Abstract
New diagnostics are needed to improve clinicians’ ability to detect tuberculosis (TB) disease in key populations such as children and persons living with HIV and to rapidly detect drug resistance. Circulating cell-free DNA (ccfDNA) in plasma is a diagnostic target in new obstetric and oncologic applications, but its utility for diagnosing TB is not known. Here we show that Mycobacterium tuberculosis complex DNA can be detected in plasma of persons with sputum smear-positive TB, even in the absence of mycobacteremia. Among 40 participants with bacteriologically-confirmed smear-positive TB disease who had plasma tested by quantitative PCR (qPCR), 18/40 (45%) had a positive result on at least one triplicate reaction. Our results suggest that plasma DNA may be a useful target for improving clinicians’ ability to diagnose TB. We anticipate these findings to be the starting point for optimized methods of TB ccfDNA testing and sequence-based diagnostic applications such as molecular detection of drug resistance.
Similar content being viewed by others
Introduction
Tuberculosis (TB) is the leading infectious cause of death globally, though it is preventable, treatable and curable. In 2015 there were an estimated 10.4 million new cases worldwide, including at least 1 million cases in children and 480,000 new cases of multi-drug resistant TB (resistant to at least rifampin and isoniazid)1. Globally, however, one third of cases go undetected and unreported, presumably due in part to inadequate diagnostics. Mycobacterial culture is the reference standard for TB diagnosis but is not widely available in resource-limited settings. Sputum microscopy, pioneered by Robert Koch in 1882, remains the mainstay of diagnosis globally. Drug susceptibility testing is critical to ensuring people with TB are on appropriate treatment but is also not widely available in resource-limited settings. The cartridge-based Xpert MTB/RIF® (“Xpert”) real-time PCR assay for molecular detection of Mycobacterium tuberculosis complex (MTBC) and rifampin resistance has improved sensitivity over microscopy and allows for rapid detection of resistance to a key drug in the treatment of TB2,3. However, important diagnostic gaps remain. Therefore, there is an urgent need for improved diagnostic approaches, both for detection of disease and for detection of drug resistance in order to guide appropriate treatment for persons with TB.
Most existing tests for detecting TB and identifying drug resistance require a sputum sample. Even when the gold standard culture is available, diagnostic yield from sputum is poor in patient populations such as young children, persons with extrapulmonary TB, and persons living with HIV. Further, bacteria that grow in culture may not be fully representative of the bacterial populations within a person with active disease4. Drug resistance testing (DST) generally relies on a culture isolate. Given the slow growth of MTBC this can delay results for months and lead to ineffective treatment regimens and acquisition of resistance to additional drugs. Blood would be an attractive sample type, particularly in persons without pulmonary TB or who are not able to produce sputum.
Human circulating cell-free DNA (ccfDNA) results from cellular turnover and release of small fragments of DNA into the bloodstream. There are examples of the diagnostic utility of detecting human DNA fragments in such applications as early prenatal fetal genetic testing, where fragments of fetal DNA are detected in maternal plasma5. Detection of cell-free DNA in plasma is also being explored as a method of “liquid biopsy” for cancers6. We sought to determine whether DNA from M. tuberculosis can be detected in the plasma of persons with TB disease. If so, it could be a possible target for improving clinicians’ ability to detect TB and to obtain molecular data in a more timely fashion than is currently available.
Methods
Study participants
We recruited adults ≥18 years from clinics and hospitals in Kisumu County, Kenya with TB diagnosed by positive sputum smear microscopy and on treatment ≤7 days.
Specimen collection procedures
Sputum and urine were collected in 50 mL falcon sterile containers (Beckton Dickinson (BD), Franklin Lakes, NJ). Blood (5 mL) was collected directly into Myco/F Lytic bottles (Becton Dickinson, Franklin Lakes, NJ) for mycobacterial culture, and 10 mL was collected directly into K2EDTA Vacutainer tubes (BD) for plasma preparation.
HIV testing was offered to all participants with unknown status or with negative results from testing performed more than three months prior to enrollment.
Urine (approximately 50 mL) was centrifuged at 3,000 x g for 10 minutes and then the supernatant was decanted to leave approximately 5 mL specimen. Sputum and concentrated urine were then processed using the standard N-acetyl-L-cysteine/4% sodium hydroxide-2.9% sodium citrate (NALC/NaOH Na-citrate, final concentration of NaOH 1%) method7. Following centrifugation, specimens were decanted and resuspended in 2.0 mL of fresh phosphate buffer (pH 6.8). The concentrated pellet was mixed completely and a total of 0.5 mL of processed specimen was inoculated into one Mycobacterial Growth Indicator Tube [(MGIT), BD]. Myco-F/Lytic blood cultures were placed directly into the BD BACTECTM 9120 instrument.
