Abstract
Dry eye disease (DED) is a highly prevalent, ocular disorder characterized by an abnormal tear film and ocular surface. Recent experimental data has suggested that the underlying pathology of DED involves inflammation of the lacrimal functional unit (LFU), comprising the cornea, conjunctiva, lacrimal gland and interconnecting innervation. This inflammation of the LFU ultimately results in tissue deterioration and the symptoms of DED. Moreover, an increase of pathogenic lymphocyte infiltration and the secretion of pro-inflammatory cytokines are involved in the propagation of DED-associated inflammation. Studies have demonstrated that the adoptive transfer of regulatory T cells (Tregs) can mediate the inflammation caused by pathogenic lymphocytes. Thus, as an approach to treating the inflammation associated with DED, we hypothesized that it was possible to enrich the body’s own endogenous Tregs by locally delivering a specific combination of Treg inducing factors through degradable polymer microspheres (TRI microspheres; TGF-β1, Rapamycin (Rapa), and IL-2). This local controlled release system is capable of shifting the balance of Treg/T effectors and, in turn, preventing key signs of dry eye disease such as aqueous tear secretion, conjunctival goblet cells, epithelial corneal integrity, and reduce the pro-inflammatory cytokine milieu in the tissue.
Similar content being viewed by others
Introduction
Dry eye disease (DED) is a common ocular disorder affecting millions of individuals with an average annual direct medical cost of $3.84 billion in the United States1,2,3,4. A myriad of risk factors have been associated with DED including: autoimmune diseases (rheumatoid arthritis, Sjögren’s Syndrome), thyroid disease, hormonal changes, and aging4. Typically, these risk factors can lead to symptoms such as ocular irritation, reduced visual acuity, and tear hyperosmolarity5,6. In turn, the increase in tear hyperosmolarity leads to ocular surface inflammation and tissue destruction7.
Recent studies strongly suggest that the ocular surface inflammation is the result of pathogenic effector T cells secreting pro-inflammatory cytokines8,9,10,11,12,13,14. Accordingly, treatments have been developed that intend to suppress the inflammatory response through the administration of anti-inflammatory treatments such as corticosteroids15. However, long-term topical use of corticosteroids have been implicated in conditions such as glaucoma and retinopathy16. An ideal treatment for DED would address the underlying inflammation mediated by the pathogenic effector T cells without serious, negative side effects.
One method that the body uses to decrease local function/prevalence of effector T cells is through enhancing the prevalence and/or function of immunosuppressive cells (regulatory T cells) Tregs to resolve inflammation12,17. Specifically, prevalent, naïve CD4+ T cell populations in the periphery are capable of differentiating into functional Tregs under the direction of a subset of antigen presenting cells known as tolerogenic dendritic cells (tDCs)18. tDCs induce differentiation of Tregs (in part) through the secretion of a combination of IL-2 and TGF-β cytokines19,20. However, the maintenance of Tregs is somewhat more complex and depends on a local microenvironment that is not only favorable to differentiation of Tregs, but also unfavorable to differentiation into other effector T cells21. One method of creating such a local microenvironment is through administration of the small molecule, rapamycin. Rapamycin (Rapa) is an mTOR inhibitor that can suppress the generation and proliferation of effector T cells22. We have previously demonstrated that sustaining the presence of TGF-β, Rapamycin and IL-2 using degradable microspheres was able to induce/differentiate naive CD4+ T cells into FoxP3+ Tregs in vitro with high efficiency22.
Here we describe the in vivo application of T-Reg Inducing (TRI) microspheres (MS) in a model of murine dry eye disease. Data suggests that this drug-delivery strategy can influence local Treg numbers and, in turn, prevent key signs of DED. Application of this new strategy could provide a potential avenue for new types of immune based treatments for DED that influence the body’s own cells to address destructive inflammation23,24.
Methods
Fabrication of Microspheres
TGF-β and IL-2 microspheres were fabricated using a double emulsion- evaporation technique. For the TGF-β microspheres, Poly (lactic-co-glycolic) acid (PLGA-50:50 lactide:glycolide, acid terminated) (MW:7,000-17,000) (viscosity: 0.16–0.24 dL/g, 0.1% (w/v) in chloroform) (Sigma Aldrich, MO) and PEG-PLGA (PolySciTech, IN) was used to encapsulate rh-TGF-β (PeproTech, NJ). Specifically, 170 mg of PLGA and 30 mg of PEG-PLGA was dissolved in 4 ml of DCM (Sigma Aldrich, MO). Then 200 µl of aqueous solution containing 10 µg of rh-TGF-β was added to the polymer DCM mixture. The mixture was sonicated using a sonicator (Vibra-Cell, Newton, CT) for 10 sec. at 25% amplitude. Next, this emulsion was then mixed with 60 ml of 2% polyvinyl-alcohol (PVA, MW ~25,000, 98% hydrolyzed; PolySciences) and homogenized (L4RT-A, Silverson, procured through Fisher Scientific) at 3,000 rpm for 1 min. The homogenized mixtures were then added to 80 ml of 1% PVA on stir plate and left for 3 hours in order for the DCM to evaporate. After 3 hours, the microparticles were centrifuged (200 g, 5 min, 4 °C), washed 5 times with deionized water, and lyophilized for 48 hours (Virtis Benchtop K freeze dryer, Gardiner, NY).
