Abstract
Inadequate sleep is a prevalent problem within our society that can result in cognitive dysfunction. Elevations in kynurenic acid (KYNA), a metabolite of the kynurenine pathway (KP) of tryptophan degradation known to impact cognition, in the brain may constitute a molecular link between sleep loss and cognitive impairment. To test this hypothesis, we investigated the impact of 6 hours of sleep deprivation on memory and KP metabolism (brain and plasma) in male and female rats. Sleep-deprived males were impaired in a contextual memory paradigm, and both sexes were impaired in a recognition memory paradigm. After sleep deprivation, hippocampal KYNA levels increased significantly only in males. The response in hippocampal KYNA levels to sleep loss was suppressed in gonadectomized males, delineating a role of circulating gonadal hormones. Circulating corticosterone, which has previously been linked to KP metabolism, correlated negatively with hippocampal KYNA in sleep-deprived females, however the relationship was not significant in male animals. Taken together, our study introduces striking sex differences in brain KYNA formation and circulating corticosterone in response to sleep deprivation. Relating these findings to sex differences in cognitive outcomes after sleep deprivation may further advance the development of novel therapeutic agents to overcome sleep loss-induced cognitive dysfunction.
Similar content being viewed by others
Introduction
Sleep loss and inadequate sleep are prevalent problems within our society1. Studies with both human and animal subjects have demonstrated that sufficient sleep is essential to protect mental health, physical health, and quality of life2. As cognitive dysfunction is one of the recurring consequences of sleep loss that impacts daily function, there is a compelling need to better understand the underlying molecular mechanism linking sleep loss and cognitive impairments. Our previous work demonstrates that kynurenic acid (KYNA), acting as an antagonist at N-methyl-d-aspartate (NMDA) and α7 nicotinic acetylcholine (α7nACh) receptors, is involved in cognitive processes in health and disease3. The current study presents evidence that KYNA may be a key player linking sleep loss and cognitive impairments.
KYNA is an endogenous astrocyte-derived neuroinhibitory molecule resulting from tryptophan degradation. Prolonged wakefulness has been shown to elevate tryptophan levels in the plasma and brain4,5. Tryptophan 2,3-dioxygenase (TDO) and indoleamine 2,3-dioxygenase (IDO) metabolize the vast majority of tryptophan to kynurenine and initiate the kynurenine pathway (KP; Fig. 1)6, while only about 5% of dietary tryptophan is degraded to serotonin and melatonin. Kynurenine promptly enters the brain from the blood, and is then degraded within local cells by kynurenine 3-monooxygenase (KMO) to 3-hydroxykynurenine (3-HK) or kynurenine aminotransferases (KATs) to KYNA.
The KP has remained relatively unexplored in sleep studies, however an association between sleep disturbances, excessive levels of KYNA, and cognitive impairments has been recently bolstered by studies in rats. Notably, increases in KP metabolism, including elevations in hippocampal KYNA, were found centrally and peripherally in a model of central fatigue induced by prolonged sleep deprivation in rodents7,8. Furthermore, we recently demonstrated that acute kynurenine treatment specifically reduces rapid eye movement (REM) sleep, REM-associated theta power, and impairs hippocampal-dependent contextual memory9.
To further investigate the hypothesized relationship between sleep and KYNA7,8,9, in designing our present studies we considered several important biological variables, including the impact of i) biological sex and circulating gonadal hormones and ii) sleep loss-induced stress. Of note, little emphasis has been placed on understanding sex differences in response to sleep deprivation. As sleep patterns10 and factors influencing KP metabolism may be sexually dimorphic11,12,13, for the present experiments we investigated the impacts of sleep deprivation in both male and female adult rats. Additionally, while the body adapts to sleep loss, several biological systems are activated, including the main neuroendocrine system regulating responses to stress, the hypothalamic-pituitary-adrenal (HPA) axis. During prolonged sleep deprivation, glucocorticoids, including cortisol in humans and corticosterone in rats, are released from the adrenal cortex and have been detected in plasma in both humans14 and rats15. As elevations in corticosterone may impact tryptophan metabolism via the KP16, we assess the relationship between KP activation and circulating corticosterone after sleep deprivation.
We demonstrated the effectiveness of our experimental paradigm, gentle handling, to induce sleep deprivation comparably in both sexes by acquiring polysomnographic recordings that combine electroencephalogram (EEG) and electromyogram (EMG). Interestingly, we determine a conspicuous sex difference in response to sleep deprivation in hippocampal-dependent contextual memory, but not recognition memory, which also relies on the perirhinal cortex. With sleep loss, male rats were significantly impaired in a passive avoidance paradigm and also showed increased hippocampal KYNA formation. To explore the mechanisms underlying the sex differences, the gonads were removed from adult male and female rats and biochemical assessments after sleep deprivation experiments were repeated. Taken together our data introduce a sex-dependent interplay between circulating gonadal hormones, the HPA axis activation, and KP metabolism in response to sleep deprivation.
Materials and Methods
Animals and experimental cohorts
Adult, male (200–300 grams; n = 102) and female (150–250 grams; n = 106) Wistar rats were obtained from Charles River Laboratories (Frederick, MD). Animals were housed in a temperature-controlled facility, fully accredited by the American Association for the Accreditation of Laboratory Animal Care, at the Maryland Psychiatric Research Center. They were kept on a 12/12 h light-dark cycle, where lights on corresponded to zeitgeber time (ZT) 0 and lights off to ZT 12, and received ad libitum access to food and water. All protocols were approved by the Institutional Animal Care and Use Committee at the University of Maryland School of Medicine and were in accordance with the National Institutes of Health Guide for the Care and Use of Laboratory Animals. All efforts were made to minimize animal suffering and to reduce the number of animals used. Experiment #1: animals underwent surgical procedures to implant telemetric transmitters to record sleep-wake behavior. Experiment #2: animals were used for behavioral testing. Experiment #3: tissue was collected from naïve animals after sleep deprivation. Experiment #4: tissue was collected from animals that underwent sham or gonad removal surgical procedures prior to sleep deprivation.
Sleep deprivation protocol
Animals were sleep deprived for 6 h by gentle handling beginning at ZT 0. Individually housed animals remained in a home cage and were presented with novel objects (i.e. wooden blocks, paper towel, cotton balls) to induce exploration. When necessary, animals were gently touched with a long cotton tip applicator and cages were rotated to prevent the initiation of sleep.
