Abstract
In the endgame of global polio eradication, serosurveillance is essential to monitor each country’s vulnerability to poliomyelitis outbreaks. Previously, we developed pseudovirus poliovirus (PV) neutralization test (pPNT) with type 1, 2, and 3 PV pseudovirus (PVpv), which possess a luciferase-encoding PV replicon in the capsids of wild-type strains (PVpv[WT]), showing that pPNT with type 2 and 3 PVpv(WT) but not type 1 shows high correlation with the conventional PV neutralization test (cPNT) performed with vaccine strains. Here, we analyse the antigenicity of PVpv(WT) and PVpv with capsid proteins of Sabin vaccine strains (PVpv[Sabin]) in human serum. Type 2 and 3 PVpv(WT) and PVpv(Sabin) show similar antigenicity in the analysed set of human sera in contrast to type 1 PVpv. The levels of PVpv(Sabin) infection (%), including about 70% of PVpv infection (%) measured in the presence of human serum diluted to the cPNT titre, serve as the optimal threshold values for pPNT (5% for type 1 and 2, 10% for type 3) to show high correlation with cPNT results. Our results suggest that pPNT with PVpv(Sabin) could serve as an alternative to cPNT and provide a rationale for pPNT threshold values.
Similar content being viewed by others
Introduction
Poliovirus (PV) is a small non-enveloped virus with a positive-sense single-stranded RNA genome of about 7500 nt belonging to the genus Enterovirus, the family Picornaviridae. After feco-oral infection, PV invades the central nervous system primarily via viremia, showing a positive correlation with PV paralytic rate1 and destroying motor neurons to cause poliomyelitis2,3. Immunization with live oral PV vaccine (OPV) or inactivated PV vaccine (IPV) induces production of anti-PV antibody in serum, which prevents PV central nervous system invasion and poliomyelitis.
Serosurveillance is performed to monitor anti-PV neutralization antibody titre in serum of potentially susceptible populations and to evaluate a country’s potential vulnerability a poliomyelitis outbreak. A conventional PV neutralization test (cPNT) using cell culture and infectious PV strains, which are usually attenuated vaccine strains, is currently performed to measure the anti-PV neutralization antibody4. Serosurveillance in Japan has been performed in prefectural laboratories every 2 to 3 years since 1974 (for about 1,100 to 1,800 individuals in 6 to 8 prefectures) in a wide age range (age of 0 to >40 year) to monitor vulnerability5. Serosurveillance is also important in Japan after the introduction of Sabin strain-based IPV (sIPV) after 20126. sIPV induces similar persistence of anti-PV antibody to conventional wild-type-stain-based IPV when used as a booster in adults with history of OPV administration7. Recent reports suggest rapid declines of the antibody titre after sIPV administration8,9,10. The persistence of anti-PV antibody in children vaccinated with sIPV without OPV remains is poorly understood.
In the endgame of polio eradication, a high level of PV biosecurity is more important than ever. The third edition of the WHO Global Action Plan to minimize poliovirus facility-associated risk after type-specific eradication of wild polioviruses and sequential cessation of oral polio vaccine use (GAP III)11 was adopted by the WHO in May 2015 before indigenous wild type 2 PV was declared eradicated. GAPIII raises the biosafety level for type 2 PV strains (Annex 2 and 3 in GAP III), corresponding to BSL3 plus additional conditions and restricts the use of type 2 strains in biological tests in laboratories with conventional biosecurity levels.
One of the major challenges in implementing GAP III is the sustainability of the serosurveillance system under restricted use of infectious PV strains. After implementation, cPNT could not be performed in laboratories with conventional biosecurity levels. We previously produced a virus-free PV pseudovirus (PVpv)12 that could serve as an alternative to infectious PV. PVpv possesses a luciferase-encoding PV replicon in the capsid and shows single cycle infection in susceptible cells (adsorption/uncoating/replication) without producing an infectious virus. PVpv has been used for quantitative analyses of antiviral effects13 and anti-type 2 PV neutralization activity in stool in the context of infection14.
