Abstract
It is not known how total homocysteine (tHcy) levels change during the transition from acute stroke to post-stroke convalescence or whether tHcy changes occurring after the acute period are associated with recurrence of cerebro-cardiovascular events. Levels of tHcy were measured during acute ischemia and again after three months. Patients were followed for a median of 18 (range: 12–36) months. A total of 2800 patients who had at least two tHcy measurements were enrolled between February 2012 and June 2014; 2587 patients presented with ischemic stroke and 213 presented with cerebral hemorrhage. During the follow-up period, 220 (7.9%) patients experienced another ischemic event. After adjusting for additional cardiovascular risk factors, patients with the highest levels of tHcy (fourth quartile; >15.5 μmol/L) had a 1.76-fold increased risk of a recurrence (adjusted HR: 1.76, 95%CI: 1.11–3.08) as compared to patients with the lowest levels of tHcy (lowest quartile; ≤9.65 μmol/L). Additional analysis by subgroup indicated that this correlation was only significant for patients with large-artery atherosclerosis ischemia (adjusted HR: 2.00, 95%CI: 1.13–3.55). Elevated tHcy during the convalescent phase of acute stroke was independently associated with an increased risk of recurrent ischemic stroke, especially in those patients with large-vessel atherosclerosis ischemia.
Similar content being viewed by others
Introduction
Accumulating data suggest elevated total serum homocysteine (tHcy) is associated with an increased risk of coronary heart disease and stroke1,2,3,4,5. Studies of patients with acute ischemia, diastolic dysfunction, and hypertension as well as large community studies have also demonstrated that elevated tHcy levels increased the risk of both all-cause and cardiovascular disease specific mortality6,7,8,9,10. By design, in all of these cases control studies, stroke “cases” are identified first and the assessment of tHcy levels follows the stroke. There is concern that the disease process itself may alter blood levels of tHcy. That is, if stroke results in an increased tHcy level after the event, then the observed elevated post stroke levels among stroke “cases” may lead to misguided conclusions regarding the role of tHcy as a risk factor for the development of the stroke. It could be, as some suggest, that elevated tHcy is an acute-phase reactant and a consequence rather than a cause of the disease process11,12.
On the basis of these studies, it has been postulated that an elevated tHcy level prior to an ischemic event acts as a risk factor for stroke. In two previous studies, tHcy levels have been shown to increase between the acute period and after several months of convalescence after the original ischemic event13,14. However, these studies included only 76–82 cases; there has not yet been a large case study of changes in tHcy levels between the acute period and the convalescent period. It is still unclear when, in relation to the ischemic event, elevated levels of tHcy represent a potentially modifiable risk factor for stroke.
The relationship between tHcy levels and the recurrence of vascular events after stroke remains inconclusive15,16,17,18. In our previous study, we found that elevated levels of tHcy in acute stroke were related to higher mortality. However, we did not analyze the relationship between serum tHcy levels and a recurrent ischemic event. Therefore, we conducted a prospective study of a large population of patients that suffered an acute stroke to examine changes in plasma tHcy levels between the acute period and a convalescent period after a stroke, with a median follow-up period of 18 (range: 12–36) months. This study allows us to analyze whether elevated plasma tHcy levels occurring during the convalescent period after an acute ischemic event contribute to the risk of recurrence.
Methods
Study design
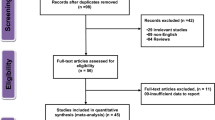
This work is based on 2800 patients who were admitted to the neurological department at Tianjin Huanhu Hospital in Tianjin, China within 48 hours after onset of cerebrovascular symptoms from February 2012 through June 2014. All patients had a magnetic resonance imaging or computed tomography (MRI or CT) scan. Individuals were diagnosed with cerebral infarction if they had a neurological deficit of presumed vascular origin that lasted 24 hours and either a normal CT brain scan or evidence of a recent infarct in the relevant area of the brain on MRI scan. The criteria for TIA was similar, but with symptoms lasting less than 24 hours and without evidence of a recent infarct in the relevant area of the brain on MRI scan. The diagnosis of intracranial hemorrhage (ICH) was based in all cases on CT showing hemorrhage. Exclusion criteria were identical to our previous study8, and patients died within three months of hospital discharge were also excluded from this study Controls were selected from individuals who had regular health checks from 2012 to 2014. Those patients with a history of acute stroke, coronary heart disease, renal function impairment (serum creatinine > 133 µmol/L), or B vitamin therapy within two weeks of screening were excluded.
