Abstract
This study evaluated the impact of mechanically stimulated saliva on initial bacterial colonization. Interaction between oral bacteria and both unstimulated and stimulated saliva was examined in vitro by laying labeled bacteria over SDS-PAGE-separated salivary proteins. The effects of chewing on in vivo biofilm, microbial composition, and spatial arrangement were examined in two human volunteers using an intraoral stent containing retrievable enamel chips. In vitro experiments showed that bacterial binding to proteins from stimulated saliva was lower than that to proteins from unstimulated saliva. Lack of binding activity was noted with Streptococcus mutans and Lactobacillus casei. Human Oral Microbe Identification Microarray (HOMIM) analyses revealed a consistent chewing-related increase in the binding of Streptococcus anginosus and Streptococcus gordonii. Immunofluorescence microscopy demonstrated the presence of multi-species colonies and cells bearing different serotypes of the coaggregation-mediating streptococcal cell-surface receptor polysaccharides (RPS). Differences in bacterial colonization were noted between the two volunteers, while the type 4 RPS-reactive serotype was absent in one volunteer. Cells reacting with antibody against Rothia or Haemophilus were prominent in the early biofilm. While analysis of the data obtained demonstrated inter-individual variations in both in vitro and in vivo bacterial binding patterns, stimulating saliva with multiple orosensory stimuli may modulate oral bacterial colonization of tooth surfaces.
Similar content being viewed by others
Introduction
Supragingival biofilm formation is widely recognized as a step-wise process in which acquired enamel pellicle is a specific binding target of early-colonizing bacteria; late-colonizing bacteria are recruited in part by cell-cell recognition called coaggregation and coadhesion1. Nascent supragingival biofilms can be detected as early as 2 hours (molecular approach) or 4 hours (microscopy) on clean enamel surfaces2,3. The daily oral hygiene regimen of toothbrushing creates a cycle of plaque removal and re-colonization. Therefore, it is important to understand the mechanism of dental biofilm formation at its initial stage as well as to create efficient plaque removal strategies. Recently, Hertel et al. used fluorescent in situ hybridization to investigate initial oral biofilm colonization patterns of selected oral bacteria from children whose DMFT scores varied4. No statistically significant differences in distribution patterns of the adherent bacteria were seen between or among the DMFT groups, although the low-DMFT group showed the least amount of Streptococcus mutans. Human saliva contains a spectrum of proteins with antimicrobial properties, among which are immunoglobulin IgA, enzymes (e.g., lysozyme, lactoferrin, and peroxidase), mucin glycoproteins, agglutinins, proline-rich proteins, and histatins. Saliva’s impact on oral bacteria has been studied from the perspective of antimicrobial activities, anti-coaggregation properties, point of adhesion, and as a carbon source5. The acquired enamel pellicle is derived mainly from salivary proteins and glycoproteins6,7,8 and mediates initial bacterial colonization on the tooth surface. Cheaib et al. demonstrated that modulation of composition in salivary proteins and glycoproteins during pellicle formation influenced subsequent adhesion of early colonizers to enamel surfaces9. Key receptor polysaccharides (RPS) that are important for coaggregations of streptococci and actinomyces have been previously elucidated10. Ito et al. demonstrated that a lectin which recognizes the Gal1-3GalNAc moiety, one of the known RPSs, may function as a potential anti-S. mutans agent11. It has been demonstrated that salivary protein composition differs between stimulated and unstimulated saliva12. The type of stimulus, such as tastants, has been known to alter salivary protein composition13,14,15. One proposed mechanism is alteration of the glandular contributions to whole-mouth saliva12,16. A caveat is that other factors may influence salivary secretions and composition, including age and inter-individual variations17,18,19,20.
An ex vivo bacterial overlay technique has been used to probe the binding patterns of oral bacteria to salivary proteins21,22. Previous studies have been limited in using either mechanically stimulated saliva or unstimulated saliva from a single subject, but not both types of saliva in comparison or from multiple subjects. Although some studies have utilized glandular saliva samples in which the contribution rate differs between stimulated and unstimulated, reports using whole saliva have been limited23,24. In addition, studies have investigated primary human dental plaque colonizers individually in vitro25. The present study focused on the impact of stimulated saliva on bacterial colonization in the oral cavity.
Our central hypothesis was that stimulating salivary secretion may alter the colonization of oral bacteria through changes in its protein composition, and this alteration can be observed through an in vitro bacterial overlay technique as well as in biofilm developed on enamel chips carried in an intraoral stent. We have previously reported a profile of microbial coaggregation partnerships during the initial phase of dental biofilm development26. Here we report the effect of chewing-gum-stimulated saliva on interactions between salivary proteins and bacterial binding properties. Unstimulated and stimulated whole saliva samples were collected from five individuals and analyzed with in vitro bacterial overlay. In addition, we conducted an in situ biofilm growth study using two individuals, comparing microflora on the enamel chip with or without gum chewing to provide a proof-of-concept that food-stimulated saliva influences bacterial binding in the human oral cavity.
