Abstract
Previous work has suggested that maternal developmental disorder traits related to autism spectrum disorder (ASD) and attention-deficit hyperactivity disorder (ADHD) are significantly associated with child maltreatment. However, there may be other important maternal characteristics that contribute to child maltreatment. We hypothesized that maternal impulse control disability may also affect child maltreatment in addition to maternal developmental disorder traits. We aimed to test this hypothesis via a cohort study performed in Tokyo (n = 1,260). Linear regression analyses using the Behavioural Inhibition/Behavioural Activation Scales, the self-administered short version of the Pervasive Developmental Disorders Autism Society Japan Rating Scale, the short form of the Adult Attention-Deficit Hyperactivity Disorder Self-Report Scale, and the Child Maltreatment Scale, revealed that excessive inhibition of behaviour and affect, which is impulse control disability, is significantly associated with child maltreatment (b = 0.031, p = 0.018) in addition to maternal developmental disorder traits (ASD: b = 0.052, p = 0.004; ADHD: b = 0.178, p < 0.001). Logistic regression analyses revealed that ASD (adjusted odds ratio [AOR] = 1.083, p = 0.014) and high behavioural inhibition (AOR = 1.068, p = 0.016) were significantly associated with moderate child maltreatment, while ADHD was associated (AOR = 1.034, p = 0.022) with severe child maltreatment. These maternal characteristics may inform the best means for prevention and management of child maltreatment cases.
Similar content being viewed by others
Introduction
Maternal developmental disorders traits related to autism spectrum disorder (ASD) and attention-deficit hyperactivity disorder (ADHD) have been suggested to associate with child maltreatment1. However, the diagnostic criteria for ASD/ADHD2 do not include any psychological characteristics directly related to child maltreatment, and these psychological characteristics may sometimes occur in individuals with ASD/ADHD but are not classified as symptoms. Furthermore, other maternal psychological characteristics besides ASD/ADHD related to child maltreatment may exist.
Wiehe et al. demonstrated abusive parents had a higher tendency of impulse control disability, leading to child maltreatment3. One of the more prominent biological vulnerability models of impulse control disability derives from Gray’s behavioural inhibition system (BIS) and behavioural activation system (BAS)4,5,6,7. Gray proposed that BIS and BAS underlie behaviour and affect resulting in impulsivity8,9. Gray’s BIS/BAS model has been used for conceptualizing theories of impulsivity (e.g.5,6,7). Negative feelings such as fear, anxiety, and frustration associated with impulsivity have been suggested to be related to BIS10,11,12. Sensitivity to reward cues and initiation of behavioural approaches related to impulsivity have been suggested with BAS8,12. At an extreme, a heightened BAS sensitivity may implicate a sociopathic personality6,13. Carver developed the BIS/BAS Scales to measure impulsivity based on the BIS/BAS model14. Impulsivity measured by the BIS/BAS Scales is posited to serve as a correlate to psychopathologic impulse control disability responsible for child maltreatment. To the best of our knowledge, previous studies on maternal psychological characteristics related to child maltreatment have not addressed this matter from the perspective of both maternal impulse control disability and developmental disorder traits such as ASD/ADHD. We hypothesized that maternal impulse control disability is significantly associated with child maltreatment in addition to maternal developmental disorder traits. We investigated this hypothesis via conducting a cohort study on prenatal and postnatal mental health pathologies. Considering the effect of developmental disorder traits, we used the data from our cohort study to investigate how impulsive control disability in mothers, as measured by the BIS/BAS Scales, may affect child maltreatment.
Results
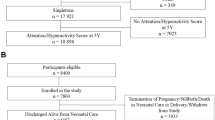
The recruitment process of study participants is shown in Figure 1. A total of 1,775 women who provided informed consent participated in this study. Among them, 1,717, 1,184, 1,383, and 1,376 of them answered the T1 (20 weeks gestation), T2 (a few days after delivery), T3 (two months after delivery), and T4 (three months after delivery) questionnaires, respectively. Table 1 shows the demographic, clinical, and socioeconomic characteristics of the participants. Data from 1,260 participants were included in the analysis, which were collected at T1, T2, and T3 (Table 1). The mean (±standard deviation [SD]) age of the participants was 35.05 (±4.38) years. Among them, 1,254 had partners and 2 did not (missing information from 4 participants). Regarding employment type, the number of full-time workers, part-time workers, temporary workers, and homemakers was 532 (42.22%), 153 (12.14%), 71 (5.63%), and 515 (40.87%), respectively. The number of participants with postgraduate, undergraduate, junior or technical college, high school, or junior high school education was 100 (7.94%), 664 (52.70%), 369 (29.29%), 118 (9.37%), and 9 (0.71%), respectively. The distribution of annual household income was 17 (1.35%) participants making <2 million yen, 250 (19.84%) making 2–4.9 million yen, 582 (46.19%) making 5–9.9 million yen, and 401 (31.83%) making >10 million yen (missing values from 13 participants). Regarding the number of deliveries, there were 895 (71.03%), 139 (11.03%), 44 (3.49%), 82 (6.51%), and 88 (6.98%) women who had had one, two, three, four, and five or more, respectively. One hundred sixty-one participants (12.78%) had a history of psychiatric treatment. The distribution of each item of the Child Maltreatment Scale (CMS)15 is shown in Table 2. The number of women whose total CMS scores were above the cut-off score for “at high risk of moderate child maltreatment” (2/3) and “at high risk of severe child maltreatment” (6/7) was 129 and 23, respectively. The means of the total scores of the CMS (±SDs) of all the participants, women at high risk of moderate child maltreatment, and women at high risk of severe child maltreatment were 1.20 (±1.68), 4.90 (±2.92), and 9.22 (±4.55), respectively. Table 3 shows the results of the cumulative ratio of the total CMS score. The ratios of the women whose total CMS scores were above the cut-off score for “at high risk of moderate child maltreatment” and “at high risk of severe child maltreatment” were 10.24% and 1.83%, respectively. Table 4 shows the multicollinearity of the linear regression analysis. The tolerance values and variance inflation factors (VIFs) in the models were less than 0.4 and 2.5, respectively, which revealed that there was no multicollinearity in Analyses 1, 2, and 3.
