Abstract
Microbial resistance against clinical used antibiotics is on the rise. Accordingly, there is a high demand for new innovative antimicrobial strategies. The host-defense peptide human beta-defensin 1 (hBD-1) is produced continuously by epithelial cells and exhibits compelling antimicrobial activity after reduction of its disulphide bridges. Here we report that proteolysis of reduced hBD-1 by gastrointestinal proteases as well as human duodenal secretions produces an eight-amino acid carboxy-terminal fragment. The generated octapeptide retains antibiotic activity, yet with distinct characteristics differing from the full-length peptide. We modified the octapeptide by stabilizing its termini and by using non-natural D-amino acids. The native and modified peptide variants showed antibiotic activity against pathogenic as well as antibiotic-resistant microorganisms, including E. coli, P. aeruginosa and C. albicans. Moreover, in an in vitro C. albicans infection model the tested peptides demonstrated effective amelioration of C. albicans infection without showing cytotoxity on human cells. In summary, protease degradation of hBD-1 provides a yet unknown mechanism to broaden antimicrobial host defense, which could be used to develop defensin-derived therapeutic applications.
Similar content being viewed by others
Introduction
Antimicrobial peptides (AMPs) are evolutionary ancient peptide antibiotics produced by all multicellular organisms. They are part of the primary defense against microbial infections and exhibit antimicrobial activity against bacteria, fungi and some enveloped viruses1,2. Humans produce different classes of AMPs, one of them are the defensins. These secreted peptides are characterized by their small size (3 to 5 kDa), cationic net charge and six conserved cysteine residues, which are connected via three disulphide bridges1,3,4. Human beta-defensin 1 (hBD-1) was the first beta-defensin identified in humans and is produced by epithelia, monocytes, plasmacyoid dendritic cells and platelets5,6,7,8. In contrast to inducible beta-defensins 2 and 3, hBD-1 is produced constitutively and its expression can be regulated by peroxisome proliferator-activated receptor gamma (PPARγ) and hypoxia-inducible factor alpha (HIF1-α)6,9,10. We could recently show that antimicrobial activity of hBD-1 is strongly increased after reduction of its three disulphide bridges independent of bacterial Gram-status11,12. Activation of the peptide could be executed by a reducing environment or enzymatically by the oxido-reductase thioredoxin11,13.
Due to their ancient evolutionary origin and the strong demand for novel antimicrobial strategies, AMPs have been considered as potential antibiotic drug candidates. Mainly because they target “Achilles heels” of microorganisms, only few resistance mechanisms have been evolved over long time14,15. Still, large-scale chemical synthesis of defensins containing three native disulphide-bridges has been a challenge and rendered the production expensive. Accordingly, the production of smaller, but yet antibiotic, fragments of defensins without disulphide bridges is a promising option. We have shown previously that reduced hBD-1 can be degraded by the intestinal protease trypsin16. Here, we evaluate a carboxy-terminal fragment of hBD-1 that is generated after proteolytic digestion by intestinal proteases. We investigate its antimicrobial activity and its potential to be exploited as a possible candidate for future antibiotic drug development.
Results
Degradation of reduced hBD-1 generates an antimicrobial octapeptide
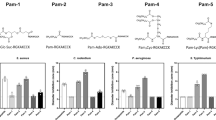
Reduction of the three disulphide bridges of hBD-1 yields a linear peptide which not only differs structurally from the oxidized form11, but is also more prone to proteolytic degradation by the protease trypsin16. To further analyze proteolytic susceptibility of hBD-1 (Fig. 1A) towards physiological gastro-intestinal proteases, we treated oxidized and reduced hBD-1 with pepsin and chymotrypsin (Fig. 1B). Similar to trypsin digestion, oxidized hBD-1 was protease resistant while the reduced form was readily digested. Focusing on the degradation products we detected a fragment having an m/z of 893.5, corresponding to the eight carboxy-terminal amino acids of hBD-1, NH2-RGKAKCCK-COOH (RGKAKCCK). To assess the in vivo relevance of our findings in more detail, we incubated oxidized and reduced hBD-1 with human duodenal secretion, which is rich in proteolytic enzymes. In agreement with our in vitro data, ex vivo digestion generated a fragment having an m/z of 893.5 (Fig. 1C) for reduced hBD-1 but not for oxidized hBD-1. While the in vivo presence of the octapeptide in the human gut remains to be proven, this finding supports the hypothesis that proteolytic cleavage of reduced hBD-1 could generate a novel antimicrobial peptide in the human intestine. To test whether antibiotic activity is retained in this degradation product we next analyzed antimicrobial activity of the terminal octapeptide. In a radial diffusion assay (RDA)17 we thus compared activity of oxidized and reduced hBD-1 with the octapeptide RGKAKCCK against selected commensal and pathogenic microorganisms (Fig. 1D). The octapeptide exhibited convincing activity against Bifidobacterium adolescentis, Streptococcus salivarius ssp. thermophilus, Escherichia coli, Candida albicans but neglectable antibiotic activity against Pseudomonas aeruginosa. While RGKAKCCK and oxidized hBD-1 generated no inhibition zones against Bifidobacterium breve, only reduced hBD-1 inhibited its growth. As expected, however, semi-quantitative evaluation on a molar base (4 µg reduced hBD-1 is equivalent to 254 µM in the RDA while 1 µg of octapeptide is equivalent to 280 µM) revealed that activity of the isolated terminus is less potent compared with the full length-peptide (Fig. 1D).
