Abstract
Our recent studies revealed that supplementation with the reduced form of coenzyme Q10 (CoQ10H2) inhibits oxidative stress and slows the process of aging in senescence-accelerated mice. CoQ10H2 inhibits adipocyte differentiation and regulates lipid metabolism. In the present study, we show that dietary supplementation with CoQ10H2 significantly reduced white adipose tissue content and improved the function of brown adipose tissue by regulating expression of lipid metabolism-related factors in KKAy mice, a model of obesity and type 2 diabetes. In the liver, CoQ10H2 reduced cytoplasmic Ca2+ levels and consequently inhibited the phosphorylation of CaMKII. CoQ10H2 also regulated the activity of the transcription factor C-FOS and inhibited gene expression of PDE4, a cAMP-degrading enzyme, via the CaMKII-MEK1/2-ERK1/2 signaling pathway, thereby increasing intracellular cAMP. This increased cAMP activated AMPK, enhanced oxidative decomposition of lipids, and inhibited de novo synthesis of fatty acids, inhibiting the development and progression of obesity and type 2 diabetes. These results suggest that CoQ10H2 supplementation may be useful as a treatment for metabolic disorders associated with obesity.
Similar content being viewed by others
Introduction
Imbalance between energy input and output can lead to the accumulation of excess fat, causing obesity. Obesity and metabolic disorders have become a global health problem1. Obesity is an important risk factor for various metabolic disorders, including insulin resistance and type 2 diabetes2, atherosclerosis3, cardiovascular disease4, and chronic kidney disease5, and can cause oxidative stress6, 7, endoplasmic reticulum (ER) stress8, 9, and mitochondrial dysfunction10, 11. Therefore, there is an urgent need to find a safe and effective treatment for obesity.
Increasing evidence suggests that increased oxidative stress caused by obesity is involved in the pathogenesis of metabolic syndrome6. Oxidative stress, caused by imbalance between the production of oxygen free radicals and the antioxidant capacity of cells, induces cell damage and abnormal production of adipocytokines, which directly leads to a series of metabolic abnormalities, including obesity-related insulin resistance, hypertension, abnormal blood lipids, and fatty degeneration of the liver12,13,14.
The ER is one of the most important intracellular signal transduction organelles15. It activates numerous cellular functions by releasing Ca2+ and inhibits them by Ca2+ re-uptake through skeletal sarco-endoplasmic reticulum Ca2+-transporting ATPase 2 (SERCA2). Recent studies showed that in obese/diabetic animal models, SERCA2 dysfunction is induced and cytoplasmic Ca2+ is increased, which then activates the cytoplasmic calcium-sensitive kinase, calcium/calmodulin dependent-protein kinase II (CaMKII), and triggers ER stress16. ER stress induced by a high fat diet and consequent metabolic disorders can be ameliorated by enhancing the function of SERCA2 and improving ER Ca2+ load capacity17, 18.
Mitochondrial dysfunction has also been shown to be associated with the development of obesity and insulin resistance10, 11. Peroxisome proliferator-activated receptor γ coactivator 1α (PGC-1α), a nuclear transcription coactivator, plays several roles in energy metabolism, including involvement in adaptive thermogenesis, mitochondrial biogenesis, hepatic gluconeogenesis, and β-oxidation of fatty acids19,20,21,22. Studies have shown that decreased PGC-1α mRNA is associated with insulin resistance23, 24. The Sirtuin family has become known as a key regulator of the nutrient-sensitive metabolic regulatory pathway25. Activation of SIRT1 promotes β-oxidation of fatty acids, prevents diet-induced nonalcoholic fatty liver disease, and reduces insulin resistance26,27,28. Obesity reduces SIRT1 activity in liver and adipose tissue29, 30. Increased expression of PGC-1α and SIRT1 promotes the browning of white adipose tissue and ameliorates obesity and metabolic disorders23, 31.
Coenzyme Q10 (CoQ10) is a fat-soluble micronutrient synthesized in nearly all human cells and plays a role in electron transport in the mitochondrial respiratory chain32, 33. CoQ10 content in organs is gradually decreased with age and this decline is closely associated with the occurrence and development of various diseases34. Therefore, intake of exogenous CoQ10 could help prevent the occurrence and progression of age-related diseases such as cardiovascular disease, metabolic syndrome, diabetes mellitus, cardiac dysfunction, and neurodegenerative diseases35,36,37,38. CoQ10 is enzymatically maintained in its reduced form (CoQ10H2) and also acts as a fat-soluble antioxidant to potently protect lipid membranes and lipoproteins from oxidative damage and to prevent DNA damage39,40,41. Our previous studies showed that CoQ10H2 increases cAMP and enhances the activity of SIRT1 and PGC-1α, thereby improving mitochondrial function and inhibiting oxidative stress42.
In addition, other studies have shown that CoQ10H2 content in adipose tissue gradually decreased with the development of obesity in both mice and humans, and that CoQ10H2 synthesis-related enzymes were upregulated as a compensatory measure43. CoQ10H2 also inhibits adipocyte differentiation and cholesterol synthesis44, but the mechanism remains unclear.
The present study shows that dietary supplementation of KKAy mice, a widely used model of diabetes and obesity, with CoQ10H2 inhibited weight gain and reduced white adipose tissue content while enhancing brown adipose tissue function, and increasing the metabolic rate. CoQ10H2 treatment also increased expression of Sirt1, Pgc-1α and Pparα, enhanced mitochondrial function and promoted β-oxidation of fatty acids in the liver, as well as increased levels of intracellular cAMP. We also found that CoQ10H2 enhanced the expression and function of SERCA2 and inhibited the increase of cytoplasmic Ca2+, and subsequently inhibited activity of the transcription factor C-FOS, which in turn inhibited the expression of phosphodiesterase 4 (PDE4) in the in vitro experiments. Our results demonstrate that dietary CoQ10H2 can suppress lipid accumulation and mitigate metabolic dysfunction.
Results
CoQ10H2 inhibited weight gain and improved metabolic syndrome in KKAy mice
In this study, dietary supplementation with CoQ10H2 was employed to investigate the effect of CoQ10H2 on metabolic syndrome in KKAy mice. Every week, all mice were weighed and food intake was calculated. Compared with the control group, the body weight of KKAy mice was reduced by 12% after 12 weeks of CoQ10H2 supplementation (Fig. 1A), although the food intake was similar between the two groups at each time point (data not shown).
