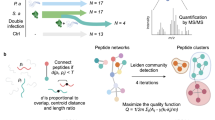
Abstract
The disease burden of failing skin repair and non-healing ulcers is extensive. There is an unmet need for new diagnostic approaches to better predict healing activity and wound infection. Uncontrolled and excessive protease activity, of endogenous or bacterial origin, has been described as a major contributor to wound healing impairments. Proteolytic peptide patterns could therefore correlate and “report” healing activity and infection. This work describes a proof of principle delineating a strategy by which peptides from a selected protein, human thrombin, are detected and attributed to proteolytic actions. With a particular focus on thrombin-derived C-terminal peptides (TCP), we show that distinct peptide patterns are generated in vitro by the human S1 peptidases human neutrophil elastase and cathepsin G, and the bacterial M4 peptidases Pseudomonas aeruginosa elastase and Staphylococcus aureus aureolysin, respectively. Corresponding peptide sequences were identified in wound fluids from acute and non-healing ulcers, and notably, one peptide, FYT21 (FYTHVFRLKKWIQKVIDQFGE), was only present in wound fluid from non-healing ulcers colonized by P. aeruginosa and S. aureus. Our result is a proof of principle pointing at the possibility of defining peptide biomarkers reporting distinct proteolytic activities, of potential implication for improved diagnosis of wound healing and infection.
Similar content being viewed by others
Introduction
Conditions, such as arterial and venous insufficiency, diabetes, or excessive pressure all predispose to the formation of non-healing ulcers. In the United States alone, about 6.5 million have chronic skin ulcers1. The economic burden on the healthcare system and on society due to failing skin repair and non-healing ulcers is extensive2. In diabetic patients, these ulcers are the leading cause (85%) of all major lower limb amputations, inflicting significant pain and reducing quality of life for patients3. With a growing diabetic population, chronic wounds affect millions of people, with high morbidity and mortality rates, emerging as a serious threat to healthcare systems around the world4. Furthermore, complications of slow or non-healing wounds also affect burn victims. In the United States alone, more than 1.25 million people per year suffer from burns, where local infections cause delayed healing and risk for invasive infections and sepsis. Also notable is that a significant part of hospital antibiotics consumption is related to postoperative prophylaxis, and the costs for postoperative infections are high.
Standard wound diagnostic procedures usually involve clinical evaluations and sometimes bacteriological identification5. Occurrence of multidrug resistant microorganisms has further complicated the wound diagnostic procedures and treatment options. In addition, the management of drug resistant microorganisms is in an urgent need for better treatment options6,7. Early diagnosis paired with prompt and effective therapeutic interventions in case of infection risk may lead to better treatments targeting the causes of wounds, as well as reduction of wound infections. Clearly, there is an unmet need for improved diagnostic approaches in order to better predict healing activity and infection in non-healing wounds.
Non-healing ulcers are characterized by the presence of an elevated level of proteases, both endogenous and of bacterial origin, which disrupts the delicate balance between acute inflammation and progression of wound healing8. Consequently, these wounds are often characterized by high inflammatory activity, excessive proteolytic processing of matrix molecules and immune mediators and impaired wound closure9,10,11. Hemostasis is the initial phase of wound healing and commences with the formation of active thrombin which in turn, mediates fibrin clot formation as well as pro-inflammatory and chemotactic effects12,13. We have previously demonstrated that proteolysis of thrombin generates host defense peptides (HDPs), particularly derived from the C-terminal part of the molecule14. These thrombin-derived C-terminal peptides (TCPs) bind to bacterial lipopolysaccharide (LPS) and display both anti-microbial and anti-inflammatory activities in vitro, with therapeutic potential against infection and septic shock in vivo 15,16. Interestingly, we found that Pseudomonas aeruginosa may mimic the formation of such HDPs, leading to generation of anti-inflammatory peptides and circumvention of host responses17. In a recent report, we also demonstrated a previously undisclosed role of larger TCPs of about 11 kDa, involving LPS- and bacteria-induced aggregation and scavenging, facilitating clearance and microbial killing18.
Previous studies have mostly dealt with identification of major HDPs of thrombin from a structural, functional, and therapeutic perspective. However, wound fluid proteolytic products, including TCPs, may also serve as a “window” into the wound microenvironment. We therefore hypothesized that the peptide profile could reflect the action of different proteases present in wounds. However, the complexity of such peptide systems, and lack of efficient analytic tools, until recently has hampered their clinical exploitation and use. Here, we set out to define cleaved thrombin fragments generated by both endogenous and bacterial proteases. Our results show that cleavage of thrombin by human and bacterial proteases yields unique peptide patterns. Multiple fragments of TCPs, generated by both human neutrophil and bacterial proteases were identified, and similar TCPs were found in human wound fluid obtained from sterile as well as infected wounds. Taken together, our study demonstrates a proof of principle of the feasibility for defining peptide biomarkers that “report” on distinct protease activities in vivo.