Proteolytic digestion of reduced hBD-1 generates an antimicrobial octapeptide. (A) Aminoacid sequence of hBD-1, depicted as one-letter code. (B) The oxidized and the reduced form of hBD-1 were digested with pepsin or chemotrypsin and fragments were analyzed by MALDI-MS. The carboxy-terminal fragment RGKAKCCK (893.5 Da, highlighted in (A) was further investigated. (C) The oxidized and the reduced hBD-1 were digested with human duodenal secretion and fragments were analyzed by MALDI-MS. Fragments were identified by comparison with an in silico digest using ExPASy software. (D) Different peptide concentrations of oxidized (ox) and reduced (red) as well as the carboxy-terminal octapeptide RGKAKCCK were tested in an antimicrobial diffusion assay against several microbial strains. Diameter of inhibition zones indicates antimicrobial activity; a diameter of 2.5 mm (dotted line) is the diameter of an empty well. (E,F) Modifications of RGKAKCCK (4 µg) were tested in an antimicrobial diffusion assay against E. coli and a fungal strain C. albicans. Letters indicate amino acid one-letter code. All diffusion assays were carried out at least three times, mean +/− SEM is shown.
We found previously that cysteine residues are crucial for antimicrobial activity of hBD-1 against E. coli and Bif. adolescentis11,12. We confirmed these results for the terminal octapeptide, as replacing both cysteines (RGKAKAAK) completely abolished activity against E. coli and C. albicans (Fig. 1E, Supplementary Fig. 1). However, replacing either Cys6 (RGKAKACK) or Cys7 (RGKAKCAK) by alanine resulted in strongly decreased activity against C. albicans, while antibiotic activity of those peptides increased against E. coli. Consequently, cysteine residues seem to have an important, yet different, role for the antibiotic mechanism against the tested fungi and bacteria.
As antimicrobial peptide activity also relies on a positive net charge18,19 we further investigated the role of positively charged amino acids (Fig. 1E). Despite having two cysteine residues, the variants lacking Arg1 (AGKAKCCK, net charge +3) or Arg1 and Lys3 (AGAAKCCK, net charge +2) were completely inactive against both tested microorganism. Thus, antimicrobial activity of the octapeptide RGKAKCCK (net charge +4) depends on cysteine residues as well as a particular positive charge. Yet, as a reversed-order peptide had lower activity than the wild-type peptide or a scrambled version, especially against C. albicans (Fig. 1F), not only the amino acid composition but also its sequential order or its position seem to be involved in the peptides’ activity.
Characterization of RGKAKCCK and its modified variants
Since the discovery of antimicrobial peptides there is anticipation to exploit them as antibiotic drugs20. To test the potential of our octapeptide to be used as a therapeutic agent, we first generated peptide variants to improve its stability. To prevent non-specific cleavage by amino-carboxypeptidases, we chemically stabilized its termini by amino-terminal acetylation and carboxy-terminal amidation (Ac-RGKAKCCK-NH2) and generated both peptides also in D-amino acid configuration (rGkakcck and Ac-rGkakcck-NH2, respectively).
Next, to evaluate the antibiotic activity, we tested wild-type and modified peptide variants in their ability to inhibit growth of (opportunistic) pathogenic microorganisms (Fig. 2A). Direct comparison revealed that those variants with stabilized termini had promising activity against E. coli and C. albicans. Moreover, while all peptides displayed antimicrobial activity at pH 7.4, a reducing environment (DTT), acidification (pH 5.7), or a combination of acidification and reducing conditions (pH 5.7 + DTT) strongly decreased antimicrobial activity against E. coli (Supplementrary Fig. 2a) and C. albicans (Supplementrary Fig. 2b). Thus, antimicrobial acitivity of the generated octapeptides can be influenced by environmental conditions, in particular by reducing conditions with an acidic pH.
Antimicrobial activity of RGKAKCCK and its modified variants. The carboxyterminal octapeptide RGKAKCCK was stabilized at its termini by acetylation of the amino-terminus and amidation of the carboxy-terminus (Ac-RGKAKCCK-NH2). Both variants were also synthesized by using D-stereoisomeric amino acids (indicated by small letters). Antimicrobial activity of octapeptides (4 µg) was tested against pathogenic microorganisms of clinical relevance (A) and with antibiotic resistance (B) in radial diffusion assay. 3-MRGN: multi-resistant Gram negative pathogen (3 out of 4 antibiotic classes), 4-MRGN: multi-resistant Gram negative pathogen (4 out of 4 antibiotic classes) MRSA: Methicillin-resistant Staphylococcus aureus, Amp/Imi: Ampicillin/Imipinem, Van: Vancomycin. (C) Different concentrations of octapeptides were tested in a turbidity liquid assay against E. coli ATCC 25922 and C. albicans ATCC 10231. Peptides were incubated with tested microorganisms and change in optical density (OD600nm) was measured and % growth of untreated control was plotted after 12 hours. (D) Aliquots were plated on agar plates and colony forming units (CFUs) were calculated the next day. Data are presented as mean +/− SEM of at least three independent experiments. The statistical significance was evaluated by using Kruskal-Wallis test compared to control and marked with *p < 0.05 and **p < 0.01.
The widespread use of antibiotics in agriculture and to treat bacterial infections has led to a rapid emergence of microbial resistance21,22. As a consequence, in hospitals several multi-drug resistant strains exist that threaten effective therapy of microbial infections23. We therefore tested if the hBD1-derived peptide and its modified forms are also active against drug-resistant clinical isolates. As shown in Fig. 2B, we identified antimicrobial activity against clinical isolates of antibiotic-resistant E. coli, Pseudomonas aeruginosa and Enterococcus faecium. In contrast, Acinetobacter baumanii was only susceptible towards Ac-rGkakcck-NH2 whereas Enterococcus faecalis and K. pneumoniae were not sensitive. Direct comparison of the tested peptide revealed that the peptides RGKAKCCK and Ac-rGkakcck-NH2 inhibited growth of the most tested antibiotic-resistant bacteria, making them the most promising candidates for further drug development among the four tested peptides.