We enrolled 2800 patients, all of whom met the inclusion criteria and provided informed consent to participate in the study. We separated patients by ischemic subtype using the criteria described in the Trial of Org 10172 in Acute Stroke Treatment (TOAST)19. No patients received B vitamin therapy after the initial ischemic event, but every patient did receive either a follow-up call or subsequent clinic visit every three months. The incidence of recurrent ischemic stroke was the primary outcome measured; median follow-up time was 18 months. Seven patients, who emigrated from Tianjin or refused to revisit, were lost to follow-up and excluded from the analysis of recurrent rate and risk factors.
The severity of neurological deficit was measured with the National Institutes of Health stroke scale (NIHSS) on admission. History of stroke or TIA and history of hypertension were defined as either self-reported or based on information from previous medical records. Comorbidities are described in our previous study8.
Ethics Statement
The study protocol was approved by the Regional Ethics Committee (Tianjin Huanhu Hospital Ethics Committee). All patients provided informed consent prior to participation. All methods were performed in accordance with Declaration of Helsinki.
Blood sample measurements
Blood samples were obtained from all patients within 24 hours of admission and three months after the acute event. Patients were invited to revisit their doctors for repeat sampling during the convalescent period. They attended the clinic as outpatients after an overnight fast and provided samples for tHcy analysis. Laboratory measurements used were as described previously8.
Statistical methods
The Mann-Whitney U test was used for data analysis of continuous variables and chi-square statistics was used for categorical variables. Cox proportional hazards regression analyses were used to calculate hazard ratio (HR) estimates associated with tHcy levels and recurrent ischemic stroke. A p-value < 0.05 was considered statistically significant.
Results
Plasma tHcy levels were measured at least twice in a total of 2800 patients with an acute cerebrovascular event. The baseline characteristics of all patients according to stroke subtype are described in Table 1. In 2429 patients with cerebral infarction and 158 patients with TIA, the geometric mean ± SD tHcy level on admission was 14.4 ± 10.3 μmol/L. In 213 patients with ICH, the geometric mean tHcy level on admission was 15.6 ± 9.1 μmol/L. The difference in geometric mean tHcy level between ischemic and hemorrhagic events was not statistically significant (p = 0.102). After three months, the tHcy level was 14.3 ± 10.0 μmol/L in patients with ischemic stroke and 14.7 ± 9.2 μmol/L in patients with ICH. The difference in geometric mean tHcy levels between ischemic and hemorrhagic events was not statistically significant (p = 0.603) (Table 2). The difference in geometric mean tHcy levels in patients immediately after acute stroke and during the convalescent phase was not statistically significant (p = 0.341).
In 232 controls, the geometric mean tHcy level was 12.1 ± 2.5 μmol/L, which was significant lower than that observed in stroke patients.
As expected, men consistently displayed higher tHcy levels than women. At baseline, the mean tHcy concentration was 15.7 ± 11.3 μmol/L for men presenting with ischemic stroke and 17.9 ± 10.3 μmol/L for men presenting with ICH versus 11.6 ± 6.4 μmol/L for women with ischemic stroke and 11.7 ± 4.4 μmol/L with women with ICH. During the three month convalescent period, mean tHcy levels were also higher in men than in women (Table 2).
The geometric mean tHcy level was not significantly different amongst ischemic stroke subtypes according to TOAST criteria, either at the acute stage or after three months of convalescence. In ischemic stroke patients with carotid or vertebral basilar artery stenosis, at three months after stroke, the geometric mean tHcy was higher than patients without stenosis (15.1 ± 12.2 μmol/L vs.13.2 ± 6.8 μmol/L, p = 0.030), but there was no significant difference in tHcy levels at the acute stage (14.1 ± 9.2 μmol/L vs.13.9 ± 9.8 μmol/L, p = 0.704). In patients age 65 or older, there was no significant difference in the geometric mean tHcy levels at the acute stage, but at three months after stroke the geometric mean tHcy was higher in patients over 65 as compared to younger patients (15.1 ± 10.2 μmol/L vs.14.0 ± 9.8μmol/L, p = 0.005) (Table 3).
