Abstract
In the United States, 100,000–300,000 patients die from venous thromboembolism (VTE) each year, with more than 500,000 people related hospitalizations. While in Europe, 500,000 people die from VTE each year. Patients with rheumatoid arthritis are at increased risk of VTE. The use of biologics in patients with rheumatoid arthritis may be associated with an increased risk of VTE. We identified all patients who had been newly approved for Catastrophic Illness Card of rheumatoid arthritis extracted the claims data from the National Health Insurance research database and Registry for Catastrophic Illness Patient Database from 2003 to 2016. VTE was defined as the presence of inpatient VTE diagnostic codes (including DVT or PE) according to the discharge diagnosis protocol. An analysis of VTE variables indicated that the incidence of VTE in the biologic group (14.33/10,000 person-years) was higher than that in the conventional drug group (12.61/10,000 person-years). As assessed by the Cox proportional hazards model, the relative HR for VTE in the biologic group (HR: 1.11; 95% CI 0.79–1.55) versus that in the conventional drug group did not reach a significant difference. In conclusion, this study found no significant differences in risk were observed between the use of conventional DMARDs and biologics.
Similar content being viewed by others
Introduction
Deep vein thrombosis (DVT) is the formation of a blood clot in a deep vein, primarily occurring in the leg, which can lead to permanent damage. Pulmonary embolism (PE) is a potentially life-threatening condition that occurs in the lungs and causes sudden death in 25% of cases1,2,3. DVT and PE occurring together constitute venous thromboembolism (VTE). In the United States, 100,000 to 300,000 patients die from VTE each year, with more than 500,000 people related hospitalizations4,5,6. While in Europe, 500,000 people die from VTE each year7.
Patients with rheumatoid arthritis (RA) are at increased risk of VTE8,9. Several cohort studies in the United States, the United Kingdom, Sweden, and Taiwan have shown a significant association between rheumatoid arthritis and VTE10,11,12,13,14,15. However, previous studies have suggested that disease-modifying anti-rheumatic drugs (DMARDs) pose different risks of VTE. According to the study by the American College of Rheumatology (ACR) and the Association of Rheumatology Health Professionals (ARHP) presented at their 2013 meeting, the initiation of biologic drugs in patients with RA was associated with a 2.5-fold increased risk of VTE in the first 180 days16. In contrast, a cohort study conducted by the British Society for Rheumatology Biologics Registers (BSRBR) showed no significant association between tumor necrosis factor alpha (TNF-α) inhibitor treatment and VTE in patients with RA17.
Research on the association between DMARDs and VTE is limited. Studies on the association between biologics and VTE are scarce. We conducted a nationwide cohort study to analyze the risk and factors associated with VTE in patients with rheumatoid arthritis using different DMARDs in Taiwan.
Results
Patient selection
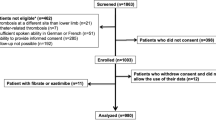
The study identified 35,409 patients with newly approved for Catastrophic Illness Card of rheumatoid arthritis using DMARDs from 2003 to 2016, and excluded: (1) 3,340 patients who had a total hip replacement or total knee replacement; (2) 123 patients who had VTE and PE prior to the index date; (3) 2060 patients who had other major injuries prior to the index date; (4) 692 patients who were under 18 years of age; and (5) 321 patients with incomplete data. (Fig. 1).
Demographic data
A total of 28,873 patients with rheumatoid arthritis were enrolled: 21,811 in the conventional drug group and 7062 in the biologic group (Table 1). In terms of sex and age, the majority of patients in both groups were female and the majority of patients in the conventional drug group were aged 45–54, while the majority of patients in the biologic group were aged 55–64. In respect of insured salary, both groups were prone to be in the range of NT$20,009–22,800. As for the CCI, the majority of patients in both groups had a score of 0, followed by a score of 1. In addition, most patients in both groups had no history of hypertension; had attended medical centers, primarily non-public hospitals and facilities; and tended to receive treatment from high-volume physicians.
