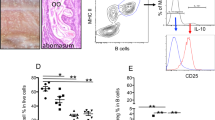
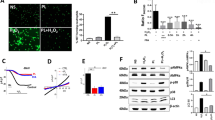
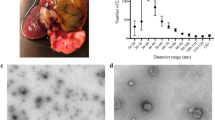
Abstract
Ostertagia ostertagi (OO) is a widespread parasite that causes chronic infection in cattle and leads to annual losses of billions of dollars in the cattle industry. It remains unclear why cattle are unable to mount an effective immune response despite a large influx of immune cells to the infected abomasal mucosa and draining lymph nodes. Neutrophils, the immune system’s first responders, have the capacity to release neutrophil extracellular traps (NETs) to contain various pathogens, including some parasites. In the present study, the mechanisms by which O. ostertagi influences bovine NET formation were investigated. O. ostertagi larval soluble extract (OO extract) was able to induce typical NETs by purified neutrophils in vitro, confirmed by co-localization of extracellular DNA with typical NET-associated proteins histone and neutrophil elastase (NE). Consistent with existing literature, inhibition assays demonstrated that these OO extract-induced NETs were dependent upon the enzymes NADPH oxidase and myeloperoxidase (MPO). Live OO stage 4 larvae (L4) stimulated neutrophils to form NETs similar to those induced by OO extract. Bovine neutrophils also released NETs in response to Caenorhabditis elegans, a free-living soil nematode, suggesting that bovine NET production may be a conserved mechanism against a broad range of nematodes. This is the first report demonstrating O. ostertagi-induced NET formation by bovine neutrophils, a potentially underappreciated mechanism in the early immune response against nematode infections.
Similar content being viewed by others
Introduction
Ostertagia ostertagi, a gastrointestinal (GI) nematode parasite of cattle and the causative agent of ostertagiasis, is considered one of the most economically most significant diseases in the cattle industry in temperate regions1. Ingested O. ostertagi third-stage larvae (L3) invade and take up residence in the gastric glands of the abomasum, causing cellular hyperplasia and leading to significant pathology2,3. Infection is attributed to an impaired protective immunity during infection4,5. The pasture is an intrinsic component of the life cycles of many livestock GI nematodes, including O. ostertagi, and serves as a natural reservoir for the infective L3 larvae; as such, grass-fed animals are at high risk of exposure to this parasite. In particular, infections can run unchecked in organic farming systems where anthelminthic drug usage is disallowed6. Moreover, while anthelmintics have been efficacious in the past, evidence of rapidly emerging anthelminthic drug resistance is mounting7,8. Thus, there is an urgent need for developing alternative nematode control strategies such as vaccination which could be used in combination with the anthelmintic treatment. However, the bovine immunity against ostertagiosis is poorly characterized. The overall goal of the present study was to understand the basic mechanisms of host-parasite interactions, in particular, neutrophil DNA release and neutrophil extracellular trap (NET) formation in response to Ostertagia infection in cattle.
O. ostertagi infection is known to elicit a mixed T helper (Th) cytokine response, distinct from the typical Th2 dominant response seen in model helminth infections9. In addition, the parasite has demonstrated a capacity to suppress immune responses such as lymphocyte proliferation and function10,11. Overall immune responses to O. ostertagi are poorly understood, and the early innate immune response to this parasite remains uncharacterized. As one of the first responders to infection and a source of local inflammation, neutrophils are recruited in significant numbers and may serve as the first line of defense against helminths12. While traditionally viewed as relatively simple and short-lived effector cells, recent findings on novel neutrophil functions have resulted in a shifting paradigm wherein neutrophils are implicated as an essential player in modulation of multiple early immune responses13. Importantly, the interactions between neutrophils and helminths such as O. ostertagi, which may represent a critical aspect of host-parasite interplay, have not been thoroughly investigated.
Neutrophils have several known effector functions against invading pathogens, including phagocytosis, release of antimicrobial molecules, production of reactive oxygen species (ROS), and release of neutrophil extracellular traps (NETs)12. NETs are large extracellular structures comprising a mesh of chromatin fibers containing an array of granule proteins such as neutrophil elastase (NE) and myeloperoxidase (MPO)14,15, which are capable of trapping and in some instances killing microbes. NETs have been characterized in several mammals including humans14, mice16, goats17, sheep18, and cattle19,20,21,22,23,24,25,26,27,28. While many studies have investigated the role of NETs on fungal29, bacterial30, viral31, and protozoan32 infections, relatively few have delved into the role of NETs in helminth infections. Neutrophils have been shown to release NETs in response to parasites33 such as Neospora caninum23, Eimeria bovis26 and Haemonchus contortus34, with this NET release shown to be MPO-, NE-, and ROS-dependent23,26,34. Recently, ROS-independent pathway has been reported35,36. These NETs have demonstrated a potential to entrap infectious nematodes such as H. contortus, suggesting NETs may be an important defense mechanism in mitigating other nematode parasite infections in general34. In addition to their direct interactions with invading pathogens, NETs can exert a direct enhancement37 or dampening38 of accompanying inflammatory responses depending upon the immunological context. The capacity for O. ostertagi to induce NET release, however, is unknown, and the role of these NETs, if released, may play in subsequent inflammation remains to be investigated.
The aim of the present study was to investigate O. ostertagi’s ability to induce NETs of bovine neutrophils and delineate the mechanisms that mediate this response, furthering our understanding of O. ostertagi pathogenesis and host responses and potentially revealing novel immunological treatment targets. The results of the present study suggest that O. ostertagi is capable of inducing NET release, without production of ROS. We also provide some evidence that this NET response may not be limited to specific nematode parasites such as O. ostertagi and may instead be a conserved response to any nematode encounter.
Results
OO extract induces NET release
Studies on other ruminant parasites have demonstrated their ability to induce NETs in bovine neutrophils, thus we hypothesized that O. ostertagi could induce NET formation as well. OO extract was able to induce NETs with typical structures (Fig. 1). Sytox Green staining revealed that stimulation of bovine neutrophils with OO extract led to the release of a dense network of DNA fibers spreading outwards from the cell (Fig. 1A-b,B-b). These DNA structures co-localized with histone (Fig. 1A-h) and NE (Fig. 1B-h), two proteins widely used as markers of NETs, confirming the existence thereof. Unstimulated neutrophils showed normal multilobed nuclei and lacked extracellular DNA structures (Fig. 1A-c,B-c). Stimulation with the well-established NET inducer PMA led to the formation of similar large extracellular DNA structures (Fig. 1A-a,B-a) which also co-localized with histone (Fig. 1A-g) and NE (Fig. 1B-g), consistent with recent reports.
Co-localization of DNA with histone (H3) (A) and neutrophil elastase (NE) (B), in PMA stimulated (a,d,g), Ostertagia ostertagi (OO) extract stimulated (b,e,h) and unstimulated (c,f,i) bovine neutrophils and associated neutrophil extracellular trap structures. (a–c) DNA stained with Sytox Green (green). (d–f) Histone (H3) staining in (A), and NE staining in (B) within NET structures (red). (g–i) Overlay of NET-DNA with histone (A) or NE (B). The neutrophils were incubated with each stimulus for 3 hours before staining.