Neutralization tests with pseudotyped viruses have been developed for viruses under the control of high biosecurity levels (e.g. Ebola virus, SARS-CoV, lyssaviruses, Nipah virus, highly pathogenic avian influenza A viruses)15,16,17,18,19,20. In a previous study, we developed a pseudovirus PV neutralization test (pPNT) using PVpv with the capsids of wild-type strains21. Following our report, other groups have also found good correlations between pPNT and cPNT22,23.
pPNT is largely characterized by three factors: (1) capsid protein type (e.g. capsid proteins of wild-type strains or vaccine strains), (2) titre or amount of PVpv, and (3) threshold values of PVpv infection to determine the neutralizing antibody titre. The capsid protein type is critical for type 1 PV, exemplified by significant antigenic differences between the type 1 Sabin strain and the parental Mahoney strain by the VP3-T60K mutation24,25, and by an emergence of the type 1 wild-type strain with significantly low antigenicity26. Absolute titre or infectious units of PVpv could be determined using focus assay12. The luciferase signal of PVpv-infected cells might be useful to determine the relative titre22. In cPNT, neutralization titre is determined by an endpoint reading for the cytopathic effect on infected cells, so it is an all-or-none reading. In pPNT, neutralization titre is determined by reading the PVpv infection, which represents a percentage of luciferase signal in the infected cells, which is not an all-or-none reading. Therefore, threshold values are required for pPNT to define apparent “neutralization” of PVpv. Threshold values of PVpv infection have been inductively estimated to give the best fit to cPNT results (2.5% to 25% of PVpv infection)21,22. Variation of reported threshold values might suggest robustness of pPNT. Seropositive rates determined at a wide range of threshold values were substantially unaffected (e.g., seropositive rates for type 2 were 92% to 95% determined in a range of threshold values of 2.5% to 10%)21. The rationale to determine the threshold values remains to be provided.
Here, we analyse the antigenicity of PVpv with capsid proteins of wild-type strains (PVpv[WT]) or of Sabin strains (PVpv[Sabin]), in a set of human sera obtained from healthy volunteers (ages of 1 to 76, total 131 samples). In addition, we provide a rationale for the threshold values for pPNT based on the distribution of PVpv infection at cPNT titre.
Results and Discussion
Development of PVpv with Sabin strain capsid proteins
In a previous study, we produced type 1, 2, and 3 PVpv, which possess a luciferase-encoding PV replicon based on the Mahoney strain in the capsids of wild-type strains (type 1 Mahoney, type 2 MEF-1, and type 3 Saukett A in PV1 pv[WT], PV2 pv[WT], and PV3pv[WT], respectively)12,21. Here, we constructed PV capsid expression vectors that express the capsid proteins of type 1, 2, and 3 Sabin strains. We also produced type 1, 2 and 3 PVpv, which possess a luciferase-encoding PV replicon based on the Mahoney strain in the capsids of type 1, 2, and 3 Sabin strains, respectively (PV1 pv[Sabin], PV2 pv[Sabin], and PV3pv[Sabin], respectively) (Fig. 1A). We obtained type 1, 2, and 3 PVpv(Sabin) with high titres (2.5 × 107, 1.2 × 107 IU, and 6.0 × 106 IU per mL, respectively), which were about 10-fold lower than PVpv(WT)12,21. Next, we optimized the amounts of PVpv(Sabin) for pPNT with standard antisera (Fig. 1B). Specific and similar neutralization profiles were observed for PVpv(Sabin) at a range of the examined amounts (200, 400, or 800 IU)21. We used 400 IU of PVpv(Sabin) in pPNT.
Optimization of the PVpv(Sabin) amounts in pPNT. (A) Schematic view of PV capsid, replicon, and PVpv used in this study. (B) Neutralization curves of PVpv(Sabin) (200, 400, or 800 IU) with standard anti-PV sera (128 U per 50 μL) are shown. PVpv infection in the absence of human serum is taken as 100%.
