Abstract
ABC transporters are conserved in prokaryotes and eukaryotes, with humans expressing 48 transporters divided into 7 classes (ABCA, ABCB, ABCC, ABCD, ABDE, ABCF, and ABCG). Throughout the human body, ABC transporters regulate cAMP levels, chloride secretion, lipid transport, and anti-oxidant responses. We used a bioinformatic approach complemented with in vitro experimental methods for validation of the 48 known human ABC transporters in airway epithelial cells using bronchial epithelial cell gene expression datasets available in NCBI GEO from well-characterized patient populations of healthy subjects and individuals that smoke cigarettes, or have been diagnosed with COPD or asthma, with validation performed in Calu-3 airway epithelial cells. Gene expression data demonstrate that ABC transporters are variably expressed in epithelial cells from different airway generations, regulated by cigarette smoke exposure (ABCA13, ABCB6, ABCC1, and ABCC3), and differentially expressed in individuals with COPD and asthma (ABCA13, ABCC1, ABCC2, ABCC9). An in vitro cell culture model of cigarette smoke exposure was able to recapitulate select observed in situ changes. Our work highlights select ABC transporter candidates of interest and a relevant in vitro model that will enable a deeper understanding of the contribution of ABC transporters in the respiratory mucosa in lung health and disease.
Similar content being viewed by others
Introduction
The respiratory mucosa, extending from the upper airways down to simple squamous epithelium, provides a continuous physical barrier with immune function that helps protect us from any potentially harmful substances contained in the air we breathe1,2. The many functions of the respiratory mucosa include the ability to produce cytokines to coordinate immune responses, regulate ion concentrations for airway surface lining fluid and mucus function, and detect viral entry into epithelial cells for antiviral immune responses. In health, these coordinated functions can ensure that infections, allergens, and exposures to air pollution are controlled to limit damage to host, while in disease, a dysfunction in any capacity of the respiratory mucosa may lead to development or exacerbation of chronic respiratory disease. It is therefore important to understand the mechanisms that regulate respiratory mucosa function.
A relatively unexplored contributor to respiratory mucosa biology is the ATP Binding Cassette (ABC) family of transporters3,4,5,6,7,8. ABC transporters are conserved in prokaryotes and eukaryotes, with humans expressing 48 transporters divided into 7 classes (ABCA, ABCB, ABCC, ABCD, ABDE, ABCF, and ABCG)9,10. The majority of ABC transporters couple ATP hydrolysis to the extracellular transport of substrates. ABC transporters have been demonstrated to transport cytokines, ions, lipids, as well as detect viral insults, although the confirmation of these functions and expression of these genes and protein has not been extensively confirmed in the respiratory mucosa of humans9,10. ABC transporter expression in human airway epithelial cells may contribute to respiratory mucosal immunity by modulating the lung environment in response to environmental exposures including cigarette smoke, allergens, air pollution, bacteria, and viruses.
The precedent for the importance of ABC transporters in respiratory mucosa biology has been set by the identification of mutations in ABC transporter genes in patients with lung pathologies. ABCC7, also known as cystic fibrosis transmembrane conductance regulator (CFTR), is the causal gene contributing to the development of cystic fibrosis11,12. Over 2000 variants in CFTR have been reported, resulting in altered chloride and bicarbonate secretion, hydration of the airway surface lining fluid, and mucus function11,12. Equally convincing of the role of ABC transporters in lung health and disease is the link between genetic loss of function variants of ABCA3 and fatal surfactant deficiency in newborns13. In addition, our group has recently confirmed that ABCC4 is expressed in airway epithelial cells4,5, is able to transport cAMP and uric acid5, and can modulate anti-inflammatory activities of long-acting beta-agonist/glucocorticoid therapies6 and potentiate CFTR in select patient populations14. These three mechanistic and clinically relevant examples represent only a fraction of the 48 transporters that remain to be more extensively studied in the respiratory mucosa for expression patterns and function in lung health and disease.
We have initiated a characterization of all 48 ABC transporters in the respiratory mucosa by performing a bioinformatic analysis of 9 distinct gene-expression datasets of primary human airway epithelial cells isolated from bronchial brushings of well-phenotyped healthy subjects and individuals that smoke cigarettes, or have been diagnosed with COPD or asthma15,16,17,18,19,20,21,22,23. Our hypothesis was that specific ABC transporter gene expression patterns would correlate with presence of a specific chronic respiratory disease and disease severity. To validate our bioinformatic analyses, we interrogated select results using an in vitro cell culture model system to provide a foundational platform for further interrogation of candidate ABC transporters identified that may be important in chronic respiratory disease pathology. Our in situ human gene expression data analysis reveals that ABC transporters are i) variably expressed in epithelial cells from different airway generations, ii) regulated by cigarette smoke exposure, iii) differentially expressed in individuals with COPD and asthma, and iv) are amenable to interrogation with in vitro cell culture systems. We conclude that continued research into the basic biology of ABC transporters in the respiratory mucosa with mechanistic approaches is required to truly define the importance of these molecules in lung health and disease.
Methods
Dataset selection and quality control
Analysis was performed on previously deposited datasets obtained from the Gene Expression Omnibus (GEO). Datasets pertaining to smoking and COPD analysis include GSE994, GSE4498, GSE11784, GSE11906, and GSE37147. Datasets focusing on asthma and severity include GSE4302, GSE63142, GSE67472, and GSE7622715,16,17,18,19,20,21,22,23.
Since the datasets were generated from a variety of studies, microarray chip selection and data normalization methods vary across the datasets. GSEs 11906, 11784, 4498, and 994 used the MAS5 normalization method without log transformation, whereas GSEs 76227, 4302, 67472, and 37147 used the Robust Multi-array Average (RMA) method with log transformation. GSE63142 used normalization method, cyclic LOESS. To avoid applying multiple compounding normalization methods, datasets were left as provided by the original studies and differences in methods noted, with specific mention of the normalization method denoted in each figure axis. Since probeset IDs and corresponding gene targets vary across microarray platforms, expression results are reported in the context of both ABC transporter name and probeset ID. All dataset demographics are available in Supplementary Table 1.
