Abstract
The field of research in bladder cancer has seen significant advances in recent years. Next-generation sequencing has identified the genes most mutated in bladder cancer. This wealth of information allowed the definition of driver mutations, and identification of actionable therapeutic targets, as well as a clearer picture of patient prognosis and therapeutic direction. In a similar vein, our understanding of the cellular aspects of bladder cancer has grown. The identification of the cellular geography and the populations of different cell types and quantifications of normal and abnormal cell types in tumours provide a better prediction of therapeutic response. Non-invasive methods of diagnosis, including liquid biopsies, have seen major advances as well. These methods will likely find considerable utility in assessing minimal residual disease following treatment and for early-stage diagnosis. A significant therapeutic impact on patients with bladder cancer is found in the use of immune checkpoint inhibitor therapeutics. These therapeutics have been shown to cure some patients with bladder cancer and significantly decrease adverse events. These developments provide patients with better monitoring opportunities, unique therapeutic options and greater hope for prolonged survival.
This is a preview of subscription content, access via your institution
Access options
Access Nature and 54 other Nature Portfolio journals
Get Nature+, our best-value online-access subscription
$29.99 / 30 days
cancel any time
Subscribe to this journal
Receive 12 print issues and online access
$209.00 per year
only $17.42 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout



Similar content being viewed by others
References
Bray, F. et al. Global cancer statistics 2018: GLOBOCAN estimates of incidence and mortality worldwide for 36 cancers in 185 countries. CA Cancer J. Clin. 68, 394–424 (2018).
Pardo, J. C. et al. Moving towards personalized medicine in muscle-invasive bladder cancer: where are we now and where are we going? Int. J. Mol. Sci 21, https://doi.org/10.3390/ijms21176271 (2020).
Witjes, J. A. et al. European association of urology guidelines on muscle-invasive and metastatic bladder cancer: summary of the 2020 guidelines. Eur. Urol. https://doi.org/10.1016/j.eururo.2020.03.055 (2020).
Lindgren, D. et al. Combined gene expression and genomic profiling define two intrinsic molecular subtypes of urothelial carcinoma and gene signatures for molecular grading and outcome. Cancer Res. 70, 3463–3472 (2010).
Sjodahl, G. et al. A molecular taxonomy for urothelial carcinoma. Clin. Cancer Res. 18, 3377–3386 (2012).
Volkmer, J. P. et al. Three differentiation states risk-stratify bladder cancer into distinct subtypes. Proc. Natl Acad. Sci. USA 109, 2078–2083 (2012).
Robertson, A. G. et al. Comprehensive molecular characterization of muscle-invasive bladder cancer. Cell 171, 540–556 e525 (2017). This study reports molecular characterization of 412 patients with MIBC, using multiple TCGA platforms, to identify mutation and expression data on mRNA, long non-coding RNA and microRNA, leading to the identification of five molecular subtypes.
Damrauer, J. S. et al. Intrinsic subtypes of high-grade bladder cancer reflect the hallmarks of breast cancer biology. Proc. Natl Acad. Sci. USA 111, 3110–3115 (2014).
Rebouissou, S. et al. EGFR as a potential therapeutic target for a subset of muscle-invasive bladder cancers presenting a basal-like phenotype. Sci. Transl Med. 6, 244ra291 (2014).
Choi, W. et al. Identification of distinct basal and luminal subtypes of muscle-invasive bladder cancer with different sensitivities to frontline chemotherapy. Cancer Cell 25, 152–165 (2014).
Seiler, R. et al. Impact of molecular subtypes in muscle-invasive bladder cancer on predicting response and survival after neoadjuvant chemotherapy. Eur. Urol. 72, 544–554 (2017).
Sjodahl, G., Eriksson, P., Liedberg, F. & Hoglund, M. Molecular classification of urothelial carcinoma: global mRNA classification versus tumour-cell phenotype classification. J. Pathol. 242, 113–125 (2017).
Marzouka, N. A. et al. A validation and extended description of the Lund taxonomy for urothelial carcinoma using the TCGA cohort. Sci. Rep. 8, 3737 (2018).
Sjodahl, G. et al. Discordant molecular subtype classification in the basal-squamous subtype of bladder tumors and matched lymph-node metastases. Mod. Pathol. 31, 1869–1881 (2018).
Tan, T. Z., Rouanne, M., Tan, K. T., Huang, R. Y. & Thiery, J. P. Molecular subtypes of urothelial bladder cancer: results from a meta-cohort analysis of 2411 tumors. Eur. Urol. 75, 423–432 (2019).
Morera, D. S. et al. Clinical parameters outperform molecular subtypes for predicting outcome in bladder cancer: results from multiple cohorts, including TCGA. J. Urol. 203, 62–72 (2020).
Lawrence, M. S. et al. Mutational heterogeneity in cancer and the search for new cancer-associated genes. Nature 499, 214–218 (2013).
Alexandrov, L. B. et al. Signatures of mutational processes in human cancer. Nature 500, 415–421 (2013).
Rachakonda, P. S. et al. TERT promoter mutations in bladder cancer affect patient survival and disease recurrence through modification by a common polymorphism. Proc. Natl Acad. Sci. USA 110, 17426–17431 (2013).
Leao, R. et al. Combined genetic and epigenetic alterations of the TERT promoter affect clinical and biological behavior of bladder cancer. Int. J. Cancer 144, 1676–1684 (2019).
Kurtis, B. et al. Recurrent TERT promoter mutations in urothelial carcinoma and potential clinical applications. Ann. Diagn. Pathol. 21, 7–11 (2016).
Allory, Y. et al. Telomerase reverse transcriptase promoter mutations in bladder cancer: high frequency across stages, detection in urine, and lack of association with outcome. Eur. Urol. 65, 360–366 (2014).
Berdik, C. Unlocking bladder cancer. Nature 551, S34–S35 (2017).
Knowles, M. A. & Hurst, C. D. Molecular biology of bladder cancer: new insights into pathogenesis and clinical diversity. Nat. Rev. Cancer 15, 25–41 (2015).
Babjuk, M. et al. EAU guidelines on non-muscle-invasive urothelial carcinoma of the bladder: update 2016. Eur. Urol. 71, 447–461 (2017).
James, A. C. & Gore, J. L. The costs of non-muscle invasive bladder cancer. Urol. Clin. North. Am. 40, 261–269 (2013).
Abdollah, F. et al. Incidence, survival and mortality rates of stage-specific bladder cancer in United States: a trend analysis. Cancer Epidemiol. 37, 219–225 (2013).
van Rhijn, B. W. et al. Molecular grading of urothelial cell carcinoma with fibroblast growth factor receptor 3 and MIB-1 is superior to pathologic grade for the prediction of clinical outcome. J. Clin. Oncol. 21, 1912–1921 (2003).
Lopez-Knowles, E. et al. PIK3CA mutations are an early genetic alteration associated with FGFR3 mutations in superficial papillary bladder tumors. Cancer Res. 66, 7401–7404 (2006).
Hernandez, S. et al. Prospective study of FGFR3 mutations as a prognostic factor in nonmuscle invasive urothelial bladder carcinomas. J. Clin. Oncol. 24, 3664–3671 (2006).
