Abstract
Structure-activity relationships (SAR) in the aurone pharmacophore identified heterocyclic variants of the (Z)-2-benzylidene-6-hydroxybenzofuran-3(2H)-one scaffold that possessed low nanomolar in vitro potency in cell proliferation assays using various cancer cell lines, in vivo potency in prostate cancer PC-3 xenograft and zebrafish models, selectivity for the colchicine-binding site on tubulin, and absence of appreciable toxicity. Among the leading, biologically active analogs were (Z)-2-((2-((1-ethyl-5-methoxy-1H-indol-3-yl)methylene)-3-oxo-2,3-dihydrobenzofuran-6-yl)oxy)acetonitrile (5a) and (Z)-6-((2,6-dichlorobenzyl)oxy)-2-(pyridin-4-ylmethylene)benzofuran-3(2H)-one (5b) that inhibited in vitro PC-3 prostate cancer cell proliferation with IC50 values below 100 nM. A xenograft study in nude mice using 10 mg/kg of 5a had no effect on mice weight, and aurone 5a did not inhibit, as desired, the human ether-à-go-go-related (hERG) potassium channel. Cell cycle arrest data, comparisons of the inhibition of cancer cell proliferation by aurones and known antineoplastic agents, and in vitro inhibition of tubulin polymerization indicated that aurone 5a disrupted tubulin dynamics. Based on molecular docking and confirmed by liquid chromatography-electrospray ionization-tandem mass spectrometry studies, aurone 5a targets the colchicine-binding site on tubulin. In addition to solid tumors, aurones 5a and 5b strongly inhibited in vitro a panel of human leukemia cancer cell lines and the in vivo myc-induced T cell acute lymphoblastic leukemia (T-ALL) in a zebrafish model.
Similar content being viewed by others
Introduction
The aurones comprise a family of plant-derived flavonoids that arise out of a mixed polyketide-shikimate pathway, contribute to the yellow coloration of certain flowers1 and possess a range of biological properties2,3,4 affecting organisms ranging from protazoans to mammals. The antineoplastic activity5 of several naturally occurring aurones led to studies of natural and semisynthetic aurones as inhibitors of in vitro cancer cell proliferation6,7,8, typically at low micromolar concentrations. Additional studies identified a panoply of roles at a molecular level: drug efflux modulators2,9,10,11,12,13,14,15 of P-glycoprotein (P-gp) or ATP-binding cassette sub-family G member 2 (ABCG2), modifiers of adenosine-receptor interactions16,17, DNA sission-promoters18, teleomerase inhibitors19, sphingosine-kinase inhibitors20, phosphatidylinositol-3-kinases (PI3−α) inhibitors21, cyclin-dependent kinase inhibitors22, inducers of cytoprotective NAD(P)H:quinone oxidoreductase-123 (NQO1), and scavengers of reactive-oxygen-species24 (ROS). Although these findings suggested that aurones would disrupt biological systems non-specifically, our studies of the aurone pharmacophore identified heterocyclic variants of the (Z)-2-benzylidene-6-hydroxybenzofuran-3(2H)-one scaffold that possessed the low nanomolar in vitro potency, encouraging in vivo potency in mouse xenograft and zebrafish models, selectivity for the colchicine-binding site in tubulin25,26,27,28,29,30,31, and the absence of appreciable toxicity.
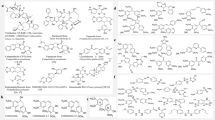
Prior SAR studies of aurones as antineoplastic agents replaced the C-2 benzylidene subunit found in naturally occurring aurones, such as sulfuretin (1a) and aureusidin (1b) (Fig. 1A), with a C-2 heteroarylmethylene group. Aurones with 2-(coumarin-4-yl)methylene groups32 or 2-(furan-2-yl)methylene groups33 displayed in vitro activity against human leukemia K562 cells; aurones with 2-(piperazin-1-yl)methylene groups possessed IC50 values in the low micromolar range against various solid tumor cell lines34; and benzofuran-3(2H)-ones with 2-(indol-3-yl)methylene groups inhibited cell proliferation in breast cancer MCF-7 and MDA-MB-231 cell lines35. The relative potencies among these heterocyclic- and heteroarylmethylene-substituted aurones, the in vivo activity of these aurones, and the specific biological target or targets in these cases was unclear.
(A) Representative naturally occurring aurones, sulfuretin (1a) and aureusidin (1b). (B) Synthesis of aurones 4 and 5. Legend: a, heterocyclic-substituted benzaldehydes or heteroaryl carboxaldehydes 3, 50% aq. KOH, 1:1 EtOH:DMF, b, BrCH2CN, K2CO3, DMF; c, ClCH2C6H3-2,6-Cl2, K2CO3, DMF. (C) Biologically active aurones 5a and 5b.
We determined that semisynthetic aurones with either 3-indolylmethylene or 4-pyridylmethylene groups at C-2 in place of the naturally occurring C-2 benzylidene group and with selected alkoxy groups at C-6 possessed in vitro potencies in the mid- to low nanomolar range using in vitro PC-3 cancer cell proliferation assays. The most potent of these aurones in these in vitro assays also displayed good activity in an in vivo PC-3 xenograft study. Although our studies focused on developing agents for the treatment of prostate cancers, the prior report that aurones with 2-(coumarin-4-yl)methylene groups32 or 2-(furan-2-yl)methylene groups33 displayed in vitro activity against human leukemia K562 cells prompted a study of myc-induced T-cell acute lymphoblastic leukemia (T-ALL) in a zebrafish model where these aurones also exhibited minimal toxicity. In summary, the aurones reported in this paper showed activity in two different animal models, displayed no apparent toxicity in two different species, and, like the literature reports cited above, showed activity against not only against prostate cancer PC-3 cells but also against leukemia cells. Finally, using a competition assay with mass spectrometry as an analytical tool, we established that these aurones functioned at a molecular level as tubulin polymerization inhibitors by binding to the colchicine-binding site.
Results
Synthesis of semisynthetic aurones
The condensation of 6-hydroxybenzofuran-3(2H)-one (2) with a spectrum of heteroaryl carboxaldehydes 3 under basic conditions led to aurones 4 (Fig. 1B). A mixture of 50% aqueous potassium hydroxide (2 eq) in 1:1 ethanol-N,N-dimethylformamide (DMF) was preferred over other conditions23,36,37,38 reported for similar condensations. The assignment of (Z)-stereochemistry in 4 was in accord with prior acid- or base-catalyzed condensations of benzofuran-3(2H)-ones with aromatic aldehydes39,40. The subsequent alkylation of the C-6 hydroxyl group in aurones 4 using various alkyl bromides and anhydrous potassium carbonate in DMF led to the 6-alkoxyaurones 5 (Fig. 1B).
Structure-activity relationships (SAR)
A reiterative process of synthesis and screening using in vitro prostate cancer PC-3 cell proliferation assays identified an intersection of modifications at the C-2 and C-6 positions in semisynthetic aurones that were the most promising for further study (Table 1). Initial screening identified heteroarylmethylene-substituted aurones 4a–4d with 1-isoquinolylmethylene, 2-quinolylmethylene, 8-methoxy-2-quinolylmethylene, and 5-methoxy-N-ethyl-3-indolylmethylene groups at C-2 and hydroxyl groups at C-6 as the most potent analogs at 10 μM concentrations but with only minimal activity at 1 μM concentrations (Table 1). Modifications at the C-4 and C-7 positions in the benzofuran ring in aurones 4 proved unrewarding in terms of increased potency (data not shown). Efforts to identify benzylidene-substituted aurones 4 with saturated, heterocyclic groups attached to the phenyl ring were equally unrewarding with the exception of (2Z)-6-hydroxy-2-(4-pyrrolidin-1-ylbenzylidene)-1-benzofuran-3(2H)-one (4e) (Table 1).
Additional efforts to improve potency in aurones 4a–4e led to the alkylation of the C-6 hydroxyl group with a range of alkylating agents to obtain 6-alkoxyaurones 5 (Fig. 1B). An SAR study involving dual modifications of the C-6 alkoxy group and the C-2 heteroarylmethyelene group identified two aurones with 90%+ inhibition of in vitro prostate cancer PC-3 cell proliferation at 300 nM concentration: (Z)-2-((2-((1-ethyl-5-methoxy-1H-indol-3-yl)methylene)-3-oxo-2,3-dihydrobenzofuran-6-yl)oxy)acetonitrile (5a) and (Z)-6-((2,6-dichlorobenzyl)oxy)-2-(pyridin-4-ylmethylene)benzofuran-3(2H)-one (5b) (Fig. 1C). In a dose-response study, aurone 5a and 5b displayed IC50 values of 58.7 ± 1.1 nM and 66 ± 1.1 nM (Fig. 2A), respectively. Aurone 5a displayed an IC50 value of 1.3 ± 0.2 μM using normal human embryo lung HEL299 cells that indicated that aurone 5a was selectively more toxic to a cancer cell line than a normal cell line.
