Abstract
It is not fully established whether leukocyte can predict the poor outcome for ruptured cerebral aneurysms (CA) or not. Here, we retrospectively analyzed the clinical data of 428 patients with ruptured CA between 2010 and 2015. Patients’ demographic data, including gender, age, history of smoking, alcohol, hypertension, diabetes and hypercholesterolemia, Hunt-Hess and Fisher grade, occurrence of hydrocephalus, aneurysm location, time to surgery, delayed ischemic neurological deficit (DIND) and peak leukocyte of blood test from day 1 to 3 after aneurysmal rupture were recorded and analyzed. In the multivariable analysis model, gender, Fisher grade, time to surgery and hydrocephalus were not relevant to poor outcome. However, Hunt-Hess grade, DIND and preoperative leukocyte count (>13.84 × 109/L) were significantly associated with adverse outcome. The respective increased risks were 5.2- (OR 5.24, 95% CI 1.67–16.50, p = 0.005), 6.2-(OR 6.24, 95% CI 3.55–10.99, p < 0.001) and 10.9-fold (OR 10.93, 95% CI 5.98–19.97, p < 0.001). The study revealed that Hunt-Hess grade, DIND and preoperative leukocyte count (>13.84 × 109/L) were independent risk factors for poor outcome of ruptured CA at 3 months. Higher leukocyte count is a convenient and useful marker to predict 3-month poor outcome for ruptured CA.
Similar content being viewed by others
Introduction
The prevalence of cerebral aneurysms (CA) affects 3–5% of the general population1, and subarachnoid hemorrhage caused by ruptured CA is a fatal or disabling stroke in these people. It was reported that several risk factors (such as older age, poor Hunt & Hess grade, higher Fisher grade, hypertension, hydrocephalus, hyperglycemia, excess weight and time to surgery) could lead to and predict the poor outcome for ruptured CA2,3.
It has been found that leukocytes are associated with the adverse prognosis in glioma4, coronary artery disease5, abdominal aortic aneurysms6. Pozzilli7 and Yoshimoto8 reported that higher leukocyte counts in peripheral blood were acute systemic inflammatory response following subarachnoid hemorrhage, and the number of leukocytes reflected the degree of brain tissue damage and predicted further secondary brain injury. Recent studies suggested that elevated leukocyte count predicted the adverse outcome in ischemic and hemorrhagic stroke9,10. Previous studies have shown a relationship between leukocytosis and cerebral aneurysm, but it is still not fully established whether leukocyte can predict the poor outcome for ruptured CA or not. A common limitation in these studies was a relatively small number of patients (less than 172) treated by surgical clipping11,12,13,14. In order to test the hypothesis that preoperative higher leukocyte count is associated with and predict the poor outcome at 3 months, we retrospectively analyzed the clinical data of a relatively large number of patients with ruptured CA treated with microsurgical clipping.
Methods
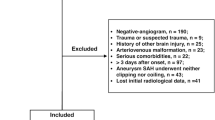
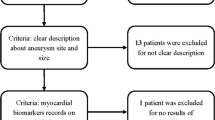
All procedures performed in this study involving human participants were in accordance with the 1964 Helsinki declaration and approved by the ethics committee of First Affiliated Hospital of Fujian Medical University. Informed consent was obtained from all individual participants included in the study. Four hundred and twenty eight patients with ruptured CA between 2010 and 2015 were collected. Gender, age, history of smoking, alcohol, hypertension, diabetes, hypercholesterolemia, Hunt-Hess and Fisher grade on admission, acute hydrocephalus, aneurysm location, time to surgery, delayed ischemic neurological deficit (DIND), peak leukocyte count of blood test from day 1–3 after ruptured were recorded. Patients were eligible for enrollment if following criteria were met: (1) Subarachnoid hemorrhages were confirmed by Computed Tomography (CT). Then the CA were diagnosed by computed tomography angiography (CTA) or digital subtraction angiography (DSA); (2) All aneurysms underwent microsurgery, and postoperative CTA and/or DSA were performed. The exclusion criteria were: (1) Ruptured CA were detected over 3 days; (2) The patients presented with herniation, or were associated with the other cerebrovascular diseases (such as arteriovenous malformations, arteriovenous fistula, and moyamoya disease) and brain tumor; (3) The patients were associated with fever (over 38 °C), infection, inflammatory process, or received any medical treatment that might have an influence on the leukocyte count in peripheral blood.
