Abstract
Currently, no clinical studies have compared the inspiratory and expiratory volumes of unilateral lung or of each lobe among supine, standing, and sitting positions. In this prospective study, 100 asymptomatic volunteers underwent both low-radiation-dose conventional (supine position, with arms raised) and upright computed tomography (CT) (standing and sitting positions, with arms down) during inspiration and expiration breath-holds and pulmonary function test (PFT) on the same day. We compared the inspiratory/expiratory lung/lobe volumes on CT in the three positions. The inspiratory and expiratory bilateral upper and lower lobe and lung volumes were significantly higher in the standing/sitting positions than in the supine position (5.3–14.7% increases, all P < 0.001). However, the inspiratory right middle lobe volume remained similar in the three positions (all P > 0.15); the expiratory right middle lobe volume was significantly lower in the standing/sitting positions (16.3/14.1% decrease) than in the supine position (both P < 0.0001). The Pearson’s correlation coefficients (r) used to compare the total lung volumes on inspiratory CT in the supine/standing/sitting positions and the total lung capacity on PFT were 0.83/0.93/0.95, respectively. The r values comparing the total lung volumes on expiratory CT in the supine/standing/sitting positions and the functional residual capacity on PFT were 0.83/0.85/0.82, respectively. The r values comparing the total lung volume changes from expiration to inspiration on CT in the supine/standing/sitting positions and the inspiratory capacity on PFT were 0.53/0.62/0.65, respectively. The study results could impact preoperative CT volumetry of the lung in lung cancer patients (before lobectomy) for the prediction of postoperative residual pulmonary function, and could be used as the basis for elucidating undetermined pathological mechanisms. Furthermore, in addition to morphological evaluation of the chest, inspiratory and expiratory upright CT may be used as an alternative tool to predict lung volumes such as total lung capacity, functional residual capacity, and inspiratory capacity in situation in which PFT cannot be performed such as during an infectious disease pandemic, with relatively more accurate predictability compared with conventional supine CT.
Similar content being viewed by others
Introduction
Although humans spend most of their daytime in an upright position, the detailed human anatomy of the lung in the standing or sitting position remains unclear. Chest radiography can be performed in the upright position1; however, chest radiography provides a two-dimensional image and cannot allow for the accurate measurement of the lung or lobe volume.
Recently, a 320-detector-row upright computed tomography (CT) scanner has been developed to evaluate human anatomy in the upright position three-dimensionally, and can be helpful to clarify the effects of gravity on the entire human body2, although there are already several studies describing the effect of gravity and posture on the lungs3,4,5. This upright CT scanner allows for the acquisition of isotropic volume data (isotropic 0.5-mm voxel size) of the whole chest within approximately 5 seconds6.
It has been reported that the total lung capacity measured by pulmonary function test (PFT) in the standing or sitting position is higher than that determined in the supine position7,8; however, unilateral lung volume or each lung lobe volume cannot be measured by PFT. Conversely, CT images can provide the volumes of the unilateral lung and each lung lobe9,10,11,12 and reportedly enables more accurate predictions of postoperative residual pulmonary function in patients with lung cancer than does the segment-counting method, which is based solely on the number of remaining pulmonary segments9,10,11. Upright CT provides images of daily-life postures (both standing and sitting positions) and possibly enables a more accurate prediction of postoperative residual pulmonary function, before lobectomy, than does conventional CT (supine position)6.
A previous, preliminary study compared lung and lobe volumes between supine and standing positions using conventional and upright CT; however, supine CT was performed with the subjects’ arms down, while conventional chest CT in the supine position is usually performed with the subject’s arms raised6. In addition, the previous study evaluated only inspiratory lung/lobe volumes in the standing position6, but not expiratory lung/lobe volume or lung/lobe volume in the sitting position. To the best of our knowledge, no clinical studies to date have accurately compared both the inspiratory and expiratory lung/lobe volumes in the supine (with the subject’s arms raised), standing, and sitting positions. We hypothesized that the inspiratory/expiratory volume change rates of each lobe of the lung between supine and upright (standing and sitting) positions would be different, because the direction of gravity relative to the chest differs between supine and upright positions.
