Abstract
Leaves of Cyclocarya paliurus are a sweet tea traditionally used to treat obesity and diabetes in China. However, its protective mechanisms against hyperglycemia remains unclear. Here, we demonstrate that the extract of C. paliurus leaves significantly decreased body loss, food intake and blood glucose level, and increased blood insulin level, β-cell number and insulin-producing β cells in high-fat diet-low dose STZ-induced diabetic mice. In vivo and in vitro studies also showed the extract of C. paliurus leaves significantly inhibited pancreatic β cell apoptosis by suppressing the expression of caspase 8, caspase 9 and cleaved caspase-3, as well as Bax/Bcl-2 ratio, down-regulating p38, ERK and JNK phosphorylation, and up-regulating Akt phosphorylation. These effects were significantly enhanced by inhibitor p-38 or ERK or JNK, and counteracted by inhibitor of PI3K. In addition, the extract of C. paliurus leaves also significantly improved hepatic steatosis, nephropathy and cardiac hypertrophy of diabetic mice. Taken together, these results provide the insight into the effects of C. paliurus leaves on pancreatic β cell preservation in standing glucolipotoxicity. Therefore, C. paliurus tea leaves may be used as a new remedy for diabetes through enhancing pancreatic β cell preservation by inhibiting β cell apoptosis.
Similar content being viewed by others
Introduction
Type 2 diabetes mellitus (T2DM) is a chronic metabolic disorder characterized by a persistent increase in blood glucose above normal values (hyperglycemia). It is estimated that by 2035, 471 million people in the world will be affected by this illness, and it is becoming a global public health concern due to its high morbidity and mortality1. Although many aspects of T2DM remain unclear, it is generally recognized that peripheral insulin resistance and pancreatic β cell failure are two major pathological changes during the progression of T2DM2. Normal pancreatic β cells have a compensation mechanism to up-regulate insulin secretion and/or β cell mass, which can maintain normoglycemia when insulin resistance occurs. Once the functional pancreatic β cell mass decreases and fails to compensate for insulin resistance, T2DM would be developed3, 4. Accordingly, enhancing β cell preservation represents a novel and important therapeutic strategy to prevent or treat T2DM.
In Traditional Chinese Medicine (TCM) system, T2DM is known as “Xiao-Ke-Zheng” whose core pathogenesis is “Yin deficiency and dryness-heat”, and bitter and cold TCMs are usually recommended to remove heat and invigorate Yin according to the TCM theory, have demonstrated good antidiabetic effects in vitro and in vivo, as well as in clinical practice5. Cyclocarya paliurus (Batal) IIjinskajia, an endemic plant belonging to Cyclocarya genus of the Juglandaceae family, mainly distributed in the southern of China6. The leaves of C. paliurus (CP) has long been used as a bitter TCM with the property of clearing heat and toxin to treat obesity and diabetes, which has also been historically used as an herbal tea in the folk7. Based on its property, in 1999, antihyperglycemic herbal tea processed by leaves of C. paliurus has been approved by the United States Food and Drug Administration (FDA) as a dietary supplement product7. Nowadays, the products derived from the leaves of C. paliurus have become a very popular health product in China6. It has been reported that the leaves of C. paliurus are composed of various active components including flavonoids, phenolic acids, triterpenoids, carbohydrates and sterols8. Pharmacological investigations revealed that the leaves of C. paliurus could decrease blood glucose and increase insulin level of diabetic rats induced by streptozotocin (STZ)9. However, its antihyperglycemic effects and underlying mechanisms have not been well documented.
In this study, we used biomedical approaches to investigate the antidiabetic activity of the leaves of C. paliurus, as well as its underlying mechanisms in STZ-induced diabetic mice fed with a high-fat diet. Our data show that the leaves of C. paliurus exert a potent hypoglycemic effect to attenuate high-fat diet-low dose STZ-induced experimental type 2 diabetes in mice through inhibiting pancreatic β cell apoptosis.
Results
Phytochemical characteristics of CP extract
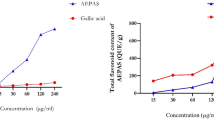
The extract of the leaves of C. paliurus was analyzed by UPLC obtaining the typical chromatogram (Supplementary Fig. 1). Compounds are identified in the chromatogram with peaks at 4.93 min to 1-caffeoylquinic acid, 7.00 min to 5-caffeoylquinic acid, 10 min to chlorogenic acid, 14.00 min to isoquercitrin, 16.00 min to kaempferol-3-glucoside, 17.00 min to kaempferol 3-rhamnoside, and 18.00 min to quercetin by comparison of the retention times (Rt) and ultraviolet (UV) absorption characteristics of external standards. As well, the contents of seven compounds in the extract of leaves of C. paliurus were measured by UPLC method and their contents were 1.4, 1.5, 4.0, 4.1, 1.6, 2.7 and 0.6 mg/g in the extract of leaves of C. paliurus, successively.
CP extract alleviates STZ and high fat diet-induced diabetes in mice
To explore the protective and therapeutic roles of CP extract on high-fat diet and low dose of STZ-induced diabetes, the CP extract was orally administrated to diabetic mice for 5 weeks. As shown in Supplementary Fig. 2A, the body weight of diabetic mice was continual deline from the initiation of treatment, whereas this reduction was reversed by CP extract treatment in a dose-dependent manner. At the end of 5 week treatment, the body weight of diabetic mice in high dose of CP extract-treated group was much higher than that of mice in diabetic model group with a significant statistical difference (P < 0.05) (Fig. 1A). In contrast, the food intake of diabetic mice was higher than that of non-diabetic mice, and also be rescued by CP extract- or glibenclamide treatment (Supplementary Fig. 2B). At checkpoint of 4 week after the initiation of treatment, the food intake of mice in CP extract- or glibenclamide treatment group was significantly lower than that of mice in diabetic group (P < 0.05) (Fig. 1B). As reported elsewhere, the mice treated with high-fat diet with low dose of STZ resulted in a drastic elevation of blood glucose level, and this elevation was continually restricted by CP extract or glibenclamide treatment (Supplementary Fig. 1C). At the end of 5 week treatment, the level of blood glucose in CP extract or glibenclamide-treated diabetic group was much lower than that of diabetic model group with significant statistical differences (P < 0.001)(Fig. 1C). To investigate the effects of CP extract on the development of diabetes, oral glucose tolerance test (OGTT) was conducted at checkpoint of 4 week after the initiation of CP extract treatment. As shown in Fig. 1D,E, after administration of glucose, the blood glucose levels of diabitic group significantly increased, as compared with non-diabetic groups, whereas the blood glucose levels of diabitic groups treated with CP extract- or glibenclamide decreased significantly. In addition, in the CP extract- or glibenclamide- treated diabitic groups, the areas under curves (AUCs) constructed from blood glucose levels were significantly decreased in comparison with that of diabitic group. These results suggested that CP extract has anti-hyperglycemic potential in high-fat diet-fed with low dose of STZ induced diabetic mice.