Results
Degradation of thrombin by endogenous human proteinases in vitro
Thrombin susceptibility to endogenous human proteases secreted by neutrophils during wounding was assessed by analyzing the in vitro peptide patterns generated by human neutrophil elastase (HNE) and cathepsin G (HCG). Both HNE and HCG cleaved thrombin completely, generating a large number of fragments (157 and 129 peptides respectively) as evident from the SDS-PAGE and mass spectrometric analysis (Figure S1). Peptide sequence comparisons of the LC-MS/MS data identified distinct TCPs, indicating that HNE and HCG cleave thrombin specifically, with low overlap (Fig. 1 and Figure S4). Furthermore, co-incubation of thrombin with HNE and HCG simultaneously did not yield additional common peptide fragments (Figure S2). Interestingly, the peptide HVF18 (HVFRLKKWIQKVIDQFGE), a fragment having anti-endotoxic effects was identified in the peptide products of HNE and HCG, both S1 peptidases (Table 1). The results support earlier reports that HNE cleaves thrombin to release bioactive thrombin-derived peptides19,20 including HVF1814.
Proteolytic digestion of thrombin by human proteases. (a) Western blot analysis of human α-thrombin digested with human neutrophil elastase (HNE) and human cathepsin G (HCG). The samples were incubated for the indicated time periods at an enzyme: substrate ratio of 1:30 (w/w) and antibody against the C-terminal part of thrombin was used for visualization. Thrombin (incubated for 0 and 180 minutes) and the synthetic thrombin C-terminal peptide HVF18 were loaded as control. (b) A Venn-diagram representing the LC-MS/MS identified unique and overlapping (purple) TCP peptide sequences generated by HNE (red) and HCG (green) in an experimental repeat of three.
Degradation of thrombin by bacterial proteinases in vitro
Next, we analysed the thrombin peptides generated by bacterial proteinases such as elastase of the Gram-negative Pseudomonas aeruginosa, and aureolysin and V8 proteases of the Gram-positive Staphylococcus aureus, two bacteria commonly found in non-healing ulcers and infected burn wounds (Figure S3). As seen in Fig. 2, P. aeruginosa elastase (PAE) generates a 21 amino acid TCP, FYT21 (FYTHVFRLKKWIQKVIDQFGE), reported recently to inhibit host inflammatory responses17. Notably, FYT21 was also found to be generated by S. aureus aureolysin (ALYS), a metalloproteinase like P. aeruginosa elastase (Fig. 2 and Table 1). Peptides generated by V8 were mainly of high molecular weight, in comparison to those generated by PAE and ALYS, possibly reflecting the limited specificity of the protease for anionic residues (D/E) at the P1 position (Figure S4). Hence, a limited number of TCPs were identified after V8 digestion (Figure S3). Taken together, similar to the findings with HNE and HCG, the results indicate that bacterial proteases cleave thrombin distinctly, yielding unique peptide patterns (Fig. 3). Notably, the TCPs HVF18 and FYT21 were identified as unique products of human and bacterial protease activity, respectively (Fig. 3 and Table 1). Figure 4 illustrates the obtained cleavage sites by the respective proteases as shown in a 3D model of thrombin (panel A), as well as indicated in the amino acid sequence (panel B). The side chain dispositions of cleavage sites, as highlighted in the 3D model, indicates that the majority of cleavage sites for both bacterial and human proteases are situated on the exterior surface of thrombin.
Bacterial proteases cleave human thrombin. (a) Western blot analysis of human α-thrombin digested with P. aeruginosa elastase (PAE), S. aureus aureolysin (ALYS) and V8 protease, incubated at 37 °C for 3 and 6 hours. Thrombin incubated for 6 hours and the synthetic peptide FYT21 were loaded as control. PAE western blot is shown at exposure time of 20 secs while the V8/ALYS blot is at 8secs. The V8/ALYS western blot at exposure time of 20 secs is provided in the supplementary information S3. (b) A Venn-diagram comparing the LC-MS/MS identified TCPs produced by bacterial proteases PAE (blue), ALYS (brown) and V8 (magenta) in an experimental repeat of three, highlights unique and overlapping peptide sequences (black and orange).
Human and bacterial proteases cleave thrombin to generate unique peptide patterns. (a) Comparison of TCPs obtained combining peptides generated by human proteases (HNE and HCG) and bacterial proteases (PAE, ALYS, and V8) highlighting HVF18 and FYT21 as unique products of digestion by human and bacterial protease, respectively. (b) 3D structure of thrombin highlighting the neutrophil elastase-cleaved thrombin C-terminal peptide fragment HVF18 (blue) and the P. aeruginosa elastase-generated peptide FYT21 (green). (c) MS/MS spectrum of the respective protease generated peptides HVF18 and FYT21.
Illustration of protease cleavage sites in human thrombin. (a) 3D model showing cleavage sites of human and bacterial proteases highlighting the exterior disposition of enzyme recognition sites in thrombin. (b) Color-coded 2D representation of the protease cleavage sites indicating similarities and differences between the human and bacterial proteases.