(A) Dose responses of aurones 5a and 5b in PC-3 cell proliferation inhibition assay. (B) Effect of aurone 5a on PC-3 tumor xenografts in nude mice (n = 5) at 10 mg/kg/day. (C) Effect on aurone 5a on body weights of the treated mice: *P < 0.05, t-test. (D) H&E analysis of tumor sections. (E). Apoptosis analysis by TUNEL assay. (F). IHC analysis of angiogenesis marker, VEGF-A.
The pairing of the cyanomethoxy group at C-6 with the (N-ethyl-5-methoxy-1H-indol-3-yl)methylene at C-2 in aurone 5a and the pairing of the 2,6-dichlorobenzyloxy group at C-6 with the (pyridin-4-yl)methylene at C-2 in aurone 5b (Fig. 1C) were essential to potency. Alternate pairings, modification in the halogenation type and pattern in the 2,6-dichlorobenzyloxy group, changes in the N-ethyl-5-methoxy-1H-indol-3-yl group (e.g., replacement of the N-ethyl with an N-methyl group; replacement of the 5-methoxy with a 5-hydroxy group), and modifications at still other positions in the benzofuran (e.g., methyl groups at C-7) led to diminished activity in the prostate cancer PC-3 cell proliferation assay relative to aurones 5a and 5b. Finally, we performed additional cell proliferation inhibition studies using other cancer cell lines, and aurones 5a and 5b showed potent low nanomolar activities against these cell lines (Table 2).
Prostate cancer PC-3 xenograft study in mice using aurone 5a
We evaluated the in vivo tumor inhibitory effect of aurone 5a using prostate cancer PC-3 xenografts in immune-defective nude mice. PC-3 cells were subcutaneously injected into both flanks of nude mice. Two weeks after the inoculation, the mice were randomized to two groups (n = 5), treated with aurone 5a or control vehicle by intraperitoneal administration for 18 days and then sacrificed. Compared to vehicle, the administration of 5a at 10 mg/kg/day showed significant, tumor-growth suppression (Fig. 2B). Importantly, aurone 5a achieved tumor regression with no apparent gross toxicity as reflected by minimal changes in mice weights (Fig. 2C). To understand the mechanisms of aurone 5a-induced tumor repression, we performed another PC-3 xenograft study by treating the tumors with vehicle and aurone 5a for one week. Tumor sections were analyzed by H&E (Fig. 2D) and immunohistochemistry (IHC) stainings (Fig. 2E,F). We observed increased apoptosis (Fig. 2E) and decreased angiogenesis marker, VEGF (Fig. 2F), in aurone 5a-treated tumors.
Effect of aurone 5a on tubulin polymerization
An analysis of the screening data (Table 3) from the NCI-60 human tumor cell lines available through the developmental therapeutics program of NCI showed excellent response to aurone 5a with IC50 values in the range of 200–500 nM. These values were consistent with the IC50 values determined by Vi-CELL XR 2.03 (Fig. 2A and Table 2). An analysis of the NCI-60 data from aurone 5a using the COMPARE algorithm41 matched the response of cell lines to aurone 5a with the response of other tubulin-polymerization inhibitors. An analysis of the effects of aurone 5a on cell cycle progression using PC-3 cells indicated significant cell cycle arrest at G2/M phases (Fig. 3A,B), again consistent with the inhibition of tubulin microtubule assembly. We then investigated the level of tubulin polymerization in PC-3 cells treated by aurone 5a at indicated concentrations. After cell treatment and lysis, we separated the cell lysates by centrifugation into supernatants and pellets, that were individually subjected to western blotting using antibodies against β-tubulin. After treatment with aurone 5a for 6 hours, the amount of tubulin in pellets was significantly less than that in cell lysates from dimethyl sulfoxide (DMSO)-treatment alone, even at a concentration as low as 300 nM (Fig. 3C). We also performed an in vitro tubulin polymerization assay in the presence and absence of aurone 5a. In the presence of glycerol and guanosine triphosphate, either aurone 5a at 5 µM or colchicine at 5 µM decreased the formation of microtubules in a similar fashion whereas a DMSO-treated control group showed, as expected, substantial tubulin polymerization (Fig. 3D).
(A,B) Aurone 5a induced cell cycle arrest. (C) Aurone 5a decreased tubulin polymerization. (D) Aurone 5a (5 µM) and colchicine (5 µM) inhibited tubulin polymerization in vitro in a similar fashion. (E) Competitive tubulin binding assay with colchicine in the presence of increasing concentrations of aurones 5a. (F–H) Aurone 5a treatment (6 h) inhibited microtubule structures and caused cell morphology change in PC-3 cells as shown in panels F, DMSO; G, 5a (1 µM); H, 5a (300 nM). Red immunofluorescence: α-tubulin; blue: DAPI.
Competition study of colchicine and aurone 5a for the colchicine-binding site on tubulin
A competitive, tubulin-binding assay42 confirmed that aurone 5a bound to the colchicine-binding site. Aurone 5a was added at various concentrations to a solution of α/β-tubulins (1.3 mg/mL) and colchicine (1.25 μM). Unbound colchicine was separated from either tubulin-colchicine or tubulin-aurone 5a complex by Amicon Ultra-0.5 mL Centrifugal Filters (30 kDa Cut-off). The level of unbound colchicine was measured by liquid chromatography-electrospray ionization-tandem mass spectrometry (LC-MS/MS). Aurone 5a released colchicine from tubulin in a dose-dependent manner (Fig. 3E) that indicated that aurone 5a bound to the colchicine-binding site on tubulin.
Effects of aurone 5a on microtubule networks
We analyzed microtubule networks in PC-3 cells by immunofluorescence staining using an anti-α-tubulin Ab (Fig. 3F–H). The control, DMSO-treated cells retained their normal microtubule network and an overall, shuttle-like morphology (Fig. 3F) whereas aurone 5a-treated cells demonstrated significant microtubule depolymerization and adopted a round morphology (Fig. 3G,H).
Molecular docking analysis
We performed molecular docking using AutoDock Vina43 to explore the possible binding of aurone 5a to the colchicine-binding site (CBS) on αβ-tubulin heterodimers because this site was well known to host a plethora of chemically unrelated compounds44. A less active aurone 4d (Fig. 4A) than aurone 5a and colchicine were also docked into the CBS for comparison. We observed that aurone 5a, 4d and colchicine occupied the CBS at the interface of the α-tubulin and α-tubulin heterodimer (Fig. 4B). A hydrophobic pocket formed by Ala, Ile and Leu residues from β-tubulin accommodated the hydrophobic indole moiety of aurone 5a (Fig. 4C). The benzofuran-3(2H)-one and cyanomethoxy groups in aurone 5a participated in hydrophobic contacts with the loop T7 and helix H8 of β-tubulin and with the loops T3, T4 and T5 from α-tubulin (Fig. 4C)45. In addition, hydrogen-bonding interactions between the carbonyl oxygen of the benzofuran-3(2H)-one and βAsn258 and hydrogen-bonding interactions between the nitrogen of the cyanomethoxy group and αTyr224 and αGln11 provided additional binding stabilization (Fig. 4D).
(A) Structures of aurone 5a, a less active aurone 4d, and colchicine. (B) Aurone 5a bound to the colchicine-binding site (CBS) in the interface of αβ-tubulin dimers (cyan for β, green for α). (C) Close-up view of the interaction environment of 5a (gray sticks) and tubulin (carton). (D) Superimposition of 5a (gray sticks) and 4d (magenta sticks) in the colchicine-binding site. Hydrogen bonding is represented by yellow, dashed lines. (E) Superimposition of 5a (gray sticks) and colchicine (purple sticks) in the colchicine-binding site.
The indole moiety and a portion of the benzofuran-3(2H)-one in aurone 5a superimposed well with the colchicine A and B rings (Fig. 4E); however, aurone 5a did not occupy the hydrophobic pocket within β-tubulin in which the colchicine C ring resided. Instead, aurone 5a formed contacts with loops T3, T4, and T5 of α-tubulin using the benzofuran-3(2H)-one and cyanomethoxy groups. Additionally, a comparison of the binding poses of 5a and 4d revealed why 5a possessed better potency than 4d. Aurone 4d had major interactions with β-tubulin but lacked the bifurcated, hydrogen-bonding between the nitrogen of the cyanomethoxy group and αTyr224 and αGln11 of α-tubulin. This deficiency weakened the binding affinity of aurone 4d relative to the potent aurone 5a (Fig. 4D).
