Abstract
Chronic prostatitis (CP) is a complex disease. Fragmentary evidence suggests that factors such as infection and autoimmunity might be associated with CP. To further elucidate potential risk factors, the current study utilized the Fangchenggang Area Male Health and Examination Survey (FAMHES) project; where 22 inflammatory/immune markers, hormone markers, tumor-related proteins, and nutrition-related variables were investigated. We also performed baseline, regression, discriminant, and receiver operating characteristic (ROC) analyses. According to NIH-Chronic Prostatitis Symptom Index (NIH-CPSI), participants were divided into chronic prostatitis/chronic pelvic pain syndrome (CP/CPPS, pain ≥ 4; divided into IIIa and IIIb sub-groups) and non-CPPS (pain = 0; divided into IV and normal sub-groups). Analyses revealed osteocalcin as a consistent protective factor for CP/CPPS, NIH-IIIb, and NIH-IV prostatitis. Further discriminant analysis revealed that ferritin (p = 0.002) and prostate-specific antigen (PSA) (p = 0.010) were significantly associated with NIH-IIIa and NIH-IV prostatitis, respectively. Moreover, ROC analysis suggested that ferritin was the most valuable independent predictor of NIH-IIIa prostatitis (AUC = 0.639, 95% CI = 0.534–0.745, p = 0.006). Together, our study revealed inflammatory/immune markers [immunoglobulin E, Complement (C3, C4), C-reactive protein, anti-streptolysin, and rheumatoid factors], hormone markers (osteocalcin, testosterone, follicle-stimulating hormone, and insulin), tumor-related proteins (carcinoembryonic and PSA), and a nutrition-related variable (ferritin) were significantly associated with CP or one of its subtypes.
Similar content being viewed by others
Introduction
Prostatitis is a common male urogenital disease, with high heterogeneity and unclear pathogenesis. In order to define the disease, in 1999, the National Institute of Diabetes and Digestive and Kidney Diseases (NIDDK) devised a new classification system1, in which four types were specified: acute prostatitis (NIH-I), chronic bacterial prostatitis (NIH-II), chronic prostatitis/chronic pelvic pain syndrome (CP/CPPS, NIH-III), and asymptomatic inflammatory prostatitis (NIH-IV). NIH-III and IV are considered as nonbacterial types of prostatitis. Among nonbacterial prostatitis, CP/CPPS (NIH-III) is characterized by pelvic or perineal pain without evidence of urinary tract infection2, with accompanying symptoms such as dysuresia, arthralgia, depression, and hysteria. Recent studies suggest that CP/CPPS is associated with many diseases, including diabetes3, prospermia4, irritable bowel syndrome5, and male reproductive dysfunction6. In contrast, NIH-IV prostatitis is asymptomatic, and only evident with the presence of inflammatory cells in expressed prostatic secretion, or histological prostate biopsy specimens.
Although nonbacterial prostatitis is not a fatal disease, one study showed that this was a problem of social cost, and had similar effects on quality of life as that on the patients with diabetes mellitus and myocardial infarction7. Furthermore, several studies indicated that it might also lead to the development of prostate cancer8, 9, whereas this was still controversial10. There are estimated five million new prostatitis cases diagnosed annually, with 2.2–9.7% prevalence worldwide11, 12. In 2009, Liang et al.13 conducted a population-based cross-sectional survey in China; where 15 000 men, aged between 15 and 60 years, were surveyed. The results showed that 8.4% of participants had prostatitis-like symptoms, and 5.4% were diagnosed with CP according to the National Institute of Health-Chronic Prostatitis Symptom Index (NIH-CPSI) criteria, with a cost of 8059 China Yuan (CNY) annually for each patient. However, to date, no effective therapeutic approaches have been proposed14.
In order to treat the enormous numbers of nonbacterial prostatitis patients (CP/CPPS and NIH-IV prostatitis), recent studies have attempted to understand the possible pathogenesis of the condition. Similar to bacterial prostatitis, infection-related factors, including bacteria, viruses, and yeast, were first under suspicion as potential causative factors for CP/CPPS (NIH-III)15,16,17,18. In 2011, Rudick et al.19 induced sustained chronic pelvic pain in mice with Uropathogenic Escherichia coli, and confirmed the role of bacteria in the development of CP/CPPS. However, another case-control study revealed no difference in the rate of positive bacteria cultures in prostatic secretion between CP/CPPS and asymptomatic men20. Therefore, infections appear not to be the single causative factor. Additionally, the episodic and relapsing symptoms, and the discovery of seminal plasma antigens in CP/CPPS, suggest that autoimmune components might contribute to symptoms in some men with prostatitis21. Moreover, prostate specific antigen (PSA) was identified to be a potential candidate antigen for further targeted therapy in CP/CPPS22. In addition, hormones and psychology might also contribute to potential etiologies23, 24. Further, a wide range of self-reported medical conditions have been suggested to play a key role CP/CPPS pathogenesis25. We have previously reported that age, smoking, alcohol consumption, and lower levels of education might be risk factors for NIH-IV prostatitis26. While the accumulating evidence point out diverse risk factors, few studies have been conducted by focusing on comprehensive biochemical markers, including inflammatory/immune markers, hormone markers, tumor-related proteins, and nutrition markers.
Here we present thus far the most comprehensive study, which is based on the Fangchenggang Area Male Health and Examination Survey (FAMHES) project in Guangxi province, China. This project was primarily conducted in the Medical Center in Fangchenggang First People’s Hospital. All participants were asked to complete a comprehensive questionnaire, which included the NIH-CPSI. Blood samples were also tested for 22 specific biochemical markers, covering the common biochemical items tested in the hospital. These 22 markers include inflammatory/immune markers, hormone markers, tumor-related proteins, and nutrition components, which could reveal the potential pathogenic factors and biomarkers involved in CP/CPPS and NIH-IV prostatitis.
