Abstract
A widespread epidemic of Zika fever, caused by Zika virus (ZIKAV) has spread throughout the Pacific islands, the Americas and Southeast Asia. The increased incidences of ocular anomalies observed in ZIKAV-infected infants and adults may be associated with the rapid spread of ZIKAV. The objective of this study was to check if ZIKAV could be detected in human tears after the first week of infection. Twenty-nine patients with PCR confirmed ZIKAV infection during the Singapore August 2016 ZIKAV outbreak were enrolled for the study. Detection and quantification of ZIKAV RNA was performed on conjunctival swabs collected from both eyes of these patients at the late convalescent phase (30 days post-illness). Efficiency of viral isolation from swab samples was confirmed by the limit of detection (as low as 0.1 PFU/µL, equivalent to copy number of 4.9) in spiked swabs with different concentrations of ZIKAV (PFU/µL). Samples from three patients were found positive by qRT-PCR for ZIKAV and the viral RNA copy numbers detected in conjunctival swabs ranged from 5.2 to 9.3 copies respectively. ZIKAV could persist in the tears of infected patients for up to 30 days post-illness, and may therefore possess a potential public health risk of transmission.
Similar content being viewed by others
Introduction
Zika virus (ZIKAV) is a mosquito-borne flavivirus which was first isolated in 1947 from a sentinel rhesus macaque in Uganda1. ZIKAV has remained in relative obscurity for nearly 60 years until the unprecedented 2007 outbreak in the Western Pacific island of Yap Federated States of Micronesia2. This was then followed by a larger epidemic in French Polynesia in 2013 and 20143. Subsequent smaller outbreaks occurred in the Pacific islands from 2014 to 20164. ZIKAV was introduced into Brazil in 2015, and within that year, it spread rapidly throughout the Americas5, 6. Reports of imported and autochthonous ZIKAV infections have also been observed in South East Asia7 where arboviral diseases are very common8, 9. Singapore reported its first case of local ZIKAV transmission on 27 August 201610.
ZIKAV infection is rarely life threatening, manifesting typically as short-lived fever, nonspecific rash, and joint pain, with many patients being completely asymptomatic2, 11. However the re-emergence of ZIKAV has been associated with severe neurological complications: Guillain-Barré syndrome (GBS) in French Polynesia12, 13 and microcephaly in Brazil14,15,16. Although the full extent of ZIKAV ophthalmologic manifestations is unclear, ocular developmental anomalies have been reported in infants with microcephaly in Brazil11, 17,18,19. To date, two cases of ZIKAV-associated uveitis in adult patients have also been reported20, 21. The occurrence of uveitis suggests a non-infective inflammatory response to systemic or ocular infection with ZIKAV, or it could actually represent an actual viral infection such as choroiditis or vitritis. In an earlier report from China, ZIKAV was found on swabs from the conjunctiva (superficial mucosa covering the globe)22. However, it was unclear if ZIKAV could be localized after the first week of infection.
In this report, we describe the detection of ZIKAV RNA from conjunctival swab samples of laboratory-confirmed ZIKAV cases collated during the 2016 ZIKAV outbreak in Singapore.
Methods
Participants
This study included conjunctival swab samples obtained from patients admitted to the Communicable Disease Centre at Tan Tock Seng Hospital from 29th August to 15th November 2016. Conjunctival samples were collected from both eyes of study subjects by pulling the lower eyelid down and drawing the tip of the sterile swab (FLOQSwabs®, Copan Flock Technologies, Brescia, Italy) gently across the inside of the lower eyelid, at visit 3 which was at day 30 post-illness. Samples were processed on the same day of collection and stored at −80 °C until use. These patients were previously confirmed to be ZIKAV-infected by quantitative reverse-transcription polymerase chain reaction (qRT-PCR) performed on serum and/or urine samples obtained during their first visit to the clinic23, 24.
Standard Protocol Approvals, Registrations and Patient Consents
Written informed consent was obtained from all participants in accordance with the tenets of the declaration of Helsinki for human research. The study protocol was approved by the SingHealth Centralized Institutional Review Board (CIRB Ref: 2016/2219) and National Healthcare Group Institutional Review Board.
