Abstract
The intestinal microbiota contributes to the global wellbeing of their host by their fundamental role in the induction and maintenance of a healthy immune system. Commensal bacteria shape the mucosal immune system by influencing the proportion and the activation state of anti-inflammatory regulatory T cells (Treg) by metabolites that are still only partially unravelled. Microbiota members such as Clostridiales provide a transforming growth factor β (TGFβ)-rich environment that promotes the accumulation of Treg cells in the gut. The intestinal epithelial cells (IECs) take a central part in this process, as they are a major source of TGFβ1 upon bacterial colonisation. In this study, we investigated which gut commensal bacteria were able to regulate the TGFB1 human promoter in IECs using supernatants from cultured bacteria. We reported that Firmicutes and Fusobacteria supernatants were the most potent TGFB1 modulators in HT-29 cells. Furthermore, we demonstrated that butyrate was the main metabolite in bacterial supernatants accounting for TGFβ1 increase. This butyrate-driven effect was independent of the G-protein coupled receptors GPR41, GPR43 and GPR109a, the transporter MCT1 as well as the transcription factors NF-κB and AP-1 present on TGFB1 promoter. Interestingly, HDAC inhibitors were inducing a similar TGFB1 increase suggesting that butyrate acted through its HDAC inhibitor properties. Finally, our results showed that SP1 was the main transcription factor mediating the HDAC inhibitor effect of butyrate on TGFB1 expression. This is, to our knowledge, the first characterisation of the mechanisms underlying TGFB1 regulation in IEC by commensal bacteria derived butyrate.
Similar content being viewed by others

Introduction
Humans are colonized by bacteria, archaea, eukaryotes and viruses, which are collectively called the microbiota. These organisms exert diverse functions often associated with beneficial physiological effects for the host. Numerous studies suggest that indigenous members of the microbiota are central for the fine regulation of the host immune system through their intimate interaction with the host epithelium1,2,3,4,5. The composition of the host intestinal microbiota shapes the mucosal and the systemic immune responses in part by influencing the proportion and the activation state of T cell subsets. Among them the intestinal Foxp3+ regulatory T cells (Treg) play a central role in maintaining immunological homeostasis and their proportion is highly related to the microbiota composition4,6,7,8,9. Two studies showed that complex mixtures of Clostridiales bacteria from clusters IV and XIVa or a single Clostridium species cluster I, provide a transforming growth factors β1 (TGFβ1)-rich environment that promotes the accumulation of induced Treg cells (iTreg)4,9. Interestingly, in inflammatory bowel diseases (IBD) known to be linked to commensal bacteria composition, Clostridiales clusters IV and XIVa are significantly less abundant and the pathology have been reported to be associated with an impairment of TGFβ signalling in numerous immune cell types including T cells10,11,12,13,14,15,16.
The molecular mechanisms of Treg cell generation by the microbiota have only been partially unravelled4,6,7,8,9. Several groups have shown that short chain fatty acids (SCFAs), such as butyrate, that derived from the bacterial fermentation of dietary fibres promote Treg cell generation6,8. Butyrate acts as an inhibitor of histone deacetylases (iHDACs) and consequently enhances histone H3 acetylation in the regulatory elements of the Foxp3 locus. However, in vitro Treg generation is not induced directly by SCFAs alone and requires TGFβ1 stimulation6,8. Moreover, TGFβ1 is essential for Treg differentiation by butyrate-producing bacteria in vivo4.
In the gut, dendritic cells (DC) and intestinal epithelial cells (IEC) are the major cellular sources of TGFβ14,9,17,18,19. Interestingly, germ-free mice colonisation by certain members of the microbiota leads to enhanced TGFβ1 expression in IECs and the almost complete restoration of colonic Treg level4,9,20,21. A recent study demonstrated that Clostridium butyricum increased iTreg generation via a Toll-like receptor 2 (TLR2)-dependent induction of TGFβ1 by DCs. This was the first demonstration of a mechanism deployed by a member of the gut microbiota to activate TGFβ1 secretion leading to Treg cells generation9.
The TGFB1 auto-induction loop is well documented. Addition of TGFβ1 activates TGFβ1 receptor leading to a SMAD and MAPK-dependent downstream signalling22. However, there are only few mechanical insights on TGFB1 regulation by exogenous signals. Indeed, TGFβ1 induction by commensal bacteria is promoting the proliferation, polarization and differentiation of T lymphocytes but the involved molecules or pathways are still unknown4. We thus decided to investigate the impact of individual cultivable commensal bacteria on TGFB1 transcriptional expression in a human IEC model and to further characterise the underlying molecular mechanisms.
In the current study, we screened bacterial supernatants derived from over 120 commensal species on a TGFB1 reporter system and showed that butyrate was the main microbiota-derived metabolite inducing TGFB1 expression in the human intestinal epithelial cell-line HT-29. We showed that the TGFB1 induction by butyrate was independent of the SCFA G-protein coupled receptors (GPR41, GPR43 and GPR109a), and of the SCFA transporter monocarboxylate transporter 1 (MCT1). Moreover, the TGFB1 up-regulation could be attributed to the HDAC inhibitory properties of SCFAs. Finally, by using specific inhibitors and point mutations of the promoter region of TGFB1, we excluded NFκB and AP1 as regulatory elements and showed that the SP1 transcription factor was involved in the butyrate-driven activation of TGFB1 expression.
Results
Metabolites derived from commensal bacteria modulate TGFβ1 expression
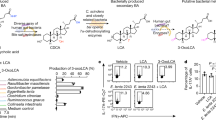
TGFβ1 expression is severely decreased in the colon of germ-free mice compared to colonised mice suggesting a crucial role of the microbiota in this process4. The impact of bacterial metabolites is particularly drastic on TGFβ1 production by IEC although no mechanism has been described at the moment. Thus, to decipher which commensal bacteria regulate TGFB1 expression; we have studied the activity of more than a hundred bacterial species, including 60% of the bacteria belonging to the human core microbiota, on a TGFB1 reporter system expressed in the human IEC line HT-2923. Previous publications have reported that active biological compounds produced by bacteria in the gut are likely to be small diffusible molecules, thus we tested bacterial supernatants on a HT-29-TGFprom reporter system (Fig. 1A)11,24,25,26. Our results showed that species belonging to the Firmicutes and Fusobacteria phyla were the main TGFB1 inducers while some members of Actinobacteria were inhibitors. At the genus level, Clostridiales and Fusobacterium were highly increasing TGFB1 expression. Lactobacillus and Bifidobacterium were decreasing TGFB1 activity however, these effects were not found in all the tested species (Supplementary Fig. 1).
