Abstract
High-density lipoprotein (HDL) interacts with various cells, particularly macrophages, in functional cell-HDL interactions. Here, we found that HDL protein quality and lipid quality play critical roles in HDL functions. HDL fractions from healthy volunteers (HDLHealthy) and patients with recurrent coronary atherosclerotic disease (HDLCAD) were prepared. To analyse functional HDL-macrophage interactions, macrophages were co-incubated with each HDL, and lipid mediator production was assessed by liquid chromatography/mass spectrometry-based metabololipidomics. HDLHealthy treatment attenuated the pro-inflammatory lipid mediator production, particularly that of leukotriene (LT) B4, and this treatment enhanced lipoxin (LX) B4 and resolvin (Rv) E2 production. HDLHealthy treatment enhanced the proteasome-mediated degradation of the LTB4-producing enzyme 5-lipoxygenase (LO) in activated macrophages; however, HDLCAD did not show these anti-inflammatory effects. HDLHealthy was engulfed by macrophages via clathrin-mediated endocytosis, which was a critical step in 5-LO/LTB4 regulation. We also found that HDLCAD showed higher levels of the LTB4-producing enzymes and thus promoted LTB4 production from HDLCAD. In addition, LTB4 attenuated HDL endocytosis, HDL-mediated 5-LO degradation in macrophages, and HDL-derived augmentation of macrophage phagocytosis. These results indicated that local LTB4 produced de novo from HDLCAD regulates HDL-macrophage functional interactions and plays critical roles in dysfunctional, inflammatory HDL characteristics.
Similar content being viewed by others
Introduction
High-density lipoprotein (HDL) has diverse anti-atherosclerotic functions, such as reversing cholesterol transport1 and inhibiting inflammation2,3. Many population studies have shown that the concentration of HDL cholesterol (HDL-C) is inversely related to the risk of coronary atherosclerotic disease (CAD)4,5. However, recent unexpected results with inhibitors of cholesteryl ester transfer protein have indicated that pharmacological increases in HDL-C are not necessarily beneficial6,7 and that more attention should be focused on HDL function.
The protein quality and lipid quality of HDL play critical roles in HDL function. Recent studies have demonstrated that myeloperoxidase (MPO), a leukocyte-derived haem protein, binds to HDL. MPO generates hypochlorous acid, which oxidizes specific tyrosine and methionine residues on apoA-I and impairs apoA-I-mediated cholesterol efflux8,9. In contrast, paraoxonase 1 (PON1), an HDL-associated lipo-lactonase10, is linked to the antioxidative, anti-inflammatory, and lipid cargo-carrying functions of HDL11,12,13. We have recently shown that the serum MPO/PON1 ratio may indicate dysfunctional HDL and is useful for risk stratification of CAD patients14. Lipid quality, particularly the imbalance between omega-3 and omega-6 fatty acids, may be a risk factor for atherosclerosis15. We have reported that eicosapentaenoic acid (EPA)-rich HDL increases cholesterol efflux capacity and PON1 activity, thus indicating that the lipid quality of HDL may regulate its functions16.
Chronic inflammation contributes to the development of advanced atherosclerosis17,18,19. The resolution of inflammation is mediated by a phagocytic process by macrophages, known as programmed cell removal or efferocytosis20. M2-differentiated macrophages contribute to the resolution of inflammation by producing pro-resolving lipid mediators (LMs) and by producing lower levels of inflammatory LMs, such as LTB4 and prostaglandins (PGs), than those produced by M1 macrophages21. Although HDL has functional interactions with macrophages during reverse cholesterol transport, little is known about HDL-macrophage interactions with regard to macrophage-dependent LM production. LMs are produced predominantly from polyunsaturated fatty acids, such as arachidonic acid (AA), EPA, and docosahexaenoic acid (DHA), and play crucial roles in the initiation and resolution of inflammatory responses. The balance between pro-inflammatory and pro-resolving mediators regulates the duration of the inflammatory response by promoting neutrophil apoptosis and macrophage efferocytosis20,22.
Here, we prepared HDL fractions from healthy volunteers (HDLHealthy) and recurrent coronary atherosclerotic disease patients (HDLCAD). We found that HDLHealthy, through endocytic engulfment into activated macrophages, showed anti-inflammatory effects, thereby limiting pro-inflammatory LTB4 production and enhancing anti-inflammatory, pro-resolving LXB4 and RvE2 production, as well as enhancing macrophage phagocytosis. Moreover, HDLCAD released de novo local LTB4, which blocked endocytic engulfment of HDL by macrophages and did not show anti-inflammatory effects. These results provide a novel mechanistic for understanding how HDLHealthy tempers pro-inflammatory responses in HDL-macrophage functional interactions and how HDLCAD becomes dysfunctional or displays pro-inflammatory characteristics.
Results
HDLHealthy, but not HDLCAD, decreases LTB4 production from macrophages via proteasome-mediated degradation of 5-LO
To investigate the functional interactions between HDL and macrophages, we prepared HDL from healthy volunteers (N = 4, defined as HDLHealthy) and recurrent CAD subjects (N = 4, defined as HDLCAD) by ultracentrifugation (Supplemental Data Table 1). Macrophages (RAW 264.7 cell line, 1 × 106 cells) were activated by zymosan (ZyA) (0.1 mg, 30 min at 37 °C), then incubated with HDLHealthy or HDLCAD (10 μg protein, 30 min at 37 °C). We used wide-targeted liquid chromatography (LC)/mass spectrometry (MS)/MS-based metabololipidomics to investigate the LM profiles of HDL-macrophage interactions (Table 1). Macrophages incubated with HDLHealthy produced significantly higher levels of anti-inflammatory/pro-resolving LXB4 and RvE2. In contrast, macrophages treated with HDLCAD produced elevated levels of prostanoids, including PGD2, PGF2α, Thromboxane B2, and LTB4. As expected from the increases in the levels of PGs and LTs, HDLCAD enhanced phosphorylation of cytosolic phospholipase A2 (cPLA2)-alpha in macrophages (Supplemental Fig. 1). We focused on LTB4 because it possesses potent pro-inflammatory activity; however, little is known about its contributions to vascular biology.
