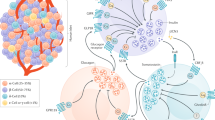
Abstract
The expression of short chain fatty acid receptors FFA2 and FFA3 in pancreatic islets raised interest in using them as drug targets for treating hyperglycemia in humans. This study aims to examine the efficacy of synthetic FFA2- and FFA3-ligands to modulate glucose-stimulated insulin secretion (GSIS) in human pseudoislets which display intact glucose responsiveness. The FFA2-agonists 4-CMTB and TUG-1375 inhibited GSIS, an effect reversed by the FFA2-antagonist CATPB. GSIS itself was not augmented by CATPB. The FFA3-agonists FHQC and 1-MCPC did not affect GSIS in human pseudoislets. For further drug evaluation we used mouse islets. The CATPB-sensitive inhibitory effect of 100 µM 4-CMTB on GSIS was recapitulated. The inhibition was partially sensitive to the Gi/o-protein inhibitor pertussis toxin. A previously described FFA2-dependent increase of GSIS was observed with lower concentrations of 4-CMTB (10 and 30 µM). The stimulatory effect of 4-CMTB on secretion was prevented by the Gq-protein inhibitor FR900359. As in human pseudoislets, in mouse islets relative mRNA levels were FFAR2 > FFAR3 and FFA3-agonists did not affect GSIS. The FFA3-agonists, however, inhibited GSIS in a pertussis toxin-sensitive manner in INS-1E cells and this correlated with relative mRNA levels of Ffar3 > > Ffar2. Thus, in humans, when FFA2-activation impedes GSIS, FFA2-antagonism may reduce glycemia.
Similar content being viewed by others
Introduction
The deorphanisation of the G-protein coupled receptors (GPCRs), GPR43 as FFA2 and GPR41 as FFA3, opens up a new pathway of interaction between the gut and the pancreatic islets1,2,3. Short chain fatty acids (SCFA) have been discovered to be physiological activators of FFA2 and FFA31. SCFAs such as acetate, propionate and butyrate are mainly produced during fermentation of dietary fibres by the gut microbiome and are taken up into the blood stream4,5. In addition, acetate is the degradation product of ethanol metabolism in the liver as well as in other tissue. It has been suggested that alcohol dehydrogenases and aldehyde dehydrogenases are expressed in the human pancreas6. Like the long chain fatty acid receptor GPR40/FFA1, FFA2 and FFA3 are both expressed by the intestinal endocrine cells that produce the incretins GLP-1 and GIP7,8,9,10,11. The entero-endocrine-islet axis mediated by incretins has been studied in great depth12. Specific receptors on islet cells, i.e. GLP-1R and GIPR, transmit signals from the intestine to beta-cells, causing a potentiation of glucose-stimulated insulin secretion (GSIS)13,14. One of the beneficial effects of gut microbiome-derived SCFAs on metabolism is their stimulatory effect on GLP-1 and GIP secretion through FFA2 and FFA3 in entero-endocrine cells7,10,15,16,17. Direct effects of SCFAs on insulin secretion have been studied in isolated islets of wild type and receptor-deficient mice and insulin secreting cell lines. However, opposing effects on glucose homeostasis and insulin secretion have been observed18,19,20,21,22. These divergent results may be interpreted in various ways. Firstly, SCFAs are not only receptor agonists but also metabolites and can affect cellular metabolism depending on the experimental conditions23. Secondly, FFA2 couples to Gq and Gi/o proteins which are known to transmit stimulatory and inhibitory effects on insulin secretion, respectively, while FFA3 only couples to Gi/o24,25. Thirdly, receptor expression on non-beta-cells within the islet may affect insulin secretion through paracrine effects26,27. Indeed, FFA2-agonists were recently reported to stimulate somatostatin secretion in mice28. While somatostatin is a potent inhibitor of insulin secretion, delta-cells are sparse and not uniformly distributed among or within the islets29,30.
The divergent effects could therefore depend on the expression levels of FFA2 and FFA3 in different islet cells. In view of the lack of specific antibodies for detection of endogenous FFA2 and FFA3 proteins, transcriptome analyses were used to estimate receptor’s expression. The mRNAs of FFA2 and FFA3 are discernible in isolated human islets using RT-qPCR18,22. Of note, in human single beta-cells the mRNA levels of FFA2 and FFA3 are barely detectable by RNAseq, suggesting that the expression of these receptors on beta-cells is low31. By comparison, the mRNA of FFA1 is highly abundant in beta- as well as in alpha- and gamma-cells31. It is worth bearing in mind that FFA2 and FFA3 are encoded in the same region of chromosome 19 (19q13) as FFA1 and that the same promoter region may regulate FFA1 and FFA3 transcription1,24,32,33. The different cellular levels of these mRNAs would then imply distinct posttranscriptional regulations.
In view of the contradictory effect of FFA2 and FFA3 on GSIS, a more detailed analysis, especially in human islets, is needed to understand the role of these receptors in glucose homeostasis in humans34. In previous studies, mainly SCFAs (acetate and propionate) were applied to isolated human islets18,19,20,21,22. In addition, FFA2-agonists which were used in two of these publications generated inconsistent results19,22. In the present study, we assessed the effects on GSIS of two FFA2-agonists (allosteric 4-CMTB and orthosteric TUG-1375), one FFA2-antagonist (CATPB), two FFA3-agonists (allosteric FHQC and orthosteric 1-MCPC) and of SCFAs (Table 1). In order to evaluate receptor expression and in view of the lack of specific and sensitive antibodies, relative mRNA levels of FFA2 and FFA3 were assessed in human islets, pseudoislets, mouse islets and INS-1E cells using semi-quantitative RT-PCR. Mouse islets and INS-1E cells were used for drug evaluation, in cases for unresponsiveness of human pseudoislets. We further discuss whether the small synthetic agonists or antagonists of FFA2 or FFA3 might be instrumental in improving insulin secretion under hyperglycaemic conditions in humans35.