CP extract alleviates STZ and high fat-induced diabetes in mice. The type 2 diabetic mice were induced by feeding with high-fat diet for 4 weeks and then injecting intraperitoneally with 25 mg/kg STZ for 3 days consecutively. The diabetic mice with consecutive 7-day hyperglycemia (11 mmol/L or greater) were selected for the experiment and then CP extract or glibenclamide were administered to mice for consecutive 5 weeks. During the experiment, the body weight, food intake and blood glucose levels of mice were monitored weekly. The body weight on week 0 and 5 at checkpoint after the initiation of CP extract treatment respectively (A); The food intake on week 0 and 4 at checkpoint after the initiation of CP extract treatment respectively (B); The blood glucose levels on week 0 and 5 at checkpoint after the initiation of CP extract treatment respectively (C). The blood glucose levels (D) and the areas under curves (AUCs) constructed from blood glucose levels (E) of oral glucose tolerance test (OGTT) on week 4 at checkpoint after the initiation of CP extract treatment. The blood glucose levels in serum were determined by a glucometer (OMRON (China) Co., Ltd, Beijing, China). All data are presented as means ± SEM (n = 8). #p < 0.05, ##p < 0.01 and ###p < 0.001, diabetic model group compared with non-diabetic groups; *p < 0.05, **p < 0.01 and ***p < 0.001, compared with diabetic model group. CON: non-diabetic control group; CON-CP: CP extract-treated non-diabetic control group; MOD: diabetic model group; GLB: glibenclamide-treated diabetic group.
CP extract prevents pancreatic β cell mass decrease in diabetic mice
To explore how the CP extract helped resist hyperglycemia, the pancreas relative weight, histopathological changes of pancreas, and serum insulin were detected. As shown in Fig. 2A, drastically decreased pancreas relative weight was observed in diabetic mice vs. control groups (P < 0.05). After treatment of CP extract, the pancreas relative weight was significantly reversed (P < 0.05). Histological examination of pancreatic sections revealed that the islet/pancreas area ratio in diabetic mice was significantly decreased in comparison with controls. In CP extract- or glibenclamide-treated groups, those decreases were largely alleviated (P < 0.05 and P < 0.01, respectively) (Fig. 2C,D). Subsequently, determination of insulin level in the serum of mice treated with STZ and high fat diet exhibited a drastic decrease, compared to control groups (P < 0.001), but this was significantly rescued after CP extract or glibenclamide treatment (P < 0.05 and P < 0.01, respectively) (Fig. 2B). Simultaneously, immunofluorescent-staining showed that the insulin-producing β-cells in the control group occupied a majority of the islet area, whereas staining was drastically diminished by treatment of STZ with high fat diet. This reduction was also prominently attenuated by the administration of CP extract or glibenclamide (P < 0.05 and P < 0.01, respectively) (Fig. 2E,F). These results indicate CP extract can preserve pancreatic islet β-cell mass.
CP extract prevents pancreatic β cell mass decrease in diabetic mice. The type 2 diabetic mice were induced by feeding with high-fat diet for 4 weeks and then injecting intraperitoneally with 25 mg/kg STZ for 3 days consecutively. The diabetic mice with consecutive 7-day hyperglycemia (11 mmol/L or greater) were selected for the experiment and then CP extract or glibenclamide were administered to mice for consecutive 5 weeks. At the end of experiment, mice were sacrificed. The samples of blood and pancreas tissues were collected. (A) Relative weight of wet pancreas; (C) Histopathological examination of pancrease tissues (H & E staining) (magnification, 100×) and (E) Immunofluorescence (IF) analysis of insulin-positive cell using insulin marker (magnification, 600×). (B) Blood insulin levels; (D) Relative islets area in total pancreatic area; (F) Insulin-positive cell intensity. Blood insulin levels were assayed using commercially available kits (Wuhan Fine Biotech Co. Ltd, China). All data are presented as means ± SEM (n = 8). #p < 0.05, ##p < 0.01 and ###p < 0.001, diabetic model group compared with non-diabetic groups; *p < 0.05, **p < 0.01 and ***p < 0.001, compared with diabetic model group. CON: non-diabetic control group; CON-CP: CP extract-treated non-diabetic control group; MOD: diabetic model group; GLB: glibenclamide-treated diabetic group.
CP extract suppresses pancreatic β cell apoptosis in diabetic mice by modulating MAPK and Akt pathways
In the development of T2DM, pancreatic β cell apoptosis contributes to the loss of β cell mass10, we therefore detected β cell apoptosis in pancreatic tissues by TUNEL staining. As shown in Fig. 3A,B, the positive TUNEL staining signals in the pancreatic islets of diabetic mice were conspicuous, however, those signals were barely detected in the pancreatic islets of mice in the control group, indicating a major increase of apoptotic β cells in the pancreatic islets of diabetic mice. After treatment of CP extract or glibenclamide, positive TUNEL staining signals in the pancreatic islets of diabetic mice was significantly reduced (P < 0.001). Because caspase-3 activation has been implicated in pancreatic β cell apoptosis11, we also performed immunohistochemistry and Western blot analysis to detect cleaved active form of caspase-3. As compared with samples from the littermate control mice, the relative area of cleaved caspase-3-positive cells was significantly increased in pancreatic islet areas of the diabetic mice, whereas this increase was drastically diminished by treatment of CP extract or glibenclamide (P < 0.05) (Fig. 3C,D). As well, Western blot analysis also revealed that the expression of cleaved caspase-3 in pancreatic tissues of diabetic mice was robustly elevated, which was also significantly rescued after CP extract or glibenclamide treatment (P < 0.05 or P < 0.001). Consistent with elevated cleaved caspase-3, the expressions of apoptosis initiators caspase-8 and caspase-9, as well as Bax/Bcl-2 ratio in the pancreatic tissues of diabetic mice were significantly increased and those were significantly reversed in the presence of CP extract or glibenclamide (Fig. 4). Collectively, these results suggest a protective function of CP extract against apoptosis of pancreatic β cells.