To further characterize the role of OO extract in NET induction, time- and dose-dependent responses were examined in vitro. The enhancement of extracellular DNA release at similar levels was detectable 30 min following incubation with PMA/LPS and OO extract (Fig. 2A), which was significantly higher in cells treated with PMA/LPS and OO extract than unstimulated cells (p < 0.01). The NET release was significantly greater up to 90 min post treatment in cells treated with PMA when compared to those induced by LPS or OO extract. In general, PMA appeared to induce higher average NETs than those stimulated by other treatments (Fig. 2A), which may reflect the ability of PMA to directly activate protein kinase C (PKC), whereas LPS and possibly OO extract may have to work through multi-stepped signal transductions39. NET release in response to OO extract illustrated a clear time-dependent pattern similar to that of LPS (Fig. 2A). With maximal NET release at 180 min for all treatments, all subsequent experiments were conducted for this amount of time. To further define the dose response of neutrophils to OO extract, purified neutrophils were incubated with different concentrations of OO extract for 3 h and displayed a dose-dependent NET release, with maximal production at 3 µg/mL of OO extract (Fig. 2B). All subsequent experiments were conducted using OO extract at this concentration (3 µg/mL). Treatment with DNase I lowered the detection to the level of controls (Fig. 2B), suggesting that the increase in detected DNA was mostly extracellular. The results were consistent with the detection of extracellular DNA in NETs induced by PMA, LPS, and OO in Fig. 1.
DNA release following Ostertagia ostertagi (OO) extract treatment of bovine neutrophils (A). Kinetics of PMA, LPS and OO extract-induced DNA release over a period of 3 hours. (B) Dose-dependent effect of OO extract on DNA release by neutrophils incubated for 3 hours. Experiments were performed using cells from five cattle. Data were expressed as mean +/− SEM. All data were analyzed by one-way ANOVA with Newman-Keuls Multiple Comparison Test. Data were representative of at least three experiments with similar results.
OO extract-induced NET release is MPO-, NE-, and NADPH oxidase-dependent
To further corroborate the characteristics of OO extract-induced NET release, inhibition experiments of these classical NET-associated molecules were performed using specific inhibitors for NE (CMK), MPO (ABAH), and NADPH oxidase (DPI). Neutrophils pre-incubated with each inhibitor demonstrated significant reductions in NET release following OO extract stimulation (p ≤ 0.01, Fig. 3A), confirming a definitive role for each of these enzymes in OO extract-induced NET release. As reported in other bovine parasite models of NET release, the ROS pathway and NADPH oxidase, in particular, appear to be an integral part of NET formation, although the role that specific ROS products have in mediating this response remains unclear. The OO extract contained whole parasite content, so may include some bacteria from their gut microbiota, which consist of many immune stimulating components, such as LPS from gram-negative bacterial walls, which binds to TLR4. To test this possibility, neutrophils were pretreated with TLR4 inhibitor before stimulated with OO extract. Inhibition of TLR4, with CLI-095, however, did not affect the NET release induced by OO extract (Fig. 3B), indicating OO extract-stimulated NET release is not dependent on TLR4. Polymixin B (PMB) has been reported to be effective in blocking LPS stimulation in human cells40,41,42. However, PMB seemed to enhance OO-induced NET release (although not significant), possibly due to direct induction of NET release by PMB itself (Supplementary Fig. 1); this has also been observed on human neutrophils43. PMB can accumulate in mitochondria leading to apoptosis44,45. Protein kinase C (PKC) is involved in PMA-induced NET formation46,47; however, PKC inhibition caused no significant changes in OO-stimulated NET formation (Supplementary Fig. 1), suggesting that NET release induced by OO may not induce signaling through PKC46,47.
Blockage of Ostertagia ostertagi extract (OO)-triggered NETosis using inhibitors. (A) Inhibition of NADPH oxidase with DPI, NE with CMK, and MPO with ABAH, respectively. Data were expressed as mean +/− SEM from five cattle. (B) Inhibition of TLR4 with its inhibitor CLI-095 (TLR4i). Data were expressed as mean +/− SEM from triplicate using cells from one cattle. All data were analyzed by one-way ANOVA with Newman-Keuls Multiple Comparison Test. Data were representative of 3-4 experiments with similar results.
DNA in serum does not correlate with infection status
NETs are formed extracellularly and thereby subjected to controls by powerful homeostatic machinery in the host, such as degradation by DNase I. Released NETs may be exposed to enzymatic digestion or enter general circulation where they can be detected. To determine if the levels of cell-free DNA in blood were associated with OO infection, which could be related to entry of OO-induced NETs into circulation, we evaluated the cell-free DNA concentration in the sera of uninfected controls and cattle infected with O. ostertagi for 15 or 29 days. Day 0 samples were collected immediately prior to infection. Serum DNA concentration did not seem to correlate to infection status and did not significantly differ between control and infected animals at days 15 and 29 post-parasite challenge (Fig. 4A). In addition, neutrophils from OO-infected cattle were able to form NET in response to stimuli (data not shown). Furthermore, the cell-free DNA concentration in sera was lower by approximately 2 log than those detected in the supernatant from stimulated neutrophils (Fig. 2). Indeed, the serum DNA was extracellular and sensitive to DNase I treatment, similar to those present in supernatants (Fig. 2B). Therefore, cell-free DNA levels in serum do not appear to be affected by O. ostertagi infection, suggesting that soluble DNA of NETs may not exit the infection sites, or be released but rapidly diluted or cleared48.
Bovine neutrophils do not produce detectable ROS following OO extract exposure
The NADPH oxidase complex mediates neutrophil production of ROS. Inhibition of NET release following incubation with the NADPH oxidase inhibitor DPI confirmed the importance of this enzyme in OO extract-induced NET formation. We speculated that ROS would be easily detected in the supernatant of neutrophils following stimulation with PMA, LPS and OO extract, based on Figs 2, 3. Supporting the dependence of ROS on NADPH oxidase complex, neutrophils treated with the inhibitor DPI showed significant reductions in ROS production following PMA stimulation (p ≤ 0.01, Fig. 5A,B). Surprisingly, OO extract did not induce significant production of ROS by neutrophils at any point over the 2 h stimulation period, compared to the strong ROS response seen in PMA-stimulated neutrophils (Fig. 5A). Similarly, when measured as total ROS released over time (the area under each curve), ROS was undetectable in the supernatant of OO extract-treated neutrophils (p ≥ 0.05, Fig. 5B); additionally, the ROS scavenger Vitamin C49 did not affect OO-induced NET release (Supplementary Fig. 1), suggesting that ROS may not be involved in the OO-induced NET formation. Taken together, these results indicate that ROS may be dispensable in OO extract-induced NET formation by neutrophils, and suggest that the lack of ROS production may partially contribute to the failure of parasite control, which warrants further investigation.
Reactive oxygen species (ROS) production by neutrophils measured by luminol-enhanced chemiluminescence assay. (A) Kinetics of ROS release by neutrophils under treatments over a period of 2 hours. (B) Total ROS production measured by area under each curve for the whole period of 2 hours. Experiments were performed in triplicate using cells from three cattle. Data are expressed as mean +/− SEM of triplicates. Data were analyzed by One-way ANOVA with Newman-Keuls Multiple Comparison Test. Data were representative of two experiments with similar results.
