Abstract
Epigenetic regulation is critical to physiological control of development, cell fate, cell proliferation, genomic integrity and, fundamentally, transcriptional regulation. This epigenetic control occurs at multiple levels including through DNA methylation, histone modification, nucleosome remodelling and modulation of the 3D chromatin structure. Alterations in genes that encode chromatin regulators are common among mesenchymal neoplasms, a collection of more than 160 tumour types including over 60 malignant variants (sarcomas) that have unique and varied genetic, biological and clinical characteristics. Herein, we review those sarcomas in which chromatin pathway alterations drive disease biology. Specifically, we emphasize examples of dysregulation of each level of epigenetic control though mechanisms that include alterations in metabolic enzymes that regulate DNA methylation and histone post-translational modifications, mutations in histone genes, subunit loss or fusions in chromatin remodelling and modifying complexes, and disruption of higher-order chromatin structure. Epigenetic mechanisms of tumorigenesis have been implicated in mesenchymal tumours ranging from chondroblastoma and giant cell tumour of bone to chondrosarcoma, malignant peripheral nerve sheath tumour, synovial sarcoma, epithelioid sarcoma and Ewing sarcoma — all diseases that present in a younger patient population than most cancers. Finally, we review current and potential future approaches for the development of sarcoma therapies based on this emerging understanding of chromatin dysregulation.
This is a preview of subscription content, access via your institution
Access options
Access Nature and 54 other Nature Portfolio journals
Get Nature+, our best-value online-access subscription
$29.99 / 30 days
cancel any time
Subscribe to this journal
Receive 12 print issues and online access
$209.00 per year
only $17.42 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout




Similar content being viewed by others
References
Cancer Genome Atlas Research Network. Comprehensive and integrated genomic characterization of adult soft tissue sarcomas. Cell 171, 950–965.e28 (2017). This paper presents a comprehensive genomic analysis of six major sarcoma histotypes, including MPNST and synovial sarcoma.
Sheffield, N. C. et al. DNA methylation heterogeneity defines a disease spectrum in Ewing sarcoma. Nat. Med. 23, 386–395 (2017).
Cancer Genome Atlas Research Network et al. Genomic and epigenomic landscapes of adult de novo acute myeloid leukemia. N. Engl. J. Med. 368, 2059–2074 (2013).
Papaemmanuil, E. et al. Genomic classification and prognosis in acute myeloid leukemia. N. Engl. J. Med. 374, 2209–2221 (2016).
Lohr, J. G. et al. Discovery and prioritization of somatic mutations in diffuse large B-cell lymphoma (DLBCL) by whole-exome sequencing. Proc. Natl Acad. Sci. USA 109, 3879–3884 (2012).
Okosun, J. et al. Integrated genomic analysis identifies recurrent mutations and evolution patterns driving the initiation and progression of follicular lymphoma. Nat. Genet. 46, 176–181 (2014).
Siegel, R. L., Miller, K. D. & Jemal, A. Cancer statistics, 2018. CA Cancer J. Clin. 68, 7–30 (2018).
National Comprehensive Cancer Network. Soft Tissue Sarcoma. NCCN https://www.nccn.org/professionals/physician_gls/PDF/sarcoma.pdf (2020).
Schaefer, I.-M., Cote, G. M. & Hornick, J. L. Contemporary sarcoma diagnosis, genetics, and genomics. J. Clin. Oncol. 36, 101–110 (2018).
Jain, S., Xu, R., Prieto, V. G. & Lee, P. Molecular classification of soft tissue sarcomas and its clinical applications. Int. J. Clin. Exp. Pathol. 3, 416–428 (2010).
Barretina, J. et al. Subtype-specific genomic alterations define new targets for soft-tissue sarcoma therapy. Nat. Genet. 42, 715–721 (2010).
Vlenterie, M. et al. Next generation sequencing in synovial sarcoma reveals novel gene mutations. Oncotarget 6, 34680–34690 (2015).
Brohl, A. S. et al. The genomic landscape of the Ewing sarcoma family of tumors reveals recurrent STAG2 mutation. PLoS Genet. 10, e1004475 (2014).
Crompton, B. D. et al. The genomic landscape of pediatric Ewing sarcoma. Cancer Discov. 4, 1326–1341 (2014).
Tirode, F. et al. Genomic landscape of Ewing sarcoma defines an aggressive subtype with co-association of STAG2 and TP53 mutations. Cancer Discov. 4, 1342–1353 (2014).
Shern, J. F. et al. Comprehensive genomic analysis of rhabdomyosarcoma reveals a landscape of alterations affecting a common genetic axis in fusion-positive and fusion-negative tumors. Cancer Discov. 4, 216–231 (2014).
Chalmers, Z. R. et al. Analysis of 100,000 human cancer genomes reveals the landscape of tumor mutational burden. Genome Med. 9, 34 (2017).
Joseph, C. G. et al. Exomic analysis of myxoid liposarcomas, synovial sarcomas, and osteosarcomas. Genes Chromosomes Cancer 53, 15–24 (2014).
Amary, M. F. et al. IDH1 and IDH2 mutations are frequent events in central chondrosarcoma and central and periosteal chondromas but not in other mesenchymal tumours. J. Pathol. 224, 334–343 (2011). This paper presents the first description of IDH1 and IDH2 mutations in chondrosarcoma.
Venneker, S., Szuhai, K., Hogendoorn, P. C. W. & Bovée, J. V. M. G. Mutation-driven epigenetic alterations as a defining hallmark of central cartilaginous tumours, giant cell tumour of bone and chondroblastoma. Virchows Arch. Path Anat. 476, 135–146 (2020).
Koelsche, C. et al. Histone 3.3 hotspot mutations in conventional osteosarcomas: a comprehensive clinical and molecular characterization of six H3F3A mutated cases. Clin. Sarcoma Res. 7, 9–11 (2017).
Nacev, B. A. et al. The expanding landscape of ‘oncohistone’ mutations in human cancers. Nature 567, 473–478 (2019).
Ho, P. J., Lloyd, S. M. & Bao, X. Unwinding chromatin at the right places: how BAF is targeted to specific genomic locations during development. Development 146, dev178780 (2019).
Sawyer, I. A., Bartek, J. & Dundr, M. Phase separated microenvironments inside the cell nucleus are linked to disease and regulate epigenetic state, transcription and RNA processing. Semin. Cell Dev. Biol. 90, 94–103 (2019).
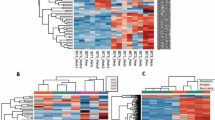
Wu, S. P. et al. DNA methylation-based classifier for accurate molecular diagnosis of bone sarcomas. JCO Precis. Oncol. 2017, 1–11 (2017).
Koelsche, C. et al. Array-based DNA-methylation profiling in sarcomas with small blue round cell histology provides valuable diagnostic information. Mod. Pathol. 31, 1246–1256 (2018).
Koelsche, C. et al. DNA methylation profiling distinguishes Ewing-like sarcoma with EWSR1–NFATc2 fusion from Ewing sarcoma. J. Cancer Res. Clin. Oncol. 145, 1273–1281 (2019).
