Abstract
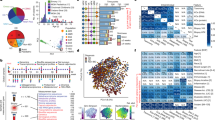
Recent work has highlighted the importance of confounder control in microbiome association studies1,2. For instance, multiple pathologies previously linked to gut ecosystem dysbiosis display concomitant changes in stool consistency3,4,5,6, a major covariate of microbiome variation2,7. In those cases, observed microbiota alterations could largely reflect variation in faecal water content. Moreover, stool moisture variation has been linked to fluctuations in faecal microbial load, inducing artefacts in relative abundance profile analyses8,9. Hence, the identification of associations between the gut microbiota and specific disease manifestations in pathologies with complex aetiologies requires a deconfounded, quantitative assessment of microbiome variation. Here, we revisit a disease association microbiome data set comprising 106 patients with primary sclerosing cholangitis (PSC) and/or inflammatory bowel disease10. Assessing quantitative taxon abundances9, we study microbiome alterations beyond symptomatic stool moisture variation. We observe an increased prevalence of a low cell count Bacteroides 2 enterotype across the pathologies studied, with microbial loads correlating inversely with intestinal and systemic inflammation markers. Quantitative analyses allow us to differentiate between taxa associated with either intestinal inflammation severity (Fusobacterium) or cholangitis/biliary obstruction (Enterococcus) among previously suggested PSC marker genera. We identify and validate a near-exclusion pattern between the inflammation-associated Fusobacterium and Veillonella genera, with Fusobacterium detection being restricted to Crohn’s disease and patients with PSC–Crohn’s disease. Overall, through absolute quantification and confounder control, we single out clear-cut microbiome markers associated with pathophysiological manifestations and disease diagnosis.
This is a preview of subscription content, access via your institution
Access options
Access Nature and 54 other Nature Portfolio journals
Get Nature+, our best-value online-access subscription
$29.99 / 30 days
cancel any time
Subscribe to this journal
Receive 12 digital issues and online access to articles
$119.00 per year
only $9.92 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout



Similar content being viewed by others
Data availability
Raw amplicon sequencing data that support the findings of this study have been deposited at the European Genome-phenome Archive (EGA), with accession no. EGAS00001003600. The genus-level QMP matrix can be downloaded at http://raeslab.org/software/QMP2/.
Code availability
The R code used to compute QMPs can be found at https://github.com/raeslab/QMP/.
References
Zhernakova, A. et al. Population-based metagenomics analysis reveals markers for gut microbiome composition and diversity. Science 352, 565–569 (2016).
Falony, G. et al. Population-level analysis of gut microbiome variation. Science 352, 560–564 (2016).
Knudsen, K. et al. Gastrointestinal transit time in Parkinson’s disease using a magnetic tracking system. J. Park. Dis. 7, 471–479 (2017).
Frøslie, K. F., Jahnsen, J., Moum, B. A. & Vatn, M. H. Mucosal healing ininflammatory bowel disease: results from a Norwegian population-based cohort. Gastroenterology 133, 412–422 (2007).
Krishnan, B., Babu, S., Walker, J., Walker, A. B. & Pappachan, J. M. Gastrointestinal complications of diabetes mellitus. World J. Diabetes 4, 51–63 (2013).
Probert, C. S., Emmett, P. M. & Heaton, K. W. Some determinants of whole-gut transit time: a population-based study. QJM 88, 311–315 (1995).
Vandeputte, D. et al. Stool consistency is strongly associated with gut microbiota richness and composition, enterotypes and bacterial growth rates. Gut 65, 57–62 (2016).
Gloor, G. B., Macklaim, J. M., Pawlowsky-Glahn, V. & Egozcue, J. J. Microbiome datasets are compositional: and this is not optional. Front. Microbiol. 8, 2224 (2017).
Vandeputte, D. et al. Quantitative microbiome profiling links gut community variation to microbial load. Nature 551, 507–511 (2017).
Sabino, J. et al. Primary sclerosing cholangitis is characterised by intestinal dysbiosis independent from IBD. Gut 65, 1681–1689 (2016).
Baumgart, D. C. & Carding, S. R. Inflammatory bowel disease: cause and immunobiology. Lancet 369, 1627–1640 (2007).
