Abstract
Sarcopenia is associated with loss of muscle mass as well as an increased risk of physical disability in elderly people. This study was aimed to investigate the effect of elastic band resistance training (ERT) on muscle mass and physical function in older women with sarcopenic obesity. A randomized controlled trial with an intention-to-treat analysis was conducted. A total of 56 women (mean ± SD age 67.3 ± 5.1 years) were randomly assigned to the experimental group receiving 12 weeks of ERT and to the control group receiving no exercise intervention. Lean mass (measured using a dual-energy X-ray absorptiometer), physical capacity (assessed using the global physical capacity score), and a 36-item short form questionnaire were conducted at the baseline examination (T0), as well as the 3-month (T1) and 9-month followups (T2). At T1 and T2, the between-group difference was measured in total skeletal mass relative to T0, with mean differences of 0.70 kg (95% CI 0.12–1.28; P < 0.05) and 0.72 kg (95% CI 0.21–1.23; P < 0.01), respectively. Similar results were found in muscle quality, physical capacity, and physical function outcomes. The ERT exerted a significant beneficial effect on muscle mass, muscle quality, and physical function in older women with sarcopenic obesity.
Similar content being viewed by others
Introduction
Sarcopenic obesity, a recently identified phenotype of obese elderly people, is engendered by the additive effect of sarcopenia and obesity1. Although sarcopenia has been termed as—and is characterized by—age-related muscle wasting2, obesity involving an increase in adipose tissue is also considered a major cause of skeletal muscle loss3. Such a decline in muscle mass followed by insufficient muscle power contributes to low physical performance in frail elderly people4,5. Furthermore, reports have associated obesity with physical disability6,7. Under these circumstances, studies have identified that sarcopenic obesity with its underlying additive effect of muscle loss is associated with a higher level of physical limitations than sarcopenia or obesity alone; moreover, sarcopenic obesity is considered a risk factor for disability and frail conditions5,8,9.
Muscle mass is maintained through regulation of the balance of skeletal muscle turnover between muscle protein synthesis and breakdown. However, both age-related sarcopenia and obesity are associated with the overexpression of myostatin, which functions as a protein inhibitor that negatively regulates skeletal muscle growth and homeostasis, as well as with the inhibition of myoblast proliferation and differentiation10,11,12. Previous trials have shown that resistance exercise training (RET) facilitates the initiation of muscle anabolism and increases the muscle protein synthesis rate in older adults13,14,15. Following RET, the net muscle protein balance, which denotes the difference between protein synthesis and breakdown, becomes less negative or even positive after protein supplementation16; this may further prevent skeletal muscle attenuation due to age. Hence, determining whether RET affects the loss of muscle mass in older adults with sarcopenic obesity is crucial.
RET has been used as an effective means of improving muscle function and increasing muscle mass in frail elderly people3,14,17. Resistance-type training using elastic bands has been frequently applied as a treatment method and is a safe approach for muscle strengthening in elderly adults18,19, with the results revealing muscle activations and self-perceived efficacy similar to those observed from free-weight resistance training20. Such training is used not only because of its simplicity and convenience but also its ability to strengthen the musculoskeletal system, which further benefits physical mobility21,22. In addition, an exercise program involving elastic tubing resistance training can provide more benefits compared with conventional free-weight resistance programs, such as increased functional strength, more effective injury prevention, greater ability to change muscle emphasis during exercises, and greater muscle power development23. Therefore, to help muscle strengthening with reduced burdens on joints, elastic tubing resistance training can be one of the most suitable resistive exercise programs for elderly people19.
Elastic band exercises are beneficial for elderly people. A study described the benefits of elastic resistance exercise involving. Theraband or tubing in preventing obesity or sarcopenia24. However, the effects of elastic band-based RET on muscle strength, body composition, and physical function (PF) in older women with sarcopenic obesity remain unclear. Therefore, in the present study, we investigated the effects of an elastic RET regime on muscle mass gain and PF in older women with this condition. In addition, we examined whether change in muscle mass was associated with physical capacity and function outcomes. We hypothesized that an elastic band RET regime could improve body composition and PF in older women with sarcopenic obesity.
Results
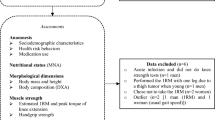
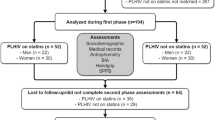
Figure 1 depicts a flowchart of this study. A total of 63 patients were recruited. After 7 patients were excluded, 56 were enrolled and randomly allocated to either the experimental group (EG, n = 33) or control group (CG, n = 23) at baseline (T0). Subsequently, 30 patients in the EG and 20 patients in the CG completed the 3-month followup (T1). Moreover, 29 patients in the EG and 18 patients in the CG completed the 9-month followup assessments (T2). Based on the intention-to-treat principle, a total of nine pieces of missing data (six at T1 and three at T2) were imputed using the last-observation-carried-forward technique. At baseline, all patients were identified as sarcopenic, with a mean (SD) percentage skeletal muscle mass index (SMI) of 24.95% (2.48%), and obese with a percentage body fat (BF %) of 41.61% (7.34%). The majority of included patients (more than 80% in each group) were considered physically inactive based on self-reported participation levels in recreational physical or leisure activities (e.g., walking and running) of less than 1 h/wk within the previous 3 months. The compliance rate of the patients who participated in exercise interventions (i.e., EG) was 97.6% without any side effects being reported during their exercise period. Patients’ characteristics are presented in Table 1. An unequal distribution of baseline characteristics was noted despite no significant between-group differences being observed in patient characteristics. Therefore, we controlled for potential confounders between the two groups using age, comorbidities, and uneven baseline scores of measures as covariates in the statistical analysis.
Muscle mass outcome
Table 2 presents the adjusted mean change in the muscle mass and muscle index outcomes at T1 and T2. In the EG, the appendicular lean mass (ALM) at T1 and appendicular muscle index (AMI) at both T1 and T2 were significantly improved (all P < 0.05), compared with those at T0. In addition, after adjusting for baseline data, significant between-group differences in the absolute muscle mass variables and relative muscle mass indices were observed at T1 and T2. Compared with the CG, the EG exhibited significantly greater changes in total skeletal mass (TSM) at T1 and T2, with a mean difference (MD) of 0.70 kg (95% CI: 0.12–1.28; P < 0.05) and 0.72 kg (95% CI: 0.21–1.23; P < 0.01), respectively; similar results were observed for ALM, AMI, total lean mass index (LMI), and SMI (Table 2).
