Abstract
Over the last decade, an increasing number of infections with livestock-associated methicillin-resistant Staphylococcus aureus of clonal complex 398 (LA-MRSA CC398) in persons without contact to livestock has been registered in Denmark. These infections have been suggested to be the result of repeated spillover of random isolates from livestock into the community. However, other studies also found emerging sub-lineages spreading among humans. Based on genome-wide SNPs and genome-wide association studies (GWAS), we assessed the population structure and genomic content of Danish LA-MRSA CC398 isolates from healthcare-associated infections from 2014 to 2016 (n = 73) and compared these to isolates from pigs in Denmark from 2014 (n = 183). Phylogenetic analyses showed that most human isolates were closely related to and scattered among pig isolates showing that the majority of healthcare-associated infections are the result of repeated spillover from pig farms, even though cases of human-to-human transmission also were identified. GWAS revealed frequent loss of antimicrobial resistance genes and acquisition of human-specific virulence genes in the human isolates showing adaptation in response to changes in selective pressures in different host environments, which over time could lead to the emergence of LA-MRSA CC398 lineages more adapted to human colonization and transmission.
Similar content being viewed by others
Introduction
Human infections with livestock-associated methicillin-resistant Staphylococcus aureus of clonal complex 398 (LA-MRSA CC398) have increased dramatically over the last decade1,2 and accounted for 16% of all MRSA infections in Denmark in 20163. Since 2012, the Danish MRSA guidelines have recommended screening of patients with livestock contact at hospital admission to limit the introduction of MRSA into healthcare institutions in Denmark4. However, an increasing number of people colonized or infected with LA-MRSA CC398 have no contact to livestock1. As opposed to livestock-onset (LO) MRSA infections, where a direct link to livestock is recorded, such cases of MRSA infection are categorized as either healthcare-onset (HO) if the positive culture was obtained ≥48 hours after admission to a healthcare facility, or community-onset (CO) if the positive culture was obtained from patients in the primary healthcare sector or within the first 48 hours of admission without having had contact to the healthcare institutions within the last 12 months. Furthermore, infections are categorized as healthcare-associated community-onset (HACO) if the patients have been admitted to a healthcare institution within the last 12 months before onset in the community. Because most of these non-LO cases have no risk factors for MRSA carriage (e.g., livestock contact), they may inadvertently introduce the bacteria into hospitals and nursing homes. This increases the risk of nosocomial transmission of LA-MRSA CC398 to other patients5,6,7, including immuno-compromised and elderly people where the bacteria can cause severe disease and occasionally death2,8,9,10.
In Denmark, the number of non-LO infections with LA-MRSA CC398 has been increasing in parallel with the number of LO infections1. This suggests a scenario where the general population is consistently exposed to a random spillover of bacteria from livestock, as described in earlier studies from Denmark11 and other European countries12,13,14. However, recent studies also report the emergence of sub-lineages spreading independently of the livestock reservoir15,16. Such lineages could be better adapted to the human host, which increases the risk of spread into healthcare institutions via non-LO cases with the present guidelines. Phylogenetic analysis based on whole-genome sequencing (WGS) is highly sensitive with regard to identifying emerging sub-lineages17,18 and has recently enabled the identification of three predominant lineages of LA-MRSA CC398 (termed L1, L2 and L3) in the Danish pig production system11. Furthermore, WGS can be used to detect genetic differences between isolates present in different host environments, such as the gain or loss of host-specific genes17,18,19,20,21,22.
The aims of this study were to: (i) determine whether the introduction of LA-MRSA CC398 into healthcare institutions is due to repeated spillover of random isolates from livestock or to circulation of sub-lineages with an increased capacity for human colonization and transmission; and (ii) investigate relevant bacterial genomes for signatures of adaptation to the human host.
Results
Temporal trends of human LA-MRSA CC398 infections in Denmark, 2007–2016
The number of LA-MRSA CC398 infections in Denmark increased from five in 2007 to 220 in 2016. Whereas the majority (64.2% [674/1050]) of cases from this period could be categorized as LO, 35.8% (376/1050) of the cases had no apparent contact to livestock. The latter were further differentiated into HO (2.6% [27/1050 cases]), HACO (7.9%, 83/1050 cases) and CO (the remaining 25.3% [266/1050] of cases). The annual numbers of CO cases increased in parallel with the prevalence of LA-MRSA CC398 in pig farms (Fig. 1), while the annual numbers of HO and HACO cases did not exceed seven and 21, respectively.
Trends in human CC398 LA-MRSA infections of different onset compared to its prevalence in livestock. The numbers of infections from 2007 to 2016 with hospital (HO, red line, and HACO, blue line), community (CO, green line) and livestock (LO, black line) are shown together with the prevalence on Danish pig farms (bars).
