Abstract
The pathological mechanism of Kashin-Beck disease (KBD), an endemic osteoarthritic disease, remains to be poorly understood. This study was designed to identify signaling pathways and crucial proteins involved in the pathological mechanism of KBD compared with osteoarthritis (OA). The knee cartilage samples were collected from gender- and age-matched KBD (n = 9) and OA (n = 9) patients. After pre-processing, samples were labeled with Tamdem Mass Tags 6plex multiplex kit, and analyzed by liquid chromatography-tandem mass spectrometry. Proteomic results were analyzed with gene ontology (GO), Kyoto Encyclopedia of Genes and Genomes (KEGG), and protein-protein interactions (PPI). The differential abundance proteins from KBD and OA were validated using western blot analysis. As a result, A total number of 375 proteins were identified to have differential abundance between KBD and OA, of which 121 and 254 proteins were observed to be up-regulated or down-regulated in KBD group. GO analysis shows that the differential abundant proteins are associated with cell junction and signal transducer activity from extracellular to intracellular. KEGG pathways enrichment and PPI network indicate four major pathways, including extracellular matrix -receptor interaction, focal adhesion, phosphatidylinositol 3-kinase (PI3K)-Protein kinase B (Akt), and Ras signaling pathways were involved in the degeneration of cartilage. Moreover, integrins, laminins, NF-κB and other regulative molecules were found as crucial proteins. In conclusion, our results demonstrated that compared with OA, the differential abundance proteins and signaling pathways may contribute to the occurrence and development of joint damage in KBD. Further investigation of their regulative roles and interaction may provide new insights into the pathological mechanisms and therapeutic targets for KBD.
Similar content being viewed by others
Introduction
Osteoarthritis (OA) is a progressive, degenerative joint disease. It is the major cause of knee pain and locomotor disability worldwide1,2. The WHO Scientific Groupon Rheumatic Diseases estimates that 10% of the world’s population who are 60 years or older have significant clinical problems attributed to OA3. Unlike OA, Kashin-Beck disease (KBD) is a chronic and serious endemic osteoarticular disease, which has been in high prevalence and morbidity in Eastern Siberia of Russia, Northeast China to Sichuan-Tibet Plateau, and North Korea4,5. According to the statistics, there were 1.04 billion people in risk of KBD and 0.57 million patients with KBD in China6. However, the etiology and pathological mechanisms of KBD are still waiting to be uncovered7, which lessen the chances of further effective prevention and treatment measures for the current KBD patients.
Several similar pathological changes have been found in KBD and OA, including degradation of extracellular matrix (ECM), cartilage lesion, reduction and disruption of proteoglycans (PGs) and collagens5,8,9,10. While the causes and pathological mechanism of the KBD and OA differ in many aspects. OA occurs mainly in the middle aged and elderly population1. The pathologic changes in OA joints include degradation of the articular cartilage, especially at the superficial zones, thickening of the subchondral bone, osteophyte formation, and variable degrees of synovial inflammation11. KBD occurs mostly in children aged 3–12 years old in endemic regions4. Most of the deformities were established at the age of 15, then subsequently become symptomatic in adults7,12,13. A typical distinction of KBD from OA or other bone and joint diseases is the damage of epiphyseal cartilage and hyaline cartilage in the deep zones of cartilage11,14. This distinction might explain the occurrence of severe joint deformities during development in young people with KBD15.
After taking some efficient efforts in the past decades, including changing the source of drinking water, using selenium supplements, exchanging grains from non-endemic areas and other controlling measures, the prevalence of KBD has been in control4,9. The incidence of KBD is rare nowadays, and only 2.24% of the current patients are under13 age6. The local farmers and the immigrating populations are the major population suffering from KBD4. KBD caused pain and deformities in joints and ability lost in doing farm work, which increased economic burdens to their family and society3,4,5. Meanwhile, the current adult KBD patients are mostly advanced KBD often accompanied by OA8,10. The lack of systematical proteomic analysis of KBD and OA cause theoretical blankness of pathological mechanism research on KBD.
This study was designed to identify the proteins in differential abundance between KBD and OA, and enrich the signaling pathways the proteins involved by using bioinformatics analysis. It is expected to reveal the initial signal transduction procession and contribute to the pathological mechanism investigation of KBD.
