Abstract
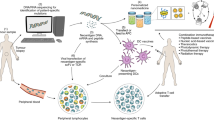
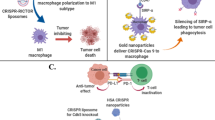
The 2018 Nobel Prize in Physiology or Medicine was awarded to pioneers in the field of cancer immunotherapy, as the utility of leveraging a patient’s coordinated and adaptive immune system to fight the patient’s unique tumour has now been validated robustly in the clinic. Still, the proportion of patients who respond to immunotherapy remains modest (~15% objective response rate across indications), as tumours have multiple means of immune evasion. The immune system is spatiotemporally controlled, so therapies that influence the immune system should be spatiotemporally controlled as well, in order to maximize the therapeutic index. Nanoparticles and biomaterials enable one to program the location, pharmacokinetics and co-delivery of immunomodulatory compounds, eliciting responses that cannot be achieved upon administration of such compounds in solution. The convergence of cancer immunotherapy, nanotechnology, bioengineering and drug delivery is opportune, as each of these fields has matured independently to the point that it can now be used to complement the others substantively and rationally, rather than modestly and empirically. As a result, unmet needs increasingly can be addressed with deductive intention. This Review explores how nanotechnology and related approaches are being applied to augmenting both endogenous leukocytes and adoptively transferred ones by informing specificity, influencing localization and improving function.
This is a preview of subscription content, access via your institution
Access options
Access Nature and 54 other Nature Portfolio journals
Get Nature+, our best-value online-access subscription
$29.99 / 30 days
cancel any time
Subscribe to this journal
Receive 12 print issues and online access
$209.00 per year
only $17.42 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout





Similar content being viewed by others
References
Khalil, D. N., Smith, E. L., Brentjens, R. J. & Wolchok, J. D. The future of cancer treatment: immunomodulation, CARs and combination immunotherapy. Nat. Rev. Clin. Oncol. 13, 273–290 (2016).
Motzer, R. J. et al. Nivolumab plus ipilimumab versus sunitinib in advanced renal-cell carcinoma. N. Engl. J. Med. 378, 1277–1290 (2018).
Reck, M. et al. Pembrolizumab versus chemotherapy for PD-L1-positive non-small-cell lung cancer. N. Engl. J. Med. 375, 1823–1833 (2016).
Binnewies, M. et al. Understanding the tumor immune microenvironment (TIME) for effective therapy. Nat. Med. 24, 541–550 (2018).
Yarchoan, M., Hopkins, A. & Jaffee, E. M. Tumor mutational burden and response rate to PD-1 inhibition. N. Engl. J. Med. 377, 2500–2501 (2017).
Sharma, P., Hu-Lieskovan, S., Wargo, J. A. & Ribas, A. Primary, adaptive, and acquired resistance to cancer immunotherapy. Cell 168, 707–723 (2017).
Jeanbart, L. & Swartz, M. A. Engineering opportunities in cancer immunotherapy. Proc. Natl Acad. Sci. USA 112, 14467–14472 (2015).
Riley, R. S., June, C. H., Langer, R. & Mitchell, M. J. Delivery technologies for cancer immunotherapy. Nat. Rev. Drug Discov. 18, 175–196 (2019).
Mitchell, M. J., Jain, R. K. & Langer, R. Engineering and physical sciences in oncology: challenges and opportunities. Nat. Rev. Cancer. 17, 659–675 (2017).
Winer, A., Bodor, J. N. & Borghaei, H. Identifying and managing the adverse effects of immune checkpoint blockade. J. Thorac. Dis. 10, S480–S489 (2018).
Dellacherie, M. O., Seo, B. R. & Mooney, D. J. Macroscale biomaterials strategies for local immunomodulation. Nat. Rev. Mater. (in the press).
Milling, L., Zhang, Y. & Irvine, D. J. Delivering safer immunotherapies for cancer. Adv. Drug Deliv. Rev. 114, 79–101 (2017).
Kwong, B., Liu, H. & Irvine, D. J. Induction of potent anti-tumor responses while eliminating systemic side effects via liposome-anchored combinatorial immunotherapy. Biomaterials 32, 5134–5147 (2011).