Propensity score matching
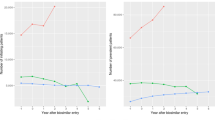
Ultimately, 14,124 patients in the conventional drug group and 7,062 patients in the biologic group were matched based on propensity score (Table 2). One hundred and ninety-five patients with VTE, including 143 in the conventional drug group and 52 in the biologic group, were hospitalized (Table 3). An analysis of VTE variables indicated that the incidence of VTE in the biologic group (14.33/10,000 person-years) was higher than that in the conventional drug group (12.61/10,000 person-years). Based on age stratification, both groups had a higher incidence of VTE among patients aged 75–100 (conventional drug group: 40.67/10,000 person-years; biologic group: 45.16/10,000 person-years). When stratified by CCI, both groups had a higher incidence of VTE in patients with CCI > 3 (conventional drug group: 37.89/10,000 person-years; biologic group: 23.55/10,000 person-years). Patients with lower extremity fractures in both groups had a higher incidence of VTE (conventional drug group: 47.34/10,000 person-years; biologic group: 167.08/10,000 person-years).
Cox proportional hazards model
As assessed by the Cox proportional hazards model (Table 3), the relative HR for VTE in the biologic group versus that in the conventional drug group was 1.11 (95% CI 0.79–1.55), but did not reach a significant difference (p > 0.05). Based on age stratification, the highest relative HR was found in the 75–100 years group (HR: 5.43, 95% CI 2.24–13.17, p < 0.05). In the stratified analysis by CCI, the highest relative HR was found in patients with CCI > 3 (HR: 2.20, 95% CI 1.26–3.24, p < 0.05). The relative HR for VTEwas 3.60 times higher in patients with lower extremity fractures than in those without (95% CI 1.58–8.02, p < 0.05).
Discussion
In this study, we compared the risk and factors associated with VTE in patients with rheumatoid arthritis using different DMARDs. The results revealed that the incidence of VTE was higher in the biologic group (14.33/10,000 person-years) than in the conventional drug group (12.61/10,000 person-years). The risk of VTE in the biologic group was 1.11 times higher than that of the conventional group, but this did not reach a level of significance.
Some studies have found that the use of TNF-α inhibitors in patients with rheumatoid arthritis reduces inflammation and coagulation markers, as well as decreases the inhibition of fibrinolysis and the incidence of VTE18,19. However, several studies have reported cases of VTE after treatment of rheumatoid arthritis or other inflammatory diseases with TNF-α inhibitors20,21,22,23,24.
The BSRBR prospective cohort study showed no significant association between TNF-α inhibitors and VTE in patients with rheumatoid arthritis, with an adjusted HR of 0.8 (95% CI 0.5–1.5)17. A French study indicated that treatment with TNF-α inhibitors increased the incidence of VTE, accounting for 4.5% of all spontaneously reported adverse reactions to the three TNF-α inhibitors in the database25. The findings presented at the 2013 meeting sponsored by the ACR and the ARHP showed that patients with rheumatoid arthritis were at an increased risk of VTE within 180 days of the initiation of biologics (HR: 2.48, 95% CI 1.14–5.40). The PS-decile stratification hazard ratio of VTE associated with biologic DMARDs was 1.83 (95% CI 0.91–3.66) versus nonbiologic DMARDs, but this did not reach significance16.
The results of this study were similar to the findings of the previously mentioned US and French studies. The adjusted HR for VTE did not reach a significance; however, given the higher incidence of VTE in the biologic group compared to the conventional drug group, possible clinical implications must be considered.
This study took into account the issue of non-differential misclassification, which may affect the results. Patients of biologic group may remain at risk of developing VTE from conventional DMARDs during the half-life of the drug following termination of treatment. For example, the most widely used MTX has an elimination half-life of 3–10 h and therefore requires a maximum of approximately 55 h for complete elimination. Furthermore, the average interval from cDMARD withdrawal, switching to bDMARD, to VTE was about 924 days based on the Table 4. In this study, the minimum time to develop VTE in the biologic group was found to be 77 days; therefore, this should not affect the results (Table 4).
As biologics are expensive, patients may choose to alter their treatment plan due to insurance coverage, and treatment deviations may affect the findings of this study. However, the current regulation for biologics use in Taiwan through national health insurance greatly reduces the possibility of such treatment deviations.
Outpatient follow-up of patients with VTE at a low risk of death (e.g., patients without congestive heart failure or severe hepatic insufficiency) was not included in this study26. Previous studies have shown that confirmation of outpatient VTE was less reliable and was not used in comparative studies of rheumatoid arthritis16,27. Therefore, despite underestimating the incidence of VTE, this study used patients with inpatient VTE only to improve comparability between treatment groups.
