Abstract
Mechanical stimulation of airway epithelial cells causes apical release of ATP, which increases ciliary beat frequency (CBF) and speeds up mucociliary clearance. The mechanisms responsible for this ATP release are poorly understood. CALHM1, a transmembrane protein with shared structural features to connexins and pannexins, has been implicated in ATP release from taste buds, but it has not been evaluated for a functional role in the airway. In the present study, Calhm1 knockout, Panx1 knockout, and wild-type mouse nasal septal epithelial cells were grown at an air-liquid interface (ALI) and subjected to light mechanical stimulation from an air puff. Apical ATP release was attenuated in Calhm1 knockout cultures following mechanical stimulation at a pressure of 55 mmHg for 50 milliseconds (p < 0.05). Addition of carbenoxolone, a PANX1 channel blocker, completely abolished ATP release in Calhm1 knockout cultures but not in wild type or Panx1 knockout cultures. An increase in CBF was observed in wild-type ALIs following mechanical stimulation, and this increase was significantly lower (p < 0.01) in Calhm1 knockout cultures. These results demonstrate that CALHM1 plays a newly defined role, complementary to PANX1, in ATP release and downstream CBF modulation following a mechanical stimulus in airway epithelial cells.
Similar content being viewed by others
Introduction
Effective mucociliary clearance, achieved through the coordination and modulation of ciliary beating, plays a critical role in respiratory defense. The cilia propel an airway surface liquid (ASL) that traps aerosolized debris and pathogens to the oropharynx, where it can be eliminated by either swallowing or expectoration1. Individuals who have immotile or dysfunctional cilia, such as those with primary ciliary dyskinesia or cystic fibrosis, are predisposed to frequent respiratory infections2, 3. When cilia are working properly, even small increases in ciliary beat frequency (CBF) can dramatically speed up clearance of the ASL4.
Several mechanisms exist in ciliated cells of the respiratory system to tightly control CBF and maintain efficiency. Many of these regulatory pathways result in increased extracellular ATP in the airway lumen5, which in turn increases the intracellular free Ca2+ concentration6,7,8, which subsequently results in an increase in CBF. Specifically, ATP binds two types of purinergic receptors, P2X and P2Y, on the apical surface7, 9, 10, with each receptor serving a unique purpose in modifying intracellular Ca2+. P2X receptors cause Ca2+ influx via ATP-gated Ca2+ permeable channels, and P2Y receptors cause Ca2+ release from intracellular stores via heterotrimeric G-protein activation of phospholipase C and the generation of inositol 1,4,5-trisphosphate (IP3)11,12,13,14. Following ATP stimulation of either receptor, the resulting free Ca2+ in the cytoplasm enhances CBF15, 16. Apyrase, a compound that degrades extracellular ATP, abolishes CBF increases following mechanical stimulation17.
The release of endogenous ATP from the cytoplasm to the airway surface involves pathways that are activated by mechanosensors on the ciliated cells18. In addition, forces generated by breathing, sneezing, or coughing result in ATP release from airway epithelial cells19,20,21. Other mechanical changes, such as liquid shear stress or hypotonicity, also reliably increase extracellular ATP concentration22,23,24. The mechanisms that mediate this ATP release have not yet been fully elucidated, but may include exocytotic release of vesicular ATP25 and ion channels, including connexin hemichannels and pannexins26,27,28.
PANX1 (pannexin 1) is a relatively non-selective ion channel26 that has been shown to mediate hypotonic stress and cellular deformation-induced ATP release in airway epithelium18. Pannexin channel blockers or siRNA knockdown of Panx1 inhibit ATP release by ~60% in response to hypotonic cell swelling in ciliated epithelial cell cultures29. Membrane stretch triggers Ca2+-independent ATP release through PANX1 channels26, 30, which is believed to play a role in local signaling to coordinate CBF increases31, 32. Carbenoxolone, a broad spectrum PANX1 channel blocker, inhibits ATP release by 54% from the nasal mucosa in response to physical deformation, while not completely abolishing the response33. The ATP release that is observed in airway epithelial cells even when PANX1 is blocked18 suggests that redundant pathways might contribute to ATP release following mechanical stimulation.
Calcium Homeostasis Modulator 1 (CALHM1) is a non-selective, weakly voltage gated Ca2+ permeable ion channel that shares structural features with connexins and pannexins34. The pore of CALHM1 is ~14 Å wide, similar to that of connexins34. It is activated in part by membrane depolarization and by decreases in extracellular Ca2+ concentration35. Originally discovered in an Alzheimer’s disease paradigm36, 37, CALHM1 plays a role in cortical neuron excitability35 as well as in peripheral taste perception38. Mice that lack the Calhm1 gene show no avoidance of bitter compounds and no preference for sweet and umami compounds because CALHM1 mediates the release of ATP from type II taste receptor cells in response to these compounds38. CALHM1-mediated ATP release is inhibited by ruthenium red, but not by heptanol or carbenoxolone, which block connexins and PANX1, respectively39.
Calhm1 is expressed in taste buds and in the brain, as well as in a variety of other human tissues, including the trachea36. We considered that CALHM1 might contribute to ATP release in the airway as other taste mediated signaling proteins have been identified in respiratory epithelial cells40, 41. In the present study, we confirmed Calhm1 gene expression in airway epithelium and investigated the role of CALHM1 in ATP release in airway epithelial cells in response to mechanical stimulation that simulates a sneeze.