Cut-off scores of the Child Maltreatment Scale
Regarding the CMS cut-off score for “at high risk of moderate child maltreatment”, we considered the total score of each item. If the cut-off score was set at 1/2 (i.e. a mother is regarded as in high risk group of moderate child maltreatment if she has the score 2 or more), 2/3 (i.e. a mother is regarded as in high risk group if she has the score 3 or more and as not in high risk group if 2 or less), and 3/4 (i.e. a mother is regarded as in high risk group if she has the score 4 or more and as not in high risk group if 3 or less) with the total score, the ratio of the mothers at high risk of moderate child maltreatment in this study were 22.22%, 10.24%, and 6.67%, respectively. We also referred an Japanese epidemiological study performed in Osaka, the second largest city in Japan16. They reported 9.7% (3,320/34,341)16 of pregnant and puerperal women with psycho-social problems related to child maltreatment. We also checked the rationale for the cut-off score of “at high risk of moderate child maltreatment” from the clinical perspective concerning each item. “Item 1: leaving the child crying” can occur in mothers not exhibiting child-maltreatment behaviour (e.g., when mothers are tired). Due to such situations, it may be normal when this item’s score is coded as 2. However, in situations in which the score of the other items besides Item 1 was 1 or 2, this may imply that a baby’s health or safety may be at high risk and thus cannot be overlooked concerning childcare and prevention of child maltreatment. If the total score was 3 or more, the mothers were considered at least “positive” for items 2–17 irrespective of a positive or negative score for item 1. Thus, the CMS cut-off score of 2/3 for “at high risk of moderate child maltreatment” was regarded as valid and was used for Analysis 2. On the other hand, an epidemiological study16 also reported that pregnant and puerperal women at high risk of severe child maltreatment was 1.2% (470/38,204). Regarding the CMS cut-off score for “at high risk of severe child maltreatment”, we also considered the total score for each item. If it was set at 5/6, 6/7, and 7/8, the mothers at high risk of severe child maltreatment were 2.86%, 1.87%, and 1.03%, respectively. According to these data, the CMS cut-off score for “at high risk of severe child maltreatment” at 6/7 was regarded as appropriate and used for Analysis 3.
Main analysis
Analysis 1: Linear regression analyses comparing four models, unadjusted and models 1–3
Table 5 shows the coefficients of the short version of the Pervasive Developmental Disorders (PDDs) Autism Society Japan Rating Scale (PARS)17 via self-administration, the short-form of the Adult ADHD Self-Report Scale (ASRS) scores18, and the subscale scores of the Japanese version of the BIS/BAS Scales14,19 for the CMS score using linear regression analysis. In the unadjusted model, one unit increase of the self-administered short version of the PARS score (coefficient (b) = 0.081, standard error of b (SE) = 0.016, and p < 0.001), ASRS score (b = 0.243, SE = 0.037, and p < 0.001), and BIS score (b = 0.057, SE = 0.012, p < 0.001) showed a significant increase in the CMS score. In Model 1 (adjusted for history of maternal psychiatric treatment and educational level) and Model 2 (adjusted for simultaneous ASD and ADHD traits in addition to adjustments in Model 1), the scores for the self-administered short version of the PARS (Model 1: b = 0.083, SE = 0.016, and p < 0.001; Model 2: b = 0.058, SE = 0.017, and p = 0.001) and ASRS (Model 1: b = 0.242, SE = 0.037, and p < 0.001; Model 2: b = 0.199, SE = 0.040, and p < 0.001) were also significantly associated with the CMS score. The BIS data showed a significant association with the CMS score in Model 1 (b = 0.060, SE = 0.012, and p < 0.001). In Model 3 (adjusted for simultaneous impulsivity [BIS and BAS] in addition to adjustments in Model 2), the BIS score remained significantly associated with the CMS score as well as the self-administered short version of the PARS and ASRS scores (BIS score: b = 0.031, SE = 0.013, and p = 0.018; the self-administered short version of the PARS score: b = 0.052, SE = 0.018, and p = 0.004; ASRS score: b = 0.178, SE = 0.041, and p < 0.001).