In previous studies, the incidence of VTE has been found to be related to age, fracture type, and chronic disease. The present study confirmed these independent risk factors. In a study from the US, increasing age was associated with a higher risk of VTE when using any conventional DMARD or biologic for therapy28. The same results were found in the present study, with incidence increasing with age. The relative hazard of VTE was higher at an older age, and patients aged 55 or older were considered a high-risk group, which could be related to reduced mobility. In addition, several studies have suggested a higher risk of VTE after lower extremity fracture29,30,31,32,33. In the present study, the risk of VTE in patients with lower extremity fractures was 3.6 times higher than that in those without, and lower extremity fractures also increased the risk of VTE. Further, previous studies have indicated that the incidence of VTE was associated with some chronic diseases34,35,36,37,38. In the present study, the risk of VTE was 2.20 times higher in patients with a CCI greater than 3. Thus, CCI modified the risk of VTE.
The strength of this study lies in the large sample size and the fact that two cohorts were collected simultaneously, which could not be achieved in a clinical trial. Despite the limitations of the observational design, the data from the two cohorts were primarily from medical facilities located throughout Taiwan and the data presented here reflect a real-world experience with DMARDs and biologics for the treatment of rheumatoid arthritis in Taiwan.
Despite great efforts to make adjustments in this study, it should be acknowledged that there may be potential bias caused by unmeasured or unknown variables. As disease severity is a criterion for RA treatment, patients using biologics tend to have more severe rheumatoid arthritis than those using conventional DMARDs39,40. A higher disease severity is appropriate in representing a pre-thrombotic state and may relate to reduced patient mobility may lead to venous stasis38,41,42,43,44. The NHIRD does not provide detailed information of RA severity scale, the data such as disease activity, functional impairment and physical damage was unavailable for the study patients. However, changes in disease severity during the follow-up period did not seem to affect the result much here. Further, some studies have shown that long-term steroid use increased the risk of VTE45,46. Since both groups of RA patients had similar conditions during the same time frame, the effect of steroid use on the results of this study would be reduced during the follow-up period.
Due to the limitation of the data contained in the NHIRD, the data related to body mass index and healthy behaviors (such as smoking, alcohol consumption, and exercise) were not available for the study patients; consequently, some important potential confounding factors were not included in the statistical analysis model for discussion. Although treatment and lifestyle changes may benefit from lack of exercise and obesity in RA patients, there is no clear evidence that these factors are related to accelerate atherosclerosis47. Besides, there may be a healthy patient effect in this study with RA patients using conventional drugs being excluded from the biologic group if they had VTE, and therefore, RA patients in the biologic group may have been in better health than those in the conventional drug group. This could have a biased effect on the study results. Additionally, this study population was a predominantly Asian population in Taiwan, and therefore, it may be inappropriate to apply the findings to other ethnic groups or regions with different rates of VTE. Because the incidence of VTE is very low and the total number of events relatively small, the confidence interval is wide, and the result lacks power. This is a study limitation, as type 2 error cannot be ruled out.
Conclusion
In summary, this study found no evidence that biologic therapy was associated with an increased risk of VTE in patients with rheumatoid arthritis, and no significant differences in risk were observed between the use of conventional DMARDs and biologics.
Methods
The study was a retrospective national population-based cohort study. We extracted the claims data from the National Health Insurance Research Database (NHIRD) and Registry for Catastrophic Illness Patient Database (RCIPD) provided by the Ministry of Health and Welfare. In Taiwan, The National Health Insurance (NHI) program covers 99.9% of the population, and under the insurance program, copayments for RA patients is waived48. The NHI administration has also included 93% of Taiwan’s health services organizations as NHI-contracted health care providers as of the end of 201448. Diagnoses of RA were coded according to the International Classification of Diseases, Ninth Revision, Clinical Modification (ICD-9-CM). Several previous studies had demonstrated the high accuracy and validity of ICD-9 diagnosis of major diseases listed in the NHIRD49,50. This study was approved by the Institutional Review Board of Taichung Veterans General Hospital (TCVGH-IRB No.: CE20255B) and was conducted in accordance with the Helsinki Declaration. Identification information of all patients was omitted prior to analysis. Since the patient identifications in the National Health Insurance Research Database have been de-identified by the Taiwan Ministry of Health and Welfare, the informed consent was waived by the Research Ethnics Committee of Taichung Veterans General Hospital.