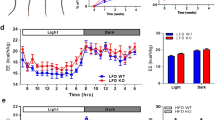
CoQ10H2 prevented the accumulation of visceral fat (iWAT) in KKAy mice and protected mice from insulin resistance and metabolic disorders. (A–C) Body weight and iWAT content changes for animals in the control and CoQ10H2 groups. Photographs show representative gross morphology of an iWAT mouse aged 20 weeks (n = 4–6, ∗p < 0.05, ∗∗p < 0.01; mean ± SD, Student’s t-test); (D–G) Serum cholesterol and triglyceride, fasting blood glucose and serum insulin levels of KKAy mice after 12 hours of fasting in each group at age 12, 16, and 20 weeks. (n = 4–6, ∗p < 0.05, ∗∗p < 0.01; mean ± SD, Student’s t-test); (H) Changes in blood glucose and area under the curve (AUC) in 20-week-old mice after intraperitoneal injection of glucose (1 g/kg body weight) following 12 hours of fasting. (n = 4–6, ∗p < 0.05, ∗∗p < 0.01; mean ± SD, Student’s t-test).
In addition, inguinal white adipose tissue (iWAT) was significantly reduced and percent adipose tissue was lower in KKAy mice supplemented with CoQ10H2 compared with the control group (Fig. 1B and C). The occurrence and development of obesity are often associated with abnormal lipid and glucose metabolism. Therefore, we next addressed whether CoQ10H2 can improve metabolic function. Serum total cholesterol and triglyceride content were significantly decreased in KKAy mice given CoQ10H2 supplementation (Fig. 1D and E). CoQ10H2 also reduced concentrations of fasting blood glucose and serum insulin in KKAy mice (Fig. 1F and G). In addition, mice with CoQ10H2 supplementation also showed better glucose tolerance in an intraperitoneal glucose tolerance test (IPGTT) (Fig. 1H). Together, these results indicate that CoQ10H2 can control obesity and improve insulin resistance in KKAy mice.
CoQ10H2 prevented an increase in adipocytes in iWAT and enhanced the function of brown adipose tissue (BAT) in KKAy mice
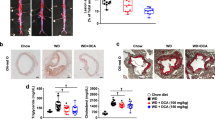
In order to demonstrate the effect of CoQ10H2 on adipocytes in iWAT from KKAy mice, iWAT from control and experimental mice was stained with hematoxylin and eosin (H&E), and expression of lipid metabolism-related factors was detected (Fig. 2A and B). Obesity in KKAy mice was primarily caused by hypertrophy of adipocytes, while CoQ10H2 supplementation significantly prevented this adipocyte hypertrophy. Expression levels of several marker genes for fatty acid synthesis (e.g., Srebp1c and others) and adipocyte differentiation (e.g., Pparγ and others) in KKAy mice iWAT showed a progressive tendency to increase with the development of obesity, whereas CoQ10H2 supplementation significantly prevented these changes, suggesting that metabolic dysfunction of adipose tissue is mitigated by dietary supplementation with CoQ10H2. BAT is involved in regulation of energy metabolism and obesity. Activation of BAT can burn fatty acids to produce heat, reduce triglyceride content, and inhibit obesity45. Effects of CoQ10H2 on BAT morphology were observed using H&E staining (Fig. 2A). KKAy mice in the control group had more abundant and larger lipid droplets in BAT, while CoQ10H2 supplementation inhibited the excessive accumulation of lipid droplets in BAT. BAT thermogenesis induces expression of uncoupling protein 1 (Ucp1) and other genes, promoting lipolysis, mitochondrial biogenesis, and β-oxidation of fatty acids. Our experiment showed that mRNA expression of Ucp1 and other thermogenesis-related genes was significantly increased in BAT from KKAy mice supplemented with CoQ10H2 compared with the control group, suggesting that the CoQ10H2 group had increased BAT thermogenic activity (Fig. 2C).
CoQ10H2 inhibited lipid accumulation in iWAT and promoted BAT function. (A) Images of iWAT and BAT stained with H&E in 20-week-old KKAy mice, and iWAT adipocyte size and percentage lipid content in BAT measured by Image-pro. Bar = 50 μm. (n = 4–6, ∗∗p < 0.01; mean ± SD, Student’s t-test); (B,C) Expression of genes involved in triglyceride and cholesterol biosynthesis and lipid mobilization related factors in iWAT and expression of genes related to mitochondrial function in BAT from mice in the control and CoQ10H2 groups at the ages of 12, 16, and 20 weeks by real-time PCR. Histograms show fold-change in mRNA level relative to 12-week-old control KKAy mice (n = 4–6, ∗p < 0.05, ∗∗p < 0.01; mean ± SD, Student’s t-test); (D) Lipid content in 3T3L1 preadipocytes after CoQ10H2 (10 μM) was added to cell cultures before (Day 0) and after (Day 5) differentiation. Quantitative analysis of lipid deposition was measured by optical density (OD) values at 510 nm after oil-red O staining. (n = 9, ∗∗p < 0.01; mean ± SD, Student’s t-test).
To directly demonstrate the effect of CoQ10H2 on adipocyte differentiation and lipolysis, 10 μM CoQ10H2 was added to pre-adipocyte 3T3L1 cultures before (Day 0) and after (Day 5) differentiation, and lipid accumulation was quantitatively determined by oil red O staining (Fig. 2D). After differentiation, mature adipocytes were round and contained a large number of lipid droplets (Day 5). Compared with the control group, the addition of CoQ10H2 before differentiation inhibited adipocyte differentiation and the accumulation of fat. Also, the addition of CoQ10H2 to differentiated adipocytes reduced the cellular lipid content and promoted lipolysis on Day 5 and Day 10, respectively, after initiating treatment. Taken together, our results demonstrate that CoQ10H2 improves lipid metabolism and inhibits obesity in KKAy mice.
CoQ10H2 regulates liver lipid metabolism
The liver plays an important role in the digestion, absorption, synthesis, and decomposition of lipids46. We observed H&E-stained liver slices and found that CoQ10H2 treatment eliminated excessive accumulation of fat in liver cells in KKAy mice (Fig. 3A).
CoQ10H2 improves cAMP levels and promotes lipid metabolism in the livers of KKAy mice. (A) Images of liver tissue stained with H&E in 20-week-old KKAy mice. Bar = 50 μm; (B) Changes in gene expressions for factors involved in triglyceride and cholesterol biosynthesis or lipid mobilization and mitochondrial function in 12-, 16-, and 20- week-old KKAy mice in the control and CoQ10H2 groups as determined by real-time PCR. Histograms show fold-change in mRNA level relative to 12-week-old control KKAy mice. (n = 4–6, ∗p < 0.05, ∗∗p < 0.01 mean ± SD, Student’s t-test); (C) Protein content of SIRT1 and PGC-1α and phosphorylation levels of AMPK and ACC in the livers of KKAy mice were measured by Western blotting. All blots were obtained under the same experimental conditions, and cropped images of the blots are shown. Densitometric quantification is depicted on the right panel. (n = 4–6, ∗p < 0.05, ∗∗p < 0.01; mean ± SD, Student’s t-test).
