Abstract
The COVID-19 pandemic, caused by the Severe Acute Respiratory Syndrome Coronavirus 2 (SARS-CoV-2), was declared on March 11, 2020 by the World Health Organization. As of the 31st of May, 2020, there have been more than 6 million COVID-19 cases diagnosed worldwide and over 370,000 deaths, according to Johns Hopkins. Thousands of SARS-CoV-2 strains have been sequenced to date, providing a valuable opportunity to investigate the evolution of the virus on a global scale. We performed a phylogenetic analysis of over 1,225 SARS-CoV-2 genomes spanning from late December 2019 to mid-March 2020. We identified a missense mutation, D614G, in the spike protein of SARS-CoV-2, which has emerged as a predominant clade in Europe (954 of 1,449 (66%) sequences) and is spreading worldwide (1,237 of 2,795 (44%) sequences). Molecular dating analysis estimated the emergence of this clade around mid-to-late January (10–25 January) 2020. We also applied structural bioinformatics to assess the potential impact of D614G on the virulence and epidemiology of SARS-CoV-2. In silico analyses on the spike protein structure suggests that the mutation is most likely neutral to protein function as it relates to its interaction with the human ACE2 receptor. The lack of clinical metadata available prevented our investigation of association between viral clade and disease severity phenotype. Future work that can leverage clinical outcome data with both viral and human genomic diversity is needed to monitor the pandemic.
Similar content being viewed by others
Introduction
In late December 2019, a cluster of atypical pneumonia cases was reported and epidemiologically linked to a wholesale seafood market in Wuhan, Hubei Province, China1. The causative agent was identified as a novel RNA virus of the family Coronaviridae and was subsequently designated SARS-CoV-2 owing to its high overall nucleotide similarity to SARS-CoV, which was responsible for previous outbreaks of severe acute respiratory syndrome in humans between 2002 and 20042,3. Previous studies of SARS-CoV-2 genomes sequenced during the early months of the epidemic (late December 2019 up to early February 2020) estimated the time of its emergence at the end of November (18th and 25th)4,5,6, approximately a month before the first confirmed cases. It has been hypothesized that SARS-CoV-2 may have undergone a period of cryptic transmission in asymptomatic or mildly symptomatic individuals, or in unidentified pneumonia cases prior to the cluster reported in Wuhan in late December 20193. Based on the high nucleotide identity of SARS-CoV-2 to a bat coronavirus isolate (96%)7, a possible scenario is that SARS-CoV-2 had undergone a period of adaptation in an as yet identified animal host, facilitating its capacity to jump species boundaries and infect humans3. The present rapid spread of the virus worldwide, coupled with its associated mortality, raises an important concern of its further potential to adapt to more highly transmissible or virulent forms.
The availability of SARS-CoV-2 genomic sequences concurrent with the present outbreak provides a valuable resource for improving our understanding of viral evolution across location and time. We performed an initial phylogenetic analysis of 749 SARS-CoV-2 genome sequences from late-December 2019 to March 13, 2020 (based on publicly available genome sequences on GISAID) and noted 152 SARS-CoV-2 sequences initially isolated in Europe beginning in February, 2020, which appear to have emerged as a distinct phylogenetic clade. Upon further investigation, we found that these strains are distinguished by a derived missense mutation in the spike protein (S-protein) encoding gene, resulting in an amino acid change from an aspartate to a glycine residue at position 614 (D614G). At the time of our study, the D614G mutation was at particularly high frequency 20/23 (87%) among Italian SARS-CoV-2 sequenced specimens, which was then emerging as the most severely affected country outside of China, with an overall case fatality rate of 7.2%8.
During the course of our analysis, the number of available SARS-CoV-2 genomes increased substantially. We subsequently analyzed a total of 2,795 genome sequences of SARS-CoV-2 (Supplementary data Table 1). For those sequences with demographics (65% of sequenced specimens), the male to female ratio was 0.56:0.44, with a median age of 49 years old, and a range from less than 1 to 99 years old. As of 30 March 2020, the D614G clade includes 954 of 1,449 (66%) of European specimens and 1,237 of 2,795 (44%) worldwide sequenced specimens. A comparison against the previous set of genomes collected for our phylogenetic and molecular dating analysis revealed that for samples submitted during the period from March 17–30, 2020, the D614G clade became increasingly prevalent worldwide, expanding from 22 to 42 countries (Fig. 1), as also reported previously9,10. The demographic distribution for this mutation, when known, (male to female ratio, 0.56:0.44; median age, 48 years old; age range, less than 1–99 years old) was not significantly different compared to the reported demographics for all sequenced SARS-CoV-2 specimens.