As the radial diffusion assay does not differentiate between microbistatic and microbicidal activity and contains immobilized bacteria or fungal cells, we complemented our antimicrobial tests with a broth microdilution assay to investigate susceptibility of E. coli and C. albicans. The tested octapeptides completely inhibited C. albicans growth at concentrations of 100 µg/ml, while the growth of E. coli was only inhibited to 40% of the untreated control by Ac-rGkakcck-NH2 (Fig. 2C). In addition, microbial cultures were incubated with the different peptides and colony forming units (CFU) were determined. For E. coli incubated with 100 µg/ml of RGKAKCCK or Ac-RGKAKCCK-NH2, a more than 100-fold decrease in CFU was observed when compared to untreated controls (Fig. 2D). In contrast, CFU reduction of C. albicans was less pronounced, thus, indicating bactericidal activity against E. coli and a combination of fungicidal and fungistatic activity against C. albicans of the tested octapeptides.
Many antimicrobial peptides target the microbial membrane24,25. To test whether this is also true for the octapeptides, we used a flow cytometric assay measuring membrane permeability by the dye propidium iodide (PI), which cannot permeate intact membranes. E. coli and C. albicans were incubated with the peptides and PI uptake, which indicated cell death, was analysed. For E. coli, all tested peptides exhibited at least 70% bacterial killing, while treatment with RGKAKCCK, Ac-RGKAKCCK-NH2 or Ac-rGkakcck-NH2 led to almost 100% cell death (Fig. 3A). In contrast, only the wild-type peptide RGKAKCCK induced up to 60% PI uptake when incubated with C. albicans.
Characterization of mode of action in E. coli and C. albicans. (A) Membrane pores or (B) Membrane depolarization of 1 × 106 CFU E. coli ATCC 25922 or C. albicans ATCC 10231 in response to 100 µg/ml octapeptides were tested. Microorganisms were treated 1 h with 100 µg/ml peptide and living organisms were analyzed by flow cytometry. As control we used hBD3 (50 µg/ml) and Amphotericin B (20 µg/ml) and untreated strains. Data are presented as mean +/− SEM of at least three independent experiments. (C) Transmission electron microcopy of E. coli (upper panel) and C. albicans (lower panel) treated with 400 µg/ml peptide. Magnification bar: 0.5 µm.
In addition to PI uptake, we analyzed cellular membrane potential by using the membrane potential sensitive dye DiBAC4(3) (Fig. 3B). When incubating the peptides with E. coli, we observed strong membrane depolarization for the same peptides that caused PI uptake. In contrast, C. albicans displayed less than 20% of membrane depolarization. Thus, our results support a bactericidal effect of RGKAKCCK and Ac-rGkakcck-NH2 against E. coli by targeting the bacterial membrane, while the antibiotic effect against C. albicans seems rather membrane-independent.
To further investigate whether octapeptide treatment leads to structural damage of the microorganisms we used transmission electron microscopy (TEM) to visualize peptide-treated bacteria and fungi. Incubation of E. coli and C. albicans with all tested variants of the octapeptide led to different degrees of structural disintegration (Fig. 3C). This was especially pronounced in E. coli, where all peptides caused detachment of the cell membrane from the cytosol, cell wall and membrane disruption as well as disintegration of cytosolic structures. In C. albicans, however, no destruction of the fungal cell wall could be observed, confirming results from the flow cytometric expriments (Fig. 3A,B). Still, disintegration of cytosolic structures could also be observed in fungal cells, similar to the damage observed in E. coli. Taken together, our results demonstrate a bactericidal and fungicidal/fungistatic effect of the tested octapeptides.
Potential of the octapeptides for therapeutic drug development
For potential therapeutic application, toxicity of the peptides needs to be excluded. We therefore analyzed cell-toxicity of all peptide variants against the intestinal epithelial cell line CaCo-2 and against erythrocytes. By utilization of a WST viability test we could not observe any cell toxicity in the relevant antimicrobial concentration ranges of 100 µg/ml (Fig. 4A) and 200 µg/ml (Supplementrary Fig. 4a) or any hemolytic effect against erythrocytes (Fig. 4B and Supplementrary Fig. 4b).
Modified octapeptides are not cytotoxic. Cytotoxicity of octapeptides (100 µg/ml) was investigated by (A) WST-1 based test against the human intestinal epithelial cell lines CaCo-2 and (B) Hemolytic Activity assay against erythrocytes, using 2% Trition-X-100 and 1.25 µM Melittin as positive control. (C) Histological analysis of model oral epithelia treated with 100 µg/ml peptide and cytotoxicity was additionally tested by lactatdehydrogenase release against this model human oral epithelium. (D) Cytokine release of model oral epithelia was analyzed by ELISA. Mean +/− SEM of three independent experiments is shown.
We furthermore tested the toxicity of the octapeptides by using in vitro reconstituted human oral epithelium (RHOE), which was analyzed by histology and lactatdehydrogenase (LDH) activity (Fig. 4C). No LDH release was detected with peptide variants, whereas the cytotoxic compound Triton-X-100, used as a positive control, induced a strong release of LDH. Similarly, when quantifying the release of the pro-inflammatory cytokines Interleukin-8 (IL-8) and IL-1α after incubation of the RHOE with the octapeptides we did not detect any inflammatory response in the RHOE (Fig. 4D).