Physical capacity and function outcomes
Table 3 presents the mean values of the physical capacity and function outcome measures at various time points and the changes in values relative to the baseline. The changes in the physical capacity and function outcomes at T1 and T2 are also shown in Fig. 2. Significant between-group differences in the outcomes of all functional mobility tasks, muscle quality (MQ), and PF were observed at T1 and T2, with the difference in values in the various mobility and physical measures significantly exceeding the minimum clinically important difference (MCID) values (Table 3; Fig. 2). At T1, the EG walked faster by 0.14 m/s (P < 0.05), reached further by 7.46 cm (P < 0.001) in the functional forward reach (FFR) task, balanced for a longer time of 9.71 s (P < 0.001) in the single leg stance (SLS) test, spent a shorter time of 1.64 s (P < 0.001) in the Timed Up & Go (TUG) test, and completed 2.99 more repetitions (P < 0.001) of the timed chair rise (TCR) task than the CG did; similar results were observed at T2 (Table 3). Relative to the baseline, the global physical capacity score (GPCS) in the EG was significantly improved at T1 and T2, with adjusted changes of 1.34 (95% CI: 0.45–2.23; P < 0.05) and 1.96 (95% CI: 0.98–2.95; P < 0.001), respectively. Significant between-group differences were also obtained at T1 (MD 3.57, 95% CI: 2.16–4.97; P < 0.001) and T2 (MD 4.22, 95% CI: 2.67–5.77; P < 0.001) after adjustment for age and comorbidity score.
Changes in physical capacity and function outcomes at the 3-month follow-up (T1) and 9-month follow-up (T2) relative to the baseline (T0). The Y-axis represents the percentage change from the baseline. The error bar represents standard error. All data are presented as percentage change from the baseline and were adjusted for age, comorbidity score, body mass index, and body fat percentage at the baseline. *Significant difference as compared with the baseline, P < 0.05; **P < 0.01; ***P < 0.001. #Significant difference compared with the control group, P < 0.05; ##P < 0.01; ###P < 0.001. MQ-UE = muscle quality of the upper extremity; MQ-LE = muscle quality of the lower extremity; GS = gait speed; TUG = timed up and go; TCR = timed chair rise; FFR = functional forward reach; SLS = single leg stance; GPCS = global physical capacity score; SF-36 PF = 36-item Short Form Health Survey, physical function subscore; SF-36 PCS = 36-item Short Form Health Survey, physical component summary.
At T1 and T2, the EG exhibited significantly greater increases in the Medical Outcomes Study Short Form-36 Questionnaire (SF-36) PF subscore, with MDs of 13.00 (95% CI: 5.03–20.98; P < 0.01) and 13.62 (95% CI: 6.47–20.76; P < 0.001), respectively, as well as in the physical component summary (PCS) score, with MDs of 13.42 (95% CI: 6.62–20.22; P < 0.001) and 15.06 (95% CI: 8.36–21.76; P < 0.001), respectively (Table 3; Fig. 2).
Muscle mass change is associated with physical capacity and function outcomes
The Pearson correlation analysis showed that the changes in the muscle mass measures correlated with improvements in MQ, GPCS, and the SF-36 PF and PCS at T2 (Table 4). All of the muscle mass measures were entered stepwise into a linear regression model. Five iterations of multiple linear regression were performed to analyze the T2 data (Table 5), and the results indicated that a change in relative muscle mass (i.e., SMI and LMI) was associated with improved changes in physical outcome measures at T2. After controlling for group allocation, age, and comorbidity score, the adjusted change in relative muscle mass was significantly associated with improved MQ (R2 = 0.68, P < 0.001), GPCS (R2 = 0.55, P < 0.001), SF-36 PF (R2 = 0.35, P < 0.001), and SF-36 PCS (R2 = 0.36, P < 0.001).
Discussion
In this study, we investigated the effects of 12-week Theraband-based elastic resistance training on body composition and PF in older women with sarcopenic obesity. The results revealed that the EG had a significantly more favorable outcome for muscle mass and physical capacity (i.e., distance of FFR, time for TUG and SLS, effort of TCR, GS, and the SF-36 PF subscore) at T1 and T2, compared with the CG; in addition, the changes in muscle mass indices were independently associated with changes in PF outcome.
Unequal distribution of characteristics occurred at the baseline. Because of the unconstrained randomization procedure and the limited sample size, an equal distribution of baseline variables among the groups was not possible. Simple randomization is considered to have a probability of treatment imbalance, the potential for selection bias, and potential effects on power25. We therefore controlled for potential confounders between groups using baseline characteristics as covariates in our analysis. In addition, controlling for baseline differences in randomized controlled trials may improve the power without introducing bias26,27. All of these factors may explain the significant differences in muscle mass and physical outcome between the two groups.
Based on the fact that type-II myofiber atrophy is associated with aging and that RET predominantly benefits type-II myofiber hypertrophy, resistance-type exercises help elderly individuals with sarcopenia or obesity to counterforce muscle-attenuated physical difficulties through increasing muscle synthesis and muscle strength3,14,17. Because type-II myofibers have a recruitment pattern characteristic of high-threshold motor units, an intensity as high as 80%–95% of one repetition maximum (1RM) is required when setting an exercise intervention regarding type-II myofiber force production28,29. However, applying a heavy load ≥80% of 1RM is difficult for older populations, we considered the physiological stress related to the exercise load and set the exercise intensity based on the rating of perceived exertion (RPE) scale and RM load29. The exercise protocol was performed with a moderate-intensity on the RPE scale up to 13, which corresponded to a 60%–70% of 1RM load30, and was utilized with a 10RM and a 20RM exercise prescription. Our results were supported by the previous study demonstrating that intermediate RM load (9–11RM) exerts dramatically hypertrophic effects whereas high RM load (20–28RM) appears better adapted for submaximal and prolonged contractions31.
Based on the size principle, our training load did not provide an adequate hypertrophic stimulus for type-II motor unit recruitment28. However, previous studies had shown that older adults receiving variable resistance (i.e., 65% 1RM) exhibited as well increases in fat free mass as those receiving high resistance (i.e., 80% 1RM) did32; the results support our findings that patients receiving elastic RET had significant gains in muscle mass compared with those in the CG after the intervention. Our results further indicate that RET not only helps elderly people with sarcopenic obesity to improve their muscle mass but also to increase muscle strength, which may further overcame physical difficulties.