Pfreundschuh, M. G. et al. Phase I study of intratumoral application of recombinant human tumor necrosis factor. Eur. J. Cancer Clin. Oncol. 25, 379–388 (1989).
van Herpen, C. M. et al. Intratumoral rhIL-12 administration in head and neck squamous cell carcinoma patients induces B cell activation. Int. J. Cancer 123, 2354–2361 (2008).
Bartsch, H. H., Pfizenmaier, K., Schroeder, M. & Nagel, G. A. Intralesional application of recombinant human tumor necrosis factor alpha induces local tumor regression in patients with advanced malignancies. Eur. J. Cancer Clin. Oncol. 25, 287–291 (1989).
Ishihara, J. et al. Matrix-binding checkpoint immunotherapies enhance antitumor efficacy and reduce adverse events. Sci. Transl. Med. 9, eaan0401 (2017).
Kwong, B., Gai, S. A., Elkhader, J., Wittrup, K. D. & Irvine, D. J. Localized immunotherapy via liposome-anchored Anti-CD137+ IL-2 prevents lethal toxicity and elicits local and systemic antitumor immunity. Cancer Res. 73, 1547–1558 (2013).
Zhang, Y., Li, N., Suh, H. & Irvine, D. J. Nanoparticle anchoring targets immune agonists to tumors enabling anti-cancer immunity without systemic toxicity. Nat. Commun. 9, 6 (2018).
Ishihara, J. et al. Targeted antibody and cytokine cancer immunotherapies through collagen affinity. Sci. Transl. Med. 11, eaau3259 (2019). This study illustrates that conjugation or fusion of a collagen-binding domain to biologics promotes their accumulation in tumours, improving the therapeutic index of systemically administered immunotherapy.
Bobisse, S. et al. Sensitive and frequent identification of high avidity neo-epitope specific CD8+ T cells in immunotherapy-naive ovarian cancer. Nat. Commun. 9, 1092 (2018).
Tran, E. et al. Cancer immunotherapy based on mutation-specific CD4+ T cells in a patient with epithelial cancer. Science 344, 641–645 (2014).
Robbins, P. F. et al. A pilot trial using lymphocytes genetically engineered with an NY-ESO-1-reactive T-cell receptor: long-term follow-up and correlates with response. Clin. Cancer Res. 21, 1019–1027 (2015).
Maude, S. L. et al. Tisagenlecleucel in children and young adults with B-cell lymphoblastic leukemia. N. Engl. J. Med. 378, 439–448 (2018).
Neelapu, S. S. et al. Axicabtagene ciloleucel CAR T-cell therapy in refractory large B-cell lymphoma. N. Engl. J. Med. 377, 2531–2544 (2017).
Schuster, S. J. et al. Chimeric antigen receptor t cells in refractory b-cell lymphomas. N. Engl. J. Med. 377, 2545–2554 (2017).
Hollyman, D. et al. Manufacturing validation of biologically functional T cells targeted to CD19 antigen for autologous adoptive cell therapy. J. Immunother. 32, 169–180 (2009).
Huang, X. et al. Sleeping beauty transposon-mediated engineering of human primary T cells for therapy of CD19+ lymphoid malignancies. Mol. Ther. 16, 580–589 (2008).
Perica, K. et al. Magnetic field-induced T cell receptor clustering by nanoparticles enhances T cell activation and stimulates antitumor activity. ACS Nano 8, 2252–2260 (2014).
Perica, K. et al. Enrichment and expansion with nanoscale artificial antigen presenting cells for adoptive immunotherapy. ACS Nano 9, 6861–6871 (2015).
Hickey, J. W. et al. Efficient magnetic enrichment of antigen-specific T cells by engineering particle properties. Biomaterials 187, 105–116 (2018). This study demonstrates the importance of optimizing particle size, concentration, ligand and ligand density for maximal enrichment, activation and expansion of antigen-specific T cells.
Sunshine, J. C., Perica, K., Schneck, J. P. & Green, J. J. Particle shape dependence of CD8+ T cell activation by artificial antigen presenting cells. Biomaterials 35, 269–277 (2014).
Hickey, J. W., Vicente, F. P., Howard, G. P., Mao, H. Q. & Schneck, J. P. Biologically inspired design of nanoparticle artificial antigen-presenting cells for immunomodulation. Nano Lett. 17, 7045–7054 (2017).
Kosmides, A. K., Necochea, K., Hickey, J. W. & Schneck, J. P. Separating T cell targeting components onto magnetically clustered nanoparticles boosts activation. Nano Lett. 18, 1916–1924 (2018).