Healthcare-associated LA-MRSA CC398 infections in Denmark, 2014–2016
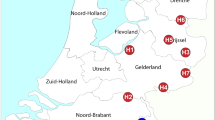
In the 3-year period from January 2014 through December 2016, 73 infections were categorized as either HO (n = 15) or HACO (n = 58). The isolates were obtained from skin and soft tissue (n = 49), nose and mouth, including tonsils and sinuses (n = 8), respiratory sites, including tracheal aspirates, sputum and induced sputum (n = 6), blood and cerebrospinal fluid (n = 4), ear or eye (n = 1), and other clinical sites, including indwelling devices and unspecified origin (n = 5). The median age of the patients was 66 years (range, 0–97 years) and the female-to-male ratio was 0.87. The geographic distribution of human LA-MRSA CC398 isolates from healthcare-associated infections did not differ significantly from the distribution of pig isolates (Table 1).
Phylogenetic analysis of LA-MRSA CC398 isolates from pigs and people with healthcare-associated infections
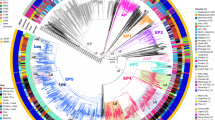
A total of 73 isolates from healthcare associated human infections were compared to the 183 isolates from pig farms in a phylogenetic analysis. The maximum-likelihood phylogeny was established based on 3,245 variable sites after removal of 873 sites falling into recombinant regions. The phylogenetic analysis showed that human isolates were scattered among pig isolates, and only a few clusters of two to three human isolates were observed. The majority (78% [57/73] of isolates from patients with healthcare-associated infections was most closely related to a pig isolate with a median distance of 36 SNPs (range 3–58 SNPs). Of the remaining 16 human isolates, eight formed four pairs with a SNP distance of ≤2 while the last eight were most closely related to other human isolates but with a median distance of 16 SNPs (range 9–73 SNPs) between them (Fig. 2). All four pairs of isolates with ≤2 SNPs had identical regional origin, and in all four cases potential epidemiological links could be determined (Table 2). In three pairs, both patients had stayed in the same healthcare unit at the same time (pairs I-III), while both patients in the last pair shared the same home care unit (pair IV). Of note, two isolates from two distinct pairs (II and IV) contained the human immune evasion cluster (IEC) carried on the ΦSa3 prophage (Table 2). Whereas pairs I and III have similar isolation dates and nosocomial transmission seems plausible, the two remaining pairs were isolated more than one year apart indicating that different transmission pathways might be involved.
Phylogenetic tree of the 256 isolates from humans and pigs. Rooted maximum-likelihood tree of the derived CC398 livestock clade containing 73 isolates from people with healthcare-associated infections (red) and 183 isolates from Danish pig farms (grey). The four pairs of closely related human isolates are indicated by roman numbers and the three major lineages (L1–L3) within the Danish pig production are highlighted. The tree is based on 3,245 variable sites after filtering for recombination tracts (823 sites). Bootstrap values above 90% are illustrated by filled black circles at the nodes. The scalebar indicates substitutions per site.
Comparison of the proportions of human and pig isolates clustering in the three most prevalent lineages of LA-MRSA CC398 in pigs (L1-L3), showed that human isolates were underrepresented in L2 (4% vs. 16%, p = 0.007), while no differences were observed in the two most prevalent lineages L1 and L3. The proportion of isolates clustering outside L1-L3 (i.e. the remainder) was higher (26% vs. 10%, p = 0.003) among human isolates than among isolates from pigs.
Host-associated SNPs
None of the variable sites from the core genome was significantly associated with either human or pig origin after correction for multiple testing.
Host association of predefined antimicrobial resistance and virulence genes
The gene content of human and pig isolates was first compared using a set of predefined resistance and virulence genes. The genes were selected based on existing databases and evidence from previous studies on LA-MRSA CC39811,18. The results showed that human isolates had a significantly lower prevalence of the antimicrobial resistance genes erm(B), lnu(B), tet(K) and czrC conferring resistance to macrolides, lincosamides, tetracycline and cadmium/zinc, respectively (Table 3), after correction for multiple testing. Similar trends of lower prevalence of resistance genes in isolates from humans with significant associations prior to correction for multiple testing were also found in lineage L3 and the remainder (Fig. 3). In contrast, there was an opposite trend for a higher prevalence of the human variants of the IEC genes, scn and sak, in human isolates belonging to lineage L3, although the difference was non-significant after correction for multiple testing (Table 3). Moreover, IEC was found in one, four, and two isolates in L1, L3, and the remainder, respectively, including scn alone or in combination with other IEC genes, which indicates several independent acquisition events. In contrast, a unique IEC element containing scn, chp, sak and sep was found in a distinct cluster of six pig isolates within L1 suggesting that the element was acquired in a single event (Fig. 2).
Presence of selected genes in LA-MRSA CC398 isolates from pigs and people with healthcare-associated infection. The paired bars show the prevalence of selected genes in isolates from humans (solid) and pigs (light) for each lineage (L1–L3), the remainder (R), and in total. The genes czrC, erm(B), lnu(B), and tet(K) confer resistance to cadmium/zinc, macrolide, lincosamide and tetracycline, respectively and IEC enables S. aureus to evade the human immune system. *Indicate significant p values as obtained from the analysis of predefined sets of genes and corrected for multiple testing. *P ≤ 0.05; **P ≤ 0.01; ***P ≤ 0.001.
