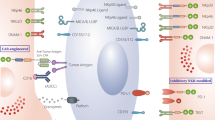
Abstract
Chimeric antigen receptor (CAR)-T cells represent a major breakthrough in cancer therapy, wherein a patient’s own T cells are engineered to recognize a tumor antigen, resulting in activation of a local cytotoxic immune response. However, CAR-T cell therapies are currently limited to the treatment of B cell cancers and their effectiveness is hindered by resistance from antigen-negative tumor cells, immunosuppression in the tumor microenvironment, eventual exhaustion of T cell immunologic functions and frequent severe toxicities. To overcome these problems, we have developed a novel class of CAR-T cells engineered to express an enzyme that activates a systemically administered small-molecule prodrug in situ at a tumor site. We show that these synthetic enzyme-armed killer (SEAKER) cells exhibit enhanced anticancer activity with small-molecule prodrugs, both in vitro and in vivo in mouse tumor models. This modular platform enables combined targeting of cellular and small-molecule therapies to treat cancers and potentially a variety of other diseases.

This is a preview of subscription content, access via your institution
Access options
Access Nature and 54 other Nature Portfolio journals
Get Nature+, our best-value online-access subscription
$29.99 / 30 days
cancel any time
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout






Similar content being viewed by others
Data availability
The authors declare that the data supporting the findings of this study are available within the article and its Supplementary Information files. Any raw data not provided therein are available from the corresponding authors upon reasonable request.
References
Feldman, S. A., Assadipour, Y., Kriley, I., Goff, S. L. & Rosenberg, S. A. Adoptive cell therapy—tumor-infiltrating lymphocytes, T-cell receptors, and chimeric antigen receptors. Semin. Oncol. 42, 626–639 (2015).
Leon, E., Ranganathan, R. & Savoldo, B. Adoptive T cell therapy: boosting the immune system to fight cancer. Semin. Immunol. 49, 101437 (2020).
Sadelain, M., Rivière, I. & Riddell, S. Therapeutic T cell engineering. Nature 545, 423–431 (2017).
Beyar-Katz, O. & Gill, S. Advances in chimeric antigen receptor T cells. Curr. Opin. Hematol. 27, 368–377 (2020).
June, C. H., O’Connor, R. S., Kawalekar, O. U., Ghassemi, S. & Milone, M. C. CAR T cell immunotherapy for human cancer. Science 359, 1361–1365 (2018).
Sermer, D. & Brentjens, R. CAR T-cell therapy: full speed ahead. Hematol. Oncol. 37, 95–100 (2019).
Sotillo, E. et al. Convergence of acquired mutations and alternative splicing of CD19 enables resistance to CART-19 immunotherapy. Cancer Discov. 5, 1282–1295 (2015).
Maude, S. L. et al. Chimeric antigen receptor T cells for sustained remissions in leukemia. N. Engl. J. Med. 371, 1507–1517 (2014).
Majzner, R. G. & Mackall, C. L. Tumor antigen escape from CAR T-cell therapy. Cancer Discov. 8, 1219–1226 (2018).
Anderson, K. G., Stromnes, I. M. & Greenberg, P. D. Obstacles posed by the tumor microenvironment to T cell activity: a case for synergistic therapies. Cancer Cell 31, 311–325 (2017).
Kasakovski, D., Xu, L. & Li, Y. T cell senescence and CAR-T cell exhaustion in hematological malignancies. J. Hematol. Oncol. 11, 91 (2018).
Neelapu, S. S. et al. Chimeric antigen receptor T-cell therapy: assessment and management of toxicities. Nat. Rev. Clin. Oncol. 15, 47–62 (2018).
Dunbar, C. E. et al. Gene therapy comes of age. Science 359, eaan4672 (2018).
Lim, W. A. & June, C. H. The principles of engineering immune cells to treat cancer. Cell 168, 724–740 (2017).
Rafiq, S. et al. Targeted delivery of a PD-1-blocking scFv by CAR-T cells enhances anti-tumor efficacy in vivo. Nat. Biotechnol. 36, 847–856 (2018).
Yeku, O. O., Purdon, T. J., Koneru, M., Spriggs, D. & Brentjens, R. J. Armored CAR T cells enhance antitumor efficacy and overcome the tumor microenvironment. Sci. Rep. 7, 10541 (2017).
Avanzi, M. P. et al. Engineered tumor-targeted T cells mediate enhanced anti-tumor efficacy both directly and through activation of the endogenous immune system. Cell Rep. 23, 2130–2141 (2018).