Results
ATP Release Following a 55-mmHg Air Puff
Prior work established that a 55-mmHg air puff for 50 milliseconds simulates the pressures and timing of a sneeze, and that this is an effective in vitro model of physiologic dynamic regulation of ciliary beat frequency17. In wild type Air-Liquid Interface (ALI) cultures, CBF is reliably increased via this mechanical stimulation, and the magnitude of the CBF increase correlates with the pressure delivered to the apical surface17, 42. Mechanical stimulation of CBF involves ATP release from the cells, purinergic stimulation, and subsequent increase in intracellular Ca2+ concentration and Protein Kinase A (PKA) activation17.
Immediately following a 50-millisecond 55-mmHg air puff, culture airway surface liquid was collected, and ATP quantified. Apical ATP concentration increased in wild-type cultures 31.6-fold (baseline ATP 0.19 ± 0.02 μM), but only 10-fold in Calhm1 knockout cultures (baseline ATP 0.31 ± 0.04 μM) and 7-fold in Panx1 knockout cultures (baseline ATP 0.55 ± 0.08 μM) (n = 5 cultures per condition, p < 0.05, ANOVA with Dunnett’s multiple comparisons test; Fig. 1). This differential ATP release suggests that CALHM1, in addition to the previously studied ATP release channel PANX1, contributes to respiratory epithelial ATP release following mechanical stimulation.
Carbenoxolone is a PANX1 channel blocker that has been shown to have no activity in blocking CALHM1 currents43, but is not specific for PANX1 as it blocks other channels, including gap junctions. We incubated wild-type, Calhm1 knockout, and Panx1 knockout ALI cultures with 150 μM carbenoxolone for 20 minutes prior to stimulation, a concentration and time period that has been previously used for successful PANX1 blockade44. Apical ATP concentration increased 39 fold in wild type cultures (baseline ATP 0.36 ± 0.09 μM), 16-fold in wild type cultures incubated with carbenoxolone (baseline ATP 0.29 ± 0.09 μM), 14-fold in Panx1 knockout cultures incubated with carbenoxolone (baseline ATP 0.25 ± 0.06 μM), and 1.5-fold in Calhm1 knockout cultures incubated with carbenoxolone (baseline ATP 0.36 ± 0.09 μM) (Fig. 2). These differences were significant (p < 0.0001, ANOVA with Holm-Sidak’s multiple comparison test). These results demonstrate that for ATP release, carbenoxolone does not have an apparent effect beyond blocking PANX1, and that Calhm1 knockout cultures with blocked PANX1 (by pre-incubation with carbenoxolone) have completely abolished ATP release in response to mechanical stimulation.
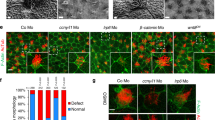
Apical ATP release 15 seconds after a 55-mmHg air puff in nasal septal epithelial cell cultures from wild-type (control) mice, and Calhm1 knockout, Panx1 knockout, and wild-type mice preincubated with 150 μM carbenoxolone. Bars are means ± SE of 5–6 cultures each. *p < 0.05, **p < 0.01, ***p < 0.001, ****p < 0.0001, ANOVA with Holm Sidak’s multiple comparisons test.
Calhm1 and Ciliary Beat Frequency Modulation
While the role of PANX1 as an airway ATP release channel has been well documented45, the presence and function of CALHM1 in the airway has not been established. Previous studies have demonstrated that PANX1 blockade attenuates ciliary beat frequency increases, which are driven by ATP release46. To further investigate the properties of the CALHM1 ATP release pathway, we asked whether the reduced ATP observed in the Calhm1 knockout cultures was also accompanied by a reduced CBF. Prior experiments have demonstrated that maximal changes in CBF occur at 15 seconds following mechanical stimulation17. In response to a 50 millisecond 55-mmHg air puff, CBF of wild-type cultures (n = 12, baseline 12.4 ± 0.9 Hz) increased above baseline frequency at 15 seconds post-stimulation, while in the Calhm1 knockout cultures (n = 12, baseline 8.7 ± 1.2 Hz), the CBF increase was significantly smaller (Fig. 3a) (p < 0.01, two-tailed t-test). The difference in baseline CBF frequency was also statistically significantly different between the two conditions (p < 0.05, two-tailed t test). While ATP release is an early event in the transduction of mechanical stimulation signals, gap junctions (which are blocked by carbenoxolone) are necessary downstream to increase CBF47. Supplemental Fig. 1 further supports this hypothesis, as all carbenoxolone pre-incubated cultures (wild type and Calhm1 knockout) show no CBF changes when stimulated with a 55 mmHg air puff.
To determine whether the reduced ATP release contributed to reduced CBF in the Calhm1 knockout cultures, 30 μl of 2-μM ATP dissolved in PBS was introduced to the apical surface of three wild-type cultures and three Calhm1 knockout cultures. Each culture had 30 μl of PBS on the apical surface before the experiment began, resulting in a final corrected ATP concentration (adjusted for an assumed ASL volume of 3.6 μl) of 16 μM, consistent with a physiologic post-stimulation ATP concentration. ATP was added at t = 0 seconds, with the post-addition recording occurring at t = 15 seconds. CBF in wild-type cultures (baseline 13.4 ± 3.7 Hz) and Calhm1 knockout cultures (baseline 13.8 ± 3.8 Hz) increased similarly at 15 seconds (Fig. 3a). Thus, ATP-dependent CBF responses were intact in the Calhm1 knockout cultures, suggesting that reduced ATP release contributed to reduced CBF responses to mechanical stimulation in the Calhm1 knockout cultures.
