Abstract
There is no safe and efficacious vaccine against human leishmaniasis available and live attenuated vaccines have been used as a prophylactic alternative against the disease. In order to obtain an attenuated Leishmania parasite for vaccine purposes, we generated L. infantum KHARON1 (KH1) null mutants (ΔLikh1). This gene was previously associated with growth defects in L. mexicana. ΔLikh1 was obtained and confirmed by PCR, qPCR and Southern blot. We also generate a KH1 complemented line with the introduction of episomal copies of KH1. Although ΔLikh1 promastigote forms exhibited a growth pattern similar to the wild-type line, they differ in morphology without affecting parasite viability. L. infantum KH1-deficient amastigotes were unable to sustain experimental infection in macrophages, forming multinucleate cells which was confirmed by in vivo attenuation phenotype. The cell cycle analysis of ΔLikh1 amastigotes showed arrested cells at G2/M phase. ΔLikh1-immunized mice presented reduced parasite burden upon challenging with virulent L. infantum, when compared to naïve mice. An effect associated with increased Li SLA-specific IgG serum levels and IL-17 production. Thus, ΔLikh1 parasites present an infective-attenuated phenotype due to a cytokinesis defect, whereas it induces immunity against visceral leishmaniasis in mouse model, being a candidate for antileishmanial vaccine purposes.
Similar content being viewed by others
Introduction
Leishmaniasis is a group of diseases caused by protozoa belonging to Leishmania genus (Ross, 1903). These diseases affect mainly poor and marginalized populations and recently, 97 countries, distributed in Africa, Asia, Americas, Europe and Oceania, reported the endemic transmission of leishmaniasis1. Leishmaniasis is a parasitic disease with the second highest mortality rate – about 20,000 to 30,000 annual deaths for visceral leishmaniasis (VL) – only behind malaria2. More than 58,000 cases of VL and 220,000 cases of cutaneous leishmaniasis (CL) are reported annually. However, due to the high underreporting rates, it is estimated that 12 million people are infected and that 2 million new cases of leishmaniasis occur annually1,2.
Decreased leishmaniasis incidence is a complex task that requires prevention and control measures to be taken in an integrated manner. Since the treatment of patients has little impact on the epidemiology of New World leishmaniasis, health education, vector and reservoir control are critical to reducing leishmaniasis cases3,4. In this scenario, the development of an effective and accessible human vaccine is the best strategy for the control of this serious disease. Despite the great effort employed in recent years, there is still no vaccine available for human use5. The main issues to be solved are the high cost, the antigenic robustness of the parasites and the great complexity of the host’s responses6.
It is known that vaccines composed of attenuated viruses and bacteria are considered gold standard against intracellular pathogens7. Studies using attenuated Leishmania have shown that this is a good strategy for producing a long-lasting protective immune response8,9,10,11. By inducing a subclinical infection, attenuated Leishmania elicit the generation of memory cells5,12,13,14. The infection with live attenuated Leishmania is similar to an infection with pathogenic parasites but has the advantages of preventing overt disease while also allowing the host immune system to interact with a large gamma of leishmanial essential antigens in the development of a protective immunity15.
The immune response in mammalian hosts infected by Leishmania involves a complex biochemical network recruiting different cell types such as, chemo- and cytokines, and therefore a thorough understanding of vaccine-induced immunity will further reveal the important mediators of a subsequent protective response5,11,12,13,14,16,17,18,19,20. In Leishmania infection, the host immune system is sorely compromised, mainly affecting the ability of T cells to proliferate, leading to defects in cytotoxic functions and IL-12 release21. For example, after an infection in susceptible mouse strains, such as BALB/c and Swiss, an induction of a Th2-type immune response characterized by secretion of anti-inflammatory or regulatory cytokines, IL-10, IL4, IL- 5, IL-6, can inhibit the production of IL-12 cytokine – inductor of macrophage leishmanicidal action – and down-regulate the activity of the enzyme inducible nitric oxide synthase (iNOS) so, the nitric oxide (NO) and IFN-γ production are often impaired, allowing parasites to disseminate and persist in the host tissue causing severe damage6,22.
Normally, a vaccination scheme that elicits both CD4 and CD8 T cell immune responses in a Th1-polarized type, with consequent production of pro-inflammatory cytokines, mainly IL-12, IFN-γ and TNF-α, can protect from further infection. However, the simplistic paradigm Th1 vs. Th2 is not always applicable to all forms of leishmaniasis caused by different Leishmania strains23. Other cell types, for example Th17 cells and regulatory T cells (Treg), play crucial roles in disease progression or remission, depending on: (I) Leishmania spp.; (II) host genetic variation and (III) phenotypic background, excluding any immunological conditions.
Recent publications on live attenuated vaccines using centrin knocked out Leishmania donovani parasites (ΔLdCen) have shown induction of Th1 type immune response in mice, hamsters, and dogs with protection from subsequent challenge by virulent Leishmania infection24. ΔLdCen induces higher expression of Th17 differentiation cytokines – IL-1β, IL-6, and TGF-β – in splenic dendritic cells and upregulates IL-17 production by splenocytes and both CD4 and CD8 T cells, resulting in protection against wild-type L. donovani challenge25.
The protein KHARON1 (KH1) was recently described through the characterization of a glucose transporter in L. mexicana (LmxGT1). KH1 is located at the base of the flagellum and associated with the cytoskeleton and the flagellar axoneme, therefore being necessary for targeting LmxGT1 from the flagellar pocket to the flagellum26. Promastigote forms of L. mexicana null mutants (ΔLmxkh1) did not present any change in fitness, but ΔLmxkh1 amastigotes have a failure in cytokinesis, generating non-viable multinucleated forms. As a consequence, ΔLmxkh1 mutants were unable to sustain infection in BALB/c mice27.
Thus, in the present study, we performed Kh1 gene disruption in L. infantum, the etiological agent of visceral leishmaniasis, and evaluated the phenotype of these mutants, regarding their growth rates in vitro, infectivity in vitro and in vivo, intracellular proliferation, morphology and cell-cycle. Furthermore, we evaluated a vaccination scheme in BALB/c mice immunized with ΔLikh1 and challenged by L. infantum wild-type. The immunogenicity was assessed by tracking seroconversion and cytokine production in vaccinated mice.
Results
Confirmation of KH1 deletion
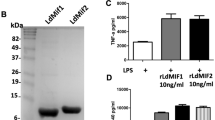
In order to evaluate the correct integration of cassettes in mutant parasites, integration PCRs were performed (Supplementary Table S1). All clones presented fragments of expected size for the integration of both cassettes (Supplementary Fig. S1), showing that both cassettes are correctly integrated into the parasite’s genome. Furthermore, copy number of KH1 gene was investigated by quantitative PCR in L. infantum Wild-Type (WT) and mutants. The pairs of primers KH1, GAPDH and DNA polymerase (Supplementary Table S1) amplified fragments of 105, 74 and 69 bp, respectively, and all of them had amplification efficiencies close to 100% (Supplementary Fig. S2). The normalization with both housekeeping genes (GAPDH and DNA polymerase) generated the same result. No amplification of KH1 gene was observed in any of the ΔLikh1 clones analyzed (Fig. 1a), while heterozygous knockout (ΔLikh1::NEO/KH1, here called ΔLikh1+) shows about half of the KH1 copy number as compared to the WT line. The add-back line ΔLikh1[pSP72αZEOα/KH1] present a 1.5-fold increase on KH1 copy number when compared to WT line (Fig. 1a). In addition, Southern blot was also performed in order to confirm KH1 deletion (Fig. 1b,d). For both probes the expected band profile was obtained. The probe that recognizes the 5’UTR region (Fig. 2c) revealed a band of about 1.2 kb, corresponding to the KH1 gene fragment only in the WT and ΔLikh1+ samples. Both ΔLikh1 clones presented bands of expected size for the NEO and HYG fragments (819 and 602 bp respectively), and no bands corresponding to the KH1 gene. Similarly, the probe that recognizes the KH1 gene revealed a band of expected size in the WT and ΔLikh1+ samples, indicating the presence of the gene in these samples. No fragment was recognized in the DNA samples from ΔLikh1 clones, confirming the success of KH1 deletion. In the complemented (add-back) line, KH1 probe revealed a very strong signal that is characteristic of extrachromosomal plasmid DNA migration in the gel, which corresponds to the construct pSP72αZEOα/KH1 (Fig. 1d). Taken together, the results of conventional PCR, qPCR and Southern blot confirm the complete deletion of KH1 in the mutants submitted to double replacements.
Confirmation of KH1 deletion in L. infantum. (a) Comparison of the copy number of KH1 gene in the genomic DNA of the mutant lines. The copy number was determined by quantitative real-time PCR relative to the housekeeping genes GAPDH, using the comparative CT method (2−ΔΔCT Method). (b) Schematic representation of KH1 locus before and after the cassettes integration. The cleavage sites of NdeI and PvuII restriction enzymes and the length of the generated fragments were represented. (c,d) Southern blot analysis performed with 10 µg of genomic DNA of L. infantum wild-type (WT), the mutants ΔLikh1+, ΔLikh1 and ΔLikh1[pSP72αZEOα/KH1] were digested with NdeI and PvuII restriction enzymes. The membranes were hybridized with 32P-labelled probes, that reconize the KH1 5′UTR (c) or Kh1 gene (d). The normalization was performed by calculating the KH1/GAPDH ratio. Similar results were obtained when normalizing with DNA polymerase as housekeeping gene. Exposures were cropped from original images available as supplementary material.