Boice, M. et al. Loss of the HVEM tumor suppressor in lymphoma and restoration by modified CAR-T cells. Cell 167, 405–418 (2016).
Kuhn, N. F. et al. CD40 ligand-modified chimeric antigen receptor T cells enhance antitumor function by eliciting an endogenous antitumor response. Cancer Cell 35, 473–488 (2019).
Brudno, J. N. & Kochenderfer, J. N. Recent advances in CAR T-cell toxicity: mechanisms, manifestations and management. Blood Rev. 34, 45–55 (2019).
Lambert, J. M. & Berkenblit, A. Antibody-drug conjugates for cancer treatment. Annu. Rev. Med. 69, 191–207 (2018).
Sharma, S. K. & Bagshawe, K. D. Translating antibody directed enzyme prodrug therapy (ADEPT) and prospects for combination. Expert Opin. Biol. Ther. 17, 1–13 (2017).
Nemunaitis, J. et al. Pilot trial of genetically modified, attenuated Salmonella expressing the E. coli cytosine deaminase gene in refractory cancer patients. Cancer Gene Ther. 10, 737–744 (2003).
Sherwood, R. F., Melton, R. G., Alwan, S. M. & Hughes, P. Purification and properties of carboxypeptidase G2 from Pseudomonas sp. strain RS-16. Use of a novel triazine dye affinity method. Eur. J. Biochem. 148, 447–453 (1985).
Fleming, P. C., Goldner, M. & Glass, D. G. Observations on the nature, distribution, and significance of cephalosporinase. Lancet 1, 1399–1401 (1963).
Jaffe, J. J., McCormack, J. J. & Meymerian, E. Trypanocidal properties of 5′-O-sulfamoyladenosine, a close structural analog of nucleocidin. Exp. Parasitol. 28, 535–543 (1970).
Rengaraju, S. et al. 5′-O-Sulfamoyladenosine (defluoronucleocidin) from a Streptomyces. Meiji Seika Kenkyu Nenpo 25, 49–55 (1986).
Francis, R. J. et al. A Phase I trial of antibody directed enzyme prodrug therapy (ADEPT) in patients with advanced colorectal carcinoma or other CEA producing tumours. Br. J. Cancer 87, 600–607 (2002).
Springer, C. J. et al. Optimization of alkylating agent prodrugs derived from phenol and aniline mustards: a new clinical candidate prodrug (ZD2767) for antibody-directed enzyme prodrug therapy (ADEPT). J. Med. Chem. 38, 5051–5065 (1995).
Yoo, B. et al. Ultrasmall dual-modality silica nanoparticle drug conjugates: design, synthesis, and characterization. Bioorg. Med. Chem. 23, 7119–7130 (2015).
Harding, F. A. et al. A beta-lactamase with reduced immunogenicity for the targeted delivery of chemotherapeutics using antibody-directed enzyme prodrug therapy. Mol. Cancer Ther. 4, 1791–1800 (2005).
Marais, R. et al. A cell surface tethered enzyme improves efficiency in gene-directed enzyme prodrug therapy. Nat. Biotechnol. 15, 1373–1377 (1997).
Brentjens, R. J. et al. Genetically targeted T cells eradicate systemic acute lymphoblastic leukemia xenografts. Clin. Cancer Res. 13, 5426–5435 (2007).
Liu, Z. et al. Systematic comparison of 2A peptides for cloning multi-genes in a polycistronic vector. Sci. Rep. 7, 2193 (2017).
Levy, C. C. & Goldman, P. The enzymatic hydrolysis of methotrexate and folic acid. J. Biol. Chem. 242, 2933–2938 (1967).
Bulychev, A. & Mobashery, S. Class C beta-lactamases operate at the diffusion limit for turnover of their preferred cephalosporin substrates. Antimicrob. Agents Chemother. 43, 1743–1746 (1999).
Santos, E. B. et al. Sensitive in vivo imaging of T cells using a membrane-bound Gaussia princeps luciferase. Nat. Med. 15, 338–344 (2009).
Gurung, N., Ray, S., Bose, S. & Rai, V. A broader view: microbial enzymes and their relevance in industries, medicine, and beyond. BioMed. Res. Int. 2013, 329121 (2013).
Mayer, A. et al. Modifying an immunogenic epitope on a therapeutic protein: a step towards an improved system for antibody-directed enzyme prodrug therapy (ADEPT). Br. J. Cancer 90, 2402–2410 (2004).
Liu, S. et al. Corticosteroids do not influence the efficacy and kinetics of CAR-T cells for B-cell acute lymphoblastic leukemia. Blood Cancer J. 10, 15 (2020).
