Abstract
Metabolic resistance to insecticides is threatening malaria control in Africa. However, the extent to which it impacts malaria transmission remains unclear. Here, we investigated the association between a marker of glutathione S-transferase mediated metabolic resistance and Plasmodium infection in field population of Anopheles funestus s.s. in comparison to the A296S-RDL target site mutation. The 119F-GSTe2 resistant allele was present in southern (Obout) (56%) and central (Mibellon) (25%) regions of Cameroon whereas the 296S-RDL resistant allele was detected at 98.5% and 15% respectively. The whole mosquito Plasmodium and sporozoite infection rates were 57% and 14.8% respectively in Obout (n = 508) and 19.7% and 5% in Mibellon (n = 360). No association was found between L119F-GSTe2 genotypes and whole mosquito infection status. However, when analyzing oocyst and sporozoite infection rates separately, the resistant homozygote 119F/F genotype was significantly more associated with Plasmodium infection in Obout than both heterozygote (OR = 2.5; P = 0.012) and homozygote susceptible (L/L119) genotypes (OR = 2.10; P = 0.013). In contrast, homozygote RDL susceptible mosquitoes (A/A296) were associated more frequently with Plasmodium infection than other genotypes (OR = 4; P = 0.03). No additive interaction was found between L119F and A296S. Sequencing of the GSTe2 gene showed no association between the polymorphism of this gene and Plasmodium infection. Glutathione S-transferase metabolic resistance is potentially increasing the vectorial capacity of resistant An. funestus mosquitoes. This could result in a possible exacerbation of malaria transmission in areas of high GSTe2-based metabolic resistance to insecticides.
Similar content being viewed by others
Introduction
Malaria control in Africa mainly relies on insecticide-based interventions such as long-lasting insecticidal nets (LLINs) and indoor residual spraying (IRS)1. A significant decrease in the incidence of malaria was reported between 2000 and 2015, with about 70% of this success credited to insecticide-based vector control tools1. However, the emergence of insecticide resistance in vector populations resulting from widespread use of insecticides in public health, combined with pesticide use in agriculture, is a major problem that is jeopardizing the control of malaria2. The two main resistance mechanisms are target-site resistance (e.g. knockdown resistance, kdr) and metabolic resistance through over-expression of detoxification genes (e.g. cytochrome P450s, glutathione S-transferases and esterases)3. Insecticide resistance genes are often associated with pleiotropic effects on mosquito life-history traits4,5 which can modify their capacity to transmit parasites to different hosts4,6. The fitness cost of resistant alleles could affect various vector life-history traits, such as adult longevity, biting behavior, and vector competence7, which are important components of the vectorial capacity to transmit pathogens. However, despite the widespread distribution of resistance, its impact on malaria transmission remains unclear in many malaria vectors including Anopheles funestus. This is particularly true for metabolic resistance mechanisms since no molecular markers were previously available to assess such an impact, in contrast to target-site resistance (such as knockdown resistance kdr) for which DNA-based diagnostic tools have been available for many years8.
A better understanding of resistance mechanisms including metabolic resistance and, more importantly, their impact on vector life traits and disease transmission, is essential to design successful resistance management strategies9. A decrease in the ability of resistant mosquitoes to transmit malaria may mean insecticide resistance is not detrimentally impeding the control of this disease7. Conversely, if insecticide resistance increased the ability of resistant mosquitoes to infect humans, this would lead to increased malaria transmission. Only a few studies mostly, in An. gambiae s.s, have investigated the impact of resistance on vectorial capacity4,6,10,11. For example, the study of Kabula et al. (2016) in Tanzania based on the target-site resistance kdr marker11, showed that the infection of field populations of An. gambiae s.s. by Plasmodium parasites was significantly associated with vgsc-1014 point mutations. Insecticide resistance was recently shown to affect the vector competence of this same mosquito species for P. falciparum field isolates as a higher prevalence of infection was observed for mutations associated with insecticide resistance10. The impact of resistance on vectorial capacity has yet to be examined for metabolic resistance which is the most common resistance mechanism in mosquitoes. Metabolic resistance has consistently been reported to be the main driver of pyrethroids and DDT resistance in the malaria vector An. funestus. No kdr mutation has been detected so far in this species12 despite the widespread report of insecticide resistance in An. funestus populations across Africa.
Indeed, pyrethroid resistance has been reported in various An. funestus populations including southern [Mozambique13,14, Malawi15,16], eastern [Uganda and Kenya17,18 and Tanzania19], central [Cameroon20,21], and western Africa [Benin22,23, Ghana24,25, Senegal26 and Nigeria23]. Noticeably, resistance to pyrethroids and DDT in these populations is consistently conferred by detoxification enzymes including glutathione S-transferases (GSTs) and cytochrome P450s. The predominance of metabolic resistance in this species makes it suitable to investigate the impact of metabolic resistance on malaria transmission. The detection of a single amino acid change (L119F) in the glutathione S-transferase epsilon 2 (GSTe2) gene conferring DDT/pyrethroid resistance in An. funestus27, further offers the opportunity to assess this impact. In addition, the presence of target site mutations in An. funestus such as the A296S-RDL associated with dieldrin resistance20 and N485I-Ace1 mutation associated with bendiocarb resistance28 also allows to compare the effect of metabolic resistance to that caused by target-site resistance on vectorial capacity of this vector.
Therefore, to assess the potential impact of metabolic resistance on malaria transmission, we investigated the association between the L119F-GSTe2 metabolic resistance marker and the natural infection of Plasmodium parasites in two pyrethroid and DDT resistant An. funestus populations from Cameroon. We established that the 119F-GSTe2 resistance allele is significantly associated with Plasmodium infection in resistant mosquitoes.
Results
Field collection and mosquito species identification
One thousand blood-fed female mosquitoes were collected in Obout and 1,147 in Mibellon after a week of collection in each site and in at least ten houses randomly selected in each village. Molecular identification of mosquitoes collected in both localities revealed that 95% of the mosquitoes belonged to the An. funestus group. The remaining 5% of mosquitoes were from An. gambiae species complex. Nearly all the An. funestus mosquitoes belonged to An. funestus s.s as only one mosquito belonging to another species of the An. funestus group (An. leesoni) was detected in Mibellon.
