Abstract
Ankylosing spondylitis (AS) has different clinical features in males and females. Fecal metabolites play significant roles in AS disorders. This study aimed to reveal gender-attributed fecal signatures of AS. Fecal samples from 87 cross-sectional individuals (healthy controls: 20 males, 18 females; AS patients: 26 males, 23 females) were analyzed by gas chromatography-mass spectroscopy (GC-MS). Partial least squares discriminant analysis (PLS-DA) was used to reveal differences in the fecal signatures of AS between males and females. Fecal signatures were defined by the significantly different fecal metabolites between AS patients and healthy individuals. Therefore, different fecal signatures of male and female AS patients were defined as gender-attributed fecal signatures. Male-specific fecal signatures in AS patients were steroid compounds, including cholestan-3-ol, tocopherol, stigmastan-3,5-diene, cholest-3-ene, cholest-4-en-6-one and 1-heptatriacotanol. Female-specific fecal signatures were ergost-5-en-3-ol, acetate and D-myo-Inositol. Gender-attributed fecal signatures of AS further reveal differences between males and females in terms of AS features.
Similar content being viewed by others
Introduction
Ankylosing spondylitis (AS) is a chronic rheumatic disorder characterized by inflammation of the spine and sacroiliac joints. The disease can cause altered physical outcomes such as reduced spinal mobility, fatigue, sleep disturbances and psychological consequences such as depression, anxiety and stress1. In addition, multiple coexisting comorbidities are frequent in AS, especially in patients with cardiovascular disease2. Currently, the occurrence of AS is considered to be triggered by genetic, infectious and endocrine factors3.
Over the years, AS has been considered to be a disease occurring predominantly in males, with an estimated male to female ratio of 2-3:14. Additionally, there are some differences in the clinical features of AS between males and females. Compared with male patients, female patients were found to have a longer delay in diagnosis and a greater age at disease onset4,5. It has also been observed that female AS patients present a more active disease6, a higher burden of disease5, and more frequent peripheral involvement than do male AS patients7,8. With respect to clinical therapy, female patients are positively associated with the use of conventional disease-modifying antirheumatic drugs (DMARD) therapy, while male patients are associated with the use of biologic therapy9. Therefore, further research is necessary to better reveal differences between male and female AS patients.
Increasing evidence has indicated that genetic risk factors and pathogenesis are similar in AS and inflammatory bowel disease (IBD)10. Frequently, AS patients suffer from severe intestinal inflammation characterized by cytokine overexpression11. Therefore, AS is closely related to intestinal disorders involving gut microbiota and fecal metabolites. Alterations in gut microbiota have been associated with the development of AS12,13 and HLA-B2714. The 1H NMR spectroscopy of fecal metabolites showed that AS patients have significantly decreased levels of butyrate, propionate, methionine and UDP-glucose and increased levels of fumarate, glucose, taurine, tryptophan and threonine15. The cross talk between gut microbiota and intestinal cells is mediated by intestinal metabolites. Therefore, characterization of intestinal metabolites may be important for revealing different AS conditions in males and females.
In this study, GC-MS was used to investigate fecal metabolite profile of AS patients and healthy individuals in a cross-sectional study. The overall goal of this study was to ascertain whether the fecal signatures of AS were associated with gender.
Materials and Methods
Patient population
After informed consent was provided, a total of 87 individuals (49 AS patients and 38 healthy individuals) were enrolled in this study. AS was diagnosed on the basis of the modified New York criteria for AS16. There was a consistent male-to-female ratio between AS patients (26 male, 23 female) and healthy controls (20 male, 18 female) (Table 1). In addition, the age and body mass index (BMI) were also matched between AS patients and healthy individuals (HDs) (Table 1). In addition, HLA-B27 had a strong positive correlation with AS in all participants (Table 1). Erythrocyte sedimentation rate (ESR) and C-reactive protein (CRP) values were significantly higher in AS patients than in HDs (Table 1). In addition, the bath Ankylosing Spondylitis Disease Activity Index (BASDAI) scores of AS patients were calculated. Regardless of AS or healthy status, there were no significant differences in the above clinical information between males and females.