(a) CBF Increases 15 seconds after 1-μM ATP addition or 55-mmHg air puff in nasal septal epithelial cell cultures from Calhm1 knockout and wild-type mice. Bars are means ± SE of 3–6 cultures each. (b) ATP degradation in Calhm1 knockout wild-type mice. 5 × 10−7 M ATP was added to the apical surface t = 0, and apical ATP concentration was measured at six distinct time intervals following this addition. All Apical ATP concentrations are adjusted for a 3.6 μl ASL volume.
The differences observed in CBF changes between Calhm1 knockout and wild-type mice following mechanical stimulation could also be accounted for by differential degradation of ATP between the two types of cultures, so we set out to demonstrate equivalence in ATP degradation rates. To test this, 0.5 μM ATP was added to the apical surface of the cell cultures, and apical samplings were aspirated at six distinct time intervals (3 per culture). At all time points (15 seconds, 30 seconds, 1 minute, 5 minutes, 15 minutes, 30 minutes), there was no difference in ATP degradation rate between the cultures (Fig. 3b).
Depolarization and CBF Changes
CALHM1 is a weakly voltage-gated channel35, so we set out to test if KCl in a known depolarizing concentration48 would induce ATP release in ALI cultures. Addition of 50 mM KCl (control) produced no significant ATP release in wild-type cultures, while addition of 150 mM KCl increased ATP concentration on the apical surface 4-fold in wild type cultures, which was significantly greater than ATP changes seen in Calhm1 knockout cultures (n = 3–5 cultures per type, p < 0.01, Kruskal-Wallis with Dunn’s multiple comparison test; Fig. 4). This increase in ATP release was a full order of magnitude smaller than that observed with mechanical stimulation in our previous experiments.
Absence of Cellular Lysis following a 55 mmHg Air Puff
To test the hypothesis that cellular lysis following a 55 mmHg air puff was driving cellular ATP release, as opposed to ATP release through CALHM1, we performed a lactate dehydrogenase (LDH) assay following cellular stimulation (Supplemental Fig. 2). LDH levels were similarly low both in the control (PBS) and 55 mmHg air puff condition, indicating minimal cellular lysis. In an air puff of doubled strength (110 mmHg), significant release of LDH was observed above control and 55 mmHg conditions (n = 3 cultures per condition, p < 0.05, ANOVA with Dunnett’s multiple comparison test).
qPCR for Calhm1 and Panx1 in Cells Grown at an Air-Liquid Interface
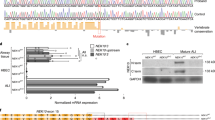
Using cDNA obtained from Panx1 knockout, Calhm1 knockout, and wild-type mouse cultures, real-time qPCR was performed to confirm Calhm1 and Panx1 gene expression in the ALI cultures. Additionally, we confirmed the relative expression levels of Calhm1 in respiratory epithelium of wild type and Panx1 knockout mice, and the relative expression levels of Panx1 in wild type and Calhm1 knockout mice. 3–6 replicates using β-actin and 3–6 replicates using target primers (Calhm1/Panx1) were performed on each cDNA sample, normalizing Calhm1/Panx1 expression to β-actin in order to determine relative expression in each condition. Calhm1 expression levels were not significantly different in Panx1 knockout and wild-type mice, and Panx1 expression levels were not significantly different in Calhm1 knockout and wild-type mice (Supplemental Fig. 3A and B). Panx1 transcripts are present in wild type samples at approximately 100 times the level of Calhm1 transcripts. Notably, no relative expression of target genes was observed in corresponding negative controls; there was no amplification of Calhm1 transcripts in Calhm1 knockout cultures or of Panx1 transcripts in Panx1 knockout cultures.
Discussion
Mechanical stimulation of airway epithelial cells causes cellular ATP release and elevated intracellular Ca2+ concentration, which in turn increases CBF16, partially due to ATP-activated P2X and P2Y receptors that are modulatory49,50,51. Exogenously administered ATP increases CBF, and apyrase (which degrades extracellular ATP) has been previously shown to abolish the CBF increase following mechanical stimulation in an air puff paradigm17. However, the mechanisms that are involved in the initial ATP release from the cells are poorly defined. PANX1 is an ion channel that is known to mediate ATP release and CBF changes in the airway46, but PANX1 channel blockers or knockdown of Panx1 only reduces this ATP release by approximately 50%18, 33, suggesting that additional channels are responsible for this persistent ATP release. CALHM1, a pore-forming channel that shares structural features with connexins and pannexins, has recently been shown to play an essential role in ATP release in taste receptor cells38. Of additional interest, several studies over the past 5 years have identified taste cell signaling molecules in ciliated cells of the respiratory epithelium41, 52, 53. Thus, we have investigated whether CALHM1 also has a role as the “missing channel” in modulation of airway ATP release. Quantitative PCR demonstrated that the Calhm1 gene was expressed in respiratory cells grown at an ALI, which were used in all of the experiments.
After mechanical stimulation by a 55-mmHg pressure air puff, apical ATP release and subsequent CBF increases were significantly lower in Calhm1 knockout cultures than in wild-type cultures. Exogenously applied ATP increased CBF to an equivalent extent in cultures derived from both Calhm1 knockout and wild-type mice. Carbenoxolone, a PANX1 channel blocker that has no effect on the CALHM1 channel, completely abolishes ATP release following mechanical stimulation when applied to Calhm1 knockout cultures, while leaving residual (presumably CALHM1-mediated) ATP release intact when applied in Panx1 knockout cultures.