Ben-Akiva, E., Meyer, R. A., Wilson, D. R. & Green, J. J. Surface engineering for lymphocyte programming. Adv. Drug Deliv. Rev. 114, 102–115 (2017).
Siefert, A. L., Fahmy, T. M. & Kim, D. Artificial antigen-presenting cells for immunotherapies. Methods Mol. Biol. 1530, 343–353 (2017).
Fadel, T. R. et al. Adsorption of multimeric T cell antigens on carbon nanotubes: effect on protein structure and antigen-specific T cell stimulation. Small 9, 666–672 (2013).
Fadel, T. R. et al. A carbon nanotube-polymer composite for T-cell therapy. Nat. Nanotechnol. 9, 639–647 (2014).
Cheung, A. S., Zhang, D. K. Y., Koshy, S. T. & Mooney, D. J. Scaffolds that mimic antigen-presenting cells enable ex vivo expansion of primary T cells. Nat. Biotechnol. 36, 160–169 (2018).
Stephan, M. T., Moon, J. J., Um, S. H., Bershteyn, A. & Irvine, D. J. Therapeutic cell engineering with surface-conjugated synthetic nanoparticles. Nat. Med. 16, 1035–1041 (2010).
Stephan, M. T., Stephan, S. B., Bak, P., Chen, J. & Irvine, D. J. Synapse-directed delivery of immunomodulators using T-cell-conjugated nanoparticles. Biomaterials 33, 5776–5787 (2012).
Huang, B. et al. Active targeting of chemotherapy to disseminated tumors using nanoparticle-carrying Tcells. Sci. Transl. Med. 7, 291ra294 (2015).
Hinrichs, C. S. & Rosenberg, S. A. Exploiting the curative potential of adoptive T-cell therapy for cancer. Immunol. Rev. 257, 56–71 (2014).
Wing, A. et al. Improving CART-cell therapy of solid tumors with oncolytic virus-driven production of a bispecific T-cell engager. Cancer Immunol. Res. 6, 605–616 (2018).
Rosenberg, S. A. & Restifo, N. P. Adoptive cell transfer as personalized immunotherapy for human cancer. Science 348, 62–68 (2015).
Sommer, C. et al. Preclinical evaluation of allogeneic CAR T cells targeting BCMA for the treatment of multiple myeloma. Mol. Ther. 27, 1126–1138 (2019).
MacLeod, D. T. et al. Integration of a CD19 CAR into the TCR alpha chain locus streamlines production of allogeneic gene-edited CAR T cells. Mol. Ther. 25, 949–961 (2017).
Lim, W. A. & June, C. H. The principles of engineering immune cells to treat cancer. Cell 168, 724–740 (2017).
Beatty, G. L. et al. Activity of mesothelin-specific chimeric antigen receptor T cells against pancreatic carcinoma metastases in a phase 1 trial. Gastroenterology 155, 29–32 (2018).
Sackstein, R., Schatton, T. & Barthel, S. R. T-lymphocyte homing: an underappreciated yet critical hurdle for successful cancer immunotherapy. Lab Invest. 97, 669–697 (2017).
Vodnala, S. K. et al. T cell stemness and dysfunction in tumors are triggered by a common mechanism. Science 363, eaau0135 (2019).
Smith, T. T. et al. In situ programming of leukaemia-specific T cells using synthetic DNA nanocarriers. Nat. Nanotechnol. 12, 813–820 (2017). This study shows that circulating T cells can be transfected in vivo to express a CAR transgene and thereby target and kill leukaemic cells, affording an off-the-shelf alternative to adoptive cell transfer.
Schmid, D. et al. T cell-targeting nanoparticles focus delivery of immunotherapy to improve antitumor immunity. Nat Commun. 8, 1747 (2017).
Wilhelm, S. et al. Analysis of nanoparticle delivery to tumours. Nat. Rev. Mater. 1, 16014 (2016).
Gajewski, T. F. The next hurdle in cancer immunotherapy: overcoming the non-T-cell-inflamed tumor microenvironment. Semin. Oncol. 42, 663–671 (2015).
Ribas, A. et al. Oncolytic virotherapy promotes intratumoral T cell infiltration and improves anti-PD-1 immunotherapy. Cell 170, 1109–1119 (2018).
Gros, A. et al. Prospective identification of neoantigen-specific lymphocytes in the peripheral blood of melanoma patients. Nat. Med. 22, 433–438 (2016).
