Abstract
Active matrix Gla protein (MGP), a potent inhibitor of calcification in large arteries, protects against macrovascular complications. Recent studies suggested that active MGP helps maintaining the integrity of the renal and myocardial microcirculation, but its role in preserving the retinal microcirculation remains unknown. In 935 randomly recruited Flemish participants (mean age, 40.9 years; 50.3% women), we measured plasma desphospho-uncarboxylated MGP (dp–ucMGP), a marker of poor vitamin K status using an ELISA-based assay at baseline (1996–2010) and retinal microvascular diameters using IVAN software (Vasculomatic ala Nicola, version 1.1) including the central retinal arteriolar (CRAE) and venular (CRVE) equivalent and the arteriole-to-venule ratio (AVR) at follow-up (2008–2015). CRAE (P = 0.005) and AVR (P = 0.080) at follow-up decreased across tertiles of the dp–ucMGP distribution. In unadjusted models, for a doubling of dp–ucMGP at baseline, CRAE and AVR at follow-up respectively decreased by 1.40 µm (95% confidence interval [CI], 0.32 to 2.48; P = 0.011) and 0.006 (CI, 0.001 to 0.011; P = 0.016). In multivariable-adjusted models accounting for sex, baseline characteristics and follow-up duration, these estimates were −1.03 µm (CI, −1.96 to −0.11; P = 0.028) and −0.007 (CI, −0.011 to −0.002; P = 0.007). Additional adjustment for changes from baseline to follow-up in major baseline characteristics yielded as estimates −0.91 µm (CI, −1.82 to −0.01; P = 0.048) and −0.006 (95% CI, −0.011 to −0.001; P = 0.014), respectively. Circulating inactive dp–ucMGP is a long-term predictor of smaller retinal arteriolar diameter in the general population. Our observations highlight the possibility that vitamin K supplementation might promote retinal health.
Similar content being viewed by others
Introduction
Non-mydriatic retinal photography allows non-invasive visualisation of the retinal microvasculature in population surveys1,2,3,4. Numerous studies demonstrated that the diameters of the retinal microvessels carry important prognostic information5,6,7, smaller arteriolar diameter6,7, wider venular calibre7, and lower arteriolar-to-venular diameter ratio5 predicting cardiovascular mortality6, coronary heart disease5 and lacunar stroke7.
Matrix Gla protein (MGP) is a 11-kD protein synthesised by vascular smooth muscle and endothelial cells8. Activation of MGP requires two posttranslational modifications: vitamin-K dependent γ-glutamate carboxylation and serine phosphorylation8. Inactive desphospho-uncarboxylated MGP (dp-ucMGP) is a marker of poor vitamin K status9,10. Once activated, MGP is a potent locally acting inhibitor of calcification in large arteries8 and protects against macrovascular complications11 and arterial stiffening10,12. MGP is expressed in renal13,14 and myocardial microvessels15, where the activated protein contributes to maintaining organ function. Similarly, MGP is abundantly expressed in the eye16,17,18,19, where it takes part in preserving the structural integrity of the trabecular meshwork (TM)16,17, the sclera18 and the retinal ganglion cells19. A naturally fluorescent MGP transgenic mouse model also demonstrated MGP expression in the retinal vasculature20. In view of these observations13,14,15,16,17,18,19,20, we hypothesised that retinal microvascular traits, as exemplified by retinal arteriolar and venular diameters, might be associated with inactive dp-ucMGP. We assessed in the Flemish Study on Environment, Genes, and Health Outcomes (FLEMENGHO)11,14 whether circulating inactive dp-ucMGP predicted retinal microvascular diameters 11 years after the measurement of the biomarker.