Correlation between bacterial metabolites production and TGFB1 gene expression. (A) Effect of bacterial supernatants on HT-29-TGFprom reporter system organised by phylum. Culture supernatants of a wide range of commensal bacteria were applied on the HT-29-TGFprom reporter system (10% vol/vol). TGFB1 expression was measured by luciferase activity and expressed as fold change towards its control: bacterial growth medium used in each experiment and bacterial culture. Dash lines draw upper and lower zones where TGFB1 was consider as significantly changed. (B) PCA analysis showing the correlation between the SCFA concentrations produced the commensal bacteria and the TGFB1 expression. (C) Representation of TGFB1 expression correlated to butyrate concentration in different bacterial cultures ordered ranked values (Spearman correlation, r = 0.455, p-value = 1.302e-15). Actinobacteria in blue, Bacteroidetes in yellow, Firmicutes in grey, Fusobacteria in red and Verrucomicrobiea in light blue.
Butyrate activates TGFB1 expression in epithelial cell line
A common characteristic of the main TGFB1 inducers, Clostridiales and Fusobacterium, is their capacity to degrade complex dietary fibres by anaerobic fermentation27. As SCFAs are major end-products of this anaerobic fermentation with important impacts on human health, we thus quantified the concentrations of acetate, butyrate, propionate, valerate as well as isobutyrate and isovalerate in bacterial supernatants (Supplementary Table 1). Global correlation analysis by principal component (PCA) of all the SCFAs concentrations and TGFB1 expression showed that butyrate was the only SCFA for which the concentration correlated to TGFB1 activity (Fig. 1B). In addition, this association was confirmed by a Spearman pairwise correlation between butyrate and TGFB1, on ranked data (Fig. 1C).
We confirmed experimentally the observed correlation by testing a large range of physiological concentrations of SCFAs on HT-29-TGFprom reporter cells. As shown in Fig. 2A, butyrate was a potent TGFB1 inducer with a significant impact at concentration starting at 1 mM. Interestingly, other SCFAs such as propionate, valerate and isovalerate activated TGFB1 but to a lesser extent (Fig. 2A,B). The most abundant SCFA produced by gut bacteria, acetate, had no impact on TGFB1 expression. Moreover, we demonstrated that SCFAs not only increased TGFB1 gene activity but also enhance TGFβ1 protein level as assayed by ELISA (Fig. 2C).
Impact of SCFAs on TGFB1 expression. (A) HT-29-TGFprom reporter cells were incubated for 24 h with a range of concentrations of acetate, propionate and butyrate (0.5, 1, 2, 4, 8 mM). (B) HT-29-TGFprom reporter cells were incubated for 24 h with a range of concentrations of isobutyrate, isovalerate and valerate (0.5, 1, 2, 4, 8 mM). TGFB1 expression was measured by luciferase activity and expressed as the mean ± SD of fold change towards un-stimulated cells, N ≥ 3, (C) HT-29 cells were incubated for 24 h with IL1β (10 ng/ml), butyrate 2 mM, propionate 4 mM or acetate 8 mM. TGFβ1 active and latent levels were measured by ELISA and expressed as median ± quartiles, expressed in pg/ml. N = 3, t-test, *P < 0.05, **P < 0.01, ***P < 0.001.
Butyrate-driven activation of TGFB1 is independent of the SCFA receptors GPR41, GPR43, GPR109a and the SCFA transporter MCT1
SCFAs induce numerous signalling pathways through their binding to three different G-protein coupled receptors (GPR): GPR41, GPR43 and GPR109a. These receptors display affinities for SCFAs leading to cellular signals28,29,30. The three GPRs were found expressed in HT-29 cell line (Supplementary Fig. 2A). To investigate the potential role of these receptors on TGFB1 expression, we tested specific agonists of GPR41 (1-MCPC and AR420626), GPR43 (Tiglic acid and 4-CMTB) and GPR109a (Niacin and MK1903) on HT-29-TGFprom reporter system. None of the agonists was able to mimic the effect of butyrate on TGFB1 expression suggesting that these GPRs were not involved in this process (Fig. 3A). Upon ligand binding, GPRs signal through two G-protein subunits activation: Gα/i (for GPR41, GPR43 and GPR109a) and Gα/q (for GPR43). To confirm our observation, we used Gi/o and Gq inhibitors, the pertussis toxin (Ptx) and phospholipase Cβ inhibitor (U73122) respectively. Interestingly, none of the inhibitors was able to block the butyrate-dependent up-regulation of TGFB1 expression (Fig. 3B). Moreover, over-expression of GPR43 and GPR109a in HT-29-TGFprom reporter cells did not impact the butyrate-dependent activation of TGFB1 expression, strengthening the hypothesis of a GPR-independent mechanism (Supplementary Fig. 2B and C).
Butyrate mediated impact on TGFB1 is independent of GPR41, GPR43, GPR109a receptors and MCT1 transporter. (A) HT-29-TGFprom reporter cells were incubated for 24 h with selective GPR agonists: GPR41: AR420626 (1 μM) and 1-MCPC (1 mM); GPR43: 4-CMTB (1 μM) and Tiglic acid (1 mM); GPR109a: Niacin (1 mM) and MK1903 (1 μM) or with DMSO (vehicle) or butyrate (2 mM). (B) HT-29-TGFprom reporter cells were incubated with GPRs sub-unit inhibitors: Pertussis toxin 2 h before (Ptx, 0.2 μg/ml) and U73122 (10 μM) prior butyrate 2 mM stimulation and left for a total 24 h of incubation. (C), HT-29-TGFprom reporter cells were incubated for 24 h with selective MCT1 inhibitors: pCMB (100 μM) and AR-C155858 (400 nM),. TGFB1 expression was measured by luciferase activity and expressed as median ± quartiles of fold change towards un-stimulated cells. N ≥ 3, Wilcoxon test, *P < 0.05, **P < 0.01, ***P < 0.001.
Monocarboxylate transporter 1 (MCT1) has been described as the main butyrate transporter in the colon and is largely expressed in HT-29 cells (Supplementary Fig. 2A)31,32. We thus investigated if butyrate uptake by monocarboxylate transporter 1 (MCT1) was involved in TGFB1 up-regulation. Incubation of HT-29-TGFprom cells with two different MCT1 inhibitors, pCMB and AR-C15858, had no impact on the butyrate-induced activation of TGFB1, suggesting that MCT1 was not involved in the butyrate-driven up-regulation of TGFB1 (Fig. 3C).