Bagshawe, K. D. & Sharma, S. K. Cyclosporine delays host immune response to antibody enzyme conjugate in ADEPT. in Proc. International Conference on New Trends in Clinical and Experimental Immunosuppression, Geneva (1996).
Smith, G. K. et al. Toward antibody-directed enzyme prodrug therapy with the T268G mutant of human carboxypeptidase A1 and novel in vivo stable prodrugs of methotrexate. J. Biol. Chem. 272, 15804–15816 (1997).
Oosterhoff, D. et al. Secreted and tumour targeted human carboxylesterase for activation of irinotecan. Br. J. Cancer 87, 659–664 (2002).
Chen, K. C. et al. Membrane-localized activation of glucuronide prodrugs by beta-glucuronidase enzymes. Cancer Gene Ther. 14, 187–200 (2007).
Peraro, L. et al. Incorporation of bacterial immunoevasins to protect cell therapies from host antibody-mediated immune rejection Mol. Ther. https://doi.org/10.1016/j.ymthe.2021.06.022 (2021).
Porter, D. L., Levine, B. L., Kalos, M., Bagg, A. & June, C. H. Chimeric antigen receptor-modified T cells in chronic lymphoid leukemia. N. Engl. J. Med. 365, 725–733 (2011).
Gardner, T. J. et al. Targeted cellular micropharmacies: cells engineered for localized drug delivery. Cancers 12, 2175 (2020).
Quintarelli, C. et al. Co-expression of cytokine and suicide genes to enhance the activity and safety of tumor-specific cytotoxic T lymphocytes. Blood 110, 2793–2802 (2007).
Garber, K. Driving T-cell immunotherapy to solid tumors. Nat. Biotechnol. 36, 215–219 (2018).
Riviere, I., Brose, K. & Mulligan, R. C. Effects of retroviral vector design on expression of human adenosine deaminase in murine bone marrow transplant recipients engrafted with genetically modified cells. Proc. Natl Acad. Sci. USA 92, 6733–6737 (1995).
Sanjana, N. E., Shalem, O. & Zhang, F. Improved vectors and genome-wide libraries for CRISPR screening. Nat. Methods 11, 783–784 (2014).
Acknowledgements
We thank E. de Stanchina and C. Hagen (MSK Antitumor Assessment Core Facility) for assistance with mouse toxicology studies, G. Sukenick and R. Wang (MSK Analytical NMR Core Facility) for expert nuclear magnetic resonance and mass spectral support, J. Fraser Glickman and C. Adura Alcaino (Rockefeller High-Throughput and Spectroscopy Resource Center) for assistance with SPE–MS experiments, G. Chiosis and S. Sharma (MSK) for assistance with LC–MS/MS experiments and B. Yoo (MSK) for helpful discussions on the synthesis of APdMG-Glu. Financial support from the NIH (grant nos. P01 CA023766 to D.A.S. and D.S.T., R01 CA55349 and R35 CA241894 to D.A.S., R01 AI118224 to D.S.T. and CCSG P30 CA008748 to C.B. Thompson), the Tudor Fund (to D.A.S.), the Lymphoma Fund (to D.A.S.), the Commonwealth Foundation and MSK Center for Experimental Therapeutics (to D.A.S. and D.S.T.) is gratefully acknowledged.
Author information
Authors and Affiliations
Contributions
T.J.G., C.M.B. and D.A.S. conceived the in vitro and in vivo experiments with technical advice from D.W. and R.J.B. T.J.G. and C.M.B. executed the in vitro and in vivo experiments with assistance from K.G.K., M.M.D., A.Y.C. and G.M. J.P.L., N.K., B.C.C. and D.S.T. conceived the chemical, biochemical and ADME-PK experiments. J.P.L., B.C.C. and K.M.N. carried out the chemical syntheses. J.P.L., N.K. and B.C.C. carried out the biochemical assays. T.J.G., J.P.L., C.M.B., D.S.T. and D.A.S. wrote the paper with input from all coauthors.
Corresponding authors
Ethics declarations
Competing interests
D.A.S., D.S.T. and R.J.B. are consultants for, have equity in and have sponsored research agreements with CoImmune, which has licensed technology described in this paper from MSK. D.A.S. has equity in or is a consultant for: Actinium Pharmaceuticals, Arvinas, Eureka Therapeutics, Iovance Biotherapeutics, OncoPep, Pfizer, Repretoire and Sellas. D.S.T. has been a consultant and/or paid speaker for Eli Lilly, Elsevier, Emerson Collective, Merck, National Institutes of Health, Venenum Biodesign, the Research Center for Molecular Medicine of the Austrian Academy of Sciences and the Institute for Research in Biomedicine, Barcelona. R.J.B. is a cofounder and receives royalties from Juno Therapeutics/Celgene. MSK has filed for patent protection behalf of T.J.G., J.P.L., D.S.T. and D.A.S. for inventions described in this paper. The remaining authors declare no competing interests.