Infection rate of An. funestus by Plasmodium parasites
In Obout, a total of 508 females (whole mosquitoes) randomly selected from the field collected individuals were tested for Plasmodium infection. The overall Plasmodium infection rate was very high in this locality with a total prevalence of 57.1% (Fig. 1a). Among the mosquitoes tested, 23% (119/508) were infected with P. falciparum (falcip+), 19% (95/508) were infected with P. ovale/vivax/malariae (OVM+), while 14.7% (76/508) were co-infected with both falcip+ and OVM+ (Table 1). In addition, the head plus thorax and abdomen were analyzed separately in 81 field-collected female mosquitoes to assess the proportion of mosquitoes harboring the infective stage of the parasite (sporozoite) and those having the oocysts. This is because sporozoites are predominantly present in the salivary glands of mosquitoes. TaqMan assay revealed a sporozoite infection rate of 14.8% (12/81) including 9.9% (8/81) falcip+, 2.5% (2/81) falcip+/OVM+ and 2.5% (2/81) OVM+. Oocysts were detected in 30.8%(25/81) mosquitoes including 19.7% (16/81) falcip+, 3.7% (3/81) falcip+/OVM+ and 7.4% (6/81) OVM+. The nested PCR performed on all the infected mosquitoes confirmed all the 16 falcip+ by Taqman (Figure S1a) whereas the three falcip+/OVM+ mosquitoes were co-infected with P. falciparum and P. malariae. Out of 18 OVM+ by Taqman, 14 were infected with P. malariae (Figure S1b) and the four remaining were not confirmed29. This observation indicates that in this locality, P. falciparum, and P. malariae are in circulation.
In Mibellon, out of the 360 whole mosquitoes tested (randomly selected from the total mosquitoes collected), 19.7% (71/360) were infected with Plasmodium parasites including 10.8% (39/360) falcip+, 4.2% (15/360) OVM+ and 4.7% (17/360) co-infection falcip+/OVM+ (Fig. 1b). Among the 60 mosquitoes dissected for head/thorax and abdomen, 20% (12/60) were oocyst-positive and 5% (3/60) sporozoite-positive with 3.3% (2/60) falcip+, 0% (0/60) falcip+/OVM+ and 1.7% (1/60) OVM+. The nested PCR validation of the TaqMan assay for oocyst positive mosquitoes confirmed all the six falcip+ whereas the two co-infected (falcip+/OVM+) were confirmed as P. falciparum and P. malariae-positive. From the four OVM-positive by Taqman assay, two were infected with P. ovale and two with P. malariae showing that P. falciparum, P. ovale (Figure S1c) and P. malariae are all present in Mibellon.
In both locations, a significant difference was found between mosquitoes harboring the oocyst stage of the parasite and those with the infective sporozoite stage (χ2 = 5.82; P = 0.01 in Obout and χ2 = 6.12; P = 0.01 in Mibellon).
Association between L119F-GSTe2 mutation and total Plasmodium infection
In total, 174 whole mosquitoes (infected and uninfected randomly selected from the 508 tested above) from Obout were genotyped for the L119F-GSTe2 mutation (Table 2). All genotypes were successfully detected and later validated by direct sequencing, supporting the robustness of the new designed Allele Specific-PCR assay (Fig. 2a,b). The 119F-GSTe2 resistant allele was found at a frequency of 56.8% when combining both infected and uninfected mosquitoes. For infected mosquitoes, 33.7% were 119F/F homozygous resistant, 47.2% L119F-RS heterozygote, and 19.1% L/L119 homozygote susceptible (Fig. 3a). A similar distribution of the three genotypes was observed for uninfected mosquitoes (x2 = 0.34; P = 0.82) with 31.7% for 119F/F, 49.4% for L119F-RS and 18.8% for L/L119 susceptible genotype. The lack of significant correlation between L119F-GSTe2 genotypes and whole mosquito Plasmodium infection was further supported by odds-ratio estimates (Table 2).
Design of a new AS-PCR for genotyping the L119F-GSTe2 mutation. (a) Amplification by PCR of GSTe2 gene in An. funestus s.s. and an overview of the polymorphism of the GSTe2 gene at the L119F point mutation where Y represents the heterozygote genotype C/T. (b) Agarose gel of AS-PCR to detect the L119F gste2 mutation in An. funestus s.s. Top band 849 bp, fragment common of all genotypes; the middle (523 bp) and the bottom (312 bp), resistant and susceptible mosquitoes respectively; heterozygote mosquitoes, 523 bp and the bottom 312 bp fragments. M: Molecular ladder 100 bp; positive controls (S: homozygous susceptible, R: homozygous resistant and H: heterozygote); N: negative control; 1–15: samples genotyped (1, 6, 10: homozygous resistant; 7, 11: heterozygote; 2–5, 8, 12, 13, 15: homozygous susceptible; 9, 14: no amplification).
Impact of the GSTe2 glutathione S-transferase metabolic resistance (L119F-GSTe2) on the infection and transmission patterns of Plasmodium parasites in natural Anopheles funestus s.s. populations (a,c,d); are whole mosquitoes, oocyst and sporozoite infection respectively in southern Cameroon (Obout); (b,e,f); whole mosquitoes, oocyst and sporozoite infection respectively in Central (Mibellon).
In Mibellon, 184 whole mosquitoes randomly selected out of the 360 field- collected females tested above were successfully genotyped. The overall frequency of 119F-GSTe2 resistant allele was 26.3% in both groups of mosquitoes (infected and uninfected). No difference was found in the distribution of the L119F-GSTe2 genotypes between infected and uninfected mosquitoes (X2 = 0.1 P = 0.95) (Fig. 3b) (Table 2).