CP extract suppresses pancreatic β cell apoptosis in diabetic mice. The type 2 diabetic mice were induced by feeding with high-fat diet for 4 weeks and then injecting intraperitoneally with 25 mg/kg STZ for 3 days consecutively. The diabetic mice with consecutive 7-day hyperglycemia (11 mmol/L or greater) were selected for the experiment and then CP extract or glibenclamide were administered to mice for consecutive 5 weeks. At the end of experiment, mice were sacrificed. The samples of pancreas tissues were collected. (A) TUNEL staining of mice pancreas tissues (magnification, 600×) and (C) Immunofluorescence analysis of cleaved caspase-3 expression in mice pancreas tissues (magnification, 600×); (B) The number of TUNEL-positive cells; (D) Cleaved caspase-3-positive area. All data are presented as means ± SEM (n = 8). #p < 0.05, ##p < 0.01 and ###p < 0.001, diabetic model group compared with non-diabetic groups; *p < 0.05, **p < 0.01 and ***p < 0.001, compared with diabetic model group. CON: non-diabetic control group; CON-CP: CP extract-treated non-diabetic control group; MOD: diabetic model group; GLB: glibenclamide-treated diabetic group.
CP extract suppresses Bax/Bcl-2 ratio, caspase-8, Caspase-9 and cleaved caspase-3 in pancrease tissues of diabetic mice. The type 2 diabetic mice were induced by feeding with high-fat diet for 4 weeks and then injecting intraperitoneally with 25 mg/kg STZ for 3 days consecutively. The diabetic mice with consecutive 7-day hyperglycemia (11 mmol/L or greater) were selected for the experiment and then CP extract or glibenclamide were administered to mice for consecutive 5 weeks. At the end of experiment, mice were sacrificed. The samples of pancreas tissues were collected. Protein expressions of Bcl-2, Bax, caspase-8, Caspase-9 and cleaved caspase-3 were determined in pancreas tissues using Western blot. (A) Representative image of Western blot; (B) Protein expressions of Bcl-2, Bax and Bax/Bcl-2 ratio; (C) Protein expressions of caspase-8, Caspase-9 and cleaved caspase-3. All data are presented as means ± SEM (n = 8). #p < 0.05, ##p < 0.01 and ###p < 0.001, diabetic model group compared with non-diabetic groups; *p < 0.05, **p < 0.01 and ***p < 0.001, compared with diabetic model group. CON: non-diabetic control group; CON-CP: CP extract-treated non-diabetic control group; MOD: diabetic model group; GLB: glibenclamide-treated diabetic group.
To identify whether Akt and mitogen-activated protein kinases are also involved in CP extract-induced pancreatic β cell protection, Western blot analysis was performed. As shown in Fig. 5, STZ and high fat induction resulted in drastic increases of ERK, JNK and p38 phosphorylation and a drastic decrease of Akt phosphorylation in pancreatic tissues of diabetic mice vs. non-diabetic mice, but those could significantly be reversed by CP extract or glibenclamide treatment, suggesting CP extract protects against pancreatic β cell apoptosis by modulating MAPK and Akt pathways.
CP extract suppresses MAPK signals and activates Akt signal in pancrease tissues of diabetic mice. The type 2 diabetic mice were induced by feeding with high-fat diet for 4 weeks and then injecting intraperitoneally with 25 mg/kg STZ for 3 days consecutively. The diabetic mice with consecutive 7-day hyperglycemia (11 mmol/L or greater) were selected for the experiment and then CP extract or glibenclamide were administered to mice for consecutive 5 weeks. At the end of experiment, mice were sacrificed. The samples of pancrease tissues were collected. Protein expressions of p-p38, p38, p-ERK, ERK, p-JNK, JNK, p-Akt and Akt were determined in pancreas tissues using Western blot. (A) Representative image of Western blot; (B) Protein expressions of p-p38, p-ERK, p-JNK and p-Akt in pancreas tissues. (C) Protein expressions of p38, ERK, JNK, and Akt in pancreas tissues. All data are presented as means ± SEM (n = 8). #p < 0.05, ##p < 0.01 and ###p < 0.001, diabetic model group compared with non-diabetic groups; *p < 0.05, **p < 0.01 and ***p < 0.001, compared with diabetic model group. CON: non-diabetic control group; CON-CP: CP extract-treated non-diabetic control group; MOD: diabetic model group; GLB: glibenclamide-treated diabetic group.
CP extract suppresses pancreatic β cell apoptosis in vitro by modulating MAPK and Akt pathways
To further explore the mechanism of CP extract-induced pancreatic β cell protection, we developed an in vitro apoptosis model of pancreatic β cells by stimulating NIT-1 cells (a pancreatic β cell line) with STZ. After STZ treatment, the cells exhibited a high apoptosis rate and 32 μM STZ was selected as the working concentration, which resulted in 30.9% cell death (Supplementary Fig. 3A). As well, cells were exposed to different concentrations of CP extract (0, 1, 25, 50, 100, 200, 500 μg/mL) for 24 h and exhibited no significant cytotoxicity to NIT-1 cells (Supplementary Fig. 3B). Then, the dose-response assay of CP extract was performed on STZ-induced NIT-1 cells.