All participants with gastrointestinal tract disorders and those undergoing treatment with antibiotics, probiotics or drugs within one month prior to the stool collection were excluded. Patients with severe systemic diseases or hepatitis were excluded. A dietary questionnaire that recorded the complete diet information and dietary habits was completed. This questionnaire was used to exclude individuals who had specific dietary habits such as alcohol consumption or a completely vegetable-based diet. In this study, all experimental protocols involving humans were approved by the Ethics Committee of Zhejiang Chinese Medical University.
Sample collection and preparation
Each participant was given a sample collection kit with instructions. One fecal sample was collected from each subject; placed in a sealed insulated container; immediately placed in ice; and subsequently delivered to the laboratory within 2 h, where it was stored at −80 °C.
Fifty milligrams of feces was used for the extraction procedure and extracted with 800 μL methanol. Then, 10 μL internal standard (2.9 mg/mL, DL-o-chlorophenylalanine) was added. All samples were ground to a fine powder using a grinding m at 65 HZ for 90 s. After grinding, the samples were vortexed for 30 s and centrifuged at 12000 rpm at 4 °C for 15 min. Then, 200 μL supernatant was transferred to a vial for concentration by centrifugation. The samples were derivatized by adding 30 μL methoxyamine hydrochloride (20 mg/mL) in pyridine and shaking them for 90 min at 37 °C, after which they were incubated for 16 h at room temperature. The samples were then trimethylsilylated by adding 30 μL BSTFA and incubating for 1 h at 70 °C; samples were then prepared for GC-MS analysis.
GC-MS analysis conditions
Metabolic profiling of fecal samples was acquired by an Agilent 7890 A/5975C GC-MS (Agilent Technologies, Santa Clara, CA, USA). Separation was performed by using a 30 m × 0.25 mm × 0.25 μm HP-5MS fused silica capillary column (Agilent J&W Scientific). The sample injection volume was 1 μL with a split ratio of 10:1. The injector, ion source and quadrupole rod temperatures were 280 °C, 230 °C and 150 °C respectively. The flow rate of the carrier gas, high-purity helium (>99.999%), was 1.2 mL/min. The GC oven temperature program consisted of 80 °C for 2 min, after which the temperature ramped to 330 °C at 10 °C/min, and held steady for 6 min. Mass spectra were acquired at ascan speed of 2 spectra per second after a solvent delay of 4.8 min, and the mass scan range was set at m/z 50–550. Fecal samples were analyzed randomly.
Data processing and statistical analysis
Raw GC-MS mass spectra were converted to CDF format files and subsequently processed using XCMS in R software as previously described17. XCMS could be employed for preprocessing automatically, including raw signal extraction, data baseline filtering, peak identification, and integration. After alignment with the statistical comparison component, the “.CSV” file was obtained with four dimension data sets including sample information, retention time, the mass-to-charge ratio and peak intensity. Identification of metabolites was conducted using the Automatic Mass Spectral Deconvolution and Identification System (AMIDS), which was searched against commercially available databases such as the National Institute of Standards and Technology (NIST) and Wiley libraries. Metabolites were identified by comparison of mass spectra and retention indices to the spectral library using a match value greater than 700. The signal integration area of each metabolite was normalized to the internal standard (DL-o-chlorophenylalanine) for each sample.
For multivariate statistical analysis, the XCMS output was further processed using Microsoft Excel (Microsoft, USA). The normalized data were transformed using SIMCA-P 11.0 software (Umetrics AB, Umea, Sweden) for principal component analysis (PCA) and partial least Squares-discriminant analysis (PLS-DA). PCA and PLS-DA were applied to the data after mean-centering and unit variance scaling (UV scaling). These analyses employed a default seven-fold internal cross validation from which the R2X and Q2 (goodness of prediction) values, representing the total explained variance and the model predictability, respectively, were extracted.