Association between L119F-GSTe2 and oocyst and sporozoite infection rates
In Obout, the distribution of L119F-GSTe2 genotypes in mosquitoes found positive for oocysts by TaqMan was as follows: 28% (7/25) homozygous resistant (119F/F), 40% (10/25) heterozygotes (L119F-RS) and 32% (8/25) homozygous susceptible (L/L119F) (Fig. 3c). No significant difference was observed in the distribution of L119F-GSTe2 genotypes between infected and uninfected mosquitoes (X2 = 3.58 P = 0.17) (Table 3). At the sporozoite stage, 50% (6/12) of infected mosquitoes were homozygous resistant, 33% (4/12) were heterozygotes and 17% (2/12) were homozygous susceptible (Fig. 3d) (Table 3). Contrary to the oocyst stage, a significant difference was observed in the distribution of L119F-GSTe2 genotypes (using the proportions) between infected and uninfected mosquitoes (X2 = 9.79 P = 0.007). Assessing the odds-ratio between sporozoite infected and uninfected mosquitoes showed that, homozygous resistant mosquitoes were significantly more likely to be infected with sporozoites compared to both heterozygote (OR = 2.10; IC 95%: 1.11–3.97; P = 0.013) and homozygous susceptible (OR = 2.46; IC 95%: 1.15–5.26; P = 0.012) mosquitoes. There was no difference between heterozygote and susceptible mosquitoes (OR = 1.17; P = 0.41) (Table 4).
In Mibellon, the 20% (12/60) of mosquitoes positive for oocysts were comprised of 8.3% (1/12) 119F/F homozygous resistant, 58.3% (7/12) L119F-RS heterozygotes and 33.3% (4/12) L/L119 homozygous susceptible (Fig. 3e). A significant difference was observed in the distribution of L119F-GSTe2 genotypes between infected and uninfected mosquitoes (X2 = 13.05 P = 0.001) with L119F-RS heterozygote mosquitoes the most often infected (Table 3). Assessing the odd ratio showed no difference between the two groups (Table 4). At the sporozoite stage, only 5% (3/60) of mosquitoes were sporozoite positive and all were genotyped to be homozygous susceptible (Fig. 3f) (Table 3). No further comparisons were done because of low sample size.
Association between A296S–RDL mutation and Plasmodium infection
The RDL mutation was genotyped using gDNA extracted from 100 and 142 whole female mosquitoes from Obout and Mibellon respectively. In Obout, all mosquitoes carried the resistant allele with a very high frequency of homozygous resistant 296 S/S genotypes (97%). In contrast, in Mibellon, only 22 (15.5%) of the mosquitoes examined had the A296S-RDL mutation including 4 (2.8%) 296S/S homozygous resistant, 18 (12.7%) A296S-RS heterozygotes and 120 homozygote susceptible (Fig. 4a). In addition, the A/A296 homozygous susceptible were present in a higher proportion among the infected mosquitoes (90%) compared to uninfected mosquitoes (79%). Assessment of the odd ratio demonstrated that mosquitoes that were A/A296 homozygous susceptible were more likely to be Plasmodium positive compared to other genotypes (OR = 4; IC 95%: 1.24–12.86; P = 0.03) (Table S1).
Combined impact of L119F-GSTe2 and A296S-RDL mutations on Plasmodium infection
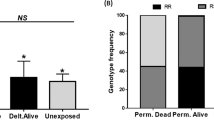
In total, 46 samples of each batch (infected and uninfected mosquitoes) were used to assess the combined impact of the two resistance mechanisms on Plasmodium infection in in An. funestus mosquitoes (Fig. 4b). The most prevalent combinations between both groups were (SS/SS), (RR/SS), (RS/SS) for GSTe2/RDL. The SS/RR and RR/RR combinations were present only among the infected mosquitoes whereas the RR/RS and RS/RS combinations were observed only among the uninfected mosquitoes. Nevertheless, no statistically significant differences were detected (χ2 = 10.5; P = 0.161). A significant difference was observed when comparing the odds ratio at the sporozoite stage between RR/RR vs SS/RR (OR = INF; P < 0.0001) and RS/RR vs SS/RR (OR = INF; P = 0.003) indicating that double homozygote mosquitoes (RR/RR) were more likely to be infected. However, no significant difference was observed at oocyst stage P ≥ 0.16) (Table S2). This supports the role of the L119F-GSTe2 allele in the ability of the mosquitoes to develop the parasite until the infective stage.
Association between GSTe2 polymorphism and Plasmodium infection
Genetic diversity of GSTe2
The full length of the GSTe2 gene (881 bp) was successfully sequenced in 26 whole mosquitoes from Mibellon including 11 infected and 15 uninfected (Fig. 5a). The genetic diversity parameters are given in Table S3, according to the status of infection and genotypes. Overall, 23 polymorphic sites defining 28 haplotypes were detected corresponding to the haplotype diversity of 0.96. Heterozygous and uninfected mosquitoes showed at lower number of polymorphic sites (3) with only 3 haplotypes (hd: 0.83). The overall nucleotide diversity was 0.005 with an average number of differences between nucleotides estimated at 4.19 showing less differences between the sequences examined. In addition, negative values were obtained for Fu and Li Tajima and F * tests in many cases.
Genetic diversity parameters of GSTe2 in An. funestus s.s. from Mibellon in relation to Plasmodium infection. (a) haplotype network and (b) phylogenetic tree (using a maximum likelihood method) between infected and uninfected mosquitoes; (c) haplotype network and (d) phylogenetic tree (using a maximum likelihood method) between 119F resistant allele and L119 susceptible allele.
Distribution of haplotypes and phylogeny
Analysis of the haplotype network of the GSTe2 gene based on L119F genotypes of the infection status shows that there are five major haplotypes (H1, H2, H3, H4 and H5) responsible for the differentiation of haplotypes in this An. funestus field population. The ancestral haplotype (H1) as well as the haplotypes (H2, H3 and H4) were identified in mosquitoes with 119 Fresistant allele. However, haplotypes H1 and H2 were found only in uninfected mosquitoes whereas haplotypes H3 and H4 were present in both infected and uninfected mosquitoes (Fig. 5b,c). Moreover, the H5 haplotype was found to be specific for mosquitoes with the L119 susceptible allele for both infected and uninfected individuals (Fig. 5d,e). Similarly, analysis of phylogeny between the haplotypes identified did not reveal any haplotype groups associated with a specific infection status. However, there was a global clustering according to the alleles associated with the L119F mutation of the GSTe2 gene (Table S3). This suggests that there is no association between the polymorphism of the GSTe2 gene and infection by Plasmodium parasite.