Virus Isolate
The ZIKAV strain H/PF/2013 used in this study was originally isolated from a French patient returning from French Polynesia during the 2013 Zika outbreak25. After passages in Vero-E6 cultures, virus stocks were washed, and precleared by centrifugation before storing at −80 °C. All virus stocks were titered by plaque assay and quantified by qRT-PCR as previously described26.
Spiked Samples for Extraction Performance
ZIKAV was first serial diluted before being added into aliquots of Minimum Essential Medium (MEM) (Sigma-Aldrich, Munich, Germany) to cover 10−4 to 103 PFU/µL. Clean swabs (FLOQSwabs®) were immersed into respective ZIKAV dilutions. Each spiked swab was then immersed in 400 µL MEM respectively and pulse-vortexed for 1 minute. Viral RNA was subsequently isolated from 140 µL viral-MEM mixture using QIAamp Viral RNA Mini Kit (Qiagen, Hilden, Germany). Spiked experiments were repeated twice for inter-experimental reproducibility.
ZIKAV Real-Time RT-PCR
Both right and left conjunctival swabs from each patient were immersed in 400 µL of MEM. Re-suspension of patient swabs (in MEM) and subsequent viral RNA extraction were carried out as described earlier. Quantification by ZIKAV real-time reverse-transcription polymerase chain reaction (RT-PCR) of ZIKAV RNA for all samples was performed by one-step TaqMan real-time RT-PCR (QuantiTect Probe RT-PCR kit, Qiagen) using primers and probes described previously24. Briefly, all reactions were performed in a final volume of 25 μL with 5 μL of RNA, 400 nM and 200 nM of primers and probe respectively, 0.25 μL of RT enzyme and 12.5 μL of QuantiTect Probe RT-PCR master mix in 7500 Real Time PCR System (Applied Biosystems, Singapore). The following cycling conditions were used: 50 °C for 30 minutes, 95 °C for 10 minutes, followed by 45 cycles of 94 °C for 15 seconds and 60 °C for 1 minute. Validation, sensitivity and specificity of the qRT-PCR assay have been previously reported and demonstrated24. Specificity of the assay was evaluated by testing the following viral RNAs, all of which yielded negative results: Dengue serotype 1–4 viruses, West Nile virus, St. Louis encephalitis virus, yellow fever virus, Powassan virus, Semliki Forest virus, o’nyong-nyong virus, chikungunya virus, and Spondweni virus24. The qRT-PCR assay has also been used in numeral studies for ZIKAV RNA quantification in patient samples27,28,29, demonstrating its specificity, feasibility and reproducibility. RNA transcripts of ZIKAV strain H/PF/2013 ranging from 109 to 1.0 copies were tested in quadruplicates to construct the standard curve for estimating the copy number of ZIKAV RNA in swab samples.
Results
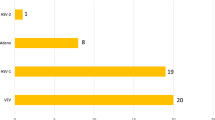
Of the 29 ZIKAV-infected patients in the study, majority were Chinese (n = 22, 75.9%), followed by Malay (n = 3, 10.3%), Indian (n = 3, 10.3%) and one from Bangladesh (Table 1). Male to female ratio was 16:13. Patient age ranged from 21 to 61 years (mean, 40). Rash (n = 28, 96.6%) and fever (n = 20, 69.0%) were the most common presenting symptoms at hospital admission. Conjunctivitis (red eye) was the ocular presentation observed in eight patients (27.5%) (Table 1). All patients with conjunctivitis experienced both watering and non-purulent discharge with discomfort. In addition, three (10.3%) patients suffered from pain in the eyes (Table 1). There was no complaint of decrease in vision in any of the patients. However, a complete ocular examination including visual acuity, fundus evaluation and conjunctival swabs could not be performed on the patients at time of first disease presentation.
Sample isolation efficiency was first investigated to assess the resultant efficiency of the extraction method using spiked swabs. The estimated PFU on the ZIKAV-spiked swab compared to the viral load derived from qRT-PCR was shown in (Table 2). The estimated detection threshold was 0.1 PFU, detected at approximately 4.9 copies after isolation.
After evaluating the efficiency of the isolation method, patient samples were processed following the established workflow. ZIKAV RNA was detected in conjunctival swabs of three infected patients at the late convalescent phase of the disease (30 days post-illness). The estimated ZIKAV RNA loads in the conjunctiva of these patients ranged from 5.2 to 9.3 copies (Table 1). Two of the three patients suffered from conjunctivitis, with one experiencing retro-ocular pain.