Recurrent ischemic stroke and tHcy levels three days after acute stroke
During the follow-up period, 220 (7.9%) patients experienced a recurrence of ischemic stroke. The risk of recurrent ischemic stroke was not significantly increased in patients with elevated tHcy levels within three days of the acute ischemic event (Table 4).
Recurrent ischemic stroke and tHcy levels 3 months after acute stroke
The rate of recurrence of ischemic stroke was significantly higher in patients in with the highest tHcy levels (fourth quartile) as compared to patients with the lowest levels (first quartile) (unadjusted HR: 1.61; 95% CI: 1.10–2.36; p = 0.011). Similarly, the rate of recurrence was significantly higher in patients with higher levels of tHcy (third quartile) than in patients with the lowest levels of tHcy (first quartile) (unadjusted HR: 1.51; 95% CI: 1.04–2.19; p = 0.032). This association remained significant for patients with high tHcy levels (fourth quartile) as compared to patients with low tHcy levels (first quartile), even after adjusting for age, sex, smoking status, LDL-C level, hsCRP level, and ApoB/ApoAI ratio and the presence of hypertension, type 2 diabetes mellitus, coronary artery disease, and obesity (adjusted HR: 1.76; 95% CI: 1.11–3.08; p = 0.031) (Table 5).
After analyzing the data by type of ischemia, we found that patients with large-artery atherosclerosis ischemia with high levels of tHcy (third or fourth quartile) had a significantly higher risk of recurrent ischemic stroke than patients in the lowest quartile (unadjusted HR: 1.75, 95% CI: 1.08–2.82; p = 0.021 or unadjusted HR: 1.65, 95% CI: 1.09–2.71; p = 0.039). There was no significant association between patients with high and low levels of tHcy in those patients with small-vessel occlusion associated ischemic events. Multivariate analysis also did not affect this association (Table 5).
Discussion
Only a few studies have reported serial measurements of tHcy concentrations after acute vascular events and all of these studies had small sample sizes. Ours is the first to measure tHcy levels during both the acute phase of a stroke and again three months after the event in a large sample. Our report provides evidence of a consistent pattern of the stable mean tHcy levels within three days after an acute stroke and after three months. Only in ischemic stroke patients with stenosis did the mean tHcy increase between the acute stage to convalescent phase. The rate of recurrence of an ischemic event was significantly higher in patients in the fourth tHcy quartile than in patients in the first quartile, even after adjusting for potential clinically relevant confounders; the association was especially prominent in those patients suffering from large-artery atherosclerosis.
Two previous reports13,14 investigated changes in tHcy from the acute to the convalescent phase of stroke (68 days to 645 days). In both, plasma tHcy levels were lower in the acute phase than in the convalescent phase, but these studies had small sample sizes. In our study, only in stroke patients with large-artery stenosis were the mean tHcy levels were lower during the acute stage than in the convalescent phase. Howard et al.20 conducted a prospective, multicenter study to examine changes in tHcy during the 2 weeks after an incident stroke. The estimated mean tHcy level at baseline was 11.3 ± 0.5 μmol/L, which increased consistently to a mean of 12.0 ± 0.05, 12.4 ± 0.5, 13.3 ± 0.5, and 13.7 ± 0.7 μmol/Lat 3, 5, 7, and 10 to 14 days after the initial event, respectively.
