Abstract
Consumption of coffee and diet drinks and the use of non-nutritive sweeteners is commonplace worldwide. We conducted a cross-sectional analysis to investigate the associations between coffee consumption and non-nutritive sweetener use and depression among populations in Atlantic Canada. During 2009 to 2013, we recruited 18838 participants aged 35–69 years (5854 men and 12984 women) for the baseline survey of the Atlantic Partnership for Tomorrow’s Health cohort study. Coffee consumption, sweetener use, and major depression were assessed using a set of standardized questionnaires. We utilized multiple logistic regression models to assess the associations of coffee drinking and non-nutritive sweetener use with major depression. Compared with non-coffee drinkers, female participants who drank coffee ≥4 cups/day had an odds ratio of 1.38 (95% confidence interval, 1.15–1.64) for major depression with adjustment for sociodemographic and behavioral factors, chronic disease status, and body mass index. We found a significant association between depression and consumption of sweeteners and diet drinks, which was more apparent among women than men. We conclude that heavy coffee drinking and non-nutritive sweetener use were associated with depression among populations in Atlantic Canada. Further studies are warranted to investigate the underlying biological mechanisms.
Similar content being viewed by others
Introduction
Depression is an increasing public health concern that influences both quality of life and disease outcome1. Risk factors associated with depression are not fully understood. Coffee is the second most popular source of beverage intake in Canada, accounting for around 80% of daily caffeine intake among Canadian adults2. Non-nutritive sweeteners (NNS) have been included in the Canadian nutritional guidelines for decades in terms of cardiometabolic disease control and prevention3. A national survey showed that Canadians consume large quantities of diet drinks2. Few studies have assessed whether depression, coffee drinking, and NNS use are correlated among Canadians.
Some evidence indicates that those who drink coffee, compared with non-coffee drinkers, have a decreased risk of developing type 2 diabetes, coronary heart disease, and stroke4. However, the relationship between heavy coffee consumption and overall health remains controversial. Recently, two large-scale population-based longitudinal studies reported contrasting associations between heavy coffee drinking (≥4 cups/day) and all-cause mortality5, 6. There are also some inconsistencies apparent in meta-analysis studies. Two meta-analyses showed that coffee consumption was inversely associated with cardiovascular disease (CVD) and all-cause mortality7, 8. One meta-analysis found that moderate coffee drinking was inversely associated with CVD mortality, with the lowest risk being observed at three to five cups per day. Heavy coffee drinking (>5 cups/day) was not related to decreased CVD mortality9. Further, a large-scale observational and Mendelian randomization study reported a U-shaped association between coffee consumption and CVD and all-cause mortality. However, genetic variations that influence caffeine intake was not related to either CVD or all-cause mortality10. Similarly, the epidemiologic evidence to date concerning coffee consumption and depression has been contradictory; studies have reported both increased and decreased risk of depression with coffee drinking11,12,13,14, though two recent systematic reviews suggested an inverse association15, 16. These findings may imply that other factors that are associated with coffee consumption may play a role in the observed associations between coffee drinking and health outcomes.
Regarding the health consequences of NNS use, a recent study from the US reported an association between consumption of diet drinks and depression17. Two systematic reviews raised a concern regarding the effects of diet drink consumption on body weight control18 and type 2 diabetes prevention19. As consumption of coffee and diet drinks and the use of artificial sweeteners is commonplace in Canada2, 3, we hypothesized that coffee drinking, diet drink consumption, and NNS use might be correlated and related to depression among Canadians. Therefore, we assessed the associations of coffee drinking, diet drink consumption, and NNS use with depression amongst people aged 35 to 69 years old participating in the baseline survey of the Atlantic Partnership for Tomorrow’s Health (Atlantic PATH) cohort study.