Growth profile, viability and morphology of axenically maintained promastigotes. (a) Growth curve of L. infantum promastigote lines of wild-type (WT) and mutants ΔLikh1+, ΔLikh1, ΔLikh1[pSP72αZEOα/KH1] and ΔLikh1[pSP72αZEOα]. The parasite number was automatically determined using the Z1 Coulter® Particle Counter (Beckman Coulter™). (b) Parasite viability at logarithmic (3rd day) and stationary (5th day) phase of growth as determined by MTT method. Columns represent the average values and the standard error of the mean from two independent experiments performed in quintuplicate analyzed by ANOVA followed by Tukey’s multicomparisons test. *p = 0.01; ***p = 0.001; ****p = 0.0001. (c) Optical microscopy of L. infantum WT, ΔLikh1 and ΔLikh1[pSP72αZEOα/KH1] promastigotes stained with rapid panoptic at logarithmic and stationary phase of growth. Images were acquired using a Nikon® L810 camera coupled Olympus BH2 Microscope System. Bars: 10 μm. (d) Scanning electron microscopy-derived images of L. infantum WT, ΔLikh1 and ΔLikh1[pSP72αZEOα/KH1] at log phase of growth. Electron micrographs were obtained using a scanning electron microscope JEOL JSM5600. Magnification: WT = 2500x; ΔLikh1 and ΔLikh1[pSP72αZEOα/KH1] = 3000x. The right down percentages indicate the number of pear-like promastigotes (see supplementary Table S2).
ΔLikh1 null mutants promastigote forms show no alteration in growth pattern
Null mutants (ΔLikh1) and the add-back line ΔLikh1[pSP72αZEOα/KH1] promastigote forms grew at similar rates compared to wild-type and the heterozygous knockouts (ΔLikh1+) parasites in axenic culture (Fig. 2a). Although no growth alteration was observed in terms of total parasite number, the morphology of ΔLikh1 mutants differs from wild-type line. L. infantum KHARON1 deficient mutants presented rounded parasites both at the log and stationary phase (Fig. 2c). Analysis by scanning electron microscopy, allowed us to observed that 30% of log-phase ΔLikh1 promastigotes presented an alteration in cell shape at the posterior region, that we called pear-like form (Fig. 2d). ΔLikh1[pSP72αZEOα/KH1] parasites do not completely recover wild-type morphology (Fig. 2c). The characteristic pear-like promastigotes were still detected in 10% of cells during growth log-phase (Fig. 2d). Although we detected altered cellular shape, the mutant parasites remained viable. Indeed, ΔLikh1 viability is increased in the stationary phase of axenic growth when compared with WT or ΔLikh1+ backgrounds (Fig. 2b). In addition, no difference was detected in glucose uptake by ΔLikh1 null mutant parasites when compared to its wild-type counterpart (Supplementary Fig. S3). Furthermore, we evaluated the SbIII sensitivity in ΔLikh1, since glucose transport could be related to SbIII in Leishmania. However, no difference in sensitivity to SbIII was observed between ΔLikh1 null mutant and wild-type lines, with SbIII IC50 at 184.9 µM and 179.8 µM respectively (Supplementary Fig. S4).
ΔLikh1 parasites are unable to sustain macrophage experimental infection
In order to evaluate infectivity and intracellular multiplication of ΔLikh1 amastigotes, murine peritoneal macrophages or monocyte-derived human macrophages (THP-1 cell line) were infected with WT, ΔLikh1 and ΔLikh1[pSP72αZEOα/KH1] parasites (Figs 3 and 4). L. infantum ΔLikh1 amastigotes are able to infect macrophages and differentiate into amastigotes. However, these ΔLikh1 mutants are unable to maintain infection in murine peritoneal and human-derived macrophages (Fig. 3). KHARON1 null mutant parasites presented a low rate replication, not exceeding 300 parasites per 100 host cell for murine or human macrophages (Fig. 3a,c). Eight days post-infection, THP-1 macrophages presented 96% reduction in total number of ΔLikh1-infected cells and 94% reduction in amastigotes/100 macrophages ratio when compared to WT (Fig. 3a). Parasite clearance was observed after 16 days of infection in murine peritoneal macrophages infected with ΔLikh1 mutants (Fig. 3c,d). The add-back cell line ΔLikh1[pSP72αZEOα/KH1] recovered the ability to replicate within murine or human macrophages, but infection rates were lower when compared with WT (Fig. 3a,c).
Experimental infection of THP-1 and murine peritoneal macrophages with ΔLikh1. THP-1 and murine peritoneal macrophages were infected with the following L. infantum lines: wild-type (WT), null mutant (ΔLikh1) and add-back (ΔLikh1[pSP72αZEOα/KH1]) and evaluated by 2 to 10 or 16 days post-infection (DPI). The columns represent the percentage of infected macrophages (MΦ) while the number of amastigote/infected macrophages are shown as overlapped lines in THP-1 (a) or murine-derived peritoneal macrophages (c). Optical photomicrographs were taken 10 and 16 DPI, respectively for THP-1 (b) and murine macrophages (d), infected with L. infantum WT and ΔLikh1. Arrows highlight intracellular amastigotes in ΔLikh1-infected THP-1 (b). Experimental infection was performed in macrophages adhered to 13 mm round sterile glass coverslips in 24-well cell culture plates (Sarstedt AG & Co., Nümbrecht, Germany), stained with panoptic rapid stained and mounted on microscope slides using Entellan® (Merk Millipore, Burlington, MA, USA). Images were acquired using a Nikon® L810 camera coupled with Olympus BH2 Microscope System.Bar: 50 µm.
Qualitative and quantitative analysis of ΔLikh1 multinucleated amastigotes. (a) Representative images of LiWT and ΔLikh1 amastigotes infecting THP-1 or murine peritoneal macrophages, showing multinucleated ΔLikh1 amastigotes. Bar represents 10 µm. Quantitative analysis of nuclei number in LiWT (b), ΔLikh1 (c) and ΔLikh1[pSP72αZEOα/KH1] (d) intracellular amastigotes infecting murine peritoneal macrophages.
ΔLiKh1 possess multinucleated intracellular amastigotes
The quantitative evaluation of amastigote nuclei revealed the presence of multinucleated cells in ΔLikh1 parasites. On the 12th-day post-infection, 95% of ΔLikh1 parasites presented more than two nuclei (Fig. 4a,c). Add-back line also presented multinucleated cells, although in smaller proportions (Fig. 4d). At twelve days post infection, while 75% of the WT parasites had 1 nucleus (Fig. 4b), only 30% of Likh1[pSP72αZEOα/KH1] parasites had 1 nucleus and 40% had more than 2 nuclei (Fig. 4d).
ΔLikh1 amastigotes displayed a cytokinesis defect with cell-cycle arrest at G2/M
Cell cycle analysis using flow cytometry was performed in order to better understand the growth defects of ΔLikh1 amastigotes compared to wild-type parasites. ΔLikh1 parasites showed a reduced number of cells at G0/G1 phase which were arrested at G2/M phase when compared to the WT counterpart (Fig. 5). This phenotype is characteristic of a growth attenuated phenotype by decreasing their cellular cycling.
Cell cycle comparative analysis of L. infantum WT and KH1 null mutants. L. infantum intracellular amastigotes were isolated from THP-1 infected macrophages and submitted to flow cytometry analysis after incubation with propidium iodide (PI). The percentage of cells in each phase is shown (a). The data represents the average of two independent experiments. Representative histograms show the DNA content of L. infantum WT (b), and L. infantum ΔLikh1 amastigotes (b). Statistical analysis was performed based on ANOVA followed by Bonferroni’s multiple comparisons test (***p ≤ 0.001).
ΔLikh1 parasites show an attenuated virulence phenotype in vivo
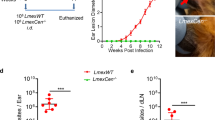
To assess whether ΔLikh1 parasites virulence was altered in vivo, different infection schemes were performed in BALB/c and immunocompromised C57BL/6 mice IFN-γ−/−. Amastigotes used in the in vivo infection assays were previously recovered from THP-1 macrophages. Infection of BALB/c mice with L. infantum WT amastigote forms were more successful when compared to infection using promastigote forms. L. infantum wild-type parasites were recovered from the spleen and liver, of all mice. However, the amastigote forms of ΔLikh1 parasites were not able to infect BALB/c mice (Fig. 6a). In order to further investigate the infectivity of these parasites, promastigote forms of WT and ΔLikh1 parasites were inoculated in IFN-γ−/− C57BL/6 mice. Results of the limiting dilution assay (Fig. 6b) showed that ΔLikh1 parasites were able to infect those mice, but lower ΔLikh1 parasite number was recovered from spleen and liver of those mice when compared to its wild-type counterpart.
Parasite load in mice infected with LiWT and ΔLikh1. Parasite load was quantified by limiting dilution from samples isolated from liver and spleen of BALB/c (a) and IFN-ɣ−/− C57BL/6 mice (b). BALB/c mice were infected with amastigotes (a) and C57BL/6 mice were infected with promastigotes forms (b). Samples were isolated on 15th-day post-infection. Statistical analysis was performed based on ANOVA followed by Bonferroni’s multiple comparisons test (**p ≤ 0.01; ***p ≤ 0.001).
