Abstract
This study intends to explore the prevalence of diabetes mellitus (DM) and its associated factors in Bangladesh. The necessary information was extracted from Bangladesh Demographic and Health Survey (BDHS) 2011. In bivariate analysis, Chi-square test was performed to assess the association between selected covariates and diabetes status. A two-level logistic regression model with a random intercept at each of the individual and regional level was considered to identify the risk factors of DM. A total of 7,535 individuals were included in this study. From the univariate analysis, the prevalence of DM was found to be 33.3% in 50–54 age group for instance. In bivariate setup, all the selected covariates except sex of the participants were found significant for DM (p < 0.05). According to the two-level logistic regression model, the chance of occurring DM increases as age of the participants’ increases. It was observed that female participants were more likely to have DM. The occurrence of DM was 62% higher for higher educated participants, 42% higher for the individuals who came from rich family and 63% higher for the individuals having hypertension. The chance of developing diabetes among overweighed people was almost double. However, the individuals engaged in physical work had less chance to have DM. This study calls for greater attention of government and other concerned entities to come up with appropriate policy interventions to lower the risk of DM.
Similar content being viewed by others
Introduction
The epidemic of the century-Diabetes Mellitus (DM), often referred as simply diabetes, is a set of metabolic disorder or syndrome recognized as chronic hyperglycemia (presence of high blood sugar) occurs due to imperfections in insulin action, insulin secretion, or both1,2. It is now prevalent across the world with multiple complications3,4,5. In 2014, around 422 million people were affected by DM and 1.5 million deaths were reported in 20126,7. According to WHO report, 2016, 8% (12.88 million) of total population of Bangladesh was affected by diabetes whereas 3% of total deaths of all-ages occurred due to diabetes8. An increasing rate in the prevalence of DM among the Bangladeshi populace is also observed over time9.
Diabetes may result in a wide range of physiological as well as psychological problems including sexual disorder10. The lower sexual functions or dysfunctions termed as loss of libido may be observed in both females and males as a consequence of DM11,12,13,14,15,16,17,18. In addition, severe vision loss, acute renal diseases which may require dialysis or kidney transplant, myocardial infarction otherwise known as heart attack, cerebrovascular diseases like stroke, and hypertension are markedly observed19,20,21,22,23,24,25,26,27. Due to the intensity of the adverse effects of diabetes, it is important to find out the determinants to address the issue in order to contribute to improving country health situation.
Diabetes mellitus (DM) is a disease that relies on many factors and may vary over time and region. Accordingly, it requires to be screened on a constant basis. Previously, many studies explored the risk factors of DM by utilizing several statistical models. Among these models, a single level logistic model was very popular. However, the single level model depends on some strict assumptions which may not be possible to follow all the time, specifically, when someone is dealing with a dataset having hierarchical formation. Alternatively, one can apply a two-level regression model. Thus, our study intends to explore the prevalence of DM and its possible risk factors in Bangladesh by applying a two-level regression model since the necessary information was obtained from Bangladesh Demographic and Health Survey (BDHS) 2011 that follows a hierarchical structure.
Materials and Methods
Data Collection
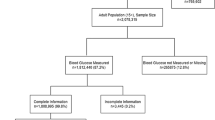
This study utilized the BDHS 2011 dataset, which was collected by the National Institute of Population Research and Training (NIPORT) with the collaboration of Mitra and Associates (Bangladesh) and ICF international (USA)28. In this survey, a total of 83,731 household members were taken from 17,141 households by applying a two-stage stratified cluster sampling28. Although BDHS 2014 data are available, the necessary information for conducting this study such as fasting plasma glucose (FPG) is not available in BDHS 2014 and is very much accessible in BDHS 2011 survey. In 2011 survey, there were 3734 men and 3831 women aged from 35 years and above who participated in FPG measurement28.