Thus, our findings are consistent with the hypothesis that CALHM1 plays a complementary and equally important role to Panx1 in ATP release following cellular stress or deformation of respiratory epithelial cells. CALHM1 also appears to be a critical channel in CBF modulation as a result of this ATP release. Wild type and Calhm1 knockout cultures did not exhibit any difference in their metabolism of ATP, strengthening the evidence that channel release is driving the alteration in net apical ATP concentration. Of additional importance is that CALHM1 does not form gap junctions54, so we suspect that the CBF decrement observed in our knockout experiment is solely due to ATP release, and not due to propagation of the downstream signal.
It is known that CALHM1 is regulated by Ca2+ and membrane voltage to gate the channel, but complete understanding of the mechanism(s) has not been determined35. CALHM1 has also been localized to the endoplasmic reticulum55, where it could influence the intracellular Ca2+ homeostasis and signaling in the cell without being the specific pathway for apical ATP release in response to mechanical stimulation. CALHM1 has also not yet been demonstrated to be selectively present at the apical membrane of airway cells, so more work is needed to definitively demonstrate its unambiguous role in mechanically transduced ATP release. Further complicating the model is that pannexins exhibit properties of ATP-induced ATP release45, so a certain degree of initial ATP release, possibly through CALHM1, may be necessary for full recruitment of this channel. These pathways are not yet fully elucidated, but defining the role of CALHM1 in initiating ATP release is a critical first step.
CBF measurements and baseline ATP secretion in culture and in tissue explants are physiologic parameters with high levels of variability. Variations in culture age, degree of culture ciliation, and day-to-day changes in culture health can cause notable differences in baseline values for these physiologic parameters. To minimize any variability due to these factors, we ensured that control cultures matched their experimental counterparts in age and experimental timing. Despite this, baseline differences in CBF persist, even within a single culture. In one of our experiments, Calhm1 knockout cultures had a statistically significantly lower baseline CBF than matched wild type cultures. This was likely reflective of day-to-day baseline variability and, based on our previous work with the mouse ALI, should have minimal effects on relative (%) change. However, it is also important to consider that the differences observed in baseline CBF could be due to effects of the CALHM1 channel. ATP release is also critical for mucin hydration, which can have effects on CBF56. While this would not affect our experimental paradigm, in which ASL was removed prior to experimentation, it is nonetheless an important consideration. However, the Calhm1 knockout mice showed no evidence of phenotypic mucus plugging, nor was there any evidence of inadequate ASL hydration in ALI culture.
The discovery of a functional role for CALHM1 outside of the brain and taste buds suggests that the channel may have yet undiscovered functions in additional tissue types. The presence of CALHM1 in the airway, and its proposed role in mechanical signal transduction, has important implications for understanding regulation of mucociliary clearance and its dysregulation in diseases such as chronic rhinosinusitis. Human upper airway tissue from patients with chronic rhinosinusitis demonstrates a blunted stimulation of CBF when presented with a mechanical stimulus17, and this may play a critical role in the pathogenesis of the disease. Additionally, tissue from chronic rhinosinusitis patients also shows a blunted response following addition of exogenous ATP57. Reduced morbidity can be achieved in chronic rhinosinusitis patients by improving mucociliary movement, and subsequent clearance of pathogens, debris, and stagnant mucus. While exact functions are not fully known, it is possible that CALHM1 could be an important therapeutic target for this type of respiratory pathology.
Methods
All protocols were reviewed and approved by the Research and Development Committee at the Philadelphia Veterans Affairs Medical Center and were carried out in accordance with both the University of Pennsylvania and The Philadelphia VA Medical Center guidelines for vertebrate animal studies from the Institutional Animal Care and Use Committee of the Philadelphia Veterans Affairs Medical Center.
Reagents
The ATP, Carbenoxolone (CBX), and KCl used in these experiments were all purchased from Sigma-Aldrich (St. Louis, MO, USA). All Dulbecco’s PBS was supplemented with Ca2+ and Mg2+ using 100 mg/L of anhydrous CaCl2 and MgCl2-6H2O, respectively. For potassium chloride (KCl) addition experiments, all KCl was dissolved in PBS without NaCl and then osmolarity of the solution was adjusted to 290 mOsm with NaCl addition.
Mice
Nasal specimens from Calhm1 knockout mice35, 36, Panx1 knockout mice58, and wild type littermates were obtained from breeding colonies maintained at the Monell Chemical Senses Center (Philadelphia, PA). Panx1 knockout mice also had a passenger mutation in caspase 4/11. Both lines were maintained by backcrossing to C57BL/6J mice. Heterozygous mice were mated brother-to-sister to produce homozygous wild type and knockout mice for the experiments reported here.
Air-Liquid Interface (ALI) Cultures
We previously described the culture of mouse nasal septal epithelium at an ALI59. Briefly, nasal septal epithelial cells were harvested from sinonasal complex specimens and were digested with collagenase and pronase. Cells were grown on Costar 6.5-mm transwell permeable filter supports (Corning Inc. Life Sciences, Lowell, MA, USA). For the first 7 days, the cells were fully submerged in culture medium, and subsequently fed from only the basal chamber. Cilia appeared within two weeks, and cultures were used within 3–5 weeks.
Unless otherwise noted, transwell inserts (#3470, Corning) were removed from media before experiments and placed in a transwell containing 600 μl of Hank’s Balanced Salt Solution (HBSS) with vitamins. 30 μl of PBS was added to the apical surface of the transwell insert unless a different volume was specified, and the cultures were allowed to adjust for 15 minutes to 26 °C to ensure a steady baseline ciliary beat frequency60, 61.