For the IL-2 microspheres, 200 mg of PLGA (PLGA-50:50 lactide:glycolide, acid terminated) (MW:7,000-17,000) (viscosity: 0.16–0.24 dL/g, 0.1% (w/v) in chloroform) (Sigma, Aldrich, MI) was dissolved in 4 ml of DCM. Subsequently, 5 µg of IL-2 and 150 µl (R&D Systems, Minneapolis MN) of deionized water was added to the organic phase. Next, the two phases were emulsified using a sonicator probe (Vibra-Cell, Newton, CT) at 25% amplitude for a period of 25 seconds. Then this emulsion was mixed with 60 ml of 2% polyvinyl-alcohol (PVA, MW ~25,000, 98% hydrolyzed; Polysciences) with 51.66 millimoles of NaCl and homogenized (L4RT-A, Silverson, procured through Fisher Scientific) at 3,000 rpm for 1 min. This secondary emulsion was then then added to 80 ml of 1% PVA on stir plate and stirred for 3 hours. After finishing stirring, the microparticles were centrifuged (200 g, 5 min, 4 °C), washed 5 times with deionized water, and lyophilized for 48 hours (Virtis Benchtop K freeze dryer, Gardiner, NY).
The rapamycin (rapa) microspheres were fabricated using a single emulsion-evaporation technique due to the hydrophobic nature. Rapamycin (Sigma Aldrich, MO) was dissolved in DMSO (Sigma, Aldrich, MO) at 10 mg/ml. Then 200 mg of PLGA (Sigma Aldrich, MI) was dissolved in 4 ml of DCM. Next, 100 µl of rapamycin (10 mg/ml) was added to the polymer/DCM mixture. The solution was then homogenized with 60 ml of 2% PVA at 3,000 rpm for 1 min. After homogenizing, the emulsion was then added to 80 ml of 1% PVA and stirred for 3 hours. At the end of stirring, microspheres were washed 5 times with deionized water and lyophilized for 48 hours.
Characterization of Microspheres
The morphology of the microspheres were characterized using scanning electron microscopy (JEOL, JSM-6330F, Peabody, MA) and volume impedance measurements were performed on a Beckman Coulter Counter (Multisizer-3, Beckman Coulter, Fullerton, CA). The release assay of the IL-2, TGF-β, and rapamycin was completed by incubating 10 mg of microspheres in 1 ml of phosphate buffered saline (PBS) and 1% BSA, which was placed onto a rotator at 37 °C. The supernant was sampled at different time intervals and the TGF-β and IL-2 release profiles were quantified using an enzyme-linked immunosorbent assay (ELISA) (R&D Systems, Minneapolis, MN). The release profile of rapamycin microspheres was determined using UV-vis spectroscopy, and the release media contained 0.2% Tween-80 in PBS (absorbance at 278 nm).
Mice
Female Balb/c mice aged 6–8 weeks were used in this experimental study. (Charles Rivers Laboratories, Wilmington, MA). The Institutional Animal Care and Use Committee, University of Pittsburgh approved all murine experiments. All methods were performed in accordance with the relevant guidelines and regulations.
Murine DED model and treatment
Dry eye disease was induced using 10 mg/ml of Concanavalin A (ConA) (Sigma Aldrich, St. Louis, MO) in phosphate buffered saline solution (PBS) was injected into the lacrimal glands with a 28.5 gauge needle using a dissecting microscope25,26. The controls for examining the effects of the TRI MS included Blank (unloaded) or TRI MS (25 mg/ml). The TRI microspheres are a combination of all three microspheres (rapamycin microspheres, IL-2 microspheres, and TGF-β microspheres) individually combined together and injected with ConA. Approximately, 8.33 mg of Rapamycin microspheres, 8.33 mg of IL-2 microspheres, and 8.33 mg of TGF-β microspheres (total 25 mg/ml), which were combined with a PBS solution of ConA (10 mg/ml) (total volume injected into lacrimal gland is 20 µl). (Olympus SZX10, Waltham, MA).
Suppression of Tregs via the administration of anti-GITR
In order to identify the role of Tregs with the administration of our preventative treatment, the function of Tregs were inhibited using anti-GITR (DTA-1) (BioXCell, Lebanon, NH) via an intraparietal injection of (500 µg per mouse) 1 day after injecting the ConA and TRI MS27.
Tear Production
Phenol red cotton threads were utilized to measure tear production. (Oasis Medical, San Dimas, CA). The thread was placed in the lateral canthus of the eye for a period of 60 seconds, and the amount of wetting on the thread was measured using a dissecting microscope (Olympus SZX10, Waltham, MA)25.
Corneal Fluorescein Staining
Fluorescein stain (1% solution) was applied to the conjunctival sac. The surface of the cornea was examined using a dissecting microscope (Olympus SZX10, Waltham, MA). The scoring of staining was completed by a masked ophthalmologist, and scored 0 for no staining, score 1 for a quarter of staining, score of 2 for less than a half, score of 3 for half, and 4 for more than half of the eye.
