018.8341 (2019).
Korre, M. et al. Recruit fitness and police academy performance: a prospective validation study. Occup. Med. (Lond). 69, 541–548 (2019).
Durand, G. et al. Firefighters’ physical activity: Relation to fitness and cardiovascular disease risk. Med. Sci. Sports Exerc. 43, 1752–1759 (2011).
Cornell, D. J., Gnacinski, S. L., Meyer, B. B. & Ebersole, K. T. Changes in health and fitness in firefighter recruits: An observational cohort study. Med. Sci. Sports. Exerc. 49, 2223–2233 (2017).
Poston, W. S. et al. The prevalence of overweight, obesity, and substandard fitness in a population-based firefighter cohort. J. Occup. Environ. Med. 53, 266–273 (2011).
Lan, F. Y. et al. The effects of fire academy training and probationary firefighter status on select basic health and fitness measurements. Med. Sci. Sports Exerc. 53, 740–748 (2021).
Andrews, K. L., Gallagher, S. & Herring, M. P. The effects of exercise interventions on health and fitness of firefighters: A meta-analysis. Scand. J. Med. Sci. Sports. 29, 780–790 (2019).
Hollerbach, B. S., Jahnke, S. A., Poston, W. S. C., Harms, C. A. & Heinrich, K. M. Examining a novel firefighter exercise training program on simulated fire ground test performance, cardiorespiratory endurance, and strength: A pilot investigation. J. Occup. Med. Toxicol. 14, 12 (2019).
Antony, J. et al. Interventions for the prevention and management of occupational stress injury in first responders: a rapid overview of reviews. Syst. Rev. 9, 121 (2020).
MacMillan, F., Kolt, G. S., Le, A. & George, E. S. Systematic review of randomised control trial health promotion intervention studies in the fire services: study characteristics, intervention design and impacts on health. Occup. Environ. Med. https://doi.org/10.1136/oemed-2020-106613 (2020).
Korre, M., Sotos-Prieto, M. & Kales, S. N. Survival Mediterranean Style: Lifestyle changes to improve the health of the US fire service. Front. Public Health. 5, 331 (2017).
Messineo, A., Cattaruzza, M. S., Prestigiacomo, C., Giordano, F. & Marsella, L. T. Sustainability of prevention practices at the workplace: Safety, simplification, productivity and effectiveness. Ann. Ig. 29, 407–421 (2017).
Lan, F.-Y., Wei, C.-F., Hsu, Y.-T., Christiani, D. C. & Kales, S. N. Work-related COVID-19 transmission in six Asian countries/areas: A follow-up study. PLoS One. 15, e0233588. https://doi.org/10.1371/journal.pone.0233588 (2020).
Lancet, T. The plight of essential workers during the COVID-19 pandemic. Lancet 395, 1587 (2020).
Walecka, I. et al. Psychological consequences of hospital isolation during the COVID-19 pandemic - research on the sample of polish firefighting academy students. Curr. Psychol. https://doi.org/10.1007/s12144-021-01982-3 (2021).
Lan, F.-Y. et al. A Mediterranean lifestyle is associated with lower hypertension prevalence and better aerobic capacity among New England firefighter recruits. J. Occup. Environ. Med. 62, 466–471 (2020).
Whelton, P. K. et al. 2017 ACC/AHA/AAPA/ABC/ACPM/AGS/APhA/ASH/ASPC/NMA/PCNA Guideline for the prevention, detection, evaluation, and management of high blood pressure in adults: Executive Summary: A report of the American College of Cardiology/American Heart Association Task Force on Clinical Practice Guidelines. Hypertension 71, 1269–1324 (2018).
Winter, L. B., Steer, R. A., Jones-Hicks, L. & Beck, A. T. Screening for major depression disorders in adolescent medical outpatients with the Beck Depression Inventory for Primary Care. J. Adolesc. Health. 24, 389–394 (1999).
Spitzer, R. L., Kroenke, K. & Williams, J. B. Validation and utility of a self-report version of PRIME-MD: the PHQ primary care study. Primary Care Evaluation of Mental Disorders. Patient Health Questionnaire. JAMA. 282, 1737–1744 (1999).
Ashbaugh, A. R., Houle-Johnson, S., Herbert, C., El-Hage, W. & Brunet, A. Psychometric validation of the English and French versions of the Posttraumatic Stress Disorder Checklist for DSM-5 (PCL-5). PLoS One. 11, e0161645. https://doi.org/10.1371/journal.pone.0161645 (2016).
Papadaki, A. et al. Validation of the English version of the 14-Item Mediterranean Diet adherence screener of the PREDIMED Study, in people at high cardiovascular risk in the UK. Nutrients 10, 138 (2018).
Godin, G., Jobin, J. & Bouillon, J. Assessment of leisure time exercise behavior by self-report: A concurrent validity study. Can. J. Public Health. 77, 359–362 (1986).
Bucher Della Torre, S., Wild, P., Dorribo, V., Amati, F. & Danuser, B. Eating habits of professional firefighters: Comparison with national guidelines and impact healthy eating promotion program. J Occup Environ Med. 61, e183-e90 (2019).