Results
General characteristics of study participants
Among the study participants, 62.4% reported coffee drinking. Of these, 52.7% drank regular coffee, 5.7% drank decaffeinated coffee, and 4.0% drank both. For NNS use, 44.3% reported the consumption of either NNS or diet drinks. Of these, 5.3% added NNS to coffee or tea, 31.9% drank diet drinks, and 7.1% reported both. The overall prevalence of major depression was 17.1% and was significantly higher in women than men (19.7% versus 11.2%, P < 0.001, Table 1 and Supplemental Tables 1 and 2). Coffee drinking and NNS use were significantly correlated, and they were also positively correlated with depressive symptom scores (Table 2).
Compared with women, men were more likely to drink regular coffee and be a heavy coffee drinker (≥4 cups/day) but less likely to consume diet drinks (Table 1). Moreover, compared with non-coffee drinkers, heavy coffee drinkers were more likely to be highly educated, be current smokers and alcohol drinkers, and have cardiovascular disease. Meanwhile, they also had higher levels of BMI, physical activity, and diet quality (Supplemental Table 1). Compared with non-NNS users, participants who both added NNS in coffee or tea and consumed diet drinks were less likely to be highly educated and were more likely to have cardiovascular disease and diabetes. They also had higher levels of BMI, physical activity, and diet quality (Supplemental Table 2).
Associations between coffee drinking and major depression
Compared with non-coffee drinkers, female participants who drank ≥4 cups/day of any form of coffee had an increased likelihood of having major depression (odds ratio [OR], 1.46; 95% confidence interval [CI], 1.24–1.73) with adjustment for age (Table 3). After further controlling for sociodemographic and lifestyle factors, health status, and BMI, the association between heavy coffee consumption and increased depression remained statistically significant (OR, 1.38; 95% CI, 1.15–1.64). The stratified analyses by two types of coffee showed that this association was apparent only in regular coffee drinkers.
Associations between sweetener use and major depression
In analyses adjusted only for age, daily addition of NNS in coffee or tea and consumption of diet drinks were associated with a significantly increased likelihood of having major depression in both men and women (Table 4). After controlling for the covariables, the association was more apparent amongst women than men. In the multivariable adjusted logistic regression analyses, compared with those who never added NNS in coffee or tea, both male and female participants who always added NNS in coffee or tea had significantly increased likelihoods for major depression (OR, 1.39; 95% CI, 1.05–1.83 for males and OR, 1.31; 95% CI, 1.13–1.53 for females). For diet drinks, the association was apparent among women only. Compared with those who never drank diet drinks, female participants who drank diet drinks ≥1 times/day had an increased likelihood for major depression (OR, 1.66; 95% CI, 1.38–2.00). In the combined analyses, female participants who both added NNS in coffee or tea and drank diet drinks had an increased likelihood for major depression (OR, 1.32; 95% CI, 1.12–1.55) compared with those who did not add NNS in coffee or tea or drink diet drinks.
In the both sexes combined analyses, both heavy coffee drinking and any NNS use were associated with increased likelihoods of having major depression after adjustment for all the covariables (Table 5). In the stratified analysis by two major depression risk factors (Table 6), heavy coffee drinking was associated with major depression across all smoking and overweight or obesity strata. Whereas, the association between NNS use and major depression was apparent only among those who were never smokers and with overweight or obesity. In the smoking and BMI combined analyses, the associations were evident among those who were never smokers with normal weight and those who were ever smokers with overweight or obesity.
Discussion
In this large-scale, population-based cross-sectional analysis, we found that coffee drinking and NNS use were popular among participant populations of the Atlantic PATH study. Depression, coffee drinking, and NNS use were positively correlated. Heavy coffee drinking and NNS use were associated with major depression. This association was independent of sociodemographic and behavioral factors, chronic disease status, and body weight, but was more evident among women than men. In addition, the associations of heavy coffee drinking and NNS use with depression appeared to be independent of smoking and obesity, which are known risk factors for major depression.