Evaluation of PVpv infection in the presence of human serum diluted to the cPNT titre
Previously, we performed pPNT with PVpv(WT) for 131 human serum samples21. We determined the threshold values by maximizing the fitness of the seropositive rates (population with neutralization titre of at least 8). However, we could not directly compare the results because cPNT was performed with Sabin strains. To analyse the direct correlation between cPNT and pPNT, we analysed the distribution of PVpv infection (%) in the presence of human serum diluted to the cPNT titre (Fig. 2). The PVpv(Sabin) infection showed a sharp peak around 0%, with medians of 2.0%, 2.1%, and 4.6%, for type 1, 2, and 3 PVpv(Sabin), respectively. The percentages of the serum samples that showed less than 5% PVpv infection at the cPNT titre were 71%, 71%, and 54% for type 1, 2, and 3 PVpv(Sabin), respectively. The percentages of the serum samples that showed less than 10% PVpv infection at the cPNT titre were 88%, 84%, and 72% for type 1, 2, and 3 PVpv(Sabin), respectively. A broader peak width for type 3 than types 1 and 2 might reflect intrinsic weak antigenicity of type 3 PV in humans vaccinated with OPV (Fig. 3). The profile of the curves of type 2 and 3 PVpv(WT) were like type 2 and 3 PVpv(Sabin)21. In contrast, the curve for PV1pv(WT) was significantly different from PV1pv(Sabin), and it showed a broad peak width (median of 15%). These results indicated substantial suppression of PVpv infection in the presence of human serum diluted to the cPNT titre and significant antigenic differences for type 1 PVpv.
Comparison of neutralization profile of PVpv (WT) and PVpv(Sabin) in human serum. Upper panel: An example of a PVpv neutralization curve with a human serum sample with a cPNT titre of 32. PVpv infection (%) at the cPNT titre is shown. PVpv infection in the absence of human serum is taken as 100%. Lower panel: Distribution of PVpv infection (%) at the cPNT titre. Results of two independent experiments with a set of human sera (total 131 samples) are shown.
Determination of the threshold values for pPNT. (A) Upper panels: Comparison of cPNT and pPNT. Distribution of neutralizing antibody titre in human serum samples (n = 131) determined by cPNT or pPNT with a range of threshold values are shown. Optimal conditions are highlighted in magenta. Lower panels: scatter plot of neutralizing antibody titre determined by cPNT and pPNT. Threshold values for pPNT are 5% for type 1 and 2 or 10% for type 3. The numbers of serum samples at the corresponding spots are visualized by the size of circles. The regression line (red), 95% confidence interval (green), and 95% prediction interval (blue) are shown. (B) Distributions of neutralizing antibody titre obtained by cPNT and pPNT in different age groups. Threshold values for pPNT are 5% for type 1 and 2 or 10% for type 3.
Threshold values for PVpv(Sabin)
Next, threshold values for PVpv(Sabin) were analysed using the seropositive rate and the degree of correlation to compare to cPNT (Fig. 3A). For type 1 and 2 PVpv(Sabin), the seropositive rates were almost equal at a range of examined threshold values (5% to 15% of threshold values) and within 10% of variation from cPNT. PV3pv(Sabin) showed relatively low seropositive rate (61%) with a threshold value of 5% (Fig. 2). The highest degree of correlation between cPNT and pPNT in terms of residual sum of square was observed for threshold values of 5%. This suggested that threshold values of 5% might be optimal for pPNT with type 1 and 2 PVpv(Sabin). For PV3pv(Sabin), a threshold value of 10% seemed to give an optimal correlation. This suggests that the levels of PVpv infection, under which about 70% of the distribution was included around the peak, serves as the optimal threshold for pPNT (Fig. 2). With threshold values of 5% for type 1 and 2 PVpv(Sabin) and 10% for PV3pv(Sabin), pPNT with PVpv(Sabin) showed high correlation with cPNT (R2 of 0.92, 0.83, and 0.79, respectively). For type 2 and 3, the results of PVpv(Sabin) were like PVpv(WT) (R2 of 0.81 and 0.77, respectively). For type 1, the correlation degree was drastically improved with PVpv(Sabin) compared to PVpv(WT) (R2 of 0.92 vs. 0.59), and the correlation between cPNT and pPNT was consistently observed among different age groups with PVpv(Sabin) in contrast to PVpv(WT) (Fig. 3B)21. For type 2 and 3 PVpv(Sabin), the correlation was also observed among the age groups, as previously observed for PVpv(WT)21. One of the critical points in PV serosurveillance is in the estimation of seropositive rate. Accurate determination of overall and age-specific seropositive rates by pPNT supports the potential of pPNT as an alternative to cPNT along with the observed high correlation.