Landgren et al.21 reported similar increases between the acute and convalescent periods in patients with MI, in which tHcy levels of 53 patients with MI increased significantly from a mean of 13.1 ± 4.6 μmol/L 24 to 36 hours after the onset of MI to 14.8 ± 4.8 μmol/L 6 weeks after the event. Senaratne et al.22 measured tHcy within 48 to 72 hours of admission in 62 patients with acute MI and again at 6 weeks after discharge. The mean tHcy level during the acute phase was 13.6 ± 0.98 mol/L, which decreased significantly to 12.1 ± 1.01 μmol/L at 6 weeks post MI. In a small study, Egerton et al.23 reported on 10 patients with MI who completed blood draws for tHcy analysis at 1, 3, 7, and 21 days and again at 6 months. Mean levels of tHcy started at 12.9 μmol/L and increased at days 3 and 7 then decreased at days 21 and 180.
During the convalescent period in stroke patients with carotid or vertebral basilar artery stenosis, the tHcy level was higher than patients without stenosis. The multiethnic population-based Northern Manhattan Study (NOMAS)24 showed that Hcy levels were independently associated with carotid plaque morphology and increased plaque area; these results are similar to those from another study of Chinese adults derived from a reference population of the Kailuan Cohort Study25. In that same reference population, elevated tHcy levels were associated with asymptomatic carotid artery stenosis (CAS)26. Our study further confirmed that carotid or vertebral basilar artery stenosis in stroke patients was related to high tHcy levels during convalescent periods. Carotid plaque formation, together with CAS, was the result of atherosclerosis, which might be caused by hyper-homocysteinemia. Hyper-homocysteinemia can produce complex changes within the blood vessel wall27.
Our study showed that an elevated tHcy level during the convalescent phase of stroke is independently associated with an increased risk of recurrent ischemic stroke after the index cerebrovascular event. Our findings corroborate those of other investigators indicating high plasma homocysteine levels contribute to the risk of stroke recurrence17,28,29. Our results are also in line with those of Del Ser et al.18 who found that tHcy levels exceeding the 75th percentile three months after an ischemic stroke was a predictor of vascular events, including stroke recurrence, acute myocardial infarction, deep venous thrombosis, and peripheral arterial disease. The incidence of other vascular illness except ischemic stroke was too low to be analyzed separately in our study. By focusing solely on ischemic stroke events, our study clearly identifies elevated tHcy levels three months after acute stroke as a risk factor for recurrent stroke, especially in the large-artery atherosclerosis stroke subtype.
In our previous study, we found that elevated tHcy levels during the acute phase of stroke were associated with higher long-term mortality, but not with recurrence of stroke8. In the present study, we found that tHcy levels changed between the acute phase and the convalescent phase; the tHcy levels observed during the convalescent phase were related to the recurrence of ischemic stroke. These results suggest that during acute stroke, tHcy levels are influenced by a reaction to acute illness, then after three months, return to a stable level. Only persistently high serum tHcy levels affect arthrosclerosis, carotid stenosis, and recurrence of stroke.
There are several limitations of our report. Most notably, this report, like previous reports, does not assess tHcy levels level before the stroke. Therefore, we could not conclude that tHcy increased after acute stroke. In addition, our study was strengthened by an assessment of tHcy taken from acute to the convalescent period. With this additional assessment, we would have been able to assess the proportion of the change between the acute and convalescent period. These data clearly documents the need for a prospective study in which tHcy levels prior a stroke event are coupled with sequential measures after the stroke event, both in the acute and convalescent period. Furthermore, there was no systematic follow-up on tHcy concentrations during the three-month observation period. We cannot reliably document the number of patients treated with folic acid three months after the index stroke as the advice regarding folic acid was given either to the patient or to the patient’s general physician. Intake of folic acid might have led to an underestimation of the effect of hyper-homocysteinemia; however, in three months after stroke, we did not advise patients regarding folic acid, vitamin B12, and vitamin B6.
Our study shows that elevated tHcy levels during the convalescent phase after stroke were independently associated with an increased risk of recurrent ischemic stroke after the index cerebrovascular event, especially for patients of the large-artery atherosclerosis subtype. These data suggest that the clinical interpretation of tHcy after stroke, and the eligibility for clinical trials assessing treatment for elevated tHcy levels, require an adjustment for time since stroke to properly interpret the observed tHcy levels.
References
Casas, J. P., Bautista, L. E., Smeeth, L., Sharma, P. & Hingorani, A. D. Homocysteine and stroke: evidence on a causal link from mendelian randomisation. Lancet (London, England) 365, 224–232, https://doi.org/10.1016/s0140-6736(05)17742-3 (2005).