Hirschfield, G. M., Karlsen, T. H., Lindor, K. D. & Adams, D. H. Primary sclerosing cholangitis. Lancet 382, 1587–1599 (2013).
Hov, J. R. & Kummen, M. Intestinal microbiota in primary sclerosing cholangitis. Curr. Opin. Gastroenterol. 33, 85–92 (2017).
Holmes, I., Harris, K. & Quince, C. Dirichlet multinomial mixtures: generative models for microbial metagenomics. PLoS ONE 7, e30126 (2012).
Ding, T. & Schloss, P. D. Dynamics and associations of microbial community types across the human body. Nature 509, 357–360 (2014).
Falony, G., Vieira-Silva, S. & Raes, J. Richness and ecosystem development across faecal snapshots of the gut microbiota. Nat. Microbiol. 3, 526–528 (2018).
Shah, S. B. & Hanauer, S. B. Treatment of diarrhea in patients with inflammatory bowel disease: concepts and cautions. Rev. Gastroenterol. Disord. 7, S3–S10 (2007).
Kostic, A. D. et al. Fusobacterium nucleatum potentiates intestinal tumorigenesis and modulates the tumor-immune microenvironment. Cell Host Microbe 14, 207–215 (2013).
van den Bogert, B., Meijerink, M., Zoetendal, E. G., Wells, J. M. & Kleerebezem, M. Immunomodulatory properties of Streptococcus and Veillonella isolates from the human small intestine microbiota. PLoS ONE 9, e114277 (2014).
Zhou, P., Li, X., Huang, I.-H. & Qi, F. Veillonella catalase protects the growth of Fusobacterium nucleatum in microaerophilic and Streptococcus gordonii-resident environments. Appl. Environ. Microbiol. 83, e01079-17 (2017).
Pohl, J., Ring, A., Stremmel, W. & Stiehl, A. The role of dominant stenoses in bacterial infections of bile ducts in primary sclerosing cholangitis. Eur. J. Gastroenterol. Hepatol. 18, 69–74 (2006).
Michaux, C. et al. SlyA is a transcriptional regulator involved in the virulence of Enterococcus faecalis. Infect. Immun. 79, 2638–2645 (2011).
Dignass, A. et al. Second European evidence-based consensus on the diagnosis and management of ulcerative colitis part 1: definitions and diagnosis. J. Crohns Colitis 6, 965–990 (2012).
Van Assche, G. et al. The second European evidence-based consensus on the diagnosis and management of Crohn’s disease: definitions and diagnosis. J. Crohns Colitis 4, 7–27 (2010).
Lindor, K. D., Kowdley, K. V. & Harrison, M. E. ACG Clinical Guideline: primary sclerosing cholangitis. Am. J. Gastroenterol. 110, 646–659 (2015).
Prest, E. I., Hammes, F., Kötzsch, S., van Loosdrecht, M. C. M. & Vrouwenvelder, J. S. Monitoring microbiological changes in drinking water systems using a fast and reproducible flow cytometric method. Water Res. 47, 7131–7142 (2013).
Kozich, J. J., Westcott, S. L., Baxter, N. T., Highlander, S. K. & Schloss, P. D. Development of a dual-index sequencing strategy and curation pipeline for analyzing amplicon sequence data on the MiSeq Illumina sequencing platform. Appl. Environ. Microbiol. 79, 5112–5120 (2013).
Magoč, T. & Salzberg, S. L. FLASH: fast length adjustment of short reads to improve genome assemblies. Bioinformatics 27, 2957–2963 (2011).
Edgar, R. C., Haas, B. J., Clemente, J. C., Quince, C. & Knight, R. UCHIME improves sensitivity and speed of chimera detection. Bioinformatics 27, 2194–2200 (2011).
Tito, R. Y. et al. Brief report: daialister as a microbial marker of disease activity in spondyloarthritis. Arthritis Rheumatol. 69, 114–121 (2017).
Callahan, B. J. et al. DADA2: high-resolution sample inference from Illumina amplicon data. Nat. Methods 13, 581–583 (2016).
Wang, Q., Garrity, G. M., Tiedje, J. M. & Cole, J. R. Naive Bayesian classifier for rapid assignment of rRNA sequences into the new bacterial taxonomy. Appl. Environ. Microbiol. 73, 5261–5267 (2007).