Delivery of Air Puff
Air puff delivery to the ALI was performed as described by Zhao17, with one notable modification. Compressed air (Airgas Corp., Radnor, PA, USA) was released at the apical surface via a 22-gauge plastic catheter (BD, Franklin Lakes, NJ, USA) for 50 milliseconds, regulated by a Pico-Spritzer II 2-valve microinjector ejector (General Valve Corp., Fairfield, NJ, USA). In contrast with the experimental methods used by Zhao et al., the catheter was placed directly in the center of the transwell to deliver a more uniform stimulation across the transwell. The catheter was attached to a micromanipulator, which allowed for placement 6 mm above the apical surface, directly in the center of the transwell (3.25 mm away from each transwell side).
A manometer (Traceable Manometer/Pressure/Vacuum Gauge, 3460; Control Co., Friendswood, TX, USA) was used to calibrate the pressure delivered to the culture. The transwell insert was sealed with a stopper that had two 22-gauge holes, with pressure being applied through one hole while the other hole was connected to the manometer.
CBF Imaging and Analysis
Ciliated areas in all cultures tested were observed using a 20X objective on an inverted microscope (Leica Microsystems, Bannockburn, IL, USA). A model A602f-2 Basler area scan high-speed monochromatic digital video camera (Basler AG, Ahrensburg, Germany) captured images at 100 frames/s with a resolution of 650 × 480 pixels. Digital image signals from the camera were sampled by an acquisition board (National Instruments, Austin, TX, USA) on a Dell XPS 710 workstation (Dell, Inc., Round Rock, TX, USA) running the Windows XP Professional operating system (Microsoft, Redmond, WA, USA). Video images were analyzed with the Sisson-Ammons Video Analysis (SAVA) software (National Instruments) that is specialized to quantify CBF62 by performing a whole-field analysis of the ciliated apical surface of the cultures, reporting a CBF that is the arithmetic mean of all of the cilia in the video field. Consistent with prior imaging analyses17, any videos in which less than 5% of the imaged field was ciliated were excluded. In reporting CBF values, changes were normalized per convention to a basal frequency of 100%, with increases and decreases in CBF reported as a percentage of this baseline frequency6, 17.
All experiments were conducted using air puff pressures of 55 mmHg. The air puff was always delivered to the middle of the transwell, 6 mm above the apical surface fluid, for 50 milliseconds. Once the cultures equilibrated to 26 °C, CBF during four 15-second intervals was recorded to determine a baseline frequency. The air puff was then delivered, and measurements were recorded every 15 seconds.
ATP Release Assay
The apical surfaces of the ALI cultures were washed 3 times with PBS, and then incubated for 30 minutes with 50 μl of fresh PBS on the apical surface. Five minutes before the air puff, 10 μl of apical fluid was aspirated and diluted 10 times in PBS, and then boiled for 2 minutes to prevent degradation of ATP. At 15 seconds following the air puff, another 10 μl of apical fluid was aspirated, diluted 10 times in PBS, and then boiled for 2 minutes. Each ATP assay was carried out immediately following the experiment. The Enliten ATP assay kit (Promega, Madison WI, USA) was used for ATP quantification. A 10-μl blank, ATP standard, or sample solution was added to the wells of a 96-well microplate, and 100 μl of luciferin-luciferase (rL/L) reagent was added. A luminometer (Luminoskan Ascent 2.5; Thermo Labsystems, Franklin, MA, USA) quantified the ATP present in each sample using a 10-second integration time. As apical fluid volume varied depending on experimental conditions, all reported values are normalized to a 3.6 μl ASL volume, which has been experimentally determined to be the residual fluid on the apical surface following aspiration or clearance63. This correction is performed to approximate a physiologically relevant ATP concentration for use in future experimental paradigms; the volume of apical fluid used in our experiments for technical feasibility is higher than would be expected in vivo.
qPCR
Wild-type, Calhm1 knockout, and Panx1 knockout cells grown for several weeks at an ALI were lysed using QiaShredder (Qiagen, cat# 79656) and total RNA was purified with an RNeasy Micro Kit (Qiagen, cat# 74004) according to standard protocols. Following purification, RNA was reverse-transcribed with an Invitrogen SuperScript III First-Strand cDNA Synthesis kit (Themo Fisher, cat# 18080051). Using this cDNA, real-time qPCR was carried out with SYBR® Green PCR Master Mix (Applied Biosystems, cat# 4309155) on an Applied Biosystems 7500 Real-Time PCR System (Applied Biosystems) for the analysis of β-actin, Calhm1, and Panx1 genes. Primers were obtained from PrimePCR™ Assays and Controls (Bio-Rad) for ActB (β-actin) and Panx1, and Calhm1 primers were obtained from Integrated DNA Technologies (F-primer: AGAACTTGCTCGCCTACTGG R-primer: CTCTTGAGAAAGGCGACCTG). β-actin was used as the house-keeping gene, and Calhm1 and Panx1 gene expression was determined by the 2−ΔΔC T method64, which uses fluorescence and threshold values (CT) to compare the relative amount of target mRNA. PCR cycling conditions were 95 °C for 30 seconds, 65 °C for 30 seconds, and 72 °C for 45 seconds. All target expression levels were normalized relative to β-actin expression levels from paired cDNA samples.
Statistics
GraphPad Prism5 (GraphPad Software, San Diego, CA, USA) was used for all statistical analyses, with results shown as means ± standard error. Kolmogorov-Smirnov (KS) testing for a Gaussian distribution was used to confirm normality of data and the use of parametric testing. An unpaired Student’s t-test was used for all comparisons unless otherwise noted, or if a non-parametric test was indicated by KS testing. A value of p < 0.05 was considered to be statistically significant.