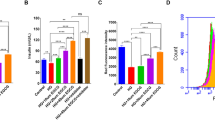
As shown in Fig. 6A, pretreatment with CP extract (50–200 μg/mL) could significantly inhibit cell death induced by STZ in a dose-dependent manner. To quantitatively examine the effect of CP extract on STZ-induced NIT-1 cell apoptosis, the percentage of apoptotic cells was detected by Annexin V/PI double staining methods. As shown in Fig. 6B,C, the percentage of apoptotic cells was significant increased after 32 μM STZ treatment, and pretreatment with CP extract (50, 100, 200 μg/mL) significantly reduced the percentage of apoptotic cells in a dose-dependent manner in comparison with the cells treated with STZ alone. Activation of caspases is responsible for apoptosis execution11. As shown in Fig. 6D–F, the expression of caspase-8, caspase-9, cleaved caspase-3 and Bax/Bcl-2 ratio was markedly up-regulated after STZ treatment. In contrast, pretreatment with CP extract significantly inhibited the up-regulation of caspase-8, caspase-9, cleaved caspase-3 and Bax/Bcl-2 ratio. To confirm Akt and MAPK kinases are also involved in CP extract-induced pancreatic β cell protection, Western blot analysis was performed. As shown in Fig. 7A–C, treatment with STZ resulted in a significant increase of phosphorylated p38, ERK and JNK and a drastic decrease of phosphorylated Akt, but have no change on total p38, ERK, JNK and Akt. As expected, increased phosphorylation of p38, JNK and ERK, as well as decreased phosphorylation of Akt were significantly rescued by CP extract with a positive dose-dependent relationship. To furter confirm the role of CP extract in regulation of MAPK and Akt signaling pathways, NIT-1 cells were treated with inhibitor of PI3K (LY294002) and/or ERK (FR180204) and/or p-38 (PD169316) and/or JNK (SP600125), respectively. As expected, the cell viability of STZ-treated NIT-1 cells treated with CP extreat in combination of PD169316 or FR180204 or SP600125, were much higher than that of CP extreat treatment alone, whereas the cell viability of STZ-treated NIT-1 cells treated with CP extreat in combination of LY294002 was much lower than that of CP extreat treatment alone (Fig. 7D). These data demonstrate that the protective effect of CP extract on STZ-induced apoptosis in NIT-1 cells is mediated by modulating MAPK and Akt signaling pathways.
CP extract prevents STZ-induced pancreatic β cell apoptosis in NIT-1 cells. NIT-1 cells were preincubated with CP extract (50, 100 and 200 μg/mL) for 2 h before 32 mM STZ treated for 24 h. (A) Cell viability was assessed by MTT assay. (B and C) The apoptotic cells were stained with annexin V-FITC and PI, and then detected by flow cytometry. (D–F) Cells were lysed and then the expression of Bcl-2, Bax, caspase-8, Caspase-9 and cleaved caspase-3 were measured using Western blot. Data were expressed as mean ± SEM from three independent experiments. ###p < 0.001, compared with untreated control group; *p < 0.05, compared with STZ-treated group.
CP extract suppresses MAPK signals and activates Akt signal in STZ-induced NIT-1 cells. NIT-1 cellswere preincubated with CP extract (50, 100 and 200 μg/mL) for 2 h before 32 mM STZ treated for 24 h. Cells were lysed and then the expression of proteins in MAPK and Akt signaling pathways were measured using Western blot. (A) Representative image of Western blot; (B and C) Protein expressions of p-p38, p38, p-ERK, ERK, p-JNK, JNK, p-Akt and Akt in NIT-1 cells. (D) NIT-1 cells were preincubated with CP extract (100 μg/mL) or PI3K inhibitor (LY294002, 1.25 μM) or ERK inhibitor (FR180204, 1.25 μM) or p-38 inhibitor (PD169316, 1.25 μM) or JNK inhibitor (SP600125, 1.25 μM) or combnation of both CP extract and LY294002 or FR180204 or PD169316 or SP600125 for 2 h before 32 mM STZ treated for 24 h, then the cell viability was assessed by MTT assay. Data were expressed as mean ± SEM from three independent experiments. ###p < 0.001, compared with untreated control group; *p < 0.05, compared with STZ-treated group; $p < 0.05 and $$p < 0.01, compared with STZ + CP extract group using Student’s t-test.
CP extract reduces diabetes-related complications in diabetic mice
Chronic hyperglycemia can cause many major health complications, such as renal disease, hepatopathy and heart disease. We also detected the protective effects of CP extract on the liver, kidney and heart of diabetic mice. As shown in Fig. 8, histological examination displayed amount of large and small vesicles of fat accumulating within hepatocytes, a typical pathological feature of hepatic steatosis, in the liver sections (Fig. 8A); and a thicker glomerular basement membrane in the kidney section (Fig. 8C), as well as observable cardiomyocyte hypertrophy in heart section (Fig. 8E,F) of diabetic mice, in comparison with samples from non-diabetic mice. After supplementation of CP extract or glibenclamide, the hepatic steatosis, glomerular basement membrane thicken and cardiac hypertrophy were greatly improved. In parallel, the data showed the heart/body weight ratio of mice in diabetic mice was higher than that of non-diabetic mice, and this rise was largely suppressed after CP extract or glibenclamide adminstration (P < 0.05)(Fig. 8F). Subsequently, we detected the blood biochemical changes of mice and showed that the levels of AST, ALT, CREA, TG, TCHO and LDL/VLDL in the serum of diabetic mice were markedly elevated, whereas HDL in the serum of diabetic mice were significantly decreased vs. those in mice of non-diabetic mice. And those elevations or decline were significantly rescued by CP extract treatment in a dose-dependent manner (Fig. 9). Collectively, these data displayed a potent beneficial effect of CP extract in prevention of diabetic complications such as hepatic steatosis, nephropathy and cardiac hypertrophy.
CP extract reduces chronic hyperglycemia-induced damages in liver, kidney and heart of diabetic mice. The type 2 diabetic mice were induced by feeding with high-fat diet for 4 weeks and then injecting intraperitoneally with 25 mg/kg STZ for 3 days consecutively. The diabetic mice with consecutive 7-day hyperglycemia (11 mmol/L or greater) were selected for the experiment and then CP extract or glibenclamide were administered to mice for consecutive 5 weeks. At the end of experiment, mice were sacrificed. The samples of liver, kidney and heart tissues were collected. Histopathological examination of liver (A), kidney (C) and heart tissues (E) (H & E staining) (magnification, 100×); Relative weight of wet liver (B), kidney (D) and heart tissues (F). All data are presented as means ± SEM (n = 8). #p < 0.05, ##p < 0.01 and ###p < 0.001, diabetic model group compared with non-diabetic groups; *p < 0.05 and **p < 0.01, compared with diabetic model group. CON: non-diabetic control group; CON-CP: CP extract-treated non-diabetic control group; MOD: diabetic model group; GLB: glibenclamide-treated diabetic group.