Results
Saliva collection and in vitro bacterial overlay
The salivary flow rates were 0.416 ml/min (s.d. 0.244 ml/min) for unstimulated saliva and 1.882 ml/min (s.d. 0.703 ml/min) for the gum-base-stimulated saliva. The total protein concentrations were 1203.5 mg/ml (s.d. 276.6 mg/ml) for unstimulated saliva and 881.9 mg/ml (s.d. 198.2 mg/ml) for stimulated saliva. Analysis of data obtained from the in vitro bacterial overlay experiments demonstrated that test bacteria Streptococcus gordonii, Streptococcus parasanguinis, Actinomyces naeslundii, Candida albicans, and Streptococcus sobrinus bound to immobilized protein components of unstimulated and stimulated human saliva samples with various band intensities (Figs 1 and 2). Distinctive positive protein bands were detected at 20–30 kDa, 40–50 kDa, and at approximately 60 kDa (Figs 1 and 2). However, except for one subject (positive bands at 10 and 160 kDa), almost no binding was detected between Streptococcus mutans and salivary proteins. Similarly, lack of binding activity was noted for Lactobacillus casei. The binding pattern of A. naeslundii An19 to salivary proteins was distinct from those of other test bacteria. A strong band near 60 kDa was noted in both stimulated and unstimulated saliva samples (Fig. 1c).
Bacterial overlay images showing binding of (a) S. gordonii ATCC 35105, (b) S. parasanguinis ATCC 15912, (c) A. naeslundii An19, and (d) C. albicans ATCC 90028, to unstimulated and stimulated saliva from 5 individuals (#1-#5). M: molecular standards (Novex® sharp Prestained protein Standard). aF: asialofetuin. F: Fetuin. Exposure time for all images was 1/2 second. (a–d) Each represents images from two separate gels ran simultaneously. The deviding line indicates the separation between the two gels.
Bacterial overlay images showing binding of (a) S. mutans NCTC 10449, (b) S. mutans Ingbritt, (c) L. casei ATCC 27319, and (d) S. sobrinus ATCC 27352, to unstimulated and stimulated saliva from 5 individuals (#1-#5). M: molecular standards (Novex® sharp Prestained protein Standard). aF: asialofetuin. F: Fetuin. Exposure time for all images was 1/2 second, except for S. mutans Ingbritt (1/4 second). (a–d) Each represents images from two separate gels ran simultaneously. The deviding line indicates the separation between the two gels.
There were clearly inter-individual differences in bacterial binding profiles among the saliva samples of the five test subjects (Fig. 1). In general, reductions in band intensities were observed in the stimulated saliva samples when compared with the unstimulated samples. For example, the protein bands at approximately 15 kDa detected in the unstimulated saliva samples were either faint (S. gordonii) or non-detectable (S. parasanguinis, S. sobrinus) in the stimulated saliva samples. Two control proteins, fetuin and asialofetuin, were used to monitor reproducibility of binding patterns for individual test bacteria.
Human Oral Microbe Identification Microarray (HOMIM) analysis of in situ biofilm samples
Sixteen probes representing 26 species and 2 probes representing genus-level groups were detected in at least half of the samples collected (Table 1). Among these, 2 probes showed a significant increase under chew-stimulated conditions compared with unstimulated conditions: those corresponding to S. parasanguinis Human Oral Taxon (HOT)-721/411 and to Veillonella atypica HOT-524. Additionally, 4 probes showed a trend to increase by chewing: Granulicatella adiacens HOT-534, Streptococcus infantis HOT-638, Streptococcus anginosus HOT-543/S. gordonii HOT-622, and Streptococcus salivarius HOT-755/Streptococcus vestibularis HOT-021. Probes that showed changes between chew-stimulated and non-chew-unstimulated conditions with significant changes at P < 0.05 and trending changes with 0.05 < P < 0.15 are summarized in Fig. 3.