Unstimulated macrophages showed limited baseline LTB4 production (0.32 ± 0.13 pg/1 × 106 cells, Fig. 1a). After ZyA activation, the levels of LTB4 production from macrophages reached 3.54 ± 0.55 pg/1 × 106 cells, and rigorous identification of LTB4 was achieved by the LC/MS/MS multiple-reaction monitoring chromatography and MS/MS spectra with more than six signature fragmentations (Fig. 1b). Notably, LTB4 as well as its pathway markers (∆6-trans LTB4, 12epi-∆6-trans LTB4 and 5 S, 12S-diHETE) were also identified, thus indicating distinct activation of the 5-LO-LTB4 pathway in macrophages. The interaction between HDLHealthy and macrophages showed significantly lower biosynthesis of LTB4; however, HDLCAD did not show lower LTB4 biosynthesis (Fig. 1a). LTB4 production by mouse bone marrow-derived macrophages was also suppressed significantly by HDLHealthy (Supplemental Fig. 2).
HDLHealthy, but not HDLCAD, decreased LTB4 production from macrophages through proteasome-mediated degradation of 5-LO. Macrophages (RAW 264.7 cell line, 1 × 106) were activated by ZyA (30 min at 37 °C), then treated with HDLHealthy or HDLCAD (10 μg protein). (a) LTB4 production from macrophages was quantified by LC/MS/MS. The results are expressed as pg/1 × 106 cells, mean ± SEM, N = 4-5 in each group. (b) Representative MRM-chromatograph and MS-MS spectrum are presented for the identification of LTB4. (c) Macrophage lysates were processed for western blot analysis of 5-LO. The results are shown as fold changes from N = 4 experiments. (d) 5-LO degradation by HDLHealthy is proteasome-dependent. ZyA-activated macrophages were pretreated for 30 min with the proteasome inhibitor MG 132 (1 µM) or vehicle, then incubated with HDLHealthy for 30 min at 37 °C. Lysates were collected for western blot analysis of 5-LO. The results are shown as the mean ± SEM from N = 4 experiments. *P < 0.05, **P < 0.01, ***P < 0.005. (e) HDLHealthy enhanced ubiquitination of 5-LO in macrophages. ZyA-activated macrophages were pretreated for 30 min with the proteasome inhibitor MG 132 (1 µM) or vehicle, then incubated with HDLHealthy or HDLCAD for 30 min at 37 °C. Lysates were immunoprecipitated with anti-5LO antibody (#3289 S, Cell Signaling), using a Dynabeads Protein A IP Kit (Thermo Fisher Scientific), and then immunoblotted with anti-ubiquitin antibody (ab140601, Abcam). (f) HDLHealthy enhanced 12/15-LO expression in macrophages. Macrophages (RAW 264.7 cell line, 1 × 106) were activated by ZyA (30 min at 37 °C), then treated with HDLHealthy or HDLCAD (10 μg protein, 30 min at 37 °C). After incubation, total RNA was extracted, and then, 12/15-LO expression was analysed by real-time PCR. The results are shown as fold change compared with the vehicle group; mean ± SEM, N = 4. *P < 0.05 vs the other groups.
After showing that HDLHealthy regulates LTB4 production from macrophages, we next focused on the protein expression of 5-LO, because it is a key enzyme in LTB4 biosynthesis from arachidonic acid. Western blot analysis revealed that stimulation of macrophages with ZyA augmented 5-LO protein expression (Fig. 1c, 2nd lane). HDLHealthy showed lower 5-LO protein expression in ZyA-activated macrophages (Fig. 1c, 3rd lane), whereas HDLCAD did not show a significant decrease in 5-LO protein expression (Fig. 1c, 4th lane). We hypothesized that ubiquitin-proteasome degradation was involved in the HDL-mediated decrease in 5-LO. To confirm this possibility, we used the proteasome inhibitor MG-13223. Pretreatment of macrophages with MG132 (1 µM, for 30 min) inhibited HDL-mediated 5-LO reduction (Fig. 1d, 4th lane); HDLHealthy also enhanced ubiquitination of 5-LO (Fig. 1e), thus indicating that HDLHealthy decreased 5-LO through ubiquitin-proteasome degradation. Moreover, HDLHealthy enhanced 12/15-LO mRNA expression in macrophages (Fig. 1f), thereby indicating that HDLHealthy induced the enzymatic pathway of pro-resolving mediator biosynthesis. HDLHealthy also suppressed production of M1-related cytokines, namely, IL-6, TNF-α, and IL-1β (Supplemental Fig. 3). However, macrophages showed pro-inflammatory cytokine profiles by HDLCAD. Together, these results indicated that HDLHealthy, but not HDLCAD, decreased LTB4 production in macrophages by proteasome-mediated degradation of 5-LO and enhanced specialized resolving mediator release.
HDLHealthy particle engulfment and localization in macrophages through clathrin-mediated endocytosis
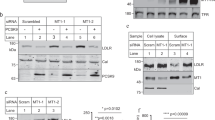
We found that HDLHealthy and HDLCAD have a distinct effect on LM production by macrophages. To investigate the details of HDL-macrophage interactions, we tracked HDL within macrophages, because specific cells other than macrophages have recently been reported to endocytose HDL holoparticles24,25,26. Macrophages were incubated with DiI-labelled HDL for 30 min at 37 °C, and this was followed by nuclear staining with DAPI. Here, we detected the engulfment of HDLHealthy into macrophages; however, low uptake of HDLCAD was observed (Fig. 2a). To confirm the uptake of human-derived HDL into macrophages, we investigated human apoA-I protein expression in the murine macrophage cell line RAW 264.7. After co-incubation with human-derived HDL, macrophages were extensively washed with phosphate-buffered saline, and then the cell lysates were analysed by western blot using an antibody specific to human apoA-I. Negligible human apoA-I protein expression was observed in murine macrophages (Fig. 2b, 1st lane). Co-incubation with human apoA-I protein (10 µg) showed human apoA-I expression in murine macrophages (Fig. 2b, 2nd lane). Macrophages co-incubated with HDLHealthy (10 µg) showed substantial human apoA-I expression (Fig. 2b, 3rd lane); however, co-incubation with HDLCAD (10 µg) did not show detectable human apoA-I protein expression in murine macrophages (Fig. 2b, 4th lane). We also confirmed that the apoA-I protein expression levels were similar between HDLHealthy and HDLCAD (Supplemental Fig. 4).
