Abstract
Patients treated for cancer frequently experience chemobrain, characterized by impaired memory and reduced attention. These deficits often persist after treatment, and no preventive or curative interventions exist. In mice, we assessed the effect of cisplatin chemotherapy on attention using the 5-choice serial reaction time task and on synaptic integrity. We also assessed the capacity of mesenchymal stem cells to normalize the characteristics of chemobrain. Mice were trained in the 5-choice serial reaction time task. After reaching advancement criteria at a 4-second stimulus time, they were treated with cisplatin followed by nasal administration of mesenchymal stem cells. Cisplatin reduced the percentage of correct responses due to an increase in omissions, indicating attention deficits. Mesenchymal stem cell treatment reversed these cisplatin-induced deficits in attention. Cisplatin also induced abnormalities in markers of synaptic integrity in the prefrontal cortex. Specifically, cisplatin decreased expression of the global presynaptic marker synaptophysin and the glutamatergic presynaptic marker vGlut2. Expression of the presynaptic GABAergic marker vGAT increased. Nasal mesenchymal stem cell administration normalized these markers of synaptic integrity. In conclusion, cisplatin induces long-lasting attention deficits that are associated with decreased synaptic integrity in the prefrontal cortex. Nasal administration of mesenchymal stem cells reversed these behavioural and structural deficits.
Similar content being viewed by others
Introduction
The American Cancer Society estimates that the number of cancer survivors in the United States will increase from more than 15.5 million in 2016 to more than 20 million by 20261. Inevitably, the number of cancer survivors dealing with the long-term adverse effects of cancer and its treatment will increase. For example, cognitive deficits, including difficulties with attention, concentration, processing speed, and language, are experienced by up to 75% percent of patients treated with chemotherapy for cancers outside the nervous system2,3,4,5,6,7. These cognitive deficits, also known as “chemobrain,” can persist for months or even years after completion of cancer treatment. Advanced neuroimaging techniques show global disruptions of connectivity in patients suffering from chemotherapy-induced cognitive impairment, along with structural alterations in white and grey matter8,9,10,11,12. To date, no interventions to prevent or reverse these adverse effects of cancer and its treatment have been approved by the US Food and Drug Administration.
Most studies on chemobrain in humans have focused on women treated for breast cancer. However, emerging evidence indicates that cognitive deficits also affect patients treated with platinum-based compounds for small cell lung carcinoma, bladder cancer, prostate cancer, or ovarian cancer13,14,15,16,17,18. Advanced imaging techniques confirm functional and structural abnormalities in the brains of patients treated with platinum-based compounds14,16,17,18.
Platinum-based compounds induce cognitive deficits and damage to the brain in rodents as well19,20,21,22. We recently showed that cisplatin treatment of young adult mice (10‒12 weeks old) impairs their performance in behavioural tasks examining short-term memory and spatial orientation, such as the novel object and place recognition task (NOPRT), and spontaneous alternations in the Y-maze21,22. These cognitive deficits were not associated with reductions in locomotor activity, food intake, total interaction times in the NOPRT, or total number of arm entries in the Y-maze, indicating that the deficit cannot be explained by a general decrease in activity21,22. More importantly, we showed that intranasal application of mesenchymal stem cells (MSCs) 48 and 96 hours after completion of cisplatin treatment completely reversed these cisplatin-induced memory and orientation deficits in young adult mice (Chiu et al.23).
As mentioned above, patients with chemobrain not only show signs of memory deficits, but also show impairment in attention and executive functioning. The 5-choice serial reaction time task (5CSRTT) has been developed to assess attention deficits in rats and mice24,25,26,27,28. We used this task in adult mice (7‒8 months old) to examine the effects of cisplatin treatment on these translationally relevant aspects of chemotherapy-induced deficits in cognitive function. We also assessed the effects of nasal MSC application on performance in the 5CSRTT. To get more insight into the structural abnormalities associated with impaired performance in this behavioural task, we examined the effects of cisplatin and MSCs on synaptic integrity in the prefrontal cortex.
Methods
Animals
The animal experiments reported herein were conducted in accordance with ARRIVE (Animal Research: Reporting of In Vivo Experiments) guidelines for ethical animal research and with National Institutes of Health guidance on the care and use of laboratory animals. All experiments were conducted at The University of Texas MD Anderson Cancer Center in Houston, Texas. All procedures were approved by the MD Anderson Institutional Animal Care and Use Committee.
Experiments were performed with male C57BL/6J mice (Jackson Laboratory, Bar Harbor, ME) housed at 22 ± 2 °C, on a 12/12-hour reverse dark–light cycle (dark 830–2030 hours) with water and food ad libitum. Mice were group-housed for the duration of the study. At an age of 5‒6 months, all mice were food restricted to 80–85% of their free-feeding body weight, as is standard for operant testing protocols. Mice were trained in the operant chamber as described below until all mice had reached the 4-second stimulus time advancement criteria. This approach was selected to ensure that all mice had learned the task before exposure to cisplatin. Mice were then returned to free feeding and treated with 2 cycles of 5 daily intraperitoneal injections of cisplatin (2.3 mg/kg/day; Fresenius Kabi USA, Lake Zurich, IL) or phosphate-buffered saline (PBS), followed by a 5-day rest without injections. This schedule was selected on the basis of our previous work21.
Experimental Plan
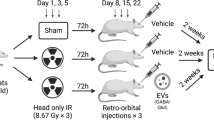
We performed 2 separate experiments. In Experiment 1 (saline n = 5 mice; cisplatin n = 7 mice), there were no further interventions. In Experiment 2, mice were treated with saline (n = 11) or cisplatin (n = 20) followed by nasal administration of MSCs or PBS (saline/PBS: n = 5; saline/MSCs: n = 6; cisplatin/PBS: n = 10; cisplatin/MSCs: n = 10) 48 hours and 96 hours after completion of cisplatin treatment. We have not detected differences between the saline/PBS and saline/MSCs groups; therefore, we pooled the results from these 2 groups for data analysis and labelled the pooled group “control”.