The purpose of this study was thus to compare inspiratory and expiratory lung/lobe volumes on CT among supine, standing, and sitting positions.
Methods
Study population
This prospective study was approved by the Keio University School of Medicine Ethics Committee (No. 20160384). Written informed consent was obtained from all participants (UMIN Clinical Trials Registry [UMIN-CTR]: UMIN000026586). All methods were performed in accordance with the relevant guidelines and regulations. From June 2017 to August 2018, 100 asymptomatic volunteers from a volunteer recruitment company were enrolled in this study. To evaluate normal whole-body anatomy, volunteers with a history of smoking, diabetes, hypertension, dyslipidemia, and dysuria; those who had any type of symptom; had undergone any surgery; or were currently undergoing treatment and pregnant or possibly pregnant volunteers were excluded from the study.
CT imaging protocol
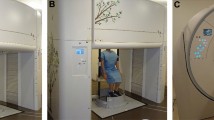
All participants underwent both conventional body trunk low-radiation-dose CT in the supine position with arms raised (Fig. 1A) performed using a 320-detector-row CT (Aquilion ONE, Canon Medical Systems, Otawara, Japan) and upright body trunk low-radiation-dose CT in standing (Fig. 1B) and sitting positions with arms down (Fig. 1C) performed using a 320-detector-row upright CT (prototype TSX-401R, Canon Medical Systems)2,6 on the same day. Subjects were scanned in the three positions in breath-hold both at the end-inspiration, near total lung capacity on PFT, and at the end-tidal expiration, near functional residual capacity on PFT, as described in a previous study13. Additionally, head and neck scans in the supine position and head scan in the sitting position were obtained for these volunteers; however, only chest-related data were analyzed in this study.
Conventional CT examination in the supine position (A), upright CT examination in the standing position (B) and upright CT examination in the sitting position (C). Conventional CT in the supine position (A) was performed with the subject’s arms raised during both deep-inspiration breath-hold and expiration breath-hold. Upright CT examinations in the standing position (B) and sitting position (C) were performed with the subject’s arms down during both deep-inspiration breath-hold and expiration breath-hold. For safety during upright CT scanning, an acrylic wall encircling the body was added to prevent falls, with a pinch prevention mechanism and contact interlock control mechanism. Furthermore, to stabilize patients while standing, a back-support pole, 2.3-m long and made of carbon, was included; it was mounted between the floor and the top of the system (B). The mounting position could be adjusted based on the subject's bodily dimensions or the scan conditions. To support patients who are frail or elderly, a Velcro band can be attached to the pole and loosely wrapped around a patient's body. In this study, the subjects were healthy volunteers; thus, we did not use the Velcro band.
For the body trunk, all low-radiation-dose CT examinations were unenhanced and were performed with automatic exposure control using a noise index of 24 for a slice thickness of 5 mm (tube current range, 10–350 mA). Other scanning parameters were also the same for supine, standing, and sitting CT scans: peak tube voltage, 100 kVp; rotation speed, 0.5 s; slice collimation, 0.5 mm × 80; and pitch factor, 0.813. The series of contiguous 0.5-mm-thick images was reconstructed with Adaptive Iterative Dose Reduction 3D (Canon Medical Systems)14. The sum of the CT dose index volume for inspiratory and expiratory CT in the supine, standing, and sitting CT positions was 14.97 ± 3.43 mGy (supine CT, 4.39 ± 1.01 mGy; standing CT, 5.39 ± 1.28 mGy; sitting CT, 5.19 ± 1.39 mGy).
Pulmonary function test
All participants underwent PFTs on the same day of CT examinations (within two hours of CT examinations). The PFT was performed in a stable condition, with the subject in a sitting position, using a spirometer (Chestac-8900, Chest M.I., Tokyo, Japan) in accordance with ATS/European Respiratory Society recommendations15,16. The residual volume and total lung capacity were measured using the multibreath helium dilution method. Predicted values of spirometric measurements were derived from the guidelines of the Japanese Respiratory Society17.