Leukemia cell study in zebrafish using aurone 5a
In addition to the in vivo PC-3 xenograft study in mice, we sought to test these aurones in a second species. Two prior reports indicated that aurones with 2-(coumarin-4-yl)methylene groups or 2-(furan-2-yl)methylene groups displayed in vitro activity against a leukemia cell line. Consequently, we tested various leukemia cell lines and found that the IC50 values for aurone 5a were in the mid-nanomolar range (Table 4). The IC50 values of two normal B-lymphoblast cells were much higher than the leukemia cell lines and suggested a preferential toxicity of aurone 5a toward leukemia cells. Because these leukemia cell lines had various mutations, we tested the activity of aurone 5a in vivo using a genetically well-defined, zebrafish myc-induced T-ALL leukemia model46,47 (Fig. 5). The zebrafish (Danio rerio) is a vertebrate system that develops tumors similar to those in humans and that provides a plaform that is easy to manipulate for in vivo assays even in large-scale screens. According to previous studies46,47, the zebrafish Rag2 promotor controlling the myc-GFP transgene specifically targets gene expression to lymphoid cells. The Rag2: myc-GFP transgene was micro-injected into wild-type zebrafish embryos at the one-cell development stage, and a small fraction of injected embryos developed c-myc induced leukemia. We treated GFP-labeled leukemia cells in zebrafish with either DMSO (Fig. 5A at day 0 and 5D at day 5); aurone 5a in DMSO (Fig. 5B at day 0 and 5E at day 5); or aurone 5b in DMSO (Fig. 5C at day 0 and 5 F at day 5). Since aurone 5a had auto-fluorescence that interfered with visualizing the loss of the GFP-labeled leukemia cells (Fig. 5E), we selected aurone 5b that lacked this auto-fluorescence and clearly displayed the loss of the GFP-labeled leukemia cells (Fig. 5F). Aurone 5a and 5b significantly blocked the progression of T-ALL in zebrafish (Fig. 5D versus 5F, Fig. 5G).
Aurones 5a and 5b inhibited myc-induce T-ALL in a zebrafish model. (A,D) Treatment of GFP-labeled thymic lymphoma cells with DMSO alone at day 0 and day 5, respectively. (B,E) Treatment of GFP-labeled thymic lymphoma cells with aurone 5a in DMSO at day 0 and day 5, respectively. (C,F) Treatment of GFP-labeled thymic lymphoma cells with aurone 5b at day 0 and day 5, respectively. (G) Percent change in fluorescence (i.e., number of GFP-labeled thymic lymphoma cells) as a function of time from administration of DMSO alone to the administration of aurone 5b in each zebrafish (n = 8).
Interaction of aurone 5a with potassium channel derived from human ether-a-go-go related gene (hERG)
Inhibition of the hERG potassium channel derived from hERG often leads to drug failure in preclinical studies or even in clinical trials. We utilized a well-established [3H]-dofetilide binding assay48 to evaluate the interaction of aurones with hERG. [3H]-Dofetilide competition binding assays using HEK-293 cell membranes stably expressing the hERG channel (hERG-HEK) correlated well with results from voltage-clamp assays and provided useful predictive screening assays for QT prolongation49. Amitriptyline (final concentration, 1 mM) was used as the positive control and exhibited an IC50 value (10.7 ± 2.25 μM) in agreement with published values50. Concentrations of aurones 5a and 5b ranging from 10−9 to 10−4 M were assayed in duplicate for these experiments (n = 3 experiments/analog). As desired, aurones 5a and 5b displayed no hERG inhibition (IC50 values > 100 μM).
Discussion
Two types of inhibitors target tubulin microtubule dynamics: stabilizing agents, such as paclitaxel, and destabilizing agents, such as the Vinca alkaloids and colchicine. These agents bind tubulin subunits at well-characterized, binding sites, some of which find broad application in cancer therapeutics, including prostate cancer. Until recently, few agents were known that targeted the colchicine-binding site, but various pharmacophores25,26,27,28,29,30,31 now appear to exhibit excellent potency and selective binding to the colchicine-tubulin site. The impetus for developing these agents derives in part from the continuing need for new tubulin-targeting drugs to meet the needs of patients experiencing resistance or developing mutations crippling the use of traditional taxol or Vinca-based therapies. The semisynthetic aurones reported here provide a new pharmacophore for the development of colchicine-targeting microtubule inhibitors for cancer treatment.
Prior reports that naturally occurring aurones, such as sulfuretin (1a) and aureusidin (1b) (Fig. 1A), and several semisynthetic aurones possessed in vitro antineoplastic activity encouraged our interest in exploring SAR relationships within the aurone pharmacophore. A straightforward condensation of 6-hydroxybenzofuran-3(2H)-one (2) with various aryl or heteroaryl carboxaldehydes 3 furnished aurones 4 in which the C-2 benzylidine groups were either substituted with or replaced by heterocycles (Fig. 1B). Using a PC-3 cell proliferation assay as a readout, we found that the aurones 4a-4e bearing nitrogen-containing heterocycles at C-2 were marginally active in a 1–10 μM concentration range (Table 1). Alkylation of the C-6 hydroxyl group in concert with alterations in the C-2 heteroarylmethylene subunit led ultimately to two aurones 5a and 5b (Fig. 1C) with IC50 values of 58.7 ± 1.1 nM and 66 ± 1.1 nM, respectively (Fig. 2A). The pairing of the unusual cyanomethoxy group at C-6 with the (N-ethyl-5-methoxy-1H-indol-3-yl)methylene at C-2 in aurone 5a and the pairing of the 2,6-dichlorobenzyloxy group at C-6 with the (pyridin-4-yl)methylene at C-2 in aurone 5b were essential to achieve nanomolar potency.
In addition to these in vitro studies, we evaluated the in vivo tumor inhibitory effect of aurone 5a using prostate cancer PC-3 xenografts in immune-defective nude mice. Compared to vehicle, the administration of aurone 5a at 10 mg/kg/day showed significant, tumor-growth suppression (Fig. 2B). Importantly, aurone 5a achieved tumor regression with no apparent gross toxicity as reflected by minimal changes in mice weights (Fig. 2C). IHC staining suggested that aurone 5a treatment induced apoptosis and decreased angiogenesis in the xenografted tumors (Fig. 2E,F), which is consistent with the function other microtubule inhibitors51. In summary, SAR studies identified aurone 5a that possessed good in vitro activity in cancer cell proliferation studies in the nanomolar range, good reduction in tumor volume in an in vivo prostate PC-3 xenograft study, and minimal gross toxicity based on minimal weight loss during the in vivo studies. Preliminary indications involving the minimal effects on normal cell proliferation, the minimal changes in mice weights during xenograft studies, the absence of hERG inhibition and absence of toxic effects on zebrafish in studies, as described below, suggested that aurone 5a had an acceptable “toxicity window” that was sufficient to warrant further study.
Knowledge about the binding site between a ligand and its biological target is pivotal for structure-guided, rational design of compounds with improved properties including potency and solubility. Molecular docking studies showed that aurone 5a binds to the colchicine-binding site between the α-tubulin and β-tubulin. The indole moiety and part of the benzofuran-3-one of aurone 5a as well as the A and B rings of colchicine occupied a hydrophobic pocket in β-tubulin (Fig. 4C,E). However, aurone 5a did not occupy another hydrophobic pocket in which the colchicine C ring normally resided. Instead, aurone 5a interacted more with α-tubulin than β-tubulin and participated in bifurcated hydrogen-bonding between the nitrogen of the cyanomethoxy group and αTyr224 and αGln11 of α-tubulin (Fig. 4D). The relatively inactive aurone 4d failed to form this same interaction because it lacked a cyanomethyl group.
To confirm that aurone 5a bound to the colchicine-binding site, we performed a tubulin polymerization assay and a competitive tubulin-binding assay42. Aurone 5a inhibited tubulin polymerization in vitro (Fig. 3D). In addition, aurone 5a bound to the CBS, resulting in an increased amount of unbound colchicine (Fig. 3E). These data were consistent with molecular docking results, and echoed the fact that the CBS would accommodate chemically diverse compounds. Mechanistically, previous crystallography studies show that free tubulin dimers are in a “straight” state and polymerized tubulin dimers in microtubules are in a “curved” conformation45,52,53,54. During tubulin polymerization, tubulin dimers structurally transitioned from a straight state to a curved state, during which the T7 loop of β-tubulin flipped inwards into the CBS. As a mechanism of action, colchicine bound to the CBS, prevented the T7 loop flipping towards the CBS, and thus inhibited tubulin polymerization53,55. Importantly, our leading compounds showed strong interaction with T7 loop (Fig. 4C,E) and reflected a similar mechanism of action seen with colchicine. As a result, aurone 5a strongly inhibited cell cycle progression at G2/M phases (Fig. 3A,B) and disrupted microtubule networks in PC-3 cells (Fig. 3F–H).