RET using elastic bands has recently been applied to obese33,34,35,36 and nonobese18,21,22,24,37,38,39 older adults safely and effectively19, regardless of the various protocols. Overall, relevant studies have used exercise protocols with an intervention period of 8–24 weeks, a frequency of 2–5 times per week, and a low to moderate-intensity. In general, studies have reported that body composition is improved through significant reductions in fat mass and increases in lean mass33,35, which also positively affect muscle structural change18, strength gain18,22,33,35,39, and functional mobility24,33,34,36,37,38,39. The results of relevant studies on elastic resistance exercise in elderly people support our findings concerning older individuals with sarcopenic obesity. Moreover, we determined that 12 weeks of moderate-intensity elastic RET exerted significant benefits on fat mass reduction, lean mass gain, strength gain, and functional mobility.
In this study, relative muscle mass indices (i.e., AMI, LMI, and SMI) generally showed greater correlations with improvements in PF measures, compared with absolute muscle mass variables (i.e., ASM and TLM); in addition, changes in relative muscle mass indices, rather than absolute muscle mass variables, were significantly associated with the improvement of physical outcomes. Sternfeld et al. reported a similar finding that absolute muscle mass was not significantly associated with functional mobility in older women40. Furthermore, in older obese people, low absolute skeletal muscle mass was not assumed to be associated with physical disability or mortality41,42. The implication of these observations is that interventions aimed at improving PF through changes in muscle mass may require a different emphasis in older women with sarcopenic obesity.
Our study has certain limitations. First, only female patients were included. Based on the sex-specific response to RET, our results might not be generalizable to all elderly populations. Second, neither lifetime physical activity nor lifestyle habits were specifically controlled; in addition, we did not objectively measure physical activity level using self-reported questionnaires such as the International Physical Activity Questionnaire or using measuring devices such as accelerometers. However, all participants were instructed to maintain their usual habits throughout the followup period. Third, we did not include an aerobic training program in our exercise regime, which mainly involved RET. The interventions combining aerobic training and RET for older adults have been reported to be more effective than those involving RET only for maintaining muscle mass3. However, the lean mass (or skeletal muscle mass) and muscle strength in older adults with obesity who received an RET-only exercise regime and in those who received a combination exercise regime (RET and aerobic exercise) have been reported as being comparable43,44. These findings justify our exercise protocol, which targeted the outcomes of muscle mass and function in older women with sarcopenic obesity.
Fourth, a discrepancy was observed between the numbers of participants in our experimental and control groups when the unrestricted randomization method was used. No significant differences were observed in the baseline characteristics of the participants between the two groups in this study, and potential confounders between the groups were controlled using baseline characteristics as covariates in the statistical analysis. However, our results were based on unequal group sizes, which may have introduced bias in the statistical analysis and may have consequently reduced the power of the study. Finally, we did not include a diet or nutrition supplement control during the exercise intervention. Therefore, we could not draw any conclusions regarding the relationship between nutrition supplements and changes in body composition during RET. Dietary patterns or nutrition supplements (e.g., protein) may interfere in changes to whole body weight or muscle mass during RET45,46.
In conclusion, this prospective study demonstrated that 12 weeks of elastic RET exerted positive benefits on muscle mass and functional capacity outcomes in older women with sarcopenic obesity. The results suggest that greater emphasis should be placed on elastic RET for muscle mass and strength gain in patients with sarcopenic obesity. The elastic RET protocol in and findings of this study can potentially assist clinician decision-making concerning the optimal treatment strategy for obese elderly women, particularly for those who are considered sarcopenic.
Methods
Study design
This prospective study was a randomized controlled trial conducted through a single-blind experimental design in a rehabilitation center at Shuang Ho Hospital, Taipei Medical University. All patients were enrolled from April 2015 to April 2016. After the patients provided consent, they were randomly assigned to one of two parallel groups: an EG receiving elastic RET and an age-matched CG. All outcome measures were assessed by a blinded examiner at the T0, at the end of the 12-week RET intervention (T1), and at 6 months following the completion of the RET intervention (T2).
Ethics statement
This study was approved by the Joint Institutional Review Board of Taipei Medical University (trial number 201306019) and registered at the Chinese Clinical Trial Registry (trial number ChiCTR-IPR-15006069) on April 3, 2015. We confirm that the study methods adopted the CONSORT 2010 guidelines and were performed in accordance with the described procedures in the approved study protocol.
Participants
Female patients aged from 60 to 80 years were recruited from the outpatient department of our rehabilitation center. Patients were included if they were identified as having sarcopenia or obesity. Patients were excluded if they had any of the following conditions: (a) Uncontrolled hypertension; (b) joint contractures or internal metal implants such as total joint arthroplasty; (c) cardiovascular or pulmonary diseases that could prevent them from engaging in an exercise study; or (d) neurological impairment.
Definition of sarcopenic obesity
Sarcopenia Low muscle mass was determined using the same method as in our previous study47. First, total skeletal muscle mass (TSM, kg) was measured using an eight-polar bioelectrical impedance analysis device with multifrequency current (Inbody™ 220, Biospace, Seoul, Republic of Korea); this device was identified to be a valid TSM estimator48. Specifically, TSM was estimated using Janssen’s equation: TSM = [(Ht2/BIA-R) × 0.401 + (sex × 3.825) + (age × −0.071) + 5.102], where Ht represents the height in centimeters, BIA-R represents BIA resistance in ohms, and age is in years; moreover, for sex, men = 1 and women = 049. The estimated TSM was converted to a percentage SMI through dividing it by total body mass in kilograms (TSM/total body mass × 100%). Patients with an SMI that was two standard deviations (SDs) lower than the sex-specific means of the younger population were considered to be sarcopenic. Because of the lack of a norm for the SMI among young adults in the local population, we used the reference value proposed by Janssen, which was derived from 3298 young women aged 18–39 years old. The cutoff value of the SMI for sarcopenia in women was less than 27.6%47.
Obesity Participants’ BF% was also measured through bioelectrical impedance analysis and was further used to determine obesity in this study. Patients with a BF% of more than 30% were considered to be obese50.