Imaging of biofilm in situ on the chips
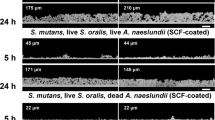
Images of antibody-stained biofilms on chips worn while subjects chewed are shown in Fig. 4 and in Supplementary Figs 1–3. Single cells made up the bulk of the biofilm biomass and, when confluent biofilm was present, it was unevenly distributed across the chip. Biomass on chips from Subject 2 was visibly lower compared with that on chips from Subject 1. Cells reactive with antibody against RPS serotypes 3 and 4 were present in high numbers in Subject 1 but were rare in Subject 2. Cells reactive with antibodies against RPS serotype 2 were seen in both individuals in low abundance. Cells reactive with antibody against RPS serotype H1 were rare in both individuals. Anti-Haemophilus- and anti-Rothia-reactive cells occurred in both subjects. Cells reactive with antibodies against Actinomyces strains were not found in either subject. Importantly, mixed-species colonies consisting of a few cells were easily found. In summary, Rothia, Haemophilus, and RPS-bearing streptococci occurred in both subjects, and interindividual differences were seen in RPS serotype abundance. However, intra-individual chewing-dependent differences in the types of RPS-reactive cells or in the amount of biomass were not apparent.
Representative images of biofilms stained with a mixture of fluorescently labeled antibodies against different RPS serotypes, against whole cells of Rothia mucilaginosa, and against whole cells of Haemophilus parainfluenzae. Note that colors for RPS, Rothia, and Haemophilus are not identical across the images. Clusters composed of several cell types are visible in each subject. Cells reactive with antibody against RPS serotypes 3 and 4 were seen in high numbers in Subject 1. RPS serotype 4-reactive cells were absent in Subject 2. Further, anti-Haemophilus-reactive cells were not seen on chips from “no chewing” experiments in Subject 2, which likely reflects the low overall biomass. Scale bar = 20 µm and applies to all panels.
Discussion
There was a consistency in binding patterns across saliva samples from multiple subjects, although some protein bands exhibited binding with higher intensity in some subjects than in others. In all strains tested except for A. naeslundii, the binding to proteins with MW above 80 kDa was diminished with stimulated saliva compared with unstimulated saliva. The salivary proteins in this molecular-weight range are often assigned as proline-rich proteins (PRPs) and mucin MUC7. Bands around 40 kDa, often assigned as the fragments of PRPs, were not affected by the type of saliva for all strains. Bands around 55 kDa, typically assigned to salivary amylase, showed decreased intensity with stimulated saliva for S. gordonii and S. parasanguinis; however, no change was observed for the other strains. No band showed a consistent increase in its intensity with stimulated saliva. Proteins and peptides with MW range between 5 and 40 kDa are comprised of statherin, histatins, cystatin, and PRPs27,28,29. These molecules are considered to play an important role in initial colonization. Two strains, S. gordonii and S. parasanguinis, showed less intense binding to the bands in this range when tested with stimulated saliva. Considering that stimulated saliva has a lower total protein concentration than does unstimulated saliva, this suggests that the key binding proteins differ between stimulated and unstimulated saliva12. Stimulated saliva is known to have a higher contribution from the parotid gland, and its flow rate remains elevated as long as masticatory stimulation continues13,30,31. Our results showed an overall agreement with results from a previous study of the interaction of S. gordonii and salivary proteins25. This work exposed S. gordonii to labeled salivary proteins, and the bacteria-bound proteins were eluted from the cell surface, separated by SDS-PAGE, and identified. They demonstrated strong positive protein bands between 50 and 60 kDa (putatively salivary amylase) and positive but faint bands between 20 and 30 kDa (putatively IgA κ and λ chains) and between 10 and 15 kDa (putatively lysozyme or cystatin)32. Our in vitro binding method involved overlaying labeled bacteria on SDS-PAGE-separated salivary proteins. Our results were similar to those previously reported, except that we observed strong binding to proteins at 160 to 170 kDa, probably putatively salivary mucin MUC7, which was not reported25. Among the strains of S. mutans tested, Ingbritt and NCTC 10449 did not demonstrate binding to the salivary proteins. This could explain why S. mutans species are not usually found as initial colonizers of dental biofilm. Similarly, we noted negative or weak binding with the other two cariogenic bacteria, L. casei and S. sobrinus. Our results suggested that there are differences in bacterial binding profiles among selected supragingival biofilm bacteria (Fig. 1), and caries-associated taxa (Fig. 2) were detected. The reduced number of bands in in vitro binding to stimulated saliva showed that chewing may affect how oral bacteria bind to enamel surfaces and provide a more competitive environment for binding scaffolds for bacteria-protein interactions when saliva is stimulated by chewing.
Between the two in situ analyses, HOMIM provides a non-selective semi-quantitative picture of the total bacterial community. Table 1 lists HOTs with threshold values of > 0 in either chewing or non-chewing samples. It is noteworthy that only 2 HOTs showed a statistically significant change when subjects chewed. An additional 4 probes representative of 6 HOTs showed a trend in changes with subjects chewing. These results suggest that chewing does not have a broad common effect on community composition across the two individuals. We understand the limitation in drawing conclusions based on an in situ study with only two subjects. Future studies with increased numbers of subjects are warranted.