ABC transporter transcript expression in human airway epithelial cells
Differential expression patterns for all 48 ABC transporter members were examined across the trachea, large airways (generation 2nd-3rd), and small airways (generation 10th-12th) using GSE11906 (Affymetrix Human Genome U133 Plus 2 microarray platform)18. A bar plot showing average expression of ABC transporters in healthy, non-smoker lung tissue was generated using the ggplot2 package in R (v. 3.4.3). In GSE11906, independent samples of epithelial cells were isolated from healthy individuals with no smoking history and normal lung function and included 17 trachea, 21 large airway, and 35 small airway samples(15).
Impact of cigarette smoke exposure on ABC transporter expression
Three datasets (GSE11906, GSE11784, and GSE4498), which were all generated from the Affymetrix Human Genome U133 Plus 2 microarray platform, were used to assess the impact of cigarette smoke exposure on ABC transporter gene expression16,17,18. All three datasets are comprised of small airway (10th-12th generation) epithelial cell transcript expression patterns in healthy subjects and those with a history of smoking without a diagnosis of COPD. In GSE11906, 54 independent samples of epithelial cells were isolated from individuals with >25 pack years smoking history with no reported COPD18. In GSE11784, 72 independent samples of epithelial cells were isolated from individuals with >25 pack years smoking history with no reported COPD17. In GSE4498, 10 independent samples of epithelial cells were isolated from individuals with >25 pack years smoking history with no reported COPD16. We independently curated these three GSE datasets to ensure that no samples were repeated across the analyses.
Impact of cigarette smoking cessation on ABC transporter expression
Two datasets (GSE37147 and GSE994) generated from two distinct microarray platforms (Affymetrix Human Gene 1 ST and Affymetrix Human Genome U133A, respectively), analyzed epithelial cells from medium (6th-8th generation) and large (2nd generation) airways, respectively, were used to assess the impact of smoking cessation on ABC transporter gene expression15,19. In GSE37147, independent samples of epithelial cells were isolated from 69 current smokers and 82 former smokers with >47 pack years smoking history with no reported COPD19. In GSE37147, the average duration of smoking cessation was 11.11 years. In GSE994, independent samples of epithelial cells were isolated from 34 current smokers, 14 former smokers, and 23 never-smokers, with >22 pack years smoking history with no reported COPD15. In GSE994, the average duration of smoking cessation was 10.49 years.
Association between COPD status and changes in ABC transporter expression
Three datasets (GSE11906, GSE11784, and GSE37147) were used to assess association of COPD status with ABC transporter gene expression profile. GSE11906 and GSE11784 collected epithelial cells from small airways (10th-12th generation) while GSE37147 collected from medium airways (6th-8th generation), with the two different sample types also analyzed on different microarray platforms (Affymetrix Human Genome U133 Plus 2 and Affymetrix Human Gene 1 ST, respectively).
In GSE11906, 20 independent samples of epithelial cells were isolated from individuals with >38 pack years smoking history with reported COPD and were compared to 54 independent samples of epithelial cells isolated from individuals with >25 pack years smoking history with no reported COPD18. In GSE11784, 36 independent samples of epithelial cells were isolated from individuals with >34 pack years smoking history with reported COPD and were compared to 72 independent samples of epithelial cells isolated from individuals with >25 pack years smoking history with no reported COPD17. In GSE37147, 87 independent samples of epithelial cells were isolated from individuals with >51 pack years smoking history with reported COPD and were compared to 151 independent samples of epithelial cells isolated from individuals with >47 pack years smoking history with no reported COPD19.
ABC transporter expression patterns in airway epithelial cells from asthmatics
For asthma-focused analyses two pairs of datasets were used: GSE4302 and GSE6747220,21,22 – which allowed for healthy control comparison to individuals with asthma and GSE63142 and GSE7622721,22,23 – which allowed for associating expression profiles with asthma severity. All studies analyzed epithelial cells from medium (3rd-5th generation) airways, while distinct microarray platforms were used (GSE4302 and GSE67472 used Affymetrix Human Genome U133 Plus 2, GSE63142 used Agilent 014850 Whole Human Genome Microarray 4 × 44K, and GSE76227 used Affymetrix HT HG U133 plus PM).
In GSE4302, independent samples of epithelial cells were isolated from 28 healthy individuals and 42 asthmatics20. In GSE67472, independent samples of epithelial cells were isolated from 43 healthy individuals and 62 asthmatics22. In GSE63142, independent samples of epithelial cells were isolated from 26 healthy individuals, 59 mild asthmatics, 19 moderate asthmatics and 51 severe asthmatics21. In GSE76227, independent samples of epithelial cells were isolated from 26 healthy individuals, 59 mild asthmatics, 19 moderate asthmatics and 51 severe asthmatics23.
In vitro validation of candidate ABC transporter gene expression changes
A cigarette smoke extract conditioned media experiment with the Calu-3 airway epithelial cell line grown was performed as previously described24. qPCR for ABCA13 (forward: 5′-TGTGCTATTGTAACTCCTCTGAGAC-3′, reverse 5′-AAGTAATGACCTCTTGCAAAATACG-3′) and ABCC1 (forward: 5′-GCCTATTACCCCAGCATCG-3′, reverse 5′- GATGCAGTTGCCCACACA-3′) was performed by quantitative-PCR. Cell viability was determined using an LDH assay.
Dataset compiling and statistical analyses
Curated datasets contained the data matrix and relevant categorical data such as smoking status, disease status or airway location from which samples were isolated. Lists of probeset IDs for each microarray platform used in the study were generated using only probes that corresponded to ABC transporter proteins. Lists were used to filter corresponding matrices to include data exclusively for probes that target ABC transporters across datasets.
Pairwise Mann-Whitney U tests were performed to assess the statistical significance of differential gene expression between conditions. Adjusted p-values (q-values) were derived using the Benjamini Hochberg multiple hypothesis testing correction as implemented in R (v 3.4.3). This statistical method was chosen because a priori analysis of all dataset distributions showed that the data was non-Normal. Non-parametric methods such as Mann-Whitney U (which is the non-parametric equivalent of the unpaired Student’s T-test) make no assumptions about distribution and are therefore preferred for the analysis of non-Normal data.
Boxplots were generated for individual probesets using the ggplot2 package in R (v. 3.4.3). Boxplots visualize the minimum value (bottom of vertical line), first to third quartile (box), median (horizontal line within box), and maximum value (top of vertical line) of a data distribution. To visualize the underlying raw data distributions, individual data values were plotted as points on top of each boxplot with randomized horizontal skew.