The variable importance in projection (VIP) values of all the metabolites from the PLS-DA model was taken as criteria to find the variable importance of differential metabolites. Those variables with a VIP >1.0 and a p-value < 0.05 were considered relevant for group discrimination. The statistical significance between two groups was evaluated by a univariate Student’s t-test. Following statistical analyses with multiple comparisons, p value were adjusted using the Benjamini-Hochberg method to control the false discovery rate (FDR). An adjusted p value of 0.05 was used as a statistically significant cutoff.
Compliance with Human Studies and Ethical standards
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional, national research committee and with the 1964 Helsinki declaration and its later amendments. Informed consent was obtained from all individual participants included in the study. All procedures involved humans in this study were approved by the Ethics Committee of Zhejiang Chinese Medical University.
Results
Metabolic profiles in fecal extracts
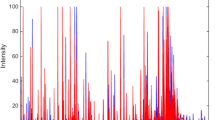
Typical GC-MS spectra of fecal extracts obtained from AS patients and HDs are shown in Fig. S1. Two thousand three hundred forty-two features were obtained from GC-MS spectra. The endogenous metabolites were then identified by similarity matching with the NIST05 mass spectra. Identified metabolites with a match value greater than 700 were used for subsequent analysis. As shown in Table S1, 84 metabolites were confirmed on the basis of their retention and MS fragmentation behavior, mainly including alkanes (11 identified), alkenes (2 identified), sugars (13 identified), organic acids (35 identified), and cholesterols (7 identified). To obtain detailed differences between groups, multivariate data analysis of these GC-MS profiles was performed.
PCA analysis
PCA based on these 84 targeted metabolites was used to give an intuitive display of metabolite differences. PC1 and PC2 explained 25.1% and 7.0% of the total variance, respectively (Fig. 1). The score plot showed a clear separation between AS patients and HDs but no separation between males and females. Therefore, the difference in the profiles of fecal metabolites caused by disease factor was greater than gender.
Gender-related differences in fecal metabolites
To uncover fecal metabolite differences by gender, a comparative PLS-DA model based on the targeted metabolites was conducted for males and females. The values for R2 and Q2 (Fig. 2a,c,e) and the results of permutation tests (Fig. S2) indicated poor results of the PLS-DA model in revealing differences between males and females. In addition, no clear separation between males and females was observed in PLS-DA scores (Fig. 2a,c,e). The above results indicated that there was little difference in fecal metabolites between males and females. Figures 2b,d,f shows the names of fecal metabolites with VIP > 1 in the PLS-DA.
PLS-DA score (a,c,e) and loading plots (b,d,f) based on the fecal metabolic profiles of male and female individuals. (a,b) comparison of results between males (black box) and females (red dots) in all individuals; (c,d) Comparison of results between males (black box) and females (red dots) in healthy individuals (HDs); (e,f) comparison of results between males (black box) and females (red dots) in AS patients (AS). Metabolites with VIP > 1.0 are shown with names in loading plots. The score t1 (first component) explains the largest variation of the X space, followed by t2 (second component). The w*[1] (first component) explains the weighting variation of metabolites, followed by w*[2] (second component).
Table 2 lists the fecal metabolites with VIP > 1 or p < 0.05 between genders in total subject, AS patients or HDs. The fecal metabolites with both VIP > 1 and p < 0.05 were considered as significantly different metabolites between males and females. There was no different metabolite between males and females in total enrolled subjects. In AS patients, a decrease in cholest-4-en-6-one and the increase in propanedioic acid were found in males compared to that of females. In healthy individuals, cholest-4-en-6-one was also the different metabolite between males and females, but its concentration was higher in males than in females. In addition, the metabolite carbazole significantly increased in males compared with females in healthy individuals. The above little differences in metabolites between males and females may be due to the inherent error in the sampling process.