Methods and Materials
Brief overview of participants
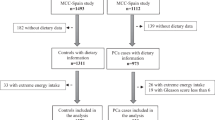
As described in our previous studies27, 28, the FAMHES project was carried out from September to December 2009, and involved a routine physical examination at the Medical Center in Fangchenggang First People’s Hospital. The sample comprised 4303 non-institutionalized Chinese men aged 17 to 88 years old, who were from the Fangchenggang area of Guangxi, China. Following this, 3593 participants were followed via interviews, and asked to complete a comprehensive demographic and health survey. The response rate was 83.5%. Before analysis, we removed juvenile subjects to ensure that only data from adult participants (aged ≥ 18 years old) were included. Written informed consent was obtained, and the study was approved by the medical ethics committee of Guangxi Medical University. All the experiments were performed in accordance with relevant guidelines and regulations of this medical ethics committee.
Selection of biochemical markers and serum measurements
Blood samples were collected from all the participants, and 22 specific biochemical markers were tested; these covered the common markers tested in the hospital, including inflammatory/immune markers, hormone markers, tumor-related proteins, and nutrition components. Specifically, the markers were: (I) inflammatory/immune markers: complement 3 (C3), complement 4 (C4), immunoglobulin E (IgE), immunoglobulin A (IgA), immunoglobulin G (IgG), immunoglobulin M (IgM), C reactive protein (CRP), antistrptolysin o (ASO), and rheumatoid factor (RF); (II) hormone markers: estradiol (E2), folic acid (FOL), follicle-stimulating hormone (FSH), luteinizing hormone (LH), osteocalcin (Osteoc), sex hormone binding globulin (SHBG), testosterone (TESTO), and insulin; (III) tumor-related proteins: alpha-fetoprotein (AFP), carcino embryonie antigen (CEA), and prostate specific antigen (PSA); and (IV) nutrition markers: vitamin B12 (B12) and ferritin (FERR).
The laboratory markers were measured in the testing center of the Department of Clinical Laboratory at the First Affiliated Hospital of Guangxi Medical University in Nanning, China. Blood samples were collected from participants between 8:00–11:00 a.m., after fasting for at least 8 h (overnight). The blood samples were centrifuged within 15–25 min, and stored at −80 °C. Further details are available in our previous reports27,28,29.
Sample screening and grouping
Strict exclusion criteria were applied to ensure the samples from eligible participants. These criteria included: (I) incomplete individual participant information; (II) incomplete NIH-CPSI score data, especially for the pain assessment section; (III) incomplete data for any of the biochemical markers investigated in this study, or refused to provide the blood samples; (IV) participants with hypertension, myocardial infarction, congestive heart failure, stroke, hyperthyroidism, rheumatoid arthritis, acquired immune deficiency syndrome, any kind of cancer, or with a history of trauma or surgery, which might influence the levels of inflammatory/immune markers, hormones, tumor-related proteins, or nutrition markers; (V) currently taking drugs which could influence the status of biochemical markers being investigated, such as vitamins, antidiabetic medicines, non-steroidal anti-inflammatory drugs, antibiotics, cimetidine, glucocorticoids, or other steroidal drugs. After application of the exclusion criteria, 1682 participants were selected.
CP/CPPS and NIH-IV prostatitis were defined according to NIH-CPSI. There are nine questions in this scoring system, with a total score of 43. These questions are classified into three parts: evaluation of pain, urinary symptoms, and impact on quality of life. In 2001, Nickel et al.30 recommended pain = 4 as the threshold to distinguish prostatitis-like symptoms from none. Based on this standard, CP/CPPS in our study was identified as a score of pain ≥ 4. For non-CPPS, a pain score of 0 was used to eliminate possible controversies among the men scoring 1–3.
In addition, the participants in our FAMHES project were also encouraged to undergo a digital rectal examination for the collection of an expressed prostatic secretion (EPS) specimen31. In total, 1779 samples were successfully acquired. All EPSs were sent immediately to the clinic laboratory. For each sample, at least 25 fields were examined, with a high power microscope (HP; 400X). Leukocytes were counted and divided to determine the mean value per HP. The degree of inflammation in each EPS specimen was classified into five groups: (I) occasional or few: 0–9 leukocytes/HP; (II) 1+: 10–20 leukocytes/HP; (III) 2+: 21–30 leukocytes/HP; (IV) 3+: 31–40 leukocytes/HP; (V) 4+: 40 leukocytes/HP. Next, according to the threshold of 10 leukocytes/HP (inflammation group ≥ 10/HP; non-inflammation group < 10/HP), the NIH-IIIa, NIH-IIIb, NIH-IV or normal sub-types were subdivided from the CP/CPPS and non-CPPS groups32.
Essential characteristics and physical examination
Information was collected from participants face-to-face interviewed by experienced personnel, using a standardized protocol. During this process, a comprehensive survey was completed. Data on essential characteristics such as age, sex, family address, jobs, smoking, alcohol consumption, etc. were collected, and physical examinations (height, weight, waistline, hipline, etc.) were performed. With regard to the essential characteristics, smoking status was divided into two categories: never a smoker or currently a smoker. Alcohol consumption was defined as the consumption of alcohol, including beer, wine, and hard liquor, within the participant’s lifetime. Waist circumference was measured at the midpoint between the inferior costal margin and the superior iliac crest on the mid-axillary line. The hipline was the maximum circumference over the buttocks. From these, the waist-hip ratio (WHR) was calculated. Additionally, body mass index (BMI) was acquired by measuring body weight with thin clothing and height without shoes. In this study, five variables (age, smoking, alcohol consumption, BMI, and WHR) were applied as covariates in all analyses.