Since biologic agents were available for treatment of RA in Taiwan in 2003, we identified all patients who had been newly approved for Catastrophic Illness Card of rheumatoid arthritis from 2003 to 2016, and the follow-up end point was set as December 31, 2017. The accuracy of diagnosis was validated based on ICD codes (ICD-9-CM 714.0–714.9) and inclusion in the RCIPD. The exclusion criteria for this study were as follows: (1) had a total hip arthroplasty or total knee arthroplasty (2) VTE and PE prior to the index date owing to a high recurrence rate of 7–14%6; (3) other major injuries or illness prior to the index date, which contains 30 categories of severe illness or injury defined by the NHI; (4) under 18 years of age; and (5) incomplete data in the NHIRD and TCRD. The exclusion period also included the years 2000–2002.
The two groups using DMARDs were defined as (1) a conventional DMARD group (cDMARD, including Methotrexate, Hydroxychloroquine, Sulfasalazine, Leflunomide, D-penicillamine, Azathioprine, Mycophenolate, Cyclosporine, Tafacitinib) and (2) a biologic DMARD group (bDMARD, including Etanercept, Adalimumab, Golimumab, Rituximab, Abatacept, Tocilizumab, Infliximab, Certolizumab). Subjects in the conventional drug group were not allowed to use biologics concurrently; however, they were allowed to use other DMARDs concurrently. In Taiwan, for the treatment with biologics should be through national health insurance requiring a detailed evaluation of the RA patient to meet the criteria including the 28 Disease Activity Score must be greater than 5.1 and failed other DMARDs therapy. Therefore, almost all patients in the bDMARD group using biologics were after cDMARDs withdrawal. And in some cases, it may switch to other bDMARDs, but not to other cDMARDs. Biologics use was defined in this study as any exposure to any biologic agent during the observation period. In both groups, the index date was defined as the date of first treatment (either with a conventional drug or biologics, dependent on group) until the date of first VTE, last follow-up, death, or end of observation period.
In this study, VTE was defined as the presence of inpatient VTE diagnostic codes (including DVT or PE) according to the discharge diagnosis protocol. The diagnostic codes for VTE were DVT (DVT: ICD-9-CM codes: 451.11, 451.19, 451.2x, 453.8x, and 453.9x) or PE (PE: ICD-9-CM codes: 415.11 and 415.19). The discharge notes and medical reimbursement of DVT and PE should be scrutinized by peer review.
Demographic data including age at the date of diagnosis confirmation were documented. The urbanization level ranged from highly developed urban cities (level 1) to remote districts (level 7)51. The degrees of comorbidity were categorized into three levels according to the Charlson comorbidity index (CCI) modified by Deyo52. The CCI score containing 19 medical issues was a useful method for evaluating medical comorbidities. Other variables included atrial fibrillation, hypertension, lower limb fracture, patients’ monthly salary, hospital level (medical centers, regional hospitals, district hospitals, and clinics), and the annual service volume of primary care physicians (low and high).
All statistical analyses were performed using SAS software, version 9.2 (SAS Institute Inc., Cary, NC, USA), and statistical significance was defined as p < 0.05. A chi-square test was applied to compare the distribution of each variable between the two groups at the beginning of the study (baseline characteristics). When we conducted the propensity score matching (PSM) method, the dependent variable was patients using conventional DMARD or biologic DMARD. The independent variables which were used in the logistic regression model included sex, age, severity of comorbidity (CCI), atrial fibrillation, and hypertension at the index date of the first biologic treatment. An SAS matching macro, %OneToManyMTCH, was used for the PSM. The PSM was performed by using the greedy nearest neighbor matching by digit without replacement to form a subject matching set with a 2:1 matching ratio on the propensity score. The algorithm performed the “best” match first, followed by the “next best” match in hierarchical sequence, until no more matches could be made. Best matches were those with the highest digit match on propensity score. Each control is selected at most once. The final matched-pair samples contain both closely matched individual pairs and balanced control and case group. Approximately 73% of total study population was matched in the final matched sample. Subsequently, a chi-square test was used to compare the incidence of VTE among patients with rheumatoid arthritis treated with different drug regimens and the Cox proportional hazards model was applied to assess the relative hazard and factors of VTE after controlling for other factors. The relative hazard was also shown using the total events of VTE, the incidence of VTE (defined as events per 10,000 person-years), the adjusted hazard ratio (HR), and 95% confidence interval (CI).