Plasma was prepared by centrifugation of blood EDTA tubes at 1,500 x g for 10 minutes (“single-spin” plasma). Plasma to be used for DNA preparation (“double-spin” plasma) was transferred to four microfuge tubes and centrifuged at 16,000 x g for 10 minutes. Supernatants were carefully removed from each tube, pooled, and stored at −80 °C. Target time from blood collection to plasma preparation was 2 hours, but samples were accepted at any time within the same day for processing.
DNA was prepared from 4 mL of plasma using the QiaAmp Circulating Nucleic Acid Kit (Qiagen, Hilden, Germany) and eluted with 20 μL buffer AVE.
HIV testing was performed according to the Kenya national guidelines using two separate rapid serologic tests. If the first rapid test was positive, a second rapid test was performed for confirmation.
Culture
MGIT cultures were incubated in the MGIT 960TM instrument and Myco/F lytic bottles were incubated in the BD BACTECTM 9120 instrument for up to 6 weeks each. Cultures flagged as positive were inoculated to brain heart infusion media to determine the presence of contamination by non-mycobacterial species; smears of culture broth were also prepared and stained using Ziehl-Neelsen stain and bright-field microscopy to confirm the presence of acid-fast bacilli (AFB). BACTEC cultures that were positive by AFB microscopy were sub-cultured to Lowenstein Jensen media and incubated at 37 °C. MGIT and BACTEC cultures demonstrating growth consistent with Mycobacterium sp. were identified using the MGIT TBc Identification Test (Beckton Dickinson Diagnostics, Spark, MD) and Capilia TB Neo (Tauns, Kozuwa, Japan), respectively. MGIT cultures with both Mycobacterium sp. and contaminating species were re-decontaminated using the standard method described above.
Xpert testing
Xpert testing (Cepheid, Sunnyvale, CA) of sputum was performed by mixing 0.75 mL of the processed sputum pellet with sample buffer at a ratio of 2:1 and processed and tested according to the manufacturer’s instructions. We performed Xpert testing on single-spin plasma according to the manufacturer’s protocol for testing of sputum. Xpert testing of plasma was discontinued after approximately 30 tests were performed with no positive results.
Real-time PCR
Real-time PCR (qPCR) was performed using primers (F: 5′-CCTACTACGACCACATCA-3′; R: 5′-CCGTAAACACCGTAGTTG-3′; probe: 5′-/56-FAM/ATGTGCTCCTTGAGTTCGCCAT/3BHQ_1/-3′, Integrated DNA Technologies, Coralville, Iowa) that amplify a 106 base pair region of IS6110 in M. tuberculosis and were found to not amplify a product when tested against a panel of non-tuberculous mycobacteria and other respiratory pathogens (M. Willby, personal communication). Reaction mixture (20 μL total) included 1X Lightcycler Mix (Roche, Basel, Switzerland) 2 or 3 μL DNA template, and 300nM final concentration each of forward and reverse primers and probe (Integrated DNA Technologies, Coralville, Iowa). Cycling and detection was performed on the Applied Biosystems 7500 Fast Real-Time PCR System using the following conditions: initial incubation at 95 °C for five minutes, 45 cycles of 95 °C for 15 seconds and 60 °C for one minute. Samples were tested in triplicate. A qPCR reaction targeting human RNAseP was used to confirm that DNA had been purified from each sample tested8.
Ethical approval
This study was reviewed and approved by the CDC and Kenya Medical Research Institute IRBs (CDC Protocol #6484) and all experiments were performed in accordance with relevant guidelines and regulations. All participants provided written informed consent.
Data availability
The datasets generated during and/or analysed during the current study are available from the corresponding author on reasonable request.
Results
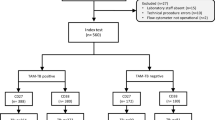
A total of 55 potential participants were screened, 51 were determined to be eligible, and of these one declined enrollment. A total of 50 participants were enrolled, including 32 (64%) with HIV and 18 (36%) without HIV infection; all but 3 participants consented to having blood drawn (Table 1). Among participants with HIV, median CD4 was 238 cells/mm3 (interquartile range 96–340). All participants were enrolled on the basis of having a positive sputum smear result as performed under routine program conditions. Of the 50 participants, 47 (94%) participants had sputum, blood, or urine positive for MTBC by Xpert and/or liquid culture (bacteriologically confirmed TB disease); all participants with blood or urine culture positive for MTBC also had a positive sputum Xpert and/or culture. Of the three participants who did not have confirmation of sputum positive for MTBC, one had sputum tested by both Xpert and culture and two had sputum tested by Xpert only.