Lung and lobe volume measurements using CT
The first lung and lobe volume measurements on CT of all 100 volunteers in each position were performed by a chest radiologist with 14 years of experience (Y.Y.), using a commercially available workstation (Synapse Vincent, Fuji Film Co., Ltd., Tokyo, Japan). This workstation incorporated a lobar computer-aided diagnosis (CAD) system that was demonstrated to measure lobar volumes precisely in a previous study18. This system automatically extracted right and left lungs, recognized lobar bronchi, and determined the locations of fissures (Fig. 2)6,19. The chest radiologist verified the CAD-determined results of segmentation and made manual corrections by delineating fissures when the CAD system failed to identify them properly, as described in a previous study6,19. Approximately one-third of the segmentations required minor manual correction (less than 10% change of the volumes in all the corrected cases). A second measurement of the first 20 volunteers was performed by the same radiologist to assess intraobserver agreement, 1 month after the first assessment. To assess interobserver agreement, lung volumes of the first 20 volunteers were measured by a different general radiologist with 5 years of experience (Y.Y.).
Representative segmentation and inspiratory/expiratory lung/lobe volume measurement in a 39-year-old male subject: axial (A), sagittal (B), and coronal (C) images, and volume rendering images (D) acquired in the supine, standing, and sitting positions. Yellow is the right upper lobe, blue is the right middle lobe, green is the right lower lobe, pink is the left upper lobe, and purple is the left lower lobe.
All measurements were performed in a randomized and blinded manner. During all measurements, the radiologists were also blinded to participants’ characteristics and results of the PFT. The proportional volumes of each lung and each lobe relative to the total lung volume, lung and lobe volume changes from expiration to inspiration on CT, and the ratio of inspiratory lung/lobe volume to expiratory lung/lobe volume were also calculated.
Statistical analysis
Data are presented as mean ± standard deviation. Paired t-tests were performed to analyze differences in the volumes of the total lungs, right lung, left lung, and each lobe among supine, standing, and sitting positions; the differences in the proportional volumes of each lung and each lobe relative to the total lung volume among the three positions; the differences in volume changes from expiration to inspiration among the three positions; and the differences in the ratio of inspiratory lung/lobe volume to expiratory lung/lobe volume among the three positions. Bonferroni correction was used for multiple comparisons. The difference in age between women and men was assessed using Student’s t-test. Interobserver and intraobserver agreements were evaluated by measuring intraclass-correlation coefficients. The correlations between the volumes on CT in each position and the measurements on PFT (total lung capacity, functional residual capacity, and inspiratory capacity) were also evaluated by measuring intraclass-correlation coefficients. The associations between the volumes on CT in each position and the measurements on PFT (total lung capacity, functional residual capacity, and inspiratory capacity) were evaluated by Pearson’s correlation coefficient test. The significance level for all tests was 5% (two-sided). All data were analyzed using a commercially available software program (JMP version 12; SAS Institute Inc, Cary, NC, USA).
Results
Participant characteristics
The clinical characteristics of all the participants (n = 100) is shown in Table 1. No significant difference was found in age between women and men (48.0 ± 11.9 years vs. 44.9 ± 10.0 years, P = 0.210).
Lung and lobe volumes on CT in supine, standing, and sitting positions
The inspiratory and expiratory bilateral upper and lower lobe and bilateral lung volumes were significantly higher in the standing and sitting positions than in the supine position (5.3–14.7% increases, all P < 0.001) (Table 2). However, no significant differences were found in the inspiratory right middle lobe volume among the three positions (all P > 0.15); the expiratory right middle lobe volume was significantly lower in standing (16.3% decrease) and sitting positions (14.1% decrease) than in the supine position (all P < 0.0001) (Table 2). No significant differences were found in the average inspiratory volumes of the total lung, right lung, left lung, and all lobes between standing and sitting positions (Table 2).
Proportional volumes of each lung and each lobe relative to the total lung volume in supine, standing, and sitting positions
In the inspiratory CT, the proportional volumes of the bilateral upper lobes and right middle lobe relative to the total lung volume were significantly lower in the standing and sitting positions than in the supine position, whereas the proportional volumes of the bilateral lower lobes were significantly higher in the standing position than in the supine position (all P < 0.001) (Table 3).