Global Distribution of SARS-CoV-2 Genome Sequences Possessing the Spike Protein D614G Mutation. G mutation as percentage of total sequences (% G) is represented with color shades as detailed in legend including data available as of (A) 17 March and (B) 30 March 2020. Hatched lines were added when less than 10 sequences were available for one country. The maps were built with the geographic information system QGIS (v2.18.21, https://qgis.org).
We employed molecular dating to estimate the time of emergence of the D614G clade. Based on a curated set of 442 genomes representing the sequence diversity of SARS-CoV-2 samples available at the time of analysis (30 March 2020), the mean time to most recent common ancestor (tMRCA) was estimated to be on 18 January 2020 (95% highest posterior density (HPD) interval: 10 January–25 January), indicating its relatively recent emergence (Fig. 2). Although the mutation appears to be clade-specific, we noted that D614G also arose another time in a single isolate belonging to a distinct lineage, Wuhan/HBCDC-HB-06/2020 (EPI 412982), collected on 7 February 2020. Given the high degree of nucleotide identity of the D614G clade (~ 99.6%), we expect that future tMRCA estimates will not differ substantially. The mean tMRCA for the root of the tree was estimated to be 13 November 2019 (95% HPD interval: 19 October 2019 to 5 December 2019) which is similar to what has been estimated previously4. Multiple factors can influence these estimates as more data become available: increased diversity and number of strains included for analysis, expanded range of sampling dates compared to earlier studies, as well as incomplete/biased sampling of available genomes. Therefore, caution should be used when inferring broad and definite conclusions about the epidemiology of the emerging outbreak in real-time, particularly as the early undocumented stages of SARS-CoV-2 transmission is largely unknown3. They should be taken as tentative estimates based on limited sampling, which are subject to change when additional epidemiological information becomes available. For instance, as different countries review and test archived specimens from cases of severe pneumonia or influenza-like illness for SARS-CoV-2, it is expected that additional cases may be identified, such as in France where a patient without travel history to China was identified to have COVID-19 in late December concurrent with the initial reported cases from Wuhan11. These retrospective analyses will provide crucial insights into the early transmission dynamics and evolution of SARS-CoV-2 and its rapid global spread.
Estimated Molecular Dating of Evolutionary History of 442 Representative Global SARS-CoV-2 Sequences (Late-December 2019–Mid-March 2020) and the Emergence of the D614G Clade. Maximum clade credibility (MCC) tree with dated branches estimated by Bayesian Evolutionary Analysis Sampling Trees (BEAST). Node colors indicate continents of isolation; x-axis indicating dates by year and days in decimal notation; D614G clade sequences are highlighted in a yellow box.
From our findings of the recent emergence of the D614G clade and the increasing number of specimens harboring the mutation identified worldwide, we sought to investigate the potential significance of the mutation on clinical disease severity phenotypes. Unfortunately, only limited clinical disease severity data was available for patients whose sequenced samples were included in our analysis (asymptomatic 64, symptomatic 8, mild symptoms 2, pneumonia 4, hospitalized 163, released 48, recovered/recovering 26, nursing home 3, live 24, intensive care unit 2, deceased 1), preventing us from being able to meaningfully correlate disease severity and genotype from these data. However, using country-wide crude case fatality data for countries from which sequencing data was available, there was no significant correlation between proportion of D614G clade sequences and crude case fatality rate as of 30 March 2020 (Spearman’s rank correlation coefficient, r 0.22, 95% CI − 0.12 to 0.51). In addition, on analysis of crude case fatality rate by age-group (available for China, Italy, South Korea, Spain, and Canada) there was no significant correlation with proportion of D614G clades in the sequences analysed for these countries (Supplementary Table 2)8,12,13,14. A major limitation of this analysis is that publicly available SARS-CoV-2 genomes are the result of convenience sampling and are not expected to provide an accurate representation of the spatial-demographic distribution of SARS-CoV-2 genotypes. Therefore, one must be cautious about making inferences about severity and transmission of variants15 from genomic sequence data alone.