Methods
Sample collection
For the proteomic analysis, 18 knee arthritic cartilage samples were collected. 9 KBD samples were obtained from the patients between 54–68 years of age, who were living in the KBD-endemic areas of Linyou in Shannxi province. 9 OA samples were obtained from non-KBD-endemic areas from Xi’an in Shaanxi province (Detailed subjects characteristics are shown in Table 1). The KBD and OA cartilage donors were age- and gender-matched Chinese Han lineage. OA was diagnosed based on the Western Ontario and McMaster Universities OA Index16. KBD was diagnosed as grade I or grade II based on the clinical criteria used for the diagnosis of KBD (WST 207–2010) in China12,13,16. The damage degrees of OA and KBD cartilage were diagnosed as grade 2–3.5 based on histopathology staining17. Articular cartilage tissues were collected from the same anatomical position of the femoral condyles. This investigation was approved by the Human Ethics Committees of Xi’an Jiaotong University. All procedures performed in this study involving human participants were in accordance with the 1964 Helsinki declaration and its later amendments or comparable ethical standards. All the donors were provided a written informed consent for the study participation and publication of their individual clinical details and images.
Sample preparation
After collection, the articular cartilage tissues were cut, snap-frozen for 5 minutes using liquid nitrogen and stored at −80 °C. For each group, 3 samples were mixed together as 1 biological replicate. then homogenized by grinding and weighted in precooled 2 ml conical tubes, and 0.8 ml solution containing 4% SDS, 100 mM Tris-HCl, 100 mM 1,4-dithiothreitol, pH 8.0 was added (10%, v/w). The mixtures were boiled and homogenized by ultrasonication in ice bath and centrifuged. The supernatant was filtered with 0.22 µm ultrafiltration device. 1 µl of each sample was quantitated with BCA kit (SK3021, Sangon Biotech, Shanghai, China), then the samples were aliquoted in tubes to contain 20 μg protein each, and stored at −80 °C.
TMT labeling and high-pH chromatography separation
The samples were weighted at 300 μg for filter aided sample preparation enzymolysis, and this procession was strictly in accordance with the protocol of universal sample preparation method for proteome analysis18. The filtrates were collected, and the peptides of the samples were quantitated by measuring optical density at 280 nm. 100 μg of the samples were labeled with Tandem Mass Tag (TMT) 6plex Isobaric Label Reagent Set (Thermo Scientific, Rockford, IL, USA). In both KBD and OA groups, 9 samples have been pooled into 3 samples, each with 3 patients, and 6 samples was acquired finally. The total 6 mixed samples were subjected to High-pH Reversed-Phase Fractionation in 1100 Series HPLC Value System (Agilent Technologies, Waldbronn, Germany) equipped with a Gemini-NX column (00F-4453-E0, 4.6 × 150 mm, 3 μm, 110 Å, Phenomenex, Torrance, CA, USA), which was eluted at a flow rate of 0.8 ml/minute. The whole elution process was monitored by measuring the absorbance at 214 nm, and fractions were collected every 1.25 minutes. Finally, the collected fractions (approximately 40) were combined into ten fractions. Each fraction was concentrated by vacuum centrifugation and reconstituted in 40 μl of 0.1% v/v trifluoroacetic acid. The samples collected were stored at −80 °C.
Quantitative LC-MS/MS Analysis
Quantitative proteomic based on liquid chromatography-tandem mass spectrometry (LC-MS/MS) was applied to proteins collected from the former procedure. LC-MS/MS analysis was performed on an Easy nLC nanoflow HPLC system connected to Thermo Scientific Orbitrap Fusion Tribrid mass spectrometer (Thermo Fisher Scientific, San Jose, CA, USA). A total of 1 μg samples were loaded with an auto-sampler onto a Thermo Scientific EASY column (2 columns, at a flow rate of 150 nl/minute), then separated in the Thermo Scientific EASY trap column (100 µm * 2 cm, 5 µm, 100 Å, C18) and analytical column (75 μm×25 µm, 5 µm, 100 Å, C18) with a segmented 2 hours gradient of solvent A (0.1% formic acid in water) to 35% of solvent B (0.1% formic acid in 84% acetonitrile) for 100 minutes, followed by 35 – 90% of solvent B for 3 minutes, and 90% of solvent B for 5 minutes. The column was re-equilibrated to its initial highly aqueous solvent composition before each analysis.