Sample size
This study implemented lean mass gain as one of the key primary outcomes. The power calculation was based on the result of a previous similar study that compared elastic resistance-based exercise with modality-based rehabilitation in older female patients51. For an allowance to identify a significant between-group difference of 0.5 kg (assuming an SD of 2.86) on lean mass gain, 20 patients were required in each group, with a statistical power of 0.80, an effect size of 0.2, a correlation of 0.5 assumed for repeated measures, and an alpha value of 0.05. We anticipated a dropout rate of 20%, and thus included a total of 50 patients or more in the study. We also estimated the smallest sample size required for the multiple linear regression models established in our study. With a statistical power of 0.80, medium Cohen’s f2 effect size of 0.2552,53, alpha value of 0.05, and four predictors, our study required 53 patients to yield reliable results.
Randomization
After the patients met the eligibility criteria and provided informed consent, we subsequently randomized patients using concealed allocation based on a list of random numbers, which was computer-generated by an independent randomization center. The principal investigator informed the patients about the treatment session schedules as allocated by the independent randomization center.
Elastic resistance exercise
Resistance exercise was performed using Theraband (Hygenic Co., Akron, OH, USA). The color of the band denotes the degree of elasticity and the resistance level (yellow, red, green, blue, black, or silver). All patients undergoing elastic resistance exercise were trained and supervised by a licensed senior physical therapist who was blinded to the study group assignment. The Borg scale was used for RPE during training sessions; this is an efficient method for describing how the subjective intensity varies with physical intensity, and it further facilitates estimating the intensity of individual rehabilitation protocols20,54. Exercise loads in terms of individual yielding elasticity (as indicated by band color) in resistance training were set at a level that the patients perceived as “somewhat hard,” which is equivalent to a 13-grade rating (representing a moderate-intensity exercise) on the RPE scale, according to the American College of Sports Medicine55. Exercise movements were designed on the basis of previously established elastic exercise regimes used for training older female adults;33,38,56 the designed movements were aimed at strengthening the main muscle groups in the trunk, upper extremities, and lower extremities that are crucial for physical mobility33,56,57. For each exercise movement, 3 sets of 10 repetitions of gentle concentric and eccentric contractions through the full range of motion were slowly performed using a yellow Theraband initially (Supplementary Appendix S1). The exercise intensity was increased when the patients were able to achieve a perceived yield strength corresponding to a 13-grade rating on the RPE scale. If the progressively advancing exercise load level could not be managed (i.e., from red to green Theraband), the previously used Theraband color was maintained with an additional set of each exercise motion until the patients could yield that exercise load.
Training protocol
The training protocol was designed on the basis of the ACSM guidelines for resistance training with older subjects55. Each patient in the EG underwent 3 training sessions every week for 12 weeks, yielding a total of 36 sessions within 3 months (Supplementary Appendix S1). Each training session comprised a 10-min warm-up, 40-min period of elastic resistance exercises, and 5-min cool-down period; the session was supervised by a senior licensed physical therapist. After the warm-up, patients performed upper body exercises (seated chest press, seated row, and seated shoulder press) followed by lower body exercises (knee extension, knee flexion, hip flexion, and hip extension). The detailed exercise regimen is presented in Supplementary Appendix S2.
Muscle mass assessment
Muscle mass was measured using a Hologic QDR-1000/W whole body dual-energy X-ray absorptiometer (Hologic, Waltham, MA, USA). All scans and analyses were conducted by the same investigator, who was blinded to the patients’ group allocation to minimize interobserver variation. Hologic enhanced whole-body analysis software (version 5.71) was used to provide estimates of the following components: whole body lean mass (kg), TSM (kg), and ALM (kg). According to the recommendations of the Asian Working Group for Sarcopenia and the European Working Group on Sarcopenia in Older People, three relative muscle mass indices were adopted to define muscle mass outcomes58,59. The first two major indices, namely AMI (kg/m2) and LMI (kg/m2), are calculated as the ALM and whole body lean mass divided by squared height in meters, respectively. The third major index was SMI (%) which as mentioned above.
Muscular strength measurement
In this study, muscle strength was assessed in terms of MQ, which is defined as the ratio of muscular strength to muscle mass, and it was reported to be an indicator of muscle function60,61. The MQ of the upper extremity is calculated by dividing handgrip strength (kg) by arm lean mass (kg), whereas that of the lower extremity is calculated by dividing the strength of isometric quadriceps (N) by leg lean mass (kg).
Upper extremity strength
Handgrip strength was measured using a standard hydraulic hand dynamometer (Baseline® Digital, Fabrication Enterprises Inc., New York City, NY, USA). Each patient’s dominant hand was tested. Patients were seated with their arms adducted, the tested forearm unsupported, the elbow flexed at an angle of 90°, and the wrist in a neutral position. The width of the dynamometer handle was adjusted to allow the middle phalange of the third digit to be comfortably perpendicular to the long axis of the handle. All patients were asked to perform a maximal contraction by squeezing the dynamometer handle as forcefully as possible for 3–5 s, with an encouraging verbal cue being provided during this task. Three trials were performed, with a rest period between trials of approximately 30 s. The force output (kg) was recorded for each trial, and the average of the three trials was considered as the representative handgrip strength value46.
Lower extremity strength
Measurement of maximal isometric quadriceps strength in the dominant leg adopted Buckinx’s method62, using a handheld dynamometer (Microfet3; Hoggan Health Industries Co., UT, USA). Each patient was seated in a chair with the knee and hip flexed at 90° and pelvis fixed. The dynamometer pad was placed just proximal to the lateral malleolus. All patients were asked to make their greatest effort to extend the leg against the dynamometer for 10 s. Three trials were performed, with a rest period between trials of approximately 30 s. Maximal force output (N) was recorded for each trial, and the average of the three trials was considered as the representative knee extensor strength.
Studies have reported that conducting the isometric strength test in older adults using a handheld dynamometer provided excellent reliability, with an intraclass correlation coefficient (ICC) ranging from 0.97 to 0.98 for handgrip strength63 and an ICC of 0.81 [95% confidence interval (CI): 0.68–0.93] for knee extensor strength62.
Physical capacity assessment
Physical capacity of patients was assessed using the physical performance battery of mobility tasks. All physical mobility tasks used in the present study have been validated in older adults64,65,66,67,68. Each patient performed a practice trial before the test, and two trials were performed. The mean score of the two tested trials of each task was calculated for statistical analysis.
Functional forward reach
We used an FFR task to assess balance performance. The FFR task provides a dynamic measure of balance regardless of the selected movement strategy69.
Single leg stance
SLS tasks were used to assess balance control. The SLS score represents the total time for which a patient can stand on the dominant leg. SLS tasks were performed separately with eyes open and closed.