Gros, A. et al. PD-1 identifies the patient-specific CD8+ tumor-reactive repertoire infiltrating human tumors. J. Clin. Invest. 124, 2246–2259 (2014).
Amoozgar, Z. & Goldberg, M. S. Targeting myeloid cells using nanoparticles to improve cancer immunotherapy. Adv. Drug Deliv. Rev. 91, 38–51 (2015).
C., N., Gustafson, H. H. & Pun, S. H. Progress in tumor-associated macrophage (TAM)-targeted therapeutics. Adv. Drug Deliv. Rev. 114, 206–221 (2017).
Rodell, C. B. et al. TLR7/8-agonist-loaded nanoparticles promote the polarization of tumour-associated macrophages to enhance cancer immunotherapy. Nat. Biomed. Eng. 2, 578–588 (2018).
Crusz, S. M. & Balkwill, F. R. Inflammation and cancer: advances and new agents. Nat. Rev. Clin. Oncol. 12, 584–596 (2015).
Li, A. V. et al. Generation of effector memory T cell-based mucosal and systemic immunity with pulmonary nanoparticle vaccination. Sci. Transl. Med. 5, 204ra130 (2013).
Nembrini, C. et al. Nanoparticle conjugation of antigen enhances cytotoxic T-cell responses in pulmonary vaccination. Proc. Natl Acad. Sci. USA 108, E989–E997 (2011).
Hanson, M. C. et al. Nanoparticulate STING agonists are potent lymph node-targeted vaccine adjuvants. J. Clin. Invest. 125, 2532–2546 (2015).
Luo, M. et al. A STING-activating nanovaccine for cancer immunotherapy. Nat. Nanotechnol. 12, 648–654 (2017).
Liu, H. et al. Structure-based programming of lymph-node targeting in molecular vaccines. Nature 507, 519–522 (2014). This study reveals that antigens and adjuvants can be efficiently delivered to lymph nodes by conjugating them to lipophilic albumin-binding tails using a polar linker that promotes solubility, thereby dramatically improving antitumour efficacy and markedly reducing systemic toxicity.
Kuai, R., Ochyl, L. J., Bahjat, K. S., Schwendeman, A. & Moon, J. J. Designer vaccine nanodiscs for personalized cancer immunotherapy. Nat. Mater. 16, 489–496 (2017).
Reddy, S. T. et al. Exploiting lymphatic transport and complement activation in nanoparticle vaccines. Nat. Biotechnol. 25, 1159–1164 (2007).
Wilson, J. T. A sweeter approach to vaccine design. Science 363, 584–585 (2019).
Tokatlian, T. et al. Innate immune recognition of glycans targets HIV nanoparticle immunogens to germinal centers. Science 363, 649–654 (2019).
Zhu, G., Zhang, F., Ni, Q., Niu, G. & Chen, X. Efficient nanovaccine delivery in cancer immunotherapy. ACS Nano 11, 2387–2392 (2017).
Pardi, N., Hogan, M. J., Porter, F. W. & Weissman, D. mRNA vaccines — a new era in vaccinology. Nat. Rev. Drug Discov. 17, 261–279 (2018).
Sahin, U., Karikó, K. & Türeci, Ö. mRNA-based therapeutics — developing a new class of drugs. Nat. Rev. Drug Discov. 13, 759–780 (2014).
Kranz, L. M. et al. Systemic RNA delivery to dendritic cells exploits antiviral defence for cancer immunotherapy. Nature 534, 396–401 (2016). This study illustrates that charge-optimized lipoparticles can efficiently deliver RNA to lymphoid organs and APCs in mice; the ability of this technique to effectively prime antigen-specific T cells was confirmed in patients with cancer.
Ramishetti, S. & Peer, D. Engineering lymphocytes with RNAi. Adv. Drug Deliv. Rev. https://doi.org/10.1016/j.addr.2018.12.002 (2018).
Moffett, H. F. et al. Hit-and-run programming of therapeutic cytoreagents using mRNA nanocarriers. Nat. Commun. 8, 389 (2017).
Junt, T. & Barchet, W. Translating nucleic acid-sensing pathways into therapies. Nat. Rev. Immunol. 15, 529–544 (2015).
Ribas, A. et al. SD-101 in combination with pembrolizumab in advanced melanoma: results of a phase Ib, multicenter study. Cancer Discov. 8, 1250–1257 (2018).