The possibility that the D614G mutation may still have a potential impact on the function of the SARS-CoV-2 spike protein could not be excluded. Previous studies of SARS-CoV have shown that the sequential accumulation of mutations in the spike protein increased its affinity to ACE2 and likely impacted its transmission and disease severity during the course of outbreaks in 2002–200416,17,18. Recently, Phan studied 86 complete SARS-CoV-2 genomes, identifying 42 missense mutations, eight of which occurred in the S-protein gene2. However, at the time of the study, the mutation D614G was only found in one sequence from Germany (collected on 28 January, 2020). Modifications in the spike protein are of interest as they might indicate the emergence of a novel strain of SARS-CoV-2 with change in transmissibility or pathogenicity. Therefore, we investigated the potential functional and epidemiological consequences of the D614G mutation with structural modeling of the SARS-CoV-2 spike (S) protein and its interaction with the angiotensin-converting enzyme 2 (ACE2) receptor.
The structure of the SARS-CoV-2 spike (S) protein is shown in Fig. 3. The S protein is a heavily glycosylated trimeric protein that mediates entry to host cells via fusion with ACE2. Recently, Wrapp and colleagues used Cryo-EM to determine the structure of the S protein and analyze its conformational changes during infection19. Using their three-dimensional model of the S protein structure, we set out to investigate the effects that a mutation in position 614 might have. First, we analyzed changes in inter-atomic contacts within a radius of 6 Å from position 614 before and after substitution of aspartate by glycine. Notably, four inter-chain destabilizing (i.e., hydrophobic-hydrophilic) contacts are lost with residues of an adjacent chain upon D614G mutation (see Table 1 and Fig. 3C). This suggests that a small repelling interaction between adjacent chains is removed upon this aspartate substitution (see Table 1). However, it is unlikely that this would have a significant effect on recognition and binding to ACE2 given the relative distal position of this mutation with respect to the receptor-binding domain (RBD) (see Fig. 3B), but further analyses would be required to assess whether the D614G mutation has an effect on the way the S protein changes its conformation after interaction with ACE2. Lan and colleagues also showed residues in the RBD act as epitopes for SARS-CoV-2 and mutations can influence antibody binding20. Given the important role that glycosylation plays in regulating the function of spike proteins in coronaviruses21, we decided to search for potential changes in a glycosylated residue (asparagine) in position 616. As shown in Fig. 3D, this residue and aspartate 614 are oriented in opposite directions, suggesting that substitution by glycine also has a null effect on this interaction. Finally, neither position 614 nor the inter-atomic contacts at positions 854, 859, 860, 861 of the spike protein lie in a polybasic cleavage region which is of importance for SARS-CoV-2 as it has been proposed to activate the protein for membrane fusion22. Our results are consistent with the work by Wrapp and colleagues, where they identified nine missense mutations (including D614G) in the spike protein that were thought to be relatively conservative and thus unlikely to affect protein function19.
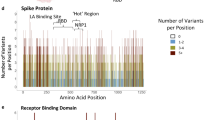
Structural analysis of SARS-CoV-2 spike protein around position 614. (A) Location and distribution of SARS-CoV-2 viral proteins. The full trimeric form of the spike protein results from a complex of three identical spike monomers (right panel). (B) Three-dimensional depiction of a spike protein monomer. The receptor-binding domain is colored purple and the location of the aspartate residue in position 614 is highlighted in green. (C) Inter-atomic contacts between aspartate 614 (green) in a reference spike monomer (blue) and four residues (pink) in its adjacent spike protein monomer chain (white). These four contacts are destabilizing and create a hydrophilic-hydrophobic repelling effect that is lost upon replacement of aspartate by glycine in the D614G mutation (see Table 1). (D) Spatial distribution of aspartate 614 residue (green) and an adjacent glycosylated asparagine residue in position 616 (orange). The two residues point in opposite directions and thus it is unlikely they share a meaningful interaction. The image (A) was drawn using Affinity Designer (v1.8) (https://affinity.serif.com/en-gb/designer/). The trimeric and monomeric structures of the Spike protein were generated using Illustrate19,41 (https://ccsb.scripps.edu/illustrate/) by rendering a protein structure from the Protein Data Bank with ID 6vsb19 (https://www.rcsb.org/structure/6vsb). The image (B–D) was generated using UCSF Chimera (v1.14) (https://www.cgl.ucsf.edu/chimera/) with monomeric protein structure rendered in Chimera 19.