ΔLikh1 parasites induced seroconversion in vivo after priming by IV or SC routes
Twenty days after the last immunization of Balb/c mice with ΔLikh1 parasites, by IV or SC route, the levels of Soluble Leishmania Antigens (SLA)-specific IgG’s subtypes in the serum were determined. Serum analysis showed significantly higher titers of SLA-specific IgGTotal, IgG1 and IgG2a in all immunized groups in comparison with the PBS group (p < 0,001) (see Supplementary Fig. S5), indicating a seroconversion at the first dose and a strong induction of Leishmania-specific antibody responses triggered by the vaccination schemes (Fig. 7a). The amount of SLA-specific IgG1 detected in the serum of mice immunized twice intravenously was greater than in those immunized subcutaneously (p < 0.001). The SC Prime-Boost vaccination scheme was able to induce significantly higher production of IgG2a than the IV scheme (p < 0.05). Although IgG2a:IgG1 ratio was higher for animals primed subcutaneously (p < 0.001) (Fig. 7b), after boosting this difference disappeared in comparison with IV immunized groups. Thus, even though SC immunization could polarize humoral response to the Th1 type, after a subsequent immunization SLA-specific IgG’s serum levels become similar in higher titers in comparison to IV ΔLikh1-immunized animals (Fig. 7b).
Humoral and cellular immune responses induced by different schemes of vaccination with ΔLikh1. Humoral immune response was evaluated by conventional ELISA measurement of serum levels of different isotypes of LiWT SLA-specific antibodies (IgG total, IgG1 and IgG2a). (a) Seroconversion of mice 20 days post-immunization with ΔLikh1. (b) IgG2a:IgG1 ratio between IV and SC prime-boosted groups. (c–h) Levels of cytokines in pg/mL in the supernatant of LiWT SLA-stimulated splenocytes. The concentration of LiWT SLA in the experiments was 25 μg/mL and splenocytes were stimulated for 72 h. CpG ODN at 5 μg/mL was used as a positive control of a Th1-response and α-MEM medium with 20% of FBS was used as negative control. Cytokines were measured by flow cytometry with the BD Cytometric Bead Array (CBA) Mouse Th1/Th2/Th17 Cytokine Kit (BD Biosciences, San Jose, CA, USA) following manufacturer instructions. The acquisition and data analyses were made in BD FACSVerse Instrument and FCAP Array Software v3. The detection limit of IL-2, IL-4, IL-6, IFN-γ, TNF, IL-17A and IL-10 cytokines were respectively 0.1; 0.03; 1.4; 0.5; 0.9; 0.8 and 16.8 pg/mL as well as cytokines secreted by LiWT SLA-stimulated splenocytes from immunized mice. Data are shown as means ± SE. Statistical analyses used One-way-ANOVA followed by Bonferroni’s multiple comparison test. ***p < 0,001. CpG ODN: CpG motifs oligodeoxynucleotides (Toll-like receptor 9 agonist); FBS: fetal bovine serum; IV: intravenous; SC: subcutaneous; SLA: soluble Leishmania antigens. Groups: 20 days after prime; 20 days after prime and boost; 20 days after challenging (vaccinated or not). PBS: LiWT- infected non-immunized mice; Prime-Boost (IV) CTRL: ΔLikh1-infected non-challenged (with LiWT) mice; Prime (IV): intravenously ΔLikh1-vaccinated mice once (prime) followed by LiWT challenge; Prime-Boost (IV): intravenously ΔLikh1-vaccinated mice twice (prime-boost) followed by LiWT challenge; Prime-Boost (SC): subcutaneously ΔLikh1-vaccinated mice twice (prime-boost) followed by LiWT challenge.
Higher IL-17 secretion is associated with lower parasite burden in ΔLikh1-immunized BALB/c mice challenged by LiWT
The cytokines secreted by splenocytes of vaccinated mice were quantified 20 days after either last immunization or challenge with the virulent LiWT parasites. The amount of all cytokines but IL-17A in the culture supernatant after incubation for 72 h with SLA were significantly higher for the SC-vaccinated group when compared with unexposed splenocytes. This indicates that the scheme used induced a strong mixed Th1/Th2 immune response, in agreement with the humoral response (Fig. 7c–g). However, LiWT SLA-treated splenocytes presented higher IFN-γ:IL-10 ratio in SC-immunized mice (Fig. 7h), when compared with those maintained in free medium, indicating the polarization of the immune response to the Th1 type, which corroborates with the higher IgG2a:IgG1 ratio following prime in this group (Fig. 7b). Nevertheless, the induction of this differentiated immune response was not able to protect mice from a subsequent infection by LiWT, as demonstrated by liver and spleen parasite load, similar to the PBS-immunized and infected mice (Fig. 8a,b). In contrast, mice immunized IV either in prime or prime-boost scheme showed significantly lower parasite burden in liver and spleen (Fig. 8a,b), compared to PBS control group, but produced significantly higher levels of only IL-17A cytokine after SLA-stimulus (Fig. 7d). Considering a strong undifferentiated humoral response, this scenario highlights the importance of IL-17A production in protecting ΔLikh1-vaccinated mice against LiWT challenge It is worth mentioning that prime-boost (IV) ΔLikh1-immunized and non-challenged mice presented a significantly lower parasite load in comparison with the challenged ones (p < 0.001) (Fig. 8b). Curiously, it also produced higher levels of IL-17A cytokine. Although the ΔLikh1 can colonize liver and spleen at a given level, the number of parasites in the organs is very low and in comparison with the LiWT parasites, the KH1 knocked out parasites are much less infective in vivo, and this control of parasitism seems to be related to an effect of IL-17A cytokine and probably its promoting or differentiated cytokines, as well as the activation of Th17 responses.
Parasite burden in liver and spleen of ΔLikh1-immunized mice followed by LiWT challenge. ΔLikh1-vaccinated animals (n = 6) were euthanized 20 days post-L. infantum challenge. Spleen (a) and liver (b) were removed, macerated and the DNA was extracted. The number of parasites in these organs was then determined by qPCR. Data are shown as median ± 95% CI. Before making statistical analysis, we performed a measurement of statistic dispersion by the IQR test (Interquartile range) in order to identify the outliers, but maintaining the minimum statistical accepted values which explains the variation in animal number per group.Analyses were done by Kruskall-Wallis, with Dunns posttest *p < 0.05; **p < 0.01. IV: intravenous; SC: subcutaneous; PBS: LiWT- infected non-immunized mice; Prime-Boost (IV) CTRL: ΔLikh1-infected non-challenged (with LiWT) mice; Prime (IV): intravenously ΔLikh1-vaccinated mice once (prime) followed by LiWT challenge; Prime-Boost (IV): intravenously ΔLikh1-vaccinated mice twice (prime-boost) followed by LiWT challenge; Prime-Boost (SC): subcutaneously ΔLikh1-vaccinated mice twice (prime-boost) followed by LiWT challenge.
Discussion
In the present study we successfully disrupted KHARON1 (KH1) gene in L. infantum based on gene replacement by conventional homologous recombination.
Promastigote forms of L. infantum KH1 null mutants exhibited similar growth pattern to WT parasites, in accordance with previous studies of KH1 gene deletion in L. mexicana27. However, morphology of ΔLikh1 parasites was altered indicating a cytoskeleton impairment. Despite functional analysis, there is no known domain described for KH1 protein. However, sequence homology modeling revealed a C-terminal similarity with the villin headpiece domain (VHP – PF02209) that contains an F-actin binding site28. Villin (or gelsolin) is a calcium-regulated actin-binding protein that modulates cytoskeleton dynamics29. The similarity with villin VHP suggests that KH1 could also alter cytoskeleton organization in promastigotes of L. infantum and not only in amastigotes forms. This observation is also supported by the fact that KHARON in African Trypanosomes localizes at subpellicular microtubules and mitotic spindle, being associated with different components of the trypanosome cytoskeleton30.
As demonstrated in L. mexicana, KH1 is responsible for targeting the glucose transporter LmxGT1 and was indirectly related to glucose transport in those parasites26. Here, we investigated the impact of the deletion of KH1 on glucose uptake in L. infantum (Supplementary Fig. S3). It was found that the deletion of KH1 in L. infantum did not interfere with glucose transport and this lack of phenotype is potentially a result of the presence of more than one Leishmania transporter capable of importing the hexoses glucose, mannose, fructose and galactose31,32,33,34. In L. infantum there is a locus encoding three glucose transporters isoforms were genes LinJ.36.6540, LinJ.36.6550, LinJ.36.6560 code respectively for LiGT3, LiGT2 and LiGT1 (tritrypdb.org). Thus they are able to maintain normal glucose uptake in ΔLikh1 parasites via bypass. Since energetic metabolism is also involved in the mechanism(s) of action of Sb-based drugs, such as beta-oxidation of fatty acids or glycolysis35,36, and because resistant-parasites present changes in fitness that result in lower glucose uptake and metabolism37,38,39, we evaluated the susceptibility of ΔLikh1 to SbIII. We observed that ΔLikh1 mutant exhibited sensitivity to trivalent antimony as the wild-type line (see Supplementary Fig. S4).