Hartmann, A. et al. Frequent genetic alterations in simple urothelial hyperplasias of the bladder in patients with papillary urothelial carcinoma. Am. J. Pathol. 154, 721–727 (1999).
Hedegaard, J. et al. Comprehensive transcriptional analysis of early-stage urothelial carcinoma. Cancer Cell 30, 27–42 (2016).
Stroggilos, R. et al. Proteome-based classification of nonmuscle invasive bladder cancer. Int. J. Cancer 146, 281–294 (2020).
Kamoun, A. et al. A consensus molecular classification of muscle-invasive bladder cancer. Eur. Urol. 77, 420–433 (2020). This work creates molecular classes of MIBC for clinical application to patient prognosis and treatment regimens.
de Jong, J. J. et al. Long non-coding RNAs identify a subset of luminal muscle-invasive bladder cancer patients with favorable prognosis. Genome Med. 11, 60 (2019).
Venter, J. C. et al. The sequence of the human genome. Science 291, 1304–1351 (2001).
Chan, K. et al. An APOBEC3A hypermutation signature is distinguishable from the signature of background mutagenesis by APOBEC3B in human cancers. Nat. Genet. 47, 1067–1072 (2015).
Roberts, S. A. et al. An APOBEC cytidine deaminase mutagenesis pattern is widespread in human cancers. Nat. Genet. 45, 970–976 (2013).
Vinagre, J. et al. Frequency of TERT promoter mutations in human cancers. Nat. Commun. 4, 2185 (2013).
Dudley, J. C. et al. Detection and surveillance of bladder cancer using urine tumor DNA. Cancer Discov. 9, 500–509 (2019). This study presents of a high-throughput screen to identify tumour DNA from a patient urine sample, with an excellent application to post-treatment surveillance.
Wu, S. et al. Whole-genome sequencing identifies ADGRG6 enhancer mutations and FRS2 duplications as angiogenesis-related drivers in bladder cancer. Nat. Commun. 10, 720 (2019).
Nickerson, M. L. et al. Concurrent alterations in TERT, KDM6A, and the BRCA pathway in bladder cancer. Clin. Cancer Res. 20, 4935–4948 (2014).
Wang, K. et al. TERT promoter mutations and TERT mRNA but not FGFR3 mutations are urinary biomarkers in Han Chinese patients with urothelial bladder cancer. Oncologist 20, 263–269 (2015).
Cheng, L. et al. Telomerase reverse transcriptase (TERT) promoter mutation analysis of benign, malignant and reactive urothelial lesions reveals a subpopulation of inverted papilloma with immortalizing genetic change. Histopathology 69, 107–113 (2016).
Pivovarcikova, K. et al. Comparative study of TERT gene mutation analysis on voided liquid-based urine cytology and paraffin-embedded tumorous tissue. Ann. Diagn. Pathol. 24, 7–10 (2016).
Pietzak, E. J. et al. Next-generation sequencing of nonmuscle invasive bladder cancer reveals potential biomarkers and rational therapeutic targets. Eur. Urol. 72, 952–959 (2017).
Isharwal, S. et al. Prognostic value of TERT alterations, mutational and copy number alterations burden in urothelial carcinoma. Eur. Urol. Focus. 5, 201–204 (2019).
Kilian, A. et al. Isolation of a candidate human telomerase catalytic subunit gene, which reveals complex splicing patterns in different cell types. Hum. Mol. Genet. 6, 2011–2019 (1997).
Borah, S. et al. Cancer. TERT promoter mutations and telomerase reactivation in urothelial cancer. Science 347, 1006–1010 (2015).
Liu, X. et al. TERT promoter mutations and their association with BRAF V600E mutation and aggressive clinicopathological characteristics of thyroid cancer. J. Clin. Endocrinol. Metab. 99, E1130–E1136 (2014).
Theodorescu, D. & Cech, T. R. Telomerase in bladder cancer: back to a better future? Eur. Urol. 65, 370–371 (2014).
Huang, D. S. et al. Recurrent TERT promoter mutations identified in a large-scale study of multiple tumour types are associated with increased TERT expression and telomerase activation. Eur. J. Cancer 51, 969–976 (2015).
Roggisch, J., Ecke, T. & Koch, S. Molecular identification of telomerase reverse transcriptase (TERT) promotor mutations in primary and recurrent tumors of invasive and noninvasive urothelial bladder cancer. Urol. Oncol. 38, 77 e17–e77 e25 (2020).
Palsgrove, D. N. et al. Targeted sequencing of plasmacytoid urothelial carcinoma reveals frequent TERT promoter mutations. Hum. Pathol. 85, 1–9 (2019).
Taylor, A. S. et al. PAX8 expression and TERT promoter mutations in the nested variant of urothelial carcinoma: a clinicopathologic study with immunohistochemical and molecular correlates. Mod. Pathol. https://doi.org/10.1038/s41379-020-0453-z (2020).
Wang, C. C., Huang, C. Y., Jhuang, Y. L., Chen, C. C. & Jeng, Y. M. Biological significance of TERT promoter mutation in papillary urothelial neoplasm of low malignant potential. Histopathology 72, 795–803 (2018).
Vail, E. et al. Telomerase reverse transcriptase promoter mutations in glandular lesions of the urinary bladder. Ann. Diagn. Pathol. 19, 301–305 (2015).
Cowan, M. et al. High prevalence of TERT promoter mutations in primary squamous cell carcinoma of the urinary bladder. Mod. Pathol. 29, 511–515 (2016).
Zheng, X. et al. High frequency of TERT promoter mutation in small cell carcinoma of bladder, but not in small cell carcinoma of other origins. J. Hematol. Oncol. 7, 47 (2014).
Roy, S. et al. Next-generation sequencing-based molecular characterization of primary urinary bladder adenocarcinoma. Mod. Pathol. 30, 1133–1143 (2017).
Kandimalla, R., van Tilborg, A. A. & Zwarthoff, E. C. DNA methylation-based biomarkers in bladder cancer. Nat. Rev. Urol. 10, 327–335 (2013).
Agger, K. et al. UTX and JMJD3 are histone H3K27 demethylases involved in HOX gene regulation and development. Nature 449, 731–734 (2007).
Kaneko, S. & Li, X. X chromosome protects against bladder cancer in females via a KDM6A-dependent epigenetic mechanism. Sci. Adv. 4, eaar5598 (2018).
Kobatake, K. et al. Kdm6a deficiency activates inflammatory pathways, promotes M2 macrophage polarization, and causes bladder cancer in cooperation with p53 dysfunction. Clin. Cancer Res. 26, 2065–2079 (2020).
Ler, L. D. et al. Loss of tumor suppressor KDM6A amplifies PRC2-regulated transcriptional repression in bladder cancer and can be targeted through inhibition of EZH2. Sci. Transl Med. https://doi.org/10.1126/scitranslmed.aai8312 (2017).
Shilatifard, A. The COMPASS family of histone H3K4 methylases: mechanisms of regulation in development and disease pathogenesis. Annu. Rev. Biochem. 81, 65–95 (2012).
Das, C., Lucia, M. S., Hansen, K. C. & Tyler, J. K. CBP/p300-mediated acetylation of histone H3 on lysine 56. Nature 459, 113–117 (2009).