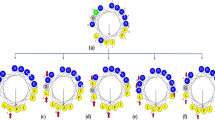
Suitability of the octapeptides as novel candidates for antimicrobial drug development was further substantiated in a model or oral candidiasis26. In this model a multilayer of RHOE was preincubated with 50 µg/ml (Fig. 5A) or 100 µg/ml octapeptides (Supplementrary Fig. 5) for 1 h before infecting the cells with C. albicans for 24 h (Fig. 5A). Epithelial damage of RHOEs was quantified by independent experts in a blinded manner on a scale between 0 and 5 (Fig. 5B). Untreated cells infected with C. albicans displayed evident epithelial damage and cell lysis and detectable fungi (coloured in red) in all layers of the epithelium. However, pre-treatment with RGKAKCCK convincingly reduced the fungal load in the epithelium and ameliorated epithelial damage. Additionally, a histological analysis confirmed the protective effect of RGKAKCCK (Fig. 5B) whereas a pre-treatment with 50 µg/ml rGkakcck moderately improved epithelial damage. In contrast, epithelial damage and a high amount of detectable fungal cells in lower epithelium were observed with a pre-treatment with the modified octapeptides Ac-RGKAKCCK-NH2 and Ac-rGkakcck-NH2: While C. albicans cells invaded the whole epithelium with a pre-treatment with Ac-RGKAKCCK-NH2, C. albicans invaded and damaged only the upper epithelium with a pre-treatment with Ac-rGkakcck-NH2. Consequently, our eight amino-acid peptide RGKAKCCK of the carboxy-terminus of hBD1 has the best potential to be optimized for topical application against infectious microbes on epithelial surfaces.
Octapeptides are potential candidates for antimicrobial drug development. (A) Reconstituted human oral epithelia were pre-incubated with PBS (control uninfected) or 50 µg/ml of octapeptides as indicated. Subsequently cells were infected with C. albicans SC5314 (highlighted in red). Representative images are shown (magnification 400x, bar = 100 µm). (B) Epithelial damage was evaluated by four independent experts and the combined evaluation (mean +/− SEM, criteria described in methods) is shown. The statistical significance was evaluated by using Kruskal-Wallis test with ns = not significant and *p < 0.05.
Discussion
So far, no multicellular organism has been identified which does not produce antimicrobial peptides. Even over a long time of evolution those host defense molecules have retained their antimicrobial capacity with only minor resistance mechanisms at the microbial target15,27. Thus, an improved knowledge of these antibacterial molecules may help to identify novel targets for antimicrobial therapy28. In fact, in the recent years short antimicrobial peptides have gained increased interest as new opportunities for therapeutics29. In here, we characterized a carboxy-terminal octapeptide of hBD-1 that was generated after proteolytic digestion by gastro-intestinal proteases and might thus occur in vivo in the human gastrointestinal tract.
While reduction of disulphide bridges increases activity of several antimicrobial peptides11,30,31, it also increases their susceptibility towards proteolytic digestion. This is especially relevant in the intestinal tract, where duodenal secretions contain high amounts of proteases to facilitate digestion of dietary proteins. However, our observation that a degradation product of hBD-1 retains antibiotic activity indicates effective utilization of a scare resource: we speculate that once the reduced peptides diffuse from the intestinal mucus layer towards the lumen, they can be degraded as soon as they come into contact with intestinal proteases. But instead of being inactivated, degradation products can retain their antimicrobial activity, thereby making the most effective use of these antimicrobial host defense molecules.
While a major shift in antimicrobial activity and activity spectrum can be observed after reduction of the oxidized hBD-1 (Fig. 1D, consistent with11,12,32, only minor alterations can be observed after degradation of the reduced peptide. However, on a molar basis the octapeptide does not exhibit the full potency of the full-length peptide, suggesting that the remaining 28 amino acids of hBD-1 hold additional features that enhance and modulate antibiotic activity as, for instance, observed for Bifidobacterium breve (Fig. 1D). Remarkably, and in contrast to hBD-1, a reducing environment diminished antimicrobial activity of the tested octapeptides against E. coli and C. albicans (Supplementrary Fig. 2). It is possible that due to their small size the peptides need to form dimers or higher-order oligomers to effectively penetrate the microbial cell wall. It is likely that such oligomerization occurs by forming intermolecular disulphide-bridges, thus explaining the strong dependence on cysteine residues for the activity of RGKAKCCK against E. coli and C. albicans (Fig. 1E). We could observe that human blood serum can influence bacterial growth and the antimicrobial activity (Supplementrary Fig. 3). Similarly, acidic pH led to lower antimicrobial activity as compared to pH 7.4 (Supplementrary Fig. 2). This is in accordance with previous studies, which could show that antimicrobial peptides can bind to human plasma proteins33,34. Thus, further optimization of a potential peptide formulation would be required to employ the octapeptide as a topical skin therapeutic, as human skin has a pH of about 5.5.
The cell envelope is a commonly discussed target for antimicrobial peptides35. While the full length hBD-1 targets the bacterial cell wall and entrapped bacteria in net-like structures, the octapeptides seem to have distinct antimicrobial mechanisms (Fig. 2D). Our methods revealed a breakdown of membrane potential and loss of membrane integrity in bacteria. In contrast, treated fungal cells displayed a functional membrane but cytosolic defects (Fig. 3). These data highlight that our octapeptides have diverse antibiotic strategies for different microorganisms. Remarkably, even for the same microbial species, we observed strain specific differences in susceptibility. While the P. aeruginosa ATCC type strain was not susceptible towards our octapeptides (Figs 1D and 2A), the multi-resistant P. aeruginosa 4-MRGN strain was susceptible (Fig. 2B). This is in accordance with previous studies, which could show that antibiotic-resistant bacteria show an increased sensitivity against antimicrobial peptides36.
Different peptides derived from β-defensins have already been investigated on their antimicrobial activity against bacteria and fungi37,38. For instance, 19-mer peptides derived from the carboxy-terminus of hBD-1 or −2 and a 22-mer derived from the terminus of hBD-3 were analyzed on their antibiotic activity. These peptides retained one disulphide bridge and had lethal concentrations in the low micromolar range. With our carboxy-terminal octapeptide we can facilitate synthesis by significantly shortening the amino acid sequence and by omitting the disulphide bridge. Most studies investigating defensin-based peptides have been focused on hBD-3, which is one of the most potent AMPs. By generating different amino-carboxy-terminal peptides, Hoover et al. identified several carboxy-terminal peptides with 9 to 14 amino acids having activity against E. coli or P. aeruginosa, but not against S. aureus39. In these peptides, cysteine residues were replaced by serine residues, which we found to be also crucial for activity in our peptides. Also, Reynold et al. described that antimicrobial activity of hBD-3 was mainly localized in the amino-terminal half40. Similar to our results, they reported that distinct amino acids are important for activity against different strains, suggesting that the strain-selectivity of such peptides can be modulated by varying the sequence.