Seki, M. et al. Integrated genetic and epigenetic analysis defines novel molecular subgroups in rhabdomyosarcoma. Nat. Commun. 6, 7557 (2015).
Röhrich, M. et al. Methylation-based classification of benign and malignant peripheral nerve sheath tumors. Acta Neuropathol. 131, 877–887 (2016).
Johann, P. D. et al. Atypical teratoid/rhabdoid tumors are comprised of three epigenetic subgroups with distinct enhancer landscapes. Cancer Cell 29, 379–393 (2016).
Srinivasan, U., Reaman, G. H., Poplack, D. G., Glaubiger, D. L. & LeVine, A. S. Phase II study of 5-azacytidine in sarcomas of bone. Am. J. Clin. Oncol. 5, 411–415 (1982).
Viré, E. et al. The Polycomb group protein EZH2 directly controls DNA methylation. Nature 439, 871–874 (2006).
Boulay, G. et al. Cancer-specific retargeting of BAF complexes by a prion-like domain. Cell 171, 163–178.e19 (2017).
Chong, S. et al. Imaging dynamic and selective low-complexity domain interactions that control gene transcription. Science 361, eaar2555 (2018).
Parsons, D. W. et al. An integrated genomic analysis of human glioblastoma multiforme. Science 321, 1807–1812 (2008).
Mardis, E. R. et al. Recurring mutations found by sequencing an acute myeloid leukemia genome. N. Engl. J. Med. 361, 1058–1066 (2009). This study identifies IDH1 mutations as a driver event in AML.
Lu, C. & Thompson, C. B. Metabolic regulation of epigenetics. Cell Metab. 16, 9–17 (2012).
Losman, J.-A. & Kaelin, W. G. What a difference a hydroxyl makes: mutant IDH, (R)-2-hydroxyglutarate, and cancer. Genes Dev. 27, 836–852 (2013).
Tarpey, P. S. et al. Frequent mutation of the major cartilage collagen gene COL2A1 in chondrosarcoma. Nat. Genet. 45, 923–926 (2013).
Pansuriya, T. C. et al. Somatic mosaic IDH1 and IDH2 mutations are associated with enchondroma and spindle cell hemangioma in Ollier disease and Maffucci syndrome. Nat. Genet. 43, 1256–1261 (2011).
Amary, M. F. et al. Ollier disease and Maffucci syndrome are caused by somatic mosaic mutations of IDH1 and IDH2. Nat. Genet. 43, 1262–1265 (2011).
Dang, L. et al. Cancer-associated IDH1 mutations produce 2-hydroxyglutarate. Nature 462, 739–744 (2009). This paper presents the first description of the neomorphic activity of IDH1 mutations to produce the oncometabolite 2HG, mechanistically explaining its association with epigenomic dysregulation.
Ward, P. S. et al. The common feature of leukemia-associated IDH1 and IDH2 mutations is a neomorphic enzyme activity converting α-ketoglutarate to 2-hydroxyglutarate. Cancer Cell 17, 225–234 (2010).
Turcan, S. et al. IDH1 mutation is sufficient to establish the glioma hypermethylator phenotype. Nature 483, 479–483 (2012).
Figueroa, M. E. et al. Leukemic IDH1 and IDH2 mutations result in a hypermethylation phenotype, disrupt TET2 function, and impair hematopoietic differentiation. Cancer Cell 18, 553–567 (2010). This paper shows that IDH1 and IDH2 mutations both alter DNA methylation and impair TET2 activity, leading to blocks in differentiation.
Lu, C. et al. IDH mutation impairs histone demethylation and results in a block to cell differentiation. Nature 483, 474–478 (2012).
Yen, K. et al. AG-221, a first-in-class therapy targeting acute myeloid leukemia harboring oncogenic IDH2 mutations. Cancer Discov. 7, 478–493 (2017).
Wang, F. et al. Targeted inhibition of mutant IDH2 in leukemia cells induces cellular differentiation. Science 340, 622–626 (2013).
Rohle, D. et al. An inhibitor of mutant IDH1 delays growth and promotes differentiation of glioma cells. Science 340, 626–630 (2013).
Kernytsky, A. et al. IDH2 mutation-induced histone and DNA hypermethylation is progressively reversed by small-molecule inhibition. Blood 125, 296–303 (2015).
DiNardo, C. D. et al. Durable remissions with ivosidenib in IDH1-mutated relapsed or refractory AML. N. Engl. J. Med. 378, 2386–2398 (2018). This clinical study translates epigenomic research into new treatments, demonstrating the efficacy of IDH1 inhibitors in IDH1-mutated AML.
Stein, E. M. et al. Enasidenib in mutant IDH2 relapsed or refractory acute myeloid leukemia. Blood 130, 722–731 (2017).
Suijker, J. et al. Inhibition of mutant IDH1 decreases d-2-HG levels without affecting tumorigenic properties of chondrosarcoma cell lines. Oncotarget 6, 12505–12519 (2015).
Jin, Y. et al. Mutant IDH1 dysregulates the differentiation of mesenchymal stem cells in association with gene-specific histone modifications to cartilage- and bone-related genes. PLoS ONE 10, e0131998 (2015).
Lu, C. et al. Induction of sarcomas by mutant IDH2. Genes Dev. 27, 1986–1998 (2013).
Hirata, M. et al. Mutant IDH is sufficient to initiate enchondromatosis in mice. Proc. Natl. Acad. Sci. USA 112, 2829–2834 (2015).
Sasaki, M. et al. d-2-Hydroxyglutarate produced by mutant IDH1 perturbs collagen maturation and basement membrane function. Genes Dev. 26, 2038–2049 (2012).
Koivunen, P. et al. Transformation by the (R)-enantiomer of 2-hydroxyglutarate linked to EGLN activation. Nature 483, 484–488 (2012).
Cleven, A. H. G. et al. IDH1 or -2 mutations do not predict outcome and do not cause loss of 5-hydroxymethylcytosine or altered histone modifications in central chondrosarcomas. Clin. Sarcoma Res. 7, 8–10 (2017).
Zhu, G. G. et al. Genomic profiling identifies association of IDH1/IDH2 mutation with longer relapse-free and metastasis-free survival in high-grade chondrosarcoma. Clin. Cancer Res. 26, 419–427 (2020).
Amary, M. F. et al. Isocitrate dehydrogenase 1 mutations (IDH1) and p16/CDKN2A copy number change in conventional chondrosarcomas. Virchows Arch. 466, 217–222 (2015).
Janeway, K. A. et al. Defects in succinate dehydrogenase in gastrointestinal stromal tumors lacking KIT and PDGFRA mutations. Proc. Natl Acad. Sci. USA 108, 314–318 (2011).
Pantaleo, M. A. et al. SDHA loss-of-function mutations in KIT–PDGFRA wild-type gastrointestinal stromal tumors identified by massively parallel sequencing. J. Natl. Cancer Inst. 103, 983–987 (2011).
Xiao, M. et al. Inhibition of α-KG-dependent histone and DNA demethylases by fumarate and succinate that are accumulated in mutations of FH and SDH tumor suppressors. Genes Dev. 26, 1326–1338 (2012).
