Abstract
Whether we should use carbon nanoparticle (CN) routinely in thyroid surgery is still controversial. 406 papillary thyroid cancer (PTC) patients who underwent total thyroidectomy (TT) with bilateral central lymph node dissection (CLND) from January 2010 to December 2012 were retrospectively analyzed. The incidence of transient hypoparathyroidism and hypocalcemia in CN group was significantly lower than the control group at second, fifth day after surgery (P = 0.004, 0.042, 0.002 and 0.045 respectively). However, no significant difference existed between the two groups about the permanent hypoparathyroidism and hypocalcemia (P = 1.000). Total number of central lymph nodes and metastatic lymph nodes in CN group were more than those in control group (P = 0.031 and 0.038 respectively). However, recurrence was not significantly different between the two groups after at least 5-year follow up (P = 0.7917). In the subgroup of prophylactic and therapeutic CLND study, no significant difference existed between the two groups (P = 0.5295 and 0.8459 respectively). CN significantly help in identifying the parathyroid glands in surgery and increased the number of lymph nodes in central compartment. However, we should not exaggerate the function of CN since it couldn’t improve the permanent hypoparathyroidism and recurrence in PTC patients who underwent TT with bilateral CLND.
Similar content being viewed by others
Introduction
Thyroid cancer is the most common endocrine malignancy. Among them, papillary thyroid carcinoma (PTC) is the most common subtype, accounting for more than 90% of all thyroid cancers. Usually, most patients with PTC obtain a 10-year survival rate of 80–90%, but the regional recurrence rate is up to 5–20%1. Central lymph node metastasis (CLNM) is proved to be an important factor influencing the tumor recurrence. As previously reported, the lymph node metastasis rate in PTC varies from 20% to 50%. Furthermore, nearly 50% of clinical-negative lymph node patients were diagnosed to be pathological-positive with micrometastases in lymph nodes2,3,4,5. Therefore, there is widely awareness that improving the central lymph node dissection (CLND) during operation can reduce the recurrence in PTC.
As a common and severe complication, the postoperative transient hypoparathyroidism incidence rate can be up to 37%6,7, which often caused by accidental resection of parathyroid glands or inadvertent injury to surrounding blood supply. Owing to negative impact on patients’ quality of life, it is particularly important to improve the identification of parathyroid glands and protect the blood supply during operation. Until now, no technique of distinguishing parathyroid glands such as methylene blue, parathyroid scintigraphy or frozen specimen biopsy has been considered as perfection.
Carbon nanoparticle (CN) is a novel lymph nodes tracer and has been widely used in the surgeries of breast cancer, stomach cancer and thyroid cancer8. During the surgery, the thyroid gland can be quickly black-stained after injecting the CN, but the anatomic color of the parathyroid will not change, which facilitates the surgeons to identify the parathyroid. Meanwhile, it can also stain the lymph nodes in the thyroid drainage area, which guides the surgeons to dissect the central lymph nodes.
In recent years, some studies suggested that CN could help to detect lymph nodes and increase the number of clinical apparent and microscopic metastatic lymph nodes9,10,11,12,13,14,15,16,17,18,19. Therefore, owing to its potential function of reflecting the metastatic condition and protecting parathyroid glands, the CN was recommended in thyroid surgery. However, Xu Liu et al. demonstrate CN is not beneficial for protecting the function of parathyroid gland in thyroid surgery from the perspective of declining intact parathyroid hormone (iPTH)20. Whether we should use CN routinely in thyroid surgery is still controversial. Moreover, the benefits of CN for recurrence of thyroid cancer are still unknown. Accordingly, we performed the retrospective study to clarify clinical benefits of CN in PTC patients with total thyroidectomy (TT) plus bilateral CLND.
Materials and Methods
Patients
406 patients with PTC were selected for this study. All selected patients underwent the total thyroidectomy (TT) with bilateral CLND (including prophylactic and therapeutic CLND). The operation was performed at the First Hospital of Jilin University from 2010 to 2012. The inclusion criteria were: (1) Patients underwent TT with bilateral CLND according to indications from America Thyroid Association (ATA) guideline in 2009; (2) Patients were diagnosed by fine needle aspiration (FNA) preoperatively; (3) Pathologically proven PTC; (4) Operations were completed by the same surgeon. The exclusion criteria were: (1) Reoperation; (2) Lateral lymph node metastasis (LLNM) and distant metastasis; (3) patients who have family history of thyroid cancer or head and neck were exposed to radiation; (4) non-PTC carcinomas (follicular/medullary/anaplastic); (5) Follow-up duration less than 6 months. During the study, CN was used on 106 patients. Meanwhile, 300 cases who did not use CN were selected as the control group. The study was approved by the First Hospital Ethics Committee of Jilin University. All of the experimental protocols and procedures were approved by the licensing committee and performed in accordance with the approved guidelines and regulations. The patients were informed that the clinical data would be used in the in this study, and informed consent was obtained from all of the subjects.