Sub-analyses
Analysis 2: Logistic regression analysis of Model 3 using the cut-off score for “at high risk of moderate child maltreatment” as the dependent variable
The results of the multivariate analysis in Analysis 2 are shown in Table 6. The BIS score (p = 0.016 and AOR = 1.068 [95% CI = 1.012–1.126]) as well as the self-administered short version of the PARS score (p = 0.014 and AOR = 1.083 [95% CI = 1.016–1.153]) showed statistically significance. The area under the curve (AUC), sensitivity, and specificity were 0.645, 0.512 and 0.755, respectively.
Analysis 3: Logistic regression analysis of Model 3 using the cut-off score for “at high risk of severe child maltreatment” as the dependent variable
The results of the multivariate analysis in Analysis 3 are shown in Table 6. The ASRS score (p = 0.022 and AOR = 1.437 [95% CI = 1.054–1.959]) showed statistically significance. The AUC, sensitivity, and specificity were 0.762, 0.696 and 0.781, respectively.
Discussion
Principal findings
This study tested the hypothesis of impulse control disability, as outlined in the BIS/BAS model, and developmental disorder traits being associated with child maltreatment. Three new findings were revealed. First, we demonstrated that excessive inhibition of behaviour and affect, thus, impulse control disability, is significantly associated with child maltreatment in addition to maternal developmental disorder traits. Second, ADHD traits were significantly associated with child maltreatment, even when ASD traits were considered. Third, ASD and ADHD traits may differentially affect the severity of child maltreatment. ASD traits and poor impulse control with excessive inhibition of behaviour and affect were shown to be important risk factors for moderate child maltreatment. ADHD traits were revealed not to be a risk factor for being in high risk group of child maltreatment tendency but high risk group of child maltreatment, with higher risk of child maltreatment.
Strengths and weaknesses of this study
To our knowledge, this is the first report that demonstrated the importance of BIS as a risk factor for child maltreatment. We performed this study in a highly-populated area of Tokyo. The women enrolled in this study were from diverse backgrounds regarding socioeconomic status. Thus, our results are representative and holistically present evidence of risk factors for child maltreatment.
However, this study has several limitations. First, we assessed child maltreatment using a self-reporting questionnaire rather than obtaining information from hospitals or child protection services. Hence, we could not confirm actual child maltreatments of the mothers. However, since self-reporting questionnaires are the primary source for estimating the prevalence of child maltreatment and have also been used to estimate the incidence of maltreatment20,21, we consider our results to be valid. The self-administered short version of the PARS, ASRS, and BIS/BAS Scales are also self-reporting questionnaires and may include measurement bias regarding self-recognition. Second, the study sample may not represent the overall Japanese population. The Setagaya Ward, where the study was conducted, is a residential area in metropolitan Tokyo. Some differences in the psychosocial characteristics analysed in this study may exist between the metropolitan and rural areas of Japan. Third, we tested our hypothesis using a previous study1’s model that investigated the association of developmental disorder traits with child maltreatment across the spectra of maternal psychiatric treatment history and educational level. While our results suggested that these models may predict child maltreatment to some extent, there are other maternal risk factors for child maltreatment22,23,24 not considered in this study.
Comparison with other studies
To note, there was a discrepancy with the previous study1 in terms of the association between ADHD traits and child maltreatment. In that study, the association was not significant when ASD traits were adjusted. In our study, however, the association remained significant when ASD traits were adjusted in Analysis 1. The previous study was conducted at one national children’s hospital, which might have resulted in substantial differences in patient cohorts, given that the 25, 50, and 75th percentile values of the ASRS total scores in that study were 0, 0, and 1 ([Min, Max] = [0, 5]) compared with 0, 1, and 2 ([Min, Max] = [0, 6]) in the present study, respectively. We postulated that the patient population in the previous study may have included a smaller number of women with ADHD than our cohort, which would have weakened the effect of ADHD traits in the association analyses. This may be the reason why that study did not show a significant association between ADHD and child maltreatment when ASD was adjusted. Our results were consistent with the results of the logistic regression analysis, which indicated that ADHD traits are an important risk factor for more severe child maltreatment cases compared with ASD traits. We found that ASD traits were important risk factors, consistent with the previous study1. The current study considered impulse control using the same linear regression models1 in which revealed an association with developmental disorder traits and child abuse.
The significant association between high BIS levels and child maltreatment suggested the importance of paying close attention to maternal characteristics related to excessively active BIS, as these mothers may be prone to child maltreatment. According to Gray’s theory, impulse control disability with high BIS levels leads to anxiety and, consequently, a shift toward the direction of avoidance12. This excessive inhibition of behaviour and affect may lead to immense anxiety concerning parenting and avoidance of childcare. Previous studies have described an association between maternal anxiety and child maltreatment25,26. It is critically important for relevant healthcare professionals to understand maternal anxieties about childcare concerning mothers with high BIS levels who are at risk of child maltreatment. Interventions to relieve maternal anxieties and to empower mothers with parenting skills to shift them from avoidance behaviour to positive attitudes towards childcare may be effective in provision of support and preventing child maltreatment.