To be utilized as potential antimicrobial molecules, it has to be excluded that the generated peptides provoke resistance of the treated microorganism. By using a host-derived antimicrobial peptide as therapeutic, this is of major importance, as resistance or cross-resistance towards other AMPs might be fatal for the host. While further testings are required to determine whether our identified peptides provoke such resistance, we believe that the octapeptide can serve as a backbone structure that could be optimized to enhance and/or specialize its activity and to diverge from its natural structure, which would decrease the risk of resistance induction. For example, due to their difference in activity against E. coli and C. albicans, optimization of the peptides RGKAKACK and RGKAKCAK (Fig. 1E) could generate a peptide that is effective against E. coli, but not against C. albicans.
In conclusion, we identified that the host can broaden its antimicrobial arsenal by generating several antibiotic molecules from the AMP hBD-1, depending on its redox state and proteolytic degradation. We believe that this strategy can be therapeutically exploited and that our identified hBD-1 derived carboxy-terminal peptides can be optimized for topical application against bacterial or fungal infections.
Materials and Methods
Bacterial and fungal strains
Bacterial strains (Bifidobacterium adolescentis Ni,29c (clinical isolate), Bifidobacterium breve (from probiotic VSL#3) and Streptococcous salivarius ssp. thermophiles DSM 20617 were obtained from Ardeypharm (Germany). Escherichia coli ATCC 25922, Escherichia coli K12, Pseudomonas aeruginosa ATCC 27853, Candida albicans ATCC 10231, Enterococcus faecalis ATCC 29212 as well as antibiotic-resistant clinical isolates of Acinetobacter baumannii, Enterococcus faecalis, Enterococcus faecium, Klebsiella pneumoniae, Escherichia coli, Staphylococcus aureus and Pseudomonas aeruginosa were provided by the Department for Laboratory Medicine at Robert-Bosch-Hospital Stuttgart, Germany. Candida albicans SC5314 was obtained from Salomé LeibundGut-Landmann (Institute of Immunology, Vetsuisse Faculty, University of Zürich, Switzerland).
Peptides
Carboxy-terminal octapeptides were chemically synthesized by EMC Microcollections (Tuebingen, Germany) and purified by precipitation. The oxidized peptides were obtained from Peptide Institute (Japan). All peptides were dissolved in 0.01% acetic acid.
Protease digestion and Matrix-assisted laser desorption/ionization mass spectrometry (MALDI-MS)
2 µg of oxidized or reduced hBD-1 were digested with pepsin or chymotrypsin at a protease: peptide ratio of 1:20 in HCl-acidified water, pH 3 (pepsin) or 10 mM sodium phosphate, pH 7.4 (chymotrypsin) for 90 min. Human duodenal secretion (pH 6.5–7) was taken during a routine gastroscopy by rinsing the duodenum with saline. Oxidized and reduced hBD-1 were incubated with human duodenal secretion for 30 min at 37 °C. As a control both peptides were incubated with 0.9% NaCl. Peptides were enriched with ZipTip (Millipore), co-crystallized with a-cyano-4-hydroxy cinnamic acid and analyzed with an ultraflex TOF/TOF machine (Bruker, Germany).
Radial diffusion assay
Antimicrobial radial diffusion assay was modified from reference17 and performed as described earlier11. Briefly, microorganisms were cultivated (anaerobic bacteria with AnaeroGen, Oxoid, UK) for up to 18 hours in liquid TSB medium. Log-phase cultures were washed and diluted to 4 × 106 colony forming units in 10 ml agar. Incubation was carried out in 10 ml of 10 mM sodium phosphate, either pH 7.4 or 5.7, containing 0.3 mg/ml of TSB powder and 1% (w/v) low EEO-agarose (AppliChem) with 0 or 1 mM dithiothreitol (DTT, Sigma-Aldrich) under anaerobic or aerobic conditions for three hours. 1 or 4 µg of synthetic, oxidized hBD-1 (Peptide Institute, Japan) and 1 or 4 µg of synthetic peptides (EMC Microcollections, Tuebingen) were filled into small punched wells in a final volume of 4 µl. This concentrated peptide solution dilutes while diffusing into the gel, thereby generating concentration-dependent, round-shaped inhibition zones when killing immobilized microorganisms.
An overlay-gel containing 6% (w/v) TSB powder, 1% agarose and 10 mM sodium phosphate buffer without DTT was poured onto the plates and after incubation for up to 48 h at 37 °C the diameter of inhibition zones was measured. Experiments were repeated at least three times; mean + SEM is shown.
Microdilution broth assay
To differentiate between microbistatic and microbicidal activity we performed a broth microdilution assay. For that, E. coli ATCC25922 bacteria were incubated overnight at 37 °C, 150 rpm. C. albicans ATCC 10231 was grown at 30 °C overnight, 150 rpm in liquid TSB. Cells were collected by centrifugation (2500 rpm, 10 min, 4 °C), washed twice and resuspended in 10 mM sodium phosphate buffer containing 1% (w/v) TSB broth. Required C. albicans cell density was adjusted using a hemocytometer. For bacteria the optical density of OD600nm = 0.1 was determined. Approximately 5 × 105 CFU/ml bacteria or fungi were mixed with indicated peptide concentrations (1.25–200 µg/ml) in a final volume of 100 µl in 10 mM sodium phosphate buffer containing 1% (w/v) TSB broth and incubated for 2 hours at 37 °C. After incubation 10 µl per well were plated on LB-/ or YPD-agar plates to determine the CFU/ml. After that 100 µl of 6% TSB (w/v) were added and absorbance was measured at 600 nm (Tecan, Switzerland) and monitored for 18 hours. Growth relative to the positive control in % was plotted against peptide concentration. Experiments were carried out at least three times; mean ± SEM is shown.