In addition, CoQ10H2 treatment increased expression of Sirt1, Pgc-1α and Pparα, enhancing mitochondrial function and promoting the β-oxidation of fatty acids, and simultaneously decreased expression of Serbp1c, Fas and Pparγ, thereby inhibiting de novo synthesis of fatty acids (Fig. 3B and C). AMP-activated protein kinase (AMPK) acts as an energy sensor to help maintain cellular energy homeostasis; AMPK activation inhibits the accumulation of liver lipids in type 2 diabetic mice and has beneficial effects against hyperlipidemia and atherosclerosis47, 48. We assessed hepatic AMPK activity in KKAy mice by measuring the phosphorylation status of AMPK and Acetyl-CoA carboxylase (ACC). We found that hepatic AMPK activity was significantly increased in mice receiving CoQ10H2 supplementation compared with controls (Fig. 3C).
CoQ10H2 inhibits expression of PDE4 in the liver
cAMP is a second messenger that regulates the activity of SIRT1 and AMPK and is involved in regulation of intracellular energy metabolism49, 50. We found that dietary supplementation with CoQ10H2 significantly increased hepatic cAMP content in KKAy mice (Fig. 4A). As a second messenger coupled to G-protein pathways, cAMP concentrations can change rapidly. As such, we measured the change in cAMP content in HepG2 cells 0.5-24 hours after addition of exogenous CoQ10H2. At 6 hours after the addition of CoQ10H2, the intracellular cAMP content did not increase significantly, but thereafter cAMP levels displayed a slight upward trend. The cAMP concentration peaked 12 hours after addition of CoQ10H2 and remained at a high level (Fig. 4B). Adenylyl cyclase (AC) is responsible for intracellular cAMP synthesis and MDL-12330A is a specific inhibitor of AC. Addition of exogenous CoQ10H2 to cultured HepG2 cells increased intracellular cAMP but was not inhibited by MDL-12330A (Fig. 4C). These results showed that the increased intracellular cAMP induced by CoQ10H2 is not due to increased cAMP synthesis.
CoQ10H2 inhibits expression of PDE4 in the liver by decreasing C-FOS binding to the PDE4 promoter. (A) Liver cAMP concentrations of KKAy mice in the control and CoQ10H2 groups at ages 12, 16, and 20 weeks. (n = 4–6, ∗p < 0.05, ∗∗p < 0.01; mean ± SD, Student’s t-test); (B) Change in intracellular cAMP concentration in HepG2 cells 0.5–24 hours after the addition of CoQ10H2 (5 μM). (n = 6, ∗∗p < 0.01; mean ± SD, one-way ANOVA followed by Tukey’s test); (C)MDL-12330A (50 μM) pre-treated or untreated HepG2 cells were supplemented with CoQ10H2 (5 μM) for 24 hours and then intracellular cAMP was measured. (n = 6, ∗∗p < 0.01; mean ± SD, one-way ANOVA followed by Tukey’s test); (D) mRNA expression levels of PDE4 in HepG2 cells 24 hours after addition of CoQ10H2 (5 μM) were determined by real-time PCR. Histograms show fold-change of the mRNA level relative to untreated control cells. (n = 9, ∗p < 0.05, ∗∗p < 0.01; mean ± SD, Student’s t-test); (E,F) PDE4 protein content in HepG2 cells (E) and KKAy mouse liver (F) was measured by western blotting. Densitometric quantification is depicted in the right panel (n = 4–6, ∗p < 0.05, ∗∗p < 0.01; mean ± SD, Student’s t-test); (G) Lineweaver-Burk plots show kinetic analysis of PDE activity at 0.3 to 40 μM cAMP. (H) Levels of C-FOS protein and its phosphorylation in HepG2 cells 24 hours after CoQ10H2 (5 μM) supplementation were measured by western blotting. All blots were obtained under the same experimental conditions, and cropped images of the blots are shown (n = 9, ∗∗p < 0.01; mean ± SD, Student’s t-test); (I) The binding capacity of C-FOS and the PDE4 promoter as detected by ChIP (n = 9, ∗p < 0.05; mean ± SD, Student’s t-test).
Phosphodiesterases (PDEs) are encoded by 21 genes that are divided into 11 families according to their structural similarity. PDEs regulate cellular signal transduction by specifically hydrolyzing cAMP (e.g., PDE3, 4, 7 and 8) and cGMP (e.g. PDE1, 5, 6, 9 and 10)51. In addition, gene expression of PDEs has significant tissue specificity (e.g., PDE3A is mainly expressed in the heart and vascular smooth muscle). Measurement of the expression of each cAMP-specific PDE subtype showed that PDE4A and PDE4C expression was reduced in HepG2 cells with CoQ10H2 addition (Figs S2 and 4D). We also confirmed that CoQ10H2 reduced the protein content of PDE4 in HepG2 cells and the liver of KKAy mice (Fig. 4E and F). To demonstrate whether CoQ10H2 can directly inhibit PDE activity, we constructed Lineweaver-Burk plots to express the relationship between PDE activity and CoQ10H2 treatment. The Vmax and Km of PDEs were not significantly altered- even in the presence of a very high concentration of CoQ10H2 (100 μM)- compared to IBMX, a nonselective competitive PDE inhibitor (Fig. 4G). These data indicate that CoQ10H2 enhanced intracellular cAMP concentrations by inhibiting PDE4 gene expression rather than activity.
Activating protein-1 (AP-1), a mammalian transcription factor, is not a single protein, but a homologous or heterologous complex consisting of proteins from the Fos and Jun families52. In this study, mRNA levels of the AP-1 component C-FOS (but not C-JUN (Fig. S3)) and C-FOS phosphorylation were significantly reduced by CoQ10H2 (Fig. 4H). Next, we investigated the regulatory effect of AP-1 on the expression of PDE4 using chromatin immunoprecipitation (Fig. 4I), and found that AP-1 directly combined with the PDE4 promoter, and that CoQ10H2 can inhibit the binding of AP-1 to PDE4. These data suggest that CoQ10H2 regulates binding of AP-1 to the PDE4 promoter, thereby reducing PDE4 levels and inhibiting cAMP hydrolysis.