Given the lack of ROS during OO extract-induced NET formation, it is important to know if bovine neutrophils were able to release NETs in response to ROS products. To test this possibility, hydrogen peroxide (H2O2) was used as an exogenous form of ROS in a range of concentration used in previous reports. Neutrophils exposed to varying concentrations of H2O2 displayed a significant, dose-dependent NET release (p ≤ 0.01, Fig. 6), equivalent to that of PMA-treated neutrophils, which was not affected by addition of DPI or PMA (data not shown). Therefore, despite the lack of detectable ROS production by neutrophils stimulated by OO extract and LPS, ROS products (H2O2) were able to directly stimulate NET formation by neutrophils, suggesting high responsiveness of bovine neutrophils to inflammatory mediators, such as ROS, that could lead to NET formation.
Hydrogen peroxide (H2O2) induces DNA release by bovine neutrophils dose-dependently. Experiments were performed in triplicate using cells from three cattle. Data were expressed as mean +/− SEM. Data were analyzed by one-way ANOVA with Newman-Keuls Multiple Comparison Test. Asterisks represented significance compared with negative control. Data were representative of two experiments with similar results.
OO extract-induced NET formation is not bovine-specific
O. ostertagi is a nematode parasite that completes the parasitic developmental stages most commonly in cattle, and to a less extent in smaller ruminants such as sheep and goats, and does not establish infection or cause disease in rodents. However, OO extract was reported to influence mouse immune cell activity. To assess if O. ostertagi elicited NET formation in neutrophils from mice, bone marrow neutrophils from C57BL/6 mice were stimulated with OO extract and their ability to release NETs was examined. Interestingly, there was a significant increase in NET release by OO extract-treated mouse neutrophils (p ≤ 0.001, Fig. 7A), which was inhibited by the NADPH oxidase inhibitor DPI (p ≤ 0.001). However, this inhibition was not complete, unlike in bovine neutrophils (Fig. 3). In addition, C. elegans, a lab adaptive strain of a soil nematode, was not able to induce murine neutrophils to form NETs (Fig. 7A). Consistent with the bovine neutrophil results, neutrophils from mice also did not produce ROS following OO extract stimulation (Fig. 7B), further suggesting that O. ostertagi mediates NET release independent of ROS production in both bovine and mouse neutrophils. Therefore, these data indicate that NET release by neutrophils is a conserved defense response across mammalian species, possibly mediated by broad host-pathogen pattern recognition mechanisms50, or other relatively conserved components such as lectin.
The induction of DNA release by neutrophils is a conserved function of the nematodes. Bone marrow-derived mouse neutrophils stimulated with O. ostertagi extract (OO) were assayed for DNA release 3 hours post-treatment (A) or ROS production over a period of 2 hours using luminol-enhanced chemiluminescence assay. (C,D) DNA release by bovine neutrophils from two cattle (C) or five cattle (D) following stimulation with live L4 Ostertagia larvae (C), or live C. elegans (D). Data were expressed as mean +/− SEM. The data in (A,B,D) represent two independent experiments in triplicates. C.el: live C. elegans. HK: heat-killed. Data were analyzed by One-way ANOVA with Newman-Keuls Multiple Comparison Test.
Bovine neutrophils release NETs in response to live free-living and parasitic nematodes
To reconcile whether whole parasites could induce NET formation, and a possible conserved mechanism across nematodes, live L4 stage O. ostertagi and C. elegans of mixed stages were tested for NETs induction in bovine neutrophils in vitro. Despite some variation among individuals, neutrophils co-cultured with either 20 or 40 per well live L4 Ostertagia larvae released significantly higher levels of NETs compared to unstimulated controls in both cattle (p < 0.05, Fig. 7C). In addition, the level of NETs induced by live L4 Ostertagia larvae was similar to the those of PMA stimulation in Cattle#2 but not Cattle#1 (Fig. 7C). C. elegans, a free-living nematode distantly related to most livestock GI nematodes, was chosen to compare against the parasite O. ostertagi. Unexpectedly, bovine neutrophils exposed to live worms of C. elegans showed significant induction of NET release (p ≤ 0.01, Fig. 7D), albeit not as large as those in PMA-stimulated neutrophils. C. elegans-induced NET release was independent of viability of the worms, as heat-killed worms (60 °C, 60 min) induced similar NET release (Fig. 7D). Inhibition experiments confirmed that these NETs by bovine neutrophils in response to C. elegans were also dependent upon NE, MPO, and NADPH oxidase (p ≤ 0.01, Fig. 7D). As such, bovine neutrophils appear to form NETs in response to different nematodes, and O. ostertagi may induce NETs in multiple host species, suggesting NET formation is a conserved defensive mechanism against a broad spectrum of pathogens including nematodes.
Discussion
Parasite-induced NET formation has been extensively studied in humans and mice. However, few of the studies have focused on the effects of nematodes51,52. Bovine neutrophils can release NETs, upon stimulation from nematode or non-nematode parasites18,22,23,24,25,27,32. In this report, we provide the first evidence of a NET response elicited by O. ostertagi, one of the most detrimental GI nematode parasites to the cattle industry53,54. OO extract can induce bovine neutrophils to form NETs, which are dependent on MPO, NE, and NADPH oxidase, proteins previously reported to be involved in parasite-dependent NET formation in cattle19,22,23,34. In addition, live OO L4 larvae induced significant NET release. Unexpectedly, C. elegans, a lab adaptive strain of soil nematode, was also able to cause NET formation in bovine neutrophils. Moreover, neutrophils from cattle and mice form NETs in response to OO extract, suggesting possible common mechanisms in NET formation shared by mammalian species in responding to nematodes.
In infected abomasal mucosa, the parasite OO concentration should be relatively low, and there is a possibility of direct interaction of parasites with immune cells, especially at the start of acute OO infection. To simulate some of these in vivo situations, we first examined whether bovine neutrophils would respond to low concentrations of adult stage OO extract. The capacity of bovine neutrophils to release significant levels of NETs in response to low concentrations of OO extract suggests that this response may be viable in vivo, where the actual abundance of parasite antigen can be quite low. To assay whether the intact parasite could induce NETs, live L4 stage O. ostertagi were co-cultured with bovine neutrophils, resulting in a NET response similar to OO extract alone. This suggests that O. ostertagi, in either soluble extract or live intact organism, can induce NETs. Despite the fact that the functional role of neutrophils in nematode infection has just begun to be unfolded55, there are several recent reports on rapid recruitment of neutrophils to the site of infection by Strongyloides stercoralis56 or Heligmosomoides polygyrus57. Such a recruitment may be resulted from tissue injury caused by migrating larvae and parasite-derived chemotactic factors55,58. The in vivo effect of this parasite on NET release should be confirmed in future studies.