Results
Characteristics of participants
All 935 participats were White Europeans, of whom 470 (50.3%) were female. The study population consisted of 138 singletons and 797 related subjects, belonging to 164 one-generation families and to 101 multi-generation pedigrees. In all participants, mean baseline values (SD) were 40.9 (14.6) years for age, 122.6 (14.9) mm Hg and 76.4 (11.0) mm Hg for systolic and diastolic blood pressure, and 25.1 (4.3) kg/m2 for body mass index. At baseline, 108 participants were on antihypertensive drug treatment, of whom 41 (4.4%) were taking diuretics, 87 (9.3%) inhibitors of the renin-angiotensin system, and 15 (1.6%) vasodilators. At baseline, the geometric mean of dp-ucMGP was 3.45 μg/L and the interquartile range encompassed 2.50 μg/L and 5.16 μg/L. The median interval between baseline and follow-up was 11.0 years (interquartile range, 9.0–13.3 years). In all participants, central retinal arteriolar (CRAE) and venular (CRVE) equivalent and arteriole-to-venule ratio (AVR) at follow-up averaged 150.6 (14.0) µm, 218.3 (19.0) µm and 0.69 (0.06), respectively. Furthermore, the prevalence of glaucoma was about 1% in participants over 40 years old. There were no statistically significant differences in plasma levels of dp-ucMGP and retinal vascular diameters between the five patients with glaucoma and the 518 participants aged 40 years or above without glaucoma (P ≥ 0.41).
Unadjusted analyses
Across tertiles of the baseline dp-ucMGP (Table 1), age, body mass index, blood pressure, total cholesterol and the frequency of hypertension increased (P ≤ 0.006), but high-density lipoprotein (HDL) cholesterol and the prevalence of smoking decreased (P ≤ 0.037). Table 2 lists the retinal microvascular traits of participants by tertiles of the distribution of dp-ucMGP. CRAE (P = 0.005) and AVR (P = 0.080) decreased with higher category of dp-ucMGP. Figure 1 demonstrates that in unadjusted analyses dp-ucMGP increased (P < 0.001) across fifths of the distributions of baseline age, whereas CRAE, CRVE and AVR decreased (P ≤ 0.022).
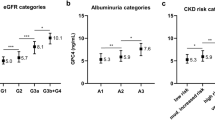
Central retinal arteriolar (CRAE, A) and venular (CRVE, B) equivalent and arteriole-to-venule ratio (AVR, C) at follow-up and baseline inactive desphospho-uncarboxylated matrix Gla protein (dp-ucMGP, D) by quintiles of the distribution of baseline age. Vertical bars indicate standard errors. P-values are for linear trend across the quintiles of baseline age.
Association with retinal microcirculation
While accounting for clustering within families (Table 3), a doubling of dp-ucMGP was associated with a 1.40 µm (95% confidence interval [CI], 0.32 to 2.48; P = 0.011) smaller CRAE. With adjustments applied for sex and age, the association size was −0.94 µm (CI, −1.84 to −0.05; P = 0.040). In a model additionally adjusted for baseline body mass index, diastolic blood pressure, serum total cholesterol and HDL cholesterol, diabetes mellitus, smoking and drinking and use of antihypertensive drugs (by class), history of cardiovascular disease and duration of follow-up and CRVE (Fig. 2 and Table 3), this estimate was −1.03 µm (CI, −1.96 to −0.11; P = 0.028). In sensitivity analyses, we additionally accounted for changes from baseline to follow-up in body mass index, diastolic blood pressure, serum total and HDL cholesterol, and we replaced baseline antihypertensive drug treatment by three indicator variables coding for starting, stopping, or continuing blood pressure lowering treatment. A doubling of dp-ucMGP was then associated with a 0.91 µm smaller CRAE (CI, 0.01 to 1.82; P = 0.048).
Multivariable-adjusted associations of central retinal arteriolar equivalent (CRAE) with circulating desphospho-uncarboxylated matrix Gla protein (dp-ucMGP) and age (A) and diastolic blood pressure (B). The plotted planes were standardised to the midpoints of the distributions (means or ratios) of sex, baseline covariables including body mass index, serum total and HDL cholesterol, diabetes mellitus, smoking and drinking, antihypertensive drug treatment (by drug class) and history of cardiovascular disease, follow-up duration and central retinal venular equivalent. The association in panel A was additionally standardised for diastolic blood pressure and in panel B for age.
While only accounting for clustering within families (Table 3), the association size between CRVE and dp-ucMGP was −0.13 µm (CI, −1.62 to 1.36; P = 0.86). With adjustments applied for sex and age, in a fully adjusted model and in the sensitivity analysis, the association sizes were 1.06 µm (CI, −0.21 to 2.32; P = 0.10), 1.83 µm (CI, 0.55 to 3.11; P = 0.005), and 1.68 µm (CI, 0.40 to 2.96; P = 0.010).
