Abstract
This study assesses the agreement between intraocular pressure (IOP) measurements taken with the Goldmann applanation tonometer (GAT) and a new experimental applanation tonometer with a convexly shaped apex (CT) after laser myopic refractive surgery. Two different CT radii (CT1 and CT2) were designed with a finite element analyser, and a prospective double masked study on 102 eyes from 102 patients was carried out. A Bland-Altman plot and intra-class correlation coefficient (ICC) were calculated to assess the agreement between GAT measurements and the measurements of both CT1 and CT2 before and after myopic laser assisted in situ keratomileusis (LASIK; n = 73) and photorefractive keratectomy (PRK; n = 29). We evaluated a subset of two subgroups (n = 36 each) for intra and inter-observer (IA/IE) error. From the whole cohort, the best IOP agreement was observed between GATpre and CT1post surgery: 16.09 ± 2.92 vs 16.42 ± 2.87 (p < 0.001); ICC = 0.675 (95% CI: 0.554–0.768). In the analysis of LASIK vs PRK, GATpre and CT1post showed the highest agreement, although LASIK measurements were more accurate than PRK, as the ICC = 0.718 (95% CI: 0.594–0.812) and ICC = 0.578 (95% CI: 0.182–0.795) respectively. Excellent agreement was observed for IA/IE, and there was an ICC > 0.8 (95% CI) in all cases. CT1 proved more accurate in the LASIK subgroup. In conclusion, our new version of GAT could be used with post-surgery LASIK patients as a more accurate measurement device compared to the current reference tonometer.
Similar content being viewed by others
Introduction
The Goldmann applanation tonometer (GAT; Haag-Streit, Switzerland) is the current reference tonometer for measuring intraocular pressure (IOP) in daily clinical practice due to its acceptably accurate measurements, reproducibility and reliability1,2,3,4. However, GAT readings are influenced by corneal central thickness (CCT) and corneal biomechanics (CB), which vary widely among normal individuals1,5,6. In myopic laser refractive surgery (LRS) patients, variations induced in both CCT and CB lead to differences in GAT readings. This change in IOP has been inconsistent in previous studies regardless of the type of surgery: Mardelli et al.7 found a significant reduction of 1 ± 2.8 mmHg in IOP measurements after ablating 23 μm in photorefractive keratectomy (PRK) patients; while Duch et al.8 found an underestimation of about 2.9 mmHg per 70 μm ablation in CCT after laser assisted in situ keratomileusis (LASIK). These IOP underestimations affect the reliability of GAT as gold standard after LASIK and PRK procedures9,10,11.
LASIK is one of the most frequent types of eye surgery and a total of 40 million people had this operation worldwide between 1991 and 201612. Moreover, the prevalence of glaucoma is 2 to 4 times higher among the myopic population13. Thus, it is very important to obtain an accurate and real estimation of IOP in order not to miss ocular hypertension after myopic LRS.
The aim of our study is to describe a new modified GAT as well as its translational application and clinical outcomes by evaluating IOP measurements before and after myopic LRS. We also evaluate the reliability of the intra and inter-observer agreement.
Methods
New device description
How corneal tissue will react in real life to external elements can be estimated with finite element analysis (FEA). Three-dimensional (3D) modelling is more accurate than two-dimensional (2D) modelling for predicting what could occur to tissue in vivo14. In our study, we used 2D (Fig. 1) and 3D (Fig. S1, supplementary data) FEA to simulate the biomechanical responses of a normal cornea and a laser operated cornea (OC) to the contact of two external forces: a plane surface (corresponding to GAT) and a convex surface (corresponding to the new CT device). Various simulations were carried out with different corneal thicknesses and elastic behaviours of the cornea (Figs. S2–S4).
FEA simulation of corneal antero-posterior displacement in response to GAT (A,B) and CT (C) contact. The graphics below correspond to force applied from the centre to the periphery of the cornea within the anterior tonometer contact surface, and the colour scale indicates the maximum corneal deformation (MCD = N/m2). A corresponds to CC. B and C correspond to OC with a 100 μm ablation of CCT. A similar arc length and a wider contact pressure profile graphic are observed when GAT contact is compared with normal corneas (A), and CT contact is compared with operated corneas (C). However, when GAT is used on an OC (B), a confluence of forces is observed at the same point (asterisk, *) from the beginning, and the arc length contact is narrower. Young’s Modulus (Y) = 0.5 MPa. CC, calibrated cornea. OC, operated cornea.
Two different individual corneas were designed. First, a regular or “calibration cornea” (CC), as described in the Orssengo-Pye algorithm6, with CCT = 520 μm, an anterior corneal curvature of 7.8 mm, and assuming radial symmetry for a cornea-GAT contact of 3.06 mm (Fig. 1A). The second FEA consisted in a “LRS OC”, whose CCT and anterior radial symmetry could be ablated as in LRS up to 420 µm and 8.43 mm for different simulations (Figs. 1B,C and 2).
In all cases, a nonlinearity material model with Mooney-Rivlin parameters15 was applied, and every simulation was calculated with Young’s Modulus (Y) = 0.5 MPa. Inverse modelling was performed to account for the IOP: a step-wise computing initial stress state of the cornea was determined by assuming IOP = 15 mmHg16.