To explore the possibility that the bovine NET response might be deployed against other nematodes and not specific to O. osteragi, the non-parasitic nematode C. elegans was added to our experiments. Interestingly, and despite its lack of pathogenicity, C. elegans also induces bovine neutrophils to form NETs following stimulation. The increasing reports of NETs from various species in response to different microbes reinforces the idea of NETs being an ancient and conserved aspect of the innate immune system shared among vertebrates and plants59,60. Still, innate immunity differs among species. In addition, OO soluble extract contains specific immunoregulators, such as lectin61. Interestingly, some members of the lectin family, such as C-type lectin receptor, Mincle, do in fact induce NETs in mouse neutrophils62. In addition, P-selectin, another member of the lectin family, is directly involved in NET formation in mice63. Therefore, NET release by murine neutrophils in response to OO soluble extract could be induced or enhanced by the presence of additional immune-triggering components, such as lectin, which is conserved across many species64.
Given the heterogeneity of the soluble extract, multiple mediators present in the extract could be independently or synergistically initiating the NET response utilizing different pathways or receptors, such the various pattern recognition receptors present on the surface or in the endosomes of neutrophils (e.g. TLRs)65. In the case of the L4 larvae and C. elegans, in addition to the possible response to size66, there may also be molecular structures present on the surfaces of these worms that neutrophils are recognizing, and the possibility of such surface molecules being present in the soluble extract cannot be discounted. For example, various Candida albicans cell surface components are capable of inducing NETs via various receptors including TLRs, members of C-lectin family (Dectin-1), and complement receptors (CD11b/CD18, Mac-1)67. It is possible that multiple signals are simultaneously mediating the O.ostertagi response, potentially indicating redundant mechanisms for NET formation, as redundancy is common in immunological functions68,69.
Previous reports on parasite-mediated NET release have shown the importance of NE, MPO, and NADPH oxidase. Using chemical inhibitors, we have shown that these proteins are also crucial for the O. ostertagi-mediated NET response. Inhibition of NADPH oxidase with DPI completely abrogated the formation of NETs following O. ostertagi stimulation, confirming the importance of this pathway even though the main function of NADPH oxidase is the production of ROS70 (Fig. 8). However, there was no detectable release of ROS throughout the assay following O. ostertagi stimulation (Fig. 8). Reports of NADPH oxidase or ROS-independent NET pathways do exist71,72, with many demonstrations of mitochondrial-derived ROS triggering NETs73,74,75. While it is difficult to exclude the possibility of a NADPH oxidase-independent pathway to O. ostertagi-mediated NET formation, the complete lack of ROS detected during stimulation diminishes the likelihood of a mitochondrial-ROS pathway. Curiously, LPS is often considered an inducer of NETs30, yet it is widely known that LPS alone is a poor stimulator of ROS76, which we also observed.
We have shown that both bovine and murine neutrophils demonstrated no measurable ROS response to O. ostertagi stimulation. This suggests a potential difference between the non-physiological PMA-induced NET pathway and the O. ostertagi pathway, a concern that has been raised previously regarding the use of PMA39. In addition, while DPI is the most widely used inhibitor of NADPH oxidase, DPI can affect various other cellular processes as well, particularly in the mitochondria77. Data resulting from use of DPI may require more cautious interpretation than has been previously considered and the discovery of specific alternative inhibitors should be actively sought.
The ability of ROS itself, independent of NADPH oxidase, to induce NETs has been reported previously in humans14 and chickens78. In the current work, we therefore assayed NET release in cattle following addition of exogenous ROS in the form of H2O2, which induced NETs, even in the presence of NADPH oxidase inhibitor, confirming that bovine neutrophils are also capable of forming NETs in the presence of ROS alone. Interestingly, it has been shown that certain organisms such as Candida albicans possess the ability to detoxify or degrade ROS utilizing superoxide dismutases (SOD) and catalases79,80 as an effective strategy against neutrophils. It is plausible that similar enzymes may be present within nematode worms such as O. ostertagi. Paradoxically, it has also been reported that C. albicans is able to produce its own ROS47, enough to rescue NET formation in CGD-isolated neutrophils. However, these explanations do not align with the demonstrated lack of discernable ROS production. In addition, the presence of the ROS scavenger Vitamin C did not affect OO-induced NET formation, further diminishing the role of ROS in OO-induced NET formation. Overall, our results suggest that the formation of NETs may be dependent upon multiple factors, of which ROS production is but one and may not be necessary (Fig. 8).
Our data clearly demonstrate the ability of O. ostertagi to induce NET formation, suggesting a potential role for NET formation in the innate immune response of cattle to the parasite O. ostertagi. Further, the response of NET formation is not specific to live, fully intact parasite but can also be induced with parasite antigen alone. Surprisingly, the O. ostertagi-mediated NET response appears to be independent of ROS, but requires NADPH oxidase activity (Fig. 8). While this result is difficult to interpret, a plausible hypothesis is that multiple pathways are involved in the NET response to O. ostertagi, which is clearly distinct from the PMA-induced NETs previously studied. In addition, it is certain that the in vivo context presents additional complexity compared to the simplified, single cell type models. The contribution of cytokines, chemokines, and interactions with other cells in the local milieu can alter the response as well as outcome, which warrants further investigations. While the actual ability of NETs to capture or even kill O. ostertagi and its relevance in vivo remain unclear, we nevertheless conclude that O. ostertagi is able to induce NETs in vitro (Fig. 8), and suggest that NETs can be a potential immune defense mechanism by against infection.
Methods
Cattle
The Wye Angus herd is a closed herd maintained by the Wye Research and Education Center, University of Maryland Experimental Station (Queenstown, MD)81. The steers The steers were maintained on the pasture of orchard grass, alfalfa, or clover, and fed with alfalfa, and bailage in winter82. Helminth-free Holstein steers were raised and maintained indoors on concrete slab since birth on the campus of Beltsville Agricultural Research Center (BARC), Beltsville, MD. Jugular venous blood was obtained for neutrophil and serum isolation. Animal Care and Use Protocols were approved by both the BARC (#16–019) and UMD (R-FEB-18-06) Institutional Animal Care and Use Committees. All methods were performed in accordance with the relevant guidelines and regulation.
Parasite propagation and parasitic antigen preparation
O. ostertagi adult worms and stage four larvae (L4) were propagated in helminth-free calves as described previously83. Briefly, 4–6 months old, helminth-free Holstein steers were inoculated with a bolus dose of O. ostertagi L3 on Day 0 and euthanized on Day 9 for L4 larvae or Day 21 for adult worm, and the abomasum and abomasal content were collected for parasite isolation. Parasites were collected from the abomasal tissue using the Baermann technique (L4) or from the abomasal content using the gel migration method (adult). Following collection by Baermanization, live L4 larvae were washed 3 times in cell culture medium containing penicillin, streptomycin, and fungizone in 5-time strength. To remove antibiotics, the larvae were washed 5 times with antibiotic-free cell culture medium. Adult parasites were washed 2 times with cold PBS and homogenized in cold PBS on ice at maximum speed for five 15-sec pulses using a Polytron homogenizer (Brinkmann Instrument, Westbury, NY). The homogenate was centrifuged at 20,000 g for 30 min at 4 °C and soluble extract (hereafter referred to as “OO extract”) was stored at −20 °C prior to experimental use.
For the Caenorhabditis elegans (C. elegans) experiments, a mixed population (early stage larvae to adult) of soil nematode Caenorhabditis elegans was grown at 20 °C in axenic liquid mCeHR-2 medium supplemented with 20 μM hemin84. Both live and heat-killed (60 °C, 60 min) worms were centrifuged at 800 g and washed twice with PBS before being resuspended in RPMI media85.