The mass spectrometer was operated in positive ion mode, and MS spectra were acquired over a range of 375–1500 m/z. The resolving powers of the MS scan and MS/MS scan at 200 m/z for the Fusion were set as 120,000 and 50,000, respectively. Data Dependent Mode was Top Speed, Cycle Time 3 seconds and ions were fragmented through higher energy collisional dissociation. The maximum ion injection times were set to 50 ms for the survey scan and 105 ms for the MS/MS scans, and the automatic gain control target values for Master scan modes were set to 4e5, and for MS/MS 1e5. The dynamic exclusion duration was 40 seconds.
Mass spectrometry and Bioinformatics analysis
Proteome Discoverer 2.1 software (Thermo Fisher Scientific) was used to analyze the raw files. (Matrix Science) embedded in Proteome Discoverer was used to search the raw data against the uniprot_human_156914_20170308.fasta (Total 156914 sequences). Peptide mass tolerances of ± 20 ppm and fragments of mass tolerance of 0.1 Da were used for parent and monoisotopic fragment ions. All data were reported based on 99% confidence for protein identification, as determined by ≤0.01 (High Confident) false discovery rate (FDR) using a decoy database. Peptides and proteins with FDR less than 0.01 were accepted and further processed. The relative quantitative analysis of the proteins in the samples based on the ratios of TMT reporter ions from all unique peptides. The relative peak intensities of the TMT reporter ions released in the MS/MS spectra were used for quantification. Then, the final ratios obtained from the relative protein quantifications were normalized based on the median average protein quantification ratio.
Principal component analysis (PCA) has been conducted to investigate the homogeneity within groups and heterogeneity between groups. Proteins in statistically differences and the changing ratio over 1.2 were further analyzed for functional and biological relevance. Differentially expressed proteins expressed with a log form were input as hierarchical clustering algorithms for gene ontology (GO) analysis derived from the UniProt-gene ontology annotation (GOA) database. The identified differentially expressed proteins were annotated as three categories, i.e. biological process, cellular component, and molecular function, based on GO enrichment analysis. Pathway enrichment analysis of differential expressed proteins was performed using KEGG database. Enriched GO terms were identified with Fisher’s Exact Test.
In addition, the identified proteins were sent to the String database (https://string-db.org/) to predict and visualize the protein-protein interactions (PPI) among the differentially expressed proteins. The represented network has been obtained at a medium confidence in data settings with min interaction score as 0.4.
Validation of protein expressions
For the validation of the differentially expressed proteins, western blotting was used for quantitative analysis. Cartilage tissues were lysed by 2% sodium dodecyl sulfate with 2 M urea, 10% glycerol, 10 mM Tris-HCl (pH 6.8), 10 mM dithiothreitol and 1 mM phenylmethylsulfonyl fluoride, then the lysates were centrifuged. The supernatants were separated by SDS-PAGE and blotted onto a nitrocellulose membrane (Bio-Rad Laboratories, Hercules, CA, USA). After blocking with 5% skimmed milk, the membrane was then analyzed using specific antibodies and visualized by enhanced chemiluminescence (ECL Kit, Amersham Biosciences, Little Chalfont, UK). The primary antibodies to Indian hedgehog (IHH, ab52919), type I collagen (COL1A1, ab138492), type II collagen (COL2A1, ab188570), aggrecan (ACAN, ab3778) and glyceraldehyde-3-phosphate dehydrogenase (GAPDH, ab9894) were obtained from Abcam (Cambridge, UK). Protein signals were detected using secondary HRP-conjugated anti-mouse or anti-rabbit antibodies by the enhanced chemiluminescence (ECL Kit, Amersham Biosciences, Little Chalfont, UK). The full-length images of individual blots were displayed in Fig. S1.
Results
Proteomic results
Considering the complex biological differences in human samples, PCA results showed the homogeneity and heterogeneity in and between KBD and OA groups (Fig. S2). The proteomics results can identify differential expressed protein between the two groups. In the result, a total of 11362 unique peptides corresponding to 2205 proteins were identified (Table S1). Protein intensity based absolute quantification values were used to describe the protein abundance. Proteins with an abundance difference ratio ≥ 1.20 and p <0.05 (t-test) were considered as up-regulated proteins, and those with ratio ≤0.83 as down-regulated proteins. Following this criterion, a total of 375 proteins (121 proteins up- and 254 down-regulated in KBD group) were defined as differentially expressed proteins in comparison with OA group (Table S2).