CoQ10H2 regulates calcium signaling pathways by promoting expression and function of SERCA2
As the most classical pathway in the Mitogen-activated protein kinase (MAPK) system, the extracellular signal-regulated kinase 1 and 2 (ERK1/2) pathway transports extracellular signals into the nucleus to activate various effector molecules and regulate biological activities such as cell proliferation and apoptosis via a series of cascade transduction systems53. Activation of ERK1/2 promotes the phosphorylation of many transcription factors, including ELK-1, C-FOS and C-MYC, to regulate nuclear translocation and transcriptional activity54. ERK1/2 inhibitors, however, inhibit the expression of C-FOS in a variety of tissues55. For these reasons, we measured phosphorylation of two phosphorylation sites in ERK1/2 in HepG2 cells and found that CoQ10H2 inhibited phosphorylation of ERK1/2 in cells, while total ERK1/2 content was not changed (Fig. 5A). It is generally believed that the ERK-activated signal cascade requires sequential activation of Ras, Raf1, MAPK/ERK kinase 1 and 2 (MEK1/2), and phosphorylation at Thr185/Tyr187. In addition, CaMKII binds to MEK1/2 and ERK1/2 to form macromolecular complexes to synergistically promote the phosphorylation of ERK1/2 at Thr202/Tyr204 and nuclear translocation56. Intracellular phosphorylation of CaMKII and MEK1/2 was inhibited by the addition of CoQ10H2 (Fig. 5B). Changes in CaMKII and MEK1/2 activity were closely related to cytoplasmic Ca2+ concentration. SERCA2 is an important regulator of cytoplasmic Ca2+ concentration and works by regulating Ca2+ uptake into the ER. CoQ10H2 increased SERCA2 expression in both HepG2 cells and KKAy mice liver tissue (Figs 5C and S3), enhanced ER calcium storage, and decreased cytoplasmic Ca2+ content (Figs 5D and S1). Our results demonstrate that CoQ10H2 regulates the activity of factors involved in the Ca2+ signaling pathway to inhibit transcriptional activity of ERK1/2 by increasing the expression of SERCA2.
CoQ10H2 inhibited the activity of CaMKII and MEK1/2 and therefore inhibited phosphorylation of ERK1/2 by enhancing the expression and function of SERCA2. (A) Phosphorylated ERK1/2 and total ERK1/2 in HepG2 cells were measured by Western blotting 24 hours after CoQ10H2 (5 μM) supplementation. All blots were obtained under the same experimental conditions, and cropped images of the blots are shown. Densitometric quantification is depicted in the right panel. (n = 9, ∗∗p < 0.01; mean ± SD, Student’s t-test); (B) Phosphorylation levels of CaMKII and MEK1/2, the upstream regulators of ERK1/2, were detected by Western blotting in HepG2 cells 24 hours after supplementation with CoQ10H2 (5 μM). All blots were obtained under the same experimental conditions, and cropped images of the blots are shown. Densitometric quantification is depicted in the right panel. (n = 9, ∗∗p < 0.01; mean ± SD, Student’s t-test); (C) Gene expression of SERCA2 in HepG2 cells was determined by real-time PCR 24 hours after CoQ10H2 (5 μM) supplementation. (n = 9, ∗∗p < 0.01; mean ± SD, Student’s t-test); (D) Determination of intracellular calcium concentration by Flou-3AM (40 μM). HepG2 cells were supplemented with CoQ10H2 (5 μM) for 24 hours, and then the SERCA2 inhibitor Thapsigargin (Tg) (200 nM) and Ca2+ (5 mM free extracellular Ca2+ final concentration) were added to the cells, and changes in fluorescence were observed (see the Supplementary Data for details).
Discussion
It is well known that CoQ10H2 is a powerful antioxidant that can potently inhibit the generation of oxygen free radicals and oxidative stress damage, thereby ameliorating age-associated disease. This effect has been shown both in mouse and cell experiments42. Obesity is a chronic metabolic disease caused by various factors including heredity, environment, dietary patterns, and living habits, and the development of obesity is accompanied by decreased CoQ10H2 content in adipose tissue, as seen in both human and mouse models43, 57. At the same time, increased CoQ10H2 synthesis can ameliorate metabolic disorders and insulin resistance caused by obesity, and significantly inhibits 3T3L1 preadipocyte differentiation and lipid accumulation44. Therefore, we hypothesized that CoQ10H2 might regulate lipid metabolism to some extent. As a widely used model of obesity and type 2 diabetes, KKAy mice develop obesity and insulin resistance accompanied by hepatic steatosis at an early age58. In our study, the development of obesity in KKAy mice was inhibited by administration of exogenous CoQ10H2, while food intake was not changed (Fig. 1A). At the same time, accumulation of visceral fat was inhibited (Fig. 1B and C) and blood cholesterol and triglyceride content were reduced by CoQ10H2 treatment (Fig. 1D and E). As a model of insulin resistance, fasting blood glucose in KKAy mice is high and is gradually increased with the aggravation of obesity. These phenomena are potently reversed by CoQ10H2 supplementation (Fig. 1F–H). We observed the effect of CoQ10H2 on adipose tissue by H&E staining of adipose tissue. Compared with the control group, adipocyte size in iWAT of KKAy mice was decreased by 42%, and the percentage of lipid droplets in BAT was decreased by 26% with CoQ10H2 supplementation (Fig. 2A). Analysis of various lipid metabolism markers in iWAT and BAT revealed that CoQ10H2 can inhibit de novo synthesis of fatty acids and promote oxidation of fatty acids (Fig. 2B and C). To determine if CoQ10H2 affects adipogenesis and lipolysis, we added CoQ10H2 to pre-adipocyte 3T3L1 cultures before and after differentiation into mature adipocytes. Our results demonstrate that CoQ10H2 reduces adipose differentiation and lipid storage in adipocytes.
The liver is the main site of lipid metabolism and lipid metabolism disorders caused by obesity are a major cause of non-alcoholic fatty liver disease. Significant hepatic steatosis occurred in the livers of KKAy mice in the control group, while the livers of mice supplemented with CoQ10H2 did not show obvious changes (Fig. 3A). PGC-1α is a transcriptional coactivator that is closely related to energy metabolism and plays an important role in the process of mitochondrial synthesis and adaptive thermogenesis59, 60. PGC-1α is also involved in glucose and lipid metabolism, and has become a new target for the treatment of diabetes, obesity, and other metabolic diseases20. Supplementation with CoQ10H2 increased PGC-1α gene expression in the liver (Fig. 3B). Previous results have shown that expression and activity of PGC-1α are regulated by AMPK and SIRT142. AMPK is an essential protein kinase involved in the regulation of energy metabolism in vivo. Activation of AMPK can inhibit ATP-consuming pathways, such as the synthesis of fat and cholesterol, and promote ATP-forming pathways, such as β-oxidation of fatty acids61. In a model system, decreased AMPK activity resulted in insulin resistance and activation of AMPK-enhanced insulin sensitivity62,63,64. In addition, AMPK activation was also directly involved in regulating the activity of fat metabolism-related factors, such as SREBP1c48. SIRT1 is widely known for its anti-aging effect65. SIRT1 also plays an important role in cellular energy metabolism66. It directly regulates the expression and activity of PPAR family genes and participates in the regulation of lipid metabolism pathways67. In addition, SIRT1 can also deacetylate the AMPK upstream kinase LBK1 and activate AMPK42. In KKAy mice, SIRT1 protein content and AMPK activity decrease with age, and this effect is ameliorated by CoQ10H2 supplementation (Fig. 3C).