Statistical analysis
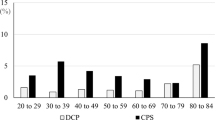
Before analysis, the distributions of the continuous variables were tested with the Shapiro-Wilks test. The biochemical markers that did not satisfy the Gaussian distribution assumption were transformed logarithmically to be relatively normal. Of the 1682 eligible participants, 1439 were included in the study based on the strict exclusion criteria; 198 of these participants were classified as CP/CPPS (pain ≥ 4) and 1241 were classified as non-CPPS (pain = 0), after excluding 243 participants with a pain score of 1–3. Further, among the 1439 samples, only 676 had results for EPS. According to the inflammation markers in the EPS, 35 participants were classified as NIH-IIIa, 86 were classified as NIH-IIIb, 139 were classified as NIH-IV prostatitis, and 416 were classified as normal. In order to investigate the association between pain and the included biochemical markers, Pearson correlation analyses were performed initially in three groups (CP/CPPS vs non-CPPS, IIIa vs normal, and IIIb vs normal). Next, baseline analyses were conducted in CP/CPPS vs non-CPPS, IIIa vs normal, IIIb vs normal, and IV vs normal groups, using the Student’s t-test, Mann-Whitney U test, and the Χ2 test, where appropriate. Additionally, both linear regression and binary logistic regression analyses were performed, in which four models (unadjusted, age-adjusted, age and smoking-adjusted, and multivariate-adjusted) were investigated. In the multivariate-adjusted model, the covariates were age, smoking, alcohol consumption, BMI, and WHR. To confirm the results obtained from these analyses, and to potentially uncover more interesting results, all biochemical markers were quartered (Q1 < 25%; 25% ≤ Q2 ≤ 50%; 50% < Q3 ≤ 75%; Q4 > 75%). The lowest level of every biochemical marker (Q1 < 25%) was treated as the reference for multinomial logistic regression analysis. In these analyses, four models were investigated [unadjusted (Model 1); age-adjusted (Model 2); age and smoking-adjusted (Model 3); multivariate-adjusted (Model 4)]. Moreover, in order to evaluate the predictive functions of these identified models for CP/CPPS and NIH-IV prostatitis, Receiver Operating Characteristic (ROC) analyses were also performed by adding the variables and covariates that were statistically associated with CP/CPSS and NIH-IV to a multivariable-adjusted logistic regression model33. Finally, discriminant analysis and principal component analysis (PCA) was performed. Associations were primarily assessed by the odd ratio (OR), 95% confidence interval (CI), and p value. An OR > 1 indicated that the biochemical marker was a risk factor for prostatitis; in contrast, an OR < 1 indicated that the biochemical marker was a protective factor. All the analyses were conducted with SPSS version 16.0 software (SPSS Inc., Chicago, IL, USA) and R. The statistical tests were two-tailed.
Results
Pain in CP/CPPS associated with inflammatory/immune factors and tumor-related proteins
In order to investigate the associations between prostatitis and the biochemical markers investigated, correlation analyses were conducted for CPPS vs non-CPPS, IIIa vs normal, and IIIb vs normal sub-groups. The results suggested that pain was significantly associated with CEA (r 2 = 0.153, p = 0.032) and C4 (r 2 = −0.154, p = 0.031) in the CP/CPPS vs non-CPPS analysis (Fig. 1a). While no association was evident in the IIIa vs normal analysis (Fig. 1b), negative correlations were observed for C3 (r 2 = −0.220, p = 0.042) and C4 (r 2 = −0.240, p = 0.026) in the IIIb vs normal analysis (Fig. 1c). These associations suggest that there may be some relationships between CP/CPPS, inflammatory/immune factors, and tumor-related proteins. Further analyses were necessary.
Inflammatory/immune markers, hormone markers, and tumor-related proteins are significantly associated with CP/CPPS
In the first step of analysis, the participants were divided into CP/CPPS (pain ≥ 4) and non-CPPS (pain = 0) groups. However, in the baseline analyses, no significant correlations were observed (Table 1). In order to investigate further, regression analyses were performed. In the logistic regression analyses, the participant category (CP/CPPS or non-CPPS) was treated as the dependent variable. Osteocalcin was the only statistically significant predictor in the unadjusted model (OR = 0.610, 95% CI = 0.379–0.983, p = 0.042) (Table S1). Furthermore, CEA (unadjusted: B = 0.087, 95% CI = 0.008–0.166, p = 0.032) and C4 (unadjusted: B = −0.179, 95% CI = −0.341–0.017, p = 0.031; age-adjusted: B = −0.187, 95% CI = −0.349–0.025, p = 0.024; age and smoking-adjusted: B = −0.195, 95% CI = −0.361–0.028, p = 0.022; multivariate-adjusted: B = −0.231, 95% CI = −0.406–0.056, p = 0.010) were also identified to be significant predictors of CP/CPPS after linear regression analysis (Table S2).
Next, the levels of all the biochemical markers were divided into quartiles. Multinomial logistic regression was conducted, with the lowest quartile as the reference. The results suggested that C3 (Q2; Model 1: OR = 0.530, 95% CI = 0.338–0.832, p = 0.006; Model 2: OR = 0.535, 95% CI = 0.341–0.840, p = 0.007; Model 3: OR = 0.513, 95% CI = 0.324–0.813, p = 0.004; Model 4: OR = 0.504, 95% CI = 0.316–0.804, p = 0.004), testosterone (Q2; Model 1: OR = 0.531, 95% CI = 0.338–0.834, p = 0.006; Model 2: OR = 0.535, 95% CI = 0.341–0.841, p = 0.007; Model 3: OR = 0.518, 95% CI = 0.328–0.818, p = 0.005; Model 4: OR = 0.522, 95% CI = 0.326–0.834, p = 0.007), and CRP (Q3; Model 1: OR = 0.605, 95% CI = 0.382–0.956, p = 0.032; Model 2: OR = 0.548, 95% CI = 0.344–0.875, p = 0.012; Model 3: OR = 0.521, 95% CI = 0.322–0.844, p = 0.008; Model 4: OR = 0.503, 95% CI = 0.303–0.834, p = 0.008) were associated with CP/CPPS (Table S3).
We next performed ROC analysis by combining the variables (Osteoc, CEA, C4, C3, TESTO, and CRP) with significant association in regression analyses. Although this model combined all the significant variables with essential participant information, the predictive function was not satisfactory (AUC = 0.583, 95% CI = 0.539–0.626, p = 0.001). On the other hand, this finding confirms the complexity of CP/CPPS, which could not be explained by the limited biochemical markers that we investigated (Table 2, Figure S1).