HDLHealthy, but not HDLCAD, was engulfed by macrophages through clathrin-mediated endocytosis. (a) Macrophages were incubated with DiI-labelled HDL (shown as red) for 30 min at 37 °C, then subjected to nuclear staining with DAPI (shown as blue). The arrows indicate HDL engulfment into macrophages (Scale bar = 10 μm). (b) Activated macrophages (1 × 106) were co-incubated with human apoA-I (10 µg) or each HDL (10 µg) for 30 min at 37 °C. After extensive washing with PBS−/−, macrophages were harvested. Cell lysates were processed for western blot analysis of human apoA-I. The image is representative of results from N = 3 experiments. (c) Macrophages were incubated with DiI-labelled HDL (10 µg) with or without 30 min pretreatment with the clathrin-mediated endocytosis inhibitor Pitstop 2 (20 μM). The arrowheads indicate HDL engulfment into macrophages (Scale bar = 10 μm). (d) Activated macrophages (1 × 106) were treated with HDLHealthy (10 µg) for 30 min at 37 °C with or without pretreatment with 20 μM Pitstop 2. After extensive washing, cell lysates were processed for western blot analysis of apoA-I and 5-LO. The image is representative of results from N = 3 experiments. (e) HDLHealthy engulfment was competitively blocked by unlabelled HDL. Macrophages were incubated with DiI-labelled HDL (shown as red) alone or in the presence of 40-fold excess of unlabelled HDL for 30 min at 37 °C, and this was followed by DAPI staining (shown as blue). The DiI-positive area in the macrophages was analysed by ImageJ as μm2/cell, N = 6. (f) Macrophages were incubated with DiI-labelled HDLHealthy (shown as red) in the presence or absence of a 40-fold excess of unlabelled apoA-I for 30 min at 37 °C, (Scale bar = 10 μm), and the DiI-positive area in macrophages was analysed by ImageJ as μm2/cell. The data are shown as the mean ± SEM of 3 independent experiments. **P < 0.01.
To address the mechanism underlying macrophage engulfment of HDLHealthy, we next used the clathrin-mediated endocytosis inhibitor Pitstop 227. Macrophages were incubated with DiI-labelled HDL with or without pretreatment with 20 μM Pitstop 2 for 30 min. HDLHealthy engulfment into macrophages was confirmed by confocal microscopy (Fig. 2c, left panel), and Pitstop 2 treatment was found to completely abolish HDL uptake (Fig. 2c, right panel). In the same experiment, macrophage cell lysates were obtained and subjected to western blot analysis of apoA-I and 5-LO (Fig. 2d). Pitstop 2 treatment attenuated human apoA-I protein expression in murine macrophages incubated with HDLHealthy (Fig. 2d, upper panel). Additionally, Pitstop 2 treatment augmented 5-LO protein expression within macrophages (Fig. 2d, lower panel). Furthermore, HDLHealthy particle engulfment was competitively blocked by excess unlabelled HDL (Fig. 2e) or apoA-I (Fig. 2f).
These findings indicated that engulfment of HDLHealthy into macrophages is regulated by clathrin-mediated endocytosis, presumably through a specific receptor that binds to apoA-I and that HDL endocytosis regulates HDL-mediated degradation of 5-LO in macrophages. HDLCAD was not endocytosed into macrophages and thus did not regulate 5-LO expression in macrophages. To explore the localization of macrophage-engulfed HDL, we performed immunohistochemical analysis of macrophages with anti-human apoA-I and anti-EEA1 (early endosomal-antigen-1) antibodies (Supplemental Fig. 5a) or anti-human apoA-I and anti-LAMP1 (lysosomal marker) antibodies (Supplemental Fig. 5b). ApoA-I and EEA1 did not co-localize; however, after 120 min of incubation with HDL, we observed partial co-localization of apoA-I and LAMP1 (Supplemental Fig. 5b), thus indicating that the engulfed HDL was localized in lysosomes at this time point.
De novo LTB4 production from HDLCAD
Local bioactive LMs play critical roles in controlling various macrophage functions28. After observing that HDLHealthy and HDLCAD had distinct effects on HDL-macrophage interactions, we examined the differences in the bioactive LMs released from each HDL. Each HDL type (10 µg protein) was incubated with a mixture of 1 µM each of deuterium-labelled AA, EPA, and DHA as substrates for 2 h at 37 °C, and then, deuterium-labelled LM production was analysed by LC/MS/MS. The deuterium-labelling approach enabled us to quantitatively analyse LM production from extra-HDL substrates. The profiles of LM production by HDLHealthy and HDLCAD during the 2-h incubation are shown in Table S2. We found that HDLCAD produced significantly higher levels of PGD2 and LTB4, as well as 5-LO-related pathway markers, including 5-HETE, 5-HEPE, 4-HDHA, and 7-HDHA, than those produced by HDLHealthy.
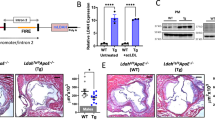
We focused on de novo LTB4 synthesis from each HDL (Fig. 3a) and found distinct differences in LTB4 production between HDLHealthy and HDLCAD. As shown in Fig. 3b, LTB4 synthesis from AA requires sequential enzymatic conversion driven by 5-LO and LTA4 hydrolase. Next, we investigated whether HDLCAD contains these critical enzymes for LTB4 production. Western blot analysis of HDLHealthy and HDLCAD revealed that HDLCAD showed an approximately 55-fold increase in the 5-LO protein levels and an approximately 90-fold increase in LTA4 hydrolase protein levels (Fig. 3c–e). Additionally, HDLCAD, but not HDLHealthy, contained FLAP (Supplemental Fig. 6). These results indicated that HDLCAD carries the neutrophil-like, functional enzymatic machinery that produces pro-inflammatory LTB4 from extra-HDL AA.
De novo LTB4 production from HDLCAD. HDL (10 μg) was incubated with 1 µM deuterium-labelled (d-) substrates (d-AA, d-EPA and d-DHA) for 2 h at 37 °C, and then, the biosynthesis of d-LMs was analysed by LC/MS/MS. (a) d-LTB4 biosynthesis from HDL. The results are shown as pg/0.01 mg of protein/2 h, mean ± SEM, N = 5. *P < 0.05. (b) The d-LTB4 biosynthesis pathway from d-arachidonic acid is shown. (c) Western blot analysis showing 5-LO and LTA4 hydrolase in HDLHealthy and HDLCAD. Fold changes in the protein expression in HDLCAD compared with those in HDLHealthy are shown. (d) 5-LO and (e) LTA4 hydrolase. The results are shown as the mean ± SEM, N = 3. **P < 0.01.