By testing the efficacy of aurone 5a in the NCI-60 and other cell lines, we found that 5a demonstrated broad-spectrum, anticancer activity (Fig. 2A, Tables 2–4). The NCI/ADR-RES cell line that was normally resistant to adriamycin and many other cancer chemotherapeutics due to the expression of P-glycoprotein exhibited inhibition by aurone 5a, and hence, aurone 5a was not a likely substrate of P-glycoprotein. As previously noted, aurone 5a showed no general toxicity in nude mice at doses that significantly inhibited PC-3 tumor xenografts (Fig. 2C). We also tested aurones 5a and 5b in zebrafish models where we again observed no gross toxicity on zebrafish but observed significant inhibition of myc-induced T-ALL in vivo (Fig. 5). The zebrafish myc-induced T-ALL model could be an important in vivo tool to screen and characterize future aurone analogs.
In summary, we identified two potent, semisynthetic aurones 5a and 5b that function as tubulin inhibitors with IC50 values of 58.7 ± 1.1 nM and 66 ± 1.1 nM, respectively (Fig. 2A). Importantly, aurone 5a displayed activity in an in vivo PC-3 prostate cancer xenograft model in nude mice at 10 mg/kg without affecting mice weight (Fig. 2B,C). Aurones 5a and 5b showed potent in vivo activity in a genetically well-defined, zebrafish myc-induced T-ALL leukemia model46,47 (Fig. 5). Aurone 5a also displayed no appreciable affinity for human hERG potassium channel and was not a substrate of P-glycoprotein. An analysis of screening data from the NCI-60 human tumor cell lines using the COMPARE algorithm41 matched the response to aurone 5a with other tubulin-polymerization inhibitors. We used combination of experimental studies to examine this prediction: a competition study of colchicine and aurone 5a for the colchicine-binding site on tubulin (Fig. 3E), a study of the comparative inhibition of tubulin polymerization with aurone 5a and colchicine (Fig. 3D), and detailed computational modeling of the binding of these agents to tubulin (Fig. 4). Liquid chromatography-electrospray ionization-tandem mass spectrometry studies further confirmed that aurone 5a targeted the colchicine-binding site on tubulin. Continued studies will define the pharmacokinetic and pharmacodynamics properties of aurones in this family.
Chemistry Materials and Methods
Chemicals were purchased from Sigma-Aldrich (St. Louis, MO) or Fisher Scientific (Pittsburgh, PA) unless otherwise noted or were synthesized according to literature procedures. Solvents were used from commercial vendors without further purification unless otherwise noted. Nuclear magnetic resonance spectra were determined on Varian instruments (1H, 400 or 500 MHz; 13C, 100 or 126 Mz). Low-resolution mass spectra were obtained using an Agilent 1100 (atmospheric pressure, chemical ionization) instrument. High resolution mass data were obtained by direct infusion electrospray ionization mass spectrometry (-MS) using a LTQ-Orbitrap mass spectrometer coupled with a Heated Electrospray Ionization (HESI-II) Probe (Thermo Fisher Scientific, Waltham, MA) and an FT analyzer at a resolution of 100,000. The reported m/z mass was a mean of 20 scans. Melting points were determined in open capillarity tubes with a Buchi B-535 apparatus and are uncorrected. Compounds were purified by chromotography on preparative layer Merck silica gel F254 unless otherwise noted.
General procedure for the synthesis of aurones 3a-3f and 4a-4o
To a suspension of 10 mmol of 6-hydroxybenzofuran-3(2H)-one (2) (Ark Pharm, Arlington Heights, IL USA) in 20 mL of a 1:1 mixture of DMF and absolute ethanol was added 2.3 mL of 50% aqueous potassium hydroxide. To this clear solution, obtained after stirring for ca. 30 min, was added 10 mmol of the appropriate carboxaldehyde. The mixture was stirred for 6–8 h at 25 °C. The mixture was diluted with 100 mL of hot water, acidified with glacial acetic acid pH 5. The resulting precipitate was collected by filtration, washed with water, dried and re-crystallized from DMF-methanol.
(2Z)-6-Hydroxy-2-(isoquinolin-1-ylmethylene)-1-benzofuran-3(2H)-one (4a)
Yellow crystals (78% yield); mp > 220 °C; 1H NMR (400 MHz, DMSO-d6) δ 6.71–6.76 (m, 2H), 7.43 (s, 1H), 7.69 (d, J = 8.3 Hz, 1H), 7.7–7.77 (m, 1H), 7.79–7.85 (m, 1H), 7.87 (d, J = 5.6 Hz, 1H), 8.03 (d, J = 8.1 Hz, 1H), 8.35 (d, J = 8.9 Hz, 1H), 8.69 (d, J = 5.6 Hz, 1H), 11.3 ppm (s, 1H); 13C NMR (100 MHz, DMSO-d6) δ 98.78, 105.12, 112.39, 113.23, 120.99, 125, 126.42, 127.44, 128.25, 130.59, 135.8, 142.65, 149.81, 151.34, 167.15, 169.05, 182.01 ppm; MS (ACPI) m/z 290.2 (MH+, 100); HRMS (ESI/HESI) m/z: [M + H]+ Calcd for C18H11NO3 290.0812; Found 290.0810.
(2Z)-6-Hydroxy-2-(quinolin-2-ylmethylene)-1-benzofuran-3(2H)-one (4b)
Yellow crystals (72% yield); mp 249–251 °C; 1H NMR (400 MHz, DMSO-d6) δ 6.75 (dd, J = 8.4, 2 Hz, 1H), 6.78–6.9 (m, 2H), 7.56–7.73 (m, 2H), 7.75–7.88 (m, 1H), 7.93–8.13 (m, 2H), 8.29 (d, J = 8.7 Hz, 1H), 8.48 (d, J = 8.7 Hz, 1H), 11.39 ppm (s, 1H); 13C NMR (126 MHz, DMSO-d6) δ 98.84, 110, 112.29, 113.41, 122.62, 126.29, 126.88, 127.47, 127.79, 129.08, 130.11, 136.72, 147.82, 149.55, 151.88, 167.13, 168.36, 181.53 ppm; MS (ACPI) m/z 290.0 (MH+, 100); HRMS (ESI/HESI) m/z: [M + H]+ Calcd for C18H11NO3 290.0812; Found 290.0806.
(2Z)-6-Hydroxy-2-[(8-methoxyquinolin-2-yl)methylene]-1-benzofuran-3(2H)-one (4c)
Yellow crystals (68% yield); mp 250–252 °C; 1H NMR (400 MHz, DMSO-d6) δ 4 (s, 3H), 6.75 (dd, J = 8.5, 2 Hz, 1H), 6.81 (s, 1H), 6.85 (d, J = 2 Hz, 1H), 7.09–7.30 (m, 1H), 7.45–7.62 (m, 2H), 7.67 (d, J = 8.5 Hz, 1H), 8.3 (d, J = 8.7 Hz, 1H), 8.42 (d, J = 8.7 Hz, 1H), 11.38 ppm (s, 1H); 13C NMR (100 MHz, DMSO-d6) δ 55.75, 98.59, 109.12, 110.09, 112.2, 113.21, 119.05, 122.67, 125.9, 127.71, 127.77, 136.19, 139.81, 149.11, 150.13, 155.13, 166.87, 168.12, 181.22 ppm; MS (ACPI) m/z 320.0 (MH+, 100); HRMS (ESI/HESI) m/z: [M + H]+ Calcd for C19H13NO4 320.0917; Found 320.0919.
(2Z)-2-[(1-Ethyl-5-methoxy-1H-indol-3-yl)methylene]-6-hydroxy-1-benzofuran-3(2H)-one (4d)
Yellow crystals (77% yield); mp 265–267 °C; 1H NMR (400 MHz, DMSO-d6); δ 1.39 (t, J = 7.2 Hz, 3H), 3.85 (s, 3H), 4.27 (q, J = 7.2 Hz, 2H), 6.72 (dd, J = 8.4, 2 Hz, 1H), 6.83 (d, J = 2 Hz, 1H), 6.87 (dd, J = 8.9, 2.4 Hz, 1H), 7.23 (s, 1H), 7.42 (d, J = 8.8 Hz, 1H), 7.56–7.64 (m, 2H), 8.18 (s, 1H), 10.98 ppm (s, 1H); 13C NMR (126 MHz, DMSO-d6); δ 15.38, 41.3, 55.46, 98.49, 101.1, 105.37, 107.42, 111.41, 112.56, 112.76, 114.38, 125.36, 128.22, 130.74, 133.5, 144.76, 155.02, 165.47, 166.52, 180.12 ppm; MS (ACPI) m/z 336.0 (MH+, 100); HRMS (ESI/HESI) m/z: [M + H]+ Calcd for C20H17NO4 336.1230; Found 336.1224.