Due to pachymetric and elastic corneal variability in our population, we considered different radii for the CT devices (radii varying from 11.5 to 14 mm) to compare contact pressure profiles (CPP) with different corneas, until a similar corneal modelling behaviour was observed between GAT and CT (Fig. 1A,C).
Finally, two different tonometers with different radii (r) (Fig. 3) were created and called CT1 (r = 13 mm) and CT2 (r = 12 mm). These were used in our clinical study to assess which tonometer correlated better with GAT measurements before LRS.
Study design
A prospective double-masked comparative study was carried out on a sample of 102 myopic subjects who were going in for LSR (LASIK or PRK) at the Barraquer Ophthalmology Center in Barcelona. These subjects first underwent a general medical history review, and a detailed eye examination. After meeting the inclusion criteria and having none of the exclusion criteria, the subjects were included and their informed consent was obtained for study participation. The study protocol is in accordance with the Declaration of Helsinki and the Institutional Ethics Committee of the Barraquer Ophthalmology Center approved this study.
Subjects
The right eye of each subject was randomly selected adding up to a total of 102 eyes. The inclusion criteria were: myopic patients aged above 18 years with a stable myopic refractive error less than spherical −9 diopters (dpts), and less than myopic astigmatism −4 dpts. Subjects who had previously been diagnosed with an ocular pathology before ocular surgery or treated with medications that could affect IOP levels were excluded from the study.
Exploration protocol
All patients underwent a standardized examination that included measuring visual acuity (spherical equivalent refraction; SER), slit-lamp anterior biomicroscopy, posterior segment ophthalmoscopy and IOP measurements. Age, gender and refractive error were also recorded.
Before IOP measurements were recorded, the corneal topography was determined with a Pentacam (Oculus, Wetzlar, Germany) to obtain anterior simulated keratometry and posterior corneal curvature (simK, PCC respectively), corneal volume (VOL) and CCT. In addition, the corneal hysteresis (CH) and corneal resistance factor (CRF) were obtained by Ocular Response Analyser (ORA; Reichert Ophthalmic instruments, New York). The maximum ablation depth (Max.Abl) and percentage of ablated tissue (PTA) were also analysed. Postoperative treatment included ofloxacin 0.3% and fluorometholone (FML) 0.1% 4 times a day for 1 week in both groups, and an additional 3 weeks of FML in the PRK group.
IOP was measured before and three months after surgery. Each measurement was carried out by the main observer (MI) using 3 different devices (GAT, CT1, CT2 pre- and post- surgery, used in the same order, respectively) and leaving 2 minutes between taking measurements with each tonometer17. The IOP measurements were taken between 10:00 and 13:00 hours (10 am and 1 pm), similarly to the 3rd month after surgery readings, which were performed at approximately the same time as the pre-operation readings18,19.
In order to assess intra-observer (IA) error, a subset of 36 patients were randomly double-masked measured by the main observer MI in the presence of a second observer (AL). To assess the inter-observer (IE) error, a different subset of 36 patients were also evaluated randomly by the main observer MI and by a second observer AL. In these cases, IOP measurements were carried out consecutively, were double-masked and after an interval of 5 minutes. In all cases, a third observer (BK) was present to ensure the double-masking.
Statistical analysis
The statistical analysis was performed using SPSS® (Statistical Package for Social Sciences, v22.0; SPSS Inc., Chicago, IL, USA). A significance level of 5% was considered in all the analyses. All quantitative variables were tested for normality with the Kolmogorov-Smirnov or the Shapiro-Wilk tests. We conducted descriptive analyses for all the variables preoperatively and 3 months after surgery. The descriptive values are presented as mean ± standard deviation unless stated otherwise.
Pre- and post-surgery values were compared considering all the cases using the paired t-test or the Wilcoxon test depending on data normality. In addition, we compared the eye characteristics of patients undergoing surgery with LASIK. PRK was performed using the independent t-test or the Mann-Whitney test depending on data normality.
To evaluate the relationship between IOP and the corneal characteristics, IOP values obtained with GAT, CT1 and CT2 in pre- and post-surgery were correlated respectively with clinical characteristics of pre- and post-surgery eyes using the Pearson or Spearman’s correlation coefficients depending on data normality.
We considered GATpre as the current reference for evaluating the concordance between IOP measures taken with the different tonometers. Different approaches were used to evaluate the differences between GATpre IOP and IOP determined with GAT, CT1 and CT2post respectively. In short, 1) the mean differences between GATpre measurements and the measurements taken with all the devices in post-surgery were calculated and the absence of differences was tested with the Wilcoxon test; 2) the Bland-Altman analysis was used to compare the agreement of measurements taken with the different tonometers; and 3) the ICC was calculated based on absolute-agreement. Values lower than 0.5, between 0.5 and 0.8, and greater than 0.8 were indicative of poor or weak, good, and excellent reliability, respectively20. To determine which factors explain the bias trend in the Bland-Altman analysis, multiple stepwise regression was used to relate the differences in IOP and the change in corneal characteristics from pre- to post-surgery.