Our results shed light on the necessity for conducting psychosocial risk assessments on pregnant women to detect impulse control disability and developmental disorder traits, which can, in turn, be useful in the context of child maltreatment prevention. In Japan, there is a form, provided by the local government, aimed at supporting mothers at high risk for psychosocial problems in order to prevent child abuse. Within this form, maternal mental health problems and other health problems are assessed. These problems include psychiatric diseases, mental retardation, anxiety, chronic diseases, and physical disability16,27. However, this form does not include any item pertaining to the assessment of impulsivity. Fujiwara et al. investigated the association between psychosocial risk factors and child abuse at 4 months postpartum28. The multivariate analysis included the following: mother’s age, gestational weeks when turning in a pregnancy notification form to the local government, parity, unwanted pregnancy, support from the baby’s grandmother after delivery, support from others after delivery, worries about pregnancy or delivery, and depression. Their work revealed that young age, primipara, and unwanted pregnancies predicted child abuse at 4 months postpartum. However, their predictive factors did not include maternal psychosocial factors related to personality. Further research is needed to develop a convenient and highly sensitive assessment tool that detects and/or evaluates maternal impulsivity and developmental disorder traits during pregnancy and postpartum periods.
Implications for clinicians and policymakers
As aforementioned, we revealed impulsivity control disability as an important risk factor for child maltreatment. Psychotherapeutics such as insight-oriented psychotherapy, cognitive behaviour therapy, contingency management, and pharmacological approaches, which are evidence-based, may be beneficial for mothers prone to child maltreatment and impulse control disorder29. In addition, this study demonstrated the importance of both ASD and ADHD traits as risk factors for child maltreatment. Individuals with ASD exhibit characteristics such as persistency, repetitive behaviours, and disabilities with social communication and social interaction across multiple contexts2. Similarly, individuals with ADHD had characteristics such as hyperactivity and inattentions2. Several effective therapies for individuals with ASD and ADHD have been developed30,31. Our results suggested that a therapeutic approach targeting developmental disorder characteristics could be beneficial for abusive mothers with ASD or ADHD traits. Additionally, assessments of developmental disorder traits and impulse control disorder for abusive mothers may help elucidate the difficulties they are facing, which may in turn lead to the creation of better support programs for them.
Unanswered questions and future research
Child maltreatment results from not only maternal characteristics such as maternal impulse control disability and developmental disorder traits but also multiple causes associated with other psychosocial factors32,33. Based on our results, further research is warranted to investigate these factors. Impulsivity was revealed as a vulnerability marker for substance-use disorders34, such as addiction35,36. Child abuse has been described as “not a psychiatric disorder” but as “other conditions that may be a focus of clinical attention” in the Diagnostic Statistical Manual of Mental Disorders Fifth Edition (DSM-5)2. Our results suggested the possibility of child abuse being related to impulsivity control disorder. At present, there is a category called “Disruptive, Impulse-Control, and Conduct Disorders” in the DSM-5. We propose that child abuse to be considered as one of its sub-categories. Child abuse often results in deep psychological scarring in children. However, psychiatric therapeutic approaches are needed not only for the children but also for the abusive mothers. Further research is needed to examine child abuse from the perspective of impulsivity control disorder.
Methods
Study design
This was a longitudinal study that began in September 2012. Participants were recruited between December 2012 and May 2013 (Figure 1). Written informed consent was obtained from all participants. We performed surveys at five time points: 20 weeks gestation and the first few days, two weeks, one month, two months, and three months after delivery. The participants were given subsequent questionnaires unless they either withdrew or did not respond to the preceding questionnaire. The data collected at T1 (20 weeks gestation) and T2 (the first few days after delivery) were paper-based self-administered questionnaires or an iPad (Apple, Inc.) questionnaire application (MMONGA; Xware Corp., Tokyo, Japan). Two months postnatal (T3) and three months postnatal (T4) questionnaires were sent to the participants and returned via mail.
Ethics approval
This study was approved by the research ethics committee of the National Centre for Child Health and Development in Tokyo, Japan and carried out in accordance with established, institutional ethical standards.
Participants
Participants included in this study were pregnant women (20 weeks gestation) who were scheduled for delivery in any of the 14 obstetrics hospitals in the Setagaya Ward. Setagaya Ward is located in the urban area of Tokyo, and its population was 860,935 on December 1, 201237. The number of live births, total fertility rate, and the birth rate per 1,000 persons were 7731, 0.98, and 9.18, respectively, in 201338. All hospitals with obstetrics wards in Setagaya were involved in this study. Participants who planned to deliver at a hospital outside of Setagaya were excluded. If a participant gave birth to a stillborn, the hospital informed our research team, and that participant was excluded from the study. Mothers with stillborn babies were cared for by the obstetricians, midwives, and nurses in the same, standard routine of clinical care. If a participant had psychiatric problems, she received care by the perinatal staff and was referred to other psychiatric clinics or hospitals according to normal protocol.