Lung and lobe volume changes from expiration to inspiration on CT in supine, standing, and sitting positions
Volume changes of the total lung, right lung, left lung, right middle lobe, and bilateral lower lobe from expiration to inspiration in the standing and sitting positions were significantly higher than those in the supine position, whereas the bilateral upper lobe volume changes from expiration to inspiration were similar in the standing, sitting, and supine positions (Table 4). No significant differences were found in the all lung and lobe volume changes from expiration to inspiration between the standing and sitting positions (Table 4).
Ratio of inspiratory lung/lobe volume to expiratory lung/lobe volume in supine, standing, and sitting positions
Differences in the ratio of inspiratory volume to expiratory volume in the total lung, right lung, right upper lobe, right lower lobe, left lung, left upper lobe, and left lower lobe between the supine and standing/sitting positions were less than 0.13, whereas the difference in the ratio of inspiratory volume to expiratory volume in the right middle lobe between the supine and standing/sitting positions were more than 0.29 (both P < 0.0001) (Table 5).
Agreements between volumes on CT in supine, standing, and sitting positions and measurements on PFT
Intraclass-correlation coefficients between the total lung volumes on inspiratory CT in the supine/standing/sitting positions and the total lung capacity on PFT were 0.831 (95% confidence interval [CI], 0.759‒0.883)/0.927 (95% CI, 0.893‒0.950)/0.946 (95% CI, 0.920‒0.963), respectively. Intraclass-correlation coefficients between the total lung volumes on expiratory CT in the supine/standing/sitting positions and the functional residual capacity on PFT were 0.834 (95% CI, 0.763‒0.885)/0.848 (95% CI, 0.782‒0.895)/0.811 (95% CI, 0.732‒0.869), respectively. The intraclass-correlation coefficients between the total lung volume changes from expiration to inspiration on CT in the supine/standing/sitting positions and the inspiratory capacity (total lung capacity minus functional residual capacity) on PFT were 0.508 (95% CI, 0.347‒0.640)/0.601 (95% CI, 0.460‒0.713)/0.625 (95% CI, 0.490‒0.731), respectively.
Associations between volumes on CT in supine, standing, and sitting positions and measurements on PFT
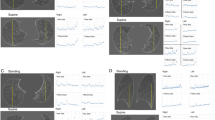
The correlation coefficient r comparing the total lung volumes on inspiratory CT in the supine/standing/sitting positions and the total lung capacity on PFT were, 0.83 (95% CI, 0.76‒0.88)/0.93 (95% CI, 0.90‒0.95)/0.95 (95% CI, 0.92‒0.96), respectively (Fig. 3A). The r comparing the total lung volumes on expiratory CT in the supine/standing/sitting positions and the functional residual capacity on PFT were 0.83 (95% CI, 0.76‒0.89)/0.85 (95% CI, 0.78‒0.90)/0.82 (95% CI, 0.73‒0.87), respectively (Fig. 3B). The r comparing the total lung volume changes from expiration to inspiration on CT in the supine/standing/sitting positions and the inspiratory capacity on PFT were 0.53 (95% CI, 0.38‒0.66)/0.62 (95% CI, 0.49‒0.73)/0.65 (95% CI, 0.52‒0.75), respectively (Fig. 3C).
Association between total lung volumes on inspiratory CT in the supine/standing/sitting positions and the total lung capacity on PFT (A), association between total lung volumes on expiratory CT in the supine/standing/sitting positions and the functional residual capacity on PFT (B), and association between total lung volume changes from expiration to inspiration on CT in the supine/standing/sitting positions and the inspiratory capacity on PFT (C), using Pearson correlation coefficient test. (A–C) Lines show estimated regression.
Interobserver and intraobserver agreements
Interobserver and intraobserver agreements (intraclass-correlation coefficients) for measuring CT-based lung and lobe volumes in the supine, standing, and sitting positions were substantial for all measurements (0.998–1.000) (Table 6).