Thrombin-derived peptides are identified in human wound fluids
In order to identify TCPs present in human wounds, wound fluids from acute surgical wounds and chronic ulcers co-infected with P. aeruginosa and S. aureus were incubated with thrombin C-terminal antibody-coated dynabeads to pull-down TCPs, followed by mass spectrometry analysis. Comparison of the in vitro generated peptides and the fragments detected in vivo showed the presence of multiple fragments of TCPs in both acute wound fluids (AWF) and chronic wound fluids (CWF) (Fig. 5 and Table 2). The peptides HVF18 and FYT21, products of human and bacterial proteases respectively, were identified in wound fluid from non-healing ulcers, while the peptides FRL16 (FRLKKWIQKVIDQFGE), LKK14 (LKKWIQKVIDQFGE), KKW13 (KKWIQKVIDQFGE) and KWI12 (KWIQKVIDQFGE), and other truncated fragments were common in wound fluids from both acute wounds and non-healing ulcers (Fig. 5 and Table 2).
Comparison of in vitro and in vivo generated thrombin C-terminal fragments. A Venn-diagram showing TCPs generated by (a) human proteases and (b) bacterial proteases found in human wound fluids from acute wounds (AWF) and non-healing ulcers (CWF). Overlapping peptides identified in wound fluid are indicated by a yellow arrow. HVF18 and FYT21 sequence is bolded. (c) MS/MS spectrum of protease generated truncated TCPs FRL16, LKK14, KKW13, and KWI12 found in the wound fluid.
Discussion
The main finding of this work is the definition of multiple fragments of TCPs which are generated by both human and bacterial proteases. Furthermore, the work shows a proof of principle that it may be technically possible to define peptides “reporting” distinct proteolytic activity patterns not only in vitro, but also in vivo. As protease activity is so fundamentally linked to the healing status of wounds9 as well as the presence of protease-producing bacteria, the work thus points at the future possibility of using peptides as biomarkers in the development of advanced wound and infection diagnostics - based on mass spectrometry technologies, antibody arrays, or other sensor-based technologies.
As mentioned in the introduction, today’s measures in the clinic to assess a wound and define whether it is infected or not, mainly depend on the clinician’s evaluation. In general practice, if there is a suspected infection, a microbiological swab is taken before antibiotics are given to the patient. It is notable that most wound swabs are prone to false positives as most will yield bacterial growth which is not always due to infection. For example, over 90% of non-healing ulcers are colonized by staphylococci - even without infection. The clinical evaluation of infection today is based on obvious signs of infection including redness, heat, swelling, purulent exudate, smell, pain, systemic illness, and the presence of fistulas, “foamy” granulation tissue, or tissue breakdown. The challenge is to detect infection before it reaches this stage.
Alternate methods to swab technique for detecting bacterial infection are based on looking at products from bacteria, or the host, or determining host responses that can report the presence of infection. At current, some developments are directed to the identification of a variety of biochemical by-products. For example, pyocyanin—the blue–green pigment secreted by many P. aeruginosa strains, has been used to detect bacteria21. Urate or uric acid is another metabolite found within wounds, which may be used as a diagnostic marker. The problem here is that bacteria may metabolize urate. Toxins produced by bacteria found in wounds may be used to trigger a sensor output indicating early infection. For example, Zhou et al. developed Trojan-like phospholipid vesicles, which release a fluorescent dye cargo when subjected to bacterial toxins22,23. Of relevance to this study is that HNE and HCG have recently been reported as early stage warning markers for non-healing ulcers24. The enzymatic nature of HNE and HCG has indeed been used to produce a sensor made from a chromophore linked by a short peptide sequence susceptible to cleavage by each of the enzymes. For example, Edwards et al. used cellulose-AP-suc-Ala-Ala-Pro-Ala-pNA substrates25. Rimmer et al. developed a method for binding either Gram-positive or Gram-negative bacteria to a polymer which alters shape upon binding and has potential as a bacterial sensor26,27. Matrix metalloproteinases (MMPs) are increased in chronic wound fluid (CWF). Gao et al. sensed MMP-2 at concentrations as low as 0.1 ng/mL by spin-coating a gelatin film on top of a pSi resonator28. Upon contact with MMP-2, the film was degraded and the generated peptides were able to enter the pores and induced color changes that could be detected by the eye.
Other researchers are focusing on protein patterns, and identification of the total proteome of wounds has been suggested as one method to obtain not only information of the pathogenesis, but also to be able to define specific protein biomarkers discriminating between various wound types29,30,31. For example, Eming et al. demonstrated the differential distribution of tissue repair proteins in exudates of healing wounds and persistent inflammatory tissue damaging mediators in non-healing wounds24. Upton’s group has established enhanced proteomics workflow to reduce sample complexity by selective depletion of high abundant protein, validating detection of proteins present in low concentrations in chronic wound fluids32. Auf dem Keller et al. applied quantitative proteomics strategies to dissect proteolytic pathways in healthy and diseased skin. In a global approach, they analysed wound fluids from a porcine vacuum assisted closure (VAC) wound models and quantitatively assessed the wound proteome and the activity of distinct protease groups along the healing process33. They also mapped proteolytic pathways in vivo and established protease-substrate relations that will help to better understand protease action in cutaneous wound repair34. Considering the above, it is of note that many approaches are based on detection of products such as pyocyanin, toxins, or proteases. Methods for detection of down-stream products reflecting inflammation are rare. Of note is that auf dem Keller´s work involves studies on such protease patterns. However, as their method focuses on “N-terminomics”, low molecular weight peptides are mainly lost during the preparation steps. Notable are also recent developments, where a labelling approach35 using trimethoxyphenyl phosphonium (TMPP) allows characterization of both N-terminal and internal digestion peptides.