Mouse MSCs (GIBCO Mouse C57BL/6; Invitrogen, Carlsbad, CA) were cultured in Dulbecco’s Modified Eagle’s medium/F12 medium with GlutaMax-I, supplemented with 10% MSC-qualified foetal bovine serum and 5 µg/mL gentamycin (all from Invitrogen). Before administration of MSCs, 3 µL per nostril of hyaluronidase in PBS (total 100 U per mouse; Sigma-Aldrich, St. Louis, MO) was administered to each nostril to increase the permeability of the nasal mucosa29,30. Thirty minutes later mice received MSCs applied as 2 doses of 3 µL to each nostril (total volume of 12 µL with 106 cells per mouse per day29,30) or PBS. We selected this schedule on the basis of our previous work in models of ischemic brain damage30,31,32,33. Three days before returning to the 5CSRTT training, mice were put back on the food-restriction schedule.
5-Choice Serial Reaction Time Task
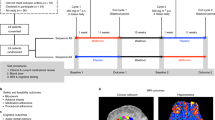
The 5-CSRTT was administered by a single investigator as described previously28 and using the schedule presented in Fig. 1A. The operant testing boxes (Modular test chamber, model ENV-307W) were obtained from Med Associates INC (Fairfax, VT). Mice were exposed to 1 session per day from Monday through Friday. They were food restricted from Sunday until end of day on Friday, and then had free access to food until Sunday morning.
Schematic overview of 5CSRTT and experimental setup. (A) Overview of the 5-choice serial reaction time task procedure. (B) Schematic overview and body weight over time for the 2 experiments. Cisplatin treatment consisted of 5 days of 2.3 mg/kg i.p, followed by 5 days of rest and another 5 days of cisplatin. Mice were allowed free access to food during the course of treatment. After cisplatin mice were exposed to the 5 CSRT for 6–7 weeks. In experiment 1, training was resumed after a 2 month-interval (4 months after cisplatin). In experiment 2, the long ITI was introduced during the last week of 5CSRT, when performance at the 1 sec stimulus time and 5 second ITI had been stable for at least 5 days. Abbreviations: 5CSRTT, 5-choice serial reaction time task; i.p., intraperitoneal; ITI, intertrial interval; LH, limit hold; MSC, mesenchymal stem cells.
Chamber Habituation, Nose Poke, and Food Magazine Pre-Training
Before starting 5CSRTT training, mice were exposed to the reward (Chocolate-flavored Dustless Precision Pellets, Med Associates, St Albans, VT) in their home cage. The next day, nose-poke training was started by introducing each mouse individually to the chamber for 20 minutes, with all 5 stimulus lights and the food magazine light illuminated. Two chocolate pellets were placed in each of the 5 light apertures, and 10 chocolate pellets were placed in the magazine. Daily training sessions were repeated until the mouse reliably consumed all pellets provided. During the subsequent food magazine training sessions, a light in 1 of the 5 stimulus holes was kept on until the mouse made a nose poke and consumed the pellet in the food magazine. This session was repeated 2–3 times, until the mouse could finish up to 50 trials (consume 50 pellets) within the 20-minute session time.
5CSRTT Training
During the 5CSRTT training, a nose poke into the illuminated hole was required to obtain the reward. Training was initiated by completion of a magazine entry, triggering an intertrial interval (ITI) of 5–10 seconds during which the animal waited for illumination of 1 of the 5 holes at the back of the chamber (Fig. 1A). A nose poke to the illuminated hole completed a correct trial and triggered delivery of the reward; the cycle was then repeated. The initial stimulus time was 16 seconds. Mice were kept at the same stimulus time for 2 consecutive sessions after meeting the advancement criterion (stimulus time of 16 seconds or 8 seconds: ≥30 correct trials and 50 trials in total over 2 consecutive days; stimulus time ≤4 seconds: >50% correct trials and 100 trials). Then timing was reduced to 8 seconds, 4 seconds, 2 seconds, and 1 second.
Only a correct response during the stimulus time and a following 2-second limit hold time initiated the reward. If the mouse nose poked correctly during the stimulus time plus the 2-second limit hold, then the food reinforcer was delivered. If the mouse nose poked a non-illuminated hole (incorrect response) or failed to respond within the stimulus time plus the 2-second limit hold period (omitted response), the chamber light was illuminated for 5 seconds (time out), after which the cycle restarted. If the mouse nose poked during the 5–10-second ITI (premature response), a 5-second time out was presented. A session was completed when the maximum number of trials (50 trials for the 16-second or 8-second stimulus time, or 100 trials for stimulus times ≤4 seconds), or the maximum session duration (30 minutes) was reached.
After a mouse met advancement criterion at a stimulus time of 4 seconds, we continued training it with a 4-second stimulus time for at least 8 days. Subsequently, the mouse was returned to free feeding, with cisplatin treatment initiated 3 days later. After completion of cisplatin treatment, mice were food restricted for 1 week, after which 5CSRTT was restarted at a stimulus time of 4 seconds. Mice continued the 5CSRTT until they met advancement criteria at a stimulus time of 1 second.
To determine whether there is spontaneous recovery of cisplatin-induced attention deficits, the mice in Experiment 1 were re-tested in the 5CSRTT starting 4 months after completion of treatment, at a 4-second stimulus time. We again tested the mice when they reached advancement criteria at the 1-second stimulus time.
The number and percentage of correct, incorrect, and omitted trials, latency times to correct and incorrect responses, and latency to collect the reward were recorded.