Data Availability
All data generated or analyzed during this study are available from the corresponding author on reasonable request.
References
Boucher, R. C. Regulation of airway surface liquid volume by human airway epithelia. Pflugers Archiv: European journal of physiology 445, 495–498, doi:10.1007/s00424-002-0955-1 (2003).
Wanner, A., Salathe, M. & O’Riordan, T. G. Mucociliary clearance in the airways. American journal of respiratory and critical care medicine 154, 1868–1902, doi:10.1164/ajrccm.154.6.8970383 (1996).
Hayashi, T. et al. ATP regulation of ciliary beat frequency in rat tracheal and distal airway epithelium. Experimental physiology 90, 535–544, doi:10.1113/expphysiol.2004.028746 (2005).
Seybold, Z. V. et al. Mucociliary interaction in vitro: effects of physiological and inflammatory stimuli. Journal of applied physiology 68, 1421–1426 (1990).
Button, B., Picher, M. & Boucher, R. C. Differential effects of cyclic and constant stress on ATP release and mucociliary transport by human airway epithelia. The Journal of physiology 580, 577–592, doi:10.1113/jphysiol.2006.126086 (2007).
Zhang, L. & Sanderson, M. J. The role of cGMP in the regulation of rabbit airway ciliary beat frequency. The Journal of physiology 551, 765–776, doi:10.1113/jphysiol.2003.041707 (2003).
Marino, A. et al. Regulation by P2 agonists of the intracellular calcium concentration in epithelial cells freshly isolated from rat trachea. Biochimica et biophysica acta 1439, 395–405 (1999).
Zhang, L. & Sanderson, M. J. Oscillations in ciliary beat frequency and intracellular calcium concentration in rabbit tracheal epithelial cells induced by ATP. The Journal of physiology 546, 733–749 (2003).
Wong, L. B. & Yeates, D. B. Luminal purinergic regulatory mechanisms of tracheal ciliary beat frequency. American journal of respiratory cell and molecular biology 7, 447–454 (1992).
Braiman, A., Gold’Shtein, V. & Priel, Z. Feasibility of a sustained steep Ca(2+)Gradient in the cytosol of electrically non-excitable cells. Journal of theoretical biology 206, 115–130, doi:10.1006/jtbi.2000.2104 (2000).
Harden, T. K., Boyer, J. L. & Nicholas, R. A. P2-purinergic receptors: subtype-associated signaling responses and structure. Annual review of pharmacology and toxicology 35, 541–579, doi:10.1146/annurev.pa.35.040195.002545 (1995).
Ralevic, V. & Burnstock, G. Receptors for purines and pyrimidines. Pharmacological reviews 50, 413–492 (1998).
Berridge, M. J. Inositol trisphosphate and calcium signalling. Nature 361, 315–325, doi:10.1038/361315a0 (1993).
Bootman, M. D. et al. Calcium signalling–an overview. Seminars in cell & developmental biology 12, 3–10, doi:10.1006/scdb.2000.0211 (2001).
Lieb, T., Frei, C. W., Frohock, J. I., Bookman, R. J. & Salathe, M. Prolonged increase in ciliary beat frequency after short-term purinergic stimulation in human airway epithelial cells. The Journal of physiology 538, 633–646 (2002).
Lansley, A. B. & Sanderson, M. J. Regulation of airway ciliary activity by Ca2+: simultaneous measurement of beat frequency and intracellular Ca2+. Biophysical journal 77, 629–638, doi:10.1016/S0006-3495(99)76919-5 (1999).
Zhao, K. Q. et al. Molecular modulation of airway epithelial ciliary response to sneezing. FASEB journal: official publication of the Federation of American Societies for Experimental Biology 26, 3178–3187, doi:10.1096/fj.11-202184 (2012).
Seminario-Vidal, L. et al. Rho signaling regulates pannexin 1-mediated ATP release from airway epithelia. The Journal of biological chemistry 286, 26277–26286, doi:10.1074/jbc.M111.260562 (2011).
Kallok, M. J., Lai-Fook, S. J., Hajji, M. A. & Wilson, T. A. Axial distortion of airways in the lung. Journal of applied physiology: respiratory, environmental and exercise physiology 54, 185–190 (1983).
Grygorczyk, R. & Hanrahan, J. W. CFTR-independent ATP release from epithelial cells triggered by mechanical stimuli. The American journal of physiology 272, C1058–1066 (1997).
Homolya, L., Steinberg, T. H. & Boucher, R. C. Cell to cell communication in response to mechanical stress via bilateral release of ATP and UTP in polarized epithelia. The Journal of cell biology 150, 1349–1360 (2000).
Guyot, A. & Hanrahan, J. W. ATP release from human airway epithelial cells studied using a capillary cell culture system. The Journal of physiology 545, 199–206 (2002).
Lazarowski, E. R. et al. Nucleotide release provides a mechanism for airway surface liquid homeostasis. The Journal of biological chemistry 279, 36855–36864, doi:10.1074/jbc.M405367200 (2004).
Tarran, R. et al. Normal and cystic fibrosis airway surface liquid homeostasis. The effects of phasic shear stress and viral infections. The Journal of biological chemistry 280, 35751–35759, doi:10.1074/jbc.M505832200 (2005).
Bodin, P. & Burnstock, G. Purinergic signalling: ATP release. Neurochemical research 26, 959–969 (2001).