Our data showed that heavy coffee drinkers and NNS users were more likely to have a worse risk factor profile for cardiometabolic disease compared with non-coffee drinkers and non-NNS users. The phenomenon has been observed in some longitudinal studies assessing the associations of coffee drinking with the risk of all-cause mortality5, 6, 20. The most consistent trend among the three large-scale population-based studies is that heavy coffee drinkers (≥4 cups/day) had significantly higher prevalence of smoking compared with non-coffee drinkers. Two out of the three studies reported that heavy coffee drinkers had either relatively higher levels of BMI5 or prevalence of overweight or obesity20 than non-coffee drinkers. Interestingly, heavy coffee drinking was associated with increased risk of all-cause mortality in the simple adjusted models among all the three studies5, 6, 20. After multivariable adjustment, two studies showed an inverse association between heavy coffee drinking and all-cause mortality6, 20. Whereas one positive association remained5. Further stratified analyses revealed that the multivariable adjusted inverse association between heavy coffee drinking and all-cause mortality existed only among those non-smokers but not current smokers6, 20. These observations might imply that the association between heavy coffee drinking and all-cause mortality might be affected by risk factor profiles of the heavy coffee drinkers who participated in these studies.
Our results are consistent with data from some studies11, 12, 21 but not others13, 22, 23 that reported associations between coffee drinking and mental health. Among these studies, Lucas et al. reported an inverse association between coffee drinking and risk of developing depression in the Nurses’ Health Study22. In this study, women who reported coffee drinking ≥4 cups/day had lower non-smoking rate compared with those who drank ≤1 cup/week, and there was no association between coffee drinking and depression risk in the age-adjusted analysis. The inverse association appeared after multivariable adjustment for major lifestyle risk factors and BMI.
In our cross-sectional analyses, we found that the positive association between heavy coffee drinking and depression was evident among both low and high risk individuals in terms of smoking and BMI levels. As coffee drinking is the primary source of caffeine intake among Canadians2, it is likely that higher coffee consumption may result in the higher intake of caffeine. Depressed individuals might choose to consume more caffeine, for example as a form of self-medication24.
In addition to individual studies, results from meta-analyses have also been inconsistent. A U-shaped association between coffee drinking and CVD mortality was reported in one study9 but not replicated by two other studies7, 8. Two meta-analyses showed that coffee consumption was consistently and inversely associated with depression, although this trend was not apparent for caffeine intake15, 16. Regarding other cognitive disorders, one study reported that the protective effect of coffee consumption on Parkinson’s disease risk was found at 3 cups/day25. By contrast, Kim et al. reported that there were no associations detected between coffee consumption and cognitive disorders26. In another study, pooled analyses did not show an association between habitual coffee consumption and risk of cognitive decline or dementia, but in sub-group analyses, there was an inverse association between coffee consumption and Alzheimer disease27. However, a major concern is that these pooled analyses rarely controlled for confounding factors across the selected studies, which also makes direct comparison with our findings problematic. Indeed, inconsistencies in findings across different studies suggests that unmeasured confounding is an important issue. A Mendelian randomization study design has a unique advantage in this respect because genetic variations in the targeted exposure are not related to the confounders28. By using this approach, a Danish study found that the genetic variations that are significantly related to caffeine intake were not associated with mortality from CVD and all-causes10. These findings imply that a Mendelian randomization study design may help elucidate whether the observed associations between coffee consumption and mental health is due to the effects of residual confounding factors or the effects of caffeine intake per se. In this regard, further well-designed studies, such as Mendelian randomization studies, are needed to confirm our findings and investigate the possible underlying biological mechanisms.