For GSE994 which includes more than 2 independent categorical variables (current, former and never smokers) we used the Kruskal-Wallis test. The Kruskal-Wallis test is a non-parametric alternative to the one-way ANOVA test that does not assume a data distribution. The Tukey Honest Significant Difference (Tukey HSD) test was used to perform post-hoc pairwise comparisons with multiple testing corrections on probeset IDs found to be significantly differentially expressed across categories as determined by the Kruskal-Wallis analysis.
To summarize the performed statistical analyses, tables were generated for each dataset that included Probeset ID, Probeset, the Benjamini Hochberg corrected p-value, and the log2 fold change. The top 10 probeset IDs were listed for each dataset based on corrected p-value, and multiple datasets used to analyze the same biological question were combined into final summary tables.
For the in vitro study of cigarette smoke extract exposure, an a one-way ANOVA was performed with a Bonferroni correction for multiple comparisons with a significance determined at p < 0.05.
Results
ABC transporter transcript expression in human airway epithelial cells
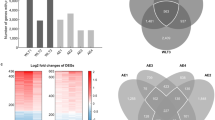
To begin our characterization of the 48 known ABC transporters in airway epithelial cells, we examined expression patterns of each member across the trachea, large airways (generation 2nd-3rd), and small airways (generation 10th-12th) (Fig. 1 – Supplement Table 2) using GSE11906. A global assessment of all ABC transporters across airway generations revealed diversity in their expression, with the highest detected expression levels for ABCA5, ABCA13, and ABCC5 (Fig. 1) and a trend for increased expression in the trachea relative to the small airways. Between the airway generations, differences were only observed between the small airways and the trachea (q < 0.05 – Supplement Table 2). The top three candidates ranked by fold-change in small airway relative to trachea were ABCC1, ABCC4, and ABCB3 (all with q < 0.05). Collectively the data suggest that ABC transporters are expressed in human airway epithelial cells with airway generation specific expression patterns.
ABC transporter transcripts are expressed in airway epithelial cells throughout airway tree generations. Gene expression levels for all 48 ABC transporter members were examined across the trachea, large airways (generation 2nd-3rd), and small airways (generation 10th-12th) using a single dataset (GSE11906, Affymetrix Human Genome U133 Plus 2 microarray platform) comprised of independent epithelial cell samples isolated from healthy, non-smoking individuals. A representative probeset for each ABC transporter was chosen and average signal intensities (with standard error) for each probeset were calculated and visualized as a bar plot using ggplot2 in R (v. 3.4.3). grey = small airways, blue = large airways, orange = trachea.
Impact of cigarette smoke exposure on ABC transporter expression
We next explored the impact of cigarette smoke exposure on ABC transporter expression profiles. For our analysis we interrogated three datasets of small airway (10th-12th generation) epithelial cells from healthy subjects and those with a history of smoking without a diagnosis of COPD (GSE11906, GSE11784, and GSE4498)16,17,18.
Cigarette smoke exposure was associated with elevated ABCB6 and ABCC3 expression levels, a feature conserved across all three independent datasets (Fig. 2 – Supplement Table 3). In 2 of 3 datasets, an elevation in ABCC1 was observed, with similar non-significant trends observed in the third dataset. In 1 of 3 datasets, lower ABCA13 expression was observed, with similar non-significant trends observed in the two other datasets.
Cigarette smoking is associated with differential gene expression patterns of select ABC transporters in small airway epithelial cells. Gene expression levels of selected ABC transporters (a, ABCA13; b, ABCB6; c, ABCC1; d, ABCC3) between healthy non-smokers (green) and smokers with no diagnosis of COPD (blue). Significant expression differences are indicated by asterisks (q < 0.05 according to Mann-Whitney U test with Benjamini Hochberg correction). All three datasets used for this analysis (GSE11906, GSE11784, and GSE4498) analyzed epithelial cells from small airways (10th-12th generation) and were generated from the Affymetrix Human Genome U133 Plus 2 microarray platform (using the Mas 5.0 Normalization method). Data distributions are visualized as boxplots (see Methods for additional details).
Impact of cigarette smoking cessation on ABC transporter expression
Cigarette smoking is a modifiable risk factor for the development of COPD with cessation advocated by the Global Initiative for Obstructive Lung Disease25. We therefore determined whether smoking cessation could normalize differences observed in ABC transporter expression for ABCA13, ABCB6, ABCC1, and ABCC3 by comparing former smokers, current smokers, and where possible, healthy never-smokers. For our analysis we examined two datasets generated from two distinct microarray platforms, GSE37147 and GSE994, which analyzed epithelial cells from medium (6th-8th generation) and large (2nd generation) airways, respectively.
Smoking cessation was associated with lower expression of ABCB6, ABCC1, and ABCC3 in both datasets (Fig. 3 – Supplement Table 4). A trend for elevated ABCA13 expression (q = 0.06) was observed in association with smoking cessation in the medium airways with no primer sets available in the large airway dataset. In GSE994, an additional group of never-smokers reveals that levels of ABCB6 and ABCC1 elevated with smoking do not normalize to never-smoker levels even with prolonged smoking cessation (average 10.7 years)15.
Cigarette smoking cessation is associated with normalization of ABC transporter gene expression patterns in airway epithelial cells. (a) Differential expression of ABCA13 between current smokers (green) and former smokers (blue) from GSE37147 (* q < 0.05, Mann-Whitney U pairwise statistical analysis with Benjamini Hochberg multiple testing correction). GSE37147 was selected as it was the only dataset including a probe matching ABCA13. (b–d) Differential expression of ABCB6, ABCC1, and ABCC3 between current smokers (green), former smokers (blue), and, where possible, never-smokers (orange) from GSE37147 and GSE994 (* q < 0.05, Kruskal-Wallis followed by the Tukey Honest Significance Difference (Tukey HSD) test). The datasets used in this analysis (GSE37147 and GSE994) were generated from two distinct microarray platforms (Affymetrix Human Gene 1 ST and Affymetrix Human Genome U133A, respectively), which analyzed epithelial cells from medium (6th-8th generation) and large (2nd generation) airways, respectively. GSE37147 used the logged RMA Normalization method and GSE994 used the Mas 5.0 Normalization method. Data distributions are visualized as boxplots (see Methods for additional details).