There were important limitations faced in our present analysis which are likely to be a significant hurdle to similar studies in the future. The lack of available clinical metadata prevented our investigation of association between viral clade and disease severity phenotype. Additionally, numbers of sequenced SARS-CoV-2 samples vary greatly between countries and may be subject to potential sampling bias. It is important to note that current country level data on crude case fatality rates and case numbers do not permit robust comparison of clinical phenotype across countries due to significant differences in population demographics, testing protocols, case definitions and implementation of public health measures. Accordingly, it was not possible to draw any conclusions regarding the clinical phenotype of the D614G clade and there is no evidence at this time to suggest this clade is associated with any differences in disease phenotype23. As a potential proxy measure for viral load, we reviewed the cycle threshold (Ct) values of the SARS-CoV-2 assay for samples sequenced from Ontario, Canada (total n = 178, with 50 and 128 samples possessing the spike protein 614-D and 614-G amino acids, respectively). In this small selection of samples, we found no significant difference in the average Ct for 614-D and 614-G amino acids (mean 22.35, SD 5.13 and mean 22.32, SD 5.188 respectively, t-test p-value = 0.978) (Fig. 4). We do note, however, that numerous factors affect the measurement and limit the reliability of Ct value measurement, including sample type, quality of swabs, quality of collection method, and time from onset to sample collection24. In contrast, another study has found a statistically significant decrease in PCR Ct values associated with the mutated amino acid G variant10 but its clinical significance remains unclear. In spite of the lack of evidence for phenotypic differences, it is interesting that in a short period of time since its emergence the D614G clade has become widespread all around the world. It is possible that even if the observed mutation does not impact the protein’s interaction with ACE2, it may not be completely neutral with respect to viral fitness. For example, given that the molecular weight of glycine is significantly smaller than that of aspartate, the mutation could be advantageous from a cost minimization point of view25. It is also possible that the mutation may be in linkage disequilibrium with a selectively advantageous variant impacting another aspect of viral reproduction. For example, most strains of the D614G clade also harbor a mutation (P4715L) in orf1ab and a subclade processes three nucleotide changes in the nucleoprotein (N) gene (GGG to AAC; G204R), which plays diverse roles in virion assembly as well as genome transcription and translation26,27. Most recently, it has been suggested that D614G introduces a new elastase cleavage site that may be differentially activated by host genomic mutations thereby facilitating spike processing, and entry into host cells in some host populations but not others28. Finally, the global spread of the D614G mutation may have nothing to do with viral biology but may simply be a consequence of the high level of interconnectedness of Europe to the rest of the world. Thus, the emergence of the D614G clade may be explained by a founder event and subsequent clonal expansion in Europe that led to its spreading worldwide.
Genomic sequencing and phylogenetic analysis are powerful approaches to track viral evolution during the course of a pandemic and help coordinate the global implementation of strategies for decreasing virus transmission and mitigating global mortality. However, our study highlights that caution is warranted in hastily drawing conclusions from limited observational data. Future work that can leverage clinical outcome data with both viral and human genomic diversity, in vitro and in vivo tests and in silico modeling will greatly enhance our ability to understand if specific SARS-CoV-2 clades are evolving with respect to virulence or transmissibility, and identify genetic variants associated with viral adaptation, transmissibility, and mortality. These data will be essential for effective vaccine development and public health responses to this emergent pandemic.
Materials and methods
Sequence data, demographics, maps and statistics
A total of 2,803 genomes of SARS-CoV-2 (excluding non-human sequences specimens) and demographics when available were obtained from GISAID (https://gisaid.org/) (downloaded on 30 March 2020) to perform the statistical analyses of the D614G mutation (8 sequences were excluded due to ambiguous or unknown nucleotide at this position). The dataset included sequences representing 55 countries. The world geographical maps were built with the geographic information system QGIS (v2.18.21, https://qgis.org). Global CFR was calculated from data according to Johns Hopkins as of 30 March 2020. CFR for age groups of different countries were extracted from country-specific published data8,12,13,14. Spearman’s rank correlation analysis was performed using GraphPad prism (v8.3.1).