Dependent variable
For measuring fasting plasma glucose (FPG), the BDHS 2011 utilizes the cut-off points recommended by WHO29. If FPG ranges from 3.9 mmol/l (70 mg/dl) to 6.0 mmol/l (108 mg/dl), it was said to be normal29. The FPG value within the range between 6.1 to 6.9 mmol/l (110–124 mg/dl) was considered as pre-diabetic, and the FPG greater than or equal to 7.0 mmol/l (126 mg/dl) was said to be diabetic29. In this study, a participant was identified as a diabetic patient if his/her FPG value was greater than 6.1 mmol/l (110 mg/dl)30.
Independent variables
A set of categorical explanatory variables was selected to fit the two level regression model. The selected variables were divided into two parts: level-1 variables and level-2 variables. At the level-1, we considered: sex (male, female), level of education (no education, primary education, secondary education, above secondary education), wealth index (poor, middle, rich), BMI (body mass index) [thin, if BMI is less than 18.5, normal, if BMI ranges from 18.5 to 24.9, overweight, if BMI is greater than 24.9] and working status (desk-work, physical work). The working status was used as a proxy variable for measuring physical activity31. Respondents were considered to be engaged in physical activities if his/her work liability includes physical activity related works31. This group includes agricultural worker, farmer, fisherman, cattle raising, poultry raising, rickshaw driver, road building, brick breaking, construction worker, domestic servant, boatman, beggar and factory worker31. The physically inactive group consists of land owner, unemployed/student, carpenter, tailor, doctor, nurse, dentist, lawyer, accountant, teacher, family welfare visitor, businessman, housewife, religious leader and retired person31. The level-2 variable includes region of residence which was classified as urban and rural.
Statistical analysis
The relationship between chosen covariates and DM was analyzed by performing both bivariate and multivariate investigations. In the bivariate arrangement, chi-square test was utilized to identify the relationship between response and explanatory variables. Weighted prevalence of diabetes among Bangladeshi people was also calculated. In the multivariate arrangement, we applied a two-level logistic regression model to examine the risk factors of DM by reducing the regional effect that exists in the dataset. However, intra-class correlation coefficient (ICC) should be calculated prior to the application of any two-level model32. The mathematical form to calculate the ICC is
Where, \(\,var({V}_{0j})\) represents the variance of random intercept (variance of level-2). The range of ICC varies from 0 to 1. A two-level regression model is applicable, if the ICC is greater than 033.
The term \(var({V}_{0j})\) should be calculated from two-level empty model. The functional form of the two-level empty model is-
in which \(logit\,({\pi }_{ij})=P({Y}_{ij}=1)\), \({\alpha }_{0}\) represents the intercept of fixed effect and \({V}_{0j}\) represents the level-2 residual33. Finally, the mathematical form of the two-level random intercept model is-
where \({x}_{ij}\,\)and Xj represent the level-1 and level-2, respectively, whereas β10 and β01 represent the fixed effects of the level-1 and level-2 variable, respectively33.
Ethical Approval
This study depends on secondary dataset collected by NIPORT (Bangladesh) and MEASURE DHS. Every legitimate strategy was performed including human participants as per the moral norms of the national research committee and with the 1964 Helsinki Declaration and its later amendments or comparable ethical standards28. The information records are unreservedly accessible from the website: www.dhsprogram.com. We got approval from the DHS program for utilizing the applicable datasets for this investigation. Ethical clearance for the BDHS 2011 data collection was taken from the ICF International’s IRB (Institutional Review Board)28. This survey confirmed international ethical standards of anonymity, confidentiality, and informed consent28. A letter of data authorization was taken from the Demographic and Health Surveys (DHS) Program, ICF International. The authority of Statistics Discipline in Khulna University, Bangladesh additionally gave us the chance to direct the examination.
Informed consent
Informed consent has been taken from all participants associated with this research.