Discussion
Our prospective study demonstrated that (1) inspiratory as well as expiratory CT-based volumes of the bilateral upper lobes, bilateral lower lobes, bilateral lungs, and total lungs were significantly higher in the standing and sitting positions than in the supine position, (2) no significant differences were found in the inspiratory right middle lobe volumes among the three positions and the expiratory right middle lobe volume was significantly lower in the standing and sitting positions than in the supine position, and (3) no significant differences were found in the inspiratory volumes of the total lung, right lung, left lung, and all lobes between the standing position and the sitting position. These data could have an impact on preoperative CT volumetry of the lung in patients with lung cancer (before lobectomy) for the prediction of postoperative residual pulmonary function. In addition, our findings of 100 asymptomatic volunteers could be used as the basis for elucidating undetermined pathological mechanisms, particularly when the symptoms of pulmonary diseases vary between supine and upright (standing and sitting) positions or when they have a predilection for a pulmonary lobe.
We found that the collapse of the right middle lobe in expiratory CT was more apparent in the standing/sitting position than in the supine position. The underlying etiology of nonobstructive right middle lobe syndrome is not yet well understood20, but there is a possibility that our data may provide clues to understanding the pathogenic mechanism of nonobstructive right middle lobe syndrome. Regarding inspiratory CT, a previous study reported that the inspiratory right middle lobe volume was similar between the supine and standing positions (with the subjects' arms down)6; with regard to the inspiratory volume, our conventional supine CT-based results with subjects’ arms raised (usually performed posture) are consistent with the previously reported results.
Our study also demonstrated that the bilateral upper lobe volume changes from expiration to inspiration were similar among the three positions. This may be explained by the previously reported phenomenon that the lower lungs undergo greater volume changes during breathing than do the upper lungs because of the effects of gravity on lung recoil6,21,22,23.
Our study showed that the total lung volume determined using inspiratory upright CT (in standing and sitting positions) was more similar to and more correlated with the total lung capacity on PFT than that determined in the supine position (intraclass-correlation coefficient, 0.927 and 0.946 vs. 0.831; r, 0.93 and 0.95 vs. 0.83). Furthermore, although associations between the total lung volumes on expiratory CT and the functional residual capacity on PFT were similar in the three positions, the total lung volume changes from expiration to inspiration determined using upright CT (in standing and sitting positions) tended to be more correlated with the inspiratory capacity on PFT than that determined using supine CT (r, 0.62 and 0.65 vs. 0.53). This may be because the PFT was performed in the sitting (upright) position, and the direction of the thorax in the PFT was more similar to that in upright CT than that in conventional supine CT6. Previous studies have reported that functional residual capacity on PFT was higher in the standing24 and sitting25 than in supine position among healthy subjects26. Our results of the total lung capacity on expiratory CT were consistent with those of these previous studies. As of June 23, 2020, there were more than 9.1 million confirmed cases of coronavirus disease 19 (COVID-19) globally27. To reduce the spread of COVID-19, many PFT laboratories have been closed or have significantly reduced their testing capacity at the time of writing this manuscript27. Considering our results, in addition to the morphological evaluation of the chest, inspiratory and expiratory upright CT could be used as an alternative tool to predict lung volumes such as total lung capacity, functional residual capacity, and inspiratory capacity in situations in which PFT cannot be performed, with relatively more accurate predictability compared with conventional supine CT. Nonetheless, in a previous study evaluating only inspiratory lung volume in the supine and standing positions (with the subject’s arms down)6, the acquired CT data could not provide a prediction of the functional residual capacity or inspiratory capacity because of the lack of expiratory CT data. In this study, to perform both inspiratory and expiratory CT, we used a tube voltage of 100 kVp and automatic exposure control with a noise index of 24 for a slice thickness of 5 mm (relatively low-radiation-dose protocol) because the low-radiation-dose CT with recent scanner technology or reconstruction methods is reported to be sufficient to detect lung cancers28, nodules29, and pneumonia including COVID-19 pneumonia30,31 and because low radiation dose is reported to be unrelated to the volume or area measurement accuracy32, whereas a previous study6 evaluating only inspiratory CT in the supine and standing positions used a tube voltage of 120 kVp and a noise index of 15.