Discussion
Little information exists on the impact of metabolic resistance on the ability of mosquitoes to transmit Plasmodium parasites. This study is among the first to assess the association between metabolic resistance and vectorial capacity of natural populations of malaria vectors. We took advantage of the recent detection of the glutathione S-transferase L119F-GSTe2 marker in An. funestus to investigate the relationship between metabolic resistance and vectorial capacity in field collected mosquitoes. Mosquitoes used were collected from the same population at the same time for them to share a common genetic background but differ only by the presence of the resistant alleles to specifically discriminate this trait. Thus, any difference observed between the three genotypes would directly be associated with the insecticide resistance alleles.
Role of An. funestus in malaria transmission
An. funestus s.s. was found to be the most abundant mosquito species from the indoor collection in the two study sites correlating with the indoor feeding/resting behavior of this species and supported by the presence of permanent large pools of water in both locations. An. funestus s.s. is playing a major role in malaria transmission in these areas with a very high infection rate recorded at all stages including sporozoite infection rates (14.8% in Obout and 5% in Mibellon) in field collected females’ mosquitoes. The high infection rate observed in Obout and Mibellon for An. funestus s.s. is similar to high levels of infection rates recorded previously for this species across the continent such as 20%30 and 50%31 observed in Burkina Faso, 13.6%32 and 18%33 observed in Benin and 12.5% in Ghana25. Although, some of the variations between these rates could be attributed to the differences in the detection methods used (TaqMan, ELISA and Nested-PCR), the consistently high levels of infection support a high vectorial capacity of An. funestus across the continent. This is of great concern for malaria control as it shows that despite ongoing control interventions, the level of malaria transmission could remain high in areas where An. funestus is the dominant vector. In this study, we noticed that P. falciparum was the predominant malaria parasite in both study sites. However, the detection of other malaria parasites, although at lower frequencies, is an indication that control and elimination efforts should not ignore other Plasmodium species especially P. malariae.
Distribution of L119F-GSTe2 metabolic and A2926S target site resistance markers
It was previously demonstrated that a single amino acid change (L119F) in the over-expressed GSTe2 enzyme in An. funestus s.s confers resistance against DDT and cross-resistance to permethrin in West Africa27. The L119F mutation was detected in both localities with a higher frequency of the resistant allele in Obout. This resistance mechanism could have been selected in this population either by past DDT based IRS34 or by the scale up of pyrethroid-based LLINs. The presence of this resistance marker at high frequency in Obout supports previous observation in northern Cameroon (Gounougou) by Menze et al.21 suggesting that this mutation is strongly associated with DDT and permethrin cross resistance in Western and Central Africa21,27,33. In Mibellon, the 119F-GSTe2 mutation was found at a lower frequency for the 119F-GSTe2 resistant allele (26.3%). Two hypotheses may explain this: either the mutation was recently introduced in that population or that a recent insecticide selection pressure is favoring its presence now.
The A296S-RDL mutation in the GABA receptor gene associated with dieldrin resistance is fixed in the Obout population. In contrast, this mutation was found only at very low frequency in Mibellon. The high frequency of 296S resistant allele in An. funestus field populations from Obout is intriguing since cyclodienes are no longer used for vector control in Cameroon. It has previously been shown that dieldrin resistant mosquitoes exhibit significant fitness costs including behaviour and mating competitiveness35,36 that should lead to a decrease in the frequency of the resistant allele from the population overtime. Therefore, reversal of the resistance was expected in this field population in the absence of dieldrin selection pressure. The persistence of this dieldrin resistance marker in the An. funestus field population from Obout may be associated with the use of pesticides in the agricultural sector such as fipronil or lindane acting on same GABA receptor as dieldrin37. A population of An. gambiae fully resistant to dieldrin (100% RR) was reported in 1961 in Mbalmayo, a location of south Cameroon close to Obout38. This suggests also that the A296S resistant allele in An. funestus population in Obout could have become fixed before the removal of dieldrin as a vector control tool, thereby limiting the possibility of reversing dieldrin resistance.
Impact of L119F-GSTe2 metabolic and A2926S target site resistances on Plasmodium infection
We did not detect any significant differences between L/L119 homozygote susceptible, L119F-RS heterozygote and 119F/F homozygote resistant genotypes and P. falciparum oocyst infection. However, mosquitoes with the A/A296 RDL susceptible genotype were found to be more often infected with Plasmodium parasites. It has previously been demonstrated that insecticide resistance mechanisms may alter the vector competence of the mosquito by affecting parasite development or susceptibility of the host to infection. This trend was not observed in this study for the A296S-RDL mutation. In a study assessing the link between insecticide resistance and vector competence, Alout and collaborators demonstrated that target site mutations (kdr and ace-1R) increased the prevalence of P. falciparum infection in pyrethroid resistant An. gambiae compared to their susceptible counterparts10. However, despite a higher prevalence of infection, the kdr resistant mosquito strain was found to harbour lower malaria parasite (oocyst) load10. Many factors can influence the ability of mosquitoes to be successfully infected by Plasmodium and harbour the parasites throughout their developmental stages until the sporozoite stage. Therefore, pleiotropic effects of insecticide resistance, immunity activation and other fitness related traits may be altered. McCarroll et al. reported that insecticide resistance in Culex quinquefasciatus mosquitoes had negative effect on the parasitic worm Wuchereria bancrofti, which causes human lymphatic filariasis4,39. Furthermore, vector immunity could also be affected by insecticide resistance7. A possible link between resistance and mosquito immunity was observed when a gene driving pyrethroid resistance was up-regulated in the mosquito mid-gut infected with malaria parasites40. An. gambiae with metabolic resistance has also been shown to have increased infection rates compared to controls10. However, esterase metabolism or ace-1 mutation (target site resistance) did not appear to effect the infection rates or parasitic load in Culex pipiens mosquitoes6. Oxidative stress is part of the mosquito’s immune response against Plasmodium but may be neutralised by overproduction of GSTs. Previously, GST resistance mechanisms were shown to protect tissues from oxidative damage in plant hoppers and increase longevity in fruit flies41. Therefore, neutralising oxidative stress could potentially predispose mosquitoes to higher parasite infection.