Results
The background characteristics of study participants by diabetes status and weighted prevalence of diabetes mellitus with 95% confidence interval were displayed in Table 1. It was observed that the prevalence of diabetes increases with increasing age of the participants. The prevalence was almost equal among female (32.4%) and male (32.5%). Considering the education level, the higher rate of DM was observed among higher educated participants. Subsequently, the rich group had highest prevalence of diabetes (36.7%) than their counterparts. Prevalence of diabetes was higher in urban area (35.9%) than the rural area (30.8%). In our study, the prevalence rate of DM was higher among thin (31.6%), overweighed (48.2%), participants having hypertension (23.2%) and not engaged in physical work (32.8%). Except the sex of the participants, all the selected covariates were found to be statistically significant (p < 0.05).
In multivariate analysis, at first, we estimated a two-level empty model to obtain the value of intra-class correlation (ICC) within the divisions. The Table 2 is showing the value of ICC which is 0.019, suggesting that the two-level regression model can be applied to identify the risk factors for diabetes mellitus. The estimates of two-level model were displayed in Table 3. From this table, it was identified that the intercept of random part was statistically significant (p < 0.001), representing that the DM varies among divisions of Bangladesh. From fixed effects, we observed that the chance of having diabetes increases with increasing age of the participant (OR = 1.919, p < 0.01). It was also interesting to find that females were more likely to have diabetes (OR = 1.468, p < 0.001) than males. The occurrence of diabetes was 62% higher for higher educated participants (OR = 1.617, p < 0.001). Compared to the participants from middle income family, the odds of developing diabetes was 42% higher for the individuals who came from the rich family (OR = 1.420, p < 0.01). It was also found that the chance of developing diabetes among overweighed individuals was almost double (OR = 2.121, p < 0.001) than normal weighted people. Moreover, the chance of developing diabetes was higher among persons with hypertension (OR = 1.629, p < 0.001). However, the individuals engaged in physical work had less chance (OR = 0.972, p < 0.05) to develop diabetes compared to their counterpart.
Discussion
In our study, we observed that the prevalence of DM was more among old age group. Different studies also found that the probability of diabetes was higher with increased age34,35,36,37,38,39,40. This may occur due to deficiency in insulin secretion following weaker pancreatic function of old people41. In addition, the demand of insulin may increase in the human body in certain context or improper utilization of insulin by the body among aged people42,43. The suggestive actions for older adults were maintaining blood pressure, blood sugar through improving lifestyle44,45,46,47,48,49,50,51.
Relation between gender and prevalence of diabetes mellitus showed a mixed result and geographical location has been found as a key determinant. Though we found almost same prevalence of diabetes in both sex, Gale and Gillespi (2001) found that females with non-European origin and males from European origin were more prone to have diabetes52. Hilawe et al. (2013) mentioned that the prevalence of DM was relatively higher in men from Middle or Eastern Africa whereas in women from Southern Africa or among respondents from Indian ethnicity53. Aregbesola et al. (2017) found a higher prevalence of diabetes risk in males54. Another study found that the risk of developing diabetes was higher among Caribbean women55. A study from China also found a higher prevalence of DM among older women compared with men56. In US context, the prevalence of DM was relatively lower among women compared to men between 2013–201657.
Lower educational attainment puts both male and female at a high risk of developing diabetes58,59,60. An inverse association between educational attainment and development of diabetes was observed in different studies61,62,63. A study revealed that low educational level was significantly related to poor glycaemic control for people having Type 2 DM in Bangladesh64. Other studies also demonstrated that higher educational level was independently related to better diabetes knowledge and having optimal glycaemic control through attending diabetes education65,66,67. However, Ali et al. (2019) found a somewhat reverse causality that hypertension, diabetes and comorbidity were higher among higher educated individuals68. Our study also showed similar result.
Prevalence of diabetes was higher amongst higher socio-economic status groups69,70,71,72. Thus, higher wealth is an independent risk factor for diabetes73. The poor socioeconomic status leaves one with a higher risk of remaining undiagnosed for diabetes74. Conversely, the richest have higher probability of being diagnosed with diabetes75. Our study also showed higher risk of developing DM among rich income group that supports other findings as they usually are less involved in physical work in Bangladesh.