Killian, J. K. et al. Succinate dehydrogenase mutation underlies global epigenomic divergence in gastrointestinal stromal tumor. Cancer Discov. 3, 648–657 (2013).
Flavahan, W. A. et al. Altered chromosomal topology drives oncogenic programs in SDH-deficient GISTs. Nature 575, 229–233 (2019).
Schwartzentruber, J. et al. Driver mutations in histone H3.3 and chromatin remodelling genes in paediatric glioblastoma. Nature 482, 226–231 (2012). This paper is one of the first demonstrations of the high frequency of histone mutations in human cancers.
Wu, G. et al. Somatic histone H3 alterations in pediatric diffuse intrinsic pontine gliomas and non-brainstem glioblastomas. Nat. Genet. 44, 251–253 (2012).
Behjati, S. et al. Distinct H3F3A and H3F3B driver mutations define chondroblastoma and giant cell tumor of bone. Nat. Genet. 45, 1479–1482 (2013). This paper demonstrates that high-frequency histone mutations occur in two distinct types of bone tumours.
Lu, C. et al. Histone H3K36 mutations promote sarcomagenesis through altered histone methylation landscape. Science 352, 844–849 (2016). This study provides a mechanistic explanation of how mesenchymal tumour-associated histone mutations broadly affect the chromatin landscape and mesenchymal differentiation.
Lewis, P. W. et al. Inhibition of PRC2 activity by a gain-of-function H3 mutation found in pediatric glioblastoma. Science 340, 857–861 (2013).
Fang, D. et al. The histone H3.3K36M mutation reprograms the epigenome of chondroblastomas. Science 352, 1344–1348 (2016).
Hübner, J.-M. et al. EZHIP/CXorf67 mimics K27M mutated oncohistones and functions as an intrinsic inhibitor of PRC2 function in aggressive posterior fossa ependymoma. Neuro-Oncology 21, 878–889 (2019).
Jain, S. U. et al. PFA ependymoma-associated protein EZHIP inhibits PRC2 activity through a H3 K27M-like mechanism. Nat. Commun. 10, 2146 (2019).
Pajtler, K. W. et al. Molecular heterogeneity and CXorf67 alterations in posterior fossa group A (PFA) ependymomas. Acta Neuropathol. 136, 211–226 (2018).
Piunti, A. et al. CATACOMB: an endogenous inducible gene that antagonizes H3K27 methylation activity of Polycomb repressive complex 2 via an H3K27M-like mechanism. Sci. Adv. 5, eaax2887 (2019).
Ragazzini, R. et al. EZHIP constrains Polycomb repressive complex 2 activity in germ cells. Nat. Commun. 10, 3858 (2019).
Fang, J. et al. Cancer-driving H3G34V/R/D mutations block H3K36 methylation and H3K36me3–MutSα interaction. Proc. Natl Acad. Sci. USA 115, 9598–9603 (2018).
Shi, L., Shi, J., Shi, X., Li, W. & Wen, H. Histone H3.3 G34 mutations alter histone H3K36 and H3K27 methylation in cis. J. Mol. Biol. 430, 1562–1565 (2018).
Zhao, S. et al. Mutational landscape of uterine and ovarian carcinosarcomas implicates histone genes in epithelial–mesenchymal transition. Proc. Natl Acad. Sci. USA 113, 12238–12243 (2016).
Arimura, Y. et al. Cancer-associated mutations of histones H2B, H3.1 and H2A.Z.1 affect the structure and stability of the nucleosome. Nucleic Acids Res. 46, 10007–10018 (2018).
Boileau, M. et al. Mutant H3 histones drive human pre-leukemic hematopoietic stem cell expansion and promote leukemic aggressiveness. Nat. Commun. 10, 2891 (2019).
Bennett, R. L. et al. A mutation in histone H2B represents a new class of oncogenic driver. Cancer Discov. 9, 1438–1451 (2019).
Widemann, B. C. & Italiano, A. Biology and management of undifferentiated pleomorphic sarcoma, myxofibrosarcoma, and malignant peripheral nerve sheath tumors: state of the art and perspectives. J. Clin. Oncol. 36, 160–167 (2018).
Lee, W. et al. PRC2 is recurrently inactivated through EED or SUZ12 loss in malignant peripheral nerve sheath tumors. Nat. Genet. 46, 1227–1232 (2014).
De Raedt, T. et al. PRC2 loss amplifies Ras-driven transcription and confers sensitivity to BRD4-based therapies. Nature 514, 247–251 (2014). Together with Lee et al. (2014), this paper shows that loss-of-function alterations in PRC2 are common in MPNSTs.
Schuettengruber, B., Bourbon, H.-M., Di Croce, L. & Cavalli, G. Genome regulation by polycomb and trithorax: 70 years and counting. Cell 171, 34–57 (2017).
Morin, R. D. et al. Somatic mutations altering EZH2 (Tyr641) in follicular and diffuse large B-cell lymphomas of germinal-center origin. Nat. Genet. 42, 181–185 (2010).
Cleven, A. H. G. et al. Loss of H3K27 tri-methylation is a diagnostic marker for malignant peripheral nerve sheath tumors and an indicator for an inferior survival. Mod. Pathol. 29, 582–590 (2016).
Marchione, D. M. et al. Histone H3K27 dimethyl loss is highly specific for malignant peripheral nerve sheath tumor and distinguishes true PRC2 loss from isolated H3K27 trimethyl loss. Mod. Pathol. 32, 1434–1446 (2019).
Pierron, G. et al. A new subtype of bone sarcoma defined by BCOR–CCNB3 gene fusion. Nat. Genet. 44, 461–466 (2012). This paper is one of the first next-generation sequencing studies to identify a novel fusion oncogene driver in undifferentiated sarcomas, involving chromatin-modifying proteins.
Specht, K. et al. Novel BCOR–MAML3 and ZC3H7B–BCOR gene fusions in undifferentiated small blue round cell sarcomas. Am. J. Surg. Pathol. 40, 433–442 (2016).
Kao, Y.-C. et al. BCOR–CCNB3 fusion positive sarcomas: a clinicopathologic and molecular analysis of 36 cases with comparison to morphologic spectrum and clinical behavior of other round cell sarcomas. Am. J. Surg. Pathol. 42, 604–615 (2018).
Wang, Z. et al. A non-canonical BCOR–PRC1.1 complex represses differentiation programs in human ESCs. Cell Stem Cell 22, 235–251.e9 (2018).
Astolfi, A. et al. BCOR involvement in cancer. Epigenomics 11, 835–855 (2019).
Koontz, J. I. et al. Frequent fusion of the JAZF1 and JJAZ1 genes in endometrial stromal tumors. Proc. Natl Acad. Sci. USA 98, 6348–6353 (2001).
Lewis, N. et al. ZC3H7B–BCOR high-grade endometrial stromal sarcomas: a report of 17 cases of a newly defined entity. Mod. Pathol. 31, 674–684 (2018).
Panagopoulos, I. et al. Fusion of the ZC3H7B and BCOR genes in endometrial stromal sarcomas carrying an X;22-translocation. Genes Chromosomes Cancer 52, 610–618 (2013).