Bovine neutrophil isolation
Jugular vein blood was collected from cattle using vacutainers containing EDTA or no additive (Becton Dickinson Vacutainer Systems, Franklin Lakes, NJ). Neutrophils were isolated as previously described84 with minor modifications; briefly, blood was transferred to 15 mL conical tubes (Fisher Scientific, Pittsburgh, PA, USA) and centrifuged for 20 min at 1,000 g at 4 °C. Following centrifugation, the plasma, buffy coat, and one-third of the red blood cell pellet were discarded. The remaining cells were resuspended in 5 mL ammonium-chloride-potassium (ACK) lysis buffer to remove red blood cells. The cell suspension was gently mixed and incubated for 5 min at room temperature (RT). The solution was then centrifuged for 10 min (200 g at 4 °C) and the supernatant was decanted. The pellet was washed with 15 mL of calcium- and magnesium-free PBS (CMF-PBS) and centrifuged for 5 min (850 g at 4 °C). For complete red blood cell lysis, ACK treatment was repeated. Cells were then washed twice with 15 mL of CMF-PBS and centrifuged for 5 min (850 g at 4 °C). After the final wash, the pellet was resuspended in 1 mL of RPMI 1640 lacking phenol red (Gibco, Fisher Scientific), and neutrophil concentrations were measured using the trypan blue exclusion method on a hemocytometer.
Mouse neutrophil isolation
Neutrophils were isolated from bone marrow of tibias and femurs of adult mice by density gradient centrifugation as described previously86,87,88 and resuspended in phenol red-free RPMI 1640 medium containing 2% FBS.
NET Quantification
Neutrophils were re-suspended in RPMI 1640 medium containing 2% FBS and lacking phenol red. Cells were deposited in triplicate into 96-well flat-bottom plates (Nunc, Fisher Scientific) and incubated for 30 min (preincubation) at 37 °C and 5% CO2 prior to stimulation. Cells were then stimulated for up to 3 hours with OO extract (3 µg/mL) or Toll-like receptor 4 (TLR4) ligand LPS (100 ng/mL, InvivoGen, San Diego, CA) in a final volume of 200 µL per well. Dose dependency of OO extract was evaluated using further dilutions (1:10 and 1:100) in RPMI medium. For live worm experiments, neutrophils were cultured with either C. elegans (20 or 40 worms/well) or O. ostertagi L4 larvae (40 worms/well) in triplicate.
Following stimulation, micrococcal nuclease was added (5 U/well, New England Biolabs, Ipswich, MA, USA) and incubated for 15 min. Samples were centrifuged (800 g, 5 min) and the supernatants (100 μL/well) were transferred to a black 96-well flat-bottom plate (Nunc). The samples were stained with the fluorescent DNA dye Sytox Green (5 µM final concentration, Invitrogen, Carlsbad CA, USA) and incubated at RT in the dark for 10 min89. NET formation was quantified in arbitrary fluorescent units (AFU) by spectrofluorometric analysis with an excitation wavelength of 485 nm and an emission wavelength of 525 nm using an automated plate reader (Biotek, Winooski, VT, USA). For negative controls, unstimulated neutrophils in regular RPMI medium lacking phenol red were used. Neutrophil stimulation with phorbol 12-myristate 13-acetate (PMA; Sigma, St. Louis, MO, USA 100 nM final concentration) served as a positive control19.
Inhibition Assays
Specific inhibitors described previously were used for blockage of NET formation and have been described previously23,34,40,46,90,91,92,93,94. The following inhibitors were used: the NE inhibitor Suc-Ala-Ala-Pro-Val chloromethyl ketone (CMK; 1 mM final concentration, Sigma), NADPH oxidase (NOX) inhibitor diphenylene iodonium (DPI; 10 μM final concentration, Sigma), the MPO inhibitor 4-Aminobenzoic acid hydrazide (ABAH; 100 μM final concentration, Sigma), TLR4 signaling inhibitor CLI-095 (1 μg/mL final concentration; InvivoGen), the TLR4 signaling inhibitor polymixin B (100 μg/mL final concentration; InvivoGen, San Diego, CA), the PKC inhibitor Bisindolylmaleimide I (310 nM final concentration, Cayman Chemical, Ann Arbor, MI), and the ROS scavenger inhibitor ascorbic acid (Vitamin C) (200 μM final concentration, Cayman Chemical, Ann Arbor, MI). Cells were pre-incubated with inhibitors for 30 min at 37 °C prior to stimulation as described above23,34.
Visualization of NETs and Detection of NET-associated proteins
Isolated neutrophils (3 × 105) were seeded on 13 mm round glass coverslips pre-treated with poly-L-lysine (Sigma) in 24-well plates and were allowed to adhere for 30 min at 37 °C95. Cells were then stimulated as described previously for up to 3 hours. Following treatment, coverslips were washed with PBS and fixed in 2% paraformaldehyde for 15 min at RT. Coverslips were then washed 3 times with PBS and blocked with 2% BSA (Sigma) for 30 min to prevent non-specific binding. To detect histone or NE, coverslips were incubated with anti-histone (H3) antibody (Fisher Scientific) at 1:1000 or anti-NE antibody (Abcam, Cambridge, MA, USA) at 1:200 for 1 h at room temperature (RT). Following first antibody incubation, coverslips were washed twice with PBS and incubated 30 min at RT with anti-mouse IgG-PE (Biolegend, San Diego, CA, USA) diluted at 1:500 in blocking buffer. Coverslips were subsequently stained with Sytox Green (1:1000, 15 min), washed twice with PBS, and mounted on glass slides using anti-fade mounting buffer (Fisher Scientific). Images were taken using a laser scanning confocal microscope (Zeiss LSM 510 system, Thornwood, NY, USA).
Measurement of DNA in sera from OO-challenges and uninfected control cattle
Cattle were infected with OO L3 and venous blood samples were collected at days 0, 15 and 29 post infection. Serum was carefully harvested, without pigment contamination96. Serum sample (10 µL) was added to 90 µL of PBS, followed by addition of 100 uL of Sytox Green (1:200) per well in a black 96-well flat bottom plate (Nunc) and incubated in the dark for 15 minutes at RT. Fluorescence was quantified as described in “NET Quantification” using a spectrofluorometer.
Chemiluminescent measurement of ROS production
ROS production was measured by chemiluminescence as described previously14,97. Neutrophils (1 × 105) were resuspended in RPMI 1640 containing 11 mM HEPES, 55 mM Luminol (Fisher), and 1.2 U/mL horse radish peroxidase (Sigma). Ninety µL of the cells was then plated in a white 96-well flat bottom microplate (Nunc) and subsequently stimulated with 10 µL of stimuli as described in “NET quantification”. Chemiluminescence was recorded for 1 s per well every 2 min for 30 min prior to addition of stimuli, and for an additional 2 h using an automated plate reader set to 37 °C.
Statistical Analysis
Statistical analysis was performed with Prism 5 (GraphPad Software, Inc., La Jolla, CA), with specific details described in figure legends. Overall, all data have passed the Kolmogorov–Smirnov normality test. All data were analyzed by one-way ANOVA with Newman-Keuls Multiple Comparison Test. Asterisks indicate statistical significance. *P < 0.05; **P < 0.01; ***P < 0.001.