AS-related differences in fecal metabolites
AS-related differences in fecal metabolites were obtained by comparing AS patients and healthy individuals. First, PLS-DA analyses were used to reveal fecal signatures in three types of samples (total samples, male samples and female samples). The values for R2X and Q2 (Fig. 3a,c,e) and the results of permutation tests (Fig. S3) indicated the goodness of fit and predictability of the models in revealing different fecal metabolites between AS patients and HDs. There were clear separations between AS patients and HDs in all three PLS-DA score plots based on total, male, and female samples (Fig. 3a,c,e, respectively). Metabolites with a VIP value greater than 1.0 were displayed with name in three corresponding loading plots (Fig. 3b,d,f) and were considered the primary contributors for classification of the groups.
PLS-DA score (a,c,e) and loading plots (b,d,f) based on the fecal metabolic profiles of healthy individuals and AS patients. (a,b) Comparison of results between healthy (black triangle) and AS (red cross) in all individuals; (c,d) comparison of results between healthy (black triangle) and AS (red cross) in male individuals; (e,f) comparison of results between healthy (black triangle) and AS (red cross) in female individuals. Metabolites with VIP > 1.0 are shown with names in loading plots. The score t1 (first component) explains the largest variation of the X space, followed by t2 (second component). The w*[1] (first component) explains the weighting variation of metabolites, followed by w*[2] (second component).
In combination with p (t-test) and VIP values, there were 19 differential metabolites between AS patients and HDs (Table 3). Nine different metabolites between AS patients and HDs were found in all three sample set. Compared with HDs, AS patients had significantly higher concentrations of 5-trimethylsilyloxy-n-valeric acid, cyclohexanecarboxylic acid, gluconic acid, serine, α-l-galactofuranoside and n-(4,5-dimethyl-thiophen-2-yl)-benzamide as well as lower concentrations of β-sitosterol, 24-ethyl-δ (22)-cloprostenol and 3-pyridinecarboxylic acid. In male subjects, the specifically different metabolites between AS patients and HDs were cholestan-3-ol, tocopherol, stigmastan-3,5-diene, cholest-3-ene, cholest-4-en-6-one and 1-heptatriacotanol, which were all significantly lower in AS patients. In female subjects, ergost-5-en-3-ol, acetate and D-myo-inositol were two distinctly different metabolites between AS patients and HDs.
According to the above results, the unique fecal signatures of AS in males were cholestan-3-ol, tocopherol, stigmastan-3,5-diene, cholest-3-ene, cholest-4-en-6-one and 1-heptatriacotanol, and the unique fecal signatures of AS in females were ergost-5-en-3-ol, acetate and D-myo-inositol.
Discussion
Intestinal disorders occurring in patients affected by ankylosing spondylitis are correlated with the severity of spine inflammation18. Increasing evidence has indicated that dysbiosis of the gut microbiome participates in the pathogenesis and development of AS19,20. Intestinal metabolites could act as crosstalk mediators in the process of gut microbiota affecting the host. There are few studies reporting that alterations of intestinal metabolites might be pathogenic factors of AS21,22. We have previously shown that fecal metabolites could distinguish AS patients from healthy individuals15. However, our previous study was limited due to the weak ability of the 1H-NMR platform to detect lipids and alkanes metabolites in fecal metabolomics23. Therefore, this study used a GC-MS metabolomics platform to explore fecal metabolites.
This study revealed the effects of gender and AS on the profiles of fecal metabolites. PLS-DA indicated that AS disease had a greater impact on fecal metabolites than gender. It has been reported that both disease and gender could affect the human fecal metabolome24,25. To the best of our ability, this study compared the effects of disease and gender on the fecal metabolome in the same population for the first time.