Association between COPD status and changes in ABC transporter expression
We next analyzed the expression profiles of ABC transporters in relation to confirmed COPD status in three datasets (GSE11906, GSE11784, and GSE37147). GSE11906 and GSE11784 collected epithelial cells from small airways (10th-12th generation) while GSE37147 collected from medium airways (6th-8th generation).
No ABC transporter showed differential expression across all three independent datasets (Fig. 4 – Supplement Table 5). Of candidates modified by cigarette smoking history, ABCC1 was ranked in the top 10 differentially expressed probesets in each dataset containing smokers with and without COPD, with a trend observed for increased expression with COPD status that was significant in the medium airways (GSE37147) (Fig. 4). ABCA13, ABCB6, and ABCC3 expression profiles did not show any association with COPD status.
ABC transporter expression patterns associated with smoking status mildly correlate with COPD diagnosis. Gene expression levels of selected ABC transporters (a, ABCA13; b, ABCB6; c, ABCC1; d, ABCC3) between smokers with COPD (blue) and smokers with no diagnosis of COPD (green). Significant ABC transporter expression differences are indicated by asterisks (q < 0.05 according to Mann-Whitney U test with Benjamini Hochberg correction). Three datasets (GSE11906, GSE11784, and GSE37147) were used for this assessment. GSE11906 and GSE11784 collected epithelial cells from small airways (10th-12th generation) while GSE37147 collected from medium airways (6th-8th generation), with the two different sample types also analyzed on different microarray platforms (Affymetrix Human Genome U133 Plus 2 and Affymetrix Human Gene 1 ST, respectively). GSEs 11906 and 11784 used the Mas 5.0 Normalization method, and GSE37147 used the logged RMA Normalization method. Data distributions are visualized as boxplots (see Methods for additional details).
ABC transporter expression patterns in airway epithelial cells from asthmatics
For our asthma-focused analysis we interrogated two pairs of datasets; GSE4302 and GSE67472 – which allowed for healthy control comparison to individuals with asthma and GSE63142 and GSE76227 – which allowed for associating expression profiles with asthma severity20,21,22,23. All studies analyzed epithelial cells from medium (2nd-5th generation) airways.
We observed that asthma status is associated with an increase in ABCC2 in both datasets (Fig. 5 – Supplement Table 6). ABCA13 and ABCC9 were decreased in one dataset (GSE67472) with a similar trend in the second dataset (q < 0.1 – GSE4302). ABCC1 expression was increased in one dataset (GSE4302) with no trend observed in the second dataset. ABCC4 expression levels showed trends towards reduced expression in samples from asthmatics in both datasets that were not significant.
A change in ABC transporter expression patterns in airway epithelial cells from asthmatics is distinct from smoking or COPD status. Gene expression levels of selected ABC transporters (a, ABCA13; b, ABCC1; c, ABCC2; d, ABCC4; e, ABCC9) between healthy controls (green) and asthmatics (blue). Significant ABC transporter expression differences are indicated by asterisks (q < 0.05 according to Mann-Whitney U test with Benjamini Hochberg correction). Both datasets (GSE4302 and GSE67472) analyzed epithelial cells from medium (3rd-5th generation) airways and were generated from the Affymetrix Human Genome U133 Plus 2 microarray platform (using the Mas 5.0 Normalization method). Data distributions are visualized as boxplots (see Methods for additional details).
In the datasets that stratified asthmatics based on disease severity (GSE63142 and GSE76227), trends for reduced ABCC4 and ABCA13 gene expression were associated with increased severity of disease (Fig. 6 – Supplement Table 7). In contrast, ABCC1, ABCC2, and ABCC9 failed to trend with disease severity (data not shown).
Select ABC transporter gene expression profiles associate with asthma severity. Gene expression levels of (a) ABCA13 and (b) ABCC4 between mild/moderate (green), moderate (blue), and severe (orange) asthmatics visualized as boxplots (see Methods for additional details). Significant ABC transporter expression differences are indicated by asterisks (q < 0.05 according to Mann-Whitney U test with Benjamini Hochberg correction). Both datasets used for this analysis (GSE63142 and GSE76227) analyzed epithelial cells from medium (3rd-5th generation) airways; however, they were generated using different microarray platforms (Agilent 014850 Whole Human Genome Microarray 4 × 44K G4112F and Affymetrix HT HG U133 plus PM, respectively). GSE63142 uses the Cyclic LOESS Normalization method and GSE76227 uses the RMA Normalization method.
In vitro validation of candidate ABC transporter gene expression changes
A priori we determined that we are unable to recapitulate a complete in vivo COPD and asthma phenotype in vitro, but are able to recapitulate the impact of cigarette smoke exposure24. We therefore set out to perform a cigarette smoke extract conditioned media experiment with the Calu-3 airway epithelial cell line grown under submerged monolayer conditions to validate an in vitro model system for interrogating candidate ABC transporters of interest. Cigarette smoke extract conditioned media exposure (10% and 20%) for 24hrs recapitulates the decrease in ABCA13 gene expression and increase in ABCC1 gene expression that is observed in human bronchial brushing samples (Fig. 7a,b) from individuals that have smoked cigarettes (Fig. 2a,c), with no changes in cell viability Fig. 7c).
In vitro cell culture model systems are capable of recapitulating in situ observations of ABC transporter expression patterns and changes with cigarette smoke exposure. Expression levels of the ABCA13 and ABCC1 genes in Calu-3 cells grown under submerged monolayer conditions were assessed after exposure of cells to 10% and 20% cigarette smoke extract (CSE) conditioned media for 24 hours. Expression is relative to GAPDH levels and also compared to a negative control (unexposed Calu-3 cells) (a) ABCC1 expression increases under these conditions, whereas (b) ABCA13 expression decreases as % CSE increased with no impact on cell viability (c). One-way ANOVA was performed with a Bonferroni correction for multiple comparisons with a significance determined at p < 0.05. n = 3 *p < 0.05 relative to control.