Though NNS use in foods is increasing, particularly among developed countries, data on the health consequences of NNS use are scarce. More recently, a study found a positive association between NNS use and depression risk among a large sample of older US adults17. We found that NNS users were more likely to report having diabetes in our study participants. Some studies reported that people with diabetes mellitus are associated with increased risk for depression29. However, we cannot rule out, due to the cross-sectional nature of the study, that the observed association we found is a result of reverse causality. Obese individuals have also been shown to be more likely to consume beverages and foods containing NNS30. Meanwhile, obese individuals are more likely to develop major depression31. Mattes and Popkin32 reported that the increasing use of NNS in foods parallels the increase in BMI in populations from industrialized countries. There is currently no direct evidence linking NNS use with obesity risk, but a Canadian study observed that daily NNS use among pregnant women was associated with increased infant BMI compared with the counterparts of non-NNS users33. Among our study participants, about a half reported the consumption of either NNS or diet drinks, and our data suggested that individuals who reported the consumption of NNS or diet drinks might have more risk factors associated with depression compared with those who did not. The association between NNS use and depression was apparent only among those who were overweight or obese. Given the high average levels of BMI in both men and women and the close relationship between obesity and depression, further studies are needed to investigate whether the interactions between heavy coffee drinking and NNS use may influence depression development.
Participants who were heavy coffee drinkers or frequent NNS users had relatively higher levels of BMI and lower levels of educational attainment. Meanwhile, they were more likely to be a current smoker and have cardiometabolic diseases. Most of these factors have been proven to be associated with the increased depression risk and are modifiable34. Our findings might imply that appropriate interventional programs tailored for cardiometabolic risk factor modifications targeting people who are heavy coffee drinkers and frequent NNS users may help ameliorate depressive symptoms and related comorbidities among participant populations.
The large sample size and well-controlled confounding factors are major advantages of this study. We also plotted depression risk factors by different levels of coffee drinking and frequencies of NNS use. Nonetheless, our analysis has some limitations. The majority of our study participants are white, and participants were not randomly selected from the populations in the Atlantic Canada provinces, this may limit the generalizability of our study findings to other populations. However, this is not necessarily a shortcoming for examining the association of depressive symptom with beverage consumption. In our analyses, we defined major depression with a set of validated questionnaires35 but did not include clinical diagnosis by a physician. This method might lead to some miss-classifications of the study outcomes and consequently result in an underestimation of the observed associations. We assessed NNS use as frequencies of daily intake but not the amount; this might compromise the strength of the observed associations as well. The associations of heavy coffee drinking and NNS use with depression were more apparent among women than men. This finding might be due to that the sample size of male participants was smaller than females and men had significantly lower prevalence of depression than women. The P values for interactions between men and women were not statistically significant indicating that men and women had similar trends in these associations. Finally, the cross-sectional nature of the study means we cannot infer causation from these results.
In summary, our findings suggested that depressive symptoms, coffee drinking, and NNS use were correlated among populations in Atlantic Canada. Participants who reported heavy coffee drinking and NNS use had increased likelihoods for major depression compared with those who never drank coffee or consumed NNS. Meanwhile, these participants also had more risk factors associated with depression development. These findings may suggest that further research is needed to elucidate how coffee and NNS influence depression development among populations in Atlantic Canada and the underlying biological mechanisms.
Methods
Study population
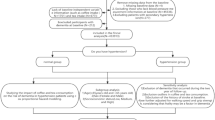
The Atlantic PATH is part of the Canadian Partnership for Tomorrow Project (CPTP), a pan-Canadian longitudinal cohort study examining the role of genetic, environmental, behavioral and lifestyle factors in the development of cancer and chronic disease36. The Atlantic PATH study is a population-based cohort in which study participants were residents of one of the four Atlantic Canada Provinces (Nova Scotia, New Brunswick, Newfoundland and Labrador, and Prince Edward Island) and aged between 35 and 69 years. Study participants were recruited from the general public through a combination of community outreach and awareness activities, advertising and media campaigns, and invitation. The 18838 Atlantic PATH study participants (5854 men and 12984 women) included in this analysis were recruited from the four Atlantic Canada provinces between 2009 and 2013. The study was approved by appropriate Research Ethics Boards (REB) in each Province, including Nova Scotia Health Authority REB, Vitalite Health Network REB, Horizon Health Network REB, Newfoundland and Labrador Health Research REB, University of Prince Edward Island REB, and Health PEI REB. All individuals provided written informed consent prior to participation. All data collection procedures followed the research protocol guidelines as approved by the Research Ethics Boards.