Discussion
In this study, we described the direct isolation and detection of ZIKAV RNA from conjunctival swab samples. Although detection of ZIKAV from conjunctiva has been previously reported22, presence of ZIKAV RNA in conjunctiva at the late convalescent phase of the disease was not known. ZIKAV RNA, however, was detected in one of the two eyes of virus-infected patients at 30 days post-illness. Due to the non-invasiveness of conjunctival swabs, testing of tear samples could be useful for diagnosis and evaluation of disease status.
Importantly, we also investigated the minimum amount of ZIKAV RNA (after swab sample isolation) required for amplification. The efficiency of such a detection assay is often dependent on the efficiency of the nucleic acid extraction from clinical specimens30, 31. Some extraction methods may interfere with the PCR reaction32. Efficiency of the isolation method was demonstrated by amplicon yield in the subsequent qRT-PCR. The ability of the isolation to yield ZIKAV RNA loads within the detection window of the qRT-PCR from a low-concentrated spiked swab substantiates the validity of the workflow. Moreover, our detection range was broad as shown by the spiked swabs. This is clinically important because ZIKAV viral loads observed in swab samples of ZIKAV-infected patients ranged from approximately 2.0 to 1788 copies/µL22.
It has been reported that ZIKAV RNA was still detected in virus-infected patients’ blood up to 11 days post-illness24, in urine and semen at 80 days33, and in tears at 7 days post-illness22. Our study demonstrated the longest persistence of ZIKAV RNA in tears at 30 days post-illness. Collection of swab samples at the late convalescent phase of disease could be a possible reason for the low viral RNA copy numbers observed. Despite the late collection, sensitivity was not compromised while the other report22 indicated only up to 7 days post-fever onset. To note, two of the patients still had detectable viral RNA copies in blood (patient 036 = 11.6 copies, patient 074 = 4.2 copies) during the time of tears collection at 30 days post-illness. Interestingly, viral load in blood for patient 036 was moderately high at 19.8 and 272.7 copies during the acute (5 days post-illness) and early convalescent (13 days post-illness) phases of the infection respectively, that persisted till late convalescence. Presence of ZIKAV RNA (81.6 copies) was also detected in the urine sample of patient 036 at early convalescence. The persistence of ZIKAV in both blood and urine could possibly explain for the presence of ZIKAV RNA in the conjunctival fluid. The qRT-PCR cycle threshold below the cut off showed that ZIKAV was present at the time (30 days post-illness) after patient 036 had recovered. Future studies with larger number of positive specimens are warranted to further establish the mechanisms of ZIKAV-induced ocular disease and viral persistence in the eye.
Nevertheless, the important clinical significance of this report is that ocular transmission of the ZIKAV through contact with ocular discharge is potentially possible even up to the late convalescent phase of ZIKAV infection. Transmission of ZIKAV through tears, although uncommon, was highlighted as a possible mode of transmission in an earlier case study34. ZIKAV infection in another individual who had close contact with a ZIKAV-infected patient with high viremia was also reported35. Similar findings were reported in a dengue patient36 and also in in vivo experiments37. These findings suggest that the spectrum of those at risk of ZIKAV infection may be broader than previously recognized. It is essential that health care personnel and community contacts are aware of the risks of virus infection and apply standard precautions while caring for ZIKAV-infected patients. Few systematic studies have examined the presence of ZIKAV in aqueous humor obtained from one and/or both eyes of infected patients after the onset of illness, so the incidence and clinical manifestations of ZIKAV ocular complications are uncertain. Interestingly, one of the patients with positive ZIKAV detection in the conjunctiva did not have any evidence of conjunctival inflammation or ocular pain at time of tears collection. This is worrying as this phenomenon suggests that a lack of clinical signs in the eye may not preclude infectious potential from the eye. Eventual investigations should determine if ZIKAV affects uveitis and other structures of the eye, such as the retinal vasculature, and determine the immunological responses that produce these clinical manifestations.
This case highlights a complication of ZIKAV with important implications for public health. It is important to assure that samples of conjunctivae and tears are tested negative for ZIKAV in patients to ensure no risk of virus spread through casual contact.