CN injection
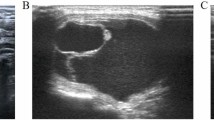
CN Suspension Injection (trade name: Kanalin) was designed by Chongqing LUMMY Pharmaceutical Co., Ltd. Specific processes (like organic solvent dissolution; magnetically stir, distillation and ultrasonic processing) changed aggregation of nanoscale carbon particles and formed polymer with 150 nm diameter. The gap between capillary lymphatic endothelial cells is 100–500 nm while that between the capillary endothelial cells is only 30–50 nm. Therefore, after being injected into the thyroid tissue, they will rapidly enter the lymphatic vessels, rather than vascular vessels, and then enter the lymphatic capillaries after having been engulfed by macrophages. Finally, they accumulated in the lymph nodes, resulting in the black-staining of the lymph nodes (Fig. 1). The CN suspension injection is mainly used for tracing the regional lymph node lesions. Usually after the exposure of the operative field, it can be injected at the amount of 25 mg with a 1 ml needle slowly and injected at the four to six points in the tumor periphery area. Each point of injection ranges from 5–15 mg and it takes about 3 minutes. Rare adverse effects are reported. Occasional fever occurred, which patients often could tolerate.
Surgical procedures for the CN group
The type of CN Suspension Injection we used is 0.5 ml containing 25 mg with batch number: GUOYAOZHUNZI H20073246. After cutting the neck middle line, the thyroid was revealed. Before both sides of the thyroid gland being separated and the capsule being damaged, CN was injected using a 1 mL syringe. Two to five spots were injected at the lesion site. Depending on the size of the thyroid gland, total amount of CN injection is 8 to 20 mg. Both sides of the lobes are injected with CN. And before being injected, CN was preheated to 37 degrees. The syringe with CN was inserted deeply and aspirated to ensure the CN would not be injected into the blood streams. After injection, gauze was applied over the site to avoid drug leakage. After five to ten minutes, TT and CLND can be continued. This study included cases with both therapeutic and prophylactic CLND. Therapeutic CLND was performed when suspicious lymph node was detected during preoperative or intraoperative examination. CLND was performed to remove of all nodes and fibro-fatty tissue extending laterally from the medial border of the common carotid artery to the midline of the trache and vertically from the hyoid bone to the thoracic inlet. All the thyroidectomy specimen and lymph node tissues were sent for pathological examination.
Date was recorded and evaluated for both groups
Both CN group and the control group were tested for the intact parathyroid hormone (iPTH), serum calcium level at second, fifth day, one month and six months after surgery. The number of lymph node was subject to the pathology postoperatively. Postoperative hypocalcemia and hypoparathyroidism, total number of central lymph nodes and metastatic lymph nodes were recorded and evaluated during the study.
Postoperative treatment and follow-up
Patients with CLNM were receiving radioactive iodine ablation (RAI) if their tumors were larger than 1 cm and the capsule was invaded. All patients were receiving endocrine repressive therapy from 2011. A period of 60 to 84 months followed-up was conducted for all patients. Neck ultrasound, computed tomography (CT) scan, thyroglobulin (Tg) level and radioiodine whole body scan were used to diagnosis of recurrence and distant metastasis; When recurrence was suspected, patients underwent FNA with or without measurement of washout Tg levels and/or a thyroid CT or a positron emission tomography/CT. In our study, recurrence was defined as the presence of tumor or metastatic lymph node at least 6 months after the initial surgery. Permanent hypoparathyroidism was diagnosed as the iPTH and calcium level in the peripheral blood were still lower than normal after six months since surgery.
Statistical analysis
SPSS version 22 software (SPSS Inc, Chicago, IL) was used for statistical analysis to identify differences between groups for specific variables. Data on categorical characteristics were expressed as absolute numbers. Continuous data were expressed as mean ± standard deviation (SD). The x2 test or Fisher’s exact test were used for categorical data, and t-tests or the Mann-Whitney test were used for continuous data. Survival curves were drawn by Kaplan-Meier method and statistically analyzed by the log-rank test. A p value < 0.05 was considered statistically significant.
Data availability
The datasets generated during and/or analyzed during the current study are available from the corresponding author on reasonable request.