Reproducibility of pPNT
We analysed the reproducibility of pPNT (Fig. 4). First, we tested the reproducibility of pPNT with PVpv(Sabin) using standard monkey anti-PV sera (128 U per 50 μL). In twenty independent experiments, median values of PVpv(Sabin) infection at the cPNT titres of standard antisera appeared like the threshold values determined for each type (medians of 3.2%, 5.1%, and 9.7% for type 1, 2, and 3 PVpv[Sabin] respectively). In 19/20 of the experiments, the pPNT titres of standard sera were determined as 64 or 128 (Fig. 4A). We also analysed lot-to-lot differences of PVpv(Sabin) with the standard monkey anti-PV sera (Fig. 4B). Two different lots of PVpv(Sabin) showed similar neutralization curves with the antisera. Next, we tested the reproducibility with a set of human sera (total 131 samples) in three independent experiments (Fig. 5, Supplementary Data 1). We found consistent seropositive rates and distribution of neutralization titre among the experiments. These results suggest high reproducibility of pPNT and robustness of established conditions.
Reproducibility of pPNT with standard monkey anti-PV sera. (A) Test with standard monkey anti-PV sera (128 U per 50 μL). PVpv infection in the absence of standard serum is taken as 100%. Results of twenty independent experiments are shown. Lower panel: Distribution of pPNT titre for standard anti-PV sera. Threshold values for pPNT are 5% for type 1 and 2 or 10% for type 3. (B) Test with different lots of PVpv(Sabin). Neutralization curve of two different lots of PVpv(Sabin) with standard monkey anti-PV sera is shown.
In summary, we clarified antigenic differences for type 1 PV strains using pPNT, and we provided a rationale for determining the threshold values for pPNT. With high reproducibility and safety without using infectious viruses, pPNT with PVpv(Sabin) could serve as an alternative to cPNT in serosurveillance in the endgame of the polio eradication program (Fig. 6).
Methods
Cells, viruses, and human sera
RD cells (human rhabdomyosarcoma cells) and HEK293 cells (human embryonic kidney cells) were cultured as monolayers in Dulbecco’s modified Eagle medium (DMEM) supplemented with 10% foetal calf serum (FCS). Vero cells (African green monkey kidney cells) were cultured as monolayers in Eagle’s Minimum Essential Medium (EMEM) supplemented with 0.11% bovine serum albumin (BSA) (fraction V, Sigma). RD cells were used for PV and pPNT titration. Vero cells were used for cPNT. HEK293 cells were used to produce PVpv. Type 1, 2, and 3 PVpv(WT) possess a luciferase-encoding PV replicon based on the Mahoney strain in capsid proteins derived from PV1(Mahoney), PV2(MEF-1), and PV3(Saukett A), respectively12,21. Human sera were collected from healthy volunteers (ages of 1 to 76) under informed consent from themselves or a parent or legal guardian for minors. Experiments performed here were approved by the Committee for Ethical Regulation of the National Institute of Infectious Diseases, Japan. All experiments were performed in accordance with relevant guidelines and regulations.
General methods of molecular cloning
Escherichia coli strain XL10gold (Stratagene) was used to prepare plasmids. Ligation of DNA fragments was performed using an In-Fusion HD Cloning Kit (Clontech). PCR was performed using KOD Plus DNA polymerase (Toyobo). Reverse transcription-PCR (RT-PCR) was performed using a ReverTra -Plus- kit (Toyobo). DNA sequencing was performed using a BigDye Terminator v3.0 cycle sequencing ready reaction kit (Applied Biosystems) and analysed with a 3130 genetic analyser (Applied Biosystems).