DM is usually a hereditary disease. In addition, there are many causal and confounding factors that contributed to develop DM such as obesity. Obesity may result in diabetes which is well documented in different studies76,77,78. Hypertension is common among patients with diabetes and DM helps facilitating hypertension79,80,81,82. Diabetes and high blood pressure complement each other due to the fact that they both contain common physiological traits83. Diabetic patients experience increased peripheral artery resistance causing elevated systemic blood pressure.
Epidemic of diabetes is associated with decreasing levels of physical activity and an increasing prevalence of obesity. Priority should be given to promote physical activity in this regard84,85,86. Physical activity reduces the risk of diabetes which is evident in different studies87,88,89. Moderate to high level of physical activity is associated with substantially lower morbidity and mortality in people with diabetes90. Physical activity can reduce the risk of diabetes complications91. It is important for diabetes management as well92. Regular physical activity (PA) is recommended for diabetic patients93. If needed, counseling on PA by physicians should be considered in this regard94.
Conclusion
Diabetes has become a major public concern across the world due to its pandemic nature. Bangladesh is not an exception. This study attempted to identify the socio-demographic determinants that condition the prevalence of diabetes mellitus among individuals in Bangladesh. It was observed that age, gender, educational attainment, possession of wealth, obesity, hypertension and level of physical activity were some significant predictors of the prevalence of diabetes mellitus among Bangladeshi adults. This study calls for greater attention of government and other concerned entities to come up with appropriate policy interventions to lower the prevalence of diabetes and associated risks.
Data availability
The secondary datasets BDHS 2011 are freely available in the following website: http://dhsprogram.com/data/available-datasets.cfm.
References
Kharroubi, A. T. & Darwish, H. M. Diabetes mellitus: The epidemic of the century. World J Diabetes. 6(6), 850–867 (2015).
American Diabetes Association. Diagnosis and classification of diabetes mellitus. Diabetes Care. 33(Suppl. 1), S62–S69 (2010).
Papatheodorou, K. et al. Complications of diabetes 2017. J. Diabetes Res. 3086167 (2018).
Rask-Madsen, C. & King, G. L. Vascular complications of diabetes: mechanisms of injury and protective factors. Cell Metab. 17(1), 20–33 (2013).
Wong, N.K.P. et al. The role of high-density lipoproteins in diabetes and its vascular complications. Int J Mol Sci. 19(6), https://doi.org/10.3390/ijms19061680 (2018).
World Health Organization. Global report on diabetes. France: WHO, https://apps.who.int/iris/handle/10665/204871 (2016).
Zhou, B. et al. Worldwide trends in diabetes since 1980: a pooled analysis of 751 population-based studies with 4.4 million participants. Lancet. 387(10027), 1513–1530, https://doi.org/10.1016/S0140-6736(16)00618-8 (2016).
World Health Organization. Diabetes country profiles, 2016: Bangladesh. France: WHO (2016).
Akter, S. et al. Prevalence of diabetes and prediabetes and their risk factors among Bangladeshi adults: a nationwide survey. Bull World Health Org. 92, 204–213A (2014).
Bak, E. et al. Does Type 1 Diabetes Modify Sexuality and Mood of Women and Men? Int. J. Environ. Res. Public Health. 15(5), 958 (2018).
Afshari, P. et al. The Relation of Diabetes Type 2 with Sexual Function among Reproductive Age Women in Iran, a Case-Control Study. Adv Med. 4838923 (2017).
Bal, M. D. et al. Does the diabetes of type 2 affect the sexual functions of women? J Sex Marital Ther. 41, 107–13 (2015).
Rehman, K., Beshay, E. & Carrier, S. Diabetes and male sexual function. J Sex Reprod Med. 1, 29–33 (2001).
Gupta, L. et al. Diabetes and Female Sexual Dysfunction. US Endocrinol. 14(1), 35–38 (2018).