Immunofluorescence Analysis of Synaptic Markers
Twelve weeks after completion of cisplatin treatment, half of the mice from Experiment 2 were perfused intracardially with ice-cold PBS followed by 4% paraformaldehyde in PBS. Brains were post-fixed in 4% paraformaldehyde for 6 hours, cryoprotected in sucrose, and frozen in optimal cutting temperature compound (O.C.T.; Sakura Finetek, Torrance, CA). Sagittal sections (8 μm) were incubated with the following antibodies: rabbit anti-synaptophysin (1:1000; Millipore), mouse anti-vGLUT2 (1:1000; Abcam, Cambridge, MA), rabbit anti-PSD95 (1:1000; Abcam), mouse anti-vGAT (1:100; Abcam), and rabbit anti-gephyrin (1:1000; Abcam) followed by Alexa-488 goat anti-rabbit (1:1000; Invitrogen, Grand Island, NY) for synaptophysin, Alexa-488 goat anti-mouse (1:500; Invitrogen) for vGLUT2 and vGAT, and Alexa-594 goat anti-rabbit (1:500; Invitrogen) for PSD95 and gephyrin. As a negative control, primary antibody was omitted. Sections were visualized using a Leica SPE confocal microscope. Expression of each synaptic marker was quantified in 3–4 sections per mouse and 4–5 mice per group. The mean intensity of fluorescence was calculated using ImageJ software.
Statistical analysis
Data are expressed as mean ± standard error of the mean. Statistical analysis was performed using 1-way or 2-way analysis of variance (ANOVA) followed by Tukey analysis. P < 0.05 was considered statistically significant.
Results
Effect of Cisplatin on Learning/Memory in the 5CSRTT
Before treatment with cisplatin, we trained adult male C57BL/6 mice aged 5‒6 months at the start of the study in the operant chamber until they met advancement criteria at a stimulus time of 4 seconds (see Fig. 1B for schematic overview). Subsequently, mice were treated with 2 cycles of cisplatin (5 days 2.3 mg/kg/day, 5 days rest, 5 days 2.3 mg/kg/day) or vehicle and body weight was monitored regularly (Fig. 1B). In Experiment 1, mice did not receive further treatments. In Experiment 2, half the mice received MSCs via the nasal route 48 and 96 hours after completion of cisplatin treatment.
After completion of cisplatin treatment, we reintroduced the mice to the 5CSRTT at a stimulus time of 4 seconds according (Fig. 1B). On the second day, all mice had reached the advancement criteria (>50 responses, with >50% correct). However, the cisplatin-treated mice showed a lower percentage of correct responses (Fig. 2). The data in Fig. 2 indicate that this was due to an increase in omissions. There were no group differences in the percentages of incorrect responses. At this early time point after MSC administration, no improvement of performance in the 5CSRTT was observed (Fig. 2D–F).
Cisplatin has an acute effect on performance in the 5CSRTT. Mice were trained to reach advancement criteria at a stimulus time of 4 seconds. Subsequently, mice were treated with cisplatin as in Fig. 1. Nine days after completion of cisplatin treatment, training in the 5CSRTT operant box resumed at a stimulus time of 4 seconds. Performance in the 5CSRT was assessed the first two sessions after the mice reached advancement criterion. The percentage of correct responses, omissions, and incorrect responses is presented. Data were analysed by 2-way ANOVA repeated measures followed by Tukey post-test. (A–C) Experiment 1 (control: n = 5; cisplatin: n = 7). (D–F) Experiment 2 (Control: n = 11; cisplatin: n = 10; cisplatin + MSC: n = 10). Correct responses: group × time interaction: F = 3.37; P < 0.05. Omissions: group × time interaction: F = 5.16; P < 0.05. *P < 0.05.
Effect of Cisplatin and MSCs on Performance in the 5CSRTT at a Short Stimulus Time
Consistent with what we observed at the 4-second interval time, cisplatin-treated mice continued to show fewer correct responses at the 1-second interval time, and this was due to a larger percentage of omissions at both time points (Fig. 3A–F). These findings indicate that cisplatin treatment induces a persistent attention deficit. Notably, nasal administration of MSCs to cisplatin-treated mice normalized the number of correct responses and omissions (Fig. 3D–F).
Cisplatin treatment induces a persistent increase in omissions that is reversed by MSC. Mice were treated with cisplatin and MSC as described in Fig. 1B and trained to advancement criteria at a stimulus time of 1 second. The percentage of correct responses, omissions, and incorrect responses was assessed. (A–C) Experiment 1 data were analysed with Student’s t-test. (D–F) Experiment 2 data were analysed with 1-way ANOVA followed by Tukey post-test. One-way ANOVA for correct responses: F = 18.56; P < 0.0001; 1-way ANOVA for omissions: F = 11.58; P < 0.001. *P < 0.05; **P < 0.01; ***P < 0.001.
We did not detect any effect of cisplatin treatment on the number of premature responses in both experiments (Fig. 4A,B), indicating that the attention deficits (increased omissions) in cisplatin-treated mice were not associated with an increase in impulsivity. In the next set of trials in experiment 2, we increased the ITI from 5 to 10 seconds. As expected, this increased the number of premature responses (Figs 4C vs B). However, we still did not detect any effect of cisplatin on premature responses, supporting the notion that cisplatin treatment did not increase impulsivity (Fig. 4C). However, at the longer ITI we no longer detected group differences in correct responses and omissions (Fig. 4D–F), which further supports the conclusion that the increase in omissions is due to inattention34.
Cisplatin does not increase premature responses. Mice were treated with cisplatin and MSC as described in Fig. 1B and trained to advancement criteria at a stimulus time of 1 second. (A–C) The number of premature responses was quantified. (A) Experiment 1. (B) Experiment 2. (C) Experiment 2, ITI increased to 10 seconds. Data represent individual values and median +/−95% confidence. There were no statistically significant group differences detected. (C–E) Performance in the 5CSRTT at stimulus time of 1 second and ITI of 10 seconds was assessed for Experiment 2. No group differences in correct response, incorrect responses and omission were detected.