Our study had several limitations. First, we included only 100 asymptomatic subjects at a single institution, and further studies in larger populations at multiple centers are required to confirm these preliminary findings. Second, in this study, although the observers independently evaluated the CT images in a randomized and blinded manner, they could recognize, to some extent, the positions of the subjects because of the absence or presence of a CT table. However, the lung and lobe volume measurements were semi-automated by using a commercially available workstation, and thus, the observer bias would have been negligible6. Furthermore, the interobserver and intraobserver agreements (intraclass-correlation coefficients) were high (> 0.99) in this study. Third, although all the participants underwent PFTs within two hours of CT examinations, PFTs were not performed simultaneously with the CT, which could have affected the results of the correlation between CT and PFT measurements. However, it was impossible to perform PFT including total lung capacity measurements in the bore of the CT.
Conclusions
Although the inspiratory and expiratory CT-based volumes of the bilateral upper lobes, bilateral lower lobes, bilateral lungs, and total lungs were significantly greater in the standing and sitting positions (with arms down) than in the supine position (with arms raised), the inspiratory right middle lobe volume did not change significantly in the three positions and the expiratory right middle lobe volume was significantly lower in the standing and sitting positions than in the supine position. The inspiratory volumes of the total lung, right lung, left lung, and all lobes were similar for the standing and sitting positions. The total lung volumes on inspiratory upright CT in the upright position (standing and sitting positions) were more similar to the total lung capacity on PFT than that on conventional CT in the supine position. Although associations between the total lung volumes on expiratory CT and the functional residual capacity on PFT were similar in the three positions, the total lung volume changes from expiration to inspiration determined using upright CT (standing and sitting positions) tended to be more closely correlated with the inspiratory capacity on PFT than volume changes determined using supine CT.
Data availability
The datasets generated during and/or analysed during the current study are available from the corresponding author on reasonable request.
References
Schaefer-Prokop, C., Neitzel, U., Venema, H. W., Uffmann, M. & Prokop, M. Digital chest radiography: an update on modern technology, dose containment and control of image quality. Eur. Radiol. 18, 1818–1830. https://doi.org/10.1007/s00330-008-0948-3 (2008).
Jinzaki, M. et al. Development of upright computed tomography with area detector for whole-body scans: phantom study, efficacy on workflow, effect of gravity on human body, and potential clinical impact. Investig. Radiol. 55, 73–83. https://doi.org/10.1097/RLI.0000000000000603 (2020).
Richard, J. C. et al. Effects of vertical positioning on gas exchange and lung volumes in acute respiratory distress syndrome. Intensive Care Med. 32, 1623–1626. https://doi.org/10.1007/s00134-006-0299-y (2006).
Zhu, M. et al. Upright position mechanical ventilation: an alternative strategy for ALI/ARDS patients?. Med. Hypotheses 73, 821–823. https://doi.org/10.1016/j.mehy.2009.03.023 (2009).
Robak, O. et al. Short-term effects of combining upright and prone positions in patients with ARDS: a prospective randomized study. Crit. Care 15, R230. https://doi.org/10.1186/cc10471 (2011).
Yamada, Y. et al. Differences in lung and lobe volumes between supine and standing positions scanned with conventional and newly developed 320-detectorrow upright CT: intra-individual comparison. Respiration 99, 598–605. https://doi.org/10.1159/000507265 (2020).
Blair, E. & Hickam, J. B. The effect of change in body position on lung volume and intrapulmonary gas mixing in normal subjects. J. Clin. Investig. 34, 383–389. https://doi.org/10.1172/jci103086 (1955).
Talaminos Barroso, A., Marquez Martin, E., Roa Romero, L. M. & Ortega Ruiz, F. Factors affecting lung function: a review of the literature. Arch. Bronconeumol. 54, 327–332. https://doi.org/10.1016/j.arbres.2018.01.030 (2018).
Kobayashi, K. et al. Three-dimensional computed tomographic volumetry precisely predicts the postoperative pulmonary function. Surg. Today 47, 1303–1311. https://doi.org/10.1007/s00595-017-1505-y (2017).