Butyrate induces TGFB1 expression via its HDAC inhibitor property
It is well established that SCFAs, and butyrate in particular, rely on their lysine and histone deacetylase inhibition (HDACi) property to modulate histone acetylation, transcription factor acetylation and binding, and consequently gene expression5,33,34,35. Butyrate targets class I and class II HDAC and thus modulates the expression of a wide range of genes36. To asses if butyrate HDACi property was involved in TGFB1 up-regulation, we tested two HDACi targeting zinc dependent class I and II HDAC families. We treated HT-29-TGFprom reporter cells with trichostatin A (TSA) and vorinostat (SAHA) both sharing a hydroxynamic acid structure, different from butyrate which belongs to the aliphatic family33,36. Interestingly, both TSA and SAHA mimicked butyrate effect by increasing TGFB1 activity, suggesting that the butyrate-driven up-regulation of TGFB1 might be a consequence of its HDAC inhibitory properties (Fig. 4).
HDAC inhibitor mimicked the butyrate-dependent activation of TGFB1 expression. HT-29-TGFprom reporter cells were incubated with butyrate (2 mM), SAHA (5 μM), trichostatin A, (TSA, 1 μM) or controls (DMSO and RPMI). TGFB1 expression was measured by luciferase activity and expressed as fold increase towards the control: un-stimulated cells. Data are represented as median ± quartiles of fold change towards un-stimulated cells. N ≥ 3, Wilcoxon test, *P < 0.05, **P < 0.01, ***P < 0.001.
Butyrate-induced TGFB1 expression is independent of NF-κB and AP-1 and relies on SP1
Regulation of gene transcription by butyrate involves a wide range of transcription factors. To delineate which transcription factors (TF) are targeted by butyrate and might directly impact TGFB1 expression, we analysed the human TGFB1 promoter sequence. As expected from previous publications, we found several binding sites for transcription factors implicated in HDACi and butyrate-regulated gene expression including Specificity Protein-1 (SP1) binding GC-rich boxes, Activator protein 1 (AP-1) and NF-κB responsive elements (Table 1)37,38,39,40,41,42,43,44,45. Previous work reported that some of these binding sites were functional. Indeed an AP-1 and a SP1 binding sites have been described as main regulators of the TGFB1 gene activity in different cell types at steady state and upon infection46,47. NF-κB was shown to increase TGFB1 expression in cooperation with AP-148.
To investigate which transcription factor controls the butyrate-induced up-regulation of TGFB1, we first treated HT-29-TGFprom reporter cells with an AP-1 specific inhibitor (SR11302) in presence or absence of butyrate (Fig. 5A). The AP-1 inhibitor was not able to block the butyrate-induced TGFB1 increase suggesting that this transcription factor was not involved. Then, we treated HT-29-TGFprom reporter cells with an NF-κB inhibitor (BAY 117082) prior to butyrate stimulation (Fig. 5B). We observed that NF-κB inhibition did not impact significantly butyrate enhancement of TGFB1. Interestingly, butyrate did not activate the NF-κB pathway in a HT-29 NF-κB reporter system confirming that this transcription factor had no role in butyrate-dependent TGFB1 induction (Supplementary Fig. 3A). To explore SP1 implication in the induction of TGFB1 in our model, we incubated HT-29-TGFprom reporter cells with butyrate or HDACi in presence of mithramycin A, a competitive SP1/SP3 inhibitor. Binding inhibition to GC rich sequence by mithramycin A drastically inhibited TGFB1 up-regulation by butyrate (Fig. 5C). We also observed a diminution of the butyrate-dependent activation of TGFB1 by inhibiting SP1 expression by siRNA thus strengthening our previous result (Supplementary Fig. 3B). These results suggest that the induction of TGFB1 expression by butyrate is mediated through SP1 binding to GC rich response element. Furthermore, TSA and SAHA impacts on TGFB1 expression were also abrogated by SP1 knockdown or mithramycin A competition (Fig. 5C and Supplementary Fig. 3B).
Butyrate activated TGFB1 expression in a NF-κB-independent, AP1-independent-manner. (A) HT-29-TGFprom reporter cells were stimulated for 24 h with SR11302 (10 µM) a specific AP-1 inhibitor in presence or absence of butyrate (But 2 mM). Wilcoxon test,, N = 4; (B) HT-29-TGFprom cells were incubated with BAY11-7082 40 µM 2 h prior incubation with butyrate (But 2 mM) or controls. T-test, N = 3; (C) HT-29-TGFprom cells were incubated for 24 h with mithramycin A (100 nM) and butyrate or HDACi, t-test, N ≥ 3. TGFB1 expression was measured by luciferase activity and expressed as fold increase towards un-stimulated cells. Data are represented as median ± quartiles of fold change. *P < 0.05, **P < 0.01, ***P < 0.001.
We further characterised which region of TGFB1 promoter was responsible for the butyrate dependent activation of TGFB1. Two truncated TGFB1 promoter constructs were generated and stably transfected into HT-29 cells. HT-29-TGF−1362/+11 and HT-29-TGF−453/+11 reporter cells were treated with butyrate and HDAC inhibitors (Fig. 6A,B). The effect of butyrate and HDACi on luciferase expression was observed in both constructs suggesting a cis-regulatory element activity present in the core promoter, close to the 5′ UTR region (Fig. 6B).
TGFB1 up-regulation by butyrate and HDACi is SP1-dependent (A) Schematic representation of the human TGFB1 promoter with a selection of binding motifs37,38,46,47. The translation (ATG) and transcription start sites (+1) were defined by65,66. Mutations of AP-1 and SP1 boxes on HT-29-TGF−453/+11 are represented. (B) HT-29-TGF−1362/+11, HT-29-TGF−453/+11, HT-29-TGF−453/+11SP1 reporter cells were stimulated for 24 h with butyrate (4 mM), TSA (1 µM) or SAHA (5 µM). TGFB1 expression was measured by luciferase activity and expressed as fold increase towards un-stimulated cells. Data are represented as median ± quartiles of fold change. N ≥ 3, t-test, *P < 0.05, **P < 0.01, ***P < 0.001.
As shown in Fig. 6A, several functional AP-1 (−416, −370) and SP1 (−216) responsive elements have been identified in the TGFB1 core promoter46,47. To assess the role of the AP-1 (−416, −370) and SP1 (−216) binding sites, we stably transfected HT-29 cells with the TGF−453/+11 reporter system with a double mutations of the AP-1 motifs or a single mutation on the SP1 motif (HT-29-TGF−453/+11AP1 and HT-29-TGF−453/+11SP1 respectively, Fig. 6A). Mutations of the AP-1 motifs did not prevent the activation by butyrate and others HDACi confirming our results with AP-1 inhibitor (Supplementary Fig. 4). Mutation of one SP1 binding site was sufficient to severely reduce the TGFB1 promoter activation by butyrate and HDACi, confirming that SP1 is involved in this process (Fig. 6B). Altogether our results showed that butyrate and HDACi induce TGFB1 up-regulation independently of NF-κB and AP-1 and through the −216 SP1 site.