To evaluate the infectiveness of ΔLikh1 amastigote forms, an in vitro experimental infection was performed in murine peritoneal and human-derived macrophages. Similar to the observed in L. mexicana27, L. infantum KH1 deficient mutant were unable to maintain the infection within macrophages for more than 16 days in vitro. 10 to 12 days after infection, almost all parasites possess more than two nuclei, a phenotype that culminates with parasite’s death. We observed that ΔLikh1 [pSP72αZEOα/KH1] add-back parasites do not completely recover the phenotype when compared to wild-type ones (Fig. 3), even though they present increased KH1 copy number revealed by qPCR and Southern blot analyses (Fig. 1). When an episomal vector was used, it is possible that the daughter cells do not receive equal amounts of the vector, and the expression level of genes may vary from cell to cell, allowing the mosaicism observed40.
The presence of multinucleated forms suggests that although the parasites are able to perform karyokinesis, they are not able to finish cytokinesis. The phenotype presented by L. infantum Δkh1 parasites resembles those presented by L. donovani Centrin1 knockout (ΔLdcen), in which there is no change in promastigote growth, and the amastigotes are multinucleated with cell-cycle arrest culminating with parasite death41. Like what was observed in the cell cycle of ΔLdcen mutants41, L. infantum ΔLikh1 also showed decreased cellular cycling, with retention at G2/M phase. This result corroborates the importance of KH1 protein for cell division in the amastigote forms of L. infantum.
Genetically modified live-attenuated L. donovani ΔLdcen and ΔLdp27 has been described as vaccine candidates10,42,43, but also several targets have been implicated in loss of virulence upon disruption in different Leishmania species that often elicit protective immunity in vivo such as: silent information regulator (SIR2)44, A245, arabino-1,4-lactone oxidase9 and biopterin transporter BT146,47 in L. donovani; HSP70-II in L. infantum48; mitochondrial superoxide dismutase in L. amazonensis49; δ-amastins in L. braziliensis50 and cysteine protease B in L. mexicana51
To assess whether the attenuation phenotype of ΔLikh1 mutants observed in vitro would also be observed in vivo, infections of BALB/c and IFN-γ−/− C57BL/6 mice were performed. The fact that ΔLikh1 parasites were not able to infect BALB/c mice and IFN-γ−/− C57BL/6 mice infected with this strain had a much lower burden when compared to WT, shows that the knockout parasites are not effective in maintaining in vivo infection. Although some authors argue that parasites ability to generate a subclinical infection is critical for immunization, to result in lasting protection, such as in the case of leishmanization15,52,53,54,55,56, parasites may generate a protective immune response without, however, infecting the host, by the activation of dendritic cells and T lymphocytes IFN-ɣ production as demonstrated in immunizations with L. tarentolae57. The fact that ΔLikh1 knockout did not infect mice efficiently, encourage the use of these parasites as a live attenuated vaccine as they can serve as a source of a broad range of immune potent antigens and induce a host protective immune response in animal models.
To confirm this hypothesis we performed immunization protocols in BALB/c mice to determine whether parasites were able to elicit humoral and cellular immune responses in the host, without causing disease, and determine if the administration route could affect the immunogenicity and the efficiency of protection from Leishmania infection. Both intravenous and subcutaneous priming of mice with the ΔLikh1 parasites caused a significant increase in SLA-specific antibodies detected in mice serum, as a result of a strong humoral stimulation by either one or two-dose vaccination schemes. It is known that organisms exposed to whole or parts of parasites can develop a specific immunological memory against the harming agent that can be easily inferred by the presence of high titers of type G antibodies (IgG’s)58. The production of antigen-specific IgG2a antibody subclass in mice may be related to the presence of the cytokine IFN-γ and to a Th1 response profile, generally more protective, whereas IgG1 is related to the presence of IL-4, associated with a Th2 type response and the increase in parasite load59,60. In our study, the increased production of IgG2a subclass compared to IgG1 in the SC group in a first moment can be attributed to the administration route and was consistent with a Th1 response profile with the presence of large amount of IFN-γ. Conversely, not only did IgG production changed but also the Th2-type cytokines evaluated were upregulated in splenocytes after second dose and challenging. In this case, the mixed Th1/Th2 response may indicate a regulatory role rather than protective, as a mechanism to reverse the chronic inflammation generated. On the other hand, IV groups showed significantly higher amounts of SLA-specific IgG1, which could point to a stimulation of a more robust humoral response, correlated with a pro-inflammatory response noted only by the high production of IL-17A in detriment of all the other Th1 or Th2-type cytokines. Also, this immune response pattern was directly related to the decrease of parasite load in liver and spleen (in one or two ΔLikh1 doses) of all IV-vaccinate mice. These findings strongly suggest that IL-17A and probably the Th17 cell activation plays a main role in mice protection. In accordance to our results, several studies using formulations with live attenuated vaccines or Leishmania isolated proteins alone or combined with immunoadjuvants, have demonstrated that the use of the isolated antigen led to the production of IgG1, but not IgG2a, whereas the use of an adjuvant – as TLR agonist like CpG’s ODNs – could drive the response to a more Th1 type, taken as required for protection against the infection61. Mice vaccination using recombinant polyprotein alone or combined with Th1-response immunostimulants results in a large production of both sub-classes of antigen-specific IgG1 and IgG2a antibodies in a Th1/Th2 mixed response. Therefore, the literature indicates that the humoral immune response to vaccines is variable and does not show a simple relationship with the protection level, depending on the form the antigen is delivered, the associated adjuvant and the experimental model57,62,63,64. In our study we noticed that the administration route is also a critical factor to direct Th1 or Th2 polarized response in live attenuated vaccines65. The protective or susceptible immune mechanisms behind Leishmania infection are not clear and can vary according to host background and immunological state strain or parasite species, virulence, as well as the formulations, immunization scheme and administration route.
Here, the main mechanistic hint was the strong IL-17A cytokine elicitation triggered by vaccination with ΔLikh1 parasites for host protection followed by virulent Leishmania infection. This cytokine and its lineage are largely described to play an important role in the clearance of pathogens as Gram-positive bacteria Mycobacterium tuberculosis, fungi, and parasites66 that require a massive inflammatory response which is not adequately dealt with Th1 or Th2 immunity leading to host protection. Furthermore, IL-17A was proven to be essential in host protection against Trypanosoma cruzi, during the acute phase of infection, being the hosts B cells the major sources of IL-1761,67. These studies highlight the importance of Th17 cells and IL-17A cytokine in controlling the development of intracellular pathogens. Thus, we can affirm that unique IV immunization with live-attenuated ΔLikh1 parasites is able to seroconvert mice and induce a protective cell immune response with IL-17A release responsible for the protection of exposition and subsequent mice infection by virulent L. infantum opening new possibility for the development of a potent and effective vaccine against visceral leishmaniasis.
The results indicate that KH1 deficient parasites obtained in this work are potential candidates for the development of an attenuated vaccine against leishmaniasis. Attenuated parasite-based vaccines are considered one of the most promising strategies for protection against Leishmaniasis, since these parasites simulate the natural course of Leishmania infection and allow the host immune system to contact a large antigenic repertoire56,68 activating antigen-presenting cells and generating memory cells69. These characteristics are crucial for the development of a lasting response8,56.
Methods
Parasites
Promastigote forms of L. infantum (MHOM/MA/67/ITMAP-263) were cultured in α-MEM medium (Gibco/Thermo Fisher Scientific, Waltham, MA, USA) supplemented with 10% fetal bovine serum, 5 μg/mL of hemin and 5 μM of biopterin, in pH 7 at 26 °C. Parasites were counted using the Z1 Coulter® Particle Counter (Beckman Coulter, Brea, CA, USA) and cultures were maintained by passing 1 × 106 parasites to 5 mL of fresh medium twice a week. Growth curves were performed in 25 cm2 cell culture flasks by seeding 1 × 106 parasite/mL and the number of parasites was determined daily – up to 6 days – by automatic counting using the Z1 Coulter Counter.
Constructs for KH1 knockout and complemented lines
The complete deletion of KH1 (LinJ.36.6110) in L. infantum was performed by homologous recombination using linear cassettes that target the open reading frame (ORF) of KH1 gene and contain the selection resistance markers neomycin phosphotransferase70 and hygromycin B phosphotransferase (HYG). The 5′UTR and 3′UTR regions flanking the open reading frame (ORF) of LinJ.36.6110 were amplified by PCR from the L. infantum genomic DNA using specific primers (Supplementary Table S1). For amplification of the resistance markers, plasmids with the sequences of interest were used as templates. The constructs were obtained by fusion PCR approach and were cloned into the pGEM-T easy vector (Promega, Madison, WI, USA). In order to confirm the presence of expected insert, the plasmids were digested with restriction enzymes SalI and XbaI, whose sites were pre-inserted into the primers for fusion PCR. The sequences were confirmed by Sanger sequencing. For plasmid complementation, KH1 ORF was subcloned into vector pSP72αZEOα71 – harboring bleomycin-binding protein gene (ZEO), conferring resistance to zeocin – at SalI and XbaI restriction sites. To confirm the presence of the correct insert, plasmids were digested with SalI and XbaI.