We also observed an increase in latency to reward in the cisplatin-treated mice (Fig. 5A,B) that was not affected by MSC treatment. An increase in the latency to reward may result from either lack of attention or a decrease in motivation. However, the latency to correct response, a measure frequently used to assess changes in motivation35,36,37,38, was not affected by cisplatin (Fig. 5C,D). Collectively, our findings indicate that cisplatin induced an increase in omissions that is mediated by a decrease in attention. However, we cannot fully exclude a contribution of decreased motivation.
Effect of cisplatin and MSC on motivation. During the 5CSRTT described in Fig. 4, the latency to correct response (A,B) and to reward (C,D) was determined. (A,C) Experiment 1; (B,D): Experiment 2; Latency to reward: 1-way ANOVA F = 11.58; ***P < 0.001. *P < 0.05; **P < 0.01.
To determine whether there is spontaneous recovery of the cisplatin-induced attention deficits, the mice in Experiment 1 were retested in the 5CSRTT starting 4 months after completion of treatment. Retesting the mice when they reached the advancement criterion at the 1-second stimulus time (approximately 8 weeks later) revealed that spontaneous recovery of cisplatin-induced attention deficits does not occur within this time frame (Fig. 6). The cisplatin-treated mice still displayed a decrease in correct responses that was fully explained by an increase in omissions.
Cisplatin-induced deficit in attention is long-lasting. The mice of Experiment 1 were retrained and tested at 4 months after completion of cisplatin. The results represent data obtained at a stimulus time of 1 second. The percentage of correct responses, omissions, and incorrect responses was assessed and data were analysed by Student t-test. **P < 0.01.
Effect of Cisplatin and MSCs on Synaptic Integrity
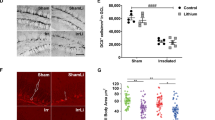
To determine the effects of cisplatin and MSCs on synaptic integrity, we quantified the expression of the presynaptic markers synaptophysin, vGAT, and vGlut2, the postsynaptic glutamatergic marker PSD95, and the γ-aminobutyric acid (GABA)ergic marker gephyrin in the prefrontal cortex after completion of the behavioural assessments 4 months after the last dose of cisplatin, when the animals were 11–12 months old. Treatment of mice with cisplatin sharply reduced the level of synaptophysin (Fig. 7) in the prefrontal cortex. This reduction in synaptophysin was associated with a decrease in the presynaptic glutamatergic marker vGLUT2 and an increase in the presynaptic GABAergic marker vGAT (Fig. 7).
Cisplatin alters expression of presynaptic markers in the prefrontal cortex and this is reversed by MSC. The mice from Experiment 2 were sacrificed at an age of 11–12 months and expression of the presynaptic markers synaptophysin (A,B), vGlut2 (C,D), and vGAT (E,F) in the prefrontal cortex was assessed by immunofluorescence analysis. For details on the areas included in density analysis see Supplementary Fig. 1. Images are representative examples; bar graphs represent mean and SEM of 5 mice per group. ***P < 0.001; **P < 0.01; *P < 0.05.
The change in the expression of the postsynaptic glutamatergic marker PSD95 did not reach statistical significance, while expression of gephyrin was increased in cisplatin-treated mice (Fig. 8). Nasal application of MSCs normalized the expression of all markers.
Effect of cisplatin and MSC on postsynaptic markers in the prefrontal cortex. The mice from Experiment 2 were sacrificed at an age of 11‒12 months. Expression of the glutamatergic postsynaptic marker PSD95 (A,B) and the GABAergic postsynaptic marker gephyrin (C,D) in the pre-frontal cortex was assessed by immunofluorescence analysis. We did not include the large bodies showing up in the gephyrin staining in our analysis. For details on the areas included in density analysis see Supplementary Fig. 1. Images are representative examples; bar graphs represent mean and SEM of 4‒5 mice per group. ***P < 0.001.
Discussion
Attention deficits and problems concentrating are frequently reported by patients during and after cancer treatment2,3,4,5,6,7. Here, we examined the effects of cisplatin on the performance of adult male mice in the 5CSRTT to assess deficits in attention and response inhibition24,25,26,27,28. Our results clearly demonstrate that treatment of adult (7‒8 months old) male mice with cisplatin induces a deficit in attention, demonstrated by increased omissions in the 5CSRTT. Importantly, we also show that nasal administration of MSCs after completion of cisplatin treatment reversed the attention deficit. The attention deficits as detected in the 5CSRTT were associated with abnormalities in the expression of markers of synaptic integrity in the prefrontal cortex, as characterized by a reduction in expression of the presynaptic marker synaptophysin and the glutamatergic marker vGlut2 and an increase in expression of the presynaptic GABAerigc marker vGAT. MSC treatment normalized expression of these markers of synaptic integrity in the prefrontal cortex of cisplatin-treated mice. Further studies are needed to determine whether cisplatin and MSCs have similar effects in female mice.
We recently demonstrated that treatment of young adult male or female mice (8‒10 weeks old at start of treatment) with cisplatin reduced performance in a number of behavioural tasks that assess spatial orientation and short-term memory, including the social recognition task and the novel object and place recognition task, and the spontaneous alternations in the Y-maze test21,22 (and Chiu et al.23). In addition, we showed that cisplatin decreases the performance of young adult mice in the puzzle box, a task developed to assess executive functioning (Chiu et al.23). We also showed that nasal application of MSCs after completion of cisplatin treatment, when mice were 11‒13 weeks-old, normalized cognitive functioning in these tasks (Chiu et al.23). In the current study, we chose to use mice who fully had reached adulthood as this is more relevant from a translational viewpoint. We show here that cisplatin treatment of 7‒8-month-old mice induces deficits in attention evidenced by an increase in omissions in the 5CSRTT. Without further intervention, the attention deficit lasts until at least 4 months after completion of cisplatin treatment. Notably, we also show that nasal administration of MSCs after completion of cisplatin treatment (when the mice are approximately 8 months old) is sufficient to reverse the behavioural deficits. This is an important finding because it shows that MSCs are capable of promoting repair not only of the young adult brain, but also of the brains of mice that have fully reached adulthood.