GO terms and GO enrichment analysis
To understand the functions and biological processes of the differentially abundant proteins involved in the KBD group, we performed GO term and GO enrichment analysis with GO enrichment software. Multiple corrections for GO has been conducted and showed with q value.
GO terms results showed that the top abundant terms are: binding, structural molecular activity, molecular transducer activity, and signal transducer activity (molecular function); macromolecular complex, membrane part, extracellular region, and cell junction (cellular component); cellular procession, metabolic process, localization, and response to stimulus (biological process) (Fig. 1). This result indicates that the differential metabolic activity in KBD could be associated with cell junction and signal transducer activity from extracellular region to intracellular.
The GO enrichment analysis shows that integral component of membrane, intrinsic component of membrane, ribosome, endoplasmic reticulum, intermediate filament, membrane, intermediate filament cytoskeleton, are the major GO terms of altered proteins (Fig. 2). The results of GO enrichment and GO term analysis are in high consistence, and the identified biological processes can be marked as entry points for the further pathological mechanism investigation.
KEGG enrichment analysis
To investigate the functions and signaling pathways, which the differentially expressed proteins were involved in, KEGG automatic annotation server (KAAS) was used to search the identified proteins in the KEGG GENES database. KEGG enrichment analysis and multiple corrections were conducted and showed with q value.
As shown in KEGG annotation, major metabolisms are carbohydrate metabolism, lipid metabolism; major genetic information processing are translation, folding, sorting and degeneration; major environmental information processing are signal transduction, signaling molecules and interaction; major cellular processes are transport and catabolism, cellular community-eukaryotes; organismal systems are endocrine systems, immune system; the detailed information was showed in Fig. 3. And the results of KEGG enrichment were showed in Fig. 4.
Total of 254 differentially expressed proteins were mapped in 245 signaling or metabolic KEGG pathways. Then the signaling pathways were ranked by the number of proteins involved. Focal adhesion, phosphatidylinositol 3-kinase (PI3K)-Akt signaling pathway, ECM-receptor interaction signaling pathway were identified in the proteins differentially expressed in KBD (Fig. 5). These signaling pathways are closely related to chondrocyte metabolisms, such as cell junction activity and signaling transducer activity from extracellular region to intracellular.
In addition, key proteins MAPK3, RELA, STAT3, ROCK1, ITGB3, ITGA1, LAMA2, COL4A1, COL1A2, COL1A1, THBS3, THBS4, RALA, GNG5, GNB1, and GNG5 were revealed to be closely related to chondrocyte metabolism (Table 2). These results implied potential targets for further research of signaling pathways involved in KBD, which might provide necessary clues for the investigation of the pathological mechanism of KBD.
Protein-protein interaction network
Different sorts of proteins interact with each other and participate in a series of biochemical reactions in order to perform their biological functions. To obtain more clues of the functions of the abundant proteins differentially expressed, protein-protein interaction networks were conducted with STRING and Cytoscape databases. As the result, the central role of proteins like Ras-related protein Ral-A (RALA), integrin alpha-1 (ITGA1), transcription factor p65 (NF-κB, RELA), signal transducer and activator of transcription 3 (STAT3), cAMP-dependent protein kinase type I-alpha regulatory subunit (PRKAR1A), collagen alpha-1(IV) chain (COL4A1) appeared crucial in the regulation of differential expression of proteins (Fig. 6).
Protein interaction network analysis of proteins differentially expressed in KBD compared with OA. The relationship of proteins differentially expressed in KBD compared with OA group. “─” means “direct relationship”; red indicates up-regulated proteins, green indicates down-regulated proteins. Confidence: 0.4.
Western blot validation
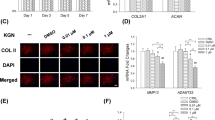
To validate the alterations in expression of these proteins in KBD and OA group, equal amounts of protein samples were analyzed by Western blot with specific antibodies. The expression level of IHH (hedgehog subfamily), COL2A1, and COL1A1 was decreased in KBD compared with OA, while aggrecan (ACAN) was increased in KBD (Fig. 7). Thus, it can be seen that the protein expression trends are in high consistency with proteomic assay results.