Discussion
The contribution of ABC transporters to respiratory mucosal immunology remains to be defined. To address this knowledge group, we performed a bioinformatic analysis of 9 distinct gene-expression datasets of primary human airway epithelial cells test our hypothesis that specific ABC transporter gene expression patterns would correlate with presence of a specific chronic respiratory disease and disease severity. The in situ human gene expression data demonstrate that ABC transporters are i) variably expressed in epithelial cells from different airway generations (top three expression levels - ABCA5, ABCA13, and ABCC5, ii) regulated by cigarette smoke exposure (ABCA13, ABCB6, ABCC1, and ABCC3), and iii) differentially expressed in individuals with COPD and asthma (ABCA13, ABCC1, ABCC2, ABCC9). Lastly, we demonstrate that an in vitro cell culture system of cigarette smoke exposure is amenable to investigate the consequences of differential gene expression patterns of candidate ABC transporters (ABCA13 and ABCC1). Our work sets a foundation for further mechanistic research into the basic biology of ABC transporters in the respiratory mucosa and suggests a potential contribution to chronic respiratory diseases.
Our analysis on ABC transporter expression profiles across airway generations was performed on samples isolated from healthy subjects at the level of the trachea, large airways (generation 2nd-3rd), and small airways (generation 10th-12th). Our data demonstrates that the expression levels of select ABC transporters are heterogeneous throughout the airway tree (e.g. ABCC1, ABCC4, & ABCB3) while others are homogenous (e.g. ABCA13, ABCC2, & ABCC3). The relative paucity of literature mechanistically describing the function of each ABC transporter in human airway epithelial cells precludes us from attributing any differential expression pattern to airway generation specific functional responses of the epithelium. Regardless, our data suggests that ABC transporter expression is differentially regulated along the airway tree, which may be important for chronic airway diseases that lead to pathology of distinct airway regions (e.g. COPD as a small airways disease26).
Environmental exposures including cigarette smoke, air pollution, allergens, viruses, and bacteria can induce immune mediator release in the airway epithelium1,2. ABC transporters may be responsible for immune mediator release, including uric acid, leukotrienes, prostaglandins, and glutathione conjugates9,10, that may be important for responding to environmental stimuli. To investigate possible ABC transporter-environment relationships, we explored the impact of cigarette smoke exposure and smoking cessation on in situ gene expression in epithelial cells. Our analyses of the impact of smoking used three datasets generated on the same microarray platform (GSE11906, GSE11784, and GSE4498)16,17,18, while our smoking cessation analysis used two additional datasets generated on two different microarray platforms (GSE37147 and GSE994)15,19. Conserved elevations in ABCB6, ABCC1, and ABCC3 gene expression in response to cigarette smoke exposure were observed, accompanied by trends for decreased gene expression with smoking cessation. ABCB6 is a broad-spectrum porphyrin transporter expressed in mitochondria and plasma membranes involved in heme biosynthesis and protective responses to reactive oxygen species27,28. ABCB6 over-expression increases catalase gene expression and stability29 and is able to inhibit arsenic cytotoxicity30, a carcinogenic component found in cigarette smoke31. Despite the potential protective consequences of elevated ABCB6 expression that we observe in cigarette smokers, it is important to note that negative consequences may also arise as elevated ABCB6 levels may lead to resistance to chemotherapeutic agents32. Therefore, the observed up-regulation in ABCB6 is likely an important initial protective response to cigarette smoke exposure that may have untoward consequences of reducing responsiveness to chemotherapeutic agents for management of lung cancers. ABCC1 and ABCC3 also provide protective effects by transporting glutathione-conjugated anions from the cytosol to the extracellular compartment to prevent cellular accumulation of toxic metabolites33,34. Similar to ABCB6, ABCC1, and ABCC3 are also capable of effluxing chemotherapeutics of broad function including anti-cancer functions. Collectively it is conceivable that ABCB6, ABCC1, and ABCC3 gene expression levels are regulated by a feedback mechanism linked to oxidative stress and toxin exposure induced by cigarette smoke exposure to help facilitate anti-oxidant activities within airway epithelial cells.
Importantly, we observe that as cigarette smokers progress to develop COPD, ABCC1 gene expression is elevated compared to individuals that do not have COPD. Linked to cigarette smoking, elevated ABCC1 gene expression has been observed in both non-small cell carcinoma and small-cell carcinoma lung cancers35. The contribution of ABCC1 biology in response to cigarette smoke exposure and to the associated development of COPD and lung carcinoma is intriguing. Our in vitro model of cigarette smoke extract conditioned media induction of ABCC1 gene expression may be valuable in further interrogating this biology and the functional consequences in the context of COPD and lung carcinomas.
In contrast to elevated gene expression levels in response to cigarette smoke exposure and COPD status, we observed a conserved decrease in the expression of ABCA13. We also observed a decrease in ABCA13 gene expression in asthmatics relative to healthy controls, suggesting this may be a non-specific response to an inflammatory lung environment. ABCA13 is an intriguing candidate as the expression levels are very high relative to other ABC family members, and there are no reports of endogenous or exogenous substrates, expression patterns in epithelium, or associations with respiratory mucosal immunology. Reports show associations between ABCA13 expression and cancers36,37,38, while ABCA13 variants are associated with mental health abnormalities39,40, although no mechanisms have been defined for either of these observations. Other ABCA family members are involved in lipid transport and dysregulation of their pathways can result in lung inflammation41. To gain insight into ABCA13 biology, we can examine other ABCA family members: Abca1-KO mice have impaired lipid transport resulting in reduced serum cholesterol and HDL, elevated intracellular lipid contents, and abnormal lung structure42. In contrast, mice over-expressing human ABCA1 gene showed reduced inflammation and pathology in a model of allergic lung inflammation43. In humans and mice, dysfunction of ABCA3 results in surfactant deficiencies and fatal respiratory failure13,44,45. Based on function of these two ABCA family members in the lung, we hypothesize that ABCA13 is important in lipid handling in airway epithelial cells, and when decreased in expression, this could result in inflammation, altered surfactant production, and impaired innate immune functions. The relatively high expression levels of ABCA13 gene throughout the airway generations and the known function of ABCA family members in lung biology warrants a further exploration of this candidate.