To analyse IA/IE, we calculated the mean difference between measurements and tested the absence of differences with the Wilcoxon or paired sample t-test. The Bland-Altman analysis was used, and the ICC was calculated based on absolute-agreement.
Results
FEA simulation results
CPP comparisons can be helpful for understanding how corneal tissue will react to contact with different tonometers, such as GAT or CT. To compare these behaviours easily, we developed a 2D graphic diagram in which a cross sagittal section of corneas and tonometers are shown with their corresponding graph below (Fig. 1).
When the flat area of GAT contacts a CC (Fig. 1A), an initial arc length rising from the centre is observed with an initial contact pressure (ICP; blue line) = 7350 N/m2. The maximum corneal deformation is (MCD) = 8 × 104 N/m2. This contrasts with a lower initial arc length converging in the centre that is observed if the GAT contacts an OC, and its ICP = 1600 N/m2 (Fig. 1B; blue line, asterisk) and MCD = 6 × 104 N/m2. However, the OC response recovers similarly to its original (from 1600 to 8500 N/m2) when an external force with a convex surface (CT) contacts the anterior corneal surface after surgery (Fig. 1C), and its MCD = 1 × 105 N/m2. On the other hand, when CT is applied to a CC (Fig. S4,A), these values increase compared to GAT values in normal cornea ICPs of 26000 N/m2.
The CPP barely changed when different elastic behaviours were introduced in a normal cornea (Fig. S2A,B). However, the CPP changed considerably with different thicknesses and when Y varied after the CCT was ablated (Figs. S2C,D–S4).
Another important element of FEA is to evaluate how pachymetry variations influence IOP estimations. With a CC (CCT = 520 μm) with an initial IOP of 15 mmHg (Fig. 2A), as the CCT was ablated we observed a linear reduction in the GAT IOP measurements (Fig. 2B) (−4.4 mmHg for a corneal ablation of 80 μm). However, an overestimation of IOP was recorded when a CC was measured with CT1pre (+6.1 mmHg) and CT2pre (+5.5 mmHg) (Fig. 2C). The same IOP underestimation was recorded parallel to GAT values when CCT was ablated and IOP was measured with CT1 or CT2: −5.7 and −5.5 mmHg, for a corneal ablation of 80 μm, respectively (Fig. 2D).
Clinical results
Demographic information and pre- and post-surgical eye characteristics
A total of 102 eyes from 102 patients (61.8% male; n = 63) were included in the study. Seventy-three (71.6%) patients underwent LASIK and 29 (28.4%) PRK. The mean age was 31.6 ± 6.1 years. The descriptive statistics of variables in the pre- and post-surgical evaluation are normally distributed and are shown in Table 1.
Relationship between IOP and corneal characteristics
IOP values obtained with GAT, CT1 and CT2 in pre- and post-surgery show a significant correlation with CRF for all patients (Table 2). The post-surgery IOP determined with any applanation device correlates with post-surgery CRF, simK, Max.Abl and PTA (Table 2). In addition, CT1 IOP measures correlate with CH.
Considering LASIK and PRK patients separately, in the LASIK subgroup CCT, CRF and PTA are correlated with values of IOP in post-surgery for all tonometers. However, in PRK patients, IOP is only related to pre- and post-surgery CRF (table not shown).
IOP evaluation using different tonometer devices
We evaluated IOP for different tonometers by analysing the concordance of the CT1 and CT2post measurements. Considering GATpre the main reference, CT1 and CT2 in pre-surgery appear to overestimate IOP (Fig. 4). However, in post-surgery, GAT underestimates the IOP, and CT1 and CT2 provide similar values to those obtained with GATpre. A similar result is obtained if LASIK and PRK patients are considered independently (Fig. S5). For all patients, the IOP values measured with different devices in post-surgery evaluation are different, and the IOP obtained with GATpre has a value near to zero similarly to CT1post (mean difference 0.32 mmHg), whereas the mean value is significantly different from zero for GATpost (−3.56 mmHg) and CT2post (0.91 mmHg) (Table 3).
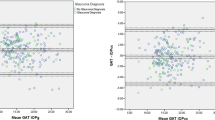
Considering LASIK and PRK patients separately, CT1post (−0.19 mmHg) showed the smallest differences with GATpre (1.62 mmHg) for both LASIK and PRK (Table 3). Considering LASIK and PRK patients together, the Bland-Altman analysis showed poor agreement between GATpre and GATpost (Fig. 5A) (mean differences: −3.56 mmHg, p < 0.001; limits of agreement: −8.10–0.96). However, a much better agreement is observed between GATpre and CT1post (Fig. 5B) (mean differences: 0.32 mmHg, p = 0.187; limits of agreement: −4.24–4.89) and CT2post (Fig. 5C) (mean differences: 0.91 mmHg, p < 0.001; limits of agreement: −3.85–5.67).
Bland-Altman analysis (n = 102) comparing the relation between GATpre and GATpost (A), CT1post (B) and CT2post (C). Continuous red line: observed mean difference; dotted red lines: lower and higher limits of agreement; dotted black line: mean difference of zero. GAT, Goldmann applanation tonometer; CT1-CT2, convex tonometers.