Palmer, A. S. & Yoos, J. L. Health promotion in volunteer firefighters: Assessing knowledge of risk for developing cardiovascular disease. Workplace Health Saf. 67, 579–583 (2019).
Kales, S. N., Tsismenakis, A. J., Zhang, C. & Soteriades, E. S. Blood pressure in firefighters, police officers, and other emergency responders. Am. J. Hypertens. 22, 11–20 (2009).
Getty, A. K. et al. Effects of circuit exercise training on vascular health and blood pressure. Prev. Med. Rep. 10, 106–112 (2018).
Romanidou, M. et al. Association of the Modified Mediterranean Diet Score (mMDS) with anthropometric and biochemical indices in US career firefighters. Nutrients 12, 3693 (2020).
Yang, J., Farioli, A., Korre, M. & Kales, S. N. Modified Mediterranean diet score and cardiovascular risk in a North American working population. PLoS One. 9, e87539; https://doi.org/10.1371/journal.pone.0087539 (2014).
Kunzler, A. M. et al. Mental health and psychosocial support strategies in highly contagious emerging disease outbreaks of substantial public concern: A systematic scoping review. PLoS One. 16, e0244748. https://doi.org/10.1371/journal.pone.0244748 (2021).
Brooks, S. K. et al. The psychological impact of quarantine and how to reduce it: Rapid review of the evidence. Lancet 395, 912–920 (2020).
Pandey, D. et al. Psychological impact of mass quarantine on population during pandemics-The COVID-19 Lock-Down (COLD) study. PLoS One. 15, e0240501. https://doi.org/10.1371/journal.pone.0240501 (2020).
Qiu, J., Shen, B., Zhao, M., Wang, Z., Xie, B. & Xu, Y. A nationwide survey of psychological distress among Chinese people in the COVID-19 epidemic: implications and policy recommendations. Gen Psychiatr. 33, e100213. https://doi.org/10.1136/gpsych-2020-100213 (2020).
Wang, C. et al. Immediate psychological responses and associated factors during the initial stage of the 2019 Coronavirus Disease (COVID-19) epidemic among the general population in China. Int. J. Environ. Res. Public Health. 17, 1729 (2020).
Ruiz-Estigarribia, L. et al. Lifestyles and the risk of depression in the “Seguimiento Universidad de Navarra” cohort. Eur. Psychiatry. 61, 33–40 (2019).
Bourdas, D. I. & Zacharakis, E. D. Impact of COVID-19 lockdown on physical activity in a sample of Greek adults. Sports (Basel). 8, 139 (2020).
To, Q. G., Duncan, M. J., Van Itallie, A. & Vandelanotte, C. Impact of COVID-19 on physical activity among 10,000 steps members and engagement with the program in Australia: Prospective study. J. Med. Internet. Res. 23, e23946. https://doi.org/10.2196/23946 (2021).
Toresdahl, B. G. & Asif, I. M. Coronavirus disease 2019 (COVID-19): Considerations for the competitive athlete. Sports Health. 12, 221–224 (2020).
Tayech, A. et al. Second wave of COVID-19 global pandemic and athletes’ confinement: Recommendations to better manage and optimize the modified lifestyle. Int. J. Environ. Res. Public Health. 17, 8385. https://doi.org/10.3390/ijerph17228385 (2020).
Paoli, A. & Musumeci, G. Elite Athletes and COVID-19 lockdown: Future health concerns for an entire sector. J. Funct. Morphol. Kinesiol. 5, 30 (2020).
Crameri, G. A. G. et al. Reduced maximal aerobic capacity after COVID-19 in young adult recruits, Switzerland, May 2020. Euro Surveill. 25, 542. https://doi.org/10.2807/1560-7917.ES.2020.25.36.2001542 (2020).
Benjamin-Chung, J. et al. Spillover effects in epidemiology: Parameters, study designs and methodological considerations. Int. J. Epidemiol. 47, 332–347 (2018).
Acknowledgements
The paper is dedicated to the memory of Captain William DeFord who continues to inspire all of us.
Funding
The present study is funded by Rappaport Institute for Greater Boston, John F. Kennedy School of Government, at Harvard University. This investigation was made possible by Grant No. T42 OH008416 from the National Institute for Occupational Safety and Health (NIOSH). Its contents are solely the responsibility of the authors and do not necessarily represent the official views of the NIOSH.
Author information
Authors and Affiliations
Contributions
F.Y.L., C.A.C., D.C.C., M.S.P., and S.N.K. formulated the study question and research design. F.Y.L. performed the statistical analyses. C.A.C., D.C.C., M.S.P., and S.N.K. consulted on the analyses. F.Y.L. and S.N.K. drafted the manuscript. F.Y.L., C.S., M.S.H., J.L.R.C., G.C.G., I.Y., A.F.M., and S.N.K. worked on data methods, data acquisition and data verification. All authors contributed to the interpretation of data and critical revision of the manuscript, and approved the final version.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Lan, FY., Scheibler, C., Hershey, M. et al. Effects of a healthy lifestyle intervention and COVID-19-adjusted training curriculum on firefighter recruits. Sci Rep 12, 10607 (2022). https://doi.org/10.1038/s41598-022-10979-2
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41598-022-10979-2
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.