References
Gasbarre, L. C., Smith, L. L., Hoberg, E. & Pilitt, P. A. Further characterization of a cattle nematode population with demonstrated resistance to current anthelmintics. Veterinary parasitology 166, 275–280 (2009).
Tuo, W. et al. Abomasal mucosal immune responses of cattle with limited or continuous exposure to pasture-borne gastrointestinal nematode parasite infection. Veterinary parasitology 229, 118–125 (2016).
Gasbarre, L.C. Effects of gastrointestinal nematode infection on the ruminant immune system. Veterinary parasitology 72, 327–337; discussion 337–343 (1997).
Klesius, P. H. Immunity to Ostertagia ostertagi. Veterinary parasitology 27, 159–167 (1988).
Fox, M. T. Pathophysiology of infection with gastrointestinal nematodes in domestic ruminants: recent developments. Veterinary parasitology 72, 285–308 (1997).
Cabaret, J., Bouilhol, M. & Mage, C. Managing helminths of ruminants in organic farming. Veterinary research 33, 625–640 (2002).
Sutherland, I. A. & Leathwick, D. M. Anthelmintic resistance in nematode parasites of cattle: a global issue? Trends in parasitology 27, 176–181 (2011).
Edmonds, M. D., Johnson, E. G. & Edmonds, J. D. Anthelmintic resistance of Ostertagia ostertagi and Cooperia oncophora to macrocyclic lactones in cattle from the western United States. Veterinary parasitology 170, 224–229 (2010).
Artis, D. & Grencis, R. K. The intestinal epithelium: sensors to effectors in nematode infection. Mucosal immunology 1, 252–264 (2008).
Gómez-Muñoz, M. T. et al. Inhibition of bovine T lymphocyte responses by extracts of the stomach worm Ostertagia ostertagi. Veterinary parasitology 120, 199–214 (2004).
Claerebout, E. & Vercruysse, J. The immune response and the evaluation of acquired immunity against gastrointestinal nematodes in cattle: a review. Parasitology 120, Suppl, S25–42 (2000).
Kolaczkowska, E. & Kubes, P. Neutrophil recruitment and function in health and inflammation. Nature Reviews Immunology 13, 159–175 (2013).
Kruger, P. et al. Neutrophils: Between host defence, immune modulation, and tissue injury. PLoS pathogens 11, e1004651 (2015).
Fuchs, T. A. et al. Novel cell death program leads to neutrophil extracellular traps. The Journal of cell biology 176, 231–241 (2007).
Hermosilla, C., Caro, T. M., Silva, L. M. R., Ruiz, A. & Taubert, A. The intriguing host innate immune response: novel anti-parasitic defence by neutrophil extracellular traps. Parasitology 141, 1489–1498 (2014).
Ermert, D. et al. Mouse Neutrophil Extracellular Traps in Microbial Infections. Journal of innate immunity 1, 181–193 (2009).
Silva, L. M. R. et al. The apicomplexan parasite Eimeria arloingi induces caprine neutrophil extracellular traps. Parasitology research 113, 2797–2807 (2014).
Yildiz, K. et al. Role of NETs in the difference in host susceptibility to Toxoplasma gondii between sheep and cattle. Veterinary Immunology and Immunopathology 189, 1–10 (2017).
Lippolis, J. D., Reinhardt, T. A., Goff, J. P. & Horst, R. L. Neutrophil extracellular trap formation by bovine neutrophils is not inhibited by milk. Veterinary Immunology and Immunopathology 113, 248–255 (2006).
Carretta, M. D. et al. Butyric acid stimulates bovine neutrophil functions and potentiates the effect of platelet activating factor. Vet Immunol Immunopathol 176, 18–27 (2016).
Alarcon, P. et al. d(−) Lactic Acid-Induced Adhesion of Bovine Neutrophils onto Endothelial Cells Is Dependent on Neutrophils Extracellular Traps Formation and CD11b Expression. Frontiers in immunology 8, 975 (2017).
Maksimov, P., Hermosilla, C., Kleinertz, S., Hirzmann, J. & Taubert, A. Besnoitia besnoiti infections activate primary bovine endothelial cells and promote PMN adhesion and NET formation under physiological flow condition. Parasitology research 115, 1991–2001 (2016).
Villagra-Blanco, R. et al. Bovine Polymorphonuclear Neutrophils Cast Neutrophil Extracellular Traps against the Abortive Parasite Neospora caninum. Frontiers in immunology 8, 606 (2017).
Munoz-Caro, T. et al. Eimeria bovis-triggered neutrophil extracellular trap formation is CD11b-, ERK 1/2-, p38 MAP kinase- and SOCE-dependent. Veterinary research 46, 23 (2015).
Munoz-Caro, T., Lendner, M., Daugschies, A., Hermosilla, C. & Taubert, A. NADPH oxidase, MPO, NE, ERK1/2, p38 MAPK and Ca2+influx are essential for Cryptosporidium parvum-induced NET formation. Developmental and comparative immunology 52, 245–254 (2015).
Behrendt, J. H., Ruiz, A., Zahner, H., Taubert, A. & Hermosilla, C. Neutrophil extracellular trap formation as innate immune reactions against the apicomplexan parasite Eimeria bovis. Veterinary immunology and immunopathology 133, 1–8 (2010).
Munoz Caro, T., Hermosilla, C., Silva, L. M., Cortes, H. & Taubert, A. Neutrophil extracellular traps as innate immune reaction against the emerging apicomplexan parasite Besnoitia besnoiti. PLoS One 9, e91415 (2014).
Gondaira, S., Higuchi, H., Nishi, K., Iwano, H. & Nagahata, H. Mycoplasma bovis escapes bovine neutrophil extracellular traps. Vet Microbiol 199, 68–73 (2017).
Urban, C. F., Reichard, U., Brinkmann, V. & Zychlinsky, A. Neutrophil extracellular traps capture and kill Candida albicans yeast and hyphal forms. Cellular microbiology 8, 668–676 (2006).
Brinkmann, V. et al. Neutrophil Extracellular Traps Kill Bacteria. Science 303 (2004).
Wardini, A. B. et al. Characterization of neutrophil extracellular traps in cats naturally infected with feline leukemia virus. Journal of General Virology 91, 259–264 (2010).
Guimarães-Costa, A. B. et al. Leishmania amazonensis promastigotes induce and are killed by neutrophil extracellular traps. PNAS 106, 6748–6753 (2009).
Silva, L. M. et al. Far beyond Phagocytosis: Phagocyte-Derived Extracellular Traps Act Efficiently against Protozoan Parasites In Vitro and In Vivo. Mediators of inflammation 2016, 5898074 (2016).
Muñoz-Caro, T. et al. Leucocyte-derived extracellular trap formation significantly contributes to Haemonchus contortus larval entrapment. Parasites & vectors 8, 607 (2015).
Kenno, S., Perito, S., Mosci, P., Vecchiarelli, A. & Monari, C. Autophagy and Reactive Oxygen Species Are Involved in Neutrophil Extracellular Traps Release Induced by C. albicans Morphotypes. Frontiers in microbiology 7, 879 (2016).