Whether the here reported method based on peptide detection will reach a sufficient sensitivity and specificity in order to be of diagnostic use has to be evaluated in future studies. For example, although a recently developed assay, Woundchek™ was shown to have a good sensitivity for detection of HNE and MMP levels, the predictive potential of protease measurements for various wound pathologies, although showing promising results36, needs further clinical studies. From this perspective, it is therefore of note that some peptide fragments were only produced by bacterial enzymes, such as the TCP FYT21. Hence, using peptide markers that are unique for bacteria should enable a high specificity, since such peptides should not be detected at all in sterile wounds. An important factor to address in future studies, of importance for evaluating the diagnostic utility of FYT21 and related fragments, is their stability and half-life in vivo. Of interest is that recent work by Böttger et al.37 showed peptides with differing cleavage sites exhibited variable proteolytic sensitivities in blood, serum, and plasma. Therefore, future developments aiming at defining peptides as biomarkers must be preceeded by a careful analysis of their potential degradation (e.g. using isotope-labelled peptides), particularly in relevant environments, such as wound fluids from acute or chronic wounds.
It is also of note that P. aeruginosa elastase belongs to a superfamily of zinc-containing metallopeptidases of the M4 (thermolysin) class, also secreted from bacteria such as Enterococcus faecalis (coccolysin) and S. aureus (aureolysin), bacteria very common in chronic wounds. The present findings confirmed the presence of FYT21 after digestion with P. aeruginosa elastase, as previously communicated17. Interestingly, we also detected the peptide after digestion with aureolysin, another staphylococcal proteinase of the M4 peptidase group. Hence, it is tempting to speculate that formation of FYT21 could be common for many M4 peptidase-producing bacteria. If so, such peptide markers may reflect bacterial actions more than the presence of bacteria per se, which from a physiological point of view should correlate better to overall bacterial load and actions, and ultimately also, the clinical status of a particular wound. Hypothetically, combining the use of specific, qualitative, peptide markers, such as the ones reported here, with Woundchek™-based analyses of HNE and MMPs or other related more quantitative approaches, could be an attractive strategy in order to attain a higher diagnostic sensitivity and specificity with respect to wound status. These evaluations in turn, could be complemented with sensitive bacterial detection methods, such as the ones mentioned above, which altogether should provide a “multi-dimensional” analysis of wound status, enabling simultaneous determination of bacteria per se, host proteolytic activities, as well as down-stream specific peptides reporting actions of host or bacterial proteases. Clearly, clinical prospective studies on larger patient groups, where bacterial types and loads, and wound proteolysis levels, are determined and correlated with the occurrence of the herein defined peptide patterns, are mandated in order to fully investigate such potential diagnostic possibilities.
From a biological perspective, our findings also illustrate the multi-functionality of thrombin. Being a major enzyme of the coagulation cascade, thrombin acts as a procoagulant converting soluble fibrinogen into insoluble fibrin to initiate wound repair. However, the biological function of thrombin expands beyond blood coagulation, as the enzyme triggers endothelial cell activation, increased adhesion of neutrophils to the endothelium38, platelet aggregation and chemotaxis of neutrophils39 and the induction of cytokine release from epithelial and endothelial cells32,40,41 through proteolytically activated receptors (PAR1, PAR3 or PAR4). Next, intermediate-sized TCPs similar to the B4 chain of γ-thrombin are subsequently formed, enabling aggregation and phagocytosis of bacteria18. Finally, small TCPs, such as FYT21 and HVF18, generated by proteolysis can block pro-inflammatory cytokine responses via binding to LPS. Apart from these fragments, our data shows that a multitude of truncated TCP variants seem to be generated, and it is tempting to speculate that such forms could have additional biological functions, or work in synergy with larger TCP fragments. In this context, it is interesting that other bioactive thrombin-related fragments, such as the peptides ELLESYIDGR and TATSEYQTFFNPR, are identified in platelet rich plasma extracts and promote angiogenesis and wound healing in vitro 42, findings exploited in the design of hybrid peptides for improved wound healing in vivo 42,43. Another peptide, AGYKPDEGKRGDACEGDSGGPFV, derived from the receptor-binding part of thrombin accelerates wound repair44. Notable is that we identified truncated forms related to the ELLESYIDGR sequence in our in vitro protease digests, whereas the sequence AGYKPDEGKRGDACEGDSGGPFV was included in longer fragments produced in vitro by HNE and ALYS (Table S4). Hence, looking beyond TCPs, it is also possible that future detailed analyses of other thrombin sequences could provide interesting clues to possible relationships between levels of such peptides in wounds and different wound healing states. Taken together, the current report, here mainly focusing on TCPs, is a proof of principle showing that unique peptide patterns can be used for definition of protease actions, of possible use in future diagnostic developments.