Associations with AVR mirrored those of CRAE (Table 3). A doubling of dp–ucMGP was associated with lower AVR (−0.006; CI, −0.010 to −0.001; P = 0.016) in models only accounting for clustering within families (Table 3). With adjustment for sex and age, in a fully adjusted model and in the sensitivity analysis, the association sizes were −0.005 (CI, −0.010 to −0.0002; P = 0.043), −0.007 (CI, −0.011 to −0.002; P = 0.007), and −0.006 (CI, −0.011 to −0.001; P = 0.014), respectively.
Discussion
To our knowledge, our study is the first longitudinal population survey assessing the association of retinal microvascular traits with circulating levels of dp-ucMGP measured approximately one decade before retinal photography. Our key finding was that even with multiple adjustments applied CRAE and AVR at follow-up were smaller with higher circulating levels of dp-ucMGP at baseline. Our findings are compatible with studies showing expression of MGP in capillaries and small arterioles15 and in particular in the glaucoma-relevant tissues of the eye and the retinal microvasculature16,17,18,19,20. Our findings underscore the pivotal role of activated MGP in maintaining ocular homeostasis and are in line with our previous report, which showed that high dp-ucMGP predicted adverse health outcomes, including total, non-cancer and cardiovascular mortality in 2318 FLEMENGHO participants followed up for a median of 14.1 years11.
A novel MGP transgenic mouse model allows visualising angiogenesis- and glaucoma-relevant tissues by natural fluorescence20. These mice have normal intra-ocular pressure. The entire retinal vasculature was red fluorescent (vascular smooth muscle cells) and the fluorescence extended into the capillary bed20. The retinal and myocardial microvasculature shared an anatomical and physiological homology21. Previously, we demonstrated that in normal and diseased human hearts carboxylated and phosphorylated MGP localises in the media and intima of muscular left ventricular microvessels15. Paulus and colleagues proposed a novel paradigm implicating the microcirculation in the pathogenesis of diastolic left ventricular dysfunction22. We confirmed the role of activated MGP in maintaining myocardial integrity and diastolic left ventricular performance15. Our current observations might therefore reflect a generalised vascular condition not only affecting the microcirculation in the eye, the kidney13,14 and the heart15, but the central elastic arteries as well12,23,24.
The TM located in the anterior chamber of the eye is a tiny porous structure composed of connective tissue beams and trabeculae covered by TM cells. The intratrabecular spaces of the TM allow passage of aqueous humour to Schlemm’s canal, a circular endothelium-lined lymphatic-like vessel, located at the basis of the iris, which is connected to the episcleral venous drainage system through an array of around 35 collector channels25. The extracellular matrix of the TM contains numerous structural and organisational proteins, including collagens, laminins, elastin, fibronectin, fibrillins and matricellular proteins. MGP, which is abundantly expressed in the TM, takes part in preserving its structural integrity17,26. The TM represents the primary site of outflow resistance to aqueous humour. Adjustment of resistance in the TM is the main mechanism by which intra-ocular pressure is regulated27. Elevated intra-ocular pressure is the most important risk factor in the development and progression of glaucoma27. In mice, MGP is also abundantly expressed in glaucoma-relevant tissues17,20, including TM and sclera as well as in the retinal microvasculature20, where MGP exhibits anti-calcification and anti-stiffness properties.
In case-control studies patients with glaucoma compared with controls had a lower distensibility of the common carotid artery23 or higher aortic pulse wave velocity24. Furthermore, previous studies demonstrated association of glaucoma with retinal microvascular traits28,29,30, including generalised arteriolar narrowing28,29. Among 3314 participants enrolled in the Blue Mountains Eye Study28, 59 (1.8%) had glaucomatous optic nerve damage and 163 (4.9%) had ocular hypertension. Eyes with glaucomatous damage had significantly narrower (183 vs. 194 µm; P = 0.0001) CRAE than eyes without glaucoma28. Among 3019 Asians enrolled in the Singapore Malay Eye Study29, CRAE and CRVE were significantly narrower in 127 (4.2%) participants with glaucoma than in those without glaucoma (136.4 µm vs. 139.7 µm, P < 0.001 and 209.2 vs. 219.7 µm, P < 0.001, respectively).