New factors discovered in association with NIH-IIIa prostatitis
The analysis of the CP/CPPS vs non-CPPS group revealed the factors that influence CP/CPPS. However, as a complex disease, CP/CPPS can also be divided into two sub-groups (NIH-IIIa and NIH-IIIb), and non-CPPS (NIH-IV and normal); thus it may have potential associations among the various sub-groups. To investigate this, the IIIa vs normal group was investigated in further analyses. As expected, new biochemical markers were identified in the baseline analysis for this group (FERR: p = 0.015; FSH: p = 0.049) (Table 3). In logistic regression analyses, FERR and FSH (unadjusted: OR = 1.813, 95% CI = 1.000–3.287, p = 0.050) were again found to be risk factors. This was particularly evident for FERR, which was statistically significant even after multivariate-adjustment (unadjusted: OR = 2.273, 95% CI = 1.190–4.341, p = 0.013; age-adjusted: OR = 2.131, 95% CI = 1.125–4.034, p = 0.020; age and smoking-adjusted: OR = 2.156, 95% CI = 1.128–4.120, p = 0.020; multivariate-adjusted: OR = 2.003, 95% CI = 1.021–3.932, p = 0.043) (Table S4). However, no new biochemical markers were discovered in the linear regression analyses (Table S5).
In the quartered analyses, FERR was confirmed to be a risk factor. With an increasing level of FERR, there was a greater risk of NIH-IIIa prostatitis (Q4; Model 1: OR = 3.128, 95% CI = 1.185–8.259, p = 0.021; Model 2: OR = 3.041, 95% CI = 1.149–8.049, p = 0.025; Model 3: OR = 3.100, 95% CI = 1.163–8.266, p = 0.024; Model 4: OR = 2.837, 95% CI = 1.019–7.898, p = 0.046; p for trend = 0.010). In addition, insulin was unexpectedly identified as a significant predictor (Q2; Model 1: OR = 0.184, 95% CI = 0.039–0.859, p = 0.031; Model 2: OR = 0.188, 95% CI = 0.040–0.881, p = 0.034; Model 3: OR = 0.188, 95% CI = 0.040–0.882, p = 0.034; Model 4: OR = 0.171, 95% CI = 0.036–0.815, p = 0.027) (Table S6).
The results of ROC analysis suggested that FERR was a stronger predictor (AUC = 0.639, 95% CI = 0.534–0.745, p = 0.006) than any other independent predictor. Even with the addition of other factors (age, smoking, alcohol consumption, BMI, WHR, FSH, and insulin), the AUC only increased slightly to 0.664 (p = 0.001) (Table 2, Fig. 2).
Inflammatory/immune factors, PSA, and osteocalcin are important in NIH-IIIb prostatitis
For the IIIb vs normal group analyses, no significant associations were identified in the baseline analyses (Table 3). In the regression analyses, several Inflammatory/immune markers (C3, C4, and CRP) were consistently found to be significant. In addition, two new biochemical markers were also identified: IgE (multivariate-adjusted: OR = 0.829, 95% CI = 0.691–0.994, p = 0.043) and ASO (un-adjusted: OR = 0.763, 95% CI = 0.588–0.989, p = 0.041; age-adjusted: OR = 0.765, 95% CI = 0.590–0.993, p = 0.044; age and smoking-adjusted: OR = 0.767, 95% CI = 0.591–0.997, p = 0.047) (Tables S7–S9). In the following quartered analyses, osteocalcin (Q3; Model 1: OR = 0.504, 95% CI = 0.257–0.987, p = 0.046; Model 2: OR = 0.512, 95% CI = 0.260–1.009, p = 0.053; Model 3: OR = 0.506, 95% CI = 0.256–0.999, p = 0.050; Model 4: OR = 0.454, 95% CI = 0.226–0.913, p = 0.027), RF (Q2; Model 1: OR = 2.441, 95% CI = 1.178–5.058, p = 0.016; Model 2: OR = 2.469, 95% CI = 1.190–5.122, p = 0.015; Model 3: OR = 2.449, 95%CI = 1.179–5.088, p = 0.016; Model 4: OR = 2.394, 95% CI = 1.148–4.991, p = 0.020), and PSA (Q3; Model 1: OR = 2.346, 95% CI = 1.173–4.693, p = 0.016; Model 2: OR = 2.325, 95% CI = 1.162–4.656, p = 0.017; Model 3: OR = 2.314, 95% CI = 1.155–4.639, p = 0.018; Model 4: OR = 2.279, 95% CI = 1.130–4.596, p = 0.021) were also found to be associated with the development of NIH-IIIb prostatitis (Table S9).
In addition, when combining all the biochemical markers (IgE, ASO, CRP, C3, and C4) and confounding factors (age, smoking, alcohol consumption, BMI, and WHR) identified in the regression analyses, the ROC AUC reached 0.619 (p = 0.001). By adding RF, PSA, and osteocalcin to the model, the AUC significantly increased to 0.676 (p < 0.001) (Table 2, Figure S2).
Osteocalcin, FSH, and PSA are also associated with NIH-IV prostatitis
With regard to type IV prostatitis, osteocalcin (p = 0.006), FSH (p = 0.037), and PSA (p < 0.001) showed significant difference in the IV vs normal group baseline analyses (Table 3). We next performed logistic regression analysis in the sub-group without pain. This analysis confirmed the association of osteocalcin (un-adjusted: OR = 0.402, 95% CI = 0.208–0.779, p = 0.007), FSH (un-adjusted: OR = 1.447, 95% CI = 1.020–2.051, p = 0.038), and PSA (un-adjusted: OR = 1.882, 95% CI = 1.358–2.609, p < 0.001; age-adjusted: OR = 1.720, 95% CI = 1.234–2.397, p < 0.001; age and smoking-adjusted: OR = 1.698, 95% CI = 1.218–2.368, p = 0.002; multivariate-adjusted: OR = 1.731, 95% CI = 1.234–2.429, p = 0.001) with type IV prostatitis (Table S10). In the subsequent quartered analysis, PSA and osteocalcin were found again to be statistically significant predictors. In addition, it appeared that, with increased levels of PSA (p for trend = 0.001) and osteocalcin (p for trend = 0.010), the risk and protective effects were enhanced, respectively (Table S11). The ROC analysis further indicated that these three biochemical markers had a potential predictive value for NIH-IV prostatitis (AUC = 0.658, 95% CI = 0.607–0.710, p < 0.001) (Table 2, Figure S3).