Results
Characteristics of patients
The clinicopathological characteristics of patients enrolled in the study are summarized in Table 1. Among the selected 406 patients, eighty-six cases were males and 320 were females, with a male-to-female ratio of 1: 3.72. The ages of patients ranges from 18–75 years with an average age of 44.88 years. There was no significant difference about patients’ age, gender, tumor location, multifocality, extrathyroidal extension (ETE), presence with thyroid nodule, presence with lymphocytic thyroiditis, tumor diameter, preoperative iPTH, preoperative calcium, RAI and follow-up period between the two groups (Table 1).
iPTH and Calcium level after surgery
The incidence rate of hypoparathyroidism in CN group was significantly lower than that of the control group at day two, day five and one month after surgery (P = 0.002,0.045 and 0.033 respectively). However, a six-month follow-up showed no significant difference between the two groups about the postoperatively permanent hypoparathyroidism (P = 1.000) (Table 2).
The number of patients with hypocalcemia in CN group was significantly less than the control group at day two, day five after surgery (P = 0.004 and 0.042 respectively). However, the long-term follow-up found no significant difference of the incidence of permanent hypocalcemia (P = 0.327 and 1.000 respectively) (Table 2).
CLND
Total number of central lymph nodes and metastatic lymph nodes in CN group were more than those in control group (P = 0.031 and 0.038 respectively; Table 3; Figs 2 and 3). The lymph node metastatic rate was 59.44% and 52% respectively in the CN group and the control group (P = 0.187; Table 4).
Recurrence in the two groups
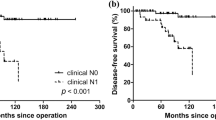
All patients were followed up from 60 to 84 months, there were 3 recurrent cases in the CN group and 8 cases in the control group. Disease-free survival curve was drawn by Kaplan-Meier method and statistically analyzed by the log-rank test to find that there was no significant difference between the two groups (P = 0.7917, Fig. 4). In the subgroup of prophylactic and therapeutic CLND study, we also found that no difference existed between the CN group and control group (P = 0.5295 and 0.8459 respectively, Figs 5 and 6).
Discussion
Total or near-total thyroidectomy plus central lymph node dissection was usually underwent for PTC. Parathyroid injury is the most common complication of TT which could induce hypoparathyroidism8. As studies reported, parathyroid injury rate has been reduced to some extent due to the awareness of the parathyroid protection and the operative skill. However, the postoperative parathyroid injury rate is still up to 0.3–49%6,7. In addition, the parathyroid blood was supplied by superior and inferior thyroid arteries, and the blood supply for parathyroid would be impaired by TT. Injury to parathyroid would lead to hypocalcemia, which is often caused by accidentally removing or destroying of the patients’ parathyroid glands or inadvertent destroying the glandular blood supply. Hypocalcemia could lead to many neuromuscular symptoms, such as sense of numbness or stiffness around face, mouth or foot; Serious symptoms would be muscle spasms and pain on hand, foot, or even suffocation caused by the serious spasm on throat and diaphragm. Therefore, protecting parathyroid and keeping its blood supply intact are always a main topic for TT21.
Recently, CN suspension injection has been used as an excellent tracer for lymph nodes in the gastric and gynecological tumors. Through the effect of the CN suspension, the surgeon would be able to identify the parathyroid, which can improve the protection of the parathyroid. In this study, we found that the incidence rate of hypoparathyroidism and hypocalcemia in CN group was significantly lower than that of the control group in a short period (P < 0.05). However, long-term follow-ups had found no significant difference between the two groups in the incidence of permanent hypoparathyroidism and hypocalcemia. The result of the CN suspension application in the thyroid surgery was consistent with the research result reported by Wang Bin et al.22. The plausible explanation is early detection of parathyroid using CN help surgeons to protect blood vessels of parathyroid, which leads to decreased rate of hypoparathyroidism and hypocalcemia at short-term follow up. At long-term (6 months), reconstruction of blood vessels for parathyroid can rescue its impaired function during surgery without CN. From the point of improving the iPTH and serum calcium level, the CN suspension has an important clinical value in protecting of parathyroid glands in the TT.
For PTC, neck regional recurrence rate after surgery is 5–20% and CLNM is an important source of recurrence2,3,4,5. Therefore, improving the thoroughness of neck lymph node dissection can reduce the rate of tumor recurrence4,5. Recurrence rate in high risk group was significantly higher than the low risk group (14% vs 34%), and the recurrence rate in lymph node metastasis is higher than those patients without metastasis23. Prophylactic CLND is still controversial in recent years. Studies have shown that there is no difference in the recurrence rate between the suspicious cervical lymph node metastasis in patients with unilateral CLND or bilateral CLND24,25,26. Some studies have also found that there is no difference in recurrence rate between the TT and TT + bilateral CLND in PTC patients, but the number of transient hypoparathyroidism was significantly increased in the CLND group27. However, prophylactic CLND is also traditional procedure for median to high-risk group of patients. Therefore, it is particularly important to dissect central lymph nodes thoroughly and reduce the hypoparathyroidism.