Additional information
Peer review information Nature Chemical Biology thanks Yuan Gao and the other, anonymous, reviewer(s) for their contribution to the peer review of this work.
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Extended data
Extended Data Fig. 1 Synthesis of AMS-Glu prodrug (2).
DMA = N,N-dimethylacetamide; DMF = N,N-dimethylformamide; TBAF = tetrabutylammonium fluoride; TBS = t-butyldimethylsilyl.
Extended Data Fig. 2 Synthesis of Ceph-AMS prodrug (3).
(a) Synthesis of protected AMS precursor 16. (b) Synthesis of Ceph-AMS (3). pyr = pyridine; TFA = trifluoroacetic acid; THF = tetrahydrofuran; TMS = trimethylsilyl.
Extended Data Fig. 3 Complete bioluminescent imaging data for in vivo efficacy in mouse intraperitoneal Raji tumor xenografts.
Mice treated with (a) CPG2-19BBz SEAKER cells and AMS-Glu (2) (50 mg/kg, ip, bid, days 2-7 post-CAR engraftment, 12 doses total, gray band) or (b) β-Lac-19BBz SEAKER cells and Ceph-AMS (3) (4 mg/kg, ip, bid, days 2–3 post-CAR engraftment, 3 doses total, gray band). Raw BLI is plotted on log scale; AUC is plotted on split linear scale. (mean ± s.d. of n = 5 mice per group; experiment was repeated with similar results.) Representative images are shown in Fig. 5d and e, respectively, of the manuscript.
Extended Data Fig. 4 Complete bioluminescent imaging data for in vivo efficacy against antigen-negative cells in intraperitoneal heterogeneous tumor xenografts.
(a) Bioluminescent imaging (BLI) and quantification of CD19+ Nalm6 cells expressing mCherry and Gaussia luciferase (Nalm6-mCherry/gLuc [CD19+]) in untreated mice or mice receiving β-Lac-19BBz SEAKER cells plus or minus 3 injections of Ceph-AMS (3: 4 mg/kg, ip, bid). Images taken at day 20 post tumor engraftment; one mouse in the group treated with SEAKER cells and prodrug showed tumor clearance but died after day 14 and is omitted. Complete radiance data is shown in the right two panels, with raw BLI plotted on log scale and AUC plotted on a linear scale. (Mean ± s.d. of n = 4 (untreated, SEAKER + prodrug) or n = 5 (SEAKER alone) mice per group; Student’s two-tailed t-test: ns = not significant; *p < 0.05; experiment was performed once). (b) BLI and quantification of CD19− Nalm6 cells expressing eGFP and firefly luciferase (Nalm6-eGFP/fLuc [CD19−]) in untreated mice or mice receiving β-Lac-19BBz SEAKER cells plus or minus 3 injections of Ceph-AMS (3: 4 mg/kg, ip, bid). Images taken at day 17 post tumor engraftment; one mouse in the group treated with SEAKER cells and prodrug died after day 14 and is omitted. The left two panels also appear in Fig. 5g,h of the manuscript. Complete radiance data is shown in the right two panels, with raw BLI plotted on log scale and AUC plotted on a linear scale. (Mean ± s.d. of n = 4 (untreated, SEAKER + prodrug) or n = 5 (SEAKER alone) mice per group; Student’s two-tailed t-test: ns = not significant; *p < 0.05; experiment was performed once).
Extended Data Fig. 5 Persistence of β-Lac enzyme activity and Ceph-AMS prodrug activation in mouse intraperitoneal Raji tumor xenografts after SEAKER cell exhaustion in vivo.
(a) Experimental scheme for rescue of relapsed Raji xenograft by treatment with Ceph-AMS (3: 4 mg/kg, ip, bid, days 4–5, 3 doses total, then days 22–23 (gray bar), 3 doses total) after exhaustion of β-Lac-19BBz SEAKER cells. (b) Quantitation of tumor bioluminescence before and after second dosing period (median with s.d. of n = 4 mice per group; experiment was performed once). (c) Persistence of β-Lac enzyme activity in β-Lac-19BBz SEAKER cells extracted from two of the mice from the experiment in panel a at day 30 (day 28 post administration), in comparison to standard 19BBz CAR-T cell controls (flow cytometry analysis: β-Lac substrate = CCF2-AM).