Results
In human pseudoislets FFA2-agonists inhibit GSIS
Adequate glucose responsiveness of insulin-secreting beta-cells is a prerequisite for functional testing. Previously, we described that reaggregation of isolated human islet cells into pseudoislets resulted in markedly improved GSIS42. The comparison of GSIS of isolated islets from human organ donors and of pseudoislets prepared thereof confirmed a better responsiveness of pseudoislets compared to islets (Fig. 1a, Table 2, Supplementary Fig. S1). In the pseudoislet preparations, insulin secretion at 12 mM glucose was ninefold higher than at 2.8 mM glucose (9.60 ± 0.93 (n = 41) and 1.09 ± 0.14 (n = 43) % of insulin content, respectively). The responsiveness was still variable, but did not correlate to the amount of stored insulin (Table 2). Interestingly, GSIS correlated positively to glucagon mRNA levels (Fig. 1b). In addition to an improved regulation of insulin secretion, glucagon secretion of pseudoislets was inhibited when raising glucose from 2.8 to 12 mM (Fig. 1c). Inhibition of glucagon secretion by raising glucose was not significant in isolated islets (Supplementary Fig. S1).
Effects of FFA2 and FFA3 ligands and SCFAs on GSIS in human pseudoislets. Human pseudoislets were prepared and incubated with test substances as indicated in each experiment and described under methods. (a,d–h) Insulin and (c) glucagon secretion are calculated as % of content and (b,i) relative mRNA levels are expressed as 2−ΔCt (RPS13 was used as housekeeping gene). In insert in b the highest value is excluded. Results are presented as mean ± SEM of 4 replicates/conditions/donor of (a–c) n = 11, (d) n = 4, (e) n = 1, (f) n = 3, (g) n = 9, (h) n = 4, (i) n = 9 donors (see Supplementary Table S1). Significance **p < 0.01, ***p < 0.001 vs 2.8 mM glucose; #p < 0.05, ##p < 0.01, ###p < 0.001 vs 12 mM glucose, §p < 0.05 vs 12 mM glucose + 1 or 10 µM 4-CMTB, respectively, one-way ANOVA, followed by Tukey´s test. &p < 0.05, unpaired Student’s t-test.
Next, we tested the effects of FFA2- and FFA3-agonists on GSIS (Table 1). Both FFA2-agonists, 4-CMTB and TUG-1375, inhibited GSIS of pseudoislets (Fig. 1d–f). In 4 pseudoislet preparations 4-CMTB inhibited GSIS by 85% at the highest concentration tested (100 µM, Fig. 1d) while lower concentrations, 1 and 10 µM, had no effect (n = 4, not shown). Only in pseudoislets of donor#8, 4-CMTB efficiently inhibited GSIS at lower concentrations (1 and 10 µM, Fig. 1e). The FFA2-antagonist CATPB counteracted the inhibition induced by 4-CMTB confirming the FFA2-dependency. Neither FFA3-agonists FHQC and 1-MCPC nor SCFA significantly affected GSIS (Fig. 1g,h). Of note, the response to SCFAs (1 mM acetate, 1 mM propionate and 1 mM butyrate) was heterogeneous (Supplementary Fig. S2). In pseudoislets of 3 donors (donor #1–#3) all three SCFAs augmented GSIS by 55%, whereas an inhibitory effect on GSIS by acetate was observed in donor #8 only. In 5 preparations (donor #4–#7, #11) SCFAs did not affect GSIS. Thus, heterogeneous effects of acetate are not a consequence of inconsistent experimental conditions between laboratories, but reflect differences between patients.
In accordance with the FFA2-effects on GSIS in pseudoislets, the relative mRNA levels of FFAR2 were always higher than those of FFAR3, especially in donor #8 that showed a pronounced acetate- and FFA2-agonist mediated inhibition of GSIS (Fig. 1i, Table 2). Of note, the mRNA levels of FFAR1, FFAR2, FFAR3 and FFAR4 as well as of INS (insulin), GCG (Glucagon) and SST (somatostatin) were comparable between pseudoislets and isolated islets of the same human donors (Fig. 1i, Table 2). These results suggest that FFA2- and FFA3-agonists are unsuitable for the treatment of insufficient insulin secretion in humans. FFA2-antagonists, in contrast, may augment GSIS, but only under conditions of FFA2-dependent inhibition of insulin secretion.
In mouse islets FFA2-agonist 4-CMTB exerted a dual concentration-dependent effect on GSIS through distinct pathways
In view of the unresponsiveness of the human preparations to FFA3-agonists and the absence of stimulatory effects of FFA2-agonists on GSIS, we evaluated the ligands in established rodent cell models, i.e. isolated mouse islets and INS-1E cells. This is possible since the FFA2- and FFA3-agonists have similar affinities and selectivity to mouse as to human receptors (Table 1). In contrast to the consistent inhibitory effect of 4-CMTB in human pseudoislets, in mouse islets the FFA2-agonist 4-CMTB displayed a concentration-dependent dual effect on GSIS (Fig. 2a). At low concentrations, 10 and 30 µM, 4-CMTB stimulated GSIS, while addition of 100 µM inhibited secretion. To examine whether the dual effect of 4-CMTB is due the activation of different G-protein regulated signalling pathways, the effects of 4-CMTB on GSIS was analysed in the presence specific inhibition of Gq/11-proteins with FR90035943 and of Gi/o-proteins with pertussis toxin44. Preincubation of mouse islets with the Gq-inhibitor FR900359 counteracted the stimulation of insulin secretion induced by 10 µM 4-CMTB (Fig. 2b). Of note, FR900359 abolished muscarinic acetylcholine receptor M3-dependent augmentation of GSIS by carbachol. In contrast, the inhibition of GSIS by 100 µM 4-CMTB was still significant in the presence of FR900359, but partly reversed by pertussis toxin (PTx) pretreatment (Fig. 2c). As control, adrenaline, a potent physiological inhibitor of GSIS, was used, which activates alpha2-adrenergic receptors linked to a PTx-sensitive G-protein45. Pertussis toxin treatment was efficient, since adrenaline-mediated inhibition of GSIS was no longer significant in PTx-treated mouse islets (Fig. 2c). The orthosteric FFA2-agonist, TUG-1375 which mimics the interaction of SCFAs with the receptor, did not influence GSIS at 1, 10 and 100 µM (Fig. 2d). Neither SCFAs nor FFA3-agonists affected GSIS (Fig. 2e,f). These results confirm that in mouse islets FFA2-agonist can activate a stimulatory but also an inhibitory pathway.