Sleep data collection and analysis
EEG and EMG recordings were conducted as described in previously published protocols9. Briefly, under isoflurane anesthesia, animals were placed in a David Kopf (Tujunga, CA) stereotaxic frame and implanted with telemetry transmitters (TL11M2-F40-EET; Data Science International, St. Paul, MN). EEG leads were wrapped around surgical screws (Plastics One, Roanoke, VA) inserted at 2.0 mm anterior/+1.5 mm lateral and 7.0 mm posterior/−1.5 mm lateral relative to bregma and secured with dental cement. EMG leads were inserted directly into the dorsal cervical neck muscle about 1.0 mm apart and sutured in place. Animals recovered for 10 days before experimentation.
All sleep data were recorded in a designated room. EEG and EMG waveform data were continuously collected using Ponemah 6.10 software (DSI). Digitized signal data were scored offline with Neuroscore 3.0 (DSI) in 10-s epochs as wake (low-amplitude, high-frequency EEG combined with high-amplitude EMG), non-REM (NREM)(high-amplitude, low-frequency EEG and low-amplitude EMG), or REM (low-amplitude, high-frequency EEG with very low EMG tone). The scored epochs were summed over 6 h during the light phase (ZT 0 to ZT 6). The total duration of time spent in each vigilance state was determined.
Cognitive behavior assessment
Contextual memory task
The passive avoidance paradigm (PAP) was used to assess hippocampal-dependent contextual memory, as previously described9. Briefly, on day 1 (training trial) at ZT 3, animals were placed in the illuminated compartment of the test box and the latency to enter the dark compartment was recorded. A door separating the two compartments was immediately closed and an inescapable foot shock (0.56 mA for 1 s) was delivered through metal rods of the floor. Twenty-four hours later, at ZT 3 on day 2 (testing trial), the rat was again placed in the illuminated compartment, the guillotine door was opened, and the avoidance latency, i.e. the time to enter the dark compartment, was recorded.
Recognition memory task
The novel object recognition (NOR) task was used to assess recognition memory, engaging both the perirhinal cortex and hippocampus17,18,19. Briefly, on three consecutive days, rats were habituated for 5 min to the testing arena. Then, on the training day, each rat was given 5 min to explore two identical objects located in the arena. Twenty-four hours later, during the testing trial, each rat was again given 5 min to explore the arena which now contained one training trial object and one new object. The training and testing trial were video recorded and analyzed with ANY-Maze behavioral tracking software (Stoelting Co., Wood Dale, Illinois). Discrimination index was calculated as the difference in exploration time during the testing trial between novel object and familiar object, then dividing this value by the total object exploration time. The index takes into account individual differences in total exploratory behavior.
Surgical procedures to remove gonads
All gonadectomy (GDX) surgeries were performed while animals were under isoflurane anesthesia. Briefly, in female animals, a small incision was made into the abdominal cavity from each flank. The ovary was withdrawn from the body, clamped and removed. The muscle wall was sutured and the incision was shut with wound clips. In male rats, a single incision was made above the scrotal sac. Each testis was withdrawn from the body cavity, clamped and removed. The incision was sutured closed. For each sex, sham surgeries were performed such that the described incisions were made, but the gonads were not removed. All animals recovered for at least 10 days before experimental testing.
Tissue collection
At the conclusion of experiments, all animals were euthanized at ZT 6 by CO2 asphyxiation. Whole trunk blood was collected in tubes containing 20 μl K3-EDTA (0.15%). The blood was centrifuged (300 × g, 10 min) to separate plasma from cells and the supernatant was frozen at −80 °C. The brain was promptly removed and hippocampus and cortex were dissected. All regions were rapidly frozen on dry ice and stored at −80 °C.
Biochemical analysis
Corticosterone measurement
Plasma corticosterone concentrations were determined by radioimmunoassay (MP Biomedicals, Solon, OH, USA). Samples were run in duplicate, with 5 μl of plasma used for each tube. The sensitivity threshold for the assay was 5 ng/mL and inter- and intra-assay coefficients of variance were less than 10%.
Plasma tryptophan, kynurenine, and KYNA determination
Plasma samples were diluted in ultrapure water (1:1,000 for tryptophan; 1:2 for kynurenine; 1:10 for KYNA). Twenty-five μl of 6% perchloric acid were added to 100 μl of the preparation. Precipitated proteins were separated by centrifugation (12,000 × g, 10 min) and analyzed by high performance liquid chromatography (HPLC). Twenty μl of the supernatant were applied to a ReproSil-Pur C18 column (4 × 150 mm; Dr. MaischGmbh, Ammerbuch, Germany), using a mobile phase containing 50 mM sodium acetate and 5% acetonitrile (pH adjusted to 6.2 with glacial acetic acid) at a flow rate of 0.5 ml/min, and detected with 500 mM zinc acetate delivered after the column with a flow rate of 0.1 ml/min. Tryptophan (excitation 285 nm, emission 365 nm), kynurenine (excitation 365 nm, emission 480 nm), and KYNA (excitation 344 nm, emission 398 nm) were detected fluorometrically in the eluate (Waters Alliance, 2475 fluorescence detector, Bedford, MA).
Brain KYNA determination
Hippocampal and cortical regions were weighed, sonicated in ultrapure water (1:10, w/v) and aliquoted. Twenty-five μl of 25% perchloric acid were used to acidify 100 μl of diluted sample. After centrifugation (12,000 × g, 10 min), 30 μl of the supernatant were subjected to HPLC as described above.
Brain 3-HK determination
Cortical samples were weighed, sonicated (1:5, w/v) in ultrapure water and aliquoted. Twenty-five μl of 6% perchloric acid were used to acidify 100 μl of diluted sample. After centrifugation (12,000 × g, 10 min), 20 μl of the supernatant was subjected to HPLC. 3-HK was eluted from a 3-μm HPLC column (HR-80; 80 × 4.6 mm; ESA) using a mobile phase of 1.5% acetonitrile, 0.9% triethylamine, and 0.59% phosphoric acid at a flow rate of 0.5 mL/min and detected electrochemically using an HTEC 500 detector (Eicom, San Diego, CA, USA; oxidation potential: + 0.5 V).
Statistical analysis
Experiment #1
The percent of time spent in each vigilance state (REM, NREM, wake duration) was analyzed by repeated measures analysis of variance (ANOVA) comparing control and sleep deprivation. Bonferroni correction was used for multiple comparisons.
Experiment #2
Latency to enter the dark compartment of the PAP was analyzed by repeated measures ANOVA. The effects of sex and sleep were assessed. Exploration time in the NOR task was analyzed by repeated measures ANOVA, with object as a within subject variable. Main effects and interaction of sex and sleep were assessed between-subjects. The outcomes of NOR task discrimination index, distance traveled on the training day, and mean speed on the training day were analyzed by two-way ANOVA, with main effects and interaction of sex and sleep. Bonferroni correction was used for multiple comparisons.