Ma, X. et al. The JAZF1–SUZ12 fusion protein disrupts PRC2 complexes and impairs chromatin repression during human endometrial stromal tumorogenesis. Oncotarget 8, 4062–4078 (2017).
Cao, R. et al. Role of hPHF1 in H3K27 methylation and Hox gene silencing. Mol. Cell. Biol. 28, 1862–1872 (2008).
Micci, F., Panagopoulos, I., Bjerkehagen, B. & Heim, S. Consistent rearrangement of chromosomal band 6p21 with generation of fusion genes JAZF1/PHF1 and EPC1/PHF1 in endometrial stromal sarcoma. Cancer Res. 66, 107–112 (2006).
Dewaele, B. et al. Identification of a novel, recurrent MBTD1–CXorf67 fusion in low-grade endometrial stromal sarcoma. Int. J. Cancer 134, 1112–1122 (2014).
Jacquet, K. et al. The TIP60 complex regulates bivalent chromatin recognition by 53BP1 through direct H4K20me binding and H2AK15 acetylation. Mol. Cell 62, 409–421 (2016).
Alfert, A., Moreno, N. & Kerl, K. The BAF complex in development and disease. Epigenetics Chromatin 12, 19–15 (2019).
Perani, M., Ingram, C. J. E., Cooper, C. S., Garrett, M. D. & Goodwin, G. H. Conserved SNH domain of the proto-oncoprotein SYT interacts with components of the human chromatin remodelling complexes, while the QPGY repeat domain forms homo-oligomers. Oncogene 22, 8156–8167 (2003).
Ishida, M., Tanaka, S., Ohki, M. & Ohta, T. Transcriptional co-activator activity of SYT is negatively regulated by BRM and Brg1. Genes Cells 9, 419–428 (2004).
de Bruijn, D. R. H. et al. The synovial-sarcoma-associated SS18–SSX2 fusion protein induces epigenetic gene (de)regulation. Cancer Res. 66, 9474–9482 (2006).
Middeljans, E. et al. SS18 together with animal-specific factors defines human BAF-type SWI/SNF complexes. PLoS ONE 7, e33834 (2012).
Su, L. et al. Deconstruction of the SS18–SSX fusion oncoprotein complex: insights into disease etiology and therapeutics. Cancer Cell 21, 333–347 (2012).
Jones, K. B. et al. SS18–SSX2 and the mitochondrial apoptosis pathway in mouse and human synovial sarcomas. Oncogene 32, 2365–71–2375.e1–e5 (2013).
Garcia, C. B., Shaffer, C. M. & Eid, J. E. Genome-wide recruitment to Polycomb-modified chromatin and activity regulation of the synovial sarcoma oncogene SYT–SSX2. BMC Genomics 13, 189 (2012).
Pretto, D. et al. The synovial sarcoma translocation protein SYT–SSX2 recruits β-catenin to the nucleus and associates with it in an active complex. Oncogene 25, 3661–3669 (2006).
Kadoch, C. & Crabtree, G. R. Reversible disruption of mSWI/SNF (BAF) complexes by the SS18–SSX oncogenic fusion in synovial sarcoma. Cell 153, 71–85 (2013). This study shows that the SSX–SS18 fusion alters the composition and targeting of the SWI/SNF complex.
McBride, M. J. et al. The SS18–SSX fusion oncoprotein hijacks BAF complex targeting and function to drive synovial sarcoma. Cancer Cell 33, 1128–1141.e7 (2018).
Wang, X. et al. SMARCB1-mediated SWI/SNF complex function is essential for enhancer regulation. Nat. Genet. 49, 289–295 (2017).
Thway, K. & Folpe, A. L. Update on selected advances in the immunohistochemical and molecular genetic analysis of soft tissue tumors. Virchows Arch. path Anat. 476, 3–15 (2020).
Alpsoy, A. & Dykhuizen, E. C. Glioma tumor suppressor candidate region gene 1 (GLTSCR1) and its paralog GLTSCR1-like form SWI/SNF chromatin remodeling subcomplexes. J. Biol. Chem. 293, 3892–3903 (2018).
McDonald, E. R. et al. Project DRIVE: a compendium of cancer dependencies and synthetic lethal relationships uncovered by large-scale, deep RNAi screening. Cell 170, 577–592.e10 (2017).
Hohmann, A. F. et al. Sensitivity and engineered resistance of myeloid leukemia cells to BRD9 inhibition. Nat. Chem. Biol. 12, 672–679 (2016).
Krämer, K. F., Moreno, N., Frühwald, M. C. & Kerl, K. BRD9 inhibition, alone or in combination with cytostatic compounds as a therapeutic approach in rhabdoid tumors. Int. J. Mol. Sci. 18, 1537 (2017).
Brien, G. L. et al. Targeted degradation of BRD9 reverses oncogenic gene expression in synovial sarcoma. eLife 7, e41305 (2018).
Michel, B. C. et al. A non-canonical SWI/SNF complex is a synthetic lethal target in cancers driven by BAF complex perturbation. Nat. Cell Biol. 20, 1410–1420 (2018). Together with Brien et al. (2018), this paper identifies a dependency on BRD9 in synovial sarcoma, and proposes a role for BRD9 degradation in translational studies.
Banito, A. et al. The SS18–SSX oncoprotein hijacks KDM2B–PRC1.1 to drive synovial sarcoma. Cancer Cell 33, 527–541.e8 (2018).
Pawel, B. R. SMARCB1-deficient tumors of childhood: a practical guide. Pediatr. Dev. Pathol. 21, 6–28 (2018).
Thway, K., Jones, R. L., Noujaim, J. & Fisher, C. Epithelioid sarcoma: diagnostic features and genetics. Adv. Anatomic Pathol. 23, 41–49 (2016).
Guillou, L., Wadden, C., Coindre, J. M., Krausz, T. & Fletcher, C. D. ‘Proximal-type’ epithelioid sarcoma, a distinctive aggressive neoplasm showing rhabdoid features. clinicopathologic, immunohistochemical, and ultrastructural study of a series. Am. J. Surg. Pathol. 21, 130–146 (1997).
Hornick, J. L., Dal Cin, P. & Fletcher, C. D. M. Loss of INI1 expression is characteristic of both conventional and proximal-type epithelioid sarcoma. Am. J. Surg. Pathol. 33, 542–550 (2009).
Laskin, W. B. & Miettinen, M. Epithelioid sarcoma: new insights based on an extended immunohistochemical analysis. Arch. Pathol. Lab. Med. 127, 1161–1168 (2003).
Lee, R. S. et al. A remarkably simple genome underlies highly malignant pediatric rhabdoid cancers. J. Clin. Invest. 122, 2983–2988 (2012).
Jamshidi, F. et al. The genomic landscape of epithelioid sarcoma cell lines and tumours. J. Pathol. 238, 63–73 (2016).
Sullivan, L. M., Folpe, A. L., Pawel, B. R., Judkins, A. R. & Biegel, J. A. Epithelioid sarcoma is associated with a high percentage of SMARCB1 deletions. Mod. Pathol. 26, 385–392 (2013).