Ocular Histology
At the conclusion of the study, the eyes were exenterated and fixed in 10% neutral buffered formalin. Sections were prepared at approximately 5 µm and stained with Periodic Acid Schiff (PAS) in order to examine goblet cell density. Histological sections were scanned and quantified using a Zeiss Axio Scan. Z1 (Thornwood, NY) and Pannoramic Viewer software (3D HISTECH Ltd.).
qRT-PCR
Total RNA was extracted from multiple excised lacrimal glands using TRI-reagent (Molecular Research Center, Cincinnati, OH), and quantified using a NanoDrop 2000 (Thermo Scientific). For the reverse transcriptase assay, 2 μg RNA was converted to cDNA using a QuantiTect Reverse Transcription Kit (Qiagen, Valencia, CA). Quantitative real-time PCR was then performed using VeriQuest Probe qPCR Mastermix (Affymetrix, Santa Clara, CA), (Thermo Scientific) specific for (IFN-γ:Mm01168134_m1, FAM-MGB dye), (IL-2:Mm00434256_m1, FAM-MGB dye), (IL-6:Mm00446190_ml, FAM-MGB dye), and (Gusb: Mm01197698_m1, VIC-MGB PL dye, endogenous control). Duplex reactions (target gene + GUSB) were run and analyzed on a StepOnePlus Real-Time PCR System (Applied Biosystems, Carlsbad, CA). Relative fold changes of IFN-γ, IL-6 and IL-2 expression were calculated and normalized based upon the 2−ΔΔCt method, with the Saline group as the untreated control.
Immunofluorescence of the lacrimal gland
At the end of the study, lacrimal glands were excised from the mice. Lacrimal glands were fixed with 4% PFA overnight, followed by cryoprotection through incubation in 30% sucrose overnight, and lastly embedded in O.C.T. medium. The cyrosections were obtained at 7 μm thick and stained with fluorescent antibodies. Specifically, 7 μm sections were blocked with 5% normal donkey serum and 1% Tween20 in PBS. Blocked sections were incubated overnight at 4 °C with rat anti-FoxP3 (FJK-16s; eBio) and rabbit anti-CD3 (SP7, monoclonal rabbit IgG; Abcam, Cambridge, MA). The sections were then incubated with a secondary antibody, Alexa Fluor 594 donkey anti-rat IgG (ThermoFisher Scientific Waltham, MA) and Alexa Fluor 647 donkey anti-rabbit IgG (Jackson ImmunoResearch Laboratories, West Grove, PA) for 1 hour at room temperature and then mounted using Fluoroshield mounting medium with DAPI (Abcam, Cambridge, MA). The images were captured using a Zeiss Axio Scanner Z.1. Only positively stained cells overlapping DAPI (nuclei) were quantified.
Statistical Analysis
Data expressed as mean ± S.D. Comparisons between multiple treatment groups were performed using one-way ANOVA, followed by Bonferroni multiple comparisons, and p ≤ 0.05 was considered statistically significant. The PCR data expressed as mean ± SEM was analyzed utilizing a t-test with Welch correction, and p ≤ 0.05 was considered statistically significant. Statistical tests were performed using GraphPad Prism Software 6.0 (GraphPad Prism, San Diego, CA).
Results
Characterization of TRI MS: IL-2, TGF-β1 and Rapamycin
TGF-β microspheres (MS) were reformulated from what was previously described [refs28,29,30,31] to eliminate the 20-day initial lag phase of release in the prior formulation. The new formulation of TGF-β MS contains a PEG-PLGA diblock copolymer (4 wt%, Mn ~5 kDa), which accelerated release by increasing matrix swelling, and the ester-terminated PLGA helped to minimize the electrostatic interactions between the PLGA polymer and the positively charged protein32. After measuring the release of TGF-β, the surface morphology of the microspheres was characterized using scanning electron microscopy (SEM). The representative SEM images indicate that the rapamycin and IL-2 MS possessed similar surface morphology and release behavior as previously reported (Supplemental Fig. 1)22. SEM images reveal spherical non-porous PLGA-based rapamycin microspheres (Supplemental Fig. 1). IL-2 MS exhibit surface porosity and a high initial burst followed by a slow continuous release for the length of the experimental study, as previously described (Supplemental Fig. 1)22. The newly fabricated TGF-β microspheres contained an uneven surface morphology, similar to a previous report utilizing PEG and PLGA microcapsules28. The average size of TRI MS was 12 µm (rapamycin), 19 µm (IL-2), and 17 µm (TGF-β) as determined by Coulter Counter (volume impedance method).
TRI MS Prevent Loss of Aqueous Tear Production
To investigate whether TRI MS were capable of preventing key signs of dry eye disease, we first examined aqueous tear secretion25. Concanavalin A (ConA) was injected into the lacrimal gland to induce DED, and for TRI MS or Blank MS treatment groups, MS were incorporated in ConA injections (Fig. 1). One week following the administration of ConA with either Blank MS or TRI MS, phenol red thread testing was performed to evaluate tear secretion. The administration of ConA alone (diseased) considerably reduced tear production as compared to an injection of Saline (non-diseased) (Fig. 2A). Notably, tear secretion was restored to non-diseased levels in DED mice treated with TRI MS, while administration of ConA + Blank MS (unloaded) had no noticeable effect on tear production in mice (Fig. 2A). In order to identify whether all three factors (TRI MS) were required to prevent loss of aqueous tear production, mice were treated with individual microsphere formulations alone (Rapa, TGF-β, or IL-2) or combinations of two microsphere formulations (Rapa + TGF-β; Rapa + IL-2; TGF-β + IL-2). Notably, the individual microspheres alone and the combinations of two microsphere formulations were unable to restore tear production inhibited by ConA (Supplemental Fig. 2), suggesting that therapeutic efficacy required the delivery of the TRI MS to prevent the loss of tear production.