All 6 probes in Fig. 3 increased their spot intensity with stimulated saliva compared with those formed under unstimulated saliva. These probes cover 8 HOTs, including S. gordonii and S. parasanguinis, which have been previously identified as initial colonizers of biofilm. V. atypica is a known coaggregation partner with S. gordonii and is also associated with S. parasanguinis in biofilm formation33,34. Veillonellae are also known to vary in phenotype during plaque accumulation35. Five of these 8 HOTs have been associated with oral health: Gr. adiacens, S. gordonii, S. parasanguinis, S. salivarius and V. atypica34.
The major HOTs found in chewing and non-chewing biofilms were much the same between subjects and visits. All organisms except Pseudomonas are frequently reported as typical and major components of supragingival plaque. The presence of Rothia, Streptococcus, and Veillonella in chip biofilm is also in agreement with their reported roles in initial biofilm formation1. In this work, we also observed high prevalence of the microorganisms previously associated with soft-tissue surfaces, including Pseudomonas spp. and Streptococcus australis. The latter is a relatively common, newly classified species (ranked as the 39th most frequent organism in the HOMD database), which has only rarely been discussed in previous HOMIM studies or in culture studies. The lack of culture study data on S. australis could likely reflect the fact that the species had not been taxonomically separated from other streptococcal species until 2001. It is noteworthy that the importance of this soft-tissue-associated bacterium did not increase after chewing in either sample. One consideration is that differences between biofilms of chewing-stimulated samples vs unstimulated samples may reflect dislodgement of bacteria from the oral epithelium rather than selective attachment related to the presence/absence of particular proteins in saliva. While it is difficult to eliminate the mechanical factors in these in situ studies, few differences were noted between biofilms on chips from stimulated-saliva volunteers and those on chips from unstimulated-saliva volunteers. Limited numbers of epithelial cells were detected on chips after their removal from the mouth, suggesting that mechanical factors play a small role (data not shown).
A parallel study on these same subjects reported a broad overview of HOMIM results from the “no chewing” arm of these experiments26. Those results demonstrated the prominence of Rothia spp. and Haemophilus parainfluenzae in the biofilms of both subjects, as well as a high degree of interaction between these species and other cells in the biofilm. Similar intimate cell-cell interactions of Rothia and Haemophilus with other cells were clear in the present study, independent of chewing. Also important is the absence of anti-Actinomyces-reactive cells in the biofilms; this was clearly corroborated by the low Actinomyces HOMIM probe values in the present study as well as in the previous study26. Thus, while an Actinomyces strain showed chewing-dependent differences in salivary binding profile (Figs 1 and 2), it is unlikely that such a difference could be detected in the imaging or the HOMIM data from these subjects. Actinomyces spp. are known to be important to early biofilm based on molecular and imaging analyses36,37, but the broad range of phenotypes makes it difficult to correlate the species- and strain-specific data acquired through in vitro studies (salivary binding) with the phenotype-independent data acquired by antibody-based imaging and HOMIM analyses.
Microscopic data collected in the present study are qualitative in nature and can be related to those reported in an earlier study25 with respect to correspondence of anti-RPS-reactive cells with RPS-bearing streptococcal isolates in these same subjects; at least one RPS-bearing isolate from both subjects corresponded to the presence of the appropriate anti-RPS-labeled cells in the biofilm. Therefore, while RPS antibodies used together with in situ imaging could be a good indicator of chewing-dependent effects on biofilm community composition, such effects were not obvious here. Also, RPS antibodies do not correlate with detailed taxonomic assignments (e.g., strains within the same species of streptococci can vary in the presence and serotype of RPS), and no HOMIM probe exists for certain prominent streptococcal species known to bear RPS26. With regard to salivary-binding profiles, it is clear that the streptococcal species showed no clear chewing-dependent differences; this supports the broader perspective gained by analysis of the imaging data. However, subject-specific differences in biofilm composition are evident in the imaging data of the present study, as well as in HOMIM data of the previous study26. Thus, in the present study, only inter-subject differences were obvious within the imaging datasets, and these were not affected by chewing.
In summary, the overlay results demonstrated binding to salivary proteins by early-colonizing species, while other bacteria important in caries did not bind well. The results also showed fewer proteins available for binding with stimulated saliva. Analysis of the HOMIM data indicates the consistent and prominent presence in all samples of commonly occurring tooth-surface bacteria. These include Gemella haemolysans, Rothia spp., Haemophilus parainfluenzae, and many different Streptococcus spp. Three common tooth isolates – Rothia mucilaginosa, S. parasanguinis, and V. atypica – showed an increase after subjects chewed. Another common oral isolate, S. gordonii, showed a trend to increase when subjects chewed. These initial colonizers are associated with health. Immunofluorescence with anti-RPS antibody provided support for the HOMIM data. A major difference was observed in the bacteria-protein interactions between subjects. Not only did the binding pattern of a type strain show clear differences between subjects, but also microscopy of in situ biofilms showed clear differences in the presence of some anti-RPS-reactive cells. This demonstrates a component of inter-individual variability not acquired with a single approach. Chewing appeared to affect bacterial binding profiles during very early colonization (4 hours) on at least some of the known early colonizers. The response of stimulated saliva to chewing seems to be individual-specific, and therefore further research should focus on functional analysis of bacteria or the impact on co-aggregation/co-adhesion.