Analysis of the presence/absence of the different genes in human isolates and their most closely related pig isolates showed that 100% (12/12), 24% (17/72), 52% (11/21) and 100% (7/7) of the human isolates lacking erm(B), lnu(B), tet(K) and czrC, respectively, were most closely related to a pig isolate that carried the corresponding gene, suggesting that they were lost during spread from the pig farms to the healthcare setting. In contrast, human isolates carrying these genes were always most closely related to a pig isolate also carrying the genes, suggesting that none of the human isolates have acquired the genes (Table 4). On the other hand, IEC (as represented by scn) was most likely acquired during or after transfer to the human host as the most closely related pig isolates of all seven positive human isolates were negative for the element.
Analysis of accessory genes
The pan-genome of all isolates as obtained from Prokka and Roary contained 4,019 genes. Of these, 4,008 could be confirmed by mapping of raw sequence reads to their reference sequences using Mykrobe predictor (0.27% false positives, 11/4,019). This re-mapping also led to an increase in the number of genes in the strict core-genome (genes present in all samples) from 2,029 to 2,302. Furthermore, 16.0% (642/4,019) of the genes were subsequently present in more samples than identified by Roary, while 3.6% (143/4,019) of the genes were found in fewer isolates.
After filtering the genes using a 1% frequency cut-off (i.e. present in more than two and less than 254 out of the 256 samples), 837 genes remained to be tested for association with either of the two host reservoirs. The results showed significant associations to pig isolates for five genes after correction for multiple testing, including the tetracycline resistance gene tet(K) together with two other genes (pre and repN) from the S0385 plasmid pS0385–1 (GenBank Accession Number NC_017334) containing tet(K) (Table 3). However, two genes (SAPIG_RS05110 and SAPIG_RS15395 on the S0385 chromosome [GenBank accession number NC_017333]) could not be confirmed by read mapping as they showed ambiguous mapping patterns with low numbers or lack of sequence reads that correlated with sequencing batches. This suggests that the significant results of these genes were due to a sequencing batch effect rather than traces of host adaptation. Lineage effects in GWAS can be circumvented by analysing associations in each lineage separately. This was specifically performed by analysing each of the three lineages L1-L3 and the remainder separately, with the result of only a single gene (SAPIG_RS05110, see above) in L3 being significantly associated with pigs after correction for multiple testing. This gene was also found associated with pigs in the analysis of all isolates (Table 3) but could not be confirmed by read mapping (see above).
Phylogeny-based association analysis
The analysis of the accessory gene presence/absence data with lineage correction using treeWAS resulted in a significant terminal score for only one gene (SAPIG_RS05110) (Table 3), which corroborates the non-phylogeny-based analyses above. No other associations were found in any of the scores. The phylogeny-based analysis of core genome-wide SNPs using treeWAS showed no association of any SNP with either of the hosts.
k-mer-based analysis of raw sequencing reads using pyseer showed that k-mers with the lowest p values mapped to the proline-rich repetitive region of the S. aureus clumping factor B (clfB) gene in the ST398 reference genome S0385 (GenBank accession number AM990992), followed by several other genes including other so called microbial surface components recognizing adhesive matrix molecules (MSCRAMMs) with repetitive regions such as the three serine-aspartate repeat protein-encoding genes, sdrC, sdrE, and sdrH (Supplementary Fig. S1). However, validation by aligning assembled gene sequences as well as raw read mapping both produced inconclusive results likely due to low local sequence depth caused by a GC-bias and/or the repetitive nature of these regions. Alignment of the 96 high-coverage amplicons of this region showed no association of repeat size, phylogenetic clustering or specific variable sites to neither host, and thus the k-mer findings could not be confirmed.
Discussion
This study shows that human LA-MRSA CC398 isolates from patients with healthcare-associated infections have their origin in pigs and that they are repeatedly introduced into healthcare facilities. The geographical distribution of healthcare-associated infections was similar to the distribution of LA-MRSA CC398 in the pig population, supporting that introduction of LA-MRSA CC398 into the healthcare system is due to spillover from nearby pig farms via human-to-human13,23 or environmental transmission chains24,25,26. This is in line with an earlier Danish study, which showed that most LA-MRSA CC398 isolates from Danish infections were more closely related to Danish pig isolates than to isolates of international origin2, and with a Dutch study where people without livestock contact were shown to carry variants known from the local livestock population12.
We found similar proportions of L1 and L3 isolates in pig farms and people with healthcare-associated infections, suggesting that they have the same capacity for spread into healthcare facilities. However, isolates from human infections were underrepresented in L2 and overrepresented among the remainder. An overrepresentation of particular lineages in LA-MRSA CC398 isolates from humans has been observed before15,27 and this can be indicative for lineages better adapted to colonize and infect humans. Indeed, the remainder are known to have a lower prevalence of antimicrobial resistance genes than the three predominant lineages in Danish pigs11. The lower fitness costs due to absence of these resistance genes may provide an advantage in the human environment in absence of the selection pressure exerted by the corresponding antimicrobial compounds. However, L2 does not have more resistance genes than L1 and L311, but still seems to cause fewer infections in humans, indicating that other factors may play a role in determination of the frequency of human infection.