Malavige, L. S. & Levy, J. C. Erectile dysfunction in diabetes mellitus. J Sex Med. 6, 1232–1247 (2009).
Isidro, M. L. Sexual dysfunction in men with type 2 diabetes. Postgrad Med J. 88, 152–159 (2012).
Owiredu, W. K. B. A. et al. Sexual dysfunction among diabetics and its impact on the SQoL of their partners. Int J Impot Res. 29(6), 250–257 (2017).
Paningbatan, J. et al. Prevalence of Sexual Dysfunction and its Associated Factors among Women with Diabetes Mellitus Type 2 at Makati Medical Center Outpatient Department. ASEAN Federation of Endocrine Societies. 33(2), 165–173 (2018).
King, K. D., Jones, J. D. & Warthen, J. Microvascular and macrovascular complications of diabetes mellitus. Am J pharm edu. 69(5), 87 (2005).
Fowler, M. J. Microvascular and macrovascular complications of diabetes. Clin Diabetes. 29(3), 116–122 (2011).
Nickerson, H. D. & Dutta, S. Diabetic complications: current challenges and opportunities. J Car Trans Res. 5(4), 375–379 (2012).
Forbes, J., M. & Cooper, M. E. Mechanisms of diabetic complications. Phys Rev. 93(1), 137–188 (2013).
Robert, A. & Al Dawish, M. A. Microvascular complications among patients with diabetes: An emerging health problem in Saudi Arabia. Diab Vasc Dis Res. 16(3), 227–235 (2019).
Stolar, M. Glycemic control and complications in type 2 diabetes mellitus. Am J Med. 123(3), S3–S11 (2010).
Hewston, P. et al. Fear of falling in older adults with diabetes mellitus: the IMIAS Study. Can J Aging. 37(3), 261–269 (2018).
Chia, C. W., Egan, J. M. & Ferrucci, L. Age-related changes in glucose metabolism, hyperglycemia, and cardiovascular risk. Circ Res. 123(7), 886–904 (2018).
Rahman, M. et al. Prevalence, treatment patterns, and risk factors of hypertension and pre-hypertension among Bangladeshi adults. J Hum Hypertens. 32(5), 334–348 (2018).
National Institute of Population Research and Training (NIPORT), Mitra and Associates, and ICF International. Bangladesh Demographic and Health Survey 2011. Dhaka, Bangladesh and Calverton, Maryland, USA: NIPORT, Mitra and Associates, and ICF International, Available on: https://dhsprogram.com/pubs/pdf/fr265/fr265.pdf (2013).
World Health Organization. Definition and Diagnosis of Diabetes Mellitus and Intermediate Hyperglycemia: Report of a WHO/IDF Consultation. Geneva: WHO. (2006).
Hoque, M. E., Khokan, M. R. & Bari, W. Impact of stature on non-communicable diseases: evidence based on Bangladesh Demographic and Health Survey, 2011 data. BMC Public Health. 14, 1007 (2014).
Talukder, A., Akter, N. & Mallick, T. S. Exploring Association between Individuals’ Stature and Type 2 Diabetes Status: Propensity Score Analysis. Environ Health Insights. 13, 1178630219836975 (2019).
Talukder, A. Risk factors associated with wasting among under-5 children residing in urban areas of Bangladesh: a multilevel modelling approach. J Public Health (Berl.), https://doi.org/10.1007/s10389-019-01163-4 (2019).
Park, S. & Lake, E. T. Multilevel modeling of a clustered continuous outcome: nurses’ work hours and burnout. Nurs Res. 54, 406–13 (2005).
Kalyani, R. R., Golden, S. H. & Cefalu, W. T. Diabetes and aging: unique considerations and goals of care. Diabetes Care. 40(4), 440–443 (2017).
Kirkman, M. S. et al. Diabetes in older adults. Diabetes care. 35(12), 2650–2664 (2012).
Selvin, E. & Parrinello, C. M. Age-related differences in glycaemic control in diabetes. Diabetologia. 56(12), 2549–2551 (2013).