Measures
Assessment of ASD traits
We used the short version of the PARS17, conducted via self-administration, in T1 to assess the mothers’ ASD traits. The original version, the Pervasive Developmental Disorders Autism Society Japan Rating Scale – Text Revision short version, is interview-based39,40 and has good reliability (α = 0.83) and validity (Pearson’s correlation of its full version with Autism Diagnostic Interview, Revised41 = 0.41)17. The short version of the PARS (interview-based) consists of 12 items17. These 12 items are based on the main symptoms of ASD as listed in the Diagnostic Statistical Manual of Mental Disorders Fourth Edition Text Revision (DSM-IV-TR)42, i.e., qualitative impairment in social interaction and communication and restricted repetitive and stereotyped patterns of behaviour, interests, and activities. In this study, we used this version via self-administration as earlier noted, which has previously been used to investigate the association between developmental disorder traits and child maltreatment1. While the Autism Spectrum Quotient (AQ)43 is known for its ability to detect ASD traits of adults, previous studies revealed that the self-administered short version of the PARS has higher association with child maltreatment than the AQ44,45,46. Therefore, we used the self-administered short version of the PARS score as a continuous variable.
Assessments of ADHD traits
T3 data involved a questionnaire on ADHD traits. ADHD traits were measured by the short-form of the Adult ADHD Self-Report Scale (ASRS)18. It consists of six questions covering attention deficit and hyperactivities based on DSM-IV-TR with valid sensitivity and specificity (68.7% and 99.5%, respectively). The ASRS score was used in the analyses as a continuous variable.
Assessments of maternal impulse control
The behavioural inhibition/behavioural activation scales (BIS/BAS Scales) were used to assess maternal impulse control in T3. The BIS/BAS Scales, which can measure impulsivity, were developed by Craver and White14 on the basis of Gray’s personality theory47,48. They tested the validity of the BIS/BAS Scales, in which, the impulsive quality measured by the Disinhibition-Constraint scale49 was correlated14. Its Japanese version has been validated19 (See Supplementary Information S1). A greater BIS score reflects a greater prone to anxiety, provided the person is exposed to proper situational cues such as punishment, non-reward, and novelty50. Greater BAS scores have also been reported to relate to psychopathy5,51.
Assessments of child maltreatment
The T4 data used in this study were based solely on the child abuse and neglect questionnaire. Hence, we used the CMS that was developed in Japan15 (See Supplementary Information S2). It is composed of 17 items; for each item, 0 (not at all), 1 (rarely), or 2 (sometimes) points are marked, and each point is summed for total score. Its validity has been previously demonstrated (α = 0.77) in an urban community in Japan15.
In Japan, most local administrative governments have two types of centres that manage child maltreatment. Child and family support centres provide advice and counselling for families and children for moderate child maltreatment cases, while child protection centres manage severe maltreatment cases to protect children. Thus, the present study classified child maltreatment into the two categories of moderate and severe child maltreatment. We determined the appropriate CMS cut-off scores for moderate and severe child maltreatment by referencing the distribution of our results and those of a previous Japanese epidemiological study16, with clinical considerations based on those data. Via our results, we set the cut-off scores of “at high risk of moderate child maltreatment” and “at high risk of severe child maltreatment” at 2/3 (i.e. a mother is regarded as in high risk group if she has the score 3 or more and as not in high risk group if 2 or less) and 6/7 (i.e. a mother is regarded as in high risk group if she has the score 7 or more and as not in high risk group if 6 or less), respectively.
Assessment of demographic, clinical, and socioeconomic characteristics
Demographic, clinical, and socioeconomic data (Table 1) were also collected at T1 (partner existence, employment, household income, history of psychiatric treatment, educational level, type of pregnancy, and fertilization) and T2 (age, delivery week, plurality, numbers of delivery, and method of birth).
Data preparation
An electronic database was developed using the collected data. All data input into the database were double-checked. All measurement ranges, means, standard deviations, distributions, outliers, and logical errors were examined.
Privacy protection
All information that could identify individual participants was not input into the database with the exception of participants’ identification numbers.