Papp, G., Krausz, T., Stricker, T. P., Szendrői, M. & Sápi, Z. SMARCB1 expression in epithelioid sarcoma is regulated by miR-206, miR-381, and miR-671-5p on both mRNA and protein levels. Genes Chromosomes Cancer 53, 168–176 (2014).
Sápi, Z. et al. Epigenetic regulation of SMARCB1 By miR-206, -381 and -671-5p is evident in a variety of SMARCB1 immunonegative soft tissue sarcomas, while miR-765 appears specific for epithelioid sarcoma. A miRNA study of 223 soft tissue sarcomas. Genes Chromosomes Cancer 55, 786–802 (2016).
Nakayama, R. T. et al. SMARCB1 is required for widespread BAF complex-mediated activation of enhancers and bivalent promoters. Nat. Genet. 49, 1613–1623 (2017).
Chun, H.-J. E. et al. Identification and analyses of extra-cranial and cranial rhabdoid tumor molecular subgroups reveal tumors with cytotoxic T cell infiltration. Cell Rep. 29, 2338–2354.e7 (2019).
Brownlee, P. M., Meisenberg, C. & Downs, J. A. The SWI/SNF chromatin remodelling complex: its role in maintaining genome stability and preventing tumourigenesis. DNA Repair. 32, 127–133 (2015).
Peng, G. et al. BRIT1/MCPH1 links chromatin remodelling to DNA damage response. Nat. Cell Biol. 11, 865–872 (2009).
Qi, W. et al. BRG1 promotes the repair of DNA double-strand breaks by facilitating the replacement of RPA with RAD51. J. Cell. Sci. 128, 317–330 (2015).
Kakarougkas, A. et al. Requirement for PBAF in transcriptional repression and repair at DNA breaks in actively transcribed regions of chromatin. Mol. Cell 55, 723–732 (2014).
Park, J.-H. et al. Mammalian SWI/SNF complexes facilitate DNA double-strand break repair by promoting γ-H2AX induction. EMBO J. 25, 3986–3997 (2006).
US National Library of Medicine. ClinicalTrials.gov https://clinicaltrials.gov/ct2/show/NCT02601950 (2020).
Daigle, S. et al. Molecular characterization of epithelioid sarcoma (ES) tumors derived from patients enrolled in a phase II study of tazemetostat (NCT02601950) [abstract 18920]. Ann. Oncol. 29, viii670–viii682 (2018).
Kohashi, K. et al. SWI/SNF chromatin-remodeling complex status in SMARCB1/INI1-preserved epithelioid sarcoma. Am. J. Surg. Pathol. 42, 312–318 (2018).
Perret, R. et al. SMARCA4-deficient thoracic sarcomas: clinicopathologic study of 30 cases with an emphasis on their nosology and differential diagnoses. Am. J. Surg. Pathol. 43, 455–465 (2019).
Rekhtman, N. et al. Thoracic SMARCA4-deficient sarcomatoid tumors represent primarily smoking-related undifferentiated carcinomas rather than primary thoracic sarcomas. J. Thorac. Oncol. 15, 231–247 (2019).
Karnezis, A. N. et al. Dual loss of the SWI/SNF complex ATPases SMARCA4/BRG1 and SMARCA2/BRM is highly sensitive and specific for small cell carcinoma of the ovary, hypercalcaemic type. J. Pathol. 238, 389–400 (2016).
Kolin, D. L. et al. SMARCA4-deficient undifferentiated uterine sarcoma (malignant rhabdoid tumor of the uterus): a clinicopathologic entity distinct from undifferentiated carcinoma. Mod. Pathol. 31, 1442–1456 (2018).
Lin, D. I. et al. SMARCA4 inactivation defines a subset of undifferentiated uterine sarcomas with rhabdoid and small cell features and germline mutation association. Mod. Pathol. 32, 1675–1687 (2019).
Lindén, M. et al. FET family fusion oncoproteins target the SWI/SNF chromatin remodeling complex. EMBO Rep. 20, 1741 (2019).
Schwartz, J. C., Cech, T. R. & Parker, R. R. Biochemical properties and biological functions of FET proteins. Annu. Rev. Biochem. 84, 355–379 (2014).
Sankar, S. & Lessnick, S. L. Promiscuous partnerships in Ewing’s sarcoma. Cancer Genet. 204, 351–365 (2011).
Couthouis, J. et al. A yeast functional screen predicts new candidate ALS disease genes. Proc. Natl Acad. Sci. USA 108, 20881–20890 (2011).
Couthouis, J. et al. Evaluating the role of the FUS/TLS-related gene EWSR1 in amyotrophic lateral sclerosis. Hum. Mol. Genet. 21, 2899–2911 (2012).
Kato, M. et al. Cell-free formation of RNA granules: low complexity sequence domains form dynamic fibers within hydrogels. Cell 149, 753–767 (2012).
Kwon, I. et al. Phosphorylation-regulated binding of RNA polymerase II to fibrous polymers of low-complexity domains. Cell 155, 1049–1060 (2013).
Schwartz, J. C., Wang, X., Podell, E. R. & Cech, T. R. RNA seeds higher-order assembly of FUS protein. Cell Rep. 5, 918–925 (2013).
Burke, K. A., Janke, A. M., Rhine, C. L. & Fawzi, N. L. Residue-by-residue view of in vitro FUS granules that bind the C-terminal domain of RNA polymerase II. Mol. Cell 60, 231–241 (2015).
Patel, A. et al. A liquid-to-solid phase transition of the ALS protein FUS accelerated by disease mutation. Cell 162, 1066–1077 (2015).
Lu, H. et al. Phase-separation mechanism for C-terminal hyperphosphorylation of RNA polymerase II. Nature 558, 318–323 (2018).
Sabari, B. R. et al. Coactivator condensation at super-enhancers links phase separation and gene control. Science 361, eaar3958 (2018).
Riggi, N. et al. EWS–FLI1 utilizes divergent chromatin remodeling mechanisms to directly activate or repress enhancer elements in Ewing sarcoma. Cancer Cell 26, 668–681 (2014).
Boulay, G. et al. Epigenome editing of microsatellite repeats defines tumor-specific enhancer functions and dependencies. Genes Dev. 32, 1008–1019 (2018).
Tomazou, E. M. et al. Epigenome mapping reveals distinct modes of gene regulation and widespread enhancer reprogramming by the oncogenic fusion protein EWS–FLI1. Cell Rep. 10, 1082–1095 (2015).
Yoshida, K.-I. et al. Absence of H3F3A mutation in a subset of malignant giant cell tumor of bone. Mod. Pathol. 32, 1751–1761 (2019).
Chen, S. et al. Diagnostic utility of IDH1/2 mutations to distinguish dedifferentiated chondrosarcoma from undifferentiated pleomorphic sarcoma of bone. Hum. Pathol. 65, 239–246 (2017).
Noujaim, J. et al. The spectrum of EWSR1-rearranged neoplasms at a tertiary sarcoma centre; assessing 772 tumour specimens and the value of current ancillary molecular diagnostic modalities. Br. J. Cancer 116, 669–678 (2017).
Qadir, M. A. et al. ChildSeq-RNA: a next-generation sequencing-based diagnostic assay to identify known fusion transcripts in childhood sarcomas. J. Mol. Diagn. 16, 361–370 (2014).