Our data show that cisplatin treatment decreased the percentage of correct responses without changing accuracy, but rather by increasing omissions. This increase in omissions could be due to a decrease in motivation; however, we did not detect changes in latency to correct response, which would be expected if motivation were reduced. In addition, we do not have evidence for an increase in omissions toward the end of a session, when the mice are expected to become less motivated because they may become satiated (not shown). Cisplatin did not induce changes in premature or perseverant responses, indicating that the reduction in attention developed without evidence for hyperactivity.
The prefrontal cortex plays a key role in the regulation of attention24,39, and our data show that impaired attention in cisplatin-treated mice is associated with changes in markers of synaptic integrity in the prefrontal cortex. More specifically, we detected a reduction in the expression of the presynaptic marker synaptophysin and in the glutamatergic presynaptic marker vGlut2. In contrast, cisplatin increased expression of the presynaptic GABAergic marker vGAT. These findings indicate a change in the inhibitory/excitatory balance in the prefrontal cortex of cisplatin-treated mice. MSC treatment prevented this change in expression of markers of synaptic integrity. Studies in rats using specific GABA-A receptor agonists or antagonists have shown that both can lead to impaired attention characterized by increased omissions40, indicating that both increases as well as decreases in GABAergic activity could lead to the behavioural phenotype observed in our cisplatin-treated mice.
The schedule of cisplatin treatment used in our study induces signs of neuropathic pain41,42,43, and there is evidence that neuropathic pain is associated with changes in excitatory/inhibitory balance44,45,46,47,48. Moreover, creating an excitatory imbalance in the brain is sufficient to induce mechanical allodynia49. It is therefore possible that cisplatin-induced changes in the inhibitory/excitatory balance contribute to the signs of peripheral neuropathy.
It has been suggested that chemotherapy accelerates the aging process in the brain50,51,52. Synaptophysin expression decreases during aging, and although the postsynaptic protein PSD95 also is reduced during aging, it is retained longer at the synapse when age increases53,54,55. Moreover, in the prefrontal cortex, GABAergic activity increases with age while it lessens over time in other areas of the brain56,57,58,59. Thus, our finding that cisplatin induces a decrease in synaptophysin and an increase in vGAT without changes in PSD95 is consistent with the hypothesis that cisplatin treatment leads to accelerated aging of the brain. Further studies are needed to gain more insight into the effect of cisplatin and other chemotherapeutics on brain aging.
It remains to be determined via which mechanism cisplatin induces long-lasting changes in presynaptic and postsynaptic markers and how nasally administered MSCs exert their beneficial effects on performance in the 5-CSRTT and the associated deficits in expression of markers of synaptic integrity. We hypothesize that these long-lasting changes in synaptic integrity are the result of mitochondrial deficiencies, as has also been described for other neurodegenerative disorders60,61. This hypothesis is supported by our recent findings showing that cisplatin induces morphological abnormalities in synaptosomal mitochondria that are associated with functional mitochondrial deficits21 (and Chiu et al.23). We also presented evidence for a causal relationship between cisplatin-induced synaptosomal mitochondrial damage and cognitive impairment. Specifically, coadministration of the mitochondrial protectant pifithrin-μ prevented both mitochondrial abnormalities and cognitive deficits21. Moreover, the beneficial effect of MSC treatment on cognitive function in mice treated with cisplatin followed by MSCs at the age of 2‒3 months was associated with normalization of synaptosomal mitochondrial function (Chiu et al.23). RNAseq analysis of the effect of MSCs on gene expression in the hippocampi of mice treated with cisplatin revealed increased expression of genes involved in mitochondrial function and oxidative phosphorylation. These previous studies were performed in mice that were much younger than those in the current study (8‒10 weeks versus 7‒8 months) at the time of exposure to cisplatin. It remains to be determined whether the beneficial effects of MSCs that we detected in the present study are also mediated by restoration of mitochondrial function.
Conclusions
Deficits in attention, focus, and concentration are frequently reported by patients with cancer who are treated with chemotherapy. In addition, objective tests of cognitive function in patients with chemobrain confirm the presence of attention deficits or concentration problems2,3,4,5,6,7,13,14,15,16,17,18. A recent imaging study in patients treated with cisplatin identified structural and functional alterations in the frontal and parietal regions of the cortex in patients treated for ovarian cancer with first-line taxane/platinum chemotherapy62. Here, we show that mice treated with cisplatin develop abnormalities in markers of synaptic integrity in the prefrontal cortex and deficits in attention, providing support for the clinical relevance of our model. Our findings that nasal application of MSCs after completion of cisplatin treatment normalizes both the deficits in attention as well as the abnormalities in synaptic integrity warrant further investigation and, potentially, clinical translation.
Data Availability
The data that support the findings of this study are available from the corresponding author upon reasonable request.
References
American Cancer Society. Cancer Treatment & Survivorship Facts & Figures 2016-2017, https://www.cancer.org/content/dam/cancer-org/research/cancer-facts-and-statistics/cancer-treatment-and-survivorship-facts-and-figures/cancer-treatment-and-survivorship-facts-and-figures-2016-2017.pdf (2016).
Ahles, T. A. & Saykin, A. J. Candidate mechanisms for chemotherapy-induced cognitive changes. Nature reviews. Cancer 7, 192–201, https://doi.org/10.1038/nrc2073 (2007).
O’Farrell, E., MacKenzie, J. & Collins, B. Clearing the air: a review of our current understanding of “chemo fog”. Current oncology reports 15, 260–269, https://doi.org/10.1007/s11912-013-0307-7 (2013).