Flow cytometry assay
Approximately 1.5 × 106 CFU log-phase bacteria or overnight cultured C. albicans ATCC 10231 were used in a final volume of 100 µl TSB (1:6 diluted H2O). We added peptides in concentrations 50 and 100 µg/ml in a final volume of 10 µl and incubated theses suspensions for 1 h at 37 °C. Subsequently 2 µl of membrane potential sensitive dye DiBAC4(3) [bis-[1,3-dibutylbarituric acid)trimethine oxonol] (Thermo Scientific, USA) (50 µg/ml) or Propidium Iodide (Thermo Scientific, USA) (50 µg/ml) were added and incubated for 10 min at room temperature. Then samples were centrifuged (5 min, 7000 rpm, RT) and re-suspended in 300 µl PBS. The percentage of fluorescent positive cells was determined using Canto II flow cytometer (BD Bioscience) with DIVA software (BD Bioscience) as described earlier41. Experiments were repeated at least three times and mean +/− SEM is shown.
Transmission electron microscopy
Approximately 1 × 108 CFU of E. coli ATCC 25922 and C. albicans ATCC 10231 were incubated with 400 µg/ml peptides or control solution for 2 hours at 37 °C. Treated microorganism were fixed with Karnovsky’s fixative (3% Paraformaldehyd, 3.6% Glutaraldehyd, pH 7,2) and embedded in 3.5% agarose at 37 °C, coagulated at room temperature, and fixed again in Karnovsky’s fixative. Post-fixed samples (1% OsO4, 1 h) were rinsed with distilled water, block-stained with uranyl acetate (2% in distilled water), dehydrated in alcohol (stepwise 30–96%), immersed in propylene oxide and embedded in glycine ether (polymerized 48 h at 60 C, Serva, Heidelberg). Ultra-thin sections were examined with a LIBRA 120 (Carl Zeiss AG, Oberkochen) at 120 kV.
Metabolic activity Assay
To assess the metobalic activity of Caco-2 cells we used the WST-1 Cell Proliferation Reagent (Roche, Germany). Briefly, 1 × 105 Cells /ml were seeded and incubated with 100 µg/ml or 200 µg/ml octapeptides for 24 h at 37 °C, 5% CO2. After incubation the supernatant was removed and cells were washed with PBS and incubated with 20 µl Cell Proliferation Reagent WST-1 for 1 h 37 °C, 5% CO2. Finally the absorbance was measured at 450 nm and 620 nm. Experiments were repeated three times, mean+/− SEM.
Hemolytic Activity of antimicrobial peptides
An hemolytic activity assay for testing antimicrobial peptides was performed as described earlier42. Briefly, 150 µl of melittin (5 µM) was added to the positive control wells and incubated overnight. On the next day 1 ml blood was added to 3 ml PBS, mixed gently and centrifuged for 8 min, 700 × g. The supernatant was discarded and cells were re-suspended in 4 ml PBS and centrifuged again. After removing the supernatant, cells were centrifuged for 8 min at 1000 × g. Supernatant was discarded. For each well we used 75 µl of 1% Red blood cell (RBC) suspension in PBS. RBC suspension was mixed with indicated peptide concentration (2.5–200 µg/ml) in a final volume of 150 µl and incubated for 1 h at 37 °C. Finally the plate was centrifuged at 1000 × g for 10 min and 60 µl of supernatant was quickly transferred into a new plate. The absorbance was measured by 405 nm and 540 nm. Hemolytic activity was plotted relative to the 0.2% Triton X-100. Experiments were repeated three times; mean +/− SEM is shown.
Culture of a model human oral epithelium
1 × 106 TR146 cells (derived from a squamous cell carcinoma of the buccal mucosa; SkinEthic, France) were seeded into polycarbonate plastic inserts (Millipore) in DMEM (Lonza) and cultured for 8 days to form a multilayered epithelium. Medium in the wells (basal) and in the inserts (apical) was changed daily. On day 5 (airlift) medium was aspired from the apical side and cells were fed from the basal side for the rest of culture time in 6-well-plates. No antibiotics were used for the entire time of culture and the experiments43. The octapeptides were diluted to 100 µg/ml in 0.01% acetic acid and 50 µl of these dilutions were applied to the apical side of the model epithelia and incubated for 24 h. The supernatant was used for cytotoxicity assays and Enzyme-linked immunosorbent assay.
LDH-Cytotoxicity Assay
To analyze the damage of the epithelial cells caused by octapeptides, release of lactate dehydrogenase (LDH) into the supernatant of RHOEs was quantified, using the cytotoxicity detection kit with L-LDH solution as standard, according to the manufacturer’s instructions (Roche, Germany). Supernatants of RHOEs were analyzed 24 h post infection.
Enzyme-linked immunosorbent assay
Interleukin 8 (IL8) and IL1α were quantified in the supernatants of RHOEs using DuoSet ELISA-Kits (RnD Systems, US) according to the manufacturer’s instructions. Further details are explained above (Culture of a model human oral epithelium).