Data collection
Data collection has been reported previously37, 38. A set of standardized questionnaires on sociodemographic, health, diet, and behavioral factors and self-measured anthropometric indexes were completed by the participants, and physical measurements (including anthropometric indexes and body composition) were measured by research nurses at an assessment center.
Assessment of coffee drinking and use of non-nutritive sweeteners
Study participants answered questions on the number of standard sized cups of regular or decaffeinated coffee consumed per day. Eight ounces (250 milliliters) is the standard coffee cup size in Canada2. We grouped coffee drinking as: never, >0–< 4 cups/day, and ≥4 cups/day, and decaffeinated coffee drinking as: never, >0–< 2 cup/day, and ≥2 cups/day. Total coffee drinking was grouped as: never, >0–< 4 cups/day, and ≥4 cups/day.
NNS use was assessed based on participants’ responses to questions on the frequencies of adding NNS to coffee or tea and the consumption of diet drinks. NNS use was classified as never, sometimes, and always. Diet drinks are sugar-free and artificially sweetened beverages without calories2. Frequencies of diet drink consumption were classified as never, <1 time/week, 1–6 times/week, and ≥1 times/day. To count for both NNS use and diet drink consumption, we classified participants as never users for those who never used NNS or drank diet drinks, either users for those who reported either use of NNS or consumption of diet drinks, and both users for those who had positive responses to questions on both use of NNS and consumption of diet or drinks.
Assessment of depressive symptoms and antidepressant use
We used the Patient Health Questionnaire (PHQ-9) to calculate a depression severity score for study participants35. The questionnaire includes nine items. Based on participants’ responses to the nine questions, a total score ranging from 0 (minimum) to 27 (maximum) was summarized for each individual. Self-reported current medication use was collected; all medications were coded according to the Nova Scotia Formulary (NSF) (www.nspharmacare.ca)39. The ATC Code N06A (antidepressants) was used to define antidepressant use. Major depression was defined as a PHQ-9 score ≥10 and/or current use of antidepressants35, 37.
Assessment of covariables
Body weight was measured using the Tanita bioelectrical impedance device (Tanita BC-418, Tanita Corporation of America Inc., Arlington Heights, Illinois)37. Height was measured with a Seca stadiometer. Among the 18838 study participants, 13581 participants undertook body weight measurements, and 13635 participants undertook body height measurements, respectively. There were 10048 participants reported self-measured body weight and 10057 participants reported self-measured body height, respectively. Totally, 13579 participants had both measured weight and height and 5259 participants had self-reported anthropometric measures. For self-reported body weight, height, and body mass index (BMI), we made sex-specific corrections derived from the measured data40. BMI was calculated as weight in kilograms divided by height in meters squared.
Dietary intake for each study participant was derived from a semi-quantitative food frequency questionnaire37, 38. A healthy eating index (HEI)37 was developed according to the methods recommended for Americans and Canadians regarding food quality and prevention of chronic disease. The HEI is a continuous variable with a perfect score of 60 and a minimum score of 0. The higher the score, the healthier the diet. HEI scores were categorized as sex-specific tertiles in the multivariable regression analyses37.
We assessed physical activity using the International Physical Activity Questionnaire (IPAQ), long form version41. Metabolic equivalent (MET) minutes per week were calculated according to the IPAQ scoring protocol42. Levels of total physical activity were categorized as low, medium, and high by the sex-specific total metabolic expenditure (MET-min/week) tertiles.
Ethnicity was grouped as white and non-white. Educational attainment was categorized as high school or lower, college level, and university level or higher. For smoking behavior, participants were grouped as never smoker, former smoker, and current smoker. For alcohol drinking, respondents were classified as abstainer, occasional drinker, regular drinker, and habitual drinker37. Self-reported chronic disease was dichotomized as yes or no for cardiovascular disease (coronary heart disease or stroke) and diabetes mellitus.