Chentli, F., Azzoug, S. & Mahgoun, S. Diabetes mellitus in elderly. Indian J Endocr Metab. 19, 744–52 (2015).
Suastika, K. et al. Age is an Important Risk Factor for Type 2 Diabetes Mellitus and Cardiovascular Diseases. In: Chackrewarthy, S. (ed.) Glucose Tolerance. London, UK, Intech Open, https://doi.org/10.5772/52397 (2012).
Ekoe, J. M., Goldenberg, R. & Katz, P. Screening for diabetes in adults. Can J Diabetes. 42, S16–S19 (2018).
Wang, S. et al. Association between obesity indices and type 2 diabetes mellitus among middle-aged and elderly people in Jinan, China: a cross-sectional study. BMJ Open. 6, e012742 (2016).
Mordarska, K. & Godziejewska-Zawada, M. Diabetes in the elderly. Prz Menopauzalny. 16(2), 38–43 (2017).
Bell, K. J., Toschi, E., Steil, G. M. & Wolpert, H. A. Optimized mealtime insulin dosing for fat and protein in type 1 diabetes: application of a model-based approach to derive insulin doses for open-loop diabetes management. Diabetes Care. 39(9), 1631–1634 (2016).
Ober, S. K., Watts, S. & Lawrence, R. H. Insulin use in elderly diabetic patients. Clin Interv Aging. 1(2), 107–113 (2006).
LeRoith, D. et al. Treatment of diabetes in older adults: an endocrine society clinical practice guideline. J Clin Endocrinol Metab. 104(5), 1520–1574 (2019).
Kalra, S. & Sharma, S. K. Diabetes in the Elderly. Diabetes Therapy. 9(2), 493–500 (2018).
Chen, W. C. et al. Blood glucose Management of Type 2 diabetes in the older people. Int. J Gerontol. 12(3), 170–174 (2018).
Bigelow, A. & Freeland, B. Type 2 Diabetes Care in the Elderly. J Nur Practition. 13(3), 181–186 (2017).
Sinclair, A., Dunning, T. & Rodriguez-Manas, L. Diabetes in older people: new insights and remaining challenges. Lancet Diabetes Endocrinol. 3(4), 275–285 (2015).
Longo, M. et al. Diabetes and aging: from treatment goals to pharmacologic therapy. Front Endocrinol. 10, 45 (2019).
Jeffrey, F. Management of hypoglycemia in older adults with type 2 diabetes. J Postgrad Med. 131(4), 241–250 (2019).
Ruedy, K. J. et al. Continuous glucose monitoring in older adults with type 1 and type 2 diabetes using multiple daily injections of insulin: results from the DIAMOND trial. J Diabetes Sci Technol. 11(6), 1138–1146 (2017).
Gale, E. A. & Gillespie, K. M. Diabetes and gender. Diabetologia. 44(1), 3–15 (2001).
Hilawe, E. H. et al. Differences by sex in the prevalence of diabetes mellitus, impaired fasting glycaemia and impaired glucose tolerance in sub-Saharan Africa: a systematic review and meta-analysis. Bull World Health Org. 91, 671–682D (2013).
Aregbesola, A. et al. Gender difference in type 2 diabetes and the role of body iron stores. Ann Clin Biochem. 54(1), 113–120 (2017).
Sobers-Grannum, N. et al. Female Gender Is a Social Determinant of Diabetes in the Caribbean: A Systematic Review and MetaAnalysis. PLoS ONE. 10(5), e0126799 (2015).
Li, J. et al. Sex Differences in the Prevalence, Awareness, Treatment, and Control of Diabetes Mellitus Among Adults Aged 45 Years and Older in Rural Areas of Northern China: A Cross-Sectional, Population-Based Study. Front. Endocrinol. 10, 147 (2019).
Peters, S. A. & Muntner, P. Woodward M. Sex differences in the prevalence of, and trends in, cardiovascular risk factors, treatment, and control in the United States, 2001 to 2016. Circulation. 139(8), 1025–1035 (2019).