AS-related differences in fecal metabolites were the fecal signatures of AS. In this study, most of the fecal signatures of AS revealed by the GC-MS platform were lipids and alkanes, most of which were associated with the disorders of AS patients (Fig. 4). Decreased cholesterol was found in AS patients26, which might be associated with cholest-3-ene, cholest-4-en-6-one and cholestan-3-ol. The imbalance of steroid hormones in AS patients27 might be associated with decreased tocopherol28 and β-Sitosterol29. In addition, tocopherol and 3-pyridinecarboxylic acid, might cause decreased antioxidant in AS patients30,31. The GC-MS platform also revealed some acids as fecal signatures of AS in this study. Gluconic acid and α-l-galactofuranoside increased in the intestine, which might be associated with increased glucose in AS patients32. As the metabolites were derived only from gut microbiota, increased valeric acid might be due to an imbalance of gut microbiota in AS patients33. Serine, as the only amino acid in fecal signatures of AS revealed by GC-MS platform, was associated with misfolding of HLA-B27 protein34. In summary, the study enriched the types of fecal signatures of AS.
Gender had little effect on fecal metabolome, but fecal signatures of AS showed gender-specific differences. The number of fecal signatures of AS in males was greater than that in females, indicating that the fecal metabolome of males was more affected by AS disease than that in females. The different fecal signatures of AS between males and females could cause disorders of AS, such as low cholesterol, decreased antioxidants and steroid hormone imbalance. The above results might be the reason that the incidence of AS in males was higher than that in females. At the onset of AS, there were few differences in fecal metabolites between males and females, including cholest-4-en-6-one and propanedioic acid. The above different fecal metabolites might be associated with different clinical features between males and females or might be caused by inherent error in the sampling process. Certainly, the above inference requires further study to verify.
This study successfully revealed differences in the fecal signatures of AS in males and females. In addition, the study also confirmed for the first time that the effect of AS disease on fecal metabolites was greater than that of gender. However, this study failed to analyze the host’s metabolome and community structure of the gut microbiome and reveal whether the different fecal signatures of AS were derived from gut microbiome. Nevertheless, this study further indicates that AS differs between males and females and provides new directions for exploring the mechanisms of the differences in AS features between males and females.
References
Baysal, O. et al. Relationship between psychological status and disease activity and quality of life in ankylosing spondylitis. Rheumatol Int 31, 795–800, https://doi.org/10.1007/s00296-010-1381-x (2011).
Ljung, L., Sundstrom, B., Smeds, J., Ketonen, M. & Forsblad-d’Elia, H. Patterns of comorbidity and disease characteristics among patients with ankylosing spondylitis-a cross-sectional study. Clin Rheumatol 37, 647–653, https://doi.org/10.1007/s10067-017-3894-0 (2018).
Tam, L. S., Gu, J. R. & Yu, D. Pathogenesis of ankylosing spondylitis. Nat Rev Rheumatol 6, 399–405, https://doi.org/10.1038/nrrheum.2010.79 (2010).
Lee, W., Reveille, J. D. & Weisman, M. H. Women with ankylosing spondylitis: A review. Arthrit Rheum-Arthr 59, 449–454, https://doi.org/10.1002/art.23321 (2008).
van der Horst-Bruinsma, I. E., Zack, D. J., Szumski, A. & Koenig, A. S. Female patients with ankylosing spondylitis: analysis of the impact of gender across treatment studies. Annals of the rheumatic diseases 72, 1221–1224, https://doi.org/10.1136/annrheumdis-2012-202431 (2013).
Landi, M. et al. Gender differences among patients with primary ankylosing spondylitis and spondylitis associated with psoriasis and inflammatory bowel disease in an iberoamerican spondyloarthritis cohort. Medicine 95, https://doi.org/10.1097/Md.0000000000005652 (2016).
Ibn Yacoub, Y., Amine, B., Laatiris, A. & Hajjaj-Hassouni, N. Gender and disease features in Moroccan patients with ankylosing spondylitis. Clin Rheumatol 31, 293–297, https://doi.org/10.1007/s10067-011-1819-x (2012).
Tournadre, A. et al. Differences Between Women and Men With Recent-Onset Axial Spondyloarthritis: Results From a Prospective Multicenter French Cohort. Arthrit Care Res 65, 1482–1489, https://doi.org/10.1002/acr.22001 (2013).