Materials and Methods
Peptides and proteins
Thrombin was from Innovative Research, USA. The peptides FYT21 (FYTHVFRLKKWIQKVIDQFGE) and HVF18 (HVFRLKKWIQKVIDQFGE), were synthesized by Biopeptide (San Diego, CA). The purity of these peptides (>95%) was confirmed with MALDI-TOF MS. The endoproteinases, human neutrophil elastase and cathepsin G were from Calbiochem, USA. V8 Glu-C endoproteinase was obtained from Roche, aureolysin from BioCol, and P. aeruginosa elastase (PAE) was purified as previously described with some modifications45.
Biological materials
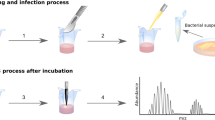
Wound fluids from non-healing venous ulcers co-infected with P. aeruginosa and S. aureus were collected under a Tegaderm dressing for 2 hours as reported earlier46. Bacteria were identified by routine bacteriological methods from swabs from the wound surface. The patients were not treated with antibiotics. Sterile wound fluids were obtained from surgical drainages after mastectomy. Collection was for 24 to 48 hours after surgery. Wound fluids were centrifuged, aliquoted and stored at −20 °C. The use of human wound fluids was approved by the Ethics Committee at Lund University (LU 708-01 and LU 509-01). All experimental methods were performed in compliance to the guidelines and regulations of the Ethics Committee at Lund University, Lund Sweden with written informed consent from all participants.
Digestion by human proteases in vitro
Thrombin (4 μg–15 μg) was incubated with either human neutrophil elastase (HNE) or human neutrophil cathepsin G (HCG) at an enzyme-substrate ratio of 1:30 (w/w) in 10 mM Tris, pH 7.4 (volume of 10 μl) at 37 °C for variable time points (30, 60 and 180 minutes). The enzyme activity was blocked after the incubation by heating the samples at 95 °C for 3 minutes and further analysed by Tricine SDS-PAGE. The in vitro digestion analysis was performed in triplicates.
In vitro digestion by bacterial proteases
Thrombin (4 μg–15 μg) was incubated at 37 °C with either V8 protease (0.2 μg/μg of thrombin), aureolysin (0.2 μg/μg of thrombin) or PAE (4 mU/μg of thrombin) separately in 10 mM NH4HCO3 (pH 7.8), 10 mM Tris containing 5 mM CaCl2 (pH 7.8) and 10 mM Tris (pH 7.4) respectively in a total volume of 10 μl for 3 hours and 6 hours. The enzyme activity was blocked by heating the sample at 95 °C for 3 minutes and analysed by Tricine SDS-PAGE. Digestion analysis was performed in triplicates.
SDS-PAGE and silver staining
Seven μl of Novex sample buffer was added to each sample, and heated at 95 °C for 10 minutes. The peptides, FYT21 and HVF18 were loaded for comparison. The samples were analysed by SDS-PAGE using a 10–20% Novex Tricine pre-cast gel run at 90 V, for 2 hours. The gel was stained with a Pierce™ Silver Stain Kit according to the manufacturer’s protocol.
Immunoblotting
Immediately following SDS-gel electrophoresis, the gels were assembled into the blot module (Invitrogen) based on the manufacturer’s protocol. The transfer was performed at 25 V for 90 minutes on ice. After the transfer, the PVDF membranes were blocked with 5% milk for an hour, followed by overnight incubation of polyclonal antibodies recognizing the peptide VFR17 (VFRLKKWIQKVIDQFGE) to a 1:5000 dilution at 4 °C. The membranes were washed 3 times for 10 minutes and incubated with HRP-conjugated secondary antibodies (Dako) at 1:10000 dilutions for an hour. The membranes were washed 3 times for 10 minutes. The C-terminal thrombin fragments were detected by SuperSignal West Dura Extended Duration Substrate (ThermoFisher Scientific, USA) for 5 minutes and thereafter imaged using a gel documentation system (Gel Doc XR + System).
LC-MS/MS and data analysis
After in vitro enzymatic digestion of thrombin, the reaction was stopped by acidifying the samples. The peptides were then dried and reconstituted in 0.1% formic acid (FA). Peptides were separated and analysed on a Dionex Ultimate 3000 RSLC nanoLC system coupled to a Q-Exactive tandem mass spectrometer (Thermo Fisher, MA). Five μl of sample was injected into an acclaim peptide trap column via the auto-sampler of the Dionex RSLC nanoLC system. Flow rate was at 300 nl/min, and mobile phase A (0.1% FA in 5% acetonitrile) and mobile phase B (0.1% FA in acetonitrile) were used to establish a 60 minute gradient. Peptides were analysed on a Dionex EASY-spray column (PepMap® C18, 3um, 100 A) using an EASY nanospray source. An electrospray potential was set at 1.5 kV. A full MS scan (350–1600 m/z range) was acquired at a resolution of 70000 at m/z 200, with a maximum ion accumulation time of 100 ms. Dynamic exclusion was set to 30 seconds. Resolution for MS/MS spectra was set to 35,000 at m/z 200. The AGC setting was 1E6 for the full MS scan and 2E5 for the MS2 scan. The 10 most intense ions above a 1000 count threshold were chosen for HCD fragmentation, with a maximum ion accumulation time of 120 milliseconds. An isolation width of 2 Da was used for the MS2 scan. Single and unassigned charged ions were excluded from MS/MS. For HCD, normalized collision energy was set to 28. The underfill ratio was defined as 0.1%. Raw data files were converted into the mascot generic file format using Proteome Discoverer version 1.4 (Thermo Electron, Bremen, Germany) with the MS2 spectrum processor for de-isotoping the MS/MS spectra. The concatenated target-decoy UniProt human database (total sequences 92867, total residues 36953354, downloaded on 25 July 2016) was used for data searches. Database search was performed with non-enzyme option using an in-house Mascot server (version 2.4.1, Matrix Science, Boston, MA). Oxidation (M) and deamidation (N and Q) were kept as variable modifications. A total of three samples with two technical replicates (3 × 2) for each in vitro digest were analysed by LC-MS/MS. The identified peptides were then sorted on the peptide score and hits with <30 were omitted from analyses. Peptide hits consistently identified in all experimental and technical replicates were considered for qualitative comparison between in vitro and in vivo samples.