(2Z)-6-Hydroxy-2-(4-pyrrolidin-1-ylbenzylidene)-1-benzofuran-3(2H)-one (4e)
Yellow crystals (83% yield); mp > 220 °C; 1H NMR (400 MHz, DMSO-d6) δ 1.83–2.07 (m, 4H), 3.26–3.32 (m, 4H), 6.61 (d, J = 8.9 Hz, 2H), 6.66–6.72 (m, 2H), 6.77 (d, J = 1.9 Hz, 1H), 7.57 (d, J = 8.4 Hz, 1H), 7.77 (d, J = 8.9 Hz, 2H), 11 ppm (s, 1H); 13C NMR (100 MHz, DMSO-d6) δ 24.95, 47.24, 98.42, 111.97, 112.58, 112.94, 113.69, 118.62, 125.39, 133.16, 144.73, 148.49, 165.58, 166.87, 180.64 ppm; MS (ACPI) m/z 308.1 (MH+, 100); HRMS (ESI/HESI) m/z: [M + H]+ Calcd for C19H17NO3 308.1281; Found 308.1279.
(Z)-2-((2-((1-Ethyl-5-methoxy-1H-indol-3-yl)methylene)-3-oxo-2,3-dihydrobenzofuran-6-yl)oxy)acetonitrile (5a)
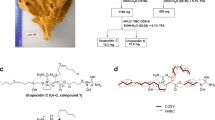
To a solution of 670 mg (2 mmol) of (2Z)-2-[(1-ethyl-5-methoxy-1H-indol-3-yl)methylene]-6-hydroxy-1-benzofuran-3(2H)-one (4d) in 10 mL of DMF was added 830 mg (6 mmol, 3 eq) of anhydrous potassium carbonate. The mixture was heated to 60 °C and 0.152 mL (2.4 mmol, 1.2 eq) of chloroacetonitrile was added. The mixture was stirred at 60 °C for an additional 8 h, cooled, and poured into 100 mL of 0.1 N aqueous sulfuric acid. The precipitate was collected by filtration, washed with water, dried and re-crystallized from DMF-methanol to afford 487 mg (65%) of 5a as yellow crystals: mp 230–232 °C; 1H NMR (400 MHz, DMSO-d6) δ 1.44 (d, J = 7.2 Hz, 3H), 3.86 (s, 3H), 4.33 (q, J = 7.2 Hz, 2H), 5.39 (s, 2H), 6.9 (dd, J = 8.9, 2.4 Hz, 1H), 6.97 (dd, J = 8.6, 2.2 Hz, 1H), 7.29 (d, J = 2.2 Hz, 1H), 7.37 (s, 1H), 7.51 (d, J = 8.9 Hz, 1H), 7.63 (d, J = 2.4 Hz, 1H), 7.77 (d, J = 8.6 Hz, 1H), 8.23 ppm (s, 1H); 13C NMR (100 MHz, DMSO-d6) δ 14.67, 40.97, 53.89, 55.34, 98.17, 101.45, 106.18, 107.17, 110.99, 111.68, 112.46, 115.45, 116.87, 124.84, 127.89, 130.8, 133.46, 144.2, 154.96, 162.6, 165.49, 179.58 ppm; MS (ACPI) m/z 375.2 (MH+, 100); HRMS (ESI/HESI) m/z: [M + H]+ Calcd for C22H19N2O4 375.1339; Found 375.1337.
(2Z)-6-[(2,6-Dichlorobenzyl)oxy]-2-(pyridin-4-ylmethylene)-1-benzofuran-3(2H)-one (5b)
To a solution of 1.5 g (10 mmol) of 6-hydroxybenzofuran-3(2H)-one (2) in 30 mL of DMF was added 4.14 g (30 mmol, 3 eq) of anhydrous potassium carbonate followed by 2.35 g (12 mmol, 1.2 eq) of 2,6-dichlorobenzyl chloride (Thermofisher Acros Organics, Geel, Belgium). The mixture was stirred at 25 °C for 8 h and diluted with 200 mL of water. The precipitate was collected, washed with water, dried and purified by column chromatography using 1:100 dichloromethane-methanol to afford 1.79 g (58%) of 6-((2,6-dichlorobenzyl)oxy)benzofuran-3(2H)-one as pale yellow crystals: mp 153–155 °C. 1H NMR (400 MHz, CDCl3) δ 4.64 (s, 2H), 5.34 (s, 2H), 6.67–6.77 (m, 2H), 7.29 (d, J = 7.2 Hz, 1H), 7.33–7.42 (m, 2H), 7.58 (d, J = 9 Hz, 1H); 13C NMR (100 MHz, CDCl3) δ 65.57, 75.56, 97.32, 111.98, 114.76, 125.15, 128.56, 130.9, 130.96, 136.97, 167.18, 176.32, 197.49 ppm; MS (ACPI) m/z 309.2 (MH+, 100). To 50 mL of a freshly prepared 0.2 M (5 eq) solution of sodium methoxide was added a solution of 618 mg (2 mmol) of 6-((2,6-dichlorobenzyl)oxy)benzofuran-3(2H)-one and 214 mg (2 mmol, 1 eq) of 4-pyridinecarboxaldehyde in 5 mL of methanol. The mixture was stirred at 25 °C for 12 h. The solution was concentrated and poured into 100 mL of water at 0 °C. The mixture was acidified with 1N aqueous hydrochloric acid solution to ca. pH 6. The precipitate was collected by filtration and recrystallized from 2:1 DMF-methanol to afford 445 mg (56%) of 5b: mp 219–222 °C; 1H NMR (400 MHz, CDCl3) δ 5.41 (s, 2H), 6.7 (s, 1H), 6.88 (dd, J = 8.6, 2.2 Hz, 1H), 6.96 (d, J = 2.2 Hz, 1H), 7.28–7.36 (m, 1H), 7.36–7.45 (m, 2H), 7.68–7.78 (m, 3H), 8.7 ppm (d, J = 5.2 Hz, 2H); 13C NMR (126 MHz, CDCl3) δ 66.04, 98, 108.3, 113.23, 114.8, 124.74, 126.45, 128.78, 130.92, 131.17, 137.19, 139.95, 150.3, 150.36, 167.19, 168.85, 182.73 ppm; MS (ACPI) m/z 398.0 (MH+, 100); HRMS (ESI/HESI) m/z: [M + H]+ Calcd for C21H13Cl2NO3 398.0345; Found 398.0349.
Biological Studies
PC-3, MCF-7 and A549 cells were cultured in the medium recommended by American Type Culture Collection at 37 °C with 5% CO2 atmosphere in a water jacketed incubator (NuAire). Ovcar-8 and NCI/ADR-RES cells were gifts from Dr. Markos Leggas, University of Kentucky, Lexington, KY USA. The beta-tubulin antibody was from Developmental Studies Hybridoma Bank. (Iowa city, IA USA).
Cell proliferation inhibition assay
Cancer cells were seeded into 24-well plates at a density of 20,000 cells per well in 1 mL of culture medium and were cultured overnight at 37 °C. Compounds and the vehicle control (DMSO) were added to the cells. After 6 days, the medium was removed, and 100 µL of trypsin was added. The cells were re-suspended in phosphate-buffered saline (PBS) and were counted by Vi-CELL XR 2.03 (Beckman Coulter, Inc. USA). The ratio R of the number of viable cells in the compound treatment group to the number of viable cells in DMSO treatment group was taken as relative growth, and the percentage growth inhibition was calculated as (1 − R)*100. For initial testing, compounds were added to the cells at a final concentration of 10 µM. Active compounds at 10 µM were tested at lower concentrations than 10 µM.
In vitro tubulin polymerization assay
An in vitro tubulin polymerization assay was performed using a protocol from Cytoskeleton, Inc. (Denver, CO USA). Tubulin powder (Cytoskeleton Inc. Denver, CO USA) was dissolved in a buffer prepared from 100 mM PIPES (pH 6.9), 2 mM MgCl2, 1 mM GTP, and 5% glycerol at 0 °C. Aliquots (80 µL, 3.75 µg/µL) of this tubulin solution were divided into the wells of a 96-well half-area plate (Corning Inc., NY USA). After adding either DMSO or testing compounds, the plate was mounted on a Spectra MRTM microplate spectrophotometer equipped with a thermal controller at 37 °C (Dynex Technologies, Inc., Chantilly, VA USA). Readings at 350 nm were recorded every 30 s for 1 h.