Zhu, G. et al. Diagnosis of known sarcoma fusions and novel fusion partners by targeted RNA sequencing with identification of a recurrent ACTB–FOSB fusion in pseudomyogenic hemangioendothelioma. Mod. Pathol. 32, 609–620 (2019).
Chang, K. T. E. et al. Development and evaluation of a pan-sarcoma fusion gene detection assay using the NanoString nCounter platform. J. Mol. Diagn. 20, 63–77 (2018).
Salguero-Aranda, C., Amaral, A. T., Olmedo-Pelayo, J., Diaz-Martin, J. & Álava, E. de. Breakthrough technologies reshape the Ewing sarcoma molecular landscape. Cells 9, 804 (2020).
Cermakova, K. & Hodges, H. C. Next-generation drugs and probes for chromatin biology: from targeted protein degradation to phase separation. Molecules 23, 1958 (2018).
Pfister, S. X. & Ashworth, A. Marked for death: targeting epigenetic changes in cancer. Nat. Rev. Drug. Discov. 16, 241–263 (2017).
Versteege, I. et al. Truncating mutations of hSNF5/INI1 in aggressive paediatric cancer. Nature 394, 203–206 (1998).
Modena, P. et al. SMARCB1/INI1 tumor suppressor gene is frequently inactivated in epithelioid sarcomas. Cancer Res. 65, 4012–4019 (2005). This paper is the first report describing loss of SMARCB1 as a common event in epithelioid sarcoma.
Valencia, A. M. et al. Recurrent SMARCB1 mutations reveal a nucleosome acidic patch interaction site that potentiates mSWI/SNF complex chromatin remodeling. Cell 179, 1342–1356.e23 (2019).
Wilson, B. G. et al. Epigenetic antagonism between polycomb and SWI/SNF complexes during oncogenic transformation. Cancer Cell 18, 316–328 (2010). This study demonstrates functional interactions between PRC2 and the SWI/SNF complex, with implications for epigenetic treatment strategies.
Knutson, S. K. et al. Durable tumor regression in genetically altered malignant rhabdoid tumors by inhibition of methyltransferase EZH2. Proc. Natl Acad. Sci. USA 110, 7922–7927 (2013). This paper demonstrates that small-molecule inhibition of the catalytic subunit of PRC2 inhibits the growth of preclinical models of SWI/SNF complex-altered sarcoma, providing a scientific rationale for subsequent clinical trials with tazemetostat.
Wang, Y. et al. The histone methyltransferase EZH2 is a therapeutic target in small cell carcinoma of the ovary, hypercalcaemic type. J. Pathol. 242, 371–383 (2017).
Stacchiotti, S. et al. Safety and efficacy of tazemetostat, a first-in-class EZH2 inhibitor, in patients (pts) with epithelioid sarcoma (ES) (NCT02601950) [abstract 11003]. JCO 37, 11003–11003 (2019).
Schöffski, P. et al. Phase 2 multicenter study of the EZH2 inhibitor tazemetostat in adults with synovial sarcoma (NCT02601950) [abstract 11057]. JCO 35, 11057–11057 (2017).
US National Library of Medicine. ClinicalTrials.gov https://clinicaltrials.gov/ct2/show/NCT02273739 (2020).
US National Library of Medicine. ClinicalTrials.gov https://clinicaltrials.gov/ct2/show/NCT02073994 (2020).
US National Library of Medicine. ClinicalTrials.gov https://clinicaltrials.gov/ct2/show/NCT04278781 (2020).
Fan, B. et al. Clinical pharmacokinetics and pharmacodynamics of ivosidenib, an oral, targeted inhibitor of mutant IDH1, in patients with advanced solid tumors. Invest. New Drugs 462, 1–12 (2019).
Tap, W. et al. Phase I study of the mutant IDH1 inhibitor ivosidenib: safety and clinical activity in patients with advanced chondrosarcoma. J. Clin. Oncol. 38, 1693–1701 (2020).
Wang, X. et al. BRD9 defines a SWI/SNF sub-complex and constitutes a specific vulnerability in malignant rhabdoid tumors. Nat. Commun. 10, 1881 (2019).
McBride, M. J. & Kadoch, C. Disruption of mammalian SWI/SNF and Polycomb complexes in human sarcomas: mechanisms and therapeutic opportunities. J. Pathol. 244, 638–649 (2018).
Cooper, J. M. et al. Overcoming BET inhibitor resistance in malignant peripheral nerve sheath tumors. Clin. Cancer Res. 25, 3404–3416 (2019).
Moffat, J. G., Rudolph, J. & Bailey, D. Phenotypic screening in cancer drug discovery — past, present and future. Nat. Rev. Drug. Discov. 13, 588–602 (2014).
Cancer Genome Atlas Research Network. Comprehensive genomic characterization defines human glioblastoma genes and core pathways. Nature 455, 1061–1068 (2008).
Demetri, G. D. et al. Efficacy and safety of imatinib mesylate in advanced gastrointestinal stromal tumors. N. Engl. J. Med. 347, 472–480 (2002).
Doebele, R. C. et al. An oncogenic NTRK fusion in a patient with soft-tissue sarcoma with response to the tropomyosin-related kinase inhibitor LOXO-101. Cancer Discov. 5, 1049–1057 (2015).
Drilon, A. et al. Efficacy of larotrectinib in TRK fusion-positive cancers in adults and children. N. Engl. J. Med. 378, 731–739 (2018).
Laetsch, T. W. et al. Larotrectinib for paediatric solid tumours harbouring NTRK gene fusions: phase 1 results from a multicentre, open-label, phase 1/2 study. Lancet Oncol. 19, 705–714 (2018).
US National Library of Medicine. ClinicalTrials.gov https://clinicaltrials.gov/ct2/show/NCT02601937 (2020).
US National Library of Medicine. ClinicalTrials.gov https://clinicaltrials.gov/ct2/show/NCT03213665 (2020).
US National Library of Medicine. ClinicalTrials.gov https://clinicaltrials.gov/ct2/show/NCT02875548 (2020).
Hyman, A. A., Weber, C. A. & Jülicher, F. Liquid–liquid phase separation in biology. Annu. Rev. Cell Dev. Biol. 30, 39–58 (2014).
Banani, S. F., Lee, H. O., Hyman, A. A. & Rosen, M. K. Biomolecular condensates: organizers of cellular biochemistry. Nat. Rev. Mol. Cell Biol. 18, 285–298 (2017).
Shin, Y. & Brangwynne, C. P. Liquid phase condensation in cell physiology and disease. Science 357, eaaf4382 (2017).
Overbeek, J. T. & Voorn, M. J. Phase separation in polyelectrolyte solutions; theory of complex coacervation. J. Cell Physiol. Suppl. 49, 7–26 (1957).
Boeynaems, S. et al. Protein phase separation: a new phase in cell biology. Trends Cell Biol. 28, 420–435 (2018).
Mao, Y. S., Zhang, B. & Spector, D. L. Biogenesis and function of nuclear bodies. Trends Genet. 27, 295–306 (2011).