Sacerdote, C. et al. Lower educational level is a predictor of incident type 2 diabetes in European countries: the EPIC-Inter Act study. Int J Epidemiol. 41(4), 1162–1173 (2012).
Bellou, V. et al. Risk factors for type 2 diabetes mellitus: An exposure-wide umbrella review of metaanalyses. PLoS ONE. 13(3), e0194127 (2018).
Borrell, L. N., Dallo, F. J. & White, K. Education and diabetes in a racially and ethnically diverse population. Am J Public Health. 96(9), 1637–1642 (2006).
Shang, X. et al. Educational Level, Obesity and Incidence of Diabetes among Chinese Adult Men and Women Aged 18–59 Years Old: An 11-Year Follow-Up Study. PLoS ONE. 8(6), e66479 (2013).
Al-Zahrani, J.M. et al. Prevalence of Prediabetes, Diabetes and Its Predictors among Females in Alkharj, Saudi Arabia: A Cross-Sectional Study. Ann Glob Health. 85(1), 109, 1–13 (2019).
Whitaker, S. M. et al. The association between educational attainment and diabetes among men in the United States. Am J Mens Health. 8(4), 349–356 (2014).
Afroz, A. et al. Glycaemic Control for People with Type 2 Diabetes Mellitus in Bangladesh-An urgent need for optimization of management plan. Sci Rep. 9(1), 1–10 (2019).
Poulimeneas, D. et al. Diabetes knowledge among Greek type 2 diabetes mellitus patients. Endocrinol Nut. 63(7), 320–326 (2016).
Fenwick, E. K. et al. Factors Associated with Knowledge of Diabetes in Patients with Type 2 Diabetes Using the Diabetes Knowledge Test Validated with Rasch Analysis. PLoS ONE. 8(12), e80593 (2013).
Kim, S. H. Educational attainment moderates the associations of diabetes education with health outcomes. Int J Nurs Pract. 22(5), 444–450 (2016).
Ali, N. et al. Sex-specific prevalence, inequality and associated predictors of hypertension, diabetes, and comorbidity among Bangladeshi adults: results from a nationwide cross-sectional demographic and health survey. BMJ Open. 9, e029364 (2019).
Mutyambizi, C. et al. Lifestyle and socioeconomic inequalities in diabetes prevalence in South Africa: A decomposition analysis. PLoS ONE. 14(1), e0211208 (2019).
Corsi, D. J. & Subramanian, S. V. Socioeconomic gradients and distribution of diabetes, hypertension, and obesity in India. JAMA Netw Open. 2(4), e190411 (2019).
Saquib, N. et al. High prevalence of type 2 diabetes among the urban middle class in Bangladesh. BMC public health. 13(1), 1032 (2013).
Adekanmbi, V. T. et al. Epidemiology of prediabetes and diabetes in Namibia, Africa: A multilevel analysis. J Diabetes. 11(2), 161–172 (2019).
Khan, M. M. H., Gruebner, O. & Kraemer, A. The Geography of Diabetes among the General Adults Aged 35 Years and Older in Bangladesh: Recent Evidence from a Cross-Sectional Survey. PLoS ONE. 9(10), e110756 (2014).
Hasan, M. et al. Socioeconomic Inequalities of Undiagnosed Diabetes in a Resource-Poor Setting: Insights from the Cross-Sectional Bangladesh Demographic and Health Survey 2011. Int J Environ Res Public Health. 16(1), 115 (2019).
Barik, A. et al. Physiological and behavioral risk factors of type 2 diabetes mellitus in rural India. BMJ Open Diabetes Res Care. 4, e000255 (2016).
Al-Goblan, A. S., Al-Alfi, M. A. & Khan, M. Z. Mechanism linking diabetes mellitus and obesity. Diabetes Metab Syndr Obes. 7, 587 (2014).