Consistent with the literature reported, the total number of lymph nodes and metastatic lymph nodes for TT in CN group was significantly more than those in the control group9,10,11,12,13,14,15,16,17,18,19. The difference was statistically significant, which indicated that CN can improve CLND without increasing the injury rate of parathyroid. As Table 3 shown in our study, CN can increase the total number and metastatic central lymph node at the same time. The total central lymph node metastasis rate was 54.25%, while the CN group was 59.44% and the control group was 49.01%. CN group is slightly higher, but the difference was not statistically significant, which indicated that CN suspension injection can improve the thoroughness of CLND. Moreover, by long-term follow up there was no significant difference between the two groups in disease-free survival. In the subgroup of prophylactic and therapeutic CLND study, we also found that no difference existed between the CN group and control group.
So far, few side effects related to CN suspension injection had been reported. During the surgery, drug staining in the exterior of thyroid tissue can affect observation in the surgical field and increase the difficulty to identify the laryngeal nerve. It can also stain the skin if medication was not carefully administered during surgery. But the risk could be avoided if the operation standards were strictly followed.
Our study is retrospective, which means the evidence we provided may not as powerful as a multi-centric pragmatic randomized controlled clinical trial with large population. Moreover, TSH suppressive hormonal therapy was applied to postoperative patients after 2011. Because at that time, there was no guideline which we could follow to recommend TSH-suppressive hormonal in China. However, to our knowledge, this is the first article in English to evaluate the long-term outcomes of PTC patients who using CN during operation, which provided significant information surgeons could used for clinical recommendation.
Conclusion
In this study, we demonstrated that the use of CN significantly helped in identifying the parathyroid glands in surgery, which improved the postoperative iPTH and serum calcium level and decreased the incidence of transient hypoparathyroidism. Moreover, it also notably increased the number of total and metastatic lymph nodes in central compartment. However, we should not exaggerate the function of CN since it couldn’t improve the permanent hypoparathyroidism and recurrence in PTC patients who underwent total thyroidectomy with bilateral central lymph node dissection.
References
Grebe, S. K. & Hay, I. D. Thyroid cancer nodal metastases: biologic significance and therapeutic considerations. Surgical Oncology Clinics of North America 1, 43–63 (1996).
Ito, Y. et al. An observation trial without surgical treatment in patients with papillary microcarcinoma of the thyroid. Thyroid 13, 381–387 (2003).
Chow, S. M. et al. Papillary microcarcinoma of the thyroid-Prognostic significance of lymph node metastasis and multifocality. Cancer 98, 31–40 (2003).
Mazzaferri, E. L. An overview of the management of papillary and follicular thyroid carcinoma. Thyroid 9, 421–427 (1999).
Chang, H. P. et al. Significance of the extracapsular spread of metastatic lymph nodes in papillary thyroid carcinoma. Clinical & Experimental Otorhinolaryngology 8, 289–294 (2015).
Sang, L. Y. et al. Postoperative complications of thyroid cancer in a single center experience. Journal of Korean Medical Science 25, 541–545 (2010).
Youngwirth, L. et al. Parathyroid hormone deficiency after total thyroidectomy: incidence and time. Journal of Surgical Research 163, 69–71 (2010).
Yang, F. et al. Magnetic functionalised carbon nanotubes as drug vehicles for cancer lymph node metastasis treatment. European Journal of Cancer 47, 1873–1882 (2011).
Yu, W. et al. Potential role for carbon nanoparticles to guide central neck dissection in patients with papillary thyroid cancer. Surgery. 160, 755–761 (2016).
Wang, Q. et al. Preoperative endoscopic localization of colorectal cancer and tracing lymph nodes by using carbon nanoparticles in laparoscopy. World J Surg Oncol. 14, 231 (2016).
Li, Z. et al. Clinical study of harvesting lymph nodes with carbon nanoparticles in advanced gastric cancer: a prospective randomized trial. World J Surg Oncol. 14, 88 (2016).
Wu, X. et al. Sentinel Lymph Node Detection Using Carbon Nanoparticles in Patients with Early Breast Cancer. PLoS One. 10, e0135714 (2015).
Wang, B. et al. Application of carbon nanoparticles accelerates the rapid recovery of parathyroid function during thyroid carcinoma surgery with central lymph node dissection: A retrospective cohort study. Int J Surg. 36, 164–169 (2016).