Of 43 plasma DNA samples tested by qPCR, 19 (44%) were positive in at least one of the triplicate reactions (Table 2). All no-DNA template control reactions were negative. Among 40 participants with bacteriologically-confirmed TB disease who had plasma tested by qPCR, 18/40 (45%) were positive in at least one triplicate reaction; of these, one was positive by culture of sputum but not by Xpert testing of sputum. One specimen was positive by qPCR but negative by Xpert testing of sputum and by culture of blood and urine; culture of sputum was not done. Of three participants with mycobacteremia, two were positive by qPCR. Cycle threshold (Ct) scores for all positive IS6110 qPCR reactions were above 33 (median 38, IQR 37–39). A comparison of individual and mean sputum Xpert Ct scores and plasma qPCR Ct scores among participants with positive results for both tests is shown in Table 3. Among the 19 participants with positive plasma qPCR results, three were positive for MTBC by blood culture. One participant with MTBC-positive blood culture had negative plasma qPCR results. Four participants had positive culture of MTBC from urine; of these, all were positive on at least one triplicate reaction. Thirty-one participants, including 29 with confirmed TB disease, had plasma tested by Xpert. Of these, 27 had a final result and two had an error on both first and second Xpert test. All 27 tests with a valid result were negative.
Discussion
We demonstrate the ability to detect MTBC DNA by real-time PCR of plasma samples from persons with sputum smear positive tuberculosis disease, even in the absence of mycobacteremia. Our finding is consistent with the presence of circulating cell-free DNA from MTBC in the plasma of persons with TB disease. Our finding that most participants did not have MTBC-positive blood culture results suggests that bacteria in the blood were not the source of MTBC DNA detected in plasma.
Use of PCR-based methods for detection of MTBC from blood or peripheral blood mononuclear cells has been reported previously with varying yields in different patient populations9,10,11,12,13,14,15,16. However, blood samples were first centrifuged for preparation of whole blood cell pellets or buffy coat/peripheral blood mononuclear cells from which DNA was then isolated, a process that may be expected to concentrate whole TB bacteria as well17. Recently, Ushio et al. reported detection of MTBC DNA in plasma using digital PCR; however, culture of blood was not done and DNA was prepared from whole blood cell pellets18. Therefore, in the Ushio study detection of genomic DNA or DNA from whole organisms cannot be excluded. To our knowledge, the study reported here is the first to detect of MTBC from plasma in the confirmed absence of mycobacteremia.
All but one participant with positive plasma qPCR result had confirmed MTBC detected in sputum using Xpert or culture; for this one participant only sputum Xpert, but not sputum culture, was performed. Although it is not possible to rule out a false positive qPCR result in this participant, it is notable that in another participant with positive qPCR result only culture of sputum, but not Xpert testing of sputum, was positive. Further, on the qPCR reaction plate for this sample none of the other three patient samples run at the same time were positive, decreasing the likelihood of a false positive result from cross-contamination. Relative to the reference standard of culturing sputum, Xpert testing of sputum has sensitivity of approximately 90%3. It is therefore possible that TB disease was not confirmed due to lack of a sufficiently sensitive test.
Only two participants with positive qPCR had positive blood culture for MTBC, and none of the plasma samples tested by Xpert were positive. Xpert was initially developed for testing sputum; however, it has been successfully used to test for MTBC in a wide variety of specimen types including pleural fluid, urine and gastric aspirate and unlike culture, a positive result does not in principle depend on bacterial viability10,19,20,21,22. Although plasma is not a standard sample type for Xpert testing, these results further suggest that bacteria in the blood were not the source of MTBC DNA detected in plasma.
All samples that were positive by qPCR had high cycle threshold (Ct) values, and not all replicates were positive in all cases. This would suggest a low-concentration DNA target near the limit of detection, and that methods for optimization of ccfDNA recovery may be important. These results indicating low template concentration are similar to a recent report of another novel sample type, oral mucosal swabs, for TB diagnosis by real-time PCR testing23. Yield of ccfDNA has been shown to vary according to collection and processing procedures21,24. Detection of target DNA may be improved by specialized blood collection tubes that minimize release of human DNA from the lysis of white blood cells25,26. Sputum Xpert MTB/RIF Ct scores did not show a clear correlation with plasma qPCR Ct values, suggesting there is not a straightforward association between sputum bacterial load as assessed by Xpert MTB/RIF Ct score and detection of plasma DNA. Alternatively, differences in specimen processing (e.g. time from collection to processing) could potentially lead to differences in yield of purified DNA and qPCR sensitivity.