Effects of FFA2 and FFA3 ligands and SCFAs on GSIS in mouse islets. (a–f) Mouse islets were isolated, overnight cultured and incubated with test substances as indicated in each experiment and described under methods. (b) FR900359 (Gq/11 inhibitor) was added into the preincubation and incubation solution. (c) Pertussis toxin (PTx) pretreatment (100 ng/ml) was performed in culture 24 h before the experiments. (g) RNA was prepared from freshly isolated mouse islets and (h) from freshly isolated islet cells as described under methods. (a–f) Insulin secretion is expressed as % of content or relative to 12 mM glucose, (g,h) relative mRNA levels are expressed as 2−ΔCt (RPS13 was used as housekeeping gene). Results are presented as mean ± SEM of n = 3 C57BL/6N mouse islet preparations with 4 replicates/condition for insulin secretion; n = 3–7 of C57BL/6N for mRNA analysis. C57B6N: C57BL/6N; GF: Germ-free mice. Significance *p < 0.05, **p < 0.01, ***p < 0.001 vs 2.8 mM glucose, #p < 0.05, ##p < 0.01, ###p < 0.001 vs 12 mM glucose, one-way ANOVA, followed by Tukey’s test. &p < 0.05, &&p < 0.01, &&&p < 0.001 unpaired Student’s T-test.
As in human islets, in mouse islets relative mRNA levels of Ffar2 were higher than of Ffar3 (Fig. 2g). The order of relative mRNA abundance was Ffar2 > Ffar3 > Ffar1 > > Ffar4. The Ffar1-4 mRNA levels of isolated islets of different mouse strains (C3HeB/FeJ and C57BL/6N) were comparable and did not change significantly when the mice were held under germ-free conditions (Fig. 2g). Using FACS-sorted GFP-labelled insulin-producing cells of C57BL/6N RIP-Cre mT/mG mice, Ffar2 mRNA levels were discernible in the beta- and non-beta-cell fractions, while Ffar3 mRNA was enriched in beta-cells (Fig. 2h).
These results suggest that the regulation of insulin secretion is comparable between human pseudoislets and mouse islets in regard to the inhibitory effect of high concentrations of FFA2-agonists and unresponsiveness to FFA3-agonists. A stimulatory effect of 4-CMTB on GSIS is only observed in mouse islets.
In rat INS-1E cells SCFAs and FFA3 agonists inhibit GSIS
Since FFA3-agonists had no effect on GSIS in human pseudoislets and mouse islets, we tested FHQC and 1-MCPC on GSIS in INS-E cells, a rat insulin-secreting cell line. At the highest concentration tested FHQC and 1-MCPC significantly reduced GSIS (Fig. 3a). A comparable inhibitory effect on GSIS was exerted by 1 mM propionate and 1 mM butyrate but not by acetate (Fig. 3b). In INS-1E cells, the relative mRNA levels of Ffar3 were remarkably high, those of Ffar2 were low (Fig. 3c). This expression pattern could explain the inhibitory effect of propionate and butyrate on GSIS in INS-1E cells, since the potency of FFA3 activation declines from butyrate = propionate > > acetate1,36. Since no specific FFA3-antagonist was available, the expression of FFA3 was reduced by transfecting INS-1E cells with siRNA against FFA3 (Fig. 3d). The efficient downregulation of FFA3 (by 85%) abrogated the inhibitory effect of FHQC and propionate on secretion without affecting GSIS (Fig. 3e).
Effects of FFA2 and FFA3 ligands and SCFAs on GSIS in INS-1E cells. (a–h) INS-1E cells were cultured and incubated with test substances as indicated and described under methods. (d,e,g) INS-1E cells were untreated (white bars), treated with non-targeting siRNA (grey bars) and treated with Ffar3 siRNA (black bars) as described under methods. (f,h) INS-1E cells were cultured in the presence of pertussis toxin (PTx;100 ng/ml) for 24 h before the experiments. (a,f,h) Insulin secretion is expressed as % of content or (b,e,g) relative to secretion at 12 mM glucose. (c,d) mRNA levels are expressed as (2−ΔCt). RPS13 was used as housekeeping gene. Results are presented as mean ± SEM of n = 3–4 independent experiments. Significance ***p < 0.001 vs the respective control at 2.8 mM glucose; #p < 0.05, ##p < 0.01, ###p < 0.001 vs the respective stimulation at 12 mM glucose, one-way ANOVA followed by Tukey’s test; n.s not significant.
Next, we examined whether the FFA3-dependent inhibition of GSIS was transmitted via a PTx sensitive Gi/o protein as suggested previously18. After PTx pretreatment of the cells, both agonists, FHQC and 1-MCPC, were unable to reduce GSIS (Fig. 3f). PTx also abrogated the inhibitory effect of adrenaline. In comparison to the pronounced inhibitory effect of adrenaline on secretion, the FFA3-agonist attenuated secretion by 40%.
Although Ffar2 mRNA levels were low, we tested the FFA2-agonist 4-CMTB in INS-1E cells. 4-CMTB at 100 µM inhibited GSIS similar to the inhibition observed in mouse islets and human pseudoislets (Fig. 3g). 4-CMTB still efficiently inhibited GSIS in the presence of siRNA against FFA3 or after PTx pretreatment of the cells (Fig. 3g,h).
In summary, FFA3-agonists FHQC and 1-MCPC inhibit GSIS through a PTx-sensitive G-protein in INS-1E cells. The ineffectiveness of the FFA3-agonists and the low abundance of FFAR3 mRNA especially in human pseudoislets suggest that FFA3 is not functionally expressed in human beta-cells. FFA2-agonists consistently inhibited insulin secretion at high concentration (100 µM) in all cell systems tested.
Discussion
This study revealed FFA2-antagonist by preventing FFA2-mediated inhibition of GSIS as putative therapeutic targets for the treatment of hyperglycaemia. The results further suggest that FFA3 is not functionally expressed in human islets since FFA3 agonists did not affect GSIS and mRNA levels of FFAR3 were very low, i.e. at the detection limit.
In human pseudoislets as well as in mouse islets and in INS-1E cells, the FFA2-agonist 4-CMTB invariably inhibited GSIS at 100 µM. In contrast to mouse islets, where 10 µM 4-CMTB augmented GSIS, in human pseudoislets, 4-CMTB at lower concentrations inhibited GSIS or had no effect. The concentration-dependent dual effect elicited by 4-CMTB in mouse islets, was observed in a Min6 cell preparation with another FFA2-agonist and might be, therefore, mouse specific46. Another, structural related FFA2-agonist stimulated GSIS in human islets at 1 µM concentration22. Using a higher number of donor preparations (n=11, Fig. 1) compared with that ones used by McNelis (n=3)22, we observed highly variable effects. Therefore, this stimulatory effect might be donor specific.