Corrales, L. et al. Direct activation of STING in the tumor microenvironment leads to potent and systemic tumor regression and immunity. Cell Rep. 11, 1018–1030 (2015).
Harrington, K. J. et al. Preliminary results of the first-in-human (FIH) study of MK-1454, an agonist of stimulator of interferon genes (STING), as monotherapy or in combination with pembrolizumab (pembro) in patients with advanced solid tumors or lymphomas [abstract LBA15]. Ann. Oncol. 29 (Suppl. 8) (2018).
Meric-Bernstam, F. et al. Phase I dose-finding study of MIW815 (ADU-S100), an intratumoral STING agonist, in patients with advanced solid tumors or lymphomas. Soc. Immunother. Cancer Abstr. 2018, 462-463 (SITC, 2018).
Luteijn, R. et al. SLC19A1 is a cyclic dinucleotide transporter. Preprint at bioRxiv https://www.biorxiv.org/content/10.1101/539767v1 (2019).
Ritchie, C., Cordova, A. F., Hess, G. T., Bassik, M. C. & Li, L. SLC19A1 is an importer of the immunotransmitter cGAMP. Mol. Cell https://doi.org/10.1016/j.molcel.2019.05.006 (2019).
Cheng, N. et al. A nanoparticle-incorporated STING activator enhances antitumor immunity in PD-L1–insensitive models of triple-negative breast cancer. JCI Insight 3, 120638 (2018).
Shae, D. et al. Endosomolytic polymersomes increase the activity of cyclic dinucleotide STING agonists to enhance cancer immunotherapy. Nat. Nanotechnol. 14, 269–278 (2019). This study demonstrates that rationally designed, multiblock, pH-sensitive polymersomes increase cytosolic delivery of cyclic dinucleotides, thereby enhancing antitumour immunity.
Jacobson, M. E., Wang-Bishop, L., Becker, K. W. & Wilson, J. T. Delivery of 5’-triphosphate RNA with endosomolytic nanoparticles potently activates RIG-I to improve cancer immunotherapy. Biomater. Sci. 7, 547–559 (2019).
Hornung, V. et al. 5’-triphosphate RNA is the ligand for RIG-I. Science 314, 994-997 (2006).
Spranger, S. & Gajewski, T. F. Impact of oncogenic pathways on evasion of antitumour immune responses. Nat. Rev. Cancer 18, 139–147 (2018).
Scheper, W. et al. Low and variable tumor reactivity of the intratumoral TCR repertoire in human cancers. Nat. Med. 25, 89–94 (2019).
Sagiv-Barfi, I. et al. Eradication of spontaneous malignancy by local immunotherapy. Sci. Transl. Med. 10, eaan4488 (2018).
Spitzer, M. H. et al. Systemic immunity is required for effective cancer immunotherapy. Cell 168, 487–502 (2017).
Marabelle, A. et al. Depleting tumor-specific Tregs at a single site eradicates disseminated tumors. J. Clin. Invest. 123, 2447–2463 (2013).
Predina, J. et al. Changes in the local tumor microenvironment in recurrent cancers may explain the failure of vaccines after surgery. Proc. Natl Acad. Sci. USA 110, E415–E424 (2013).
Horowitz, M., Neeman, E., Sharon, E. & Ben-Eliyahu, S. Exploiting the critical perioperative period to improve long-term cancer outcomes. Nat. Rev. Clin. Oncol. 12, 213–226 (2015).
Krall, J. A. et al. The systemic response to surgery triggers the outgrowth of distant immune-controlled tumors in mouse models of dormancy. Sci. Transl. Med. 10, eaan3464 (2018).
Hiller, J. G., Perry, N. J., Poulogiannis, G., Riedel, B. & Sloan, E. K. Perioperative events influence cancer recurrence risk after surgery. Nat. Rev. Clin. Oncol. 15, 205–218 (2018).
Hugo, W. et al. Genomic and transcriptomic features of response to anti-PD-1 therapy in metastatic melanoma. Cell 165, 35–44 (2016).
Wang, C. et al. In situ activation of platelets with checkpoint inhibitors for post-surgical cancer immunotherapy. Nat. Biomed. Eng. 1, 1–10 (2017).
Stephan, S. B. et al. Biopolymer implants enhance the efficacy of adoptive T-cell therapy. Nat. Biotechnol. 33, 97–101 (2015).