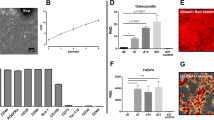
TRI MS prevent clinical signs of inflammation associated with DED. (A) Wetting of phenol red threads were measured in millimeters using a dissecting microscope (n = 6) shown as mean ± S.D. (B) Representative images of histological sections of the eyes (20X) were quantified to identify differences in the TRI MS group compared to the diseased groups and non-diseased group (100 µm scale bar). (C) Goblet cells shown are the pink/purple (Periodic Acid Schiff stained) cells located in the conjunctiva labeled with arrows and the groups are shown as mean ± S.D. *p ≤ 0.05; **p ≤ 0.01; ***p ≤ 0.001, ****p ≤ 0.0001.
Goblet Cell Density Maintained with the Administration of TRI MS
Mucin is a key component associated with a healthy tear film, which is produced by goblet cells located in the conjunctiva29,30. As the density of goblet cells are diminished this can contribute to an unstable tear film and lead to ocular surface destruction30. Upon examination of ocular tissue histology, we observed a substantial decrease in the density of Periodic Acid Schiff (PAS)-stained goblet cells (pink/purple cells in conjunctiva epithelium layer) in the ConA group as compared to the Saline group (Fig. 2B,C)25,26,29,31,33. Treatment with TRI MS led to maintenance of goblet cell density, unlike mice with ConA-induced DED (Fig. 2B). Interestingly, the individual microspheres alone and the combinations of two microsphere formulations were unable to prevent goblet cell loss (Supplemental Fig. 3). Overall, histological sections revealed that TRI MS treatment markedly inhibited ConA-induced attenuation of goblet cells.
Corneal Fluorescein Staining Reduced with TRI MS
To determine the health of the ocular surface, corneal fluorescein staining was performed, with the degree of punctate staining as an indicator of disease severity34. Fluorescent images of the ocular surface were captured and scored by a masked ophthalmologist on a scale of 0 to 4, with 0 corresponding to no staining, and 4 corresponding to staining on more than 50% of the cornea, as seen in (Fig. 3A). The ocular staining score was considerably lower for the Saline and TRI MS groups as compared to the ConA + Blank MS group (Fig. 3B). We also examined eyes from mice treated with ConA plus individual microsphere formulations alone or combinations of two microspheres. Neither individual microspheres alone and combinations of two microsphere formulations, were able to reduce corneal fluorescein staining to the same extent as the TRI MS treatment (Supplemental Fig. 2), suggesting that local administration of TRI MS is necessary to restore ocular surface health that is impaired by ConA.
TRI MS Decrease Pro-Inflammatory Cytokines
Several cytokines in the local milieu of the lacrimal glands was examined following treatment. Notably, while ConA induced expression of pro-inflammatory IFN-γ, IL-6, and IL-2 in the lacrimal gland (Fig. 4), TRI MS treatment substantially reduced expression of each of these cytokines, compared to the administration of ConA alone (Fig. 4)25,26. The relative expression of pro-inflammatory cytokines in the lacrimal glands can be correlated with infiltration of CD3+ T cells, which was increased in the ConA + Blank MS group and reduced with TRI MS treatment (Fig. 5)35. Together these data indicate that the TRI MS treatment was able to reduce the ConA-induced expression of pro-inflammatory cytokines in the lacrimal gland tissue.
Representative lacrimal gland fixed frozen cryosections (10X magnification) stained for T-cells (CD3+ T cells-Cyan), Regulatory T-cells (FoxP3+ T cells - Red), and nuclei (DAPI-blue). Scale bars are 100 μm. Quantification of lacrimal gland T cells per imaged field and % Treg, based on IHC images with FoxP3 staining (n = 4–5 per group) as shown as mean ± S.D *p ≤ 0.05; **p ≤ 0.01; ***p ≤ 0.001.
TRI MS Increase the Percentage of FoxP3+ Tregs of overall CD3+ T cells in the Lacrimal Gland
In order to examine the local immune environment of T-cells in the lacrimal gland, we performed immunofluorescence staining of lacrimal gland sections with anti-CD3 and anti-FoxP3 monoclonal antibodies. While there were fewer total numbers of infiltrating CD3+ T cells with TRI MS treatment, there was a larger ratio of those FoxP3+ Tregs of overall CD3+ T cells, compared to the ConA alone and ConA + Blank MS groups (Fig. 5). Collectively, this data suggest that the sustained delivery of TRI MS is capable of locally enriching Treg populations as compared to effector T cells in the lacrimal gland tissue.
Suppression of Tregs via Administration of Anti-GITR
An agonistic antibody (DTA-1) specific for GITR (glucocorticoid tumor necrosis factor) was administered 1 day after the injection of the ConA and TRI MS to determine whether the prevention of dry eye symptoms are mediated by the expanded Treg population36. Monoclonal antibody anti-GITR (DTA-1) acts to systemically attenuate the suppressive function of Tregs by inhibiting the ability of conventional T cells to be suppressed by Tregs37,38,39. Mice were administered anti-GITR, one day after ConA and TRI MS. The anti-GITR group (with TRI MP administration) exhibited restored pathological features of DED as indicated by the decrease of aqueous tear secretion (Fig. 1A), reduction of goblet cells in the conjunctiva (Fig. 2B,E) and increase of fluorescein staining (Fig. 3C,D) as compared to the TRI MS group without anti-GITR. Moreover, with the administration of anti-GITR, expression of pro-inflammatory cytokines were considerably increased in the lacrimal gland as compared to the TRI MS with no anti-GITR (Fig. 5).