Decker, C. J. & Parker, R. P-bodies and stress granules: possible roles in the control of translation and mRNA degradation. Cold Spring Harb. Perspect. Biol. 4, a012286–a012286 (2012).
Li, P. et al. Phase transitions in the assembly of multivalent signalling proteins. Nature 483, 336–340 (2012).
Wang, J. et al. A molecular grammar governing the driving forces for phase separation of prion-like RNA binding proteins. Cell 174, 688–699.e16 (2018).
Banjade, S. & Rosen, M. K. Phase transitions of multivalent proteins can promote clustering of membrane receptors. eLife 3, 641 (2014).
Su, X. et al. Phase separation of signaling molecules promotes T cell receptor signal transduction. Science 352, 595–599 (2016).
Romero, P. et al. Sequence complexity of disordered protein. Proteins 42, 38–48 (2001).
Vucetic, S., Brown, C. J., Dunker, A. K. & Obradovic, Z. Flavors of protein disorder. Proteins 52, 573–584 (2003).
Brangwynne, C. P., Tompa, P. & Pappu, R. V. Polymer physics of intracellular phase transitions. Nat. Phys. 11, 899–904 (2015).
King, O. D., Gitler, A. D. & Shorter, J. The tip of the iceberg: RNA-binding proteins with prion-like domains in neurodegenerative disease. Brain Res. 1462, 61–80 (2012).
Boija, A. et al. Transcription factors activate genes through the phase-separation capacity of their activation domains. Cell 175, 1842–1855.e16 (2018).
Alberti, S. & Dormann, D. Liquid–liquid phase separation in disease. Annu. Rev. Genet. 53, 171–194 (2019).
Alberti, S., Gladfelter, A. & Mittag, T. Considerations and challenges in studying liquid–liquid phase separation and biomolecular condensates. Cell 176, 419–434 (2019).
McSwiggen, D. T., Mir, M., Darzacq, X. & Tjian, R. Evaluating phase separation in live cells: diagnosis, caveats, and functional consequences. Genes Dev. 33, 1619–1634 (2019).
Acknowledgements
The authors thank P. Stirling, T. M. Underhill, M. Hirst, B. Dickson and E. Demicco for helpful discussions about some of the topics covered in this review, and A. Soshnev, M. Hirst and L. Wang for assistance in figure preparation. B.A.N is supported by the National Cancer Institute (NCI) (1K08CA245212-01) and the QuadW Foundation/American Association for Cancer Research (AACR) (19-40-37-NACE). This research was funded in part through the NIH/NCI Cancer Center Support Grant P30 CA008748, NIH/NCI P01CA196539, the Canadian Cancer Society (705615) and the Terry Fox Research Institute (1082).
Author information
Authors and Affiliations
Contributions
B.A.N., K.B.J., A.M.I., J.S.E.Y., W.D.T. and T.O.N. researched data for the article. B.A.N., K.B.J., A.M.I., W.D.T., M.L., C.D.A. and T.O.N. provided a substantial contribution to discussion of the content. All authors contributed to writing the article and to the review and/or editing of the manuscript before submission.
Corresponding author
Ethics declarations
Competing interests
A.M.I. previously consulted for Foundation Medicine, Inc. W.D.T. reports personal fees from Agios Pharmaceuticals, Eli Lilly, EMD Serono, Eisai, Janssen, Immune Design, Daiichi Sankyo, Blueprint, Loxo, GlaxoSmithKline, NanoCarrier and Deciphera outside the submitted work. In addition, W.D.T. has a patent Companion Diagnostic for CDK4 inhibitors (14/854,329 pending to Memorial Sloan Kettering Cancer Center (MSKCC)/Sloan Kettering Institute (SKI). W.D.T. is also on the scientific Advisory Board of Certis Oncology Solutions and Atropos Therapeutics (both stock ownership) and is a consultant for Daiichi Sankyo (FDA Oncologic Drugs Advisory Committee (ODAC) meeting, pexidartinib). T.O.N. has a patent on the Prosigna breast cancer diagnostic (Veracyte Technologies) outside the submitted work. B.A.N., K.B.J., J.S.E.Y., C.D.A. and M.L. declare no competing interests.
Additional information
Peer review information
Nature Reviews Cancer thanks B. Bernstein, H. Kovar and the other, anonymous, reviewer(s) for their contribution to the peer review of this work.
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Glossary
- Undifferentiated pleomorphic sarcoma
-
A malignant mesenchymal tumour of undefined histogenesis, with histologically characterized high-grade spindle cells producing a non-specific collagenous matrix. Previously termed malignant fibrous histiocytoma, this sarcoma is classified as a diagnosis of exclusion.
- Ewing sarcoma
-
A malignant bone or soft tissue tumour comprising uniform small blue round cells, typically affecting children and adolescents. Driven by chromosomal translocations resulting in transcripts fusing FET genes with genes encoding ETS family transcription factors, Ewing sarcoma breakpoint region 1 (EWSR1)–friend leukaemia virus integration 1 (FLI1) being the most common variant.
- Synovial sarcoma
-
A malignant translocation-associated sarcoma driven by the SS18–SSX gene fusion. Although frequently arising in extremities near joints, the term is a misnomer as the cell of origin is unknown and the tumour is not derived from synovium and does not differentiate into synovial-type tissue. Synovial sarcoma exists as monophasic spindle cell forms or as a biphasic type with areas of epithelial differentiation.
- Gastrointestinal stromal tumours
-
(GISTs). Mesenchymal neoplasm of the gastrointestinal tract, derived from the interstitial cells of Cajal. Activating mutations in the KIT (or PDGFRA) receptor tyrosine kinases are the key initiating oncogenic events in the majority of cases, making imatinib and related tyrosine kinase inhibitors an effective targeted therapy for this disease.
- Chondrosarcomas
-
Malignant cartilaginous matrix-producing tumours often driven by isocitrate dehydrogenase 1 (IDH1) or IDH2 mutations. Typically arising in the axial skeleton of middle-aged patients, these sarcomas can be slow growing but resistant to existing systemic therapy and radiotherapy.
- Nucleosomes
-
Basic repeating structural units of the chromosome consisting of 8 histone proteins (2 each of 4 core histones: H3, H4, H2A and H2B) with 147 base pairs of DNA wrapping the structure.
- Giant cell tumour of bone
-
A benign but often locally aggressive neoplasm of bone in young adults driven by missense histone mutations at the histone H3.3 G34 variant. These tumours have a propensity for local recurrence and present as radiolytic lesions that destroy bone underneath articular surfaces.
- Chondroblastoma
-
A benign cartilaginous neoplasm that characteristically arises at the ends of long bones, close to the joints, and occurs predominantly in adolescents. It is driven by the histone H3.3 K36M mutation.
- Malignant peripheral nerve sheath tumours
-
(MPNSTs). Sarcomas arising within peripheral nerves, about half of which are sporadic and half of which occur in the context of congenital NF1 (neurofibromatosis type 1) inactivating mutations. Development of MPNSTs is additionally driven by (often mutually exclusive) loss-of-function alterations in suppressor of zeste 12 (SUZ12) or embryonic ectoderm development (EED).