Duex, J. E. et al. Functional impact of chromatin remodeling gene mutations and predictive signature for therapeutic response in bladder cancer. Mol. Cancer Res. 16, 69–77 (2018).
Shen, J. et al. ARID1A deficiency impairs the DNA damage checkpoint and sensitizes cells to PARP inhibitors. Cancer Discov. 5, 752–767 (2015).
Okamura, R. et al. ARID1A alterations function as a biomarker for longer progression-free survival after anti-PD-1/PD-L1 immunotherapy. J. Immunother. Cancer https://doi.org/10.1136/jitc-2019-000438 (2020).
Su, S. et al. CD10+GPR77+ cancer-associated fibroblasts promote cancer formation and chemoresistance by sustaining cancer stemness. Cell 172, 841–856 e816 (2018).
Ozdemir, B. C. et al. Depletion of carcinoma-associated fibroblasts and fibrosis induces immunosuppression and accelerates pancreas cancer with reduced survival. Cancer Cell 25, 719–734 (2014).
Rhim, A. D. et al. Stromal elements act to restrain, rather than support, pancreatic ductal adenocarcinoma. Cancer Cell 25, 735–747 (2014).
Costa, A. et al. Fibroblast heterogeneity and immunosuppressive environment in human breast cancer. Cancer Cell 33, 463–479 e410 (2018). CAFs are known to provide an immunosuppressive environment, and this study identifies four subsets of CAFs, while identifying the mechanism of immunosuppression in one particular subset.
Alexa, A., Baderca, F., Lighezan, R. & Izvernariu, D. Myofibroblasts reaction in urothelial carcinomas. Rom. J. Morphol. Embryol. 50, 639–643 (2009).
Mezheyeuski, A. et al. Fibroblasts in urothelial bladder cancer define stroma phenotypes that are associated with clinical outcome. Sci. Rep. 10, 281 (2020). Analysing a cohort of 344 patients with bladder cancer, this study uses five fibroblast markers to highlight the need for multiple marker analysis when one is generating a prognosis using fibroblasts.
Calvete, J. et al. The coexpression of fibroblast activation protein (FAP) and basal-type markers (CK 5/6 and CD44) predicts prognosis in high-grade invasive urothelial carcinoma of the bladder. Hum. Pathol. 91, 61–68 (2019).
Schulte, J. et al. Expression of the E-cadherin repressors Snail, Slug and Zeb1 in urothelial carcinoma of the urinary bladder: relation to stromal fibroblast activation and invasive behaviour of carcinoma cells. Histochem. Cell Biol. 138, 847–860 (2012).
Long, X. et al. Cancer-associated fibroblasts promote cisplatin resistance in bladder cancer cells by increasing IGF-1/ERbeta/Bcl-2 signalling. Cell Death Dis. 10, 375 (2019).
Tran, L. & Theodorescu, D. Determinants of resistance to checkpoint inhibitors. Int. J. Mol. Sci. 21, https://doi.org/10.3390/ijms21051594 (2020).
Martinez-Lostao, L., Anel, A. & Pardo, J. How do cytotoxic lymphocytes kill cancer cells? Clin. Cancer Res. 21, 5047–5056 (2015).
Pfannstiel, C. et al. The tumor immune microenvironment drives a prognostic relevance that correlates with bladder cancer subtypes. Cancer Immunol. Res. 7, 923–938 (2019).
Wang, L. et al. EMT- and stroma-related gene expression and resistance to PD-1 blockade in urothelial cancer. Nat. Commun. 9, 3503 (2018). This study finds that non-haematopoietic stromal cells are a major source of EMT-related gene expression and that higher EMT-related and stromal gene expression is associated with poorer response to nivolumab and shorter progression-free and overall survival.
Mariathasan, S. et al. TGFbeta attenuates tumour response to PD-L1 blockade by contributing to exclusion of T cells. Nature 554, 544–548 (2018). This study illustrates the impact that transforming growth factor-β signalling from fibroblasts and collagen-rich stromal cells has on promoting cytotoxic T cell exclusion in patients with metastatic bladder cancer.
Salmon, H. et al. Matrix architecture defines the preferential localization and migration of T cells into the stroma of human lung tumors. J. Clin. Invest. 122, 899–910 (2012).
Sweis, R. F. et al. Molecular drivers of the non-T-cell-inflamed tumor microenvironment in urothelial bladder cancer. Cancer Immunol. Res. 4, 563–568 (2016).
Henze, A. T. & Mazzone, M. The impact of hypoxia on tumor-associated macrophages. J. Clin. Invest. 126, 3672–3679 (2016).
Qiu, S. et al. Tumor-associated macrophages promote bladder tumor growth through PI3K/AKT signal induced by collagen. Cancer Sci. 110, 2110–2118 (2019).
Chen, C. et al. LNMAT1 promotes lymphatic metastasis of bladder cancer via CCL2 dependent macrophage recruitment. Nat. Commun. 9, 3826 (2018).
Jeong, H. et al. Tumor-associated macrophages enhance tumor hypoxia and aerobic glycolysis. Cancer Res. 79, 795–806 (2019).
Chen, Y. et al. Tumor-associated macrophages: an accomplice in solid tumor progression. J. Biomed. Sci. 26, 78 (2019).
Cassetta, L. et al. Human tumor-associated macrophage and monocyte transcriptional landscapes reveal cancer-specific reprogramming, biomarkers, and therapeutic targets. Cancer Cell 35, 588–602 e510 (2019).
Mantovani, A., Sica, A. & Locati, M. Macrophage polarization comes of age. Immunity 23, 344–346 (2005).
Takayama, H. et al. Increased infiltration of tumor associated macrophages is associated with poor prognosis of bladder carcinoma in situ after intravesical bacillus Calmette-Guerin instillation. J. Urol. 181, 1894–1900 (2009).
Qi, Y. et al. Tumor-associated macrophages expressing galectin-9 identify immunoevasive subtype muscle-invasive bladder cancer with poor prognosis but favorable adjuvant chemotherapeutic response. Cancer Immunol. Immunother. 68, 2067–2080 (2019).
Hu, B. et al. Blockade of DC-SIGN+ tumor-associated macrophages reactivates antitumor immunity and improves immunotherapy in muscle-invasive bladder cancer. Cancer Res. 80, 1707–1719 (2020). This study identifies of TAMs expressing a dendritic cell-specific C-type lectin which is shown to promote an anti-inflammatory environment. Neutralization of the lectin with an antibody augments pembrolizumab antitumour activity.
Bernardo, M. E. & Fibbe, W. E. Mesenchymal stromal cells: sensors and switchers of inflammation. Cell Stem Cell 13, 392–402 (2013).
Fu, C. & Jiang, A. Dendritic cells and CD8 T cell immunity in tumor microenvironment. Front. Immunol. 9, 3059 (2018).
Amodio, G. et al. Role of myeloid regulatory cells (MRCs) in maintaining tissue homeostasis and promoting tolerance in autoimmunity, inflammatory disease and transplantation. Cancer Immunol. Immunother. 68, 661–672 (2019).