The inhibition of GSIS by 4-CMTB was efficiently reversed by the FFA2-antagonist CATPB confirming that the effect of 4-CMTB was transmitted through FFA2. Furthermore, in INS-1E cells siRNA against Ffar3 did not affect the inhibition by 4-CMTB. Since the antagonist had no effect on GSIS, a favourable effect on insulin secretion is expected only under FFA2-stimulation. This conclusion endorses the proposal made by Stefan Offermann that FFA2-antagonists may be useful for the treatment of hyperglycaemic episodes by improving insulin secretion but our results suggest utility limitations as the antagonist only counteracted FFA2-mediated inhibition of GSIS18.
Physiological stimuli of FFA2 and FFA3 so far identified are SCFAs, acetate, propionate and butyrate. Using static incubations, we observed a heterogeneous response of human pseudoislets to SCFAs. A significant inhibition of GSIS comparable to the 4-CMTB-induced inhibition was observed in one out of 9 preparations. This inhibition by acetate and low concentration of 4-CMTB correlated with 10-times higher relative mRNA levels of FFA2 compared to the other donors (2−ΔCt of 0.133 vs < 0.02, respectively; Table 2). Due to restricted information available from organ donors we are unable to speculate about the reason of this heterogeneous expression of FFA2 and response to SCFAs. Acetate, the main SCFA in blood derives mainly from the gut microbiome or from alcohol consumption. That the gut microbiome does not impact on FFA2 and FFA3 expression in islets is corroborated by the finding that FFA2 and FFA3 mRNA levels were not affected by the maintenance of mice under germ-free conditions. Alcohol consumption increases blood acetate levels above 1 mM and associates with decreased fasting and 2 h-postload insulin levels compared to non-drinker47,48. In contrast to acetate, plasma concentrations of propionate and butyrate remain at low micromolar range, concentrations which do not activate the receptors.
Our results confirm previous observations that both stimulatory and inhibitory effects can be triggered by SCFAs, and suggest that this heterogeneity is not just a result of different experimental settings49. In three previous studies using static incubations of human islets, acetate either inhibited18 or did not alter GSIS19,22. In other studies using perifused human islets, acetate and propionate potentiated GSIS20,21. We found in static incubations of pseudoislets stimulation, inhibition or no effect of SCFAs on GSIS, even though glucose stimulated insulin secretion to the same extent and the FFAR2 and FFAR3 mRNA levels were similar in responsive and unresponsive pseudoislets.
Another explanation for the heterogeneous effect of SCFAs and FFA2 agonists on GSIS in human pseudoislets could be a heterogeneous composition of beta:alpha:delta-cells. Somatostatin (from delta-cells) is a potent inhibitor not only of insulin but also of glucagon secretion in humans and rodents30. On average, less than 10% of the endocrine islet cells are delta-cells. A recent publication convincingly demonstrated that FFA2-agonists stimulate somatostatin secretion in mice28. FFA2 may be expressed in delta-cells, as suggested by the expression pattern of FACS-separated mouse beta-cells and non-beta-cells (Fig. 2h). A variable number of delta-cells may affect the efficiency of the paracrine inhibition of GSIS by somatostatin. In the pseudoislet preparation of donor #8 FFA2-agonists and acetate potently inhibit GSIS and the mRNA levels of somatostatin and FFA2 were higher compared to pseudoislets of the other donors. However, somatostatin acts via PTx-sensitive pathways. In mouse islets, the inhibitory effect of high concentrations of 4-CMTB was only partially reversed by PTx. This indicates both, an activation of a receptor which links to PTx-sensitive Gi/o proteins but also the involvement of a PTx-insensitive pathway as has been observed previously19.
We decided to use pseudoislets, since they display a much better GSIS than the isolated islets from the same human donor42. The mRNA levels of insulin, somatostatin and of the fatty acid receptors FFAR1-4, were comparable between islets and pseudoislets, suggesting that expression of hormones and receptors is not significantly different between islets and pseudoislets (Table 2)42. Interestingly, glucagon mRNA levels were higher in pseudoislets compared to islets yielding in a positive correlation between glucagon mRNA levels and insulin secretion. A higher glucose responsiveness has been found in glucagon rich, dorsal islets compared to glucagon poor, ventral islets isolated from the same rat suggesting that islet glucagon contributes to higher glucose responsiveness50. Further studies will help to understand the mechanism underlying the increased production of glucagon in pseudoislets.
The specificity of FFA2-agonists, the FFA2-antagonist37,38,39,51,52 and FFA3 agonists, FHQC and 1-MCPC53,54 have been evaluated in expression systems and, at the concentrations used, they activate the respective murine and human receptors (Table 1). However, the FFA3-agonists had no significant effect on GSIS in human pseudoislets and mouse islets. Only in INS-1E cells a significant inhibitory effect on GSIS was observed and correlated with higher mRNA levels of Ffar3 compared to Ffar2. Thus, the absence, or very low expression of FFA2 in INS-1E cells could uncover a FFA3-dependent inhibition of GSIS. The assumption that the relative ratio of FFA2/FFA3 expression in beta-cells determines stimulation or inhibition may explain the results obtained in transgenic (tg) mice overexpressing FFA355. In the FFA3 tg mice, i.e. 40-fold higher expression of FFA3 over FFA2 in beta-cells, plasma glucose excursions during glucose stimulation (oGTT) were increased (due to FFA3-mediated inhibition of GSIS), whereas the absence of FFA3 slightly attenuated the elevation of plasma glucose during oGTT (due to FFA2-mediated stimulation of GSIS). Accordingly, the deletion of FFA2 was not sufficient to overcome the inhibitory effect of acetate on GSIS in isolated mouse islets18. Only a deletion of both FFA2 and FFA3 overcame the inhibitory effect of acetate on insulin secretion. The results in our sorted mouse islet cells suggest that FFA3 is enriched in the beta-cell fraction, while FFA2 is expressed on beta- and non-beta-cells. The reason for the very different Ffar2 mRNA levels (more than 2 orders of magnitude) of mouse islets and rat INS-1E cells remains elusive, but expression of FFA2 in non-beta-cell population could contribute to the high islet mRNA levels.