Comparison of LA-MRSA CC398 genomes from pigs and humans revealed a lower prevalence of predefined antimicrobial resistance genes in human isolates. All of these genes are encoded on mobile genetic elements (MGEs) including plasmids for erm(B), lnu(B) and tet(K)28,29,30 and the highly dynamic staphylococcal cassette chromosome mec (SCCmec) element for czrC and in most cases also tet(K)31. The lower prevalence of these genes in humans could be due to transmission of isolates that already lack these genes or to gain and loss of MGEs during transmission from pig farms to the human environment. Our analysis supports the latter scenario, with frequent loss of antimicrobial resistance genes and gain of IEC in human isolates. The lost genes confer resistance to antimicrobials commonly used in the pig production. Thus, the genes are likely lost because they do not provide a fitness advantage in absence of the corresponding antimicrobial compounds in the human hosts. Likewise, LA-MRSA CC398 is generally considered as poorly adapted for transmission among humans, in particular because of the absence of the ΦSa3 prophage carrying IEC18,32. The scn gene is always present in IEC33 and encodes the staphylococcal chemotaxis inhibitor protein (SCIN), which plays an important role in the bacterium’s ability to evade the innate immune response in humans34. Our analysis indicates that IEC and scn have been acquired by several human strains. Taken together, these results show that LA-MRSA CC398 is capable of repeated re-adaptation to the human environment by acquisition and loss of genes carried on MGEs.
In order to confirm the absence of genomic changes other than those related to MGEs, a highly sensitive k-mer-based GWAS was performed. This analysis showed highly significant associations of genomic regions with the hosts (Supplementary Fig. S1), but these associations could not be confirmed in the subsequent analysis of sequenced amplicons of these regions. This might be due to the regions showing sequence patterns known to cause sequencing biases such as palindromes, inverted repeats, long homopolymers or other repetitive regions35,36,37, highlighting the importance of uniform sequencing data and the need to confirm positive results when using such highly sensitive bioinformatic methods as k-mer-based GWAS from short read sequencing data.
Four pairs of closely related human isolates were identified in the phylogenetic analysis and subsequent epidemiological investigations showed that in all cases, nosocomial transmissions may have occurred, although there is differences in the gene content of some of the isolates and the large timespan between the isolation dates in two of the four pairs may suggest different transmission pathways. These findings are consistent with a previously reported outbreak of LA-MRSA CC398 in an intensive care unit10, and together they provide strong evidence of human-to-human transmission of LA-MRSA CC398 within the Danish healthcare system. However, whether the transmissions were directly between humans or via surfaces or items remains unclear, and the phylogenetic analysis showed that three of the four pairs occurred in different pig-associated lineages indicating that nosocomial transmission of LA-MRSA CC398 is rare and sporadic.
In accordance with the here substantiated scenario of a repeated spillover of random LA-MRSA CC398 isolates from livestock to the community, the number of CO infections from 2007 to 2016 increased in parallel with the prevalence in Danish pig farms. On the other hand, the numbers of HO and HACO infections remained low in the same period, indicating that LA-MRSA CC398 is successfully kept out of healthcare institutions thanks to effective measures such as the Danish screening program during admission to healthcare institutions and a high standard of infection control measures in general.
The present study is limited by the relatively low number of isolates from healthcare-related infections, which represent only a small proportion of those caused by LA-MRSA CC398 in the community. However, the collection represents an unbiased nationwide sample of isolates from cases where strong epidemiological data ascertains the absence of a link to livestock. Furthermore, the focus on isolates from human infections might lead to an underestimation of nosocomial transmission since transmission from and to asymptomatic carriers, including e.g. healthcare workers who might have indirect pig contact, is not detected.
In conclusion, the present study showed that the vast majority of healthcare-associated infections with LA-MRSA CC398 in humans can be explained by repeated spillover of random isolates from pig farms. This suggests that a reduction of LA-MRSA CC398 in pigs would be mirrored in a reduction of infections in high-risk patients in hospitals and other healthcare units. Furthermore, the present study identified at least two healthcare-associated transmission events and showed that the host transition of LA-MRSA CC398 from pigs back to humans was accompanied by repeated, independent loss of antimicrobial resistance genes and occasional gain of the ΦSa3 prophage carrying IEC genes. Over time and with increased occurrence, this process of parallel evolution could lead to re-adaptation of LA-MRSA CC398 to the human host and eventually the emergence and spread of lineages more adapted (and potentially more virulent) to humans. A continued surveillance of LA-MRSA CC398 in both pigs and humans is therefore essential for early detection of and action against such potentially emerging lineages.
Methods
Isolate collection and classification
All primary LA-MRSA CC398 isolates recovered from Danish patients who had a healthcare-associated (i.e. HO or HACO) infection during a 3-year period from January 2014 through December 2016 were included in this study and subjected to whole-genome sequencing as described below. The LA-MRSA CC398 isolates were selected based on the national MRSA registry and strain repository at Statens Serum Institut in Copenhagen. All data collection and analyses were in accordance with guidelines and regulations as approved by the Danish Data Protection Agency (protocol number 2001-14-0021). The same protocol approves for use of Danish surveillance data, hence obtaining informed consent from all subjects was not necessary. All isolates were typed at Statens Serum Institut as part of the national MRSA surveillance program4. For each patient, the infection was defined as LO, CO, HO, or HACO through review of the medical records, using the criteria described above. To describe temporal trends of LA-MRSA CC398 in Denmark, all primary LA-MRSA CC398 isolates recovered from human infections from 01 January 2007 through 31 December 2016 were used.