In vivo microtubule assembly assay
The amount of insoluble polymerized microtubules and soluble tubulin dimers in cells after exposure to aurones were detected using a reported method. Cells were seeded in 6-well plates at 50% confluency and cultured overnight. DMSO or aurones in DMSO solution were added, and the cells were incubated for additional 6 h. The medium was removed, and cells were washed with PBS three times followed by the addition of a lysis buffer prepared from 20 mM Tris-HCl (pH 6.8), 1 mM MgCl2, 2 mM EGTA, 20 µg/mL aprotinin, 20 µg/mL leupeptin, 1 mM PMSF, 1 mM orthovanadate, and 0.5% NP40. The lysates were centrifuged at 12,000 g for 10 min to obtain supernatants and pellets that were mixed with loading buffer and heated to 100 °C. Standard western blotting against α-tubulin was performed as described previously56.
Immunofluorescence imaging
Tubulin networks were examined by confocal immunofluorescence imaging. Briefly, PC3 cells were placed at a density of 80,000/mL to 24-well plates equipped with round microscope glass cover slides. After culturing at 37 °C for 24 hours, DMSO or compounds were added to the cells and incubated for additional 6 hours. Then the medium was removed and the cells were washed with PBS three times. Primary anti-α-tubulin antibody was added and incubated overnight at 4 °C. After additional washing, secondary TRITC-conjugated anti-rabbit antibody was added for 40 min, followed by additional washing and staining with DAPI. Final washing was performed and the cover slides were inverted onto glass slides. Images (40x) were taken using a Nikon confocal microscope with excitation at 557 nm and emission at 576 nm.
Molecular docking studies
An X-ray crystal structure of αβ-tubulin binding with colchicine (pdb: 4O2B) was downloaded from RCSB Protein Data Bank and manipulated using AutoDockTools-1.5.6 (Molecular Graphics Laboratory, The Scripps Research Institute, La Jolla, CA 92037 USA).The αβ-Tubulin dimer was separated from 4O2B using PyMOL (Version 1.7.4.5 Edu). Water molecules were removed, and polar hydrogens and Kollman charges were added. The docking pocket (colchicine-binding site) was defined as follows: Search space: 18 × 18 × 18 Å3; Center_x, y, z = 14.815, 9.422, −20.186. The aurones 4d, 5a, and colchicine were manipulated by Openbabel. Molecular docking of 4d, 5a, and colchicine to the colchicine-binding site was executed using AutoDock vina-1.1.2 using the iterated gradient-based local search method with a Broyden–Fletcher–Goldfarb–Shanno (BFGS) method for local optimization43. Exhaustiveness was set at 14 and the number of modes was nine. Other parameters were left at default values.
hERG binding studies
An HEK-293 cell line stably expressing the hERG potassium channel (accession number U04270) referred to as hERG-HEK cells were received at passage 11 (P11) from Millipore (CYL3006, lot 2, Billerica, MA USA). [3H]-Dofetilide (specific activity of 80 Ci/mmol; labeled on the N-methyl group) was obtained from American Radiolabeled Chemicals, St. Louis, MO USA). Other chemicals and solvents were obtained from Sigma-Aldrich (Milwaukee, WI USA) with exceptions of polyethylenimine (PEI), which was obtained from Fluka/Sigma-Aldrich (St. Louis, MO USA), and Minimium Essential Medium (MEM) with GlutaMAXTM and phenol red, MEM non-essential amino acids solution (NEAA, 100X), G418 disulfate salt solution, fetal bovine serum (FBS), 0.05% Trypsin-EDTA 1X with phenol red, and Hank’s balanced salt solution (HBSS), which were obtained from Life Technologies (Carlsbad, CA USA).
hERG-HEK Cell Culture
The hERG-HEK cells were cultured according to the protocol provided by Merck Millipore (Burlington, MA USA). Cells were maintained in MEM (with glutamax and phenol red) supplemented with 10% FBS, 1% NEAA and 400 μg/ml geneticin, and incubated at 37 °C in a humidified atmosphere with 5% CO2. Frozen aliquots of cells were transferred into T-75 cm2 flasks and allowed to adhere for 4–8 h. The medium was replaced every 2 days. Passages were carried out at least 3 times after thawing at 6 day intervals. Cells were dissociated with trypsin/EDTA and seeded into new 150 × 25 mm dishes at 2–3 × 106 cells per dish and placed at 30 °C, 5% CO2, for 40–48 h prior to membrane preparation. Membrane preparation occurred 6 days after the last passage (passage 20).
Membrane preparation
Cell membrane preparation was based on previous methods49,50,57. Cells were rinsed twice with HBSS at 37 °C and collected by scraping the dishes in ca. 20 mL of ice-cold 0.32 M sucrose and homogenized on ice with a Teflon pestle using a Maximal Digital homogenizer (Fisher Scientific, Pittsburgh, PA USA) at ~280 rpm for 30 sec. Homogenates were centrifuged at 300 g and 800 g for 4 min each at 4 °C. Pellets were resuspended in 9 mL of ice-cold Milli-Q water and osmolarity restored by addition of 1 mL of 500 mM Tris buffer (pH 7.4) followed by suspension and centrifugation at 20,000 g for 30 min at 4 °C. Pellets were homogenized in 2 mL assay buffer (50 mM Tris, 10 mM KCl, and 1 mM MgCl2, 4 °C) and aliquots of cell membrane suspensions were stored at −80 °C and thawed the day of the [3H]-dofetilide binding assay. Protein content was determined prior to the assay using a Bradford protein assay with bovine albumin as the standard.
[3H]-Dofetilide binding assay
[3H]-Dofetilide binding assays using hERG-HEK293 cell membranes were based on previous methods. Assays determining concentration-response were performed in duplicate, and three independent assays were performed for each analog evaluated. Cell membrane suspension (5 μg) was added to duplicate tubes containing assay buffer, 25 μL of a single concentration of FIDAS agent (concentration range of 10 nM-100 µM for each experiment), and 25 μL of [3H]-dofetilide (5 nM, final concentration) for an assay volume of 250 μL. Binding occurred for 60 min at 25 °C and was terminated by rapid filtration through Whatman GF/B filters, which were pre-soaked in 0.25% PEI overnight, using a Brandel cell/membrane harvester (M-48; Brandel Inc., Gaithersburg, MD USA). Filters were washed three times with ca. 1 mL of ice-cold assay buffer. Radioactivity was determined by liquid scintillation spectrometry using the Tri-Carb 2100-TR Liquid Scintillation Analyzer (Perkin-Elmer Life and Analytical Sciences).
In vivo evaluation of anti-leukemia activity in the zebrafish model
Zebrafish studies were carried out with approval from the Institutional Animal Care and Use Committees of the University of Kentucky (2015–2225). All methods were performed in accordance with the relevant guidelines and regulations according to protocols. Rag2: myc-GFP zebrafish (n = 8) at 21 days of age were treated with DMSO, either aurones 5a or 5b in 1.5 mL of fish-system water in 12-well plates. Zebrafish were treated with compound for 2 days, removed from drug for 1 day, and treated for two more days with freshly prepared solutions of compound. Animals were imaged at the start and end of treatment using a fluorescence-equipped dissecting microscope at 350 ms exposure. The GFP image was overlaid onto the bright-field image of each animal in Photoshop, and the percent change in leukemia burden was calculated by normalizing the GFP+ area to the total area of the animal in ImageJ (National Institute of Health, USA).
In vivo evaluation of anti-cancer activity and gross toxicity in PC-3 xenografts
Mouse studies were carried out with approval from the Institutional Animal Care and Use Committees of the University of Kentucky (2009–1064). All methods were performed in accordance with the relevant guidelines and regulations according to protocols. PC-3 cells suspended in PBS were subcutaneously injected in the lower flanks of immune-deficient nude mice (5 mice in each group, two tumors on each mouse) at a density of 2 × 106 cells in 200 μL of PBS. After tumors were established (in about two weeks), aurone 5a formulated in a mixture of Tween-80 (5%), DMSO (10%), PEG400 (25%) and PBS (60%) was intraperitoneally administered to mice at a daily dose of 10 mg of aurone 5a/kg (mouse). The first day of treatment was set as day 1. At day 18 treatment was ceased and mice were sacrificed. Blank vehicle was used as a control. Tumors and mouse weights were measured, and tumor volumes were calculated as Length × width2/2. For H&E and IHC studies, the tumors were treated with vehicle and aurone 5a for 1 week. H&E and TUNEL staining was performed based on standard protocol by the Markey Cancer Center Biospecimen Procurement & Translational Pathology Shared Resource Facility (BPTP SRF) at the University of Kentucky. For IHC staining, the following antibody was used: anti- VEGF-A (Santa Cruz, sc-152, 1:100).