Discriminant and principal component analyses
Next, we performed discriminant analysis, and found that osteocalcin was a statistically significant predictor for CPPS, with a false positive rate (FPR) = 45.59%. For NIH-IV prostatitis, osteocalcin and PSA were identified as predictors, with a lower FPR (original: 39.10%; cross-validated: 39.64%). Unexpectedly, only FERR was confirmed to be significantly associated with NIH-IIIa prostatitis, with the lowest FPR (38.36%) (Table 4). These results suggest that PSA, osteocalcin, and FERR are most probably vital factors in the development of CP/CPPS and other types of prostatitis. However, with the inclusion of all the significant biochemical markers for each group, CP/CPPS, NIH-IIIa, NIH-IIIb, and NIH-IV types of prostatitis could not be distinguished from each other (Figure S4).
Discussion
Chronic prostatitis is a complex syndrome diagnosed worldwide. Despite its high morbidity and impact on the health of numerous men, little is known about the environmental and inherited risk factors to the pathogenesis of prostatitis. In order to define the disease severity, the NIH-CPSI was developed. On the basis of this system, our study was performed to uncover potential risk factors in association with CP/CPPS and NIH-IV prostatitis, and to evaluate their predictive effects for the disease. After the comprehensive analysis, we discovered several types of associations (CPPS vs non-CPPS: Osteoc, CEA, C4, C3, TESTO, and CRP; IIIa vs normal: FERR, FSH, and insulin; IIIb vs normal: IgE, ASO, CRP, C3, C4, RF, PSA, and Osteoc; IV vs normal: Osteoc, FSH, and PSA), in which osteocalcin was reproducibly found to be a protective factor in three groups, including CP/CPPS, NIH-IIIb, and NIH-IV prostatitis. Despite the fact that various predictors were discovered for the different groups, our further discriminant analysis only revealed FERR and PSA in association with NIH-IIIa and NIH-IV prostatitis, respectively.
Osteocalcin contains a 46–50 amino acid residues and is a molecular weight of 5.6 kDa secreted protein, which is produced primarily by osteoblasts34. Osteocalcin was initially isolated by Price et al.35, 36 from bovine and human bone. In human, osteocalcin is encoded by the BGLAP gene, locating at 1q25–q31, and encoding an 11 kD pre-pro-protein with 98 amino acid residues37. Some early studies mainly focused on its function in bone growth38. However, recent reports showed that this protein has extensive functions, not limited in bone. In 2007, Lee et al.39 revealed endocrine effects of osteocalcin, probably playing roles in glucose metabolism. Ferron et al.40 further confirmed this function and indicated that osteocalcin might be valuable in the treatment of metabolic diseases. In addition, osteocalcin may function in Leydig cells of the testis to stimulate testosterone biosynthesis, and therefore affect male fertility41. The mechanism might be related to the pancreas-bone-testis axis42. Although there is no direct evidence of an association of osteocalcin with CP/CPPS and type IV prostatitis, researchers observed that osteocalcin may play a role in brain function. In 2013, Oury et al.43 revealed that, compared to control, the cognition of osteocalcin null mice was impaired, with anxiety and depression-related behavior. These manifestations were similar, to some extent, as those observed in CP/CPPS44. In addition, Woodworth et al.45 identified unique microstructural changes in the brain of urological chronic pelvic pain syndrome (UCPPS). These results suggested that osteocalcin might be a protective factor, which is consistent with our results, especially with regard to the psychological aspect. The possible mechanism might be that osteocalcin functions as a neuropeptide in the brain of CP/CPPS (NIH-III prostatitis) patients46. On the other hand, NIH-IV prostatitis is asymptomatic with persistent leukocytosis. Unlike NIH-III prostatitis, recent studies suggested that the inflammatory process may play a potential role in the pathogenesis47, 48. Moreover, our previous studies identified that osteocalcin might be a protective factor for low-grade inflammation49, 50. Therefore, it seems reasonable that osteocalcin could influence the inflammatory process of NIH-IV prostatitis.
PSA is also known as gamma-seminoprotein or kallikrein-3 (KLK3). As member of the kallikrein-related peptidase family, PSA is mainly secreted by the epithelial cells of the prostate gland. Its main functions are believed to be liquefying semen and dissolving cervical mucus51. In the serum of men, small quantities are present. Nowadays it is widely applied in the diagnosis of prostate cancer and other types of prostate diseases52, including the prostatitis. In 2011, Korrovits et al.48 found that in type IV prostatitis, both IL-6 in seminal plasma and PSA in blood serum were significantly increased. Similarly, Gui-Zhong et al.53 discovered an elevation of serum PSA in asymptomatic prostatitis, thus helping to prevent unnecessary repeated biopsies. On the other hand, there may be a correlation between PSA level and prostatitis to some extent. In the study by Ponniah et al.22, an autoimmune component was identified to contribute to symptoms in some men. In a follow-up study, they confirmed this finding and recommended that PSA can be the candidate antigen for further targeted therapy in CP/CPPS23. In our study, we validated the assertion that PSA might be a risk factor for CP/CPPS and asymptomatic type IV prostatitis. ROC analysis also showed that PSA level may be one of the elements predicting CP/CPPS. However, some studies did not observe this correlation. For examples, Engelhardt et al.47, 54, 55 focused on asymptomatic type IV prostatitis and benign prostatic hyperplasia (BPH) and did not observe any association between NIH-IV prostatitis and PSA level. In our study, the evaluation and classification of chronic prostatitis was based on the NIH-CPSI Score and EPS, whereas Engelhardt et al. used histopathology for evaluation and classification, which may have not strictly excluded NIH-II prostatitis patients. Furthermore, PSA has been identified to be elevated upon inflammation56. Therefore, we could not ignore the influence of PSA level on NIH-II prostatitis. Future studies are needed to examine more strategies to diagnose prostatitis, especially for NIH-IV, and to investigate the role of PSA in NIH-IV prostatitis.