Experiment #3
Biochemical analysis (plasma tryptophan, plasma kynurenine, plasma KYNA, cortical KYNA, cortical 3-HK, hippocampal KYNA, plasma corticosterone) of samples collected from naïve animals were analyzed by two-way ANOVA. For each analysis, main effects and the interaction of sex and sleep condition were assessed. Bonferroni correction was used for multiple comparisons.
Experiment #4
Biochemical analysis (plasma tryptophan, plasma kynurenine, plasma KYNA, hippocampal KYNA, plasma corticosterone) of samples collected from animals that underwent sham or gonadectomy surgery were analyzed by three-way ANOVA. For each analysis, sleep condition, sex, and surgery and possible interactions were assessed. The final model was selected by using a model selection procedure: when factors did not interact in three-way ANOVA (P > 0.05), analyses were followed up with appropriate two-way interactions; and analyses were focused on the main effects of sleep, sex, and surgery when two- way interactions were not statistically significant. Bonferroni correction was used for multiple comparisons.
In all analyses, where appropriate, significant main effects were followed up with the Bonferroni post hoc test. Spearman correlation analysis was performed to determine the relationship between peripheral corticosterone and hippocampal KYNA. All statistical analyses were performed using GraphPad Prism 6.0 (Graphpad Software, La Jolla, CA, USA) or SPSS 24 software (IBM Corporation, Armonk, USA). Statistical significance was defined as P < 0.05. See supplemental Fig. 1 for further details.
Data Availability
The data generated in the present study are available from the corresponding author upon reasonable request.
Results
Gentle handling unequivocally disrupts sleep in male and female rats
Sleep deprivation by gentle handling from ZT 0 to ZT 6 resulted in 95% elimination of NREM and 100% elimination of REM sleep in male and female animals (Fig. 2).
Acute sleep deprivation differentially disrupts memory in male and female rats
We tested both sexes of rats in two behavioral tasks to assess learning and memory after sleep deprivation, the PAP to probe contextual memory and the NOR to evaluate recognition memory. As shown in Fig. 3A, animals were sleep deprived from ZT 0 to ZT 6 and underwent behavioral task training at ZT 3. Twenty-four hours after training, animals were assessed in the testing trial. Sleep condition significantly impacted the latency to enter the dark compartment on the test day of the PAP (F1,37 = 12.5, P < 0.01), while there were no significant effects of sex alone (F1,37 = 3.9, P = 0.1) or a sex x sleep condition interaction (F1,37 = 3.1, P = 0.09) (Fig. 3B). In male rats, sleep deprivation induced significant PAP deficits, evidenced as decreased avoidance latency on day 2 (P < 0.01). However, in female animals, compared to the control condition, the latency to enter the dark compartment was not significantly reduced on the test day with sleep loss (P = 0.40). Females that were sleep deprived displayed a significant increase in latency between the training and testing trial (P < 0.05), similar to control females (P < 0.05), thus indicating the ability to ordinarily learn in the PAP.
Sleep deprivation impairs both contextual and recognition memory in male rats, but only recognition memory in female rats. (A) Schematic representation of standard behavioral task to assess contextual memory, passive avoidance paradigm (PAP), and recognition memory, novel object recognition (NOR). Male and female animals were sleep deprived for 6 h from ZT 0 to ZT 6. (B) PAP Latency. (C) NOR exploration time during testing trial. (D) NOR discrimination index during testing trial. (E) Distance traveled during training trial of NOR. (F) Mean speed during training trail of NOR. All data are mean ± SEM. *P < 0.05, **P < 0.01. N = 8−12 per group.
Both sexes of rats were significantly impaired in the NOR task after sleep deprivation. While control male and control female rats spent significantly more time with the novel object, sleep deprived animals failed to differentiate and spent equal time with the familiar and novel object during the test trial (Fig. 3C). Analysis of the discrimination index between objects revealed no significant sleep condition x sex interaction (F1,41 = 0.1, P = 0.75), but a significant main effect of sleep condition (F1,41 = 13.5, P < 0.0001) (Fig. 3D). Both male and female sleep deprived animals had a significantly lower discrimination index (P < 0.05) compared to counterpart controls. Of note, during the training trial in the NOR task, distance traveled during the task was significantly impacted by sex (F1,41 = 20.7, P < 0.0001), sleep condition (F1,41 = 4.6, P < 0.05) and an interaction between sex x sleep condition (F1,41 = 8.0, P < 0.01) (Fig. 3E). Additionally, the mean speed during the training trial was also impacted by sex (F1,41 = 20.2, P < 0.0001), sleep condition (F1,41 = 4.5, P < 0.05) and an interaction between sex x sleep condition (F1,41 = 7.9, P < 0.01) (Fig. 3F). Sleep-deprived males traveled a greater distance (P < 0.01) and also had an increase in mean speed (P < 0.01) in the testing apparatus on the training day, suggesting that loss of sleep induced a hyperactive state in males alone.
No change to peripheral tryptophan, kynurenine, or KYNA after sleep deprivation
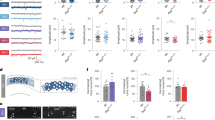
To examine the impact of acute sleep loss on the dynamics of KP metabolism, we determined tryptophan, kynurenine and KYNA levels in the plasma immediately after sleep deprivation in both sexes of rats. In the plasma, we found no significant effect of sleep condition on tryptophan (F1,31 = 1.8, P = 0.19) (Fig. 4A), kynurenine (F1,32 = 0.6, P = 0.44) (Fig. 4B) or KYNA (F1,32 = 1.4, P = 0.25) (Fig. 4C). Sex significantly impacted plasma tryptophan (F1,31 = 22.1, P < 0.001) and kynurenine (F1,32 = 10.6, P < 0.01). Post-hoc analysis revealed a significant difference between tryptophan and kynurenine among control male and female animals (P < 0.05) and tryptophan among sleep-deprived animals (P < 0.001).
Sleep deprivation specifically impacts hippocampal KYNA in a sex-dependent manner
Levels of KP metabolites KYNA and 3-HK were also assessed in the cortical tissue immediately after sleep deprivation. KYNA levels were significantly impacted by sex alone (F1,29 = 4.9, P < 0.05), but no main effect of sleep (F1,29 = 0.14, P = 0.7) or interaction (F1,29 = 3.4, P = 0.08) were found (Fig. 5A). Cortical KYNA levels were significantly less in sleep-deprived females than counterpart males (P < 0.05). Levels of 3-HK, the initial product of the alternative branch of kynurenine metabolism, were assessed in the cortical samples. 3-HK levels were not impacted by sleep deprivation (F1,16 = 0.21, P = 0.65), sex (F1,16 = 2.4, P = 0.14), and we found no significant sleep condition x sex interaction (F1,16 = 1.6, P = 0.22)(control male: 202 ± 13 fmoles/mg protein; sleep-deprived male: 179 ± 25 fmoles/mg protein; control female: 210 ± 38 fmoles/mg protein; sleep-deprived female: 260 ± 34 fmoles/mg protein).