Wefel, J. S. & Schagen, S. B. Chemotherapy-related cognitive dysfunction. Current neurology and neuroscience reports 12, 267–275, https://doi.org/10.1007/s11910-012-0264-9 (2012).
Selamat, M. H., Loh, S. Y., Mackenzie, L. & Vardy, J. Chemobrain experienced by breast cancer survivors: a meta-ethnography study investigating research and care implications. PloS one 9, e108002, https://doi.org/10.1371/journal.pone.0108002 (2014).
Moore, H. C. An Overview of Chemotherapy-Related Cognitive Dysfunction, or ‘Chemobrain’. Oncology (Williston Park) 28 (2014).
Vardy, J. & Tannock, I. Cognitive function after chemotherapy in adults with solid tumours. Critical reviews in oncology/hematology 63, 183–202, https://doi.org/10.1016/j.critrevonc.2007.06.001 (2007).
Simo, M., Rifa-Ros, X., Rodriguez-Fornells, A. & Bruna, J. Chemobrain: a systematic review of structural and functional neuroimaging studies. Neuroscience and biobehavioral reviews 37, 1311–1321, https://doi.org/10.1016/j.neubiorev.2013.04.015 (2013).
Simó, M. et al. Cognitive and Brain Structural Changes in Lung Cancer Population. Journal of thoracic oncology: official publication of the International Association for the Study of Lung Cancer, https://doi.org/10.1097/JTO.0000000000000345 (2014).
Lepage, C. et al. A prospective study of grey matter and cognitive function alterations in chemotherapy-treated breast cancer patients. SpringerPlus 3, 444, https://doi.org/10.1186/2193-1801-3-444 (2014).
Janelsins, M. C., Kesler, S. R., Ahles, T. A. & Morrow, G. R. Prevalence, mechanisms, and management of cancer-related cognitive impairment. Int. Rev. Psychiatry 26, 102–113, https://doi.org/10.3109/09540261.2013.864260 (2014).
Cheng, H. et al. Altered resting-state hippocampal functional networks associated with chemotherapy-induced prospective memory impairment in breast cancer survivors. Scientific reports 7, 45135, https://doi.org/10.1038/srep45135 (2017).
Whitney, K. A. et al. Is “chemobrain” a transient state? A prospective pilot study among persons with non-small cell lung cancer. The journal of supportive oncology 6, 313–321 (2008).
Gan, H. K. et al. Cognitive functioning after radiotherapy or chemoradiotherapy for head-and-neck cancer. International journal of radiation oncology, biology, physics 81, 126–134, https://doi.org/10.1016/j.ijrobp.2010.05.004 (2011).
Fung, C. & Vaughn, D. J. Complications associated with chemotherapy in testicular cancer management. Nat Rev Urol 8, 213–222, https://doi.org/10.1038/nrurol.2011.26 (2011).
Schagen, S. B. et al. Cognitive complaints and cognitive impairment following BEP chemotherapy in patients with testicular cancer. Acta Oncol 47, 63–70, https://doi.org/10.1080/02841860701518058 (2008).
Skoogh, J. et al. Testicular-cancer survivors experience compromised language following chemotherapy: findings in a Swedish population-based study 3–26 years after treatment. Acta Oncol 51, 185–197, https://doi.org/10.3109/0284186X.2011.602113 (2012).
Yang, J. C. et al. Symptom control and quality of life in LUX-Lung 3: a phase III study of afatinib or cisplatin/pemetrexed in patients with advanced lung adenocarcinoma with EGFR mutations. Journal of clinical oncology: official journal of the American Society of Clinical Oncology 31, 3342–3350, https://doi.org/10.1200/JCO.2012.46.1764 (2013).
Lomeli, N., Di, K., Czerniawski, J., Guzowski, J. F. & Bota, D. A. Cisplatin-induced mitochondrial dysfunction is associated with impaired cognitive function in rats. Free Radic Biol Med 102, 274–286, https://doi.org/10.1016/j.freeradbiomed.2016.11.046 (2017).
Mu, L. et al. Impairment of cognitive function by chemotherapy: association with the disruption of phase-locking and synchronization in anterior cingulate cortex. Mol Brain 8, 32, https://doi.org/10.1186/s13041-015-0125-y (2015).
Chiu, G. S. et al. Pifithrin-mu Prevents Cisplatin-Induced Chemobrain by Preserving Neuronal Mitochondrial Function. Cancer research 77, 742–752, https://doi.org/10.1158/0008-5472.CAN-16-1817 (2017).
Zhou, W., Kavelaars, A. & Heijnen, C. J. Metformin prevents cisplatin-induced cognitive impairment and brain damage in mice. PloS one 11, e0151890, https://doi.org/10.1371/journal.pone.0151890.eCollection2016 (2015).
Chiu, G. S. et al. Nasal administration of mesenchymal stem cells restores cisplatin-induced cognitive impairment and brain damage in mice. Oncotarget 9, 35581–35597, http://www.oncotarget.com/index.php?journal=oncotarget&page=article&op=view&path%5B%5D=26272 (2018).
Robbins, T. W. The 5-choice serial reaction time task: behavioural pharmacology and functional neurochemistry. Psychopharmacology (Berl) 163, 362–380, https://doi.org/10.1007/s00213-002-1154-7 (2002).
Asinof, S. K. & Paine, T. A. The 5-choice serial reaction time task: a task of attention and impulse control for rodents. J Vis Exp, e51574, https://doi.org/10.3791/51574 (2014).
Dalley, J. W., Cardinal, R. N. & Robbins, T. W. Prefrontal executive and cognitive functions in rodents: neural and neurochemical substrates. Neurosci. Biobehav. Rev. 28, 771–784, https://doi.org/10.1016/j.neubiorev.2004.09.006 (2004).