Statistical analyses
Differences in study participant characteristics between men and women and across total coffee consumption and NNS use were tested with the Student-t test for continuous variables, except for physical activity which was examined with the Wilcoxon rank sum test, and the chi-square test for categorical variables. We computed Spearman partial correlation coefficients between depressive symptom score, coffee drinking, and NNS use with adjustment for age and sex.
Multivariable logistic regression was used to evaluate the associations of coffee drinking and NNS use with major depression. In the multivariable regression analyses, we controlled for sociodemographic and behavioral factors, chronic disease, and BMI. We computed P values for trend by treating variables of coffee drinking and NNS use as the continuous variable and P values for interaction between men and women by including the interaction terms of sex and coffee drinking or NNS use in the models. Moreover, we explored the possible interactions between total coffee consumption and NNS use in relation to risk of major depression with adjustment for all of the covariables. In addition, we did a stratified analysis among those with non-missing values in both smoking and BMI (n = 17894), as we previously found that smoking and obesity were associated with major depression37. In the stratified analysis, participants were classified as never smoker or ever smoker and normal weight or overweight or obesity (BMI ≥ 25 kg/m2). ORs and 95% CIs were computed for major depression according to coffee drinking and NNS use in each stratum with appropriate adjustment for the covariables. Statistical significance was defined as P < 0.05 (two-sided). Data management and analyses were performed with SAS for Windows, version 9.4 (SAS Institute, Cary, North Carolina).
Data availability statement
No datasets were generated during the current study. Data from the Atlantic PATH study is not publically available to researchers without an approved data access request to Atlantic PATH, as per the Atlantic PATH consent form and study protocol. While the authors cannot provide data to a third party directly, the dataset can be provided by Atlantic PATH following a data access request approval. Interested researchers should contact Atlantic PATH (http://atlanticpath.ca/).
Disclosure statement
This study was partly presented at the 2013 Canadian Society for Epidemiology and Biostatistics Biennial Conference, St. John’s, Newfoundland, June 24–27, 2013.
References
Salomon, J. A. et al. Common values in assessing health outcomes from disease and injury: disability weights measurement study for the Global Burden of Disease Study 2010. Lancet 380, 2129–2143 (2012).
Garriguet, D. Beverage consumption of Canadian adults. Health Rep. 19, 23–29 (2008).
Gougeon, R., Spidel, M., Lee, K. & Field, C. J. Canadian Diabetes Association National Nutrition Committee Technical Review: non-nutritive intense sweeteners in diabetes management. Can. J. Diabetes 28, 385–399 (2004).
Bhatti, S. K., O’Keefe, J. H. & Lavie, C. J. Coffee and tea: perks for health and longevity? Curr. Opin. Clin. Nutr. Metab. Care 16, 688–697 (2013).
Liu, J. et al. Association of coffee consumption with all-cause and cardiovascular disease mortality. Mayo Clin. Proc. 88, 1066–1074 (2013).
Freedman, N. D., Park, Y., Abnet, C. C., Hollenbeck, A. R. & Sinha, R. Association of coffee drinking with total and cause-specific mortality. N. Engl. J. Med. 366, 1891–1904 (2012).
Malerba, S. et al. A meta-analysis of prospective studies of coffee consumption and mortality for all causes, cancers and cardiovascular diseases. Eur. J. Epidemiol. 28, 527–539 (2013).
Crippa, A., Discacciati, A., Larsson, S. C., Wolk, A. & Orsini, N. Coffee consumption and mortality from all causes, cardiovascular disease, and cancer: a dose-response meta-analysis. Am. J. Epidemiol. 180, 763–775 (2014).
Ding, M., Bhupathiraju, S. N., Satija, A., van Dam, R. M. & Hu, F. B. Long-term coffee consumption and risk of cardiovascular disease: a systematic review and a dose-response meta-analysis of prospective cohort studies. Circulation 129, 643–659 (2014).