PCR and sequencing
SARS-CoV-2 E-gene PCR on respiratory specimens (e.g. nasopharyngeal swabs and bronchoalveolar lavages) submitted to Public Health Ontario Laboratory was performed as previously described29. Specimens with Ct values of 32 or less were selected for whole genome sequencing. Briefly, rRNA depleted RNA was reverse transcribed with SuperScript III Reverse Transcriptase (Invitrogen/Life Technologies, Carlsbad, CA) to cDNA using tagged random primer (5′-GTTTCCCAGTCACGATA-(N9)-3′) followed by second strand DNA synthesis using Sequenase (Thermo Fisher Scientific, Waltham, MA). Amplification of double stranded cDNA was done with primer 5′-GTTTCCCAGTCACGATA-3′ using AccuTaq LA DNA Polymerase according to manufacture recommendation. Amplified products were purified using 1.0 × ratio of Agencourt AMPure XP beads (Beckman Coulter) and quantified with Qubit 2.0 Fluorometer by using Qubit dsDNA HS Assay Kit (Thermo Fisher Scientific). Nextera XT DNA Library Preparation kit (Illumina) following manufacturer’s instructions was used for Library preparation and indexing. The sequencing library was quantified using Qubit 2.0 (Invitrogen, Waltham, MA, USA) and average size was determined by 4200 TapeStation using the D5000 ScreenTape assay (Agilent Technologies, US). The library was normalized to 4 nMol and sequenced on the Illumina MiSeq platform, using Illumina MiSeq reagent kit v2 (2 × 150 bp), according to the manufacturer’s instructions. CLC Genomics Workbench version 8.0.1 (CLC bio, Germantown, MD, USA) was used for both reference assembly and de novo assembly. Additionally, we used protocol published by Artic Network30. The method is based on overlapping specific primers producing short amplicon covering entire genome. Briefly, cDNA synthesis and amplicon generation using 2 individual pools of primers was done according to the published protocol30. The two pools of amplicons were combined together and cleaned by Agencourt AMPure XP beads (Beckman Coulter) prior to library preparation using Nextera XT (Illumina) following the manufacturer protocol except that half volume of the reagent was used throughout the protocol. Agencourt AMPure XP beads (Beckman Coulter) in ratio of 1.0 were used for the final purification step followed by measurement by Qubit 2.0 and average size determination, using 2,200 TapeStation (Agilent Technologies, USA). All libraries were manually normalized to 4 nMol. Libraries were combined in equal volumes for denaturation and subsequent dilution according to MiSeq protocol recommended by manufacturer.
Molecular evolution
A total of 2,803 SARS-CoV-2 genomes were obtained from GISAID (downloaded on March 30th 2020). Initial quality filtering was performed by iteratively removing redundant sequences with 100% nucleotide identity, having less than 2,940 informative positions, and lacking informative sampling dates. The resulting 2,017 curated sequences were aligned using mafft31 (v7.450: –retree 2 –maxiterate 2 –auto settings), and unaligned ends and gap positions from the resulting alignment were removed using Geneious (vR10.2.6, https://www.geneious.com). A Maximum-likelihood tree was constructed using IQTree32 (v1.6.1: -model HKY) and used for identification and removal of highly divergent sequences with Treetime33 (clock setting). Following previous recommendations (adapted from https://virological.org/t/issues-with-sars-cov-2-sequencing-data/473)34 to account for regions which might potentially be the result of hypervariability or sequencing artifacts, alignment positions showing significant homoplasy were first identified using Treetime (homoplasy setting). Top-10 significant homoplastic positions were merged from three separate analyses, using all sequences from the initial alignment, and sequence subsets generated using Illumina (1,450 samples) or Nanopore (341 samples) sequencing technologies. Next, recombinant clusters of mutations were identified with ConalFrameML35. Identified positions were masked using a custom-written python script, and further filtered for sequences with 100% nucleotide identity, resulting in an alignment of 1,225 sequences. Finally, to reduce sampling bias only one sample per country was kept for date of sampling, leading to 442 sequences. Molecular dating analysis was performed by the Markov chain Monte Carlo (MCMC) method implemented by Bayesian Evolutionary Analysis on Sampling Trees (BEAST) 1.10.436. A HKY85 nucleotide substitution model was used. Fixed and relaxed molecular clock models were fitted, and constant population size was compared with exponential population growth. All models were run using default priors except for the exponential growth rate (Laplace distribution) in which scale was set to 100. The chain length was set to 100 million states and burn-in of 10 million. Convergence was checked with Tracer 1.7.137. Based on ESS values, estimates for tMRCA of the European Clade spike protein mutation and root age are reported under the strict molecular clock and constant population growth (ESSs > 900). The resulting coalescent tree was generated using TreeAnnotator38 and visualized using ggtree package39 in R version 3.6.1 (https://www.r-project.org/).