Data availability
Regarding the data availability, data were obtained from the National Health Insurance Research Database published by the Ministry of Health and Welfare, Taiwan. Due to legal restrictions imposed by the Taiwan government related to the Personal Information Protection Act, the database cannot be made publicly available. We confirm that the data used in our study can be used by any future researchers and we did not receive special privileges from the Ministry of Health and Welfare, Taiwan. All researchers can apply for using the databases to conduct their studies in the Science Center of the Ministry of Health and Welfare (http://www.mohw.gov.tw/EN/Ministry/Index.aspx). Any raw data are not allowed to be brought out from the Health and Welfare Data Science Center. The restrictions prohibited the authors from making the minimal data set publicly available. This study used anonymized secondary data retrieved from the Taiwan Cancer Registry Database and Taiwan’s National Health Insurance Research Database; consequently, the requirement for informed consent was waived by the ethics committee.
Code availability
Due to privacy and proprietary natures, no code in this study can be made available.
References
Caprini, J. A. et al. Economic burden of long-term complications of deep vein thrombosis after total hip replacement surgery in the United States. Value Health 6, 59–74 (2003).
Heit, J. A. et al. Relative impact of risk factors for deep vein thrombosis and pulmonary embolism: A population-based study. Arch. Int. Med. 162, 1245–1248 (2002).
Ollendorf, D. A., Vera-Llonch, M. & Oster, G. Cost of venous thromboembolism following major orthopedic surgery in hospitalized patients. Am. J. Health Syst. Pharm. 59, 1750–1754 (2002).
Heit, J. A., Cohen, A. T., & Anderson Jr, F. A. Estimated annual number of incident and recurrent, non-fatal and fatal venous thromboembolism (VTE) events in the US. Blood. 106, 910–910 (2005).
Geerts, W. H. et al. Prevention of venous thromboembolism: The seventh ACCP conference on antithrombotic and thrombolytic therapy. Chest 126, 338–400 (2004).
MacDougall, D. A., Feliu, A. L., Boccuzzi, S. J. & Lin, J. Economic burden of deep-vein thrombosis, pulmonary embolism, and post-thrombotic syndrome. Am. J. Health Syst. Pharm. 63(20 Suppl 6), S5–S15 (2006).
Cohen, A. et al. E Impact Assessment Group in Europe (VITAE). Venous thromboembolism (VTE) in Europe. The number of VTE events and associated morbidity and mortality. Thromb. Haemost. 98, 756–764 (2007).
Lazzerini, P. E. et al. Hyperhomocysteinemia, inflammation and autoimmunity. Autoimmun. Rev. 6, 503–509 (2007).
McLaughlin, G. E. Sudden death in rheumatoid arthritis: pulmonary embolism—A fatal complication of iliopsoas bursitis. J. Clin. Rheumatol. 8, 208–211 (2002).
Bacani, A. K., Gabriel, S. E., Crowson, C. S., Heit, J. A. & Matteson, E. L. Noncardiac vascular disease in rheumatoid arthritis: Increase in venous thromboembolic events?. Arthritis. Rheum. 64, 53–61 (2012).
Choi, H. K. et al. The risk of pulmonary embolism and deep vein thrombosis in rheumatoid arthritis: A UK population-based outpatient cohort study. Ann. Rheum. Dis. 72, 1182–1187 (2013).
Chung, W.-S. et al. Rheumatoid arthritis increases the risk of deep vein thrombosis and pulmonary thromboembolism: A nationwide cohort study. Ann. Rheum. Dis. 73, 1774–1780 (2014).
Kim, S. C., Schneeweiss, S., Liu, J. & Solomon, D. H. Risk of venous thromboembolism in patients with rheumatoid arthritis. Arthritis Care Res. 65, 1600–1607 (2013).
Ramagopalan, S. V., Wotton, C. J., Handel, A. E., Yeates, D. & Goldacre, M. J. Risk of venous thromboembolism in people admitted to hospital with selected immune-mediated diseases: Record-linkage study. BMC Med. 9, 1–8 (2011).
Zöller, B., Li, X., Sundquist, J. & Sundquist, K. Risk of pulmonary embolism in patients with autoimmune disorders: A nationwide follow-up study from Sweden. Lancet 379, 244–249 (2012).
Kim, S. C. et al. Risk of venous thromboembolism in patients with rheumatoid arthritis: Initiating disease-modifying antirheumatic drugs. Am. J. Med. 128(539), e537-539 (2015).
Davies, R. et al. Venous thrombotic events are not increased in patients with rheumatoid arthritis treated with anti-TNF therapy: Results from the British Society for Rheumatology Biologics Register. Ann. Rheum. Dis. 70, 1831–1834 (2011).