Our observation that cigarette smoke exposure, and to a small extent COPD status, was associated with changes in ABC transporter gene expression warranted further exploration to determine if these observations were non-specific responses to inflammatory airway environments. Although changes in ABCA13 gene expression associate with both cigarette smoking and asthma status, unique changes in ABC transporter expression profiles are observed in samples isolated from asthmatics. Elevated ABCC2 expression in asthmatics relative to healthy subjects was observed while reductions in ABCC9 were observed. ABCC2 is similar in function to ABCC1 with the shared ability to transport glutathione-conjugated xenobiotics and control intracellular oxidative stress46,47,48. Elevations in ABCC2 that are observed in airway epithelial cells in asthmatics may aid in control of oxidative environments in the asthmatic lung and epithelial cells49,50,51, but could also lead to extracellular transport of pharmacological agents used to control asthma due to the broad specificity of this transporter. Similar to ABCC1 in smokers, changes in ABCC2 in asthmatics may be both beneficial (management of oxidative stress) and detrimental (reduction in intracellular bioavailability of pharmacological agents). In contrast to elevations in ABCC2, we observed reductions in ABCC9 in airway epithelial cells from asthmatics. ABCC9 is also known as the sulfonylurea receptor 2 (SUR2) protein and functions as an ATP sensitive K + channel that helps coordinate calcium levels in skeletal and cardiac muscle52,53. Reduced ABCC9 levels could conceivably dysregulate K + and calcium concentrations within airway epithelial cells, which in turn could impact K + regulated mechanisms of epithelial cell migration, proliferation, and tissue repair54. Irrespective of the proposed functions of these ABC transporters that are differentially expressed in epithelial cells from asthmatics, we can conclude that the different patterns observed in cells from asthmatics, smokers, or individuals with COPD suggests that regulation and function of ABC transporters is specific to a given chronic inflammatory lung disease or environmental insult.
Our bioinformatic study has some limitations that need to be recognized due to the use of publically available datasets in the NCBI GEO. The deposited datasets were developed from different microarray platforms, probesets, and epithelial cells isolated from different airway generations. Where the information was available, we have attempted to clearly disclose this in our methods and correspondingly the results sections have axes of figures labeled based on the pre-processing analysis performed by the original contributors of the datasets (including different normalization methods). Irrespective of these limitations and our inability to control for differences in microarray platform and source of epithelial cells, we emphasize that we observed common trends across independent datasets, suggesting validity of our approach and the available datasets.
In closing, we have initiated a characterization of the 48 known ABC transporters in human airway epithelial cells in the context of chronic airway diseases. Using 9 distinct gene-expression datasets of primary human airway epithelial cells, we tested our hypothesis that specific ABC transporter gene expression patterns would correlate with presence of a specific chronic respiratory disease and disease severity. It is clear that ABC transporters are i) variably expressed in epithelial cells from different airway generations, ii) regulated by cigarette smoke exposure, and iii) differentially expressed in individuals with COPD and asthma, We further demonstrate that an in vitro cell culture system is amenable to investigate the consequences of differential expression patterns of candidate ABC transporters, creating a foundation for further mechanistic research into the basic biology of ABC transporters in lung health and disease.
Data Availability
All data will be made available upon request to the corresponding author.
References
Hirota, J. A. & Knight, D. A. Human airway epithelial cell innate immunity: relevance to asthma. Curr Opin Immunol 24, 740–746, https://doi.org/10.1016/j.coi.2012.08.012 (2013).
Parker, D. & Prince, A. Innate immunity in the respiratory epithelium. Am J Respir Cell Mol Biol 45, 189–201, https://doi.org/10.1165/rcmb.2011-0011RT (2011).
van der Deen, M. et al. ATP-binding cassette (ABC) transporters in normal and pathological lung. Respir Res 6, 59, https://doi.org/10.1186/1465-9921-6-59 (2005).
Conner, G. E., Ivonnet, P., Gelin, M., Whitney, P. & Salathe, M. HO Stimulates CFTR Through an Autocrine Prostaglandin Pathway Using MRP4. Am J Respir Cell Mol Biol. https://doi.org/10.1165/rcmb.2013-0156OC (2013).
Gold, M. J. et al. Mucosal production of uric acid by airway epithelial cells contributes to particulate matter-induced allergic sensitization. Mucosal Immunol 9, 809–820, https://doi.org/10.1038/mi.2015.104 (2016).
Huff, R. D. et al. Inhibition of ABCC4 potentiates combination beta agonist and glucocorticoid responses in human airway epithelial cells. J Allergy Clin Immunol. https://doi.org/10.1016/j.jaci.2017.10.011 (2017).
Sonett, J. et al A critical role for ABC transporters in persistent lung inflammation in the development of emphysema after smoke exposure. FASEB J, fj201701381, https://doi.org/10.1096/fj.201701381 (2018).
Jubinville, E. et al Interplay between cigarette smoking and pulmonary reverse lipid transport. Eur Respir J 50, https://doi.org/10.1183/13993003.00681-2017 (2017).
Fukuda, Y. & Schuetz, J. D. ABC transporters and their role in nucleoside and nucleotide drug resistance. Biochem Pharmacol 83, 1073–1083, https://doi.org/10.1016/j.bcp.2011.12.042 (2012).
Cheepala, S. et al. Cyclic nucleotide compartmentalization: contributions of phosphodiesterases and ATP-binding cassette transporters. Annu Rev Pharmacol Toxicol 53, 231–253, https://doi.org/10.1146/annurev-pharmtox-010611-134609 (2013).
Riordan, J. R. et al. Identification of the cystic fibrosis gene: cloning and characterization of complementary DNA. Science 245, 1066–1073 (1989).
Veit, G. et al. From CFTR biology toward combinatorial pharmacotherapy: expanded classification of cystic fibrosis mutations. Mol Biol Cell 27, 424–433, https://doi.org/10.1091/mbc.E14-04-0935 (2016).
Shulenin, S. et al. ABCA3 gene mutations in newborns with fatal surfactant deficiency. N Engl J Med 350, 1296–1303, https://doi.org/10.1056/NEJMoa032178 (2004).
Ahmadi, S. et al Phenotypic profiling of CFTR modulators in patient-derived respiratory epithelia Nature Genomic Medicine In Press (2017).
Spira, A. et al. Effects of cigarette smoke on the human airway epithelial cell transcriptome. Proc Natl Acad Sci USA 101, 10143–10148, https://doi.org/10.1073/pnas.0401422101 (2004).
Harvey, B. G. et al. Modification of gene expression of the small airway epithelium in response to cigarette smoking. J Mol Med (Berl) 85, 39–53, https://doi.org/10.1007/s00109-006-0103-z (2007).