Construction of expression vectors for the capsid proteins of type 1, 2, or 3 Sabin strains
To construct expression vectors of capsid proteins of type 1, 2, and 3 Sabin strains (GenBank: AY184219, AY184220, and AY184221, respectively), the enhanced green fluorescence protein (EGFP) gene was fused to capsid-protein-coding regions of type 1, 2, and 3 Sabin strains using PCR before being inserted into pHEK293 Ultra Expression Vector I (TaKaRa) digested by SmaI and SalI. EGFP coding regions were amplified using PCR with pIRES2-EGFP (Clontech) as the template and the following primer set (coding regions of EGFP with a linker in the primers are underlined): 5′TGCTTAAGCCTCCCCACCATGGGAGCTCTGAGCAAGGGCGAGGAG3′ 5′GTAGGTGGTCAGGCCCTTCTTGTACAGCTCGTCC3′. The PV capsid-protein-coding region was amplified using RT-PCR with viral genomic RNA as the template and the following primer sets (coding regions of the capsid proteins in the primers are underlined):
Type 1 Sabin:
5′GGCCTGACCACCTACGGTGCTCAGGTTTCATCACAGAAAGTGGGC3′
5′TGCCTGCAGGTCGACTTAATATGTGGTCAGATCCTTGGTGGAGAG3′
Type 2 Sabin:
5′GGCCTGACCACCTACGGCGCCCAAGTTTCATCACAGAAAGTTGG3′
5′TGCCTGCAGGTCGACTTAATAAGTCGTTAATCCCTTTTCTGGTAG3′
Type 3 Sabin:
5′GGCCTGACCACCTACGGAGCTCAAGTATCATCCCAAAAAGTAGGC3′
5′TGCCTGCAGGTCGACTTAATATGTGGTCAAACCTTTCTCAGATAA3′
Preparation of PVpv
PVpv was prepared as previously reported with modifications12. Briefly, a six-well plate (Falcon) with a 10% confluent monolayer of HEK293 cells was transfected with 2 μg of corresponding PV capsid-expression vectors per well using Lipofectamine 3000 reagent (Invitrogen). The cells were incubated at 35 °C in 2 ml DMEM supplemented with 10% FCS per well for 24 h. RNA transcripts of PV replicons were obtained using a RiboMAX large-scale RNA production system – T7 kit (Promega) with DraI-linearized DNA of pPV-Fluc mc, which encodes a PV replicon based on PV1(Mahoney) that has firefly luciferase gene instead of the capsid-coding region as the template. RNA transcripts were transfected into the monolayer of HEK293 cells transiently expressing PV capsid proteins at 24 h post-transfection using Lipofectamine MessengerMAX reagent (Invitrogen). Cells were harvested at 24 h post-transfection of the RNA transcripts when most of the cells show CPE. The cells were then stored at −20 °C. The infectious unit of the PVpv stock solution was determined by counting the number of HEp-2c cells infected with PVpv 8 h post-infection (p.i.), which were stained using the 2C protein by indirect immunofluorescence as described previously12.
cPNT
cPNT was performed according to the standard procedure recommended by the WHO with modifications4 as described previously21. Briefly, a 2-fold dilution series of human sera was prepared with EMEM supplemented with 0.11% BSA resulting in 1/4 to 1/1024 dilutions. 50 μL of diluted sera or EMEM supplemented with 0.11% BSA was added to three 96-well plates. 50 μL of type 1, 2, or 3 Sabin strains (100 50% cell culture infective dose (CCID50)) was added to each well of the plates (one plate for each serotype of PV with a total of 3 plates), and incubated at 37 °C 3 h. After incubation, 100 μL of Vero cell suspension in EMEM supplemented with 0.11% BSA (1.0 to 2.0 × 105 cells) was added to each well of the plates, and the plates were incubated at 37 °C for 7 days. Neutralizing antibody titre of the serum was determined as 50% endpoints of the serum determined by the presence or absence of CPE in the cells.
pPNT
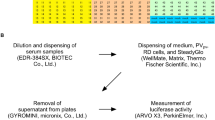
pPNT was performed as reported previously with modifications21. 25 μL of human sera samples and standard anti-PV sera (128 U per 50 μL, positive control) were diluted with DMEM supplemented with 1% FCS by 4-fold (1/4 dilution). A 2-fold dilution series was made, resulting in 1/4 to 1/1024 dilutions. 5 μL of diluted sera or DMEM supplemented with 1% FCS (mock treatment) was added to three 384-well plates (Greiner Bio-One, 781080). Next, 5 μL of type 1, 2, or 3 PVpv solution (400 IU) was added to each well of the plates (one plate for each serotype of PVpv for a total of 3 plates). The plates were centrifuged (700 × g, 10 sec) (PlateSpin, KUBOTA). After centrifugation, plates were incubated at 4 °C overnight. After incubation, 20 μL of RD cell suspension in DMEM supplemented with 5% FCS (5.0 × 103 cells) was added to each well of the plates. The plates were incubated at 37 °C for 7 h. Luciferase signal of the infected cells was measured at 7 h p.i. with Steady-Glo Luciferase Assay System (Promega) using a 2030 ARVO X luminometer (PerkinElmer) according to the manufacturer’s instructions. PVpv infection was calculated as a percentage of luciferase signal of the infected cells. The luciferase signal in mock-treated cells was taken as 100%. Neutralizing antibody titre was determined as a reciprocal number of the highest dilution of the serum that suppressed PVpv infection to less than 5%.