Management of ruptured CA
CTA or DSA was performed during the first 24 hours after admission. After being confirmed, aneurysms were repaired with microsurgical treatment. After aneurysmal clipping, the patients were managed with a traditional treatment of aneurysmal subarachnoid hemorrhage, including prevention of cerebral vasospasm, improving cerebral blood flow, prevention of stress ulcers and nutritional support. CT scanning for detecting postoperative complications has been performed within 24 hours after surgical treatment. The neurological outcome was assessed at the 3-month follow-up and categorized according to the patients’ modified Rankin Scale (mRS) score. A favorable outcome was defined as mRS 0–3, while a poor outcome as mRS 4–6.
Statistical Analysis
All the statistical analyses were performed using SPSS version 22.0 (IBM Corp., Armonk, NY, USA). The significance of differences in continuous data was determined with one-way variance (ANOVA) and Student’s t test. Qualitative data were compared using a chi-squared test (χ2 test) or Fisher’s exact test. Multivariable analysis logistic regression analyses included all variables significance level at p < 0.15 in univariate analysis. For inclusion in the multivariable analysis model, age was dichotomized as “less than 60 years” and “more than 60 years”15, Hunt-Hess grade as “low grade (Grade I-III)” and “high grade (Grade IV-V)”, Fisher grade as “low grade (Grade 1, 2, 3)” and “high grade (Grade 4)”, surgical time as “less than 3 days” and “more than 3 days”, leukocyte counts as “≤ optimal cutoff value” and “> optimal cutoff value”. P < 0.05 was deemed statistically significant. A MedCalc 15.2.2 (MedCalc Software, Mariakerke, Belgium) was used to generate the receiver operating curve (ROC) and analyze the specificity, sensitivity, negative predictive values of leukocytes and positive predictive values of leukocytes for mRS.
Results
Four hundred and twenty eight patients were included in the retrospective study according to the upper inclusion and exclusion criteria. The clinical characteristics of these patients with ruptured CA are shown in Table 1. The mean age of 307 (72%) patients in the good outcome group was55.8 ± 10.6 years, and 121 (28%) patients with a poor outcome was 56.6 ± 10.8 years (p > 0.05). The univariate analysis indicated there were significant differences were detected in gender, Fisher grade, hydrocephalus, time to surgery, DIND, leukocyte count between favorable and poor groups (p < 0.05). One hundred and ninety-four patients (45%) were male, 234 (55%) were female, the difference of the gender distribution between the two groups was statistically significant (p < 0.05). There were no significant statistical differences in the number of the patients with history of smoking, alcohol, hypertension, diabetes, hypercholesterolemia between the two groups (p > 0.05). The aneurysm location between the two groups was not significantly statistical difference (p > 0.05). There was no significant difference of preoperative rebleeding between the two groups (6 patients in the favorable and 4 in the poor outcome group) (p > 0.05).
The median peak leukocyte count (×109/L) in the good outcome group (10.34 ± 3.23) was lower than that in the poor outcome group (15.24 ± 5.47). The receiver operating characteristic (ROC) curve is shown in Fig. 1. The optimal cutoff value for leukocyte as a predictor for 3-month status was determined as 13.84 (×109/L) in the ROC curve (sensitivity was 60.3%, and the specificity was 88.3%). In addition, the mean of leukocyte count in patients with Hunt-Hess grade IV-V (16.98 ± 6.54) was higher than that in Hunt-Hess grade I-III (11.33 ± 4.12), the difference was statistically significant (p < 0.001).