Tang, M., Diao, J. & Cattral, M. S. Molecular mechanisms involved in dendritic cell dysfunction in cancer. Cell. Mol. Life Sci. 74, 761–776 (2017).
Schneider, A. K., Chevalier, M. F. & Derre, L. The multifaceted immune regulation of bladder cancer. Nat. Rev. Urol. 16, 613–630 (2019).
Chevalier, M. F. et al. Conventional and PD-L1-expressing regulatory T cells are enriched during BCG therapy and may limit its efficacy. Eur. Urol. 74, 540–544 (2018). It was discovered that BCG therapy recruits T cells but a significant portion of those are Treg cells, with significant expression of PDL1. This supports trials which look at BCG in combination with ICIs.
Mu, X. Y. et al. RS 504393 inhibits M-MDSCs recruiting in immune microenvironment of bladder cancer after gemcitabine treatment. Mol. Immunol. 109, 140–148 (2019).
Said, N., Sanchez-Carbayo, M., Smith, S. C. & Theodorescu, D. RhoGDI2 suppresses lung metastasis in mice by reducing tumor versican expression and macrophage infiltration. J. Clin. Invest. 122, 1503–1518 (2012).
Takeyama, Y. et al. Myeloid-derived suppressor cells are essential partners for immune checkpoint inhibitors in the treatment of cisplatin-resistant bladder cancer. Cancer Lett. 479, 89–99 (2020).
Ayari, C. et al. Bladder tumor infiltrating mature dendritic cells and macrophages as predictors of response to bacillus Calmette-Guerin immunotherapy. Eur. Urol. 55, 1386–1395 (2009).
Chevalier, M. F. et al. ILC2-modulated T cell-to-MDSC balance is associated with bladder cancer recurrence. J. Clin. Invest. 127, 2916–2929 (2017).
Baras, A. S. et al. The ratio of CD8 to Treg tumor-infiltrating lymphocytes is associated with response to cisplatin-based neoadjuvant chemotherapy in patients with muscle invasive urothelial carcinoma of the bladder. Oncoimmunology 5, e1134412 (2016).
Lee, H. W. et al. Single-cell RNA sequencing reveals the tumor microenvironment and facilitates strategic choices to circumvent treatment failure in a chemorefractory bladder cancer patient. Genome Med. 12, 47 (2020).
Sfakianos, J. P. et al. Epithelial plasticity can generate multi-lineage phenotypes in human and murine bladder cancers. Nat. Commun. 11, 2540 (2020).
Oh, D. Y. et al. Intratumoral CD4+ T cells mediate anti-tumor cytotoxicity in human bladder cancer. Cell 181, 1612–1625 e1613 (2020).
Wang, Y., Chang, Q. & Li, Y. Racial differences in urinary bladder cancer in the united states. Sci. Rep. 8, 12521 (2018).
Schinkel, J. K. et al. Overall and recurrence-free survival among black and white bladder cancer patients in an equal-access health system. Cancer Epidemiol. 42, 154–158 (2016).
Kaye, D. R., Canner, J. K., Kates, M., Schoenberg, M. P. & Bivalacqua, T. J. Do African American patients treated with radical cystectomy for bladder cancer have worse overall survival? Accounting for pathologic staging and patient demographics beyond race makes a difference. Bladder Cancer 2, 225–234 (2016).
Casey, M. F. et al. The impact of regionalization of cystectomy on racial disparities in bladder cancer care. J. Urol. 194, 36–41 (2015).
Danforth, K. N. et al. Disparities in stage at diagnosis in an equal-access integrated delivery system: a retrospective cohort study of 7244 patients with bladder cancer. Clin. Genitourin. Cancer 18, e91–e102 (2020).
Dobruch, J. et al. Gender and bladder cancer: a collaborative review of etiology, biology, and outcomes. Eur. Urol. 69, 300–310 (2016).
Radkiewicz, C. et al. Sex differences in urothelial bladder cancer survival. Clin. Genitourin. Cancer 18, 26–34 e26 (2020).
McGrath, M., Michaud, D. S. & De Vivo, I. Hormonal and reproductive factors and the risk of bladder cancer in women. Am. J. Epidemiol. 163, 236–244 (2006).
Daugherty, S. E. et al. Reproductive factors and menopausal hormone therapy and bladder cancer risk in the NIH-AARP diet and health study. Int. J. Cancer 133, 462–472 (2013).
Pearce, M. M. et al. The female urinary microbiome: a comparison of women with and without urgency urinary incontinence. mBio 5, e01283–e01314 (2014).
Shrestha, E. et al. Profiling the urinary microbiome in men with positive versus negative biopsies for prostate cancer. J. Urol. 199, 161–171 (2018).
Miyamoto, H. et al. Expression of androgen and oestrogen receptors and its prognostic significance in urothelial neoplasm of the urinary bladder. BJU Int. 109, 1716–1726 (2012).
Miyamoto, H. et al. Promotion of bladder cancer development and progression by androgen receptor signals. J. Natl Cancer Inst. 99, 558–568 (2007).
Hsu, I. et al. Estrogen receptor alpha prevents bladder cancer via INPP4B inhibited Akt pathway in vitro and in vivo. Oncotarget 5, 7917–7935 (2014).
Hsu, I. et al. Suppression of ERbeta signaling via ERbeta knockout or antagonist protects against bladder cancer development. Carcinogenesis 35, 651–661 (2014).
Shiota, M. et al. Secondary bladder cancer after anticancer therapy for prostate cancer: reduced comorbidity after androgen-deprivation therapy. Oncotarget 6, 14710–14719 (2015).
Izumi, K. et al. Androgen deprivation therapy prevents bladder cancer recurrence. Oncotarget 5, 12665–12674 (2014).
Shiota, M. et al. Suppressed recurrent bladder cancer after androgen suppression with androgen deprivation therapy or 5alpha-reductase inhibitor. J. Urol. 197, 308–313 (2017).
Li, P., Chen, J. & Miyamoto, H. Androgen receptor signaling in bladder cancer. Cancers 9, 20 (2017).
Ide, H. et al. Androgen receptor signaling reduces radiosensitivity in bladder cancer. Mol. Cancer Ther. 17, 1566–1574 (2018).
Batista, R. et al. Biomarkers for bladder cancer diagnosis and surveillance: a comprehensive review. Diagnostics 10, 39 (2020).
van Rhijn, B. W., van der Poel, H. G. & van der Kwast, T. H. Urine markers for bladder cancer surveillance: a systematic review. Eur. Urol. 47, 736–748 (2005).
Konety, B. R. Molecular markers in bladder cancer: a critical appraisal. Urol. Oncol. 24, 326–337 (2006).
Sidransky, D. et al. Identification of p53 gene mutations in bladder cancers and urine samples. Science 252, 706–709 (1991).
Santoni, G., Morelli, M. B., Amantini, C. & Battelli, N. Urinary markers in bladder cancer: an update. Front. Oncol. 8, 362 (2018).
Miyamoto, D. T., Mouw, K. W., Feng, F. Y., Shipley, W. U. & Efstathiou, J. A. Molecular biomarkers in bladder preservation therapy for muscle-invasive bladder cancer. Lancet Oncol. 19, e683–e695 (2018).