Structural analyses
Visualization, analysis and in silico mutations of protein structures were done in UCSF Chimera18. First, we downloaded the molecular structure of the spike protein from the Protein Data Bank (PDB). This structure corresponds to that resolved by Wrapp and colleagues19 and deposited in PDB with identifier number 6vsb. We replaced the aspartate residue in position 614 by glycine using the “Rotamers” function in Chimera with default parameters. Then, inter-atomic contacts of both residues at position 614 were derived with the CSU package19 freely available at https://oca.weizmann.ac.il/oca-bin/lpccsu.
Ethics statement
Specimens were collected from patients by submitters and sent to PHOL for testing as part of routine clinical service. These data are also used for routine laboratory surveillance, which is a mandate of Public Health Ontario. Therefore, consultation with our organization’s privacy office or ethics committee was not required. To protect patient privacy and confidentiality, data are reported in an anonymized format.
References
Zhu, N. et al. A novel coronavirus from patients with pneumonia in China, 2019. N. Engl. J. Med. 382, 727–733 (2020).
Phan, T. Genetic diversity and evolution of SARS-CoV-2. Infect. Genet. Evol. 81, 104260 (2020).
Zhang, Y.-Z. & Holmes, E. C. A genomic perspective on the origin and emergence of SARS-CoV-2. Cell 1, 1–5. https://doi.org/10.1016/j.cell.2020.03.035 (2020).
Andersen, K. G., Rambaut, A., Lipkin, W. I., Holmes, E. C. & Garry, R. F. The proximal origin of SARS-CoV-2. Nat. Med. 2–4 (2020) doi:https://doi.org/10.1038/s41591-020-0820-9.
Benvenuto, D. et al. The global spread of 2019-nCoV: a molecular evolutionary analysis. Pathog. Glob. Health 114, 64–67 (2020).
Lai, A., Bergna, A., Acciarri, C., Galli, M. & Zehender, G. Early phylogenetic estimate of the effective reproduction number of SARS-CoV-2. J. Med. Virol. https://doi.org/10.1002/jmv.25723 (2020).
Zhou, P. et al. A pneumonia outbreak associated with a new coronavirus of probable bat origin. Nature 579, 270–273 (2020).
Onder, G., Rezza, G. & Brusaferro, S. Case-fatality rate and characteristics of patients dying in relation to COVID-19 in Italy. JAMA J. Am. Med. Assoc. 2019, 2019–2020 (2020).
Kiyotani, K., Toyoshima, Y., Nemoto, K. & Nakamura, Y. Bioinformatic prediction of potential T cell epitopes for SARS-Cov-2. J. Hum. Genet. https://doi.org/10.1038/s10038-020-0771-5 (2020).
Korber, B. et al. Tracking changes in SARS-CoV-2 spike: evidence that D614G increases infectivity of the COVID-19 virus. Cell https://doi.org/10.1016/j.cell.2020.06.043 (2020).
Deslandes, A. et al. SARS-CoV-2 was already spreading in France in late December 2019. Int. J. Antimicrob. Agents 106006 (2020) https://doi.org/10.1016/j.ijantimicag.2020.106006.
COVID-19 National Emergency Response Center Korea Centers for Disease Control and Prevention, E. and C. M. T. Coronavirus Disease-19: The First 7,755 Cases in the Republic of Korea. Osong public Heal. Res. Perspect. 11, 85–90 (2020).