Whole-genome sequencing and analyses
A schematic overview over the methods used in this study can be found in Supplementary Fig. S2. The human LA-MRSA CC398 isolates identified in this study were whole-genome sequenced on an Illumina MiSeq (n = 27) with 2 × 251 bp paired-end reads or Illumina NextSeq. 550 (n = 46) with 2 × 151 bp paired-end reads after library preparation using the Nextera XT DNA Library Preparation Kit (Illumina, San Diego, USA). The sequences were compared to 183 LA-MRSA CC398 genomes from pigs representing all available LA-MRSA CC398 isolates from a nationwide survey in Danish breeding farms (46 isolates) and production farms (137 isolates) in 201411. Single nucleotide polymorphisms (SNPs) were called and filtered using NASP version 1.038 and a maximum-likelihood phylogenetic tree was calculated in IQ-TREE version 1.6.139 using default settings with a GTR substitution model after removal of recombinant regions, as described previously11. The tree was rooted according to Sieber et al.11 and the three predominant lineages of LA-MRSA CC398 in Danish pigs were determined according to Sieber et al.11. The genetic distance between isolates was calculated as the number of sites that differ between each pair of sequences in the detected core genome.
To determine whether a genotype in human isolates was the result of transmission of a pig isolate with the same genotype or whether the genotype evolved during this transmission, the most probable scenario for the human genotype was inferred by comparison of each human isolate to its most closely related pig isolate.
Genome-wide association analyses
Gene presence was determined using Mykrobe predictor version 0.4.340 with reference graphs generated either from a predefined set of genes containing all entries from the ResFinder41 and VirulenceFinder42 databases (http://www.cge.dtu.dk, accessed 01 October 2018) and the czrC gene encoding resistance to cadmium and zinc (GenBank accession no. KF593809), or from the pan-genome of all isolates as determined by Prokka43 and Roary44 using SPAdes-assembled45 genomes and default settings. Genes classified as present by Mykrobe predictor were further filtered for median depth (≥5×).
A total of 3,245 high quality SNPs were identified in the core-genome using NASP (see above) and analysed for association with either of the host groups using Fisher’s exact tests.
Phylogenetic tree-based genome-wide association analyses were performed in the R-package treeWAS46 for the presence/absence of genes and SNPs and using the python software pyseer47 for a k-mer-based analysis to account for genomic differences other than presence/absence of detected genes or SNPs. The latter was performed on k-mers produced from raw sequencing reads with a minimum per k-mer count of eight per sample using a linear mixed effects model with a similarity matrix inferred from the maximum-likelihood phylogenetic tree. The k was chosen as the median of the range of ks which the k-mer generator distributed with pyseer uses by default (k = 54). Significant k-mer hits were annotated by mapping to the S. aureus CC398 reference chromosome S038548.
PCR and sequencing of amplicons
The clfB region with the lowest detected p value was chosen as a representative to be investigated by targeted sequencing of PCR amplicons in 96 randomly sampled isolates. The proline-rich region of the clfB gene was amplified using KAPA HiFi HotStart ReadyMixPCR Kit in 25 μL PCR reactions (Kapa Biosystems, Wilmington, USA) with forward (5′-CCCAAATGACTCTAACCT-3′) and reverse (5′-GCTCTTATCTCCTGTTTCT-3′) primers designed from the S. aureus reference chromosome S038548 using CLC Genomic Workbench Version 12.0 (QIAGEN, Aarhus, Denmark), and the following PCR conditions: 95 °C for 3 min, 25 cycles of 95 °C for 30 sec, 58 °C for 30 sec, 72 °C for 2 min, and final extension at 72 °C for 7 min. The obtained amplicons were depleted of excess primer using Beckman Coulter AMPure XP beads and libraries were prepared with the Nextera XT DNA Library Preparation Kit (Illumina, San Diego, USA). After normalization and pooling, libraries were sequenced on an Illumina MiSeq instrument with 2 × 251 bp paired-end reads. The resulting sequences were assembled using SPAdes45 with “careful” option and contigs were filtered for a minimum average depth of 500× before a consensus sequence for each isolate was generated in Geneious version 11.1.5 (Biomatters Ltd., Auckland, New Zealand). The resulting sequences of the clfB region were aligned using MAFFT version 1.3.749 as implemented in Geneious (Biomatters Ltd.) to identify length variations and variable sites in the proline-rich repeat region.
Statistical analyses
Statistical analyses were performed in R version 3.5.050. p values were obtained from Fisher’s exact tests and corrected for multiple testing using false discovery rate (FDR) where appropriate.
Data availability
The whole-genome sequence data generated in this study have been submitted to the European Nucleotide Archive under BioProject accession number PRJEB25608. Datasets analysed and scripts used during the current study are available in the Sourceforge repository, https://sourceforge.net/projects/mrsa-cc398-haco-vs-pigs/files.