In conclusion, although SCFAs have direct effects on insulin secretion in human islets, these effects are highly heterogeneous among individuals. While SCFAs indirectly augment GSIS by increasing incretin secretion, they may inhibit insulin secretion and subdue the incretin effects via direct effects within the islets56. Further experimental evidence is needed to determine whether the beneficial metabolic effects of fibre ingestion include SCFA-effects on beta-cell’s differentiation, survival and protection against stress factors57,58. This study suggests that FFA2, but not FFA3, is functionally expressed in human islets and that FFA2-antagonists may exert beneficial effects on hyperglycaemic episodes by counteracting FFA2-dependent inhibition of GSIS.
Methods
Human islet and pseudoislet preparations
Human pancreatic islets from organ donors were provided by the European Center for Islet Transplantation (ECIT, JDRF award 31-2008-416 for basic research programme) or purchased from Tebu-Bio (Offenbach, Germany). Donors gave informed consent for the use of their islets preparations in scientific research. The use and the procedures and protocols involved in handling of human islets were approved by the Ethics Commission of the Medical Faculty of the Eberhard Karls University and the University Hospital Tübingen (098/2017BO1). All experiments involving human material were performed in accordance with the above mentioned approvals, guidelines and regulations. The characteristics of human pancreatic donors are provided in Supplementary Table S1. The islets were cultured overnight in CMRL1066, containing 5 mM glucose, 10% (v/v) FCS (Serva, Heidelberg, Germany), 10 mM HEPES, 2 mM l-glutamine, and 1% penicillin/streptomycin at 37 °C in a 5% CO2-humidified atmosphere. The pseudoislets were prepared after dissociation of islets into single cells with 0.25% Trypsin–EDTA in PBS at 37 °C for 5 min as already described in detail42. In brief, 2000 cells were reaggregated in hanging drops of 20 µl medium on the top of a petri dish. After 3d of culture, the reaggregated pseudoislets were harvested and placed into 24-well plates with one pseudoislet in 0.5 ml medium/well and cultured for further 2d.
Mouse islets and FACS isolated beta-cells
Islets from adult C3HeB/FeJ, C57BL/6N, germ-free (C57BL/6N) and RIP-Cre mT/mG (C57BL/6N) transgenic mice were isolated by collagenase digestion (1 mg/ml #NB8, Serva, Heidelberg, Germany) and rinsed with Hank’s balanced salt solution supplemented with 0.5% BSA. The islets were cultured overnight in RPMI1640 medium (Lonza, Basel, Switzerland) containing 11 mM glucose and supplemented with 10% FCS, 10 mM HEPES, 2 mM l-glutamine, 1 mM Na-pyruvate. Dissociated cell preparations of isolated islets from RipCre mT/mG mice were used to separate green (beta) cells from red (non-beta) cells by fluorescence-activated cell sorting (FACS). FACS was performed with a BD FACS Aria cell sorter (BD Biosciences, Heidelberg, Germany) using BD Diva Software. Cells were sorted with a 100 µm nozzle on a high-purity sort option, and sheath pressure was set to 20 psi. The enrichment of insulin and glucagon/somatostatin mRNA levels was used to confirm efficient separation. The generation of transgenic mice, animal handling, islet isolation and experimentation were approved by the review board of the Land Baden-Württemberg (Regierungspräsidium Tübingen). All animal experiments were performed in compliance with the guidelines and regulations for the welfare of experimental animals issued by the local committee (Notification in accordance with §4 Abs. 3 TierSchG from 21.02.2014 and 19.10.2016 to the Regierungspräsidium Tübingen, Referat 35, Konrad Adenauer Strasse 20, 72072 Tübingen by the Animal Welfare Officer of the University of Tübingen).
INS-1E cell culture
INS-1E cells, kindly provided by P. Maechler and C.B. Wollheim (University of Geneva, Switzerland) were cultured in RPMI1640 medium (Lonza, Basel, Switzerland) containing 11 mM glucose and supplemented with 10% FCS (Serva, Heidelberg, Germany), 10 mM HEPES, 2 mM l-glutamine, 1 mM Na-pyruvate and 10 µM 2-mercapthoethanol. INS-1E cells and islets were pretreated with 100 ng/ml of pertussis toxin (PTx) for 24 h to block the Gi/o-dependent pathway. Cells were transfected with siRNA against FFAR3 (ON-TARGETplus rat FFAR3 (365228), individual; Dharmacon Inc, Chicago, USA) or control siRNA (ON-TARGET plus Non-targeting Pool, Dharmacon) using DharmaFect Transfection Reagent 3 (Dharmacon). Cells were analysed two days after transfection. We used the PCR Mycoplasma Test Kit (AppliChem, Darmstadt, Germany) to ensure that the INS-1E cell line was free of mycoplasma.
Semi-quantitative analysis of cellular mRNA
For cellular mRNA detection and quantification, islets, pseudoislets, sorted islet cells and INS-1E cells were lysed and the Nucleospin RNA isolation kit (Macherey Nagel, Düren, Germany) was used to isolate RNA. Following an evaluation of RNA integrity (Agilent Technologies, Santa Clara, CA, USA), cDNA of 0.1 µg RNA was synthesised using the Transcriptor first strand cDNA synthesis kit (Roche Diagnostics, Rotkreuz, Switzerland). Semi-quantitative PCR was performed with the LightCycler 480 system (Roche Diagnostics) using the primers (Invitrogen, Carlsbad, CA, USA) listed in Supplementary Table S2.