Much to our surprise, FERR was found to be associated with NIH-IIIa prostatitis, and had the highest predictive function, compared to the other independent biochemical markers (all predictors combined with FERR: AUC = 0.652, 95% CI = 0.550–0.753, p = 0.003). In addition, in the discriminant analysis, FERR was shown to have lower FPR. Further, the finding indicated that the risk of NIH-IIIa prostatitis was elevated with increasing level of FERR. Although there was no direct evidence in the literature to suggest an association between FERR and prostatitis, some studies have hypothesized a potential correlation. Ferritin is a 24-subunit globular protein composed of two types of subunits (H and L). The ratio of H to L subunits varies according to the tissue type and developmental stage57. This protein is a universal intracellular protein, which is produced by almost all living organisms. Its main function is storing and releasing iron in a controlled fashion. Previous studies have revealed that elevated levels of serum ferritin also occurr in patients with hematologic malignancies, such as Hodgkin’s disease and acute leukemia, accompanied by impaired cell-mediated immunity58, 59. This suggests that ferritin might be associated to some extent with the immune system60. Additionally, excess iron can induce oxidative stress and inflammation61. As an ubiquitous intracellular protein that can store and release iron, serum ferritin was also identified to be associated with a wide range of inflammatory conditions62, such as renal disease63, autoimmune disease64, and infection. NIH-IIIa prostatitis is characterized by pain and obvious leukocytes in EPS, indicating that an inflammation/immune reaction is occurring. On the basis of this observation, we assumed that serum ferritin would be significantly increased in the type IIIa prostatitis.
In addition to osteocalcin, FERR, and PSA, other inflammatory/immune factors have been identified as the predictive factors. Autoimmunity might be the etiology of CP/CPPS as reported in previous studies22, 65. Based on this, Rudick et al.66 developed an experimental autoimmune prostatitis. In their study, prostate glands from rats were collected to inject into mice. Following this, persistent pelvic pain and inflammatory infiltrates in prostate lobes were found. In addition, neuronal fiber distribution was also significantly increased. These results confirmed the role of autoimmune factors in the development of CP/CPPS in an animal model. In our study, several significant biochemical markers were also observed in the regression analyses, including IgE, C3, C4, CRP, ASO, and RF. As important aspects of the immune response, the association between CP/CPPS and these factors seemed to be reasonable. However, these inflammatory/immune factors were mainly associated with NIH-IIIb prostatitis, rather than NIH-IIIa and NIH-IV. Based on previous studies, and the known function of these biochemical markers, we speculate that IgE, C3, C4, CRP, ASO, and RF might contribute to the pain experienced in CP/CPPS. On the other hand, Osteoc could influence the psychological symptoms of CP/CPPS. Additionally, hormonal elements (Osteoc, TESTO, FSH, and insulin), tumor-related proteins (CEA and PSA), and nutrition markers (FERR) might take part in the systematic low-grade inflammation recruiting the leukocytes to EPS. Further studies with larger sample size, with molecular experiments are needed.
Current study primarily investigated the function of inflammatory/immune markers, hormone markers, tumor-related proteins, and nutrition markers in the development of CP/CPPS (NIH-III prostatitis) and NIH-IV prostatitis. Twenty-two specific biochemical markers, covering the common biochemical markers checked in the hospital, were examined. However, some other more significant factors, such as interleukin, TNF-Alpha, etc. were not investigated. Further, in process of screening samples, strict exclusion criteria were applied. To some extent, the eligible participants included in this current study may not fully represent CP/CPPS and NIH-IV prostatitis patients. Therefore, there might have some biases in the association between the investigated biochemical markers and prostatitis. Considering these issues, we suggest that future studies could investigate more cytokines among definite non-bacterial prostatitis patients (evaluated with NIH-CPSI score, EPS, urine cultures, ejaculatory cultures, and histology for classification).
Limitations
As discussed above, some limitations of this study need to be pointed out: (I) only 22 common biochemical markers were investigated in our FAMHES project. These markers covered inflammatory/immune markers, hormone markers, tumor-related proteins, and nutrition markers. Some potentially more important factors, such as interleukin, TNF-Alpha, etc. were not investigated; (II) strict exclusion criteria were applied in screening the sample, which excluded some confounding factors that could have influenced the association analyses. On the other hand, these eligible participants may not represent the real population of patients; (III) in this study, chronic prostatitis was evaluated and classified by the NIH-CPSI score and EPS only, which could result in a classification bias, and may have influenced the association between PSA and prostatitis; (IV) statistical power was not assessed in this study; (V) some significant biochemical markers were observed only in one of the adjusted models. In order to confirm these findings, analysis of larger sample size is needed, together with further molecular experiments; (VI) only five common confounding factors (age, smoking, alcohol consumption, BMI, and WHR) were included, which would influence the results of ROC analysis and observed associations.
Conclusion
CP is a complex male urologic disease. In order to investigate the potentially associated risk factors, and evaluate their predictive value, 22 different biochemical markers were investigated, covering inflammatory/immune markers, hormone markers, tumor-related proteins, and nutrition markers. Our results indicated that inflammatory/immune factors (IgE, C3, C4, CRP, ASO, and RF), hormone elements (Osteoc, TESTO, FSH, and insulin), tumor-related proteins (CEA and PSA), and a nutrition marker (FERR) were significantly associated with CP/CPPS or one of its sub-types. Among them, osteocalcin was consistently found to be a protective factor for CP/CPPS, NIH-IIIb, and NIH-IV prostatitis. Additionally, ferritin was more valuable in predicting NIH-IIIa prostatitis, independently. Further molecular and epidemiological studies with larger sample size are needed.
References
Krieger, J. N., Nyberg, L. Jr & Nickel, J. C. NIH consensus definition and classification of prostatitis. JAMA. 282, 236–237 (1999).
Schaeffer, A. J. Epidemiology and evaluation of chronic pelvic pain syndrome in men. Int J Antimicrob Agents. 31, S108–111 (2008).
Wenninger, K. et al. Sickness impact of chronic nonbacterial prostatitis and its correlates. J Urol. 155, 965–968 (1996).
Hu, Y. et al. Chronic prostatitis/chronic pelvic pain syndrome impairs erectile function through increased endothelial dysfunction, oxidative stress, apoptosis, and corporal fibrosis in a rat model. Andrology. (2016).
Liao, C. H., Lin, H. C. & Huang, C. Y. Chronic Prostatitis/Chronic Pelvic Pain Syndrome is associated with Irritable Bowel Syndrome: A Population-based Study. Sci Rep. 6, 26939 (2016).
Henkel, R. et al. Chronic pelvic pain syndrome/chronic prostatitis affect the acrosome reaction in human spermatozoa. World J Urol. 24, 39–44 (2006).
Murphy, A. B. & Nadler, R. B. Pharmacotherapy strategies in chronic prostatitis/chronic pelvic pain syndrome management. Expert Opin Pharmacother. 11, 1255–1261 (2010).