Data Availability
Raw data sets not included in the manuscript or in the supplementary information are available from the corresponding author upon request.
References
Bodian, D. Viremia in experimental poliomyelitis. I. General aspects of infection after intravascular inoculation with strains of high and of low invasiveness. Am. J. Hyg. 60, 339–357 (1954).
Bodian, D. Histopathologic basis of clinical findings in poliomyelitis. Am. J. Med. 6, 563–578 (1949).
Couderc, T. et al. Molecular pathogenesis of neural lesions induced by poliovirus type 1. J. Gen. Virol. 70, 2907–2918 (1989).
World Health Organization. Manual of laboratory methods for potency testing of vaccines used in the WHO Expanded Programme on Immunization. WHO publication no. WHO/BLG/95.1. World Health Organization, Geneva (1995).
Iwai, M. et al. Evaluation of a two-dose administration of live oral poliovirus vaccine for wild and virulent vaccine-derived poliovirus type 1, 2, 3 strains in Japan. Scand. J. Infect. Dis. 40, 247–253, https://doi.org/10.1080/00365540701596003 (2008).
Shimizu, H. Development and introduction of inactivated poliovirus vaccines derived from Sabin strains in Japan. Vaccine 34, 1975–1985, https://doi.org/10.1016/j.vaccine.2014.11.015 (2016).
Resik, S. et al. Decay of Sabin inactivated poliovirus vaccine (IPV)-boosted poliovirus antibodies. Trials Vaccinol. 4, 71–74, https://doi.org/10.1016/j.trivac.2015.08.001 (2015).
Hotta, C., Ogawa, T. & Shirasawa, H. Surveillance of immunity acquired from poliovirus immunization including vaccination with the Sabin strain-derived inactivated vaccine. Hum. Vaccin. Immunother., https://doi.org/10.1080/21645515.2019.1572408 (2019).
Nakayama, T., Suga, S., Okada, K. & Okabe, N. Persistence of Antibodies against Diphtheria, Tetanus, Pertussis, and Poliovirus Types I, II, and III Following Immunization with DTaP Combined with Inactivated Wild-Type Polio Vaccine (DTaP-wIPV). Jpn. J. Infect. Dis. 72, 49–52, https://doi.org/10.7883/yoken.JJID.2018.314 (2019).
Satoh, H. et al. Polio vaccination coverage and seroprevalence of poliovirus antibodies after the introduction of inactivated poliovirus vaccines for routine immunization in Japan. Vaccine 37, 1964–1971, https://doi.org/10.1016/j.vaccine.2019.02.034 (2019).
WHO http://www.polioeradication.org/Portals/0/Document/Resources/PostEradication/GAPIII_2014.pdf.
Arita, M., Nagata, N., Sata, T., Miyamura, T. & Shimizu, H. Quantitative analysis of poliomyelitis-like paralysis in mice induced by a poliovirus replicon. J. Gen. Virol. 87, 3317–3327, https://doi.org/10.1099/vir.0.82172-0 (2006).
Arita, M. & Bigay, J. Poliovirus Evolution toward Independence from the Phosphatidylinositol-4 Kinase III beta/Oxysterol-Binding Protein Family I Pathway. ACS Infect. Dis. 5, 962–973, https://doi.org/10.1021/acsinfecdis.9b00038 (2019).
Brickley, E. B. et al. Intestinal Immune Responses to Type 2 Oral Polio Vaccine (OPV) Challenge in Infants Previously Immunized With Bivalent OPV and Either High-Dose or Standard Inactivated Polio Vaccine. J. Infect. Dis. 217, 371–380, https://doi.org/10.1093/infdis/jix556 (2018).