Measurement of insulin and glucagon secretion
Isolated islets (5 islets/0.5 ml), pseudoislets (1 pseudoislet/0.1 ml) or INS-1E cells (2 × 105 cells/0.5 ml) were pre-incubated in Krebs–ringer buffer (KRB) containing 2.8 mM glucose as described previously59. INS-1E cells and islets were then incubated in the presence of test substances. These were comprised of SCFAs such as acetate (sodium acetate, Millipore, Burlington, MA, USA), propionate (sodium propionate, Sigma-Aldrich, Munich, Germany) and butyrate (sodium butyrate, Millipore, Burlington, MA, USA); the synthetic allosteric FFA3-agonists FHQC (4-(furan-2-yl)-2-methyl-5-oxo-N-(o-tolyl)-1,4,5,6,7,8-hexahydroquinoline-3-carboxamide)40, the orthosteric FFA3-agonist 1-MCPC (1-methylcyclopropane carboxylate)41 (Sigma-Aldrich, Schnelldorf, Germany), the allosteric FFA2-agonist 4-CMTB ((S)-2-(4-chlorophenyl)-3-methyl-N-(thiazol-2-yl)butanamide)38, the orthosteric FFA2-agonist TUG-1375 ((2R,4R)-2-(2-chlorophenyl)-3-(4-(3,5-dimethylisoxazol-4-yl)benzoyl)thiazolidine-4-carboxylic acid)39 and the allosteric FFA2-antagonist CATPB ((S)-3-(2-(3-chlorophenyl)acetamido)-4-(4-(trifluoromethyl)phenyl)butanoic acid)36 (Sigma-Aldrich, Munich, Germany) were synthesized as previously described in the cited literature or purchased from the indicated provider. Properties of synthetic ligands are shown in Table 1. FR900359 was prepared as previously described, used at a final concentration of 1 µM and added to the cell preparations 1 h before the incubation43. A radioimmunoassay (Millipore, Burlington, MA, USA) or a sensitive ELISA (Mercodia, Uppsala, Sweden) was used to measure insulin and glucagon in the supernatant and in the islets/cells following extraction with acid ethanol (80%(v/v) ethanol).
Statistical analysis
Data are presented as mean ± SEM, and the analysis was performed in GraphPad Prism (Graphpad Software, Inc, La Jolla, CA, USA) using ANOVA and Tukey’s as post-test. Student’s unpaired t-test was performed to facilitate a comparison between the two groups. Deviations of p < 0.05 were considered statistically significant.
References
Brown, A. J. et al. The orphan G protein-coupled receptors GPR41 and GPR43 are activated by propionate and other short chain carboxylic acids. J. Biol. Chem. 278, 11312–11319. https://doi.org/10.1074/jbc.M211609200 (2003).
Le Poul, E. et al. Functional characterization of human receptors for short chain fatty acids and their role in polymorphonuclear cell activation. J. Biol. Chem. 278, 25481–25489. https://doi.org/10.1074/jbc.M301403200 (2003).
Nilsson, N. E., Kotarsky, K., Owman, C. & Olde, B. Identification of a free fatty acid receptor, FFA2R, expressed on leukocytes and activated by short-chain fatty acids. Biochem. Biophys. Res. Commun. 303, 1047–1052. https://doi.org/10.1016/s0006-291x(03)00488-1 (2003).
Louis, P. & Flint, H. J. Formation of propionate and butyrate by the human colonic microbiota. Environ. Microbiol. 19, 29–41. https://doi.org/10.1111/1462-2920.13589 (2017).
Koh, A., De Vadder, F., Kovatcheva-Datchary, P. & Backhed, F. From dietary fiber to host physiology: Short-chain fatty acids as key bacterial metabolites. Cell 165, 1332–1345. https://doi.org/10.1016/j.cell.2016.05.041 (2016).
Chiang, C. P. et al. Expression pattern, ethanol-metabolizing activities, and cellular localization of alcohol and aldehyde dehydrogenases in human pancreas: Implications for pathogenesis of alcohol-induced pancreatic injury. Alcohol Clin. Exp. Res. 33, 1059–1068. https://doi.org/10.1111/j.1530-0277.2009.00927.x (2009).
Tolhurst, G. et al. Short-chain fatty acids stimulate glucagon-like peptide-1 secretion via the G-protein-coupled receptor FFAR2. Diabetes 61, 364–371. https://doi.org/10.2337/db11-1019 (2012).
Karaki, S. et al. Short-chain fatty acid receptor, GPR43, is expressed by enteroendocrine cells and mucosal mast cells in rat intestine. Cell Tissue Res. 324, 353–360. https://doi.org/10.1007/s00441-005-0140-x (2006).
Karaki, S. et al. Expression of the short-chain fatty acid receptor, GPR43, in the human colon. J. Mol. Histol. 39, 135–142. https://doi.org/10.1007/s10735-007-9145-y (2008).
Psichas, A. et al. The short chain fatty acid propionate stimulates GLP-1 and PYY secretion via free fatty acid receptor 2 in rodents. Int. J. Obes. 39, 424–429. https://doi.org/10.1038/ijo.2014.153 (2015).
Tazoe, H. et al. Roles of short-chain fatty acids receptors, GPR41 and GPR43 on colonic functions. J. Physiol. Pharmacol. 59(Suppl 2), 251–262 (2008).
Creutzfeldt, W. The entero-insular axis in type 2 diabe. Exp. Clin. Endocrinol. Diabetes 109, S288–S303 (2001).
Holz, G. G. IV., Leech, C. A. & Habener, J. F. Activation of a cAMP-regulated Ca2+-signaling pathway in pancreatic β-cells by the insulinotropic hormone glucagon-like peptide-1. J. Biol. Chem 270, 17749–17757 (1995).
Flamez, D. et al. Altered cAMP and Ca2+ signaling in mouse pancreatic islets with glucagon-like peptide-1 receptor null phenotype. Diabetes 48, 1979–1986 (1999).
Lu, V. B., Gribble, F. M. & Reimann, F. Free fatty acid receptors in enteroendocrine cells. Endocrinology 159, 2826–2835. https://doi.org/10.1210/en.2018-00261 (2018).
Tappenden, K. A., Albin, D. M., Bartholome, A. L. & Mangian, H. F. Glucagon-like peptide-2 and short-chain fatty acids: A new twist to an old story. J. Nutr. 133, 3717–3720. https://doi.org/10.1093/jn/133.11.3717 (2003).
Lin, H. V. et al. Butyrate and propionate protect against diet-induced obesity and regulate gut hormones via free fatty acid receptor 3-independent mechanisms. PLoS ONE 7, e35240. https://doi.org/10.1371/journal.pone.0035240 (2012).
Tang, C. et al. Loss of FFA2 and FFA3 increases insulin secretion and improves glucose tolerance in type 2 diabetes. Nat. Med. 21, 173–177. https://doi.org/10.1038/nm.3779 (2015).