Discussion
Dry eye disease (DED) is an ocular disorder that accounts for approximately 25 percent of patient visits to an eye care specialist40. Due to the prominent number of patients suffering from symptoms of DED, a number of investigations are examining the underlying cause of the disease4,5,11. Specifically, DED is thought to be mediated by CD4+ T cells41,42. Hallmarks of CD4+ T cell-mediated inflammation associated with DED include epithelial apoptosis, abnormal tear film composition and an increase of pro-inflammatory cytokines within the ocular tissue43,44. Furthermore, these claims have been substantiated adoptive transfer of pathogenic CD4+ T cells from a mouse with DED-like symptoms to a normal recipient, leading to the development of DED10. Conversely, when a subset population of CD4+ T cells known as regulatory T cells (Tregs) were adoptively transferred to a mouse with DED, immune-mediated ocular surface inflammation was attenuated45. Moreover, the local recruitment of Tregs to the lacrimal gland utilizing controlled release of CCL22 (chemokine) effectively prevented signs of DED46. Notably, however, Tregs can represent low total numbers of T-cells in the periphery, which could possibly make it non-trivial to achieve enough functional Treg to shift the homeostatic balance47. For this reason, we hypothesized that inducing (differentiating) Tregs from a more prevalent, naive CD4+ population could also be a viable strategy that was worth exploration.
Typically, signs of DED in patients can include ocular dryness due to a reduction in tears, which can lead to a decrease of visual acuity30,48. Within the tears there are three main components that support the ocular surface; water, mucin, and lipid49. All of these three components play an integral role in lubricating the ocular surface and maintaining health50. As ocular dryness ensues, a lack of lubrication and epithelial surface protection can result51. Due to the integral role tears play in maintaining a healthy ocular surface, tear secretion was evaluated to determine whether the preventative treatment (TRI MS) decreased tear loss thereby subsequently preserving ocular lubrication. Our data suggest there was a substantial reduction of tears in the ConA alone as compared to the Saline (Fig. 2), as expected25,26,46. Notably, the TRI MS considerably prevented the reduction of tears as compared to the ConA alone group (Fig. 2). However, when either the individual microsphere formulations alone (Rapa, TGF-β, IL-2) or the combination of two microsphere formulations (Rapa + TGF-β; Rapa + IL-2; TGF-β + IL-2) were administered, there was no substantial restoration of tear production observed (Supplemental Fig. 2). These data suggest the combination of all three factors (TRI MS) are required to achieve prevention of tear loss.
In addition to tear production, we also investigated the effects of the treatment on goblet cells, which produce the tear film (mucin)52; a key component that provides a protective and stabilizing function for the ocular surface53. The histological sections of the eye tissue were examined to identify if goblet cells were preserved with the administration of TRI MS. Notably, there was a considerable preservation of goblet cells in the TRI MS group as compared to the ConA alone and ConA + Blank MS groups (Fig. 2). This may be due to reduced expression of IFN-γ in lacrimal glands of mice treated with TRI MS, compared to the ConA alone treated mice (Fig. 4), as increased expression of IFN-γ has been attributed to the sustained proliferation of CD4+ effector T cells (Th1 cells)41,43. For example, mice with DED exhibit increased frequencies of the pro-inflammatory Th1 cytokine IFN-γ, which can infiltrate the conjunctiva, causing a reduction of goblet cells18. Notably, previously published data suggest that the overall number of goblet cells were not affected in IFN-γ knock out mice with DED, demonstrating the potential specific involvement of IFN-γ in DED pathogenesis54. Indeed, the protective effects of TRI MS may be a result of reduced infiltrating Th1 cells in general, or a reduction in IFN-γ specifically (Fig. 4)44.
As goblet cells undergo apoptosis, potentially due to IFN-γ, the composition of the tear film can become abnormal, which may lead to a disruption of the corneal epithelial tissue51. For this reason, an ocular staining test was performed to determine if the reductions in tear secretion and goblet cell density corresponded to an increase of corneal fluorescein staining55. Specifically, the increase in corneal staining may be due to the fluorescein dye remaining in areas left by desquamated epithelial cells55. As expected, corneas from the ConA alone and ConA + Blank MS groups showed a considerable increase of corneal fluorescein staining compared to the Saline and TRI MS groups (Fig. 3).
Previous reports have shown that a potential explanation for the reduction of fluorescein staining may be reduced levels of pro-inflammatory cytokines11,56. To investigate whether the reduction in corneal epithelial destruction in our studies corresponded with a decrease in pro-inflammatory cytokines, qRT-PCR was performed on the lacrimal gland tissue to detect changes in expression of IL-2, IL-6 and IFN-γ. In addition to the better-known inflammatory function of IL-2 and IFN-γ, there has been observed increases of the pro-inflammatory cytokine IL-6 in dry eye patients11. As expected, IL-2 and IFN-γ levels were considerably decreased in the TRI MS as compared to the ConA alone and ConA + Blank MS groups, which may be due to TRI MS mitigating the effects of ConA causing inflammation26,57. A decrease of IL-6 expression levels was also detected in the TRI MS as compared to ConA alone group. Overall, there was a substantial difference between the ConA alone and ConA + Blank MS and TRI MS groups levels of pro-inflammatory cytokines within the lacrimal gland. These results likely correlate to the observed decrease of CD3+ T cells in the TRI MS as compared to the ConA alone group (Fig. 5).