Bacterial induction of TGFB1 is butyrate and SP1-dependent
The main purpose of this study was to investigate the molecular mechanism by which commensal bacteria induce TGFB1 expression in epithelial cells. We thus incubated a selection of TGFB1-inducing bacterial supernatants on HT-29-TGFprom cells in presence of SP1/SP3 inhibitor (mithramycin A). As shown in Fig. 7, inhibition of SP1/SP3 binding motifs had a similar impact on butyrate and bacterial-induced up-regulation of TGFB1. The commensal bacteria selected throughout our screen due to their ability to increase TGFB1, were all butyrate-producing bacteria. Our results demonstrate the crucial role of SP1 in the TGFB1 expression induced by butyrate from commensal bacteria.
SP1-inhibitor mithramycin inhibited TGFB1 induction by the butyrate-producing bacteria. HT-29-TGFprom cells were incubated for 24 h with bacterial supernatants (10% (v/v)) or butyrate (But 2 mM) ± mithramycin A (100 nM). TGFB1 expression was measured by luciferase activity and expressed as fold increase towards un-stimulated cells. Data are represented as median ± quartiles of fold change.
Discussion
TGFβ1 is a pleiotropic cytokine highly conserved among metazoan and secreted in its latent form. Produced by many cell and tissue types, TGFβ1 is involved in various biological functions including pluripotency, tissue morphogenesis, cellular differentiation and regeneration49. As a crucial cytokine of tissue homeostasis, TGFβ misregulations are involved in many pathologies such as cancer, fibrosis, asthma, infections and inflammatory diseases. More specifically, TGFβ1, the most abundant TGFβ isoform, plays complex roles in the gut immune response regulation50.
Several studies highlighted the importance of TGFβ1 as a negative regulator of mucosal inflammatory responses and showed that defects in its expression or signalling lead to colitis4,9,13,14,15. In human, SMAD3 an intracellular molecule involved in the TGFβ signalling pathway is among the loci associated with high IBD susceptibility22,51. Moreover, defective TGFβ1 signalling in IBD patients has been associated with high SMAD7 expression, an inhibitor of SMAD2/3 phosphorylation. SMAD7 deleterious effects can be reversed by treatment with a SMAD7 antisense nucleotide13,14,15. Many studies demonstrated the involvement of gut microbiota in the development of the local and systemic immune system notably by the modification of regulatory T cell (Treg) differentiation4,6,7,8,9. In the gut, dendritic cells (DC) and intestinal epithelial cells (IECs) are the major cellular sources of TGFβ1 induced by the microbiota that is essential for the generation of Treg cells4,9,17,20. Although IECs are not the main TGFβ1 producers per se, yet they are an important source of this cytokine when considering the huge number of cells they represent in the gut19. Moreover, IECs are at the interface between the microbiota and the lamina propria and are thus more likely to be influenced by commensal bacteria in particular in making the gut a TGFβ1-rich environment17,52.
Here, we demonstrated that, amongst the microbial metabolites produced by the commensal bacteria tested, short chain fatty acids (SCFAs), and more specifically butyrate, had a major impact on human TGFB1 expression in IECs (Fig. 1). We showed that physiological concentrations of butyrate up-regulated the expression of TGFB1 in HT-29 (Fig. 2). Our findings confirmed previous studies showing that butyrate is a potent TGFB1 inducer in diverse cell types including IECs4,53,54,55. We investigated the mechanism of butyrate-driven TGFB1 induction. In assays using GPRs ligands, G-protein sub-units inhibitors and GPR over-expression, we established that butyrate impact on TGFB1 was independent of GPR43, GPR41 and GPR109a. Similarly, inhibition of the MCT1 transporter did not abrogate butyrate effect, pointing out that butyrate uptake by MCT1 was dispensable (Fig. 3). Yet, MCT1 belongs to a large family of transporter (MCTs) mediating monocarboxylate uptake from gut lumen to cell cytoplasm. Among MCTs, MCT1 is the most expressed in the human large intestine but we cannot exclude that other expressed isoforms such as MCT4 may be involved in butyrate transport56,57. It is also possible that butyrate enters the cell via passive transport or diffusion31,32,56,57. SCFAs, particularly butyrate, impact the host biological responses by the direct regulation of gene transcription via their properties of histone deacetylase inhibitors (HDACi) that consequently favours acetylation of histones5,34,35,58. We demonstrate that two HDAC inhibitors structurally and metabolically unrelated to SCFAs were inducing TGFB1 expression similarly to butyrate. Thus it is likely that the butyrate-induced TGFB1 up-regulation was a consequence of its HDAC inhibitory properties. To our knowledge up-regulation of TGFB1 expression by HDACi has never been reported, especially in IECs.
Regulation of gene transcription by HDACi involves a wide range of transcription factors that can bind TGFB1 promoter and that includes NF-κB, AP-1 and SP140,42,43,44,45. Several responsive elements of these transcription factors were shown to be involved in TGFB1 induction by different stimuli. Indeed, it has been described that immune signals such as IL1β, TNFα and Toll-like receptors ligands can activate TGFB1 transcription through NF-κB activation9,48. Two AP-1 motifs were shown to be functional in hepatic and mesangial cells and confirmed in our study by using phorbol ester46,47,59 (Supplementary Fig. 4). Moreover, previous publications demonstrated that the Specific protein 1 (SP1) binding motifs are particularly enriched in TGFB1 promoter and that one of them modulates TGFB1 expression in various models, at steady state and upon infection. We investigated the role of these transcription factors in TGFB1 up-regulation by butyrate. NF-κB and AP-1 inhibitors did not impact on butyrate-driven up-regulation of TGFB1 suggesting that these two transcription factors were not involved. These results were confirmed by the fact that butyrate did not activate a NF-κB reporter system in HT-29 and that a TGFB1 promoter construct mutated for the 2 functional AP-1 motifs responded to butyrate similarly to the wild-type TGFB1 promoter. TGFB1 promoter has a high number of GC-rich motifs that are potential targets for the transcription factors SP1 and SP3. By using a SP1/SP3 inhibitor and inhibiting SP1 expression by siRNA, we showed a pivotal role of SP1 in the butyrate and HDACi induction of TGFB1 expression (Fig. 6 and Supplementary Fig. 3B). Furthermore by mutating the functional SP1 motif in the core promoter of TGFB1 (TGF−453/+11SP1) neither butyrate nor HDACi were able to modulate TGFB1 expression anymore. This result confirmed that butyrate was enhancing TGFB1 transcription via SP1 binding on the core promoter. Eventually we confirmed that SP1 binding to TGFB1 promoter was also essential for bacterial supernatant mediated induction of TGFB1.