Alterations in KYNA formation were also assessed in the hippocampus after sleep deprivation. KYNA in the hippocampus was impacted by both sleep deprivation (F1,26 = 8.4, P < 0.01) and sex (F1,26 = 7.4, P < 0.05) (Fig. 5B). However, there was no significant sleep condition x sex interaction (F1,26 = 2.9, P = 0.1). In male rats, there was a significant increase in hippocampal KYNA after sleep deprivation (P < 0.01). Within the sleep deprivation cohorts, females had significantly less hippocampal KYNA than male rats (P < 0.01).
Impact of sleep deprivation on peripheral tryptophan, kynurenine, or KYNA in gonadectomized rats
To decipher if our sex-specific findings were mediated by circulating gonadal hormones, we next assessed KP biochemical changes in gonadectomized rats. Tryptophan in the plasma was not significantly affected by a three-way sleep condition x sex x gonadectomy surgery interaction (F1,70 = 1.0, P = 0.3) (Fig. 6A). Two-way analysis revealed a significant sex x surgery interaction (F1,70 = 7.5, P < 0.01), but no impact of sleep condition x surgery (F1,70 = 0.01, P = 0.93) or sleep condition x sex (F1,70 = 0.7, P = 0.4). As in the naïve condition (see Fig. 4A), plasma tryptophan was significantly impacted by sex (F1,70 = 11.2, P < 0.01), however there were no main effects of sleep condition (F1,70 = 2.0, P = 0.16) or surgery (F1,70 = 0.13, P = 0.72). Plasma tryptophan was elevated in sham control and sleep-deprived females compared to sham control and sleep-deprived males, as we previously determined.
Gonadectomy (GDX) in male animals attenuates an elevation in hippocampal KYNA levels after sleep deprivation. Sham-operated or GDX male and female animals were sleep deprived for 6 h from ZT 0 to ZT 6. (A) Plasma tryptophan. (B) Plasma kynurenine. (C) Plasma KYNA. (D) Hippocampal KYNA. All data are mean ± SEM. *P < 0.05, **P < 0.01. N = 5–11 per group.
Plasma kynurenine was not impacted by a three-way sleep condition x sex x surgery interaction (F1,53 = 0.3, P = 0.59) (Fig. 6B). Additionally, no significant two-way interactions were determined (sleep x sex: F1,53 = 0.7, P = 0.39; sleep x surgery: F1,53 = 0.9, P = 0.35; sex x surgery: F1,53 = 0.1, P = 0.77). While there was no main effect of sleep (F1,53 = 0.2, P = 0.68), plasma kynurenine was significantly impacted by sex (F1,53 = 7.8, P < 0.01) and surgery (F1,53 = 8.3, P < 0.01) alone. Post-hoc analysis revealed significantly reduced plasma kynurenine in sham control females compared to sham control males, as we previously determined.
When plasma KYNA levels were assayed, no three-way interaction between sleep x sex x surgery was determined (F1,72 = 0.2, P = 0.68) (Fig. 6C). Additionally, no significant two-way interactions were found (sleep x sex: F1,72 = 0.03, P = 0.86; sleep x surgery: F1,72 = 1.4, P = 0.24; sex x surgery: F1,72 = 0.4, P = 0.52). Sleep condition (F1,72 = 0.002, P = 0.96) and sex (F1,72 = 0.2, P = 0.67) had no main effect, but notably surgery significantly impacted plasma KYNA (F1,72 = 4.7, P < 0.05). There were no significant post-hoc findings.
Male gonadectomy attenuates hippocampal KYNA elevation in response to sleep deprivation
Next, we assessed hippocampal KYNA levels in response to sleep deprivation in gonadectomized rats (Fig. 6D). No three-way interaction between sleep condition, sex, and surgery (F1,63 = 2.1, P = 0.15) was determined for hippocampal KYNA. Additionally, no significant two-way interactions were determined (sleep x sex: F1,63 = 0.6, P = 0.46; sleep x surgery: F1,63 = 3.0, P = 0.09; sex x surgery: F1,63 = 1.6, P = 0.46). There was a significant main effect of sleep condition (F1,63 = 7.4, P < 0.01), but no main effect of sex (F1,63 = 0.4, P = 0.55) or surgery (F1,63 = 2.4, P = 0.13). Sham sleep-deprived males had significantly more hippocampal KYNA than sham control males, but KYNA levels were not significantly different between control GDX males and sleep-deprived GDX males. KYNA remained unchanged after sleep deprivation in both sham and GDX females.
Sleep deprivation by gentle handling dimorphically elevates plasma corticosterone in male and female rats
Due to the distinct behavioral and KP biochemical outcomes in male and female rats, we examined the stress response hormone corticosterone in the plasma after sleep deprivation. In the intact cohort, plasma corticosterone was significantly impacted by sleep condition (F1,32 = 11.4, P < 0.01) and sex (F1,32 = 9.2, P < 0.01) (Fig. 7A). Corticosterone was elevated by 130% in sleep-deprived females compared to control females. Male animals, however, did not have significantly higher corticosterone after sleep deprivation.
To determine whether gonadal hormones play a role in the observed differential response in circulating corticosterone, sleep deprivation experiments were conducted in the gonadectomized cohort of adult male and female rats. Plasma corticosterone was not impacted by a three-way sleep condition x sex x surgery interaction (F1,72 = 0.095, P = 0.76) (Fig. 7B). There was a significant interaction between sleep condition and sex (F1,72 = 8.8, P < 0.01), sleep condition and surgery (F1,72 = 5.2, P < 0.05), but no significant interaction between sex and surgery (F1,72 = 1.7, P = 0.20). Analysis of main effects determined that plasma corticosterone was impacted significantly by sleep (F1,72 = 36.1, P < 0.001), sex (F1,72 = 34.4, P < 0.001), and surgery (F1,72 = 14.0, P < 0.001). Sleep-deprived GDX males had significantly more plasma corticosterone than control GDX males (P < 0.01), while corticosterone was not elevated in response to sleep deprivation in sham-operated males (P = 0.53). Sleep deprivation significantly increased plasma corticosterone in both GDX females (P < 0.001) and sham-operated females (P < 0.05), compared to respective controls.