Nordestgaard, A. T. & Nordestgaard, B. G. Coffee intake, cardiovascular disease and all-cause mortality: observational and Mendelian randomization analyses in 95 000-223 000 individuals. Int. J. Epidemiol. doi:10.1093/ije/dyw325 (2016).
Rihs, M., Müller, C. & Baumann, P. Caffeine consumption in hospitalized psychiatric patients. Eur. Arch. Psychiatry Clin. Nuerosci. 246, 83–92 (1996).
Leibenluft, E. et al. Depressive symptoms and the self-reported use of alcohol, caffeine, and carbohydrates in normal volunteers and four groups of psychiatric outpatients. Am. J. Psychiatry 150, 294–301 (1993).
Ruusunen, A. et al. Coffee, tea and caffeine intake and the risk of severe depression in middle-aged Finnish men: the Kuopio Ischaemic Heart Disease Risk Factor Study. Public Health Nutr. 13, 1215–1220 (2010).
Lucas, M. et al. Coffee, caffeine, and risk of depression among women. Arch. Intern. Med. 171, 1571–1578 (2011).
Wang, L., Shen, X., Wu, Y. & Zhang, D. Coffee and caffeine consumption and depression: a meta-analysis of observational studies. Aust. N. Z. J. Psychiatry doi:10.1177/0004867415603131 (2015).
Grosso, G., Micek, A., Pajak, A., Castellano, S. & Galvano, F. Coffee, tea, caffeine and risk of depression: a systematic review and dose-response meta-analysis of observational studies. Mol. Nutr. Food Res. doi:10.1002/mnfr.201500620 (2015).
Guo, X. et al. Sweetened beverages, coffee, and tea and depression risk among older US adults. PLoS ONE 9, e94715 (2014).
Borges, M. C. et al. Artificially sweetened beverages and the response to the global obesity crisis. PLOS Medicine 14, e1002195 (2017).
Imamura, F. et al. Consumption of sugar sweetened beverages, artificially sweetened beverages, and fruit juice and incidence of type 2 diabetes: systematic review, meta-analysis, and estimation of population attributable fraction. BMJ 351, h3576 (2015).
Loftfield, E. et al. Association of coffee consumption with overall and cause-specific mortality in a large US prospective cohort study. Am. J. Epidemiol. 182, 1010–1022 (2015).
Tanskanen, A. et al. Heavy coffee drinking and the risk of suicide. Eur. J. Epidemiol. 16, 789–791 (2000).
Lucas, M. et al. Coffee, caffeine, and risk of depression among women. Arch. Intern. Med. 171, 1571–1578 (2011).
Kawachi I, W. W. A prospective study of coffee drinking and suicide in women. Arch. Intern. Med. 156, 521–525 (1996).
Fredholm, B. B., Bättig, K., Holmén, J., Nehlig, A. & Zvartau, E. E. Actions of caffeine in the brain with special reference to factors that contribute to its widespread use. Pharmacol. Rev. 51, 83–133 (1999).
Qi, H. & Li, S. Dose-response meta-analysis on coffee, tea and caffeine consumption with risk of Parkinson’s disease. Geriatr. Gerontol. Int. 14, 430–439 (2014).
Kim, Y.-S., Kwak, S. M. & Myung, S.-K. Caffeine intake from coffee or tea and cognitive disorders: a meta-analysis of observational studies. Neuroepidemiology 44, 51–63 (2015).
Liu, Q.-P. et al. Habitual coffee consumption and risk of cognitive decline/dementia: A systematic review and meta-analysis of prospective cohort studies. Nutrition 32, 628–636 (2016).
Smith, G. D. & Ebrahim, S. ‘Mendelian randomization’: can genetic epidemiology contribute to understanding environmental determinants of disease? Int. J. Epidemiol. 32, 1–22 (2003).
Roy, T. & Lloyd, C. E. Epidemiology of depression and diabetes: a systematic review. J. Affect. Disord. 142(Suppl), S8–21 (2012).