Jiang., J. et al. The role of prostatitis in prostate cancer: meta-analysis. PLoS One. 8, e85179 (2013).
Boehm., K. et al. Prostatitis, other genitourinary infections and prostate cancer: results from a population-based case-control study. World J Urol. 34, 425–430 (2016).
Engelhardt, P. F. et al. Chronic asymptomatic inflammation of the prostate type IV and carcinoma of the prostate: is there a correlation? Scand. J Urol. 47, 230–235 (2013).
Krieger, J. N. et al. Epidemiology of prostatitis. Int J Antimicrob Agents. 31, S85–90 (2008).
Collins, M. M. et al. Prevalence and correlates of prostatitis in the health professionals follow-up study cohort. J Urol. 167, 1363–1366 (2002).
Liang, C. Z. et al. Treatment of chronic prostatitis in Chinese men. Asian J Androl. 11, 153–156 (2009).
Anothaisintawee, T. et al. Management of chronic prostatitis/chronic pelvic pain syndrome: a systematic review and network meta-analysis. JAMA. 305, 78–86 (2011).
Krieger, J. N. & Riley, D. E. Bacteria in the chronic prostatitis-chronic pelvic pain syndrome: molecular approaches to critical research questions. J Urol. 6, 2574–2583 (2002).
Doble, A., Harris, J. R. & Taylor-Robinson, D. Prostatodynia and herpes simplex virus infection. Urology. 3, 247–248 (1991).
Benson, P. J. & Smith, C. S. Cytomegalovirus prostatitis. Urology. 2, 165–167 (1992).
Golz, R. & Mendling, W. Candidosis of the prostate: a rare form of endomycosis. Mycoses. 9–10, 381–384 (1991).
Rudick, C. N. et al. Uropathogenic Escherichia coli induces chronic pelvic pain. Infect Immun. 79, 628–635 (2011).
Nickel, J. C. et al. Leukocytes and bacteria in men with chronic prostatitis/chronic pelvic pain syndrome compared to asymptomatic controls. J Urol. 170, 818–822 (2003).
Alexander, R. B., Brady, F. & Ponniah, S. Autoimmune prostatitis: evidence of T cell reactivity with normal prostatic proteins. Urology. 50, 893–899 (1997).
Ponniah, S., Arah, I. & Alexander, R. B. PSA is a candidate self-antigen in autoimmune chronic prostatitis/chronic pelvic pain syndrome. Prostate. 44, 49–54 (2000).
Krsmanovic, A. et al. Psychosocial mechanisms of the pain and quality of life relationship for chronic prostatitis/chronic pelvic pain syndrome (CP/CPPS). Can Urol Assoc J. 8, 403–408 (2014).
Naslund, M. J., Strandberg, J. D. & Coffey, D. S. The role of androgens and estrogens in the pathogenesis of experimental nonbacterial prostatitis. J Urol. 140, 1049–1053 (1988).
Pontari, M. A. et al. A case-control study of risk factors in men with chronic pelvic pain syndrome. BJU Int. 96, 559–565 (2005).
Wu, C. et al. Prevalence of and risk factors for asymptomatic inflammatory (NIH-IV) prostatitis in Chinese men. PLoS One. 8, e71298 (2013).
Chen, Y. et al. Immunization associated with erectile dysfunction based on cross-sectional and genetic analyses. PLoS One 9, e111269 (2014).
Li, T. et al. Serum Homocysteine Concentration Is Significantly Associated with Inflammatory/Immune Factors. PLoS One 10, e0138099 (2015).
Yang, C. et al. Genome-wide association study identifies TNFSF13 as a susceptibility gene for IgA in a South Chinese population in smokers. Immunogenetics. 64, 747–753 (2012).
Nickel, J. C. et al. Prevalence of prostatitis-like symptoms in a population based study using the National Institutes of Health chronic prostatitis symptom index. J Urol. 165, 842–845 (2001).
Wu, Y. et al. Distribution characteristics of leukocytes in EPS and correlation with serum PSA levels: results from a Chinese male population survey. Urology. 81, 384–389 (2013).
Ludwig, M. et al. Comparison of expressed prostatic secretions with urine after prostatic massage-a means to diagnose chronic prostatitis/inflammatory chronic pelvic pain syndrome. Urology. 55, 175–177 (2000).
Lu, Y. et al. Metabolic signatures and risk of type 2 diabetes in a Chinese population: an untargeted metabolomics study using both LC-MS and GC-MS. Diabetologia. 59, 2349–2359 (2016).
Price, P. A., Poser, J. W. & Raman, N. Primary structure of the gamma-carboxyglutamic acid-containing protein from bovine bone. Proc Natl Acad Sci USA 73, 3374–3375 (1976).
Price, P. A. et al. Characterization of a gamma-carboxyglutamic acid-containing protein from bone. Proc Natl Acad Sci USA. 73, 1447–1451 (1976).
Price, P. A., Urist, M. R. & Otawara, Y. Matrix Gla protein, a new gamma-carboxyglutamic acid-containing protein which is associated with the organic matrix of bone. Biochem Biophys Res Commun. 117, 765–771 (1983).
Puchacz, E. et al. Chromosomal localization of the human osteocalcin gene. Endocrinology. 124, 2648–2650 (1989).
Ducy, P. et al. Increased bone formation in osteocalcin-deficient mice. Nature. 382, 448–452 (1996).
Lee, N. K. et al. Endocrine regulation of energy metabolism by the skeleton. Cell. 130, 456–469 (2007).
Ferron, M. et al. Osteocalcin differentially regulates beta cell and adipocyte gene expression and affects the development of metabolic diseases in wild-type mice. Proc Natl Acad Sci USA 105, 5266–5270 (2008).
Karsenty, G. & Oury, F. Regulation of male fertility by the bone-derived hormone osteocalcin. Mol Cell Endocrinol. 382, 521–526 (2014).
Oury, F. et al. Osteocalcin regulates murine and human fertility through a pancreas-bone-testis axis. J Clin Invest. 125, 2180 (2015).
Oury, F. et al. Maternal and offspring pools of osteocalcin influence brain development and functions. Cell. 155, 228–241 (2013).