Discussion
TMT labeling combined with high-pH chromatography separation and quantitative LC-MS/MS analysis is an efficient, high-throughput, and accurate technology method to analyze the expression levels, locations, functions, and interactions of proteins. More proteins can be identified with TMT labeling proteomics than 2-D DIGE proteomics. Previous study has conducted proteomics analysis between KBD and health group with 2-D DIGE proteomics14. Previous study and our study both identified down regulated phosphoglycerate kinases (PGKs) in KBD. PGK1 was identified in the previous study and PGK2 in our study. Furthermore, in our results, four central pathways (ECM-receptor interaction, focal adhesion, PI3K-Akt signaling pathway, Ras signaling pathway) were identified in the proteins differentially expressed in KBD. These results may provide potential signaling pathways for further investigation of KBD pathological mechanism.
Articular cartilage ECM consists of a complex mixture of PGs, collagens, aggrecan, and serves an important role in the maintenance of tissue morphogenesis and function19. Former studies observed decreased content of PGs and aggrecan in the deep zone of KBD cartilage20,21,22,23. In this study, the protein-protein interaction and KEGG pathways analyses indicated that collagens (COL1A1, COL1A2, and COL4A1), were relatively decreased in the KBD group. Besides, certain other ECM components, such as aggrecan (ACAN), CHAD, LAMA2, THBS3, THBS4, and transmembrane ECM receptor protein integrin (ITGA1, ITGB3) are in differential abundance in KBD group.
Integrin is a family of transmembrane proteins, which can bind ECM macromolecules and the specificity depending on the pairing of one α- and one β-chain24. The interacting of integrin and ECM molecules participate in many signaling pathways of the chondrocytes, and function in cell survival, growth, differentiation and tissue remodeling. Integrin-mediated cell adhesion is known to be crucial for mechanical and structural support of ECM25,26. The disruption of integrin-mediated cell-matrix interactions has remarkable effects on cartilage metabolism and maintenance of cartilage homeostasis24. Deficiency of α2β1 integrin (collagen receptor) was associated with lowered severity of arthritic symptoms in mouse model of osteoarthritic disease27. As a member of collagen receptor dimer, the relative down-regulation of ITGA1 is in line with the expressions of COL1A1, COL1A2, and COL4A1. Previous studies have indicated that integrins can transduce signals from the ECM into the intracellular processes, and participate in regulation of cell differentiation, matrix remodeling, responses to stimulation, and cell survival26,28. The molecular functions of differentially expressed integrin in the pathological mechanism of KBD would warrant further studies.
Focal adhesion is a key ECM-receptor interaction signaling pathway, which integrins also participate in. The ECM binding to integrins signals cells to phosphorylate focal adhesion kinase (FAK), and integrin/FAK interaction has been shown to mediate mechanochemical transduction in chondrocytes29. Focal adhesion distribution was known to be important in osteogenic, adipogenic and chondrogenic guidance30. Dynamics of actin cytoskeleton is dependent on Rho-associated coiled-coil containing protein kinases 1 and 2 (ROCK1 and ROCK2). And Rho/ROCK pathway was reported to regulate the expression of chondrocyte-specific genes Sox9, ACAN and COL2A131,32. Laminins are a family of heterotrimeric ECM proteins33. Previous studies have shown the expressions of specific laminins were differentially regulated during development, adhesion, migration and regeneration34,35,36. In our study, LAMA2 was observed to be up-regulated in KBD group in comparison to OA. These proteins were involved in ECM-receptor interaction signaling pathway, which might suggest the regulative functions in chondrocyte related gene expression.
Our proteomic results showed the expression of NF-κB, GNG5, GNB1, and other guanine nucleotide-binding (G) proteins in Ras and PI3K-Akt signaling pathways altered in KBD. The G-proteins are participated in transmitting extracellular signals to intracellular signal pathways, and evidence indicated G-proteins can affect the pathophysiology of arthritic diseases37. NF-κB is a vital protein in cartilage metabolism. NF-κB-regulated gene products are involved in inflammation and cartilage degradation11,38. Moreover, NF-κB pathway enhances the articular damage by promoting the synthesis of catabolic factors, cartilage inflammation and apoptosis of chondrocyte39,40. RALA is an important protein in chondrocytes, it was reported that the knockdown of RALA during chondrogenesis was noticed to remarkably increase Sox9 protein41. Former research indicated that bone morphogenetic proteins (BMPs) can stimulate both chondrocyte ECM synthesis and chondrocyte differentiation42. Besides, BMPs can prevent apoptosis in chondrocytes via PI3K/AKT-mediated activation of NF-κB43.