Bari, A. & Robbins, T. W. Inhibition and impulsivity: behavioral and neural basis of response control. Prog Neurobiol 108, 44–79, https://doi.org/10.1016/j.pneurobio.2013.06.005 (2013).
Young, J. W., Light, G. A., Marston, H. M., Sharp, R. & Geyer, M. A. The 5-choice continuous performance test: evidence for a translational test of vigilance for mice. PloS one 4, e4227, https://doi.org/10.1371/journal.pone.0004227 (2009).
Donega, V. et al. Intranasal mesenchymal stem cell treatment for neonatal brain damage: long-term cognitive and sensorimotor improvement. PloS one 8, e51253, https://doi.org/10.1371/journal.pone.0051253 (2013).
Donega, V. et al. Intranasally administered mesenchymal stem cells promote a regenerative niche for repair of neonatal ischemic brain injury. Exp. Neurol. 261, 53–64, https://doi.org/10.1016/j.expneurol.2014.06.009 (2014).
Donega, V. et al. Assessment of long-term safety and efficacy of intranasal mesenchymal stem cell treatment for neonatal brain injury in the mouse. Pediatric research, https://doi.org/10.1038/pr.2015.145 (2015).
van Velthoven, C. T., Kavelaars, A., van Bel, F. & Heijnen, C. J. Nasal administration of stem cells: a promising novel route to treat neonatal ischemic brain damage. Pediatric research 68, 419–422, https://doi.org/10.1203/00006450-201011001-00834 (2010).
Nijboer, C. H. et al. Intranasal Stem Cell Treatment as a Novel Therapy for Subarachnoid Hemorrhage. Stem cells and development 27, 313–325, https://doi.org/10.1089/scd.2017.0148 (2018).
Risbrough, V., Bontempi, B. & Menzaghi, F. Selective immunolesioning of the basal forebrain cholinergic neurons in rats: effect on attention using the 5-choice serial reaction time task. Psychopharmacology (Berl) 164, 71–81, https://doi.org/10.1007/s00213-002-1170-7 (2002).
de Bruin, N. M., Fransen, F., Duytschaever, H., Grantham, C. & Megens, A. A. Attentional performance of (C57BL/6Jx129Sv)F2 mice in the five-choice serial reaction time task. Physiol Behav 89, 692–703, https://doi.org/10.1016/j.physbeh.2006.08.009 (2006).
Greco, B. & Carli, M. Reduced attention and increased impulsivity in mice lacking NPY Y2 receptors: relation to anxiolytic-like phenotype. Behavioural brain research 169, 325–334, https://doi.org/10.1016/j.bbr.2006.02.002 (2006).
Humby, T., Laird, F. M., Davies, W. & Wilkinson, L. S. Visuospatial attentional functioning in mice: interactions between cholinergic manipulations and genotype. The European journal of neuroscience 11, 2813–2823 (1999).
Marston, H. M., Spratt, C. & Kelly, J. S. Phenotyping complex behaviours: assessment of circadian control and 5-choice serial reaction learning in the mouse. Behavioural brain research 125, 189–193 (2001).
Rossi, A. F., Pessoa, L., Desimone, R. & Ungerleider, L. G. The prefrontal cortex and the executive control of attention. Exp. Brain Res. 192, 489–497, https://doi.org/10.1007/s00221-008-1642-z (2009).
Pezze, M., McGarrity, S., Mason, R., Fone, K. C. & Bast, T. Too little and too much: hypoactivation and disinhibition of medial prefrontal cortex cause attentional deficits. J. Neurosci. 34, 7931–7946, https://doi.org/10.1523/JNEUROSCI.3450-13.2014 (2014).
Krukowski, K., Nijboer, C. H., Huo, X., Kavelaars, A. & Heijnen, C. J. Prevention of chemotherapy-induced peripheral neuropathy by the small-molecule inhibitor pifithrin-mu. Pain 156, 2184–2192, https://doi.org/10.1097/j.pain.0000000000000290 (2015).
Krukowski, K. et al. HDAC6 inhibition effectively reverses chemotherapy-induced peripheral neuropathy. Pain 158, 1126–1137, https://doi.org/10.1097/j.pain.0000000000000893 (2017).
Maj, M. A., Ma, J., Krukowski, K. N., Kavelaars, A. & Heijnen, C. J. Inhibition of Mitochondrial p53 Accumulation by PFT-mu Prevents Cisplatin-Induced Peripheral Neuropathy. Front Mol Neurosci 10, 108, https://doi.org/10.3389/fnmol.2017.00108 (2017).
Bittar, A. et al. Reactive oxygen species affect spinal cell type-specific synaptic plasticity in a model of neuropathic pain. Pain 158, 2137–2146, https://doi.org/10.1097/j.pain.0000000000001014 (2017).
Zeitler, A. et al. Favouring inhibitory synaptic drive mediated by GABA(A) receptors in the basolateral nucleus of the amygdala efficiently reduces pain symptoms in neuropathic mice. The European journal of neuroscience 43, 1082–1088, https://doi.org/10.1111/ejn.13217 (2016).
Chen, J. et al. The alpha2delta-1-NMDA Receptor Complex Is Critically Involved in Neuropathic Pain Development and Gabapentin Therapeutic Actions. Cell Rep 22, 2307–2321, https://doi.org/10.1016/j.celrep.2018.02.021 (2018).
Xie, J. D., Chen, S. R. & Pan, H. L. Presynaptic mGluR5 receptor controls glutamatergic input through protein kinase C-NMDA receptors in paclitaxel-induced neuropathic pain. The Journal of biological chemistry 292, 20644–20654, https://doi.org/10.1074/jbc.M117.818476 (2017).