Infection of model human oral epithelium with C. albicans
Octapeptides were diluted to 50 µg/ml in PBS, or an equivalent volume of 0.01% acetic acid were applied to the apical side of the RHOEs and incubated for 1 h. C. albicans SC5314 was synchronized as described previously26. Yeast cells were washed three times in PBS and 1 × 105 CFU were used for infection of pre-treated RHEs. After 24 h RHEs were fixed with Karnovsky’s fixative. Post-fixed samples (1% OsO4, 1 h) were rinsed with distilled water, block-stained with uranyl acetate (2% in distilled water), dehydrated in alcohol (stepwise 30–96%), immersed in propylene oxide and embedded in glycide ether (polymerized 48 h at 60 °C, Serva, Heidelberg). Semi-thin sections were stained with toluidine blue and examined with a Nikon Eclipse 80i light microscope (magnification 1:400). Afterwards, fungal cells were simply coloured in red. Epithelial damage was evaluated by two independent experts in a blinded manner on a scale between 0 and 5 with 0 = intact epithelia, 1 = damage only in topmost cell layer; 2 = damage in top third of epithelium; 3 = damage in top half of epithelium; 4 = damage in all cell layers except lowermost; 5 = damage in all epithelial layers.
Ethics statement
The study protocol was previously approved by the Ethical Committee of the University Hospital, Tuebingen, Germany. Patients and controls who were included in this study all gave their written and informed consent after the study purpose, samples procedure, and potential adjunctive risks were explained. All experiments were conducted in accordance with the relevant guidelines and regulations.
Statistical analysis
Results are presented as mean +/− SEM from at least three independent experiments. Statistical analysis was performed using GraphPad Prism 7.03. The Data were not normally distributed and a Kruskal-Wallis test was performed. *Indicate statistically signifant differences compared to infected control. P-values, showing the statistical significance, were displayed by asterisks: p > 0.05 = ns; *p ≤ 0.05; **p ≤ 0.01; ***p ≤ 0.001; ****p ≤ 0.0001.
References
Zasloff, M. Antimicrobial peptides of multicellular organisms. Nature 415, 389–395 (2002).
Bevins, C. L. Antimicrobial peptides as effector molecules of mammalian host defense. Contrib. Microbiol. 10, 106–148 (2003).
Martin, E., Ganz, T. & Lehrer, R. I. Defensins and other endogenous peptide antibiotics of vertebrates. J. Leukoc. Biol. 58, 128–136 (1995).
Harder, J., Gläser, R. & Schröder, J.-M. Human antimicrobial proteins effectors of innate immunity. J. Endotoxin Res. 13, 317–338 (2007).
Bensch, K. W., Raida, M., Mägert, H. J., Schulz-Knappe, P. & Forssmann, W. G. hBD-1: a novel beta-defensin from human plasma. FEBS Lett. 368, 331–335 (1995).
Zhao, C., Wang, I. & Lehrer, R. I. Widespread expression of beta-defensin hBD-1 in human secretory glands and epithelial cells. FEBS Lett. 396, 319–322 (1996).
Ryan, L. et al. Modulation of human beta-defensin-1 (hBD-1) in plasmacytoid dendritic cells (PDC), monocytes, and epithelial cells by influenza virus, Herpes simplex virus, and Sendai virus and its possible role in innate immunity. J. Leukoc. Biol. 90, 343–399 (2011).
Kraemer, B. F. et al. Novel anti-bacterial activities of β-defensin 1 in human platelets: suppression of pathogen growth and signaling of neutrophil extracellular trap formation. PLoS Pathog. 7 (2011).
Peyrin-Biroulet, L. et al. Peroxisome proliferator-activated receptor gamma activation is required for maintenance of innate antimicrobial immunity in the colon. Proc. Natl. Acad. Sci. USA 107, 8772–8777 (2010).
Kelly, C. J. et al. Fundamental role for HIF-1α in constitutive expression of human β defensin-1. Mucosal Immunol, https://doi.org/10.1038/mi.2013.6 (2013).
Schroeder, B. O. et al. Reduction of disulphide bonds unmasks potent antimicrobial activity of human β-defensin 1. Nature 469, 419–423 (2011).
Raschig, J. et al. Ubiquitously expressed Human Beta Defensin 1 (hBD1) forms bacteria-entrapping nets in a redox dependent mode of action. PLOS Pathog. 13, e1006261 (2017).
Jaeger, S. U. et al. Cell-mediated reduction of human β-defensin 1: a major role for mucosal thioredoxin. Mucosal Immunol, https://doi.org/10.1038/mi.2013.17 (2013).
Andersson, D. I., Hughes, D. & Kubicek-Sutherland, J. Z. Mechanisms and consequences of bacterial resistance to antimicrobial peptides. Drug Resist. Updat. Rev. Comment. Antimicrob. Anticancer Chemother. 26, 43–57 (2016).
Fleitas, O., Agbale, C. M. & Franco, O. L. Bacterial resistance to antimicrobial peptides: an evolving phenomenon. Front. Biosci. Landmark Ed. 21, 1013–1038 (2016).
Schroeder, B. O., Stange, E. F. & Wehkamp, J. Waking the wimp: redox-modulation activates human beta-defensin 1. Gut Microbes 2, 262–266 (2011).
Lehrer, R. I., Rosenman, M., Harwig, S. S., Jackson, R. & Eisenhauer, P. Ultrasensitive assays for endogenous antimicrobial polypeptides. J. Immunol. Methods 137, 167–173 (1991).
Taylor, K., Barran, P. & Dorin, J. Structure-activity relationships in beta-defensin peptides. Biopolymers 90, 1–8 (2008).
Lehrer, R. I. Immunology: Peptide gets in shape for self-defence. Nature 469, 309–310 (2011).
Kruse, T. & Kristensen, H.-H. Using antimicrobial host defense peptides as anti-infective and immunomodulatory agents. Expert Rev. Anti Infect. Ther. 6, 887–895 (2008).
Taubes, G. The bacteria fight back. Science 321, 356–361 (2008).
Chait, R., Vetsigian, K. & Kishony, R. What counters antibiotic resistance in nature? Nat. Chem. Biol. 8, 2–5 (2012).
Ventola, C. L. The Antibiotic Resistance Crisis. Pharm. Ther. 40, 277–283 (2015).