If the shift in the pro-inflammatory milieu of the ocular tissue were a result of the TRI MS expanding the expression of FoxP3+, then it would be expected that there would be a greater number of Tregs (or at least an increase in the ratio of Treg-to-effector T-cells) in the lacrimal gland tissue. Accordingly, immunofluorescent staining of total CD3+ T cells and FoxP3+ Tregs was performed on the lacrimal gland tissue. We indeed observed a considerable increase in total numbers of CD3+ T cells in the lacrimal glands of ConA alone and ConA + Blank MS groups, as compared to the Saline and TRI MS groups (Fig. 5). We also observed a considerable increase in the ratio of Treg-to-effector T-cells in the TRI MS as compared to the ConA alone and ConA + Blank MS groups (Fig. 5), supporting the hypothesis that TRI MS are expanding the percentage of Tregs to overall CD3+ T cells. To further test whether TRI MS were preventing signs of DED through the expansion of Tregs, anti-GITR was administered to impair Treg function38. Specifically, treatment with the agonistic anti-GITR monoclonal antibody (DTA-1) both inhibits the suppressive function of Tregs (via signaling through GITR on Tregs)39,58,59 and causes effector CD4+ and CD8+ T cells (effector T cells) to become resistant to Treg-mediated suppression (via signaling through GITR on conventional T cells)39,59,60. We observed that anti-GITR reversed the beneficial effects of the TRI MS (Figs 2A–C and 3B). Also, there was an observed increase in the overall numbers of CD3+ T cells, and a substantial reduction in the percentage of FoxP3+ of overall CD3+ T cells in the lacrimal gland, potentially indicating that Tregs may be needed to mediate the therapeutic effects of TRI MS. Ultimately, the current study provides proof-in-principle for prevention of DED through induction of endogenous Treg in an experimental murine model. Future studies would be geared toward evaluating this drug-delivery strategy as a treatment for pre-existing DED, as well as testing the efficacy of the TRI MS in a pre-clinical larger animal model such as rabbits. Additionally, future studies geared toward translation would determine pharmacokinetic distribution of factors (which would need to be radiolabeled in order to distinguish them from endogenously produced factors) dose-dependent toxicity, and the exploration of other modes of delivery such as subconjunctival and topical placement. One possible mode of delivery that would be relevant for treating patients may be to use new thermogelling formulations that can provide long-term topical delivery to the surface of the eye61.
In conclusion, our data suggest TRI MS were able to reduce the local pro-inflammatory milieu of the lacrimal gland tissue. TRI MS prevented tear loss, preserved goblet cell density and reduced corneal fluorescein staining, which indicate that the therapy prevented signs of DED. Importantly, TRI MS were able to decrease the total number of CD3+ T cells infiltrating the lacrimal gland tissue and enhance the frequency of FoxP3+ T cells among infiltrating T cells. Ultimately, this experimental murine study provides one potential strategy for future anti-inflammatory therapies to focus on harnessing Tregs to restore the local immunological homeostasis within the ocular tissue.
References
Yu, J., Asche, C. V. & Fairchild, C. J. The economic burden of dry eye disease in the United States: a decision tree analysis. Cornea 30, 379–87 (2011).
Zhou, R. et al. “The Living Eye Disarms” Uncommitted Autoreactive T Cells by Converting Them to Foxp3 + Regulatory Cells following Local Antigen Recognition. J. Immunol. 188(4), 1742–1750 (2012).
Pflugfelder, S. C., Solomon, A., Stern, M. E. & Ph, D. The Diagnosis and Management of Dry Eye. Cornea 19, 644–649 (2000).
Friedman, N. J. Impact of dry eye disease and treatment on quality of life. Curr. Opin. Ophthalmol. 21, 310–6 (2010).
Lemp, M. A. Advances in understanding and managing dry eye disease. Am. J. Ophthalmol. 146, 350–356 (2008).
Okanobo, A., Chauhan, S. K., Dastjerdi, M. H., Kodati, S. & Dana, R. Efficacy of topical blockade of interleukin-1 in experimental dry eye disease. Am. J. Ophthalmol. 154, 63–71 (2012).
Stern, M. E., Gao, J., Siemasko, K. F., Beuerman, R. W. & Pflugfelder, S. C. The role of the lacrimal functional unit in the pathophysiology of dry eye. Exp. Eye Res. 78, 409–416 (2004).
Brusko, T. M., Putnam, A. L. Human regulatory T cells: role in autoimmune disease and therapeutic opportunities 371–390 (2008).
Chauhan, S. K. et al. Autoimmunity in dry eye is due to resistance of Th17 to Treg suppression. J. Immunol. 182, 1247–52 (2009).
Niederkorn, J. Y. et al. Desiccating Stress Induces T Cell-Mediated Sjogren’ s Syndrome-Like Lacrimal Keratoconjunctivitis. J. Immunol. 176, 3950–3957 (2006).
Stevenson, W., Chauhan, S. K. & Dana, R. Dry Eye Disease. Arch. Ophthamology 130, 90–100 (2012).
Miyara, M. & Sakaguchi, S. Natural regulatory T cells: mechanisms of suppression. Trends Mol. Med. 13, 108–116 (2007).
Stein-Streilein, J. & Taylor, A. W. An eye’s view of T regulatory cells. J. Leukoc. Biol. 81, 593–8 (2007).
Rudensky, A. Y. Regulatory T Cells and Foxp3. Immunol Rev 241, 260–268 (2011).
Perry, H. D. et al. Evaluation of Topical Cyclosporine for the Treatment of Dry Eye Disease. Arch. Ophthalmol. 126, 1046 (2008).
Kersey, J. P. & Broadway, D. C. Corticosteroid-induced glaucoma: a review of the literature. Eye 20, 407–16 (2006).