Gait speed (GS)
The GS was measured using the time required for the patient to walk 10 m on a track at a self-determined pace65. The GS was calculated in meters per second for each patient.
Timed Up & Go test
The TUG test measures the time required for a patient to rise from a chair (height 42 cm, depth 26 cm), walk 3 m, turn around, and return to a seated position in the chair at a self-determined speed. A walking aid was used by patients during the test if necessary.
Timed chair rise
In the TCR assessment, patients were asked to stand upright from a seated position in a chair (height 43 cm) with their arms folded across their chest and return to a seated position as many times as possible within a 30-s period.
Global physical capacity score
The GPCS used in the present study was adapted from approaches in relevant studies9,70. Each of the five mobility tests (FFR, SLS, GS, TUG, and TCR) was assigned a score from 1 to 4 using quartiles of performance (i.e., fourth, third, second, and first quartiles were coded as 4, 3, 2, and 1 points, respectively). Patients who could not complete the test were assigned a score of 0. Scores for all tests were summed to obtain a GPCS for each patient (possible score range: 0–20).
Compared with each individual test, one advantage of GPCS is that it provides an overall measure of patient performance through considering several tasks related to daily activities. Consequently, we used the GPCS to identify whether patients with sarcopenic obesity receiving RET had a higher functional capacity than did the CG.
Medical Outcomes Study Short Form-36 Questionnaire (SF-36)
Health-related quality of life was assessed using the Chinese version of the Medical Outcomes Study SF-3671. It comprises 36 items divided into 8 domains for which a subscale score is calculated. From the SF-36, four subscales (i.e., PF, role physical, bodily pain, and general health) are incorporated into a summary measure called the PCS. The domains and PCS are transformed into a score from 0 to 100, where 100 indicates no symptoms and 0 indicates extreme symptoms. Good validity (ICC = 0.72–0.88) and reliability (ICC = 0.66–0.94) has been established for the Chinese version of the SF-3672.
The well-established values of minimum detectable change at a 90% level of confidence (MDC90) of the outcome measures used in the present study (i.e., handgrip, isometric quadriceps strength, FFR, SLS, GS, and SF-36 PF subscore) for older adults are available in relevant studies64,67,73,74, or can be estimated using the formula MDC90 = z × SEM × 2½, where z is 1.65 at a 90% CI75 and SEM is the standard error of the mean. All available MDC90 values are presented in Table 3.
Statistical analysis
Independent t-tests and chi-squared analyses were used to compare the patient characteristics and outcome measures of the EG with those of the CG at the baseline. The Kolmogorov–Smirnov test was used to confirm whether all variables were normally distributed. An intent-to-treat analysis based on the last-observation-carried-forward technique was used to manage any missing data and minimize bias related to losses during followup. A 2 × 3 repeated measures analysis of covariance (ANCOVA) was used to analyze all outcome variables. In the ANCOVA, time served as the repeated measures factor (T0, T1, and T2), and the allocated group (RET vs. control) served as the between-groups factor. In addition, the baseline score for each outcome measure was considered a potentially confounding covariate to improve the precision of the effect estimates. All comparison results that had P < 0.05 were considered statistically significant, and are presented as mean values with SDs. The SPSS statistical software package for Windows (Version 17.0. Chicago: SPSS Inc) was used for all analyses.
To test whether the intragroup changes were clinically significant, we compared the MCID of each outcome measure with either the 95% CI or the percentage of postintervention change. The following established MCIDs for the outcome measures of older adults were obtained from the literature: 0.1 m/s for GS76; 2.0–2.6 repetitions for the TCR77; 1.2 s for the TUG77; and 3.3 and 2.0 for SF-36 PF and PCS, respectively78.
When controlling for the exercise intervention mode and baseline characteristics, we determined the associations between the changes in muscle mass and those in physical outcomes at T2 through conducting a multiple stepwise linear regression analysis on the collapsed data. In these data, the changes in the physical outcome measures (i.e., the MQ of the upper and lower extremity, GPCS, SF-36 PF, and SF-36 PCS) were treated as dependent variables, and the changes in the muscle mass measures (i.e., the ALM, TSM, AMI, LMI, and SMI) were treated as exploratory covariates.
Chinese Clinical Trial Registration Numbers
ChiCTR-IPR-15006069, www.chictr.org.cn, Registration date: April 03, 2015.
References
Molino, S., Dossena, M., Buonocore, D. & Verri, M. Sarcopenic Obesity: An Appraisal of the Current Status of Knowledge and Management in Elderly People. J Nutr Health Aging 20, 780–788, https://doi.org/10.1007/s12603-015-0631-8 (2016).
von Haehling, S., Morley, J. E. & Anker, S. D. From muscle wasting to sarcopenia and myopenia: update 2012. J Cachexia Sarcopenia Muscle 3, 213–217, https://doi.org/10.1007/s13539-012-0089-z (2012).
Vincent, H. K., Raiser, S. N. & Vincent, K. R. The aging musculoskeletal system and obesity-related considerations with exercise. Ageing Res Rev 11, 361–373, https://doi.org/10.1016/j.arr.2012.03.002 (2012).
Janssen, I., Baumgartner, R. N., Ross, R., Rosenberg, I. H. & Roubenoff, R. Skeletal muscle cutpoints associated with elevated physical disability risk in older men and women. Am J Epidemiol 159, 413–421 (2004).
Visser, M. et al. Leg muscle mass and composition in relation to lower extremity performance in men and women aged 70 to 79: the health, aging and body composition study. J Am Geriatr Soc 50, 897–904 (2002).
Zoico, E. et al. Physical disability and muscular strength in relation to obesity and different body composition indexes in a sample of healthy elderly women. Int J Obes Relat Metab Disord 28, 234–241, https://doi.org/10.1038/sj.ijo.0802552 (2004).
Vincent, H. K., Vincent, K. R. & Lamb, K. M. Obesity and mobility disability in the older adult. Obes Rev 11, 568–579, https://doi.org/10.1111/j.1467-789×.2009.00703.x (2010).
Rolland, Y. et al. Difficulties with physical function associated with obesity, sarcopenia, and sarcopenic-obesity in community-dwelling elderly women: the EPIDOS (EPIDemiologie de l’OSteoporose) Study. Am J Clin Nutr 89, 1895–1900, https://doi.org/10.3945/ajcn.2008.26950 (2009).