The effects of CP extract on the blood biochemical changes of diabetic mice. The type 2 diabetic mice were induced by feeding with high-fat diet for 4 weeks and then injecting intraperitoneally with 25 mg/kg STZ for 3 days consecutively. The diabetic mice with consecutive 7-day hyperglycemia (11 mmol/L or greater) were selected for the experiment and then CP extract or glibenclamide were administered to mice for consecutive 5 weeks. At the end of experiment, mice were sacrificed. The samples of blood were collected and relevant blood biochemicals in serum were measured by using corresponding commercially available kits. Blood (A) ALT, (B) AST, (C) ALP, (D) CREA, (E)TG, (F) TCHO, (G) LDL and (H) HDL levels. All data are presented as means ± SEM (n = 8). #p < 0.05, ##p < 0.01 and ###p < 0.001, diabetic model group compared with non-diabetic groups; *p < 0.05, **p < 0.01 and ***p < 0.001, compared with diabetic model group. CON: non-diabetic control group; CON-CP: CP extract-treated non-diabetic control group; MOD: diabetic model group; GLB: glibenclamide-treated diabetic group.
Discussion
Current research in diabetes reveals that insufficient insulin secretion due to β cell loss is the common and major component in the pathogenesis of diabetes, and a significant reduction in pancreatic β cell populations is the primary mechanisms for β cell loss1, 12. Inhibiting pancreatic β cell apoptosis thus represent a potential strategy to combat diabetes and its complications. In the present study, we explored the protective role of C. paliurus tea leaves on pancreatic β cells. Our data consistently revealed that CP extract exhibit a potential anti-hyperglycemic effect in diabetic mice and has obvious protective effects against the apoptosis of pancreatic β cells, in agreement with previous studies demonstrating that C. paliurus is benefcial to diabetics. Our data support a clear antidiabetic effect of C. paliurus tea leaves through regulating β cell preservation by protection against pancreatic β cell apoptosis.
To characterize the antidiabetic effect of CP extract in vivo, high-fat diet with low dose of STZ-induced type 2 diabetic mice were enrolled in the study. It is well known that high-fat diet would lead to insulin resistance and/or glucose intolerance, and the subsequent administration of multiple low dose of STZ, a β cell toxin, would result in a severe reduction in functional β cell mass13,14,15. Based on this model, we oral administration of CP extract to the diabetic mice and accessed its therapeutic effect. Our findings demonstrate the body loss, food intake and serum plasma glucose levels were significantly decreased in the CP extract-treated groups, while the wet pancreas/body weight ratio, serum plasma insulin levels, β-cell area and insulin-producing β cells were markedly increased, which are in line with our findings that TUNEL-positive cells, the expression of caspase-8, caspase-9 and cleaved caspase-3 in the islets of CP extract -treated group were lower than those of diabetic model group. NIT-1, a pancreatic cell line, showed many characteristics and ultrastructural features of normal differentiated mouse pancreatic β cells16. Using this cell line, we also developed in vitro apoptosis model of pancreatic β cells by challenging with STZ. Our results showed that CP extract could significantly reduce the percentage of apoptotic cells, as well as inhibit the up-regulation of cleaved caspase-3 and caspase-9 induced by STZ in a dose-dependent manner. Collectively, those data reveal potential antidiabetic effect of C. paliurus tea through protecting against pancreatic β cell apoptosis.
Kinase signaling pathways are regulated in response to various extracellular physical (e.g., UV radiation, and temperature) and chemical (many agents) stimuli. They can be involved, depending on cell type, in the regulation of many cellular processes such as proliferation, differentiation, inflammatory response, autophagy, senescence, and also in apoptosis. Šrámek J. et al. reviewed that Akt kinases and kinases in MAPK superfamily such as ERKs, JNK and p38, play important roles in regulating apoptosis of pancreatic β cells17. We further explored whether the Akt, p38, ERK, and JNK signaling pathways in pancreas islets of diabetic mice can be influenced by the treatment of CP extract. Our data showed that treatment with CP extract significantly suppressed ERK, JNK and p38 phosphorylation, and increased Akt phosphorylation in pancreatic tissues of diabetic mice. In line with results from in vivo, treatment of CP extract is effective to suppress the increased ERK, JNK and p38 phosphorylation, and elevate the decreased Akt phosphorylation in NIT-1 cells, which are induced by STZ, in a dose-dependent manner. In vitro study also showed that ERK, JNK and p38 inhibitors could greatly enhance, whereas PI3K inhibitor could significantly weaken the protective effect of CP extract against STZ-induced apoptosis. These findings suggest that CP extract protects pancreatic β cells from apoptosis via affecting MAPK and Akt signaling pathways.
It is well known that chronic hyperglycemia may lead to multi-organ damage through activating different mechanisms such as an increased polyol pathway, advanced-glycation end product formation, activation of Protein Kinase C and hexosamine pathway, resulting in overproduction of reactive oxygen species to impair various tissues18. These associated lesions of diabetes are termed as diabetic complications. Based on the tissue affected, these complications are named accordingly as diabetic hepatopathy, diabetic nephropathy, and diabetic cardiomyopathy, etc. Hepatic steatosis is a typical pathological feature of diabetic hepatopathy with abnormalities in lipid metabolism19. The alterations in the plasma lipid profile (elevated triglycerides, total cholesterol, LDL/VLDL; and reduced HDL) and liver injury markers (elevated AST, ALT and ALP) of the diabetic mice in this study are in agreement with the alterations of high-fat diet with low dose of STZ induced type 2 diabetic mice reported by other researchers20, 21. The decrease in the pathological changes on hepatic steatosis and levels of AST, ALT, TG, TCHO and LDL/VLDL in plasma, as well as an increase of plasma HDL in the diabetic mice fed CP extract-supplemented diets, in comparison with the diabetic model group indicates a potent hepatoprotective effect of CP extract. Diabetic nephropathy is another complication of diabetes, which begins with glomerular hyperfiltration caused by hyperglycemia, and further results in glomerular hypertrophy and glomerular basement membrane thickening22. Our data showed CP extract is also effective to improve the nephropathy of diabetic mice evidenced by decreasing glomerular basement membrane thickening, reducing the wet kidney/body weight ratio and lowering the level of plasma CREA. In the myocardium, chronic hyperglycemia can cause cardiac hypertrophy directly23. As well, compared to diabetic model group, the decrease in both the pathological changes on cardiac hypertrophy and wet heart/body weight ratio in CP extract-treated diabetic mice also indicates cardioprotective potential of CP extract. Collectively, these data suggest that CP extract plays a beneficial role in protection against diabetes-related complications hepatic steatosis, nephropathy and cardiac hypertrophy or inhibit their development.