Statistical analyses
Main analysis
Analysis 1: linear regression analyses comparing four models
To investigate the association of maternal developmental disorder traits and impulse control with child maltreatment, linear regression analyses were performed based on the same models outlined in a previous study1. We analysed four models (the unadjusted model and Models 1–3): the unadjusted model; Model 1 was adjusted by a history of psychiatric treatment and educational level (i.e., Y [child maltreatment] = β0 + β1*[psychiatric treatment history] + β2*[educational level] + β3*[ASD trait or ADHD trait or BIS score or BAS score]; Model 2 was simultaneously adjusted by ASD and ADHD traits in addition to adjustments detailed in Model 1 (i.e., Y [child maltreatment] = β0 + β1*[psychiatric treatment history] + β2*[educational level] + β3*[ASD trait] + β4*[ADHD trait]); and Model 3 was simultaneously adjusted by ASD and ADHD traits and BIS/BAS in addition to the adjustments of Model 1 (i.e., Y [child maltreatment] = β0 + β1*[psychiatric treatment history] + β2*[educational level] + β3*[ASD trait] + β4*[ADHD trait] + β5*[BIS score] + β6*[BAS score]). The adjustment variables of Model 1 were determined via a history of psychiatric treatment theoretically associated with developmental traits and child maltreatment52,53,54,55 as per a previous study1. Multicollinearities of the linear regression models were estimated. The presence of multicollinearity was judged with a tolerance value and VIF (less than 0.4 and greater than 2.5, respectively)56. To investigate the validity of Model 3 for predicting moderate child maltreatment and severe child maltreatment, we performed two types of logistic regression analyses: Analyses 2 and 3.
Sub-analyses
Analysis 2: logistic regression analysis of Model 3 using the cut-off score for “at high risk of moderate child maltreatment” as the dependent variable
We used logistic regression analysis to determine if maternal impulsivity (BIS/BAS) was associated with moderate child maltreatment, adjusting for maternal psychiatric treatment history and educational level, ASD traits, and ADHD traits. The participants were classified into two groups, “at high risk of moderate child maltreatment” and “not at high risk of moderate child maltreatment,” by the cut-off score for “at risk of moderate child maltreatment” (2/3). A logistic regression was performed with the two groups as the dependent variables and with the same independent variables as that of Model 3 (i.e., maternal psychiatric treatment history, educational level, ASD traits, ADHD traits, behaviour inhibition system, and behaviour activation system). The sensitivity and specificity of the model were evaluated using the Youden’s Index.
Analysis 3: logistic regression analysis of Model 3 using the cut-off score for “at high risk of severe child maltreatment” as the dependent variable
Analysis 3 was performed to investigate if maternal impulsivity (BIS/BAS) was associated with severe child maltreatment, adjusting for ‘current or past psychiatric treatment history,’ education level, ASD traits, and ADHD traits. The participants were classified into two groups, “at high risk of severe child maltreatment” and “not at high risk of severe child maltreatment,” by the cut-off score for severe child maltreatment (6/7). As per Analysis 2, Analysis 3 was performed using the two groups with the cut-off score for “at high risk of severe child maltreatment” as the dependent variable. The variables with p values of 0.05 or less were considered as statistically significant for all analyses. Data analyses were conducted using JMP version 11.2 for Windows (SAS Inc., Tokyo, Japan).
References
Fujiwara, T., Kasahara, M., Tsujii, H. & Okuyama, M. Association of maternal developmental disorder traits with child mistreatment: a prospective study in Japan. Child Abuse Negl 38, 1283–1289, https://doi.org/10.1016/j.chiabu.2014.04.007 (2014).
American_Psychiatric_Association. Diagnostic and Statistical Manual of Mental Disorders, 5th Edition: DSM-5 (American Psychiatric Association, 2013).
Wiehe, V. R. Empathy and narcissism in a sample of child abuse perpetrators and a comparison sample of foster parents. Child abuse & neglect 27, 541–555 (2003).
Kimbrel, N. A., Mitchell, J. T., Hundt, N. E., Robertson, C. D. & Nelson-Gray, R. O. BIS and BAS interact with perceived parental affectionless control to predict personality disorder symptomatology. Journal of personality disorders 26, 203–212 (2012).
Newman, J. P. Reaction to punishment in extraverts and psychopaths: Implications for the impulsive behavior of disinhibited individuals. Journal of Research in Personality 21, 464–480 (1987).
Newman, J. P., Widom, C. S. & Nathan, S. Passive avoidance in syndromes of disinhibition: psychopathy and extraversion. Journal of personality and social psychology 48, 1316 (1985).
Wallace, J. F., Newman, J. P. & Bachorowski, J.-A. Failures of response modulation: Impulsive behavior in anxious and impulsive individuals. Journal of Research in Personality 25, 23–44 (1991).
Gray, J. A. The neuropsychology of emotion and personality (1987).
Gray, J. A. Perspectives on anxiety and impulsivity: A commentary. Journal of research in personality 21, 493–509 (1987).
Gray, J. A. The psychology of fear and stress. Vol. 5 (CUP Archive, 1987).
Gray, J. A. Brain systems that mediate both emotion and cognition. Cognition & Emotion 4, 269–288 (1990).
Gray, J. A. & McNaughton, N. The neuropsychology of anxiety: An enquiry into the function of the septo-hippocampal system (Oxford university press, 2003).
Fowles, D. C. The three arousal model: Implications of Gray’s two‐factor learning theory for heart rate, electrodermal activity, and psychopathy. Psychophysiology 17, 87–104 (1980).
Carver, C. S. & White, T. L. Behavioral inhibition, behavioral activation, and affective responses to impending reward and punishment: the BIS/BAS scales. Journal of personality and social psychology 67, 319 (1994).