Mario, M., Stelvio, T., Vincenzo, R., Manuela, R. & Filippo, R. Near infrared laser irradiation induces NETosis via oxidative stress and autophagy. Lasers in medical science (2018).
Huang, H. et al. Damage-associated molecular pattern-activated neutrophil extracellular trap exacerbates sterile inflammatory liver injury. Hepatology (Baltimore, Md.) 62, 600–614 (2015).
Schauer, C. et al. Aggregated neutrophil extracellular traps limit inflammation by degrading cytokines and chemokines. Nature Medicine 20, 511–517 (2014).
van der Linden, M., Westerlaken, G. H. A., van der Vlist, M., van Montfrans, J. & Meyaard, L. Differential Signalling and Kinetics of Neutrophil Extracellular Trap Release Revealed by Quantitative Live Imaging. Scientific reports 7, 6529 (2017).
Lindemann, R. A. Bacterial activation of human natural killer cells: role of cell surface lipopolysaccharide. Infect Immun 56, 1301–1308 (1988).
Cardoso, L. S. et al. Polymyxin B as inhibitor of LPS contamination of Schistosoma mansoni recombinant proteins in human cytokine analysis. Microbial cell factories 6, 1 (2007).
Danner, R. L., Joiner, K. A. & Parrillo, J. E. Inhibition of endotoxin-induced priming of human neutrophils by lipid X and 3-Aza-lipid X. J Clin Invest 80, 605–612 (1987).
Neumann, A. et al. The antimicrobial peptide LL-37 facilitates the formation of neutrophil extracellular traps. The Biochemical journal 464, 3–11 (2014).
Azad, M. A. et al. Major pathways of polymyxin-induced apoptosis in rat kidney proximal tubular cells. Antimicrobial agents and chemotherapy 59, 2136–2143 (2015).
Vattimo Mde, F. et al. Polymyxin B Nephrotoxicity: From Organ to Cell Damage. PLoS One 11, e0161057 (2016).
Gray, R. D. et al. Activation of conventional protein kinase C (PKC) is critical in the generation of human neutrophil extracellular traps. Journal of inflammation (London, England) 10, 12 (2013).
Kenny, E. F. et al. Diverse stimuli engage different neutrophil extracellular trap pathways. eLife 6 (2017).
Park, J.-H. et al. Evaluation of Circulating Markers of Neutrophil Extracellular Trap (NET) Formation as Risk Factors for Diabetic Retinopathy in a Case-Control Association Study. Experimental and clinical endocrinology & diabetes: official journal, German Society of Endocrinology [and] German Diabetes Association 124, 557–561 (2016).
Ahmadinejad, F., Geir Moller, S., Hashemzadeh-Chaleshtori, M., Bidkhori, G. & Jami, M.S. Molecular Mechanisms behind Free Radical Scavengers Function against Oxidative Stress. Antioxidants (Basel, Switzerland) 6(2017).
Thomas, C. J. & Schroder, K. Pattern recognition receptor function in neutrophils. Trends in immunology 34, 317–328 (2013).
Pinegin, B., Vorobjeva, N. & Pinegin, V. Neutrophil extracellular traps and their role in the development of chronic inflammation and autoimmunity. Autoimmunity reviews 14, 633–640 (2015).
Delgado-Rizo, V. et al. Neutrophil Extracellular Traps and Its Implications in Inflammation: An Overview. Frontiers in immunology 8, 81 (2017).
Morgan, E. et al. Global Change and Helminth Infections in Grazing Ruminants in Europe: Impacts, Trends and Sustainable Solutions. Agriculture 3, 484–502 (2013).
Charlier, J., Höglund, J., von Samson-Himmelstjerna, G., Dorny, P. & Vercruysse, J. Gastrointestinal nematode infections in adult dairy cattle: Impact on production, diagnosis and control. Veterinary parasitology 164, 70–79 (2009).
Makepeace, B. L., Martin, C., Turner, J. D. & Specht, S. Granulocytes in helminth infection–who is calling the shots? Current medicinal chemistry 19, 1567–1586 (2012).
Galioto, A. M. et al. Role of eosinophils and neutrophils in innate and adaptive protective immunity to larval strongyloides stercoralis in mice. Infect Immun 74, 5730–5738 (2006).
Anthony, R. M. et al. Memory T(H)2 cells induce alternatively activated macrophages to mediate protection against nematode parasites. Nat Med 12, 955–960 (2006).
Horii, Y., Owhashi, M., Fujita, K., Nakanishi, H. & Ishii, A. A comparative study on eosinophil and neutrophil chemotactic activities of various helminth parasites. Parasitology research 75, 76–78 (1988).
Hawes, M. et al. Root Border Cells and Their Role in Plant Defense. Annual Review of Phytopathology 54, 143–161 (2016).
Pijanowski, L. et al. Carp neutrophilic granulocytes form extracellular traps via ROS-dependent and independent pathways. Fish & Shellfish Immunology 34, 1244–1252 (2013).
Klesius, P. H. Regulation of immunity to Ostertagia ostertagi. Veterinary parasitology 46, 63–79 (1993).
Sharma, A., Simonson, T. J., Jondle, C. N., Mishra, B. B. & Sharma, J. Mincle-Mediated Neutrophil Extracellular Trap Formation by Regulation of Autophagy. The Journal of infectious diseases 215, 1040–1048 (2017).
Etulain, J. et al. P-selectin promotes neutrophil extracellular trap formation in mice. Blood 126, 242–246 (2015).
Sattler, S., Ghadially, H. & Hofer, E. Evolution of the C-type lectin-like receptor genes of the DECTIN-1 cluster in the NK gene complex. The Scientific World Journal 2012, 931386 (2012).
Schönrich, G. & Raftery, M. J. Neutrophil Extracellular Traps Go Viral. Frontiers in immunology 7, 366 (2016).
Branzk, N. et al. Neutrophils sense microbe size and selectively release neutrophil extracellular traps in response to large pathogens. Nature immunology 15, 1017–1025 (2014).
Zawrotniak, M. et al. Aspartic Proteases and Major Cell Wall Components in Candida albicans Trigger the Release of Neutrophil Extracellular Traps. Frontiers in cellular and infection microbiology 7, 414 (2017).
Rosen, H. & Michel, B. R. Redundant contribution of myeloperoxidase-dependent systems to neutrophil-mediated killing of Escherichia coli. Infection and immunity 65, 4173–4178 (1997).
Soehnlein, O. An elegant defense: how neutrophils shape the immune response. Trends in immunology 30, 511–512 (2009).
Bedard, K. & Krause, K.-H. The NOX Family of ROS-Generating NADPH Oxidases: Physiology and Pathophysiology. Physiological Reviews 87, 245–313 (2007).
Rochael, N. C. et al. Classical ROS-dependent and early/rapid ROS-independent release of Neutrophil Extracellular Traps triggered by Leishmania parasites. Scientific reports 5, 18302 (2015).
Pilsczek, F. H. et al. A Novel Mechanism of Rapid Nuclear Neutrophil Extracellular Trap Formation in Response to Staphylococcus aureus. The Journal of Immunology 185, 7413–7425 (2010).
Douda, D. N., Khan, M. A., Grasemann, H. & Palaniyar, N. SK3 channel and mitochondrial ROS mediate NADPH oxidase-independent NETosis induced by calcium influx. PNAS 112, 2817–2822 (2015).