Botezatu, I. et al. Genetic analysis of DNA excreted in urine: a new approach for detecting specific genomic DNA sequences from cells dying in an organism. Clin. Chem. 46, 1078–1084 (2000).
Togneri, F. S. et al. Genomic complexity of urothelial bladder cancer revealed in urinary cfDNA. Eur. J. Hum. Genet. 24, 1167–1174 (2016).
Kinde, I. et al. TERT promoter mutations occur early in urothelial neoplasia and are biomarkers of early disease and disease recurrence in urine. Cancer Res. 73, 7162–7167 (2013).
Ward, D. G. et al. Multiplex PCR and next generation sequencing for the non-invasive detection of bladder cancer. PLoS ONE 11, e0149756 (2016).
Critelli, R. et al. Detection of multiple mutations in urinary exfoliated cells from male bladder cancer patients at diagnosis and during follow-up. Oncotarget 7, 67435–67448 (2016).
Scott, S. N. et al. Next-generation sequencing of urine specimens: A novel platform for genomic analysis in patients with non-muscle-invasive urothelial carcinoma treated with bacille Calmette-Guerin. Cancer Cytopathol. 125, 416–426 (2017).
Descotes, F. et al. Non-invasive prediction of recurrence in bladder cancer by detecting somatic TERT promoter mutations in urine. Br. J. Cancer 117, 583–587 (2017).
Springer, S. U. et al. Non-invasive detection of urothelial cancer through the analysis of driver gene mutations and aneuploidy. eLife 7, e32143 (2018).
Stasik, S. et al. Evaluation of TERT promoter mutations in urinary cell-free DNA and sediment DNA for detection of bladder cancer. Clin. Biochem. 64, 60–63 (2019).
Hurst, C. D., Platt, F. M. & Knowles, M. A. Comprehensive mutation analysis of the TERT promoter in bladder cancer and detection of mutations in voided urine. Eur. Urol. 65, 367–369 (2014).
Hosen, M. I. et al. Urinary TERT promoter mutations are detectable up to 10 years prior to clinical diagnosis of bladder cancer: evidence from the Golestan Cohort study. EBioMedicine 53, 102643 (2020). This study performs urinary analysis of TERT promoter mutations in 38 asymptomatic persons who later developed bladder, finding that about 50% of patients exhibited detectable TERT promoter mutations in their urine up to 10 years in advance.
Stroun, M. et al. Neoplastic characteristics of the DNA found in the plasma of cancer patients. Oncology 46, 318–322 (1989).
Leon, S. A., Shapiro, B., Sklaroff, D. M. & Yaros, M. J. Free DNA in the serum of cancer patients and the effect of therapy. Cancer Res. 37, 646–650 (1977).
Razavi, P. et al. High-intensity sequencing reveals the sources of plasma circulating cell-free DNA variants. Nat. Med. 25, 1928–1937 (2019).
Stroun, M., Anker, P., Lyautey, J., Lederrey, C. & Maurice, P. A. Isolation and characterization of DNA from the plasma of cancer patients. Eur. J. Cancer Clin. Oncol. 23, 707–712 (1987).
Wan, J. C. M. et al. Liquid biopsies come of age: towards implementation of circulating tumour DNA. Nat. Rev. Cancer 17, 223–238 (2017).
Christensen, E. et al. Early detection of metastatic relapse and monitoring of therapeutic efficacy by ultra-deep sequencing of plasma cell-free DNA in patients with urothelial bladder carcinoma. J. Clin. Oncol. 37, 1547–1557 (2019).
Birkenkamp-Demtroder, K. et al. Genomic alterations in liquid biopsies from patients with bladder cancer. Eur. Urol. 70, 75–82 (2016). This work reports molecular characterization of 12 patients with recurring bladder cancer using urine and identifies correlations between next-generation sequencing and Droplet Digital PCR.
Birkenkamp-Demtroder, K. et al. Monitoring treatment response and metastatic relapse in advanced bladder cancer by liquid biopsy analysis. Eur. Urol. 73, 535–540 (2018).
Christensen, E. et al. Optimized targeted sequencing of cell-free plasma DNA from bladder cancer patients. Sci. Rep. 8, 1917 (2018).
Chen, X. et al. Non-invasive early detection of cancer four years before conventional diagnosis using a blood test. Nat. Commun. 11, 3475 (2020).
Babjuk, M. et al. European association of urology guidelines on non-muscle-invasive bladder cancer (TaT1 and carcinoma in situ) - 2019 update. Eur. Urol. 76, 639–657 (2019).
Messing, E. M. et al. Effect of intravesical instillation of gemcitabine vs saline immediately following resection of suspected low-grade non-muscle-invasive bladder cancer on tumor recurrence: SWOG S0337 randomized clinical trial. JAMA 319, 1880–1888 (2018).
Gote, V., Sikder, S., Sicotte, J. & Pal, D. Ocular drug delivery: present innovations and future challenges. J. Pharmacol. Exp. Ther. 370, 602–624 (2019).
US National Library of Medicine. ClinicalTrials.gov, https://clinicaltrials.gov/ct2/show/NCT02720367 (2016).
US National Library of Medicine. ClinicalTrials.gov, https://clinicaltrials.gov/ct2/show/NCT03404791 (2018).
US National Library of Medicine. ClinicalTrials.gov, https://clinicaltrials.gov/ct2/show/NCT02307487 (2014).
US National Library of Medicine. ClinicalTrials.gov, https://clinicaltrials.gov/ct2/show/NCT03558503 (2018).
FDA. FDA approves first therapy for treatment of low-grade upper tract urothelial cancer. https://www.fda.gov/news-events/press-announcements/fda-approves-first-therapy-treatment-low-grade-upper-tract-urothelial-cancer (2020).
McKiernan, J. M. et al. Phase II trial of intravesical nanoparticle albumin bound paclitaxel for the treatment of nonmuscle invasive urothelial carcinoma of the bladder after bacillus Calmette-Guerin treatment failure. J. Urol. 192, 1633–1638 (2014).
Seager, C. M. et al. Intravesical delivery of rapamycin suppresses tumorigenesis in a mouse model of progressive bladder cancer. Cancer Prev. Res. 2, 1008–1014 (2009).
Tamura, K. et al. Therapeutic effect of intravesical administration of paclitaxel solubilized with poly(2-methacryloyloxyethyl phosphorylcholine-co-n-butyl methacrylate) in an orthotopic bladder cancer model. BMC Cancer 15, 317 (2015).
US National Library of Medicine. ClinicalTrials.gov, https://clinicaltrials.gov/ct2/show/NCT03053635 (2017).
Monro, S. et al. Transition metal complexes and photodynamic therapy from a tumor-centered approach: challenges, opportunities, and highlights from the development of TLD1433. Chem. Rev. 119, 797–828 (2019).
US National Library of Medicine. ClinicalTrials.gov, https://clinicaltrials.gov/ct2/show/NCT03945162 (2019).
Sylvester, R. J., van der, M. A. & Lamm, D. L. Intravesical bacillus Calmette-Guerin reduces the risk of progression in patients with superficial bladder cancer: a meta-analysis of the published results of randomized clinical trials. J. Urol. 168, 1964–1970 (2002).