Based on our results, plasma DNA may be a useful target for TB diagnostic testing. Given the modest sensitivity of qPCR compared to Xpert, along with the delayed Ct values observed, improvements in the sensitivity of plasma DNA recovery and detection would be important. This is particularly true as the target for plasma qPCR in this study, IS6110, is a repetitive genetic element in M. tuberculosis, and therefore sensitivity of qPCR for this target may be higher than for other common targets for TB detection including those for detection of drug resistance, such as rpoB. The qPCR assay tested here also generates a very short amplicon which, depending on the size of target DNA in plasma, could enhance its sensitivity compared to alternate qPCR assays dependent on longer amplicons.
Improvements in the sensitivity of plasma TB detection would be important for its potential utility as a diagnostic test. Based on studies of human ccfDNA, methods of optimizing target DNA recovery may be expected to improve molecular detection of TB DNA in plasma. Improvements in the detection rate of ccfDNA in oncologic applications using developing technologies gives reason to be optimistic that improvements in the sensitivity of detection of plasma tuberculosis DNA may be feasible6. This proof-of-principle study included only persons with tuberculosis disease readily diagnosed by sputum smear. Positive sputum smear result is generally indicative of high burden of disease in the lung, but tuberculosis can affect many organ systems and also disseminate widely in the body without resulting in sputum smear positivity. Further study is needed to better determine characteristics of persons with TB disease in whom ccfTB DNA might be detected in plasma. If detected over a broad range of clinical manifestations and severity of disease, TB plasma DNA could provide a target for improving clinicians’ ability to diagnose TB in patients in whom collection or testing of sputum has poor diagnostic yield (e.g., children, people living with HIV, people with extrapulmonary TB). In addition, because we demonstrate detection of TB DNA in plasma, these findings suggest that DNA-based applications such as molecular drug resistance testing may be feasible from plasma. If true, this would represent a significant advantage over methods that rely on sputum or on slow mycobacterial culture.
References
WHO, Global Tuberculosis Report.: Geneva (2016).
Boehme, C. C. et al. Rapid molecular detection of tuberculosis and rifampin resistance. N Engl J Med 363(11), 1005–15 (2011).
Boehme, C. C. et al. Feasibility, diagnostic accuracy, and effectiveness of decentralised use of the Xpert MTB/RIF test for diagnosis of tuberculosis and multidrug resistance: a multicentre implementation study. Lancet. 377(9776), 1495–505 (2011).
Dartois, V. et al. New Evidence for the Complexity of the Population Structure of Mycobacterium tuberculosis Increases the Diagnostic and Biologic Challenges. Am J Respir Crit Care Med 194(12), 1448–1451 (2016).
Gregg, A. R. et al. Noninvasive prenatal screening by next-generation sequencing. Annu Rev Genomics Hum Genet 15, 327–47 (2014).
Parsons, H. A., Beaver, J. A. & Park, B. H. Circulating Plasma Tumor DNA. Adv Exp Med Biol 882, 259–76 (2016).
Kent, P. T. & K., G. Public Health Mycobacteriology: A Guide for the Level III Laboratory (Atlanta, Georgia: U.S. Department of Health and Human Services, Public Health Service, Centers for DiseaseControl 1985).
Agresti, A. et al. Simultaneous confidence intervals for comparing binomial parameters. Biometrics 64(4), 1270–5 (2008).
Feasey, N. A. et al. Evaluation of Xpert MTB/RIF for detection of tuberculosis from blood samples of HIV-infected adults confirms Mycobacterium tuberculosis bacteremia as an indicator of poor prognosis. J Clin Microbiol 51(7), 2311–6 (2013).
Shenai, S. et al. Exploring alternative biomaterials for diagnosis of pulmonary tuberculosis in HIV-negative patients by use of the GeneXpert MTB/RIF assay. J Clin Microbiol 51(12), 4161–6 (2013).
Bwanga, F. et al. Higher blood volumes improve the sensitivity of direct PCR diagnosis of blood stream tuberculosis among HIV-positive patients: an observation study. BMC Infect Dis 15, 48 (2015).
Rebollo, M. J. et al. Blood and urine samples as useful sources for the direct detection of tuberculosis by polymerase chain reaction. Diagn Microbiol Infect Dis 56(2), 141–6 (2006).
Richter, C. et al. PCR detection of mycobacteraemia in tanzanian patients with extrapulmonary tuberculosis. Eur J Clin Microbiol Infect Dis 15(10), 813–7 (1996).