Tilley, A. E. et al. Biologic phenotyping of the human small airway epithelial response to cigarette smoking. PLoS One 6, e22798, https://doi.org/10.1371/journal.pone.0022798 (2011).
Raman, T. et al. Quality control in microarray assessment of gene expression in human airway epithelium. BMC Genomics 10, 493, https://doi.org/10.1186/1471-2164-10-493 (2009).
Steiling, K. et al. A dynamic bronchial airway gene expression signature of chronic obstructive pulmonary disease and lung function impairment. Am J Respir Crit Care Med 187, 933–942, https://doi.org/10.1164/rccm.201208-1449OC (2013).
Woodruff, P. G. et al. T-helper type 2-driven inflammation defines major subphenotypes of asthma. Am J Respir Crit Care Med 180, 388–395, https://doi.org/10.1164/rccm.200903-0392OC (2009).
Modena, B. D. et al. Gene expression in relation to exhaled nitric oxide identifies novel asthma phenotypes with unique biomolecular pathways. Am J Respir Crit Care Med 190, 1363–1372, https://doi.org/10.1164/rccm.201406-1099OC (2014).
Christenson, S. A. et al. Asthma-COPD overlap. Clinical relevance of genomic signatures of type 2 inflammation in chronic obstructive pulmonary disease. Am J Respir Crit Care Med 191, 758–766, https://doi.org/10.1164/rccm.201408-1458OC (2015).
Kuo, C. S. et al. & dagger, U. B. P. T. d. A Transcriptome-driven Analysis of Epithelial Brushings and Bronchial Biopsies to Define Asthma Phenotypes in U-BIOPRED. Am J Respir Crit Care Med 195, 443–455, https://doi.org/10.1164/rccm.201512-2452OC (2017).
Huff, R. D. et al. Regulation of xanthine dehydrogensase gene expression and uric acid production in human airway epithelial cells. PLoS One 12, e0184260, https://doi.org/10.1371/journal.pone.0184260 (2017).
Vestbo, J. et al. Global strategy for the diagnosis, management, and prevention of chronic obstructive pulmonary disease: GOLD executive summary. Am J Respir Crit Care Med 187, 347–365, https://doi.org/10.1164/rccm.201204-0596PP (2013).
McDonough, J. E. et al. Small-airway obstruction and emphysema in chronic obstructive pulmonary disease. N Engl J Med 365, 1567–1575, https://doi.org/10.1056/NEJMoa1106955 (2011).
Krishnamurthy, P. C. et al. Identification of a mammalian mitochondrial porphyrin transporter. Nature 443, 586–589, https://doi.org/10.1038/nature05125 (2006).
Paterson, J. K. et al. Human ABCB6 localizes to both the outer mitochondrial membrane and the plasma membrane. Biochemistry 46, 9443–9452, https://doi.org/10.1021/bi700015m (2007).
Lynch, J., Fukuda, Y., Krishnamurthy, P., Du, G. & Schuetz, J. D. Cell survival under stress is enhanced by a mitochondrial ATP-binding cassette transporter that regulates hemoproteins. Cancer Res 69, 5560–5567, https://doi.org/10.1158/0008-5472.CAN-09-0078 (2009).
Chavan, H., Oruganti, M. & Krishnamurthy, P. The ATP-binding cassette transporter ABCB6 is induced by arsenic and protects against arsenic cytotoxicity. Toxicol Sci 120, 519–528, https://doi.org/10.1093/toxsci/kfr008 (2011).
Pappas, R. S., Fresquez, M. R., Martone, N. & Watson, C. H. Toxic metal concentrations in mainstream smoke from cigarettes available in the USA. J Anal Toxicol 38, 204–211, https://doi.org/10.1093/jat/bku013 (2014).
Boswell-Casteel, R. C., Fukuda, Y. & Schuetz, J. D. ABCB6, an ABC Transporter Impacting Drug Response and Disease. AAPS J 20, 8, https://doi.org/10.1208/s12248-017-0165-6 (2017).
Leslie, E. M., Deeley, R. G. & Cole, S. P. Multidrug resistance proteins: role of P-glycoprotein, MRP1, MRP2, and BCRP (ABCG2) in tissue defense. Toxicol Appl Pharmacol 204, 216–237, https://doi.org/10.1016/j.taap.2004.10.012 (2005).
Zeng, H., Liu, G., Rea, P. A. & Kruh, G. D. Transport of amphipathic anions by human multidrug resistance protein 3. Cancer Res 60, 4779–4784 (2000).
Wright, S. R. et al. Immunohistochemical detection of multidrug resistance protein in human lung cancer and normal lung. Clin Cancer Res 4, 2279–2289 (1998).
Araujo, T. M. et al. Recurrent amplification of RTEL1 and ABCA13 and its synergistic effect associated with clinicopathological data of gastric adenocarcinoma. Mol Cytogenet 9, 52, https://doi.org/10.1186/s13039-016-0260-x (2016).
Gellert, P. et al. & Trialists. Impact of mutational profiles on response of primary oestrogen receptor-positive breast cancers to oestrogen deprivation. Nat Commun 7, 13294, https://doi.org/10.1038/ncomms13294 (2016).
Hlavata, I. et al. The role of ABC transporters in progression and clinical outcome of colorectal cancer. Mutagenesis 27, 187–196, https://doi.org/10.1093/mutage/ger075 (2012).
Dwyer, S. et al. Investigation of rare non-synonymous variants at ABCA13 in schizophrenia and bipolar disorder. Mol Psychiatry 16, 790–791, https://doi.org/10.1038/mp.2011.2 (2011).
Knight, H. M. et al. A cytogenetic abnormality and rare coding variants identify ABCA13 as a candidate gene in schizophrenia, bipolar disorder, and depression. Am J Hum Genet 85, 833–846, https://doi.org/10.1016/j.ajhg.2009.11.003 (2009).
Chai, A. B., Ammit, A. J. & Gelissen, I. C. Examining the role of ABC lipid transporters in pulmonary lipid homeostasis and inflammation. Respir Res 18, 41, https://doi.org/10.1186/s12931-017-0526-9 (2017).
Bates, S. R., Tao, J. Q., Collins, H. L., Francone, O. L. & Rothblat, G. H. Pulmonary abnormalities due to ABCA1 deficiency in mice. Am J Physiol Lung Cell Mol Physiol 289, L980–989, https://doi.org/10.1152/ajplung.00234.2005 (2005).