Of potential relevance to our current study, is the strong well-documented protein-protein interaction between MGP and bone morphogenetic protein (BMP), including BMP231 and BMP432, whereby bound MGP reduces BMP signalling. BMPs belong to the transforming growth factor β (TGF-β) superfamily. Following signalling activation via BMP type-1 or type-2 receptors, phosphorylated receptor-regulated SMADs form heterodimeric complexes with the common mediator SMAD4 and translocate to the nucleus to regulate gene expression. In the heart, BMP pathways play a pivotal role in the embryogenesis of the left ventricular chamber33, the differentiation of cardiac progenitor cells into functional cardiomyocytes34, maintenance of the balance between left ventricular growth and apoptosis35, initiation of fibrosis35, and Ca2+ channel remodelling36. In analogy with the cardiac findings, previous studies demonstrated that BMP and TGF-β2 signalling pathways are also active in the eye26,37,38,39. Expression of BMP-4 and its receptors plays a pivotal role in the early embryogenesis of the eye37. Rat studies also demonstrated expression of BMP4 and its receptors in the adult eye, including the corneal microvascular endothelium38. TGF-β2 is associated with increased extracellular matrix deposition (fibronectin) in the TM, which leads to an increased resistance of aqueous humour outflow39. In this context39, the BMP and TGF-β2 signalling pathways antagonise each other’s antifibrotic and profibrotic actions. Less activated MGP might also be involved, via increased BMP signalling, in higher arteriolar stiffness and smaller CRAE in the eye.
Several of our observations are in line with the literature and support the validity of our findings40. For instance, in the baseline data from the Inter99 Eye Study, CRAE was 0.2 µm smaller for each unit increase in age or systolic blood pressure and 4.0 µm larger in smokers compared with non-smokers40. The corresponding estimates in our current study were: −0.2 µm, −0.2 µm and +3.5 µm, respectively. On the other hand, our current study must also be interpreted within the context of its potential limitations. First, we did not take retinal photographs at baseline, so that we could not assess whether MGP is a modulator of retinal arteriolar narrowing in relation to age, blood pressure, body mass index or other risk factors. Second, an observational study cannot assess causality. However, our study satisfies the Bradford-Hill criteria of temporality (a baseline marker predicting a trait of interest), plausibility and coherence (between clinical and experimental observations). Nevertheless, further experimental and clinical studies are required to substantiate our current observations. MGP staining studies using conformation-specific MGP antibodies15 to identify the exact localisation of MGP in the human TM and the retinal microvasculature is one possible approach. Third, in view of the prevalence of glaucoma in European populations estimated to run at a rate of approximately 3%41 and our limited sample size, we could not ascertain the association of symptomatic glaucoma with arteriolar retinal narrowing or circulating dp-ucMGP. Fourth, we did not measure circulating levels of vitamin K, which is rarely done in research or clinical practice, because of the complexity of the assay and the lack of a high-throughput method42 and because plasma levels only reflect dietary intake (vitamin K1; phylloquinone) and production by the gut microflora (vitamin K2; menaquinones) without giving any indication of functionality, i.e. the amount of MGP undergoing carboxylation9. Finally, our current findings in white Flemish cannot be extrapolated to other ethnicities.
Notwithstanding potential limitations, our findings may have important clinical implications. High levels of plasma dp-ucMGP are a proxy for vitamin K deficiency9,10. Levels ranging from 1.4 to 4.6 μg/L are probably optimal in terms of the risk of mortality and macrovascular cardiovascular complications11. In Flemish, the 4.6 μg/L threshold corresponds with the 65th percentile of the dp-ucMGP distribution, indicating that nearly 35% of Flemish might be vitamin K deficient. Vitamin K supplementation reduced aortic pulse wave velocity in healthy postmenopausal women10. Assuming reversibility, our current findings extend the protective role of vitamin K to the retinal microcirculation and TM. Vitamin K has a very wide safety range. Sources are leafy vegetables (phylloquinone; vitamin K1), fermented foods (menaquinones; vitamin K2) or dietary supplements.
In the general population, CRAE and AVR at follow-up were smaller with higher levels of circulating inactive dp-ucMGP at baseline, a biomarker of vitamin K deficiency. Our study highlight the possibility that vitamin K supplementation might promote ocular health. Further studies should clarify the underlying molecular pathways and substantiate the speculation that vitamin K supplementation might promote ocular health and prevent glaucoma-induced optic nerve damage.