Assessing the association between the L119F-GSTe2 mutation and the ability of mosquitoes to develop malaria parasites to the sporozoite stage
The high sporozoite infection rate of 14.8% observed in Obout was similar to recent observations in some GSTe2 related insecticide resistant populations of An. funestus in Benin33 and in Democratic Republic of Congo42. On the other hand, it was higher than the infection rates recorded in other pyrethroid resistant An. funestus populations in southern Africa such as in Malawi (4.8%)43 or in many African countries for other malaria vectors such as An. gambiae11,22. This high Plasmodium infection rate in An. funestus highlights the active transmission of malaria in southern Cameroon by this species. Furthermore, a significant association was found between the 119F/F-GSTe2 resistant genotype and the presence of P. falciparum sporozoite in An. funestus in Obout. The sporozoite infection rate in 119F/F homozygous resistant mosquitoes was three times higher than that of the homozygous susceptible mosquitoes. This suggests that parasites developed better in resistant mosquitoes than in susceptible counterparts which should be a cause for concern as possession of this resistance allele may potentially be allowing higher malaria transmission. A similar result was previously found in An. gambiae s.s. for the target-site vgsc-L1014S mutation11. The association between Plasmodium sporozoite infection and GSTe2-based resistant mosquitoes observed in this study could be due to three main possibilities. First, this could be caused by the phenotypic expression of L119F-GSTe2 such that the 119F/F homozygous resistant mosquitoes could live longer due to their ability to withstand exposure to insecticides in the field. In this case they are more likely to allow the Plasmodium parasites to complete their extrinsic incubation period compared to homozygous susceptible mosquitoes. This suggestion is supported by the fact that glutathione S-transferases have been shown to be associated with resistance27 and also to protect insect tissues from the damaging effects of oxidative stress and extent life span of insects by increasing solubility and excretion of free radicals7,44,45,46. The second possibility of the higher likelihood of sporozoite infection in mosquitoes with GSTe2–119F/F genotype is that insecticide resistance could alter mosquito immunity. Indeed, it is possible as suggested previously7 that the over-expression of GSTs in homozygous mosquitoes could be protecting Plasmodium parasites against the damaging effects of reactive oxidative species (ROS). These ROS are known as key component of the mosquito immune responses against Plasmodium infection47. It is likely that over-expression of GSTs may affect parasite development or susceptibility of the mosquito to infection by neutralizing the oxidative response of the 119F/F mosquitoes to Plasmodium and thus potentially increasing their susceptibility to infection. This will need to be fully established possibly through experimental infection studies. Thirdly, the higher Plasmodium infection rate seen in homozygous resistant 119F/F mosquitoes could be due the potential reduction of immune-competence through a resource trade-off between increased over-expression of GSTs and the mosquito’s immune response. It has been shown that when certain energy resources are redirected towards the production of large amounts of detoxification enzymes such as GSTs, a resource-based trade-off is usually involved and affects the vector immuno-competence48. As a result, there is likely to be a depletion of energy resources which limits the vector’s ability to mount a sufficient immune response against Plasmodium leading to increased infection in those resistant mosquitoes as observed in our study. However, more studies are needed to establish the extent to which insecticide resistance affects the mosquito’s vectorial capacity to confirm the impact of resistance on malaria transmission.
Conclusion
This study investigated the association between a molecular marker of GST-mediated metabolic resistance and Plasmodium infection in natural populations of a major malaria vector, An. funestus. The study revealed that mosquitoes that were homozygous for the resistance allele were more likely to harbor Plasmodium sporozoites. This suggests that the proliferation of this metabolic resistance marker could exacerbate malaria transmission in the field and thus have important public health consequences.
Methods
Study site and sample collection
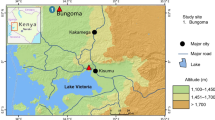
Mosquito collections were performed in Cameroon in May 2016 and February 2017 in Obout (Southern Region, 3°28′17.0″N 11°44′09.4″E) and Mibellon (Adamaoua Region, 6°46′N, 11°70′E) for one week per site. Prior to mosquito collection, verbal consent was obtained from the village council chairpersons and from each household representative. Indoor resting female mosquitoes were collected using electric aspirators in both locations and transported to the insectary of LSTM Research Unit at OCEAC in Yaoundé, Cameroon.
DNA extraction
Genomic DNA (gDNA) was extracted via the LIVAK method49. Following extraction, NanoDrop™ spectrophotometer (Thermo Scientific, Wilmington, USA) was used to determine the concentration and purity of the extracted gDNA before storage at −20 °C.
Species identification
The females used for oviposition were morphologically identified using the key of Gillies and De Meillon50. Molecular identification was achieved through a cocktail polymerase chain (PCR) reaction described by Koekemoer51 to determine species composition of An. funestus group in the two study sites.
Detection of Plasmodium parasites
A TaqMan assay described by Bass et al.29 was used to establish the Plasmodium infection status of field collected mosquitoes. Two probes were used in this assay. The first, labelled with FAM, detects P. falciparum, and the second, labelled with VIC, to detect P. vivax, P. ovale and/or P. malariae (OVM). Firstly, gDNA was extracted from the whole mosquitoes to assess the overall proportion of An. funestus infected by Plasmodium parasites in the field. Secondly, another sets of field collected mosquitoes were dissected in two parts: the abdomens, used for the detection of Plasmodium infection at the oocyst stage, and the head plus thorax for the assessment of sporozoite infection rate. Results of TaqMan assay were confirmed by performing a nested PCR assay as previously described52.