Long, M. et al. A carbon nanoparticle lymphatic tracer protected parathyroid glands during radical thyroidectomy for papillary thyroid non-microcarcinoma. Surg Innov. 24, 29–34 (2017).
Xu, X. F. & Gu, J. The application of carbon nanoparticles in the lymph node biopsy of cN0 papillary thyroid carcinoma: A randomized controlled clinical trial. Asian J Surg. 40, 345–349 (2017).
Gao, Q. & Zhao, D. Clinical application of carbon nanoparticles labeled lymph node in cervical lymph node dissection with papillary thyroid cancer staged preoperatively as N0. Lin Chung Er Bi Yan Hou Tou Jing Wai Ke Za Zhi. 28, 1938–1940 (2014).
Wang, X. L., Wu, Y. H., Xu, Z. G., Ni, S. & Liu, J. Parathyroid glands are differentiated from lymph node by activated-carbon particles. Zhonghua Er Bi Yan Hou Tou Jing Wai Ke Za Zhi. 44, 136–140 (2009).
Gu, J., Wang, J., Nie, X., Wang, W. & Shang, J. Potential role for carbon nanoparticles identification and preservation in situ of parathyroid glands during total thyroidectomy and central compartment node dissection. Int J Clin Exp Med. 8, 9640–9648 (2015).
Wu, G. et al. Role of carbon nanoparticles in patients with thyroid carcinoma undergoing total thyroidectomy plus bilateral central neck dissection. Zhonghua Yi Xue Za Zhi. 95, 912–916 (2015).
Liu, X., Chang, S., Jiang, X., Huang, P. & Yuan, Z. Identifying parathyroid glands with carbon nanoparticle suspension does not help protect parathyroid function in thyroid surgery: a prospective, randomized control clinical study. Surg Innov. 23, 381–389 (2016).
Ellis, H. Anatomy of the thyroid, parathyroid and suprarenal (adrenal) glands. Surgery 21, 289–291 (2003).
Wang, B. et al. The role of carbon nanoparticles in identifying lymph nodes and preserving parathyroid in total endoscopic surgery of thyroid carcinoma. Surgical Endoscopy 29, 1–7 (2015).
Kobayashi, K. et al. Recurrence pattern after conservative surgery for papillary thyroid carcinoma. Auris Nasus Larynx 41, 548–551 (2014).
Cisco, R. M., Shen, W. T. & Gosnell, J. E. Extent of surgery for papillary thyroid cancer: preoperative imaging and role of prophylactic and therapeutic neck dissection. Current Treatment Options in Oncology 13, 1–10 (2012).
Gyorki, D. E. et al. Prophylactic Central Neck Dissection in Differentiated Thyroid Cancer: An Assessment of the Evidence. Annals of Surgical Oncology 20, 2285–2289 (2013).
Tobias, C., Long, W. D. & Robert, U. Controversy surrounding the role for routine central lymph node dissection for differentiated thyroid cancer. Current Opinion in Oncology 22, 30–34 (2010).
Lee, D. Y. et al. The benefits and risks of prophylactic central neck dissection for papillary thyroid carcinoma: prospective cohort study. International Journal of Endocrinology, International Journal of Endocrinology 2015, 571480 (2015).
Acknowledgements
We would like to thank statistician Yan Yao, PhD, of Epidemiology and Health Statistics Institute for his assistance with statistical analysis.
Author information
Authors and Affiliations
Contributions
All authors contributed to the design of the study and writing of the manuscript. Conceptualization, G.C. and S.X.; Resource, S.X. and P.Y.R.; Data collection, S.X., P.S.W. and P.Y.R.; Writing, S.X. All authors reviewed the manuscript.
Corresponding author
Ethics declarations
Competing Interests
The authors declare no competing interests.
Additional information
Publisher's note: Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made. The images or other third party material in this article are included in the article’s Creative Commons license, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons license and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this license, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Xue, S., Ren, P., Wang, P. et al. Short and Long-Term Potential Role of Carbon Nanoparticles in Total Thyroidectomy with Central Lymph Node Dissection. Sci Rep 8, 11936 (2018). https://doi.org/10.1038/s41598-018-30299-8
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41598-018-30299-8
This article is cited by
-
Do carbon nanoparticles really improve thyroid cancer surgery? A retrospective analysis of real-world data
World Journal of Surgical Oncology (2020)
-
Comparison of indocyanine green and carbon nanoparticles in endoscopic techniques for central lymph nodes dissection in patients with papillary thyroid cancer
Surgical Endoscopy (2020)
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.