Xie, J. D., Chen, S. R., Chen, H. & Pan, H. L. Bortezomib induces neuropathic pain through protein kinase C-mediated activation of presynaptic NMDA receptors in the spinal cord. Neuropharmacology 123, 477–487, https://doi.org/10.1016/j.neuropharm.2017.06.027 (2017).
Watson, C. J. Insular balance of glutamatergic and GABAergic signaling modulates pain processing. Pain 157, 2194–2207, https://doi.org/10.1097/j.pain.0000000000000615 (2016).
Kesler, S. R., Rao, V., Ray, W. J. & Rao, A. & Alzheimer’s Disease Neuroimaging, I. Probability of Alzheimer’s disease in breast cancer survivors based on gray-matter structural network efficiency. Alzheimers Dement (Amst) 9, 67–75, https://doi.org/10.1016/j.dadm.2017.10.002 (2017).
Ahles, T. A. et al. Longitudinal assessment of cognitive changes associated with adjuvant treatment for breast cancer: impact of age and cognitive reserve. J. Clin. Oncol. 28, 4434–4440, https://doi.org/10.1200/JCO.2009.27.0827 (2010).
Koppelmans, V., Breteler, M. M., Boogerd, W., Seynaeve, C. & Schagen, S. B. Late effects of adjuvant chemotherapy for adult onset non-CNS cancer; cognitive impairment, brain structure and risk of dementia. Crit. Rev. Oncol. Hematol. 88, 87–101, https://doi.org/10.1016/j.critrevonc.2013.04.002 (2013).
Ojo, B. et al. Age-related changes in the hippocampus (loss of synaptophysin and glial-synaptic interaction) are modified by systemic treatment with an NCAM-derived peptide, FGL. Brain. Behav. Immun. 26, 778–788, https://doi.org/10.1016/j.bbi.2011.09.013 (2012).
Adams, M. M. et al. Caloric restriction and age affect synaptic proteins in hippocampal CA3 and spatial learning ability. Exp. Neurol. 211, 141–149, https://doi.org/10.1016/j.expneurol.2008.01.016 (2008).
Head, E. et al. Synaptic proteins, neuropathology and cognitive status in the oldest-old. Neurobiol Aging 30, 1125–1134, https://doi.org/10.1016/j.neurobiolaging.2007.10.001 (2009).
Rozycka, A. & Liguz-Lecznar, M. The space where aging acts: focus on the GABAergic synapse. Aging Cell 16, 634–643, https://doi.org/10.1111/acel.12605 (2017).
Potier, B., Jouvenceau, A., Epelbaum, J. & Dutar, P. Age-related alterations of GABAergic input to CA1 pyramidal neurons and its control by nicotinic acetylcholine receptors in rat hippocampus. Neuroscience 142, 187–201, https://doi.org/10.1016/j.neuroscience.2006.06.040 (2006).
Stanley, D. P. & Shetty, A. K. Aging in the rat hippocampus is associated with widespread reductions in the number of glutamate decarboxylase-67 positive interneurons but not interneuron degeneration. J. Neurochem. 89, 204–216, https://doi.org/10.1111/j.1471-4159.2004.02318.x (2004).
Bories, C., Husson, Z., Guitton, M. J. & De Koninck, Y. Differential balance of prefrontal synaptic activity in successful versus unsuccessful cognitive aging. J. Neurosci. 33, 1344–1356, https://doi.org/10.1523/JNEUROSCI.3258-12.2013 (2013).
Bose, A. & Beal, M. F. Mitochondrial dysfunction in Parkinson’s disease. Journal of neurochemistry 139(Suppl 1), 216–231, https://doi.org/10.1111/jnc.13731 (2016).
Gao, J. et al. Abnormalities of Mitochondrial Dynamics in Neurodegenerative Diseases. Antioxidants (Basel) 6, https://doi.org/10.3390/antiox6020025 (2017).
Correa, D. D. et al. Brain structure and function in patients with ovarian cancer treated with first-line chemotherapy: a pilot study. Brain Imaging Behav 11, 1652–1663, https://doi.org/10.1007/s11682-016-9608-4 (2017).
Acknowledgements
The authors gratefully acknowledge Jeanie F. Woodruff, BS, ELS, Department of Symptom Research at The University of Texas MD Anderson Cancer Center, Houston, Texas for scientific editing and Nabila Boukelmoune, Neuroimmunology Laboratory, Department of Symptom Research, for culturing the mesenchymal stem cells. This work was supported by the Dr. Marnie Rose Foundation and by the National Institutes of Health [grant numbers R01 CA308271, and RO1CA227064 Principal Investigators: CJH and AK]. The funding sources played no role in the design of the study; in the collection, analysis and interpretation of data; in the writing of the report; or in the decision to submit the article for publication.
Author information
Authors and Affiliations
Contributions
XJ.H. performed the experiments and analysed the data; XJ.H., T.M.R., C.J.H. and A.K. designed the studies and interpreted the data. All authors contributed to writing and editing of the manuscript.
Corresponding author
Ethics declarations
Competing Interests
The authors declare no competing interests.
Additional information
Publisher’s note: Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made. The images or other third party material in this article are included in the article’s Creative Commons license, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons license and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this license, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Huo, X., Reyes, T.M., Heijnen, C.J. et al. Cisplatin treatment induces attention deficits and impairs synaptic integrity in the prefrontal cortex in mice. Sci Rep 8, 17400 (2018). https://doi.org/10.1038/s41598-018-35919-x
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41598-018-35919-x
Keywords
This article is cited by
-
Four decades of chemotherapy-induced cognitive dysfunction: comprehensive review of clinical, animal and in vitro studies, and insights of key initiating events
Archives of Toxicology (2022)
-
Animal models of chemotherapy-induced cognitive decline in preclinical drug development
Psychopharmacology (2021)
-
Mitochondrial transfer from mesenchymal stem cells to neural stem cells protects against the neurotoxic effects of cisplatin
Acta Neuropathologica Communications (2018)
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.