Abstract
Development of effective therapeutics and treatment strategy to promote recovery after cerebral ischemia-reperfusion injury necessitates further understandings of the complex pathophysiology of ischemic stroke. Given that α5-GABAAR inhibition has been shown to be involved in functional recovery after stroke, the present study was designed to evaluate the effects of treatment timing of α5 GABAAR inhibition on post-middle cerebral artery occlusion (MCAO) functional recovery. To this end, we examined the effects of L655,708 (α5 GABAAR inverse agonist) treatment at 3 or 7 days post-ischemia on apoptosis and neurogenesis in the peri-infarct region, brain infarction size, as well as modified neurological severity score (mNSS) and rotarod test time in rats. Consistent with previous reports, we found that when the treatment of L655,708 was initiated at post-MCAO day 3, it did not alter the functional recovery in rats. However, when the treatment of L655,708 was initiated at post-MCAO day 7, it demonstrated beneficial effects on functional recovery in rats. Interestingly, this phenomenon was not associated with altered brain infarction size nor with changes in brain cell apoptosis. However, we found that delayed treatment of L655,708 at post-MCAO day 7 significantly increased neurogenesis in peri-infarct zone in rats. These results suggested that removing α5 GABAAR-mediated tonic inhibition after cerebral ischemia-reperfusion injury may be an effective therapeutic strategy for promoting functional recovery from stroke.
Similar content being viewed by others
Introduction
Ischemic stroke is a common type of stroke and is a major cause of neurological disability worldwide1. Restoration of blood flow following ischemic stroke can be achieved by means of thrombolysis or mechanical recanalization. However, reperfusion may exacerbate the injury initially caused by ischemia. Thus, it will bring significant societal and health impacts by preventing cerebral ischemia-reperfusion injury and/or promoting function recovery to reduce dependence and improve the quality of life of stroke survivors. However, development of effective therapeutics and treatment strategy necessitates further understandings of the complex pathophysiology of ischemic stroke.
Previous studies suggested that recovery of function following acute brain injury to the cortical regions can be promoted by the reduction of brain GABA availability2. These findings suggest targeting of GABA receptors that mediate tonic inhibition could be a novel strategy to promote post-stroke functional recovery. However, recent studies indicated that GABA receptor, specifically α5-GABAAR, may play distinct roles in a time-dependent manner after stroke during the recovery. Specifically, in a cortical stroke model, treatment with α5-GABAAR inverse agonist immediately after stroke increased size of the cortical lesion3. However, the same study also demonstrated that treatment with α5-GABAAR inverse agonist at 3 days after stroke significantly promoted functional recovery in mice3. However, the neurobiological mechanisms underlying this phenomenon are still not clear. In fact, neuronal plasticity can occur after stroke, particularly in the peri-infarct zone that is adjacent to the region damaged by the stroke4. In addition to irreversible neuronal damage, brain ischemia can trigger apoptosis5 and induce neurogenesis6,7, which can contribute to functional recovery after stroke5,6. Hence, α5-GABAAR inverse agonist induced functional recovery may be resulted from a complex interplay among apoptosis and neurogenesis following brain ischemia.
Therefore, in the present study, we tested the hypothesis that delayed treatment with α5-GABAAR inverse agonists can enhance functional recovery after MCAO-induced brain ischemia-reperfusion injury in rodents. To this end, we examined the effects of L655,708 treatment at 3 or 7 days post-ischemia on apoptosis and neurogenesis in the peri-infarct region, brain infarction size, as well as modified neurological severity score (mNSS) and rotarod test time in rats.
Materials and Methods
Animals
Adult male Sprague–Dawley (SD) rats weighing between 250 and 300 g were ordered from Shanghai Experimental Animal Center. Upon arrival, animals were housed in a 12–12-hour light-dark cycle environment. The room temperature was controlled at 25 °C, and animals were allowed to access food and water ad libitum throughout the study. The use of animal was approved by the Institutional Animal Care and Use Committee of National Institute for Viral Disease Control and Prevention, China Center for Disease Control and Prevention, Beijing, and all animal experiments were conducted in accordance with the Guide for the Use of Laboratory Animals.