Ingegnoli, F. et al. Anti-tumor necrosis factor alpha therapy normalizes fibrinolysis impairment in patients with active rheumatoid arthritis. Clin. Exp. Rheumatol. 28, 254–257 (2010).
Sarlos, P. et al. Steroid but not biological therapy elevates the risk of venous thromboembolic events in inflammatory bowel disease: A meta-analysis. J. Crohns. Colitis. 12, 489–498 (2018).
Ingegnoli, F. et al. Inflammatory and prothrombotic biomarkers in patients with rheumatoid arthritis: Effects of tumor necrosis factor-alpha blockade. J. Autoimmun. 31, 175–179 (2008).
Makol, A., Grover, M., Guggenheim, C. & Hassouna, H. Etanercept and venous thromboembolism: A case series. J. Med. Case Rep. 4, 12 (2010).
Mortimore, M., Gibson, P. R., Selby, W. S., Radford-Smith, G. L. & Florin, T. H. Early Australian experience with infliximab, a chimeric antibody against tumour necrosis factor-alpha, in the treatment of Crohn’s disease: Is its efficacy augmented by steroid-sparing immunosuppressive therapy? The Infliximab User Group. Int. Med. J. 31, 146–150 (2001).
Yazici, Y., et al. FRI0009 Infliximab in the treatment of rheumatoid arthritis (ra): Referral patterns, response to treatment, and adverse events in a real world setting. Ann. Rheum. Dis. 60, A448–A449 (2001).
Yee, A. M. & Pochapin, M. B. Treatment of complicated sarcoidosis with infliximab anti-tumor necrosis factor-alpha therapy. Ann. Int. Med. 135, 27–31 (2001).
Petitpain, N. et al. Arterial and venous thromboembolic events during anti-TNF therapy: A study of 85 spontaneous reports in the period 2000–2006. Biomed. Mater. Eng. 19, 355–364 (2009).
Roy, P. M., Moumneh, T., Penaloza, A. & Sanchez, O. Outpatient management of pulmonary embolism. Thromb. Res. 155, 92–100 (2017).
Kim, S. C., Schneeweiss, S., Liu, J. & Solomon, D. H. Risk of venous thromboembolism in patients with rheumatoid arthritis. Arthritis Care. Res. (Hoboken) 65, 1600–1607 (2013).
Ketfi, C., et al. Risk of Venous Thromboembolism in Rheumatoid Arthritis. Joint Bone Spine 88(3), 105122 (2020).
Abelseth, G., Buckley, R. E., Pineo, G. E., Hull, R. & Rose, M. S. Incidence of deep-vein thrombosis in patients with fractures of the lower extremity distal to the hip. J. Orthop. Trauma 10, 230–235 (1996).
Knudson, M. M., Ikossi, D. G., Khaw, L., Morabito, D. & Speetzen, L. S. Thromboembolism after trauma: An analysis of 1602 episodes from the American College of Surgeons National Trauma Data Bank. Ann. Surg. 240, 490–496 (2004) (discussion 496–498).
Niikura, T. et al. Rate of venous thromboembolism after complex lower-limb fracture surgery without pharmacological prophylaxis. J. Orthop. Surg. (Hong Kong) 23, 37–40 (2015).
Magetsari, R., Dewo, P., Nugroho, A. S. & Lanodiyu, Z. Deep vein thrombosis in elderly patients following surgery for fracture of the proximal femur. Malays. Orthop. J. 8, 7–10 (2014).
Sun, J., Wang, X., Yue, X. & Zhang, Y. Factors affecting the formation of deep vein thrombosis in the lower extremities after orthopedic surgery. Int. J. Clin. Exp. Med. 12, 12506–12511 (2019).
Anderson, F. A. Jr. et al. A population-based perspective of the hospital incidence and case-fatality rates of deep vein thrombosis and pulmonary embolism. The Worcester DVT Study. Arch. Int. Med. 151, 933–938 (1991).
Daneschvar, H. L., Seddighzadeh, A., Piazza, G. & Goldhaber, S. Z. Deep vein thrombosis in patients with chronic kidney disease. Thromb. Haemost. 99, 1035–1039 (2008).
Goldhaber, S. Z. Risk factors for venous thromboembolism. J. Am. Coll. Cardiol. 56, 1–7 (2010).