Folgueira, L. et al. Rapid diagnosis of Mycobacterium tuberculosis bacteremia by PCR. J Clin Microbiol 34(3), 512–5 (1996).
Crump, J. A. et al. Performance of nucleic acid amplification following extraction of 5 milliliters of whole blood for diagnosis of Mycobacterium tuberculosis bacteremia. J Clin Microbiol 50(1), 138–41 (2012).
Schluger, N. W. et al. Amplification of DNA of Mycobacterium tuberculosis from peripheral blood of patients with pulmonary tuberculosis. Lancet 344(8917), 232–3 (1994).
Damsker, B. & Bottone, E. J. Mycobacteria and cryptococci cultured from the buffy coat of AIDS patients prior to symptomatology: a rationale for early therapy. AIDS Res 2(4), 343–8 (1986).
Ushio, R. et al. Digital PCR assay detection of circulating Mycobacterium tuberculosis DNA in pulmonary tuberculosis patient plasma. Tuberculosis (Edinb) 99, 47–53 (2016).
Denkinger, C. M. et al. Xpert MTB/RIF assay for the diagnosis of extrapulmonary tuberculosis: a systematic review and meta-analysis. Eur Respir J. (2014).
Marcy, O. et al. Performance of Xpert MTB/RIF and Alternative Specimen Collection Methods for the Diagnosis of Tuberculosis in HIV-Infected Children. Clin Infect Dis. (2016).
Maynard-Smith, L. et al. Diagnostic accuracy of the Xpert MTB/RIF assay for extrapulmonary and pulmonary tuberculosis when testing non-respiratory samples: a systematic review. BMC Infect Dis 14, 709 (2014).
Boyles, T. H. et al. False-positive Xpert(R) MTB/RIF assays in previously treated patients: need for caution in interpreting results. Int J Tuberc Lung Dis 18(7), 876–8 (2014).
Wood, R. C. et al. Detection of Mycobacterium tuberculosis DNA on the oral mucosa of tuberculosis patients. Sci Rep 5, 8668 (2015).
Sherwood, J. L. et al. Optimised Pre-Analytical Methods Improve KRAS Mutation Detection in Circulating Tumour DNA (ctDNA) from Patients with Non-Small Cell Lung Cancer (NSCLC). PLoS One 11(2), e0150197 (2016).
Norton, S. E. et al. A new blood collection device minimizes cellular DNA release during sample storage and shipping when compared to a standard device. J Clin Lab Anal 27(4), 305–11 (2013).
Norton, S. E. et al. A stabilizing reagent prevents cell-free DNA contamination by cellular DNA in plasma during blood sample storage and shipping as determined by digital PCR. Clin Biochem 46(15), 1561–5 (2013).
Acknowledgements
The findings and conclusions in this report are those of the authors and do not necessarily represent the official position of funding agencies. We thank the Director of the Kenya Medical Research Institute for partnership in this study and Peter Cegielski for critical review of the manuscript. This study was funded by US Agency for International Development (USAID). USAID did not participate in study design, data collection, or interpretation of results.
Author information
Authors and Affiliations
Contributions
E.S.C. conceived of and designed the study, analyzed the data and wrote the first draft of the manuscript, W.M. performed P.C.R. experiments, interpreted P.C.R. data, and provided oversight for laboratory procedures; G.O. designed and oversaw clinical enrollment procedures; K.M. developed laboratory standard operating procedures and provided oversight for laboratory procedures; M.W. designed P.C.R. primers and conditions and interpreted P.C.R. data; S.M. provided laboratory quality assurance; H.A. and E.P. contributed to study design and interpretation; J. Posey contributed to study design and supervised development of laboratory procedures; K.C. contributed to study design and supervised the field study. All authors contributed to results interpretation and manuscript development.
Corresponding author
Ethics declarations
Competing Interests
The authors declare that they have no competing interests.
Additional information
Publisher's note: Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made. The images or other third party material in this article are included in the article’s Creative Commons license, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons license and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this license, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Click, E.S., Murithi, W., Ouma, G.S. et al. Detection of Apparent Cell-free M. tuberculosis DNA from Plasma. Sci Rep 8, 645 (2018). https://doi.org/10.1038/s41598-017-17683-6
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41598-017-17683-6
This article is cited by
-
Genome-wide tiled detection of circulating Mycobacterium tuberculosis cell-free DNA using Cas13
Nature Communications (2023)
-
GeneXpert Ultra in Urine Samples for Diagnosis of Extra-Pulmonary Tuberculosis
Current Microbiology (2023)
-
Rapid and sensitive identification of pleural and peritoneal infections by droplet digital PCR
Folia Microbiologica (2021)
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.