We hypothesized that exosome components might be transferred to HDL in circulating plasma. To provide evidence for this concept, PlasmaHealthy and PlasmaCAD were immunoprecipitated with anti-CD9 antibody to collect exosomes using an ExoTrapTM Exosome Isolation Spin Column Kit, and samples were then immunoblotted with anti-CD9 and anti-ApoA-I antibodies. As shown in Supplemental Fig. 7, ExoTrapTM successfully isolated plasma-derived exosomes from each type of plasma (upper panel), and we found that these exosomes also possessed ApoA-I, thus indicating the presence of HDL particles. In this experiment, we did not use separation by ultracentrifugation; therefore, this result suggests that HDL might acquire exosome-derived components during systemic circulation.
LTB4 attenuates HDLHealthy particle engulfment into macrophages and HDL-mediated 5-LO degradation
Given that HDLCAD locally releases de novo LTB4, we investigated the effect of HDL-derived LTB4 on the functional interactions between HDL and macrophages. Macrophages were incubated with 1-100 nM LTB4 for 30 min, then incubated with HDLHealthy for 30 min at 37 °C. Macrophages in specific experiments were pretreated with the LTB4 receptor antagonist U7530229 (300 nM) for 30 min at 37 °C. We also confirmed BLT1 mRNA expression in RAW macrophages (Supplemental Fig. 8.) Here, we found that 1-100 nM LTB4 significantly suppressed HDL engulfment into macrophages (Fig. 4a,b), whereas U75302 treatment rescued HDL engulfment (Fig. 4a,b, 5th lane). LTB4-mediated suppression of macrophage engulfment appeared to be specific for clathrin-mediated endocytosis. LTB4 selectively attenuated transferrin engulfment into macrophages (Supplemental Fig. 9, upper panels), which was endocytosed via clathrin-mediated machinery30,31; however, LTB4 had no effect on engulfment of dextran (Supplemental Fig. 9, lower panels), which is internalized via macropinocytosis32,33. Notably, LTB4 treatment did not affect the expression of ApoA-I receptors in macrophages, including ABCA1, ABCG1, SR-B1, and SR-A (Supplemental Fig. 10). Next, we investigated whether pretreatment of LTB4 might reverse HDL-initiated 5-LO degradation in macrophages. We pretreated macrophages with LTB4 (1-100 nM) or vehicle for 30 min, then incubated them with HDLHealthy for 30 min at 37 °C. Cell lysates were processed for western blot analysis of 5-LO (Fig. 4c). We confirmed HDL-mediated reduction of 5-LO (Fig. 4c, 2nd lane). Additionally, 1-100 nM LTB4 reversed this HDL-mediated decrease in 5-LO in a dose-dependent manner, resulting in augmented expression of 5-LO in macrophages (Fig. 4c, 3rd-5th lanes). Pretreatment with U75302 (300 nM) inhibited the effects of 100 nM LTB4, thus resulting in lower 5-LO expression in macrophages by HDL-mediated degradation (Fig. 4c, 6th lane).
LTB4 attenuated HDL engulfment and HDL-mediated 5-LO degradation. (a) Macrophages were pretreated for 30 min at 37 °C with the BLT1 inhibitor U75302 (300 nM) or vehicle, and then incubated with LTB4 (100 nM) for 30 min at 37 °C and subsequently with DiI-labelled HDLHealthy (shown as red) for 30 min at 37 °C. (b) The DiI-positive area in macrophages (μm2/cell) was quantified by ImageJ (Scale bar = 10 μm). The data are shown as the mean ± SEM of 3 independent experiments. *P < 0.05, **P < 0.01, ***P < 0.005. (c) Macrophages were pretreated for 30 min at 37 °C with U75302 (300 nM) or vehicle and were then incubated with LTB4 (1-100 nM) for 30 min at 37 °C and subsequently with 10 μg of HDLHealthy for 30 min at 37 °C. Lysates were collected for western blot analysis of 5-LO. The data are shown as the mean ± SEM of 3 independent experiments. *P < 0.05, **P < 0.01.
LTB4 receptor antagonist promoted HDLCAD engulfment into macrophages
After showing that HDLCAD locally produced LTB4 de novo and that local LTB4 suppressed HDL engulfment into macrophages in a dose-dependent manner, we investigated the effect of the LTB4 receptor antagonist on HDLCAD-macrophage interactions. Macrophages were pretreated with the BLT1 antagonist U75302 (300 nM), or left untreated, before incubation with DiI-labelled HDLHealthy and HDLCAD. Pretreatment with U75302 had no effect on HDLHealthy engulfment into macrophages (Fig. 5a, upper panels and Fig. 6b, 1st-2nd lanes); however, HDLCAD engulfment was significantly increased by U75302 pretreatment, and the particle engulfment was similar to that of HDLHealthy (Fig. 5a, lower panels and Fig. 6b, 3rd-4th lanes).
LTB4 receptor antagonist promoted HDLCAD engulfment into macrophages. (a) Macrophages were pretreated for 30 min at 37 °C with or without LTB4 receptor (BLT1) antagonist, U75302 (300 nM) and then were incubated with DiI-labelled HDLHealthy (upper panels) or DiI-labelled HDLCAD (lower panels) for 30 min at 37 °C. Scale bars = 10 μm. (b) The DiI-positive area in macrophages (μm2/cell) was quantified by ImageJ. The data are shown as the mean ± SEM of 3 independent experiments. *P < 0.05.
HDLHealthy enhanced macrophage phagocytosis. Macrophages (0.5 × 105) were pretreated with each HDL (10 µg) for 1 h or 2 h at 37 °C and then incubated with fluorescent-labelled zymosan for 30 min at 37 °C. In specific experiments, LTB4 (100 nM) or BLT1 antagonist LY293111 (300 nM) or U75302 (300 nM) were used as pretreatment. The results are percentage increases of phagocytosis compared with that after vehicle treatment and are shown as the mean ± SEM, N = 4. † P < 0.05 compared to vehicle. *P < 0.05, **P < 0.01, versus HDLHealthy.