Multivariate logistic regression model for mRS was built, and we included all preoperative variables (gender, Fisher grade, time to surgery, hydrocephalus, DIND and leukocyte count) with a significance level at p < 0.15 in the univariate analysis. The results revealed that Hunt-Hess grade, Fisher grade, hydrocephalus, DIND and leukocyte count were associated with 3-month poor outcome. After adjustment for potential confounding variables, gender, Fisher grade, time to surgery and hydrocephalus were not relevant to poor outcome, while Hunt-Hess grade, DIND and preoperative leukocyte count (greater than 13.84 × 109/L) remained significantly associated with adverse outcome (Table 2), the respective increased risks were 5.2-[odd ratio (OR)5.24, 95% confidence interval (CI)1.67–16.50, p = 0.005], 6.2-(OR6.24, 95% CI 3.55–10.99, p < 0.001) and 10.9-fold (OR10.93, 95% CI 5.98–19.97, p < 0.001) (Table 2).
Multivariate logistic regression model for DIND was also built to include the preoperative variables with a significance level at p < 0.15 in the univariate analysis. The results revealed that Hunt-Hess grade IV-V and a serum leukocyte count greater than 13.84 × 109/L were associated with DIND, the increased risks were 2.4-fold (OR2.41, 95% CI 1.40–5.60, p = 0.040) and 1.7-fold (OR1.73, 95% CI 1.08–2.78, p = 0.023) respectively (Table 3).
Discussion
The incidence of poor outcome reported in previous studies ranged from 20 to 40%16,17. In this 6-year review of 428 consecutive patients with ruptured CA, the risk factors including gender, Fisher grade on admission, time of surgery, hydrocephalus and preoperative higher leukocyte count between the two groups are statistically significant, which may be associated with 3-month poor outcome. Previous studies indicated that hydrocephalus and time to surgery were associated with poor outcome of ruptured CA18,19. However, in the logistic regression models, it was found that only three variables (Hunt-Hess grade, DIND and preoperative higher leukocyte count) were the independent risk factors for predicting 3-month poor outcome, while female gender, higher Fisher grade, hydrocephalus and time to surgery not.
Neuronal and axonal damage may occur in the pathophysiological process after aneurysmal rupture20, and a deterioration of the clinical neurological condition was observed. It is no doubt that poor Hunt-Hess grade on admission strongly predicted the poor outcome in aneurysmal subarachnoid hemorrhage, and our finding is consistent with prior report21. We found that the leukocyte count in the patients with Hunt-Hess grade I-III on admission was lower than that in Hunt-Hess grade IV-V within 3 days after aneurysm rupture. Thus, leukocyte count in peripheral blood may be associated with the severity of the acute primary injury of the brain tissue. Furthermore, our findings suggested that Hunt-Hess grade IV-V and a serum leukocyte count greater than 13.84 × 109/L in this study were associated with developing DIND, which was related to poor outcome22,23,24.
As we know, the increased leukocyte count may be the result of acute phase response and reflects the severity of disease and tissue inflammatory response. In 1974, Neil-Dwyer and Cruichshank14 firstly revealed that higher leukocyte count was associated with the unfavorable outcome of ruptured CA. On the contrary, Spallone12 found no relationship between the admission higher leukocyte count and ischemic complications. Therefore, studies assessing the role of leukocyte in the adverse outcome of ruptured CA have yielded conflicting conclusions12,13.
Interestingly, the main finding of our study revealed that higher leukocyte count before microsurgical treatment was an independent risk factor for poor outcome of ruptured CA at 3 months. Previous results showed that the inflammatory reaction occured after cerebral aneurysm rupture. Leukocytes in peripheral blood would be recruited within the first several hours because of the blood released into the subarachnoid space25, which would increase intracranial pressure and lead to early brain injury (EBI). Accompanying with releasing chemotactic factor into the central nervous system and an increase in the number of leukocytes in peripheral blood, the leukocyte will be recruited in the brain microvasculature26, which is associated with blood–brain barrier disruption and basal lamina degradation27. As a result, brain edema might occur or be aggravated together with neuroinflammation-promoted apoptosis in sympathetic neurons, which would further aggravate secondary brain damage28.
It is noteworthy that several molecular mechanisms including Angiotensin II (Ang II)29, myeloperxidase30, NF-κB31, cyclooxygenase-2 (COX-2) and microsomal prostaglandin E2 synthase-1 (mPGES-1)32, were associated with the adverse outcome after aneurysm rupture, but the detailed mechanisms of leukocyte in cerebral aneurysm remain obscure. A growing body of evidence suggested that leukocyte infiltration in the aneurysmal wall contributed to the formation, growth and rupture of cerebral aneurysm, which is increasingly recognized as an inflammatory process33. Furthermore, histopathological findings of aneurysmal wall indicated that the more leukocytes were observed, the more fragile aneurysms became34.