Alzate, M. A. et al. Differences in Clinical Presentation by Gender in Colombian Patients with Spondyloarthropathies. Annals of the rheumatic diseases 76, 928–928, https://doi.org/10.1136/annrheumdis-2017-eular.3560 (2017).
Robinson, P. C. et al. Exome-wide study of ankylosing spondylitis demonstrates additional shared genetic background with inflammatory bowel disease. NPJ genomic medicine 1, 16008, https://doi.org/10.1038/npjgenmed.2016.8 (2016).
Ciccia, F., Rizzo, A. & Triolo, G. Subclinical gut inflammation in ankylosing spondylitis. Curr Opin Rheumatol 28, 89–96, https://doi.org/10.1097/BOR.0000000000000239 (2016).
Wen, C. et al. Quantitative metagenomics reveals unique gut microbiome biomarkers in ankylosing spondylitis. Genome Biol 18, 142, https://doi.org/10.1186/s13059-017-1271-6 (2017).
Costello, M. E. et al. Brief Report: Intestinal Dysbiosis in Ankylosing Spondylitis. Arthritis Rheumatol 67, 686–691, https://doi.org/10.1002/art.38967 (2015).
Gill, T., Asquith, M., Brooks, S. R., Rosenbaum, J. T. & Colbert, R. A. Effects of HLA-B27 on Gut Microbiota in Experimental Spondyloarthritis Implicate an Ecological Model of Dysbiosis. Arthritis Rheumatol 70, 555–565, https://doi.org/10.1002/art.40405 (2018).
Shao, T. J. et al. Characterization of ankylosing spondylitis and rheumatoid arthritis using H-1 NMR-based metabolomics of human fecal extracts. Metabolomics 12, https://doi.org/10.1007/s11306-016-1000-2 (2016).
van der Linden, S., Valkenburg, H. A. & Cats, A. Evaluation of diagnostic criteria for ankylosing spondylitis. A proposal for modification of the New York criteria. Arthritis and rheumatism 27, 361–368 (1984).
Xiao, M. et al. Gas Chromatography/Mass Spectrometry-Based Metabolomic Profiling Reveals Alterations in Mouse Plasma and Liver in Response to Fava Beans. PloS one 11, https://doi.org/10.1371/journal.pone.0151103 (2016).
Rizzo, A., Guggino, G., Ferrante, A. & Ciccia, F. Role of Subclinical Gut Inflammation in the Pathogenesis of Spondyloarthritis. Frontiers in medicine 5, 63, https://doi.org/10.3389/fmed.2018.00063 (2018).
Manasson, J. et al. Gut Microbiota Perturbations in Reactive Arthritis and Postinfectious Spondyloarthritis. Arthritis Rheumatol 70, 242–254, https://doi.org/10.1002/art.40359 (2018).
Gilis, E. et al. The Role of the Microbiome in Gut and Joint Inflammation in Psoriatic Arthritis and Spondyloarthritis. J Rheumatol 45, 36–39, https://doi.org/10.3899/jrheum.180135 (2018).
Asquith, M. et al. Intestinal Metabolites Are Profoundly Altered in the Context of HLA-B27 Expression and Functionally Modulate Disease in a Rat Model of Spondyloarthritis. Arthritis Rheumatol 69, 1984–1995, https://doi.org/10.1002/art.40183 (2017).
Stoll, M. L. et al. Fecal metabolomics in pediatric spondyloarthritis implicate decreased metabolic diversity and altered tryptophan metabolism as pathogenic factors. Genes and immunity 17, 400–405, https://doi.org/10.1038/gene.2016.38 (2016).
Karu, N. et al. A review on human fecal metabolomics: Methods, applications and the human fecal metabolome database. Analytica chimica acta 1030, 1–24, https://doi.org/10.1016/j.aca.2018.05.031 (2018).