Transient middle cerebral artery occlusion (MCAO) model and animal treatment
Rats were under isoflurane anesthesia. We exposed the right middle cerebral artery (MCA) through a cranial burr hole, which was located approximately 2.5 mm lateral and 2.0 mm posterior to the bregma. The blood flow of MCA was monitored using a Laser Doppler flowmetry (Moor Instruments Inc., Wilmington, USA). The blood flow of MCA was above 500 min/div before MCAO procedure. We then exposed both the right common carotid artery (CCA) and internal carotid artery (ICA) via a neck midline incision, followed by the ligation of the pterygopalatine artery proximal to its branch. We then inserted a 3–0 nylon filament suture coated with poly-L-lysine (Sigma-Aldrich, Shanghai, China) into the right external carotid artery through the CCA and moved it up to the ICA at a distance of 20–25 mm to block the right MCA. As a result, the blood flow of MCA was decreased to less than 100 min/div (>80%). Blood flow from the right MCA was blocked for 15 minutes, followed by removing the suture for reperfusion (a return to >7% of the baseline within 10 min of suture withdrawal). Sham-operated rats received the same surgery process without the MCAO. The treatment with L655,708 (α5-GABAAR inverse agonist, 0, 1, or 5 mg/kg) was initiated at post-MCAO days 3 and 7. Rats received intraperitoneal injections of vehicle (i.e., saline) or L655,708 once daily for 4 consecutive days. Sham-operated rats received no treatment, and a separate group of MCAO rats received vehicle injections once daily for 4 consecutive days starting at post-MCAO day 1.
Modified neurological severity score (mNSS) assessment and rotarod test (RRT)
Modified neurological severity score (mNSS) assessment was performed at post-MCAO day 14 by a well-trained research associated who was blinded to the experimental conditions. The mNSS scale provides a behavior deficit score, reflecting motor, sensory, balance, and reflex functions as described previously8,9. A normal score was represented by 0 and the maximal deficit score was 18. The rotarod test was conducted in an apparatus (Harvard Apparatus, Holliston, MA, USA) consisted of a striated rod. In the present study, each rat was first trained for 3 days on a rotarod cylinder before testing, as described previously10. At post-MCAO day 14, rats were tested for the time performed during the rotarod test.
Triphenyltetrazolium chloride (TTC) staining
We sectioned the rat brain from the frontal pole into six slices with 2 mm thickness. The brain slices were stained with 2% 2,3,5-triphenyl tetrazolium chloride (Sigma-Aldrich, Shanghai, China) for 15 minutes. The ischemic infarction area was stained white, and the non-ischemic infarction area was stained red. We took the images of each brain slice (n = 8), and the ratio of the ischemic area to the ipsilateral hemisphere area (I/H ratio) was calculated using total ischemic area divided by total ipsilateral hemisphere area with NIH Image J.
Tissue preparation for histochemistry
All rats were sacrificed after the completion of behavioral function tests at day 14 after MCAO (n = 8 per group at each time point) with an overdose of 10% chloral hydrate. Rats were then perfused transcardially with 0.9% saline at 4 °C followed by 4% paraformaldehyde in phosphate buffer (0.1 mol/L, pH 7.4) based on the methods described previously11. Rat brains were quickly removed, fixed in 4% paraformaldehyde for at least 8 hours at 4 °C, and then restored in 20% and 30% sucrose. 10-μm thick coronal sections were prepared using a cryostat (CM1900; Leica, Shanghai, China) from bregma + 4.0 to −6.0 mm. Tissues were then used for subsequent immunoflourescence staining or TUNEL staining.
Immunofluorescence staining
Brain sections were first pretreated with citrate buffer (0.01 mol/L, pH 6.0) for 5 minutes at 85 °C, followed by incubation with 5% normal goat serum for 1 hour at room temperature. Sections were then incubated with anti-Ki67 (rabbit monoclonal antibody to Ki67, 1:500; Cat# ab16667 RRID: AB_302459; Abcam, Shanghai, China) and anti-NeuN (rabbit monoclonal antibody to NeuN, 1:500; Cat# ab190565, RRID:AB_2732785; Abcam, Shanghai, China), overnight at 4 °C. Sections were then rinsed in phosphate-buffered saline 3 times, followed by incubation with rabbit secondary antibody (anti-rabbit IgG, 1:1000, Cell Signaling, Shanghai, China) for 1 hour at room temperature. Fluorescence signals were then detected under a microscope (BX51; Olympus, Japan). Negative control was conducted by incubating sections with PBS instead of primary antibodies. No positive signals were shown in negative control.