Several inflammatory mediators synthesized and/or expressed by leukocyte, such as IL-1β, IL-6, TNF-α, TLR4, and matrix metalloproteinases, will further aggravate the local inflammatory response which is closely related to an adverse outcome35. Maiuri, et al.36 and McGirt, et al.11 came to a common conclusion that leukocyte counts had a high prognostic value in predicting cerebral vasospasm which was associated with neurological deterioration and poor outcome. Inhibiting the inflammatory response and reducing leukocyte activity was highly beneficial in limiting secondary brain injury and increasing survival after aneurysm rupture37.
Limitation
In the retrospective study, the other biomarkers, such as Erythrocyte Sedimentation Rate (ESR), C Reactive Protein (CRP), complement C3 and C9, were not included in the study. Further other biomarkers examination should be performed.
Conclusion
Hunt-Hess grade, DIND and preoperative higher leukocyte count (>13.84 × 109/L) before microsurgical treatment were independent risk factors for poor outcome of ruptured CA at 3 months. Higher leukocyte count before microsurgical treatment is a convenient and useful marker to predict poor outcome of ruptured cerebral aneurysm at 3 months.
Change history
24 August 2018
A correction to this article has been published and is linked from the HTML and PDF versions of this paper. The error has been fixed in the paper.
References
Brisman, J. L., Song, J. K. & Newell, D. W. Cerebral aneurysms. The New England journal of medicine 355, 928–939, https://doi.org/10.1056/NEJMra052760 (2006).
Juvela, S., Siironen, J. & Kuhmonen, J. Hyperglycemia, excess weight, and history of hypertension as risk factors for poor outcome and cerebral infarction after aneurysmal subarachnoid hemorrhage. Journal of neurosurgery 102, 998–1003, https://doi.org/10.3171/jns.2005.102.6.0998 (2005).
Zipfel, G. J. Ultra-early surgery for aneurysmal subarachnoid hemorrhage. Journal of neurosurgery 122, 381–382, https://doi.org/10.3171/2014.8.JNS141613 (2015).
Chen, Y. et al. High leukocyte mitochondrial DNA content contributes to poor prognosis in glioma patients through its immunosuppressive effect. British journal of cancer 113, 99–106, https://doi.org/10.1038/bjc.2015.184 (2015).
Madjid, M., Awan, I., Willerson, J. T. & Casscells, S. W. Leukocyte count and coronary heart disease: implications for risk assessment. Journal of the American College of Cardiology 44, 1945–1956, https://doi.org/10.1016/j.jacc.2004.07.056 (2004).
Onuk, T. et al. Increased Neutrophil to Lymphocyte Ratio is Associated with In-Hospital Mortality in Patients with Aortic Dissection. Clinical laboratory 61, 1275–1282 (2015).
Pozzilli, C. et al. Peripheral white blood cell count in cerebral ischemic infarction. Acta neurologica Scandinavica 71, 396–400 (1985).
Yoshimoto, Y., Tanaka, Y. & Hoya, K. Acute systemic inflammatory response syndrome in subarachnoid hemorrhage. Stroke; a journal of cerebral circulation 32, 1989–1993 (2001).
Agnihotri, S., Czap, A., Staff, I., Fortunato, G. & McCullough, L. D. Peripheral leukocyte counts and outcomes after intracerebral hemorrhage. Journal of neuroinflammation 8, 160, https://doi.org/10.1186/1742-2094-8-160 (2011).
Furlan, J. C., Vergouwen, M. D., Fang, J. & Silver, F. L. White blood cell count is an independent predictor of outcomes after acute ischaemic stroke. European journal of neurology 21, 215–222, https://doi.org/10.1111/ene.12233 (2014).
McGirt, M. J. et al. Leukocytosis as an independent risk factor for cerebral vasospasm following aneurysmal subarachnoid hemorrhage. Journal of neurosurgery 98, 1222–1226, https://doi.org/10.3171/jns.2003.98.6.1222 (2003).