Competitive tubulin binding assay and Liquid Chromatography-Electrospray Ionization-Tandem Mass Spectrometry (LC-ESI-MS/MS) method
Competitive tubulin binding assay was performed as described to demonstrate that aurones bind to the colchicine-binding site of tubulins. The colchicine quantification was performed at the University of Kentucky Proteomics Core using a protocol modified from a previously published method. LC-MS/MS analysis was carried out using an TSQ Vantage mass spectrometer (Thermo Fisher Scientific, Waltham, MA USA) coupled with a Shimadzu high performance liquid chromatography (HPLC) system (Shimadzu Scientific Instruments, Inc., Columbia, MD USA) through an electrospray ionization source. The colchicine-containing samples were separated with a Kinetex® reversed phase 2.6 μm XB-C18 100 Å LC column (100 × 4.6 mm) (Phenomenex Inc., Torrance, CA USA) at a flow rate of 300 μL/min. Mobile phase A was water with 0.1% (v/v) formic acid while mobile phase B was acetonitrile with 0.1% (v/v) formic acid. A 16 min gradient condition was applied: initial 60% mobile phase B was increased linearly to 100% in 3 min, remained 100% for 3 min, and quickly (0.01 min) decreased to 60% for re-equilibration. Multiple reaction monitoring (MRM) mode was used to scan from m/z 400 to m/z 310 in the positive mode to obtain the most sensitive signals for colchicine. The spraying voltage was set at 4000 V, vaporize temperature at 300 °C, capillary temperature at 350 °C and sheath gas pressure at 45 (arbitrary units). Collision energies (CE) were set at 25 volts. Xcalibur software (Ver. 2.1.0, Thermo Fisher Scientific, Waltham, MA USA) was used for the data acquisition and quantitative processing. A series of colchicine at concentrations of 20, 40, 80, 200, 400, 800 nM were prepared to establish a linear calibration curve with a coefficient of correlation R2 = 0.9944.
Statistics
Biological assays have been performed at least twice. Data were shown as mean ± SD or the 95% confidence intervals were provided. For the mice study, five mice with two tumors on the lower flanks of each mouse were used in each treatment group. The data for the mouse study were analyzed by t-test. For the zebrafish study, eight fish were used in each treatment group.
Data Availability
The data related to this manuscript during the current study are available from the corresponding authors on reasonable request.
References
Nakayama, T. et al. Specificity analysis and mechanism of aurone synthesis catalyzed by aureusidin synthase, a polyphenol oxidase homolog responsible for flower coloration. FEBS Lett 499, 107–111 (2001).
Boumendjel, A. Aurones: a subclass of flavones with promising biological potential. Curr Med Chem 10, 2621–2630 (2003).
Zwergel, C. et al. Aurones: interesting natural and synthetic compounds with emerging biological potential. Nat Prod Commun 7, 389–394 (2012).
Haudecoeur, R. & Boumendjel, A. Recent advances in the medicinal chemistry of aurones. Curr Med Chem 19, 2861–2875 (2012).
Liu, H. L., Jiang, W. B. & Xie, M. X. Flavonoids: recent advances as anticancer drugs. Recent Pat Anticancer Drug Discov 5, 152–164 (2010).
Cheng, H. et al. Design, synthesis and discovery of 5-hydroxyaurone derivatives as growth inhibitors against HUVEC and some cancer cell lines. Eur J Med Chem 45, 5950–5957, https://doi.org/10.1016/j.ejmech.2010.09.061 (2010).
Zheng, X., Cao, J. G., Meng, W. D. & Qing, F. L. Synthesis and anticancer effect of B-ring trifluoromethylated flavonoids. Bioorg Med Chem Lett 13, 3423–3427 (2003).
Lawrence, N. J., Rennison, D., McGown, A. T. & Hadfield, J. A. The total synthesis of an aurone isolated from Uvaria hamiltonii: aurones and flavones as anticancer agents. Bioorg Med Chem Lett 13, 3759–3763 (2003).
Hadjeri, M. et al. Modulation of P-glycoprotein-mediated multidrug resistance by flavonoid derivatives and analogues. J Med Chem 46, 2125–2131, https://doi.org/10.1021/jm021099i (2003).
Sim, H. M., Lee, C. Y., Ee, P. L. & Go, M. L. Dimethoxyaurones: Potent inhibitors of ABCG2 (breast cancer resistance protein). Eur J Pharm Sci 35, 293–306, https://doi.org/10.1016/j.ejps.2008.07.008 (2008).
Sim, H. M., Loh, K. Y., Yeo, W. K., Lee, C. Y. & Go, M. L. Aurones as modulators of ABCG2 and ABCB1: synthesis and structure-activity relationships. Chem Med Chem 6, 713–724, https://doi.org/10.1002/cmdc.201000520 (2011).
Cherigo, L., Lopez, D. & Martinez-Luis, S. Marine natural products as breast cancer resistance protein inhibitors. Mar Drugs 13, 2010–2029, https://doi.org/10.3390/md13042010 (2015).
Boumendjel, A. et al. 4-Hydroxy-6-methoxyaurones with high-affinity binding to cytosolic domain of P-glycoprotein. Chem Pharm Bull (Tokyo) 50, 854–856 (2002).
Boumendjel, A., Di Pietro, A., Dumontet, C. & Barron, D. Recent advances in the discovery of flavonoids and analogs with high-affinity binding to P-glycoprotein responsible for cancer cell multidrug resistance. Med Res Rev 22, 512–529, https://doi.org/10.1002/med.10015 (2002).
Vaclavikova, R., Boumendjel, A., Ehrlichova, M., Kovar, J. & Gut, I. Modulation of paclitaxel transport by flavonoid derivatives in human breast cancer cells. Is there a correlation between binding affinity to NBD of P-gp and modulation of transport? Bioorg Med Chem 14, 4519–4525, https://doi.org/10.1016/j.bmc.2006.02.025 (2006).
Jacobson, K. A., Moro, S., Manthey, J. A., West, P. L. & Ji, X. D. Interactions of flavones and other phytochemicals with adenosine receptors. Adv Exp Med Biol 505, 163–171 (2002).
Gao, Z. G. et al. Structural determinants of A(3) adenosine receptor activation: nucleoside ligands at the agonist/antagonist boundary. J Med Chem 45, 4471–4484 (2002).
Huang, L. et al. New compounds with DNA strand-scission activity from the combined leaf and stem of Uvaria hamiltonii. J Nat Prod 61, 446–450, https://doi.org/10.1021/np9703609 (1998).
Ballinari, D. B, Ermoli, A. G., Moll, M. J. & Vanotti, E. Aurones as telomerase inhibitors (2002).
Smith, C. D., French, K. J. & Yun, J. K. Sphingosine kinase inhibitors (2003).
Bursavich, M. G. et al. Novel benzofuran-3-one indole inhibitors of PI3 kinase-alpha and the mammalian target of rapamycin: hit to lead studies. Bioorg Med Chem Lett 20, 2586–2590, https://doi.org/10.1016/j.bmcl.2010.02.082 (2010).
Schoepfer, J. et al. Structure-based design and synthesis of 2-benzylidene-benzofuran-3-ones as flavopiridol mimics. J Med Chem 45, 1741–1747 (2002).
Lee, C. Y., Chew, E. H. & Go, M. L. Functionalized aurones as inducers of NAD(P)H:quinone oxidoreductase 1 that activate AhR/XRE and Nrf2/ARE signaling pathways: synthesis, evaluation and SAR. Eur J Med Chem 45, 2957–2971, https://doi.org/10.1016/j.ejmech.2010.03.023 (2010).
Westenburg, H. E. et al. Activity-guided isolation of antioxidative constituents of Cotinus coggygria. J Nat Prod 63, 1696–1698 (2000).
Mirzaei, H. & Emami, S. Recent advances of cytotoxic chalconoids targeting tubulin polymerization: Synthesis and biological activity. European journal of medicinal chemistry 121, 610–639, https://doi.org/10.1016/j.ejmech.2016.05.067 (2016).
Ji, Y. T., Liu, Y. N. & Liu, Z. P. Tubulin colchicine binding site inhibitors as vascular disrupting agents in clinical developments. Curr Med Chem 22, 1348–1360 (2015).
Li, W., Sun, H., Xu, S., Zhu, Z. & Xu, J. Tubulin inhibitors targeting the colchicine binding site: a perspective of privileged structures. Future Med Chem 9, 1765–1794, https://doi.org/10.4155/fmc-2017-0100 (2017).
Dong, M., Liu, F., Zhou, H., Zhai, S. & Yan, B. Novel Natural Product- and Privileged Scaffold-Based Tubulin Inhibitors Targeting the Colchicine Binding Site. Molecules 21, https://doi.org/10.3390/molecules21101375 (2016).
Dumontet, C. & Jordan, M. A. Microtubule-binding agents: a dynamic field of cancer therapeutics. Nat Rev Drug Discov 9, 790–803, https://doi.org/10.1038/nrd3253 (2010).