Pull-down of thrombin C-terminal peptides from wound fluids
Dyanbeads M-280 sheep anti-rabbit IgG (Novex Life Technologies) were used according to the manufacturer’s instructions and as per the methods described earlier17. Briefly, 100 μl of dynabeads pre-coated with sheep anti rabbit IgG antibodies were coupled with rabbit polyclonal antibodies (50 μl) recognizing the peptide sequence VFR17 (VFRLKKWIQKVIDQFGE) (Innovagen, Lund, Sweden) by incubation overnight at 4 °C. The coated dynabeads were subsequently washed according to the manufacturer´s protocol and incubated with 100 μl of AWF and/or CWF for 1 hour at RT, which was followed by elution with 20 μl of citric acid monohydrate (100 mM, pH 2).
Mass spectrometry analysis of wound fluid
Acute (AWF) and chronic wound fluids (CWF) from two patients each (n = 2 for AWF and CWF) were utilised in this study. Wound fluid samples were acidified and analysed by online nanoflow liquid chromatography coupled to tandem mass spectrometry (LC-MS/MS). LC-MS/MS experiments were performed on an EASY-nLC system (Thermo Scientific) connected to a LTQ orbitrap Velos Pro (Thermo Scientific) through a nanoelectrospray ion source and analysed as described earlier17.
Data availability
All data generated or analysed during this study are included in this published article (and its Supplementary Information files). The mass spectrometry proteomics data have been deposited to the ProteomeXchange47 Consortium via the PRIDE48 partner repository with the dataset identifier PXD006992.
References
Brigham, P. A. & McLoughlin, E. Burn incidence and medical care use in the United States: estimate, trends, and data sources. The Journal of Burn Care and Rehabilitation 17, 95–107 (1996).
Singer, A. J. & Clark, R. A. Cutaneous wound healing. The New England journal of medicine 341, 738–746, https://doi.org/10.1056/NEJM199909023411006 (1999).
Vinh, D. C. & Embil, J. M. Rapidly progressive soft tissue infections. The Lancet. Infectious diseases 5, 501–513, https://doi.org/10.1016/S1473-3099(05)70191-2 (2005).
Chen, W. Y. & Rogers, A. A. Recent insights into the causes of chronic leg ulceration in venous diseases and implications on other types of chronic wounds. Wound repair and regeneration: official publication of the Wound Healing Society [and] the European Tissue Repair Society 15, 434–449, https://doi.org/10.1111/j.1524-475X.2007.00250.x (2007).
Giacometti, A. et al. Epidemiology and microbiology of surgical wound infections. Journal of clinical microbiology 38, 918–922 (2000).
Neu, H. C. The crisis in antibiotic resistance. Science 257, 1064–1073 (1992).
Taubes, G. The bacteria fight back. Science 321, 356–361, https://doi.org/10.1126/science.321.5887.356 (2008).
Trengove, N. J. et al. Analysis of the acute and chronic wound environments: the role of proteases and their inhibitors. Wound repair and regeneration: official publication of the Wound Healing Society [and] the European Tissue Repair Society 7, 442–452 (1999).
Agren, M. S. et al. Causes and effects of the chronic inflammation in venous leg ulcers. Acta dermato-venereologica. Supplementum 210, 3–17 (2000).
Herrick, S. et al. Up-regulation of elastase in acute wounds of healthy aged humans and chronic venous leg ulcers are associated with matrix degradation. Laboratory investigation; a journal of technical methods and pathology 77, 281–288 (1997).
Yager, D. R. & Nwomeh, B. C. The proteolytic environment of chronic wounds. Wound repair and regeneration: official publication of the Wound Healing Society [and] the European Tissue Repair Society 7, 433–441 (1999).
Chen, L. B. & Buchanan, J. M. Mitogenic activity of blood components. I. Thrombin and prothrombin. Proceedings of the National Academy of Sciences of the United States of America 72, 131–135 (1975).
Carney, D. H. & Cunningham, D. D. Role of specific cell surface receptors in thrombin-stimulated cell division. Cell 15, 1341–1349 (1978).
Papareddy, P. et al. Proteolysis of human thrombin generates novel host defense peptides. PLoS pathogens 6, e1000857, https://doi.org/10.1371/journal.ppat.1000857 (2010).