Correlational analysis
Given that across multiple experiments we determined sexually differentiated responses in peripheral corticosterone and hippocampal KYNA elevation after sleep deprivation, we assessed a relationship between these two factors. No relationship between plasma corticosterone and hippocampal KYNA in intact control males (r = 0.03, P = 0.91) and intact control females (r = −0.21, P = 0.46) was found. In addition, while no relationship between corticosterone and hippocampal KYNA was determined in intact sleep-deprived males (r = 0.48, P = 0.07), interestingly, a significant negative correlation was found in intact sleep-deprived females (r = −0.44, P < 0.05). Taken together, these data suggest a sex-specific relationship between brain KYNA and peripheral corticosterone in response to sleep deprivation.
Discussion
The results of our present study, which was designed to assess the short-term impact of sleep deprivation on KP metabolism, revealed several intriguing phenomena and sexually differentiated responses. We determined subtle sex differences in behavioral outcomes after sleep deprivation and found an elevation in hippocampal KYNA, specifically in male animals, in response to sleep deprivation. While female animals did not present significantly elevated brain KYNA, we report a female-specific elevation in circulating corticosterone, demonstrating a differential response in HPA reactivity after acute sleep loss. Taken together, our findings yield an unexpected sex difference and a selective impact of sleep deprivation on the KYNA branch of kynurenine metabolism in the brain.
In experimental animals, sleep deprivation has been induced by various techniques, including the platform over water method, which selectively deprives animals of paradoxical sleep or gentle handling, which is very effective at inducing total sleep deprivation and strongly models sleep loss in humans20. While prolonged methods of sleep deprivation activate sleep loss-induced stress, the HPA axis, and influence several biological systems21, studies conducted mostly in male animals have suggested that gentle handling does not activate the HPA axis and serves as a useful tool to delineate impacts of stress and sleep loss20. In our first experiments, we verified the efficacy of gentle handling as a method of sleep deprivation and determined unequivocal elimination of NREM (95%) and REM (100%) sleep in male and female rats. Of note, corticosterone levels were significantly higher only in the female sleep-deprived group immediately after sleep loss, suggesting prompt stress reactivity in females. Several studies have indicated that male rodents habituate more efficiently to stressors than female rodents22, providing a feasible explanation for the differential corticosterone response to sleep deprivation by gentle handling. Additionally, testosterone has been shown to inhibit glucocorticoid activation23,24, supporting our findings of potentiated corticosterone elevation in response to sleep deprivation in GDX males that lacked circulating testosterone. Circulating estradiol in females may account for their susceptibility to elevations in corticosterone22, but our subsequent experiment in GDX females challenges the notion that estrogens alone contribute to the phenomena in females. In the future, investigations involving gonad removal with sex hormone replacement will further clarify the role of the circulating hormones on HPA axis activation after sleep deprivation.
The fact that female rats were shielded from impairments in contextual memory as well as an elevation in brain KYNA after sleep deprivation deserves special consideration. Perhaps in part due to growing evidence that alterations in female circulating hormones influence various sleep-wake parameters10, the majority of sleep-wake studies have focused on male animals and our understanding of the impacts of sleep disruptions between sexes remains relatively elusive. In this context, we were outwardly surprised to find such striking sex differences, particularly because prolonged sleep deprivation in female rats alone has been shown to impair cognitive function25,26 and elevate cerebral KP metabolism7,8.
The implications of elevated KYNA after acute sleep loss in the hippocampus, which mediates learning and memory and is particularly compromised by sleep loss27,28, deserves discussion. Herein, we demonstrate functionally detrimental levels of hippocampal KYNA3 in intact males after sleep loss. Only the male animals in our studies were compromised cognitively by sleep deprivation in both the PAP and NOR tasks. These tasks were chosen based on several considerations, including i) the ability to train rats in a single trial and test 24 hours later and ii) the participation of the hippocampus in the execution of both tasks19,29,30. Our findings suggest a resilient advantage of female animals to acute sleep loss in the PAP task, but not the NOR task. Importantly, the NOR task relies on an interaction between the perirhinal cortex and hippocampus to engage recognition memory, particularly, as in our study design, when the inter trial delay is greater than 10 min19,31. To further understand the role of KYNA in mediating the relationship between sleep loss and recognition memory deficits, KYNA formation in the perirhinal cortex will be assessed in future experiments. In addition, we report sex differences in response to sleep deprivation in locomotor activity during the NOR training trial. Our data show that during the sleep deprivation period, males were hyperactive, evidenced as moving a greater distance and also at a greater speed. Taken together, while the underlying mechanisms governing these behaviors and the interplay of sex hormones remain to be elucidated, similar sex differences in cognitive performance are speculated in human studies wherein physiological responses to sleep deprivation are not equal among women and men32,33.
In rodents, sleep deprivation studies have focused extensively on narrow time windows of memory consolidation and identified that memory appears most sensitive to sleep loss after acquisition. Recovery from sleep deprivation, termed rebound sleep, is regulated by both a homeostatic and circadian drive34. This rebound sleep is characteristically more intense and promotes performance recovery in cognitive domains impacted by sleep loss35. An increase in KYNA in the hippocampus during this rebound sleep may be particularly detrimental for memory consolidation processes. In rodents, nanomolar and low micromolar concentrations of KYNA itself, or stimulation of KYNA synthesis with the direct bioprecursor kynurenine, causes a spectrum of cognitive deficits, including disruptions in hippocampus-mediated contextual learning and memory3,36,37. Through its inhibitory actions at α7nACh and NMDA receptors, KYNA has been hypothesized to impact cognition. In addition, we also recently demonstrated that acute elevations in KYNA disrupt sleep-wake architecture9, introducing a novel physiological role for KYNA and taken together with our present findings, we speculate that an increase in KYNA after sleep deprivation may negatively impact rebound sleep and contribute to impairments in memory consolidation. Thus, we predict that inhibition of KYNA synthesis may serve as an efficacious strategy to overcome sleep-loss induced memory problems, as decreases in brain KYNA levels have been associated with pro-cognitive benefits3,38. However, it certainly remains to be seen if this treatment strategy would be only effective in male animals.