Priyadarshini, M. et al. An acetate-specific GPCR, FFAR2, regulates insulin secretion. Mol. Endocrinol. 29, 1055–1066. https://doi.org/10.1210/me.2015-1007 (2015).
Pingitore, A. et al. Short chain fatty acids stimulate insulin secretion and reduce apoptosis in mouse and human islets in vitro: Role of free fatty acid receptor 2. Diabetes Obes. Metab. 21, 330–339. https://doi.org/10.1111/dom.13529 (2019).
Pingitore, A. et al. The diet-derived short chain fatty acid propionate improves beta-cell function in humans and stimulates insulin secretion from human islets in vitro. Diabetes Obes. Metab. 19, 257–265. https://doi.org/10.1111/dom.12811 (2017).
McNelis, J. C. et al. GPR43 potentiates beta-cell function in obesity. Diabetes 64, 3203–3217. https://doi.org/10.2337/db14-1938 (2015).
Putman, C. T., Spriet, L. L., Hultman, E., Dyck, D. J. & Heigenhauser, G. J. Skeletal muscle pyruvate dehydrogenase activity during acetate infusion in humans. Am. J. Physiol. 268, E1007-1017. https://doi.org/10.1152/ajpendo.1995.268.5.E1007 (1995).
Briscoe, C. P. et al. The orphan G protein-coupled receptor GPR40 is activated by medium and long chain fatty acids. J. Biol. Chem. 278, 11303–11311 (2003).
Sharp, G. W. Mechanisms of inhibition of insulin release. Am. J. Physiol. 271, C1781–C1799 (1996).
Wollheim, C. B., Winiger, B. P., Ullrich, S., Wuarin, F. & Schlegel, W. Somatostatin inhibition of hormone release: Effects on cytosolic Ca++ and interference with distal secretory events. Metab. Clin. Exp. 39, 101–104 (1990).
Svendsen, B. et al. Insulin secretion depends on intra-islet glucagon signaling. Cell Rep. 25, 1127–1134. https://doi.org/10.1016/j.celrep.2018.10.018 (2018).
Orgaard, A., Jepsen, S. L. & Holst, J. J. Short-chain fatty acids and regulation of pancreatic endocrine secretion in mice. Islets 11, 103–111. https://doi.org/10.1080/19382014.2019.1587976 (2019).
Brereton, M. F., Vergari, E., Zhang, Q. & Clark, A. Alpha-, Delta- and PP-cells: Are they the architectural cornerstones of islet structure and co-ordination?. J. Histochem. Cytochem. 63, 575–591. https://doi.org/10.1369/0022155415583535 (2015).
Hauge-Evans, A. C. et al. Somatostatin secreted by islet delta-cells fulfills multiple roles as a paracrine regulator of islet function. Diabetes 58, 403–411. https://doi.org/10.2337/db08-0792 (2009).
Segerstolpe, A. et al. Single-cell transcriptome profiling of human pancreatic islets in health and type 2 diabetes. Cell Metab. 24, 593–607 (2016).
Itoh, Y. et al. Free fatty acids regulate insulin secretion from pancreatic beta cells through GPR40. Nature 422, 173–176 (2003).
Bahar, H. K., Veprik, A., Rubins, N., Naaman, O. & Walker, M. D. GPR41 gene expression is mediated by internal ribosome entry site (IRES)-dependent translation of bicistronic mRNA encoding GPR40 and GPR41 proteins. J. Biol. Chem. 287, 20154–20163 (2012).
Liu, J. L., Segovia, I., Yuan, X. L. & Gao, Z. H. Controversial roles of gut microbiota-derived short-chain fatty acids (SCFAs) on pancreatic beta-cell growth and insulin secretion. Int. J. Mol. Sci. https://doi.org/10.3390/ijms21030910 (2020).
Grundmann, M. et al. A molecular mechanism for sequential activation of a G protein-coupled receptor. Cell Chem. Biol. 23, 392–403. https://doi.org/10.1016/j.chembiol.2016.02.014 (2016).
Hudson, B. D., Tikhonova, I. G., Pandey, S. K., Ulven, T. & Milligan, G. Extracellular ionic locks determine variation in constitutive activity and ligand potency between species orthologs of the free fatty acid receptors FFA2 and FFA3. J. Biol. Chem. 287, 41195–41209. https://doi.org/10.1074/jbc.M112.396259 (2012).
Smith, N. J. et al. Extracellular loop 2 of the free fatty acid receptor 2 mediates allosterism of a phenylacetamide ago-allosteric modulator. Mol. Pharmacol. 80, 163–173. https://doi.org/10.1124/mol.110.070789 (2011).
Lee, T. et al. Identification and functional characterization of allosteric agonists for the G protein-coupled receptor FFA2. Mol. Pharmacol. 74, 1599–1609. https://doi.org/10.1124/mol.108.049536 (2008).
Hansen, A. H. et al. Discovery of a potent thiazolidine free fatty acid receptor 2 agonist with favorable pharmacokinetic properties. J. Med. Chem. 61, 9534–9550. https://doi.org/10.1021/acs.jmedchem.8b00855 (2018).
Hudson, B. D. et al. Complex pharmacology of novel allosteric free fatty acid 3 receptor ligands. Mol. Pharmacol. 86, 200–210. https://doi.org/10.1124/mol.114.093294 (2014).
Schmidt, J. et al. Selective orthosteric free fatty acid receptor 2 (FFA2) agonists: Identification of the structural and chemical requirements for selective activation of FFA2 versus FFA3. J. Biol. Chem. 286, 10628–10640. https://doi.org/10.1074/jbc.M110.210872 (2011).
Lorza-Gil, E. et al. Glucose, adrenaline and palmitate antagonistically regulate insulin and glucagon secretion in human pseudoislets. Sci. Rep. 9, 10261. https://doi.org/10.1038/s41598-019-46545-6 (2019).
Schrage, R. et al. The experimental power of FR900359 to study Gq-regulated biological processes. Nat. Commun. 6, 10156. https://doi.org/10.1038/ncomms10156 (2015).
Katada, T., Oinuma, M. & Ui, M. Mechanisms for inhibition of the catalytic activity of adenylate cyclase by the guanine nucleotide-binding proteins serving as the substrate of islet-activating protein, pertussis toxin. J. Biol. Chem. 261, 5215–5221 (1986).