Lamm, D. L. et al. Maintenance bacillus Calmette-Guerin immunotherapy for recurrent TA, T1 and carcinoma in situ transitional cell carcinoma of the bladder: a randomized Southwest oncology group study. J. Urol. 163, 1124–1129 (2000).
Peyton, C. C. et al. Updates on the use of intravesical therapies for non-muscle invasive bladder cancer: how, when and what. World J. Urol. 37, 2017–2029 (2019).
Saluja, M. & Gilling, P. Intravesical bacillus Calmette-Guerin instillation in non-muscle-invasive bladder cancer: a review. Int. J. Urol. 25, 18–24 (2018).
Gupta, M., Kates, M. & Bivalacqua, T. J. Immunotherapy in nonmuscle invasive bladder cancer: current and emerging treatments. Curr. Opin. Oncol. 31, 183–187 (2019).
Shore, N. D. et al. Intravesical rAd-IFNalpha/Syn3 for patients with high-grade, bacillus Calmette-Guerin-refractory or relapsed non-muscle-invasive bladder cancer: a phase II randomized study. J. Clin. Oncol. 35, 3410–3416 (2017).
Steinberg, R. L., Nepple, K. G., Velaer, K. N., Thomas, L. J. & O’Donnell, M. A. Quadruple immunotherapy of bacillus Calmette-Guerin, interferon, interleukin-2, and granulocyte-macrophage colony-stimulating factor as salvage therapy for non-muscle-invasive bladder cancer. Urol. Oncol. 35, 670 e677–670 e614 (2017).
Bellmunt, J. et al. Pembrolizumab as second-line therapy for advanced urothelial carcinoma. N. Engl. J. Med. 376, 1015–1026 (2017).
FDA. FDA approves pembrolizumab for BCG-unresponsive, high-risk non-muscle invasive bladder cancer. https://www.fda.gov/drugs/resources-information-approved-drugs/fda-approves-pembrolizumab-bcg-unresponsive-high-risk-non-muscle-invasive-bladder-cancer (2020).
US National Library of Medicine. ClinicalTrials.gov, https://clinicaltrials.gov/ct2/show/NCT02625961 (2015).
US National Library of Medicine. ClinicalTrials.gov, https://clinicaltrials.gov/ct2/show/NCT03171493 (2017).
US National Library of Medicine. ClinicalTrials.gov, https://clinicaltrials.gov/ct2/show/NCT04089163 (2019).
US National Library of Medicine. ClinicalTrials.gov, https://clinicaltrials.gov/ct2/show/NCT02773849 (2016).
US National Library of Medicine. ClinicalTrials.gov, https://clinicaltrials.gov/ct2/show/NCT03421236 (2018).
US National Library of Medicine. ClinicalTrials.gov, https://clinicaltrials.gov/ct2/show/NCT03552796 (2018).
US National Library of Medicine. ClinicalTrials.gov, https://clinicaltrials.gov/ct2/show/NCT03022825 (2017).
US National Library of Medicine. ClinicalTrials.gov, https://clinicaltrials.gov/ct2/show/NCT03719300 (2018).
Nadal, R. & Bellmunt, J. Management of metastatic bladder cancer. Cancer Treat. Rev. 76, 10–21 (2019).
Hermans, T. J. N. et al. Neoadjuvant treatment for muscle-invasive bladder cancer: the past, the present, and the future. Urol. Oncol. 36, 413–422 (2018).
Tse, J., Ghandour, R., Singla, N. & Lotan, Y. Molecular predictors of complete response following neoadjuvant chemotherapy in urothelial carcinoma of the bladder and upper tracts. Int. J. Mol. Sci. 20, 793 (2019).
Dancik, G. M. & Theodorescu, D. Pharmacogenomics in bladder cancer. Urol. Oncol. 32, 16–22 (2014).
Howell, S. B., Safaei, R., Larson, C. A. & Sailor, M. J. Copper transporters and the cellular pharmacology of the platinum-containing cancer drugs. Mol. Pharmacol. 77, 887–894 (2010).
Kilari, D. et al. Copper transporter-CTR1 expression and pathological outcomes in platinum-treated muscle-invasive bladder cancer patients. Anticancer Res. 36, 495–501 (2016).
Bellmunt, J. et al. Gene expression of ERCC1 as a novel prognostic marker in advanced bladder cancer patients receiving cisplatin-based chemotherapy. Ann. Oncol. 18, 522–528 (2007).
Font, A. et al. BRCA1 mRNA expression and outcome to neoadjuvant cisplatin-based chemotherapy in bladder cancer. Ann. Oncol. 22, 139–144 (2011).
Teo, M. Y. et al. DNA damage response and repair gene alterations are associated with improved survival in patients with platinum-treated advanced urothelial carcinoma. Clin. Cancer Res. 23, 3610–3618 (2017).
Kim, J. et al. Somatic ERCC2 mutations are associated with a distinct genomic signature in urothelial tumors. Nat. Genet. 48, 600–606 (2016).
US National Library of Medicine. ClinicalTrials.gov, https://clinicaltrials.gov/ct2/show/NCT02788201 (2016).
US National Library of Medicine. ClinicalTrials.gov, https://clinicaltrials.gov/ct2/show/NCT02177695 (2014).
Goldberg, H. ASCO 2019: SWOG S1314: a randomized phase II study of co-expression extrapolation with neoadjuvant chemotherapy for localized, muscle-invasive bladder cancer. https://www.urotoday.com/conference-highlights/asco-2019-annual-meeting/asco-2019-bladder-cancer/113039-asco-2019-swog-s1314-a-randomized-phase-ii-study-of-co-expression-extrapolation-with-neoadjuvant-chemotherapy-for-localized-muscle-invasive-bladder-cancer.html (2019).
Gallagher, D. J. et al. Germline single nucleotide polymorphisms associated with response of urothelial carcinoma to platinum-based therapy: the role of the host. Ann. Oncol. 24, 2414–2421 (2013).
Lim, Y. W. et al. Germline genetic polymorphisms influence tumor gene expression and immune cell infiltration. Proc. Natl Acad. Sci. USA 115, E11701–E11710 (2018).
di Martino, E., Tomlinson, D. C., Williams, S. V. & Knowles, M. A. A place for precision medicine in bladder cancer: targeting the FGFRs. Future Oncol. 12, 2243–2263 (2016).
FDA. FDA approves first targeted therapy for metastatic bladder cancer. https://www.fda.gov/news-events/press-announcements/fda-approves-first-targeted-therapy-metastatic-bladder-cancer (2019).
Javle, M. et al. Phase II study of BGJ398 in patients with FGFR-altered advanced cholangiocarcinoma. J. Clin. Oncol. 36, 276–282 (2018).
US National Library of Medicine. ClinicalTrials.gov, https://clinicaltrials.gov/ct2/show/NCT02657486 (2016).
US National Library of Medicine. ClinicalTrials.gov, https://clinicaltrials.gov/ct2/show/NCT04197986 (2019).
Slater, H. FDA Grants Breakthrough Therapy Designation to Enfortumab Vedotin. Cancernetwork.com. https://www.cancernetwork.com/view/fda-grants-breakthrough-therapy-designation-enfortumab-vedotin (2020)
US National Library of Medicine. ClinicalTrials.gov, https://clinicaltrials.gov/ct2/show/NCT03219333 (2017).