We chose to consider KP metabolism and elevated KYNA as a possible outcome after sleep deprivation based on several considerations. As an essential amino acid and precursor to serotonin and melatonin, tryptophan has been extensively studied as a modulator of sleep and its accumulation in the plasma and brain has been confirmed after sleep deprivation4,5. The bioavailability of tryptophan can directly influence kynurenine and KYNA formation. When developing a rodent model of chronic fatigue, Yamashita and Yamamoto demonstrated that several days of sleep loss in rats activates the KP by elevating blood tryptophan and kynurenine, as well as enhancing kynurenine and KYNA formation in specific brain regions, including the hippocampus7,8. As free forms of tryptophan and kynurenine readily enter the brain, it is plausible that an activation of KYNA formation is due to an increase in bioprecursor availability. Presently, analysis of tryptophan, kynurenine, and KYNA levels demonstrated no significant alterations after acute sleep deprivation, despite hippocampal elevations in KYNA levels in intact male animals. Our findings suggest a brain-specific mechanism for these alterations after an acute episode of sleep deprivation. While several methodological details differ between our studies, namely method of deprivation and total duration of sleep loss, our findings concur that KYNA formation is enhanced in the hippocampus after sleep deprivation, and we synergistically support the notion that these elevations may have detrimental impacts on cognition.
Mechanistically several factors that influence KYNA synthesis in the brain may be altered after sleep deprivation. From the blood, kynurenine is rapidly accumulated in astrocytes and irreversibly transaminated by several KATs, including KAT II, to KYNA3. Sleep deprivation can impact processes that regulate KAT II activity, such as alterations in energy metabolism or bioavailability of pyruvate39,40, a co-substrate of the KAT reaction41. Alternatively, changes in KMO activity and subsequent 3-HK formation can also impact KYNA levels42. As 3-HK levels were not altered after sleep deprivation, variations in KMO activity may not be the contributing factor, but follow-up studies are necessary to further elucidate these dynamics.
Increases in kynurenine levels, or activity of the catabolic enzymes, are not the only mechanisms that determine the formation of KYNA in the brain. Alternatively, accumulation of pro-oxidant factors after sleep deprivation43 may promote non-enzymatic degradation of kynurenine to KYNA44,45. In addition, accumulating literature implicates astrocytes and gliotransmitters in modulating sleep pressure. After prolonged wakefulness, a buildup of adenosine46 may stimulate KYNA production, as suggested in a microdialysis study wherein local brain infusions of adenosine or an A1 receptor agonist elevated extracellular KYNA47. Lastly, as degradative enzymes for KYNA are not present in the mammalian brain48, and the metabolite has strikingly stable chemical properties, no specific processes are known to break down KYNA. Extracellular KYNA must compete with other acidic compounds endogenous to the brain for reuptake by organic anion transporters49 or be removed from the cerebrum by probenecid-sensitive process50, which may be impacted by periods of sleep loss. It remains to be seen, however, the exact mechanism by which KYNA levels fluctuate in the brain upon sleep loss.
In rats, physiological stressors have been shown to induce tryptophan metabolism, resulting in increased levels of kynurenine and downstream KP metabolites both in the brain and periphery16,51,52. Stimulation of the enzymes TDO and/or IDO, by elevations in corticosterone or immunological activation that occurs with stress reactivity respectively16,53, is thought to activate KP metabolism by promoting the catabolism of tryptophan. These effects could also play a role in enhanced inflammation with sleep-loss54, and contribute to misbalance in the KP in health and disease processes12,55. Importantly, our present data draw additional attention to sex as an important biological variable in KP studies12,13,56,57, and introduce a novel interplay between the HPA responses to sleep deprivation and downstream KP metabolism. The specific mechanisms governing the causes and physiological ramifications of these responses will be further explored and clarified in future studies.
Lastly, distinct abnormalities in tryptophan metabolism via KP are found in several psychiatric and neurological conditions58 that exhibit cognitive dysfunction and sleep disturbances as core symptoms. Sleep disturbances in patients with schizophrenia and depression may aggravate the severity of the disorders and often negatively impact the patients’ quality of life59. Conceivable hypotheses suggest that cognitive impairments and abnormalities in sleep are connected, and the potential contribution of KYNA in mechanistically mediating a relationship between sleep and cognition in schizophrenia patients remains under investigation55,60.
In conclusion, the present study demonstrates a significant elevation in brain KYNA levels after acute sleep deprivation in male animals, supporting the notion that KYNA serves as a key molecular link between sleep disturbances and cognitive dysfunction. Defining a causal relationship between sleep disturbances and KP metabolism may unravel KYNA as a novel nexus between sleep and cognition.
References
Strine, T. W. & Chapman, D. P. Associations of frequent sleep insufficiency with health-related quality of life and health behaviors. Sleep Med 6, 23–27, https://doi.org/10.1016/j.sleep.2004.06.003 (2005).
Banks, S. & Dinges, D. F. Behavioral and physiological consequences of sleep restriction. J Clin Sleep Med 3, 519–528 (2007).
Pocivavsek, A., Notarangelo, F. M., Wu, H. Q., Bruno, J. P. & Schwarcz, R. in Modeling the Psychophathological Dimensions of Schizophrenia - From Molecules to Behavior Vol. 23 (eds M.V. Pletnikov & J. L. Waddington) Ch. 25, 423–443 (Elsevier, 2016).
Davies, S. K. et al. Effect of sleep deprivation on the human metabolome. Proc Natl Acad Sci USA 111, 10761–10766, https://doi.org/10.1073/pnas.1402663111 (2014).
Toru, M., Mitsushio, H., Mataga, N., Takashima, M. & Arito, H. Increased brain serotonin metabolism during rebound sleep in sleep-deprived rats. Pharmacol Biochem Behav 20, 757–761 (1984).
Leklem, J. E. Quantitative aspects of tryptophan metabolism in humans and other species: a review. Am J Clin Nutr 24, 659–672 (1971).
Yamashita, M. & Yamamoto, T. Tryptophan and kynurenic Acid may produce an amplified effect in central fatigue induced by chronic sleep disorder. Int J Tryptophan Res 7, 9–14, https://doi.org/10.4137/IJTR.S14084 (2014).
Yamashita, M. & Yamamoto, T. Tryptophan circuit in fatigue: from blood to brain and cognition. Brain Res. https://doi.org/10.1016/j.brainres.2017.09.002 (2017).
Pocivavsek, A., Baratta, A. M., Mong, J. A. & Viechweg, S. S. Acute Kynurenine Challenge Disrupts Sleep-Wake Architecture and Impairs Contextual Memory in Adult Rats. Sleep 40, https://doi.org/10.1093/sleep/zsx141 (2017).
Mong, J. A. & Cusmano, D. M. Sex differences in sleep: impact of biological sex and sex steroids. Philos Trans R Soc Lond B Biol Sci 371, 20150110, https://doi.org/10.1098/rstb.2015.0110 (2016).