Smith, T. T. et al. Biopolymers codelivering engineered T cells and STING agonists can eliminate heterogeneous tumors. J. Clin. Invest. 127, 2176–2191 (2017).
Chen, Q. et al. In situ sprayed bioresponsive immunotherapeutic gel for post-surgical cancer treatment. Nat. Nanotechnol. 14, 89–97 (2019).
Tseng, D. et al. Anti-CD47 antibody-mediated phagocytosis of cancer by macrophages primes an effective antitumor T-cell response. Proc. Natl Acad. Sci. USA 110, 11103–11108 (2013).
Park, C. G. et al. Extended release of perioperative immunotherapy prevents tumor recurrence and eliminates metastases. Sci. Transl. Med. 10, eaar1916 (2018). This study shows that reprogramming the post-resection milieu from immunosuppressive to immunostimulatory not only prevents local recurrence but also eradicates disseminated disease, and that sustaining drug exposure locally is required in order to achieve a durable survival benefit.
Kim, K. et al. Eradication of metastatic mouse cancers resistant to immune checkpoint blockade by suppression of myeloid-derived cells. Proc. Natl Acad. Sci. USA 111, 11774–11779 (2014).
Moynihan, K. D. et al. Eradication of large established tumors in mice by combination immunotherapy that engages innate and adaptive immune responses. Nat. Med. 22, 1402–1410 (2016).
US National Library of Medicine. ClinicalTrials.gov https://clinicaltrials.gov/ct2/show/NCT03815682 (2019).
Tang, L. et al. Enhancing T cell therapy through TCR-signaling-responsive nanoparticle drug delivery. Nat. Biotechnol. 36, 707-716 (2018). This study reveals that cytokines can be conjugated to the surface of T cells using a reversible crosslinker that enables triggered release of native protein in the context of TCR activation, and that adoptive transfer of such ‘backpacked’ cells confers antitumour responses vastly superior to those from unmodified cells plus free cytokine.
Milhem, M. et al. Intratumoral toll-like receptor 9 (TLR9) agonist, CMP-001, in combination with pembrolizumab can reverse resistance to PD-1 inhibition in a phase Ib trial in subjects with advanced melanoma [abstract CT144]. Cancer Res. 78 (13 Suppl.) (2018).
US National Library of Medicine. ClinicalTrials.gov https://clinicaltrials.gov/ct2/show/NCT03086278 (2019).
Radovic-Moreno, A. F. et al. Immunomodulatory spherical nucleic acids. Proc. Natl Acad. Sci. USA 112, 3892–3897 (2015).
US National Library of Medicine. ClinicalTrials.gov https://clinicaltrials.gov/ct2/show/NCT02410733 (2019).
US National Library of Medicine. ClinicalTrials.gov https://clinicaltrials.gov/ct2/show/NCT01753089 (2019).
Ali, O. A., Emerich, D., Dranoff, G. & Mooney, D. J. In situ regulation of DC subsets and T cells mediates tumor regression in mice. Sci. Transl. Med. 1, 8ra19 (2009).
Bencherif, S. A. et al. Injectable cryogel-based whole-cell cancer vaccines. Nat. Commun. 6, 7556 (2015).
Kim, J. et al. Injectable, spontaneously assembling, inorganic scaffolds modulate immune cells in vivo and increase vaccine efficacy. Nat. Biotechnol. 33, 64–72 (2015).
Nature Collection: Nobel Prize in Physiology or Medicine 2018, https://www.nature.com/collections/gqznlfngkz (2018).
Zheng, Y., Tang, L., Mabardi, L., Kumari, S. & Irvine, D. J. Enhancing adoptive cell therapy of cancer through targeted delivery of small-molecule immunomodulators to internalizing or noninternalizing receptors. ACS Nano 11, 3089–3100 (2017).
Editorial. Time to deliver. Nat. Biotechnol. 961, 10 (2014).
Kim, S., Shah, S. B., Graney, P. L. & Singh, A. Multiscale engineering of immune cells and lymphoid organs. Nat. Rev. Mater. 4, 355–378 (2019).
Gosselin, E. A., Eppler, H. B., Bromberg, J. S. & Jewell, C. M. Designing natural and synthetic immune tissues. Nat. Mater. 17, 484–498 (2018).
Dura, B. et al. Profiling lymphocyte interactions at the single-cell level by microfluidic cell pairing. Nat. Commun. 6, 5940 (2015).