Terminal deoxynucleotidyl transferase dUTP nick end labeling (TUNEL)
TUNEL staining was performed as previously described12 using recombinant terminal deoxynucleotidyl transferase (TdT), following the manufacturer’s instructions (Roche, Shanghai, China). TUNEL signal was detected with Alexa 488-labelled secondary antibody for streptavidin. Cell nuclei were stained with DAPI. Negative controls of TUNEL staining were performed without TdT.
Image analysis and quantification
Image-Pro Plus image analysis software (Media Cybernetics, Silver Spring, MD, USA) was used for images data analysis. Data analysis was conducted by a researcher who was blinded to the experimental conditions. We focused on the region in the peri-infarct zone, which was immediately outside the infarct zone. To count TUNEL/Ki67-immunopositive cells, 8 consecutive sections from bregma 0.20 to −2.20 mm with 240-μm interval were included for analysis. The number of TUNEL/Ki67-immunopositive cells in the peri-infarct region was counted in 3 separate, non-overlapping fields (425 μm × 320 μm) under ×400 magnification. The average cell number per field was used for each section, the average cell number of all the sections was used as the final cell number per rat13.
Statistical analysis
All data were presented as mean ± SEM. Statistical analysis was performed using SPSS 18.0 for Windows (SPSS Inc, Chicago, IL, USA). One-way ANOVA or t-test were used to evaluate mNSS, rotarod time, Ki67-positive and TUNEL-positive cell numbers for each treatment starting time groups. *p < 0.05 is considered to be significant when comparison was made.
Results
Effects of delayed treatment of L655,708EA on MNSS in MCAO rats
We evaluated the effects of L655,708 treatment on neurological function using Modified Neurological Severity Score (MNSS) scale (Fig. 1). When the treatment was initiated at post-MCAO day 3 for 7 consecutive days, the MNSS of vehicle-treated rats was 6.3 ± 1.1. Similarly, the MNSS of 1 mg/kg or 5 mg/kg L655,708-treated rats were 6.5 ± 0.9 and 6.2 ± 1.0, respectively. In contrast, when the treatment was initiated at post-MCAO day 7 for 7 consecutive days, L655,708-treated rats exhibited significantly (p < 0.05) lower MNSS. Specifically, the MNSS of vehicle-treated rats was 6.4 ± 0.8. However, the MNSS of 1 mg/kg or 5 mg/kg L655,708-treated rats were 4.7 ± 0.9 and 3.6 ± 0.9, respectively.
Effects of delayed treatment of L655,708EA on rotarod test time in MCAO rats
The rotarod test times were higher in the sham group (183.2 ± 14.1 s) than in vehicle-treated MCAO control group (56.5 ± 12.4 s; Fig. 2). When the treatment was initiated at post-MCAO day 3 for 7 consecutive days, the rotarod test time of vehicle-treated rats was 61.3 ± 14.2. Similarly, the rotarod test time of 1 mg/kg or 5 mg/kg L655,708-treated rats were 58.5 ± 12.9 and 54.6 ± 13.7, respectively. In contrast, when the treatment was initiated at post-MCAO day 7 for 7 consecutive days, L655,708-treated rats exhibited significantly (p < 0.05) lower rotarod test time. Specifically, the rotarod test time of vehicle-treated rats was 65.2 ± 14.7. However, the rotarod test time of 1 mg/kg or 5 mg/kg L655,708-treated rats were 90.9 ± 15.2 and 128.8 ± 13.7, respectively.
Effects of delayed treatment of L655,708 on the volume of the infarct area
To test the effects of treatment of L655,708 on the volume of the infarct area, when the treatment was initiated at post-MCAO day 7, we collected rat brains at post-MCAO day 14, and carried out TTC staining (Fig. 3A). We found that the relative infarct volume was 30.1 ± 4.6% in vehicle-treated group at post-MCAO day 14 (Fig. 3B). The relative infarct volumes of 1 mg/kg or 5 mg/kg L655,708-treated rats were 28.5 ± 7.1% and 32.1 ± 6.7% respectively, at post-MCAO day 14 (p = 0.31; Fig. 3B). These results indicated that delayed treatment of L655,708 after MCAO did not alter the volume of the infarct area.