The second messenger cAMP plays a key role in transduction of various extracellular signals in cells. Our previous work demonstrated that CoQ10H2 increases cAMP content in the liver and regulates lipid metabolism in mice42. These results were confirmed in the present study (Fig. 4A). We found that specific inhibition of PDE4 expression in cultured cells increased cAMP (Fig. 4D). Interestingly, as shown in Fig. 4G, the specific activity of PDE4 was not changed, indicating that CoQ10H2 and resveratrol, a known cAMP-SIRT1 activator that acts by directly inhibiting activity of PDE4, do not share the same mechanism of action50. We further demonstrated that CoQ10H2 inhibited transcriptional activity of the transcription factor AP-1 and that of C-FOS, a component of AP-1, and that CoQ10H2 inhibited the ability of AP-1 to bind to the PDE4 gene promoter (Fig. 4I). By measuring changes in signaling factors upstream of C-FOS, we confirmed that CoQ10H2 inhibits the transcriptional activity of C-FOS by inhibiting the phosphorylation of ERK1/2. CaMKII and MEK1/2 are both upstream regulatory factors for ERK1/2, and CaMKII and MEK1/2 activity is influenced by changes in cytoplasmic Ca2+ concentration (Fig. 5A and B).
Ca2+ is one of the most abundant ions in cells. Changes in intracellular Ca2+ concentration are a key factor in the maintenance of organelle function and resistance to stress in many metabolic tissues, such as liver and adipose tissue68. Regulation of Ca2+ levels in the cytoplasm and organelles requires synergistic effects of various signal transduction mechanisms, including the ability to pump Ca2+ from the cytosol to the extracellular space or into intracellular reservoirs, such as the ER and mitochondria. Transportation of Ca2+ from the cytoplasm into the ER against a concentration gradient requires SERCA2 and energy released from the hydrolysis of ATP. The development of many metabolic diseases, especially obesity and diabetes, is often accompanied by damage to SERCA2, which increases cytoplasmic Ca2+ levels, leading to enhanced insulin resistance9, 18. CoQ10H2 inhibits the metabolic disease-induced increase in cytoplasmic Ca2+ concentration, but the mechanism is unclear69, 70. Our results demonstrate that CoQ10H2 promotes the expression of SERCA2 and increases ER Ca2+ in cultured cells, but has no effect on calcium channels (Fig. 5C and D). Similarly, dietary supplementation with CoQ10H2 inhibited SERCA2 damage induced by obesity in KKAy mice (Fig. S4).
Our results demonstrate that CoQ10H2 promotes the expression of SERCA2 and reduces cytoplasmic Ca2+ in the liver cells (Fig. 5C and D). Alteration of Ca2+ concentration inhibited the CaMKII-MEK1/2-ERK1/2 signaling pathway, and consequently the transcriptional activity of AP-1. Furthermore, by inhibiting the ability of AP-1 to bind the PDE4 promoter, expression of PDE4 was inhibited and intracellular cAMP was increased. The de novo synthesis of fatty acids was inhibited and β-oxidation of fatty acids was enhanced due to CoQ10H2-induced alterations in the activity of factors such as AMPK and PGC-1α. CoQ10H2 supplementation also inhibited the accumulation of fat in adipose tissue, promoted fat mobilization, and reduced body weight (Fig. 6). In conclusion, our results suggest that CoQ10H2 could serve as a safe and effective supplement to improve lipid metabolism and insulin resistance in the future.
Proposed mechanism by which CoQ10H2 improves metabolic function and inhibits insulin resistance in KKAy mice. In the liver, CoQ10H2 inhibited phosphorylation of CaMKII by enhancing the function of SERCA2, and reduced cytoplasmic Ca2+, thereby inhibiting the transcriptional activity of the transcription factor C-FOS by regulating the CaMKII-MEK1/2-ERK1/2 signaling pathway. PDE4 gene expression was then inhibited and intracellular cAMP was increased. The increase in cAMP, however, promoted AMPK activity. On the one hand, expression of SIRT1 and PGC-1α was increased and mitochondrial function was enhanced to promote the decomposition of fatty acids. On the other hand, triglyceride and cholesterol biosynthesis was inhibited. In adipose tissue, CoQ10H2 can prevent the excessive accumulation of visceral fat and promote the function of BAT, thereby improving obesity, insulin resistance, and metabolic syndrome.
Methods
Animals
7-week-old female KKAy mice were purchased from CLEA Japan Inc. (Tokyo, Japan) and raised in the Division of Laboratory Animal Research, Research Center for Support of Advanced Science, Shinshu University, under specific pathogen-free (SPF) conditions at 24 ± 2 °C with a light-controlled regimen (12 hours light/dark cycle). The mice were randomly distributed into two experimental groups. Body weight and serum triglyceride and total cholesterol levels were determined and no statistically significant differences were found between the two groups at baseline (data not shown). Animals were fed either CoQ10H2-supplemented feed (final concentration of 0.3%, mixed with CE-2 standard mouse feed) or CE-2 feed starting from the age of 8 weeks; both diets were purchased from CLEA Japan. All mice were allowed free access to food and water, and body weight was recorded and food intake calculated twice a week. Mice were examined daily. Mice in both groups were fasted for 12 hours at the ages of 12, 16, and 20 weeks, and were anesthetized with sevoflurane (Wako, Osaka, Japan), followed by blood and tissue collection at the end of the experiment.
For the IPGTT, mice were fasted for 12 hours and then given an intraperitoneal injection of glucose (1 g/kg body weight) 3 days before autopsy. Blood samples were collected at different time intervals after injection (0–180 minutes) for blood glucose measurement. Blood glucose levels were measured using Accu-Chek Aviva glucose monitors (Roche, Indianapolis IN). To determine serum levels of insulin, triglyceride and total cholesterol, blood samples were collected from the heart during dissection and stored in test tubes. Serum insulin was measured by ELISA (Morinaga, Yokohama, Japan), and serum triglyceride and total cholesterol levels were measured using enzymatic kits (Wako, Osaka, Japan), according to the manufacturer’s instructions.