Recently, Yoshimori’s group demonstrated that Clostridium butyricum increases TGFβ1 via a specific mechanism involving Toll-like receptor-2 (TLR2)-dependent signalling and a SMAD auto-induction loop in dendritic cells (DC) present in the lamina propria9. This TLR2-dependent generation of tolerogenic DC favours regulatory T-cells induction which is similar to what was reported for Bacteroides fragilis suggesting a more general mechanism used by several commensal bacteria60,61. Kenya Honda’s laboratory also reported that a mixture of Clostridiales bacteria from phylogenetic clusters IV and XIVa is sufficient to restore colonic Treg in germ-free mice and this phenotype was dependent on the TGFβ1 produced by IECs4,21. Strikingly, the immunosuppressive property of these Clostridiales was independent of several known bacterial associated pattern recognition receptors-related signalling pathways such as MYD88 and was related to SCFA production suggesting a mechanism independent to the pathway reported by Yoshimura’s group. From these results, it can be hypothesized that TGFB1 gene expression can be regulated by cell-type specific transcription factors and signalling pathways.
Here, we describe for the first time the mechanism by which the butyrate-producer of the gut microbiota impacts on the TGFB1 gene regulation in intestinal epithelial cells that implicates HDACi and the transcription factor SP1. Despite being limited to HT-29 cell-line, we think our results may not be limited to this cell-line. Indeed, previous studies have shown that butyrate activates TGFB1 expression in diverse cell types including intestinal epithelial cell-lines, such as HCT116 and Caco-2, suggesting that the described mechanism generally impacts IEC4,53,54,55. Therefore, further validation in human primary IECs or intestinal organoids is a future challenge to improve our understanding of the complex impact of butyrate on IECs. Long co-evolution of microbiota and host cells appears to have resulted in multiple mechanisms to increase TGFB1 expression by IECs and DCs with an overlapping finality, the generation of protective Tregs. Our study supports this hypothesis and contributes to the understanding of the mechanisms developed by the gut microbiota and especially butyrate-producing bacteria to promote local and systemic immune tolerance.
Materials and Methods
Cell Culture
The human epithelial cell lines HT-29 was obtained from the American Type Culture Collection (ATCC, Rockville, MD). HT29 cells were grown in RPMI 1640 supplemented with 10% of heat-inactivated fetal calf serum, 2 mM L-glutamine, 50 U/mL penicillin, 50 U/mL streptomycin in a humidified 5% CO2 atmosphere at 37 °C. All culture media and supplements were supplied by Sigma-Aldrich. Mycoplasma contamination was regularly tested using MycoAlert (Lonza) and PlasmoTest (Invivogen).
Plasmids and reporter cell-lines
A 3.2Kb (−1864/+1370 section, TGFprom and a 1.3 Kb (−1362/+11 section, TGF−1362/+11) of the human TGFβ1 promoter were cloned into the pGL4.14 (Promega) luciferase plasmid. The TGF−453/+11 construct and its derived mutants (TGF−453/+11SP1 and TGF−453/+11AP1) were a kind gift of C. Weigert and transferred into pGL4.14 backbone46. These constructs were used to establishing the stable HT-29-TGFprom, HT-29-TGF−1362/+11, HT-29-TGF−453/+11, HT-29-TGF−453/+11SP1 and HT-29-TGF−453/+11AP1 reporter cell-lines after antibiotic selection (hygromycin, 600 µg.mL, InvivoGen). HT-29-NFκB cell line was stably transfected with pNiFty2-SEAP (Invivogen) and has been describe previously25.
Human Ffar2 (GPR43) and Hcar2 (GPR109a) were cloned after EcoRI and XhoI digestion in pCMV-eGFP-N1 vector (Addgene). Oligonucleotides used for amplification of FFAR2 were aaaactcgagatgctgccggactggaa and aaaagaattcctactctgtagtgaagtccga. Oligonucleotides used for amplification of HCAR2 were aaaactcgagatgaatcggcaccatctgcaggat and aaaagaattcttaaggagaggttgggcccaga.
Luciferase Reporter and cell viability Assays
For each experiment, cells were seeded at 3.104 cells per well in 96-well plates 24 h prior to incubation with bacterial supernatants or reagents. The cells were stimulated for 24 h with bacterial supernatants, SCFA or controls (TNFα, IL1β, PMA and RPMI) in a total culture volume of 100 μL per well prior to the luciferase assay. The luciferase activity was quantified as relative luminescence units by a microplate reader (Infinite200, Tecan) and the Neolite Luminescence Reporter Assay System (Perkin-Elmer) according to the manufacturer’s instructions. Secreted embryonic alkaline phosphatase (SEAP) was revealed with the Quanti-Blue reagent (Invivogen) using microplate reader (655 nm Infinite 200, Tecan). The TGFB1 and NF-κB activities were normalized to the controls, i.e., the unstimulated cells or cells in presence of non-inoculated bacteria culture medium. Experiments were performed in triplicates for at least three independent assays. Cell viability was monitored by MTS measurement using the CellTiter 96 Aqueous One solution (Promega) according to the manufacturer’s recommendations.
Culture of commensal Strains, preparation of bacterial supernatants and SCFA concentration assessment
135 human intestinal commensal bacterial strains which include 111 different species from the in-house INRA-Micalis collection or from DSMZ were grown. Anaerobic culture conditions were done using the Hungate method62. Screened species and strains, corresponding growth media, optical densities (OD), short chain fatty acids (SCFAs) concentrations are listed in Supplementary Table 1. Composition of home-made growth media is listed in Supplementary Table 1. Bacterial cultures were cultured to reach the maximum OD and centrifuged at 3,000 g for 10 to 20 min. Cultures were controlled using Gram staining method, aerobic growth test and fresh observation on microscope. Bacterial supernatants were then collected and filtered on a 0.22 μm PES filters and conserved at −80 °C. Non-inoculated bacteria culture medium served as control. Concentrations of SCFAs produced by cultured bacteria were measured by HPLC and gas chromatography as described63,64.
ELISA
HT-29 cells were seeded at 1 × 106 cells per well in 6 well-plates 24 h prior incubation with Serum-free medium and drugs. Supernatants were collected 24 h later and immediately assessed by ELISA following manufacturer instructions using the TGFβ1 DuoSet kit (R&D systems).