Puurunen, M. K. et al. Epidemiology of venous thromboembolism in the framingham heart study. Thromb. Res. 145, 27–33 (2016).
Hirsh, J., Hull, R. D. & Raskob, G. E. Epidemiology and pathogenesis of venous thrombosis. J. Am. Coll. Cardiol. 8(6 Suppl B), 104B–113B (1986).
Gerhold, K. et al. Health-related quality of life in patients with long-standing rheumatoid arthritis in the era of biologics: Data from the German biologics register RABBIT. Rheumatology (Oxford) 54, 1858–1866 (2015).
Jani, M. et al. Drug-specific risk and characteristics of lupus and vasculitis-like events in patients with rheumatoid arthritis treated with TNFi: Results from BSRBR-RA. RMD Open 3, 000314 (2017).
Borensztajn, K. S., von der Thüsen, J. H. & Spek, C. A. The role of coagulation in chronic inflammatory disorders: A jack of all trades. Curr. Pharm. Des. 17, 9–16 (2011).
Hansson, G. K., Libby, P. & Tabas, I. Inflammation and plaque vulnerability. J. Int. Med. 278, 483–493 (2015).
Mukubo, Y. & Kawamata, M. Perioperative hypercoagulability in patients with rheumatoid arthritis: Sonoclot study. J. Anesth. 18, 62–64 (2004).
Xu, J., Lupu, F. & Esmon, C. T. Inflammation, innate immunity and blood coagulation. Hamostaseologie 30(5–6), 8–9 (2010).
Huerta, C., Johansson, S., Wallander, M. A. & García Rodríguez, L. A. Risk factors and short-term mortality of venous thromboembolism diagnosed in the primary care setting in the United Kingdom. Arch. Int. Med. 167, 935–943 (2007).
Johannesdottir, S. A. et al. Use of glucocorticoids and risk of venous thromboembolism: A nationwide population-based case-control study. JAMA Int. Med. 173, 743–752 (2013).
Caplan, L. et al. Body mass index and the rheumatoid arthritis swollen joint count: An observational study. Arthritis Care Res. (Hoboken) 65, 101–106 (2013).
Hsieh, H. C., Hsu, J. C. & Lu, C. Y. 10-year trends in statin utilization in Taiwan: A retrospective study using Taiwan’s National Health Insurance Research Database. BMJ Open 7(5), e014150 (2017).
Cheng, C. L., Kao, Y. H., Lin, S. J., Lee, C. H. & Lai, M. L. Validation of the national health insurance research database with ischemic stroke cases in Taiwan. Pharmacoepidemiol. Drug. Saf. 20, 236–242 (2011).
Hsieh, C. Y., Chen, C. H., Li, C. Y. & Lai, M. L. Validating the diagnosis of acute ischemic stroke in a National Health Insurance claims database. J. Formos. Med. Assoc. 114, 254–259 (2015).
Liu, C.-Y. et al. Incorporating development stratification of Taiwan townships into sampling design of large scale health interview survey. J. Health Manage. 4, 1–22 (2006).
Deyo, R. A., Cherkin, D. C. & Ciol, M. A. Adapting a clinical comorbidity index for use with ICD-9-CM administrative databases. J. Clin. Epidemiol. 45, 613–619 (1992).
Acknowledgements
We appreciate for the use of the National Health Insurance Research Database and Causes of Death File provided by the Science Center, Ministry of Health and Welfare, Taiwan. We are grateful to Health Data Science Center, China Medical University Hospital for providing administrative, technical and funding support.
Funding
This study was supported by the grants (ASIA-109-CMUH-09) from Asia University and China Medical University Hospital, Taiwan. None of the funding sources had any role or input into the design and conduct of the study or approval of the manuscript.
Author information
Authors and Affiliations
Contributions
C.-P.C. conceived the study concepts. C.-P.C., P.-T.K and W.-C.T. contributed to the study design. C.-P.C., P.-T.K, W.-Y.C. and W.-C.T. participated in the proposal. C.-P.C., P.-T.K, W.-Y.C. and W.-C.T. performed the data analysis and interpretation. All authors discussed the results and wrote the manuscript.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Chen, CP., Kung, PT., Chou, WY. et al. Effect of introducing biologics to patients with rheumatoid arthritis on the risk of venous thromboembolism: a nationwide cohort study. Sci Rep 11, 17009 (2021). https://doi.org/10.1038/s41598-021-96508-z
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41598-021-96508-z
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.