All experiments using animals were performed with the approval of the Committee for Animal Experiments of Shinshu University and approved protocols were strictly followed. Permit number: 260066 (from 2015).
Cell Culture
The human hepatoma HepG2 cell line was provided by the RIKEN BRC through the National Bio-Resource Project of the MEXT, Japan, and 3T3L1 cells were purchased from the Japanese Cancer Research Resources Bank. HepG2 cells were resuscitated and then cultured in an incubator with 5% CO2 at 37 °C in DMEM medium (4.5 g/l glucose) supplemented with 10% fetal bovine serum (FBS) and 0.2% antibiotics, and the medium was changed every 3 days. When HepG2 cells reached 90% confluence, CoQ10H2 (5 μM) was added and cells were cultured for another 24 hours. Cells were then collected with a scraper. Refer to the supplementary data for the experimental protocol for 3T3L1 cells.
Western blotting and immunoprecipitation
Tissues and cells were lysed in cell lysis buffer (Cell Signaling Technology, MA) supplemented with protease inhibitors (Sigma Aldrich, MO). Protein samples were sonicated, followed by centrifugation at 15,000 g for 10 minutes. Supernatants were collected, and protein concentrations were determined using the BCA protein Assay Kit (Thermo Fisher Scientific, CO). Proteins were separated by electrophoresis at 20 mA for 4 hours on Tris-Tricine/SDS-12% polyacrylamide gels (SDS-PAGE). After electrophoresis, proteins were transferred to a polyvinylidene difluoride (PVDF) membrane using a semidry western blot apparatus at 150 mA for 1.5 hours. The membrane was then probed with the given antibody in 5% milk in TBS-T for 1 hour at room temperature (antibodies are shown in Supplemental Information). Subsequently, membranes were incubated for 1 hour with horseradish peroxidase (HRP)-conjugated anti-rabbit IgG. Target proteins were detected with the enhanced chemiluminescence (ECL) system and quantified using a densitometric image analyzer with Image-Pro Plus 4.5 software (Media Cybernetics Inc., MD).
For immunoprecipitation, lysate (100 μg of protein) was brought to a total volume of 1 ml with lysis buffer containing 0.5 μg antibody and 20 μl protein A/G PLUS–agarose beads (Santa Cruz Biotechnology, CA). The mixture was rotated in a 1.5 ml microfuge tube at 4 °C for 14 hours. Immune complexes were collected by centrifugation at 16,000 g and washed 4 times with chilled lysis buffer and analysed by SDS–PAGE.
Real-time RT-PCR
Total RNA was extracted using TRIzol Reagent (Invitrogen, CA), followed by treatment with DNA-Free (Applied Biosystems, CA) to remove contaminating DNA and then subjected to reverse transcription using an Omniscript RT kit (Applied Biosystems, CA) with random primers (Applied Biosystems, CA). Quantitative real-time RT-PCR analysis was carried out using an ABI PRISM 7500 Sequence Detection System (Applied Biosystems, CA) with SYBR Green (Takara Bio, Tokyo, Japan). Primer sequences are listed in Supplementary Table 1.
Cyclic AMP Measurement
Cyclic AMP levels were determined using a cyclic AMP chemiluminescence kit (Cell Signaling Technology, MA) according to the manufacturer’s instructions.
PDEs activity
For kinetic analysis of PDEs activity, the PDEs, 3′,5′-nucleotides, and cAMP (Abcam plc, Cambridge, UK), were used at concentrations ranging from 0.3 μM to 40 μM of cAMP and the reaction interval was 30 min according to the instrumental procedure. Blanks for spontaneous cAMP hydrolysis contained the corresponding buffer. The kinetic data were plotted as 1/[cAMP] vs. 1/v observed. Michaelis constant (Km) and maximum enzyme activity (Vmax) values were calculated from the X and Y intercepts.
Chromatin immunoprecipitation (ChIP)
The ChIP assay was performed using anti-C-FOS antibody (Santa Cruz Biotechnology, CA) and the Chromatin Immunoprecipitation Kit (Epigentek, NY) per the manufacturer’s instructions. Enrichment analysis was carried out using real-time PCR with specific primers.
Statistical analysis
All data are presented as means ± SD. Data were analyzed using Student’s t-test or one-way ANOVA followed by Tukey’s test using SPSS for Windows software (version 13.0; SPSS Inc, Chicago, IL). P < 0.05 was considered to be statistically significant.
References
Kopelman, P. G. Obesity as a medical problem. Nature 404, 635–643 (2000).
Kahn, S. E., Hull, R. L. & Utzschneider, K. M. Mechanisms linking obesity to insulin resistance and type 2 diabetes. Nature 444, 840–846 (2006).
Barrett-connor, E. L. Obesity, atherosclerosis, and coronary artery disease. Annals of Internal Medicine 103, 1010–1019 (1985).
Kratz, M., Baars, T. & Guyenet, S. The relationship between high-fat dairy consumption and obesity, cardiovascular, and metabolic disease. European Journal of Nutrition 52, 1–24 (2013).
Wahba, I. M. & Mak, R. H. Obesity and obesity-initiated metabolic syndrome: mechanistic links to chronic kidney disease. Clinical Journal of the American Society of Nephrology 2, 550–562 (2007).
Furukawa, S. et al. Increased oxidative stress in obesity and its impact on metabolic syndrome. The Journal of Clinical Investigation 114, 1752–1761 (2004).
Keaney, J. F. et al. Obesity and systemic oxidative stress. Arteriosclerosis, Thrombosis, and Vascular Biology 23, 434–439 (2003).
Özcan, U. et al. Endoplasmic reticulum stress links obesity, insulin action, and type 2 diabetes. Science 306, 457–461 (2004).
Fu, S. et al. Aberrant lipid metabolism disrupts calcium homeostasis causing liver endoplasmic reticulum stress in obesity. Nature 473, 528–531 (2011).
Mantena, S. K. et al. Mitochondrial dysfunction and oxidative stress in the pathogenesis of alcohol-and obesity-induced fatty liver diseases. Free Radical Biology and Medicine 44, 1259–1272 (2008).
Bournat, J. C. & Brown, C. W. Mitochondrial dysfunction in obesity. Current Opinion in Endocrinology, Diabetes, and Obesity 17, 446–452 (2010).
Matsuoka, T. et al. Glycation-dependent, reactive oxygen species-mediated suppression of the insulin gene promoter activity in HIT cells. Journal of Clinical Investigation 99, 144–150 (1997).
Rahmouni, K. Obesity-associated hypertension: recent progress in deciphering the pathogenesis. Hypertension 64, 215–221 (2014).