References
Dick, G. W., Kitchen, S. F. & Haddow, A. J. Zika virus. I. Isolations and serological specificity. Trans R Soc Trop Med Hyg. 46, 509–520 (1952).
Duffy, M. R. et al. Zika virus outbreak on Yap Island, Federated States of Micronesia. N Engl J Med. 360, 2536–2543 (2009).
Cao-Lormeau, V. M. et al. Zika virus, French polynesia, South pacific, 2013. Emerg Infect Dis. 20, 1085–1086 (2014).
Petersen, L. R., Jamieson, D. J., Powers, A. M. & Honein, M. A. Zika Virus. N Engl J Med. 374, 1552–1563 (2016).
Campos, G. S., Bandeira, A. C. & Sardi, S. I. Zika virus outbreak, Bahia, Brazil. Emerg Infect Dis. 21, 1885–1886 (2015).
Fauci, A. S. & Morens, D. M. Zika virus in the Americas - Yet another arbovirus threat. N Engl J Med. 374, 601–604 (2016).
Duong, V., Dussart, P. & Buchy, P. Zika virus in Asia. Int J Infect Dis. 54, 121–128 (2016).
Dash, A. P., Bhatia, R., Sunyoto, T. & Mourya, D. T. Emerging and re-emerging arboviral diseases in Southeast Asia. J Vector Borne Dis. 50, 77–84 (2013).
Mackenzie, J. S. et al. Emerging viral diseases of Southeast Asia and the Western Pacific. Emerg Infect Dis. 7, 497–504 (2001).
Maurer-Stroh, S. et al. South-east Asian Zika virus strain linked to cluster of cases in Singapore, August 2016. Euro Surveill. 21 (2016).
Brasil, P. et al. Zika Virus Infection in Pregnant Women in Rio de Janeiro. N Engl J Med. 375, 2321–2334 (2016).
Cao-Lormeau, V. M. et al. Guillain-Barre Syndrome outbreak associated with Zika virus infection in French Polynesia: a case-control study. Lancet. 387, 1531–1539 (2016).
Oehler, E. et al. Zika virus infection complicated by Guillain-Barre syndrome–case report, French Polynesia, December 2013. Euro Surveill. 19 (2014).
Mlakar, J. et al. Zika virus associated with microcephaly. N Engl J Med. 374, 951–958 (2016).
Moron, A. F. et al. Microcephaly associated with maternal Zika virus infection. BJOG. 123, 1265–1269 (2016).
Driggers, R. W. et al. Zika virus infection with prolonged maternal viremia and fetal brain abnormalities. N Engl J Med. 374, 2142–2151 (2016).
Ventura, C. V., Maia, M., Bravo-Filho, V., Gois, A. L. & Belfort, R. Jr. Zika virus in Brazil and macular atrophy in a child with microcephaly. Lancet. 387, 228 (2016).
Ventura, C. V. et al. Ophthalmological findings in infants with microcephaly and presumable intra-uterus Zika virus infection. Arq Bras Oftalmol. 79, 1–3 (2016).
de Paula Freitas, B. et al. Ocular findings in infants with microcephaly associated with presumed Zika virus congenital infection in Salvador, Brazil. JAMA Ophthalmol. (2016).
Kodati, S. et al. Bilateral posterior uveitis associated with Zika virus infection. Lancet. 389, 125–126 (2016).
Furtado, J. M., Esposito, D. L., Klein, T. M., Teixeira-Pinto, T. & da Fonseca, B. A. Uveitis associated with Zika virus infection. N Engl J Med. 375, 394–396 (2016).
Sun, J. et al. Presence of Zika virus in conjunctival fluid. JAMA Ophthalmol. 134, 1330–1332 (2016).
Chia, P. Y. et al. Clinical features of patients with Zika and dengue virus co-infection in Singapore. J Infect (2017).
Lanciotti, R. S. et al. Genetic and serologic properties of Zika virus associated with an epidemic, Yap State, Micronesia, 2007. Emerg Infect Dis. 14, 1232–1239 (2008).
Baronti, C. et al. Complete coding sequence of zika virus from a French polynesia outbreak in 2013. Genome Announc. 2, e00500–00514 (2014).
Lum, F. M. et al. Zika virus infects human brain fetal microglia and induces a strong inflammatory response. Clin Infect Dis. (2017).