Lood, C. et al. Neutrophil extracellular traps enriched in oxidized mitochondrial DNA are interferogenic and contribute to lupus-like disease. Nature Medicine 22, 146–153 (2016).
Hosseinzadeh, A., Thompson, P. R., Segal, B. H. & Urban, C. F. Nicotine induces neutrophil extracellular traps. Journal of leukocyte biology 100, 1105–1112 (2016).
Doerfler, M. E., Danner, R. L., Shelhamer, J. H. & Parrillo, J. E. Bacterial lipopolysaccharides prime human neutrophils for enhanced production of leukotriene B4. The Journal of clinical investigation 83, 970–977 (1989).
Holland, P. C. & Sherratt, H. S. Biochemical effects of the hypoglycaemic compound diphenyleneiodonnium. Catalysis of anion-hydroxyl ion exchange across the inner membrane of rat liver mitochondria and effects on oxygen uptake. The Biochemical journal 129, 39–54 (1972).
Chuammitri, P. et al. Chicken heterophil extracellular traps (HETs): Novel defense mechanism of chicken heterophils. Veterinary Immunology and Immunopathology 129, 126–131 (2009).
Frohner, I. E., Bourgeois, C., Yatsyk, K., Majer, O. & Kuchler, K. Candida albicans cell surface superoxide dismutases degrade host-derived reactive oxygen species to escape innate immune surveillance. Molecular microbiology 71, 240–252 (2009).
Hosseinzadeh, A. & Urban, C. F. Novel Insight into Neutrophil Immune Responses by Dry Mass Determination of Candida albicans Morphotypes. PLoS ONE 8, e77993 (2013).
Zhao, C. et al. Muscle transcriptomic analyses in Angus cattle with divergent tenderness. Mol Biol Rep 39, 4185–4193 (2012).
Carrillo, J. A. et al. Integrated metabolomic and transcriptome analyses reveal finishing forage affects metabolic pathways related to beef quality and animal welfare. Scientific reports 6, 25948 (2016).
Qu, G. et al. Ostertagia ostertagi macrophage migration inhibitory factor is present in all developmental stages and may cross-regulate host functions through interaction with the host receptor. International journal for parasitology 44, 355–367 (2014).
Garcia, M., Elsasser, T. H., Biswas, D. & Moyes, K. M. The effect of citrus-derived oil on bovine blood neutrophil function and gene expression in vitro. Journal of dairy science 98, 918–926 (2015).
Sinclair, J. et al. Inter-organ signalling by HRG-7 promotes systemic haem homeostasis. Nature cell biology 19, 799–807 (2017).
Feng, Y., Zou, L., Si, R., Nagasaka, Y. & Chao, W. Bone marrow MyD88 signaling modulates neutrophil function and ischemic myocardial injury. American journal of physiology. Cell physiology 299, C760–C769 (2010).
Swamydas, M. & Lionakis, M.S. Isolation, purification and labeling of mouse bone marrow neutrophils for functional studies and adoptive transfer experiments. Journal of visualized experiments: JoVE, e50586 (2013).
Bruhn, K. W., Dekitani, K., Nielsen, T. B., Pantapalangkoor, P. & Spellberg, B. Ly6G-mediated depletion of neutrophils is dependent on macrophages. Results in immunology 6, 5–7 (2016).
Martinelli, S. et al. Induction of Genes Mediating Interferon-dependent Extracellular Trap Formation during Neutrophil Differentiation. Journal of Biological Chemistry 279, 44123–44132 (2004).
Duff, G. W. & Atkins, E. The inhibitory effect of polymyxin B on endotoxin-induced endogenous pyrogen production. J Immunol Methods 52, 333–340 (1982).
Jonas, E., Dwenger, A. & Hager, A. In vitro effect of ascorbic acid on neutrophil-endothelial cell interaction. Journal of bioluminescence and chemiluminescence 8, 15–20 (1993).
Carcamo, J. M., Borquez-Ojeda, O. & Golde, D. W. Vitamin C inhibits granulocyte macrophage-colony-stimulating factor-induced signaling pathways. Blood 99, 3205–3212 (2002).
Roberts, N. A., Haworth, R. S. & Avkiran, M. Effects of bisindolylmaleimide PKC inhibitors on p90RSK activity in vitro and in adult ventricular myocytes. British journal of pharmacology 145, 477–489 (2005).
Mohammed, B. M. et al. Vitamin C: a novel regulator of neutrophil extracellular trap formation. Nutrients 5, 3131–3151 (2013).
Gabriel, C., McMaster, W. R., Girard, D. & Descoteaux, A. Leishmania donovani Promastigotes Evade the Antimicrobial Activity of Neutrophil Extracellular Traps. The Journal of Immunology 185, 4319–4327 (2010).
Lawson, C., Smith, S. A., O’Brien, M. & McMichael, M. Neutrophil Extracellular Traps in Plasma from Dogs with Immune-mediated Hemolytic Anemia. Journal of veterinary internal medicine/American College of Veterinary Internal Medicine 32, 128–134 (2018).
Liu, L., Dahlgren, C., Elwing, H. & Lundqvist, H. A simple chemiluminescence assay for the determination of reactive oxygen species produced by human neutrophils. Journal of immunological methods 192, 173–178 (1996).
Acknowledgements
The authors are grateful to Lei Li, Shu-Wei Wu, Yuqing He, Xiaojing Yuan and Edward Draper of UMD, and Mr. Eliseo Miramontes of USDA/ARS for excellent technical assistance. Research was supported by USDA NIFA GRANT11885997 (ZX), USDA/ARS Specific Cooperative Agreement with University of Maryland (WT, ZX), Jorgensen Foundation (ZX), MAES program in University of Maryland (ZX) and funds from USDA/ARS (WT). Authors are grateful to the inspiring discussions with and/or critical reviews by Dr. Meiqing Shi of UMD, and great help from Dr. Li Ma (UMD) in improving statistical analysis.
Author information
Authors and Affiliations
Contributions
Z.X., W.T. and J.M. conceived the study. Z.X. and W.T. coordinated the study. Z.X., J.M. and D.S. designed, performed and analyzed the experiments. J.M., Z.X. and W.T. wrote the manuscript.
Corresponding authors
Ethics declarations
Competing Interests
The authors declare no competing interests.
Additional information
Publisher’s note: Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made. The images or other third party material in this article are included in the article’s Creative Commons license, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons license and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this license, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Mendez, J., Sun, D., Tuo, W. et al. Bovine neutrophils form extracellular traps in response to the gastrointestinal parasite Ostertagia ostertagi. Sci Rep 8, 17598 (2018). https://doi.org/10.1038/s41598-018-36070-3
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41598-018-36070-3
Keywords
This article is cited by
-
Trichinella spiralis excretory/secretory products from adult worms inhibit NETosis and regulate the production of cytokines from neutrophils
Parasites & Vectors (2023)
-
Fasciola hepatica soluble antigens (FhAg) induce ovine PMN innate immune reactions and NET formation in vitro and in vivo
Veterinary Research (2023)
-
Characterization of IL-10-producing neutrophils in cattle infected with Ostertagia ostertagi
Scientific Reports (2019)
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.