Kalle, M. et al. Host defense peptides of thrombin modulate inflammation and coagulation in endotoxin-mediated shock and Pseudomonas aeruginosa sepsis. PloS one 7, e51313, https://doi.org/10.1371/journal.pone.0051313 (2012).
Hansen, F. C. et al. The Thrombin-Derived Host Defense Peptide GKY25 Inhibits Endotoxin-Induced Responses through Interactions with Lipopolysaccharide and Macrophages/Monocytes. Journal of immunology 194, 5397–5406, https://doi.org/10.4049/jimmunol.1403009 (2015).
van der Plas, M. J. et al. Pseudomonas aeruginosa elastase cleaves a C-terminal peptide from human thrombin that inhibits host inflammatory responses. Nature communications 7, 11567, https://doi.org/10.1038/ncomms11567 (2016).
Petrlova, J. et al. Aggregation of thrombin-derived C-terminal fragments - a novel host defense mechanism. PNAS in press (2017).
Brower, M. S., Walz, D. A., Garry, K. E. & Fenton, J. W. 2nd Human neutrophil elastase alters human alpha-thrombin function: limited proteolysis near the gamma-cleavage site results in decreased fibrinogen clotting and platelet-stimulatory activity. Blood 69, 813–819 (1987).
Bar-Shavit, R. et al. An Arg-Gly-Asp sequence within thrombin promotes endothelial cell adhesion. The Journal of cell biology 112, 335–344 (1991).
Sharp, D., Gladstone, P., Smith, R. B., Forsythe, S. & Davis, J. Approaching intelligent infection diagnostics: Carbon fibre sensor for electrochemical pyocyanin detection. Bioelectrochemistry 77, 114–119, https://doi.org/10.1016/j.bioelechem.2009.07.008 (2010).
Zhou, J., Loftus, A. L., Mulley, G. & Jenkins, A. T. A thin film detection/response system for pathogenic bacteria. Journal of the American Chemical Society 132, 6566–6570, https://doi.org/10.1021/ja101554a (2010).
Zhou, J. et al. Development of a prototype wound dressing technology which can detect and report colonization by pathogenic bacteria. Biosensors & bioelectronics 30, 67–72, https://doi.org/10.1016/j.bios.2011.08.028 (2011).
Eming, S. A. et al. Differential proteomic analysis distinguishes tissue repair biomarker signatures in wound exudates obtained from normal healing and chronic wounds. Journal of proteome research 9, 4758–4766, https://doi.org/10.1021/pr100456d (2010).
Edwards, J. V., Caston-Pierre, S., Howley, P. S., Condon, B. D. & Arnold, J. W. A Bio-Sensor for Human Neutrophil Elastase Employs A Bio-Sensor for Human Neutrophil Elastase Employs Peptide-p-nitroanilide Cellulose Conjugates. Sensor Letters 6, 518–523 (2008).
Sarker, P. et al. Highly branched polymers with polymyxin end groups responsive to Pseudomonas aeruginosa. Biomacromolecules 12, 1–5, https://doi.org/10.1021/bm100922j (2011).
Shepherd, J. et al. Binding bacteria to highly branched poly(N-isopropyl acrylamide) modified with vancomycin induces the coil-to-globule transition. Journal of the American Chemical Society 132, 1736–1737, https://doi.org/10.1021/ja907466y (2010).
Gao, L., Mbonu, N., Cao, L. & Gao, D. Label-free colorimetric detection of gelatinases on nanoporous silicon photonic films. Analytical chemistry 80, 1468–1473, https://doi.org/10.1021/ac701870y (2008).
Cravatt, B. F., Simon, G. M. & Yates, J. R. 3rd The biological impact of mass-spectrometry-based proteomics. Nature 450, 991–1000, https://doi.org/10.1038/nature06525 (2007).
Broadbent, J., Walsh, T. & Upton, Z. Proteomics in chronic wound research: potentials in healing and health. Proteomics. Clinical applications 4, 204–214, https://doi.org/10.1002/prca.200900152 (2010).
Yager, D. R., Zhang, L. Y., Liang, H. X., Diegelmann, R. F. & Cohen, I. K. Wound fluids from human pressure ulcers contain elevated matrix metalloproteinase levels and activity compared to surgical wound fluids. The Journal of investigative dermatology 107, 743–748 (1996).
Kranzhofer, R. et al. Thrombin potently stimulates cytokine production in human vascular smooth muscle cells but not in mononuclear phagocytes. Circulation research 79, 286–294 (1996).
Sabino, F. et al. In vivo assessment of protease dynamics in cutaneous wound healing by degradomics analysis of porcine wound exudates. Molecular & cellular proteomics: MCP 14, 354–370, https://doi.org/10.1074/mcp.M114.043414 (2015).
Pascal Schlage, T. K., Jayachandran N. Kizhakkedathu and Ulrich auf dem Keller. Monitoring matrix metalloproteinase activity at the epidermal–dermal interface by SILAC-iTRAQ-TAILS. Proteomics 15, 2491–2502 (2015).
Westermann, B., Jacome, A. S. V., Rompais, M., Carapito, C. & Schaeffer-Reiss, C. Doublet N-Terminal Oriented Proteomics for N-Terminomics and Proteolytic Processing Identification. Methods in molecular biology 1574, 77–90, https://doi.org/10.1007/978-1-4939-6850-3_6 (2017).