Methods
Study population
The Ethics Committee of the University of Leuven approved the FLEMENGHO protocol11. FLEMENGHO complies with the Helsinki declaration for research in humans43. At each contact, participants gave or renewed informed written consent. FLEMENGHO is a family-based population study, for which recruitment started in 198511,14. Of 3343 participants, 1285 underwent retinal photography (2008–2015). The participation rate was 78.0% at enrolment and 76.0% for retinal photography. In the context of this article, baseline refers to blood sampling for the measurement of dp-ucMGP (1996–2010) and follow-up to retinal imaging (2008–2015). We excluded participants from analysis if the retinal photographs were of too low quality to be reliably graded (n = 221) or if baseline plasma dp-ucMGP (n = 106) or biochemical (n = 7) measurements were missing. This left 951 participants with plasma dp-ucMGP measured at baseline, with gradable retinal photographs at follow-up, and with all covariables available at baseline and follow-up. Finally, we excluded participants from analysis, if they were taking warfarin (n = 1), or if retinal microvascular diameters (n = 8), plasma dp-ucMGP (n = 3) or blood pressure (n = 4) were more than 3 SDs away from the population mean. Thus, the number of participants statistically analysed totalled 935.
Retinal photography
Participants were asked to refrain from heavy exercise, smoking, drinking alcohol or caffeine-containing beverages for at least 3 hours prior to retinal imaging. We applied a non-mydriatic approach in a dimly lit room to acquire retinal photographs, one image per eye in each participant, with the Canon Cr-DGi retinal visualisation system combined with the Canon D 50 digital camera (Canon Inc, Medical Equipment Group, Utsunomiya, Japan). We measured the CRAE and CRVE equivalent, which represent the retinal arteriolar and venular diameter. We used the validated computer-assisted programme IVAN (Vasculomatic ala Nicola, version 1.1, Department of Ophthalmology and Visual Science, University of Wisconsin-Madison, Madison, WI) based on formulae published by Parr44 and Hubbard45. The IVAN software returns average vessel diameters according to the revised Knudtson formula46. The AVR was CRAE divided by CRVE. For analysis, we averaged each participant’s measurements at both eyes. Intra-observer variability according to the Bland and Altman method47 was 11.7% for CRAE, 9.6% for CRVE and 12.5% for AVR1. The corresponding estimates for interobserver variability were 10.8%, 9.9% and 14.6%, respectively1.
Baseline clinical and biochemical measurements
Blood pressure was the average of five consecutive auscultatory readings obtained with a standard mercury sphygmomanometer. Hypertension was a blood pressure of at least 140 mm Hg systolic or 90 mm Hg diastolic or use of antihypertensive drugs. The study nurses also administered questionnaires inquiring into each participant’s medical history, smoking and drinking habits, and intake of medications. At baseline and follow-up, fasting blood samples were analysed for plasma glucose, serum total and HDL cholesterol and serum creatinine, using automated methods in a single certified laboratory. dp-ucMGP was measured on citrated plasma by pre-commercial ELISA kits at VitaK (Maastricht University, The Netherlands)48. This dual-antibody MGP assay performed satisfactory with respect to intra-assay (5.6%) and inter-assay (9.9%) variation and the detection limit (0.22 μg/L)48. Diabetes mellitus was a fasting plasma glucose of 7.0 mmol/L (126 mg/dL) or higher or use of antidiabetic agents.
Statistical analyses
For database management and statistical analysis, we used SAS software, version 9.4 (SAS Institute Inc., Cary, NC). We compared means and proportions by the large-sample z-test or ANOVA and by the χ2-statistic, respectively. We normalised the distributions of dp-ucMGP by a logarithmic transformation. Statistical significance was a two-sided significance of 0.05.
In unadjusted and multivariable-adjusted analyses, we expressed association sizes between the retinal phenotypes at follow-up and baseline dp-ucMGP for a doubling of the biomarker. As in previous publications49,50, we adjusted for sex and the baseline covariables age, body mass index, diastolic blood pressure, serum total and HDL cholesterol, diabetes mellitus, smoking and drinking and antihypertensive drug treatment, broken down into diuretics (thiazides, loop diuretics and aldosterone antagonists), inhibitors of the renin-angiotensin system (β-blockers, angiotensin-converting enzyme inhibitors and angiotensin type-1 receptor blockers), vasodilators (calcium-channel blockers and α-blockers), history of cardiovascular disease and follow-up duration. In sensitivity analyses, we additionally accounted for changes in body mass index, diastolic blood pressure, serum total and HDL cholesterol, and three indicator variables coding for starting, stopping, or continuing antihypertensive drug treatment from baseline to follow-up. For CRAE, we additionally adjusted for CRVE. The final multivariable-adjusted analyses relied on mixed models as implemented in SAS 9.4, which accounted for family clusters modelled as a random effect and the other covariables modelled as fixed effects.