Effects of delayed treatment of L655,708 on apoptosis in the peri-infarct region
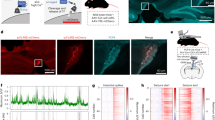
We conducted TUNEL assays to examine the cell apoptosis in the peri-infarct region at post-MCAO day 14. We first found that TUNEL-positive cells were limited in sham-operated group (Fig. 4A,B) and in the contra-lateral hemisphere (data not shown). In contrast, MCAO robustly increased the number of TUNEL-positive cells in peri-infarct region at post-MCAO day 14 (Fig. 4A,B). MCAO rats that received vehicle treatment initiated at post-MCAO day 1, 3, and 7 once daily for 7 consecutive days exhibited increased number of TUNEL-positive cells in the ipsilateral hemisphere (Fig. 4A,B). Furthermore, neither 1 mg/kg nor 5 mg/kg of L655,708 treatment initiated at post-MCAO day 3 and 7 once daily for 7 consecutive days altered the number of TUNEL-positive cells in the ipsilateral hemisphere compared with vehicle (Fig. 4A,B).
Effects of delayed treatment of L655,708 on apoptosis in the peri-infarct region. TUNEL assays were performed to examine the cell apoptosis in the peri-infarct region at post-MCAO day 14 (n = 8/group). Representative images of cresyl violet-stained brain sections (scale bar = 1 mm) and terminal deoxynucleotidyl transferase-mediated dUTPnick end-labeling (TUNEL)-stained section (scale bar = 50 µm). Squares in the cresyl violet-stained section are the three regions used to quantify TUNEL + cells. TUNEL-stained section shows the infarct border. Scale bar = 1 mm.
Effects of delayed treatment of L655,708 on neurogenesis in the peri-infarct region
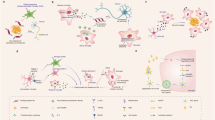
We used Ki67, a proliferative marker, and NeuN, a neuronal marker, to evaluate neurogenesis in the peri-infarct region. We first found that Ki67-positive cells were limited in sham-operated group and in the contra-lateral hemisphere (data not shown). In contrast, MCAO robustly increased the number of Ki67-positive cells in peri-infarct region at post-MCAO day 14. MCAO rats that received vehicle treatment initiated at post-MCAO day 1, 3, and 7 once daily for 7 consecutive days exhibited increased number of Ki67-positive/NeuN-positive cells in the ipsilateral hemisphere (Fig. 5A,B). Furthermore, 1 mg/kg or 5 mg/kg of L655,708 treatment initiated at post-MCAO day 3 and 7 once daily for 7 consecutive days significantly (p < 0.05) increased the number of Ki67-positive cells in the ipsilateral hemisphere compared with vehicle (p < 0.05; Fig. 5C).
Effects of delayed treatment of L655,708 on neurogenesis in the peri-infarct region. Ki67, a proliferative marker, and NeuN, a neuronal marker, were used to evaluate neurogenesis in the peri-infarct region. The nuclei were counter-stained with DAPI. Asterisk represents the significant difference from vehicle (n = 8/group; p < 0.05). Pond represents the significant difference from 1 mg group (n = 8/group; p < 0.05). Scale bar = 25 µm.
Discussion
The present study was designed the evaluate the effects of treatment timing of α5 GABAAR inverse agonist on post-MCAO functional recovery. Consistent with previous reports, we found that when the treatment with L655,708, selective α5 GABAAR inverse agonist, was initiated at post-MCAO day 3, it did not alter the functional recovery in rats. However, when the treatment of L655,708 was initiated at post-MCAO day 7, it demonstrated beneficial effects on functional recovery in rats. Interestingly, this phenomenon was not associated with altered brain infarction size nor with changes in brain cell apoptosis. However, we found that delayed treatment of L655,708 at post-MCAO day 7 significantly increased neurogenesis in peri-infarct zone in rats. These results suggested that removing α5 GABAAR-mediated tonic inhibition after stroke may be an effective therapeutic strategy for promoting functional recovery from stroke.