In the LASIK group, GATpost proved to have a poor agreement (mean differences: −3.94 mmHg, p < 0.001; limits of agreement: −8.42–0.50). A better agreement was found for CT1 (mean differences: −0.19 mmHg, p = 0.410; limits of agreement: −4.30–3.92) and CT2post (mean differences: −0.42 mmHg, p = 0.092; limits of agreement: −3.77–4.62) respectively. The PRK group also showed poor agreement for GATpost (mean differences: −2.62 mmHg, p < 0.001; limits of agreement: −6.79–1.55). A better agreement was found for CT1post (mean differences: 1.62 mmHg, p = 0.002; limits of agreement: −0.70–2.54) and CT2post (mean differences: 2.13 mmHg, p = 0.001; limits of agreement: 1.11–2.16) (Table 3).
Nevertheless, in all cases a bias trend was observed. Bland-Altman analysis and the regression bias results for LASIK and PRK patients show best agreements for CT1 followed by CT2. To determine which factors explain the bias trend, multiple stepwise regression was used to relate the IOP differences and the change in corneal characteristics from pre- to post-surgery. For all patients and for subgroups (LASIK and PRK), differences between GATpre and the measurements in post GAT, CT1 and CT2 appeared to be correlated with the differences in CRF before and after surgery (p < 0.001) (Table 2).
The ICC, calculated for all the patients and considering LASIK and PRK separately, had poor or moderate agreement between pre- and post-surgery GAT measurements. However, a good agreement was observed for CT1 and CT2, and the highest values were obtained when the agreement was tested between GATpre – CT1post (p < 0.001) (ICC = 0.718; 95% CI: 0.594–0.812) in the LASIK soubgroup (Table 4).
Intra and inter-observer errors
In terms of the IE of the measurements between the main and second observer in 36 patients pre- and post-surgery, mean differences between measurements performed with several devices do not show significant differences (Table 5). In all cases, the ICC is higher than 0.8 (p < 0.001), and the values are lower in the postoperative period: GATpost ICC = 0.833 (95% CI: 0.697–0.911), CT1post ICC = 0.857 (95% CI: 0.738–0.924), and CT2 post ICC = 0.833 (95% CI: 0.698–0.911). Concerning IA error measurements, in all cases the ICC is higher than 0.9 (p < 0.001) and the values are lower in the postoperative period: GATpost ICC = 0.948 (95% CI: 0.895–0.975), CT1post ICC = 0.933 (95% CI: 0.866–0.967), and CT2post ICC = 0.966 (95% CI: 0.927–0.984) (Table 6).
Discussion
The applicability of the Imbert-Fick law for applanation tonometry is compromised after myopic LRS3,5,8,21,22,23. CB modifications after LRS alter CPP with GAT, so that the corneal force exerted from the centre is much lower in LRS operated eyes compared to standard corneas. We have confirmed that the flattened centre of an OC (3.06 mm area of applanation) is consistent with the idea of Imbert-Fick behaviour24, but not the edges when the GAT is applied. Shih23 also described the area of highest stress to be located around the ablated edge under applanation when CB and IOP were compared between LASIK and PRK. However, we have demonstrated that a different phenomenon can be observed when a convex force (CT) is applied towards the centre of an ablated zone: the initial contact pressure increases in the centre, resulting in a balance of forces similar to that which existed before surgery.
Multiple theoretical models have been described with very different Y estimations (0.1–1.24 MPa)5,6,23,25. Hamilton6 found a 5.35 mmHg error caused by an increase from 0.16 MPa to 0.40 MPa, and a 4.67 mmHg IOP difference across the CCT sample (487.7 to 599.9 μm). This means that both Y and CCT influence IOP measurements in vivo estimations. In our Y = 0.5 MPa ex vivo calculations we found some mathematical results that, without being absolute, correspond to what was obtained in the clinical study: FEA analysis showed that GATpost recorded a −4.4 mmHg as CCT was ablated 80 μm. Considering that LASIK reduces CCT more than PRK (with Max.Abl = 71.23 μm in our sample) this value nearly corresponds to the GATpost underestimation of −3.94 mmHg shown in our LASIK results.
The FEA analysis of CT1post and CT2post compared to GATpre showed IOP differences of 0.4 and 0.0 mmHg respectively, which correlates similarly to our clinical results of a CT1post of −0.19 mmHg and a CT2post of 0.42 mmHg. According to these comparisons, this should have a large impact on the model for explaining what may be truly measured in real life. Hence, these simulations seem valid to compare differential behaviours among different tonometers or between corneas with different thicknesses.
However, we must make a conservative interpretation. FEA has several limitations, mainly due to the complexity of representing ocular tissues mathematically, which affects the range of applicability of the Imbert-Fick law. Furthermore, from a mechanical point of view, the structural geometry of the eye cannot be perfectly represented as it is limited by the numerical viability of the simulation. FEA simulations are complex and require multiple models to achieve hypothetical geometric pre- and postoperative corneas26. The main limitation of our numerical models is that they do not take into account the viscoelastic behaviour of the cornea. In addition, they were designed for PRK and not LASIK. Nevertheless, previous results23 have found similar corneal deformation patterns in 3D and 2D FEA between PRK and LASIK. Therefore, the two surgical approaches are comparable in terms of central corneal displacement. Since our goal was not to compare different corneal biomechanics between LASIK and PRK, but rather to evaluate areas of applanation (corneal displacement) contacted by different external tonometers after LRS, we decided to simplify our comparisons and use a PRK shaped cornea.