Jain, R. K., Martin, J. D. & Stylianopoulos, T. The role of mechanical forces in tumor growth and therapy. Annu. Rev. Biomed. Eng. 16, 321–346 (2014).
Huse, M. Mechanical forces in the immune system. Nat. Rev. Immunol. 17, 679–690 (2017).
Jenkins, R. W. et al. Ex vivo profiling of PD-1 blockade using organotypic tumor spheroids. Cancer Discov. 8, 196–215 (2018).
Muraro, M. G. et al. Ex-vivo assessment of drug response on breast cancer primary tissue with preserved microenvironments. Oncoimmunology 6, e1331798 (2017).
Angelo, M. et al. Multiplexed ion beam imaging of human breast tumors. Nat. Med. 20, 436–442 (2014).
Keren, L. et al. A structured tumor-immune microenvironment in triple negative breast cancer revealed by multiplexed ion beam imaging. Cell 174, 1373–1387 (2018). This study demonstrates that novel technologies can be applied in order to elucidate spatial relationships and features in the context of human tumour tissue, providing insights into patient stratification.
Lin, J. R., Fallahi-Sichani, M. & Sorger, P. K. Highly multiplexed imaging of single cells using a high-throughput cyclic immunofluorescence method. Nat. Commun. 6, 8390 (2015).
Lin, J. R. et al. Highly multiplexed immunofluorescence imaging of human tissues and tumors using t-CyCIF and conventional optical microscopes. eLife 7, e31657 (2018).
Weiden, J., Tel, J. & Figdor, C. G. Synthetic immune niches for cancer immunotherapy. Nat. Rev. Immunol. 18, 212–219 (2018).
Kobayashi, Y. & Watanabe, T. Gel-trapped lymphorganogenic chemokines trigger artificial tertiary lymphoid organs and mount adaptive immune responses in vivo. Front. Immunol. 7, 316 (2016).
Fan, Y. et al. Bioengineering thymus organoids to restore thymic function and induce donor-specific immune tolerance to allografts. Mol. Ther. 23, 1262–1277 (2015).
Reinisch, A. et al. A humanized bone marrow ossicle xenotransplantation model enables improved engraftment of healthy and leukemic human hematopoietic cells. Nat. Med. 22, 812–821 (2016).
Shah, N. J. et al. An injectable bone marrow-like scaffold enhances T cell immunity after hematopoietic stem cell transplantation. Nat. Biotechnol. 37, 293–302 (2019). This study illustrates that a scaffold can be used to release factors that promote the recruitment of specific cells and induce differentiation of progenitor cells to particular lineages, underscoring the utility of macroscale devices that can establish defined niches to program immunity in situ.
Rothschilds, A. et al. Order of administration of combination cytokine therapies can decouple toxicity from efficacy in syngeneic mouse tumor models. Oncoimmunology 8, e1558678 (2019).
Messenheimer, D. J. et al. Timing of PD-1 blockade is critical to effective combination immunotherapy with anti-OX40. Clin. Cancer Res. 23, 6165–6177 (2017).
Rothschilds, A. M. & Wittrup, K. D. What, why, where, and when: bringing timing to immuno-oncology. Trends Immunol. 40, 12–21 (2019).
Goldberg, M. S. Immunoengineering: how nanotechnology can enhance cancer immunotherapy. Cell 161, 201–204 (2015).
Bartlett, D. W., Su, H., Hildebrandt, I. J., Weber, W. A. & Davis, M. E. Impact of tumor-specific targeting on the biodistribution and efficacy of siRNA nanoparticles measured by multimodality in vivo imaging. Proc. Natl Acad. Sci. USA 104, 15549–15554 (2007).
Grivennikov, S. I., Greten, F. R. & Karin, M. Immunity, inflammation, cancer. Cell 140, 883–899 (2010).
Xie, Y. Q. et al. Redox-responsive interleukin-2 nanogel specifically and safely promotes the proliferation and memory precursor differentiation of tumor-reactive T-cells. Biomater Sci. 7, 1345–1357 (2019).
Wang, H. & Mooney, D. J. Biomaterial-assisted targeted modulation of immune cells in cancer treatment. Nat. Mater. 17, 761–772 (2018).
Liebers, R. & Jager, D. Surgical wound immunotherapy. Nat. Nanotechnol. 14, 7–8 (2019).