GABA, as a primary inhibitory neurotransmitter in central nervous system, has received increasing attention in ischemic brain injury14,15. Recent reports have demonstrated that increasing GABAergic synaptic transmission might display neuroprotective effects against brain ischemia-reperfusion injury16,17. GABA can activate three types of specific receptors: GABAA, GABAB and GABAC receptors18. Among them, GABAA receptors play an important role in regulating the dynamic balance between neuronal inhibition and excitation19. Importantly, a previous study has shown that in a cortical stroke model, treatment with α5-GABAAR inverse agonist immediately after ischemia-reperfusion injury increased size of the cortical lesion3, suggesting that activation of α5-GABAAR may be protective. Hence, future studies will test whether activation of α5-GABAAR prior the occurrence of stroke can reduce subsequent ischemia-reperfusion injury.
Currently, physical rehabilitation is the only available therapy for patient with ischemic stroke to promote functional recovery, and no pharmacological therapy has been approved by the FDA for this indication20,21. Despite this situation, studies have demonstrated that limited capacity for functional recovery after stroke exist in the brain. These post-stroke neural repair process involves recovery of physiological functions in tissue adjacent to or connected with the stroke22,23, including changes in neuronal excitability that alter the brain’s representation of motor and sensory functions. Studies have shown that enhancing neuronal excitability in peri-infarct zone can have beneficial outcome in recovery. Specifically, it has been demonstrated that stimulation of peri-infarct cortex alters sensorimotor maps and improves use of affected limbs22,23,24,25. One possible mechanism underlying this phenomenon might involve altered GABAergic transmission. This is because GABAergic transmission plays a critical role in the changes of sensory maps during cortical development26, a phenomenon resembling the changes of sensorimotor maps that occur after stroke27,28. Furthermore, numerous studies have demonstrated that GABAergic neurotransmission play a fundamental role in neuronal excitability29. GABAAR-mediated cortical GABAergic signaling consist of both synaptic and extrasynaptic components. Tonically active extrasynaptic GABAARs is involved in controlling the excitability threshold of neurons30,31,32. Among these extrasynaptic GABAARs, α5 or δ-subunit-containing receptors are the majority30,31,32. Pharmacological inhibition and genetic knockdown of α5 GABAAR can enhance LTP and improve performance on learning and memory tasks33,34. These studies suggested that α5-GABAAR is critical for cellular excitability and plasticity. Recent studies showed that enhancing levels of cell-intrinsic neuronal activity could increase survival of new neurons. Therefore, it is likely that removing α5 GABAAR-mediated tonic inhibition after stroke that promoted functional recovery from stroke may involve changes in neuronal excitability in the peri-infarct cortex after stroke leading to enhance survival of new neurons. Hence, future studies will be necessary to clarify the role of neuronal excitability in the peri-infarct cortex after stroke in neurogenesis.
One of the important factors that should be considered for pharmacotherapy development is the timing of pharmacological treatment. It has been shown that activation of GABAARs at the onset of stroke can reduce stroke size35. Therefore, it is likely that inhibition of GABAAR at earlier time after ischemic stroke may increase cell death and stroke size. In fact, previous studies using L655,708 have shown that stroke volume was significantly increased in animals treated with L655,708 at the onset of stroke, but when the same treatment was introduced to rats with a 3-day delay, stroke volumes were similar between mice treated with vehicle and L655,708. These results clearly indicate there is a critical timeframe to introduce the therapeutic to allow for inhibition of tonic GABAAR: inhibition of tonic GABAAR too early would promote stroke damage, while delaying inhibition of tonic GABAAR would promote functional recovery without altering stroke size. Adding to this literature, our study further demonstrated that a longer delay (i.e., 7 days after stroke) before the introduction of L655,708 can promote functional recovery.
In summary, our study confirmed that α5-GABAAR in the peri-infarct zone plays a critical role in neurogenesis and functional recovery for ischemic stroke. These results may provide an important pharmacological target that allows for promoting recovery after stroke.
References
Kwakkel, G., Kollen, B. & Lindeman, E. Understanding the pattern of functional recovery after stroke: facts and theories. Restorative neurology and neuroscience 22, 281–299 (2004).
Levy, L. M., Ziemann, U., Chen, R. & Cohen, L. G. Rapid modulation of GABA in sensorimotor cortex induced by acute deafferentation. Ann Neurol 52, 755–761 (2002).