Yoshimoto, K. et al. Prediction of pulmonary function after lung lobectomy by subsegments counting, computed tomography, single photon emission computed tomography and computed tomography: a comparative study. Eur. J. Cardiothorac. Surg. 35, 408–413. https://doi.org/10.1016/j.ejcts.2008.10.057 (2009).
Wu, M. T. et al. Use of quantitative CT to predict postoperative lung function in patients with lung cancer. Radiology 191, 257–262. https://doi.org/10.1148/radiology.191.1.8134584 (1994).
Tenda, E. D., Ridge, C. A., Shen, M., Yang, G. Z. & Shah, P. L. Role of quantitative computed tomographic scan analysis in lung volume reduction for emphysema. Respiration 98, 86–94. https://doi.org/10.1159/000498949 (2019).
Bhatt, S. P. et al. Association Between expiratory central airway collapse and respiratory outcomes among smokers. JAMA 315, 498–505. https://doi.org/10.1001/jama.2015.19431 (2016).
Yamada, Y. et al. Dose reduction in chest CT: comparison of the adaptive iterative dose reduction 3D, adaptive iterative dose reduction, and filtered back projection reconstruction techniques. Eur. J. Radiol. 81, 4185–4195. https://doi.org/10.1016/j.ejrad.2012.07.013 (2012).
Miller, M. R. et al. Standardisation of spirometry. Eur. Respir. J 26, 319–338. https://doi.org/10.1183/09031936.05.00034805 (2005).
Graham, B. L. et al. Standardization of spirometry 2019 update. An official American Thoracic Society and European Respiratory Society technical statement. Am. J. Respir. Crit. Care Med. 200, e70–e88. https://doi.org/10.1164/rccm.201908-1590ST (2019).
The Committee of Pulmonary Physiology JRS. Forced expiratory curve, flow volume curve and peak flow. In The Clinical Respiratory Function Test 8th edn (ed. The Committee of Pulmonary Physiology JRS) 312–321 (Medical Review, Tokyo, 2016) (in Japanese).
Iwano, S. et al. Pulmonary lobar volumetry using novel volumetric computer-aided diagnosis and computed tomography. Interact. Cardiovasc. Thorac. Surg. 17, 59–65. https://doi.org/10.1093/icvts/ivt122 (2013).
Kitano, M. et al. Lobar analysis of collapsibility indices to assess functional lung volumes in COPD patients. Int. J. Chronic Obstr. Pulm. Dis. 9, 1347–1356. https://doi.org/10.2147/copd.s72616 (2014).
Gudbjartsson, T. & Gudmundsson, G. Middle lobe syndrome: a review of clinicopathological features, diagnosis and treatment. Respiration 84, 80–86. https://doi.org/10.1159/000336238 (2012).
Ratnovsky, A., Elad, D. & Halpern, P. Mechanics of respiratory muscles. Respir. Physiol. Neurobiol. 163, 82–89. https://doi.org/10.1016/j.resp.2008.04.019 (2008).
Tanaka, R. et al. Detectability of regional lung ventilation with flat-panel detector-based dynamic radiography. J. Digit. Imaging 21, 109–120. https://doi.org/10.1007/s10278-007-9017-8 (2008).
Yamada, Y. et al. Difference in the craniocaudal gradient of the maximum pixel value change rate between chronic obstructive pulmonary disease patients and normal subjects using sub-mGy dynamic chest radiography with a flat panel detector system. Eur. J. Radiol. 92, 37–44. https://doi.org/10.1016/j.ejrad.2017.04.016 (2017).
Chang, A. T., Boots, R. J., Brown, M. G., Paratz, J. D. & Hodges, P. W. Ventilatory changes following head-up tilt and standing in healthy subjects. Eur. J. Appl. Physiol. 95, 409–417. https://doi.org/10.1007/s00421-005-0019-2 (2005).
Yap, J. C., Moore, D. M., Cleland, J. G. & Pride, N. B. Effect of supine posture on respiratory mechanics in chronic left ventricular failure. Am. J. Respir. Crit. Care Med 162, 1285–1291. https://doi.org/10.1164/ajrccm.162.4.9911097 (2000).