Materials and Method
Unstimulated and stimulated saliva collection
Five adult non-smokers (three male and two female 18 to 65 years old) who did not chew gum regularly and had no reported health condition or medication intake were enrolled in the study. Their resting unstimulated saliva was collected first by the drooling method38. Then their stimulated saliva was collected when they spit into a 50-ml centrifuge tube for 10 minutes while chewing a 1-g piece of unflavored unsweetened gum base (Mars-Wrigley Confectionery, Chicago, IL, USA). Samples were placed on ice immediately upon collection, and phenylmethylsulfonyl fluoride was added at a final concentration of 1 μM. Saliva samples were clarified by centrifugation at 12,000 × g for 10 minutes at 4 °C, and the supernatant was stored at −80 °C until further analysis. Total protein was measured by the Lowry method (Sigma-Aldrich, St. Louis, MO, USA). All experimental protocols were preapproved by the University of Illinois at Chicago (UIC) Institutional Review Board (IRB #2006-0916). All parcipants provided informed consent prior to the initiation of the study procedures.
Test microorganisms and growth
Actinomyces naeslundii (strain An19), Streptococcus gordonii ATCC 35105, Streptococcus mutans NCTC 10449, S. mutans subsp. Ingbritt, Streptococcus sobrinus ATCC 27352, and Streptococcus parasanguinis ATCC 15912 were grown in Brain Heart Infusion broth (BHI, Bacto Laboratories, Mt Pritchard, NSW, Australia). Lactobacillus casei ATCC 27319 was grown in the MRS medium (BD Difco, Franklin Lakes, NJ, USA). Candida albicans ATCC 90028 was grown in RPMI 1640 medium (Sigma-Aldrich). All test organisms for the overlay study were grown in 10-ml tubes of broth without shaking at 37 °C in a 5% CO2 incubator.
In vitro bacterial binding to salivary proteins
Bacterial binding to salivary proteins was studied by an overlay method21 in which saliva samples (20 μg protein per lane) were separated by SDS-PAGE on a 4–12% Bis-Tris gel (NuPAGETM, Invitrogen, Carlsbad, CA, USA). Proteins were then electro-blotted onto a PVDF membrane (BIO-RAD, Hercules, CA, USA) and overlaid with 9.0 ml of FITC-labeled bacterial cells (5 × 108 cells/ml) suspended in block solution (TBS buffer with 5% BSA, 1 mM CaCl2, 1 mM MgCl2). The bacteria-protein binding patterns were identified as fluorescent bands under UV epi-illumination (ImageQuant LAS4000; ex 494 nm/em 518 nm). Two standard proteins, namely, fetuin and asialofetuin (Sigma-Aldrich), were loaded onto separate lanes in each of the SDS-PAGE gels as controls.
In situ biofilm growth, community composition analysis, and biofilm imaging
Fourteen adults (18 to 64 years old) were recruited for an initial screening. Inclusion criteria were: healthy (self-reported medical history) adults at least 18 years old and having good oral health as determined by a dentist’s examination. Exclusion criteria were: active caries, oral cancer, or more than mild gingivitis; history of medical conditions affecting salivary flow; a history of immunosuppressant therapy; history of cardiac, kidney, liver, or lung disorders; use of tobacco within the last year: use of antibiotics within the preceding four months; use of medications or radiation therapy thought to affect salivary flow, such as head/neck radiation, diuretics, or nitrates; current steroid therapy (other than topical) within the preceding 30 days; auto-immune or immune diseases such as ulcerative colitis or systemic lupus erythematosus; active dental caries; moderate to severe gingivitis; and periodontal probing depths of >3 mm on two or more molars and premolars. These criteria resulted in the recruitment of only those subjects with excellent oral health. All studies were carried out in accordance with approved National Institute of Health (NIH) guidelines including prior review by the NIH intramural Institutional Review Board, and in accordance with the standards indicated by the Declaration of Helsinki. All study participants provided informed consent prior to the initiation of any study procedures. Two male subjects (hereafter referred to as Subject 1 and Subject 2) were selected to continue with the study based on the above criteria, and after confirmation that biofilm on intra-orally carried retrievable enamel chips contained bacteria that stained with anti-RPS antibodies (see below).