References
Larsen, J. et al. Meticillin-resistant Staphylococcus aureus CC398 is an increasing cause of disease in people with no livestock contact in Denmark, 1999 to 2011. Eurosurveillance 20, https://doi.org/10.2807/1560-7917.ES.2015.20.37.30021 (2015).
Larsen, J. et al. Emergence of livestock-associated methicillin-resistant Staphylococcus aureus bloodstream infections in Denmark. Clin Infect Dis 65, 1072–1076, https://doi.org/10.1093/cid/cix504 (2017).
DANMAP. Danish Integrated Antimicrobial Resistance Monitoring and Research Programme. DANMAP 2016 - Use of antimicrobial agents and occurrence of antimicrobial resistance in bacteria from food animals, food and humans in Denmark, https://www.danmap.org/-/media/arkiv/projekt-sites/danmap/danmap-reports/danmap-2016/danmap_2016_web.pdf (2019).
Danish Health and Medicines Authority. Vejledning om forebyggelse af spredning af MRSA [Guideline on the prevention of spread of MRSA]. Danish Health and Medicines Authority (2016).
van Cleef, B. A. et al. Livestock-associated Methicillin-Resistant Staphylococcus aureus in Humans, Europe. Emerging Infectious Disease journal 17, 502–505, https://doi.org/10.3201/eid1703.101036 (2011).
Witte, W., Strommenger, B., Stanek, C. & Cuny, C. Methicillin-resistant Staphylococcus aureus ST398 in Humans and Animals, Central Europe. Emerging Infectious Diseases 13, 255–258, https://doi.org/10.3201/eid1302.060924 (2007).
Wulf, M. et al. First outbreak of methicillin-resistant Staphylococcus aureus ST398 in a Dutch hospital, June 2007. Eurosurveillance 13, https://doi.org/10.2807/ese.13.09.08051 (2008).
van der Mee-Marquet, N. L. et al. Emergence of a novel subpopulation of CC398 Staphylococcus aureus infecting animals is a serious hazard for humans. Frontiers in Microbiology 5, 652, https://doi.org/10.3389/fmicb.2014.00652 (2014).
Smith, T. C. & Wardyn, S. E. Human Infections with Staphylococcus aureus CC398. Current Environmental Health Reports 2, 41–51, https://doi.org/10.1007/s40572-014-0034-8 (2015).
Nielsen, R. et al. Fatal Septicemia Linked to Transmission of MRSA Clonal Complex 398 in Hospital and Nursing Home, Denmark. Emerging Infectious Diseases 22, 900–902, https://doi.org/10.3201/eid2205.151835 (2016).
Sieber, R. N. et al. Drivers and Dynamics of Methicillin-Resistant Livestock-Associated Staphylococcus aureus CC398 in Pigs and Humans in Denmark. mBio 9, e02142–18, https://doi.org/10.1128/mBio.02142-18 (2018).
Lekkerkerk, W. et al. What Is the Origin of Livestock-Associated Methicillin-Resistant Staphylococcus aureus Clonal Complex 398 Isolates from Humans without Livestock Contact? An Epidemiological and Genetic Analysis. Journal of Clinical Microbiology 53, 1836–1841, https://doi.org/10.1128/JCM.02702-14 (2015).
Köck, R. et al. Livestock-associated methicillin-resistant Staphylococcus aureus (MRSA) as causes of human infection and colonization in Germany. PloS one 8, e55040, https://doi.org/10.1371/journal.pone.0055040 (2013).
Cuny, C., Wieler, L. H. & Witte, W. Livestock-Associated MRSA: The Impact on Humans. Antibiotics (Basel, Switzerland) 4, 521–543, https://doi.org/10.3390/antibiotics4040521 (2015).
Bosch, T. et al. Changing characteristics of livestock-associated meticillin-resistant Staphylococcus aureus isolated from humans - emergence of a subclade transmitted without livestock exposure, the Netherlands, 2003 to 2014. Eurosurveillance 21, 22–31, https://doi.org/10.2807/1560-7917.ES.2016.21.21.30236 (2016).
Lekkerkerk, W. et al. Emergence of MRSA of unknown origin in the Netherlands. Clinical Microbiology and Infection 18, 656–661, https://doi.org/10.1111/j.1469-0691.2011.03662.x (2012).
Lowder, B. V. et al. Recent human-to-poultry host jump, adaptation, and pandemic spread of Staphylococcus aureus. Proceedings of the National Academy of Sciences of the United States of America 106, 19545–19550, https://doi.org/10.1073/pnas.0909285106 (2009).
Price, L. B. et al. Staphylococcus aureus CC398: Host Adaptation and Emergence of Methicillin Resistance in Livestock. mBio 3, e00305–11, https://doi.org/10.1128/mBio.00305-11 (2012).
Fitzgerald, R. J. & Holden, M. Genomics of Natural Populations of Staphylococcus aureus. Annual Review of Microbiology 70, 459–478, https://doi.org/10.1146/annurev-micro-102215-095547 (2016).
Larsen, J. et al. Evidence for Human Adaptation and Foodborne Transmission of Livestock-Associated Methicillin-Resistant Staphylococcus aureus. Clinical Infectious Diseases 63, 1349–1352, https://doi.org/10.1093/cid/ciw532 (2016).