Genotyping of the L119F-GSTe2 mutation
The L119F-GSTe2 mutation previously shown to play a major role in DDT and permethrin resistance in An. funestus27 was genotyped in F0 field-collected mosquitoes using a newly designed allele-specific PCR (AS-PCR) diagnostic assay. Two pairs of primers were needed for the AS-PCR (two outer and two inner primers). Specific primers were designed manually to match the mutation and an additional mismatched nucleotide was added in the 3th nucleotide from the 3′ end of each inner primer to enhance the specificity. More details on the primer sequences are given in Table S4. PCR was carried out using 10 mM of each primer and 1ul of genomic DNA as template in 15 μl reactions containing 10X Kapa Taq buffer A, 0.2 mM dNTPs, 1.5 mM MgCl2, 1U Kapa Taq (Kapa biosystems). The cycle parameters were: 1 cycle at 95 °C for 2 min; 30 cycles of 94 °C for 30 s, 58 °C for 30 s, 72 °C for 1 min and then a final extension step at 72 °C for 10 min. PCR products were separated on 2% agarose gel by electrophoresis. This method detects homozygote resistant (119F/F) at 523 bp, homozygote susceptible (L119F-RS) at 312 bp, and heterozygote (L/L119) with both bands. Association between the GSTe2 mutation and malaria transmission potential was assessed by calculating the odds ratio of sporozoite infection rate between the homozygous resistant (119F/F), heterozygote (L119F-RS) and homozygous susceptible (L/L119) individuals compared to uninfected individuals, with statistical significance was computed based on the Fisher’s exact probability test.
Association between the genetic diversity of the GSTe2 gene and Plasmodium infection in An. funestus
The entire GSTe2 gene of 881 bp in An. funestus was amplified in 26 whole mosquitoes [11 infected by Plasmodium parasites (both stages) and 15 non-infected]. Two primers; GSTe2F, 5′GGA ATT CCA TAT GAC CAA GCT AGT TCT GTA CAC GCT 3′ and GSTe2R, 5′ TCT AGA TCA AGC TTT AGC ATT TTC CTC CTT 3′ were used to amplify the gene in 15 μl reaction containing 10 mM of each primer, 10X Kapa Taq buffer A, 0.2 mM dNTPs, 1.5 mM MgCl2, 1U Kapa Taq (Kapa biosystems). PCR conditions were 1 cycle at 95 °C for 5 min; 30 cycles of 94 °C for 30 s, 55 °C for 30 s, 72 °C for 1 min and then final extension at 72 °C for 10 min. PCR product was firstly visualized on 1.5% agarose gel stained with Midori green dye (Nippon Genetics Europe, Germany) and then purified using ExoSAP (Thermo Fisher Scientific, Waltham, MA, USA) according to manufacturer recommendations and directly sequenced on both strands. Sequences were visualized and corrected using BioEdit v7.2.5 software53. Alignment of these sequences was done using ClustalW Multiple Alignment integrated in BioEdit54. Genetic diversity parameters were assessed using DnaSP v5.10.0155 and MEGA v7.0.2156 softwares.
Genotyping of the A296S-RDL GABA receptor mutation
To compare the role of metabolic resistance to that of target-site resistance mechanism, we genotyped the A296S-RDL mutation associated with dieldrin resistance20 in Plasmodium infected and uninfected mosquitoes. The A296S-RDL mutation was genotyped using a protocol previously described by Riveron et al.43. Furthermore, the combined effect of harboring both alleles of A296S-RDL and L119F-GSTe2 on the infection status of field collected mosquitoes was also assessed.
References
Bhatt, S. et al. The effect of malaria control on Plasmodium falciparum in Africa between 2000 and 2015. Nature 526, 207 (2015).
Ranson, H. & Lissenden, N. Insecticide Resistance in African Anopheles Mosquitoes: A Worsening Situation that Needs Urgent Action to Maintain Malaria Control. Trends Parasitol 32, 187–196, https://doi.org/10.1016/j.pt.2015.11.010 (2016).
Alout, H., Labbé, P., Chandre, F. & Cohuet, A. Malaria vector control still matters despite insecticide resistance. Trends in parasitology 33, 610–618 (2017).
McCarroll, L. & Hemingway, J. Can insecticide resistance status affect parasite transmission in mosquitoes? Journal Insect Biochemistry and Molecular Biology 32, 1345–1351 (2002).
Raymond, M., Berticat, C., Weill, M., Pasteur, N. & Chevillon, C. In Microevolution Rate, Pattern, Process 287–296 (Springer, 2001).
Vezilier, J., Nicot, A., Gandon, S. & Rivero, A. Insecticide resistance and malaria transmission: infection rate and oocyst burden in Culex pipiens mosquitoes infected with Plasmodium relictum. Malaria Journal 9 (2010).
Rivero, A., Vézilier, J., Weill, M., Read, A. F. & Gandon, S. Insecticide Control of Vector-Borne Diseases: When Is Insecticide Resistance a Problem? PLoS Pathog 6, e1001000, https://doi.org/10.1371/journal.ppat.1001000 (2010).
Martinez-Torres, D. et al. Molecular characterization of pyrethroid knockdown resistance (kdr) in the major malaria vector Anopheles gambiae s.s. Insect Mol Biol 7, 179–184 (1998).
WHO. Global plan for insecticide resistance management in malaria vectors (GPIRM). 2012. ISBN 978, 4 (2012).
Alout, H. et al. Insecticide resistance alleles affect vector competence of Anopheles gambiae s.s. for Plasmodium falciparum field isolates. PLoS ONE 8, e63849 (2013).
Kabula, B. et al. A significant association between deltamethrin resistance, Plasmodium falciparum infection and the Vgsc-1014S resistance mutation in Anopheles gambiae highlights the epidemiological importance of resistance markers. Malar J 15, 289, https://doi.org/10.1186/s12936-016-1331-5 (2016).
Irving, H. & Wondji, C. S. Investigating knockdown resistance (kdr) mechanism against pyrethroids/DDT in the malaria vector Anopheles funestus across Africa. BMC Genet 18, 76, https://doi.org/10.1186/s12863-017-0539-x (2017).
Casimiro, S. L., Hemingway, J., Sharp, B. L. & Coleman, M. Monitoring the operational impact of insecticide usage for malaria control on Anopheles funestus from Mozambique. Malar J 6, 142, https://doi.org/10.1186/1475-2875-6-142 (2007).
Cuamba, N., Morgan, J. C., Irving, H., Steven, A. & Wondji, C. S. High level of pyrethroid resistance in an Anopheles funestus population of the Chokwe District in Mozambique. PLoS One 5, e11010, https://doi.org/10.1371/journal.pone.0011010 (2010).