Stoddard, S. F., Smith, B. J., Hein, R., Roller, B. R. K. & Schmidt, T. M. rrnDB: improved tools for interpreting rRNA gene abundance in bacteria and archaea and a new foundation for future development. Nucleic Acids Res. 43, D593–D598 (2015).
Dereeper, A. et al. Phylogeny.fr: robust phylogenetic analysis for the non-specialist. Nucleic Acids Res. 36, W465–W469 (2008).
Oksanen, J. et al. vegan: community ecology package. R package version 2.2-1 https://CRAN.R-project.org/package=vegan (2015).
McMurdie, P. J. & Holmes, S. phyloseq: an R package for reproducible interactive analysis and graphics of microbiome census data. PLoS ONE 8, e61217 (2013).
Ogle, D. H. FSA: fisheries stock analysis. R package version 0.8.13 https://github.com/droglenc/FSA (2017).
Hothorn, T., Hornik, K., van de Wiel, M. A. & Zeileis, A. A Lego system for conditional inference. Am. Stat. 60, 257–263 (2006).
Morgan, M. DirichletMultinomial: Dirichlet-multinomial mixture model machine learning for microbiome data. R package version 1.18.0 http://bioconductor.org/packages/DirichletMultinomial/ (2017).
Delignette-Muller, M. & Dutang, C. fitdistrplus: an R package for fitting distributions. J. Stat. Softw. 64, 1–34 (2015).
Acknowledgements
We thank all study participants for their valuable contribution. We thank K. Verbeke for facilitating moisture content determinations. The development of QMP analysis was funded by a KU Leuven CREA grant. S.V.-S., G.K. and M.V.-C. were supported by a (post-)doctoral fellowship from the Research Foundation Flanders (FWO Vlaanderen). S.V. and S.v.d.M. are Senior Clinical Researchers of the FWO Vlaanderen. This work was co-funded by VIB, the Rega Institute for Medical Research, KU Leuven, the FWO EOS program (30770923), FP7 METACARDIS (305312) and H2020 SYSCID (733100).
Author information
Authors and Affiliations
Contributions
This study was conceived by J.S., S.V. and J.R. Experiments were designed by J.S., G.F. and J.R. Sampling of the different cohorts was set up and carried out by J.S., S.v.d.M., S.V.-S., C.C. and G.F. Experiments were performed by J.S. (calprotectin measurements), G.K. (flow cytometry analysis and moisture content) and C.C. (QMP analysis of the validation cohort). Statistical analyses were planned and executed by J.S., S.V.-S., M.V.-C., I.C. and G.F. S.V.-S., G.F., S.V. and J.R. drafted the manuscript. All authors revised the article and approved the final version for publication.
Corresponding authors
Ethics declarations
Competing interests
J.R., S.V., S.V.-S., J.S., M.V.-C., G.F. and G.K. are inventors on the patent application PCT/EP2018/084920 in the name of VIB VZW, Katholieke Universiteit Leuven, KU Leuven R&D and Vrije Universiteit Brussel covering the microbiome features associated with inflammation described in this article.
Additional information
Publisher’s note: Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Supplementary Information
Supplementary Figs. 1–9, Supplementary Table legends.
Supplementary Data 1
Supplementary Tables 1–11.
Rights and permissions
About this article
Cite this article
Vieira-Silva, S., Sabino, J., Valles-Colomer, M. et al. Quantitative microbiome profiling disentangles inflammation- and bile duct obstruction-associated microbiota alterations across PSC/IBD diagnoses. Nat Microbiol 4, 1826–1831 (2019). https://doi.org/10.1038/s41564-019-0483-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41564-019-0483-9
This article is cited by
-
Cluster-specific associations between the gut microbiota and behavioral outcomes in preschool-aged children
Microbiome (2024)
-
The gut-liver axis in hepatobiliary diseases
Inflammation and Regeneration (2024)
-
Functional host-specific adaptation of the intestinal microbiome in hominids
Nature Communications (2024)
-
Microbiome confounders and quantitative profiling challenge predicted microbial targets in colorectal cancer development
Nature Medicine (2024)
-
Research progress of ferroptosis and inflammatory bowel disease
BioMetals (2024)