Extended Data Fig. 6 Construction and characterization of β-Lac-expressing murine SEAKER cells.
(a) SEAKER construct encoding secreted β-Lac and a murine CAR: β-Lac-MUC28z (β-Lac/α-MUC16/CD28/CD3ζ). LTR = long terminal, Ψ = psi packaging element, FLAG = FLAG epitope tag (pink), P2A = 2A self cleaving peptide, α-MUC16 scFv = MUC-16-specific mouse-derived single chain variable fragment, myc = Myc epitope tag (brown), mCD28 = mouse CD28 costimulatory domain (green), mCD3ζ = mouse CD3 zeta chain (red). (b) Flow cytometry analysis of α-MUC16 CAR expression in retrovirally-transduced primary mouse T cells (fluorescently (phycoerythrin, PE) labeled anti-idiotype antibody; representative data from 5 independent experiments). (c) Trans-cytotoxicity of supernatant fluid (sn) from β-Lac-MUC28z SEAKER cells with or without Ceph-AMS (3: 107 nM) against mouse EL4 lymphoma cells, compared to prodrug alone and parent drug AMS (1: 500 nM) (24 h, CellTiter-Glo assay; mean ± s.d. of n = 3 technical replicates; Student’s two-tailed t-test: ns = not significant, ***p < 0.001; experiment was perfomed once).
Extended Data Fig. 7 Assessment of SEAKER cell immunogenicity in an immunocompetent mouse model.
Assessment of SEAKER cell immunogenicity in an immunocompetent mouse model. (a) Experimental scheme to assess immunogenicity of β-Lac-MUC28z SEAKER cells in a syngeneic intraperitoneal ID8 tumor model. Sera were collected on Days 21, 24, 28, and 31 and tested for anti-β-Lac antibodies in panel b. In a separate experiment, ascites were recovered on Day 28 by peritoneal lavage and tested for the presence of SEAKER cells in panels c,d and β-Lac enzyme activity in panel e. (b) Detection anti-β-Lac antibodies in sera over 10 days following SEAKER cell engraftment (Days 21–31) (median with lines representing each individual mouse of n = 12; experiment was performed once). (c,d) Flow cytometry analysis of SEAKER cell (myc+) persistence among T cells (CD3+) and (e) nitrocefin cleavage-based quantitation of β-Lac enzyme activity in ascites recovered 7 days after SEAKER cell engraftment (Day 28) (representative data shown from n = 2 mice per group; on average, 25% of T cells were SEAKER-positive; experiment was performed once). SSC = side scatter. (f) In a third experiment, mice were treated as in panel a, but without cyclophosphamide pretreatment to maximize the antibody response, then sera were recovered 5 days after SEAKER cell engraftment (Day 26) and analyzed for anti-β-Lac antibodies (n = 1 mouse in untreated group; n = 5 mice in treated group; mean ± s.d. of n = 3 technical replicates from each mouse; experiment was performed once). Sera from the 4 mice showing anti-β-Lac antibodies were used for the ex vivo enzyme activity experiment in panel g. (g) Nitrocefin cleavage-based quantitation of enzyme activity of recombinant β-Lac treated with sera from untreated or SEAKER-treated mice from panel f (n = 2 mice in untreated group; mean ± s.d. of n = 4 mice in treated group; experiment was performed once).
Supplementary information
Supplementary Information
Supplementary Tables 1–3, Figs 1–15 and Note (chemistry).
Supplementary Data
Original western blots from Supplementary Figs. 5, 6 and 8; representative ancestry gate for flow cytometry analysis.
Rights and permissions
About this article
Cite this article
Gardner, T.J., Lee, J.P., Bourne, C.M. et al. Engineering CAR-T cells to activate small-molecule drugs in situ. Nat Chem Biol 18, 216–225 (2022). https://doi.org/10.1038/s41589-021-00932-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41589-021-00932-1
This article is cited by
-
Programmable synthetic receptors: the next-generation of cell and gene therapies
Signal Transduction and Targeted Therapy (2024)
-
CAR T cells as micropharmacies against solid cancers: Combining effector T-cell mediated cell death with vascular targeting in a one-step engineering process
Cancer Gene Therapy (2023)
-
Mechanisms of resistance to chimeric antigen receptor-T cells in haematological malignancies
Nature Reviews Drug Discovery (2023)
-
Empowering gene delivery with protein engineering platforms
Gene Therapy (2023)
-
CAR-T cells SEAK help from enzymes
Nature Chemical Biology (2022)