Brown, R. R., Rose, D. P., Leklem, J. E. & Linkswiler, H. M. Effects of oral contraceptives on tryptophan metabolism and vitamin B6 requirements in women. Acta Vitaminol Enzymol 29, 151–157 (1975).
Meier, T. B. et al. Kynurenic acid is reduced in females and oral contraceptive users: Implications for depression. Brain Behav Immun, https://doi.org/10.1016/j.bbi.2017.08.024 (2017).
Jayawickrama, G. S., Nematollahi, A., Sun, G., Gorrell, M. D. & Church, W. B. Inhibition of human kynurenine aminotransferase isozymes by estrogen and its derivatives. Sci Rep 7, 17559, https://doi.org/10.1038/s41598-017-17979-7 (2017).
Leproult, R., Copinschi, G., Buxton, O. & Van Cauter, E. Sleep loss results in an elevation of cortisol levels the next evening. Sleep 20, 865–870 (1997).
Tobler, I., Murison, R., Ursin, R., Ursin, H. & Borbely, A. A. The effect of sleep deprivation and recovery sleep on plasma corticosterone in the rat. Neurosci Lett 35, 297–300 (1983).
Miura, H. et al. A link between stress and depression: shifts in the balance between the kynurenine and serotonin pathways of tryptophan metabolism and the etiology and pathophysiology of depression. Stress 11, 198–209, https://doi.org/10.1080/10253890701754068 (2008).
Ennaceur, A. & Delacour, J. A new one-trial test for neurobiological studies of memory in rats. 1: Behavioral data. Behav Brain Res 31, 47–59 (1988).
Dere, E. & Huston, J. P. & De Souza Silva, M. A. The pharmacology, neuroanatomy and neurogenetics of one-trial object recognition in rodents. Neurosci Biobehav Rev 31, 673–704, https://doi.org/10.1016/j.neubiorev.2007.01.005 (2007).
Cohen, S. J. & Stackman, R. W. Jr. Assessing rodent hippocampal involvement in the novel object recognition task. A review. Behav Brain Res 285, 105–117, https://doi.org/10.1016/j.bbr.2014.08.002 (2015).
Revel, F. G., Gottowik, J., Gatti, S., Wettstein, J. G. & Moreau, J. L. Rodent models of insomnia: a review of experimental procedures that induce sleep disturbances. Neurosci Biobehav Rev 33, 874–899, https://doi.org/10.1016/j.neubiorev.2009.03.002 (2009).
Meerlo, P., Koehl, M., van der Borght, K. & Turek, F. W. Sleep restriction alters the hypothalamic-pituitary-adrenal response to stress. J Neuroendocrinol 14, 397–402 (2002).
Palanza, P. Animal models of anxiety and depression: how are females different? Neurosci Biobehav Rev 25, 219–233 (2001).
Hardy, M. P. et al. Stress hormone and male reproductive function. Cell Tissue Res 322, 147–153, https://doi.org/10.1007/s00441-005-0006-2 (2005).
Hardy, M. P. et al. Trends of reproductive hormones in male rats during psychosocial stress: role of glucocorticoid metabolism in behavioral dominance. Biol Reprod 67, 1750–1755 (2002).
Hajali, V., Sheibani, V., Esmaeili-Mahani, S. & Shabani, M. Female rats are more susceptible to the deleterious effects of paradoxical sleep deprivation on cognitive performance. Behav Brain Res 228, 311–318, https://doi.org/10.1016/j.bbr.2011.12.008 (2012).
Hajali, V. et al. Ovariectomy does not exacerbate the negative effects of sleep deprivation on synaptic plasticity in rats. Physiology & behavior 144, 73–81, https://doi.org/10.1016/j.physbeh.2015.03.010 (2015).
Graves, L. A., Heller, E. A., Pack, A. I. & Abel, T. Sleep deprivation selectively impairs memory consolidation for contextual fear conditioning. Learn Mem 10, 168–176, https://doi.org/10.1101/lm.48803 (2003).
Vecsey, C. G. et al. Sleep deprivation impairs cAMP signalling in the hippocampus. Nature 461, 1122–1125, https://doi.org/10.1038/nature08488 (2009).
Impey, S. et al. Stimulation of cAMP response element (CRE)-mediated transcription during contextual learning. Nat Neurosci 1, 595–601, https://doi.org/10.1038/2830 (1998).
Stubley-Weatherly, L., Harding, J. W. & Wright, J. W. Effects of discrete kainic acid-induced hippocampal lesions on spatial and contextual learning and memory in rats. Brain Res 716, 29–38, https://doi.org/10.1016/0006-8993(95)01589-2 (1996).
Barker, G. R. & Warburton, E. C. When is the hippocampus involved in recognition memory? The Journal of neuroscience: the official journal of the Society for Neuroscience 31, 10721–10731, https://doi.org/10.1523/JNEUROSCI.6413-10.2011 (2011).
Alhola, P. & Polo-Kantola, P. Sleep deprivation: Impact on cognitive performance. Neuropsychiatr Dis Treat 3, 553–567 (2007).
Santhi, N. et al. Sex differences in the circadian regulation of sleep and waking cognition in humans. Proc Natl Acad Sci USA 113, E2730–2739, https://doi.org/10.1073/pnas.1521637113 (2016).
Borbely, A. A. A two process model of sleep regulation. Human neurobiology 1, 195–204 (1982).
Bjorness, T. E., Kelly, C. L., Gao, T., Poffenberger, V. & Greene, R. W. Control and function of the homeostatic sleep response by adenosine A1 receptors. The Journal of neuroscience: the official journal of the Society for Neuroscience 29, 1267–1276, https://doi.org/10.1523/JNEUROSCI.2942-08.2009 (2009).
Pocivavsek, A. et al. Fluctuations in endogenous kynurenic acid control hippocampal glutamate and memory. Neuropsychopharmacology 36, 2357–2367, https://doi.org/10.1038/npp.2011.127 (2011).
Chess, A. C., Simoni, M. K., Alling, T. E. & Bucci, D. J. Elevations of endogenous kynurenic acid produce spatial working memory deficits. Schizophr Bull 33, 797–804, https://doi.org/10.1093/schbul/sbl033 (2007).
Potter, M. C. et al. Reduction of endogenous kynurenic acid formation enhances extracellular glutamate, hippocampal plasticity, and cognitive behavior. Neuropsychopharmacology 35, 1734–1742, https://doi.org/10.1038/npp.2010.39 (2010).
Porkka-Heiskanen, T. & Kalinchuk, A. V. Adenosine, energy metabolism and sleep homeostasis. Sleep Med Rev 15, 123–135, https://doi.org/10.1016/j.smrv.2010.06.005 (2011).