Clarkson, A. N., Huang, B. S., Macisaac, S. E., Mody, I. & Carmichael, S. T. Reducing excessive GABA-mediated tonic inhibition promotes functional recovery after stroke. Nature 468, 305–309 (2010).
Murphy, T. H. & Corbett, D. Plasticity during stroke recovery: from synapse to behaviour. Nat Rev Neurosci 10, 861–872 (2009).
Zheng, Y. Q., Liu, J. X., Li, X. Z., Xu, L. & Xu, Y. G. RNA interference-mediated downregulation of Beclin1 attenuates cerebral ischemic injury in rats. Acta Pharmacol Sin 30, 919–927 (2009).
Nygren, J., Wieloch, T., Pesic, J., Brundin, P. & Deierborg, T. Enriched environment attenuates cell genesis in subventricular zone after focal ischemia in mice and decreases migration of newborn cells to the striatum. Stroke 37, 2824–2829 (2006).
Ziemka-Nalecz, M. & Zalewska, T. Endogenous neurogenesis induced by ischemic brain injury or neurodegenerative diseases in adults. Acta Neurobiol Exp (Wars) 72, 309–324 (2012).
Lin, Y.-W. & Hsieh, C.-L. Electroacupuncture at Baihui acupoint (GV20) reverses behavior deficit and long-term potentiation through N-methyl-d-aspartate and transient receptor potential vanilloid subtype 1 receptors in middle cerebral artery occlusion rats. Journal of integrative neuroscience 9, 269–282 (2010).
Cheng, C.-Y. et al. Ferulic acid reduces cerebral infarct through its antioxidative and anti-inflammatory effects following transient focal cerebral ischemia in rats. The American journal of Chinese medicine 36, 1105–1119 (2008).
Sunwoo, Y.-Y. et al. A pilot study for the neuroprotective effect of Gongjin-dan on transient middle cerebral artery occlusion-induced ischemic rat brain. Evidence-Based Complementary and Alternative Medicine 2012 (2012).
Hu, X. et al. Physical exercise induces expression of CD31 and facilitates neural function recovery in rats with focal cerebral infarction. Neurol Res 32, 397–402 (2010).
De Bilbao, F. et al. Cell death is prevented in thalamic fields but not in injured neocortical areas after permanent focal ischaemia in mice overexpressing the anti‐apoptotic protein Bcl‐2. European Journal of Neuroscience 12, 921–934 (2000).
Zhang, J. et al. Autophagosomes accumulation is associated with β‐amyloid deposits and secondary damage in the thalamus after focal cortical infarction in hypertensive rats. Journal of neurochemistry 120, 564–573 (2012).
Mao, X. et al. Topiramate attenuates cerebral ischemia/reperfusion injury in gerbils via activating GABAergic signaling and inhibiting astrogliosis. Neurochem Int 60, 39–46 (2012).
Qi, S.-H., Liu, Y., Wang, W.-W., Wang, M. & Zhang, G.-Y. Neuroprotection of ethanol against cerebral ischemia/reperfusion induced brain injury through GABA receptor activation. Brain research 1276, 151–158 (2009).
Green, A. R., Hainsworth, A. H. & Jackson, D. M. GABA potentiation: a logical pharmacological approach for the treatment of acute ischaemic stroke. Neuropharmacology 39, 1483–1494 (2000).
Galeffi, F., Sinnar, S. & Schwartz‐Bloom, R. D. Diazepam promotes ATP recovery and prevents cytochrome c release in hippocampal slices after in vitro ischemia. Journal of neurochemistry 75, 1242–1249 (2000).
Johnston, G. GABAA receptor pharmacology. Pharmacology & therapeutics 69, 173–198 (1996).
Jacob, T. C., Moss, S. J. & Jurd, R. GABA A receptor trafficking and its role in the dynamic modulation of neuronal inhibition. Nature Reviews Neuroscience 9, 331 (2008).
Dobkin, B. H. Training and exercise to drive poststroke recovery. Nat Clin Pract Neurol 4, 76–85 (2008).
Cramer, S. C. Drugs to Enhance Motor Recovery After Stroke. Stroke 46, 2998–3005 (2015).
Carmichael, S. T. Cellular and molecular mechanisms of neural repair after stroke: making waves. Ann Neurol 59, 735–742 (2006).