In summary, CP extract exhibit a potential anti-hyperglycemic effect in high-fat diet with low dose of STZ-induced type 2 diabetic mice, and protecting against diabetes-related complications. Those effects are associated with protecting pancreatic β cells from apoptosis via modulating MAPK and Akt signaling pathways.
Materials and Methods
Preparation of CP extract
The leaves of Cyclocarya paliurus (Batal.) Iljinskaja were collected in the garden of Nanjing Forestry University, China (Nanjing, Jiangsu, China) in March, 2015. The sample was authenticated by Prof. Hu biao Chen of School of Chinese Medicine, Hong Kong Baptist University, and voucher specimens (No. CP20151201) was stored in our Research Laboratory, School of Chinese Medicine, Hong Kong Baptist University, Hong Kong. For preparation of the extract of C. paliurus leaves (CP extract), the air-dried leaves of C. paliurus (5 Kg) were boiled with water (60 L water for the first time and 50 L water for the second time) for twice (boiled 2 h for the first time and boiled 1 h for the second time). The extract was then concentrated and dried under reduced pressure to yield the crude extract (830 g). The residue was stored at 4 °C, and the desired dose was reconstituted in 0.5% CMC-Na solution.
Phytochemical analysis
The powder of CP extract was extracted twice for 30 min each time by ultrasound in 70% methanol (1:10, w/v). After being filtered and combined, the filtrate was passed through a 0.22 μm membrane before using for Ultra Performance Liquid Chromatography (UPLC) analysis. The chromatographic analysis was performed on a Waters ACQUITY UPLC system equipped with an auto sampler, binary gradient pump, and PDA detector, connected to an Empowder ChemStation software (Waters, MA, USA). The system was operated at 30 °C and a water ACQUITY UPLC HSS T3 column (150 × 2.1 mm, 1.7 μm) was used. The injection volume was 5 μL and the mobile phase flow rate was 0.4 mL/min. Solvents that constituted the mobile phase were (A) 0.2% aqueous acetic acid and (B) acetonitrile. The elution conditions were as follows: 0–5 min, linear gradient 2–5% B; 5–10 min, linear gradient 5–10% B; 10–15 min, linear gradient 10–25% B; 15–25 min, linear gradient 25–40% B; 25–28 min, linear gradient 40–90% B. Peaks were detected at 254 nm.
Animals and experimental procedures
Male C57/BL6J mice of 8-week-old were purchased from the Laboratory Animal Services Center, The Chinese University of Hong Kong. The animals were fed a standard rodent diet with free access to water, and were kept in rooms maintained at 22 ± 1 °C with a 12 h light/dark cycle following international recommendations. All experimental protocols were approved by the Animal Ethics Committees of Hong Kong Baptist University, in accordance with “Institutional Guidelines and Animal Ordinance” (Department of Health, Hong Kong Special Administrative Region) (Registration No. LIUYE/15-16/01-CLNC).
The inducement of diabetic animals was carried out according to a previous reported procedure24. In brief, the animals were fed with high-fat diet (Adjusted Calories Diet (42% from fat) (No. 881372)) (Harlan Laboratories, Inc, IN Indianapolis, USA) for 4 weeks before consecutive intraperitoneal (i.p) injection with 25 mg/kg streptozotocin (STZ, Sigma-Aldrich, St. Louis, MO, USA) for 3 days. An equal volume of vehicle was injected into the control mice. The blood glucose levels in serum were determined by a glucometer (OMRON (China) Co., Ltd, Beijing, China). The mice with fasting glucose level higher than 11 mmol/L were considered as diabetic mice, and the diabetic mice with consecutive 7-day hyperglycemia (11 mmol/L or greater) were used for the experiment. The diabetic mice were randomly divided into five groups: diabetic group, glibenclamide-treated diabetic group, low dose of CP extract-treated diabetic group, medium dose of CP extract-treated diabetic group, and high dose of CP extract-treated diabetic group. The untreated mice were matched in age and divided into two groups: vehicle control group and CP extract-treated control group. For the treatment, CP extract was orally administrated to diabetic mice at doses of 1, 2, 4 g/kg/day according to the result of preliminary experiment. Glibenclamide (Sigma-Aldrich, St. Louis, MO, USA) was used as a reference positive agent and it was given at 15 mg/kg/day according to literature25. CP extract-treated control group was given CP extract at a dose of 2 g/kg/day, whereas the vehicle control group and diabetic model group were orally fed with the same volume of 0.5% CMC-Na solution instead of CP extract or glibenclamide. Both CP extract and glibenclamide were freshly dissolved in 0.5% CMC-Na solution respectively and orally administrated to the mice for 5 weeks after the onset of treatment. Body weight, food consumption and blood glucose levels in each mice were monitored every 7 days. Blood samples were obtained from the tail vein of the mice and blood glucose levels in serum were determined by a glucometer (OMRON (China) Co., Ltd, Beijing, China).
Glucose tolerance test (GTT)
The glucose tolerance test (GTT) was carried out after 4 weeks of treatment. Mice were oral administrated with 2 g/kg body weight of D-glucose (Sigma-Aldrich, St. Louis, MO, USA) after 16 h fast. Blood samples were taken from the tail vein of the mice at 0, 30, 60, 90 and 120 min after glucose administration, respectively. The GTT was carried out on awake mice without anesthetization. The glucose levels in serum were also determined by a glucometer (OMRON (China) Co., Ltd, Beijing, China).