Dai, C. et al. ATP-binding cassette transporter 1 attenuates ovalbumin-induced neutrophilic airway inflammation. Am J Respir Cell Mol Biol 51, 626–636, https://doi.org/10.1165/rcmb.2013-0264OC (2014).
Besnard, V. et al. Conditional deletion of Abca3 in alveolar type II cells alters surfactant homeostasis in newborn and adult mice. Am J Physiol Lung Cell Mol Physiol 298, L646–659, https://doi.org/10.1152/ajplung.00409.2009 (2010).
Rindler, T. N., et al Alveolar injury and regeneration following deletion of ABCA3. JCI Insight 2, https://doi.org/10.1172/jci.insight.97381 (2017).
Keppler, D., Leier, I. & Jedlitschky, G. Transport of glutathione conjugates and glucuronides by the multidrug resistance proteins MRP1 and MRP2. Biol Chem 378, 787–791 (1997).
Konig, J., Nies, A. T., Cui, Y., Leier, I. & Keppler, D. Conjugate export pumps of the multidrug resistance protein (MRP) family: localization, substrate specificity, and MRP2-mediated drug resistance. Biochim Biophys Acta 1461, 377–394 (1999).
Terlouw, S. A., Masereeuw, R., van den Broek, P. H., Notenboom, S. & Russel, F. G. Role of multidrug resistance protein 2 (MRP2) in glutathione-bimane efflux from Caco-2 and rat renal proximal tubule cells. Br J Pharmacol 134, 931–938, https://doi.org/10.1038/sj.bjp.0704284 (2001).
Janssen-Heininger, Y. M. et al. Nuclear factor kappaB, airway epithelium, and asthma: avenues for redox control. Proc Am Thorac Soc 6, 249–255, https://doi.org/10.1513/pats.200806-054RM (2009).
Riedl, M. A. & Nel, A. E. Importance of oxidative stress in the pathogenesis and treatment of asthma. Curr Opin Allergy Clin Immunol 8, 49–56, https://doi.org/10.1097/ACI.0b013e3282f3d913 (2008).
Chan, T. K., Tan, W. S. D., Peh, H. Y. & Wong, W. S. F. Aeroallergens Induce Reactive Oxygen Species Production and DNA Damage and Dampen Antioxidant Responses in Bronchial Epithelial Cells. J Immunol 199, 39–47, https://doi.org/10.4049/jimmunol.1600657 (2017).
Kane, G. C., Liu, X. K., Yamada, S., Olson, T. M. & Terzic, A. Cardiac KATP channels in health and disease. J Mol Cell Cardiol 38, 937–943, https://doi.org/10.1016/j.yjmcc.2005.02.026 (2005).
Flagg, T. P., Enkvetchakul, D., Koster, J. C. & Nichols, C. G. Muscle KATP channels: recent insights to energy sensing and myoprotection. Physiol Rev 90, 799–829, https://doi.org/10.1152/physrev.00027.2009 (2010).
Girault, A. & Brochiero, E. Evidence of K + channel function in epithelial cell migration, proliferation, and repair. Am J Physiol Cell Physiol 306, C307–319, https://doi.org/10.1152/ajpcell.00226.2013 (2014).
Acknowledgements
We would like to thank the individuals and research groups that have deposited their datasets to the NCBI GEO. Specific mentions of gratitude for Drs. Ian Adcock, Scott Kuo, Sally Wenzel, Prescott Woodruff, Srilaxmi Nerella for their time in addressing specific questions regarding datasets deposited in NCBI GEO. Lastly, we would like to thank Dr. Fiona Whelan for helping bring together the authors of the present manuscript for this collaboration. This work was supported by the Canadian Institutes of Health Research.
Author information
Authors and Affiliations
Contributions
J.A.A. Responsible for drafting the manuscript, collecting the datasets from GEO, quality control on the datasets, performing the analysis, figure generation, and editing the manuscript. A.T. Responsible for collecting the datasets from GEO, quality control on the datasets, performing the analysis, figure generation, and editing the manuscript. B.L. Responsible for quality control on the datasets, supervising the analysis, figure generation, and editing the manuscript. R.D.H. Responsible for the in vitro experiments, in vitro figure generation, and editing the manuscript. J.P.N. Responsible for manuscript conception, literature review, drafting the manuscript, and editing the manuscript. Y.K. Responsible for manuscript conception, literature review, drafting the manuscript, and editing the manuscript. A.D.G. Responsible for supervision and review of the bioinformatic data analysis and editing the manuscript. M.R.S. Responsible for conceptual design of manuscript, identification of appropriate datasets, and editing the manuscript. A.C.D. Responsible for oversight of the entire study (data collection, analysis, drafting, finalization) and supervision of the trainees, and submission of the manuscript. J.A.H. Corresponding author, responsible for oversight of the entire study (data collection, analysis, drafting, finalization) and supervision of the trainees, and submission of the manuscript.
Corresponding author
Ethics declarations
Competing Interests
The authors declare no competing interests.
Additional information
Publisher’s note: Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made. The images or other third party material in this article are included in the article’s Creative Commons license, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons license and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this license, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Aguiar, J.A., Tamminga, A., Lobb, B. et al. The impact of cigarette smoke exposure, COPD, or asthma status on ABC transporter gene expression in human airway epithelial cells. Sci Rep 9, 153 (2019). https://doi.org/10.1038/s41598-018-36248-9
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41598-018-36248-9
This article is cited by
-
GLUT3-mediated cigarette smoke-induced epithelial-mesenchymal transition in chronic obstructive pulmonary disease through the NF-kB/ZEB1 pathway
Respiratory Research (2024)
-
TNF-α and Poly(I:C) induction of A20 and activation of NF-κB signaling are independent of ABCF1 in human airway epithelial cells
Scientific Reports (2023)
-
Transcriptomic Response of Primary Human Bronchial Cells to Repeated Exposures of Cigarette and ENDS Preparations
Cell Biochemistry and Biophysics (2022)
-
Bidirectional Associations among Nicotine and Tobacco Smoke, NeuroHIV, and Antiretroviral Therapy
Journal of Neuroimmune Pharmacology (2020)
-
Direct Observation of Deformation in Microgel Filtration
Scientific Reports (2019)
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.