Centro de Coordinación de Alertas y Emergencias Sanitarias. Actualización no 71. Enfermedad por el coronavirus (COVID-19). (2020).
Government of Canada. Coronavirus Disease 2019 (COVID-19) Daily epidemiology update. vol. 2019 (2020).
MacLean OA, Orton R, Singer JB, R. D. Response to “On the origin and continuing evolution of SARS-CoV-2”. http://virological.org/t/response-to-on-the-origin-and-continuing-evolution-of-sars-cov-2/418/4 (2020).
Li, W. et al. Receptor and viral determinants of SARS-coronavirus adaptation to human ACE2. EMBO J. 24, 1634–1643 (2005).
He, J. F. et al. Molecular evolution of the SARS coronavirus, during the course of the SARS epidemic in China. Science (80-) 303, 1666–1669 (2004).
Song, H. D. et al. Cross-host evolution of severe acute respiratory syndrome coronavirus in palm civet and human. Proc. Natl. Acad. Sci. U. S. A. 102, 2430–2435 (2005).
Wrapp, D. et al. Cryo-EM structure of the 2019-nCoV spike in the prefusion conformation. Science (80-) 367, 1260–1263 (2020).
Lan, J. et al. Structure of the SARS-CoV-2 spike receptor-binding domain bound to the ACE2 receptor. Nature 581, 215–220 (2020).
Shen, S., Tan, T. H. P. & Tan, Y.-J. Expression, glycosylation, and modification of the spike (S) glycoprotein of SARS CoV. Methods Mol. Biol. 379, 127–135 (2007).
Walls, A. C. et al. Structure, function, and antigenicity of the SARS-CoV-2 spike glycoprotein. Cell 181, 281-292.e6 (2020).
Grubaugh, N. D., Hanage, W. P. & Rasmussen, A. L. Making sense of mutation: what D614G means for the COVID-19 pandemic remains unclear. Cell https://doi.org/10.1016/j.cell.2020.06.040 (2020).
Chan, J.F.-W. et al. Improved molecular diagnosis of COVID-19 by the novel, highly sensitive and specific COVID-19-RdRp/Hel real-time reverse transcription-PCR assay validated in vitro and with clinical specimens. J. Clin. Microbiol. 58, 1 (2020).
Seligmann, H. Cost-minimization of amino acid usage. J. Mol. Evol. 56, 151–161 (2003).
Chang, C.-K. et al. Multiple nucleic acid binding sites and intrinsic disorder of severe acute respiratory syndrome coronavirus nucleocapsid protein: implications for ribonucleocapsid protein packaging. J. Virol. 83, 2255–2264 (2009).
Pachetti, M. et al. Emerging SARS-CoV-2 mutation hot spots include a novel RNA-dependent-RNA polymerase variant. J. Transl. Med. 18, 179 (2020).
Bhattacharyya, C. et al. Global spread of SARS-CoV-2 subtype with spike protein mutation D614G is shaped by human genomic variations that regulate expression of TMPRSS2 and MX1 genes. Preprint. bioRxiv 2020.05.04.075911 (2020). https://doi.org/10.1101/2020.05.04.075911.
Marchand-Senécal, X. et al. Diagnosis and management of first case of COVID-19 in Canada: lessons applied from SARS. Clin. Infect. Dis. https://doi.org/10.1093/cid/ciaa227 (2020).
Quick, J. nCoV-2019 sequencing protocol. protocols.io 1–24 (2020) https://doi.org/10.17504/protocols.io.bbmuik6w.
Katoh, K. & Standley, D. M. MAFFT multiple sequence alignment software version 7: improvements in performance and usability. Mol. Biol. Evol. 30, 772–780 (2013).
Nguyen, L.-T., Schmidt, H. A., von Haeseler, A. & Minh, B. Q. IQ-TREE: a fast and effective stochastic algorithm for estimating maximum-likelihood phylogenies. Mol. Biol. Evol. 32, 268–274 (2015).
Miura, S. et al. A new method for inferring timetrees from temporally sampled molecular sequences. PLoS Comput. Biol. 16, e1007046 (2020).