Yadav, M., Stephan, S. & Bluestone, J. A. Peripherally induced Tregs-role in immune homeostasis and autoimmunity. Front. Immunol. 4, 1–12 (2013).
De Paiva, C. S. et al. Dry eye-induced conjunctival epithelial squamous metaplasia is modulated by interferon-gamma. Invest. Ophthalmol. Vis. Sci. 48, 2553–60 (2007).
Horwitz, D. A., Zheng, S. G., Wang, J. & Gray, J. D. Critical role of IL-2 and TGF-β in generation, function and stabilization of Foxp3 + CD4 + Treg. Eur. J. Immunol. 38, 912–915 (2008).
Li, H. & Shi, B. Tolerogenic dendritic cells and their role in transplantation. Cell. Mol. Immunol. 12, 24–30 (2015).
Vignali, D. A., Collison, L. W. & Workman, C. J. How regulatory T cells work. Nat. Rev. Immunol. 8, 523–532 (2009).
Jhunjhunwala, S. et al. Controlled release formulations of IL-2, TGF-β1 and rapamycin for the induction of regulatory T cells. J. Control. release 159, 78–84 (2012).
Perez, V. L., Pflugfelder, S. C., Zhang, S., Shojaei, A. & Haque, R. Lifitegrast, a Novel Integrin Antagonist for Treatment of Dry Eye Disease. Ocul. Surf. 14 (2016).
Hou, J. et al. Design of a superior cytokine antagonist for topical ophthalmic use. Proc. Natl. Acad. Sci. USA 110, 3913–8 (2013).
Lee, M. J. et al. Mesenchymal stem/stromal cells protect the ocular surface by suppressing inflammation in an experimental dry eye. Mol. Ther. 1–8, https://doi.org/10.1038/mt.2014.159 (2014).
Lee, M. J. et al. Topical TSG-6 administration protects the ocular surface in two mouse models of inflammation-related dry eye. Investig. Ophthalmol. Vis. Sci. 56, 5175–5181 (2015).
Glowacki, A. J. et al. Prevention of inflammation-mediated bone loss in murine and canine periodontal disease via recruitment of regulatory lymphocytes. Proc. Natl. Acad. Sci. USA 110, 18525–30 (2013).
Pisani, E. et al. Tuning microcapsules surface morphology using blends of homo- and copolymers of PLGA and PLGA-PEG. Soft Matter 5, 3054 (2009).
Kunert, K. S., Tisdale, A. S. & Gipson, I. K. Goblet cell numbers and epithelial proliferation in the conjunctiva of patients with dry eye syndrome treated with cyclosporine. Arch. Ophthalmol. 120, 330–7 (2002).
Rolando, M. & Zierhut, M. The ocular surface and tear film and their dysfunction in dry eye disease. Surv. Ophthalmol. 45(Suppl 2), S203–10 (2001).
Zhang, Z. et al. Therapeutic effects of topical doxycycline in a benzalkonium chloride-induced mouse dry eye model. Investig. Ophthalmol. Vis. Sci. 55, 2963–2974 (2014).
Balmert, S. C. et al. Positive charge of ‘sticky’ peptides and proteins impedes release from negatively charged PLGA matrices. J. Mater. Chem. B 3, 4723–4734 (2015).
Baudouin, C. et al. Role of hyperosmolarity in the pathogenesis and management of dry eye disease: Proceedings of the ocean group meeting. Ocul. Surf. 11, 246–258 (2013).
Lin, Z. et al. A mouse dry eye model induced by topical administration of benzalkonium chloride. Mol.Vis. 17, 257–264 (2011).
Gantner, F., Leist, M., Lohse, A. W., Germann, P. G. & Tiegs, G. Concanavalin A-induced T-cell-mediated hepatic injury in mice: the role of tumor necrosis factor. Hepatology 21, 190–198 (1995).
You, S. et al. Key role of the GITR/GITRLigand pathway in the development of murine autoimmune diabetes: A potential therapeutic target. PLoS One 4, 1–13 (2009).
Cohen, A. D. et al. Agonist anti-GITR monoclonal antibody induces melanoma tumor immunity in mice by altering regulatory T cell stability and intra-tumor accumulation. PLoS One 5 (2010).
Coe, D. et al. Depletion of regulatory T cells by anti-GITR mAb as a novel mechanism for cancer immunotherapy. Cancer Immunol. Immunother. 59, 1367–1377 (2010).
Shimizu, J., Yamazaki, S., Takahashi, T., Ishida, Y. & Sakaguchi, S. Stimulation of CD25(+) CD4(+) regulatory T cells through GITR breaks immunological self-tolerance. Nat. Immunol. 3, 135–142 (2002).
Lin, M. C. et al. Dry eye disease. Optom. Vis. Sci. 92, 922–924 (2015).
Pflugfelder, S. C., Corrales, R. M. & de, Paiva, C. S. T helper cyotkines in dry eye disease. Exp. Eye Res. 117, 520–529 (2013).
Coursey, T. G. et al. Chemokine receptors CCR6 and CXCR3 are necessary for CD4+ T cell mediated ocular surface disease in experimental dry eye disease. PLoS One 8 (2013).
El Annan, J. et al. Characterization of effector T cells in dry eye disease. Invest. Ophthalmol. Vis. Sci. 50, 3802–7 (2009).
Guzmán, M. et al. Desiccating-stress-induced disruption of ocular surface immune tolerance drives dry eye disease. Clin. Exp. Immunol. 184, 248–256 (2015).