Bao, L., Locovei, S. & Dahl, G. Pannexin membrane channels are mechanosensitive conduits for ATP. FEBS letters 572, 65–68, doi:10.1016/j.febslet.2004.07.009 (2004).
Qiu, F. & Dahl, G. A permeant regulating its permeation pore: inhibition of pannexin 1 channels by ATP. American journal of physiology. Cell physiology 296, C250–255, doi:10.1152/ajpcell.00433.2008 (2009).
Shestopalov, V. I. & Panchin, Y. Pannexins and gap junction protein diversity. Cellular and molecular life sciences: CMLS 65, 376–394, doi:10.1007/s00018-007-7200-1 (2008).
Ransford, G. A. et al. Pannexin 1 contributes to ATP release in airway epithelia. American journal of respiratory cell and molecular biology 41, 525–534, doi:10.1165/rcmb.2008-0367OC (2009).
Okada, S. F., Nicholas, R. A., Kreda, S. M., Lazarowski, E. R. & Boucher, R. C. Physiological regulation of ATP release at the apical surface of human airway epithelia. The Journal of biological chemistry 281, 22992–23002, doi:10.1074/jbc.M603019200 (2006).
Praetorius, H. A. & Leipziger, J. ATP release from non-excitable cells. Purinergic signalling 5, 433–446, doi:10.1007/s11302-009-9146-2 (2009).
MacVicar, B. A. & Thompson, R. J. Non-junction functions of pannexin-1 channels. Trends in neurosciences 33, 93–102, doi:10.1016/j.tins.2009.11.007 (2010).
Ohbuchi, T. et al. Possible contribution of pannexin-1 to ATP release in human upper airway epithelia. Physiological reports 2, e00227, doi:10.1002/phy2.227 (2014).
Siebert, A. P. et al. Structural and functional similarities of calcium homeostasis modulator 1 (CALHM1) ion channel with connexins, pannexins, and innexins. The Journal of biological chemistry 288, 6140–6153, doi:10.1074/jbc.M112.409789 (2013).
Ma, Z. et al. Calcium homeostasis modulator 1 (CALHM1) is the pore-forming subunit of an ion channel that mediates extracellular Ca2+ regulation of neuronal excitability. Proceedings of the National Academy of Sciences of the United States of America 109, E1963–1971, doi:10.1073/pnas.1204023109 (2012).
Dreses-Werringloer, U. et al. A polymorphism in CALHM1 influences Ca2+ homeostasis, Abeta levels, and Alzheimer’s disease risk. Cell 133, 1149–1161, doi:10.1016/j.cell.2008.05.048 (2008).
Lambert, J. C. et al. The CALHM1 P86L polymorphism is a genetic modifier of age at onset in Alzheimer’s disease: a meta-analysis study. Journal of Alzheimer’s disease: JAD 22, 247–255, doi:10.3233/JAD-2010-100933 (2010).
Taruno, A. et al. CALHM1 ion channel mediates purinergic neurotransmission of sweet, bitter and umami tastes. Nature 495, 223–226, doi:10.1038/nature11906 (2013).
Ma, Z. M. et al. CALHM1 is an Extracellular Ca2+- and Voltage-Gated ATP Permeable Ion Channel. Biophysical journal 104, 631A (2013).
Lee, R. J. et al. Bitter and sweet taste receptors regulate human upper respiratory innate immunity. The Journal of clinical investigation 124, 1393–1405, doi:10.1172/JCI72094 (2014).
Lee, R. J. et al. T2R38 taste receptor polymorphisms underlie susceptibility to upper respiratory infection. The Journal of clinical investigation 122, 4145–4159, doi:10.1172/JCI64240 (2012).
Gwaltney, J. M. Jr. et al. Nose blowing propels nasal fluid into the paranasal sinuses. Clinical infectious diseases: an official publication of the Infectious Diseases Society of America 30, 387–391, doi:10.1086/313661 (2000).
Taruno, A., Matsumoto, I., Ma, Z., Marambaud, P. & Foskett, J. K. How do taste cells lacking synapses mediate neurotransmission? CALHM1, a voltage-gated ATP channel. BioEssays: news and reviews in molecular, cellular and developmental biology 35, 1111–1118, doi:10.1002/bies.201300077 (2013).
Sridharan, M. et al. Pannexin 1 is the conduit for low oxygen tension-induced ATP release from human erythrocytes. American journal of physiology. Heart and circulatory physiology 299, H1146–1152, doi:10.1152/ajpheart.00301.2010 (2010).
Dahl, G. ATP release through pannexon channels. Philosophical transactions of the Royal Society of London. Series B, Biological sciences 370, doi:10.1098/rstb.2014.0191 (2015).
Ohbuchi, T. et al. Possible contribution of pannexin-1 to capsaicin-induced ATP release in rat nasal columnar epithelial cells. Channels, 1–8, doi:10.1080/19336950.2017.1293209 (2017).
Sanderson, M. J., Charles, A. C. & Dirksen, E. R. Mechanical stimulation and intercellular communication increases intracellular Ca2+ in epithelial cells. Cell regulation 1, 585–596 (1990).
Huang, Y. A. et al. Knocking out P2X receptors reduces transmitter secretion in taste buds. The Journal of neuroscience: the official journal of the Society for Neuroscience 31, 13654–13661, doi:10.1523/JNEUROSCI.3356-11.2011 (2011).
Davis, C. W. & Dickey, B. F. Regulated airway goblet cell mucin secretion. Annual review of physiology 70, 487–512, doi:10.1146/annurev.physiol.70.113006.100638 (2008).