Bouchard, D. R., Dionne, I. J. & Brochu, M. Sarcopenic/obesity and physical capacity in older men and women: data from the Nutrition as a Determinant of Successful Aging (NuAge)-the Quebec longitudinal Study. Obesity (Silver Spring) 17, 2082–2088, https://doi.org/10.1038/oby.2009.109 (2009).
Elliott, B., Renshaw, D., Getting, S. & Mackenzie, R. The central role of myostatin in skeletal muscle and whole body homeostasis. Acta Physiol (Oxf) 205, 324–340, https://doi.org/10.1111/j.1748-1716.2012.02423.x (2012).
Allen, D. L., Hittel, D. S. & McPherron, A. C. Expression and function of myostatin in obesity, diabetes, and exercise adaptation. Med Sci Sports Exerc 43, 1828–1835, https://doi.org/10.1249/MSS.0b013e3182178bb4 (2011).
Yarasheski, K. E., Bhasin, S., Sinha-Hikim, I., Pak-Loduca, J. & Gonzalez-Cadavid, N. F. Serum myostatin-immunoreactive protein is increased in 60-92 year old women and men with muscle wasting. J Nutr Health Aging 6, 343–348 (2002).
Hasten, D. L., Pak-Loduca, J., Obert, K. A. & Yarasheski, K. E. Resistance exercise acutely increases MHC and mixed muscle protein synthesis rates in 78–84 and 23–32 yr oldt. American Journal of Physiology - Endocrinology and Metabolism 278, E620–E626 (2000).
Yarasheski, K. E. Exercise, aging, and muscle protein metabolism. J Gerontol A Biol Sci Med Sci 58, M918–922 (2003).
Schulte, J. N. & Yarasheski, K. E. Effects of resistance training on the rate of muscle protein synthesis in frail elderly people. Int J Sport Nutr Exerc Metab 11(Suppl), S111–118 (2001).
Kumar, V., Atherton, P., Smith, K. & Rennie, M. J. Human muscle protein synthesis and breakdown during and after exercise. J Appl Physiol (1985) 106, 2026–2039, https://doi.org/10.1152/japplphysiol.91481.2008 (2009).
Liu, C. J. & Latham, N. K. Progressive resistance strength training for improving physical function in older adults. Cochrane Database Syst Rev, CD002759, https://doi.org/10.1002/14651858.CD002759.pub2 (2009).
Yasuda, T. et al. Effects of Low-Load, Elastic Band Resistance Training Combined With Blood Flow Restriction on Muscle Size and Arterial Stiffness in Older Adults. J Gerontol A Biol Sci Med Sci 70, 950–958, https://doi.org/10.1093/gerona/glu084 (2015).
Chen, K. M., Tseng, W. S., Huang, H. T. & Li, C. H. Development and feasibility of a senior elastic band exercise program for aged adults: a descriptive evaluation survey. J Manipulative Physiol Ther 36, 505–512, https://doi.org/10.1016/j.jmpt.2013.08.002 (2013).
Andersen, L. L. et al. Muscle activation and perceived loading during rehabilitation exercises: comparison of dumbbells and elastic resistance. Phys Ther 90, 538–549, https://doi.org/10.2522/ptj.20090167 (2010).
Fukumoto, Y. et al. Effects of high-velocity resistance training on muscle function, muscle properties, and physical performance in individuals with hip osteoarthritis: a randomized controlled trial. Clin Rehabil 28, 48–58, https://doi.org/10.1177/0269215513492161 (2014).
Cho, I., Hwangbo, G., Lee, D. & Lee, S. The effects of closed kinetic chain exercises and open kinetic chain exercises using elastic bands on electromyographic activity in degenerative gonarthritis. J Phys Ther Sci 26, 1481–1484, https://doi.org/10.1589/jpts.26.1481 (2014).
Melchiorri, G. & Rainoldi, A. Muscle fatigue induced by two different resistances: Elastic tubing versus weight machines. J Electromyogr Kinesiol 21, 954–959, https://doi.org/10.1016/j.jelekin.2011.07.015 (2011).
Franzke, B. et al. The effect of six months of elastic band resistance training, nutritional supplementation or cognitive training on chromosomal damage in institutionalized elderly. Exp Gerontol 65, 16–22, https://doi.org/10.1016/j.exger.2015.03.001 (2015).
Lachin, J. M. Properties of simple randomization in clinical trials. Control Clin Trials 9, 312–326 (1988).
Hernandez, A. V., Steyerberg, E. W. & Habbema, J. D. Covariate adjustment in randomized controlled trials with dichotomous outcomes increases statistical power and reduces sample size requirements. J Clin Epidemiol 57, 454–460, https://doi.org/10.1016/j.jclinepi.2003.09.014 (2004).
Kahan, B. C., Jairath, V., Dore, C. J. & Morris, T. P. The risks and rewards of covariate adjustment in randomized trials: an assessment of 12 outcomes from 8 studies. Trials 15, 139, https://doi.org/10.1186/1745-6215-15-139 (2014).
Duchateau, J. & Enoka, R. M. Human motor unit recordings: origins and insight into the integrated motor system. Brain Res 1409, 42–61, https://doi.org/10.1016/j.brainres.2011.06.011 (2011).
Fry, A. C. The role of resistance exercise intensity on muscle fibre adaptations. Sports Med 34, 663–679 (2004).
Row, B. S., Knutzen, K. M. & Skogsberg, N. J. Regulating explosive resistance training intensity using the rating of perceived exertion. J Strength Cond Res 26, 664–671, https://doi.org/10.1519/JSC.0b013e31822ac367 (2012).
Campos, G. E. et al. Muscular adaptations in response to three different resistance-training regimens: specificity of repetition maximum training zones. Eur J Appl Physiol 88, 50–60, https://doi.org/10.1007/s00421-002-0681-6 (2002).
Hunter, G. R. et al. High-resistance versus variable-resistance training in older adults. Med Sci Sports Exerc 33, 1759–1764 (2001).
Egana, M., Reilly, H. & Green, S. Effect of elastic-band-based resistance training on leg blood flow in elderly women. Appl Physiol Nutr Metab 35, 763–772, https://doi.org/10.1139/h10-071 (2010).
Maris, S. A. et al. The combined effects of tai chi, resistance training, and diet on physical function and body composition in obese older women. J Aging Res 2014, 657851, https://doi.org/10.1155/2014/657851 (2014).