Transfections and parasite clone selection
Transfections were made by electroporation, performed using the Gene Pulser XCellTM (BioRad, Hercules, CA, USA) by applying two sequential pulses of 1,500 V and 25 μF each as described previously72,73. The clonal selection was performed in semi-solid medium by addition of the antibiotics in the following concentrations: 600 µg/mL of Hygromicin (Invitrogen, Life Technologies), 80 µg/mL of Geneticin (G418) (Gibco/Thermo Fisher Scientific, Waltham, MA, USA) and 800 µg/mL Zeocin (Invitrogen/Thermo Fisher Scientific, Waltham, MA, USA). Mutant parasites were maintained in the presence of specific antibiotics for the resistance markers acquired at transfection. KH1 gene deletion was confirmed by PCR, real-time qPCR and Southern blot. Conventional PCR was applied to verify the correct integration of KH1 knockout cassette by using a reverse primer on HYG or NEO sequences and an external forward primer outside the cassette (Supplementary Fig. S1). Quantitative PCR was performed using genomic DNA to measure KH1 gene copy number and Southern blot directly detected KH1 by DNA probing hybridization.
Quantitative real-time PCR
Genomic DNA was isolated from L. infantum WT, heterozygous knockout (ΔLikh1+), null mutant (ΔLikh1) and complemented add-back (ΔLikh1 [pSP72αZEOα/KH1]) lines by phenol method according to the protocol previously described74. KH1 gene was amplified from genomic DNA by real-time PCR in order to investigate KH1 copy number. The housekeeping genes GAPDH (LinJ.36.2480) and DNA polymerase (LinJ.16.1640) were used as constitutive normalizer (Supplementary Table S1). Amplifications were performed using the Applied Biosystems 7500 thermocycler (Thermo Fisher Scientific, Waltham, MA, USA). PCR was carried out in a final volume of 20 µL of reaction mixture containing 10 pmol of forward and reverse primers, 1x SYBR GREEN reaction mix (Applied Biosystems/Thermo Fisher Scientific, Waltham, MA, USA) and 100 ng of template DNA. The PCR conditions were as follows: initial denaturation step at 95 °C for 10 min followed by 40 cycles of denaturation at 95 °C for 15 s and annealing/extension at 60 °C for 1 min. Fluorescence was measured at the end of each extension step. The copy number was determined using the comparative CT method (2−ΔΔCT Method).
Southern blot
About 10 µg of genomic DNA from L. infantum WT, ΔLikh1+, ΔLikh1 and ΔLikh1[pSP72αZEOα/KH1] were digested with restriction enzymes PvuII and NdeI (Promega, Madison, WI, USA). The fragments were separated by electrophoresis on 1% agarose gel and transferred by capillarity onto nylon membranes (Hybond-N+, GE Healthcare Life Sciences, Malborough, MA, USA). The blots were hybridized with [α-32P]dCTP labeled KH1 and 5′UTR KH1 gene probes amplified with specific primers (Supplementary Table S1) according to standard protocols70. GAPDH probe was used as load control. Densitometric analyzes and semi-quantification were performed using ImageJ software (imagej.nih.gov/ij).
Promastigote viability assay
Leishmania promastigote viability was assessed using the classical 3-(4,5-dimethylthiazol-2-yl)-2,5 diphenyltetrazolium bromide (MTT) method75. Briefly, promastigote forms at 3rd and 5th days of culture (log and stationary phase of growth, respectively) were washed in Hepes-NaCl solution (20 mM Hepes, 0.15 M NaCl, 10 mM glucose, pH 7.2), and cell suspension was seeded in 96-well flat bottom plates (5 × 106 parasites/well in 0.2 mL final volume). Promastigote forms of L. infantum WT, ΔLikh1+, ΔLikh1 and ΔLikh1[pSP72αZEOα/KH1] were exposed to 0.5 mg/mL of MTT and incubated 4 h at 37 °C in humid atmosphere containing 5% CO2. The plates were centrifuged, the supernatant was aspirated and added 0.1 mL of DMSO to dissolve formazan crystals. MTT formazan product was measured spectrophotometrically at 570 nm and cell viability calculated relative to WT growth.
Ultrastructural evaluation
Scanning Electron Microscopy (SEM) was used to evaluate the morphological differences between L. infantum WT, ΔLikh1+, ΔLikh1 and ΔLikh1[pSP72αZEOα/KH1]. The parasites were fixed using a solution of paraformaldehyde 4%, sodium cacodilate 0.1 M, glutaraldehyde 1% and calcium chloride 1 mM for 2 h at room temperature. The samples were then attached to a coverslip treated with Poly L-Lysine (SigmaAldrich, St. Louis, MI, USA) for 30 min in a wet chamber. After parasites adhesion onto coverslips, the samples were post-fixed in osmium tetroxide 1% for 2 h. Samples were dehydrated in a graded series of acetone, critical point dried with CO2 (Emitech K850), sputter coated with gold particles (Emitech K550), mounted on stubs and analyzed with Scanning Electron Microscopy Jeol - JSM5600.
ΔLikh1 cell cycle
To perform intracellular amastigote purification, infected THP-1 macrophages were collected on the 4th day of infection using cell scrapper (Nunc™, Nalge Nunc International, Penfield, NY, USA). Macrophages were passed 30 times through a 27-gauge needle for macrophage disruption and amastigote release. Amastigotes were separated from the cell fragments by differential centrifugation: first centrifugation at 134 × g for 5 min was performed in order to remove macrophage fragments. The supernatant with amastigotes was collected and washed 4 times with Hepes-NaCl solution (20 mM Hepes, 0.15 M NaCl, 10 mM glucose, pH 7.2) and centrifuged at 1200 × g for 5 min. Amastigotes were counted and suspended in hypotonic fluorochromic solution (HFS) [0.1% sodium citrate, 0.1% triton × 100, 50 μg/mL propidium iodide (PI)]. Samples were incubated for 4 h at 4 °C, protected from light. The readings were performed on flow cytometer (FacsCalibur®, BD, Franklin Lakes, NJ, USA), acquiring 50,000 events/sample. Data analysis was performed using FlowJo® software (FlowJo, LLC).
Experimental infection
THP-1 human monocytic lineage were cultured in complete RPMI-1640 medium (supplemented 10% fetal bovine serum, 2 mM glutamine, 100 U/mL penicillin and 100 μg/mL streptomycin) and differentiated into macrophages by the adding 20 ng/mL phorbol myristate acetate (PMA) in culture. Cells (3 × 105 macrophages/well) were seeded in 24 well cell culture plate containing 13 mm round coverslips and incubated for 72 h at 37 °C in a humid atmosphere containing 5% CO2. Similarly, the murine peritoneal macrophages elicited by thioglycollate were collected by washing the peritoneal cavity of BALB/c mice with RPMI-1640 medium and seeded as above. Macrophages (THP-1 and murine-derived ones) were incubated with parasites in the stationary phase (10 Leishmania per macrophage). After 3 h, uninternalized parasites were removed by successive washes. Parasite’s infectivity was monitored every 48 h. The coverslips were collected and stained by rapid panoptic method76. Briefly, the coverslips containing adhered infected macrophages were immersed in fixative solution (fast green in methanol) for 10 s, followed by the same procedure using stain solution 1 (eosin G in phosphate buffer – red colour) and stain solution 2 (thiazine dye in phosphate buffer – blue color). The coverslips were washed, dried and mounted in microscopy slides using Entellan® (Merk Millipore, Burlington, MA, USA). The infection was quantified by counting intracellular amastigotes using ImageJ software (imagej.nih.gov/ij).
Mice infection and parasite recovery
To evaluate the infectivity of the knockout mutants, BALB/c mice and IFN-γ−/− C57BL/6 mice were infected with WT and ΔLikh1 parasites. BALB/c mice were infected with amastigotes while C57BL/6 mice were infected with promastigotes forms. Amastigotes were previously recovered from THP-1 macrophages, as described in previous section ΔLikh1 cell cycle. In order to recover the parasites, spleens and livers of infected animals were collected 15 days after infection. Limiting dilution assays were performed as proposed by Titus et al.77. The organs of infected mice were processed using cell strainer (Corning, Corning, NY, USA) and the samples centrifuged at 134 × g for 10 min. The infected cells obtained from liver and spleen maceration were not lysed but suspended in α-MEM medium and added to the first wells of 96-well plates. From that initial concentration of cells, successive dilutions were made to the 12th well, using 10x dilution factor. Plates were incubated for 15 days at 26 °C and then evaluated for parasite growth.
Immunization and challenging assays
BALB/c female mice aged between 4–6 weeks old were divided into groups of at least 6 animals and immunized with 107 ΔLikh1 null mutant parasites, via tail vein (IV) in one or two dose schemes (Prime or Prime-Boost). A group receiving the same dose of parasites, but subcutaneously (SC) were also tested and the interval between the prime and boost were 20 days for all groups. Blood was collected at day 20 after priming and boosting, and serum was stored at −20 °C until analysis of IgG’s levels by ELISA. 20 days after the last immunization animals were infected with 107 LiWT virulent parasites given intravenously. 20 days after challenging animals were euthanized and evaluated for immunogenicity and protective effects induced by the vaccination schemes. The groups were established as following: PBS: LiWT- infected non-immunized mice; Prime-Boost (IV) CTRL: ΔLikh1-infected non-challenged (with LiWT) mice; Prime (IV): intravenously ΔLikh1-vaccinated mice once (prime) followed by LiWT challenge; Prime-Boost (IV): intravenously ΔLikh1-vaccinated mice twice (prime-boost) followed by LiWT challenge; Prime-Boost (SC): subcutaneously ΔLikh1-vaccinated mice twice (prime-boost) followed by LiWT challenge.