HDLHealthy enhances macrophage phagocytosis
Because macrophage phagocytosis plays critical roles in the anti-atherogenic machinery34,35, we evaluated whether each HDL type might have distinct effects on macrophage phagocytosis. Pretreatment with HDLHealthy significantly enhanced macrophage phagocytosis, as compared with treatment with the vehicle (Fig. 6). Notably, pretreatment with HDLCAD and pretreatment with HDLHealthy + LTB4 (100 nM) resulted in significant decreases in phagocytosis, and treatment with either BLT1 antagonist LY293111 or U75302 rescued macrophage phagocytosis. These results indicated that functional interactions between HDLHealthy and macrophages contribute to enhanced macrophage efferocytosis, and local low-dose LTB4 may suppress these anti-atherogenic functions.
Proposed HDL functions: regulation of LTB4 from activated macrophages via HDL holoparticle endocytosis
To address the functional interactions between HDL and macrophages, we propose novel HDL-initiated regulation of macrophages via HDL holoparticle endocytosis. HDLHealthy was engulfed by macrophages via clathrin-mediated endocytosis and 5-LO expression attenuated by ubiquitin proteasome degradation, thus resulting in lower LTB4 production from activated macrophages (Fig. 7a). HDLHealthy also enhanced LXB4 and RvE2 production, as well as phagocytosis in macrophages. In contrast, HDLCAD carries neutrophil-like enzymatic machinery, which produced higher levels of local de novo LTB4. This enzymatic machinery may be transferred to HDL particle from neutrophil-derived exosomes. Locally produced de novo LTB4 interfered with HDL engulfment into macrophages (Fig. 7b). Here, 5-LO escaped from HDL-mediated degradation, thus resulting in continuous LTB4 production from activated macrophages.
Proposed HDL functions: regulation of LTB4 production from activated macrophages via HDL engulfment. (a) HDLHealthy is engulfed by macrophages via clathrin-mediated endocytosis and attenuates 5-LO expression by the ubiquitin proteasome system, thus resulting in decreased LTB4 from activated macrophages. HDLHealthy enhances LXB4 and RvE2 production, as well as phagocytosis in macrophages. (b) HDLCAD produces de novo LTB4, which interferes with HDL engulfment into macrophages. Here, 5-LO escapes from HDL-mediated degradation, thereby resulting in continuous LTB4 production from activated macrophages.
Discussion
In the present study, we demonstrated that HDLHealthy contributes to anti-inflammatory and pro-resolving functions during HDL-macrophage interactions through HDL holoparticle endocytosis. We also found that HDLCAD releases de novo pro-inflammatory LM LTB4, which locally interferes with the anti-inflammatory function of HDL by suppressing HDL particle engulfment into macrophages.
Only hepatocytes and endothelial cells have previously been reported to engulf HDL holoparticles24,25,26. Here, we reported human HDL engulfment into macrophages by tracking DiI-stained HDL (Fig. 2a) and human apoA-I protein expression within murine macrophages (Fig. 2b). After the addition of the clathrin inhibitor Pitstop 2, HDL engulfment was nearly completely abrogated (Fig. 2c), thus indicating that HDL engulfment is driven by clathrin mediated endocytosis. We observed that excess non-labelled HDL or apoA-I competitively decreased DiI-labelled HDL engulfment (Fig. 2e,f), thus suggesting the presence of an HDL-specific, apoA-I-dependent receptor for HDL engulfment. We next investigated the intracellular localization of HDL particles after engulfment into macrophages; however, we did not observe co-localization of HDL with early endosomes at 10-120 min after co-incubation (Supplemental Fig. 5a). HDL showed partial co-localization with lysosomes after 120 min co-incubation (Supplemental Fig. 5b). Further studies are required to identify the receptor for HDL engulfment and HDL trafficking within macrophages.
HDL engulfment into macrophages attenuated 5-LO expression by proteasome degradation (Fig. 1c,d), thus decreasing LTB4 production from activated macrophages (Fig. 1a,b). It remains unclear how HDL engulfment regulates proteasome-mediated degradation of 5-LO. Notably, engulfment of HDLHealthy promoted anti-inflammatory, pro-resolving LM LXB4 and RvE2 release from macrophages (Table 1), and this release orchestrates resolution programs20,21, including enhanced phagocytosis of macrophages, as shown in Fig. 6. HDLCAD did not enhance macrophage phagocytosis but instead resulted in decreased phagocytic functions. Recent studies have indicated that advanced atherosclerotic lesions are characterized by the pathological accumulation of diseased vascular cells and apoptotic cellular debris and that the removal of these cells and cellular debris appears to be significantly impaired in diseased blood vessels34,35. HDLCAD may contribute to impaired macrophage phagocytosis and pathogenesis of atherosclerosis.
HDL carries several enzymes involved in lipid metabolism, such as lecithin-cholesterol acyltransferase and lipoprotein-associated phospholipase A2 (also known as platelet-activating factor acetylhydrolase)36. Using our LC/MS/MS-based metabololipidomics approach, we confirmed de novo LM production from HDL particles. Notably, we identified pro-inflammatory LTB4 production from HDLCAD (Fig. 3a), as well as critical enzymes for LTB4 biosynthesis, particularly 5-LO, LTA4 hydrolase, and FLAP (Fig. 3c and Supplemental Fig. 6), which are enriched in activated neutrophils37. Our results indicated that the HDLCAD carries LTB4-related enzymes and that this enzymatic machinery may be transferred to HDLCAD via activated leukocyte-derived exosomes and microparticles, which may contain 5-LO, LTA4 hydrolase, and FLAP.
LTB4 promotes monocyte chemotaxis and conversion of monocytes to foam cells, thus resulting in accelerated atherosclerosis38. The LTB4 receptor (BLT1) is expressed in macrophages39,40. The contribution of the LTB4/BLT1 signalling pathway to atherosclerosis has been demonstrated by using a BLT1 antagonist and BLT1-deficient mice41,42. Additionally, 5-LO gene expression in peripheral blood mononuclear cells and LTB4 concentration in the plasma were augmented in patients with carotid atherosclerosis43. In our study, local de novo LTB4 release from HDLCAD suppressed HDL engulfment into macrophages, thereby inhibiting HDL-mediated 5-LO degradation. The LTB4 antagonist U75302 rescued HDL engulfment (Figs 4a,b and 5a,b) and HDL-mediated 5-LO degradation (Fig. 4c) in macrophages, thus indicating a specific contribution of LTB4/BLT1 signalling pathways to HDL-macrophage functional interactions.