Lee, J. S., Kim, C. G., Seo, T. B., Kim, H. G. & Yoon, S. J. Effects of 8-week combined training on body composition, isokinetic strength, and cardiovascular disease risk factors in older women. Aging Clin Exp Res 27, 179–186, https://doi.org/10.1007/s40520-014-0257-4 (2015).
Fahlman, M. M., McNevin, N., Boardley, D., Morgan, A. & Topp, R. Effects of resistance training on functional ability in elderly individuals. American Journal of Health Promotion 25, 237–243 (2011).
Hasegawa, R., Islam, M. M., Watanabe, R., Tomiyama, N. & Taaffe, D. R. Effects of periodic task-specific test feedback on physical performance in older adults undertaking band-based resistance exercise. J Aging Res 2014, 171694, https://doi.org/10.1155/2014/171694 (2014).
Chang, T. F., Liou, T. H., Chen, C. H., Huang, Y. C. & Chang, K. H. Effects of elastic-band exercise on lower-extremity function among female patients with osteoarthritis of the knee. Disabil Rehabil 34, 1727–1735, https://doi.org/10.3109/09638288.2012.660598 (2012).
Zion, A. A home-based resistance-training program using elastic bands for elderly patients with orthostatic hypotension. Clin Auton Res 13, 286–292 (2003).
Sternfeld, B., Ngo, L., Satariano, W. A. & Tager, I. B. Associations of body composition with physical performance and self-reported functional limitation in elderly men and women. Am J Epidemiol 156, 110–121 (2002).
Visser, M. et al. Body fat and skeletal muscle mass in relation to physical disability in very old men and women of the Framingham Heart Study. J Gerontol A Biol Sci Med Sci 53, M214–221 (1998).
Newman, A. B. et al. Strength, but not muscle mass, is associated with mortality in the health, aging and body composition study cohort. J Gerontol A Biol Sci Med Sci 61, 72–77 (2006).
Chen, H. T., Chung, Y. C., Chen, Y. J., Ho, S. Y. & Wu, H. J. Effects of Different Types of Exercise on Body Composition, Muscle Strength, and IGF-1 in the Elderly with Sarcopenic Obesity. J Am Geriatr Soc 65, 827–832, https://doi.org/10.1111/jgs.14722 (2017).
Agergaard, J. et al. Light-load resistance exercise increases muscle protein synthesis and hypertrophy signaling in elderly men. Am J Physiol Endocrinol Metab 312, E326–E338, https://doi.org/10.1152/ajpendo.00164.2016 (2017).
Oesen, S. et al. Effects of elastic band resistance training and nutritional supplementation on physical performance of institutionalised elderly - A randomized controlled trial. Exp Gerontol 72, 99–108 (2015).
Leenders, M. et al. Protein supplementation during resistance-type exercise training in the elderly. Med Sci Sports Exerc 45, 542–552 (2013).
Janssen, I., Heymsfield, S. B. & Ross, R. Low relative skeletal muscle mass (sarcopenia) in older persons is associated with functional impairment and physical disability. J Am Geriatr Soc 50, 889–896 (2002).
Anderson, L. J., Erceg, D. N. & Schroeder, E. T. Utility of multifrequency bioelectrical impedance compared with dual-energy x-ray absorptiometry for assessment of total and regional body composition varies between men and women. Nutr Res 32, 479–485, https://doi.org/10.1016/j.nutres.2012.05.009 (2012).
Janssen, I., Heymsfield, S. B., Baumgartner, R. N. & Ross, R. Estimation of skeletal muscle mass by bioelectrical impedance analysis. J Appl Physiol (1985) 89, 465–471 (2000).
Liu, P., Ma, F., Lou, H. & Zhu, Y. Utility of obesity indices in screening Chinese postmenopausal women for metabolic syndrome. Menopause 21, 509–514, https://doi.org/10.1097/GME.0b013e3182a170be (2014).
Stout, J. R. et al. Effect of calcium beta-hydroxy-beta-methylbutyrate (CaHMB) with and without resistance training in men and women 65 + yrs: a randomized, double-blind pilot trial. Exp Gerontol 48, 1303–1310, https://doi.org/10.1016/j.exger.2013.08.007 (2013).
Cohen, J. Statistical power analysis for the behavioral sciences. 2nd ed. edn, (NJ: Erlbaum, 1988).
Ferguson, C. J. An effect size primer: A guide for clinicians and researchers. Professional Psychology: Research and Practice 40, 532 (2009).
Borg, G. Psychophysical scaling with applications in physical work and the perception of exertion. Scand J Work Environ Health 16(Suppl 1), 55–58 (1990).
Nelson, M. E. et al. Physical activity and public health in older adults: recommendation from the American College of Sports Medicine and the American Heart Association. Circulation 116, 1094–1105, https://doi.org/10.1161/circulationaha.107.185650 (2007).
de Vreede, P. L. et al. Functional tasks exercise versus resistance exercise to improve daily function in older women: a feasibility study. Arch Phys Med Rehabil 85, 1952–1961 (2004).
Shoepe, T. C., Ramirez, D. A., Rovetti, R. J., Kohler, D. R. & Almstedt, H. C. The Effects of 24 weeks of Resistance Training with Simultaneous Elastic and Free Weight Loading on Muscular Performance of Novice Lifters. J Hum Kinet 29, 93–106, https://doi.org/10.2478/v10078-011-0043-8 (2011).
Cruz-Jentoft, A. J. et al. Sarcopenia: European consensus on definition and diagnosis: Report of the European Working Group on Sarcopenia in Older People. Age Ageing 39, 412–423, https://doi.org/10.1093/ageing/afq034 (2010).
Chen, L. K. et al. Sarcopenia in Asia: consensus report of the Asian Working Group for Sarcopenia. J Am Med Dir Assoc 15, 95–101, https://doi.org/10.1016/j.jamda.2013.11.025 (2014).
Newman, A. B. et al. Strength and muscle quality in a well-functioning cohort of older adults: the Health, Aging and Body Composition Study. J Am Geriatr Soc 51, 323–330 (2003).
Barbat-Artigas, S., Rolland, Y., Zamboni, M. & Aubertin-Leheudre, M. How to assess functional status: a new muscle quality index. J Nutr Health Aging 16, 67–77 (2012).
Buckinx, F. et al. Reliability of muscle strength measures obtained with a hand-held dynamometer in an elderly population. Clin Physiol Funct Imaging In press (2015).