Reagents and cytokines
All agonists, drugs and inhibitors were dissolved in glycerol, DMSO or water following the manufacturer’s recommendations. SCFAs were from Sigma-Aldrich and used in a range of concentrations from 0.5 to 8 mM. GPRs agonists used were: GPR41: 4-CMTB (1 μM, Tocris 4642) and Tiglic acid (1–10 mM, Sigma); GPR43: AR420626 (1 μM, Cayman) and MCPC (1 mM, Sigma); GPR109a: Niacine (1 mM–10 mM, Sigma) and MK1903 (1 μM, Tocris). GPRs sub-unit inhibitors used were: Pertussis toxin (Ptx, 0.2 μg/ml, Sigma) and U73122 (Sigma 10 μM). MCT inhibitors used were: AR-C155858 (0.4 μM, Tocris), p-Chloromercuribenzoate acid (pCMB, 100 μM, Sigma). HDAC inhibitors used were: Trichostatin A (TSA, 1 μM, Sigma), SAHA (5 μM, Sigma). SP1 competitive inhibitor used was the Mithramycin A (0.1 μM) from Sigma. IL1β (10 ng/ml) and TNFα (10 ng/ml) were from Peprotech. Phorbol 12-myristate 13-acetate (PMA, 100 nM) was from Sigma.
siRNA assays
4.105 HT29- TGFprom cells were seeded in 12-well plates and transient transfections were done on day 2 and day 3 with 2.5 µL of DharmaFECT 1 (Dharmacon) and 25 nM of ON-TARGETplus smart Pool siRNA SP1 (L-026959-00-0005, NM_001251825.1) or Negative Control (D-001810-10-05). On day 4 cells were plated to 2.103 on 96 wells, on day 5 incubation with reagents was done and incubated for an additional 24 h prior luciferase activity measurement.
Real-Time PCR
HT-29 cells were seeded in 6 well culture plates at densities of 1.106 per well 24 h before stimulation and total RNA was extracted using RNeasy mini-Kit (Qiagen) according to the manufacturer’s recommendations with Dnase I treatment (R&D). cDNA was synthesized from 2 µg of RNA using the High-Capacity cDNA Reverse Transcription Kit (Applied Biosystems) and 100 ng were used to conduct qPCRs on ABI Prism 7700 (Applied Biosystems) or StepOnePlus Real-Time PCR System (ThermoFischer Scientific). The following Taqman Gene expression assay probes were used: GAPDH Hs02758991_g1, GPR43 Hs00271142_s1, GPR41 Hs02519193_g1, GPR109a Hs02341584_s1, SMCT1 Hs00377618_m1, and MCT1 Hs01585687_m1. GAPDH was used for normalization. Samples were tested in experimental duplicates and at least biological triplicates.
Promoter analysis
To search for potential transcription factor binding sites on HT-29-TGFprom, we used the MatInspector software tool (Genomatix, Munich, Germany) and Jaspar database.
Statistical analysis and Graphics
Data were analysed using R and RStudio software. PCA analysis was done with prcomp package and correlation matrix was done with Hmisc package. Graphics were produced with ggplot2 package. Statistical test used were two-tailed, T test or Wilcoxon rank test on medians with a confidence level of 95%. P value: *P < 0.05, **P < 0.01, ***P < 0.001, NS: non-significant. Data come from at least 3 independent biological experimentations.
References
Gaboriau-Routhiau, V. et al. The key role of segmented filamentous bacteria in the coordinated maturation of gut helper T cell responses. Immunity 31, 677–689, https://doi.org/10.1016/j.immuni.2009.08.020 (2009).
Ivanov, I. I. et al. Induction of intestinal Th17 cells by segmented filamentous bacteria. Cell 139, 485–498 (2009).
Atarashi, K. et al. Th17 Cell Induction by Adhesion of Microbes to Intestinal Epithelial Cells. Cell 163, 367–380, https://doi.org/10.1016/j.cell.2015.08.058 (2015).
Atarashi, K. et al. Induction of colonic regulatory T cells by indigenous Clostridium species. Science 331, 337–341 (2011).
Schilderink, R., Verseijden, C. & de Jonge, W. J. Dietary inhibitors of histone deacetylases in intestinal immunity and homeostasis. Frontiers in immunology 4, 226, https://doi.org/10.3389/fimmu.2013.00226 (2013).
Furusawa, Y. et al. Commensal microbe-derived butyrate induces the differentiation of colonic regulatory T cells. Nature 504, 446–450, https://doi.org/10.1038/nature12721 (2013).
Smith, P. M. et al. The microbial metabolites, short-chain fatty acids, regulate colonic Treg cell homeostasis. Science 341, 569–573, https://doi.org/10.1126/science.1241165 (2013).
Arpaia, N. et al. Metabolites produced by commensal bacteria promote peripheral regulatory T-cell generation. Nature 504, 451–455, https://doi.org/10.1038/nature12726 (2013).
Kashiwagi, I. et al. Smad2 and Smad3 Inversely Regulate TGF-beta Autoinduction in Clostridium butyricum-Activated Dendritic Cells. Immunity 43, 65–79, https://doi.org/10.1016/j.immuni.2015.06.010 (2015).
Frank, D. N. et al. Molecular-phylogenetic characterization of microbial community imbalances in human inflammatory bowel diseases. Proceedings of the National Academy of Sciences of the United States of America 104, 13780–13785 (2007).
Sokol, H. et al. Faecalibacterium prausnitzii is an anti-inflammatory commensal bacterium identified by gut microbiota analysis of Crohn disease patients. Proceedings of the National Academy of Sciences of the United States of America 105, 16731–16736 (2008).
Sokol, H. et al. Low counts of Faecalibacterium prausnitzii in colitis microbiota. Inflammatory bowel diseases 15, 1183–1189 (2009).
Marafini, I., Zorzi, F., Codazza, S., Pallone, F. & Monteleone, G. TGF-Beta signaling manipulation as potential therapy for IBD. Curr Drug Targets 14, 1400–1404 (2013).
Ardizzone, S., Bevivino, G. & Monteleone, G. Mongersen, an oral Smad7 antisense oligonucleotide, in patients with active Crohn’s disease. Therap Adv Gastroenterol 9, 527–532, https://doi.org/10.1177/1756283X16636781 (2016).
Monteleone, G. et al. Blocking Smad7 restores TGF-beta1 signaling in chronic inflammatory bowel disease. The Journal of clinical investigation 108, 601–609, https://doi.org/10.1172/JCI12821 (2001).
Andoh, A. et al. Faecal microbiota profile of Crohn’s disease determined by terminal restriction fragment length polymorphism analysis. Aliment Pharmacol Ther 29, 75–82 (2009).
Iliev, I. D., Mileti, E., Matteoli, G., Chieppa, M. & Rescigno, M. Intestinal epithelial cells promote colitis-protective regulatory T-cell differentiation through dendritic cell conditioning. Mucosal immunology 2, 340–350 (2009).