Wald, D. S., Law, M. & Morris, J. K. Homocysteine and cardiovascular disease: evidence on causality from a meta-analysis. BMJ (Clinical research ed) 325, 1202 (2002).
Collaboration, H. S. Homocysteine and risk of ischemic heart disease and stroke: a meta-analysis. Jama 288, 2015–2022 (2002).
Bostom, A. G. et al. Nonfasting plasma total homocysteine levels and stroke incidence in elderly persons: the Framingham Study. Annals of internal medicine 131, 352–355 (1999).
Iso, H. et al. Serum total homocysteine concentrations and risk of stroke and its subtypes in Japanese. Circulation 109, 2766–2772, https://doi.org/10.1161/01.cir.0000131942.77635.2d (2004).
Sacco, R. L. et al. Homocysteine and the risk of ischemic stroke in a triethnic cohort: the NOrthern MAnhattan Study. Stroke 35, 2263–2269, https://doi.org/10.1161/01.str.0000142374.33919.92 (2004).
Cui, R. et al. Serum total homocysteine concentrations and risk of mortality from stroke and coronary heart disease in Japanese: The JACC study. Atherosclerosis 198, 412–418, https://doi.org/10.1016/j.atherosclerosis.2007.09.029 (2008).
Shi, Z. et al. Elevated Total Homocysteine Levels in Acute Ischemic Stroke Are Associated With Long-Term Mortality. Stroke 46, 2419–2425, https://doi.org/10.1161/strokeaha.115.009136 (2015).
Luo, J. L. et al. Association between plasma homocysteine concentration and the risk of all-cause death in adults with diastolic dysfunction in a community: A 13-year cohort study. Medicine 96, e6716, https://doi.org/10.1097/md.0000000000006716 (2017).
Xu, B. et al. Homocysteine and all-cause mortality in hypertensive adults without pre-existing cardiovascular conditions: Effect modification by MTHFR C677T polymorphism. Medicine 96, e5862, https://doi.org/10.1097/md.0000000000005862 (2017).
Christen, W. G., Ajani, U. A., Glynn, R. J. & Hennekens, C. H. Blood levels of homocysteine and increased risks of cardiovascular disease: causal or casual? Archives of internal medicine 160, 422–434 (2000).
Brattstrom, L. & Wilcken, D. E. Homocysteine and cardiovascular disease: cause or effect? The American journal of clinical nutrition 72, 315–323 (2000).
Lindgren, A. et al. Plasma homocysteine in the acute and convalescent phases after stroke. Stroke 26, 795–800 (1995).
Meiklejohn, D. J., Vickers, M. A., Dijkhuisen, R. & Greaves, M. Plasma homocysteine concentrations in the acute and convalescent periods of atherothrombotic stroke. Stroke 32, 57–62 (2001).
Toole, J. F. et al. Lowering homocysteine in patients with ischemic stroke to prevent recurrent stroke, myocardial infarction, and death: the Vitamin Intervention for Stroke Prevention (VISP) randomized controlled trial. Jama 291, 565–575, https://doi.org/10.1001/jama.291.5.565 (2004).
Bostom, A. G., Selhub, J., Jacques, P. F. & Rosenberg, I. H. Power Shortage: clinical trials testing the “homocysteine hypothesis” against a background of folic acid-fortified cereal grain flour. Annals of internal medicine 135, 133–137 (2001).
Boysen, G., Brander, T., Christensen, H., Gideon, R. & Truelsen, T. Homocysteine and risk of recurrent stroke. Stroke 34, 1258–1261, https://doi.org/10.1161/01.str.0000069017.78624.37 (2003).
Del Ser, T. et al. Hyperhomocyst(e)inemia is a risk factor of secondary vascular events in stroke patients. Cerebrovascular diseases (Basel, Switzerland) 12, 91–98, doi:47687 (2001).
Adams, H. P. et al. Classification of subtype of acute ischemic stroke. Definitions for use in a multicenter clinical trial. TOAST. Trial of Org 10172 in Acute Stroke Treatment. Stroke 24, 35–41 (1993).