Lazaro, J. L. et al. Elevated levels of matrix metalloproteinases and chronic wound healing: an updated review of clinical evidence. Journal of wound care 25, 277–287, https://doi.org/10.12968/jowc.2016.25.5.277 (2016).
Bottger, R., Hoffmann, R. & Knappe, D. Differential stability of therapeutic peptides with different proteolytic cleavage sites in blood, plasma and serum. PloS one 12, e0178943, https://doi.org/10.1371/journal.pone.0178943 (2017).
Toothill, V. J., Van Mourik, J. A., Niewenhuis, H. K., Metzelaar, M. J. & Pearson, J. D. Characterization of the enhanced adhesion of neutrophil leukocytes to thrombin-stimulated endothelial cells. Journal of immunology 145, 283–291 (1990).
Bizios, R., Lai, L., Fenton, J. W. 2nd & Malik, A. B. Thrombin-induced chemotaxis and aggregation of neutrophils. Journal of cellular physiology 128, 485–490, https://doi.org/10.1002/jcp.1041280318 (1986).
Stankova, J., Rola-Pleszczynski, M. & D’Orleans-Juste, P. Endothelin 1 and thrombin synergistically stimulate IL-6 mRNA expression and protein production in human umbilical vein endothelial cells. Journal of cardiovascular pharmacology 26(Suppl 3), S505–507 (1995).
Ueno, A., Murakami, K., Yamanouchi, K., Watanabe, M. & Kondo, T. Thrombin stimulates production of interleukin-8 in human umbilical vein endothelial cells. Immunology 88, 76–81 (1996).
Demidova-Rice, T. N., Wolf, L., Deckenback, J., Hamblin, M. R. & Herman, I. M. Human platelet-rich plasma- and extracellular matrix-derived peptides promote impaired cutaneous wound healing in vivo. PloS one 7, e32146, https://doi.org/10.1371/journal.pone.0032146 (2012).
Sheets, A. R., Massey, C. J., Cronk, S. M., Iafrati, M. D. & Herman, I. M. Matrix- and plasma-derived peptides promote tissue-specific injury responses and wound healing in diabetic swine. Journal of translational medicine 14, 197, https://doi.org/10.1186/s12967-016-0946-1 (2016).
Stiernberg, J. et al. Acceleration of full-thickness wound healing in normal rats by the synthetic thrombin peptide, TP508. Wound repair and regeneration: official publication of the Wound Healing Society [and] the European Tissue Repair Society 8, 204–215 (2000).
Morihara, K., Tsuzuki, H., Oka, T., Inoue, H. & Ebata, M. Pseudomonas Aeruginosa Elastase. Isolation, Crystallization, and Preliminary Characterization. The Journal of biological chemistry 240, 3295–3304 (1965).
Schmidtchen, A. Degradation of antiproteinases, complement and fibronectin in chronic leg ulcers. Acta dermato-venereologica 80, 179–184 (2000).
Vizcaino, J. A. et al. ProteomeXchange provides globally coordinated proteomics data submission and dissemination. Nature biotechnology 32, 223–226, https://doi.org/10.1038/nbt.2839 (2014).
Vizcaino, J. A. et al. update of the PRIDE database and its related tools. Nucleic acids research 44, 11033, https://doi.org/10.1093/nar/gkw880 (2016).
Acknowledgements
This research was supported by the Lee Kong Chian School of Medicine, Nanyang Technological University Start-Up Grant, Singapore Ministry of Education under its Singapore Ministry of Education Academic Research Fund Tier 1 (2015-T1-001-082), the Swedish Research Council (project 2012-1883), the Knut and Alice Wallenberg Foundation, and the Swedish Foundation for Strategic Research. RS was supported by a Lee Kong Chian School of Medicine Postdoctoral Fellowship, Nanyang Technological University.
Author information
Authors and Affiliations
Contributions
A.S., R.S., S.A., M.P., J.P., S.K. designed the research; R.S., S.A., Y.K.C., M.P., J.P. and S.K. performed the experiments and analysed the results; R.S. and A.S. wrote the manuscript. S.S. supported with mass spectrometry facility. All authors reviewed the manuscript; A.S. and R.S. arranged funding for this work.
Corresponding author
Ethics declarations
Competing Interests
The authors declare that they have no competing interests.
Additional information
Publisher's note: Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made. The images or other third party material in this article are included in the article’s Creative Commons license, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons license and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this license, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Saravanan, R., Adav, S.S., Choong, Y.K. et al. Proteolytic signatures define unique thrombin-derived peptides present in human wound fluid in vivo . Sci Rep 7, 13136 (2017). https://doi.org/10.1038/s41598-017-13197-3
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41598-017-13197-3
This article is cited by
-
Targeting Toll-like receptor-driven systemic inflammation by engineering an innate structural fold into drugs
Nature Communications (2023)
-
Interaction of host and Staphylococcus aureus protease-system regulates virulence and pathogenicity
Medical Microbiology and Immunology (2019)
-
Structural basis for endotoxin neutralisation and anti-inflammatory activity of thrombin-derived C-terminal peptides
Nature Communications (2018)
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.