Besides, another significant limitation still affects the tonometry: the internal variability in corneal idiosyncrasies. As discussed previously27, it is almost impossible to find a single universal number for corneal clinical properties. Assessing how the strength or weakness of a cornea can influence IOP readings seems unrealistic beyond a single pachymetric or biomechanical parameter. This implies that tonometry is not reliable, not only due to CCT variability28, but also due to the alteration of the corneal structure. Therefore, correction algorithms for GAT are not reliable since they are based only on changes in CCT6,29.
It has been described30,31,32 that the bias in internal patient variability in CCT can be minimized with modified versions of GAT, which opens a new horizon for GAT modifications in the near future. Mccafferty et al. demonstrated that a bi-curved concave-convex surface modified GAT can significantly reduce GAT prism sensitivity to CCT in standard corneas. However, our FEA analysis and clinical results show that a central convex modification of GAT seems to be accurate for measuring IOP in OCs. Therefore, this study is the first to show that a unique convex surface modified version of GAT could be reproducible for post operated LASIK or PRK IOP measurements.
Concerning other devices, the Pascal tonometry (PDCT) does not appear to be as influenced by CB after LASIK as other tonometers33. After reducing the mean corneal pachymetry of 90.2 μm, Pepose et al. found no statistically significant differences in pre- and post-surgery IOP measurements taken with PDCT (−0.5 ± 2.6 mmHg, p = 0.27), compared to pre-and post-measurements taken with GAT (−1.8 ± 2.8 mmHg p < 0.01). Sales-Sanz34 found that the Schiøtz tonometer has less disparity in terms of coefficient ocular rigidity (Ko) than PDCT and GAT after the LASIK procedure, although it is not commonly used in clinical practice. There are other devices that are more extensively used, such as the rebound tonometer iCare (Tiolat Oy, Helsinki, Finland); however, it underestimates IOP in post LASIK like GAT. Previous reports35 described no statistically significantly difference between iCare and GAT in 96 myopic patients after LASIK with a mean underestimation of −4.9 ± 2.5 mmHg and −3.4 ± 2.5 mmHg, respectively.
With respect to tonometers that are less influenced by CB36, different IOP measurements between the Corvis ST tonometer, GAT and ORA (corneal compensated IOP and Goldmann-correlated IOP) have been described in 50 myopic patients after LASIK: 3.4, 1.0 and 3.8 mmHg Bland-Atlmann bias respectively (95% limits of agreement of −0.7 to 7.5, −2.1 to 4.2, and −0.4 to 8.0 mmHg). In our LASIK subgroup of 73 patients, the mean difference for CT1post was 0.19 mmHg (limits of agreement: −4.30–3.92), and 0.42 mmHg for CT2post (limits of agreement: −3.77–4.62), indicating that IOP estimations with CT1post are similar to those provided with GATpre. Therefore, it seems that CT1 offers a more accurate estimation in patients with LASIK than GAT. Nevertheless, tonometry after LRS may not be interchangeable due to the diversity in the results. We believe it is relevant which tonometer and which IOP are taken as baseline after LRS, and that GATpost should not be taken as IOP reference. Our new device correlated with GATpre in our LASIK group, but an important remark of our study is that GATpre is an estimation of IOP and could not be accurate. Besides, CT must not be used in subjects whose CB properties have not been strongly modified by laser -as in PRK corneas- because it seems to overestimate IOP. On the other side, we have not compared it with other non-applanation tonometers in pre or post-surgery. Future studies are necessary to evaluate agreement between CT and PDCT, Corvis ST, or corneal compensated IOP in this subgroup of patients.
In contrast to the LASIK group, our PRK patients showed greater deviation, indicating that the CT device is not as accurate as for LASIK patients. In our Bland-Altman analysis, the IOP readings obtained with CT1post were similar to those obtained with GATpre for all patients. However, for PRK patients the deviation was higher than in LASIK patients, indicating that CT performed less accurately for the PRK approach. Moreover, GATpost showed a relatively good agreement in the PRK group, which means GAT could be reproducible in PRK patients. This is consistent with previous research7, which found minimal changes with GAT (0.5 ± 2.4 mmHg; p < 0.01) in 111 PRK patients with a mean ablation of 23 ± 23 μm in corneal thickness. Furthermore, the PRK group received FML during 4 weeks after surgery. Despite topical steroids (TS) could have elevated IOP37, we believe that differences in IOP in both groups are due to CB changes, not to TS effect. FML has proven to be less ocular hypertensive than other topical steroids37, and TS effect on IOP recovers to baseline within 1 to 3 weeks of discontinuing treatment38. Our PRK IOP was measured after 8 weeks of stopping TS, so it seems steroids could not influence the IOP measurements at this point.