Iliev, I. D. et al. Human intestinal epithelial cells promote the differentiation of tolerogenic dendritic cells. Gut 58, 1481–1489 (2009).
Di Sabatino, A. et al. Blockade of transforming growth factor beta upregulates T-box transcription factor T-bet, and increases T helper cell type 1 cytokine and matrix metalloproteinase-3 production in the human gut mucosa. Gut 57, 605–612, https://doi.org/10.1136/gut.2007.130922 (2008).
Geuking, M. B. et al. Intestinal bacterial colonization induces mutualistic regulatory T cell responses. Immunity 34, 794–806 (2011).
Atarashi, K. et al. Treg induction by a rationally selected mixture of Clostridia strains from the human microbiota. Nature 500, 232–236, https://doi.org/10.1038/nature12331 (2013).
Li, M. O. & Flavell, R. A. TGF-beta: a master of all T cell trades. Cell 134, 392–404, https://doi.org/10.1016/j.cell.2008.07.025 (2008).
Qin, J. et al. A human gut microbial gene catalogue established by metagenomic sequencing. Nature 464, 59–65 (2010).
Mazmanian, S. K., Round, J. L. & Kasper, D. L. A microbial symbiosis factor prevents intestinal inflammatory disease. Nature 453, 620–625 (2008).
Lakhdari, O. et al. Functional metagenomics: a high throughput screening method to decipher microbiota-driven NF-kappaB modulation in the human gut. PloS one 5 (2010).
Cohen, L. J. et al. Functional metagenomic discovery of bacterial effectors in the human microbiome and isolation of commendamide, a GPCR G2A/132 agonist. Proceedings of the National Academy of Sciences of the United States of America 112, E4825–4834, https://doi.org/10.1073/pnas.1508737112 (2015).
Vital, M., Howe, A. C. & Tiedje, J. M. Revealing the bacterial butyrate synthesis pathways by analyzing (meta)genomic data. mBio 5, e00889, https://doi.org/10.1128/mBio.00889-14 (2014).
Le Poul, E. et al. Functional characterization of human receptors for short chain fatty acids and their role in polymorphonuclear cell activation. The Journal of biological chemistry 278, 25481–25489, https://doi.org/10.1074/jbc.M301403200 (2003).
Brown, A. J. et al. The Orphan G protein-coupled receptors GPR41 and GPR43 are activated by propionate and other short chain carboxylic acids. The Journal of biological chemistry 278, 11312–11319, https://doi.org/10.1074/jbc.M211609200 (2003).
Thangaraju, M. et al. GPR109A is a G-protein-coupled receptor for the bacterial fermentation product butyrate and functions as a tumor suppressor in colon. Cancer Res 69, 2826–2832, https://doi.org/10.1158/0008-5472.CAN-08-4466 (2009).
Cuff, M., Dyer, J., Jones, M. & Shirazi-Beechey, S. The human colonic monocarboxylate transporter Isoform 1: its potential importance to colonic tissue homeostasis. Gastroenterology 128, 676–686 (2005).
Thibault, R. et al. Butyrate utilization by the colonic mucosa in inflammatory bowel diseases: a transport deficiency. Inflammatory bowel diseases 16, 684–695, https://doi.org/10.1002/ibd.21108 (2010).
Dokmanovic, M., Clarke, C. & Marks, P. A. Histone deacetylase inhibitors: overview and perspectives. Mol Cancer Res 5, 981–989, https://doi.org/10.1158/1541-7786.MCR-07-0324 (2007).
Candido, E. P., Reeves, R. & Davie, J. R. Sodium butyrate inhibits histone deacetylation in cultured cells. Cell 14, 105–113 (1978).
Sealy, L. & Chalkley, R. The effect of sodium butyrate on histone modification. Cell 14, 115–121 (1978).
Gallinari, P., Di Marco, S., Jones, P., Pallaoro, M. & Steinkuhler, C. HDACs, histone deacetylation and gene transcription: from molecular biology to cancer therapeutics. Cell Res 17, 195–211, https://doi.org/10.1038/sj.cr.7310149 (2007).
Kim, S. J. et al. Activation of the second promoter of the transforming growth factor-beta 1 gene by transforming growth factor-beta 1 and phorbol ester occurs through the same target sequences. The Journal of biological chemistry 264, 19373–19378 (1989).
Kim, S. J., Glick, A., Sporn, M. B. & Roberts, A. B. Characterization of the promoter region of the human transforming growth factor-beta 1 gene. The Journal of biological chemistry 264, 402–408 (1989).
Geiser, A. G. et al. Regulation of the transforming growth factor-beta 1 and -beta 3 promoters by transcription factor Sp1. Gene 129, 223–228 (1993).
Davie, J. R. Inhibition of histone deacetylase activity by butyrate. J Nutr 133, 2485S–2493S (2003).
Nakano, K. et al. Butyrate activates the WAF1/Cip1 gene promoter through Sp1 sites in a p53-negative human colon cancer cell line. The Journal of biological chemistry 272, 22199–22206 (1997).
Nepelska, M. et al. Butyrate produced by commensal bacteria potentiates phorbol esters induced AP-1 response in human intestinal epithelial cells. PloS one 7, e52869, https://doi.org/10.1371/journal.pone.0052869 (2012).
Yu, D. C., Waby, J. S., Chirakkal, H., Staton, C. A. & Corfe, B. M. Butyrate suppresses expression of neuropilin I in colorectal cell lines through inhibition of Sp1 transactivation. Mol Cancer 9, 276, https://doi.org/10.1186/1476-4598-9-276 (2010).
Thakur, B. K., Dasgupta, N., Ta, A. & Das, S. Physiological TLR5 expression in the intestine is regulated by differential DNA binding of Sp1/Sp3 through simultaneous Sp1 dephosphorylation and Sp3 phosphorylation by two different PKC isoforms. Nucleic Acids Res 44, 5658–5672, https://doi.org/10.1093/nar/gkw189 (2016).
Inan, M. S. et al. The luminal short-chain fatty acid butyrate modulates NF-kappaB activity in a human colonic epithelial cell line. Gastroenterology 118, 724–734 (2000).
Weigert, C. et al. AP-1 proteins mediate hyperglycemia-induced activation of the human TGF-beta1 promoter in mesangial cells. J Am Soc Nephrol 11, 2007–2016 (2000).
Presser, L. D., McRae, S. & Waris, G. Activation of TGF-beta1 promoter by hepatitis C virus-induced AP-1 and Sp1: role of TGF-beta1 in hepatic stellate cell activation and invasion. PloS one 8, e56367, https://doi.org/10.1371/journal.pone.0056367 (2013).