Samstein, R. M. et al. Tumor mutational load predicts survival after immunotherapy across multiple cancer types. Nat. Genet. 51, 202–206 (2019).
Cristescu, R. et al. Pan-tumor genomic biomarkers for PD-1 checkpoint blockade-based immunotherapy. Science 362, eaar3593 (2018).
Goodman, A. M. et al. Tumor mutational burden as an independent predictor of response to immunotherapy in diverse cancers. Mol. Cancer Ther. 16, 2598–2608 (2017).
Hodi, F. S. et al. Improved survival with ipilimumab in patients with metastatic melanoma. N. Engl. J. Med. 363, 711–723 (2010).
Borghaei, H. et al. Nivolumab versus docetaxel in advanced nonsquamous non-small-cell lung cancer. N. Engl. J. Med. 373, 1627–1639 (2015).
Herbst, R. S. et al. Pembrolizumab versus docetaxel for previously treated, PD-L1-positive, advanced non-small-cell lung cancer (KEYNOTE-010): a randomised controlled trial. Lancet 387, 1540–1550 (2016).
Fehrenbacher, L. et al. Atezolizumab versus docetaxel for patients with previously treated non-small-cell lung cancer (POPLAR): a multicentre, open-label, phase 2 randomised controlled trial. Lancet 387, 1837–1846 (2016).
US National Library of Medicine. ClinicalTrials.gov, https://clinicaltrials.gov/ct2/show/NCT02807636 (2016).
Suzman, D. L. et al. FDA approval summary: atezolizumab or pembrolizumab for the treatment of patients with advanced urothelial carcinoma ineligible for cisplatin-containing chemotherapy. Oncologist 24, 563–569 (2019).
Grivas, P. et al. Immune checkpoint inhibitors as switch or continuation maintenance therapy in solid tumors: rationale and current state. Target. Oncol. 14, 505–525 (2019).
US National Library of Medicine. ClinicalTrials.gov, https://clinicaltrials.gov/ct2/show/NCT03390595 (2018).
US National Library of Medicine. ClinicalTrials.gov, https://clinicaltrials.gov/ct2/show/NCT02603432 (2015).
FDA. FDA approves avelumab for urothelial carcinoma maintenance treatment. https://www.fda.gov/drugs/drug-approvals-and-databases/fda-approves-avelumab-urothelial-carcinoma-maintenance-treatment (2020)
Tu, M. M. et al. Targeting DDR2 enhances tumor response to anti-PD-1 immunotherapy. Sci. Adv. 5, eaav2437 (2019). This study uses functional genomics to find rational and effective therapeutic combinations of small molecules with checkpoint inhibitors in bladder and other cancer types.
Moad, M. et al. A novel model of urinary tract differentiation, tissue regeneration, and disease: reprogramming human prostate and bladder cells into induced pluripotent stem cells. Eur. Urol. 64, 753–761 (2013).
Pauli, C. et al. Personalized in vitro and in vivo cancer models to guide precision medicine. Cancer Discov. 7, 462–477 (2017).
Lee, S. H. et al. Tumor evolution and drug response in patient-derived organoid models of bladder cancer. Cell 173, 515–528 e517 (2018).
Puzio-Kuter, A. M. et al. Inactivation of p53 and Pten promotes invasive bladder cancer. Genes Dev. 23, 675–680 (2009).
Theodorescu, D., Cornil, I., Fernandez, B. J. & Kerbel, R. S. Overexpression of normal and mutated forms of HRAS induces orthotopic bladder invasion in a human transitional cell carcinoma. Proc. Natl Acad. Sci. USA 87, 9047–9051 (1990).
Overdevest, J. B. et al. CD24 expression is important in male urothelial tumorigenesis and metastasis in mice and is androgen regulated. Proc. Natl Acad. Sci. USA 109, E3588–E3596 (2012).
Sottnik, J. L. et al. Elucidating the role of Agl in bladder carcinogenesis by generation and characterization of genetically engineered mice. Carcinogenesis 40, 194–201 (2019).
Zuiverloon, T. C. M., de Jong, F. C., Costello, J. C. & Theodorescu, D. Systematic review: characteristics and preclinical uses of bladder cancer cell lines. Bladder Cancer 4, 169–183 (2018).
Avogbe, P. H. et al. Urinary TERT promoter mutations as non-invasive biomarkers for the comprehensive detection of urothelial cancer. EBioMedicine 44, 431–438 (2019).
Russo, I. J. et al. Toward personalised liquid biopsies for urothelial carcinoma: characterisation of ddPCR and urinary cfDNA for the detection of the TERT 228G>A/T mutation. Bladder Cancer 4, 41–48 (2018).
Hayashi, Y. et al. Diagnostic potential of TERT promoter and FGFR3 mutations in urinary cell-free DNA in upper tract urothelial carcinoma. Cancer Sci. 110, 1771–1779 (2019).
Eich, M. L. et al. Incidence and distribution of UroSEEK gene panel in a multi-institutional cohort of bladder urothelial carcinoma. Mod. Pathol. 32, 1544–1550 (2019).
Ward, D. G. et al. Targeted deep sequencing of urothelial bladder cancers and associated urinary DNA: a 23-gene panel with utility for non-invasive diagnosis and risk stratification. BJU Int. 124, 532–544 (2019).
Cheng, T. H. T. et al. Noninvasive detection of bladder cancer by shallow-depth genome-wide bisulfite sequencing of urinary cell-free DNA for methylation and copy number profiling. Clin. Chem. 65, 927–936 (2019).
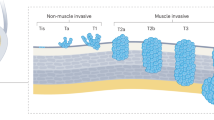
Kandori, S., Kojima, T. & Nishiyama, H. The updated points of TNM classification of urological cancers in the 8th edition of AJCC and UICC. Jpn. J. Clin. Oncol. 49, 421–425 (2019).
Hoadley, K. A. et al. Cell-of-origin patterns dominate the molecular classification of 10,000 tumors from 33 types of cancer. Cell 173, 291–304 e296 (2018).
Choudhury, N. J. et al. Afatinib activity in platinum-refractory metastatic urothelial carcinoma in patients with ERBB alterations. J. Clin. Oncol. 34, 2165–2171 (2016).
US National Library of Medicine. ClinicalTrials.gov, https://clinicaltrials.gov/ct2/show/NCT02872714 (2016).
US National Library of Medicine. ClinicalTrials.gov, https://clinicaltrials.gov/ct2/show/NCT02710734 (2016).
US National Library of Medicine. ClinicalTrials.gov, https://clinicaltrials.gov/ct2/show/NCT00030615 (2003).
US National Library of Medicine. ClinicalTrials.gov, https://clinicaltrials.gov/ct2/show/NCT03179943 (2017).
US National Library of Medicine. ClinicalTrials.gov, https://clinicaltrials.gov/ct2/show/NCT02546661 (2016).
Lloyd-Price, J., Abu-Ali, G. & Huttenhower, C. The healthy human microbiome. Genome Med. 8, 51 (2016).
Garrett, W. S. Cancer and the microbiota. Science 348, 80–86 (2015).