Other limitations affect our research: First, post-surgery IOP was not validated by comparing it with intracameral IOP readings39 due to its invasive nature. Second, the sequence in which we measured IOP could imply certain bias in the second and third IOP measurements: repeated tonometry may induce changes in the anterior chamber volume and thus, in the registered pressure. AlMubrad et al.40 found a statistically significant IOP reduction (1.5 ± 1.2 mmHg; p < 0.05) on subsequent measurements performed with a non-contact tonometer (Topcon CT80) after GAT in 65 patients. Gaton et al.41 recorded a significant IOP decrease between first and second successive measurements with GAT (15.94 mmHg vs 14.9 mmHg, p < 0.0001) in 70 glaucomatous eyes. We believe that repeated contact of any external force with the eye may produce occasional IOP fluctuations. This would lead to significant underestimations that could be transcendent regarding glaucoma diagnosis. However, other considerations should be taken into account, such as IOP levels beyond the normal range or CB. A third source of bias in our study could be related to IOP diurnal fluctuation in time. Baseline IOP could be unbalanced across measurements after 3 months even if measurements are taken at the exact same time42. Further research could determine whether CT performs accurately.
Regarding variables that could influence our measurements, CRF showed a significant correlation for all the tonometers pre- and post-surgery. As in other reported studies33,43, CRF decreased after both procedures but mainly in LASIK as opposed to PRK. It is evident that PRK is less invasive than LASIK, which implies that CB properties are better conserved. We believe this could be the reason why CT overestimates IOP before surgery and performs less accurately in PRK corneas. This would coincide with our clinical findings for CT1 and CT2pre, which were not useful in non-operated corneas since they overestimated IOP measurements.
The posterior corneal shift after LRS procedures has been widely evaluated to detect possible ectasia44,45,46. However, no previous studies have specifically addressed how PCC changes could influence GAT IOP readings after LRS procedures. In 50 normal subjects, Firat et al.47 found that anterior and posterior curvature values and corneal volume do not influence IOP readings made with GAT. These results coincide with our pre-surgery results in which no IOP reading of any tonometer was correlated with PCC, simK or VOL in 102 normal patients. In the post operated subgroups, PCC and VOL also did not seem to influence IOP readings. We believe this could be related to posterior corneal curvature changes recovering three months after surgery46, which was the time our measurements were taken. On the other hand, CCT, Max. abl, and PTA could explain the differences among GATpre, CT1 and CT2post in the LASIK group. As more corneal tissue is removed in high myopia in the anterior stroma, it is expected that CB is more altered. Therefore, a bias could be expected for all the tonometers, which would have a significant impact on GAT readings, compared to the PRK group.
Both pre- and post-surgery tissue characteristics should be taken into account when IOP measurements are considered in post LRS corneas. Although we could expect post-surgery measurements to be close to those prior to surgery, a range of known variability (as we find in GAT with normal corneas) can be expected because tonometry is not personalized. In addition, the most accurate options for measuring IOP in LRS patients are not usually available or accessible to all ophthalmologists. This new simple and affordable option could solve a problem that has not yet been solved and make it available for universal use. Notwithstanding, new studies will be necessary to confirm the data analysis, make comparisons with other tonometers, and verify whether CT could also be used in patients with hypermetropic LRS, keratoconus, or after corneal transplantation.
Nevertheless, our device has demonstrated good agreement between GAT and CT1post in the LASIK subgroup, and thus minimizes the effect of the loss of central tissue in this type of surgery. The IA/IE results also indicate that there were no significant differences between observers, and therefore it could be a reproducible and convenient alternative for any ophthalmologist, and suitable for a currently very frequent and specific patient profile10,11. In conclusion, we have designed a new version of the applanation tonometer that could be used after LASIK instead of the current tonometer reference. This provides a new applanation tonometry option that is appropriate for supporting the diagnosis of ocular hypertension in this subgroup of patients.
Data availability
The datasets generated and/or analysed during the current study are not publicly available due to exclusive rights to intellectual property of the new “CT” convex tonometer secured by a Spanish patent filed P201631280, but are available from the corresponding author upon reasonable request.
References
Pfeiffer, N. et al. Central corneal thickness in the European Glaucoma Prevention Study. Ophthalmology 114, 454–459 (2007).
Moses, R. A. The Goldmann applanation tonometer. Am. J. Ophthalmol. 46, 865–869 (1958).
De Moraes, C. G. V., Prata, T. S. & Liebmann, J. R. R. Modalities of Tonometry and their Accuracy with Respect to Corneal Thickness and Irregularities. J. Optom. 1(2), 43–49 (2008).
Society, E. G. Terminology Guidelines. European Glaucoma Society Foundation (2017).
Liu, J. & Roberts, C. J. Influence of corneal biomechanical properties on intraocular pressure measurement: Quantitative analysis. J. Cataract Refract. Surg. 31, 146–155 (2005).
Hamilton, K. E. & Pye, D. C. Young’s modulus in normal corneas and the effect on applanation tonometry. Optom. Vis. Sci. 85, 445–450 (2008).