Enamel chips (3 mm × 3 mm) were cut from extracted third molars that had been thoroughly rinsed and air-dried. The chips were then sonicated in a low-power bath (model 1510, Branson, Danbury, CT, USA) for 10 minutes. Efficacy of the cleaning procedure was demonstrated by epifluorescence microscopy; a chip that had been stained with DAPI bore no bacterial or cellular debris. After sterilization by ethylene oxide, three chips each were affixed to both the left and the right buccal sides of a full-mandibular stent by means of dental wax. The stent was then worn by the participants for 4 hours, after which the enamel chips were removed and investigated by confocal microscopy and microbial community analysis (HOMIM). In a cross-over design, both subjects reported for 6 visits, 3 visits in which gum was chewed, and 3 in which no gum-chewing took place. For chewing experiments, subjects chewed a piece of chewing gum (2.7 g; Wrigley Extra®) for 10 minutes without the stent in place, immediately after which the stent was inserted. After 4 hours, the stent was removed, and DNA was extracted from the biofilm as described previously26. Briefly, the enamel chips were gently dipped in sterile water three times, then sonicated. DNA was extracted from the sonicate by means of a DNAeasy Blood and Tissue kit (QIAGEN, Valencia, CA, USA), then sent to The Forsyth Institute (Boston, MA, USA) for biofilm community composition analysis by HOMIM39. In this procedure, extracted sample DNA is amplified with a universal 16S primer, then resulting amplicons are fluorescently labeled and hybridized to the array that bears short DNA sequences (probes) corresponding to 16S ribosomal gene sequences of taxa (Human Oral Taxon; HOTs) within the Human Oral Microbiome Database (HOMD; http://expanded.homd.org/). Fluorescent signal intensity (values of 0–5) is read for each spot, which corresponds to the amount of a particular phylotype (or, in cases of multiply-reactive probes, to several phylotypes) in the sample.
In addition, the biofilm on at least one chip from each experiment was stained with a mixture of fluorescently labeled primary antibodies raised against purified RPS and against whole cells of Actinomyces, Rothia, and Haemophilus strains, as well as with DAPI (to reveal antibody-unreactive cells)26. The biofilms were visualized by means of a 0.9NA 60x water-immersible (dipping) lens mounted on a Zeiss LSM 710 confocal microscope.
Statistical analysis
HOMIM results are reported as probe abundance with values ranging from 0 (absent) to 5 (abundant). The rate at which each probe was detected from all visits was defined as prevalence. Only probes with a value > 0 in at least half the visits of either ‘chew’ or ‘non-chew’ were used for analysis, i.e., prevalence >0.5; these were defined as the major probes. Analyses were performed on the absolute intensity of HOMIM data (0–5) by non-metric MDS (MultiDimensional Scaling) and a non-parametric ANOVA with PAST 3.08 (Paleontological Museum, University of Oslo, Oslo, Norway). For the change in individual probe values, the Mann-Whitney test was performed with IBM SPSS 23.0 (IBM Corp., Armonk, NY, USA). A P value of < 0.05 was considered statistically significant after the Benjamini-Hochberg correction40.
References
Kolenbrander, P. E. Multispecies communities: interspecies interactions influence growth on saliva as sole nutritional source. International Journal of Oral Science 3, 49–54, https://doi.org/10.4248/IJOS11025 (2011).
Nyvad, B. & Fejerskov, O. Scanning electron microscopy of early microbial colonization of human enamel and root surfaces in vivo. Scandinavian journal of dental research 95, 287–296 (1987).
Heller, D. et al. Microbial Diversity in the Early In Vivo-Formed Dental Biofilm. Applied and Environmental Microbiology 82, 1881–1888, https://doi.org/10.1128/aem.03984-15 (2016).
Hertel, S. et al. Initial microbial colonization of enamel in children with different levels of caries activity: An in situ study. Am J Dent 30, 171–176 (2017).
Ruhl, S. The scientific exploration of saliva in the post-proteomic era: from database back to basic function. Expert Review of Proteomics 9, 85–96, https://doi.org/10.1586/epr.11.80 (2012).
Carlén, A., Börjesson, A., Nikdel, K. & Olsson, J. Composition of Pellicles Formed in vivo on Tooth Surfaces in Different Parts of the Dentition, and in vitro on Hydroxyapatite. Caries Research 32, 447–455 (1998).
Siqueira, W. L., Zhang, W., Helmerhorst, E. J., Gygi, S. P. & Oppenheim, F. G. Identification of Protein Components in in vivo Human Acquired Enamel Pellicle Using LC-ESI-MS/MS. Journal of Proteome Research 6, 2152–2160, https://doi.org/10.1021/pr060580k (2007).