Kam, Y. W., Leite, J. A., Lum, F. M., Tan, J. L. J. & Lee, B. Specific biomarkers associated with neurological complications and congenital CNS abnormalities from Zika virus-infected patients in Brazil. J Infect Dis (2017).
Li, J. et al. Characteristics of Zika Virus Disease in Children: Clinical, Hematological, and Virological Findings from an Outbreak in Singapore. Clin Infect Dis 64, 1445–1448 (2017).
Ho, Z. J. M. et al. Outbreak of Zika virus infection in Singapore: an epidemiological, entomological, virological, and clinical analysis. Lancet Infect Dis (2017).
Knepp, J. H., Geahr, M. A., Forman, M. S. & Valsamakis, A. Comparison of automated and manual nucleic acid extraction methods for detection of enterovirus RNA. J Clin Microbiol. 41, 3532–3536 (2003).
Shipley, M. A., Koehler, J. W., Kulesh, D. A. & Minogue, T. D. Comparison of nucleic acid extraction platforms for detection of select biothreat agents for use in clinical resource limited settings. J Microbiol Methods. 91, 179–183 (2012).
Verheyen, J. et al. Extraction of viral nucleic acids: comparison of five automated nucleic acid extraction platforms. J Clin Virol. 54, 255–259 (2012).
Matheron, S. et al. Long-Lasting Persistence of Zika Virus in Semen. Clin Infect Dis. 63, 1264 (2016).
Swaminathan, S., Schlaberg, R., Lewis, J., Hanson, K. E. & Couturier, M. R. Fatal Zika virus infection with secondary nonsexual transmission. N Engl J Med. 375, 1907–1909 (2016).
Brent, C. et al. Preliminary findings from an investigation of Zika virus infection in a patient with no known risk factors - Utah, 2016. MMWR Morb Mortal Wkly Rep. 65, 981–982 (2016).
Chen, L. H. & Wilson, M. E. Transmission of dengue virus without a mosquito vector: nosocomial mucocutaneous transmission and other routes of transmission. Clin Infect Dis. 39, e56–60 (2004).
Miner, J. J. et al. Zika virus infection in mice causes panuveitis with shedding of virus in tears. Cell Rep. 16, 3208–3218 (2016).
Acknowledgements
We thank the study subjects for their participation, clinical team at the Communicable Disease Centre/Tan Tock Seng Hospital contribution in patient recruitment and sample collection. The work is supported by the National Medical Research Council (Singapore) grant NMRC/CSA/045/2012 and BMRC A*STAR-led Zika Virus Consortium Fund (Singapore) project number 15/1/82/27/001. The funders had no role in study design, data collection and analysis, decision to publish, or preparation of the manuscript.
Author information
Authors and Affiliations
Contributions
Y.S.L., L.T. and R.A. contributed the samples, virological and clinical data. J.J.L.T., P.K.B., L.F.P.N. and R.A. conceived and designed the experiments. J.J.L.T. and P.K.B. performed the experiments. J.J.L.T., P.K.B., Y.S.L., L.T., L.F.P.N. and R.A. analyzed the data. J.J.L.T., P.K.B., L.T. and L.F.P.N. drafted the manuscript.
Corresponding authors
Ethics declarations
Competing Interests
The authors declare that they have no competing interests.
Additional information
Publisher's note: Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made. The images or other third party material in this article are included in the article’s Creative Commons license, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons license and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this license, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Tan, J.J.L., Balne, P.K., Leo, YS. et al. Persistence of Zika virus in conjunctival fluid of convalescence patients. Sci Rep 7, 11194 (2017). https://doi.org/10.1038/s41598-017-09479-5
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41598-017-09479-5
This article is cited by
-
Ocular manifestations of emerging viral diseases
Eye (2021)
-
Mucocutaneous Features of Zika—a Review
Current Infectious Disease Reports (2019)
-
The emergence of Zika virus and its new clinical syndromes
Nature (2018)
-
Zika virus: epidemiology, clinical aspects, diagnosis, and control of infection
European Journal of Clinical Microbiology & Infectious Diseases (2018)
-
Efficient detection of Zika virus RNA in patients’ blood from the 2016 outbreak in Campinas, Brazil
Scientific Reports (2018)
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.