Tokunaga, M. et al. Survey of child maltreatment among general population in Greater Tokyo. Kosei no Shihyo (in Japanese) 47, 3–10 (2000).
Mitsuda, N. et al. Predictive Value of Pregnant and Puerperal Women with Risks of Child Maltreatment. Report of the Ministry of Health, Labor and Welfare of Japan (H27-Sukoyaka-Ippan-001) (in Japanese) 5–57 (2015).
Adachi, J. et al. Reliability and validity of short version of Pervasive Developmental Disorders Autism Society Japan Rating Scale (PARS); a behavior checklist for people with PDD. Seishin Igaku (in Japanese) 50, 431–438 (2008).
Kessler, R. C. et al. The World Health Organization Adult ADHD Self-Report Scale (ASRS): a short screening scale for use in the general population. Psychological medicine 35, 245–256 (2005).
Takahashi, Y. et al. Gray’s temperament model: development of Japanese version of BIS/BAS scales and a behavior genetic investigation using the twin method. Japanese Journal of Personality (in Japanese) 15, 276–289 (2007).
Fallon, B. et al. Methodological challenges in measuring child maltreatment. Child abuse & neglect 34, 70–79 (2010).
Finkelhor, D., Ormrod, R., Turner, H. & Hamby, S. L. The victimization of children and youth: A comprehensive, national survey. Child maltreatment 10, 5–25 (2005).
Sidebotham, P., Golding, J. & Team, A. S. Child maltreatment in the “Children of the Nineties”: A longitudinal study of parental risk factors. Child abuse & neglect 25, 1177–1200 (2001).
Brown, J., Cohen, P., Johnson, J. G. & Salzinger, S. A longitudinal analysis of risk factors for child maltreatment: Findings of a 17-year prospective study of officially recorded and self-reported child abuse and neglect. Child abuse & neglect 22, 1065–1078 (1998).
Sidebotham, P., Heron, J. & Team, A. S. Child maltreatment in the “children of the nineties”: A cohort study of risk factors. Child Abuse & Neglect 30, 497–522 (2006).
Stith, S. M. et al. Risk factors in child maltreatment: A meta-analytic review of the literature. Aggression and violent behavior 14, 13–29 (2009).
Whipple, E. E. & Webster-Stratton, C. The role of parental stress in physically abusive families. Child abuse & neglect 15, 279–291 (1991).
Division of Local Medical Care, D. o. H. M., Osaka Prefectural Govermment. The Contact Sheet of the Information for Supporting Mothers with Psychosocial Problems http://www.pref.osaka.lg.jp/attach/3964/00016793/ninpuban.pdf (in Japanese) (2016).
Fujiwara, T., Sanpei, M. & Isumi, A. Research for detecting pregnant women with high risk of child abuse using pregnancy notification form Report of the Ministry of Health, Labor and Welfare of Japan (H27-Sukoyaka-Ippan-001) (in Japanese) 94–100 (2016).
Moeller, F. G., Barratt, E. S., Dougherty, D. M., Schmitz, J. M. & Swann, A. C. Psychiatric aspects of impulsivity. American journal of psychiatry 158, 1783–1793 (2001).
Palmen, A., Didden, R. & Lang, R. A systematic review of behavioral intervention research on adaptive skill building in high-functioning young adults with autism spectrum disorder. Research in Autism Spectrum Disorders 6, 602–617 (2012).
Wilens, T. E. et al. Cognitive therapy in the treatment of adults with ADHD: A systematic chart review of 26 cases. Journal of Cognitive Psychotherapy 13, 215–226 (1999).
Stanley, J. & Goddard, C. The effect of child abuse and other family violence on the child protection worker and case management. Australian Social Work 46, 3–10 (1993).
Murphy-Berman, V. A conceptual framework for thinking about risk assessment and case management in child protective service. Child abuse & neglect 18, 193–201 (1994).
Verdejo-García, A., Lawrence, A. J. & Clark, L. Impulsivity as a vulnerability marker for substance-use disorders: review of findings from high-risk research, problem gamblers and genetic association studies. Neuroscience & Biobehavioral Reviews 32, 777–810 (2008).
Jaffe, J. H. Drug addiction and drug abuse. The pharmacological basis of therapeutics 8, 522–573 (1990).
Volkow, N., Fowler, J., Wang, G., Baler, R. & Telang, F. Imaging dopamine’s role in drug abuse and addiction. Neuropharmacology 56, 3–8 (2009).
Ward, S. Population of Setagya Ward. Setagaya Ward Statistical Report (2013).
Setagaya_Ward. The Setagaya Ward Child Welfare Plan 2nd Phase and its new child welfare policy Setagaya Ward Child Welfare Plan: 2nd Phase (in Japanese) (2015).
Ito, H. et al. Validation of an interview-based rating scale developed in Japan for pervasive developmental disorders. Research in Autism Spectrum Disorders 6, 1265–1272 (2012).