Vermeulen, J. et al. Measuring grip strength in older adults: comparing the grip-ball with the Jamar dynamometer. J Geriatr Phys Ther 38, 148–153, https://doi.org/10.1519/jpt.0000000000000034 (2015).
Choi, Y. M., Dobson, F., Martin, J., Bennell, K. L. & Hinman, R. S. Interrater and intrarater reliability of common clinical standing balance tests for people with hip osteoarthritis. Phys Ther 94, 696–704, https://doi.org/10.2522/ptj.20130266 (2014).
Takacs, J., Garland, S. J., Carpenter, M. G. & Hunt, M. A. Validity and Reliability of the Community Balance and Mobility Scale in Individuals With Knee Osteoarthritis. Phys Ther 94, 866–874, https://doi.org/10.2522/ptj.20130385 (2014).
Shumway-Cook, A., Brauer, S. & Woollacott, M. Predicting the probability for falls in community-dwelling older adults using the Timed Up & Go Test. Phys Ther 80, 896–903 (2000).
Gill, S. & McBurney, H. Reliability of performance-based measures in people awaiting joint replacement surgery of the hip or knee. Physiother Res Int 13, 141–152, https://doi.org/10.1002/pri.411 (2008).
Jones, C. J., Rikli, R. E. & Beam, W. C. A 30-s chair-stand test as a measure of lower body strength in community-residing older adults. Res Q Exerc Sport 70, 113–119 (1999).
Duncan, P. W., Weiner, D. K., Chandler, J. & Studenski, S. Functional reach: a new clinical measure of balance. J Gerontol 45, M192–197 (1990).
Guralnik, J. M. et al. A short physical performance battery assessing lower extremity function: association with self-reported disability and prediction of mortality and nursing home admission. J Gerontol 49, M85–94 (1994).
Fuh, J. L., Wang, S. J., Lu, S. R., Juang, K. D. & Lee, S. J. Psychometric evaluation of a Chinese (Taiwanese) version of the SF-36 health survey amongst middle-aged women from a rural community. Qual Life Res 9, 675–683 (2000).
Thumboo, J. et al. Reliability and validity of the English (Singapore) and Chinese (Singapore) versions of the Short-Form 36 version 2 in a multi-ethnic urban Asian population in Singapore. Qual Life Res 22, 2501–2508, https://doi.org/10.1007/s11136-013-0381-1 (2013).
Kennedy, D. M., Stratford, P. W., Wessel, J., Gollish, J. D. & Penney, D. Assessing stability and change of four performance measures: a longitudinal study evaluating outcome following total hip and knee arthroplasty. BMC Musculoskelet Disord 6, 3, https://doi.org/10.1186/1471-2474-6-3 (2005).
Busija, L., Osborne, R. H., Nilsdotter, A., Buchbinder, R. & Roos, E. M. Magnitude and meaningfulness of change in SF-36 scores in four types of orthopedic surgery. Health Qual Life Outcomes 6, 55, https://doi.org/10.1186/1477-7525-6-55 (2008).
Stratford, P. W. Getting more from the literature: estimating the standard error of measurement from reliability studies. Physiotherapy Canada 56, 27–30 (2004).
Chui, K., Hood, E. & Klima, D. Meaningful Change in Walking Speed. Topics in Geriatric Rehabilitation 28, 97–103, https://doi.org/10.1097/TGR.0b013e3182510195 (2012).
Wright, A. A., Cook, C. E., Baxter, G. D., Dockerty, J. D. & Abbott, J. H. A comparison of 3 methodological approaches to defining major clinically important improvement of 4 performance measures in patients with hip osteoarthritis. J Orthop Sports Phys Ther 41, 319–327, https://doi.org/10.2519/jospt.2011.3515 (2011).
Angst, F., Aeschlimann, A. & Stucki, G. Smallest detectable and minimal clinically important differences of rehabilitation intervention with their implications for required sample sizes using WOMAC and SF-36 quality of life measurement instruments in patients with osteoarthritis of the lower extremities. Arthritis Rheum 45, 384–391, https://doi.org/10.1002/1529-0131(200108)45:4<384::aid-art352>3.0.co;2-0 (2001).
Acknowledgements
This study was funded by the Ministry of Science and Technology, Taiwan (NSC 102–2314-B-038-053-MY3; MOST 105-2314-B-038-075); Shuang Ho Hospital, Taipei Medical University (W106HCP-14); and Taipei Medical University (106TMU-SHH-05). The funding sources played no role in the design, implementation, data analysis, interpretation, or reporting of the study. The contents of this publication are solely the responsibility of the authors and do not necessarily represent the official view of the funding sources. This manuscript was edited by Wallace Academic Editing.
Author information
Authors and Affiliations
Contributions
Study concept and design: Liao and Liou. Acquisition of data: Liao and Ku. Collection and assembly of data: Liao, Huang, and Ku. Analysis and interpretation of data: Liao, Liou, and Huang. Drafting of the manuscript: Liao and Liou. Critical revision of the manuscript for vital intellectual content: Liou, Liao, Tsauo, and Huang. Statistical expertise: Huang and Liao. Study supervision and responsibility for the integrity of the work as a whole: Liao, Hsiao, Liou, and Huang.
Corresponding author
Ethics declarations
Competing Interests
The authors declare that they have no competing interests.
Additional information
Publisher's note: Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made. The images or other third party material in this article are included in the article’s Creative Commons license, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons license and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this license, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Liao, CD., Tsauo, JY., Huang, SW. et al. Effects of elastic band exercise on lean mass and physical capacity in older women with sarcopenic obesity: A randomized controlled trial. Sci Rep 8, 2317 (2018). https://doi.org/10.1038/s41598-018-20677-7
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41598-018-20677-7
This article is cited by
-
Sarcopenic obesity does not impair lower limb strength and physical performance in sufficiently active older adults: a cross-sectional study
Scientific Reports (2024)
-
Effectiveness of elastic band training and group-based dance on physical-functional performance in older women with sarcopenia: a pilot study
BMC Public Health (2023)
-
Effects of Exercise Training on Muscle Quality in Older Individuals: A Systematic Scoping Review with Meta-Analyses
Sports Medicine - Open (2023)
-
Is moderate resistance training adequate for older adults with sarcopenia? A systematic review and network meta-analysis of RCTs
European Review of Aging and Physical Activity (2023)
-
Effects of Nutrition and Exercise Interventions on Persons with Sarcopenic Obesity: An Umbrella Review of Meta-Analyses of Randomised Controlled Trials
Current Obesity Reports (2023)
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.