Blood biochemical analysis and tissue preparation
At the end of the experiment, mice were sacrificed and blood samples were obtained from the abdominal vein with a microsyringe. Serum was separated at 3000 rpm for 15 min. Blood insulin, high-density lipoprotein cholesterol (HDL) and low-density and very low lipoprotein cholesterol (LDL/VLDL) levels, AST, ALT, ALP, TG, TCHO and CREA were measured in a biochemical analyzer (Hitachi 902 Automatic Analyzer; Hitachi, Japan) with adapted reagents from Shanghai Kehua Bio-engineering Co., Ltd (Shanghai, China). As well, pancreas, liver, kidney and heart were immediately separated and collected.
Histological analysis
Pancreas, liver, kidney and heart tissues were post-fixed in 4% PFA for 24 hr and sectioned after embedding in paraffin. The sections were prepared and stained with H&E using standard procedures. All slides in the current study were examined under a light microscope (Olympus BX51, Olympus Co., Tokyo, Japan) and photographed at high resolution with a digital camera (Olympus C-5050, Olympus Co., Tokyo, Japan) unless otherwise noted.
Immunoblotting
Immunoblotting was performed as previously described26. Briefly, proteins were extracted from the pancreas tissues and NIT-1 cells in the presence of a cocktail of protease inhibitors and phenylmethylsulfonyl fluoride (PMSF) (Roche Applied Science, Branford, CT, USA), resolved and separated by 12–15% SDS-PAGE, and transferred to PVDF membranes. The membranes were then probed with the primary antibodies caspase-8, caspase-9, cleaved caspase-3, Bax, Bcl-2, ERK, JNK, p38, p-ERK, p-JNK,p-p38, Akt, p-Akt and β-actin (Cell Signaling Technology, Inc. Beverly, MA, USA), followed by incubation with the corresponding horseradish peroxidase-conjugated secondary antibodies. The protein bands were visualized with enhanced chemiluminescence reagents (GE Healthcare Bio-Sciences Corp, Piscataway, NJ, USA), detected using the ECL system, and quantifed using NIH ImageJ sofware (National Institutes of Health, Bethesda, Maryland, USA).
Immunohistochemistry and immunofluorescence
In Situ Cell Apoptosis Detection Kit (Millipore, Danvers, MA, USA) was used to evaluate the β cell apoptosis in pancreas following the manufacturer’s instructions. Briefly, the sections were heated at 60 °C for 2 h, followed by deparaffinization and rehydration. Then the sections of pancreas were treated with proteinase K for 5 min at room temperature, and washed twice with PBS. After incubation with 60 μl TUNEL reaction mixture (Label Solution and Enzyme Solution; 5:1) following the manufacturer’s recommendations, for 60 min at 37 °C without light, then the slides sections were incubated with the prediluted anti-digoxin antibody, followed with ABC for 30 min. Apoptotic cells were detected by incubation with the 3,3-diaminobenzidine (DAB) chromogen.
For immunofluorescence staining, sections were permeabilized in PBS with 0.1% Triton X-100 for 10 min after deparaffinized and rehydrating. Then the blocking was performed using PBS with 5% normal goat serum for 1 h at room temperature, followed by incubation with rabbit anti-insulin antibody and mouse anti-cleaved caspase-3 antibody (Cell Signaling Technology, Danvers, MA, USA) diluted 1:100 at 4 °C overnight. Three consecutive washes with PBS for 5 min each were followed by sequential incubation with Alexa Fluor 595 and 488 goat anti-rabbit and anti-mouse IgG secondary antibodies (1:200) at room temperature for 1 h. The slides were washed three times with PBS and mounted using an anti-fade mounting medium containing 4′,6-diamidino-2-phenylindole (DAPI) (Vector Laboratories, Burlingame, CA, USA). Images were captured under a fluorescence microscope (Carl Zeiss AG; Oberkochen, Germany).
Cell Culture
NIT-1 cells were obtained from American Type Tissue Culture Collection (passage 40–60) and cultured under an atmosphere of 5% CO2 and 95% O2 at 37 °C in RPMI 1640 medium (Gibco Chemical, USA) containing 10% (v/v) fetal bovine serum (FBS), 11.1 mM glucose, 100 U/mL penicillin, and 0.1 mg/mL streptomycin.
Cell viability assay and flow cytometry
Cell viability assay was determined by MTT method, the live cell number was determined using a microplate reader based on absorbance values. Relative cell apoptosis was measured by flow cytometry (Becton Dickinson, San Jose, CA, USA)using Annexin V-FITC Apoptosis Detection Kit (eBioscience, Bender MedSystems, GmbH, Vienna, Austria).
Statistical analysis
All data were analyzed with GraphPad PRISM 5.0 (GraphPad Software Inc., San Diego, CA, USA) sofware using one-way ANOVA, followed by Duncan’s multiple range tests unless otherwise noted. All quantitative values are expressed as the mean ± SEM. Differences were deemed signifcant when P < 0.05.
Change history
04 November 2020
An amendment to this paper has been published and can be accessed via a link at the top of the paper.
References
Jiang, H. et al. The Soybean Peptide Vglycin Preserves the Diabetic beta-cells through Improvement of Proliferation and Inhibition of Apoptosis. Sci Rep 5, 15599 (2015).
Lakshmipathi, J. et al. PKCζ Is Essential for Pancreatic β-Cell Replication During Insulin Resistance by Regulating mTOR and Cyclin-D2. Diabetes 65, 1283–1296 (2016).
Brereton, M. F. et al. Hyperglycaemia induces metabolic dysfunction and glycogen accumulation in pancreatic beta-cells. Nat Commun 7, 13496 (2016).
Avall, K. et al. Apolipoprotein CIII links islet insulin resistance to beta-cell failure in diabetes. Proc Natl Acad Sci USA 112, E2611–2619 (2015).