Hunt, R. H., Edwardes, M. & Coetzee, M. Pyrethroid resistance in southern African Anopheles funestus extends to Likoma Island in Lake Malawi. Parasites & Vectors 3, 122, https://doi.org/10.1186/1756-3305-3-122 (2010).
Wondji, C. S. et al. Impact of pyrethroid resistance on operational malaria control in Malawi. Proc Natl Acad Sci USA 109, 19063–19070, https://doi.org/10.1073/pnas.1217229109 (2012).
Morgan, J. C., Irving, H., Okedi, L. M., Steven, A. & Wondji, C. S. Pyrethroid resistance in an Anopheles funestus population from Uganda. PLoS One 5, e11872, https://doi.org/10.1371/journal.pone.0011872 (2010).
Mulamba, C. et al. Widespread pyrethroid and DDT resistance in the major malaria vector Anopheles funestus in East Africa is driven by metabolic resistance mechanisms. PLoS One 9, e110058, https://doi.org/10.1371/journal.pone.0110058 (2014).
Lwetoijera, D. W. et al. Increasing role of Anopheles funestus and Anopheles arabiensis in malaria transmission in the Kilombero Valley, Tanzania. Malar J 13, 331, https://doi.org/10.1186/1475-2875-13-331 (2014).
Wondji, C. S. et al. Identification and distribution of a GABA receptor mutation conferring dieldrin resistance in the malaria vector Anopheles funestus in Africa. Insect Biochem Mol Biol 41, 484–491, https://doi.org/10.1016/j.ibmb.2011.03.012 (2011).
Menze, B. D. et al. Multiple Insecticide Resistance in the Malaria Vector Anopheles funestus from Northern Cameroon Is Mediated by Metabolic Resistance Alongside Potential Target Site Insensitivity Mutations. PLoS One 11, e0163261, https://doi.org/10.1371/journal.pone.0163261 (2016).
Djouaka, R., Irving, H., Tukur, Z. & Wondji, C. S. Exploring Mechanisms of Multiple Insecticide Resistance in a Population of the Malaria Vector Anopheles funestus in Benin. PLoS One 6, e27760, https://doi.org/10.1371/journal.pone.0027760 (2011).
Djouaka, R. J. et al. Evidence of a multiple insecticide resistance in the malaria vector Anopheles funestus in South West Nigeria. Malar J 15, 565, https://doi.org/10.1186/s12936-016-1615-9 (2016).
Okoye, P. N., Brooke, B. D., Koekemoer, L. L., Hunt, R. H. & Coetzee, M. Characterisation of DDT, pyrethroid and carbamate resistance in Anopheles funestus from Obuasi, Ghana. Trans R Soc Trop Med Hyg 102, 591–598, https://doi.org/10.1016/j.trstmh.2008.02.022 (2008).
Riveron, J. M. et al. Multiple insecticide resistance in the major malaria vector Anopheles funestus in southern Ghana: implications for malaria control. Parasit Vectors 9, 504, https://doi.org/10.1186/s13071-016-1787-8 (2016).
Samb, B. et al. Investigating molecular basis of lambda-cyhalothrin resistance in an Anopheles funestus population from Senegal. Parasit Vectors 9, 449, https://doi.org/10.1186/s13071-016-1735-7 (2016).
Riveron, J. M. et al. A single mutation in the GSTe2 gene allows tracking of metabolically-based insecticide resistance in a major malaria vector. Genome Biol 15, R27, https://doi.org/10.1186/gb-2014-15-2-r27 (2014).
Ibrahim, S. S., Ndula, M., Riveron, J. M., Irving, H. & Wondji, C. S. The P450 CYP6Z1 confers carbamate/pyrethroid cross-resistance in a major African malaria vector beside a novel carbamate-insensitive N485I acetylcholinesterase-1 mutation. Mol Ecol 25, 3436–3452, https://doi.org/10.1111/mec.13673 (2016).
Bass, C. et al. PCR-based detection of Plasmodium in Anopheles mosquitoes: a comparison of a new high-throughput assay with existing methods. Malar.J. 7(177), 177 (2008).
Dabire, K. R. et al. Anopheles funestus (Diptera: Culicidae) in a humid savannah area of western Burkina Faso: bionomics, insecticide resistance status, and role in malaria transmission. J Med Entomol 44, 990–997 (2007).
Costantini, C., Sagnon, N., Ilboudo-Sanogo, E., Coluzzi, M. & Boccolini, D. Chromosomal and bionomic heterogeneities suggest incipient speciation in Anopheles funestus from Burkina Faso. Parassitologia 41, 595–611 (1999).
Sandeu, M. M. et al. Optimized Pan-species and speciation duplex real-time PCR assays for Plasmodium parasites detection in malaria vectors. PLoS One 7, e52719, https://doi.org/10.1371/journal.pone.0052719PONE-D-12-23281 (2012).
Djouaka, R. et al. Multiple insecticide resistance in an infected population of the malaria vector Anopheles funestus in Benin. Parasit Vectors 9, 453, https://doi.org/10.1186/s13071-016-1723-y (2016).
Antonio-Nkondjio, C. et al. Review of the evolution of insecticide resistance in main malaria vectors in Cameroon from 1990 to 2017. Parasites & Vectors 10, 472, https://doi.org/10.1186/s13071-017-2417-9 (2017).
Rowland, M. Behaviour and fitness of γHCH/dieldrin resistant and susceptible female Anopheles gambiae and An.stephensi mosquitoes in the absence of insecticide. Medical and Veterinary Entomology 5, 193–206, https://doi.org/10.1111/j.1365-2915.1991.tb00542.x (1991).
Rowland, M. Activity and mating competitiveness of gamma HCH/dieldrin resistant and susceptible male and virgin female Anopheles gambiae and An.stephensi mosquitoes, with assessment of an insecticide-rotation strategy. Med Vet Entomol 5, 207–222 (1991).