Bergmann, B. M. et al. Sleep deprivation in the rat: V. Energy use and mediation. Sleep 12, 31–41 (1989).
Hodgkins, P. S. & Schwarcz, R. Metabolic control of kynurenic acid formation in the rat brain. Dev Neurosci 20, 408–416 (1998).
Giorgini, F. et al. Targeted deletion of kynurenine 3-monooxygenase in mice: a new tool for studying kynurenine pathway metabolism in periphery and brain. J Biol Chem 288, 36554–36566, https://doi.org/10.1074/jbc.M113.503813 (2013).
Villafuerte, G. et al. Sleep deprivation and oxidative stress in animal models: a systematic review. Oxidative medicine and cellular longevity 2015, 234952, https://doi.org/10.1155/2015/234952 (2015).
Blanco Ayala, T. et al. Alternative kynurenic acid synthesis routes studied in the rat cerebellum. Frontiers in cellular neuroscience 9, 178, https://doi.org/10.3389/fncel.2015.00178 (2015).
Lugo-Huitron, R. et al. On the antioxidant properties of kynurenic acid: free radical scavenging activity and inhibition of oxidative stress. Neurotoxicology and teratology 33, 538–547, https://doi.org/10.1016/j.ntt.2011.07.002 (2011).
Porkka-Heiskanen, T. et al. Adenosine: a mediator of the sleep-inducing effects of prolonged wakefulness. Science 276, 1265–1268 (1997).
Wu, H. Q., Fuxe, K. & Schwarcz, R. Neuronal A1 receptors mediate increase in extracellular kynurenic acid after local intrastriatal adenosine infusion. J Neurochem 90, 621–628, https://doi.org/10.1111/j.1471-4159.2004.02531.x (2004).
Turski, W. A. & Schwarcz, R. On the disposition of intrahippocampally injected kynurenic acid in the rat. Experimental brain research 71, 563–567 (1988).
Uwai, Y., Honjo, H. & Iwamoto, K. Interaction and transport of kynurenic acid via human organic anion transporters hOAT1 and hOAT3. Pharmacological research 65, 254–260, https://doi.org/10.1016/j.phrs.2011.11.003 (2012).
Moroni, F., Russi, P., Lombardi, G., Beni, M. & Carla, V. Presence of kynurenic acid in the mammalian brain. J Neurochem 51, 177–180 (1988).
Pawlak, D., Takada, Y., Urano, T. & Takada, A. Serotonergic and kynurenic pathways in rats exposed to foot shock. Brain research bulletin 52, 197–205 (2000).
Miura, H., Ozaki, N., Shirokawa, T. & Isobe, K. Changes in brain tryptophan metabolism elicited by ageing, social environment, and psychological stress in mice. Stress 11, 160–169, https://doi.org/10.1080/10253890701685908 (2008).
Dantzer, R., O’Connor, J. C., Lawson, M. A. & Kelley, K. W. Inflammation-associated depression: from serotonin to kynurenine. Psychoneuroendocrinology 36, 426–436, https://doi.org/10.1016/j.psyneuen.2010.09.012 (2011).
Irwin, M. R. & Olmstead, R. & Carroll, J. E. Sleep Disturbance, Sleep Duration, and Inflammation: A Systematic Review and Meta-Analysis of Cohort Studies and Experimental Sleep Deprivation. Biol Psychiatry 80, 40–52, https://doi.org/10.1016/j.biopsych.2015.05.014 (2016).
Cho, H. J. et al. Sleep disturbance and kynurenine metabolism in depression. Journal of psychosomatic research 99, 1–7, https://doi.org/10.1016/j.jpsychores.2017.05.016 (2017).
de Bie, J., Lim, C. K. & Guillemin, G. J. Kynurenines, Gender and Neuroinflammation; Showcase Schizophrenia. Neurotox Res 30, 285–294, https://doi.org/10.1007/s12640-016-9641-5 (2016).
Eskelund, A., Budac, D. P., Sanchez, C., Elfving, B. & Wegener, G. Female Flinders Sensitive Line rats show estrous cycle-independent depression-like behavior and altered tryptophan metabolism. Neuroscience 329, 337–348, https://doi.org/10.1016/j.neuroscience.2016.05.024 (2016).
Schwarcz, R., Bruno, J. P., Muchowski, P. J. & Wu, H. Q. Kynurenines in the mammalian brain: when physiology meets pathology. Nature reviews. Neuroscience 13, 465–477, https://doi.org/10.1038/nrn3257 (2012).
Freeman, D. et al. The effects of improving sleep on mental health (OASIS): a randomised controlled trial with mediation analysis. The lancet. Psychiatry, https://doi.org/10.1016/S2215-0366(17)30328-0 (2017).
Pocivavsek, A. & Rowland, L. M. Basic Neuroscience Illuminates Causal Relationship between Sleep and Memory: Translating to Schizophrenia. Schizophr Bull 44, 7–14, https://doi.org/10.1093/schbul/sbx151 (2018).
Acknowledgements
The present study was supported in part by the National Institutes of Health grants K12 HD43489–14, PD50 MH103222, R01 NS102209 and a donation from the Clare E. Forbes Trust. Special thank you to Shaun Viechweg for technical assistance.
Author information
Authors and Affiliations
Contributions
Conceived and designed experiments: A.M.B., S.A.B., J.A.M., A.P. Performed experiments and analyzed data: A.M.B., S.A.B., A.D.B., C.B.F., S.C., A.P. Wrote the manuscript: A.M.B., J.A.M., A.P.
Corresponding author
Ethics declarations
Competing Interests
The authors declare no competing interests.
Additional information
Publisher's note: Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made. The images or other third party material in this article are included in the article’s Creative Commons license, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons license and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this license, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Baratta, A.M., Buck, S.A., Buchla, A.D. et al. Sex Differences in Hippocampal Memory and Kynurenic Acid Formation Following Acute Sleep Deprivation in Rats. Sci Rep 8, 6963 (2018). https://doi.org/10.1038/s41598-018-25288-w
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41598-018-25288-w
This article is cited by
-
Two human metabolites rescue a C. elegans model of Alzheimer’s disease via a cytosolic unfolded protein response
Communications Biology (2021)
-
Sex and Menstrual Phase Influences on Sleep and Memory
Current Sleep Medicine Reports (2021)
-
RAS inhibition modulates kynurenine levels in a CKD population with and without type 2 diabetes mellitus
International Urology and Nephrology (2020)
-
Relationship of Interferon-γ to Cognitive Function in Midlife Women with Schizophrenia
Psychiatric Quarterly (2018)
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.