The proteomic results also identified several proteins and signal pathways worthy of investigation, such as MAPK, Jak-STAT signaling pathways, phagosomes, ribosomes, and metabolic pathways. It has been reported that PI3K, PKC, and p38-MAPK pathways can regulate the chondrogenic phenotype44. The activation of MAPK signaling pathway was critical during embryonic cartilage and joint development45, and research also indicated that both MAPK and Wnt family participate in chondrogenesis and cartilage development42, which is consistent with our results that several proteins involved in Wnt signaling pathway were in differential expression. The inhibition of STAT is known to transactivate the expression of alkaline phosphatase and type X collagen46,47, and our results also indicated that the NF-κB protein involved in Jak-STAT signaling pathway was up-regulated, and STAT protein down-regulated, which can influence the process of chondrogenesis48. In general, signaling pathways involved in KBD have important regulative roles in the pathogenesis and progression of KBD, and the cellular metabolism are compromised by the production of antianabolic, pro-catabolic and pro-inflammatory factors49.
In conclusion, this research identified the key signal pathways from with proteomics, which were connected by the key proteins, such as LAMA2, integrins, NF-κB, and G proteins. Although the roles of the signaling pathways have not been completely understood, we speculate that these signaling pathways are involved in the pathological mechanisms of KBD. The PPI results showed the key information nodes of different signaling pathway networks, which reflected the intracellular behavior of gene and protein expression stimulated by extracellular mechanical or biochemical information. Thus, the key proteins or pathways are potential targets for pathological mechanisms and therapies. Further investigations are expected to provide new insights into the molecular regulation between ECM and chondrocytes, and contribute to the pathological mechanisms of KBD.
References
Mcalindon, T. E. et al. OARSI guidelines for the non-surgical management of knee osteoarthritis. Osteoarthritis and Cartilage 22, 363–388 (2014).
Zhang, Y. & Jordan, J. M. Epidemiology of osteoarthritis. Clinics in Geriatric Medicine 26, 355–369 (2010).
Pereira, D. et al. The effect of osteoarthritis definition on prevalence and incidence estimates: a systematic review. Osteoarthritis and Cartilage 19, 1270–1285 (2011).
Guo, X. et al. Recent advances in the research of an endemic osteochondropathy in China: Kashin-Beck disease. Osteoarthritis and Cartilage 22, 1774–1783 (2014).
Li, Y. et al. Clinical features of Kashin–Beck disease in adults younger than 50 years of age during a low incidence period: severe elbow and knee lesions. Clinical Rheumatology 32, 317–324 (2013).
NHFPC. China Health and Family Planning Statistical Yearbook, Peking Union Medical College Press: Beijing, pp 272 (2017).
Karin, S., Engelbert, R. H. H., Visser, M. M., Yu, C. & Rien, D. V. Kashin Beck disease: more than just osteoarthrosis. International Orthopaedics 35, 767–776 (2011).
Li, S., Cao, J., Caterson, B. & Hughes, C. E. Proteoglycan metabolism, cell death and Kashin-Beck disease. Glycoconjugate Journal 29, 241–248 (2012).
Duan, C. et al. Comparative analysis of gene expression profiles between primary knee osteoarthritis and an osteoarthritis endemic to Northwestern China, Kashin-Beck disease. Arthritis and Rheumatology 62, 771–780 (2010).
Luo, M. et al. Changes in the metabolism of chondroitin sulfate glycosaminoglycans in articular cartilage from patients with Kashin-Beck disease. Osteoarthritis and Cartilage 22, 986–995 (2014).
Han, J. et al. Role of inflammation in the process of clinical Kashin-Beck disease: latest findings and interpretations. Inflammation Research 64, 853–860 (2015).
Guo, X. Diagnostic, clinical and radiological characteristics of Kashin-Beck disease in Shaanxi Province, PR China. International Orthopaedics 25, 147–150 (2001).
Fu, Q. et al. Radiographic features of hand osteoarthritis in adult Kashin-Beck disease (KBD): the Yongshou KBD study. Osteoarthritis and Cartilage 23, 868–873 (2015).
Ma, W. et al. Proteomic changes in articular cartilage of human endemic osteoarthritis in China. Proteomics 11, 2881–2890 (2011).
Cao, C., Zhang, Y., Wu, S., Younas, M. I. & Guo, X. Association of clinical features of bone and joint lesions between children and parents with Kashin–Beck disease in Northwest China. Clinical Rheumatology 32, 1309–1316 (2013).
Preedy, V. R., Watson, R. R. Western ontario and mcMaster universities osteoarthritis index, Springer, New York, (2010).