Gibbins, H. L., Proctor, G. B., Yakubov, G. E., Wilson, S. & Carpenter, G. H. Concentration of salivary protective proteins within the bound oral mucosal pellicle. Oral Dis. 20, 707–713, https://doi.org/10.1111/odi.12194 (2014).
Cheaib, Z., Rakmathulina, E., Lussi, A. & Eick, S. Impact of Acquired Pellicle Modification on Adhesion of Early Colonizers. Caries Research 49, 626–632 (2015).
Cisar, J. O., Sandberg, A. L., Reddy, G. P., Abeygunawardana, C. & Bush, C. A. Structural and antigenic types of cell wall polysaccharides from viridans group streptococci with receptors for oral actinomyces and streptococcal lectins. Infection and Immunity 65, 5035–5041 (1997).
Ito, T. et al. Effects of Lectins on initial attachment of cariogenic Streptococcus mutans. Glycoconjugate Journal 35, 41–51, https://doi.org/10.1007/s10719-017-9795-2 (2018).
Whelton, H. In Saliva and Oral Health (eds Michael Edgar, C. Dawes, & D. O’Mullane) Ch. 1, 1–13 (British Dental Association, 2004).
Neyraud, E., Sayd, T., Morzel, M. & Dransfield, E. Proteomic analysis of human whole and parotid salivas following stimulation by different tastes. Journal of Proteome Research 5, 2474–2480, https://doi.org/10.1021/pr060189z (2006).
Denny, P. et al. The proteomes of human parotid and submandibular/sublingual gland salivas collected as the ductal secretions. Journal of Proteome Research 7, 1994–2006, https://doi.org/10.1021/pr700764j (2008).
Quintana, M. et al. Short-Term Modification of Human Salivary Proteome Induced by Two Bitter Tastants, Urea and Quinine. Chemosensory Perception 2, 133–142, https://doi.org/10.1007/s12078-009-9048-2 (2009).
Walz, A. et al. Proteome analysis of glandular parotid and submandibular-sublingual saliva in comparison to whole human saliva by two-dimensional gel electrophoresis. Proteomics 6, 1631–1639, https://doi.org/10.1002/pmic.200500125 (2006).
Cabras, T. et al. Age-Dependent Modifications of the Human Salivary Secretory Protein Complex. Journal of Proteome Research 8, 4126–4134, https://doi.org/10.1021/pr900212u (2009).
Quintana, M. et al. Inter-individual variability of protein patterns in saliva of healthy adults. Journal of Proteomics 72, 822–830, https://doi.org/10.1016/j.jprot.2009.05.004 (2009).
Sondej, M. et al. Glycoprofiling of the Human Salivary Proteome. Clinical Proteomics 5, 52–68, https://doi.org/10.1007/s12014-008-9021-0 (2009).
Prodan, A. et al. Interindividual variation, correlations, and sex-related differences in the salivary biochemistry of young healthy adults. European Journal of Oral Sciences 123, 149–157, https://doi.org/10.1111/eos.12182 (2015).
Ruhl, S., Cisar, J. O. & Sandberg, A. L. Identification of Polymorphonuclear Leukocyte and HL-60 Cell Receptors for Adhesins of Streptococcus gordonii and Actinomyces naeslundii. Infection and Immunity 68, 6346–6354, https://doi.org/10.1128/iai.68.11.6346-6354.2000 (2000).
Walz, A. et al. Identification of glycoprotein receptors within the human salivary proteome for the lectin-like BabA and SabA adhesins of Helicobacter pylori by fluorescence-based 2-D bacterial overlay. Proteomics 9, 1582–1592, https://doi.org/10.1002/pmic.200700808 (2009).
Newman, F., Beeley, J. A. & MacFarlane, T. W. Adherence of oral microorganisms to human parotid salivary proteins. Electrophoresis 17, 266–270, https://doi.org/10.1002/elps.1150170146 (1996).
Seemann, R. et al. Levels of parotid and submandibular/sublingual salivary immunoglobulin A in response to experimental gingivitis in humans. Clinical Oral Investigations 8, 233–237, https://doi.org/10.1007/s00784-004-0280-5 (2004).
Heo, S.-M., Ruhl, S. & Scannapieco, F. A. Implications of salivary protein binding to commensal and pathogenic bacteria. Journal of Oral Biosciences 55, 169–174, https://doi.org/10.1016/j.job.2013.06.004 (2013).
Palmer, R. J. et al. Interbacterial adhesion networks within the early oral biofilm of individual human hosts. Applied and Environmental Microbiology 83, e00407–00417, https://doi.org/10.1128/aem.00407-17 (2017).
Dawes, C. et al. The functions of human saliva: A review sponsored by the World Workshop on Oral Medicine VI. Archives of Oral Biology 60, 863–874, https://doi.org/10.1016/j.archoralbio.2015.03.004 (2015).