Mardelli, P. G., Piebenga, L. W., Whitacre, M. M., Siegmund, K. D. & Argus, W. A. The effect of excimer laser photorefractive keratectomy on intraocular pressure measurements using the Goldmann applanation tonometer. Ophthalmology 104, 945–949 (1997).
Duch, S., Serra, a, Castanera, J., Abos, R. & Quintana, M. Tonometry after laser in situ keratomileusis treatment. J. Glaucoma 10, 261–5 (2001).
Yang, E. & Roberts, C. J. A Review of Corneal Biomechanics after LASIK and SMILE and the Current Methods of Corneal Biomechanical Analysis. J. Clin. Exp. Ophthalmol. 06, (2015).
Sánchez-Navés J, Furfaro L, Piro O, B. S. Impact and permanence of LASIK-induced structural changes in the cornea on pneumotonometric measurements: contributions of flap cutting and stromal ablation. J Glaucoma Dec;17(8) (2008).
Knorz, M. C., Liesenhoff, H. & Liewnann, A. Laser In Situ Keratomileusis for Moderate and High Myopia and Myopic Astigmatism. Ophthalmology 105, 932–940 (1998).
Cummings, A. et al. LASIK Volume Around the Globe. April 2016. (2018).
Rochtchina, E., Mitchell, P. & Wang, J. J. Relationship between age and intraocular pressure: The Blue Mountains Eye Study. Clin. Exp. Ophthalmol. 30, 173–175 (2002).
Kling, S. & Hafezi, F. Corneal biomechanics – a review. Ophthalmic Physiol. Opt. 37, 240–252 (2017).
Su, P., Yang, Y., Xiao, J. & Song, Y. Corneal hyper-viscoelastic model: Derivations, experiments, and simulations. Acta Bioeng. Biomech. 17, 73–84 (2015).
Pinsky, P. M., Van Der Heide, D. & Chernyak, D. Computational modeling of mechanical anisotropy in the cornea and sclera. J. Cataract Refract. Surg. 31, 136–145 (2005).
Recep, Ö. F., Hasiripi, H., Vayisoǧlu, E., Kalayci, D. & Sankatipoǧlu, H. Accurate time interval in repeated tonometry. Acta Ophthalmol. Scand. 76, 603–605 (1998).
Shen, M. et al. Diurnal variation of ocular hysteresis, corneal thickness, and intraocular pressure. Optom. Vis. Sci. 85, 1185–1192 (2008).
Fernández, J., Rodríguez-Vallejo, M., Martínez, J., Tauste, A. & Piñero, D. P. Corneal biomechanics after laser refractive surgery: Unmasking differences between techniques. J. Cataract Refract. Surg. 390–398, (2018).
Landis, J. R. & Koch, G. G. The Measurement of Observer Agreement for Categorical Data Data for Categorical of Observer Agreement The Measurement. 33, 159–174 (2012).
Alonso-Muñoz, L. et al. Assessment of appla- nation tonometry after hyperopic laser in situ keratomileusis. Cornea. 21, 156–160 (2002).
Agudelo LM, Molina CA, A. D. Changes in intraocular pressure after laser in situ keratomileusis for myopia, hyperopia, and astigmatism. J Refract Surg. Jul-Aug;18 (2002).
Shih, P., Wang, I., Cai, W. & Yen, J. Biomechanical Simulation of Stress Concentration and Intraocular Pressure in Corneas Subjected to Myopic Refractive Surgical Procedures. Sci. Rep. 1–15, (2017).
Shimmyo, M., Ross, A. J., Moy, A. & Mostafavi, R. Intraocular pressure, Goldmann applanation tension, corneal thickness, and corneal curvature in Caucasians, Asians, Hispanics, and African Americans. Am. J. Ophthalmol. 136, 603–613 (2003).
Yen, J.-Y., Wang, I.-J. & Shih, P.-J. On the in Vivo Estimation of the Corneal Young’s Modulus. JOJ Ophthalmol. 5, 1–8 (2017).
Sinha Roy, A., Dupps, W. J. & Roberts, C. J. Comparison of biomechanical effects of small-incision lenticule extraction and laser in situ keratomileusis: Finite-element analysis. J. Cataract Refract. Surg. 40, 971–980 (2014).
Roberts, C. J. Concepts and misconceptions in corneal biomechanics. J. Cataract Refract. Surg. 40, 862–869 (2014).
Chang, D. H. & Stulting, R. D. Change in intraocular pressure measurements after LASIK: The effect of the refractive correction and the lamellar flap. Ophthalmology 112, 1009–1016 (2005).
Brandt, J. D. et al. Adjusting intraocular pressure for central corneal thickness does not improve prediction models for primary open-angle glaucoma. Ophthalmology 119, 437–42 (2012).
Mccafferty, S., Lim, G., Duncan, W., Enikov, E. & Schwiegerling, J. Goldmann Tonometer Prism with an Optimized Error Correcting Applanation Surface. 5, (2016).
Mccafferty, S. et al. Goldmann tonometer error correcting prism: clinical evaluation. 835–840 (2017).
Mccafferty, S., Tetrault, K., Mccolgin, A., Levine, J. & Muller, M. Intraocular pressure measurement accuracy and repeatability of a modified Goldmann prism: Multi-center randomized clinical trial. Am. J. Ophthalmol. 196, 145–153 (2018).