Pritzker, K. P. et al. Osteoarthritis cartilage histopathology: grading and staging. Osteoarthritis and Cartilage 14, 13–29 (2006).
Wisniewski, J. R., Zougman, A., Nagaraj, N. & Mann, M. Universal sample preparation method for proteome analysis. Nature Methods 6, 359–362 (2009).
Umlauf, D., Frank, S., Pap, T. & Bertrand, J. Cartilage biology, pathology, and repair. Cellular Molecular Life Sciences 67, 4197–4211 (2010).
Guo X, et al Endemic Disease in China, People’s Medical Publishing House, Beijing (2017).
Wang, W., Guo, X., Chen, J., Xu, P. & Lammi, M. J. Morphology and phenotype expression of types I, II, III, and X collagen and MMP-13 of chondrocytes cultured from articular cartilage of Kashin-Beck disease. Journal of Rheumatology 35, 696–702 (2008).
Gao, Z. et al. Altered aggrecan synthesis and collagen expression profiles in chondrocytes from patients with Kashin-Beck disease and osteoarthritis. Journal of International Medical Research 40, 1325–1334 (2012).
Han, J. et al. Altered expression of chondroitin sulfate structure modifying sulfotransferases in the articular cartilage from adult osteoarthritis and Kashin-Beck disease. Osteoarthritis and Cartilage 25, 1372–1375 (2017).
Knudson, W. & Loeser, R. F. CD44 and integrin matrix receptors participate in cartilage homeostasis. Cellular Molecular Life Sciences 59, 36–44 (2002).
Kim, S. H., Turnbull, J. & Guimond, S. Extracellular matrix and cell signalling: the dynamic cooperation of integrin, proteoglycan and growth factor receptor. Journal of Endocrinology 209, 139–151 (2011).
Loeser, R. F. Integrins and chondrocyte-matrix interactions in articular cartilage. Matrix Biology 39, 11–16 (2014).
Peters, M. A. et al. The loss of α2β1 integrin suppresses joint inflammation and cartilage destruction in mouse models of rheumatoid arthritis. Arthritis and Rheumatology 64, 1359–1368 (2012).
Gao, Y. et al. The ECM-cell interaction of cartilage extracellular matrix on chondrocytes. BioMed Research International 2014, 648459 (2014).
Cheng, K. et al. Effects of low-intensity pulsed ultrasound on integrin-FAK-PI3K/Akt mechanochemical transduction in rabbit osteoarthritis chondrocytes. Ultrasound in Medicine and Biology 40, 1609–1618 (2014).
Mathieu, P. S. & Loboa, E. G. Cytoskeletal and focal adhesion influences on mesenchymal stem cell shape, mechanical properties, and differentiation down osteogenic, adipogenic, and chondrogenic pathways. Tissue Engineering Part B: Reviews 18, 436–444 (2012).
Piltti, J., Bygdell, J., Fernandezechevarria, C., Marcellino, D. & Lammi, M. J. Rho-kinase inhibitor Y-27632 and hypoxia synergistically enhance chondrocytic phenotype and modify S100 protein profiles in human chondrosarcoma cells. Scientific Reports 7, 3708 (2017).
Woods, A., Wang, G. & Beier, F. RhoA/ROCK signaling regulates Sox9 expression and actin organization during chondrogenesis. Journal of Biological Chemistry 280, 11626–11634 (2005).
Aumailley, M. The laminin family. Cell Adhesion Migration 7, 48–55 (2013).
Sun, Y., Wang, T., Toh, W. S. & Pei, M. The role of laminins in cartilaginous tissues: from development to regeneration. European Cells Materials 34, 40–54 (2017).
Foldager, C. B., Toh, W. S., Gomoll, A. H., Olsen, B. R. & Spector, M. Distribution of Basement Membrane Molecules, Laminin and Collagen Type IV, in Normal and Degenerated Cartilage Tissues. Cartilage 5, 123–132 (2014).
Wu, C. et al. Long noncoding RNA expression profile reveals lncRNAs signature associated with extracellular matrix degradation in kashin-beck disease. Scientific Reports 7, 17553 (2017).
Neumann, E., Khawaja, K. & Mullerladner, U. G protein-coupled receptors in rheumatology. Nature Reviews Rheumatology 10, 429–436 (2014).