In summary, our results suggested that HDL holoparticle endocytosis plays critical roles in functional HDL-cell interactions. Additionally, HDL carries specific LM-producing enzymes that may be transferred from specific exosomes, and it releases de novo local LM, which controls HDL holoparticle engulfment and HDL-mediated regulation of cellular functions. Notably, de novo local LTB4 release from HDLCAD interferes with HDL-macrophage interactions. The new pathway elucidated here suggests that therapeutic administration of an LTB4/BLT1 pathway antagonist may be beneficial for improving HDL-mediated anti-inflammatory and pro-resolving functions in cardiovascular disease patients.
Methods
Clinical participants and HDL preparation
HDLHealthy (n = 4) and HDLCAD (n = 4) were prepared from our previous study14, on the basis of serum MPO/PON1 ratios. Plasma was stored at −80 °C until use, HDL was isolated by ultracentrifugation as previously described44, and the purity of HDL isolation was confirmed by SDS-PAGE and subsequent Coomassie staining. This study was conducted in accordance with the Declaration of Helsinki. The study protocols complied with the Guidelines of the Ethical Committee of the Kobe University Graduate School of Medicine and was approved by the Institutional Review Board of Kobe University Graduate School of Medicine. Written informed consent for participation was obtained from all subjects before the study.
LC/MS/MS-based LM metabololipidomics
Deuterated internal standards d4-LTB4, d8-5-HETE, d4-PGE2, and d5-RvD2, representing each chromatographic region of identified LMs, were added to the samples (500 pg each) to facilitate quantification. The samples were extracted by SPE on C18 columns as previously described45 and were subjected to LC-MS/MS. The system consisted of a Q-Trap 6500 (Sciex) equipped with a Shimadzu LC-30AD HPLC system. A ZORBAX Eclipse Plus C18 column (100 mm × 4.6 mm, 3.5 µm, Agilent Technologies) was used with a methanol/water/acetic acid gradient of 55:45:0.01 to 98:2:0.01 (v/v/v) at a 0.4 ml/min flow rate. For monitoring and quantifying the levels of targeted LMs, the multiple reaction monitoring (MRM) method was developed with signature ion pairs Q1 (parent ion)/Q3 (characteristic fragment ion) for each molecule. Identification was conducted with published criteria using the LC retention time, specific fragmentation patterns, and at least six diagnostic fragmentation ions. Quantification was carried out on the basis of the peak area of the MRM chromatograph, and the linear calibration curves were obtained with authentic standards for each compound.
Macrophage-HDL interactions
RAW 264.7 macrophages were cultured in DMEM supplemented with 10% FBS. In total, 1 × 106 macrophages were activated by opsonized ZyM particles (100 µg, 30 min at 37 °C) in PBS, and this was followed by co-incubation with HDLHealthy or HDLCAD (10 μg protein, 30 min at 37 °C). After incubation, a 2 × volume of ice-cold methanol was added for targeted LM metabololipidomics, and 200 µl of lysis buffer (20 mM HEPES (pH 7.4), 150 mM NaCl, 1% NP40, 1% SDS) was added for western blot analysis. The expression levels of 5-LO were monitored using an anti-5-LO antibody (3289, Cell Signaling Technology). In select experiments, macrophages were pretreated with the proteasome inhibitor MG132 (10012628, Cayman Chemical) before co-incubation with HDL.
HDL engulfment into macrophages
Each HDL was stained with Dil (1704526, Molecular Probes) as previously described46. Briefly, HDL was incubated with CM-DiI for 15 min at 37 °C, and the mixture was dialyzed overnight to remove the residual staining solution. Macrophages (1 × 106) were incubated with each DiI-labelled HDL (10 µg) for 30 min at 37 °C. HDL particle uptake into macrophages was investigated using confocal microscopy (LSM700, LEICA). For detection of human HDL-derived apoA-I from murine macrophages, macrophages (1 × 106) were co-incubated with human apoA-I (SLBN8688V, SIGMA-ALDRICH, 10 µg) or each HDL (10 µg) for 30 min at 37 °C. After extensive washing with PBS, macrophages were harvested. Cell lysates were processed for western blot analysis of human apoA-I with an anti-human apoA-I antibody (23030485, CHEMICON INTERNATIONAL). In specific experiments, macrophages were pretreated with the clathrin-mediated endocytosis inhibitor Pitstop 2 (20 µM, ab120687, Abcam) for 30 min or the LTB4 receptor antagonist U75302 (300 nM, 70705, Cayman CHEMICAL). For analysis of the effects of LTB4 on HDL uptake into macrophages, the latter was pretreated with 1, 10, or 100 nM LTB4 (20110, Cayman CHEMICAL) for 30 min at 37 °C, and this was followed by incubation with DiI-labelled HDLHealthy for 30 min. HDL uptake was analysed with confocal microscopy. In the same experiment, 5-LO protein expression in raw macrophages was also monitored by western blot analysis. After 2-h co-incubation with macrophages and HDL at 37 °C, the cells were washed in PBS, fixed with 4% formaldehyde for 15 min at 4 °C, and rinsed three times in PBS. The cells were permeabilized in 0.1% Triton X-100 for 10 min, blocked in 5% BSA/PBS for 1 h, and incubated with primary antibodies to apoA-I (23030485, CHEMICON INTERNATIONAL), EEA-1 (ab2900, Abcam) and LAMP-1 (816001, BioLegend) in 5% BSA/PBS overnight. Proteins were detected with Alexa Flour-labelled secondary antibodies.
HDL-derived LM production
For analysis of HDL-derived LM production, each HDL (10 μg) was dialyzed with PBS+/+ to remove EDTA and then was incubated with 1 µM deuterium-labelled substrates (d-AA, d-EPA and d-DHA) for 2 h at 37 °C. Deuterium-labelled LMs were analysed with our targeted LM metabololipidomics. HDL-carrying proteins were analysed by western blotting. Briefly, 10 µg of each HDL was boiled for 5 min at 95 °C in SDS buffer, then subjected to SDS-PAGE. Specific proteins were detected using primary antibodies against 5-LO (3289, Cell Signaling) and LTA4 hydrolase (ab133512, Abcam).