Kamio, Y. et al. Checklist for behaviors on pervasive developmental disorder among adolescents and adults: Reliability and validity of the Pervasive Developmental Disorders Autism Society Japan Rating Scale (PARS). Seishin Igaku (in Japanese) 48, 1586–1590 (2006).
Lord, C., Rutter, M. & Le Couteur, A. Autism Diagnostic Interview-Revised: a revised version of a diagnostic interview for caregivers of individuals with possible pervasive developmental disorders. Journal of autism and developmental disorders 24, 659–685 (1994).
American_Psychiatric_Association. Diagnostic and Statistical Manual of Mental Disorders: Text Revision. (American Psychiatric Association, 2000).
Baron-Cohen, S., Wheelwright, S., Skinner, R., Martin, J. & Clubley, E. The autism-spectrum quotient (AQ): Evidence from asperger syndrome/high-functioning autism, malesand females, scientists and mathematicians. Journal of autism and developmental disorders 31, 5–17 (2001).
Koizumi, T., Tsujii, H. & Kasahara, M. Predictive factors for parenting difficulties in pregnancy periods. The proceeding of the 28th Annual Meeting of the Association of the Japanese Family Psychology (in Japanese) (2011).
Koizumi, T. et al. Predicting parenting difficuluties from pegnancy periods. The Proceedings of the 46th Annual Meeting of the Japan Society of Perinatal and Neonatal Medicine (in Japanese) (2010).
Kasahara, M., Tsujii, H. & Okuyama, M. Perinatal mental health and child abuse. Report of Research Development Grant for Child Health and Development from National Center for Child Health and Development (in Japanese) (2011).
Gray, J. A. A critique of Eysenck fs theory of personality. A model for personality 246–276 (1981).
Gray, J. A. The neuropsychology of anxiety: An enquiry into the functions of the septo-hippocampal system </i>. Behavioral and Brain Sciences 5, 469–484 (1982).
Watson, D. & Clark, L. A. Behavioral disinhibition versus constraint: A dispositional perspective. Handbook of mental control, Available at: http://works.bepress.com/david_watson/243/ New York (1993).
Beauchaine, T. P. & Neuhaus, E. Impulsivity and vulnerability to psychopathology. Child and adolescent psychopathology 129–156 (2008).
Newman, J. P., MacCoon, D. G., Vaughn, L. J. & Sadeh, N. Validating a distinction between primary and secondary psychopathy with measures of Gray’s BIS and BAS constructs. Journal of abnormal psychology 114, 319 (2005).
Lundström, S. et al. Autistic-like traits and their association with mental health problems in two nationwide twin cohorts of children and adults. Psychological Medicine 41, 2423–2433 (2011).
May, T., Rinehart, N., Wilding, J. & Cornish, K. The role of attention in the academic attainment of children with autism spectrum disorder. Journal of autism and developmental disorders 43, 2147–2158 (2013).
Simonoff, E. et al. The persistence and stability of psychiatric problems in adolescents with autism spectrum disorders. Journal of Child Psychology and Psychiatry 54, 186–194 (2013).
Sizoo, B. et al. Treatment seeking adults with autism or ADHD and co-morbid substance use disorder: prevalence, risk factors and functional disability. Drug and alcohol dependence 107, 44–50 (2010).
Allison, P. Logistic regression using the SAS system: theory and application. SAS Institute, Cary, NC, 167–168 (1999).
Acknowledgements
This study was supported by Grant-in-Aid for Scientific Research from the Ministry of Health, Labour, and Welfare of Japan (H24-Jisedai-Shitei-006, H25-Seisin-Wakate-013, H28-Sukoyaka-Ippan-005, and H29-Sukoyaka-Ippan-004), the Ministry of Education, Culture, Sports, Science, and Technology (Wakate B 312268). We would like to thank Dr. Julian Tang of the Department of Education for Clinical Research, National Centre for Child Health and Development, for proofreading, editing and writing part of this manuscript.
Author information
Authors and Affiliations
Contributions
Y.T., T. Kubo, R.M., and K.T. conceived and designed the experiments. K.T. and N.K. managed the data acquisitions. Y.T. analysed the data with supports by M.M., E.I., and E.O. Y.T. wrote the paper. M.O. and T. Koizumi supported the development of this study design from the viewpoints of experts.
Corresponding author
Ethics declarations
Competing Interests
The authors declare that they have no competing interests.
Additional information
Publisher's note: Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made. The images or other third party material in this article are included in the article’s Creative Commons license, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons license and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this license, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Tachibana, Y., Takehara, K., Kakee, N. et al. Maternal impulse control disability and developmental disorder traits are risk factors for child maltreatment. Sci Rep 7, 15565 (2017). https://doi.org/10.1038/s41598-017-14666-5
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41598-017-14666-5
This article is cited by
-
An integrated community mental healthcare program to reduce suicidal ideation and improve maternal mental health during the postnatal period: the findings from the Nagano trial
BMC Psychiatry (2020)
-
ERP study on the associations of peripheral oxytocin and prolactin with inhibitory processes involving emotional distraction
Journal of Physiological Anthropology (2019)
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.