Weiterer, S. et al. Tumor necrosis factor alpha induces a serotonin dependent early increase in ciliary beat frequency and epithelial transport velocity in murine tracheae. PloS one 9, e91705, doi:10.1371/journal.pone.0091705 (2014).
Kunzelmann, K. et al. Control of ion transport in mammalian airways by protease activated receptors type 2 (PAR-2). FASEB journal: official publication of the Federation of American Societies for Experimental Biology 19, 969–970, doi:10.1096/fj.04-2469fje (2005).
Shah, A. S., Ben-Shahar, Y., Moninger, T. O., Kline, J. N. & Welsh, M. J. Motile cilia of human airway epithelia are chemosensory. Science 325, 1131–1134, doi:10.1126/science.1173869 (2009).
Lee, R. J., Chen, B., Redding, K. M., Margolskee, R. F. & Cohen, N. A. Mouse nasal epithelial innate immune responses to Pseudomonas aeruginosa quorum-sensing molecules require taste signaling components. Innate immunity 20, 606–617, doi:10.1177/1753425913503386 (2013).
Ma, Z., Tanis, J. E., Taruno, A. & Foskett, J. K. Calcium homeostasis modulator (CALHM) ion channels. Pflugers Archiv: European journal of physiology 468, 395–403, doi:10.1007/s00424-015-1757-6 (2016).
Gallego-Sandin, S., Alonso, M. T. & Garcia-Sancho, J. Calcium homoeostasis modulator 1 (CALHM1) reduces the calcium content of the endoplasmic reticulum (ER) and triggers ER stress. The Biochemical journal 437, 469–475, doi:10.1042/BJ20110479 (2011).
Button, B., Okada, S. F., Frederick, C. B., Thelin, W. R. & Boucher, R. C. Mechanosensitive ATP release maintains proper mucus hydration of airways. Science signaling 6, ra46, doi:10.1126/scisignal.2003755 (2013).
Chen, B. et al. Altered sinonasal ciliary dynamics in chronic rhinosinusitis. American journal of rhinology 20, 325–329 (2006).
Dvoriantchikova, G. et al. Genetic ablation of Pannexin1 protects retinal neurons from ischemic injury. PloS one 7, e31991, doi:10.1371/journal.pone.0031991 (2012).
Antunes, M. B. et al. Murine nasal septa for respiratory epithelial air-liquid interface cultures. BioTechniques 43, 195–196 (2007). 198, 200 passim.
Zhang, L. et al. Effects of ephedrine on human nasal ciliary beat frequency. ORL; journal for oto-rhino-laryngology and its related specialties 70, 91–96, doi:10.1159/000114531 (2008).
Zhou, H. et al. Increased nasal epithelial ciliary beat frequency associated with lifestyle tobacco smoke exposure. Inhalation toxicology 21, 875–881, doi:10.1080/08958370802555898 (2009).
Sisson, J. H., Stoner, J. A., Ammons, B. A. & Wyatt, T. A. All-digital image capture and whole-field analysis of ciliary beat frequency. Journal of microscopy 211, 103–111 (2003).
Harvey, P. R., Tarran, R., Garoff, S. & Myerburg, M. M. Measurement of the airway surface liquid volume with simple light refraction microscopy. American journal of respiratory cell and molecular biology 45, 592–599, doi:10.1165/rcmb.2010-0484OC (2011).
Livak, K. J. & Schmittgen, T. D. Analysis of relative gene expression data using real-time quantitative PCR and the 2(-Delta Delta C(T)) Method. Methods 25, 402–408, doi:10.1006/meth.2001.1262 (2001).
Acknowledgements
This work was supported by a grant from a philanthropic contribution from the RLG Foundation, Inc. (NAC), and USPHS grants R01DC013588 (NAC), R01DK046791 and DC10393 (MGT).
Author information
Authors and Affiliations
Contributions
N.A.C. and A.D.W. designed research, A.D.W., R.M.C., R.J.L., and C.J.S. analyzed data, A.D.W., R.M.C., and B.C. performed research, A.D.W. wrote the manuscript, M.G.T. provided live animals, P.M., C.H.M., R.J.L. and M.G.T. contributed reagents and analytic tools in addition to scientific expertise in manuscript preparation.
Corresponding author
Ethics declarations
Competing Interests
The authors declare that they have no competing interests.
Additional information
Publisher's note: Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made. The images or other third party material in this article are included in the article’s Creative Commons license, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons license and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this license, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Workman, A.D., Carey, R.M., Chen, B. et al. CALHM1-Mediated ATP Release and Ciliary Beat Frequency Modulation in Nasal Epithelial Cells. Sci Rep 7, 6687 (2017). https://doi.org/10.1038/s41598-017-07221-9
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41598-017-07221-9
This article is cited by
-
Control of astrocytic Ca2+ signaling by nitric oxide-dependent S-nitrosylation of Ca2+ homeostasis modulator 1 channels
Biological Research (2024)
-
Effectiveness of paranasal air suction on acute migraine using portable air sucker – a randomized, double blind study
BMC Neurology (2021)
-
Human Pannexin 1 channel: Insight in structure–function mechanism and its potential physiological roles
Molecular and Cellular Biochemistry (2021)
-
Motile cilia genetics and cell biology: big results from little mice
Cellular and Molecular Life Sciences (2021)
-
Influenza A virus enhances ciliary activity and mucociliary clearance via TLR3 in airway epithelium
Respiratory Research (2020)
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.