Verkade, E. & Kluytmans, J. Livestock-associated Staphylococcus aureus CC398: Animal reservoirs and human infections. Infection, genetics and evolution: journal of molecular epidemiology and evolutionary genetics in infectious diseases 21, 523–530, https://doi.org/10.1016/j.meegid.2013.02.013 (2014).
Lilje, B. et al. Whole-genome sequencing of bloodstream Staphylococcus aureus isolates does not distinguish bacteraemia from endocarditis. Microbial genomics 3, e000138 (2017).
McCarthy, A. J. et al. Staphylococcus aureus CC398 clade associated with human-to-human transmission. Applied and Environmental Microbiology 78, 8845–8848, https://doi.org/10.1099/mgen.0.000138 (2012).
Schulz, J. et al. Longitudinal study of the contamination of air and of soil surfaces in the vicinity of pig barns by livestock-associated methicillin-resistant Staphylococcus aureus. Applied and environmental microbiology 78, 5666–5671, https://doi.org/10.1128/AEM.00550-12 (2012).
Beresin, G. A., Wright, M. J., Rice, G. E. & Jagai, J. S. Swine exposure and methicillin-resistant Staphylococcus aureus infection among hospitalized patients with skin and soft tissue infections in Illinois: A ZIP code-level analysis. Environmental Research 159, 46–60, https://doi.org/10.1016/j.envres.2017.07.037 (2017).
Carrel, M., Schweizer, M. L., Sarrazin, M. V., Smith, T. C. & Perencevich, E. N. Residential proximity to large numbers of swine in feeding operations is associated with increased risk of methicillin-resistant Staphylococcus aureus colonization at time of hospital admission in rural Iowa veterans. Infection control and hospital epidemiology 35, 190–193, https://doi.org/10.1086/674860 (2014).
Wulf, M., Verduin, C., van Nes, A., Huijsdens, X. & Voss, A. Infection and colonization with methicillin resistant Staphylococcus aureus ST398 versus other MRSA in an area with a high density of pig farms. European Journal of Clinical Microbiology & Infectious Diseases 31, 61–65, https://doi.org/10.1007/s10096-011-1269-z (2012).
Lyon, B. & Skurray, R. Antimicrobial resistance of Staphylococcus aureus: genetic basis. Microbiological reviews 51, 88–134; PMID: 3031442 (1987).
Lozano, C. et al. Genetic environment and location of the lnu(A) and lnu(B) genes in methicillin-resistant Staphylococcus aureus and other staphylococci of animal and human origin. Journal of Antimicrobial Chemotherapy 67, 2804–2808, https://doi.org/10.1093/jac/dks320 (2012).
Guay, G. G., Khan, S. A. & Rothstein, D. M. The tet(K) Gene of Plasmid pT181 of Staphylococcus aureus Encodes an Efflux Protein That Contains 14 Transmembrane Helices. Plasmid 30, 163–166, https://doi.org/10.1006/plas.1993.1045 (1993).
Li, S. et al. Novel types of staphylococcal cassette chromosome mec elements identified in clonal complex 398 methicillin-resistant Staphylococcus aureus strains. Antimicrobial agents and chemotherapy 55, 3046–3050, https://doi.org/10.1128/AAC.01475-10 (2011).
Foster, T. J., Geoghegan, J. A., Ganesh, V. K. & Höök, M. Adhesion, invasion and evasion: the many functions of the surface proteins of Staphylococcus aureus. Nature Reviews Microbiology 12, 49–62, https://doi.org/10.1038/nrmicro3161 (2014).
van Wamel, W. J., Rooijakkers, S. H., Ruyken, M., van Kessel, K. P. & van Strijp, J. A. The innate immune modulators staphylococcal complement inhibitor and chemotaxis inhibitory protein of Staphylococcus aureus are located on beta-hemolysin-converting bacteriophages. Journal of bacteriology 188, 1310–1315, https://doi.org/10.1128/JB.188.4.1310-1315.2006 (2006).
Rooijakkers, S. H. et al. Immune evasion by a staphylococcal complement inhibitor that acts on C3 convertases. Nature Immunology 6, 920–927, https://doi.org/10.1038/ni1235 (2005).
Ross, M. G. et al. Characterizing and measuring bias in sequence data. Genome Biology 14, R51, https://doi.org/10.1186/gb-2013-14-5-r51 (2013).
Aird, D. et al. Analyzing and minimizing PCR amplification bias in Illumina sequencing libraries. Genome Biology 12, R18, https://doi.org/10.1186/gb-2011-12-2-r18 (2011).
den Hoecke, S., Verhelst, J. & Saelens, X. Illumina MiSeq sequencing disfavours a sequence motif in the GFP reporter gene. Scientific Reports 6, 26314, https://doi.org/10.1038/srep26314 (2016).
Sahl, J. W. et al. NASP: an accurate, rapid method for the identification of SNPs in WGS datasets that supports flexible input and output formats. Microbial genomics 2, e000074, https://doi.org/10.1099/mgen.0.000074 (2016).