Wolfe, A. J. et al. Evidence of uncultivated bacteria in the adult female bladder. J. Clin. Microbiol. 50, 1376–1383 (2012).
Burger, M. et al. Epidemiology and risk factors of urothelial bladder cancer. Eur. Urol. 63, 234–241 (2013).
Zaghloul, M. S. Bladder cancer and schistosomiasis. J. Egypt. Natl Canc. Inst. 24, 151–159 (2012).
Adebayo, A. S. et al. The microbiome in urogenital schistosomiasis and induced bladder pathologies. PLoS Negl. Trop. Dis. 11, e0005826 (2017).
Xu, W. et al. Mini-review: perspective of the microbiome in the pathogenesis of urothelial carcinoma. Am. J. Clin. Exp. Urol. 2, 57–61 (2014).
Bucevic Popovic, V. et al. The urinary microbiome associated with bladder cancer. Sci. Rep. 8, 12157 (2018). This study compares patients with bladder cancer and 11 healthy individuals and identifies unique urinary microbiota signatures as a potential means of prognosis and surveillance.
Wu, P. et al. Profiling the urinary microbiota in male patients with bladder cancer in China. Front. Cell Infect. Microbiol. 8, 167 (2018).
Liu, F. et al. Dysbiosis signatures of the microbial profile in tissue from bladder cancer. Cancer Med. 8, 6904–6914 (2019).
Routy, B. et al. Gut microbiome influences efficacy of PD-1-based immunotherapy against epithelial tumors. Science 359, 91–97 (2018). This study highlights the negative impact antibiotics may have on immune checkpoint blockade and illuminates the potential that faecal microbiota transplantation may have in promoting patient response to immunotherapy.
Naito, S. et al. Prevention of recurrence with epirubicin and lactobacillus casei after transurethral resection of bladder cancer. J. Urol. 179, 485–490 (2008).
Acknowledgements
This work was supported in part by NIH grants CA075115 and CA143971 to D.T.
Author information
Authors and Affiliations
Contributions
L.T., J-F.X., N.A. and J.E.D. contributed to researching data for and writing the article. J.E.D. also substantially contributed to discussion of the content. D.T. contributed to all aspects of the article.
Corresponding author
Ethics declarations
Competing interests
D.T. is on the scientific advisory board for Urogen. J.E.D. receives compensation from Invitae. The other authors declare no competing interests.
Additional information
Peer review information
Nature Reviews Cancer thanks L. Derre, L. Dyrskjøt and C. L. Mendelsohn for their contribution to the peer review of this work.
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Related links
CBioportal: https://www.cbioportal.org/
NCI Patient-Derived Models Repository (NCI at Frederick, Frederick National Laboratory for Cancer Research, Frederick, MD, USA): https://pdmr.cancer.gov/
Supplementary information
Glossary
- Cystoscopy
-
A process whereby an imaging device is inserted into a patient’s urethra for the purpose of imaging the urethra and bladder lining to look for abnormalities.
- Uroplakins
-
Protein complexes normally expressed on the surface of luminal cells of the bladder and that are an indicator of terminal differentiation. Loss of uroplakin III expression is therefore indicative of disease progression and is correlated with poor prognosis.
- Regulons
-
Groups of genes regulated as a unit and controlled by the same regulatory gene that expresses a protein acting as a repressor or activator.
- Gene promoter
-
Sequence of DNA to which RNA polymerase and transcription factors bind to initiate RNA synthesis of a gene.
- Telomere
-
Cap made of a repetitive nucleotide sequence at the ends of a chromosome to protect it from deterioration.
- Plasmacytoid variant
-
Infiltrating urothelial carcinoma that is characterized by tumour cells that have a striking morphologic resemblance to and immunohistochemical overlap with plasma cells, and that harbours a CDH1 mutation.
- Nested variant
-
A rare neoplasm that is histologically characterized by large numbers of small, closely packed, haphazardly arranged nests of urothelial cells infiltrating the lamina propria and the muscularis propria.
- Papillary urothelial carcinomas
-
Tumours with thin, finger-like growths that start in the bladder lining and extend into the centre of the bladder.
- Glandular lesions
-
An intriguing group of clinically and morphologically diverse neoplasms, encompassing benign processes to malignant growths.
- Inverted papillomas
-
Rare yet benign neoplasms that is are moderate significance due to their similarity to inverted urothelial carcinoma, which has a much more aggressive prognosis.
- Complex of proteins associated with Set1
-
(COMPASS). Methyltransferase protein complex that controls gene transcription by specifically methylating histone H3 on the lysine at position 4 of the protein.
- Immune checkpoint inhibitors
-
(ICIs). A class of therapies (antibodies) that reactivate dormant or exhausted cytotoxic T cells.
- Intravesical instillations
-
Administration of therapeutics directly to the bladder through a soft catheter inserted through the urethra.
- Bacillus Calmette–Guérin
-
(BCG). A live attenuated strain of Mycobacterium bovis. Used as a vaccine against tuberculosis (first given to patients in 1921). Since 1977, it has been used as an immunotherapeutic agent in patients with bladder cancer.
- Radical cystectomy
-
Complete removal of the bladder in cases of advanced muscle-invasive bladder cancer with the aim of removing bladder cancer entirely from the patient.
- Androgen deprivation therapy
-
A clinical approach to inhibit signalling of the hormone androgen, either by chemical or surgical castration, with the goal of preventing androgen-dependent cancer cells from growing.
- 5α-Reductase
-
Enzyme that catalyses conversion of testosterone to dihydrotestosterone.
- Hydroxyflutamide
-
An active metabolite of flutamide used as an androgen antagonist.
- Urine cytology
-
A process whereby cells from a patient’s urine are collected and analysed under a microscope to look for cellular abnormalities such as those found in bladder cancer.
- Metastatic relapse
-
Relapse of cancer after treatment with the cancer spreading to distant organs.
- Transurethral resection of the bladder
-
A surgical technique used to harvest tissue samples for pathology analysis and remove non-muscle-invasive bladder cancer tumours.
- Photodynamic therapy
-
A therapy involving localized activation of photosensitive molecules that are selectively taken up by cancer cells, reducing toxicity to normal cells.
Rights and permissions
About this article
Cite this article
Tran, L., Xiao, JF., Agarwal, N. et al. Advances in bladder cancer biology and therapy. Nat Rev Cancer 21, 104–121 (2021). https://doi.org/10.1038/s41568-020-00313-1
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41568-020-00313-1
This article is cited by
-
Single-cell sequencing reveals the heterogeneity of B cells and tertiary lymphoid structures in muscle-invasive bladder cancer
Journal of Translational Medicine (2024)
-
Identification of clinical prognostic factors and analysis of ferroptosis-related gene signatures in the bladder cancer immune microenvironment
BMC Urology (2024)
-
CRISPR-based gene expression platform for precise regulation of bladder cancer
Cellular & Molecular Biology Letters (2024)
-
IGF2BP3 prevent HMGB1 mRNA decay in bladder cancer and development
Cellular & Molecular Biology Letters (2024)
-
Artificial intelligence assisted patient blood and urine droplet pattern analysis for non-invasive and accurate diagnosis of bladder cancer
Scientific Reports (2024)