Soluble Antigen (SLA) preparation and antibody response
SLA was prepared as previously described78. Stationary-phase parasites were recovered, washed three times with PBS and suspended in lysis buffer containing 50 mM of Tris-HCl and 5 mM of EDTA at pH 7 (1 mL for every 109 cells). Parasites were then frozen and thawed 10 times in liquid nitrogen and water bath at 40 °C followed by 3 cycles of pulsed sonication, 20 seconds each, at 40 W (Q500 Ultrasonicator, QSonica®, Newtown, CT, USA). The preparation was centrifuged at 5000 × g for 20 minutes, suspended in the same buffer and the total amount of protein was quantified by spectrophotometry at ABS of 200 and 260 nm (Synergy 2 reader, BioTek Instruments, Inc., Winooski, VT, USA) with the predefined application of protein measurements in the Take3 Section of Gen5TM software v3.03. For IgG specific Ab responses, conventional ELISA method was used. Serum was analyzed for Th2-associated Ab, IgG1, and for Th1-associated Ab, IgG2a. Briefly, 96-wells plates were coated with 100 μL of a 25 μg/mL LiWT SLA solution and incubated at 4 °C overnight. After washes with PBS Tween 20 at 0.02% (PBST), serial dilutions of mice serums were added starting from 1:50. Peroxidase-conjugated rabbit anti-mouse IgG Total, IgG1 and IgG2 antibodies were added at a 1:5000 dilution for 1 h. The reaction was performed by addition of o-phenylenediamine and H2O2 (SigmaAldrich, St. Louis, MI, USA). After 15 min, the reaction was stopped by the addition of 100 μL of H2SO4 at 0.5 M. Absorbance at 492 nm. Cut-off values were calculated using the mean average OD of 60 negative samples plus 2 standard deviation and the endpoint IgG’s titers were calculated as previously described79.
Cytokine production assessments
Twenty days after priming (for one-dose vaccinated mice), boosting (for two-doses vaccinated mice) and challenging, 6 mice per group were euthanized, spleens were harvested and splenocytes were isolated as previously described80. Singled-cells preparations were adjusted for 107/mL and plated in 96-well flat-bottom tissue culture plate (Costar, Cambridge, MA, USA). Splenocytes were cultured at 37 °C, in 5%CO2 atmosphere in presence of 25 μg/mL SLAs, CpG-ODN (as a Th1-response inducer control) or supplemented medium (as a negative control). After 72 h incubation plates were centrifuged at 1000 × g for 10 min and supernatants were collected and analyzed for multiple cytokine production by flow cytometry with the BD Cytometric Bead Array (CBA) Mouse Th1/Th2/Th17 Cytokine Kit (BD Biosciences, San Jose, CA, USA) following manufacturer instructions. The acquisition and data analyses were made in BD FACSVerse Instrument and FCAP Array Software v3. The limit of detection of IL-2, IL-4, IL-6, IFN-γ, TNF, IL-17A and IL-10 cytokines were respectively 0,1; 0,03; 1,4; 0,5; 0,9; 0,8 and 16,8 pg/mL.
Evaluation of parasite burden
Twenty days after challenging, 6 mice per group were euthanized and their liver and spleen were collected in separated tubes containing PBS. The organs were macerated and an aliquot was added in a microtube containing lysis buffer and Proteinase K, vortexed and incubated at 56 °C overnight. After incubation, DNA was extracted with Illustra tissue & cells genomic Prep Mini Spin Kit (GE, Healthcare Lifesciences, Malborough, MA, USA), according to the manufacturer’s instructions. The gDNA concentrations were measured by spectrophotometry (Abs at 280/260 nm) and adjusted to 10 ng/μL. 5 μL of each sample was used to a final volume of 20 μL per reaction that included ultrapure water, SYBR Green/ROX qPCR Master Mix (Thermo Fisher Scientific, Waltham, MA, USA), sense (forward, 5′-CCTATTTTACACCAACCCCCAGT-3′, and antisense primers (reverse, 5′-GGGTAGGGGCGTTC TGCGAAA-3′), constructed for amplification of the mini-circle region present in the kinetoplast DNA (kDNA) of approximately 120 bp. The standard curve was constructed with serial dilutions of the known concentrations of gDNA of L. infantum, extracted from promastigote culture. Ultrapure water was used as negative control. The amplification protocol included an annealing temperature and extension of 60 °C, with melting curve construction, on the ABI 7500 equipment (Applied Biosystems, Thermo Fisher Scientific, Waltham, MA, USA) and the analysis were made using the 7500 System Software. The standard curve correlated the known amount of L. infantum gDNA with the cycle threshold (Ct) given by the amplification of each point of the curve. A linear regression analysis was applied to the curve and the amount of parasite gDNA in mass of each sample was obtained by interpolation in standard curve and converted into number of parasites, considering that each genomic DNA of L. infantum has about 0.1 pg of mass81. Before making data variance analysis, we performed a measurement of statistic dispersion by the IQR test (Interquartile range) in order to identify the outliers, but maintaining the minimum statistical accepted values which explains the variation in animal number per group.
Ethical statement
All procedures using animal models were previously approved by the institutional animal care committee: Ethics Committee for the Use of Animals – Oswaldo Cruz Foundation – CEUA/Fiocruz. All methods were performed in accordance with the guidelines and regulations from the National Council for the Control of Animal Experimentation – CONCEA and Canadian Council on Animal Care – CCAC, under license: CEUA #LW-28/14.
Statistical analysis
Statistical analyzes were performed with Kruskal Wallis non-parametric test and Dunns posttest (or Mann Whitney test) for non-normal distribution data; and the One-way ANOVA followed by Bonferroni’s multiple comparisons test (or students’ t test) for normal distribution data.
References
Alvar, J. et al. Leishmaniasis worldwide and global estimates of its incidence. PLoS One 7, e35671, https://doi.org/10.1371/journal.pone.0035671 (2012).
Kevric, I., Cappel, M. A. & Keeling, J. H. New World and Old World Leishmania Infections: A Practical Review. Dermatol Clin 33, 579–593, https://doi.org/10.1016/j.det.2015.03.018 (2015).
Deane, L. d. M. Visceral leishmaniasis in Brazil: studies on reservoirs and transmitters conducted in the state of Ceara. “Leishmaniose visceral no Brasil: estudo sobre reservatórios e transmissores realizados no Estado do Ceará.” Manuscript in Portuguese only PhD thesis, (São Paulo University, 1956).
Brazil, M. o. H. (ed. Publishing House of the Ministry of Health) 120 (Brasilia, 2006).
Srivastava, S., Shankar, P., Mishra, J. & Singh, S. Possibilities and challenges for developing a successful vaccine for leishmaniasis. Parasit Vectors 9, 277, https://doi.org/10.1186/s13071-016-1553-y (2016).
Singh, B. & Sundar, S. Leishmaniasis: vaccine candidates and perspectives. Vaccine 30, 3834–3842, https://doi.org/10.1016/j.vaccine.2012.03.068 (2012).
Seder, R. A. & Hill, A. V. Vaccines against intracellular infections requiring cellular immunity. Nature 406, 793–798, https://doi.org/10.1038/35021239 (2000).
Selvapandiyan, A. et al. Generation of growth arrested Leishmania amastigotes: a tool to develop live attenuated vaccine candidates against visceral leishmaniasis. Vaccine 32, 3895–3901, https://doi.org/10.1016/j.vaccine.2014.05.009 (2014).
Anand, S. & Madhubala, R. Genetically Engineered Ascorbic acid-deficient Live Mutants of Leishmania donovani induce long lasting Protective Immunity against Visceral Leishmaniasis. Sci Rep 5, 10706, https://doi.org/10.1038/srep10706 (2015).
Bhattacharya, P. et al. Genetically Modified Live Attenuated Leishmania donovani Parasites Induce Innate Immunity through Classical Activation of Macrophages That Direct the Th1 Response in Mice. Infect Immun 83, 3800–3815, https://doi.org/10.1128/IAI.00184-15 (2015).
Fiuza, J. A. et al. Vaccination using live attenuated Leishmania donovani centrin deleted parasites induces protection in dogs against Leishmania infantum. Vaccine 33, 280–288, https://doi.org/10.1016/j.vaccine.2014.11.039 (2015).
Silvestre, R., Cordeiro-da-Silva, A. & Ouaissi, A. Live attenuated Leishmania vaccines: a potential strategic alternative. Arch Immunol Ther Exp (Warsz) 56, 123–126, https://doi.org/10.1007/s00005-008-0010-9 (2008).
Kaye, P. M. & Aebischer, T. Visceral leishmaniasis: immunology and prospects for a vaccine. Clin Microbiol Infect 17, 1462–1470, https://doi.org/10.1111/j.1469-0691.2011.03610.x (2011).
Chhajer, R. & Ali, N. Genetically modified organisms and visceral leishmaniasis. Front Immunol 5, 213, https://doi.org/10.3389/fimmu.2014.00213 (2014).