Katz, S., Arish, N., Rokach, A., Zaltzman, Y. & Marcus, E. L. The effect of body position on pulmonary function: a systematic review. BMC Pulm. Med. 18, 159. https://doi.org/10.1186/s12890-018-0723-4 (2018).
Kouri, A. et al. Addressing reduced laboratory-based pulmonary function testing during a pandemic. Chest https://doi.org/10.1016/j.chest.2020.06.065 (2020).
Aberle, D. R. et al. Reduced lung-cancer mortality with low-dose computed tomographic screening. N. Engl. J. Med. 365, 395–409. https://doi.org/10.1056/NEJMoa1102873 (2011).
Yamada, Y. et al. Model-based iterative reconstruction technique for ultralow-dose computed tomography of the lung: a pilot study. Investig. Radiol. 47, 482–489. https://doi.org/10.1097/RLI.0b013e3182562a89 (2012).
Kalra, M. K., Homayounieh, F., Arru, C., Holmberg, O. & Vassileva, J. Chest CT practice and protocols for COVID-19 from radiation dose management perspective. Eur. Radiol. https://doi.org/10.1007/s00330-020-07034-x (2020).
Kang, Z., Li, X. & Zhou, S. Recommendation of low-dose CT in the detection and management of COVID-2019. Eur. Radiol. 30, 4356–4357. https://doi.org/10.1007/s00330-020-06809-6 (2020).
Yamada, Y. et al. CT Dose Reduction for visceral adipose tissue measurement: effects of model-based and adaptive statistical iterative reconstructions and filtered back projection. AJR Am. J. Roentgenol. 204, W677–W683. https://doi.org/10.2214/ajr.14.13411 (2015).
Acknowledgements
This study was supported by Japan Society for the Promotion of Science (JSPS) KAKENHI (grant number 17H04266, 17K16482, and 20K08056), Uehara Memorial Foundation, and Canon Medical Systems (Otawara, Japan). The authors would like to acknowledge all of the volunteers for their willingness to participate in the study. The authors thank Dr. Keiichi Narita, Dr. Takehiro Nakahara, Naomi Tamaki, and Kyoko Komatsu for their valuable assistance.
Author information
Authors and Affiliations
Contributions
Y.Y., M.Y., Y.Y., and M.J. were responsible for the conception or design of the work; Y.Y., M.Y., Y.Y., S.M., A.T., and Y.N. were responsible for the acquisition of data; Y.Y., M.Y., S.C., and Y.Y analyzed and interpreted the data; and Y.Y., M.Y., S.C., Y.Y., S.M., A.T., Y.N., M.M., K.F., and M.J. drafted or revised the paper for important intellectual content and provided a final approval of the data.
Corresponding author
Ethics declarations
Competing interests
Masahiro Jinzaki received a grant from Canon Medical Systems. However, Canon Medical Systems was not involved in the design and conduct of the study; in the collection, analysis, and interpretation of the data; or in the preparation, review, and approval of the manuscript. The remaining authors have no conflicts of interest to declare (Y. Y., M. Y., S. C., Y. Y., S. M., A. T., Y. N., M. M., and K. F.).
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Yamada, Y., Yamada, M., Chubachi, S. et al. Comparison of inspiratory and expiratory lung and lobe volumes among supine, standing, and sitting positions using conventional and upright CT. Sci Rep 10, 16203 (2020). https://doi.org/10.1038/s41598-020-73240-8
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41598-020-73240-8
This article is cited by
-
Verification of acromion marker cluster and scapula spinal marker cluster methods for tracking shoulder kinematics: a comparative study with upright four-dimensional computed tomography
BMC Musculoskeletal Disorders (2024)
-
Upright CT-based evaluation of the effects of posture on skull-base reconstruction after endoscopic endonasal surgery
Scientific Reports (2024)
-
Three-dimensional analysis reveals a high incidence of lung adenocarcinoma in the upper region
Surgery Today (2024)
-
Volume changes of diseased and normal areas in progressive fibrosing interstitial lung disease on inspiratory and expiratory computed tomography
Japanese Journal of Radiology (2024)
-
High resolution propagation-based lung imaging at clinically relevant X-ray dose levels
Scientific Reports (2023)
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.