Data Availability Statement
The corresponding author will make anonymized data available to researchers who present an outstanding research plan that will move the field forward.
References
Liu, Y. P., Richart, T., Jin, Y., Struijker-Boudier, H. A. & Staessen, J. A. Retinal arteriolar and venular phenotypes in a Flemish population: Reproducibility and correlates. Artery Res 5, 72–79 (2011).
Cheung, C. Y., Ikram, M. K., Sabanayagam, C. & Wong, T. Y. Retinal microvasculature as a model to study the manifestations of hypertension. Hypertension 60, 1094–1103 (2012).
Wong, T. Y., Shankar, A., Klein, R., Klein, B. E. & Hubbard, L. D. Prospective cohort study of retinal vessel diameters and risk of hypertension. Br Med J. 329, 79 (2004).
Wong, T. Y. et al. Retinal arteriolar diameter and risk for hypertension. Ann Intern Med 140, 248–255 (2004).
Wong, T. Y. et al. Retinal ateriolar narrowing and risk of coronary heart disease in men and women. The Atherosclerosis Risk in Communities study. J Am Med Ass 287, 1153–1159 (2002).
Wong, T. Y. et al. Retinal microvascular abnormalities and 10-year cardiovascular mortality. A population-based case-control study. Ophthalmology 110, 933–940 (2003).
Yatsuya, H. et al. Retinal microvascular abnormalities and risk of lacunar stroke: Atherosclerosis Risk in Communities Study. Stroke 41, 1349–1355 (2010).
Schurgers, L. J., Cranenburg, E. C. M. & Vermeer, C. Matrix Gla-protein: the calcification inhibitor in need of vitamin K. Thromb Haemost 100, 593–603 (2008).
Dalmeijer, G. W. et al. The effect of menaquinone-7 supplementation on circulating species of matrix Gla protein. Atherosclerosis 225, 397–402 (2012).
Knapen, M. H. J. et al. Menaquinone-7 supplementation improves arterial stiffness in healthy postmenopausal women. Thromb Haemost 113, 1135–1144 (2015).
Liu, Y. P. et al. Inactive matrix gla protein is causally related to adverse health outcomes: a Mendelian randomization study in a Flemish population. Hypertension 65, 463–470 (2015).
Pivin, E. et al. Inactive matrix Gla-protein is associated with arterial stiffness in an adult population-based study. Hypertension 66, 85–92 (2015).
Wei, F. F. et al. Vitamin K dependent protection of renal function in multi-ethnic population studies. EBioMed 4, 162–169 (2016).
Wei, F. F. et al. Desphospho-uncarboxylated matrix Gla protein is a novel circulating biomarker predicting deterioration of renal function in the general population. Nephrol Dial Transplant 33, 1122–1128 (2018).
Wei, F. F. et al. Epidemiological and histological findings implicate matrix Gla protein in diastolic left ventricular dysfunction. PLoS One 13, e0193967 (2018).
Gonzales, P., Epstein, D. L. & Borrás, T. Characterization of gene expression in human trabecular meshwork using single-pass sequencing of 1060 clones. Invest Ophthalmol Vis Sci 41, 3678–3693 (2000).
Borrás, T., Smith, M. H. & Buie, L. K. A novel mgp-cre knock-in mouse reveals an anticalcification/antistiffness candidate gene in the trabecular meshwork and peripapillary scleral region. Invest Ophthalmol Vis Sci 56, 2203–2214 (2015).
Young, T. L. et al. Microarray analysis of gene expression in human donor sclera. Mol Vis 10, 163–176 (2004).
Göritz, C. et al. Glia-induced neuronal differentiation by transcriptional regulation. Glia. 55, 1108–1122 (2007).