Pepose, J. A. Y. S., Feigenbaum, S. K., Qazi, M. A., Sanderson, J. P. & Roberts, C. J. Changes in Corneal Biomechanics and Intraocular Pressure Following LASIK Using Static, Dynamic, and Noncontact Tonometry. 39–48, (2007).
Sales-Sanz, M. et al. Effect of Laser in Situ Keratomileusis on Schiøtz, Goldmann, and Dynamic Contour Tonometric Measurements. J. Glaucoma 25, e419–23 (2016).
Lam, A. K. C. et al. Effect of laser in situ keratomileusis on rebound tonometry and Goldmann applanation tonometry. J. Cataract Refract. Surg. 36, 631–636 (2010).
Hong, J. et al. A new tonometer-the corvis ST tonometer: Clinical comparison with noncontact and goldmann applanation tonometers. Investig. Ophthalmol. Vis. Sci. 54, 659–665 (2013).
Busool, Y. et al. Risk factors predicting steroid-induced ocular hypertension after photorefractive keratectomy. J. Cataract Refract. Surg. 43, 389–393 (2017).
Shokoohi-Rad, S., Daneshvar, R., Jafarian-Shahri, M. & Rajaee, P. Comparison between Betamethasone, Fluorometholone and Loteprednol Etabonate on intraocular pressure in patients after keratorefractive surgery. J. Curr. Ophthalmol. 30, 130–135 (2018).
Feltgen, N., Leifert, D. & Funk, J. Correlation between central corneal thickness, applanation tonometry, and direct intracameral iop readings. Br. J. Ophthalmol. 85, 85–87 (2001).
Almubrad, T. M. & Ogbuehi, K. C. The effect of repeated applanation on subsequent IOP measurements. Clin. Exp. Optom. 91, 524–529 (2008).
Gaton, D. D. et al. Effect of repeated applanation tonometry on the accuracy of intraocular pressure measurements. Curr. Eye Res. 35, 475–479 (2010).
Kim, S. H. et al. The effect of diurnal fluctuation in intraocular pressure on the evaluation of risk factors of progression in normal tension glaucoma. PLoS One 11, 1–14 (2016).
Kamiya, K., Shimizu, K. & Ohmoto, F. Comparison of the changes in corneal biomechanical properties after photorefractive keratectomy and laser in situ keratomileusis. Cornea 28, 765–9 (2009).
Ciolino, J. B. & Belin, M. W. Changes in the posterior cornea after laser in situ keratomileusis and photorefractive keratectomy. J. Cataract Refract. Surg. 32, 1426–1431 (2006).
Wang, L., Guo, H.-K., Zeng, J., Jin, H.-Y. & Meng, Q.-L. Stability of the posterior corneal surface after laser in situ keratomileusis for myopia. Int. J. Ophthalmol. 12, 52–54 (2012).
Roberts, C. J. & Dupps, W. J. Paired versus unpaired significance testing: How improper statistical analysis altered interpretation of posterior surface changes after LASIK. J. Cataract Refract. Surg. 40, 858–861 (2014).
Firat, P. G., Orman, G., Doganay, S. & Demirel, S. Influence of corneal parameters in keratoconus on IOP readings obtained with different tonometers. Clin. Exp. Optom. 96, 233–237 (2013).
Acknowledgements
The authors would like to thank Emilio Iglesias Touriño MD, PhD, an ophthalmologist whose extraordinary knowledge and advice was indispensable in the development of the new CT device. GRANT INFORMATION: MI received a personal research grant from the Catalonian Ophthalmology Society 2016–2018 Barcelona, Spain. This society played no role in the design or conduct of this research.
Author information
Authors and Affiliations
Contributions
M.I. collected, analysed and interpreted the sample data and was a major contributor in writing the original manuscript. F.Y. analysed and interpreted the physics analysis. B.K. analysed and interpreted the clinical results. C.S. interpreted the statistical analysis. L.A. and B.K. contributed to collecting double-masked inter-observer data. R.P.C.M., J.N. and R.B. reviewed the manuscript. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Competing interests
Each of the co-authors has seen and agrees with the competing interests statement presented by M. Iglesias, MD (as corresponding author) on behalf of all the authors of the paper. Financial competing interests: M. Iglesias, MD has personal financial interests, being the inventor of the new “CT” applanation tonometer. M. Iglesias, MD has exclusive personal rights to the intellectual property of this invention secured by a Spanish patent filed P201631280 (awarded patent), and an international patent PCT/ES2017/070626 application (patent pending). M. Iglesias, MD declares no other financial competing interests. The rest of the co-authors declare no financial competing interests. Non-financial competing interests: M. Iglesias, MD and the rest of the co-authors declare they do not have non-financial competing interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made. The images or other third party material in this article are included in the article’s Creative Commons license, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons license and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this license, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Iglesias, M., Yebra, F., Kudsieh, B. et al. New applanation tonometer for myopic patients after laser refractive surgery. Sci Rep 10, 7053 (2020). https://doi.org/10.1038/s41598-020-64013-4
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41598-020-64013-4
This article is cited by
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.