Eckel, R. H. et al. Obesity and type 2 diabetes: what can be unified and what needs to be individualized? J Clin Endocrinol Metab 96(6), 1654–1663 (2011).
Conway, B. N. et al. The obesity epidemic and rising diabetes incidence in a low income racially diverse southern US cohort. PLoS ONE. 13(1), e0190993 (2018).
Song, J. et al. Management of hypertension and diabetes mellitus by cardiovascular and endocrine physicians: a China registry. J Hypertens. 34(8), 1648 (2016).
Petrie, J. R., Guzik, T. J. & Touyz, R. M. Diabetes, hypertension, and cardiovascular disease: clinical insights and vascular mechanisms. Can J Cardiol. 34(5), 575–584 (2018).
Ferrannini, E. & Cushman, W. C. Diabetes and hypertension: the bad companions. The Lancet 380(9841), 601–610 (2012).
Cryer, M. J., Horani, T. & Di Pette, D. J. Diabetes and hypertension: a comparative review of current guidelines. J Clin Hypertens. 18(2), 95–100 (2016).
Anwer, Z. et al. Hypertension management in diabetic patients. Eur Rev Med Pharmacol Sci. 15(11), 1256–1263 (2011).
Kennerly, A. M. & Kirk, A. Physical activity and sedentary behaviour of adults with type 2 diabetes: a systematic review. Prac Diabetes. 35(3), 86–89 (2018).
Wilmot, E. G. et al. Sedentary time in adults and the association with diabetes, cardiovascular disease and death: systematic review and meta-analysis. Diabetologia. 55, 2895–2905 (2012).
Fagour, C. et al. Low physical activity in patients with type 2 diabetes: the role of obesity. Diabetes Metab J. 39(1), 85–87 (2013).
Duclos, M. et al. Physical activity and type 2 diabetes. Recommendations of the SFD (Francophone Diabetes Society) diabetes and physical activity working group. Diabetes Metab J. 39(3), 205–216 (2013).
Brugnara, L. et al. Low Physical Activity and Its Association with Diabetes and Other Cardiovascular Risk Factors: A Nationwide, Population-Based Study. PLoS ONE. 11(8), e0160959 (2016).
Walsh, E. I. et al. Physical Activity and Blood Glucose Effects on Weight Gain Over 12 Years in Middle-Aged Adults. J Obes Chronic Dis. 2(1), 20–25 (2018).
Sigal, R. J. et al. Physical activity and diabetes. Can J Diabetes. 42, S54–S63 (2018).
Miller, Y. D. & Dunstan, D. W. The effectiveness of physical activity interventions for the treatment of overweight and obesity and type 2. diabetes. J Sci Med in Sport 7(1), 52–59 (2004).
Hayes, C. & Kriska, A. Role of physical activity in diabetes management and prevention. J Am Diet Assoc. 108(4), S19–S23 (2008).
Herbst, A. et al. Effects of regular physical activity on control of glycemia in pediatric patients with type 1 diabetes mellitus. Arch Pediatr Adolesc Med. 160(6), 573–577 (2006).
Pati, S. et al. Type 2 diabetes and physical activity: barriers and enablers to diabetes control in Eastern India. Prim Health Care Res Dev. 20(e44), 1–6 (2019).
Acknowledgements
We would like to thank the National Institute of Population Research and Training NIPORT, Bangladesh and MEASURE DHS for allowing us to use BDHS, 2011 data for our analysis. No fund has been received.
Author information
Authors and Affiliations
Contributions
A.T. had the original idea for the study. A.T. and M.Z.H. participated in the statistical analysis and helped to draft the manuscript. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made. The images or other third party material in this article are included in the article’s Creative Commons license, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons license and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this license, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Talukder, A., Hossain, M.Z. Prevalence of Diabetes Mellitus and Its Associated Factors in Bangladesh: Application of Two-level Logistic Regression Model. Sci Rep 10, 10237 (2020). https://doi.org/10.1038/s41598-020-66084-9
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41598-020-66084-9
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.