Sylvetsky, A. C., Welsh, J. A., Brown, R. J. & Vos, M. B. Low-calorie sweetener consumption is increasing in the United States. Am J Clin Nutr 96, 640–646 (2012).
Luppino, F. S. et al. Overweight, obesity, and depression: a systematic review and meta-analysis of longitudinal studies. Arch. Gen. Psychiatry 67, 220–229 (2010).
Mattes, R. D. & Popkin, B. M. Nonnutritive sweetener consumption in humans: effects on appetite and food intake and their putative mechanisms. Am. J. Clin. Nutr. 89, 1–14 (2009).
Azad, M. B. et al. Association between artificially sweetened beverage consumption during pregnancy and infant body mass index. JAMA Pediatr. 170, 662–670 (2016).
Moussavi, S. et al. Depression, chronic diseases, and decrements in health: results from the World Health Surveys. Lancet 370, 851–858 (2007).
Kroenke, K., Spitzer, R. L. & Williams, J. B. The PHQ-9: validity of a brief depression severity measure. J. Gen. Intern. Med. 16, 606–613 (2001).
Borugian, M. J. et al. The Canadian Partnership for Tomorrow Project: building a pan-Canadian research platform for disease prevention. CMAJ 182, 1197–1201 (2010).
Yu, Z. M., Parker, L. & Dummer, T. J. B. Depressive symptoms, diet quality, physical activity, and body composition among populations in Nova Scotia, Canada: report from the Atlantic Partnership for Tomorrow’s Health. Prev. Med. 61, 106–113 (2014).
Yu, Z. M., Fung, B., Murimboh, J. D., Parker, L. & Dummer, T. J. B. What is the role of obesity in the aetiology of arsenic-related disease? Environ. Int. 66, 115–123 (2014).
Pahor, M. et al. Drug data coding and analysis in epidemiologic studies. Eur. J. Epidemiol. 10, 405–411 (1994).
Shields, M., Connor Gorber, S., Janssen, I. & Tremblay, M. S. Bias in self-reported estimates of obesity in Canadian health surveys: an update on correction equations for adults. Health Rep. 22, 35–45 (2011).
Craig, C. L. et al. International physical activity questionnaire: 12-country reliability and validity. Med. Sci. Sports Exerc. 35, 1381–1395 (2003).
IPAQ scoring protocol - International Physical Activity Questionnaire. Available at: https://sites.google.com/site/theipaq/scoring-protocol. (Accessed: 28th October 2016).
Acknowledgements
We acknowledge the support of all participants in the Atlantic PATH Project. We thank the Atlantic PATH team members for data collection and management. Production of this study has been made possible through the financial support from the Canadian Partnership Against Cancer and Health Canada. The study funders had no involvement in the study design; in the collection, analysis and interpretation of data; in the writing of the report; and in the decision to submit the article for publication. The views expressed herein represent the views of the authors and do not necessarily represent the views of the funders.
Author information
Authors and Affiliations
Contributions
Study conception and design: L.P. and T.D. Acquisition, analysis, and interpretation of data and drafting of manuscript: Z.Y. Critical revision of the article: L.P. and T.D. All authors have full access to all the data in the study, take responsibility for the integrity of the data and the accuracy of the data analysis, and give final approval of the version to be submitted.
Corresponding author
Ethics declarations
Competing Interests
The authors declare that they have no competing interests.
Additional information
Publisher's note: Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made. The images or other third party material in this article are included in the article’s Creative Commons license, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons license and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this license, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Yu, Z.M., Parker, L. & Dummer, T.J.B. Associations of Coffee, Diet Drinks, and Non-Nutritive Sweetener Use with Depression among Populations in Eastern Canada. Sci Rep 7, 6255 (2017). https://doi.org/10.1038/s41598-017-06529-w
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41598-017-06529-w
This article is cited by
-
Young women’s food consumption and mental health: the role of employment
BMC Women's Health (2022)
-
Dietary phytochemical index in relation to risk of glioma: a case-control study in Iranian adults
Nutrition Journal (2021)
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.