Ohara, Y., Peterson, T. E. & Harrison, D. G. Hypercholesterolemia increases endothelial superoxide anion production. Journal of Clinical Investigation 91, 2546–2551 (1993).
Berridge, M. J. The endoplasmic reticulum: a multifunctional signaling organelle. Cell Calcium 32, 235–249 (2002).
Ozcan, L. et al. Calcium signaling through CaMKII regulates hepatic glucose production in fasting and obesity. Cell Metabolism 15, 739–751 (2012).
Park, S. W. et al. Sarco (endo) plasmic reticulum Ca2+-ATPase 2b is a major regulator of endoplasmic reticulum stress and glucose homeostasis in obesity. Proceedings of the National Academy of Sciences of USA 107, 19320–19325 (2010).
Ozcan, L. et al. Activation of calcium/calmodulin-dependent protein kinase II in obesity mediates suppression of hepatic insulin signaling. Cell Metabolism 18, 803–815 (2013).
Puigserver, P. & Spiegelman, B. M. Peroxisome proliferator-activated receptor-γ coactivator 1α (PGC-1α): transcriptional coactivator and metabolic regulator. Endocrine Reviews 24, 78–90 (2003).
Liang, H. & Ward, W. F. PGC-1α: a key regulator of energy metabolism. Advances in Physiology Education 30, 145–151 (2006).
Wright, D. C. et al. Exercise-induced mitochondrial biogenesis begins before the increase in muscle PGC-1α expression. Journal of Biological Chemistry 282, 194–199 (2007).
Lehman, J. J. et al. The transcriptional coactivator PGC-1α is essential for maximal and efficient cardiac mitochondrial fatty acid oxidation and lipid homeostasis. American Journal of Physiology-Heart and Circulatory Physiology 295, H185–H196 (2008).
Lagouge, M. et al. Resveratrol improves mitochondrial function and protects against metabolic disease by activating SIRT1 and PGC-1α. Cell 127, 1109–1122 (2006).
Lira, V. A. et al. PGC-1α regulation by exercise training and its influences on muscle function and insulin sensitivity. American Journal of Physiology-Endocrinology and Metabolism 299, E145–E161 (2010).
Chalkiadaki, A. & Guarente, L. Sirtuins mediate mammalian metabolic responses to nutrient availability. Nature Reviews. Endocrinology 8, 287–296 (2012).
Pfluger, P. T. et al. Sirt1 protects against high-fat diet-induced metabolic damage. Proceedings of the National Academy of Sciences of USA 105, 9793–9798 (2008).
Colak, Y. et al. SIRT1 as a potential therapeutic target for treatment of nonalcoholic fatty liver disease. Medical Science Monitor 17, HY5–HY9 (2011).
Liang, F., Kume, S. & Koya, D. SIRT1 and insulin resistance. Nature Reviews. Endocrinology 5, 367–373 (2009).
Chalkiadaki, A. & Guarente, L. High-fat diet triggers inflammation-induced cleavage of SIRT1 in adipose tissue to promote metabolic dysfunction. Cell Metabolism 16, 180–188 (2012).
Costa Cdos, S. et al. SIRT1 transcription is decreased in visceral adipose tissue of morbidly obese patients with severe hepatic steatosis. Obesity Surgery 20, 633–639 (2010).
Banks, A. S. et al. SirT1 gain of function increases energy efficiency and prevents diabetes in mice. Cell Metabolism 8, 333–341 (2008).
Lenaz, G. et al. The function of coenzyme Q in mitochondria. Journal of Molecular Medicine 71, S66–S70 (1993).
Lenaz, G. Quinone specificity of complex I. Biochimica et Biophysica Acta (BBA)-Bioenergetics 1364, 207–221 (1998).
Kalén, A., Appelkvist, E. L. & Dallner, G. Age-related changes in the lipid compositions of rat and human tissues. Lipids 24, 579–584 (1989).
Yang, Y. K. et al. Coenzyme Q10 treatment of cardiovascular disorders of ageing including heart failure, hypertension and endothelial dysfunction. Clinica Chimica Acta 450, 83–89 (2015).
Safarinejad, M. R. et al. Effects of the reduced form of coenzyme Q10 (ubiquinol) on semen parameters in men with idiopathic infertility: a double-blind, placebo controlled, randomized study. The Journal of Urology 188, 526–531 (2012).
Toyama, K. et al. Rosuvastatin combined with regular exercise preserves coenzyme Q10 levels associated with a significant increase in high-density lipoprotein cholesterol in patients with coronary artery disease. Atherosclerosis 217, 158–164 (2011).
Someya, S. et al. Age-related hearing loss in C57BL/6J mice is mediated by Bak-dependent mitochondrial apoptosis. Proceedings of the National Academy of Sciences of USA 106, 19432–19437 (2009).
Tomasetti, M. et al. Coenzyme Q10 enrichment decreases oxidative DNA damage in human lymphocytes. Free Radical Biology and Medicine 27, 1027–1032 (1999).
Miyamae, T. et al. Increased oxidative stress and coenzyme Q10 deficiency in juvenile fibromyalgia: amelioration of hypercholesterolemia and fatigue by ubiquinol-10 supplementation. Redox Report 18, 12–19 (2013).
Schmelzer, C. & Döring, F. Micronutrient special issue: Coenzyme Q10 requirements for DNA damage prevention. Mutation Research/Fundamental and Molecular Mechanisms of Mutagenesis 733, 61–68 (2012).
Tian, G. et al. Ubiquinol-10 supplementation activates mitochondria functions to decelerate senescence in senescence-accelerated mice. Antioxidants & Redox Signaling 20, 2606–2620 (2014).
Bour, S. et al. Coenzyme Q as an antiadipogenic factor. Antioxidants & Redox Signaling 14, 403–413 (2011).
Lee, S. K. et al. Coenzyme Q10 increases the fatty acid oxidation through AMPK-mediated PPARα induction in 3T3-L1 preadipocytes. Cellular Signalling 24, 2329–2336 (2012).
Himms-Hagen, J. Thermogenesis in brown adipose tissue as an energy buffer: implications for obesity. New England Journal of Medicine 311, 1549–1558 (1984).
Nguyen, P. et al. Liver lipid metabolism. Journal of Animal Physiology and Animal Nutrition 92, 272–283 (2008).
Cantó, C. et al. AMPK regulates energy expenditure by modulating NAD + metabolism and SIRT1 activity. Nature 458, 1056–1060 (2009).
Li, Y. et al. AMPK phosphorylates and inhibits SREBP activity to attenuate hepatic steatosis and atherosclerosis in diet-induced insulin-resistant mice. Cell Metabolism 13, 376–388 (2011).