Tantely, M. L. et al. Insecticide resistance in Culex pipiens quinquefasciatus and Aedes albopictus mosquitoes from La Reunion Island. Insect Biochem Mol Biol 40, 317–324, https://doi.org/10.1016/j.ibmb.2010.02.005 (2010).
Gariou, J. & Mouchet, J. [Appearance of a dieldrin-resistant strain of Anopheles gambiae in the antimalaria campaign zone in southern Cameroon’s]. Bull Soc Pathol Exot Filiales 54, 870–875 (1961).
McCarroll, L. et al. Insecticides and mosquito-borne disease. Nature 407, 961 (2000).
Felix, R. C., Muller, P., Ribeiro, V., Ranson, H. & Silveira, H. Plasmodium infection alters Anopheles gambiae detoxification gene expression. BMC Genomics 11, 312, https://doi.org/10.1186/1471-2164-11-312 (2010).
McElwee, J. J. et al. Evolutionary conservation of regulated longevity assurance mechanisms. Genome Biol 8, R132, https://doi.org/10.1186/gb-2007-8-7-r132 (2007).
Riveron, J. M., Watsenga, F., Irving, H., Irish, S. R. & Wondji, C. S. High Plasmodium Infection Rate and Reduced Bed Net Efficacy in Multiple Insecticide-Resistant Malaria Vectors in Kinshasa, Democratic Republic of Congo. The Journal of infectious diseases 217, 320–328, https://doi.org/10.1093/infdis/jix570 (2018).
Riveron, J. M. et al. Rise of multiple insecticide resistance in Anopheles funestus in Malawi: a major concern for malaria vector control. Malar J 14, 344, https://doi.org/10.1186/s12936-015-0877-y (2015).
Parkes, T. L., Hilliker, A. J. & Phillips, J. P. Genetic and biochemical analysis of glutathione-S-transferase in the oxygen defense system of Drosophila melanogaster. Genome 36, 1007–1014 (1993).
Hayes, J. D. & McLellan, L. I. Glutathione and glutathione-dependent enzymes represent a co-ordinately regulated defence against oxidative stress. Free Radic Res 31, 273–300 (1999).
Vontas, J. G., Small, G. J. & Hemingway, J. Glutathione S-transferases as antioxidant defence agents confer pyrethroid resistance in Nilaparvata lugens. Biochem J 357, 65–72 (2001).
Kumar, S. et al. The role of reactive oxygen species on Plasmodium melanotic encapsulation in Anopheles gambiae. Vol. 100 (2003).
Després, L. et al. Chemical and biological insecticides select distinct gene expression patterns in Aedes aegypti mosquito. Biology Letters 10, 20140716, https://doi.org/10.1098/rsbl.2014.0716 (2014).
Livak, K. J. Organization and mapping of a sequence on the Drosophila melanogaster X and Y chromosomes that is transcribed during spermatogenesis. Genetics 107, 611–634 (1984).
Gillies, M. & De Meillon, B. The Anophelinae of Africa South of the Sahara (Ethiopian Zoogeographical Region). Inst Med Res 54, 343 (1968).
Koekemoer, L. L., Kamau, L., Hunt, R. H. & Coetzee, M. A cocktail polymerase chain reaction assay to identify members of the Anopheles funestus (Diptera: Culicidae) group. Am J Trop Med Hyg 66, 804–811 (2002).
Snounou, G. et al. High sensitivity of detection of human malaria parasites by the use of nested polymerase chain reaction. Molecular and Biochemical Parasitology 61, 315–320, https://doi.org/10.1016/0166-6851(93)90077-B (1993).
Hall, T. BioEdit: a user-friendly biological sequence alignment editor and analysis program for Windows 95/98/NT. Nucleic Acids Symposium Series 41, 95–98 (1999).
Thompson, J., Higgins, D. & Gibson, T. CLUSTALW: improving the sensitivity of progressive miltiple sequence alignment through sequence weighting, position specific gap penalties and weght matrix choice. Nucleic Acids Research 22, 4673–4680 (1994).
Librado, P. & Rozas, J. DnaSP v5: a software for comprehensive analysis of DNA polymorphism data. Bioinformatics 25, 1451–1452 (2009).
Kumar, S., Stecher, G. & Tamura, K. MEGA7: Molecular Evolutionary Genetics Analysis Version 7.0 for Bigger Datasets. Molecular Biology and Evolution 33, 1870–1874 (2016).
Acknowledgements
This study was funded by a Wellcome Trust Senior Fellowship in Biomedical Sciences to CSW (101893/13/Z).
Author information
Authors and Affiliations
Contributions
C.S.W. conceived and designed the study; M.C.C., J.M.R. and M.T. carried out the sample collection and performed WHO susceptibility assays; M.T., M.C.C., M.J.W., C.K.K., M.K. and M.T. performed the Molecular analyses; M.T., N.A.A., C.K.K., C.N., J.M.R. and C.S.W. analyzed the data. M.T., J.M.R. and C.S.W. wrote the manuscript with contribution from other co-authors. All authors read and approved the final manuscript.
Corresponding authors
Ethics declarations
Competing Interests
The authors declare no competing interests.
Additional information
Publisher’s note: Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made. The images or other third party material in this article are included in the article’s Creative Commons license, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons license and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this license, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Tchouakui, M., Chiang, MC., Ndo, C. et al. A marker of glutathione S-transferase-mediated resistance to insecticides is associated with higher Plasmodium infection in the African malaria vector Anopheles funestus. Sci Rep 9, 5772 (2019). https://doi.org/10.1038/s41598-019-42015-1
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41598-019-42015-1
This article is cited by
-
Key gene modules and hub genes associated with pyrethroid and organophosphate resistance in Anopheles mosquitoes: a systems biology approach
BMC Genomics (2024)
-
Gene drives: an alternative approach to malaria control?
Gene Therapy (2024)
-
Genetic markers associated with the widespread insecticide resistance in malaria vector Anopheles funestus populations across Tanzania
Parasites & Vectors (2024)
-
High efficacy of chlorfenapyr-based net Interceptor® G2 against pyrethroid-resistant malaria vectors from Cameroon
Infectious Diseases of Poverty (2023)
-
Impact of insecticide resistance on malaria vector competence: a literature review
Malaria Journal (2023)
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.