Lee, K. Y. et al. NF-kappaB and activator protein 1 response elements and the role of histone modifications in IL-1beta-induced TGF-beta1 gene transcription. Journal of immunology 176, 603–615 (2006).
Weiss, A. & Attisano, L. The TGFbeta superfamily signaling pathway. Wiley Interdiscip Rev Dev Biol 2, 47–63, https://doi.org/10.1002/wdev.86 (2013).
Ihara, S., Hirata, Y. & Koike, K. TGF-beta in inflammatory bowel disease: a key regulator of immune cells, epithelium, and the intestinal microbiota. J Gastroenterol, https://doi.org/10.1007/s00535-017-1350-1 (2017).
Lees, C. W., Barrett, J. C., Parkes, M. & Satsangi, J. New IBD genetics: common pathways with other diseases. Gut 60, 1739–1753, https://doi.org/10.1136/gut.2009.199679 (2011).
Kagnoff, M. F. The intestinal epithelium is an integral component of a communications network. The Journal of clinical investigation 124, 2841–2843, https://doi.org/10.1172/JCI75225 (2014).
Staiano-Coico, L. et al. TGF-alpha and TGF-beta expression during sodium-N-butyrate-induced differentiation of human keratinocytes: evidence for subpopulation-specific up-regulation of TGF-beta mRNA in suprabasal cells. Exp Cell Res 191, 286–291 (1990).
Nathan, D. F., Burkhart, S. R. & Morin, M. J. Increased cell surface EGF receptor expression during the butyrate-induced differentiation of human HCT-116 colon tumor cell clones. Exp Cell Res 190, 76–84 (1990).
Schroder, O., Hess, S., Caspary, W. F. & Stein, J. Mediation of differentiating effects of butyrate on the intestinal cell line Caco-2 by transforming growth factor-beta 1. Eur J Nutr 38, 45–50 (1999).
Gill, R. K. et al. Expression and membrane localization of MCT isoforms along the length of the human intestine. Am J Physiol Cell Physiol 289, C846–852, https://doi.org/10.1152/ajpcell.00112.2005 (2005).
Hadjiagapiou, C., Schmidt, L., Dudeja, P. K., Layden, T. J. & Ramaswamy, K. Mechanism(s) of butyrate transport in Caco-2 cells: role of monocarboxylate transporter 1. American journal of physiology. Gastrointestinal and liver physiology 279, G775–780 (2000).
Hinnebusch, B. F., Meng, S., Wu, J. T., Archer, S. Y. & Hodin, R. A. The effects of short-chain fatty acids on human colon cancer cell phenotype are associated with histone hyperacetylation. J Nutr 132, 1012–1017 (2002).
Birchenall-Roberts, M. C. et al. Transcriptional regulation of the transforming growth factor beta 1 promoter by v-src gene products is mediated through the AP-1 complex. Mol Cell Biol 10, 4978–4983 (1990).
Round, J. L. et al. The Toll-like receptor 2 pathway establishes colonization by a commensal of the human microbiota. Science 332, 974–977 (2011).
Round, J. L. & Mazmanian, S. K. Inducible Foxp3+ regulatory T-cell development by a commensal bacterium of the intestinal microbiota. Proceedings of the National Academy of Sciences of the United States of America 107, 12204–12209 (2010).
Hungate, R. E. The anaerobic mesophilic cellulolytic bacteria. Bacteriol Rev 14, 1–49 (1950).
Lakhdari, O. et al. Identification of NF-kappaB modulation capabilities within human intestinal commensal bacteria. Journal of biomedicine & biotechnology 2011, 282356, https://doi.org/10.1155/2011/282356 (2011).
Bourriaud, C. et al. Lactate is mainly fermented to butyrate by human intestinal microfloras but inter-individual variation is evident. J Appl Microbiol 99, 201–212, https://doi.org/10.1111/j.1365-2672.2005.02605.x (2005).
Derynck, R. et al. Human transforming growth factor-beta complementary DNA sequence and expression in normal and transformed cells. Nature 316, 701–705 (1985).
Shah, R., Rahaman, B., Hurley, C. K. & Posch, P. E. Allelic diversity in the TGFB1 regulatory region: characterization of novel functional single nucleotide polymorphisms. Hum Genet 119, 61–74, https://doi.org/10.1007/s00439-005-0112-y (2006).
Acknowledgements
The authors are grateful to Drs Véronique Douard (INRA UMR1319), Marion Espeli (INSERM UMR-S996) and Pierre Larraufie (University of Cambridge, UK) for helpful discussions and critical comments on the manuscript. The authors are grateful to members of the team for helpful discussions. The authors are grateful to Dr Cora Weigert (University of Tübingen) for sharing the TGF promoter constructs and Agnès David (UMR1280 PHAN) for SCFA analysis. This work was supported by the Institut National de la Recherche Agronomique (INRA), by grants funded by EU-FP7 METACARDIS (HEALTH-F4-2012-305312), by the ANR FunMetagen (ANR-11-BSV6-0013). CMG was the recipient of a fellowship from the Ministère de la Recherche et de l’Education Nationale (Sorbonne Université).
Author information
Authors and Affiliations
Contributions
Conceived and designed the experiments: C.M.G., N.L.; performed most of the experiments: C.M.G.; performed some experiments: F.B.C., L.M., A.G., F.L., A.J., N.L.; analysed the data: C.M.G., N.L.; wrote the paper: C.M.G., N.L.; edited and revised the manuscript: H.M.B.
Corresponding author
Ethics declarations
Competing Interests
The authors declare no competing interests.
Additional information
Publisher's note: Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made. The images or other third party material in this article are included in the article’s Creative Commons license, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons license and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this license, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Martin-Gallausiaux, C., Béguet-Crespel, F., Marinelli, L. et al. Butyrate produced by gut commensal bacteria activates TGF-beta1 expression through the transcription factor SP1 in human intestinal epithelial cells. Sci Rep 8, 9742 (2018). https://doi.org/10.1038/s41598-018-28048-y
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41598-018-28048-y
This article is cited by
-
Gut microbial metabolites SCFAs and chronic kidney disease
Journal of Translational Medicine (2024)
-
Postbiotic butyrate: role and its effects for being a potential drug and biomarker to pancreatic cancer
Archives of Microbiology (2024)
-
Dietary oregano aqueous extract improves growth performance and intestinal health of broilers through modulating gut microbial compositions
Journal of Animal Science and Biotechnology (2023)
-
Human milk oligosaccharides modulate the intestinal microbiome of healthy adults
Scientific Reports (2023)
-
Langerhans cells shape postnatal oral homeostasis in a mechanical-force-dependent but microbiota and IL17-independent manner
Nature Communications (2023)
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.