Trimigno, A. et al. Identification of weak and gender specific effects in a short 3 weeks intervention study using barley and oat mixed linkage beta-glucan dietary supplements: a human fecal metabolome study by GC-MS. Metabolomics 13, https://doi.org/10.1007/S11306-017-1247-2 (2017).
Bjerrum, J. T. et al. Metabonomics of human fecal extracts characterize ulcerative colitis, Crohn’s disease and healthy individuals. Metabolomics 11, 122–133, https://doi.org/10.1007/s11306-014-0677-3 (2015).
Mathieu, S., Gossec, L., Dougados, M. & Soubrier, M. Cardiovascular profile in ankylosing spondylitis: a systematic review and meta-analysis. Arthritis Care Res (Hoboken) 63, 557–563, https://doi.org/10.1002/acr.20364 (2011).
Franck, H., Meurer, T. & Hofbauer, L. C. Evaluation of bone mineral density, hormones, biochemical markers of bone metabolism, and osteoprotegerin serum levels in patients with ankylosing spondylitis. J Rheumatol 31, 2236–2241 (2004).
Barella, L., Rota, C., Stocklin, E. & Rimbach, G. Alpha-tocopherol affects androgen metabolism in male rat. Annals of the New York Academy of Sciences 1031, 334–336, https://doi.org/10.1196/annals.1331.036 (2004).
Subbiah, M. T. & Kuksis, A. Conversion of beta-sitosterol to steroid hormones by rat testes in vitro. Experientia 31, 763–764 (1975).
Naziroglu, M., Akkus, S. & Celik, H. Levels of lipid peroxidation and antioxidant vitamins in plasma and erythrocytes of patients with ankylosing spondylitis. Clinical biochemistry 44, 1412–1415, https://doi.org/10.1016/j.clinbiochem.2011.09.005 (2011).
Corona-Bustamante, A. et al. Antioxidant activity of butyl- and phenylstannoxanes derived from 2-, 3- and 4-pyridinecarboxylic acids. Molecules 15, 5445–5459, https://doi.org/10.3390/molecules15085445 (2010).
Gao, P. et al. Integrated GC-MS and LC-MS plasma metabonomics analysis of ankylosing spondylitis. The Analyst 133, 1214–1220, https://doi.org/10.1039/b807369d (2008).
Yuille, S., Reichardt, N., Panda, S., Dunbar, H. & Mulder, I. E. Human gut bacteria as potent class I histone deacetylase inhibitors in vitro through production of butyric acid and valeric acid. PloS one 13, https://doi.org/10.1371/journal.pone.0201073 (2018).
Ruuska, M., Sahlberg, A. S., Colbert, R. A., Granfors, K. & Penttinen, M. A. Enhanced phosphorylation of STAT-1 is dependent on double-stranded RNA-dependent protein kinase signaling in HLA-B27-expressing U937 monocytic cells. Arthritis and rheumatism 64, 772–777, https://doi.org/10.1002/art.33391 (2012).
Acknowledgements
This study was financially supported by National Natural Science Foundation of China (No. 81703864, 81873269) and Natural Science Foundation of Zhejiang Province (No. LQ17H270002).
Author information
Authors and Affiliations
Contributions
Z.H. and C.W. designed the experiments. M.W. and H.L. performed the experiments. Z.H. analyzed the data. Z.H. and M.W. wrote the manuscript. All authors reviewed the manuscript.
Corresponding author
Ethics declarations
Competing Interests
The authors declare no competing interests.
Additional information
Publisher’s note: Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made. The images or other third party material in this article are included in the article’s Creative Commons license, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons license and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this license, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
He, Z., Wang, M., Li, H. et al. GC-MS-based fecal metabolomics reveals gender-attributed fecal signatures in ankylosing spondylitis. Sci Rep 9, 3872 (2019). https://doi.org/10.1038/s41598-019-40351-w
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41598-019-40351-w
This article is cited by
-
Lactobacillus maintains healthy gut mucosa by producing L-Ornithine
Communications Biology (2019)
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.