Selvapandiyan, A. et al. Immunity to visceral leishmaniasis using genetically defined live-attenuated parasites. J Trop Med 2012, 631460, https://doi.org/10.1155/2012/631460 (2012).
Mitchell, G. F., Handman, E. & Spithill, T. W. Vaccination against cutaneous leishmaniasis in mice using nonpathogenic cloned promastigotes of Leishmania major and importance of route of injection. Aust J Exp Biol Med Sci 62(Pt 2), 145–153 (1984).
Gorczynski, R. M. Immunization of susceptible BALB/c mice against Leishmania braziliensis. II. Use of temperature-sensitive avirulent clones of parasite for vaccination purposes. Cell Immunol 94, 11–20 (1985).
Rivier, D., Shah, R., Bovay, P. & Mauel, J. Vaccine development against cutaneous leishmaniasis. Subcutaneous administration of radioattenuated parasites protects CBA mice against virulent Leishmania major challenge. Parasite Immunol 15, 75–84 (1993).
Kimsey, P. B., Theodos, C. M., Mitchen, T. K., Turco, S. J. & Titus, R. G. An avirulent lipophosphoglycan-deficient Leishmania major clone induces CD4+ T cells which protect susceptible BALB/c mice against infection with virulent L. major. Infect Immun 61, 5205–5213 (1993).
Daneshvar, H., Coombs, G. H., Hagan, P. & Phillips, R. S. Leishmania mexicana and Leishmania major: attenuation of wild-type parasites and vaccination with the attenuated lines. J Infect Dis 187, 1662–1668, https://doi.org/10.1086/374783 (2003).
Kaye, P. & Scott, P. Leishmaniasis: complexity at the host-pathogen interface. Nat Rev Microbiol 9, 604–615, https://doi.org/10.1038/nrmicro2608 (2011).
Liew, F. Y., Millot, S., Parkinson, C., Palmer, R. M. & Moncada, S. Macrophage killing of leishmania parasite in vivo is mediated by nitric oxide from L-arginine. J Immunol 144 (1990).
Nylen, S. & Gautam, S. Immunological perspectives of leishmaniasis. J Glob Infect Dis 2, 135–146, https://doi.org/10.4103/0974-777X.62876 (2010).
Bhattacharya, P. et al. Live Attenuated Leishmania donovani Centrin Knock Out Parasites Generate Non-inferior Protective Immune Response in Aged Mice against Visceral Leishmaniasis. PLoS Negl Trop Dis 10, e0004963, https://doi.org/10.1371/journal.pntd.0004963 (2016).
Banerjee, A. et al. Live Attenuated Leishmania donovani Centrin Gene-Deleted Parasites Induce IL-23-Dependent IL-17-Protective Immune Response against Visceral Leishmaniasis in a Murine Model. J Immunol 200, 163–176, https://doi.org/10.4049/jimmunol.1700674 (2018).
Tran, K. D. et al. KHARON1 mediates flagellar targeting of a glucose transporter in Leishmania mexicana and is critical for viability of infectious intracellular amastigotes. J Biol Chem 288, 22721–22733, https://doi.org/10.1074/jbc.M113.483461 (2013).
Tran, K. D. et al. Kharon1 null mutants of Leishmania mexicana are avirulent in mice and exhibit a cytokinesis defect within macrophages. PLoS One 10, e0134432, https://doi.org/10.1371/journal.pone.0134432 (2015).
Meng, J. et al. High-resolution crystal structures of villin headpiece and mutants with reduced F-actin binding activity. Biochemistry 44, 11963–11973, https://doi.org/10.1021/bi050850x (2005).
Friederich, E., Vancompernolle, K., Louvard, D. & Vandekerckhove, J. Villin function in the organization of the actin cytoskeleton. Correlation of in vivo effects to its biochemical activities in vitro. J Biol Chem 274, 26751–26760 (1999).
Sanchez, M. A. et al. KHARON Is an Essential Cytoskeletal Protein Involved in the Trafficking of Flagellar Membrane Proteins and Cell Division in African Trypanosomes. J Biol Chem 291, 19760–19773, https://doi.org/10.1074/jbc.M116.739235 (2016).
Cazzulo, J. J. Aerobic fermentation of glucose by trypanosomatids. FASEB J 6, 3153–3161 (1992).
Langford, C. K., Burchmore, R. J., Hart, D. T., Wagner, W. & Landfear, S. M. Biochemistry and molecular genetics of Leishmania glucose transporters. Parasitology 108(Suppl), S73–83 (1994).
Burchmore, R. J. & Landfear, S. M. Differential regulation of multiple glucose transporter genes in Leishmania mexicana. J Biol Chem 273, 29118–29126 (1998).
Burchmore, R. J. et al. Genetic characterization of glucose transporter function in Leishmania mexicana. Proc Natl Acad Sci USA 100, 3901–3906, https://doi.org/10.1073/pnas.0630165100 (2003).
Berman, J. D., Gallalee, J. V. & Best, J. M. Sodium stibogluconate (Pentostam) inhibition of glucose catabolism via the glycolytic pathway, and fatty acid beta-oxidation in Leishmania mexicana amastigotes. Biochem Pharmacol 36, 197–201 (1987).
Ashutosh, S. S. & Goyal, N. Molecular mechanisms of antimony resistance in Leishmania. J Med Microbiol 56, 143–153, https://doi.org/10.1099/jmm.0.46841-0 (2007).
Uzcategui, N. L., Figarella, K., Camacho, N. & Ponte-Sucre, A. Substrate preferences and glucose uptake in glibenclamide-resistant Leishmania parasites. Comp Biochem Physiol C Toxicol Pharmacol 140, 395–402, https://doi.org/10.1016/j.cca.2005.04.002 (2005).
Machuca, C., Rodriguez, A., Herrera, M., Silva, S. & Ponte-Sucre, A. Leishmania amazonensis: metabolic adaptations induced by resistance to an ABC transporter blocker. Exp Parasitol 114, 1–9, https://doi.org/10.1016/j.exppara.2006.02.008 (2006).
Monte-Neto, R. L. et al. Gene expression profiling and molecular characterization of antimony resistance in Leishmania amazonensis. PLoS Negl Trop Dis 5, e1167, https://doi.org/10.1371/journal.pntd.0001167 (2011).
Roberts, S. C. The genetic toolbox for Leishmania parasites. Bioeng Bugs 2, 320–326, https://doi.org/10.4161/bbug.2.6.18205 (2011).
Selvapandiyan, A. et al. Centrin gene disruption impairs stage-specific basal body duplication and cell cycle progression in Leishmania. J Biol Chem 279, 25703–25710, https://doi.org/10.1074/jbc.M402794200 (2004).
Dey, R. et al. Live attenuated Leishmania donovani p27 gene knockout parasites are nonpathogenic and elicit long-term protective immunity in BALB/c mice. J Immunol 190, 2138–2149, https://doi.org/10.4049/jimmunol.1202801 (2013).
Avishek, K. et al. Gene deleted live attenuated Leishmania vaccine candidates against visceral leishmaniasis elicit pro-inflammatory cytokines response in human PBMCs. Sci Rep 6, 33059, https://doi.org/10.1038/srep33059 (2016).
Mittal, N., Muthuswami, R. & Madhubala, R. The mitochondrial SIR2 related protein 2 (SIR2RP2) impacts Leishmania donovani growth and infectivity. PLoS Negl Trop Dis 11, e0005590, https://doi.org/10.1371/journal.pntd.0005590 (2017).
Zhang, W. W. & Matlashewski, G. Loss of virulence in Leishmania donovani deficient in an amastigote-specific protein, A2. Proc Natl Acad Sci USA 94, 8807–8811 (1997).
Papadopoulou, B. et al. Reduced infectivity of a Leishmania donovani biopterin transporter genetic mutant and its use as an attenuated strain for vaccination. Infect Immun 70, 62–68 (2002).
Gannavaram, S. et al. Whole genome sequencing of live attenuated Leishmania donovani parasites reveals novel biomarkers of attenuation and enables product characterization. Sci Rep 7, 4718, https://doi.org/10.1038/s41598-017-05088-4 (2017).
Solana, J. C. et al. Vaccination with a Leishmania infantum HSP70-II null mutant confers long-term protective immunity against Leishmania major infection in two mice models. PLoS Negl Trop Dis 11, e0005644, https://doi.org/10.1371/journal.pntd.0005644 (2017).
Mittra, B., Laranjeira-Silva, M. F., Miguel, D. C., Perrone Bezerra de Menezes, J. & Andrews, N. W. The iron-dependent mitochondrial superoxide dismutase SODA promotes Leishmania virulence. J Biol Chem 292, 12324–12338, https://doi.org/10.1074/jbc.M116.772624 (2017).
Paiva, R. M. et al. Amastin Knockdown in Leishmania braziliensis Affects Parasite-Macrophage Interaction and Results in Impaired Viability of Intracellular Amastigotes. PLoS Pathog 11, e1005296, https://doi.org/10.1371/journal.ppat.1005296 (2015).
Buxbaum, L. U. et al. Cysteine protease B of Leishmania mexicana inhibits host Th1 responses and protective immunity. J Immunol 171, 3711–3717 (2003).