De Maio, N. et al. Issues with SARS-CoV-2 sequencing data. http://virological.org/t/issues-with-sars-cov-2-sequencing-data/473 (2019).
Didelot, X. & Wilson, D. J. ClonalFrameML: efficient inference of recombination in whole bacterial genomes. PLoS Comput. Biol. 11, e1004041 (2015).
Bouckaert, R. et al. BEAST 2: a software platform for Bayesian evolutionary analysis. PLoS Comput. Biol. 10, e1003537 (2014).
Rambaut, A., Drummond, A. J., Xie, D., Baele, G. & Suchard, M. A. Posterior summarization in Bayesian phylogenetics using Tracer 1.7. Syst. Biol. 67, 901–904 (2018).
Bouckaert, R. et al. BEAST 2.5: an advanced software platform for Bayesian evolutionary analysis. PLoS Comput. Biol. 15, e1006650 (2019).
Yu, G., Smith, D. K., Zhu, H., Guan, Y. & Lam, T. T. Y. Ggtree: an R package for visualization and annotation of phylogenetic trees with their covariates and other associated data. Methods Ecol. Evol. 8, 28–36 (2017).
Sobolev, V., Sorokine, A., Prilusky, J., Abola, E. E. & Edelman, M. Automated analysis of interatomic contacts in proteins. Bioinformatics 15, 327–332 (1999).
Goodsell, D. S., Autin, L. & Olson, A. J. Illustrate: software for biomolecular illustration. Structure 27, 1716-1720.e1 (2019).
Acknowledgements
We are very grateful to Dr William P. Hanage for his expert comments and advice on the preparation of this manuscript. We would like to thank Manon Tetreault for data collection. We are grateful to the numerous scientists who have shared their genome data with the world on GISAID (Supplementary data Table3). Funding was provided by the Canadian Institutes of Health Research and the Natural Sciences and Engineering Research Council of Canada Collaborative Health Research Project Grant [CP-151952] and Public Health Ontario.
Author information
Authors and Affiliations
Contributions
S.I., H.E.G., S.M.P.: study design, data analyses, manuscript redaction. L.G.-M., C.B.T., D.S.G.: study design, phylogenetic analyses, created Fig. 2, manuscript redaction. J.M.G., T.P.: study design, protein function analyses, created Fig. 3, manuscript redaction. M.R.I.: geographic data analysis, created Fig. 1, manuscript redaction. A.E., S.N.P., J.B.G.: study design, sequencing, manuscript redaction.
Corresponding author
Ethics declarations
Competing interests
Dr. Gubbay has received research Grants from GlaxoSmithKline Inc. and Hoffman-La Roche Ltd to study antiviral resistance in influenza, and from Pfizer Inc. to conduct microbiological surveillance of Streptococcus pneumoniae. These activities are not relevant to this study. Dr. Poutanen has received honoraria from Merck related to advisory boards and talks, honoraria from Verity, Cipher, and Paladin Labs related to advisory boards, partial conference travel reimbursement from Copan, and research support from Accelerate Diagnostics and bioMerieux, all outside the submitted work. All other authors declared that they have no competing interests.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Isabel, S., Graña-Miraglia, L., Gutierrez, J.M. et al. Evolutionary and structural analyses of SARS-CoV-2 D614G spike protein mutation now documented worldwide. Sci Rep 10, 14031 (2020). https://doi.org/10.1038/s41598-020-70827-z
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41598-020-70827-z
This article is cited by
-
Genetic determination of regional connectivity in modelling the spread of COVID-19 outbreak for more efficient mitigation strategies
Scientific Reports (2023)
-
The high mutation rate at the D614G hotspot-furin cleavage site region increases the priming efficiency of the Spike protein by furin protease: analysis of Indonesian SARS-CoV-2 G614 variants obtained during the early COVID-19 pandemic
VirusDisease (2023)
-
Cross-protection and cross-neutralization capacity of ancestral and VOC-matched SARS-CoV-2 adenoviral vector-based vaccines
npj Vaccines (2023)
-
A random priming amplification method for whole genome sequencing of SARS-CoV-2 virus
BMC Genomics (2022)
-
Epidemiological characterization of SARS-CoV-2 variants in children over the four COVID-19 waves and correlation with clinical presentation
Scientific Reports (2022)
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.