Spallone, A., Acqui, M., Pastore, F. S. & Guidetti, B. Relationship between leukocytosis and ischemic complications following aneurysmal subarachnoid hemorrhage. Surgical neurology 27, 253–258 (1987).
Parkinson, D. & Stephensen, S. Leukocytosis and subarachnoid hemorrhage. Surgical neurology 21, 132–134 (1984).
Neil-Dwyer, G. & Cruickshank, J. The blood leucocyte count and its prognostic significance in subarachnoid haemorrhage. Brain: a journal of neurology 97, 79–86 (1974).
Degos, V. et al. Elderly age as a prognostic marker of 1-year poor outcome for subarachnoid hemorrhage patients through its interaction with admission hydrocephalus. Anesthesiology 117, 1289–1299, https://doi.org/10.1097/ALN.0b013e318267395b (2012).
Kassell, N. F., Sasaki, T., Colohan, A. R. & Nazar, G. Cerebral vasospasm following aneurysmal subarachnoid hemorrhage. Stroke; a journal of cerebral circulation 16, 562–572 (1985).
Oliveira-Filho, J. et al. Fever in subarachnoid hemorrhage: relationship to vasospasm and outcome. Neurology 56, 1299–1304 (2001).
Hasan, D., Vermeulen, M., Wijdicks, E. F., Hijdra, A. & van Gijn, J. Management problems in acute hydrocephalus after subarachnoid hemorrhage. Stroke; a journal of cerebral circulation 20, 747–753 (1989).
Phillips, T. J., Dowling, R. J., Yan, B., Laidlaw, J. D. & Mitchell, P. J. Does treatment of ruptured intracranial aneurysms within 24 hours improve clinical outcome? Stroke; a journal of cerebral circulation 42, 1936–1945, https://doi.org/10.1161/STROKEAHA.110.602888 (2011).
Helbok, R. et al. Early neurological deterioration after subarachnoid haemorrhage: risk factors and impact on outcome. Journal of neurology, neurosurgery, and psychiatry 84, 266–270, https://doi.org/10.1136/jnnp-2012-302804 (2013).
Kremer, C., Groden, C., Hansen, H. C., Grzyska, U. & Zeumer, H. Outcome after endovascular treatment of Hunt and Hess grade IV or V aneurysms: comparison of anterior versus posterior circulation. Stroke; a journal of cerebral circulation 30, 2617–2622 (1999).
Marquardt, L. et al. Inflammatory response after acute ischemic stroke. Journal of the neurological sciences 236, 65–71, https://doi.org/10.1016/j.jns.2005.05.006 (2005).
Intiso, D. et al. Tumor necrosis factor alpha serum levels and inflammatory response in acute ischemic stroke patients. Neurological sciences: official journal of the Italian Neurological Society and of the Italian Society of Clinical Neurophysiology 24, 390–396, https://doi.org/10.1007/s10072-003-0194-z (2004).
Provencio, J. J. et al. CSF neutrophils are implicated in the development of vasospasm in subarachnoid hemorrhage. Neurocritical care 12, 244–251, https://doi.org/10.1007/s12028-009-9308-7 (2010).
Aronowski, J. & Zhao, X. Molecular pathophysiology of cerebral hemorrhage: secondary brain injury. Stroke; a journal of cerebral circulation 42, 1781–1786, https://doi.org/10.1161/STROKEAHA.110.596718 (2011).
Carvalho-Tavares, J. et al. A role for platelets and endothelial selectins in tumor necrosis factor-alpha-induced leukocyte recruitment in the brain microvasculature. Circulation research 87, 1141–1148 (2000).
Khatri, R., McKinney, A. M., Swenson, B. & Janardhan, V. Blood-brain barrier, reperfusion injury, and hemorrhagic transformation in acute ischemic stroke. Neurology 79, S52–57, https://doi.org/10.1212/WNL.0b013e3182697e70 (2012).
Carson, M. J., Thrash, J. C. & Walter, B. The cellular response in neuroinflammation: The role of leukocytes, microglia and astrocytes in neuronal death and survival. Clinical neuroscience research 6, 237–245, https://doi.org/10.1016/j.cnr.2006.09.004 (2006).