Asokan, P., Mitra, R. N., Periasamy, R., Han, Z. & Borrás, T. A naturally fluorescent mgp transgenic mouse for angiogenesis and glaucoma longitudinal studies. Invest Ophthalmol Vis Sci 59, 746–756 (2018).
Tedeschi-Reiner, E., Strozzi, M., Skoric, B. & Reiner, Z. Relation of atherosclerotic changes in retinal arteries to the extent of coronary artery disease. Am J Cardiol 96, 1107–1109 (2005).
Paulus, W. J. & Tschöpe, C. A novel paradigm for heart failure with preserved ejection fraction. J Am Coll Cardiol 62, 263–271 (2013).
Visontai, Z., Mersich, B. & Holló, G. Carotid artery elasticity and baroreflex sensitivity in patients with glaucoma. J Glaucoma 14, 30–35 (2005).
Türkyilmaz, K., Oner, V., Ciçek, Y., Kurt, A. & Durmus, M. Systemic arterial stiffness in patients with pseudoexfoliation glaucoma. J Glaucoma 23, e108–e111 (2014).
Abu-Hassan, D. W., Acott, T. S. & Kelley, M. J. The trabecular meshwork: a basic review of form and function. J Ocul Biol 2, http://fulltextarticles.avensonline.org/JOCB-2334-2838-02-0017.html (2014).
Xue, W., Wallin, R., Olmsted-Davis, E. A. & Borrás, T. Matrix GLA protein function in human trabecular meshwork cells: inhibition of BMP2-induced calcification process. Invest Ophthalmol Vis Sci 47, 997–1007 (2006).
Vranka, J. A., Kelley, M. J., Acott, T. S. & Keller, K. E. Extracellular matrix in the trabecular meshwork: intraocular pressure regulation and dysregulation in glaucoma. Exp Eye Res 133, 112–125 (2015).
Mitchell, P. et al. Retinal vessel diameter and open-angle glaucoma: the Blue Mountains Eye Study. Ophthalmology 112, 245–250 (2005).
Amerasinghe, N. et al. Evidence of retinal vascular narrowing in glaucomatous eyes in an Asian population. Invest Ophthalmol Vis Sci 49, 5397–5402 (2008).
Chou, J. C. et al. Fundus densitometry findings suggest optic disc hemorrhages in primary open-angle glaucoma have an arterial origin. Am J Ophthalmol 187, 108–116 (2018).
Zebboudj, A. F., Imura, M. & Boström, K. Matrix GLA protein, a regulatory protein for bone morphogenetic protein-2. J Biol Chem 277, 4388–4394 (2002).
Yao, Y., Zebboudj, A. F., Shao, E., Perez, M. & Boström, K. Regulation of bone morphogenetic protein-4 by matrix GLA protein in vascular endothelial cells involves activin-like kinase receptor 1. J Biol Chem 281, 33921–33930 (2006).
Han, P. et al. Coordinating cardiomyocyte interactions to direct ventricular chamber morphogenesis. Nature 534, 700–704 (2016).
Cagavi, E. et al. Functional cardiomyocytes derived from Isl1 cardiac progenitors via BMP4 stimulation. PLoS One 9, e110752 (2014).
Sun, B. et al. Bone morphogenetic protein-4 mediates cardiac hypertrophy, apoptosis, and fibrosis in experimentally pathological cardiac hypertrophy. Hypertension 61, 352–360 (2013).
Hu, C. W. et al. Bone morphogenetic protein-4 induces upregulation of Cav3.1 Ca2+ channels in HL-1 atrial myocytes. Pflügers Arch - Eur J Physiol 466, 2049–2057 (2014).
Huang, J., Liu, Y., Filas, B., Gunhaga, L. & Beebe, D. C. Negative and positive auto-regulation of BMP expression in early eye development. Dev Biol 407, 256–264 (2015).
Maruyama-Koide, Y., Mikawa, S., Sasaki, T. & Sato, K. Bone morphogenetic protein-4 and bone morphogenetic protein receptors expressions in the adult rat eye. Eur J Histochem 61, 2797 (2017).
Tovar-Vidales, T., Fitzgerald, A. M. & Clark, A. F. Human trabecular meshwork cells express BMP antagonist mRNAs and proteins. Exp Eye Res 147, 156–160 (2016).
Drobnjak, D. et al. Retinal vessel diameters and their relationship with cardiovascular risk and all-cause mortality in the Inter99 Eye Study: a 15-year follow-up. J Ophtalmol 2016, 6138659 (2016).