Siemasko, K. F. et al. In vitro Expanded CD4+ CD25+ FoxP3+ Regulatory T Cells Maintain a Normal Phenotype and Suppress Immune-Mediated Ocular Surface Inflammation. Invest. Ophthalmol. Vis. Sci. 9(12), 5434–40 (2008).
Ratay, M. L. et al. Treg-recruiting microspheres prevent inflammation in a murine model of dry eye disease. J. Control. Release 258, 208–217 (2017).
Sakaguchi, S., Wing, K., Onishi, Y., Prieto-Martin, P. & Yamaguchi, T. Regulatory T cells: How do they suppress immune responses? Int. Immunol. 21, 1105–1111 (2009).
Brady, M. T. & Yanni, J. M. Preservation of Tear Film Integrity and Inhibition of Lacrimal Gland Inflammation – Induced Dry Eye. J. Ocul. Pharmacol. Ther. 21 (2005).
Baudouin, C. The pathology of Dry Eye. Surv. Ophthalmol. 45, S211–S220 (2001).
Brewitt, H. & Sistani, F. Dry eye disease: the scale of the problem. Surv. Ophthalmol. 45, 199–202 (2001).
Tiffany, J. M. Tears in health and disease. Eye (Lond). 17, 923–926 (2003).
Yoon, K.-C. et al. Tear production and ocular surface changes in experimental dry eye after elimination of desiccating stress. Invest. Ophthalmol. Vis. Sci. 52, 7267–73 (2011).
Pflugfelder, S. C., Corrales, R. M. & de Paiva, C. S. T helper cytokines in dry eye disease. Exp. Eye Res. 117, 118–125 (2013).
Pflugfelder, S. C. et al. Aqueous Tear Deficiency Increases Conjunctival Interferon-γ (IFN-γ) Expression and Goblet Cell Loss. Investig. Opthalmology Vis. Sci. 56, 7545 (2015).
Bron, A. J., Argueso, P., Irkec, M. & Bright, F. V. Clinical staining of the ocular surface: Mechanisms and interpretations. Prog. Retin. Eye Res. 44, 36–61 (2015).
De Paiva, C. S. et al. Corticosteroid and doxycycline suppress MMP-9 and inflammatory cytokine expression, MAPK activation in the corneal epithelium in experimental dry eye. Exp. Eye Res. 83, 526–535 (2006).
Palacios, R. C. A triggers T lymphocytes by directly interacting with their receptors for activation. J. Immunol. 128, 337–342 (1982).
Valzasina, B. et al. Triggering of OX40 (CD134) on CD4 (+) CD25 (+) T cells blocks their inhibitory activity: a novel regulatory role for OX40 and its comparison with GITR. Blood. 105, 2845–2851 (2005).
Bushell, A. & Wood, K. GITR ligation blocks allograft protection by induced CD25+ CD4+ regulatory T cells without enhancing effector T-cell function. Am. J. Transplant. 7, 759–768 (2007).
Stephens, G. L. et al. Engagement of glucocorticoid-induced TNFR family-related receptor on effector T cells by its ligand mediates resistance to suppression by CD4+ CD25+ T cells. J. Immunol. 173, 5008–5020 (2004).
Fedorchak, M. V., Conner, I. P., Schuman, J. S., Cugini, A. & Little, S. R. Long Term Glaucoma Drug Delivery Using a Topically Retained Gel/Microsphere Eye Drop. Sci. Rep. 7, 8639 (2017).
Acknowledgements
This work was supported in part by the National Institutes of Health (NIH) CORE Grant P30 EY008098, the University of Pittsburgh, Pittsburgh, PA; an unrestricted grant from Research to Prevent Blindness, NY; Howard Hughes Medical Institute, Medical Fellows Program. Research reported in this publication was supported by the National Center for Advancing Translational Sciences of the National institutes of Health under Award Number TL1R001858. The content is solely the responsibility of the authors and does not necessarily represent the official view of the National Institute of Health. We would also like to acknowledge Katherine A. Davoil for assisting with sectioning/staining the ocular histology and Dr. Julia K. Polat for scoring the corneal fluorescein images.
Author information
Authors and Affiliations
Contributions
M.L.R. wrote the manuscript and completed all murine studies. S.C.B. performed qRT-PCR and counted images in a masked fashion. A.P.A. contributed to counting cells in a masked fashion and editing manuscript. A.C.G. contributed to the particle fabrication and characterization. T.M. performed sectioning and immunofluorescent staining on the lacrimal gland tissue. S.R.L. revised the manuscript. All authors reviewed the manuscript.
Corresponding author
Ethics declarations
Competing Interests
The authors declare that they have no competing interests.
Additional information
Publisher's note: Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made. The images or other third party material in this article are included in the article’s Creative Commons license, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons license and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this license, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Ratay, M.L., Balmert, S.C., Acharya, A.P. et al. TRI Microspheres prevent key signs of dry eye disease in a murine, inflammatory model. Sci Rep 7, 17527 (2017). https://doi.org/10.1038/s41598-017-17869-y
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41598-017-17869-y
This article is cited by
-
Local induction of regulatory T cells prevents inflammatory bone loss in ligature-induced experimental periodontitis in mice
Scientific Reports (2022)
-
Cranberry extract-based formulations for preventing bacterial biofilms
Drug Delivery and Translational Research (2021)
-
Auto-antigen and Immunomodulatory Agent–Based Approaches for Antigen-Specific Tolerance in NOD Mice
Current Diabetes Reports (2021)
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.