Huang, M. et al. Antidiabetic activity of perylenequinonoid-rich extract from Shiraia bambusicola in KK-Ay mice with spontaneous type 2 diabetes mellitus. J Ethnopharmacol 191, 71–81 (2016).
Xie, J. H. et al. Extraction, chemical composition and antioxidant activity of flavonoids from Cyclocarya paliurus (Batal.) Iljinskaja leaves. Food Chem 186, 97–105 (2015).
Ma, Y. et al. Antihyperlipidemic effect of Cyclocarya paliurus (Batal.) Iljinskaja extract and inhibition of apolipoprotein B48 overproduction in hyperlipidemic mice. J Ethnopharmacol 166, 286–296 (2015).
Gao, Y., He, C., Bi, W., Wu, G. & Altman, E. Bioassay Guided Fractionation Identified Hederagenin as a Major Cytotoxic Agent from Cyclocarya paliurus Leaves. Planta Med 82, 171–179 (2016).
Wang, Q. et al. Antihyperglycemic, antihyperlipidemic and antioxidant effects of ethanol and aqueous extracts of Cyclocarya paliurus leaves in type 2 diabetic rats. J Ethnopharmacol 150, 1119–1127 (2013).
Ardestani, A. & Maedler, K. MST1: a promising therapeutic target to restore functional beta cell mass in diabetes. Diabetologia 59, 1843–1849 (2016).
Fernandez-Millan, E. et al. Cocoa-rich diet attenuates beta cell mass loss and function in young Zucker diabetic fatty rats by preventing oxidative stress and beta cell apoptosis. Mol Nutr Food Res 59, 820–824 (2015).
Tomita, T. Apoptosis in pancreatic beta-islet cells in Type 2 diabetes. Bosn J Basic Med Sci 16, 162–179 (2016).
Skovsø, S. Modeling type 2 diabetes in rats using high fat diet and streptozotocin. J Diabetes Investig 5, 349–358 (2014).
Zhang, Y. et al. Lentinan protects pancreatic beta cells from STZ-induced damage. J Cell Mol Med 20, 1803–1812 (2016).
Irondi, E. A., Oboh, G. & Akindahunsi, A. A. Antidiabetic effects of Mangifera indica Kernel Flour‐supplemented diet in streptozotocin‐induced type 2 diabetes in rats. Food Sci Nutr 4, 828–839 (2016).
Lei, H. et al. Effects of sesamin on streptozotocin (STZ)-induced NIT-1 pancreatic beta-cell damage. Int J Mol Sci 13, 16961–16970 (2012).
Sramek, J., Nemcova-Furstova, V. & Kovar, J. Kinase Signaling in Apoptosis Induced by Saturated Fatty Acids in Pancreatic beta-Cells. Int J Mol Sci 17 (2016).
Adeshara, K. A., Diwan, A. G. & Tupe, R. S. Diabetes and Complications: Cellular Signaling Pathways, Current Understanding and Targeted Therapies. Curr Drug Targets 17, 1309–1328 (2016).
Kong, Q. et al. Tangshen formula attenuates hepatic steatosis by inhibiting hepatic lipogenesis and augmenting fatty acid oxidation in db/db mice. Int J Mol Med 38, 1715–1726 (2016).
Li, Y. G., Ji, D. F., Zhong, S., Lin, T. B. & Lv, Z. Q. Hypoglycemic effect of deoxynojirimycin-polysaccharide on high fat diet and streptozotocin-induced diabetic mice via regulation of hepatic glucose metabolism. Chem Biol Interact 225, 70–79 (2015).
Kusunoki, M. et al. Lipoprotein lipase activator NO-1886 improves fatty liver caused by high-fat feeding in streptozotocin-induced diabetic rats. Metabolism 53, 260–263 (2004).
Gnudi, L. Angiopoietins and diabetic nephropathy. Diabetologia 59, 1616–1620 (2016).
Ku, P. M. et al. Molecular role of GATA binding protein 4 (GATA-4) in hyperglycemia-induced reduction of cardiac contractility. Cardiovasc Diabetol 10, 57 (2011).
Xue, J., Ding, W. & Liu, Y. Anti-diabetic effects of emodin involved in the activation of PPARgamma on high-fat diet-fed and low dose of streptozotocin-induced diabetic mice. Fitoterapia 81, 173–177 (2010).
Juarez-Reyes, K. et al. Hypoglycemic, antihyperglycemic, and antioxidant effects of the edible plant Anoda cristata. J Ethnopharmacol 161, 36–45 (2015).
Walker, J. et al. Nonivamide, a capsaicin analogue, exhibits anti-inflammatory properties in peripheral blood mononuclear cells and U-937 macrophages. Mol Nutr Food Res 61 (2017).
Acknowledgements
This work was supported by grants from Kong Baptist University Research Grant (No. LIUYE/15-16/01-CLNC) and Shenzhen Science and Technology Innovation Committee Grant (No. JCYJ20140419130444178).
Author information
Authors and Affiliations
Contributions
Z.X. Bian conceived of and designed the study. H.T. Xiao, B. Wen, C.Y. Lin, H.X. Mu and C.H. Liao performed the cell and animal experiments. Z.W. Ning and L.X. Zhai performed phytochemical analysis. H.T. Xiao and B. Wen performed the statistical analysis. Z.X. Bian and H.T. Xiao finalized the manuscript. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Competing Interests
The authors declare that they have no competing interests.
Additional information
Publisher's note: Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made. The images or other third party material in this article are included in the article’s Creative Commons license, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons license and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this license, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Xiao, Ht., Wen, B., Ning, Zw. et al. Cyclocarya paliurus tea leaves enhances pancreatic β cell preservation through inhibition of apoptosis. Sci Rep 7, 9155 (2017). https://doi.org/10.1038/s41598-017-09641-z
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41598-017-09641-z
This article is cited by
-
Functional characterization of genes related to triterpene and flavonoid biosynthesis in Cyclocarya paliurus
Planta (2024)
-
Simultaneous UPLC–TQ-MS/MS determination of six active components in rat plasma: application in the pharmacokinetic study of Cyclocarya paliurus leaves
Chinese Medicine (2019)
-
Role of medicinal plants in the management of diabetes mellitus: a review
3 Biotech (2019)
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.