Peterhoff, M. et al. Inhibition of insulin secretion via distinct signaling pathways in alpha2-adrenoceptor knockout mice. Eur. J. Endocrinol. 149, 343–350 (2003).
Villa, S. R. et al. Homology modeling of FFA2 identifies novel agonists that potentiate insulin secretion. J. Investig. Med. 65, 1116–1124. https://doi.org/10.1136/jim-2017-000523 (2017).
Korri, U. M., Nuutinen, H. & Salaspuro, M. Increased blood acetate: A new laboratory marker of alcoholism and heavy drinking. Alcohol Clin. Exp. Res. 9, 468–471. https://doi.org/10.1111/j.1530-0277.1985.tb05585.x (1985).
Mayer, E. J., Newman, B., Quesenberry, C. P., Friedman, G. D. & Selby, J. V. Alcohol consumption and insulin concentrations. Role of insulin in associations of alcohol intake with high-density lipoprotein cholesterol and triglycerides. Circulation 88, 2190–2197. https://doi.org/10.1161/01.cir.88.5.2190 (1993).
Tang, C. & Offermanns, S. FFA2 and FFA3 in metabolic regulation. Handb. Exp. Pharmacol. 236, 205–220. https://doi.org/10.1007/164_2016_50 (2017).
Trimble, E. R., Halban, P. A., Wollheim, C. B. & Renold, A. E. Functional differences between rat islets of ventral and dorsal pancreatic origin. J. Clin. Investig. 69, 405–413 (1982).
Sergeev, E. et al. A single extracellular amino acid in free fatty acid receptor 2 defines antagonist species selectivity and G protein selection bias. Sci. Rep. 7, 13741. https://doi.org/10.1038/s41598-017-14096-3 (2017).
Hudson, B. D. et al. Defining the molecular basis for the first potent and selective orthosteric agonists of the FFA2 free fatty acid receptor. J. Biol. Chem. 288, 17296–17312. https://doi.org/10.1074/jbc.M113.455337 (2013).
Tikhonova, I. G. & Poerio, E. Free fatty acid receptors: Structural models and elucidation of ligand binding interactions. BMC Struct. Biol. 15, 16. https://doi.org/10.1186/s12900-015-0044-2 (2015).
Tikhonova, I. G. et al. Discovery of novel agonists and antagonists of the free fatty acid receptor 1 (FFAR1) using virtual screening. J. Med. Chem. 51, 625–633 (2008).
Veprik, A., Laufer, D., Weiss, S., Rubins, N. & Walker, M. D. GPR41 modulates insulin secretion and gene expression in pancreatic beta-cells and modifies metabolic homeostasis in fed and fasting states. Faseb J. 30, 3860–3869. https://doi.org/10.1096/fj.201500030R (2016).
Christiansen, C. B. et al. The impact of short-chain fatty acids on GLP-1 and PYY secretion from the isolated perfused rat colon. Am. J. Physiol. Gastrointest. Liver Physiol. 315, G53–G65. https://doi.org/10.1152/ajpgi.00346.2017 (2018).
Villa, S. R. et al. Loss of free fatty acid receptor 2 leads to impaired islet mass and beta cell survival. Sci. Rep. 6, 28159. https://doi.org/10.1038/srep28159 (2016).
Li, L. et al. Combination of GLP-1 and sodium butyrate promote differentiation of pancreatic progenitor cells into insulin-producing cells. Tissue Cell 40, 437–445. https://doi.org/10.1016/j.tice.2008.04.006 (2008).
Sabrautzki, S. et al. Point mutation of Ffar1 abrogates fatty acid-dependent insulin secretion, but protects against HFD-induced glucose intolerance. Mol. Metab. 6, 1304–1312. https://doi.org/10.1016/j.molmet.2017.07.007 (2017).
Acknowledgements
We thank Sieglinde Haug and Elisabeth Metzinger (University Hospital of Tübingen, Department of Internal Medicine IV) for excellent technical assistance. We express our gratitude to Dr. Rita Nano (Hospital San Raffaele, Center of Human Islet Isolation, Diabetes Research Institute-DRI, Milano) for the excellent human islet preparations. We thank Prof. Dr. Julia Frick (Department of Microbiology, University Hospital Tübingen) for providing the germ-free mice. This research was supported by a grant (01GI0925) from the German Federal Ministry of Education and Research (BMBF) to the German Center for Diabetes Research (DZD e.V.). E.L.-G. is a research fellow of the DZD e.V. E.R.U. is supported by the Lundbeck Foundation (grants R181–2014–3247, R307-2018-2950). T.U. is supported by the Innovation Fund Denmark (0603-00452B). E.K. and G.M.K. gratefully acknowledge support of this work by the DFG-funded Research Unit FOR2372 with the grants KO 1582/10-1 and KO 1582/10-2 (to E.K.), as well as KO 902/17-1 and KO 902/17-2 (to G.M.K.). The human islets were provided by the JDRF award 31-2008-416 (ECIT Islet for Basic Research program) as stated.
Funding
Open Access funding enabled and organized by Projekt DEAL.
Author information
Authors and Affiliations
Contributions
S.U. and E.L.-G. conceptualised and designed experiments. E.L.-G. and M.B.O. performed human islet experiments, E.L.-G. and F.G. performed experiments with mice, G.K. performed RT-qPCR and INS-1E cell experiments, E.R.U. and T.U. synthesized agonists and antagonist. EK and GMK provided FR900359. S.U., E.L.-G., T.U., E.K., H.U.H. and A.B. contributed to data analysis and interpretation. E.L.-G. and S.U. compiled the manuscript. All authors approved the manuscript. S.U. is the guarantor of this work and, as such, had full access to all the data in the study and assumes responsibility for the integrity of the data and the accuracy of the data analysis.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Lorza-Gil, E., Kaiser, G., Rexen Ulven, E. et al. FFA2-, but not FFA3-agonists inhibit GSIS of human pseudoislets: a comparative study with mouse islets and rat INS-1E cells. Sci Rep 10, 16497 (2020). https://doi.org/10.1038/s41598-020-73467-5
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41598-020-73467-5
This article is cited by
-
Glucose-stimulated insulin secretion depends on FFA1 and Gq in neonatal mouse islets
Diabetologia (2023)
-
Short-chain fatty acids: possible regulators of insulin secretion
Molecular and Cellular Biochemistry (2023)
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.