Nudo, R. J. Mechanisms for recovery of motor function following cortical damage. Curr Opin Neurobiol 16, 638–644 (2006).
Alonso-Alonso, M., Fregni, F. & Pascual-Leone, A. Brain stimulation in poststroke rehabilitation. Cerebrovasc Dis 24(Suppl 1), 157–166 (2007).
Di Lazzaro, V. et al. Motor cortex plasticity predicts recovery in acute stroke. Cereb Cortex 20, 1523–1528 (2010).
Hensch, T. K. Critical period plasticity in local cortical circuits. Nat Rev Neurosci 6, 877–888 (2005).
Donoghue, J., Suner, S. & Sanes, J. Dynamic organization of primary motor cortex output to target muscles in adult rats II. Rapid reorganization following motor nerve lesions. Experimental Brain Research 79, 492–503 (1990).
Foeller, E., Celikel, T. & Feldman, D. E. Inhibitory sharpening of receptive fields contributes to whisker map plasticity in rat somatosensory cortex. J Neurophysiol 94, 4387–4400 (2005).
Hess, G., Aizenman, C. D. & Donoghue, J. P. Conditions for the induction of long-term potentiation in layer II/III horizontal connections of the rat motor cortex. J Neurophysiol 75, 1765–1778 (1996).
Glykys, J. & Mody, I. Hippocampal network hyperactivity after selective reduction of tonic inhibition in GABA A receptor alpha5 subunit-deficient mice. J Neurophysiol 95, 2796–2807 (2006).
Carver, C. M. & Reddy, D. S. Neurosteroid interactions with synaptic and extrasynaptic GABA(A) receptors: regulation of subunit plasticity, phasic and tonic inhibition, and neuronal network excitability. Psychopharmacology (Berl) 230, 151–188 (2013).
Walker, M. C. & Semyanov, A. Regulation of excitability by extrasynaptic GABA(A) receptors. Results Probl Cell Differ 44, 29–48 (2008).
Collinson, N. et al. Enhanced learning and memory and altered GABAergic synaptic transmission in mice lacking the alpha 5 subunit of the GABAA receptor. J Neurosci 22, 5572–5580 (2002).
Atack, J. R. et al. L-655,708 enhances cognition in rats but is not proconvulsant at a dose selective for α5-containing GABA A receptors. Neuropharmacology 51, 1023–1029 (2006).
Cui, Y. et al. Neurofibromin regulation of ERK signaling modulates GABA release and learning. Cell 135, 549–560 (2008).
Acknowledgements
The Doctoral Scientific Research Foundation of Affiliated Hospital of Inner Mongolia University for the Nationalities (2018BS001).
Author information
Authors and Affiliations
Contributions
W.-M.H. performed experiments, analyzed results and wrote first draft, Y.-F.L. performed experiments and analyzed results, H.W. analyzed results, prepared figures and helped in first draft, Y.-P.P. helped in concept development, provided resources and approved manuscript.
Corresponding author
Ethics declarations
Competing Interests
The authors declare no competing interests.
Additional information
Publisher’s note: Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made. The images or other third party material in this article are included in the article’s Creative Commons license, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons license and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this license, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
He, WM., Ying-Fu, L., Wang, H. et al. Delayed treatment of α5 GABAA receptor inverse agonist improves functional recovery by enhancing neurogenesis after cerebral ischemia-reperfusion injury in rat MCAO model. Sci Rep 9, 2287 (2019). https://doi.org/10.1038/s41598-019-38750-0
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41598-019-38750-0
This article is cited by
-
Effect of prior exposure to enriched environment on cellular apoptosis after experimental stroke
Molecular Biology Reports (2022)
-
Hippocampal Inhibitory Synapsis Deficits Induced by α5-Containing GABAA Receptors Mediate Chronic Neuropathic Pain–Related Cognitive Impairment
Molecular Neurobiology (2022)
-
GABAB receptor antagonist promotes hippocampal neurogenesis and facilitates cognitive function recovery following acute cerebral ischemia in mice
Stem Cell Research & Therapy (2021)
-
NT3P75-2 gene-modified bone mesenchymal stem cells improve neurological function recovery in mouse TBI model
Stem Cell Research & Therapy (2019)
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.