Detection of ubiquitinated 5-LO
ZyA-activated macrophages were pretreated for 30 min with MG 132 (1 µM) or vehicle, and this was followed by incubation with HDLHealthy for 30 min at 37 °C. Lysates were collected with 1% SDS containing lysis buffer, boiled for 5 min and sonicated. Immunoprecipitation (IP) was performed with anti-5-LO Ab (#3289, Cell Signaling) using Dynabeads Protein A IP Kit (Thermo Fisher Scientific). After IP, western blot analysis was carried out with poly-UB antibody (ab140601, linkage-specific K48 antibody, Abcam).
PCR analysis
Macrophage total RNA was extracted with TRIzol reagent (Invitrogen). cDNA was prepared from 1 µg total RNA by using PrimeScript RT reagent (RR047, Takara). Real-time polymerase chain reaction (real-time PCR) was performed with SYBRTM Premix Ex Taq II (RR820, Takara). Primers were obtained from Takara Bio Inc. Amplification reactions were performed in duplicate using a LightCycler 96 Real-Time PCR system (Roche), and fluorescence curves were analysed with the included software. GAPDH was used as an internal control. Relative quantification was performed on the basis of the ΔΔCt method.
Macrophage phagocytosis
Macrophages (0.5 × 105) were cultured on 96-well plates and preincubated with or without 5 µg of HDL for 1 h or 2 h at 37 °C, and cells were treated with 5 µl of fluorescent-labelled opsonized zymosan (Molecular Probes Z2850) at a 10:1 ratio (zymosan:macrophages) for 30 min at 37 °C47. In specific experiments, LTB4 (100 nM) or BLT1 antagonist LY293111 or U75302 (300 nM) were used as pretreatment. After the incubations, macrophages were gently washed, extracellular fluorescence was quenched by addition of a 5-fold diluted trypan blue solution, and phagocytosis was measured with a fluorescent plate reader (EnSpire, PerkinElmer).
Statistical Analysis
Results are expressed as the mean ± SEM. Statistical significance was determined using two-tailed Student’s t test for two-group comparisons and one-way ANOVA for multiple comparisons with post hoc analysis using Tukey’s test (GraphPad Prism). A P value < 0.05 was considered to be significant.
References
Khera, A. V. et al. Cholesterol efflux capacity, high-density lipoprotein function, and atherosclerosis. The New England journal of medicine 364, 127–135 (2011).
Barter, P. J. et al. Antiinflammatory properties of HDL. Circulation research 95, 764–772 (2004).
Murphy, A. J. et al. High-density lipoprotein reduces the human monocyte inflammatory response. Arteriosclerosis, thrombosis, and vascular biology 28, 2071–2077 (2008).
Gordon, T., Castelli, W. P., Hjortland, M. C., Kannel, W. B. & Dawber, T. R. High density lipoprotein as a protective factor against coronary heart disease. The Framingham Study. The American journal of medicine 62, 707–714 (1977).
Miller, G. J. & Miller, N. E. Plasma-high-density-lipoprotein concentration and development of ischaemic heart-disease. Lancet (London, England) 1, 16–19 (1975).
Barter, P. J. et al. Effects of torcetrapib in patients at high risk for coronary events. The New England journal of medicine 357, 2109–2122 (2007).
Schwartz, G. G. et al. Effects of dalcetrapib in patients with a recent acute coronary syndrome. The New England journal of medicine 367, 2089–2099 (2012).
Shao, B., Tang, C., Heinecke, J. W. & Oram, J. F. Oxidation of apolipoprotein A-I by myeloperoxidase impairs the initial interactions with ABCA1 required for signaling and cholesterol export. Journal of lipid research 51, 1849–1858 (2010).
Huang, Y. et al. An abundant dysfunctional apolipoprotein A1 in human atheroma. Nature medicine 20, 193–203 (2014).
Huang, Y. et al. Myeloperoxidase, paraoxonase-1, and HDL form a functional ternary complex. The Journal of clinical investigation 123, 3815–3828 (2013).
Bhattacharyya, T. et al. Relationship of paraoxonase 1 (PON1) gene polymorphisms and functional activity with systemic oxidative stress and cardiovascular risk. Jama 299, 1265–1276 (2008).
Besler, C. et al. Mechanisms underlying adverse effects of HDL on eNOS-activating pathways in patients with coronary artery disease. The Journal of clinical investigation 121, 2693–2708 (2011).
Davidson, W. S. et al. Proteomic analysis of defined HDL subpopulations reveals particle-specific protein clusters: relevance to antioxidative function. Arteriosclerosis, thrombosis, and vascular biology 29, 870–876 (2009).
Haraguchi, Y. et al. Serum myeloperoxidase/paraoxonase 1 ratio as potential indicator of dysfunctional high-density lipoprotein and risk stratification in coronary artery disease. Atherosclerosis 234, 288–294 (2014).
Iso, H. et al. Intake of fish and n3 fatty acids and risk of coronary heart disease among Japanese: the Japan Public Health Center-Based (JPHC) Study Cohort I. Circulation 113, 195–202 (2006).
Tanaka, N. et al. Administration of high dose eicosapentaenoic acid enhances anti-inflammatory properties of high-density lipoprotein in Japanese patients with dyslipidemia. Atherosclerosis 237, 577–583 (2014).
Tabas, I. Macrophage death and defective inflammation resolution in atherosclerosis. Nature reviews. Immunology 10, 36–46 (2010).
Ross, R. Atherosclerosis–an inflammatory disease. The New England journal of medicine 340, 115–126 (1999).
Libby, P., Tabas, I., Fredman, G. & Fisher, E. A. Inflammation and its resolution as determinants of acute coronary syndromes. Circulation research 114, 1867–1879 (2014).
Serhan, C. N. Pro-resolving lipid mediators are leads for resolution physiology. Nature 510, 92–101 (2014).
Dalli, J. & Serhan, C. N. Specific lipid mediator signatures of human phagocytes: microparticles stimulate macrophage efferocytosis and pro-resolving mediators. Blood 120, e60–72 (2012).
Fredman, G. et al. An imbalance between specialized pro-resolving lipid mediators and pro-inflammatory leukotrienes promotes instability of atherosclerotic plaques. Nature communications 7, 12859 (2016).
Rock, K. L. et al. Inhibitors of the proteasome block the degradation of most cell proteins and the generation of peptides presented on MHC class I molecules. Cell 78, 761–771 (1994).