Rimoin, A. W. et al. Ebola Virus Neutralizing Antibodies Detectable in Survivors of theYambuku, Zaire Outbreak 40 Years after Infection. J. Infect. Dis. 217, 223–231, https://doi.org/10.1093/infdis/jix584 (2018).
Fukushi, S. et al. Evaluation of a novel vesicular stomatitis virus pseudotype-based assay for detection of neutralizing antibody responses to SARS-CoV. J. Med. Virol. 78, 1509–1512, https://doi.org/10.1002/jmv.20732 (2006).
Han, D. P., Kim, H. G., Kim, Y. B., Poon, L. L. & Cho, M. W. Development of a safe neutralization assay for SARS-CoV and characterization of S-glycoprotein. Virology 326, 140–149, https://doi.org/10.1016/j.virol.2004.05.017, S0042682204003678 [pii] (2004).
Wright, E. et al. Investigating antibody neutralization of lyssaviruses using lentiviral pseudotypes: a cross-species comparison. J. Gen. Virol. 89, 2204-2213, https://doi.org/10.1099/vir.0.2008/000349-0 (2008).
Tamin, A. et al. Development of a neutralization assay for Nipah virus using pseudotype particles. J. Virol. Methods 160, 1–6, https://doi.org/10.1016/j.jviromet.2009.02.025 (2009).
Wang, W. et al. Establishment of retroviral pseudotypes with influenza hemagglutinins from H1, H3, and H5 subtypes for sensitive and specific detection of neutralizing antibodies. J. Virol. Methods 153, 111–119, https://doi.org/10.1016/j.jviromet.2008.07.015 (2008).
Arita, M., Iwai, M., Wakita, T. & Shimizu, H. Development of a poliovirus neutralization test with poliovirus pseudovirus for measurement of neutralizing antibody titer in human serum. Clin. Vaccine Immunol. 18, 1889–1894, https://doi.org/10.1128/CVI.05225-11 (2011).
Liu, S. et al. A safe and reliable neutralization assay based on pseudovirus to measure neutralizing antibody titer against poliovirus. J. Med. Virol. 89, 2075–2083, https://doi.org/10.1002/jmv.24909 (2017).
Jiang, Z. et al. A simple and safe antibody neutralization assay based on polio pseudoviruses. Hum Vaccin Immunother 15, 349–357, https://doi.org/10.1080/21645515.2018.1526553 (2019).
Diamond, D. C. et al. Antigenic variation and resistance to neutralization in poliovirus type 1. Science 229, 1090–1093 (1985).
Blondel, B. et al. Mutations conferring resistance to neutralization with monoclonal antibodies in type 1 poliovirus can be located outside or inside the antibody-binding site. J. Virol. 57, 81–90 (1986).
Drexler, J. F. et al. Robustness against serum neutralization of a poliovirus type 1 from a lethal epidemic of poliomyelitis in the Republic of Congo in 2010. Proc. Natl. Acad. Sci. USA 111, 12889–12894, https://doi.org/10.1073/pnas.1323502111 (2014).
Acknowledgements
We are grateful to Yuzuru Aoi for excellent technical assistance, and to Hiroyuki Shimizu and Masamichi Muramatsu for kind support. This study was supported in part by AMED under Grant Number 19fk0108085j0001 to M.A.
Author information
Authors and Affiliations
Contributions
M.A. conceived the project. M.A. designed the study. M.I. performed cPNT with Sabin strains. M.A. performed pPNT. M.A. wrote the manuscript. M.I. commented on the manuscript.
Corresponding author
Ethics declarations
Competing Interests
The authors declare no competing interests.
Additional information
Publisher’s note: Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made. The images or other third party material in this article are included in the article’s Creative Commons license, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons license and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this license, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Arita, M., Iwai-Itamochi, M. Evaluation of antigenic differences between wild and Sabin vaccine strains of poliovirus using the pseudovirus neutralization test. Sci Rep 9, 11970 (2019). https://doi.org/10.1038/s41598-019-48534-1
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41598-019-48534-1
This article is cited by
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.