Nadim, A., Javadian, E., Tahvildar-Bidruni, G., Amini, H. & Pezechki, Y. Control of zoonotic cutaneous leishmaniasis by mass leishmanization in hyperendemic area of Isfahan. Medical Journal of the Islamic Republic of Iran 2, 2 (1988).
Nadim, A., Javandian, E. & Mohebali, M. The experience of leishmanization in the islamic republic of Iran. La Revue de Santé de la Méditerranée orientale 3, 6 (1997).
Streit, J. A., Recker, T. J., Filho, F. G., Beverley, S. M. & Wilson, M. E. Protective immunity against the protozoan Leishmania chagasi is induced by subclinical cutaneous infection with virulent but not avirulent organisms. J Immunol 166, 1921–1929 (2001).
Dunnig, N. Leishmania vaccines: from leishmanization to the era of DNA technology. The International Journal of Student Research 2, 9, https://doi.org/10.1093/biohorizons/hzp004 (2009).
Saljoughian, N., Taheri, T. & Rafati, S. Live vaccination tactics: possible approaches for controlling visceral leishmaniasis. Front Immunol 5, 134, https://doi.org/10.3389/fimmu.2014.00134 (2014).
Breton, M., Tremblay, M. J., Ouellette, M. & Papadopoulou, B. Live nonpathogenic parasitic vector as a candidate vaccine against visceral leishmaniasis. Infect Immun 73, 6372–6382, https://doi.org/10.1128/IAI.73.10.6372-6382.2005 (2005).
Moore, J. W. et al. B cell: T cell interactions occur within hepatic granulomas during experimental visceral leishmaniasis. PLoS One 7, e34143, https://doi.org/10.1371/journal.pone.0034143 (2012).
Ghosh, A., Zhang, W. W. & Matlashewski, G. Immunization with A2 protein results in a mixed Th1/Th2 and a humoral response which protects mice against Leishmania donovani infections. Vaccine 20, 59–66 (2001).
Snapper, C. M. & Paul, W. E. Interferon-gamma and B cell stimulatory factor-1 reciprocally regulate Ig isotype production. Science 236, 944–947 (1987).
Miyazaki, Y. et al. IL-17 is necessary for host protection against acute-phase Trypanosoma cruzi infection. J Immunol 185, 1150–1157, https://doi.org/10.4049/jimmunol.0900047 (2010).
Bertholet, S. et al. Optimized subunit vaccine protects against experimental leishmaniasis. Vaccine 27, 7036–7045, https://doi.org/10.1016/j.vaccine.2009.09.066 (2009).
Coler, R. N., Goto, Y., Bogatzki, L., Raman, V. & Reed, S. G. Leish-111f, a recombinant polyprotein vaccine that protects against visceral Leishmaniasis by elicitation of CD4+ T cells. Infect Immun 75, 4648–4654, https://doi.org/10.1128/IAI.00394-07 (2007).
Goto, Y., Bogatzki, L. Y., Bertholet, S., Coler, R. N. & Reed, S. G. Protective immunization against visceral leishmaniasis using Leishmania sterol 24-c-methyltransferase formulated in adjuvant. Vaccine 25, 7450–7458, https://doi.org/10.1016/j.vaccine.2007.08.001 (2007).
Grimaldi, G. Jr. et al. Clinical and parasitological protection in a Leishmania infantum-macaque model vaccinated with adenovirus and the recombinant A2 antigen. PLoS Negl Trop Dis 8, e2853, https://doi.org/10.1371/journal.pntd.0002853 (2014).
Korn, T., Bettelli, E., Oukka, M. & Kuchroo, V. K. IL-17 and Th17 Cells. Annu Rev Immunol 27, 485–517, https://doi.org/10.1146/annurev.immunol.021908.132710 (2009).
Bermejo, D. A. et al. Trypanosoma cruzi trans-sialidase initiates a program independent of the transcription factors RORgammat and Ahr that leads to IL-17 production by activated B cells. Nat Immunol 14, 514–522, https://doi.org/10.1038/ni.2569 (2013).
Sporri, R. & Reis e Sousa, C. Inflammatory mediators are insufficient for full dendritic cell activation and promote expansion of CD4+ T cell populations lacking helper function. Nat Immunol 6, 163–170, https://doi.org/10.1038/ni1162 (2005).
Foulds, K. E., Wu, C. Y. & Seder, R. A. Th1 memory: implications for vaccine development. Immunol Rev 211, 58–66, https://doi.org/10.1111/j.0105-2896.2006.00400.x (2006).
Silva, J. L. et al. IL-17-expressing CD4(+) and CD8(+) T lymphocytes in human toxoplasmosis. Mediators Inflamm 2014, 573825, https://doi.org/10.1155/2014/573825 (2014).
Monte-Neto, R. et al. Intrachromosomal amplification, locus deletion and point mutation in the aquaglyceroporin AQP1 gene in antimony resistant Leishmania (Viannia) guyanensis. PLoS Negl Trop Dis 9, e0003476, https://doi.org/10.1371/journal.pntd.0003476 (2015).
Cruz, A. & Beverley, S. M. Gene replacement in parasitic protozoa. Nature 348, 171–173, https://doi.org/10.1038/348171a0 (1990).
Robinson, K. A. & Beverley, S. M. Improvements in transfection efficiency and tests of RNA interference (RNAi) approaches in the protozoan parasite Leishmania. Mol Biochem Parasitol 128, 217–228 (2003).
Green, M. R. & Sambrook, J. Molecular Cloning a Laboratory Manual. 4th edn, Vol. 1 1881 (Cold Spring Harbor Laboratory Press, 2012).
Mosmann, T. Rapid colorimetric assay for cellular growth and survival: application to proliferation and cytotoxicity assays. J Immunol Methods 65, 55–63 (1983).
Mallik, M. K., Das, D. K. & Haji, B. E. Fine needle aspiration cytology diagnosis of cutaneous leishmaniasis in a 6-month-old child: a case report. Acta Cytol 45, 1005–1007, https://doi.org/10.1159/000328345 (2001).
Titus, R. G., Marchand, M., Boon, T. & Louis, J. A. A limiting dilution assay for quantifying Leishmania major in tissues of infected mice. Parasite Immunol 7, 545–555 (1985).
Carrillo, E. et al. Cytokine Release Assays as Tests for Exposure to Leishmania, and for Confirming Cure from Leishmaniasis, in Solid Organ Transplant Recipients. PLoS Negl Trop Dis 9, e0004179, https://doi.org/10.1371/journal.pntd.0004179 (2015).
Graham, D. A. et al. Standardization of enzyme-linked immunosorbent assays (ELISAs) for quantitative estimation of antibodies specific for infectious bovine rhinotracheitis virus, respiratory syncytial virus, parainfluenza-3 virus, and bovine viral diarrhea virus. J Vet Diagn Invest 9, 24–31, https://doi.org/10.1177/104063879700900105 (1997).
Scott, P., Natovitz, P., Coffman, R. L., Pearce, E. & Sher, A. Immunoregulation of cutaneous leishmaniasis. T cell lines that transfer protective immunity or exacerbation belong to different T helper subsets and respond to distinct parasite antigens. J Exp Med 168, 1675–1684 (1988).
Nicolas, L., Prina, E., Lang, T. & Milon, G. Real-time PCR for detection and quantitation of leishmania in mouse tissues. J Clin Microbiol 40, 1666–1669 (2002).
Acknowledgements
The authors thank the Program for Technological Development in Tools for Health-PDTIS-FIOCRUZ and its facilities. We thank Dr. Marc Ouellette, CHU de Québec – Université Laval, QC, Canada, for assistance on southern blot as well as for providing Leishmania infantum strain pSP72αHYGα vector. We thank the MSc student Ana Carolina Borges de Oliveira for technical assistance on in vivo assays. We thank Celeste Romero, San Diego State University, CA, USA, for her constructive criticism and diligent proofreading of this manuscript. This work was funded by the National Council for Scientific and Technological Development (CNPq Chamada Universal – grant number: 429625/2016-2). RLMN and SMFM are CNPq Research Productivity Fellows. AMM Santi received a Master’s Fellowship from CNPq and LGT receives a PhD fellowship from CAPES – Coordination for the improvement of higher education personnel.
Author information
Authors and Affiliations
Contributions
Conceptualization and design the experiments: J.A.F., F.F., J.S.L., R.L.M.N. Investigation: A.M.M.S., J.S.L., L.G.T., G.R. Analyzed the data: A.M.M.S., J.S.L., A.T.C. Contributed with reagents/materials/analysis/tools: S.M.F.M., A.T.C., F.F., A.S.O., A.L.B.B. Supervision: S.M.F.M., R.L.M.N. Writing – original draft: S.M.F.M., A.M.M.S. Writing – review and editing: L.G.T., J.S.L., J.A.F., F.F., A.L.B.B., R.L.M.N.
Corresponding author
Ethics declarations
Competing Interests
The authors declare no competing interests.
Additional information
Publisher's note: Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made. The images or other third party material in this article are included in the article’s Creative Commons license, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons license and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this license, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Santi, A.M.M., Lanza, J.S., Tunes, L.G. et al. Growth arrested live-attenuated Leishmania infantum KHARON1 null mutants display cytokinesis defect and protective immunity in mice. Sci Rep 8, 11627 (2018). https://doi.org/10.1038/s41598-018-30076-7
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41598-018-30076-7
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.