Nguyen, L.-T., Schmidt, H. A., von Haeseler, A. & Minh, B. IQ-TREE: A Fast and Effective Stochastic Algorithm for Estimating Maximum-Likelihood Phylogenies. Molecular Biology and Evolution 32, 268–274, https://doi.org/10.1093/molbev/msu300 (2015).
Bradley, P. et al. Rapid antibiotic-resistance predictions from genome sequence data for Staphylococcus aureus and Mycobacterium tuberculosis. Nature communications 6, 10063, https://doi.org/10.1038/ncomms10063 (2015).
Zankari, E. et al. Identification of acquired antimicrobial resistance genes. The Journal of antimicrobial chemotherapy 67, 2640–2644, https://doi.org/10.1093/jac/dks261 (2012).
Joensen, K. G. et al. Real-time whole-genome sequencing for routine typing, surveillance, and outbreak detection of verotoxigenic Escherichia coli. Journal of clinical microbiology 52, 1501–1510, https://doi.org/10.1128/JCM.03617-13 (2014).
Seemann, T. Prokka: rapid prokaryotic genome annotation. Bioinformatics 30, 2068–2069, https://doi.org/10.1093/bioinformatics/btu153 (2014).
Page, A. J. et al. Roary: rapid large-scale prokaryote pan genome analysis. Bioinformatics 31, 3691–3693, https://doi.org/10.1093/bioinformatics/btv421 (2015).
Bankevich, A. et al. SPAdes: a new genome assembly algorithm and its applications to single-cell sequencing. Journal of computational biology: a journal of computational molecular cell biology 19, 455–477, https://doi.org/10.1089/cmb.2012.0021 (2012).
Collins, C. & Didelot, X. A phylogenetic method to perform genome-wide association studies in microbes that accounts for population structure and recombination. PLOS Computational Biology 14, e1005958, https://doi.org/10.1371/journal.pcbi.1005958 (2018).
Lees, J., Galardini, M., Bentley, S. D., Weiser, J. N. & Corander, J. pyseer: a comprehensive tool for microbial pangenome-wide association studies. Bioinformatics 34, 4310–4312, https://doi.org/10.1093/bioinformatics/bty539 (2018).
Schijffelen, M. J., Boel, E. C., Strijp, J. A. & Fluit, A. C. Whole genome analysis of a livestock-associated methicillin-resistant Staphylococcus aureus ST398 isolate from a case of human endocarditis. BMC Genomics 11, 376, https://doi.org/10.1186/1471-2164-11-376 (2010).
Katoh, K. & andley, D. MAFFT Multiple Sequence Alignment Software Version 7: Improvements in Performance and Usability. Molecular Biology and Evolution 30, 772–780, https://doi.org/10.1093/molbev/mst010 (2013).
R Core Team R: A language and environment for statistical computing. R Foundation for Statistical Computing, Vienna, Austria, https://www.R-project.org (2018).
Acknowledgements
The authors would like to thank the technical staff of the Danish reference laboratory for Staphylococci at Statens Serum Institut who performed initial typing of the isolates. This work was supported by the Ministry of Environment and Food of Denmark through The Danish Agrifish Agency (33010-NIFA-14-612 to R.N.S., A.R.L., C.H.M., R.L.S., and J.L.) and the National Institute of Allergy and Infectious Diseases, National Institutes of Health (1R01AI101371-01A1 to A.R.L., R.L.S., J.L., and M.S.). The funders had no role in study design, data collection and interpretation, or the decision to submit the work for publication.
Author information
Authors and Affiliations
Contributions
R.N.S., R.L.S., A.R.L., J.L. and M.S. designed the study and R.N.S. and M.S. prepared the initial manuscript. All authors contributed to the subsequent editorial revisions. T.R.U. and C.H.M. made epidemiological research. R.N.S. and J.L. performed epidemiological and statistical analyses. S.I. performed laboratory analyses. R.N.S. and M.S. conducted whole-genome sequencing and bioinformatic analysis.
Corresponding authors
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made. The images or other third party material in this article are included in the article’s Creative Commons license, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons license and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this license, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Sieber, R.N., Larsen, A.R., Urth, T.R. et al. Genome investigations show host adaptation and transmission of LA-MRSA CC398 from pigs into Danish healthcare institutions. Sci Rep 9, 18655 (2019). https://doi.org/10.1038/s41598-019-55086-x
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41598-019-55086-x
This article is cited by
-
Time-calibrated phylogenetic and chromosomal mobilome analyses of Staphylococcus aureus CC398 reveal geographical and host-related evolution
Nature Communications (2024)
-
Transmission of livestock-associated methicillin-resistant Staphylococcus aureus between animals, environment, and humans in the farm
Environmental Science and Pollution Research (2023)
-
Shared antibiotic resistance and virulence genes in Staphylococcus aureus from diverse animal hosts
Scientific Reports (2022)
-
Population genomics of Group B Streptococcus reveals the genetics of neonatal disease onset and meningeal invasion
Nature Communications (2022)
-
Genome-wide association studies reveal candidate genes associated to bacteraemia caused by ST93-IV CA-MRSA
BMC Genomics (2021)
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.