Pena Silva, R. A. et al. Angiotensin 1-7 reduces mortality and rupture of intracranial aneurysms in mice. Hypertension 64, 362–368, https://doi.org/10.1161/HYPERTENSIONAHA.114.03415 (2014).
Chu, Y. et al. Myeloperoxidase is increased in human cerebral aneurysms and increases formation and rupture of cerebral aneurysms in mice. Stroke; a journal of cerebral circulation 46, 1651–1656, https://doi.org/10.1161/STROKEAHA.114.008589 (2015).
Aoki, T. et al. NF-kappaB is a key mediator of cerebral aneurysm formation. Circulation 116, 2830–2840, https://doi.org/10.1161/CIRCULATIONAHA.107.728303 (2007).
Hasan, D. et al. Upregulation of cyclooxygenase-2 (COX-2) and microsomal prostaglandin E2 synthase-1 (mPGES-1) in wall of ruptured human cerebral aneurysms: preliminary results. Stroke; a journal of cerebral circulation 43, 1964–1967, https://doi.org/10.1161/STROKEAHA.112.655829 (2012).
Chalouhi, N. et al. Biology of intracranial aneurysms: role of inflammation. Journal of cerebral blood flow and metabolism: official journal of the International Society of Cerebral Blood Flow and Metabolism 32, 1659–1676, https://doi.org/10.1038/jcbfm.2012.84 (2012).
Kataoka, K. et al. Structural fragility and inflammatory response of ruptured cerebral aneurysms. A comparative study between ruptured and unruptured cerebral aneurysms. Stroke; a journal of cerebral circulation 30, 1396–1401 (1999).
Fennell, V. S., Kalani, M. Y., Atwal, G., Martirosyan, N. L. & Spetzler, R. F. Biology of Saccular Cerebral Aneurysms: A Review of Current Understanding and Future Directions. Frontiers in surgery 3, 43, https://doi.org/10.3389/fsurg.2016.00043 (2016).
Maiuri, F., Gallicchio, B., Donati, P. & Carandente, M. The blood leukocyte count and its prognostic significance in subarachnoid hemorrhage. Journal of neurosurgical sciences 31, 45–48 (1987).
Starke, R. M., Chalouhi, N., Ding, D. & Hasan, D. M. Potential role of aspirin in the prevention of aneurysmal subarachnoid hemorrhage. Cerebrovasc Dis 39, 332–342, https://doi.org/10.1159/000381137 (2015).
Acknowledgements
The study was supported by special fund for public health of Fujian province department of finance (NO.BPB-LZY2013 to Zhang-Ya Lin), key clinical specialty discipline construction program of Fujian, P.R.C, major project of Fujian provincial department of science and technology (NO.2014YZ0003 and NO. 2014YZ01 to De-Zhi Kang) and the Young and Middle-aged Backbone Key Research Project of National Health and Family Planning Commission of Fujian Province (No. 2017-ZQN-46 to Pei-Sen Yao).
Author information
Authors and Affiliations
Contributions
Study concept and design: Shu-Fa Zheng, Zhang-Ya Lin and De-Zhi Kang. Acquisition of data: Pei-Sen Yao, Guo-Rong Chen, Xue-Ling Xie, Huang-Cheng Shang-Guan and Jin-Zhen Gao. Analysis and interpretation of data: Pei-Sen Yao,Guo-Rong Chen, Xue-Ling Xie, Huang-Cheng Shang-Guan and Jin-Zhen Gao. Study supervision: Pei-Sen Yao, Guo-Rong Chen, Xue-Ling Xie and Yuan-Xiang Lin. Critical revision of manuscript for intellectual content: Shu-Fa Zheng.
Corresponding authors
Ethics declarations
Competing Interests
The authors declare no competing interests.
Additional information
Publisher's note: Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made. The images or other third party material in this article are included in the article’s Creative Commons license, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons license and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this license, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Yao, PS., Chen, GR., Xie, XL. et al. Higher leukocyte count predicts 3-month poor outcome of ruptured cerebral aneurysms. Sci Rep 8, 5799 (2018). https://doi.org/10.1038/s41598-018-23934-x
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41598-018-23934-x
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.