Acknowledgements
The author thanks W. Rindler for helpful comments.
Author information
Authors and Affiliations
Corresponding author
Additional information
Peer review information
Nature Reviews Cancer thanks J. T. Wilson, J. Tel and the other, anonymous, reviewer for their contribution to the peer review of this work.
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Glossary
- Therapeutic index
-
The ratio of efficacy to safety, which compares the amount of a drug that produces the therapeutic effect to the amount that causes toxicity.
- Immune tolerance
-
A state of unresponsiveness by the immune system to antigens that allows for discrimination of self from non-self and is inappropriately fostered by tumours.
- Area under the curve
-
(AUC). A pharmacokinetic parameter that represents total drug exposure by describing a quantitative relationship between drug concentration in the blood and time.
- Immunoengineering
-
A burgeoning field that incorporates the tools and approaches of bioengineering, materials science, nanotechnology, drug delivery and immunology to influence the immune system — particularly, to elicit robust antitumour immune responses — in a manner not achieved by the administration of the same molecules in solution.
- Pattern recognition receptors
-
Host sensors that can detect molecules associated with pathogens and/or cellular damage, thus inducing innate immunity, typically through the production of pro-inflammatory cytokines.
- Liposomes
-
Spherical vesicles composed of at least one lipid bilayer that are often used to entrap and deliver therapeutics.
- Enhanced permeability and retention
-
(EPR). A proposed effect that suggests that molecules and particles of a certain size concentrate in tumours more so than in other tissues, owing to the leaky vasculature and poor lymphatic drainage of solid tumours.
- Mesoporous silica rods
-
A biomaterial that exhibits a high aspect ratio, enabling spontaneous assembly to form a three-dimensional microenvironment for host immune cells.
- Synthetic biology
-
An intersection of biotechnology and molecular biology in which biological modules and systems are devised and created, with a particular emphasis on the incorporation of logic gates and other computer-like operations involving inputs, signal integration and outputs.
- Lyophilization
-
Also known as freeze drying, a process in which water is removed from a sample under vacuum via sublimation following freezing.
- Adjuvant
-
A molecule that augments immune responses to antigens (for example, Toll-like receptor agonists).
- Neoantigens
-
An antigen that is created by a gene fusion or somatic mutation.
- Nanodiscs
-
Structures comprising a lipid bilayer and amphipathic membrane-stabilizing proteins.
- Immunogens
-
Antigens that are immunogenic, provoking a cellular and/or humoral immune response.
- Aptamer
-
An oligonucleotide, typically identified through in vitro selection, that binds to a target of interest.
- Cyclic dinucleotide pharmacophores
-
Molecular structures defined by a closed ring comprising two nucleotides that are recognized by the innate immune pattern recognition receptor stimulator of interferon genes (STING).
- Polymersomes
-
Polymeric analogues of liposomes that can serve as an artificial vesicle to entrap drug-containing solutions, often affording greater control over particle stability and drug release rate.
- Block copolymer
-
A polymer comprising two or more homopolymer blocks, connected via covalent bonds, that can confer blended or combined properties of the individual blocks.
- Nanogels
-
Nanoparticulate forms of a hydrogel (a crosslinked hydrophilic polymer network).
- Mass cytometry
-
Also known as cytometry by time of flight (CyTOF), a mass spectrometry-based variation of flow cytometry in which antibodies are labelled with heavy metal ions that have discrete masses, rather than with fluorophores that can have spectral overlap.
Rights and permissions
About this article
Cite this article
Goldberg, M.S. Improving cancer immunotherapy through nanotechnology. Nat Rev Cancer 19, 587–602 (2019). https://doi.org/10.1038/s41568-019-0186-9
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41568-019-0186-9
This article is cited by
-
NIR-II responsive Janus nanoparticles amplify immunogenic cell death for enhanced cancer immunotherapy
Science China Technological Sciences (2024)
-
A holistic review of recent advances in nano-based drug delivery systems for the treatment of triple-negative breast cancer (TNBC)
Journal of Nanoparticle Research (2024)
-
Therapeutic applications of nanobiotechnology
Journal of Nanobiotechnology (2023)
-
Nanobiomaterials: exploring mechanistic roles in combating microbial infections and cancer
Discover Nano (2023)
-
Nanomedicine-based adjuvant therapy: a promising solution for lung cancer
Journal of Nanobiotechnology (2023)