Lu, Y., Chen, J., Xiao, M., Li, W. & Miller, D. D. An overview of tubulin inhibitors that interact with the colchicine binding site. Pharm Res 29, 2943–2971, https://doi.org/10.1007/s11095-012-0828-z (2012).
Bueno, O. et al. High-affinity ligands of the colchicine domain in tubulin based on a structure-guided design. Sci Rep 8, 4242, https://doi.org/10.1038/s41598-018-22382-x (2018).
Zwergel, C. V. et al. benzofuran-chromone and -coumarin derivatives: synthesis and biological activity in K562 human leukemia cells. Med. Chem. Commun. 4, 1571–1579 (2013).
Guo, Q. N., Zhou, L., Yu, Y. & Teng, Y. P. Design, synthesis and biological evaluation of the novel antitumor agent aurone derivatives. Ad. Mat. Res. 781-784, 1235–1239 (2013).
Huang, W., Liu, M. Z., Li, Y., Tan, Y. & Yang, G. F. Design, syntheses, and antitumor activity of novel chromone and aurone derivatives. Bioorg Med Chem 15, 5191–5197, https://doi.org/10.1016/j.bmc.2007.05.022 (2007).
Pathak, N. P. J. Design and synthesis of indole integrated aurones as potent anti breast cancer agents. Ind. J. App. Res. 6, 800–802 (2016).
Okombi, S. et al. Discovery of benzylidenebenzofuran-3(2H)-one (aurones) as inhibitors of tyrosinase derived from human melanocytes. J Med Chem 49, 329–333, https://doi.org/10.1021/jm050715i (2006).
Haudecoeur, R. et al. Discovery of naturally occurring aurones that are potent allosteric inhibitors of hepatitis C virus RNA-dependent RNA polymerase. J Med Chem 54, 5395–5402, https://doi.org/10.1021/jm200242p (2011).
Sheng, R. et al. Design, synthesis and AChE inhibitory activity of indanone and aurone derivatives. Eur J Med Chem 44, 7–17, https://doi.org/10.1016/j.ejmech.2008.03.003 (2009).
Hastings, J. H. H. The stereochemistry of aurones [2-substituted benzylidenebenzofuran-3-(2H)-ones]. J. Chem. Soc., Perkin Trans. 1, 2128–2132 (1972).
King, T. J. H., Heller, J. S. & X-ray, H. G. analysis of (Z)-2-p-methoxyphenylmethylenebenzofuran-3-(2H)-one. J. Chem. Soc., Perkin Trans. 1, 1455–1457 (1975).
Paull, K. D. et al. Display and analysis of patterns of differential activity of drugs against human tumor cell lines: development of mean graph and COMPARE algorithm. J Natl Cancer Inst 81, 1088–1092 (1989).
Li, C. M. et al. Competitive mass spectrometry binding assay for characterization of three binding sites of tubulin. J Mass Spectrom 45, 1160–1166, https://doi.org/10.1002/jms.1804 (2010).
Trott, O. & Olson, A. J. AutoDock Vina: improving the speed and accuracy of docking with a new scoring function, efficient optimization, and multithreading. J Comput Chem 31, 455–461, https://doi.org/10.1002/jcc.21334 (2010).
Sanghai, N. et al. Combretastatin A-4 inspired novel 2-aryl-3-arylamino-imidazo-pyridines/pyrazines as tubulin polymerization inhibitors, antimitotic and anticancer agents. MedChemComm 5, 766–782 (2014).
Lowe, J., Li, H., Downing, K. H. & Nogales, E. Refined structure of alpha beta-tubulin at 3.5 A resolution. J Mol Biol 313, 1045–1057, https://doi.org/10.1006/jmbi.2001.5077 (2001).
Blackburn, J. S. et al. Notch signaling expands a pre-malignant pool of T-cell acute lymphoblastic leukemia clones without affecting leukemia-propagating cell frequency. Leukemia 26, 2069–2078, https://doi.org/10.1038/leu.2012.116 (2012).
Langenau, D. M. et al. Myc-induced T cell leukemia in transgenic zebrafish. Science 299, 887–890, https://doi.org/10.1126/science.1080280 (2003).
Sviripa, V. M. et al. 2′,6′-Dihalostyrylanilines, pyridines, and pyrimidines for the inhibition of the catalytic subunit of methionine S-adenosyltransferase-2. J Med Chem 57, 6083–6091, https://doi.org/10.1021/jm5004864 (2014).
Greengrass, P. M. S. & Wood, M. C. M. Affinity-assay for the human ERG potassium channell (2003).
Jo, S. H., Youm, J. B., Lee, C. O., Earm, Y. E. & Ho, W. K. Blockade of the HERG human cardiac K(+) channel by the antidepressant drug amitriptyline. Br J Pharmacol 129, 1474–1480, https://doi.org/10.1038/sj.bjp.0703222 (2000).
Pasquier, E., Andre, N. & Braguer, D. Targeting microtubules to inhibit angiogenesis and disrupt tumour vasculature: implications for cancer treatment. Curr Cancer Drug Targets 7, 566–581 (2007).
Prota, A. E. et al. The novel microtubule-destabilizing drug BAL27862 binds to the colchicine site of tubulin with distinct effects on microtubule organization. J Mol Biol 426, 1848–1860, https://doi.org/10.1016/j.jmb.2014.02.005 (2014).
Ravelli, R. B. et al. Insight into tubulin regulation from a complex with colchicine and a stathmin-like domain. Nature 428, 198–202, https://doi.org/10.1038/nature02393 (2004).
Ayaz, P., Ye, X., Huddleston, P., Brautigam, C. A. & Rice, L. M. A. TOG:alphabeta-tubulin complex structure reveals conformation-based mechanisms for a microtubule polymerase. Science 337, 857–860, https://doi.org/10.1126/science.1221698 (2012).
Dorleans, A. et al. Variations in the colchicine-binding domain provide insight into the structural switch of tubulin. Proc Natl Acad Sci USA 106, 13775–13779, https://doi.org/10.1073/pnas.0904223106 (2009).
Zhang, W. et al. Fluorinated N, N-dialkylaminostilbenes repress colon cancer by targeting methionine S-adenosyltransferase 2A. ACS Chem Biol 8, 796–803, https://doi.org/10.1021/cb3005353 (2013).
Chen, T. A Practical Guide to Assay Development and High-throughput Screening in Drug Discovery. (CRC Press Taylor and Francis Group, 2010).
Acknowledgements
C.L. and D.S.W. were supported by NIH R01 CA172379. D.S.W. was also supported by the Office of the Dean of the College of Medicine, the Markey Cancer Center, and the Center for Pharmaceutical Research and Innovation (CPRI) in the College of Pharmacy, NIH R21 CA205108 (to J. Mohler), Department of Defense Idea Development Award PC150326P2, and NIH P20 RR020171 from the National Institute of General Medical Sciences (to L. Hersh). The authors also thank the University of Kentucky Proteomics Core mass spectrometric measurements using a LTQ-Orbitrap mass spectrometer that was acquired by NIH grant S10 RR029127 to Professor H. Zhu. This research was also supported by the Flow Cytometry and Cell Sorting Shared Resource Facility of the University of Kentucky Markey Cancer Center (P30CA177558). We thank Markey Biospecimen Procurement & Translational Pathology Shared Resource Facility (BPTP SRF) for processing, H&E and TUNEL staining of the tumor tissues.
Author information
Authors and Affiliations
Contributions
Y.X., L.M.K., M.S.F., S.P.B., K.M.K., P.P.W. and V.M.S., performed chemical synthesis and characterization. Y.X., T.Y., W.Z., E.H., Z.M.M., A.D. and J.C., performed biological analysis. Y.X., T.Y., X.L., L.P.D., H.Z., C.G.Z., J.B., D.S.W. and C.L., analyzed the data. Y.X., D.S.W. and C.L., write the manuscript.
Corresponding authors
Ethics declarations
Competing Interests
C.L. and D.S.W. have partial ownership in a private venture, Epionc Inc., incorporated to develop small-molecule inhibitors for cancer treatment. In accord with University of Kentucky policies, C.L. and D.S.W. have disclosed this work to the University of Kentucky’s Intellectual Property Committee and complied with stipulations of the University’s Conflict of Interest Oversight Committee.
Additional information
Publisher’s note: Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made. The images or other third party material in this article are included in the article’s Creative Commons license, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons license and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this license, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Xie, Y., Kril, L.M., Yu, T. et al. Semisynthetic aurones inhibit tubulin polymerization at the colchicine-binding site and repress PC-3 tumor xenografts in nude mice and myc-induced T-ALL in zebrafish. Sci Rep 9, 6439 (2019). https://doi.org/10.1038/s41598-019-42917-0
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41598-019-42917-0
This article is cited by
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.