Tham, Y. C. et al. Global prevalence of glaucoma and projections of glaucoma burden through 2040: a systematic review and meta-analysis. Ophthalmology 121, 2081–2090 (2014).
Riphagen, I. J. et al. Measurement of plasma vitamin K1 (phylloquinone) and K2 (menaquinones-4 and -7) using HPLC-tandem mass spectrometry. Clin Chem Lab Med. 54, 1201–1210 (2016).
World Medical Association. World Medical Association Declaration of Helsinki. Ethical principles for medical research involving human subjects. J Am Med Ass. 310, 2191–2194 (2013).
Parr, J. C. & Spears, G. F. General caliber of the retinal arteries expressed as the equivalent width of the central retinal artery. Am J Ophtalmol 77, 472–477 (1974).
Hubbard, L. D. et al. Methods for evaluation of retinal microvascular abnormalities associated with hypertension/sclerosis in the Atherosclerosis Risk in Communities Study. Ophtalmology 106, 2269–2280 (1999).
Knudtson, M. D. et al. Revised formulas for summarizing retinal vessel diameters. Curr Eye Res 27, 143–149 (2003).
Dewitte, K., Fierens, C., Stockl, D. & Thienpont, L. M. Application of the Bland-Altman plot for interpretation of method-comparison studies: a critical investigation of its practice. Clin Chem 48, 799–801 (2002).
Cranenburg, E. C. et al. Characterisation and potential diagnostic value of circulating matrix gla protein (MGP) species. Thromb Haemost 104, 811–822 (2010).
Gu, Y. M. et al. Renal glomerular dysfunction in relation to retinal arteriolar narrowing and high pulse pressure in seniors. Hypertens Res 39, 138–143 (2016).
Wei, F. F. et al. Conventional and ambulatory blood pressure as predictors of retinal arteriolar narrowing. Hypertension 68, 511–520 (2016).
Acknowledgements
The European Union (HEALTH-F7-305507-HOMAGE), the European Research Council (Advanced Researcher Grant 2011-294713-EPLORE and Proof-of-Concept Grant 713601-uPROPHET), the European Research Area Net for Cardiovascular Diseases (JTC2017-046-PROACT), and the Fonds voor Wetenschappelijk Onderzoek Vlaanderen, Ministry of the Flemish Community, Brussels, Belgium (G.0881.13 and 11Z0916N) currently support the Studies Coordinating Centre in Leuven. The authors gratefully acknowledge the clerical assistance of Vera De Leebeeck, Yvette Piccart, and Renilde Wolfs.
Author information
Authors and Affiliations
Contributions
J.A.S. conceived and coordinated the Flemish Study on Environment, Genes and Health Outcomes (FLEMENGHO). L.T. and J.A.S. constructed the FLEMENGHO database. F.-F.W., Z.-Y.Z., W.-Y.Y. and N.C. did field work in Flanders. T.K., K.A., P.V. and J.A.S. supervised the fieldwork. Q.-F.H., K.V.K., S.T., B.M., T.K., H.A.J.S.B. and P.V. advised on the interpretation of the microcirculatory and ophthalmological data. C.V. supervised the measurements of matrix Gla protein. F.-F.W. and J.A.S. wrote the first and last draft of the manuscript. All authors interpreted the results, commented on successive versions of the manuscript and approved the final version.
Corresponding author
Ethics declarations
Competing Interests
C.V. is an employee of the R&D Group VitaK. The other authors have not declared any conflicts of interest.
Additional information
Publisher's note: Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made. The images or other third party material in this article are included in the article’s Creative Commons license, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons license and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this license, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Wei, FF., Huang, QF., Zhang, ZY. et al. Inactive matrix Gla protein is a novel circulating biomarker predicting retinal arteriolar narrowing in humans. Sci Rep 8, 15088 (2018). https://doi.org/10.1038/s41598-018-33257-6
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41598-018-33257-6
Keywords
This article is cited by
-
Inactive matrix Gla protein in relation to diabetic retinopathy in type 2 diabetes
Journal of Diabetes & Metabolic Disorders (2023)
-
Generation of a Matrix Gla (Mgp) floxed mouse, followed by conditional knockout, uncovers a new Mgp function in the eye
Scientific Reports (2020)
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.