Kwon, J. K. & Chang, I. H. Pain, catastrophizing, and depression in chronic prostatitis/chronic pelvic pain syndrome. Int Neurourol J. 17, 48–58 (2013).
Woodworth, D. et al. Unique Microstructural Changes in the Brain Associated with Urological Chronic Pelvic Pain Syndrome (UCPPS) Revealed by Diffusion Tensor MRI, Super-Resolution Track Density Imaging, and Statistical Parameter Mapping: A MAPP Network Neuroimaging Study. PLoS One. 10, e0140250 (2015).
Patterson-Buckendahl, P. et al. Decreased sensory responses in osteocalcin null mutant mice imply neuropeptide function. Cell Mol Neurobiol. 32, 879–889 (2012).
Engelhardt, P. F. et al. Tumor necrosis factor-α expression in patients with obstructive benign prostatic hyperplasia is associated with a higher incidence of asymptomatic inflammatory prostatitis NIH category IV and prostatic calcification. Scand J Urol. 1–7 [Epub ahead of print] (2015)
Korrovits, P. et al. Seminal interleukin-6 and serum prostate-specific antigen as possible predictive biomarkers in asymptomatic inflammatory prostatitis. Urology. 78, 442–446 (2011).
Tan, A. et al. Low serum osteocalcin level is a potential marker for metabolic syndrome: results from a Chinese male population survey. Metabolism: Clinical and Experimental. 60, 1186–1192 (2011).
Liao, M. et al. Serum Osteocalcin Is Associated with Inflammatory Factors in Metabolic Syndrome: A Population-Based Study in Chinese Males. Mediators Inflamm. 2015, 683739 (2015).
Balk, S. P., Ko, Y. J. & Bubley, G. J. Biology of prostate-specific antigen. J Clin Oncol. 21, 383–391 (2003).
Catalona, W. J. et al. Comparison of digital rectal examination and serum prostate specific antigen in the early detection of prostate cancer: results of a multicenter clinical trial of 6,630 men. J Urol. 151, 1283–1290 (1994).
Gui-Zhong, L. et al. The correlation of extent and grade of inflammation with serum PSA levels in patients with IV prostatitis. Int Urol Nephrol. 43, 295–301 (2011).
Engelhardt, P. F. et al. Association between asymptomatic inflammatory prostatitis NIH category IV and prostatic calcification in patients with obstructive benign prostatic hyperplasia. Minerva Urol Nefrol. 68, 242–249 (2016).
Engelhardt, P. F. et al. Immunohistochemical expression of interleukin-2 receptor and interleukin-6 in patients with prostate cancer and benign prostatic hyperplasia: association with asymptomatic inflammatory prostatitis NIH category IV. Scand J Urol. 49, 120–126 (2015).
Kandirali, E. et al. Association of extent and aggressiveness of inflammation with serum PSA levels and PSA density in asymptomatic patients. Urology. 70, 743–747 (2007).
Wang, W. et al. Serum ferritin: Past, present and future. Biochim Biophys Acta. 1800, 760–769 (2010).
Schier, W. W. et al. Hodgkin’s disease and immunity. Am J Med. 20, 94–99 (1956).
Izak, G. et al. The immune response in acute myelocytic leukemia: effect of the methanol extraction residue fraction of tubercle bacilli (MER) on T and B cell functions and their relation to the course of the disease. Isr J Med Sci. 13, 677–693 (1977).
Hazard, J. T. & Drysdale, J. W. Ferritinaemia in cancer. Nature. 265, 755–756 (1977).
Van, B. P., Velez, R. L., Vaziri, N. D. & Zhou, X. J. Iron overdose: a contributor to adverse outcomes in randomized trials of anemia correction in CKD. Int Urol Nephrol. 44, 499–507 (2012).
Gabay, C. & Kushner, I. Acute-phase proteins and other systemic responses to inflammation. N Engl J Med. 340, 448–454 (1999).
Kalantar-Zadeh, K., Kalantar-Zadeh, K. & Lee, G. H. The fascinating but deceptive ferritin: to measure it or not to measure it in chronic kidney disease? Clin J Am Soc Nephrol. 1, S9–S18 (2006).
Zandman-Goddard, G. & Shoenfeld, Y. Ferritin in autoimmune diseases. Autoimmun Rev. 6, 457–463 (2007).
John, H. et al. Immunological alterations in the ejaculate of chronic prostatitis patients: clues for autoimmunity. Andrologia. 35, 294–299 (2003).
Rudick, C. N., Schaeffer, A. J. & Thumbikat, P. Experimental autoimmune prostatitis induces chronic pelvic pain. Am J Physiol Regul Integr Comp Physiol. 294, R1268–1275 (2008).
Acknowledgements
This study was funded by Guangxi Natural Science Fund for Innovation Research Team (2013GXNSFFA019002), Innovation Project of Guangxi Graduate Education (YCBZ2017037), Guangxi Collaborative Innovation Center for genomic and personalized medicine (201319), The Science and technology development plan of Guangxi (Guikegong 1355005-3-17), National Program on Key Basic Research Project (973 Program) (2012CB518303), Natural Science Foundation of China (81460388).
Author information
Authors and Affiliations
Contributions
Y.C., J.L., Q.Y.W. and Z.N.M. participated in design, writing and modification of all the paper. Y.C. and J.L. took part in the statistical analysis. G.H.W. provided important advices for this paper. Y.L.H., H.Y.Z., X.B.Y., Y.H.J., Z.T.Y., Y.C.C., Y.G., A.H.T., M.L, Z.L., C.L.W., X.Y.X., S.C.W., Z.F.Z., W.C. mainly participated in the sample collection and field investigation.
Corresponding authors
Ethics declarations
Competing Interests
The authors declare that they have no competing interests.
Additional information
Publisher's note: Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made. The images or other third party material in this article are included in the article’s Creative Commons license, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons license and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this license, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Chen, Y., Li, J., Hu, Y. et al. Multi-factors including Inflammatory/Immune, Hormones, Tumor-related Proteins and Nutrition associated with Chronic Prostatitis NIH IIIa+b and IV based on FAMHES project. Sci Rep 7, 9143 (2017). https://doi.org/10.1038/s41598-017-09751-8
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41598-017-09751-8
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.