- Malignant rhabdoid tumours
-
Highly aggressive, malignant tumours that occur in infants and young children. Three presentations exist — kidney, extrarenal and brain (the latter being termed atypical teratoid/rhabdoid tumour) — and all are characterized by bi-allelic deletion of SWI/SNF-related matrix-associated actin-dependent regulator of chromatin subfamily B member 1 (SMARCB1).
- Epithelioid sarcoma
-
Malignant soft tissue sarcoma in distal extremities, with mixed features of mesenchymal and epithelial differentiation. It typically affects adolescents and young adults, metastasizes aggressively and is resistant to conventional chemotherapies. Epithelioid sarcoma is characterized by inactivating mutations in SWI/SNF-related matrix-associated actin-dependent regulator of chromatin subfamily B member 1 (SMARCB1).
- Chromatin remodelling complexes
-
Multiple families of protein complexes that alter chromatin structure (that is, histone–DNA and histone–histone contacts) to regulate gene expression in an ATP-dependent fashion. Their functions include alteration of nucleosome assembly (maturation and spacing), chromatin access (nucleosome repositioning or ejection) and nucleosome editing (histone exchange or eviction). SWI/SNF complexes are one such family of chromatin remodelling complexes.
- Enhancer
-
A gene regulatory element that binds transcription factors and cofactors to activate transcription of target genes that may be located a relatively far linear distance away, and independent of their orientation on DNA.
- Bisulfite sequencing
-
The current gold-standard sequencing strategy for detecting DNA methylation based on the conversion of unmethylated cytosine to uracil after treatment with sodium bisulfite (without modification of methylated cytosine). Reduced representation bisulfite sequencing is a variation on this method that selects for areas of the genome rich in CpG islands, including promoters, with less starting material required and lower cost.
- CpG islands
-
Segments of genomic DNA, several hundred base pairs in length, that contain a large number of CpG dinucleotide (where a cytosine is followed by a guanine) repeats. When occurring near promoters of expressed genes, CpG islands are usually unmethylated; in contrast, CpG dinucleotides occurring in other contexts tend to be methylated.
- Small blue round cell sarcomas
-
Undifferentiated mesenchymal tumours with uniform round nuclei and very little cytoplasm that are histologically difficult to distinguish, including not only Ewing family tumours but several rarer and emerging entities with distinctive molecular drivers, prognoses and responses to therapy.
- Polycomb group
-
(PcG). A group of proteins originally discovered in Drosophila involved in the establishment and maintenance of developmental gene expression programmes through formation of polycomb repressive complexes (PRCs) that repress gene expression by methylation of histone H3 K27 (PRC2) and ubiquitylation of H2A K119 (PRC1).
- DNA hydroxymethylation
-
A type of DNA modification in which the oxidation of methylated cytosines at CpG dinucleotides to 5-hydroxymethylcytosine is catalysed by the TET family of methylcytosine dioxygenases. This process serves as an intermediate step in DNA demethylation.
- Contact inhibition
-
A fundamental property of normal cells to cease proliferation or migration when in contact with neighbouring cells.
- Chromatin insulator
-
DNA elements and protein binding partners, including CCCTC-binding factor (CTCF), that protect nearby genes from adjacent chromatin regulatory domains and can limit enhancer–promoter interactions.
- Endometrial stromal sarcomas
-
(ESSs). Uterine malignancies with low and high-grade forms that are associated with distinct genetic rearrangements and fusion oncogenes. Typically presenting in middle age, the disease is relatively slower to progress than most other types of sarcoma.
- Angiosarcoma
-
An aggressive, malignant endothelial cell tumour of vascular or lymphatic origin that can arise anywhere in the body, sporadically or sometimes in association with radiation exposure or lymphoedema. Angiosarcomas are especially infiltrative and prone to metastatic spread.
- Desmoplastic small round cell tumour
-
An aggressive, malignant neoplasm and member of the small blue round cell tumour family that typically presents as a large mass in the abdomen of adolescent and young males. It is characterized by a translocation resulting in Ewing sarcoma breakpoint region 1 (EWSR1)–WT1 fusion transcripts; this sarcoma does not respond well to any currently available systemic therapies.
- Homologous recombination
-
The exchange of nucleotide sequences between two similar or identical DNA strands that is used to generate sequence variation during meiosis or to direct error-free repair of DNA double-strand breaks.
- Sarcomatoid tumours
-
A descriptive term for neoplasms of non-mesenchymal origin that develop a sarcoma-like histological phenotype (characterized by spindle cell cytomorphology, matrix production and cell–matrix interactions); for example, carcinomas that have undergone epithelial–mesenchymal transition.
- Mediastinal tumours
-
A term for primary neoplasms of the thoracic cavity, other than lung cancers.
- Phase separation
-
A physical process in which a single homogeneous liquid phase spontaneously separates into two distinct phases owing to changes in the environment, such as pH, temperature, salt or protein concentration.
- Microsatellite regions
-
Arrays of repetitive short DNA sequences, which tend to accumulate mutations owing to the risk of strand slippage during DNA replication. These mutations are normally repaired unless there is loss of function in the mismatch repair system, which leads to microsatellite instability.
- Super-enhancers
-
Clusters of enhancers in close genomic proximity with high concentrations of bound transcriptional co-activators that control gene expression programmes to regulate cell identity.
- Chromatin looping
-
A model for long-range control of gene expression to allow for direct contact of promoters and enhancers over long linear distances by looping out the intervening chromatin. Loops are mediated and stabilized by proteins and complexes including CCCTC-binding factor (CTCF), mediator and cohesin.
- Chromatin immunoprecipitation followed by sequencing
-
(ChIP–seq). A technique used to identify the DNA sequences that are in close physical proximity to a chromatin-associated protein, transcription factor or other protein of interest. In this technique, the genomic DNA is fragmented and then the protein of interest is immunoprecipitated along with associated DNA fragments, which are subsequently sequenced.
- Chemical degraders
-
Compounds that bind a target protein through one chemical domain and through a second domain recruit the cereblon E3 ubiquitin ligase complex leading to degradation of the target protein. Degradation can have a distinct biological effect from small-molecule inhibition of the target in cases where the target protein has non-enzymatic functions.
Rights and permissions
About this article
Cite this article
Nacev, B.A., Jones, K.B., Intlekofer, A.M. et al. The epigenomics of sarcoma. Nat Rev Cancer 20, 608–623 (2020). https://doi.org/10.1038/s41568-020-0288-4
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41568-020-0288-4
This article is cited by
-
Epigenetics in diabetic cardiomyopathy
Clinical Epigenetics (2024)
-
Are orthopedic clinical trials representative? An analysis of race and ethnicity reported in clinical trials between 2007 and 2022
Archives of Orthopaedic and Trauma Surgery (2024)
-
HMGA1 regulates trabectedin sensitivity in advanced soft-tissue sarcoma (STS): A Spanish Group for Research on Sarcomas (GEIS) study
Cellular and Molecular Life Sciences (2024)
-
Epigenetic regulation in metabolic diseases: mechanisms and advances in clinical study
Signal Transduction and Targeted Therapy (2023)
-
(B)On(e)-cohistones and the epigenetic alterations at the root of bone cancer
Cell Death & Differentiation (2023)