Mathew, B. & Nagaraj, R. Variations in the interaction of human defensins with Escherichia coli: Possible implications in bacterial killing. PloS One 12, e0175858 (2017).
Mukherjee, S. et al. Antibacterial membrane attack by a pore-forming intestinal C-type lectin. Nature 505, 103–107 (2014).
Schaller, M., Zakikhany, K., Naglik, J. R., Weindl, G. & Hube, B. Models of oral and vaginal candidiasis based on in vitro reconstituted human epithelia. Nat. Protoc. 1, 2767–2773 (2006).
Peschel, A. & Sahl, H.-G. The co-evolution of host cationic antimicrobial peptides and microbial resistance. Nat. Rev. Microbiol. 4, 529–536 (2006).
Nizet, V. Antimicrobial peptide resistance mechanisms of human bacterial pathogens. Curr. Issues Mol. Biol. 8, 11 (2006).
Fosgerau, K. & Hoffmann, T. Peptide therapeutics: current status and future directions. Drug Discov. Today 20, 122–128 (2015).
Masuda, K., Sakai, N., Nakamura, K., Yoshioka, S. & Ayabe, T. Bactericidal Activity of Mouse α-Defensin Cryptdin-4 Predominantly Affects Noncommensal Bacteria. Journal of Innate Immunity 3(3), 315–326 (2011).
Schroeder, B. O. et al. Paneth cell α-defensin 6 (HD-6) is an antimicrobial peptide. Mucosal Immunology 8(3), 661–671 (2015).
Wendler, J. et al. Bacterial Periplasmic Oxidoreductases Control the Activity of Oxidized Human Antimicrobial β-Defensin 1. Infect. Immun. 86, e00875–17 (2018).
De Breij, A. et al. The antimicrobial peptide SAAP-148 combats drug-resistant bacteria and biofilms. Sci. Transl. Med. 10 (2018).
Wang, Y., Johansson, J., Agerberth, B., Jörnvall, H. & Griffiths, W. J. The antimicrobial peptide LL-37 binds to the human plasma protein apolipoprotein A-I. Rapid Commun. Mass Spectrom. 18, 588–589 (2004).
Wilmes, M., Cammue, B. P. A., Sahl, H.-G. & Thevissen, K. Antibiotic activities of host defense peptides: more to it than lipid bilayer perturbation. Nat. Prod. Rep. 28, 1350–1358 (2011).
Lázár, V. et al. Antibiotic-resistant bacteria show widespread collateral sensitivity to antimicrobial peptides. Nat. Microbiol. 3, 718–731 (2018).
Krishnakumari, V., Singh, S. & Nagaraj, R. Antibacterial activities of synthetic peptides corresponding to the carboxy-terminal region of human beta-defensins 1-3. Peptides 27, 2607–2613 (2006).
Krishnakumari, V., Rangaraj, N. & Nagaraj, R. Antifungal activities of human beta-defensins HBD-1 to HBD-3 and their C-terminal analogs Phd1 to Phd3. Antimicrob. Agents Chemother. 53, 256–260 (2009).
Hoover, D. M., Wu, Z., Tucker, K., Lu, W. & Lubkowski, J. Antimicrobial characterization of human beta-defensin 3 derivatives. Antimicrob. Agents Chemother. 47, 2804–2809 (2003).
Reynolds, N. et al. Peptide fragments of a beta-defensin derivative with potent bactericidal activity. Antimicrob. Agents Chemother. 54, 1922–1931 (2010).
Nuding, S., Fellermann, K., Wehkamp, J., Mueller, H. A. G. & Stange, E. F. A flow cytometric assay to monitor antimicrobial activity of defensins and cationic tissue extracts. J. Microbiol. Methods 65, 335–345 (2006).
Oddo, A. & Hansen, P. R. Hemolytic Activity of Antimicrobial Peptides. Methods Mol. Biol. Clifton NJ 1548, 427–435 (2017).
Mailänder-Sánchez, D. et al. Antifungal defense of probiotic Lactobacillus rhamnosus GG is mediated by blocking adhesion and nutrient depletion. PloS One 12, e0184438 (2017).
Acknowledgements
We thank Marion Strauß for excellent technical assistance and Birgit Fehrenbacher, Renate Nordin and Theresia Schneider (University Hospital Tuebingen, Department of Dermatology) for performing electron microscopic analyses. This work was supported by Deutsche Forschungsgemenischaft (DFG) and Heisenberg Professorship (JW).
Author information
Authors and Affiliations
Contributions
Ju.W. and B.O.S. wrote the first manuscript draft. B.O.S., D.E. and Ju.W. performed the majority of the experiments and revised the manuscript. L.K., D.M.S., C.L. and S.W. performed some of the electron microscopy experiments and assisted in the maintenance of human oral epithelium model and antimicrobial assays. M.S., E.F.S., N.P.M., C.W. and S.L. were involved in data discussion and writing the manuscript. J.W. was involved in data discussion, evaluation of experiments, writing of the manuscript and design on the study. All autorhs were involved in data discussion and the final version of the manuscript.
Corresponding author
Ethics declarations
Competing Interests
The authors J.W., B.S., E.F.S. filed a patent application on therapeutic usage of reduced hBD-1.
Additional information
Publisher’s note: Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made. The images or other third party material in this article are included in the article’s Creative Commons license, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons license and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this license, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Wendler, J., Schroeder, B.O., Ehmann, D. et al. Proteolytic Degradation of reduced Human Beta Defensin 1 generates a Novel Antibiotic Octapeptide. Sci Rep 9, 3640 (2019). https://doi.org/10.1038/s41598-019-40216-2
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41598-019-40216-2
This article is cited by
-
Curbing gastrointestinal infections by defensin fragment modifications without harming commensal microbiota
Communications Biology (2021)
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.