Gorr, S.-U. Antimicrobial peptides of the oral cavity. Periodontology 2000 51, 152–180, https://doi.org/10.1111/j.1600-0757.2009.00310.x (2009).
Johnson, D. A., Yeh, C. K. & Dodds, M. W. J. Effect of donor age on the concentrations of histatins in human parotid and submandibular/sublingual saliva. Archives of Oral Biology 45, 731–740, https://doi.org/10.1016/S0003-9969(00)00047-9 (2000).
Dawes, C. The unstimulated salivary flow rate after prolonged gum chewing. Archives of Oral Biology 50, 561–563, https://doi.org/10.1016/j.archoralbio.2004.10.016 (2005).
Dodds, M., Roland, S., Edgar, M. & Thornhill, M. Saliva A review of its role in maintaining oral health and preventing dental disease. Bdj Team 2, 15123, https://doi.org/10.1038/bdjteam.2015.123 (2015).
Heo, S.-M. et al. Host Defense Proteins Derived from Human Saliva Bind to Staphylococcus aureus. Infection and Immunity 81, 1364–1373, https://doi.org/10.1128/iai.00825-12 (2013).
Egland, P. G., Palmer, R. J. & Kolenbrander, P. E. Interspecies communication in Streptococcus gordonii–Veillonella atypica biofilms: Signaling in flow conditions requires juxtaposition. Proceedings of the National Academy of Sciences of the United States of America 101, 16917–16922, https://doi.org/10.1073/pnas.0407457101 (2004).
Takahashi, N. Oral Microbiome Metabolism: From “Who Are They?” to “What Are They Doing?”. Journal of Dental Research 94, 10, https://doi.org/10.1177/0022034515606045 (2015).
Palmer, R. J., Diaz, P. I. & Kolenbrander, P. E. Rapid Succession within the Veillonella Population of a Developing Human Oral Biofilm In Situ. Journal of Bacteriology 188, 4117–4124, https://doi.org/10.1128/jb.01958-05 (2006).
Palmer, R. J., Gordon, S. M., Cisar, J. O. & Kolenbrander, P. E. Coaggregation-Mediated Interactions of Streptococci and Actinomyces Detected in Initial Human Dental Plaque. Journal of Bacteriology 185, 3400–3409, https://doi.org/10.1128/jb.185.11.3400-3409.2003 (2003).
Aas, J. A., Paster, B. J., Stokes, L. N., Olsen, I. & Dewhirst, F. E. Defining the normal bacterial flora of the oral cavity. Journal of Clinical Microbiology 43, 5721–5732, https://doi.org/10.1128/JCM.43.11.5721-5732.2005 (2005).
Vissink, A., Wolff, A. & Veerman, E. C. In Salivary Diagnostics (ed. Wong, D. T.) Ch. 4, 37–59 (Wiley-Blackwell, 2008).
Colombo, A. P. V. et al. Comparisons of Subgingival Microbial Profiles of Refractory Periodontitis, Severe Periodontitis, and Periodontal Health Using the Human Oral Microbe Identification Microarray. Journal of Periodontology 80, 1421–1432, https://doi.org/10.1902/jop.2009.090185 (2009).
Hochberg, Y. & Benjamini, Y. More powerful procedures for multiple significance testing. Statistics in Medicine 9, 811–818, https://doi.org/10.1002/sim.4780090710 (1990).
Acknowledgements
This work was supported by Mars-Wrigley Confectionery and by the NIDCR Intramural Research Program. The authors thank Luxia Zhang (NIDCR) for technical assistance and the UIC Department of Pharmacology for use of the Image Quant LAS4000 Imager. N.S. was supported as an IRTA technical fellow through CRADA agreement T-2011-1291 between NIDCR and Wrigley.
Author information
Authors and Affiliations
Contributions
T.I., R.J.P., N.S. and J.O.C. were involved in study design, experimentation, and data analysis for the in situ biofilm study (HOMIM and biofilm imaging). T.I., W.L. and C.D.W. were invoilved in the salivary protein-bacteria binding studies. T.I., R.J.P., W.L. and C.D.W. prepared the manuscript. All authors reviewed and approved the final version of the manuscript.
Corresponding author
Ethics declarations
Competing Interests
The authors declare no competing interests.
Additional information
Publisher’s note: Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made. The images or other third party material in this article are included in the article’s Creative Commons license, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons license and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this license, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Inui, T., Palmer, R.J., Shah, N. et al. Effect of mechanically stimulated saliva on initial human dental biofilm formation. Sci Rep 9, 11805 (2019). https://doi.org/10.1038/s41598-019-48211-3
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41598-019-48211-3
This article is cited by
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.