Montaseri, A., et al IGF-1 and PDGF-bb suppress IL-1β-induced cartilage degradation through down-regulation of NF-κB signaling: involvement of Src/PI-3K/AKT pathway. Plos One 6 (2011).
Rigoglou, S. & Papavassiliou, A. G. The NF-κB signalling pathway in osteoarthritis. The International Journal of Biochemistry Cell Biology 45, 2580–2584 (2013).
Novack, D. V. Role of NF-κB in the skeleton. Cell Research 21, 169–182 (2011).
Karlsen, T. A., Jakobsen, R. B., Mikkelsen, T. S. & Brinchmann, J. E. microRNA-140 targets RALA and regulates chondrogenic differentiation of human mesenchymal stem cells by translational enhancement of SOX9 and ACAN. Stem Cells and Development 23, 290–304 (2014).
Zhang, Y., Pizzute, T. & Pei, M. A review of crosstalk between MAPK and Wnt signals and its impact on cartilage regeneration. Cell Tissue Research 358, 633–649 (2014).
Sugimori, K. et al. BMP-2 prevents apoptosis of the N1511 chondrocytic cell line through PI3K/Akt-mediated NF-κB activation. Journal of Bone and Mineral Metabolism 23, 411–419 (2005).
Rottmar, M. et al. Interference with the contractile machinery of the fibroblastic chondrocyte cytoskeleton induces re-expression of the cartilage phenotype through involvement of PI3K, PKC and MAPKs. Experimental Cell Research 320, 175–187 (2014).
Gunnell, L. M. et al. TAK1 regulates cartilage and joint development via the MAPK and BMP signaling pathways. Journal of Bone and Mineral Metabolism 25, 1784–1797 (2010).
Mikami, Y., Asano, M., Honda, M. J. & Takagi, M. Bone morphogenetic protein 2 and dexamethasone synergistically increase alkaline phosphatase levels through JAK/STAT signaling in C3H10T1/2 cells. Journal of Cellular Physiology 223, 123–133 (2009).
Beneliezer, M., Phillip, M. & Gatyablonski, G. Leptin regulates chondrogenic differentiation in ATDC5 cell-line through JAK/STAT and MAPK pathways. Endocrine 32, 235–244 (2007).
Gueritdavid et al. FOXO3A regulation by miRNA-29a controls chondrogenic differentiation of mesenchymal stem cells and cartilage formation. Stem Cells Development 23, 1195–1205 (2014).
Mobasheri, A. et al. The role of metabolism in the pathogenesis of osteoarthritis. Nature Reviews Rheumatology 13, 302–311 (2017).
Acknowledgements
We thank Dr. Ruiyu Liu and Dr. Weizhuo Wang from the Second Affiliated Hospital of Xian Jiaotong University, Dr. Chao Xu from Linyou County Hospital and all the staff from Linyou County Endemic Disease Control Center for their support and cooperation in the collection of cartilage specimens. And we thank our lab fellows Yan Ran, Huan Deng, Yiqiao Hua, and Abebe Belete Woldetsadik for their generous help in this experiment. This study was supported by National Natural Science Foundation of China (81872567, 81402639) and Shenzhen Science and Technology Project (JCYJ20170816100755047). The study sponsors did not involve in the study design, data collection, analysis or interpretation, or in the writing of the manuscript, neither did they affect the decision to submit the manuscript for publication.
Author information
Authors and Affiliations
Contributions
All authors participated in drafting the article and critically modifying the important content of knowledge, with all authors endorsing the final version. Mr. Lei had full access to all the data in the study and takes responsibility for the integrity of the data and accuracy of the data analysis. Study conception and design: Han, Guo. Acquisition of data: Lei, Han, Gao. Analysis and interpretation of data: Lei, Han, Lammi, Wang, Lv, Deng. Drafting the article or revising it critically for important intellectual content: Lei, Han, Lammi, Lv, Deng, Feyissa. Final approval of the version of the article to be published: Lei, Feyissa, Wang, Lv, Deng, Gao, Guo, Han, Lammi.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made. The images or other third party material in this article are included in the article’s Creative Commons license, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons license and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this license, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Lei, J., Amhare, A.F., Wang, L. et al. Proteomic analysis of knee cartilage reveals potential signaling pathways in pathological mechanism of Kashin-Beck disease compared with osteoarthritis. Sci Rep 10, 6824 (2020). https://doi.org/10.1038/s41598-020-63932-6
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41598-020-63932-6
This article is cited by
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.