Gerhart-Hines et al. The cAMP/PKA pathway rapidly activates SIRT1 to promote fatty acid oxidation independently of changes in NAD+. Molecular Cell 44, 851–863 (2011).
Park, S. J. et al. Resveratrol ameliorates aging-related metabolic phenotypes by inhibiting cAMP phosphodiesterases. Cell 148, 421–433 (2012).
Bender, A. T. & Beavo, J. A. Cyclic nucleotide phosphodiesterases: molecular regulation to clinical use. Pharmacological Reviews 58, 488–520 (2006).
Angel, P. & Karin, M. The role of Jun, Fos and the AP-1 complex in cell-proliferation and transformation. Biochimica et Biophysica Acta (BBA)-Reviews on Cancer 1072, 129–157 (1991).
Kolch, W. Meaningful relationships: the regulation of the Ras/Raf/MEK/ERK pathway by protein interactions. Biochemical Journal 351, 289–305 (2000).
Roux, P. P. & Blenis, J. ERK and p38 MAPK-activated protein kinases: a family of protein kinases with diverse biological functions. Microbiology and Molecular Biology Reviews 68, 320-344 (2004).
Goetze, S. et al. TNFα induces expression of transcription factors c-fos, Egr-1, and Ets-1 in vascular lesions through extracellular signal-regulated kinases 1/2. Atherosclerosis 159, 93–101 (2001).
Cipolletta, E. et al. Calmodulin-dependent kinase II mediates vascular smooth muscle cell proliferation and is potentiated by extracellular signal regulated kinase. Endocrinology 151, 2747–2759 (2010).
Grenier-Larouche et al. Omental adipocyte hypertrophy relates to coenzyme Q10 redox state and lipid peroxidation in obese women. Journal of Lipid Research 56, 1985–1992 (2015).
Iwatsuka, H., Shino, A. & Suzuoki, Z. General survey of diabetic features of yellow KK mice. Endocrinologia Japonica 17, 23–35 (1970).
Ventura-Clapier, R., Garnier, A. & Veksler, V. Transcriptional control of mitochondrial biogenesis: the central role of PGC-1α. Cardiovascular Research 79, 208–217 (2008).
Gerhart-Hines, Z. et al. Metabolic control of muscle mitochondrial function and fatty acid oxidation through SIRT1/PGC-1α. The EMBO Journal 26, 1913–1923 (2007).
Carling, D., Zammit, V. A. & Hardie, D. G. A common bicyclic protein kinase cascade inactivates the regulatory enzymes of fatty acid and cholesterol biosynthesis. FEBS Letters 223, 217–222 (1987).
Salminen, A., Hyttinen, J. M. & Kaarniranta, K. AMP-activated protein kinase inhibits NF-κB signaling and inflammation: impact on healthspan and lifespan. Journal of Molecular Medicine 89, 667–676 (2011).
Steinberg, G. R. & Kemp, B. E. AMPK in health and disease. Physiological Reviews 89, 1025–1078 (2009).
Ruderman, N. B. et al. AMPK and SIRT1: a long-standing partnership? American Journal of Physiology-Endocrinology and Metabolism 298, E751–E760 (2010).
Guarente, L. Sirtuins in aging and disease. In Cold Spring Harbor Symposia on Quantitative Biology (Cold Spring Harbor Laboratory Press), pp. 483-488 (2007).
Houtkooper, R. H., Pirinen, E. & Auwerx, J. Sirtuins as regulators of metabolism and healthspan. Nature Reviews Molecular Cell Biology 13, 225–238 (2012).
Picard, F. et al. Sirt1 promotes fat mobilization in white adipocytes by repressing PPAR-γ. Nature 429, 771–776 (2004).
Arruda, A. P. & Hotamisligil, G. S. Calcium homeostasis and organelle function in the pathogenesis of obesity and diabetes. Cell Metabolism 22, 381–397 (2015).
Chang, Y., Huang, S. K. & Wang, S. J. Coenzyme Q10 inhibits the release of glutamate in rat cerebrocortical nerve terminals by suppression of voltage-dependent calcium influx and mitogen-activated protein kinase signaling pathway. Journal of Agricultural and Food Chemistry 60, 11909–11918 (2012).
Durán-Prado, M. et al. Coenzyme Q10 protects human endothelial cells from β-amyloid uptake and oxidative stress-induced injury. PloS One 9, e109223 (2014).
Acknowledgements
We thank the Kaneka Corporation of Japan for providing the mouse feed. We also thank Drs. Kiyoshi Matsumoto and Takahiro Yoshizawa (Research Center for Support to Advanced Science, Shinshu University) for technical assistance and care of mice. We thank Mr. Kiyokazu Kametani and Ms. Kayo Suzuki (Research Center for Support to Advanced Science, Shinshu University) for their skillful technical assistance.
Author information
Authors and Affiliations
Contributions
Z.X., M.M., K.Hi., and J.S. conceived and designed experiments. Z.X., J.H., D.X., M.Y., L.L. and J.D. performed the experiments. Z.X., L.L., and J.S. analyzed the data. K.Ho. and H.K. contributed reagents and materials. Z.X., K.Hi., and J.S. wrote the paper.
Corresponding author
Ethics declarations
Competing Interests
The authors declare that they have no competing interests.
Additional information
Publisher's note: Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made. The images or other third party material in this article are included in the article’s Creative Commons license, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons license and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this license, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Xu, Z., Huo, J., Ding, X. et al. Coenzyme Q10 Improves Lipid Metabolism and Ameliorates Obesity by Regulating CaMKII-Mediated PDE4 Inhibition. Sci Rep 7, 8253 (2017). https://doi.org/10.1038/s41598-017-08899-7
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41598-017-08899-7
This article is cited by
-
The pleiotropic functions of reactive oxygen species in cancer
Nature Cancer (2024)
-
Investigation of the effects of catharanthine and Q10 on Nrf2 and its association with MMP-9, MRP1, and Bcl-2 and apoptosis in a model of hepatocellular carcinoma
Naunyn-Schmiedeberg's Archives of Pharmacology (2024)
-
Vitamin B12 and coenzyme Q10 ameliorated alcohol-driven impairment of hematological parameters, inflammation, and organ damage in a mouse model
Nutrire (2023)
-
Coenzyme Q10 prevented Trypanosoma brucei rhodesiense-mediated breach of the blood brain barrier, inflammation and organ damage in late stage of Human African Trypanosomiasis
Journal of Parasitic Diseases (2023)
-
Post-Covid Asthenia Syndrome
Neuroscience and Behavioral Physiology (2023)
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.