Perisa, D., Rohrer, L., Kaech, A. & von Eckardstein, A. Itinerary of high density lipoproteins in endothelial cells. Biochimica et biophysica acta 1861, 98–107 (2016).
Pagler, T. A. et al. SR-BI-mediated high density lipoprotein (HDL) endocytosis leads to HDL resecretion facilitating cholesterol efflux. The Journal of biological chemistry 281, 11193–11204 (2006).
Eckhardt, E. R. et al. High density lipoprotein endocytosis by scavenger receptor SR-BII is clathrin-dependent and requires a carboxyl-terminal dileucine motif. The Journal of biological chemistry 281, 4348–4353 (2006).
Robertson, M. J. et al. Synthesis of the Pitstop family of clathrin inhibitors. Nature protocols 9, 1592–1606 (2014).
Dalli, J. & Serhan, C. Macrophage Proresolving Mediators-the When and Where. Microbiology spectrum 4 (2016).
Lin, A. H., Morris, J., Wishka, D. G. & Gorman, R. R. Novel molecules that antagonize leukotriene B4 binding to neutrophils. Annals of the New York Academy of Sciences 524, 196–200 (1988).
Tacheva-Grigorova, S. K., Santos, A. J., Boucrot, E. & Kirchhausen, T. Clathrin-mediated endocytosis persists during unperturbed mitosis. Cell reports 4, 659–668 (2013).
Sandvig, K. & van Deurs, B. Selective modulation of the endocytic uptake of ricin and fluid phase markers without alteration in transferrin endocytosis. The Journal of biological chemistry 265, 6382–6388 (1990).
Swanson, J. A. & Watts, C. Macropinocytosis. Trends in cell biology 5, 424–428 (1995).
Li, L. et al. The effect of the size of fluorescent dextran on its endocytic pathway. Cell biology international 39, 531–539 (2015).
Kojima, Y. et al. CD47-blocking antibodies restore phagocytosis and prevent atherosclerosis. Nature 536, 86–90 (2016).
Kojima, Y., Weissman, I. L. & Leeper, N. J. The Role of Efferocytosis in Atherosclerosis. Circulation 135, 476–489 (2017).
Kontush, A. & Chapman, M. J. Functionally defective high-density lipoprotein: a new therapeutic target at the crossroads of dyslipidemia, inflammation, and atherosclerosis. Pharmacological reviews 58, 342–374 (2006).
Zaitsu, M. et al. New induction of leukotriene A(4) hydrolase by interleukin-4 and interleukin-13 in human polymorphonuclear leukocytes. Blood 96, 601–609 (2000).
Subbarao, K. et al. Role of leukotriene B4 receptors in the development of atherosclerosis: potential mechanisms. Arteriosclerosis, thrombosis, and vascular biology 24, 369–375 (2004).
Li, P. et al. LTB4 promotes insulin resistance in obese mice by acting on macrophages, hepatocytes and myocytes. Nature medicine 21, 239–247 (2015).
Okamoto, F., Saeki, K., Sumimoto, H., Yamasaki, S. & Yokomizo, T. Leukotriene B4 augments and restores Fc gammaRs-dependent phagocytosis in macrophages. The Journal of biological chemistry 285, 41113–41121 (2010).
Heller, E. A. et al. Inhibition of atherogenesis in BLT1-deficient mice reveals a role for LTB4 and BLT1 in smooth muscle cell recruitment. Circulation 112, 578–586 (2005).
Aiello, R. J. et al. Leukotriene B4 receptor antagonism reduces monocytic foam cells in mice. Arteriosclerosis, thrombosis, and vascular biology 22, 443–449 (2002).
Sanchez-Galan, E. et al. Leukotriene B4 enhances the activity of nuclear factor-kappaB pathway through BLT1 and BLT2 receptors in atherosclerosis. Cardiovascular research 81, 216–225 (2009).
Havel, R. J., Eder, H. A. & Bragdon, J. H. The distribution and chemical composition of ultracentrifugally separated lipoproteins in human serum. The Journal of clinical investigation 34, 1345–1353 (1955).
Colas, R. A., Shinohara, M., Dalli, J., Chiang, N. & Serhan, C. N. Identification and signature profiles for pro-resolving and inflammatory lipid mediators in human tissue. American journal of physiology. Cell physiology 307, C39–54 (2014).
Angius, F. et al. High-density lipoprotein contribute to G0-G1/S transition in Swiss NIH/3T3 fibroblasts. Scientific reports 5, 17812 (2015).
Chiang, N. et al. Inhaled carbon monoxide accelerates resolution of inflammation via unique proresolving mediator-heme oxygenase-1 circuits. Journal of immunology 190, 6378–6388 (2013).
Acknowledgements
We thank all of the members in our laboratory (Department of Cardiology, Epidemiology, and Evidence-based Laboratory Medicine) for their support and valuable suggestions. This work was supported by JSPS KAKENHI Grant Number 16H01361.
Author information
Authors and Affiliations
Contributions
S.T. and M.S. designed the study, performed the experiments, analyzed data and wrote paper. T.O., M.N., N.T. and T.M. analyzed data. T.H., Y.I., R.T., T.I. and K.H. edited the manuscript. All authors discussed the results and commented on the manuscript.
Corresponding author
Ethics declarations
Competing Interests
The authors declare that they have no competing interests.
Additional information
Publisher's note: Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made. The images or other third party material in this article are included in the article’s Creative Commons license, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons license and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this license, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Tsuda, S., Shinohara, M., Oshita, T. et al. Novel mechanism of regulation of the 5-lipoxygenase/leukotriene B4 pathway by high-density lipoprotein in macrophages. Sci Rep 7, 12989 (2017). https://doi.org/10.1038/s41598-017-13154-0
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41598-017-13154-0
This article is cited by
-
Specialized pro-resolving mediators in vascular inflammation and atherosclerotic cardiovascular disease
Nature Reviews Cardiology (2024)
-
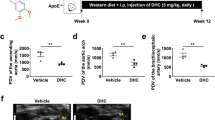
Alveolar socket healing in 5-lipoxygenase knockout aged female mice treated or not with high dose of zoledronic acid
Scientific Reports (2021)
-
High-density lipoprotein-mediated cardioprotection in heart failure
Heart Failure Reviews (2021)
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.