Howard, V. J. et al. Changes in plasma homocyst(e)ine in the acute phase after stroke. Stroke 33, 473–478 (2002).
Landgren, F. et al. Plasma homocysteine in acute myocardial infarction: homocysteine-lowering effect of folic acid. Journal of internal medicine 237, 381–388 (1995).
Senaratne, M. P., Griffiths, J. & Nagendran, J. Elevation of plasma homocysteine levels associated with acute myocardial infarction. Clinical and investigative medicine. Medecine clinique et experimentale 23, 220–226 (2000).
Egerton, W. et al. Serial measures of plasma homocyst(e)ine after acute myocardial infarction. The American journal of cardiology 77, 759–761 (1996).
Alsulaimani, S. et al. Elevated homocysteine and carotid plaque area and densitometry in the Northern Manhattan Study. Stroke 44, 457–461, https://doi.org/10.1161/strokeaha.112.676155 (2013).
Yang, X. et al. Homocysteine and carotid plaque stability: a cross-sectional study in Chinese adults. PloS one 9, e94935, https://doi.org/10.1371/journal.pone.0094935 (2014).
Jia, J. et al. Homocysteine and Its Relationship to Asymptomatic Carotid Stenosis in a Chinese Community Population. Scientific reports 6, 37361, https://doi.org/10.1038/srep37361 (2016).
Faraci, F. M. & Lentz, S. R. Hyperhomocysteinemia, oxidative stress, and cerebral vascular dysfunction. Stroke 35, 345–347, https://doi.org/10.1161/01.str.0000115161.10646.67 (2004).
Zhang, W. et al. High plasma homocysteine levels contribute to the risk of stroke recurrence and all-cause mortality in a large prospective stroke population. Clinical science (London, England: 1979) 118, 187–194, https://doi.org/10.1042/cs20090142 (2009).
Bos, M. J., van Goor, M. L., Koudstaal, P. J. & Dippel, D. W. Plasma homocysteine is a risk factor for recurrent vascular events in young patients with an ischaemic stroke or TIA. Journal of neurology 252, 332–337, https://doi.org/10.1007/s00415-005-0647-9 (2005).
Acknowledgements
The study was supported by the Natural Science Foundation of China (funding number: 81571057 and 81300947), the Science and Technology Project of Tianjin Municipal Health Bureau (funding number: 2014KR10 and 2013KY15), the Tianjin Science and Technology Project (funding number: 16ZXMJSY00010) and the Key Research Project of Tianjin Public Health (funding number: 14KG117).
Author information
Authors and Affiliations
Contributions
Z.S., S.L., J.X. and Y.J. conceived and designed this study. M.Z. directed data analysis. Z.S. and S.L. wrote the paper. Y.G., H.L., W.Y. B.Z. and M.L. prepared the database and reviewed the paper. J.X. and Y.J. conducted the quality assurance and reviewed and edited the paper. All authors reviewed the manuscript.
Corresponding authors
Ethics declarations
Competing Interests
The authors declare no competing interests.
Additional information
Publisher's note: Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made. The images or other third party material in this article are included in the article’s Creative Commons license, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons license and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this license, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Shi, Z., Liu, S., Guan, Y. et al. Changes in total homocysteine levels after acute stroke and recurrence of stroke. Sci Rep 8, 6993 (2018). https://doi.org/10.1038/s41598-018-25398-5
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41598-018-25398-5
This article is cited by
-
Higher serum homocysteine levels are associated with an increased risk of hemorrhagic transformation in patients with acute ischemic stroke
BMC Neurology (2023)
-
Stroke in Parkinson’s disease: a review of epidemiological studies and potential pathophysiological mechanisms
Acta Neurologica Belgica (2023)
-
ALDH7A1 rs12514417 polymorphism may increase ischemic stroke risk in alcohol-exposed individuals
Nutrition & Metabolism (2022)
-
Binary effects of intravascular laser irradiation of blood on motor recovery and homocysteine reduction in a case with ischemic hemiparesis: portrayed with brain perfusion images
BMC Neurology (2022)
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.